Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
3 viewsEN + Eosinofilia
EN + Eosinofilia
Uploaded by
Ana Flavia BaptistaCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You might also like
- Risk Factors & Prognosis For USMLE STEP 3 PDFDocument182 pagesRisk Factors & Prognosis For USMLE STEP 3 PDFSadia GhaniNo ratings yet
- Color Atlas of Pediatrics PDFDocument1,399 pagesColor Atlas of Pediatrics PDFJose Guaman100% (10)
- 2 Step Dermoscopedia SmallDocument4 pages2 Step Dermoscopedia SmallAndreea Barbuta100% (2)
- Dermoscopy Pathology Correlation in MelanomaDocument8 pagesDermoscopy Pathology Correlation in MelanomaDaniela SerbanNo ratings yet
- Disease Cheat SheetDocument393 pagesDisease Cheat Sheetjhk0428100% (1)
- 04.the Cleveland Clinic Intensive Review of Pediatrics 2nd EdDocument513 pages04.the Cleveland Clinic Intensive Review of Pediatrics 2nd EdSav GaNo ratings yet
- Lucivero Et Al 2011 Lupus Mastitis in Systemic Lupus Erythematosus A Rare Condition Requiring A Minimally InvasiveDocument5 pagesLucivero Et Al 2011 Lupus Mastitis in Systemic Lupus Erythematosus A Rare Condition Requiring A Minimally Invasiveruthdaniel6041No ratings yet
- Somorin SsDocument8 pagesSomorin SsChikezie OnwukweNo ratings yet
- Abstract: Kimura Disease Is A Rare Form of Chronic Inflammatory Disorder InvolvingDocument4 pagesAbstract: Kimura Disease Is A Rare Form of Chronic Inflammatory Disorder InvolvingpriyokNo ratings yet
- Hypopituitarism in Langerhans Cell Histiocytosis Seven Cases and Literature ReviewDocument8 pagesHypopituitarism in Langerhans Cell Histiocytosis Seven Cases and Literature ReviewafdtfngqbNo ratings yet
- Tsai (2007) - NSDocument2 pagesTsai (2007) - NSIlma ArifaniNo ratings yet
- Pi Is 0190962214011566Document2 pagesPi Is 0190962214011566LewishoppusNo ratings yet
- Bizkova 2009Document8 pagesBizkova 2009mario256No ratings yet
- UntitledDocument3 pagesUntitledShintaNo ratings yet
- PIIS0008418219302121Document4 pagesPIIS0008418219302121J MNo ratings yet
- Zoon's Plasma Cell Balanitis Associated With Male Genital Lichen SclerosusDocument4 pagesZoon's Plasma Cell Balanitis Associated With Male Genital Lichen SclerosusMircea-Dan Apopei-RusuNo ratings yet
- Lichenoid Skin Lesions - A Rare Manifestation in Secondary SyphilisDocument3 pagesLichenoid Skin Lesions - A Rare Manifestation in Secondary SyphilisShintaNo ratings yet
- Kikuchi' S Disease of The Mesenteric Lymph Nodes Presenting As Acute AppendicitisDocument3 pagesKikuchi' S Disease of The Mesenteric Lymph Nodes Presenting As Acute AppendicitisZulfikar Adi GumawangNo ratings yet
- Congenital Scalp Tumor With Ulceration: Jeremy Udkoff MA, MAS - Ralph E. Holmes MD - Magdalene A. Dohil MDDocument2 pagesCongenital Scalp Tumor With Ulceration: Jeremy Udkoff MA, MAS - Ralph E. Holmes MD - Magdalene A. Dohil MDAna MariaNo ratings yet
- Jcad 6 8 23Document6 pagesJcad 6 8 23Hadi FirmansyahNo ratings yet
- Phleboliths and The Vascular Maxillofacial LesionDocument4 pagesPhleboliths and The Vascular Maxillofacial LesionVinay KumarNo ratings yet
- Kikuchi's Disease: Malathi Sathiyasekaran R. Varadharajan So. ShivbalanDocument3 pagesKikuchi's Disease: Malathi Sathiyasekaran R. Varadharajan So. Shivbalanzulfikar adiNo ratings yet
- J Clin Pathol 1980 Brook 1099 101Document4 pagesJ Clin Pathol 1980 Brook 1099 101ysh_girlNo ratings yet
- Cutaneous Polyarteritis Nodosa in A Child FollowinDocument2 pagesCutaneous Polyarteritis Nodosa in A Child FollowinandresrogersNo ratings yet
- Prurigo Nodularis of HydeDocument12 pagesPrurigo Nodularis of HydeAugusto MonjardimNo ratings yet
- Iaet 12 I 2 P 135Document2 pagesIaet 12 I 2 P 135leonjunchan_66965707No ratings yet
- Brar (2007) - NS Resemples Lymphoreticular ProcessDocument2 pagesBrar (2007) - NS Resemples Lymphoreticular ProcessIlma ArifaniNo ratings yet
- (2017) BELOUSOVA, Irena E. Mycosis Fungoides Manifesting As Giant Cell Lichenoid DermatitisDocument3 pages(2017) BELOUSOVA, Irena E. Mycosis Fungoides Manifesting As Giant Cell Lichenoid DermatitisCassandra VérasNo ratings yet
- Cancer de Testiculo e Down 2Document4 pagesCancer de Testiculo e Down 2paulinhamericoNo ratings yet
- Sarcoidosis (Heerfordt Syndrome) : A Case Report: Tiia Tamme, Edvitar Leibur, Andres KullaDocument4 pagesSarcoidosis (Heerfordt Syndrome) : A Case Report: Tiia Tamme, Edvitar Leibur, Andres KullajaquelineartNo ratings yet
- Yayli (2013) - NS Resembles KaposiDocument3 pagesYayli (2013) - NS Resembles KaposiIlma ArifaniNo ratings yet
- Eosinophilic Cellulitis Arch Arg PediatrDocument5 pagesEosinophilic Cellulitis Arch Arg PediatrElianaNo ratings yet
- 108 Orbitorhinocerebral MucormycosisDocument10 pages108 Orbitorhinocerebral MucormycosisrgumralNo ratings yet
- A Case of Pemphigus Vulgaris Associated With Ulcerative ColitisDocument4 pagesA Case of Pemphigus Vulgaris Associated With Ulcerative ColitisfakhmiyogiiNo ratings yet
- Extraordinary Case Unique Presentation of EBVmucocutaneousulcerDocument4 pagesExtraordinary Case Unique Presentation of EBVmucocutaneousulcerRogério Ramos MarquesNo ratings yet
- ScrofulodermDocument4 pagesScrofulodermIzmi AzizahNo ratings yet
- Masquerade SyndromesDocument10 pagesMasquerade Syndromestony_chrisNo ratings yet
- 18 Extra-GuptaNDocument3 pages18 Extra-GuptaNGalih rarang gatiNo ratings yet
- Acne Urticata Associated With Chronic Myelogenous Leukemia: of Be of ofDocument4 pagesAcne Urticata Associated With Chronic Myelogenous Leukemia: of Be of ofGo McFlyNo ratings yet
- Reversal Reaction With Nodules That Initially Diagnosed As Erythema Nodosum Leprosum in Borderline Lepromatous LeprosyDocument6 pagesReversal Reaction With Nodules That Initially Diagnosed As Erythema Nodosum Leprosum in Borderline Lepromatous Leprosysilvavitria mandenasNo ratings yet
- Case Report: Langerhans Cell Histiocytosis of The Mandible in A Six-Year-Old ChildDocument0 pagesCase Report: Langerhans Cell Histiocytosis of The Mandible in A Six-Year-Old ChildElvina Agnestin HarianjaNo ratings yet
- Dermoscopy of Necrobiosis LipoidicaDocument4 pagesDermoscopy of Necrobiosis LipoidicaAndrés WunderwaldNo ratings yet
- Kimura DiseaseDocument4 pagesKimura DiseasewitariNo ratings yet
- Case Report: Subcorneal Pustular Dermatosis in Childhood: A Case Report and Review of The LiteratureDocument6 pagesCase Report: Subcorneal Pustular Dermatosis in Childhood: A Case Report and Review of The LiteratureIrsalinaHusnaAzwirNo ratings yet
- Scrofuloderma: A Common Type of Cutaneous Tuberculosis. A Case ReportDocument5 pagesScrofuloderma: A Common Type of Cutaneous Tuberculosis. A Case ReportIndah IndrianiNo ratings yet
- 2006 Gosche Vick SemPedSurgeryDocument8 pages2006 Gosche Vick SemPedSurgeryResya I. NoerNo ratings yet
- Primary Conjunctival Tuberculosis-2Document3 pagesPrimary Conjunctival Tuberculosis-2puutieNo ratings yet
- Cerebellopontine Angle Epidermoid CYST: Case ReportDocument3 pagesCerebellopontine Angle Epidermoid CYST: Case ReportTamajyoti GhoshNo ratings yet
- Liken PlanusDocument6 pagesLiken PlanusAmirahShalehaNo ratings yet
- Parakeratosis Variegata: A Possible Role of Environmental Hazards?Document4 pagesParakeratosis Variegata: A Possible Role of Environmental Hazards?Ega AihenaNo ratings yet
- Pi Is 0190962208009328Document2 pagesPi Is 0190962208009328Nabhya MaheshwariNo ratings yet
- Art Acta - Neurol.belgicaDocument6 pagesArt Acta - Neurol.belgicaAna GabrielaNo ratings yet
- Rare Cases in ENTDocument5 pagesRare Cases in ENTshadia sameerNo ratings yet
- AD1110894Document5 pagesAD1110894dhawalduvey95No ratings yet
- Papuloerythroderma of Ofuji - A Case ReportDocument4 pagesPapuloerythroderma of Ofuji - A Case ReportLidwina ApyakaNo ratings yet
- Early - Stage Hodgkins Lymphoma in A Child A CaseDocument6 pagesEarly - Stage Hodgkins Lymphoma in A Child A CaseХарш Навнітбхаі НімаватNo ratings yet
- Ecthyma Contagiosum (Human Orf)Document2 pagesEcthyma Contagiosum (Human Orf)Deba P SarmaNo ratings yet
- Aimee - Cutaneous and Systemic PlasmacytosisDocument3 pagesAimee - Cutaneous and Systemic PlasmacytosisEva YustianaNo ratings yet
- Human OrfDocument3 pagesHuman OrfDeba P SarmaNo ratings yet
- 2011 Ulcerated Cutaneous Epithelioid Hemangioendothelioma in An 8-Month Old InfantDocument2 pages2011 Ulcerated Cutaneous Epithelioid Hemangioendothelioma in An 8-Month Old InfantpsicobastoNo ratings yet
- JournalDocument5 pagesJournalgabbynengNo ratings yet
- Ring B Lymphoma B Highly Indicat Source Graefes Arch Clin Exp Ophthalmol 2021 Mar 2 Doi 10 1007 s00417 021 05075 6 Online Ahead of PrintDocument4 pagesRing B Lymphoma B Highly Indicat Source Graefes Arch Clin Exp Ophthalmol 2021 Mar 2 Doi 10 1007 s00417 021 05075 6 Online Ahead of Print381098891No ratings yet
- Calvarial Tuberculosis: E Ünüvar, F O Guz, B Sadiko Glu, M Sidal, Ü One S and S TetikkurtDocument2 pagesCalvarial Tuberculosis: E Ünüvar, F O Guz, B Sadiko Glu, M Sidal, Ü One S and S Tetikkurtkbianca26No ratings yet
- Diagnosis in OncologyDocument22 pagesDiagnosis in OncologyAndi SuryajayaNo ratings yet
- Lethal Midline Granuloma Importance of Early Diagnosis: A Case ReportDocument0 pagesLethal Midline Granuloma Importance of Early Diagnosis: A Case ReportdeolukmanaNo ratings yet
- (Download PDF) Dermatoscopy A Z 1St Edition Aimilios Lallas Online Ebook All Chapter PDFDocument42 pages(Download PDF) Dermatoscopy A Z 1St Edition Aimilios Lallas Online Ebook All Chapter PDFsusan.brown255100% (12)
- Multiple Skin Neoplasms at One Site MUSK IN A NEST A Comprehensive Review of Basal Cell Carcinoma and Benign or Malignant Collision Tumors at TheDocument12 pagesMultiple Skin Neoplasms at One Site MUSK IN A NEST A Comprehensive Review of Basal Cell Carcinoma and Benign or Malignant Collision Tumors at The23712047No ratings yet
- SKIN, HAIR, and NAILSDocument17 pagesSKIN, HAIR, and NAILSkhalidNo ratings yet
- Buzz Word Cheat Sheet (Derm)Document5 pagesBuzz Word Cheat Sheet (Derm)emilyjvaldez99No ratings yet
- Nursing Care Plan: A Client With Malignant MelanomaDocument2 pagesNursing Care Plan: A Client With Malignant MelanomaLorina Lynne ApelacioNo ratings yet
- LMRDocument8 pagesLMRVarsha L KenkareNo ratings yet
- 2 GYNE 1a - Benign Lesions of The Vagina, Cervix and UterusDocument11 pages2 GYNE 1a - Benign Lesions of The Vagina, Cervix and UterusIrene FranzNo ratings yet
- General Dermatology NotesDocument6 pagesGeneral Dermatology NotesPenny_Teoh_3451No ratings yet
- Approach To The Patient With A Skin DisorderDocument2 pagesApproach To The Patient With A Skin DisorderElrey InocianNo ratings yet
- Dermoscopy The Essentials - Soyer - 2nd Ed - 2012Document247 pagesDermoscopy The Essentials - Soyer - 2nd Ed - 2012impresionespribianNo ratings yet
- Benign Skin TumoursDocument7 pagesBenign Skin TumoursMan LorNo ratings yet
- Melanin-Associated Pigmented Lesions of The Oral Mucosa: Presentation, Differential Diagnosis, and TreatmentDocument10 pagesMelanin-Associated Pigmented Lesions of The Oral Mucosa: Presentation, Differential Diagnosis, and TreatmentFalling InsideNo ratings yet
- Skin Path NotesDocument15 pagesSkin Path NoteszeeathrNo ratings yet
- Skin PathologyDocument59 pagesSkin PathologyNeill CelesteNo ratings yet
- Ddg.13546.Doc BenerDocument25 pagesDdg.13546.Doc Benernailatul fadhilaNo ratings yet
- Group 1 QbankDocument10 pagesGroup 1 QbankBatch ElysianNo ratings yet
- A Case Series of Variants in Nevus DepigmentosusDocument4 pagesA Case Series of Variants in Nevus DepigmentosusIJAR JOURNALNo ratings yet
- وسام عوض Benign Skin Tumor-5 (Muhadharaty)Document6 pagesوسام عوض Benign Skin Tumor-5 (Muhadharaty)Alaa AhmedNo ratings yet
- Access Medicine - TableDocument2 pagesAccess Medicine - Tablecode-24No ratings yet
- Management of Malignant Melanoma DR Kiagus Handrian ParikersitDocument19 pagesManagement of Malignant Melanoma DR Kiagus Handrian ParikersitHandrian ParikesitNo ratings yet
- Analysis of Skin Morphological Features and Real-Time Monitoring Using Snapshot Hyperspectral ImagingDocument14 pagesAnalysis of Skin Morphological Features and Real-Time Monitoring Using Snapshot Hyperspectral Imagingthomasie1No ratings yet
- Dermoscopy: Malignant and Non-Malignant Skin LesionsDocument63 pagesDermoscopy: Malignant and Non-Malignant Skin LesionsZain ButtNo ratings yet
- Skin Cancer Detection Using Deep Learning Models - IpynbDocument189 pagesSkin Cancer Detection Using Deep Learning Models - Ipynblokeshpaarvai659No ratings yet
- Skin Lesion Classification Using Deep Learning Architectures: Abhishek C. Salian Shalaka Vaze Pragya SinghDocument6 pagesSkin Lesion Classification Using Deep Learning Architectures: Abhishek C. Salian Shalaka Vaze Pragya Singhz123No ratings yet
EN + Eosinofilia
EN + Eosinofilia
Uploaded by
Ana Flavia Baptista0 ratings0% found this document useful (0 votes)
3 views3 pagesOriginal Title
EN + eosinofilia
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
3 views3 pagesEN + Eosinofilia
EN + Eosinofilia
Uploaded by
Ana Flavia BaptistaCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 3
A congenital melanocytic nevus of the scalp is occa-
sionally associated with intracranial pigmentation, which
can be a benign asymptomatic coexisting melanomatosis
or an invasive extension of the cutaneous lesion or a
paracrinopathy from the overlying nevus.
6
Although the differential diagnosis of pigmentation and
bone abnormality includes Albright syndrome, it could be
excluded based on pathologic diagnosis of pigmentary
lesion. In Albright syndrome, pigmentation should be of
type caf-au-lait spots, not melanocytic nevus.
10
To our
knowledge, this is the rst case of congenital melanocytic
nevus of the scalp with underlying skull defect.
Although the association between a congenital melano-
cytic nevus of the scalp, underlying skull defect, and the
development of melanoma from the congenital melanocy-
tic nevus of the scalp are unclear, we suggest that clini-
cians should evaluate the skull in the patients who have
congenital melanocytic nevi of the scalp and have regular
follow-up examinations.
In our case, the small size of the specimen obtained by
a 3-mm punch biopsy instead of total excision might not
be representative for histopathological examination and
patient was informed and recommended regular visits at
least every 6 months.
Yeon Sook Kwon, MD
Jin Mo Park, MD
Hee Jung Kim, MD
Min-Geol Lee, MD, PhD
Department of Dermatology and Cutaneous Biology
Research Institute
Yonsei University College of Medicine
Seoul
Korea
E-mail: mglee@yuhs.ac
Funding sources: None.
Conict of interest to disclosure: None declared.
The authors have no relevant nancial interest in this
article.
References
1 Tannous ZS, Mihm MC Jr, Sober AJ, et al. Congenital
melanocytic nevi: clinical and histopathologic features,
risk of melanoma, and clinical management. J Am Acad
Dermatol 2005; 52: 197203.
2 Reed WB, Becker SW Sr, Becker SW Jr, et al. Giant
pigmented nevi, melanoma, and leptomeningeal
melanocytosis. Arch Dermatol 1965; 91: 100118.
3 Ho N, Roig C, Diadori P. Epidermal nevi and localized
cranial defects. Am J Med Genet 1999; 83: 187190.
4 Menter MA, Griessel PJC, de Klerk DJ. Giant blue
naevus of the scalp with underlying skull defect. Br J
Dermatol 1971; 85: 7375.
5 Silverberg GD, Kadin ME, Dorfman RF, et al. Invasion
of the brain by a cellular blue nevus of the scalp. A case
report with light and electron microscopic studies. Cancer
1971; 27: 349355.
6 Findler G, Hoffman HJ, Thomson HG, et al. Giant
nevus of the scalp associated with intracranial
pigmentation. Case report. J Neurosurg 1981; 54: 108
112.
7 Marano SR, Brooks RA, Spetzler RF, et al. Giant
congenital cellular blue nevus of the scalp of a newborn
with an underlying skull defect and invasion of the dura
mater. Neurosurgery 1986; 18: 8589.
8 Madaree A, Ramdial PK, Du Trevou M. Giant congenital
naevus of the scalp and cranium: case report and review
of the literature. Br J Plast Surg 1997; 50: 2025.
9 Kousseff BG. Hypothesis: Jadassohn nevus phakomatosis:
a paracrinopathy with variable phenotype. Am J Med
Genet 1992; 43: 651661.
10 Albright F, Butler AM, Hampton AO, Smith P.
Syndrome characterized by osteitis brosa disseminata,
areas of pigmentation and endocrine dysfunction, with
precocious puberty in females: report of ve cases. New
Eng J Med 1937; 16: 727746.
Erythema nodosum with eosinophilic panniculitis
Erythema nodosum (EN) is manifested by the sudden
onset of tender erythematous nodules and plaques on the
legs. The lesions show septal panniculitis chiey inl-
trated by lymphohistiocytes. Inltrated eosinophils are
usually in a minority. We describe here a patient with EN
who showed septal panniculitis with an admixture of
numerous eosinophils.
A 41-year-old Japanese woman visited our hospital
with a 3-month history of a painful eruption affecting the
left lower leg. She was in otherwise good health and used
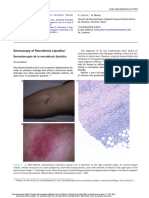
no medication. Examination showed a subcutaneous nod-
ule, 9 10 cm, with an erythematous surface on the ante-
rior of left lower leg (Fig. 1). A skin biopsy specimen
showed the presence of lymphohistiocytic inltrate chiey
in the septa of the subcutaneous tissues with minor inl-
tration near the septa (Fig. 2a). The overlying dermis had
a moderate, deep perivascular inltration. In the subcutis,
the inltrate was admixed with a number of eosinophils,
some of which showed degranulation (Fig. 2b). Clusters
of eosinophils were also present. Staining for fungi or
acid-fast bacilli was negative. Based on clinical and histo-
pathologic ndings, we diagnosed this case as EN with
eosinophilic panniculitis. Full blood count, electrolytes,
2010 The International Society of Dermatology International Journal of Dermatology 2010, 49, 960969
Correspondence 965
liver function tests, and antistreptolysin O titer were all
within normal limits. No peripheral eosinophilia was
found. An intradermal tuberculin test was positive
(20 18 mm induration). However, there were no abnor-
mal shadows on chest X-ray and no colonies of Mycobac-
terium tuberculosis in the sputum culture. Two months
later the lesion cleared spontaneously, and the patient has
had no recurrence of the skin lesion over the following
period of 12 months.
The inltrates in EN chiey consist of lymphohistio-
cytes, and eosinophils are usually in a minority. On the
other hand, eosinophilic panniculitis shows prominent
inltration with eosinophils in septa and/or lobules of the
subcutis. As eosinophilic panniculitis is associated with a
diverse range of local and systemic diseases including EN,
parasitic infection, and hypereosinophilic syndrome,
eosinophilic panniculitis is a histopathologic pattern
rather than a distinct entity.
14
We consider our case as
EN with eosinophilic panniculitis, because the clinical
and histopathologic features were consistent with those of
EN except numerous eosinophil inltration. EN is
thought to be a reactive phenomenon that may occur in
response to antigen stimuli. In our case, the exact patho-
mechanism is not understood, but the inltration may be
the result of some antigen expression which induces
eosinophils in the subcutis. In addition, eosinophilic inl-
tration may develop in several diseases, including non-
episodic type of angioedema with eosinophila, insect bite,
drug eruption, and Wells syndrome. However, our case
did not match that noted in them. Eosinophilic
inltration in EN may be more common than has been
thought.
Teie Egawa, MD, PhD
Ryuhei Okuyama, MD, PhD
Hachiro Tagami, MD, PhD
Setsuya Aiba, MD, PhD
(a)
(b)
Figure 2 Histopathologic nding: inltration in and near the
septa (a) and the admixture of eosinophils (b), some of which
showed degranulation (hematoxylin and eosin stain: a 100;
b 400)
Figure 1 Clinical nding: a subcutaneous nodule with an
erythematous surface on the lower leg
International Journal of Dermatology 2010, 49, 960969 2010 The International Society of Dermatology
Correspondence 966
Department of Dermatology,
Tohoku University Graduate School of Medicine,
Aoba-ku,
Sendai, Japan
Ryuhei Okuyama
Department of Dermatology
Tohoku University Graduate School of Medicine
1-1 Seiryo-machi
Aoba-ku, Sendai 980-8574
Japan
E-mail: rokuyama@mail.tains.tohoku.ac.jp
References
1 Adame J, Cohen PR. Eosinophilic panniculitis: diagnostic
considerations and evaluation. J Am Acad Dermatol 1996;
34: 229234.
2 Burket JM, Burket BJ. Eosinophilic panniculitis. J Am
Acad Dermatol 1985; 12: 161164.
3 Winkelmann RK, Frigas E. Eosinophilic panniculitis: a
clinicopathologic study. J Cutan Pathol 1986; 13: 112.
4 Wolff K, Goldsmith LA, Katz SI, Gilchrest BA, et al.
Fitzpatricks Dermatology in General Medicine. 7th
edn; New York: Mcgraw-Hill, 2008; 585.
Primary cutaneous peripheral T-cell non-Hodgkin
lymphoma, not otherwise specied, with cytotoxic
features
We have read with great interest the recently published
case report by Yamamoto et al.
1
describing a patient with
primary cutaneous aggressive T-cell lymphoma that
exhibited cytotoxic phenotype, however, without the
expression of CD8 antigen. In the light of this publica-
tion, we would like to present a similar patient history,
which, in our opinion, provides further data in regard of
this unique type of cutaneous lymphoma.
A 53-year-old man, with a 25-year history of tobacco
smoking, presented with a large, slightly painful ulcera-
tion in the right groin. The lesion started as a small, dark
reddish nodule that progressed within 2 weeks into a rap-
idly growing ulceration. About 6 months later, when the
patient came to our department, a moist ulceration of
about 35 cm diameter with a raised, inltrated border
was found (Fig. 1a). Until then only topical and systemic
antimicrobial agents were administered by the patient as
treatment. The patient was in good general condition;
peripheral lymph nodes were not enlarged and no other
clinically relevant abnormalities were stated during physi-
cal examination. The family history was irrelevant. Abdo-
men sonography revealed only mild hepatomegaly. The
patient also had slight leukocytosis (11 000 ll) with neu-
trophilia (74%) and accelerated erythrocyte sedimentation
rate (76 mm after 1 h). No other abnormalities were
found in laboratory and imaging examination (including
chest CT scan). To establish the diagnosis, a biopsy was
performed from the ulcer edge. The histology showed a
dense inltrate of medium- to large-sized lymphoid cells,
involving mainly dermis and lower layers of epidermis
(Fig. 2a,b). Majority of these cells were positive for CD3
(Fig. 2c), CD5, CD7, Ki-67, granzyme B (Fig. 2e), and
TIA-1 (Fig. 2f), while only some of them (< 20%) showed
expression of CD30. The tumor cells were also negative
for CD4, CD8, CD20, CD25, CD34, CD56, CD57,
CD68, CD117, pancytokeratin, HMB-45, Melan A, S100
protein, myeloperoxidase, perforin, ALK-1, and alfa-
actin. The CD8 positive staining was only restricted to
small cells representing a reactive inltrate (Fig. 2d). In
(a)
(b)
Figure 1 (a) Primary cutaneous epidermotropic cytotoxic lym-
phoma manifesting as an isolated, large ulceration with a
raised border in the right groin. (b) Local relapse of the tumor
2010 The International Society of Dermatology International Journal of Dermatology 2010, 49, 960969
Correspondence 967
You might also like
- Risk Factors & Prognosis For USMLE STEP 3 PDFDocument182 pagesRisk Factors & Prognosis For USMLE STEP 3 PDFSadia GhaniNo ratings yet
- Color Atlas of Pediatrics PDFDocument1,399 pagesColor Atlas of Pediatrics PDFJose Guaman100% (10)
- 2 Step Dermoscopedia SmallDocument4 pages2 Step Dermoscopedia SmallAndreea Barbuta100% (2)
- Dermoscopy Pathology Correlation in MelanomaDocument8 pagesDermoscopy Pathology Correlation in MelanomaDaniela SerbanNo ratings yet
- Disease Cheat SheetDocument393 pagesDisease Cheat Sheetjhk0428100% (1)
- 04.the Cleveland Clinic Intensive Review of Pediatrics 2nd EdDocument513 pages04.the Cleveland Clinic Intensive Review of Pediatrics 2nd EdSav GaNo ratings yet
- Lucivero Et Al 2011 Lupus Mastitis in Systemic Lupus Erythematosus A Rare Condition Requiring A Minimally InvasiveDocument5 pagesLucivero Et Al 2011 Lupus Mastitis in Systemic Lupus Erythematosus A Rare Condition Requiring A Minimally Invasiveruthdaniel6041No ratings yet
- Somorin SsDocument8 pagesSomorin SsChikezie OnwukweNo ratings yet
- Abstract: Kimura Disease Is A Rare Form of Chronic Inflammatory Disorder InvolvingDocument4 pagesAbstract: Kimura Disease Is A Rare Form of Chronic Inflammatory Disorder InvolvingpriyokNo ratings yet
- Hypopituitarism in Langerhans Cell Histiocytosis Seven Cases and Literature ReviewDocument8 pagesHypopituitarism in Langerhans Cell Histiocytosis Seven Cases and Literature ReviewafdtfngqbNo ratings yet
- Tsai (2007) - NSDocument2 pagesTsai (2007) - NSIlma ArifaniNo ratings yet
- Pi Is 0190962214011566Document2 pagesPi Is 0190962214011566LewishoppusNo ratings yet
- Bizkova 2009Document8 pagesBizkova 2009mario256No ratings yet
- UntitledDocument3 pagesUntitledShintaNo ratings yet
- PIIS0008418219302121Document4 pagesPIIS0008418219302121J MNo ratings yet
- Zoon's Plasma Cell Balanitis Associated With Male Genital Lichen SclerosusDocument4 pagesZoon's Plasma Cell Balanitis Associated With Male Genital Lichen SclerosusMircea-Dan Apopei-RusuNo ratings yet
- Lichenoid Skin Lesions - A Rare Manifestation in Secondary SyphilisDocument3 pagesLichenoid Skin Lesions - A Rare Manifestation in Secondary SyphilisShintaNo ratings yet
- Kikuchi' S Disease of The Mesenteric Lymph Nodes Presenting As Acute AppendicitisDocument3 pagesKikuchi' S Disease of The Mesenteric Lymph Nodes Presenting As Acute AppendicitisZulfikar Adi GumawangNo ratings yet
- Congenital Scalp Tumor With Ulceration: Jeremy Udkoff MA, MAS - Ralph E. Holmes MD - Magdalene A. Dohil MDDocument2 pagesCongenital Scalp Tumor With Ulceration: Jeremy Udkoff MA, MAS - Ralph E. Holmes MD - Magdalene A. Dohil MDAna MariaNo ratings yet
- Jcad 6 8 23Document6 pagesJcad 6 8 23Hadi FirmansyahNo ratings yet
- Phleboliths and The Vascular Maxillofacial LesionDocument4 pagesPhleboliths and The Vascular Maxillofacial LesionVinay KumarNo ratings yet
- Kikuchi's Disease: Malathi Sathiyasekaran R. Varadharajan So. ShivbalanDocument3 pagesKikuchi's Disease: Malathi Sathiyasekaran R. Varadharajan So. Shivbalanzulfikar adiNo ratings yet
- J Clin Pathol 1980 Brook 1099 101Document4 pagesJ Clin Pathol 1980 Brook 1099 101ysh_girlNo ratings yet
- Cutaneous Polyarteritis Nodosa in A Child FollowinDocument2 pagesCutaneous Polyarteritis Nodosa in A Child FollowinandresrogersNo ratings yet
- Prurigo Nodularis of HydeDocument12 pagesPrurigo Nodularis of HydeAugusto MonjardimNo ratings yet
- Iaet 12 I 2 P 135Document2 pagesIaet 12 I 2 P 135leonjunchan_66965707No ratings yet
- Brar (2007) - NS Resemples Lymphoreticular ProcessDocument2 pagesBrar (2007) - NS Resemples Lymphoreticular ProcessIlma ArifaniNo ratings yet
- (2017) BELOUSOVA, Irena E. Mycosis Fungoides Manifesting As Giant Cell Lichenoid DermatitisDocument3 pages(2017) BELOUSOVA, Irena E. Mycosis Fungoides Manifesting As Giant Cell Lichenoid DermatitisCassandra VérasNo ratings yet
- Cancer de Testiculo e Down 2Document4 pagesCancer de Testiculo e Down 2paulinhamericoNo ratings yet
- Sarcoidosis (Heerfordt Syndrome) : A Case Report: Tiia Tamme, Edvitar Leibur, Andres KullaDocument4 pagesSarcoidosis (Heerfordt Syndrome) : A Case Report: Tiia Tamme, Edvitar Leibur, Andres KullajaquelineartNo ratings yet
- Yayli (2013) - NS Resembles KaposiDocument3 pagesYayli (2013) - NS Resembles KaposiIlma ArifaniNo ratings yet
- Eosinophilic Cellulitis Arch Arg PediatrDocument5 pagesEosinophilic Cellulitis Arch Arg PediatrElianaNo ratings yet
- 108 Orbitorhinocerebral MucormycosisDocument10 pages108 Orbitorhinocerebral MucormycosisrgumralNo ratings yet
- A Case of Pemphigus Vulgaris Associated With Ulcerative ColitisDocument4 pagesA Case of Pemphigus Vulgaris Associated With Ulcerative ColitisfakhmiyogiiNo ratings yet
- Extraordinary Case Unique Presentation of EBVmucocutaneousulcerDocument4 pagesExtraordinary Case Unique Presentation of EBVmucocutaneousulcerRogério Ramos MarquesNo ratings yet
- ScrofulodermDocument4 pagesScrofulodermIzmi AzizahNo ratings yet
- Masquerade SyndromesDocument10 pagesMasquerade Syndromestony_chrisNo ratings yet
- 18 Extra-GuptaNDocument3 pages18 Extra-GuptaNGalih rarang gatiNo ratings yet
- Acne Urticata Associated With Chronic Myelogenous Leukemia: of Be of ofDocument4 pagesAcne Urticata Associated With Chronic Myelogenous Leukemia: of Be of ofGo McFlyNo ratings yet
- Reversal Reaction With Nodules That Initially Diagnosed As Erythema Nodosum Leprosum in Borderline Lepromatous LeprosyDocument6 pagesReversal Reaction With Nodules That Initially Diagnosed As Erythema Nodosum Leprosum in Borderline Lepromatous Leprosysilvavitria mandenasNo ratings yet
- Case Report: Langerhans Cell Histiocytosis of The Mandible in A Six-Year-Old ChildDocument0 pagesCase Report: Langerhans Cell Histiocytosis of The Mandible in A Six-Year-Old ChildElvina Agnestin HarianjaNo ratings yet
- Dermoscopy of Necrobiosis LipoidicaDocument4 pagesDermoscopy of Necrobiosis LipoidicaAndrés WunderwaldNo ratings yet
- Kimura DiseaseDocument4 pagesKimura DiseasewitariNo ratings yet
- Case Report: Subcorneal Pustular Dermatosis in Childhood: A Case Report and Review of The LiteratureDocument6 pagesCase Report: Subcorneal Pustular Dermatosis in Childhood: A Case Report and Review of The LiteratureIrsalinaHusnaAzwirNo ratings yet
- Scrofuloderma: A Common Type of Cutaneous Tuberculosis. A Case ReportDocument5 pagesScrofuloderma: A Common Type of Cutaneous Tuberculosis. A Case ReportIndah IndrianiNo ratings yet
- 2006 Gosche Vick SemPedSurgeryDocument8 pages2006 Gosche Vick SemPedSurgeryResya I. NoerNo ratings yet
- Primary Conjunctival Tuberculosis-2Document3 pagesPrimary Conjunctival Tuberculosis-2puutieNo ratings yet
- Cerebellopontine Angle Epidermoid CYST: Case ReportDocument3 pagesCerebellopontine Angle Epidermoid CYST: Case ReportTamajyoti GhoshNo ratings yet
- Liken PlanusDocument6 pagesLiken PlanusAmirahShalehaNo ratings yet
- Parakeratosis Variegata: A Possible Role of Environmental Hazards?Document4 pagesParakeratosis Variegata: A Possible Role of Environmental Hazards?Ega AihenaNo ratings yet
- Pi Is 0190962208009328Document2 pagesPi Is 0190962208009328Nabhya MaheshwariNo ratings yet
- Art Acta - Neurol.belgicaDocument6 pagesArt Acta - Neurol.belgicaAna GabrielaNo ratings yet
- Rare Cases in ENTDocument5 pagesRare Cases in ENTshadia sameerNo ratings yet
- AD1110894Document5 pagesAD1110894dhawalduvey95No ratings yet
- Papuloerythroderma of Ofuji - A Case ReportDocument4 pagesPapuloerythroderma of Ofuji - A Case ReportLidwina ApyakaNo ratings yet
- Early - Stage Hodgkins Lymphoma in A Child A CaseDocument6 pagesEarly - Stage Hodgkins Lymphoma in A Child A CaseХарш Навнітбхаі НімаватNo ratings yet
- Ecthyma Contagiosum (Human Orf)Document2 pagesEcthyma Contagiosum (Human Orf)Deba P SarmaNo ratings yet
- Aimee - Cutaneous and Systemic PlasmacytosisDocument3 pagesAimee - Cutaneous and Systemic PlasmacytosisEva YustianaNo ratings yet
- Human OrfDocument3 pagesHuman OrfDeba P SarmaNo ratings yet
- 2011 Ulcerated Cutaneous Epithelioid Hemangioendothelioma in An 8-Month Old InfantDocument2 pages2011 Ulcerated Cutaneous Epithelioid Hemangioendothelioma in An 8-Month Old InfantpsicobastoNo ratings yet
- JournalDocument5 pagesJournalgabbynengNo ratings yet
- Ring B Lymphoma B Highly Indicat Source Graefes Arch Clin Exp Ophthalmol 2021 Mar 2 Doi 10 1007 s00417 021 05075 6 Online Ahead of PrintDocument4 pagesRing B Lymphoma B Highly Indicat Source Graefes Arch Clin Exp Ophthalmol 2021 Mar 2 Doi 10 1007 s00417 021 05075 6 Online Ahead of Print381098891No ratings yet
- Calvarial Tuberculosis: E Ünüvar, F O Guz, B Sadiko Glu, M Sidal, Ü One S and S TetikkurtDocument2 pagesCalvarial Tuberculosis: E Ünüvar, F O Guz, B Sadiko Glu, M Sidal, Ü One S and S Tetikkurtkbianca26No ratings yet
- Diagnosis in OncologyDocument22 pagesDiagnosis in OncologyAndi SuryajayaNo ratings yet
- Lethal Midline Granuloma Importance of Early Diagnosis: A Case ReportDocument0 pagesLethal Midline Granuloma Importance of Early Diagnosis: A Case ReportdeolukmanaNo ratings yet
- (Download PDF) Dermatoscopy A Z 1St Edition Aimilios Lallas Online Ebook All Chapter PDFDocument42 pages(Download PDF) Dermatoscopy A Z 1St Edition Aimilios Lallas Online Ebook All Chapter PDFsusan.brown255100% (12)
- Multiple Skin Neoplasms at One Site MUSK IN A NEST A Comprehensive Review of Basal Cell Carcinoma and Benign or Malignant Collision Tumors at TheDocument12 pagesMultiple Skin Neoplasms at One Site MUSK IN A NEST A Comprehensive Review of Basal Cell Carcinoma and Benign or Malignant Collision Tumors at The23712047No ratings yet
- SKIN, HAIR, and NAILSDocument17 pagesSKIN, HAIR, and NAILSkhalidNo ratings yet
- Buzz Word Cheat Sheet (Derm)Document5 pagesBuzz Word Cheat Sheet (Derm)emilyjvaldez99No ratings yet
- Nursing Care Plan: A Client With Malignant MelanomaDocument2 pagesNursing Care Plan: A Client With Malignant MelanomaLorina Lynne ApelacioNo ratings yet
- LMRDocument8 pagesLMRVarsha L KenkareNo ratings yet
- 2 GYNE 1a - Benign Lesions of The Vagina, Cervix and UterusDocument11 pages2 GYNE 1a - Benign Lesions of The Vagina, Cervix and UterusIrene FranzNo ratings yet
- General Dermatology NotesDocument6 pagesGeneral Dermatology NotesPenny_Teoh_3451No ratings yet
- Approach To The Patient With A Skin DisorderDocument2 pagesApproach To The Patient With A Skin DisorderElrey InocianNo ratings yet
- Dermoscopy The Essentials - Soyer - 2nd Ed - 2012Document247 pagesDermoscopy The Essentials - Soyer - 2nd Ed - 2012impresionespribianNo ratings yet
- Benign Skin TumoursDocument7 pagesBenign Skin TumoursMan LorNo ratings yet
- Melanin-Associated Pigmented Lesions of The Oral Mucosa: Presentation, Differential Diagnosis, and TreatmentDocument10 pagesMelanin-Associated Pigmented Lesions of The Oral Mucosa: Presentation, Differential Diagnosis, and TreatmentFalling InsideNo ratings yet
- Skin Path NotesDocument15 pagesSkin Path NoteszeeathrNo ratings yet
- Skin PathologyDocument59 pagesSkin PathologyNeill CelesteNo ratings yet
- Ddg.13546.Doc BenerDocument25 pagesDdg.13546.Doc Benernailatul fadhilaNo ratings yet
- Group 1 QbankDocument10 pagesGroup 1 QbankBatch ElysianNo ratings yet
- A Case Series of Variants in Nevus DepigmentosusDocument4 pagesA Case Series of Variants in Nevus DepigmentosusIJAR JOURNALNo ratings yet
- وسام عوض Benign Skin Tumor-5 (Muhadharaty)Document6 pagesوسام عوض Benign Skin Tumor-5 (Muhadharaty)Alaa AhmedNo ratings yet
- Access Medicine - TableDocument2 pagesAccess Medicine - Tablecode-24No ratings yet
- Management of Malignant Melanoma DR Kiagus Handrian ParikersitDocument19 pagesManagement of Malignant Melanoma DR Kiagus Handrian ParikersitHandrian ParikesitNo ratings yet
- Analysis of Skin Morphological Features and Real-Time Monitoring Using Snapshot Hyperspectral ImagingDocument14 pagesAnalysis of Skin Morphological Features and Real-Time Monitoring Using Snapshot Hyperspectral Imagingthomasie1No ratings yet
- Dermoscopy: Malignant and Non-Malignant Skin LesionsDocument63 pagesDermoscopy: Malignant and Non-Malignant Skin LesionsZain ButtNo ratings yet
- Skin Cancer Detection Using Deep Learning Models - IpynbDocument189 pagesSkin Cancer Detection Using Deep Learning Models - Ipynblokeshpaarvai659No ratings yet
- Skin Lesion Classification Using Deep Learning Architectures: Abhishek C. Salian Shalaka Vaze Pragya SinghDocument6 pagesSkin Lesion Classification Using Deep Learning Architectures: Abhishek C. Salian Shalaka Vaze Pragya Singhz123No ratings yet