Professional Documents
Culture Documents
Cystic Fibrosis
Cystic Fibrosis
Uploaded by
zarasarOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Cystic Fibrosis
Cystic Fibrosis
Uploaded by
zarasarCopyright:
Available Formats
2.
4 In-depth study of a genetic
disease
Cystic Fibrosis
Caused by a recessive gene.
About CFTR protein
Cystic fibrosis transmembrane regulatory channel protein.
It is an enormous protein, made of 1480 amino acids the gene
that codes it is also very large & found on chromosome 7.
A mutation in any part of the gene for making the CFTR protein
can cause cystic fibrosis.
In normal people:
The CFTR protein is found in epithelial cells. It allows the Cl - ions found
inside the cell to leave & inhibits the movement of Na+ into the cell
from outside. The ions outside the cell attract water (from the cells),
making the mucus around their membranes diluted & watery and
easier for the body to handle.
In people suffering from cystic fibrosis:
The CFTR protein is not functioning normally, if not at all. Cl - ions
cannot leave the cell, and Na+ ions are welcome to enter. If the ions are
inside the cell, water moves inside the cell by osmosis from the fluid
surrounding cells, making the mucus thick and sticky.
The inheritance of cystic fibrosis
Many people may not know they are carriers until they reproduce
offspring with cystic fibrosis as they are phenotypically normal.
Symptoms of cystic fibrosis
The respiratory system:
Builds up in tiny airways of lungs and block air supply to alveoli &
blocks smaller bronchioles completely reduces surface area
available in lungs for gaseous exchange severe coughing fits to
attempt to get rid of the mucus & feel breathless & often short of
oxygen tired.
Cilia cannot move mucus up and out of respiratory track as its
too thick & sticky lungs gradually fill up with mucus less
effective for gaseous exchange.
Bacteria & pathogens breathed in & trapped in mucus cannot be
coughed out of the respiratory system builds up in lungs
provides bacteria with the ideal conditions in which to grow.
Body normally secretes antibodies into the mucus to deactivate
the pathogens. The solutes become more concentrated.
Dehydrated surfaces lose their natural bacterial properties
WBCs & antibodies cannot function effectively in thick mucus.
This can be fixed by rehydrating the surface of the cell.
The digestive system:
2.4 In-depth study of a genetic
disease
Thin mucus is produced in the pancreatic duct by the cells lining the
tube.
A faulty CFTR proteins means that the mucus is thick & sticky blocks
the pancreatic duct enzymes do not reach the duodenum food is
not digested properly so you dont get enough nutrients from the food
& digestive enzymes stay in pancreas and start to digest it and may
lead to diabetes.
Mucus is also produced in the gut to protect it from damage from the
enzymes & to act as a lubricant. In cystic fibrosis, the thick mucus
forms a barrier between the contents of the gut and the lining of the
intestine, clogging up the villi & reducing the surface area for
absorption.
Cystic fibrosis patients are at a huge risk of malnutrition & struggle to
maintain their body mass.
The reproductive system:
In women:
Mucus normally changes throughout the menstrual cycle. When a
woman is fertile, it becomes thinner to help the sperm through the
cervix. In cystic fibrosis, healthy eggs are generally produced, but the
thick mucus blocks the cervix & can block the oviducts so sperm
cannot reach them.
In men:
Men are often infertile. They may lack the vas deferens (tube that
carries sperm out of testes into semen). If the vas deferens is present,
it is either partially or completely blocked with thick mucus, so a
reduced/no number of sperm can leave the testes.
The sweat glands:
Sweat is normally more concentrated & salty than normal.
Normally, as sweat passes along the duct of a sweat gland, salt is
reabsorbed CFTR protein moves Cl- into cells & Na+ follows along the
concentration gradient. This prevents the body from losing too much
salt.
In cystic fibrosis, Cl- is moved out of cells, remaining in sweat.
Balance of ions on body affected nervous system & heart affected.
If too much salt is lost concentration of body fluids changes
affects heart.
Treating Cystic Fibrosis Now
There are no cures for cystic fibrosis. Treatments aim to reduce
symptoms & allow body systems to work as effectively as possible.
Physiotherapy
2.4 In-depth study of a genetic
disease
Important for removing thick, sticky mucus from lungs easier to
breathe & take in O2 reduces risk of serious lung infections.
Usually done a couple of times a day.
New devices that change the pressure in airways help people clear the
mucus without using more vigorous physiotherapy.
Diet & Enzymes
People take enzymes when they have a meal.
Need to eat a carefully balanced diet & eat more than other people to
make up for what they cannot digest.
Need more high energy foods & and an adult needs twice as much
protein.
Drug therapies
Antibiotics: destroy bacteria that could potentially cause lifethreatening lung infections. Inhalers (aerosols) used to breathe
them deep into lungs.
Vaccines: need flu vaccines every year & a vaccine against
pneumonia.
Mucolytics: drugs that make the mucus runnier easier to move.
Asthma drugs: used to open airways & reduce lung inflammation.
DNAase enzymes: make mucus thinner & easier to cough up.
Insulin.
Transplant Surgery
Lung damage may be so severe that lungs cant function properly &
heart may be affected lung/heart & lung transplant.
New organs wont be affected by cystic fibrosis, but the rest of the
body will still have the other problems.
Patient must take immunosuppressant drugs for the rest of their life
suppressing the immune system harder to fight infections.
People with cystic fibrosis who have lung transplants usually do well.
Infertility treatments
Some women use IVF, while for others, their reproductive system is not
badly affected.
Sperm can be taken from testes & fertilise eggs in vitro. Resulting
embryos are returned to mothers uterus to develop normally.
2.4 In-depth study of a genetic
disease
Gene therapy for cystic fibrosis
DNA can be replicated artificially by the polymerase chain reaction.
The enzyme DNA polymerase is used to make new double stranded
DNA by synthesising a new complementary strand to a pre-existing
strand, just as in natural replication.
PCR makes it possible to synthesise large numbers of copies of very
small samples of DNA.
DNA fragments can be separated by gel electrophoresis. A voltage is
applied to the gel and the negatively charged DNA fragments move
towards the positive electrode. Smaller fragments move faster than
large ones.
The bands of DNA can be seen if radioactive nucleotides are used in
the PCR. The pattern of banding in the gel can be made visible by
placing the gel next to a sheet of unexposed photographic film
overnight. the radioactive bands cause the film to turn black.
Cystic fibrosis is a genetic disorder caused by a mutant allele that
produces a defective form of the channel protein, called CFTR. This
protein normally transports chloride ions out of the cells.
The defective CFTR protein causes chloride ions to build up in the cells.
This causes those cells to retain water. In the lungs and intestines this
is a particular problem. Water fails to pass into the mucus that lines the
airways and gut, causing the mucus to become thick and sticky. In the
lungs, this leads to breathing difficulties and the risk of infection; in the
gut, the mucus blocks the ducts that carry digestive enzymes.
Some severe genetic disorders can be treated by gene therapy.
Healthy genes are cloned and then transferred to target cells in the
body to take over the function of defective genes that cause the
disorder.
Two forms of gene therapy are being developed to treat cystic fibrosis.
In the first, healthy CFTR genes are inserted into liposomes, which fuse
with the cell membranes and take the genes into the cells. In the other,
harmless viruses are used to insert the CFTR genes into the cells.
In genetic engineering genes are taken from one organism and
inserted into another. Genes that code for useful substances, such as
hormones, enzymes and antibiotics, are often transferred into microorganisms, which then produce large quantities of these substances.
The gene is cut out from the DNA of the donor organism using a
restriction endonuclease enzyme. This cuts out the relevant section of
the organism's DNA, leaving sticky ends - which consist of a single
strand with a few base pairs - that will enable the gene to be inserted
into a small circular piece of bacterial DNA called a plasmid.
2.4 In-depth study of a genetic
disease
Plasmids are often used as vectors to take the selected gene into
bacterial cells. Plasmids occur naturally in cells and replicate
independently of the main bacterial DNA.
The same restriction endonuclease is used to cut the plasmid. This
leaves complementary sticky ends to which the selected gene can be
attached
The sticky ends of the gene and the open plasmid are joined together
by ligase which is another enzyme.
The plasmids are then introduced into the target organism, and
transformed cells are selected and cloned.
Genetic markers in the plasmids, such as genes that confer antibiotic
resistance, enable genetic engineers to identify bacteria that have
successfully taken up the selected gene.
Transformed bacteria are cultured on a large scale in industrial
fermenters and the useful product is then extracted.
Genetic engineering is a very young discipline, and is only possible due
to the development of techniques from the 1960s onwards. These
techniques have been made possible from our greater understanding
of DNA and how it functions following the discovery of its structure by
Watson and Crick in 1953. Although the final goal of genetic
engineering is usually the expression of a gene in a host, in fact most
of the techniques and time in genetic engineering are spent isolating a
gene and then cloning it. This table lists the techniques that we'll look
at in detail.
Restriction Enzymes
To cut DNA at specific points, making small fragments
DNA Ligase
To join DNA fragments together
Vectors
To carry DNA into cells and ensure replication
Plasmids
Common kind of vector
Genetic Markers
To identify cells that have been transformed
PCR
To amplify very small samples of DNA
cDNA
To make a DNA copy of mRNA
DNA probes
To identify and label a piece of DNA containing a certain sequence
Gene Synthesis
2.4 In-depth study of a genetic
disease
To make a gene from scratch
Electrophoresis
To separate fragments of DNA
DNA Sequencing
To read the base sequence of a length of DNA
Restriction Enzymes
These are enzymes that cut DNA at specific sites. They are properly
called restriction endonucleases because they cut the bonds in the
middle of the polynucleotide chain. Most restriction enzymes make a
staggered cut in the two strands, forming sticky ends.
The cut ends are "sticky" because they have short stretches of singlestranded DNA. These sticky ends will stick (or anneal) to another piece
of DNA by complementary base pairing, but only if they have both
been cut with the same restriction enzyme. Restriction enzymes are
highly specific, and will only cut DNA at specific base sequences, 4-8
base pairs long.
Restriction enzymes are produced naturally by bacteria as a defence
against viruses (they "restrict" viral growth), but they are enormously
useful in genetic engineering for cutting DNA at precise places
("molecular scissors"). Short lengths of DNA cut out by restriction
enzymes are called restriction fragments. There are thousands of
different restriction enzymes known, with over a hundred different
recognition sequences. Restriction enzymes are named after the
bacteria species they came from, so EcoR1 is from E. coli strain R.
DNA Ligase
This enzyme repairs broken DNA by joining two nucleotides in a DNA
strand. It is commonly used in genetic engineering to do the reverse of
a restriction enzyme, i.e. to join together complementary restriction
fragments.
The sticky ends allow two complementary restriction fragments to
anneal, but only by weak hydrogen bonds, which can quite easily be
broken, say by gentle heating. The backbone is still incomplete.
DNA ligase completes the DNA backbone by forming covalent bonds.
Restriction enzymes and DNA ligase can therefore be used together to
join lengths of DNA from different sources.
Vectors
In biology a vector is something that carries things between species.
E.g. the mosquito is a vector that carries the malaria parasite into
humans. In genetic engineering a vector is a length of DNA that carries
the gene we want into a host cell. A vector is needed because a length
of DNA containing a gene on its own wont actually do anything inside
2.4 In-depth study of a genetic
disease
a host cell. Since it is not part of the cells normal genome it wont be
replicated when the cell divides, it wont be expressed, and in fact it
will probably be broken down pretty quickly. A vector gets round these
problems by having these properties:
It is big enough to hold the gene we want
It is circular (or more accurately a closed loop), so that it is less likely
to be broken down
It contains control sequences, such as a transcription promoter, so that
the gene will be replicated or expressed.
It contain marker genes, so that cells containing the vector can be
identified.
Type of vector
Max length of DNA insert
Plasmid
10 kbp
Virus or phage
30 kbp
Plasmids (the most common vectors)
Plasmids are by far the most common kind of vector, so we shall look
at how they are used in some detail. Plasmids are short circular bits of
DNA found naturally in bacterial cells. A typical plasmid contains 3-5
genes and there are around 10 copies of a plasmid in a bacterial cell.
Plasmids are copied when the cell divides, so the plasmid genes are
passed on to all daughter cells. They are also used naturally for
exchange of genes between bacterial cells (the nearest they get to
sex), so bacterial cells will take up a plasmid. Because they are so
small, they are easy to handle in a test tube, and foreign genes can
quite easily be incorporated into them using restriction enzymes and
DNA ligase.
One of the most common plasmids used is the R-plasmid (or pBR322).
This plasmid contains a replication origin, several recognition
sequences for different restriction enzymes (with names like EcoRI),
and two marker genes, which confer resistance to different antibiotics
(ampicillin and tetracycline).
The diagram below shows how DNA fragments can be incorporated
into a plasmid using restriction and ligase enzymes. The restriction
enzyme used here (PstI) cuts the plasmid in the middle of one of the
marker genes (well see why this is useful later). The foreign DNA
anneals with the plasmid and is joined covalently by DNA ligase to
form a hybrid vector (in other words a mixture or hybrid of bacterial
and foreign DNA). Several other products are also formed: some
plasmids will simply re-anneal with themselves to re-form the original
2.4 In-depth study of a genetic
disease
plasmid, and some DNA fragments will join together to form chains or
circles. Theses different products cannot easily be separated, but it
doesnt matter, as the marker genes can be used later to identify the
correct hybrid vector.
Cystic fibrosis (CF) is the most common genetic disease in the UK,
affecting about 1 in 2500. It is caused by a mutation in the gene for
protein called CFTR (Cystic Fibrosis Transmembrane Regulator). The
gene is located on chromosome 7, and there are actually over 300
different mutations known, although the most common mutation is a
deletion of three bases, removing one amino acid out of 1480 amino
acids in the protein. CFTR is a chloride ion channel protein found in the
cell membrane of epithelial (lining) tissue cells, and the mutation stops
the protein working, so chloride ions cannot cross the cell membrane.
Chloride ions build up inside these cells, which cause sodium ions to
enter to balance the charge, and the increased concentration of the
both these ions inside the epithelial cells decreases the osmotic
potential. Water is therefore retained inside the cells, which means that
the mucus secreted by these cells is drier and more sticky than normal.
This sticky mucus block the tubes into which it is secreted, such as the
small intestine, pancreatic duct, bile duct, sperm duct, bronchioles and
alveoli.
These blockages lead to the symptoms of CF: breathlessness, lung
infections such as bronchitis and pneumonia, poor digestion and
absorption, and infertility. Of these symptoms the lung effects are the
most serious causing 95% of deaths. CF is always fatal, though life
expectancy has increased from 1 year to about 20 years due to
modern treatments. These treatments include physiotherapy many
times each day to dislodge mucus from the lungs, antibiotics to fight
infections, DNAse drugs to loosen the mucus, enzymes to help food
digestion and even a heart-lung transplant.
Given these complicated (and ultimately unsuccessful) treatments, CF
is a good candidate for gene therapy, and was one of the first diseases
to be tackled this way. The gene for CFTR was identified in 1989 and a
cDNA clone was made soon after. The idea is to deliver copies of this
good gene to the epithelial cells of the lung, where they can be
incorporated into the nuclear DNA and make functional CFTR chloride
channels. If about 10% of the cells could be corrected, this would cure
the disease.
2.4 In-depth study of a genetic
disease
Two methods of delivery are being tried: liposomes and adenoviruses,
both delivered with an aerosol inhaler, like those used by asthmatics.
Clinical trials are currently underway, but as yet no therapy has been
shown to be successful.
It is important to appreciate the different between somatic cell therapy
and germ-line therapy.
Somatic cell therapy means genetically altering specific body (or
somatic) cells, such as bone marrow cells, pancreas cells, or whatever,
in order to treat the disease. This therapy may treat or cure the
disease, but any genetic changes will not be passed on their offspring.
Germ-line therapy means genetically altering those cells (sperm cells,
sperm precursor cell, ova, ova precursor cells, zygotes or early
embryos) that will pass their genes down the "germ-line" to future
generations. Alterations to any of these cells will affect every cell in the
resulting human, and in all his or her descendants.
Germ-line therapy would be highly effective, but is also potentially
dangerous (since the long-term effects of genetic alterations are not
known), unethical (since it could easily lead to eugenics) and immoral
(since it could involve altering and destroying human embryos). It is
currently illegal in the UK and most other countries, and current
research is focussing on somatic cell therapy only. All gene therapy
trials in the UK must be approved by the Gene Therapy Advisory
Committee (GTAC), a government body that reviews the medical and
ethical grounds for a trial. Germ-line modification is allowed with
animals, and indeed is the basis for producing GMOs.
You might also like
- FINAL EXAM Advanced Health Assessment and Diagnostic ReasoningDocument15 pagesFINAL EXAM Advanced Health Assessment and Diagnostic ReasoningGeorge Ekai100% (2)
- Basic Pharmacokinetics: Mohsen A. HedayaDocument14 pagesBasic Pharmacokinetics: Mohsen A. HedayaJai Jai Maharashtra100% (1)
- NUR 3032 Immune System Study PlanDocument5 pagesNUR 3032 Immune System Study PlanThalia Fortune100% (1)
- MicrobiologyDocument4 pagesMicrobiologyHannah Grace CorveraNo ratings yet
- Yousaf Ali (Auth.) - Self Assessment Questions in Rheumatology-Humana Press (2009)Document147 pagesYousaf Ali (Auth.) - Self Assessment Questions in Rheumatology-Humana Press (2009)Amr AmalNo ratings yet
- Maternity 17 Newborn Transitioning 2019Document51 pagesMaternity 17 Newborn Transitioning 2019Marvin AnciroNo ratings yet
- Integumentary System: Quick Review Notes Chapter 5From EverandIntegumentary System: Quick Review Notes Chapter 5Rating: 5 out of 5 stars5/5 (1)
- Duck RaisingDocument12 pagesDuck RaisingRosel Gonzalo-Aquino60% (10)
- Nature of DiseaseDocument14 pagesNature of DiseaseLambo Ignacio Queen Quin100% (1)
- Microbial Genetics: Julia Hartati, DRDocument21 pagesMicrobial Genetics: Julia Hartati, DRerwan_mivecNo ratings yet
- Biology NotesDocument5 pagesBiology NotesGlaukaNo ratings yet
- The Study of Very Small Living Organism Called MicroorganismDocument15 pagesThe Study of Very Small Living Organism Called MicroorganismTeresita Aviles100% (1)
- Sirs, Shock, Sepsis, ModsDocument8 pagesSirs, Shock, Sepsis, ModsthubtendrolmaNo ratings yet
- Lymphoid SystemDocument11 pagesLymphoid SystemSheena PasionNo ratings yet
- FAQ in MicrobiologyDocument117 pagesFAQ in MicrobiologyVenkatesh Arumugam100% (2)
- Blood and Immunity Study GuideDocument4 pagesBlood and Immunity Study GuideKimberly PollyNo ratings yet
- A Level Chemistry CIE: 1.3 Chemical BondingDocument79 pagesA Level Chemistry CIE: 1.3 Chemical Bondingeleonora josimovicNo ratings yet
- The Immune System: Department of Histology & EmbryologyDocument68 pagesThe Immune System: Department of Histology & EmbryologymookandpoppyNo ratings yet
- MicroparasitologyDocument28 pagesMicroparasitologyMj BrionesNo ratings yet
- Act.03 Cell Membrane Transport Part 1Document5 pagesAct.03 Cell Membrane Transport Part 1CatNo ratings yet
- FINALDocument4 pagesFINALKaren Mae Santiago AlcantaraNo ratings yet
- NursingBulletin Respiratory SystemDocument35 pagesNursingBulletin Respiratory Systemseigelystic100% (3)
- Alteration in Immune ResponseDocument29 pagesAlteration in Immune ResponsePachita AlexandruNo ratings yet
- Controlling Microbial Growth in Vivo Using Antimicrobial AgentsDocument30 pagesControlling Microbial Growth in Vivo Using Antimicrobial AgentsJen PanganibanNo ratings yet
- Anticholinergic MnemonicDocument1 pageAnticholinergic Mnemonictainah07No ratings yet
- Complete Blood CountDocument3 pagesComplete Blood CountivantototaeNo ratings yet
- Chapter 1: MicrobiologyDocument18 pagesChapter 1: MicrobiologyShanz HadjirulNo ratings yet
- Asthma: A. Practice EssentialsDocument8 pagesAsthma: A. Practice EssentialsCandha NurcahyaNo ratings yet
- Concept 3 Notes - Anatomy Basics For StudentsDocument39 pagesConcept 3 Notes - Anatomy Basics For StudentsKaranNo ratings yet
- Innate ImmunityDocument9 pagesInnate Immunitynascha dumpNo ratings yet
- Inflammatory Response PathophysiologyDocument34 pagesInflammatory Response PathophysiologyBernardo Mucha100% (1)
- Bacterial Flash Cards (Part 1 of 4)Document25 pagesBacterial Flash Cards (Part 1 of 4)Nafis Shamsid-DeenNo ratings yet
- Pharma Unit 1-2 Anti - Adrenergic DrugsDocument21 pagesPharma Unit 1-2 Anti - Adrenergic DrugsMIbrahimNo ratings yet
- Body Fluids (Post Lab)Document56 pagesBody Fluids (Post Lab)Dorothy Silva-JameroNo ratings yet
- Introduction of AnatomyDocument115 pagesIntroduction of AnatomyVina Kristi DiscarNo ratings yet
- Classification of BacteriaDocument10 pagesClassification of BacteriaSajid Ali100% (1)
- Drugs For Immune SystemDocument75 pagesDrugs For Immune SystemDhonat FlashNo ratings yet
- Maricris Q. Marquita-Uy R.N, M.DDocument42 pagesMaricris Q. Marquita-Uy R.N, M.DAdrian Mai AlanNo ratings yet
- Microbial Diseases of The Respiratory SystemDocument30 pagesMicrobial Diseases of The Respiratory SystemChristopher Eria Santiañez0% (1)
- General Characteristics of Neisseria Spp.Document62 pagesGeneral Characteristics of Neisseria Spp.hamada99967% (3)
- MICRO (1) Fundamentals of Microbiology - Dra - AbuevaDocument16 pagesMICRO (1) Fundamentals of Microbiology - Dra - AbuevaCindy Mae Macamay100% (1)
- Diabetes MellitusDocument16 pagesDiabetes MellitusApril Joy V. QuinoNo ratings yet
- Disorders of The Immune Response and Inflammation 3Document47 pagesDisorders of The Immune Response and Inflammation 3Cres Padua QuinzonNo ratings yet
- Classification of BacteriaDocument21 pagesClassification of BacteriaGosa MohammedNo ratings yet
- Nursing Interventions and Clinical Skills 5th Edition Perry Test BankDocument6 pagesNursing Interventions and Clinical Skills 5th Edition Perry Test BankSerenaNo ratings yet
- Differential White Blood Cell CountDocument20 pagesDifferential White Blood Cell CountNada hasan100% (2)
- Lesson Overview 20.2 ProkaryotesDocument38 pagesLesson Overview 20.2 ProkaryotesConnie Gomez100% (1)
- Physiology Finals ReviewerDocument22 pagesPhysiology Finals ReviewerDeomicah SolanoNo ratings yet
- Bio 2 Quiz ReviewerDocument2 pagesBio 2 Quiz ReviewerAlexandra RoderoNo ratings yet
- The Bacteria Singular: Bacterium) Are A Large Group of UnicellularDocument3 pagesThe Bacteria Singular: Bacterium) Are A Large Group of UnicellularlshyneNo ratings yet
- AsepsisDocument6 pagesAsepsisMarcus, RN100% (5)
- Overview of The Immune SystemDocument9 pagesOverview of The Immune SystemAyadi P. AkinwandeNo ratings yet
- Immune Response: Cell Biology and Its Application BI-1202Document35 pagesImmune Response: Cell Biology and Its Application BI-1202Eriani Wulandari100% (1)
- Viruses, Viroids, and PrionsDocument45 pagesViruses, Viroids, and PrionsJillian LaoNo ratings yet
- EENT Disorders StudentsDocument26 pagesEENT Disorders StudentsPye Antwan DelvaNo ratings yet
- Biochemistry: Molecules of LifeDocument20 pagesBiochemistry: Molecules of Lifeapi-464344582No ratings yet
- Adaptive Immunity - Humoral ImmunityDocument21 pagesAdaptive Immunity - Humoral ImmunityDaniel Atieh100% (1)
- Virus Family Envelope Stuff To Know Treatment/ VaccineDocument10 pagesVirus Family Envelope Stuff To Know Treatment/ Vaccinebtoy1No ratings yet
- Cardiovascular System (Report)Document2 pagesCardiovascular System (Report)Arlan AbraganNo ratings yet
- 03 Adaptive Immune SystemDocument14 pages03 Adaptive Immune SystemEnea NastriNo ratings yet
- CompleteBloodCounts NORMAL VALUEDocument4 pagesCompleteBloodCounts NORMAL VALUEWoro Hapsari Wahyuningrum100% (1)
- 6-Health Problems Common in PreschoolerDocument36 pages6-Health Problems Common in PreschoolerPam Lala100% (2)
- Man Meets Microbes: An Introduction to Medical MicrobiologyFrom EverandMan Meets Microbes: An Introduction to Medical MicrobiologyNo ratings yet
- Syphilis "The Great Pretender": By: Bruce MartinDocument28 pagesSyphilis "The Great Pretender": By: Bruce MartinChatie PipitNo ratings yet
- Katlu, A Traditional Functional Food From Gujarat, IndiaDocument10 pagesKatlu, A Traditional Functional Food From Gujarat, IndiaEditor IJTSRDNo ratings yet
- Masterclass ProgrammeDocument8 pagesMasterclass ProgrammewmogtNo ratings yet
- Hallmarks of Cancer: DR Arnab Kalita PG Fellow Head Neck Oncology BbciDocument40 pagesHallmarks of Cancer: DR Arnab Kalita PG Fellow Head Neck Oncology BbciArnab KalitaNo ratings yet
- Physical Therapy Approaches For Wound CareDocument94 pagesPhysical Therapy Approaches For Wound CarewirdhaNo ratings yet
- UWB Microwave Imaging For Non-Invasive Anomaly Detection in Human Lung and Possible Application in COVID-19 Diagnosis: A ReviewDocument5 pagesUWB Microwave Imaging For Non-Invasive Anomaly Detection in Human Lung and Possible Application in COVID-19 Diagnosis: A ReviewJulia GuintoNo ratings yet
- Opening Speech OutlineDocument2 pagesOpening Speech OutlineAnaNo ratings yet
- Legal Medicines LLOYD B. VALIENTEDocument27 pagesLegal Medicines LLOYD B. VALIENTEVal IronmanNo ratings yet
- Glypican-3 As A Useful Diagnostic Marker That Distinguishes Hepatocellular Carcinoma From Benign Hepatocellular Mass LesionsDocument6 pagesGlypican-3 As A Useful Diagnostic Marker That Distinguishes Hepatocellular Carcinoma From Benign Hepatocellular Mass LesionsBlake_jjNo ratings yet
- Cvac 176Document18 pagesCvac 176Helder LezamaNo ratings yet
- FNCP CHNDocument4 pagesFNCP CHNMariaNo ratings yet
- Phobic EncounterDocument1 pagePhobic EncounterEmanuel PeraltaNo ratings yet
- Fatal Vision GogglesDocument26 pagesFatal Vision Gogglesapi-282144674No ratings yet
- National NORCET-3 - FinalDocument90 pagesNational NORCET-3 - FinalSHIVANIINo ratings yet
- Chagas DiseaseDocument6 pagesChagas DiseaseFranciscoNo ratings yet
- 10.1016/j.ymgme.2016.11.045: Abstracts / Molecular Genetics and Metabolism 120 (2016) S17 - S145 S29Document2 pages10.1016/j.ymgme.2016.11.045: Abstracts / Molecular Genetics and Metabolism 120 (2016) S17 - S145 S29Larisa IliescuNo ratings yet
- THEORIES of CRIME CAUSATION NOTESDocument12 pagesTHEORIES of CRIME CAUSATION NOTESLombroso's follower100% (1)
- Air SamplingDocument10 pagesAir SamplingBudiawan PramonoNo ratings yet
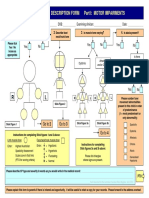
- Cerebral Palsy Description Form Part I: Motor ImpairmentsDocument2 pagesCerebral Palsy Description Form Part I: Motor Impairmentsnavuru5kNo ratings yet
- Bacillus Coagulans Probiotic of Choice Nutracos March April 2012Document3 pagesBacillus Coagulans Probiotic of Choice Nutracos March April 2012Gabriel ManriquezNo ratings yet
- Aiims Neet-Pg 2017 Pediatrics Mcqs 81-90Document4 pagesAiims Neet-Pg 2017 Pediatrics Mcqs 81-90DrHassan Ahmed Shaikh100% (1)
- Kerene - 2006 Ivory Coast Toxic Waste DumpDocument11 pagesKerene - 2006 Ivory Coast Toxic Waste DumpOPGJrNo ratings yet
- Aviagenbrief: Best Practice Management in The Absence of Antibiotics at The HatcheryDocument5 pagesAviagenbrief: Best Practice Management in The Absence of Antibiotics at The HatcherymahmudNo ratings yet
- NCBI Help Manuel 5Document53 pagesNCBI Help Manuel 5api-3725327No ratings yet
- Journal of The American Academy of Dermatology Volume 77 Issue 4 2017 (Doi 10.1016 - J.jaad.2017.01.036) Chaowattanapanit, Suteeraporn Silpa-Archa, Narumol Kohli, Inde - Postinflammatory HyperpigmeDocument15 pagesJournal of The American Academy of Dermatology Volume 77 Issue 4 2017 (Doi 10.1016 - J.jaad.2017.01.036) Chaowattanapanit, Suteeraporn Silpa-Archa, Narumol Kohli, Inde - Postinflammatory HyperpigmedikativiNo ratings yet
- Safety Awareness2Document23 pagesSafety Awareness2nasyaa1111No ratings yet
- Food at 40 YearsDocument14 pagesFood at 40 YearsOmeche I. OmecheNo ratings yet