Professional Documents
Culture Documents
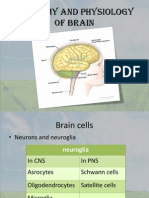
Basic Anatomy Brain
Basic Anatomy Brain
Uploaded by
DrSumit GandhiCopyright:
Available Formats
You might also like
- 1st Year Basic BSC Nursing Anatomy Word Notes in DetailsDocument2 pages1st Year Basic BSC Nursing Anatomy Word Notes in DetailsShreyas WalvekarNo ratings yet
- STUDY NOTES-The Urinary SystemDocument3 pagesSTUDY NOTES-The Urinary Systempeterneil75% (4)
- Gastrointestinal Anatomy and Physiology: The EssentialsFrom EverandGastrointestinal Anatomy and Physiology: The EssentialsJohn F. ReinusNo ratings yet
- Orthopedic Assessment For PhysiotherapistDocument3 pagesOrthopedic Assessment For Physiotherapistsenthilkumar76% (21)
- McKenzie Self-Treatments For SciaticaDocument3 pagesMcKenzie Self-Treatments For SciaticaSenthilkumar Thiyagarajan80% (5)
- Anaesthesia and Analgesia: Sample Chapter From BSAVA Manual of Canine and Feline 2nd EditionDocument19 pagesAnaesthesia and Analgesia: Sample Chapter From BSAVA Manual of Canine and Feline 2nd EditionMaca Muñoz EscobedoNo ratings yet
- Open Letter To Mark McGowan - Signed - PDFDocument4 pagesOpen Letter To Mark McGowan - Signed - PDFNathan Hondros100% (5)
- Introduction To Human PhysiologyDocument31 pagesIntroduction To Human PhysiologyKaranja Gitau100% (3)
- Body System ChecklistDocument6 pagesBody System Checklistapi-422967453No ratings yet
- Peripheral ANS Complete A To ZDocument65 pagesPeripheral ANS Complete A To ZSherwan R ShalNo ratings yet
- Introduction To Human Anatomy and PhysiologyDocument42 pagesIntroduction To Human Anatomy and PhysiologyDump Acc 2100% (1)
- Soojeedes Human Anatomy and Physiology PDFDocument119 pagesSoojeedes Human Anatomy and Physiology PDFmaxamed Buule IsaaqNo ratings yet
- Chapter 3 Basic Anatomy and PhysiologyDocument6 pagesChapter 3 Basic Anatomy and PhysiologyAini LutfiNo ratings yet
- Anatomy and PhysiologyDocument5 pagesAnatomy and PhysiologyKenNo ratings yet
- The Adrenal GlandDocument41 pagesThe Adrenal GlandRujha Haniena Ahmad RidzuanNo ratings yet
- Sheep Brain Observation LAB 2015Document4 pagesSheep Brain Observation LAB 2015Leo MatsuokaNo ratings yet
- Anatomy and Physiology Nursing Mnemonics TipsDocument8 pagesAnatomy and Physiology Nursing Mnemonics TipsariNo ratings yet
- Dr. Niranjan Murthy H L Asst. Prof. of Physiology SSMC, TumkurDocument39 pagesDr. Niranjan Murthy H L Asst. Prof. of Physiology SSMC, Tumkurnirilib100% (1)
- Anatomy and PhysiologyDocument5 pagesAnatomy and PhysiologyYuri De VeraNo ratings yet
- Respiratory System Anatomy and PhysiologyDocument19 pagesRespiratory System Anatomy and PhysiologyKBDNo ratings yet
- Nomad:Endocrine Physiology IntroductionDocument40 pagesNomad:Endocrine Physiology IntroductionDr.M.Anthony David100% (12)
- The A To Z of The HeartDocument259 pagesThe A To Z of The HeartAspenPharma100% (2)
- Thyroidglanddrdina 191014171805Document40 pagesThyroidglanddrdina 191014171805Ayesha100% (1)
- Physiology Final Exam QuestionsDocument3 pagesPhysiology Final Exam QuestionsRohini Selvarajah100% (1)
- Endocrine SystemDocument6 pagesEndocrine SystemAnny AlvrzNo ratings yet
- Chapt 05Document83 pagesChapt 05emmielyaNo ratings yet
- Lecture 3 Cardiovascular System 1Document54 pagesLecture 3 Cardiovascular System 1hafiz patah100% (1)
- Cell Biology Lecture NotesDocument108 pagesCell Biology Lecture NotesMert PolatNo ratings yet
- Nervous System - GeneralDocument84 pagesNervous System - GeneralAman SharmaNo ratings yet
- Cutaneous Innervation of HeadDocument4 pagesCutaneous Innervation of HeadAlexandros LazarouNo ratings yet
- 1 Cholinergic & Noradrenergic Transmission IDocument37 pages1 Cholinergic & Noradrenergic Transmission IGeraldine Ong100% (2)
- 337 Pdfsam NMS PhysiologyDocument166 pages337 Pdfsam NMS PhysiologydrpnnreddyNo ratings yet
- Endocrinology Learning Goals - IPHY 4440Document9 pagesEndocrinology Learning Goals - IPHY 4440Geline Joy D. SamillanoNo ratings yet
- Digestion and NutritionDocument122 pagesDigestion and NutritionMarkBell100% (5)
- Sources Hormone FunctionDocument2 pagesSources Hormone FunctionKatherine Joy MaderajeNo ratings yet
- Gland Hormone Function Target Organ (Name or Picture) : HypothalamusDocument2 pagesGland Hormone Function Target Organ (Name or Picture) : HypothalamusRoya ImaniNo ratings yet
- Central Nervous SystemDocument25 pagesCentral Nervous System786waqar786100% (1)
- Introduction To Physiology: General Physiology The Cell HomeostasisDocument38 pagesIntroduction To Physiology: General Physiology The Cell HomeostasisAnanta Subedi100% (1)
- Introduction To Anatomy and PhysiologyDocument43 pagesIntroduction To Anatomy and Physiologyaarti HingeNo ratings yet
- 05 Cardiovascular System PhysiologyDocument34 pages05 Cardiovascular System PhysiologyKaye Alyssa EnriquezNo ratings yet
- Kines Anatomy Ch. 14-16Document36 pagesKines Anatomy Ch. 14-16icedragon727No ratings yet
- Axial Skeleton PDFDocument48 pagesAxial Skeleton PDFSharadambigai SamarasanNo ratings yet
- Anatomy of The NeckDocument2 pagesAnatomy of The NeckTabassum ADNo ratings yet
- Anatomy and Physiology of BrainDocument21 pagesAnatomy and Physiology of BrainNavjot BrarNo ratings yet
- Autonomic Nervous System Bio FactsheetDocument4 pagesAutonomic Nervous System Bio FactsheetEleanor WilliamsNo ratings yet
- Chapter 2.1 - Nervous SystemDocument50 pagesChapter 2.1 - Nervous SystemHaizmeer BonzieNo ratings yet
- Lab11 Endocrine GlandsDocument16 pagesLab11 Endocrine Glandsapi-30634291950% (2)
- By: Rahul Malik January, 2016Document22 pagesBy: Rahul Malik January, 2016Rahul MalikNo ratings yet
- Malignant Hyperthermia: Review and Case Studies Holly Price, CRNADocument48 pagesMalignant Hyperthermia: Review and Case Studies Holly Price, CRNAnurse_kellyNo ratings yet
- Hormones TableDocument84 pagesHormones TableSaajid AmraNo ratings yet
- Sheep Brain Dissection With Labeled ImagesDocument13 pagesSheep Brain Dissection With Labeled Imagesapi-275510930No ratings yet
- The Origins of The History and Physical ExaminationDocument21 pagesThe Origins of The History and Physical ExaminationNEuRoLoGisT CoFFeeCuPNo ratings yet
- Urea CycleDocument8 pagesUrea CycleManohar PattarNo ratings yet
- Acid Base ImbalanceDocument50 pagesAcid Base ImbalanceDian Pratiwi BurnamaNo ratings yet
- Extraction of Eugenol From ClovesDocument1 pageExtraction of Eugenol From ClovesVivian Li100% (1)
- Pituitary GlandDocument15 pagesPituitary GlandPutri Agustin Mere100% (1)
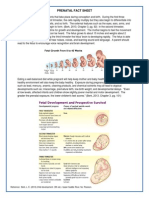
- Prenatal Fact SheetDocument2 pagesPrenatal Fact Sheetapi-276693463No ratings yet
- Peripheral Nervous System NotesDocument9 pagesPeripheral Nervous System NotesSaoirseNo ratings yet
- BloodDocument197 pagesBloodNimesh Sharma100% (1)
- LECTURE 2 Biological Basis of BehaviorDocument74 pagesLECTURE 2 Biological Basis of BehaviorColossal Heart50% (2)
- Muscular System WorksheetDocument1 pageMuscular System Worksheetapi-238647540No ratings yet
- Anatomy of The Head: Nervous System (PNS) - The Former Consists of The Brain and Spinal Cord, While The LatterDocument6 pagesAnatomy of The Head: Nervous System (PNS) - The Former Consists of The Brain and Spinal Cord, While The LatterHafiz Idul FitranulNo ratings yet
- Ankle TappingDocument4 pagesAnkle TappingSenthilkumar ThiyagarajanNo ratings yet
- Active Cycle Breathing Technique-Easy DemoDocument3 pagesActive Cycle Breathing Technique-Easy DemoSenthilkumar ThiyagarajanNo ratings yet
- Cervical ExerciseDocument1 pageCervical ExerciseSenthilkumar Thiyagarajan100% (1)
- Abdominal Stretching ExsDocument1 pageAbdominal Stretching ExsSenthilkumar ThiyagarajanNo ratings yet
- Postromedial Dic ProlapsDocument3 pagesPostromedial Dic ProlapsSenthilkumar Thiyagarajan100% (1)
- Abdominal IncisionsDocument9 pagesAbdominal IncisionsSenthilkumar ThiyagarajanNo ratings yet
- Above Knee Amputation Good One PDFDocument9 pagesAbove Knee Amputation Good One PDFSenthilkumar Thiyagarajan100% (1)
- Aids To The Examination of Peripheral Nervous SystemDocument67 pagesAids To The Examination of Peripheral Nervous SystemSenthilkumar ThiyagarajanNo ratings yet
- Anatomymnemonics PDFDocument28 pagesAnatomymnemonics PDFSenthilkumar ThiyagarajanNo ratings yet
- C:/Documents and Settings/student/Desktop/physiotherapy Protocol FOR HEMIPLEGIC PDFDocument13 pagesC:/Documents and Settings/student/Desktop/physiotherapy Protocol FOR HEMIPLEGIC PDFSenthilkumar ThiyagarajanNo ratings yet
- Post Natal Exercise PrescriptionDocument8 pagesPost Natal Exercise PrescriptionSenthilkumar ThiyagarajanNo ratings yet
- Above Knee Amputation Exc PDFDocument5 pagesAbove Knee Amputation Exc PDFSenthilkumar ThiyagarajanNo ratings yet
- All Orthopedic TestsDocument7 pagesAll Orthopedic Testschandran2679No ratings yet
- !!!-MBS Skin Item Numbers Nov 2016Document3 pages!!!-MBS Skin Item Numbers Nov 2016abu ubaidahNo ratings yet
- Patient ProfileDocument3 pagesPatient ProfileKhaled GharaibehNo ratings yet
- 1 KMCDocument4 pages1 KMCahid3safitraNo ratings yet
- Achilles TendonDocument49 pagesAchilles TendonArifHidayatNo ratings yet
- Optimizing Fluid Therapy in Shock.10Document6 pagesOptimizing Fluid Therapy in Shock.10Paulo Victor100% (1)
- Full Download Introduction To Operations and Supply Chain Management 3rd Edition Bozarth Test BankDocument36 pagesFull Download Introduction To Operations and Supply Chain Management 3rd Edition Bozarth Test Bankcoraleementgen1858100% (48)
- EAU Guidelines On Urolithiasis 2018 Large Text PDFDocument88 pagesEAU Guidelines On Urolithiasis 2018 Large Text PDFYennie AyuNo ratings yet
- DrugsDocument61 pagesDrugsPrabir SahaNo ratings yet
- Prediction Score For Postoperative NeurologicDocument10 pagesPrediction Score For Postoperative NeurologicLusy Octavia SaputriNo ratings yet
- Ashleigh Resume 2016Document2 pagesAshleigh Resume 2016api-355193947No ratings yet
- Complete Denture Copy Technique-A Practical ApplicationDocument6 pagesComplete Denture Copy Technique-A Practical ApplicationDiana Ecaterina NechiforNo ratings yet
- Scanned Dictionary PDFDocument16 pagesScanned Dictionary PDFDennia AlexandraNo ratings yet
- Bowel Preparation: Penyusun: Nicholas David Marcellis Pembimbing: Dr. Mangalindung O, SPBDocument18 pagesBowel Preparation: Penyusun: Nicholas David Marcellis Pembimbing: Dr. Mangalindung O, SPBbocah_britpopNo ratings yet
- Progesterone in Prevention of PreeclampsiaDocument12 pagesProgesterone in Prevention of PreeclampsiaVishal WahaneNo ratings yet
- Nursing Practice IIIDocument8 pagesNursing Practice IIIClarence AnescoNo ratings yet
- Glyceryl Trinitrate Ointment As A Potential Treatment For Primary VaginismusDocument2 pagesGlyceryl Trinitrate Ointment As A Potential Treatment For Primary VaginismusFernando Bonat BarbieriNo ratings yet
- Downloadfile 2Document416 pagesDownloadfile 2SayanDuttaNo ratings yet
- General Hospital Prog.Document6 pagesGeneral Hospital Prog.AlamiN RayMan ArNobNo ratings yet
- The Ergot AlkaloidsDocument9 pagesThe Ergot AlkaloidsAna LucaNo ratings yet
- Titanium Ring & Tandem Set AL13017000 2011-04-06 enDocument8 pagesTitanium Ring & Tandem Set AL13017000 2011-04-06 enBhaveen JoshiNo ratings yet
- The Difficult Parent: A Reflective Pediatrician's Response : Case DR Martin T. SteinDocument6 pagesThe Difficult Parent: A Reflective Pediatrician's Response : Case DR Martin T. SteinJames WangNo ratings yet
- 2018 Medtronic Analyst Meeting RTG Presentation - MarthaDocument16 pages2018 Medtronic Analyst Meeting RTG Presentation - MarthamedtechyNo ratings yet
- Diagnostic Services:-2D Echo, Audiometry, Bronchoscopy, CTDocument196 pagesDiagnostic Services:-2D Echo, Audiometry, Bronchoscopy, CTLalita NaiduNo ratings yet
- Abortion Nursing Care Planning and ManagementDocument11 pagesAbortion Nursing Care Planning and ManagementSyamsiah ChandrawatiNo ratings yet
- Tamil Nadu Dental Council: Affix Your Recent P.P Size PhotoDocument3 pagesTamil Nadu Dental Council: Affix Your Recent P.P Size PhotokerminkNo ratings yet
- Home Birth Setting Versus Hospital Birth SettingDocument4 pagesHome Birth Setting Versus Hospital Birth SettingAmanda Bonita PersaudNo ratings yet
- Indian Public Health Standard IIDocument19 pagesIndian Public Health Standard IIKailash NagarNo ratings yet
- Nursing Journal: Labor and DeliveryDocument1 pageNursing Journal: Labor and DeliveryAngelika PadawanNo ratings yet
Basic Anatomy Brain
Basic Anatomy Brain
Uploaded by
DrSumit GandhiCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Basic Anatomy Brain
Basic Anatomy Brain
Uploaded by
DrSumit GandhiCopyright:
Available Formats
25
2 Basic Anatomy and Physiology of the Human Brain
This chapter contains some basic background on the anatomy and physiology of the human brain relevant to this project. The final section focuses on the neonatal brain and some common pathologies.
2.1 Anatomy of the head
The human nervous system consists of the central nervous system (CNS) and peripheral nervous system (PNS). The former consists of the brain and spinal cord, while the latter composes the nerves extending to and from the brain and spinal cord. The primary functions of the nervous system are to monitor, integrate (process) and respond to information inside and outside the body. The brain consists of soft, delicate, non-replaceable neural tissue. It is supported and protected by the surrounding skin, skull, meninges and cerebrospinal fluid.
Figure 21 Skin and underlying subcutaneous tissue. (Reproduced from [Marieb 1991]).
26
Skin The skin constitutes a protective barrier against physical damage of underlying tissues, invasion of hazardous chemical and bacterial substances and, through the activity of its sweat glands and blood vessels, it helps to maintain the body at a constant temperature. Together with the sweat and oil glands, hairs and nails it forms a set of organs called the integumentary system. Figure 21 shows a cross-section of the skin and underlying subcutaneous tissue. The skin consists of an outer, protective layer, the epidermis and an inner layer, the dermis. While the top layer of the epidermis, the stratum corneum, consists of dead cells, the dermis is composed of vascularised fibrous connective tissue. The subcutaneous tissue, located underneath the skin, is primarily composed of adipose tissue (fat). Skull Depending on their shape, bones are classified as long, short, flat or irregular. Bones of different types contain different proportions of the two types of osseous tissue: compact and spongy bone. While the former has a smooth structure, the latter is composed of small needle-like or flat pieces of bone called trabeculae, which form a network filled with red or yellow bone marrow. Most skull bones are flat and consist of two parallel compact bone surfaces, with a layer of spongy bone sandwiched between. The spongy bone layer of flat bones (the diplo) predominantly contains red bone marrow and hence has a high concentration of blood.
Figure 22 Skull. (Reproduced from [Marieb 1991]).
The skull is a highly complex structure consisting of 22 bones altogether. These can be divided into two sets, the cranial bones (or cranium) and the facial bones. While the latter form the framework of the face, the cranial bones form the cranial cavity that encloses and protects the brain. All bones of the adult skull are firmly connected by sutures. Figure 22 shows the most important bones of the skull. The frontal bone forms the forehead and contains the frontal sinuses, which are air filled cells within the bone. Most superior and lateral aspects of the skull are formed by the parietal bones while the occipital bone forms the posterior aspects. The base of the occipital bone contains the foramen magnum, which
27
is a large hole allowing the inferior part of the brain to connect to the spinal cord. The remaining bones of the cranium are the temporal, sphenoid and ethmoid bones. Meninges The meninges (Figure 23) are three connective tissue membranes enclosing the brain and the spinal cord. Their functions are to protect the CNS and blood vessels, enclose the venous sinuses, retain the cerebrospinal fluid, and form partitions within the skull. The outermost meninx is the dura mater, which encloses the arachnoid mater and the innermost pia mater.
Figure 23 Meninges. (Reproduced from [Marieb 1991]).
Figure 24 Cerebrospinal Fluid. (Reproduced from [Marieb 1991]).
28
Cerebrospinal fluid Cerebrospinal fluid (CSF) is a watery liquid similar in composition to blood plasma. It is formed in the choroid plexuses and circulates through the ventricles into the subarachnoid space, where it is returned to the dural venous sinuses by the arachnoid villi. The prime purpose of the CSF is to support and cushion the brain and help nourish it. Figure 24 illustrates the flow of CSF through the central nervous system.
2.2 Major regions of the brain and their functions
The major regions of the brain (Figure 25) are the cerebral hemispheres, diencephalon, brain stem and cerebellum.
Figure 25 Major Regions of the Brain. (Reproduced from [Marieb 1991]).
Cerebral hemispheres The cerebral hemispheres (Figure 26), located on the most superior part of the brain, are separated by the longitudinal fissure. They make up approximately 83% of total brain mass, and are collectively referred to as the cerebrum. The cerebral cortex constitutes a 2-4 mm thick grey matter surface layer and, because of its many convolutions, accounts for about 40% of total brain mass. It is responsible for conscious behaviour and contains three different functional areas: the motor areas, sensory areas and association areas. Located internally are the white matter, responsible for communication between cerebral areas and between the cerebral cortex and lower regions of the CNS, as well as the basal nuclei (or basal ganglia), involved in controlling muscular movement. Diencephalon The diencephalon is located centrally within the forebrain. It consists of the thalamus, hypothalamus and epithalamus, which together enclose the third ventricle. The thalamus acts as a grouping and relay station for sensory inputs ascending to the sensory cortex and association areas. It also mediates motor activities, cortical arousal and memories. The hypothalamus, by controlling the autonomic (involuntary) nervous system, is responsible for maintaining the bodys homeostatic balance. Moreover it forms a part of the limbic system, the emotional brain. The epithalamus consists of the pineal gland and the CSFproducing choroid plexus.
29
Figure 26 Major Regions of the cerebral hemispheres. (Reproduced from [Marieb 1991]).
Brain stem The brain stem is similarly structured as the spinal cord: it consists of grey matter surrounded by white matter fibre tracts. Its major regions are the midbrain, pons and medulla oblongata. The midbrain, which surrounds the cerebral aqueduct, provides fibre pathways between higher and lower brain centres, contains visual and auditory reflex and subcortical motor centres. The pons is mainly a conduction region, but its nuclei also contribute to the regulation of respiration and cranial nerves. The medulla oblongata takes an important role as an autonomic reflex centre involved in maintaining body homeostasis. In particular, nuclei in the medulla regulate respiratory rhythm, heart rate, blood pressure and several cranial nerves. Moreover, it provides conduction pathways between the inferior spinal cord and higher brain centres. Cerebellum The cerebellum, which is located dorsal to the pons and medulla, accounts for about 11% of total brain mass. Like the cerebrum, it has a thin outer cortex of grey matter, internal white matter, and small, deeply situated, paired masses (nuclei) of grey matter. The cerebellum processes impulses received from the cerebral motor cortex, various brain stem nuclei and sensory receptors in order to appropriately control skeletal muscle contraction, thus giving smooth, coordinated movements.
2.3 The cerebral circulatory system
Blood is transported through the body via a continuous system of blood vessels. Arteries carry oxygenated blood away from the heart into capillaries supplying tissue cells. Veins collect the blood from the capillary bed and carry it back to the heart. The main purpose of blood flow through body tissues is to deliver oxygen and nutrients to and waste from the cells, exchange gas in the lungs, absorb nutrients from the digestive tract, and help forming urine in the kidneys. All the circulation besides the heart and the pulmonary circulation is called the systemic circulation. Since it is the ultimate aim of this research project to image cerebral oxygenation and haemodynamics some aspects of the cerebral circulatory system are described below.
30
Figure 27 Major cerebral arteries and the circle of Willis. (Reproduced from [Marieb 1991]).
Blood supply to the brain Figure 27 shows an overview of the arterial system supplying the brain. The major arteries are the vertebral and internal carotid arteries. The two posterior and single anterior communicating arteries form the circle of Willis, which equalises blood pressures in the brains anterior and posterior regions, and protects the brain from damage should one of the arteries become occluded. However, there is little communication between smaller arteries on the brains surface. Hence occlusion of these arteries usually results in localised tissue damage. Cerebral haemodynamics The cardiac output is about 5 l/min of blood for a resting adult. Blood flow to the brain is about 14% of this, or 700 ml/min. For any part of the body, the blood flow can be calculated using the simple formula Pressure Blood flow = (2.1) Resistance Pressure in the arteries is generated by the heart which pumps blood from its left ventricle into the aorta. (Since pressure was historically measured with a mercury manometer, the units are commonly expressed in terms of [mm Hg], although the official SI unit is the Pascal [Pa].) Resistance arises from friction, and is proportional to the following expression Vessel Length Resistance Viscosity (2.2) (Vessel Diameter) 4 Hence blood flow is slowest in the small vessels of the capillary bed, thus allowing time for the exchange of nutrients and oxygen to surrounding tissue by diffusion through the capillary walls. Approximately 75% of total blood volume is stored in the veins which, because of their high capacity, act as reservoirs. Their walls distend and contract in response to the amount of blood available in the circulation. However, the function of cerebral veins,
31
formed from sinuses in the dura mater, is somewhat different from other veins of the body, as they are non-collapsible. Autoregulation [Panerai 1998] describes autoregulation of blood flow in the cerebral vascular bed as the mechanism by which cerebral blood flow (CBF) tends to remain relatively constant despite changes in cerebral perfusion pressure (CPP). With a constant metabolic demand, changes in CPP or arterial blood pressure that would increase or reduce CBF, are compensated by adjusting the vascular resistance. This maintains a constant O2 supply and constant CBF. Therefore cerebral autoregulation allows the blood supply to the brain to match its metabolic demand and also to protect cerebral vessels against excessive flow due to arterial hypertension. Cerebral blood flow is autoregulated much better than in almost any other organ. Even for arterial pressure variations between 50 and 150 mm Hg, CBF only changes by a few percent. This can be accomplished because the arterial vessels are typically able to change their diameter about 4-fold, corresponding to a 256-fold change in blood flow. Only when the brain is very active is there an exception to the close matching of blood flow to metabolism, which can rise by up to 30-50% in the affected areas. It is an aim of PET, functional MRI, near infrared spectroscopy (NIRS), and, possibly, near infrared imaging, to detect or image such localised changes in cortical activity and associated blood flow.
2.4 Structure and pathologies of the neonatal brain
Having introduced some basics of the anatomy and physiology of the adult brain, this section focuses on the specific differences in the neonate, as well as common neonatal pathologies which have motivated the construction of an instrument capable of imaging cerebral oxygenation, blood volume and, possibly, myelination. The embryonic brain and spinal cord develop from the neural tube, which is formed by the fourth week of pregnancy. The brain grows immensely in both size and complexity during pregnancy and even soon after birth. Because a membranous skull restricts expansion, the forebrain is bent towards the brain stem, and the cerebral hemispheres almost completely envelop the diencephalon and midbrain. Moreover, the spatial restrictions cause the cerebral hemispheres to increase their surface area by becoming highly convoluted such that about two thirds of its surface are hidden in its folds. The skull bones of the foetus and neonate are soft and the sutures are not yet fused. Hence the skull is very flexible and deforms under light pressure. Brain development of the foetus, neonate and infant are more thoroughly reviewed by [Herschkowitz 1988]. Compared to the adult, neonates have a smaller head size (ca. 6-12 cm in diameter), thinner surface tissue, skull and CSF layers, lower scattering coefficients of grey and white matter (due to lesser myelination in the case of white matter), as well as a comparatively small mismatch between the two (see also Table 41). These anatomical features are all favourable to NIR imaging. The neonatal skull, because it is less mineralised, may also have a lower scattering coefficient, but there is no data at present. All these factors greatly benefit penetration of light deep into the white matter and enable measurements to be made across the head, which is essential for tomographic imaging. Arterial and venous haemoglobin saturation values for the foetus in utero are relatively low at 56 % and 18% [Rooth 1963], respectively, compared to about 97% and 67% for adults. This is because there is a gradient in oxygen concentration across the placenta which ensures diffusion of sufficient amounts of oxygen from maternal blood into the foetal bloodstream. A higher oxygen affinity of neonatal haemoglobin (dissociation curve shifted to the left, c.f. Figure 43) compensates for this. Over a period of about 6 months after
32
delivery the neonatal haemoglobin is gradually substituted by the adult haemoglobin, which has a lower oxygen affinity. The autoregulation mechanism of the (adult) brain was discussed in the previous section. However, in the newborn infant, and particularly in the very preterm infant, there is no consensus on whether, or to what extent, autoregulation in the brain occurs. It is also not clear what effect ischaemia has on cerebral blood flow and the evolution of haemorrhage. Neurodevelopmental disorders in some preterm infants are due to either hypoxicischaemic damage to the periventricular white matter, or to intraventricular haemorrhage and its consequences. The period of highest risk is between 26 and 32 weeks of gestation. In preterm infants the majority of haemorrhages occur into the ventricles and the surrounding white matter, the periventricular region. Hypoxic-ischaemic damage is caused by cerebral underperfusion, often combined with a global oxygen deficiency due to an impaired lung function. It also affects the periventricular white matter, which is thought to be a result of the following two effects: Increased vulnerability due to high metabolic demands at this phase of the brain development. The area is at a watershed of perfusion from the territories of the posterior and middle cerebral arteries (c.f. Figure 27). Enduring neurodevelopmental disorders can lead to diminished neurological function in later life, and in particular spasticity, since motor fibres run through this region of the white matter. Given the potential of the premature infants developing brain to repair some damage, spasticity is often restricted to stiff limbs and/or subtle learning disabilities. Cerebral damage in the mature infant is most commonly a result of perinatal (birth) asphyxia, leading initially to cerebral oedema (resulting in compressed ventricles and flattening of the convolutions of the brain), and later to tissue necrosis (tissue death) and apoptosis (cell suicide). The subcortical white matter, basal ganglia, cerebellum and brainstem are the areas predominantly affected, frequently leading to learning disabilities or global developmental delay and cerebral palsy. Sample neonatal brain images, including that of a patient with hypoxic-ischaemia (Figure 34), can be found in chapter 3, which describes various conventional imaging modalities. A comprehensive review of common neurologic disorders is given by [Hill 1996].
33
34
You might also like
- 1st Year Basic BSC Nursing Anatomy Word Notes in DetailsDocument2 pages1st Year Basic BSC Nursing Anatomy Word Notes in DetailsShreyas WalvekarNo ratings yet
- STUDY NOTES-The Urinary SystemDocument3 pagesSTUDY NOTES-The Urinary Systempeterneil75% (4)
- Gastrointestinal Anatomy and Physiology: The EssentialsFrom EverandGastrointestinal Anatomy and Physiology: The EssentialsJohn F. ReinusNo ratings yet
- Orthopedic Assessment For PhysiotherapistDocument3 pagesOrthopedic Assessment For Physiotherapistsenthilkumar76% (21)
- McKenzie Self-Treatments For SciaticaDocument3 pagesMcKenzie Self-Treatments For SciaticaSenthilkumar Thiyagarajan80% (5)
- Anaesthesia and Analgesia: Sample Chapter From BSAVA Manual of Canine and Feline 2nd EditionDocument19 pagesAnaesthesia and Analgesia: Sample Chapter From BSAVA Manual of Canine and Feline 2nd EditionMaca Muñoz EscobedoNo ratings yet
- Open Letter To Mark McGowan - Signed - PDFDocument4 pagesOpen Letter To Mark McGowan - Signed - PDFNathan Hondros100% (5)
- Introduction To Human PhysiologyDocument31 pagesIntroduction To Human PhysiologyKaranja Gitau100% (3)
- Body System ChecklistDocument6 pagesBody System Checklistapi-422967453No ratings yet
- Peripheral ANS Complete A To ZDocument65 pagesPeripheral ANS Complete A To ZSherwan R ShalNo ratings yet
- Introduction To Human Anatomy and PhysiologyDocument42 pagesIntroduction To Human Anatomy and PhysiologyDump Acc 2100% (1)
- Soojeedes Human Anatomy and Physiology PDFDocument119 pagesSoojeedes Human Anatomy and Physiology PDFmaxamed Buule IsaaqNo ratings yet
- Chapter 3 Basic Anatomy and PhysiologyDocument6 pagesChapter 3 Basic Anatomy and PhysiologyAini LutfiNo ratings yet
- Anatomy and PhysiologyDocument5 pagesAnatomy and PhysiologyKenNo ratings yet
- The Adrenal GlandDocument41 pagesThe Adrenal GlandRujha Haniena Ahmad RidzuanNo ratings yet
- Sheep Brain Observation LAB 2015Document4 pagesSheep Brain Observation LAB 2015Leo MatsuokaNo ratings yet
- Anatomy and Physiology Nursing Mnemonics TipsDocument8 pagesAnatomy and Physiology Nursing Mnemonics TipsariNo ratings yet
- Dr. Niranjan Murthy H L Asst. Prof. of Physiology SSMC, TumkurDocument39 pagesDr. Niranjan Murthy H L Asst. Prof. of Physiology SSMC, Tumkurnirilib100% (1)
- Anatomy and PhysiologyDocument5 pagesAnatomy and PhysiologyYuri De VeraNo ratings yet
- Respiratory System Anatomy and PhysiologyDocument19 pagesRespiratory System Anatomy and PhysiologyKBDNo ratings yet
- Nomad:Endocrine Physiology IntroductionDocument40 pagesNomad:Endocrine Physiology IntroductionDr.M.Anthony David100% (12)
- The A To Z of The HeartDocument259 pagesThe A To Z of The HeartAspenPharma100% (2)
- Thyroidglanddrdina 191014171805Document40 pagesThyroidglanddrdina 191014171805Ayesha100% (1)
- Physiology Final Exam QuestionsDocument3 pagesPhysiology Final Exam QuestionsRohini Selvarajah100% (1)
- Endocrine SystemDocument6 pagesEndocrine SystemAnny AlvrzNo ratings yet
- Chapt 05Document83 pagesChapt 05emmielyaNo ratings yet
- Lecture 3 Cardiovascular System 1Document54 pagesLecture 3 Cardiovascular System 1hafiz patah100% (1)
- Cell Biology Lecture NotesDocument108 pagesCell Biology Lecture NotesMert PolatNo ratings yet
- Nervous System - GeneralDocument84 pagesNervous System - GeneralAman SharmaNo ratings yet
- Cutaneous Innervation of HeadDocument4 pagesCutaneous Innervation of HeadAlexandros LazarouNo ratings yet
- 1 Cholinergic & Noradrenergic Transmission IDocument37 pages1 Cholinergic & Noradrenergic Transmission IGeraldine Ong100% (2)
- 337 Pdfsam NMS PhysiologyDocument166 pages337 Pdfsam NMS PhysiologydrpnnreddyNo ratings yet
- Endocrinology Learning Goals - IPHY 4440Document9 pagesEndocrinology Learning Goals - IPHY 4440Geline Joy D. SamillanoNo ratings yet
- Digestion and NutritionDocument122 pagesDigestion and NutritionMarkBell100% (5)
- Sources Hormone FunctionDocument2 pagesSources Hormone FunctionKatherine Joy MaderajeNo ratings yet
- Gland Hormone Function Target Organ (Name or Picture) : HypothalamusDocument2 pagesGland Hormone Function Target Organ (Name or Picture) : HypothalamusRoya ImaniNo ratings yet
- Central Nervous SystemDocument25 pagesCentral Nervous System786waqar786100% (1)
- Introduction To Physiology: General Physiology The Cell HomeostasisDocument38 pagesIntroduction To Physiology: General Physiology The Cell HomeostasisAnanta Subedi100% (1)
- Introduction To Anatomy and PhysiologyDocument43 pagesIntroduction To Anatomy and Physiologyaarti HingeNo ratings yet
- 05 Cardiovascular System PhysiologyDocument34 pages05 Cardiovascular System PhysiologyKaye Alyssa EnriquezNo ratings yet
- Kines Anatomy Ch. 14-16Document36 pagesKines Anatomy Ch. 14-16icedragon727No ratings yet
- Axial Skeleton PDFDocument48 pagesAxial Skeleton PDFSharadambigai SamarasanNo ratings yet
- Anatomy of The NeckDocument2 pagesAnatomy of The NeckTabassum ADNo ratings yet
- Anatomy and Physiology of BrainDocument21 pagesAnatomy and Physiology of BrainNavjot BrarNo ratings yet
- Autonomic Nervous System Bio FactsheetDocument4 pagesAutonomic Nervous System Bio FactsheetEleanor WilliamsNo ratings yet
- Chapter 2.1 - Nervous SystemDocument50 pagesChapter 2.1 - Nervous SystemHaizmeer BonzieNo ratings yet
- Lab11 Endocrine GlandsDocument16 pagesLab11 Endocrine Glandsapi-30634291950% (2)
- By: Rahul Malik January, 2016Document22 pagesBy: Rahul Malik January, 2016Rahul MalikNo ratings yet
- Malignant Hyperthermia: Review and Case Studies Holly Price, CRNADocument48 pagesMalignant Hyperthermia: Review and Case Studies Holly Price, CRNAnurse_kellyNo ratings yet
- Hormones TableDocument84 pagesHormones TableSaajid AmraNo ratings yet
- Sheep Brain Dissection With Labeled ImagesDocument13 pagesSheep Brain Dissection With Labeled Imagesapi-275510930No ratings yet
- The Origins of The History and Physical ExaminationDocument21 pagesThe Origins of The History and Physical ExaminationNEuRoLoGisT CoFFeeCuPNo ratings yet
- Urea CycleDocument8 pagesUrea CycleManohar PattarNo ratings yet
- Acid Base ImbalanceDocument50 pagesAcid Base ImbalanceDian Pratiwi BurnamaNo ratings yet
- Extraction of Eugenol From ClovesDocument1 pageExtraction of Eugenol From ClovesVivian Li100% (1)
- Pituitary GlandDocument15 pagesPituitary GlandPutri Agustin Mere100% (1)
- Prenatal Fact SheetDocument2 pagesPrenatal Fact Sheetapi-276693463No ratings yet
- Peripheral Nervous System NotesDocument9 pagesPeripheral Nervous System NotesSaoirseNo ratings yet
- BloodDocument197 pagesBloodNimesh Sharma100% (1)
- LECTURE 2 Biological Basis of BehaviorDocument74 pagesLECTURE 2 Biological Basis of BehaviorColossal Heart50% (2)
- Muscular System WorksheetDocument1 pageMuscular System Worksheetapi-238647540No ratings yet
- Anatomy of The Head: Nervous System (PNS) - The Former Consists of The Brain and Spinal Cord, While The LatterDocument6 pagesAnatomy of The Head: Nervous System (PNS) - The Former Consists of The Brain and Spinal Cord, While The LatterHafiz Idul FitranulNo ratings yet
- Ankle TappingDocument4 pagesAnkle TappingSenthilkumar ThiyagarajanNo ratings yet
- Active Cycle Breathing Technique-Easy DemoDocument3 pagesActive Cycle Breathing Technique-Easy DemoSenthilkumar ThiyagarajanNo ratings yet
- Cervical ExerciseDocument1 pageCervical ExerciseSenthilkumar Thiyagarajan100% (1)
- Abdominal Stretching ExsDocument1 pageAbdominal Stretching ExsSenthilkumar ThiyagarajanNo ratings yet
- Postromedial Dic ProlapsDocument3 pagesPostromedial Dic ProlapsSenthilkumar Thiyagarajan100% (1)
- Abdominal IncisionsDocument9 pagesAbdominal IncisionsSenthilkumar ThiyagarajanNo ratings yet
- Above Knee Amputation Good One PDFDocument9 pagesAbove Knee Amputation Good One PDFSenthilkumar Thiyagarajan100% (1)
- Aids To The Examination of Peripheral Nervous SystemDocument67 pagesAids To The Examination of Peripheral Nervous SystemSenthilkumar ThiyagarajanNo ratings yet
- Anatomymnemonics PDFDocument28 pagesAnatomymnemonics PDFSenthilkumar ThiyagarajanNo ratings yet
- C:/Documents and Settings/student/Desktop/physiotherapy Protocol FOR HEMIPLEGIC PDFDocument13 pagesC:/Documents and Settings/student/Desktop/physiotherapy Protocol FOR HEMIPLEGIC PDFSenthilkumar ThiyagarajanNo ratings yet
- Post Natal Exercise PrescriptionDocument8 pagesPost Natal Exercise PrescriptionSenthilkumar ThiyagarajanNo ratings yet
- Above Knee Amputation Exc PDFDocument5 pagesAbove Knee Amputation Exc PDFSenthilkumar ThiyagarajanNo ratings yet
- All Orthopedic TestsDocument7 pagesAll Orthopedic Testschandran2679No ratings yet
- !!!-MBS Skin Item Numbers Nov 2016Document3 pages!!!-MBS Skin Item Numbers Nov 2016abu ubaidahNo ratings yet
- Patient ProfileDocument3 pagesPatient ProfileKhaled GharaibehNo ratings yet
- 1 KMCDocument4 pages1 KMCahid3safitraNo ratings yet
- Achilles TendonDocument49 pagesAchilles TendonArifHidayatNo ratings yet
- Optimizing Fluid Therapy in Shock.10Document6 pagesOptimizing Fluid Therapy in Shock.10Paulo Victor100% (1)
- Full Download Introduction To Operations and Supply Chain Management 3rd Edition Bozarth Test BankDocument36 pagesFull Download Introduction To Operations and Supply Chain Management 3rd Edition Bozarth Test Bankcoraleementgen1858100% (48)
- EAU Guidelines On Urolithiasis 2018 Large Text PDFDocument88 pagesEAU Guidelines On Urolithiasis 2018 Large Text PDFYennie AyuNo ratings yet
- DrugsDocument61 pagesDrugsPrabir SahaNo ratings yet
- Prediction Score For Postoperative NeurologicDocument10 pagesPrediction Score For Postoperative NeurologicLusy Octavia SaputriNo ratings yet
- Ashleigh Resume 2016Document2 pagesAshleigh Resume 2016api-355193947No ratings yet
- Complete Denture Copy Technique-A Practical ApplicationDocument6 pagesComplete Denture Copy Technique-A Practical ApplicationDiana Ecaterina NechiforNo ratings yet
- Scanned Dictionary PDFDocument16 pagesScanned Dictionary PDFDennia AlexandraNo ratings yet
- Bowel Preparation: Penyusun: Nicholas David Marcellis Pembimbing: Dr. Mangalindung O, SPBDocument18 pagesBowel Preparation: Penyusun: Nicholas David Marcellis Pembimbing: Dr. Mangalindung O, SPBbocah_britpopNo ratings yet
- Progesterone in Prevention of PreeclampsiaDocument12 pagesProgesterone in Prevention of PreeclampsiaVishal WahaneNo ratings yet
- Nursing Practice IIIDocument8 pagesNursing Practice IIIClarence AnescoNo ratings yet
- Glyceryl Trinitrate Ointment As A Potential Treatment For Primary VaginismusDocument2 pagesGlyceryl Trinitrate Ointment As A Potential Treatment For Primary VaginismusFernando Bonat BarbieriNo ratings yet
- Downloadfile 2Document416 pagesDownloadfile 2SayanDuttaNo ratings yet
- General Hospital Prog.Document6 pagesGeneral Hospital Prog.AlamiN RayMan ArNobNo ratings yet
- The Ergot AlkaloidsDocument9 pagesThe Ergot AlkaloidsAna LucaNo ratings yet
- Titanium Ring & Tandem Set AL13017000 2011-04-06 enDocument8 pagesTitanium Ring & Tandem Set AL13017000 2011-04-06 enBhaveen JoshiNo ratings yet
- The Difficult Parent: A Reflective Pediatrician's Response : Case DR Martin T. SteinDocument6 pagesThe Difficult Parent: A Reflective Pediatrician's Response : Case DR Martin T. SteinJames WangNo ratings yet
- 2018 Medtronic Analyst Meeting RTG Presentation - MarthaDocument16 pages2018 Medtronic Analyst Meeting RTG Presentation - MarthamedtechyNo ratings yet
- Diagnostic Services:-2D Echo, Audiometry, Bronchoscopy, CTDocument196 pagesDiagnostic Services:-2D Echo, Audiometry, Bronchoscopy, CTLalita NaiduNo ratings yet
- Abortion Nursing Care Planning and ManagementDocument11 pagesAbortion Nursing Care Planning and ManagementSyamsiah ChandrawatiNo ratings yet
- Tamil Nadu Dental Council: Affix Your Recent P.P Size PhotoDocument3 pagesTamil Nadu Dental Council: Affix Your Recent P.P Size PhotokerminkNo ratings yet
- Home Birth Setting Versus Hospital Birth SettingDocument4 pagesHome Birth Setting Versus Hospital Birth SettingAmanda Bonita PersaudNo ratings yet
- Indian Public Health Standard IIDocument19 pagesIndian Public Health Standard IIKailash NagarNo ratings yet
- Nursing Journal: Labor and DeliveryDocument1 pageNursing Journal: Labor and DeliveryAngelika PadawanNo ratings yet