Professional Documents
Culture Documents
Dislocation Shoulder Good
Dislocation Shoulder Good
Uploaded by
Zahiera NajibOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Dislocation Shoulder Good
Dislocation Shoulder Good
Uploaded by
Zahiera NajibCopyright:
Available Formats
http://morphopedics.wikidot.
com/shoulder-dislocation
I. Description
True shoulder dislocation occurs when the head of the humerus becomes dislodged from the glenoid cavity. It is the joint that is most prevalent for dislocation. The shoulder normally dislocates anteriorly but it can also be displaced posteriorly or inferiorly. If the humerus is dislocated once, there is a greater chance that it can later be dislocated again, especially if the person is 30 years or younger. Many times when a shoulder dislocation occurs, ligaments and other tissues are damaged and movement of the humerus is highly limited. Once the shoulder is relocated normal function is usually restored but structures around the glenoid area may still be damaged. The two most common injuries associated with an anteriorly dislocated shoulder are a Bankart lesion and a Hill-Sachs lesion. A Bankart lesion occurs when the anterior labrum is torn. A Hill-Sachs lesion takes place when the humeral head impacts the glenoid fossa causing a fracture of the head of the humerus. These lesions can also occur in the posterior joint with posterior dislocation, and are known as reverse Bankart and Hill-Sachs lesions.1,2,4 All About Shoulder Dislocation
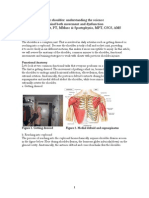
II. Anatomy
The anatomy of the glenohumeral joint consists of the humeral head of the humerus and the glenoid fossa of the scapula. These two structures together create a cavity with a surrounding capsule. Attached to the glenoid cavity is the glenoid labrum which acts as a fibrocartilaginous bumper between the humeral head and the glenoid fossa. The capsule is supported by the rotator cuff muscles which are the supraspinatus, infraspinatus, subscapularis, and teres minor. The deltoid muscle and the biceps tendon also offer some support for the capsule. The superior glenohumeral ligament (SGHL), middle glenohumeral ligament (MGHL), and inferior glenohumeral ligament (IGHL) are three structures that provide support as well.3
III. Prevalence & Etiology
Anterior dislocations occur in 98% of shoulder dislocations. The other 2% of shoulder dislocations take place posteriorly. The majority of dislocations occur from a traumatic incidence. Forced external rotation and abduction of the humerus is the most prevalent cause of anterior dislocation. About 5% occur atraumatically, usually because of excessive laxity of the capsule. Recurrence of dislocation can also be problematic. In people aged 20 years or younger, dislocation can recur in 66% to 100% of cases. For people between 20 and 40 years old 13% to 63% of dislocations recur and for people 40 years and over 0% to 16% dislocate their shoulder again. 4
IV. Clinical Presentation
Most patients will state that they heard a popping sound at the time of injury. Anterior dislocation is the most common form of shoulder dislocation and normally the patient will have had their arm abducted and externally rotated at the time of injury. It may also present this way in clinic if it has not been relocated. They may have also felt numbness or tingling down the arms after injury if a nerve was affected. If the shoulder was not put back into place, then AROM will be decreased and painful, and the humeral head may be palpable anteriorly. Brusing may be visible if blood vessels were ruptured. With a posterior dislocation, ROM and strength tests are usually normal unless a rotator cuff muscle or nerve has been damaged. Crepitus may be present when the shoulder is internally rotated and the posterior joint line may be tender to palpation. If the humeral head has not been relocated, the humerus may appear internally rotated and will not be able to externally rotate.1,2,5
V. Diagnostic Tests
With both anterior and posterior shoulder instability, an anteroposterior (AP) view and a Y-view image should be obtained. The AP view can show anterior dislocation and a reverse Hill-Sachs sign for posterior dislocation. The Yview can show a Hill-Sachs lesion for anterior dislocation and a posterior dislocation.6,7 Anterior Dislocation
Hill-Sach's Lesion
Posterior Dislocation
Reverse Hill-Sach's Lesion
CT scans can also be used to assess the integrity of the labrum. An MRI shows Bankart lesions and any soft tissue injuries.6,7 CT Labrum
MRI Bankart Lesion
VI. Special Orthopedic Tests
Anterior Instability The three tests that are most reliable for anterior shoulder instability are the apprehension, relocation, and anterior release tests.8,9 Apprehension Test Pain or apprehension indicate a positive test. Relocation Test Decreased pain or apprehension indicate a positive test. Anterior Release Test Pain or apprehension upon release of the humeral head indicate a positive test.
Posterior Instability The two most reliable tests for posterior instability are the posterior stress test and the jerk test.5 Posterior Stress Test (Posterior Apprehension Test) Pain or apprehension indicates a positive test. Jerk Test A clunk, or jerk, upon axial load or horizontal adduction indicates a positive test. Another clunk may also occur upon relocation (horizontal abduction).
VII. Conservative Treatment
Immobilization
If immobilization is the sole treatment, the arm is usually immobilized anywhere from 2 to 6 weeks. Combined with exercise, it will usually be immobilized for a lesser time period. For anterior dislocations, the humerus is normally placed in a traditional internally rotated position. However, new studies are being conducted which may show that placing the humerus in an externally rotated position may be more beneficial for healing especially if a Bankart lesion is present. For posterior dislocations the humerus is normally placed in a slightly extended and externally rotated position.4,5,10 Exercise Exercise is normally used in conjunction with immobilization. The shoulder will usually be immobilized for 1-3 weeks. During this time period, wrist and elbow range of motion exercises can be performed so that it is not lost. After immobilization, range of motion of the shoulder can begin followed by strengthening. In the case of anterior
dislocation, strengthening programs should emphasize the internal rotators, adductors, scapular muscles. For posterior dislocation, programs to strengthen the external rotators, posterior deltoid, and scapular muscles are performed. Conservative protocols may take up to 3 months for full recovery.4,5,10 click on the link below to view PT management of shoulder dislocation:
Physical Therapy Management of Shoulder Dislocation VIII. Surgical Treatment
For an anterior dislocation, open or arthroscopic surgeries may be performed. During an open Bankart repair, the subscapularis is detached so that the labrum can be repaired on the anterior glenoid. The shoulder is reduced and sutures are applied to hold it in place. In an arthroscopic procedure, portals are made and the anterior labrum is reattached and the humerus is reduced. For a posterior dislocation, open surgery or arthroscopic surgery may be performed as well. In an open posteroinferior capsular shift, the humerus is placed in 20 degrees of abduction. The incision is made in the posterior axilla. The humerus is placed back into the capsule and the posterior capsule is repaired. During arthroscopic surgery, three or four portals are used anteriorly and posteriorly. If a reverse Bankart lesion is present it is then repaired with sutures. The humerus is placed back into the capsule and the portals are stitched back up. Both open and arthroscopic surgeries have their advantages and disadvantages. With open surgery there is a lesser rate of redislocation. However, there is usually a greater loss in external rotation than with arthroscopic surgery. Treatment following surgery is basically the same as a conservative protocol consisting of range of motion and strengthening exercises for the shoulder. Depending on the type of surgery, full recovery time may take anywhere from 4 to 9 months.4,5,10 Arthroscopic Bankart Repair Animation
IX. Additional Web-Based Resources
For information all about shoulder dislocations visit: http://www.ori.org.au/bonejoint/shoulder/contents.htm and http://shoulderdislocation.net/ For an extensive list of special orthopedic tests visit: http://www.shoulderdoc.co.uk/article.asp?section=497. For treatment protocols visit: http://www.pt.armstrong.edu/davies/pdf/Anterior%20Shoulder%20Dislocation.pdf and http://www.tsaog.com/phyForms/Acute%20Anterior%20Shoulder%20Dislocation%20Physical%20Therapy%2 0Protocol.pdf
X. References
1. Seade EL, Josey R. Shoulder Dislocation. Medscape Reference Website. Available at:http://emedicine.medscape.com/article/93323-overview. Accessed October 28th, 2011. 2. Mayo Clinic Staff. Dislocated Shoulder. Mayo Foundation for Medical Education and Research. Available at:http://www.mayoclinic.com/health/dislocated-shoulder/DS00597. Accessed November 26th, 2011. 3. Sizer PS, Phelps V, Gilbert K. Diagnosis and management of the painful shoulder. Part 1: clinical anatomy and pathomechanics. Pain Practice, 2003;3(1):40-57. 4. Hayes K, Callanan M, Walton J, Paxinos A, Murrell G. Shoulder instability: management and rehabilitation. Journal of Orthopaedic & Sports Physical Therapy, 2002;32(10):1-13. 5. Millett PJ, Clavert PC, Hatch RGF, Warner JJP. Recurrent posterior shoulder instability. Journal of the American Academy of Orthopaedic Surgeons, 2006;14(8):464-476. 6. Satterwhite YE. Evaluation and management of recurrent anterior shoulder instability. Journal of Athletic Training, 2000;35(3):273-277. 7. Tseng GY, Peh WCG. Shoulder Dislocation Imaging. Medscape Reference Website. Available at:http://emedicine.medscape.com/article/395520-overview. Accessed November 26, 2011. 8. Hegedus EJ, Goode A, Campbell S, Morin A, Tamaddoni M, Moorman CT, Cook C. Physical examination tests of the shoulder: a systematic review with meta-analysis of individual tests. Journal of Sports Medicine,
2008;42(1):80-92. 9. Farber AJ, Castillo R, Clough M, Bahk M, McFarland EG. Clinical assessment of three common tests for traumatic anterior shoulder instability. Journal of Bone and Joint Surgery, 2006;88(7):1467-1474. 10. Handoll HHG, Al-Maiyah MA. Surgical versus non-surgical treatment for acute anterior shoulder dislocation. The Cochrane Collaboration, 2010;(5):1-34.
You might also like
- Shoulder Dislocation and Reduction - UpToDateDocument64 pagesShoulder Dislocation and Reduction - UpToDateCatedra 2018No ratings yet
- Erik Dalton Blog: Scoliosis and Massage TherapyDocument15 pagesErik Dalton Blog: Scoliosis and Massage TherapyMAR1601No ratings yet
- Microcontroller Based Digital Control - Dogan IbrahimDocument191 pagesMicrocontroller Based Digital Control - Dogan IbrahimMuuo WambuaNo ratings yet
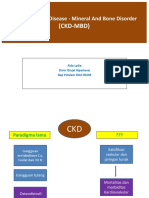
- CKD MBD - Dr. AidaDocument41 pagesCKD MBD - Dr. AidaFITRINo ratings yet
- RulebookDocument296 pagesRulebookRogerio Lucena100% (2)
- Runner Design Guide Lines-Issue 5Document15 pagesRunner Design Guide Lines-Issue 5sivanandp100% (1)
- Shoulder Dislocation Background: Shoulder Dislocations Traumatic InjuryDocument7 pagesShoulder Dislocation Background: Shoulder Dislocations Traumatic Injuryanastasiaanggita_265No ratings yet
- Assignment 14a Final PaperDocument11 pagesAssignment 14a Final Paperapi-665233380No ratings yet
- William C. Cottrell, MD AbstractDocument4 pagesWilliam C. Cottrell, MD AbstractmalaNo ratings yet
- Rotator Cuff InjuryDocument29 pagesRotator Cuff InjuryArko duttaNo ratings yet
- Fracture-Dislocation of The Hip-KaizarDocument69 pagesFracture-Dislocation of The Hip-KaizarKaizar Ennis100% (1)
- Aaos 2002Document120 pagesAaos 2002Yusufa ArdyNo ratings yet
- Shoulder DislocationDocument28 pagesShoulder DislocationQueen SofiaNo ratings yet
- Rotator CuffDocument46 pagesRotator CuffLiza Perez- Pagatpatan100% (2)
- Coxa SaltansDocument6 pagesCoxa SaltansignashyaNo ratings yet
- The Shoulder: Understanding The Science Behind Both Movement and Dysfunction by Chris Gellert, PT, MMusc & Sportsphysio, MPT, CSCS, AMSDocument9 pagesThe Shoulder: Understanding The Science Behind Both Movement and Dysfunction by Chris Gellert, PT, MMusc & Sportsphysio, MPT, CSCS, AMSChrisGellertNo ratings yet
- Shoulder DislocationDocument12 pagesShoulder DislocationSam Witwicky50% (2)
- Dislokasi Panggul & BahuDocument42 pagesDislokasi Panggul & BahuAnton TrihartantoNo ratings yet
- Joint Instability: Hendradi Khumarga SPOT. FICSDocument48 pagesJoint Instability: Hendradi Khumarga SPOT. FICSJoshua ObrienNo ratings yet
- SM Bankart Repair PDFDocument6 pagesSM Bankart Repair PDFRano AskarNo ratings yet
- Glenoid LabrumDocument26 pagesGlenoid LabrumluizamgoNo ratings yet
- Shoulder Dislocation SubluxationDocument4 pagesShoulder Dislocation SubluxationSisca Dwi AgustinaNo ratings yet
- Hip Dislocation ResearchDocument8 pagesHip Dislocation Researchapi-268839011No ratings yet
- Reversetotalshoulder Arthroplasty: Early Results of Forty-One Cases and A Review of The LiteratureDocument11 pagesReversetotalshoulder Arthroplasty: Early Results of Forty-One Cases and A Review of The LiteratureBruno FellipeNo ratings yet
- SM-192627 LatarJet Procedure Rehab FinalDocument7 pagesSM-192627 LatarJet Procedure Rehab FinalNico BrantesNo ratings yet
- Shoulder 6 ExaminationDocument21 pagesShoulder 6 ExaminationAnil SoodNo ratings yet
- Shoulder Arthroplasty WIC - Dr. LSDocument56 pagesShoulder Arthroplasty WIC - Dr. LSDifitasari Cipta Perdana100% (1)
- The Shoulder Replacement Book: Frank Norberg, MDDocument8 pagesThe Shoulder Replacement Book: Frank Norberg, MDRammah EmadNo ratings yet
- Shoulder ExamDocument24 pagesShoulder ExamMuhammad FahmyNo ratings yet
- Fractures of The Upper LimbDocument20 pagesFractures of The Upper LimbWendy Francisca Borquez PerezNo ratings yet
- Biomechanics of The Shoulder: Dennis L. Hart, Mpa, PT, Stephen W. Carmichael, PHDTDocument6 pagesBiomechanics of The Shoulder: Dennis L. Hart, Mpa, PT, Stephen W. Carmichael, PHDTPrem KumarNo ratings yet
- Anterior Labral (Bankart) RepairsDocument13 pagesAnterior Labral (Bankart) RepairsChris CarmenNo ratings yet
- 34995Document27 pages34995Truly GracevaNo ratings yet
- Achilles Tendon RuptureDocument6 pagesAchilles Tendon RuptureBn Wahyu AjiNo ratings yet
- Achilles Tendon RuptureDocument6 pagesAchilles Tendon RupturechloramphenicolNo ratings yet
- Shoulder PDFDocument11 pagesShoulder PDFteresaioana100% (1)
- Anterior Shoulder InstabilityDocument19 pagesAnterior Shoulder InstabilitySiti Nur JannahNo ratings yet
- Extremity and Upper TraumaDocument13 pagesExtremity and Upper TraumaAlt F4 -Another Laughing Time-No ratings yet
- Elbow - Fractures in Children: Fracture MechanismDocument31 pagesElbow - Fractures in Children: Fracture MechanismhendoramuNo ratings yet
- Posterior Shoulder Fracture-Dislocation A SystematDocument7 pagesPosterior Shoulder Fracture-Dislocation A SystematMarcos Burón100% (1)
- Hip DislocationDocument4 pagesHip DislocationcrunkestNo ratings yet
- Dislocation of Hip-1Document44 pagesDislocation of Hip-1lionhearteagleNo ratings yet
- BiomechanicDocument15 pagesBiomechanicMuhamad SdeqNo ratings yet
- Develop Med Child Neuro - 2009 - ROOT - Surgical Treatment For Hip Pain in The Adult Cerebral Palsy PatientDocument8 pagesDevelop Med Child Neuro - 2009 - ROOT - Surgical Treatment For Hip Pain in The Adult Cerebral Palsy PatientSitthikorn StrikerrNo ratings yet
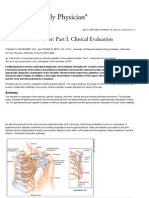
- The Painful Shoulder - Part I. Clinical Evaluation PDFDocument17 pagesThe Painful Shoulder - Part I. Clinical Evaluation PDFOscar FrizziNo ratings yet
- Libs Condition Chart FinalDocument14 pagesLibs Condition Chart Finalapi-507829086No ratings yet
- PrinciplesofOsteopathicMedicine PDFDocument5 pagesPrinciplesofOsteopathicMedicine PDFsuso73No ratings yet
- Elbow InjuriesDocument35 pagesElbow Injurieskarthik venegallaNo ratings yet
- The Terrible Triad of The ElbowDocument5 pagesThe Terrible Triad of The Elbowapi-250084607No ratings yet
- Recurrent Anterior Shoulder Dislocation Treated by Openinferior Glenohumeral Ligament ReconstructionDocument9 pagesRecurrent Anterior Shoulder Dislocation Treated by Openinferior Glenohumeral Ligament ReconstructionIJAR JOURNALNo ratings yet
- Shoulder InstabilitiesDocument16 pagesShoulder InstabilitiesLokesh BhardwajNo ratings yet
- Acute Traumatic Posterior Shoulder Dislocation PDFDocument8 pagesAcute Traumatic Posterior Shoulder Dislocation PDFMuhammad Pringgo ArifiantoNo ratings yet
- Shoulder Application SolutionsDocument3 pagesShoulder Application SolutionsDNo ratings yet
- Scapular Dyskinesis Presented By: Scott Sevinsky MSPTDocument24 pagesScapular Dyskinesis Presented By: Scott Sevinsky MSPTldletkemanNo ratings yet
- Scapular DyskinesisDocument24 pagesScapular DyskinesisbarbaraNo ratings yet
- Uva-Dare (Digital Academic Repository) : Bruinsma, W.EDocument11 pagesUva-Dare (Digital Academic Repository) : Bruinsma, W.EDirga Rasyidin LNo ratings yet
- Rehabilitation of Shoulder Impingement Syndrome and Rotator Cuff Injuries: An Evidence-Based ReviewDocument10 pagesRehabilitation of Shoulder Impingement Syndrome and Rotator Cuff Injuries: An Evidence-Based ReviewEduardo Santana SuárezNo ratings yet
- Anatomy, Back, Scapula: Paul T. Cowan Matthew VaracalloDocument6 pagesAnatomy, Back, Scapula: Paul T. Cowan Matthew Varacalloaccounts 3 lifeNo ratings yet
- Shoulder Injures and Management 2Document94 pagesShoulder Injures and Management 2Khushboo IkramNo ratings yet
- A Simple Guide to The Posture, Spine Diseases and Use in Disease DiagnosisFrom EverandA Simple Guide to The Posture, Spine Diseases and Use in Disease DiagnosisNo ratings yet
- Healthy Shoulder Handbook: Second Edition: 100 Exercises for Treating Common Injuries and Ending Chronic PainFrom EverandHealthy Shoulder Handbook: Second Edition: 100 Exercises for Treating Common Injuries and Ending Chronic PainNo ratings yet
- The Natural Rotator Cuff Healing Guide: Heal Your Cuff, Rid the Pain All On Your Own With Natural ExercisesFrom EverandThe Natural Rotator Cuff Healing Guide: Heal Your Cuff, Rid the Pain All On Your Own With Natural ExercisesRating: 5 out of 5 stars5/5 (1)
- Healthy Shoulder Handbook: 100 Exercises for Treating and Preventing Frozen Shoulder, Rotator Cuff and other Common InjuriesFrom EverandHealthy Shoulder Handbook: 100 Exercises for Treating and Preventing Frozen Shoulder, Rotator Cuff and other Common InjuriesRating: 2 out of 5 stars2/5 (1)
- Mathematics HL - Practice QuestionsDocument152 pagesMathematics HL - Practice QuestionsPyjama ManNo ratings yet
- RB Cagmat Review Center: Central Mindanao University, CMU, Musuan, BukidnonDocument6 pagesRB Cagmat Review Center: Central Mindanao University, CMU, Musuan, BukidnonshakiraNo ratings yet
- Chapter 5 - Introduction To Differential Analysis of Fluid MotionDocument4 pagesChapter 5 - Introduction To Differential Analysis of Fluid MotionBin RenNo ratings yet
- Ralph Menikoff and Thomas D Sewell - Constituent Properties of HMX Needed For Mesoscale SimulationsDocument23 pagesRalph Menikoff and Thomas D Sewell - Constituent Properties of HMX Needed For Mesoscale SimulationsKommissar1981No ratings yet
- Bai Tap On Thi Hoc Ki 2 Lop 4 Mon Tieng AnhDocument8 pagesBai Tap On Thi Hoc Ki 2 Lop 4 Mon Tieng AnhMsPhuong ChiNo ratings yet
- IUPAC & Nomenclature PDFDocument6 pagesIUPAC & Nomenclature PDFjaspreet singh100% (1)
- 640-822 Certkiller Questions and Answers: Number: 640-822 Passing Score: 825 Time Limit: 120 Min File Version: 16.8Document130 pages640-822 Certkiller Questions and Answers: Number: 640-822 Passing Score: 825 Time Limit: 120 Min File Version: 16.8ﻣﺤﻤﺪ ﻭﻫﻴﺐ ﺍﻟﻌﺒﺴﻲNo ratings yet
- Use Code INDIA5 For Extra Discount (Till 17 Aug) : (A) Mitotic Cell Division OnlyDocument6 pagesUse Code INDIA5 For Extra Discount (Till 17 Aug) : (A) Mitotic Cell Division OnlyrajatNo ratings yet
- Socket WeldingDocument35 pagesSocket Weldingreddy543100% (1)
- HVAC Designing Drafting Estimation & InstallationDocument3 pagesHVAC Designing Drafting Estimation & Installationnoha azamali50% (2)
- Kepco KpsDocument27 pagesKepco Kps허준No ratings yet
- Postpartum Anxiety Symptoms, Treatment & How Long Does It LastDocument1 pagePostpartum Anxiety Symptoms, Treatment & How Long Does It LastSathidevi SNo ratings yet
- Science 9 1st Periodical TestDocument4 pagesScience 9 1st Periodical TestKebu Yen100% (1)
- Naskah IschialgiaDocument9 pagesNaskah IschialgiaPuspo Wardoyo100% (1)
- Davenport Blumenberg On HistoryDocument75 pagesDavenport Blumenberg On HistoryWillem OuweltjesNo ratings yet
- DC DC: Table 5.13: Overhead Line Conductor - Hard Drawn CopperDocument8 pagesDC DC: Table 5.13: Overhead Line Conductor - Hard Drawn CopperVino VinoNo ratings yet
- SelectaDocument55 pagesSelectaHuong Cam ThuyNo ratings yet
- 1976 Melling Turbulent Flow in A Rectangular DuctDocument27 pages1976 Melling Turbulent Flow in A Rectangular Ductedward agimNo ratings yet
- Lesson Notes For Atoms and MoleculesDocument3 pagesLesson Notes For Atoms and MoleculesQurrat Ul AinNo ratings yet
- GALLO-SCYTHIANS - Celtic Ukraine (By Mac Congail)Document22 pagesGALLO-SCYTHIANS - Celtic Ukraine (By Mac Congail)Toma100% (1)
- HPhys Unit 02 BFPM Packet 2013Document16 pagesHPhys Unit 02 BFPM Packet 2013Kelly O'Shea100% (3)
- Bonn & Gaston 2005 Richness Ecosystem Conserv SAfDocument18 pagesBonn & Gaston 2005 Richness Ecosystem Conserv SAfKellyta RodriguezNo ratings yet
- Agri Sample Csec Ag Sci Sba Crop Livestock Investigative Projects - 05.06.2017 3Document53 pagesAgri Sample Csec Ag Sci Sba Crop Livestock Investigative Projects - 05.06.2017 3Shakwan Waterman100% (1)
- NN ST661 (CPH)Document42 pagesNN ST661 (CPH)Patrice PaulNo ratings yet
- HP ExpertOne Certification PathsDocument34 pagesHP ExpertOne Certification PathsSaurabh0% (1)
- 2008 Computer Testing Supplement For IA Testing Ct-8080-8d - WebDocument675 pages2008 Computer Testing Supplement For IA Testing Ct-8080-8d - Webgerezair100% (1)