Professional Documents
Culture Documents
Antimicrob. Agents Chemother. 1988 Shelton 268 70
Antimicrob. Agents Chemother. 1988 Shelton 268 70
Uploaded by
Engr Syed Bilal AliOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Antimicrob. Agents Chemother. 1988 Shelton 268 70
Antimicrob. Agents Chemother. 1988 Shelton 268 70
Uploaded by
Engr Syed Bilal AliCopyright:
Available Formats
In vitro susceptibilities of common pediatric pathogens to LY163892.
S Shelton and J D Nelson Antimicrob. Agents Chemother. 1988, 32(2):268. DOI: 10.1128/AAC.32.2.268.
Updated information and services can be found at: http://aac.asm.org/content/32/2/268 Downloaded from http://aac.asm.org/ on January 5, 2014 by guest These include:
CONTENT ALERTS
Receive: RSS Feeds, eTOCs, free email alerts (when new articles cite this article), more
Information about commercial reprint orders: http://journals.asm.org/site/misc/reprints.xhtml To subscribe to to another ASM Journal go to: http://journals.asm.org/site/subscriptions/
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Feb. 1988, p. 268-270 0066-4804/88/020268-03$02.00/0 Copyright C) 1988, American Society for Microbiology
Vol. 32, No. 2
In Vitro Susceptibilities of Common Pediatric Pathogens to LY163892
SHARON SHELTON AND JOHN D. NELSON* Department of Pediatrics, The University of Texas Health Science Center at Dallas, 5323 Harry Hines Boulevard, Dallas, Texas 75235
Received 31 August 1987/Accepted 30 November 1987
LY163892 is a carbacephem antibiotic for oral administration with an antibacterial spectrum similar to that of cefaclor and amoxicillin-clavulanic acid. It has greater stability than cefaclor and greater activity against ,3-lactamase-producing Haemophilus influenzae and Escherichia coli. LY163892 is less active than amoxicillin against streptococci and less active than amoxicillin-clavulanic acid against Branhamella catarrhalis but comparable against other pathogens.
Downloaded from http://aac.asm.org/ on January 5, 2014 by guest
LY163892 is a carbacephem synthetic antibiotic for oral administration. Its chemical name is 7-[D-(aminophenylacetyl) amino]-3-chloro-8-oxo-1-azabicyclo[4.2.0]oct-2-ene2-carboxylic acid. Structurally it is similar to cefaclor, with the major difference being the substitution of a sulfur molecule for carbon at position 1 in the dihydrothiazine ring. In preliminary tests by the manufacturer, it had a spectrum of in vitro activity comparable to that of cefaclor. The purpose of this study was to examine the in vitro activity of LY163892 against common bacterial pathogens that cause upper and lower respiratory tract infections, urinary tract infections, and infections of the skin and skin structures in comparison with cefaclor, amoxicillin, and amoxicillin-clavulanic acid. Laboratory-standard powders were obtained from the manufacturers. The Streptococcus pyogenes isolates were from throat (n = 52) and middle ear fluid (n = 11) cultures. The Escherichia coli strains were from urine cultures. Branhamella catarrhalis, Haemophilus influenzae, Streptococcus pneumoniae, and Staphylococcus aureus strains (all methicillin susceptible) were mainly from middle ear fluid cultures. The bacterial isolates had been collected from clinical specimens between 1980 and 1986. Mueller-Hinton agar (B. catarrhalis, S. aureius, E. coli), 5% sheep blood agar (S. pyogenes, S. pneumoniae), and chocolate agar (H. influenzae) were used for agar dilution studies. Twofold dilutions of antibiotic from 8 to 0.03 ,ug/ml were added to the liquefied agar. Amoxicillin and clavulanic acid were in a 4:1 ratio, with the concentration expressed as the amoxicillin component. Seed cultures of the bacterial strains were grown overnight at 37C in appropriate broth media and diluted in Mueller-Hinton broth so that the prongs of a Steers-Foltz replicator (which deliver 0.007 ml) would deliver an inoculum of 104 to 105 CFU. Actual colony counts were done on each strain tested and ranged from 9 x 103 to 9 x 105, with most being 105. The agar plates were incubated at 37C for 18 h. The MIC was the smallest amount of drug resulting in no growth or fewer than 10 colonies. Disk testing was done with a 30-p.g LY163892 disk by using the National Committee for Clinical Laboratory Standards modification of the Kirby-Bauer method (2). According to the manufacturer, a zone size of <14 mm indicates
*
TABLE 1. Effect of bacterial inoculum size on susceptibility
Concn (,ug/ml) at inoculum size (CFU):
Organism
MIC
102
104
106
MBC MIC MBC MIC MBC
B. catarrhalis, ,B-lactamase positive (N86-0121E) B. catarrhalis, P-lactamase
0.5
1.0
0.5 1.0 8.0 >8.0 0.25 0.5 0.5
0.12
0.12 0.12 0.12 0.25
negative (N86-O111E) H. influenzae, ,B-lactamase positive (N84-047-0) H. influenzae, P-lactamase negative (N84-014-0) S. aureus, 1-lactamase positive (N86-0204-E) S. pyogenes S. pneumoniae, relatively resistant (N86-0188E) S. pneumoniae, penicillin susceptible (N86-0189E)
<0.008 0.5
0.06 0.5 0.5
0.016 0.016 0.12 0.12 0.5
0.5
1.0
1.0 2.0 8.0 >8.0
0.25 2.0
0.25 0.12 0.12 0.25 2.0 2.0 4.0 4.0
0.25 4.0
0.12
0.12
0.12 0.12 0.12 0.12
TABLE 2. Effect of fresh human serum on susceptibility
Concn (pLg/ml) in:
Organism"
MIC
Broth
Broth with 50%
serum
MBC
MIC
MBC
B. catarrhalis, ,3-lactamase
0.5 0.12
0.06
1.0
0.12
0.5
0.25
0.06
0.06
0.25
0.12 0.25 0.25 2.0
positive B. catarrhalis, 3-lactamase negative H. influenzae, 1B-lactamase positive H. influenzae, P-lactamase negative S. aureus, P-lactamase positive S. pyogenes S. pneumoniae, relatively
resistant
0.12 1.0
0.25 2.0
0.12
2.0
0.03
2.0 0.25 4.0 0.25
0.25 4.0
0.12
0.25 4.0
0.25
S. pneumoniae, penicillin
0.12
susceptible
Corresponding author.
268
" Strain identification numbers are the same as in Table 1.
VOL. 32, 1988
NOTES
-
269
8r
E
at
._
~~~vv
TABLE 3. Agar dilution susceptibility test results
V
vW
V 7"l
v
Organism (no. of strains tested)
o
MIC (,g/mi)b Dru rugRange 50
90
1 1
0
0
2_
B. catarrhalis,
c 0
P-lactamase
1
v
4c
positive (40)
0
LY CEF AMOX AMOX-CA
1-
Rage5-29P/
0.5-2
s0.03-2 <0.03->8 s0.03-0.25 s0.03-0.5
.0.03-0.5
0.5 1 1
0.12
4 0.25 0.12 0.25
<0.03 <0.03
.0
C 0
0.5 _
0.2.5
v S. oureus
Str. pneumonioe
cJ
(Relatively Resistant)
a
B. catarrhalis, lactamase negative (8)
0
E
C
Str. pneumoniae
68a
68,
LY CEF AMOX AMOX-CA LY CEF AMOX AMOX-CA
LY CEF AMOX AMOX-CA
0.12 0.12
.0.03 .0.03
s0.03-0.12 s0.03
0.12-0.5 1-8 1->8 <0.03-2
<0.03-1 0.25-8 s0.03-0.5 s0.03-0.5 0.12-1 2->8 2->8 0.05-4 0.25-1 1->8 0.12-0.5 0.25-0.5
0.5-8 1->8 0.12->8 0.12-2
(Penicillin Susceptible)
0.125
0.06
Str. pyogenes
o0
r._
H. influenzae type b, P-lactamase positive (24)
H. influenzae type b, P-lactamase negative (25) H. influenzae NTC,
0.25 0.5 4 4 >8 >8 1 1
0.25 4 0.25 0.25
0.5 8 >8 2
Downloaded from http://aac.asm.org/ on January 5, 2014 by guest
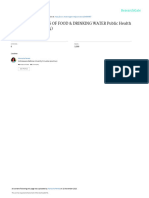
40lo_ o_ s 0.03 20 lO 30 40 Zone Size (mm) Around 30Etg DISC FIG. 1. LY163892 disk zone diameters and MICs for grampositive bacteria.
L
0.o
0.5 8 0.5 0.5
1
P-lactamase positive (14)
H. influenzae NT,
LY CEF AMOX AMOX-CA
LY CEF AMOX AMOX-CA
LY CEF AMOX AMOX-CA LY CEF AMOX AMOX-CA LY CEF AMOX AMOX-CA
LY CEF AMOX AMOX-CA
>8
>8 2
resistance, 15 to 17 mm indicates intermediate, and -18 mm indicates susceptibility. Initially, a representative strain of each type of organism was tested for inoculum effect and for the effect of human serum on MICs and MBCs determined by the broth microdilution method described by Barry (1). The manufacturer considers strains for which MICs are 8 p,g/ml or less to be susceptible. Haemophilus strains were tested in MuellerHinton broth with supplement C (Difco Laboratories), Branhamella and staphylococcal strains were tested in MuellerHinton broth, and streptococcal strains were tested in Todd-Hewitt broth with 5% sheep erythrocytes. With ino8
P-lactamase negative (31)
S.
aureus
0.5 8 0.5 0.5 2-4 4 4 2
1 >8 0.5 0.5
4
(25)
8 >8 2
S.
pyogenes
(63)
s0.03-0.5 s0.03-0.25
.0.03
s0.03
0.25->8 1->8 0.5->8 0.5->8
81 >82 81,>82 0.51,22 0.51,22
0.06 0.12 0.12 0.12 .0.03 <0.03 s0.03 <0.03 0.5 4 4 4
2 >8 >8 >8
E. coli (51)
E
4
-
S. pneumoniae,
2
C,
penicillin resistant (MIC, >1.0
0
.0
-
p.g/ml) (3)
NA" NA NA NA
0.5 0.5 0.12 0.06
NA NA NA NA 4 1 0.12 0.12
c 0
1I
o0 bgeB400
0.5 _
El
0
._
S. pneumoniae, rel- LY CEF atively resistant AMOX (MIC, 0.1-1.0 AMOX-CA ,ug/ml) (17)
0.12-8 0.25-8 <0.03-0.25 .0.03-0.12
0.25 _ 0.125
< 0.06
10
cotorrhalis v E. co/i
o
8.
18
0
S. pneumoniae,
op8
0
o
._
H. influenzoe
0
1
penicillin susceptible (MIC, <0.1 p.g/ml) (26)
LY CEF AMOX AMOX-CA
<0.03-1 0.12-1 <0.03 <0.03-0.06
1 0.5 0.5 0.5 .0.03 <0.03 <0.03 <0.03
._
40 30 Zone Size (mm) Around 30,4g D)ISC
20
' LY, LY163892; CEF, cefaclor; AMOX, amoxicillin; AMOX-CA, amoxicillin-clavulanic acid. 'b 50% and 90%, MIC for 50 and 90% of strains tested, respectively. c NT, Nontypable. d Subscripts indicate the numbers of strains for which MIC was as indi-
cated.
FIG. 2. LY163892 disk negative bacteria.
zone
diameters and MICs for gram-
e NA,
Not applicable.
270
NOTES
ANTIMICROB. AGENTS CHEMOTHER.
cula of 102, 104, and 106 CFU, results were similar except with P-lactamase-positive B. catarrhalis and S. aureus for which MICs and MBCs increased approximately eightfold with the largest inoculum (Table 1). There was no increase in MIC or MBC in broth containing 50% freshly drawn human serum compared with plain broth, and in the case of ,Blactamase-positive B. catarrhalis the MIC and MBC were two- to fourfold lower in broth with 50% serum (Table 2). Results of agar dilution susceptibility testing results are shown in Table 3. LY163892 exhibited good in vitro activity against all bacterial strains tested except two strains of E. coli that were resistant to 8 ,ug/ml. Those two strains were also resistant to 8 ,ug of the other three drugs tested per ml. In comparison with cefaclor, LY163892 had approximately 16-fold-greater activity against ,-lactamase-positive or -negative H. influenzae, approximately 8-fold-greater activity against E. coli, and comparable activity against the other pathogens. In comparison with amoxicillin and amoxicillin-clavulanic acid, LY163892 was less active against S. pyogenes, S.
pneumoniae, and B. catarrhalis, more active against E. coli, and comparably active against the other pathogens. The 30-,ug LY163892 disk did not discriminate well the various MICs for gram-positive cocci (Fig. 1), but zone sizes correlated with MICs for gram-negative organisms (Fig. 2). Because of its in vitro spectrum of activity, LY163892 has the potential for clinical use in upper and lower respiratory tract infections, skin and skin structure infections, and urinary tract infections caused by susceptible bacteria. Its greater stability in comparison with cefaclor is an advantage.
This study was supported by a grant from Eli Lilly & Co.
LITERATURE CITED 1. Barry, A. L. 1986. The antimicrobic susceptibility test: principles and practices, p. 95. Lea & Febiger, Philadelphia. 2. Jones, R. N. (ed.). 1984. Performance standards for antimicrobial disk susceptibility tests, 3rd ed. National Committee for Clinical Laboratory Standards. Viltanova. Pa.
Downloaded from http://aac.asm.org/ on January 5, 2014 by guest
You might also like
- Bacteriostat Bacteriosid 24ab C.jejuni - FullDocument5 pagesBacteriostat Bacteriosid 24ab C.jejuni - FullLalalala Gabriella KristianiNo ratings yet
- Antibacterial Activity of Mometasone Furoate: ObjectiveDocument3 pagesAntibacterial Activity of Mometasone Furoate: Objectiveminerva_stanciuNo ratings yet
- High-Throughput Identification of Antibacterials Against Methicillin-Resistant Staphylococcus Aureus (MRSA) and The TransglycosylaseDocument18 pagesHigh-Throughput Identification of Antibacterials Against Methicillin-Resistant Staphylococcus Aureus (MRSA) and The Transglycosylasepimpaliukas1No ratings yet
- With Activities of Amphotericin B and in Vitro Activity of SCH-56592 and ComparisonDocument4 pagesWith Activities of Amphotericin B and in Vitro Activity of SCH-56592 and ComparisonMaria Marta SampietroNo ratings yet
- 2009 8 4 12 DulgerDocument5 pages2009 8 4 12 DulgerHajrah SuhardiNo ratings yet
- Tris-EDTA Significantly Enhances Antibiotic Efficacy Against Multidrug-Resistant Pseudomonas Aeruginosa in VitroDocument7 pagesTris-EDTA Significantly Enhances Antibiotic Efficacy Against Multidrug-Resistant Pseudomonas Aeruginosa in VitroWilliam ChandlerNo ratings yet
- LarissaDocument6 pagesLarissalharhasouzaNo ratings yet
- Nordmann 2016Document17 pagesNordmann 2016Yousra SoumaNo ratings yet
- Dr. Adrian Marinescu Matei Bals Virgil Musta, Medic Primar de Boli InfecțioaseDocument17 pagesDr. Adrian Marinescu Matei Bals Virgil Musta, Medic Primar de Boli InfecțioaseDragosAurNo ratings yet
- Research LabDocument7 pagesResearch LabJessa Nicole ReteracionNo ratings yet
- EJHM Volume 77 Issue 6 Pages 5804-5816Document13 pagesEJHM Volume 77 Issue 6 Pages 5804-5816فردوس يسNo ratings yet
- Germ Tube TestDocument3 pagesGerm Tube TestirnaresaNo ratings yet
- Staphylococcus Aureus, The Most Virulent Staphylococcus Species, Is Also The Prevalent Pathogen IsolatedDocument6 pagesStaphylococcus Aureus, The Most Virulent Staphylococcus Species, Is Also The Prevalent Pathogen IsolatedVivi RocheNo ratings yet
- Anti-HIV Activity Directed Fractionation of The Extracts of Margyricarpus SetosusDocument4 pagesAnti-HIV Activity Directed Fractionation of The Extracts of Margyricarpus SetosuskhnumdumandfullofcumNo ratings yet
- Trimethoprim-Sulfamethoxazole: Effect of Minimal Amounts of Thymidine On Activity of Against Staphylococcus EpidermidisDocument4 pagesTrimethoprim-Sulfamethoxazole: Effect of Minimal Amounts of Thymidine On Activity of Against Staphylococcus EpidermidisEmad MoradNo ratings yet
- Activity of Sulbactam in Combination With Ceftriaxone in Vitro and in Experimental Endocarditis AAC 1990Document6 pagesActivity of Sulbactam in Combination With Ceftriaxone in Vitro and in Experimental Endocarditis AAC 1990AMIT JAINNo ratings yet
- Clindamicina (Inglés)Document6 pagesClindamicina (Inglés)Gonzalo Daniel Llarrull BatistaNo ratings yet
- Meier Et Al, 1996Document4 pagesMeier Et Al, 1996boni_sebayangNo ratings yet
- High ThroutDocument7 pagesHigh ThroutashrafbookNo ratings yet
- Microbial Contamination of Pharmaceutical PreparationsDocument6 pagesMicrobial Contamination of Pharmaceutical PreparationsReiamury AzraqNo ratings yet
- Bacteriocin Purification Research ProposalDocument7 pagesBacteriocin Purification Research ProposalThanh Nguyen LeNo ratings yet
- Muñoz Et Al 2010Document9 pagesMuñoz Et Al 2010Eleazar Valenzuela LopezNo ratings yet
- Optimization of Medium Composition For The Production of AntimicrobialDocument8 pagesOptimization of Medium Composition For The Production of AntimicrobialArmanNo ratings yet
- Microbial Analysis of FoodDocument77 pagesMicrobial Analysis of FoodAbdurrazaq YakubuNo ratings yet
- Rapid Identification ..Document4 pagesRapid Identification ..Nithyakalyani AsokanNo ratings yet
- Trabajos de Diferentes MateriasDocument4 pagesTrabajos de Diferentes Materiasnaruto gamerNo ratings yet
- Aac 05348-11Document3 pagesAac 05348-11Ainul MardhiyahNo ratings yet
- Cefaclor For Oral Suspension - DailymedDocument15 pagesCefaclor For Oral Suspension - DailymedThuy Khanh LeNo ratings yet
- Antimicrob. Agents Chemother. 1995 Von Eiff 268 70Document3 pagesAntimicrob. Agents Chemother. 1995 Von Eiff 268 70Charisse Jan PercalesNo ratings yet
- Chatterjee 2006Document10 pagesChatterjee 2006Yunita MarwahNo ratings yet
- Inhibitory and Killing Activities of Medicinal Plants Against Multiple Antibiotic-Resistant Helicobacter PyloriDocument8 pagesInhibitory and Killing Activities of Medicinal Plants Against Multiple Antibiotic-Resistant Helicobacter PyloriNyayu_FitrianiNo ratings yet
- International Refereed Journal of Engineering and Science (IRJES)Document4 pagesInternational Refereed Journal of Engineering and Science (IRJES)www.irjes.comNo ratings yet
- Ruiz Et AlDocument6 pagesRuiz Et AlAnonymous WmO2l4VNo ratings yet
- PK PD Relationships SummaryDocument2 pagesPK PD Relationships Summarynick224No ratings yet
- 1 - Detection of Hemolysins in AeromonasDocument11 pages1 - Detection of Hemolysins in AeromonasandymicdNo ratings yet
- Budu BiotekDocument5 pagesBudu BiotekIndra Yusuf PratamaNo ratings yet
- Demetrio L. Valle JR., MD, MSC., FPSP, Fascp, Ifcap Anatomic and Clinical PathologistDocument26 pagesDemetrio L. Valle JR., MD, MSC., FPSP, Fascp, Ifcap Anatomic and Clinical Pathologistodin3zNo ratings yet
- CoenyeDocument19 pagesCoenyeTrustia RizqandaruNo ratings yet
- 10 5740@jaoac 10-385Document7 pages10 5740@jaoac 10-385nephylymNo ratings yet
- Novel Chalcones and 1,3,5 Triphenyl 2 PyrazolineDocument6 pagesNovel Chalcones and 1,3,5 Triphenyl 2 PyrazolineMaria PappovaNo ratings yet
- Development, Validation, and Applications of A New Laboratory-Scale Indirect Impedancemeter For Rapid Microbial ControlDocument7 pagesDevelopment, Validation, and Applications of A New Laboratory-Scale Indirect Impedancemeter For Rapid Microbial ControloldpenguinNo ratings yet
- In Vitro Effect of Karathane LC (Dinocap) On Human LymphocytesDocument4 pagesIn Vitro Effect of Karathane LC (Dinocap) On Human LymphocytesRisa PenaNo ratings yet
- Evaluacion of Diffusion and Dilution Methods To Detemine The Antibacterial Activity of Plants ExtractsDocument6 pagesEvaluacion of Diffusion and Dilution Methods To Detemine The Antibacterial Activity of Plants ExtractsLuis Alberto AnguianoNo ratings yet
- Antibacterial Activity of Lantana Camara Linn and Lantana: Montevidensis Brig Extracts From Cariri-Ceará, BrazilDocument3 pagesAntibacterial Activity of Lantana Camara Linn and Lantana: Montevidensis Brig Extracts From Cariri-Ceará, BrazilevilbioNo ratings yet
- Ekinci BDocument4 pagesEkinci BreclinpharmaNo ratings yet
- Antimicrobial Sensitivity TestingDocument6 pagesAntimicrobial Sensitivity TestingKate CamachoNo ratings yet
- Antibacterial Activity of Mupirocin (Pseudomonic Acid), Antibiotic TopicalDocument4 pagesAntibacterial Activity of Mupirocin (Pseudomonic Acid), Antibiotic TopicalMaria UlfaNo ratings yet
- Microbiology and Immunology - 2010 - Iorio - A Combination of Methods To Evaluate Biofilm Production May Help To DetermineDocument6 pagesMicrobiology and Immunology - 2010 - Iorio - A Combination of Methods To Evaluate Biofilm Production May Help To DetermineAriane Barcellos Dos SantosNo ratings yet
- Synthesis and Anti-Mycobacterial Activity of (E) - N - (Monosubstituted-Benzylidene) Isonicotinohydrazide DerivativesDocument4 pagesSynthesis and Anti-Mycobacterial Activity of (E) - N - (Monosubstituted-Benzylidene) Isonicotinohydrazide DerivativeslistiaadindaNo ratings yet
- Presentation On Harmonized Microbial Enumeration MethodsDocument29 pagesPresentation On Harmonized Microbial Enumeration MethodsOsman AitaNo ratings yet
- (Onobrychis Viciifolia Scop.) Condensed Tannins Proteolysis byDocument5 pages(Onobrychis Viciifolia Scop.) Condensed Tannins Proteolysis byRama DhanulNo ratings yet
- Linezolida NovoDocument6 pagesLinezolida NovoGabriel EstevesNo ratings yet
- Candida 1Document10 pagesCandida 1mufqifitra160491No ratings yet
- Quantitative and Qualitative Model Reveals A Combined PharmacodynamicDocument17 pagesQuantitative and Qualitative Model Reveals A Combined PharmacodynamicIsabelle de MéloNo ratings yet
- Cigarette Smoke Increases Staphylococcus Aureus Biofilm Formation Via Oxidative StressDocument9 pagesCigarette Smoke Increases Staphylococcus Aureus Biofilm Formation Via Oxidative StressEdson BonfimNo ratings yet
- A Study OnDocument4 pagesA Study OnJiff Solis TrinidadNo ratings yet
- Antibacterial Effect of Cassia Fistula Extract On Pathogenic Bacteria of Veterinary ImportanceDocument5 pagesAntibacterial Effect of Cassia Fistula Extract On Pathogenic Bacteria of Veterinary ImportanceAsif MajeedNo ratings yet
- The Fundamentals of Scientific Research: An Introductory Laboratory ManualFrom EverandThe Fundamentals of Scientific Research: An Introductory Laboratory ManualNo ratings yet
- Endophyte Biotechnology: Potential for Agriculture and PharmacologyFrom EverandEndophyte Biotechnology: Potential for Agriculture and PharmacologyAlexander SchoutenNo ratings yet
- Thoracic Outlet Syndrome Exercises IIDocument2 pagesThoracic Outlet Syndrome Exercises IIRiaz KhanNo ratings yet
- Time of Useful ConsciousnessDocument7 pagesTime of Useful ConsciousnessJosé LavadoNo ratings yet
- KoshtaDocument15 pagesKoshtaPanchakarma DepartmentNo ratings yet
- Therapeutic Drug Monitoring: By: Adewale Akinseloyin Oluwatimilehin Agboola Oluwatosin AjibadeDocument33 pagesTherapeutic Drug Monitoring: By: Adewale Akinseloyin Oluwatimilehin Agboola Oluwatosin AjibadeJoe AjibadeNo ratings yet
- Physiology of The Cerebrospinal FluidDocument6 pagesPhysiology of The Cerebrospinal FluidShereen Al-ObinayNo ratings yet
- Obstetric AnesthesiaDocument440 pagesObstetric Anesthesiamonir61100% (1)
- Guideline Screening and Treatment of Malnutrition English July 2012Document30 pagesGuideline Screening and Treatment of Malnutrition English July 2012Putri WibisonoNo ratings yet
- Re-Purposing Drugs To Combat COVID-19: Niel Karrow, Department of Animal Biosciences, University of GuelphDocument12 pagesRe-Purposing Drugs To Combat COVID-19: Niel Karrow, Department of Animal Biosciences, University of GuelphKraft DinnerNo ratings yet
- 2-Preschool Parent QuestionnaireDocument3 pages2-Preschool Parent QuestionnaireION677No ratings yet
- Aisyah HPTDocument10 pagesAisyah HPTBesari Md DaudNo ratings yet
- Details ProgramDocument9 pagesDetails ProgramphysiologyNo ratings yet
- Gi MapDocument5 pagesGi MapBethany MosesNo ratings yet
- Thesis - Final (2) (Repaired)Document61 pagesThesis - Final (2) (Repaired)Alexis MutuyimanaNo ratings yet
- Nursing Cheat SheetDocument1 pageNursing Cheat Sheetramesh kumarNo ratings yet
- Radio PsaDocument3 pagesRadio Psaapi-356356986No ratings yet
- 1 Administering OxygenDocument6 pages1 Administering OxygentlokingNo ratings yet
- Glycogen Storage DisordersDocument8 pagesGlycogen Storage DisordersCha CanceranNo ratings yet
- Ulcirex CapsuleDocument3 pagesUlcirex Capsulehk_scribdNo ratings yet
- Kantor Cabang: BANJARMASIN - 1701 FKTP: Kertak Hanyar - 17040601Document6 pagesKantor Cabang: BANJARMASIN - 1701 FKTP: Kertak Hanyar - 17040601Ic-tika Siee ChuabbieNo ratings yet
- Prostate Ca Flow ChartDocument5 pagesProstate Ca Flow ChartDanekka Tan100% (1)
- RH NegativeDocument4 pagesRH NegativeMitch LeeNo ratings yet
- CCRNDocument17 pagesCCRNNílo Stárn100% (1)
- War Card GameDocument2 pagesWar Card Gameapi-541744798No ratings yet
- Gynaecology - Riley HarrisonDocument45 pagesGynaecology - Riley HarrisonFiras AliNo ratings yet
- GONORRHOEADocument23 pagesGONORRHOEADwi Fikha AprilyantiNo ratings yet
- Exercise 4.1Document1 pageExercise 4.1Belle LatNo ratings yet
- Measles EpiDocument22 pagesMeasles Epiمحمد صالحNo ratings yet
- Instructions For Completing The CMS 1500 Claim FormDocument6 pagesInstructions For Completing The CMS 1500 Claim FormHarry CanabaNo ratings yet
- Group 3 QUIZDocument4 pagesGroup 3 QUIZJessa Mae OhaoNo ratings yet
- What Is BacteriaDocument33 pagesWhat Is Bacteriaapi-19862227100% (1)