Professional Documents
Culture Documents
Gestational Trophoblastic Disease
Gestational Trophoblastic Disease
Uploaded by
Deborah Reyes0 ratings0% found this document useful (0 votes)
5 views1 pagegtd
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentgtd
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
5 views1 pageGestational Trophoblastic Disease
Gestational Trophoblastic Disease
Uploaded by
Deborah Reyesgtd
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 1
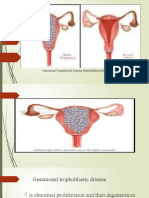
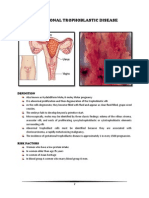
Gestational Trophoblastic Disease abnormal proliferation and then
degeneration of the trophoblastic villi.
- In in every 1500 pregnancies.
- Choriocarcinoma rapidly metasizing malignancy
Risk factors:
Women who have low protein intake
Older than 35 years old.
Younger than 18 years old
Women of Asian heritage.
Type of Molar Growth
1. Complete Mole all trophoblastic villi well and become cystic
- If embryo forms, it dies early at only 1-2 mm in size, no fetal blood
- Karyotype: normal 46XX or 46 XY from dads chromosomes x2, empty
ovum
- Leads to choriocarcinoma
2. Partial Mole the syncytiotrophoblastic layer is swollen and misshapen
- Macerated embryo of approximately 9 wks may be present and fetal blood
may be present in the villi.
- Karyotype: 69 chromosomes (a triploid formation in w/c there are three
chromosomes instead of 2 for every pair)
- Rarely leads to choriocarcinoma
Diagnostic tests:
Urine test: hCG (1-2 million IU, normal: 400,000 IU)
UTZ: dense growth (snowflake pattern) but no fetal growth
Signs and Symptoms
Uterus expand faster than normal before the usual time (over the symphysis
brim at 12 wks, at the umbilicus 20-24 wks)
n/v
no fetal heart sounds
symptoms of PIH: htn, edema, proteinuria before 20 wks
vaginal bleeding at 16 wks (vaginal spotting of dark brown blood or as a
profuse fresh flow)
bleeding accompanied by discharge of the clear fluid-filled vesicles
Therapeutic Management:
D&C
Monitor hCG 3 times after surgery (every 2 weeks)
- Half of women still have a positive reading at 3 wks, women still positive at
40 days
Baseline pelvic examination, chest xray, and a serum test for the beta
subunit of hCG (every 4 wks for 6-12 mos)
oral contraceptives for 12 mos
methotrexate, dactinomycin if metastasis occurs
You might also like
- Molar PregnancyDocument15 pagesMolar Pregnancyapi-3705046No ratings yet
- Molar PregnancyDocument53 pagesMolar Pregnancyboragam.saisharanyaNo ratings yet
- Gestational Trophoblastic DiseaseDocument22 pagesGestational Trophoblastic DiseaseBright KumwendaNo ratings yet
- Gestational Trophoblastic Disease (Hydatidiform Mole)Document4 pagesGestational Trophoblastic Disease (Hydatidiform Mole)Zhane Inamac CezarNo ratings yet
- M3 - ReviewerDocument8 pagesM3 - ReviewerKristine KimNo ratings yet
- Gestational Trophoblastic Disease WordDocument3 pagesGestational Trophoblastic Disease WordsahaniNo ratings yet
- Hydatidiform Mole-Is A Type of Gestational Trophoblastic Neoplasm ThatDocument4 pagesHydatidiform Mole-Is A Type of Gestational Trophoblastic Neoplasm ThatjhelabooNo ratings yet
- MSC Zahraa Abdul Ghani M.A: Done byDocument9 pagesMSC Zahraa Abdul Ghani M.A: Done byFahima SekandaryNo ratings yet
- Dr. Maryam Al - Jaber Consultant, Family Medicine March, 2015 Dr. Omnia Darweesh Resident, Family MedicineDocument57 pagesDr. Maryam Al - Jaber Consultant, Family Medicine March, 2015 Dr. Omnia Darweesh Resident, Family MedicineFaizyabNo ratings yet
- OBGYN Study Guide 1Document48 pagesOBGYN Study Guide 1Dayana FrazerNo ratings yet
- 3-Ammar Notes (Ob - Gyn)Document6 pages3-Ammar Notes (Ob - Gyn)Dr-Hashem Al-ShareefNo ratings yet
- History:: Obs-Gyn Antepartum HaemorrhageDocument2 pagesHistory:: Obs-Gyn Antepartum HaemorrhagejNo ratings yet
- 2nd Trimester BleedingDocument50 pages2nd Trimester BleedingRaiden VizcondeNo ratings yet
- Gestational Trophoblastic DiseaseDocument4 pagesGestational Trophoblastic DiseasePrincess PlateroNo ratings yet
- Gestational Trophoblastic Disease (GTD) : Ahmed Refaat Abd ElzaherDocument41 pagesGestational Trophoblastic Disease (GTD) : Ahmed Refaat Abd ElzaherJessica NadiaNo ratings yet
- Gestational Trophoblastic DiseaseDocument37 pagesGestational Trophoblastic DiseaseOlisa 'phage' Onyebuchi100% (1)
- Antepartum HaemorrhageDocument48 pagesAntepartum HaemorrhageDuncan JacksonNo ratings yet
- Case PresentationDocument36 pagesCase PresentationTara LeungNo ratings yet
- Ghen ReviewDocument6 pagesGhen ReviewGenesis Marie Felices GonzalesNo ratings yet
- Gestational Trophoblastic DiseaseDocument40 pagesGestational Trophoblastic DiseaseAayupta Mohanty100% (2)
- Gestational - PrematureDocument3 pagesGestational - PrematureBench AvilaNo ratings yet
- Molar PregnancyDocument14 pagesMolar Pregnancyfardeal_mckk100% (1)
- GYN Module 3 Case 1: Gestational Trophoblastic NeoplasiaDocument21 pagesGYN Module 3 Case 1: Gestational Trophoblastic NeoplasiaElaine Marie Rendon PalmejarNo ratings yet
- Placenta Previa 08Document42 pagesPlacenta Previa 08Sam Ngugi100% (1)
- HmoleDocument30 pagesHmoleevaNo ratings yet
- Obesteric Gynacology Short Notes For Usmle Step 2Document32 pagesObesteric Gynacology Short Notes For Usmle Step 2Rodaba Ahmadi Meherzad100% (1)
- Maternal Chil Nursing AbnormalDocument68 pagesMaternal Chil Nursing AbnormalNicole Virtudez SeriñaNo ratings yet
- Vesicular MoleDocument46 pagesVesicular Moledhisazainita0% (1)
- Lecture 11 Antepartum HaemorrhageDocument24 pagesLecture 11 Antepartum HaemorrhageMihraban OmerNo ratings yet
- Bleeding in Early PregnancyDocument4 pagesBleeding in Early Pregnancynur1146No ratings yet
- 12 Antepartum HemorrhageDocument10 pages12 Antepartum HemorrhageJuan RamirezNo ratings yet
- Management of Pregnancy Related BleedingDocument75 pagesManagement of Pregnancy Related BleedingChuah Wei Hong100% (1)
- GYN Module 3 Case 1: Gestational Trophoblastic NeoplasiaDocument21 pagesGYN Module 3 Case 1: Gestational Trophoblastic NeoplasiaElaine Marie Rendon PalmejarNo ratings yet
- OBS Review Session Suzanne Ectopic PregnancyDocument7 pagesOBS Review Session Suzanne Ectopic PregnancyhitowaNo ratings yet
- Gestational and Placental DisordersDocument2 pagesGestational and Placental DisordersIdelisse Marie SuarezNo ratings yet
- Postpartum Hemorrhage Case Report: Hanisah Idris Norfarah Izzati AzmanDocument51 pagesPostpartum Hemorrhage Case Report: Hanisah Idris Norfarah Izzati AzmanWanieSariffNo ratings yet
- Pregnancy Diagnosis: Peng Xuebing, M.D. Dept of Obs/Gyn Beijing Fu Xing Hospital Capital Medical UniversityDocument48 pagesPregnancy Diagnosis: Peng Xuebing, M.D. Dept of Obs/Gyn Beijing Fu Xing Hospital Capital Medical UniversityAhmed TarigNo ratings yet
- Untitled 1Document16 pagesUntitled 1Nita Corry AgustineNo ratings yet
- Clinical Activities: A. Pre - ConsultationDocument13 pagesClinical Activities: A. Pre - ConsultationerykafadsNo ratings yet
- CCD Obstetric GynecologyDocument43 pagesCCD Obstetric GynecologyHanif GandohNo ratings yet
- Postpartal HemorrhageDocument9 pagesPostpartal HemorrhageJkimNo ratings yet
- Case Study 29-APHDocument31 pagesCase Study 29-APHZarul Naim Mohd TamiziNo ratings yet
- Case Presentation Group A 1Document91 pagesCase Presentation Group A 1Tiffany AdriasNo ratings yet
- Seminar Gestational Trophoblastic DiseaseDocument27 pagesSeminar Gestational Trophoblastic Diseasehusnajihah18No ratings yet
- H MoleDocument12 pagesH MoleRisqi YuliNo ratings yet
- Gestational Trophoblastic DiseaseDocument53 pagesGestational Trophoblastic Diseaseahmad danil fatahNo ratings yet
- Bleeding in Early Late PregnancyDocument46 pagesBleeding in Early Late PregnancyAndrada Catrinoiu100% (2)
- Chapter 21 Reviewer TillesDocument16 pagesChapter 21 Reviewer Tillescutiepie creampieNo ratings yet
- Gestational Trophoblastic DiseasesDocument43 pagesGestational Trophoblastic DiseasesAnironOrion100% (1)
- Pregnancy (Y)Document64 pagesPregnancy (Y)Mohamed AbbasNo ratings yet
- ObsGyn RR @academycerebellumDocument180 pagesObsGyn RR @academycerebellumNeeladri DawnNo ratings yet
- MCQ's 3 Flashcards - QuizletDocument12 pagesMCQ's 3 Flashcards - Quizletbmhsh100% (1)
- Kuliah PK2 TESKehamilanJULI2010Document38 pagesKuliah PK2 TESKehamilanJULI2010Fetty NataliaNo ratings yet
- (Ob) Paper Case 1Document4 pages(Ob) Paper Case 1Sam MataNo ratings yet
- H MoleDocument71 pagesH MoleDoc AchondoNo ratings yet
- Ante Partum Hemorrhage: DR Haddis (MD)Document42 pagesAnte Partum Hemorrhage: DR Haddis (MD)Getasil GetawmarNo ratings yet
- Menses: Dr. Said SarahnehDocument41 pagesMenses: Dr. Said Sarahnehpal_pal_palNo ratings yet
- Post Partum Hemorrhage (PPH) : Nasheel Kaur Gill Supervisor: DR KosillaDocument40 pagesPost Partum Hemorrhage (PPH) : Nasheel Kaur Gill Supervisor: DR KosillaHaziq MarsNo ratings yet