Professional Documents
Culture Documents
Trauma Transfer Checklist
Trauma Transfer Checklist
Uploaded by
Tumee Dash0 ratings0% found this document useful (0 votes)
72 views1 pageCopyright
© © All Rights Reserved
Available Formats
PDF or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF or read online from Scribd
Download as pdf
0 ratings0% found this document useful (0 votes)
72 views1 pageTrauma Transfer Checklist
Trauma Transfer Checklist
Uploaded by
Tumee DashCopyright:
© All Rights Reserved
Available Formats
Download as PDF or read online from Scribd
Download as pdf
You are on page 1of 1
Trauma Transfer Checklist
For all trauma patients being transferred to a higher level Trauma Centre after contacting the Trauma Control
Physician
Continue to care:
Establish and maintain spinal immobilization (collar, board, straps and head blocks)
for all polytrauma
Document vital signs and neuro signs q15 min
Document vital signs and neuro signs q15 min
All documentation on Trauma Notes if available
Airway and breathing
Confirm ability to maintain adequate oxygenation/ventilation
* Consider need for ETT (GCS <8 or declining)
* Consider need for chest tube
IF intubated
Will require escort for ground transportation
Confirm ETT position via auscultation and/or endtidal CO.
Secure ETT
Insert Gastric tube
Provide sedation/analgesic prn
Circulation
* Control all active bleeding sites ~ consider pressure dressing
+ Establish 2 large bore peripheral IVs with extension tubing (Infusing
well? Secured?)
+ Ensure patient and fluids are warmed
* Apply pelvic stabilization (if applicable)
+ Insert Foley catheter with urometer
Disability
* Respond to any change in GCS or pupils
* Cover open fractures with saline dressing
* Splint extremity fractures (avoid air splints)
Consider logistics
Team required for transfer:
* If by ground: Consider RN, RRT, MD
+ If by Air: In consultation with ANB AirCare
Equipment required for ground transfer
* Airway management
+ Analgesics/sedatives/paralytics
Consult TCP for guidance
on the following:
Orders required for transfer
* Resuscitation: airway control/defibrillation
* Medications, including seizure control prn
* _ Blood/blood preducts and fluid
Documentation to accompany patient
* Photocopies of all ED physician notes, nurses’ notes & initial ambulance
call report
If overall patient condition deteriorates at any time pre-transfer,
re-establish contact with the Trauma Control Physician
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5820)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (845)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (898)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (349)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Digestion Skin Other PatternsDocument1 pageDigestion Skin Other PatternsTumee Dash100% (8)
- Acup Points by Dr. Zheng Tian ZhiDocument2 pagesAcup Points by Dr. Zheng Tian ZhiTumee Dash100% (1)
- BM ChartDocument2 pagesBM ChartTumee Dash100% (4)
- A Cup Otomo LogyDocument4 pagesA Cup Otomo LogyTumee DashNo ratings yet
- Trauma Theory Abbreviated Sandra BloomDocument14 pagesTrauma Theory Abbreviated Sandra BloomTumee DashNo ratings yet
- Heat HormonalDocument1 pageHeat HormonalTumee Dash100% (2)
- MedwebmonDocument5 pagesMedwebmonTumee DashNo ratings yet
- Pediatric Consultation and Transfer Guidelines: Washington State Department of Health Office of Community Health SystemsDocument11 pagesPediatric Consultation and Transfer Guidelines: Washington State Department of Health Office of Community Health SystemsTumee DashNo ratings yet
- TFA Bas Brochure Santa Fe 10Document2 pagesTFA Bas Brochure Santa Fe 10Tumee DashNo ratings yet
- DR Tan Chicago 2015 Seminar - Notes by Sam Shay - Day 1Document11 pagesDR Tan Chicago 2015 Seminar - Notes by Sam Shay - Day 1Tumee Dash100% (14)
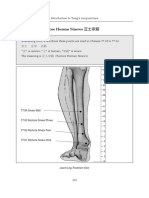
- Three Sinews: Restore Human Sinews 正士宗筋: Lower Leg, Posterior ViewDocument1 pageThree Sinews: Restore Human Sinews 正士宗筋: Lower Leg, Posterior ViewTumee DashNo ratings yet