Professional Documents
Culture Documents
Thyroid Hormone Synthesis
Thyroid Hormone Synthesis
Uploaded by
BRTate1124100%(2)100% found this document useful (2 votes)
379 views1 pageThe synthesis of thyroid hormones takes place in the follicular cells of the thyroid gland through a multi-step process. Iodine from the blood is actively transported into the follicular cells and oxidized to form iodine. Thyroglobulin, a protein produced by the endoplasmic reticulum, transports tyrosine residues to the cell membrane where iodine attaches to form the hormone precursors T3 and T4. Lysosomes then break down thyroglobulin, releasing the hormones into capillaries while recycling iodine. TSH stimulates this entire synthesis and secretion process.
Original Description:
Copyright
© Attribution Non-Commercial (BY-NC)
Available Formats
DOC or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe synthesis of thyroid hormones takes place in the follicular cells of the thyroid gland through a multi-step process. Iodine from the blood is actively transported into the follicular cells and oxidized to form iodine. Thyroglobulin, a protein produced by the endoplasmic reticulum, transports tyrosine residues to the cell membrane where iodine attaches to form the hormone precursors T3 and T4. Lysosomes then break down thyroglobulin, releasing the hormones into capillaries while recycling iodine. TSH stimulates this entire synthesis and secretion process.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as DOC or read online from Scribd
Download as doc
100%(2)100% found this document useful (2 votes)
379 views1 pageThyroid Hormone Synthesis
Thyroid Hormone Synthesis
Uploaded by
BRTate1124The synthesis of thyroid hormones takes place in the follicular cells of the thyroid gland through a multi-step process. Iodine from the blood is actively transported into the follicular cells and oxidized to form iodine. Thyroglobulin, a protein produced by the endoplasmic reticulum, transports tyrosine residues to the cell membrane where iodine attaches to form the hormone precursors T3 and T4. Lysosomes then break down thyroglobulin, releasing the hormones into capillaries while recycling iodine. TSH stimulates this entire synthesis and secretion process.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as DOC or read online from Scribd
Download as doc
You are on page 1of 1
2.
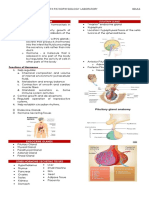
Synthesis and release of thyroid hormones
The synthesis in the thyroid gland takes place in the following way:
A. Dietary iodine (I2) is reduced to iodide (I-) in the stomach and gut is rapidly absorbed
and circulates as iodide.
B. Follicular cells in the thyroid gland possess an active iodide trap that requires and
concentrates iodide from the circulating blood Iodide is transported into the cell against
an electrochemical gradient (more than 50 mV) by a Na+-I--symport. The iodide pump is
linked to a Na+-K+-pump, which requires energy in the form of oxidative phosphorylation
(ATP) and is inhibited by ouabain. The thyroid absorption of iodide is also inhibited by
negative ions (such as perchlorate, pertechnetate, thiocyanate and nitrate), because they
compete with the iodide at the trap. In the follicular cell, iodide passes down its
electrochemical gradient through the apical membrane and into the follicular colloid.
Iodide is instantly oxidised – with hydrogen peroxide as oxidant - by a thyroid
peroxidase to atomic or molecular iodine (I0 or I2) at the colloid surface of the apical
membrane. Thiouracil and sulfonamides block this peroxidase.
C. The rough endoplasmic reticulum synthesises a large storage molecule called
thyroglobulin. This compound is build up by a long peptide chain with tyrosine units and
a carbohydrate unit completed by the Golgi apparatus. Iodide-free thyroglobulin is
transported in vesicles to the apical membrane, where they fuse with the membrane and
finally release thyroglobulin at the apical membrane.
D. At the apical membrane the oxidised iodide is attached to the tyrosine units (L-
tyrosine) in thyroglobulin at one or two positions, forming the hormone precursors mono-
iodotyrosine (MIT), and di-iodotyrosine (DIT), respectively. This and the following
reactions are dependent on thyroid peroxidase in the presence of hydrogen peroxide -both
located at the apical membrane. As MIT couples to DIT it produces tri-iodothyronine
(3,5,3`-T3), whereas two DIT molecules form tetra-iodothyronine (T4), or thyroxine.
These two molecules are the two thyroid hormones. Small amounts of the inactive
reverse T3 (3,3`,5`- T3) is also synthesised.
E. Each thyroglobulin molecule contains up to 4 residues of T4 and zero to one T3.
Thyroglobulin is retrieved back into the follicular cell as colloid droplets by pinocytosis.
Pseudopods engulf a pocket of colloid. These colloid droplets pass towards the basal
membrane and fuse with lysosomes forming phagolysosomes.
F. Lysosomal exopeptidases break the binding between thyroglobulin and T4 (or T3).
Large quantities of T4 are released to the capillary blood. Only minor quantities of T3
are secreted from the thyroid gland.
G. The proteolysis of thyroglobulin also releases MIT and DIT. These molecules are
deiodinated by the enzyme deiodinase, whereby iodide can be reused into T4 or T3.
Normally, only few intact thyroglobulin molecules leave the follicular cells.
H. TSH stimulates almost all processes involved in thyroid hormone synthesis and
secretion.
You might also like
- 1 - Introduction To The Gene Keys - Gene KeysDocument1 page1 - Introduction To The Gene Keys - Gene KeysCarmen AndersonNo ratings yet
- Mechanical Completion and Handover ProcedureDocument3 pagesMechanical Completion and Handover Procedureleong100% (1)
- Patai, Wigs - The Myth of The Jewish RaceDocument392 pagesPatai, Wigs - The Myth of The Jewish Racee-jajam100% (2)
- Thyroid and Its Functions: DR Raghuveer ChoudharyDocument61 pagesThyroid and Its Functions: DR Raghuveer ChoudharyPhysiology by Dr RaghuveerNo ratings yet
- Synthesis of Thyroid HormonesDocument1 pageSynthesis of Thyroid HormonesAndioNo ratings yet
- Thyroid GlandDocument78 pagesThyroid GlandSatyam ChoubeyNo ratings yet
- Thyroid Gland 1 UMST White BackgroundDocument41 pagesThyroid Gland 1 UMST White Backgroundعوض الكريمNo ratings yet
- Thyroid GlandDocument52 pagesThyroid Glandhamid mohammedNo ratings yet
- Thyroid HormoneDocument53 pagesThyroid Hormoneambrosekiplangat6No ratings yet
- 3 - Thyroid Metabolism-OkDocument12 pages3 - Thyroid Metabolism-Okcaroline.fragniere6464No ratings yet
- Thyroid HormonesDocument7 pagesThyroid Hormonesgoldengoal19079No ratings yet
- Endocrine System NotesDocument6 pagesEndocrine System NotesHannah Grace CorveraNo ratings yet
- Doc3 - Objetivo 3, 6 e 7-Thyroid Metabolic HormonesDocument13 pagesDoc3 - Objetivo 3, 6 e 7-Thyroid Metabolic HormonesBruna SofiaNo ratings yet
- 10 Diversity of Endocrine System IIDocument23 pages10 Diversity of Endocrine System IIcutethoybaNo ratings yet
- Regulation of Oxidative PhosphorylationDocument14 pagesRegulation of Oxidative Phosphorylationmaaz629No ratings yet
- Endocrine Physiology: ThyroidDocument49 pagesEndocrine Physiology: ThyroidriaNo ratings yet
- Thyroid Gland and Calcium HomeostasisDocument5 pagesThyroid Gland and Calcium HomeostasisAlexis BondadNo ratings yet
- GH Chap 3Document13 pagesGH Chap 3Shellz2428No ratings yet
- AcetylcholineDocument2 pagesAcetylcholineHarshitNo ratings yet
- EN2 - HypothyroidismDocument17 pagesEN2 - Hypothyroidismsbobine.imsNo ratings yet
- Guyton and Hall Textbook of Medical Physiology 14th Ed - ExportedDocument13 pagesGuyton and Hall Textbook of Medical Physiology 14th Ed - Exportedhassnfiras04No ratings yet
- Topic3.3 Physiology Thyroid HormoneDocument7 pagesTopic3.3 Physiology Thyroid HormoneRen AlvNo ratings yet
- THYROID GLAND ModuleDocument8 pagesTHYROID GLAND ModuleBJ BermasNo ratings yet
- VND Ms-Powerpoint&rendition 1Document49 pagesVND Ms-Powerpoint&rendition 1Muhammad SamiNo ratings yet
- Report Group 11Document5 pagesReport Group 11Boyd benson kayomboNo ratings yet
- Anatomy and PhysiologyDocument3 pagesAnatomy and PhysiologyDavid RefuncionNo ratings yet
- Bioenergetics and Oxidative PhosphorylationDocument32 pagesBioenergetics and Oxidative PhosphorylationShimmering MoonNo ratings yet
- Superior Thyroid Artery (Right and Left) Dipercabangkan Dari External Carotid Artery Inferior Thyroid Artery (Right and Left) Arises From The Thyrocervical Trunk (Which in TurnDocument9 pagesSuperior Thyroid Artery (Right and Left) Dipercabangkan Dari External Carotid Artery Inferior Thyroid Artery (Right and Left) Arises From The Thyrocervical Trunk (Which in TurnDapot SianiparNo ratings yet
- 1 - Pharmacology - Thyroid & Antibone DrugsDocument20 pages1 - Pharmacology - Thyroid & Antibone DrugsSoc Gerren TuasonNo ratings yet
- 2s Finals Pharma BeshyDocument60 pages2s Finals Pharma BeshyJohanei Mae PeraltaNo ratings yet
- Thyroxine and OxytocinDocument53 pagesThyroxine and OxytocinUshna SiddiquiNo ratings yet
- 3 Use Thyroid Gland Use TTDocument55 pages3 Use Thyroid Gland Use TTMathy MtenjeNo ratings yet
- Biological Oxidation ETCDocument37 pagesBiological Oxidation ETCsanofazal786No ratings yet
- West African College of Physicians: Physiology of The Thyroid GlandDocument21 pagesWest African College of Physicians: Physiology of The Thyroid GlandRuchi VatwaniNo ratings yet
- PhysioLec 8 Thyroid Metabolic Hormones (Dr. Queenie)Document4 pagesPhysioLec 8 Thyroid Metabolic Hormones (Dr. Queenie)Lafayette DelantarNo ratings yet
- Bio - Biological Oxidation and ETCDocument39 pagesBio - Biological Oxidation and ETCMahmoud hilmyNo ratings yet
- The Thyroid Gland PDFDocument13 pagesThe Thyroid Gland PDFDEVANGI PANCHALNo ratings yet
- Metabolic Endocrinology (Week-2)Document8 pagesMetabolic Endocrinology (Week-2)wasimsafdarNo ratings yet
- Thyroid and Anti Thyroid DrugDocument5 pagesThyroid and Anti Thyroid Drugtamberahul1256No ratings yet
- Anatomy of ThyroidDocument9 pagesAnatomy of ThyroidStephanie Villanueva AdvinculaNo ratings yet
- HormonesDocument9 pagesHormonesChandanaNo ratings yet
- 15 PhotosynthesisDocument10 pages15 PhotosynthesisEarl Adam LambacoNo ratings yet
- DykensDocument5 pagesDykensy.lteifNo ratings yet
- 1 Oxidative PhosphorylationDocument10 pages1 Oxidative PhosphorylationRoland ToroNo ratings yet
- Biology Notes Unit TwoDocument158 pagesBiology Notes Unit TwoBlohsh KeenenNo ratings yet
- Cells and Sugars 09 Mitochondria and Ox Phos StudentDocument21 pagesCells and Sugars 09 Mitochondria and Ox Phos StudenttyhbbhhNo ratings yet
- Ch. 9 Biological OxidationDocument71 pagesCh. 9 Biological OxidationKrishna KanthNo ratings yet
- Cellular Energy TransactionsDocument3 pagesCellular Energy TransactionsDrAmit VermaNo ratings yet
- Photosynthesis Cell Biology FileDocument16 pagesPhotosynthesis Cell Biology FileRei KaplanNo ratings yet
- Photosynthesis Cell Biology FileDocument16 pagesPhotosynthesis Cell Biology FileRei KaplanNo ratings yet
- The Thyroid GlandDocument74 pagesThe Thyroid GlandAboubakar Moalim Mahad moh'dNo ratings yet
- BBT 301 Unit 3a: by Dr. Sharad Agrawal Asst. Prof., SBSR Sharda UniversityDocument18 pagesBBT 301 Unit 3a: by Dr. Sharad Agrawal Asst. Prof., SBSR Sharda UniversityDristi Namchoom GohainNo ratings yet
- Thyroid Gland: Synthesis and ChemistryDocument3 pagesThyroid Gland: Synthesis and ChemistryWay FarerNo ratings yet
- Biology Lets Crack With MeDocument11 pagesBiology Lets Crack With MeFairy QueenNo ratings yet
- Cellular RespirationDocument25 pagesCellular RespirationLouie Joice MartinezNo ratings yet
- Antithyroid Drugs by Sejal Khuman Advanced phARMACOLGY 2Document29 pagesAntithyroid Drugs by Sejal Khuman Advanced phARMACOLGY 2Sejal khumanNo ratings yet
- Energy Supply To Heart 3 IIDocument31 pagesEnergy Supply To Heart 3 IIHamza ShoaibNo ratings yet
- Photosynthesis: Leaves and Leaf StructureDocument11 pagesPhotosynthesis: Leaves and Leaf StructureMatthew BetinolNo ratings yet
- Antithyroid DrugsDocument32 pagesAntithyroid DrugsLUMUMBA OluwatomisinNo ratings yet
- Title: Electron Transport System (Aerobic)Document4 pagesTitle: Electron Transport System (Aerobic)GISRemoteSensingNo ratings yet
- Photosynthesis COMPLETEDocument44 pagesPhotosynthesis COMPLETEsantoshnairsNo ratings yet
- Thyroid, Obesity and Metabolism: Exploring Links Between Thyroid Function, Obesity, Metabolism and LifestyleFrom EverandThyroid, Obesity and Metabolism: Exploring Links Between Thyroid Function, Obesity, Metabolism and LifestyleNo ratings yet
- LESSON PLAN On Planning Sanjaya Mam WalaDocument5 pagesLESSON PLAN On Planning Sanjaya Mam WalaAshish GuptaNo ratings yet
- Bs en 15651-1 2012Document30 pagesBs en 15651-1 2012Veronica GozdalskaNo ratings yet
- Biology Investigatory Project: To Study The Working and Functions of The Human HeartDocument19 pagesBiology Investigatory Project: To Study The Working and Functions of The Human HeartADCHAYAGANESH S50% (2)
- VL2020210500609 DaDocument24 pagesVL2020210500609 Dashubhamrpawar2021No ratings yet
- Conducting A Literature Review Jennifer RowleyDocument6 pagesConducting A Literature Review Jennifer Rowleyafdtwudac100% (1)
- Phonetic and Phonological Differences Between British and American EnglishDocument6 pagesPhonetic and Phonological Differences Between British and American EnglishKrizz TambagoNo ratings yet
- Logos (Heraclitus, Fragment B 50) : Ouk E Uou DXXD Tou Adyou Dkouoavraq OocpdvDocument20 pagesLogos (Heraclitus, Fragment B 50) : Ouk E Uou DXXD Tou Adyou Dkouoavraq OocpdvdugNo ratings yet
- Application of Raman Spectroscopy For Characterization of Natural Stonesludge WasteDocument4 pagesApplication of Raman Spectroscopy For Characterization of Natural Stonesludge WasteKateřina InachisNo ratings yet
- Summary of The R by Peter Weill and Stephanie L. Woerner Published in The Summer of 2015Document3 pagesSummary of The R by Peter Weill and Stephanie L. Woerner Published in The Summer of 2015RoheenNo ratings yet
- Heat and Mass PDFDocument4 pagesHeat and Mass PDFonyxNo ratings yet
- Transiluminador BenchtopDocument11 pagesTransiluminador BenchtopWendy Lilian Gómez MonsivaisNo ratings yet
- Unilabs Covid-19 U222021221 PDFDocument1 pageUnilabs Covid-19 U222021221 PDFFatih GündoganNo ratings yet
- Mathematics Question BankDocument38 pagesMathematics Question BankSurabhi H NNo ratings yet
- Cap BitucoatDocument2 pagesCap BitucoatMedrar TareqNo ratings yet
- Mw61a Ti All Sv6.01a enDocument11 pagesMw61a Ti All Sv6.01a enpradeepNo ratings yet
- DetailaDocument5 pagesDetailaNoneta MotsiNo ratings yet
- Amity International School, Noida Class-Ix Ch. Gravitation (Term-Ii) (2022-23)Document3 pagesAmity International School, Noida Class-Ix Ch. Gravitation (Term-Ii) (2022-23)Priya AgrawalNo ratings yet
- Proonounss AntecedentDocument5 pagesProonounss Antecedentclairesrpn16No ratings yet
- What Is OsteosarcomaDocument3 pagesWhat Is OsteosarcomadhinahafizNo ratings yet
- 12 - Deflection by Conjugate Beam MethodDocument7 pages12 - Deflection by Conjugate Beam MethodFrancis Ko Badongen-Cawi Tabaniag Jr.No ratings yet
- Quantitative Chapter 7 - Indices and SurdsDocument9 pagesQuantitative Chapter 7 - Indices and SurdsDeeksha KapoorNo ratings yet
- Tech 1 34Document34 pagesTech 1 34Mohamed JaleelNo ratings yet
- Lec 01 IntroductionDocument41 pagesLec 01 IntroductionHasib RyanNo ratings yet
- Encapsulation Zno Nanoparticles by Using Beeswax: Roya Namdariyan, Afshin Farahbakhsh and Hossain Alizade GolestaniDocument3 pagesEncapsulation Zno Nanoparticles by Using Beeswax: Roya Namdariyan, Afshin Farahbakhsh and Hossain Alizade GolestaniSahil GuptaNo ratings yet
- Trigonometry Formulas For Class 10: Utm - Source Website&utm - Medium Byjusclasses&utm - Campaign Topbar)Document12 pagesTrigonometry Formulas For Class 10: Utm - Source Website&utm - Medium Byjusclasses&utm - Campaign Topbar)Luv AggarwalNo ratings yet
- Failure Modes of Rocks Under Uniaxial Compression Tests - HBRP PublicationDocument8 pagesFailure Modes of Rocks Under Uniaxial Compression Tests - HBRP PublicationVijay KNo ratings yet
- TPG - CT 1Document2 pagesTPG - CT 1HBr26No ratings yet