Professional Documents
Culture Documents
Cauda Equina Syndrome
Cauda Equina Syndrome
Uploaded by
Ramadhani Syafitri0 ratings0% found this document useful (0 votes)
65 views10 pagesA slipped disc occurs when the outer layer of a spinal disc ruptures, causing the gel-like interior material to bulge out. This puts pressure on the spinal cord or nerves, resulting in back pain that may radiate to other areas. A common symptom is sciatica, involving pain down the leg. Treatment focuses on physical therapy, medications, and sometimes surgery for severe cases. Cauda equina syndrome is a rare but serious condition where multiple spinal nerves become compressed, potentially causing leg paralysis and loss of bladder control.
Original Description:
From NHS
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentA slipped disc occurs when the outer layer of a spinal disc ruptures, causing the gel-like interior material to bulge out. This puts pressure on the spinal cord or nerves, resulting in back pain that may radiate to other areas. A common symptom is sciatica, involving pain down the leg. Treatment focuses on physical therapy, medications, and sometimes surgery for severe cases. Cauda equina syndrome is a rare but serious condition where multiple spinal nerves become compressed, potentially causing leg paralysis and loss of bladder control.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
65 views10 pagesCauda Equina Syndrome
Cauda Equina Syndrome
Uploaded by
Ramadhani SyafitriA slipped disc occurs when the outer layer of a spinal disc ruptures, causing the gel-like interior material to bulge out. This puts pressure on the spinal cord or nerves, resulting in back pain that may radiate to other areas. A common symptom is sciatica, involving pain down the leg. Treatment focuses on physical therapy, medications, and sometimes surgery for severe cases. Cauda equina syndrome is a rare but serious condition where multiple spinal nerves become compressed, potentially causing leg paralysis and loss of bladder control.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 10
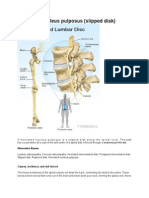
A slipped disc, also known as a prolapsed or herniated disc, is where one of the discs in the spine
ruptures and the gel inside leaks out.
This can cause back pain as well as pain in other areas of the body.
The sciatic nerve is often affected in cases of slipped disc. It is the longest nerve in the body and runs
from the back of the pelvis, through the buttocks, down both legs to the feet.
If pressure is placed on the sciatic nerve it can cause:
a lasting, aching pain
numbness
a tingling sensation in one or both legs
Read more about the symptoms of a slipped disc.
The spine
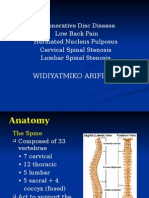
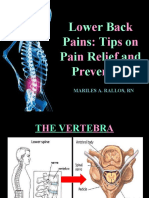
The spine consists of 24 individual bones called vertebrae which are stacked on top of each other.
In between each vertebra there are protective, circular pads of cartilage (connective tissue) called discs.
They have a tough, fibrous case that contains a softer, gel-like substance. The discs help to cushion the
vertebrae when you move around.
The spinal cord is highly sensitive and passes through the middle of the vertebral column. It
contains nerve cells and bundles of nerve fibres that connect all parts of the body to the brain.
What causes a slipped disc?
A slipped disc occurs when the outer case of the disc ruptures (splits), resulting in the gel inside bulging
and protruding out of the disc.
The damaged disc can put pressure on the whole spinal cord or on a single nerve root. This means that a
slipped disc can cause pain both in the area of the protruding disc and in the area of the body that is
controlled by the nerve that the disc is pressing on.
It is not always clear what causes a disc to break down, although age is a common factor in many cases.
As you get older, your spinal discs start to lose their water content, making them less flexible and more
likely to rupture.
Read more about what causes a slipped disc.
Diagnosing a slipped disc
Your GP will usually be able to diagnose a slipped disc from your symptoms and medical history. They
may also carry out a physical examination to test:
reflexes
muscle strength
walking ability
sensation in your limbs
Read more about how a slipped disc is diagnosed.
Treating a slipped disc
It can take about four to six weeks to recover from a slipped disc. Treatment usually involves a
combination of physical therapy, such as massage and exercise, and medication to relieve the pain.
Surgery to release the compressed nerve and remove part of the disc may be considered in severe
cases, or if the pain continues for longer than six weeks.
In many cases, a slipped disc will eventually shrink back away from the nerve, and the pain will ease as
the disc stops pressing on the affected nerve.
If you have a slipped disc, it is very important to keep active. Initially, moving may be difficult but after
resting for a few days you should start to move around. This will help keep your back mobile and speed
up your recovery.
Any exercise you do should be gentle and not put a strain on your back. Swimming is ideal because the
water supports your weight and little strain is placed on your joints.
Read more about treating a slipped disc.
Preventing a slipped disc
Taking a few sensible precautions, such as leading a healthy lifestyle, can help prevent back pain and
lower your risk of getting a slipped disc. For example, you should:
take regular exercise
use a safe technique when lifting heavy objects
always maintain a good posture when sitting and standing
Most people who have a slipped disc experience pain which usually begins in the lower
back beforesometimes spreading to other parts of the body.
However, some people with a slipped disc do not have any obvious symptoms. This is usually because
the part of the disc that bulges out is small or does not press on nerves or spinal cord.
Sciatica
In most cases of slipped disc, pain is caused when part of the disc begins to press on one of the nerves
that run along the spine. Parts of the sciatic nerve are most commonly affected.
The sciatic nerve is the longest nerve in the body and is made up of several smaller nerves. It runs from
the back of the pelvis, through the buttocks and down the legs to the feet.
Pressure placed on the sciatic nerve can cause:
a lasting, aching pain
numbness
a tingling sensation in one or both legs
These symptoms often start in the lower back and travel down the buttocks, into either of the legs.
Read more about sciatica.
Other nerves
If the slipped disc presses on any of the other nerves that run down your spinal cord, your symptoms may
include:
muscle paralysis
muscle spasms where your muscles contract suddenly and painfully
urinary incontinence (loss of bladder control)
Muscle spasms and paralysis tend to occur in your arms, legs and buttocks. The pain you experience
when a disc presses on a nerve is often worse when you put pressure on the nerve. This can happen
when you cough, sneeze or sit down.
Cauda equina syndrome
Low back pain affects millions of people every year, and in most cases, it improves without
surgery. But severe back pain can be a symptom of a serious condition that is not well
known and is often misdiagnosed. Cauda equina syndrome (CES) occurs when the nerve
roots of the cauda equina are compressed and disrupt motor and sensory function to the
lower extremities and bladder. Patients with this syndrome are often admitted to the
hospital as a medical emergency. CES can lead to incontinence and even permanent
paralysis.
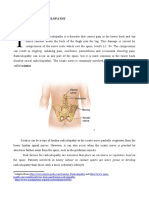
The collection of nerves at the end of the spinal cord is known as the cauda equina, due to
its resemblance to a horse's tail. The spinal cord ends at the upper portion of the lumbar
(lower back) spine. The individual nerve roots at the end of the spinal cord that provide
motor and sensory function to the legs and the bladder continue along in the spinal canal.
The cauda equina is the continuation of these nerve roots in the lumbar region. These
nerves send and receive messages to and from the lower limbs and pelvic organs.
Cauda equina syndrome is a serious condition where the nerves at the very bottom of the spinal cord
become compressed. Symptoms include:
lower back pain
numbness in your groin
paralysis of one or both legs
rectal pain
bowel disturbance
inability to pass urine or incontinence
pain in the inside of your thighs
A slipped disc occurs when the circle of connective tissue surrounding the disc breaks down.
This allows the soft, gel-like part of the disc to swell and protrude out.
It is not always clear what causes the connective tissue to break down. However, slipped discs are often
the result of increasing age.
As you get older, your spinal discs start to lose their water content. This makes them less flexible and
more likely to rupture (split).
There are a number of other factors that can put increased pressure and strain on your spine. These
include:
bending awkwardly
jobs that involve heavy or awkward lifting
jobs that involve lots of sitting, particularly driving
smoking
being overweight
weight-bearing sports, such as weight lifting
a traumatic injury to your back, such as a fall or car accident
Situations such as these can weaken the disc tissue and can sometimes lead to a slipped disc.
Your GP will usually be able to diagnose a slipped disc from your symptoms and medical history.
You will also have a physical examination, during which your GP will test your:
reflexes
muscle strength
walking ability
sensation in your limbs
Cauda equina syndrome is difficult to diagnose. It is rare and its symptoms mimic those of other
conditions. Besides a herniated disk, other conditions with similar symptoms to cauda equina
syndrome include peripheral nerve disorder, spinal cord compression, and irritation or compression of
the nerves after they exit the spinal column and travel through the pelvis, a condition known as
lumbosacral plexopathy.
Another difficulty in diagnosing cauda equina syndrome is that its symptoms may vary in intensity and
evolve slowly over time. Also, an x-ray will often not be helpful in detecting the cause of the syndrome.
How then is a physician to know to look for cauda equina syndrome?
Physicians need to be aware of certain red flags that indicate cauda equina syndrome. Red flags in
someone with back pain include saddle anesthesia, recent onset of bladder dysfunction (such as
urinary retention or incontinence), bowel incontinence and motor weakness in the lower extremity. The
presence of these symptoms warn of cauda equina compression.
Red flags also may be present in a patients history. Recent trauma, a history of cancer or a severe
infection may predispose a person to cauda equina syndrome. Any of these diseases can involve the
discs or the bones of the lumbar spine and result in cauda equina syndrome. Other conditions that
may rarely lead to cauda equina syndrome include osteoporotic vertebral fractures and spinal stenosis.
Besides the classic red flag symptoms, physicians suspecting the syndrome look for reflex
abnormalities such as the loss or diminution of reflexes, sensory abnormality in the legs, bladder or
rectum, and muscle weakness or wasting in the legs.
MRI (magnetic resonance imaging) or myelograms are diagnostic tools valuable in discovering cauda
equina syndrome. MRI uses energy from a powerful magnet to produce cross-sectional images of the
back. The MRI is especially helpful in detecting damage or disease of soft tissue such as discs. A
myelogram is a liquid dye injected into the spinal column. A myelogram can show pressure on the
cauda equina from herniated discs and other conditions.
The incidence of cauda equina syndrome is not related to sex or race. It occurs primarily in adults,
though trauma-related cauda equina syndrome is not age specific.
Patients with back pain should be aware of the following "red flag" symptoms that may
indicate CES:
Severe low back pain
Motor weakness, sensory loss, or pain in one, or more commonly both legs
Saddle anesthesia (unable to feel anything in the body areas that sit on a saddle)
Recent onset of bladder dysfunction (such as urinary retention or incontinence)
Recent onset of bowel incontinence
Sensory abnormalities in the bladder or rectum
Recent onset of sexual dysfunction
A loss of reflexes in the extremities
Medical history implications:
Recent violent injury to the back
Recent lumbar spine surgery
A history of cancer
Recent severe infection
Straight leg-raising test
While you are lying flat, your GP will slowly raise each of your legs, one at a time, to see if it causes any
pain or discomfort in your legs or back. This is known as the straight leg raising test.
Most people with a slipped disc will not be able to raise their leg more than two thirds of the way up
without feeling tingling, numbness and pain.
Further tests
Further tests are not usually required because in most cases the symptoms of a slipped disc settle down
within a few weeks.
However, if your symptoms do not ease after four to six weeks, further tests may be required to rule out
other conditions and investigate the size and position of the slipped disc.
Some of the tests that you may have are described below.
Magnetic resonance imaging scan
A magnetic resonance imaging (MRI) scan uses a strong magnetic field and radio waves to produce
detailed images of the inside of your body.
MRI scans are effective at showing the position and size of a slipped disc. They can also pinpoint the
affected nerves.
Read more about MRI scans.
Computerised tomography scan
A computerised tomography (CT) scan uses a series of X-rays to scan parts of your body. A computer is
then used to build up detailed images of your body.
This produces cross-sectional images of your spinal column and the structures that surround it. Like an
MRI scan, a CT scan can pinpoint a slipped disc, although it is often not as effective.
Read more about CT scans.
Discography
A discography is a test where a special dye is injected into the disc in your spine.
An X-ray will then be taken to show how the dye has spread around your back. The image will reveal any
tears or leaks from your disc.
Other causes
The tests listed above can be used to check that your back painis not being caused by another health
condition such as:
a tumour (growth)
an infection
arthritis a painful condition that affects the joints and bones
In most cases, a slipped disc will eventually shrink back spontaneously. Any pain will usually
ease as the disc stops pressing on the affected nerve.
It usually takes four to six weeks to recover from a slipped disc. Most people will need to do some gentle
exercises and may need to take painkilling medication.
Keeping active
It is very important that you keep active if you have a slipped disc.
Initially, it may be difficult to move around and if you are in severe pain, you may need to rest completely
for the first couple of days.
However, after this period, you should start to move around as soon as you can. This will keep your back
mobile and speed up your recovery.
You should ensure that any exercise you do is gentle and does not put a strain on your back. Swimming
is an ideal form of exercise because the water supports your weight and it puts very little strain on your
joints.
Movement and exercise will also help to strengthen any muscles that have become weak. Avoid any
activities that could aggravate your condition such as those that involve:
reaching
lifting
sitting for a prolonged period of time
Physiotherapy
As part of your treatment programme, you may be referred to a physiotherapist. Physiotherapists
are healthcare professionals who use physical methods, such as massage and manipulation.
A physiotherapist will be able to draw up an individually tailored exercise plan for you. This will keep you
active, minimise pain and help prevent any further damage to your back.
Read more about physiotherapy.
Osteopathy and chiropractic
Some people choose to try osteopathy or to see a chiropractor. Both types of therapy are used to treat
back pain.
Osteopathy and chirpractic are not widely available on the NHS and you will usually have to pay for
treatment privately.
Read more about osteopathy and chiropractic.
Medication
Treatment of cauda equina syndrome is necessary to maximize the likelihood of the bladder and bowel
function. Treatment may also prevent further weakness in the lower extremities. Left untreated, cauda equina
syndrome can result in paraplegia.
Those experiencing any of the red flag syndromes should seriously consider seeing a neurosurgeon, who
provides the operative and non-operative management of neurological disorders. Prompt surgery is the best
treatment for patients with cauda equina syndrome. Treating patients within 48 hours after the onset of the
syndrome provides a significant advantage in improving sensory and motor deficits as well as urinary and rectal
function. Even patients who undergo surgery after the 48-hour ideal time frame may experience significant
improvement. Although short-term recovery of bladder function may lag behind reversal of lower extremity
motor deficits, the function may continue to improve years after surgery. Following surgery, drug therapy
coupled with intermittent self-catheterization can help lead to slow but steady recovery of bladder and sphincter
function.
Although steroids have proven useful in the treatment of spinal cord injury and some physicians advocate
steroids for cauda equina syndrome, no evidence suggests that they are useful in treatment of cauda equina
compression. In fact, some physicians point to the potential risks of high-dose steroid use and do not advocate
their use to treat cauda equina syndrome.
You may be prescribed a number of different medicines to help ease any painful symptoms of a slipped
disc. These are outlined below.
Analgesics
Analgesics are painkillers, such as paracetamol. They are available over-the-counter from pharmacies,
or on prescription.
Always read the manufacturers instructions before using analgesics.
Non-steroidal anti-inflammatory drugs
Non-steroidal anti-inflammatory drugs (NSAIDs), such asibuprofen, diclofenac and naproxen, can help
relieve pain and reduce any inflammation.
NSAIDs may not be suitable for people with hypertension(high blood perssure), asthma, heart failure,
or kidney failure. Again, you should always read the manufacturers instructions before use.
Read more about NSAIDs.
Codeine
Codeine is a stronger painkiller that is often taken in combination with paracetamol. It is usually only
prescribed when other painkillers and NSAIDs have not worked.
Codeine can cause side effects, such as constipation (an inability to empty your bowels).
Corticosteroids
Corticosteroids are a type of medication that contain hormones (powerful chemicals that have a wide
range of effects on your body). They may be injected into your lower spine to help reduce inflammation.
Read more about corticosteroids.
Muscle relaxants
You may be prescribed a muscle relaxant, such asdiazepam, to take for a few days if your back or leg
muscles are very tense.
Surgery
Surgery is required in about 1 in 10 cases of a slipped disc. It may be considered if:
there is evidence of severe nerve compression
your symptoms have not improved using other treatments
you are having difficulty standing or walking
you have very severe symptoms, such as progressive muscle weakness or altered
bladder function
The aim of surgery is to cut away the piece of the disc that bulges out. This is known as a discectomy and
it can be done in several ways.
Some of these procedures are explained in more detail below.
Open discectomy
An open discectomy is a procedure to remove part or all of the slipped disc. It will be carried
out under anaesthetic(painkilling medication).
An incision is made in your spine and the disc is removed. For more information about this type of
surgery, see the lumbar decompressive surgery topic.
Prosthetic intervertebral disc replacement
Prosthetic intervertebral disc replacement involves having a prosthetic (artificial) disc inserted into your
back to replace the slipped disc.
An incision is made in your spine and the damaged disc is either partially or completely removed. A
replacement disc is then inserted into the space.
One study found that 87% of people felt their quality of life had improved three months after having a
prosthetic intervertebral disc replacement. However, as the procedure is still quite new, long-term results
are not yet available.
Endoscopic laser discectomy
During endoscopic laser surgery, a small incision will be made to gain access to the spine and an
endoscope will be used to view the disc. An endoscope is a long, thin, flexible tube with a light and
camera at one end.
The procedure is performed under either local anaestheticor general anaesthetic, depending on where in
your spine your slipped disc is.
After the incision has been made, the compressed nerve that is causing you pain will be released and
part of your disc will be removed with a laser.
A study has found that 67% of people could move around more easily six months after having endoscopic
laser surgery, and around 30% needed less pain relieving medication. Around 2-4% of people needed
another operation.
Another study reported that after having endoscopic laser surgery, on average, people returned to work
after seven weeks.
As endoscopic laser surgery is still a relatively new procedure, it is often only performed with special
arrangements for example, as part of a clinical trial (a type of medical research that tests one type of
treatment against another).
Recovery
For most people with severe symptoms of a slipped disc, back surgery helps to ease their symptoms.
You will usually be able to return to work after two to six weeks. However, the surgery does not work for
everyone, and you may need to have further operations and treatment if the initial surgery is not effective.
Possible complications resulting from surgery may include:
infection
nerve injury
haemorrhage (severe bleeding)
temporary dysaesthesia (impaired sense for example, losing the sense of touch)
Exercise
Regular exercise can slow down the age-related deterioration of the discs in your back. It can also help
keep your supporting back muscles strong and supple.
Before and after any workout or sports activity, you should warm up and cool down properly. Your warm
up and cool down should incorporate stretching exercises.
If you are recovering from a slipped disc, avoid high impact activities, such as running and aerobics.
Read more about how to warm up before exercising and how to stretch after exercising.
Lifting
It is very important when lifting that you use the correct technique. When lifting heavy objects you should:
think before you lift and make sure you can manage the weight
slightly bend your back, hips and knees at the start of the lift
keep the load close to your waist
avoid twisting your back or leaning sideways
keep your head up and look ahead as you carry the load
Read more about how to lift safely.
Sitting
When sitting or driving for long periods make sure that your seat is comfortable and supportive. If
possible, take regular breaks to stretch and walk around.
If your job involves using a computer, take regular breaks away from the computer screen. Make sure that
the computer screen is at eye level and directly in front of you so that you do not have to twist or bend to
see it.
Sit in a comfortable position with enough space to move around, and do not stay in the same position for
too long.
Your employer should give you information about working with computers and provide advice about the
best way to sit and position your equipment.
Read more about how to sit correctly.
Posture
Always try to keep good posture. Walk or stand with your head and shoulders slightly back.
When sitting at a desk, make sure that your chair is the correct height for the desk. Your feet should be
able to rest flat on the floor with your knees bent at 90 degrees.
You might also like
- Asphalt Plant Inspection ChecklistDocument16 pagesAsphalt Plant Inspection ChecklistJagan Mohana Rao Chinnala100% (2)
- Cauda Equina Syndrome Is A Medical Emergency That Calls For Urgent Surgical InterventionDocument11 pagesCauda Equina Syndrome Is A Medical Emergency That Calls For Urgent Surgical Interventiondezi981No ratings yet
- Lec3 DiscDocument50 pagesLec3 Discsana mumtazNo ratings yet
- Spinal Stenosis 3Document8 pagesSpinal Stenosis 3hunter_axl01No ratings yet
- Degenerative Disc DiseaseDocument13 pagesDegenerative Disc Diseasehouki shanaNo ratings yet
- Prolapsed Disc (Slipped Disc) : Post Your Experience See OthersDocument5 pagesProlapsed Disc (Slipped Disc) : Post Your Experience See OthersBharat VishwamitraNo ratings yet
- Degenerative Disk DiseaseDocument3 pagesDegenerative Disk DiseasevishwanathNo ratings yet
- SciaticaDocument25 pagesSciaticaBenita Putri MD100% (1)
- Sciatica Nerve (Causes and Treatment)Document4 pagesSciatica Nerve (Causes and Treatment)esmollahanNo ratings yet
- Lumbage SciaticaDocument2 pagesLumbage SciaticaNisar AhmedNo ratings yet
- Spinal Cord CompressionDocument7 pagesSpinal Cord CompressionDashNo ratings yet
- Generic NameDocument4 pagesGeneric NameupinandipinNo ratings yet
- Lumbar Disk HerniationDocument6 pagesLumbar Disk HerniationShivaji DeshmukhNo ratings yet
- Backache-Prevention and Cure: DR Abhinav GuptaDocument48 pagesBackache-Prevention and Cure: DR Abhinav GuptaAbhinav GuptaNo ratings yet
- Low Back Pain and SciaticaDocument24 pagesLow Back Pain and SciaticaOVVCMOULINo ratings yet
- Herniated Nucleus PulposusDocument3 pagesHerniated Nucleus Pulposusdrin21No ratings yet
- What Structures Make Up The Back?Document11 pagesWhat Structures Make Up The Back?MariaTheresiaNo ratings yet
- Low Back Pain 20-ns-5161 March 2020 508cDocument24 pagesLow Back Pain 20-ns-5161 March 2020 508cRajib ChowdhuryNo ratings yet
- Lumbar Disc Herniation: Prof - Dr.Hidayet Sarı Physical Medicine and Rehabilitation DepartmentDocument19 pagesLumbar Disc Herniation: Prof - Dr.Hidayet Sarı Physical Medicine and Rehabilitation DepartmentAnonymous pJfAvlNo ratings yet
- Spondylosis Information LeafletDocument3 pagesSpondylosis Information LeafletAnis Azizah MogilNo ratings yet
- Lumbar DiscectomyDocument4 pagesLumbar Discectomyapi-549337910No ratings yet
- Anatomy: Cervical Disk DegenerationDocument5 pagesAnatomy: Cervical Disk DegenerationSUALI RAVEENDRA NAIKNo ratings yet
- Sciatic NerveDocument2 pagesSciatic NerveLulu SupergirlNo ratings yet
- Dr. K.B.Sudhikumar Prof. & HOD Dept. of Salyatantra, GAC, TripunithuraDocument69 pagesDr. K.B.Sudhikumar Prof. & HOD Dept. of Salyatantra, GAC, Tripunithuraapi-73271717No ratings yet
- Lumbar Disc Herniation: Prof - Dr.Hidayet Sarı Physical Medicine and Rehabilitation DepartmentDocument20 pagesLumbar Disc Herniation: Prof - Dr.Hidayet Sarı Physical Medicine and Rehabilitation DepartmentraraNo ratings yet
- Lumbar Radiculopathy SyndromeDocument2 pagesLumbar Radiculopathy SyndromeAqsa KiranNo ratings yet
- HNP 1Document4 pagesHNP 1Kirsten CajayonNo ratings yet
- Low Back Pain-Orthoinfo - AaosDocument13 pagesLow Back Pain-Orthoinfo - AaosBang mantoNo ratings yet
- Total Rehabilitation: The Benefits of Aquatic TherapyDocument6 pagesTotal Rehabilitation: The Benefits of Aquatic TherapyAleCsss123No ratings yet
- What Structures Make Up The Back?: CongenitalDocument5 pagesWhat Structures Make Up The Back?: Congenitalselvi lestariNo ratings yet
- Lumbar Disc HerniationDocument19 pagesLumbar Disc HerniationPutri WulandariNo ratings yet
- SciaticaDocument4 pagesSciaticaLev KalikaNo ratings yet
- Sciatica: Pseudosciatica or Non-Discogenic Sciatica, Which Causes Symptoms Similar To Spinal NerveDocument5 pagesSciatica: Pseudosciatica or Non-Discogenic Sciatica, Which Causes Symptoms Similar To Spinal NerveLeah BakerNo ratings yet
- Lumbar Spinal Stenosis: A Definitive GuideDocument4 pagesLumbar Spinal Stenosis: A Definitive GuideGuyNo ratings yet
- Cauda Equina Syndrome: A Beginner's Overview to Managing CES Through Natural Methods and Diet, With Sample Recipes Kindle EditionFrom EverandCauda Equina Syndrome: A Beginner's Overview to Managing CES Through Natural Methods and Diet, With Sample Recipes Kindle EditionNo ratings yet
- Herniated Nucleus PulposusDocument5 pagesHerniated Nucleus PulposusNestle FolienteNo ratings yet
- Jawahar Navodaya Vidyalaya Kagal KolhapurDocument27 pagesJawahar Navodaya Vidyalaya Kagal KolhapurSujay NirmaleNo ratings yet
- Herniated Nucleus Pulposus - Herniated DiscDocument4 pagesHerniated Nucleus Pulposus - Herniated DiscArvieDelfinNo ratings yet
- NeckDocument40 pagesNeckPrabhat Kumar SinghNo ratings yet
- Herniated Disk in The Lower Back: AnatomyDocument6 pagesHerniated Disk in The Lower Back: AnatomyLate ArtistNo ratings yet
- SciaticaDocument4 pagesSciaticaVenkatesan VidhyaNo ratings yet
- Herniated Nucleus Pulposus - TrixieDocument7 pagesHerniated Nucleus Pulposus - TrixieThelma P. SabileNo ratings yet
- Spinal Nerve PicDocument6 pagesSpinal Nerve PicJacklynlim LkcNo ratings yet
- Herniated Disk (Princess)Document4 pagesHerniated Disk (Princess)Evangel PaduaNo ratings yet
- Herniated Lumbar Disc HLDDocument4 pagesHerniated Lumbar Disc HLDShobhit GajbhiyeNo ratings yet
- Types of Spine Curvature DisordersDocument7 pagesTypes of Spine Curvature DisordersNicu MacariNo ratings yet
- 6 - Lumbar Disc HerniationDocument24 pages6 - Lumbar Disc HerniationHADI BADWANNo ratings yet
- Bahan Kuliah Degeneratif SpineDocument51 pagesBahan Kuliah Degeneratif SpineDudy HumaediNo ratings yet
- Sciatica and MassageDocument61 pagesSciatica and MassageAllisynNo ratings yet
- Lower Back PainsDocument35 pagesLower Back PainsMary Les RN100% (1)
- Cervical Laminectomy: AnatomyDocument9 pagesCervical Laminectomy: AnatomyAgung Choro de ObesNo ratings yet
- Ergo Experiment 2Document15 pagesErgo Experiment 2John Paul Espineli FeranilNo ratings yet
- Low Back PainDocument8 pagesLow Back PainLev KalikaNo ratings yet
- Spondylosis: Vertebral ColumnDocument12 pagesSpondylosis: Vertebral ColumnVdct MglNo ratings yet
- Cervical Spondylosis Info ExercisesDocument8 pagesCervical Spondylosis Info ExercisesSylvia GraceNo ratings yet
- Intervertebral Disc Prolapse: AnnulusDocument2 pagesIntervertebral Disc Prolapse: AnnulusIndra KurniawanNo ratings yet
- Back PainDocument22 pagesBack PainmelissaparkonNo ratings yet
- Lumbar Radioculopathy HomeworkDocument12 pagesLumbar Radioculopathy Homeworkbeta100% (1)
- Spinal Stenosis And Pinched Nerve A Simple Guide to These conditionsFrom EverandSpinal Stenosis And Pinched Nerve A Simple Guide to These conditionsRating: 5 out of 5 stars5/5 (1)
- Reading Tháng 8-23Document11 pagesReading Tháng 8-23Phạm LinhNo ratings yet
- Topic 2: Biology, Biotechnology & Health SciencesDocument4 pagesTopic 2: Biology, Biotechnology & Health SciencesSmail TayebNo ratings yet
- Clariant - Hydroperm RPU New Liq C - FTDocument4 pagesClariant - Hydroperm RPU New Liq C - FTAna AntunesNo ratings yet
- PSI Online Proctored Exam Setup Guide Sep 2020Document7 pagesPSI Online Proctored Exam Setup Guide Sep 2020JoaoNo ratings yet
- Ben Senouci Douidi: Certificate of AchievementDocument2 pagesBen Senouci Douidi: Certificate of AchievementDakota624No ratings yet
- AV157 ManualDocument8 pagesAV157 ManualtbelhumeurNo ratings yet
- Intelidrive Lite 2 5 0 New FeaturesDocument19 pagesIntelidrive Lite 2 5 0 New Featuresluat1983No ratings yet
- Industrial Department IncentivesDocument5 pagesIndustrial Department IncentivesKUMARNo ratings yet
- 07 - ATA-38 - E170 - 86pgsDocument86 pages07 - ATA-38 - E170 - 86pgsAlexander Mcfarlane100% (1)
- LABOR LAW I - Finals Case DigestsDocument8 pagesLABOR LAW I - Finals Case DigestsLDNo ratings yet
- Programming For Competitive CrossfitDocument53 pagesProgramming For Competitive CrossfitcamilcaNo ratings yet
- Santosh - Sep - 2021Document1 pageSantosh - Sep - 2021santoshkumarNo ratings yet
- Kirloskar Brothers LimitedDocument36 pagesKirloskar Brothers Limitedgopalakrishnannrm1202No ratings yet
- Iep-Case 8Document9 pagesIep-Case 8api-238729229No ratings yet
- ANT-ATR4517R10v06-2579 DatasheetDocument2 pagesANT-ATR4517R10v06-2579 DatasheetSilviuSNo ratings yet
- Living Magazine doTERRA Spring 2018 Living MagazineDocument29 pagesLiving Magazine doTERRA Spring 2018 Living Magazineczinege_zoltan3079No ratings yet
- 05 Steam TurbineDocument11 pages05 Steam TurbineJohn Paulo ArchinueNo ratings yet
- Interim Valuation 1Document11 pagesInterim Valuation 1musthaqhassan100% (1)
- Column Piping: Study Layout, Nozzle Orientation & Platforms RequirementsDocument23 pagesColumn Piping: Study Layout, Nozzle Orientation & Platforms RequirementsArindomNo ratings yet
- Dying Without A Will in PennsylvaniaDocument2 pagesDying Without A Will in PennsylvaniaStephen Garrett100% (7)
- The Potential of 3D Printing To Reduce The Environmental Impacts of ProductionDocument9 pagesThe Potential of 3D Printing To Reduce The Environmental Impacts of ProductionAlexi WiedemannNo ratings yet
- Shrimp Farming in Biofloc System - PDFDocument33 pagesShrimp Farming in Biofloc System - PDFrajansingNo ratings yet
- Urg OftaDocument6 pagesUrg OftaDANIELANo ratings yet
- People vs. Siao, G.R. No. 126021 March 3, 2000Document3 pagesPeople vs. Siao, G.R. No. 126021 March 3, 2000Ria Evita RevitaNo ratings yet
- Pretes OBGYNEDocument4 pagesPretes OBGYNEAltheaNo ratings yet
- Chapter 13Document31 pagesChapter 13DrakzNo ratings yet
- Mobile Train Radio Communication PPT SlideshareDocument28 pagesMobile Train Radio Communication PPT SlideshareSuchith RajNo ratings yet
- 2019 Bece Integrated Science 2Document3 pages2019 Bece Integrated Science 2Divine Kofi AgedeNo ratings yet
- Parasitology For DummiesDocument8 pagesParasitology For DummiesimranNo ratings yet