Professional Documents
Culture Documents
Management of Frontal Sinus Fractures: Summary
Management of Frontal Sinus Fractures: Summary
Uploaded by
Alexandru Badea0 ratings0% found this document useful (0 votes)
43 views17 pagesfrontal bone
Original Title
Management
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentfrontal bone
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
43 views17 pagesManagement of Frontal Sinus Fractures: Summary
Management of Frontal Sinus Fractures: Summary
Uploaded by
Alexandru Badeafrontal bone
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 17
CRANIOFACIAL
Management of Frontal Sinus Fractures
Spiros Manolidis, M.D.
Larry H. Hollier, Jr., M.D.
New York, N.Y.; and Houston, Texas
Summary: Frontal sinus fractures are relatively uncommon maxillofacial inju-
ries, making up only 5 to 12 percent of all facial fractures. Associated intracra-
nial, ophthalmologic, and other maxillofacial injuries are very common because
of the force of injury required to fracture the frontal bone. High-resolution
computed tomography of the frontal region in multiple planes is essential for
predicting the degree of frontal injury, associated injuries, and the type of proce-
dure indicated. Exploration of the frontal sinus with reduction alone is reserved for
a small minority of very simple fractures. Most frontal sinus fractures will require the
obliteration of the sinus. This is achieved in the majority of instances with preser-
vation of the posterior wall. Those with more extensive injuries and the presence
of a cerebrospinal fluid leak will require frontal sinus cranialization after repair of
the dural injuries. In rare instances, primary bone grafts will be required. In both
cranialization and obliteration procedures, the nasofrontal ducts must be managed
appropriately to avoid complications. Newer techniques involving endoscopic im-
age-guidedsurgery may offer analternative for a small subset of patients withfrontal
sinus injury. (Plast. Reconstr. Surg. 120 (Suppl. 2): 32S, 2007.)
F
rontal sinus fractures account for 5 to 15
percent of all maxillofacial fractures.
1,2
As-
saults and vehicular trauma account for the
majority of frontal sinus injuries. Frontal sinus frac-
tures have been associated with severe maxillofacial
and systemic injuries, with a high rate of morbidity
and mortality.
3,4
The management of frontal sinus
injury is an important topic, as inappropriate man-
agement of these injuries not only leads to cosmetic
deformities and functional problems but may give
rise to serious complications, including the devel-
opment of mucoceles, osteomyelitis, and potentially
fatal central nervous system complications such as
meningitis and brain abscesses.
1,5,6
Several aspects of frontal sinus injury treatment
remain controversial secondary to the relatively
small numbers of patients reviewed in the literature
andthedifficulty inmaintaininglong-termfollow-up
in these patients.
6
Areas of controversy include the
roles of frontal sinus obliteration, cranialization, and
nasofrontal duct stenting in the acute trauma setting.
7
BIOMECHANICS
The frontal bone is the strongest component
of the craniofacial skeleton. It can withstand be-
tween 800 and 2200 pounds of force before
fracturing.
8
In an average size adult human, these
forces can be reached with a frontal collision at 30
mph for an unrestrained passenger.
9,10
Because of
its projectionandthe large surface area it occupies
relative to the rest of the facial skeleton, the frontal
region is frequently the first site of exposure in
both vehicular and assault injuries.
The anterior table of the frontal sinus is the
stronger component of the two bone tables of the
frontal sinus because of its overall thickness, es-
pecially along the supraorbital buttress. The pos-
terior table is thinner and is not part of this but-
tress system. The dura is densely adherent to the
deep surface of the posterior table. The dura be-
comes thinner and more adherent along the cau-
dal edge, where it turns to cover the roof of the
ethmoid air cells (fovea ethmoidalis). When sig-
nificant fractures of the frontal bone occur, these
propagate easily and extensively along the orbital
and nasoethmoid complexes, which have signifi-
cantly weaker tolerances.
9,10
Injuring forces capa-
From the Department of OtolaryngologyHead and Neck Sur-
gery, Beth Israel Hospital, and Baylor College of Medicine and
Department of Plastic Surgery, Ben Taub General Hospital.
Received for publication May 8, 2006; accepted January 18,
2007.
Copyright 2007 by the American Society of Plastic Surgeons
DOI: 10.1097/01.prs.0000260732.58496.1b
Disclosures: Neither of the authors has received
funds or support or has a financial interest in any
of the products, devices, or drugs mentioned in this
article. Dr. Manolidis lectures as part of the faculty
for the North American AO-ASIF group and for
that, in the past, has received stipends for attend-
ing/lecturing at their educational conferences.
www.PRSJournal.com 32S
ble of disrupting the anterior table will frequently
involve the posterior table and the elements of the
floor of the anterior cranial fossa: the fovea eth-
moidalis and cribriform plate. Injuring forces capa-
ble of disrupting the anterior table will frequently
involve the posterior table and the elements of the
floor of the anterior cranial fossa: the fovea eth-
moidalis andcribriformplate. This leads to the com-
monintraoperative finding of comminutedanterior
table with posterior table fractures and associated
dural tears capable of producing cerebrospinal fluid
leaks.
The nasofrontal duct opening usually lies in
the posteromedial floor of the sinus and runs cau-
dally to the anterior middle meatus. Significant
anatomical variations exist in the width, length,
and shape of the nasofrontal duct.
7
These ana-
tomical variations make it difficult to predict with
accuracy the future functioning of the nasofrontal
duct in the face of frontal sinus injury.
In addition, forces that are capable of fractur-
ing the supraorbital buttress will frequently cause
comminuted, displaced fractures of the superior
orbital rim that typically involve the frontonasal
duct. These fractures are associated with a dispro-
portionate number of ocular injuries and other
orbital injuries withlong-termeffects onvision.
11,12
Occasionally, fractures of the frontal region will
extend to the skull base beyond the anterior cra-
nial fossa into the middle cranial fossa fractures
that course throughthe foramina of the skull base.
In severe injuries, attention should be given to the
temporal bone, as these fractures canextendthrough
the temporal bone with severe consequences for
both hearing and facial nerve function, and with
the potential for a cerebrospinal fluid leak through
the temporal bone.
2,13
Occasionally, forces will be transmitted through
the anterior table, without its fracturing, to struc-
tures posterior to it. Such patterns of injury account
for isolated nasofrontal duct injuries, with subse-
quent frontal sinus complications if left untreated.
14,15
Rarely, suchforces canbetransmittedmoreposteriorly
toinvolvetheopticcanal or thesuperior orbital fissure,
causing visual loss and/or superior orbital fissure syn-
drome, respectively
1618
(Fig. 1).
The geometry of the impact is also a significant
factor in frontal sinus fractures. Sharp objects that
impart much greater force in a smaller surface
area and blunt heavy objects that transfer larger
amounts of energy will cause increasing amounts
of trauma, such as that commonly seen in assault.
Gunshot injuries, especially high velocity, and in-
dustrial accidents will invariably fracture both an-
terior and posterior tables of the frontal sinus and
breach the anterior cranial fossa. Under these cir-
cumstances, posterior table fractures are invari-
ably associated with dural tears and fractures ex-
tending to the anterior cranial base to involve the
cribriform plate and fovea ethmoidalis.
ANATOMY AND EMBRYOLOGY
The frontal sinus is in critical approximation
to anatomical structures, which underscores the
importance of its management in injury. Posteri-
orly, the cribriform plate, dura mater, and frontal
lobes are in close apposition to one another and
to the posterior wall of the sinus. The dura is
densely adherent to the deep surface of the pos-
terior table and becomes more adherent and thin-
ner along the caudal edge, where it turns to cover
the fovea ethmoidalis.
The frontal sinus develops starting at infancy
from the middle meatus, with continuous growing
through early adulthood, attaining an average vol-
ume of 5 cm
3
. The frontal sinuses are absent at birth
and do not begin to develop until the second year of
life.
19
The frontal sinus itself cannot be identified
radiographically until approximately the age of 8
years, and it does not reach adult size until age 12
years or older. In 10 percent of persons, the frontal
sinus develops unilaterally, in 5 percent it is a rudi-
mentary structure, and in 4 percent it is absent al-
together, so that almost one-fifth of individuals have
aberrant sinus development.
20
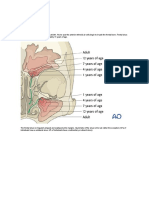
The frontal sinuses develop from the ethmoid
infundibular air cells by invagination of the frontal
bone throughthe frontal recess or fromthe superior
meatus
21
(Fig. 2). The size of the adult frontal sinus
shows exceptional variability in the degree of pneu-
matization. Sinus pneumatization begins from the
Fig. 1. Fractures involvingthesuperior orbital ssureandopticca-
nal region(left side) andthe lateral orbital wall posteriorly at the re-
gionof thesuperior orbital ssure(right side). Thispatient presented
with minimal frontal sinus trauma and bilateral loss of vision.
Volume 120, Number 7 Suppl. 2 Frontal Sinus Fractures
33S
nasal part of the frontal bone by several ethmoid air
cells at once, which are termed frontal bullae. This
multiplicity of pneumatization results in variability
and tortuosity of the frontal sinus drainage pathway
(nasofrontal duct).
An intersinus septum separates the two sides.
The frontal sinus may consist of one or more com-
partments, depending on the source of pneuma-
tization. The intersinus septum, which separates
these compartments, is continuous with the crista
galli inferiorly, whereas its superior attachment to
the sinus walls is frequently asymmetrical. When
this septum is asymmetrical, the crista galli shows
varying degrees of pneumatization and protrusion
within the sinus. In this situation, a surgical risk
exists for entering the anterior cranial fossa at the
cribriform plate (olfactory groove) if this area is
mistaken for the posterior wall of the frontal sinus
(Fig. 3).
The lateral floor of the frontal sinus is the roof
of the orbit, whereas the medial floor of the frontal
sinus contains the opening of the nasofrontal
duct.
7
The nasofrontal duct is the exclusive drain-
age of the frontal sinus and thus of utmost clinical
significance in the management of frontal sinus
injury. Its course is highly variable, running cau-
dally from a few millimeters to up to 2 cm.
22
A true
identifiable duct may be absent inup to 85 percent
of frontal sinuses. In this situation, the frontal
sinus drains indirectly throughethmoid air cells to
the middle meatus
7
(Fig. 4).
The nasofrontal duct terminates at the unci-
nate process in the nasal cavity, which is a thin
bone plate that is covered on either side by mu-
cosa. On computed tomographic scans, the infe-
rior portion of the uncinate process is mostly vis-
ible, whereas the superior portion of the uncinate
Fig. 2. Development of thefrontal sinusthroughinvaginationof
the frontal bone by ethmoidal air cells.
Fig. 3. Variations inthedepth(relativedownwarddisplacement of thecribriformplate) is relatedtothelocationof the
fovea ethmoidalis, that is, the pneumatization of the ethmoid air cells. In this gure, the fovea ethmoidalis is the intra-
cranial surface that overlies the ethmoid air cell labyrinth.
Plastic and Reconstructive Surgery December Supplement 2, 2007
34S
process cannot be identified in up to 40 percent
of cases.
23
There are twoidentifiable patterns of drainage
of the frontal sinus. When the uncinate process is
attached to the lamina papyracea, the drainage is
medial to the uncinate process through the mid-
dle meatus. This type of drainage pattern is seen
in 66 to 88 percent of cases.
20,24
When the uncinate
process attaches superiorly to more medial struc-
tures (middle turbinate, cribriform, or skull base),
the drainage of the sinus is lateral to the uncinate
process. This type of drainage pattern is seen in 12
to 34 percent of cases.
24,25
A significant feature of the frontal sinus is
the mucosal lining, which is contiguous with
that of the ethmoid air cells and nasofrontal
ducts. The mucosal lining of the frontal sinus
consists of ciliated columnar epithelium. The
cilia of these cells are bathed by a proteinaceous
solution (mucus). Through ciliary motion, this
mucous layer moves in a clockwise fashion to-
ward the nasofrontal duct, from where it is ul-
timately expelled into the hiatus semilunaris
and then nasal cavity (Fig. 5).
The frontal sinus is unique in that it is the only
sinus that has a recirculation phenomenon. The
mucus travels along the lateral side of the sinus
and turns medially over the sinus floor and down
the lateral frontal recess wall. Of the secretion, 60
percent is directed back into the sinus cavity as it
reaches the frontal recess.
26
Mucus is produced by goblet cells interspersed
in the ciliated mucosa of the frontal sinus. Clinically
significant anatomical structures of the mucosa of
the frontal sinus are the foramina of Breschet, first
described over 60 years ago.
27
These foramina are
sites of venous drainage of the mucosa andcanserve
as the route of intracranial spread of infection.
3
The
mucosais founddeeply invaginatingtheseforamina.
If mucosa is not completely removed microscopi-
cally from these foramina in obliteration or crani-
alizationprocedures, there is a highriskof mucocele
formation.
2831
CLASSIFICATION OF INJURIES
Numerous classificationschemes of frontal sinus
fractures have been described. The lack of unifor-
mity intreatment andsmall numbers of suchinjuries
have contributed to this situation. Most classifica-
tions are based on anatomical location and obser-
vations of intraoperativefindings incomparisonwith
preoperative evaluations by high-resolution com-
puted tomography.
1,32,33
Early work by Manson and
others derived classification schemes of frontal and
midface injuries basedonthese principles that are in
wide use today.
3436
Elaborate classification schemes with multiple
subdivisions do not add significantly in the manage-
ment of frontal sinus injuries, as the operative op-
tions are limited.
37
Most authors agree that three
components related to the frontal sinus must be
taken into account: the anterior table, the posterior
table, and the nasofrontal duct.
1,7,15,33,38
In addition,
injury to the dura, presence of cerebrospinal fluid
leak, and open cerebral trauma, most frequently
associated with tissue loss, must be taken into ac-
count ina classificationof frontal sinus injury. Three
further observations cansimplify the classificationof
frontal injuries: (1) isolated posterior table fractures
are rare entities of questionable significance; (2)
involvement of the anterior and posterior tables in-
Fig. 4. Sagittal transparency viewof thenasofrontal duct andits
relation to the ethmoidal labyrinth. Drainage is through the hia-
tus semilunaris underneath the middle turbinate.
Fig. 5. Mucociliaryowof thefrontal sinus, invaginations of mu-
cosa into the bone at the foramina of Breschet.
Volume 120, Number 7 Suppl. 2 Frontal Sinus Fractures
35S
variably leads to frontonasal duct injury; and (3)
involvement of the nasoethmoid complex and me-
dial orbital riminthe fracture patternalsoinvariably
leads to frontonasal duct injury.
32,33
A classification
scheme that might include these principles would
appear similar to that presented in Figure 6.
ASSOCIATED INJURIES
Ocular Injuries
Ophthalmologic injury is seen in as many as 25
percent of those with frontal sinus injuries. The
range of these ophthalmologic problems in these
Fig. 6. Classication of frontal sinus injuries: type 1, linear, minimally displaced fractures of
the outer wall; type 2, comminuted or depressed anterior table fractures (may or may not
involve the nasofrontal duct); type 3, bothanterior andposterior frontal sinus walls involved
by comminuted fractures; type 4, comminuted anterior and posterior wall fractures with
dural injury and potential cerebrospinal uid leak; and type 5, comminuted anterior and
posterior wall fractures withdural injury andpotential cerebrospinal uidleak inadditionto
tissue and/or bone loss. (Reprinted with permission from Semin. Plast. Surg. 16: 2002.)
Plastic and Reconstructive Surgery December Supplement 2, 2007
36S
patients is wide. The most common abnormal
finding, in up to 10 percent of those with a frontal
sinus fracture, is an afferent pupillary defect sec-
ondary to optic nerve involvement (Fig. 1). Such
optic nerve involvement must be assessed carefully
by high-resolution computed tomography. The
management of optic nerve involvement by high-
dose steroids versus optic nerve decompression is
controversial. The treatment of optic nerve in-
volvement supersedes the correction of frontal
sinus fractures with the exception of central ner-
vous system injury requiring acute management,
severe soft-tissue loss, and/or exposure of brain
parenchyma.
Involvement of the superior orbital rim and/or
orbital roof will increase the chance of ocular injury
to 25 percent.
11,39
The most significant of these in-
juries, open globe or globe rupture, though rarely
seen, is usually a devastating injury that results in
visual loss. In this situation, concurrent enucleation
must be considered along with preparation of the
anophthalmic socket for an ocular implant. Lesser
degrees of injury, such as hyphema, retinal detach-
ments, andcorneal lacerations, shouldbe diagnosed
and treated before surgical intervention for the cor-
rection of frontal sinus injuries. Particular attention
should be given to factors that might result in cor-
neal exposure: facial paralysis froma temporal bone
injury or other injury to the facial nerve. Lid lacer-
ations should be repaired primarily as early as pos-
sible. A complete ophthalmologic examination
should be carried out as soon as feasible and visual
acuity tests should be performed as soon as the pa-
tient is awake and cooperative.
Neurologic Injuries
Over half of the patients with frontal sinus
fractures present with some form of neurologic
injury, and these span a wide range.
1,7,15,33,38,40
The
majority of patients who sustain a frontal sinus
fracture will have experienced loss of conscious-
ness. Closed head injury with evidence of cerebral
contusion by computed tomography and/or mag-
netic resonance imaging is very common. Sub-
dural and epidural hematomas requiring imme-
diate neurosurgical intervention occur in 10
percent of patients.
1
Open cerebral injuries are
seen in the most severe form of frontal sinus frac-
tures and are found in 2.5 to 13 percent of these
patients.
1,40,41
Depressed skull fractures other than
those of the frontal bone are also a common fea-
ture in severe motor vehicleassociated frontal si-
nus fractures.
3
A worrisome aspect of frontal sinus
fractures is the presence of a cerebrospinal fluid
leak on presentation or on exploration. Up to
one-third of patients with frontal sinus fractures
will present with a cerebrospinal fluid leak.
7,30,38,42
This may be the result of injury to the posterior
wall and subsequent disruption of the attached
dura and/or the result of a disruption of the an-
terior cranial fossa floor at the level of the cribri-
form plate or the fovea ethmoidalis.
43
Pneumo-
cephalus is frequently seenoncomputedtomography
in injuries of the frontal sinus. Pneumocephalus is not
a reliable or consistent signfor neurologic injury or for
the presence of a cerebrospinal fluid leak. Pneumo-
cephalus frominjury tothefrontal sinus may becaused
by involvement of the cribriform, the fovea ethmoida-
lis, the orbit, or other regions of the skull and/or skull
base; thus, it is not a specific or sensitive measure of a
potential cerebrospinal fluid leak. In instances of se-
vere frontobasilar injury with or without tissue loss,
cerebrospinal fluid leaks are obvious (Fig. 7).
Associated Maxillofacial Injuries
One-third to one-half of patients with frontal
injuries will have associated midface fractures.
These fractures lie in close proximity and it is safe
to assume that they will involve the nasofrontal
duct region, which predisposes to early and late
complications. Both medial orbital rim and naso-
orbito-ethmoid fractures are associated with a very
high involvement of the nasofrontal duct
15,32,33
(Fig. 8). This necessitates management of the
frontal sinus by obliteration or cranialization.
7,32
Medial orbital rim fractures, seen as part of the
supraorbital bar involvement in frontal sinus frac-
tures, are seen in up to 20 percent of frontal sinus
injuries. With increasing involvement of the na-
soethmoid/midface region, progressive collapse/
telescoping of the ethmoid labyrinth is seen. In
addition to the obvious implications for orbital
reconstruction vis-a`-vis the medial canthal com-
plex, the potential for involvement of the fovea
ethmoidalis (the roof of the ethmoid labyrinth)
and the cribriform plate increases. Naso-orbito-
ethmoid fractures are addressed after the frontal
sinus is obliterated/cranialized and its fractures
reduced in the sequencing of complex craniofa-
cial injuries.
With orbital involvement along with frontal
sinus injury, the goal is to reconstitute the pre-
morbid orbital volume and achieve the centric
position of the globe by proper positioning of the
canthal tendons and suspensory ligaments of the
globe. This is achieved easier when only one orbit
is injured along with the frontal sinus, as the intact
side can function as a radiographic template, by
Volume 120, Number 7 Suppl. 2 Frontal Sinus Fractures
37S
three-dimensional high-resolution computed to-
mography or through the use of an intraoperative
stereolithography template. When both orbits are
injured, such reconstruction is more difficult and
based solely on precise reduction of fragments. In
either situation and in more extensive, panfacial
fractures, correction of frontal sinus fractures as-
sumes greater importance, as this region provides
the central stable reduction on which the rest of
the craniofacial skeleton may be referenced.
EXAMINATION AND
RADIOLOGIC INVESTIGATIONS
Physical Examination
Facial pain is experienced in the majority of
conscious patients (82 percent), and over half
have frontal lacerations and in a quarter of pa-
tients withfrontal sinus injury there will be a visible
depression.
18
Cerebrospinal fluid rhinorrhea or
cerebrospinal fluid in the wound is present in up
to one-third of these patients.
3
The finding of
cerebrospinal fluid in conjunction with extensive
injury places the patient in a priority for operative
intervention. When cerebrospinal fluid leak is
present with minimal injury, this presents a diag-
nostic dilemma. In this circumstance, operative
intervention of the frontal sinus is not indicated in
the absence of fractures. Acerebrospinal fluidleak
under these circumstances should then be inves-
tigated radiographically. Suspicion of a cerebro-
spinal fluid leak can be heightened with a positive
halo test. In this test, a drop of the bloody fluid is
placed on a cloth surface. If it contains cerebro-
spinal fluid, this will diffuse in a radial pattern
along with the blood. However, the fluid will mi-
grate farther than the blood, forming a halo
effect. A definite confirmation can be made by
sending a specimen for 2-transferrin analysis.
44,45
A complete ophthalmologic examination should
be carried out as soon as feasible and visual
acuity tests should be performed as soon as the
patient is awake and cooperative. Any evidence
in the drop of visual acuity and/or limitation of
extraocular movement should be further inves-
tigated by appropriate computed tomographic
scanning. The remainder of the craniofacial skele-
tonshouldbe examinedandscannedbecause of the
high incidence of associated craniomaxillofacial
injuries.
Radiographic Evaluation
Plain skull radiographs were used in the past
to screen and evaluate for fractures of the frontal
sinus, with the Caldwell and lateral views being the
most useful. When plain films are available, evi-
dence of air-fluidlevels andclouding of the frontal
sinus should be investigated further. In most cir-
cumstances, plain radiographs should be avoided,
Fig. 7. Severe cranio-orbitofrontal injury. The globe is displaced
intothe maxilla/oral cavity andthere is extensive dural exposure
and separation of the upper nasal skeleton from the skull base.
Fig. 8. View after reduction of the naso-orbito-ethmoid and
frontal region. For the displacement of the bicoronal ap, the
superior orbital nerves were downfractured and the bicoronal
incision was extended to the tragal/helical junction.
Plastic and Reconstructive Surgery December Supplement 2, 2007
38S
because their sensitivity and specificity is very low
and are time consuming to obtain, especially in a
critically ill patient. However, if a frontal sinus
obliteration/cranialization is planned, it is helpful
to obtain a 1:1 ratio frontal projection plain ra-
diograph to use as an intraoperative template for
entering the frontal sinus.
All patients with forehead lacerations and/or
palpable deformities in which the magnitude of
the injury raises suspicion for a fracture should
undergo computed tomographic scanning of the
craniofacial skeleton. In those with altered mental
status or other evidence of neurologic injury, the
evaluationshouldincludea noncontrast-enhanced
brain computed tomographic scan to assess for he-
matomas, contusions, and other brain injuries. In
patients with evidence of decrease in visual acuity or
loss of color vision, the computed tomographic scan
shouldinclude the optic foramina, orbital apex, and
sella region.
Pneumocephalus can be seen on computed
tomography with a number of injuries that may or
may not involve the frontal sinus. These may in-
volve the cribriform, the fovea ethmoidalis, and
the orbit, and thus it is not a specific or sensitive
measure of a potential cerebrospinal fluid leak. In
the absence of intracranial injury, and with min-
imal frontal injury that does not merit operative
intervention, cerebrospinal fluid leaks are best in-
vestigated with high-resolution computed tomo-
graphic cisternography and/or nasal endoscopy
after the administration of intrathecal fluorescein.
MANAGEMENT OF FRONTAL
SINUS FRACTURES
Historical Perspective
The need to surgically address the frontal si-
nus arose from infection and the related compli-
cations of frontal sinusitis. Complications of fron-
tal sinusitis in the preantibiotic era were fearsome,
with high morbidity and mortality secondary to
intracranial spread. The first reported procedure
on the frontal sinus for a mucopyocele was per-
formed by Wells in 1870.
46
Numerous operations
of limited extent that involved puncturing the an-
terior table of the frontal bone were subsequently
introduced, some with limited removal of the mu-
cosa and others with packing of the sinus or cre-
ation of an external draining sinus tract.
46
Reidel
first described ablation of the anterior sinus wall
in 1898. This was a radical, disfiguring operation
that involved removal of the frontal bone and
supraorbital bar to the posterior table of the fron-
tal sinus. Few patients could be convinced to un-
dergo this operation, even under the threat of
complications with high mortality.
46
Killian intro-
duced a variation of this procedure by preserving
the supraorbital bar but still removing the anterior
table and contents of the frontal sinus and then
collapsing the skin to the posterior table of the
frontal sinus. The Killian procedure produced less
disfigurement but had significant rates of failure
because of persistent disease at the nasofrontal
ducts and incomplete removal of all frontal sinus
mucosa.
47
After Skillern published a review of the
morbidity and mortality on the Killian procedure,
it was abandoned as a treatment option.
48
The
next significant advance in dealing with frontal
sinus infection was the Lynch operation, which
relied on exenteration of the anterior ethmoid air
cells to create a wide communication from the
frontal sinus to the nasal cavity through a medial
periorbital incision.
49
Disappointing results with
this procedure were soon realized because of re-
stenosis of the nasofrontal duct, either by scarring
or by herniation of the orbital tissues into the
created communication with the nasal cavity.
5052
Several modifications of this approachusing stents
of silicone and mucoperiosteal flap were devised
in an attempt to maintain this artificial conduit
patent. These met with various degrees of success.
The osteoplastic flap procedure, as reported by Ber-
gara and Itoiz in 1955, hinged the anterior frontal
sinus wall on an inferior pedicle of pericranium.
53
This procedure allowed easy visualization of the
damaged sinus, replacement of the bone on com-
pletion of the surgery, and improved forehead cos-
mesis. Goodale and Montgomery carried this pro-
cedure one step further, as they recognized the
importance of nasofrontal duct injury and often re-
moved the sinus contents and obliterated the sinus
with autologous fat.
5153
The osteoplastic flap oper-
ation has been subsequently modified for use in
trauma of the frontal sinus by elevating the pericra-
nium with the scalp flap and exploring the frontal
sinus by removal of the free bone fragments. Con-
sistently excellent results withminimal complication
rates and a less than 1 percent incidence of infec-
tious complications after mucosal exenteration and
fat graft obliteration of sinuses with injured naso-
frontal ducts have been reported.
15,32,33,43,54,55
A vari-
ety of materials such as bone, muscle, fascia, and
hydroxyapatite have been successfully used to oblit-
erate the sinus cavity.
29,5659
Cranialization of the
frontal sinus was specifically developed to address
severe frontal sinus fractures whenthe posterior wall
is damaged.
3,30
Volume 120, Number 7 Suppl. 2 Frontal Sinus Fractures
39S
Classification of Frontal Sinus Procedures and
Their Indications
Observation
The variables that determine which patients
canbe safely observed, rather thantreatedby open
surgery, are as follows: degree of injury, ability/will
to follow-up, availability of expertise in functional
endoscopic sinus surgery, and evolution of mini-
mally invasive techniques. Minimally displaced
frontal sinus anterior table fractures can be clearly
observed. Minimally displaced fractures in the re-
gion of the frontonasal duct would traditionally
require exploration and management. If there is
expertise available to endoscopically open the na-
sofrontal duct at a later time and the patient is
willing and reliable in terms of follow-up, it may be
reasonable to observe these patients. These pa-
tients will have to be followed on a frequent basis
with serial radiographic investigations. Symptoms
or findings suggestive of obstruction and/or de-
velopment of a complication such as a mucocele
would be indications for intervention at a later
date. The frequency and length of radiographic
and clinical follow-up required in these instances
has not been defined. Other factors to consider
are the need for operative intervention of associ-
ated injuries. The following general indications
should be considered for frontal sinus surgery in
the face of frontal sinus fractures:
1. To avoid immediate and short-term compli-
cations such as cerebrospinal fluid leak,
meningitis, and spreading infection.
2. To avoid long-term complications such as
frontal bone osteomyelitis, chronic frontal
sinusitis, mucocele, mucopyocele, and brain
abscess.
3. To provide adequate exposure for anatomi-
cal reduction of naso-orbito-ethmoid frac-
tures.
4. To restore proper aesthetic contour of the
forehead.
Applying these indications to the classification
system of frontal sinus injury presented in Figure
2 leads to a simplified management algorithm.
There are four basic choices for managing the
frontal sinus when it is injured: observation, ex-
ploration and fracture reduction without obliter-
ation/cranialization, obliteration, and cranializa-
tion. Variations in these approaches are related to
the methods of soft-tissue access, the type of ma-
terial used for obliteration, the requirement for
bone grafting, whether dural repairs are required,
and variations of surgical technique.
Soft-Tissue Access
There are three ways to access the frontal si-
nus. In limited outer table frontal sinus injuries
without involvement of the nasofrontal duct
and/or the medial orbital rim, in the absence of
other associated regional craniofacial injuries, the
fractures can be reduced and fixed through the
laceration. In this instance, the sinus mucosa is left
intact. Very rarely, in a hypopneumatized frontal
sinus with outer table fractures, one can adequately
remove the mucosa throughanextensive laceration.
As a general rule, this should be avoided if possible.
Endoscopic repair of frontal sinus fractures has
been performed satisfactorily with the use of bone
substitutes to recreate the frontal contour.
60,61
The
approachis similar tothat of anendoscopic browlift.
However, the indication for this minimally invasive
approach is limited at the present time to nondis-
placed outer table fractures that do not involve the
medial orbital rim and/or frontonasal duct. This
wouldbe a subset of type 1 fractures according tothe
classificationscheme providedhere. Inaddition, the
use of bone substitute in the face of acute injury is
associated with the risk of secondary infection and
should be monitored closely. However, as tech-
niques of endoscopy improve and as the instrumen-
tation for endoscopic surgery becomes increasingly
sophisticated, more involved frontal sinus fractures
will surely become amenable to treatment with min-
imally invasive approaches.
The accepted method for soft-tissue access to
the frontal, nasofrontal, and orbital craniofacial
skeletal structures is the bicoronal incision. Though
a large incision, the panoramic access it provides is
unparalleledandthe placement inthe hairline com-
pletely conceals the incision. Cosmetic problems
may arise in the following situations: visibility of in-
cision in subjects with alopecia; injury to the frontal
branches of the facial nerve, which will give both a
cosmetic and functional problem; and devascular-
ization of the temporal fat pad, with subsequent
hollowing of the temporal fossa. Specific sharp dis-
section under the superficial temporal fascia later-
ally and under the pericranium medially/centrally
will avoid injury to the facial nerve and maximize
exposure. In the region of the temporal fat pad, a
combination of blunt and sharp dissection to the
zygomatic arch is performed, with the goal of min-
imizing injury to the blood supply of the fat pad. If
access to the lateral orbit is required, the bicoronal
incisionshouldbe extendedtothe preauricular area
to the junction of the tragus and helix of the auricle;
this allows better downward displacement of the bi-
coronal flap(Fig. 8). However, it must be notedthat,
for isolated access to the zygomatic arch/temporal
Plastic and Reconstructive Surgery December Supplement 2, 2007
40S
region, a full bicoronal incision is not required, and
this can be achieved through a limited hemicoronal
access without extension to the nonhair-bearing
skin inferiorly. Meticulous technique with hemosta-
sis andthe avoidance of clips at the edges of the flaps
will prevent hair loss around the incision.
18
It is also
important to make the incision of the scalp parallel
to the hair follicles. Avoiding the transection of hair
follicles further avoids alopecia at the edges of the
wound.
62,63
At the orbital rim, the superior orbital
nerve foramina are outfractured to further facilitate
exposure at the nasion and orbits.
Exploration and Fracture Reduction Alone
without Obliteration or Cranialization
Type 1 and some type 2 fractures can be man-
aged with a simple exploration and fracture re-
duction without the requirement for frontal sinus
obliteration. A contraindication for exploration
alone is a type 2 fracture that involves the naso-
ethmoid complex and/or the medial superior or-
bital rim or orbital floor. These associated injuries
will invariably involve the nasofrontal duct, neces-
sitating an obliteration procedure.
With obliteration of the frontal sinus, the an-
terior bone fragments are removed and debrided
of mucosal elements and the sinus is irrigated with
saline. If there is no evidence of posterior wall
injury and nasofrontal duct involvement, reduc-
tion in anatomical position with low-profile mi-
croplates completes the procedure. If there is ev-
idence of injury to the nasofrontal ducts, the
procedure is converted to an obliteration.
Frontal Sinus Obliteration
Most type 2 fractures that are associated with
naso-orbito-ethmoid and superior orbital rimfrac-
tures and all type 3 fractures require a frontal sinus
obliteration. A bicoronal incision access is re-
quired in almost all of these frontal sinus fractures
(Fig. 9).
Sinus exploration: Frontal bone fragments are re-
moved and debrided of mucosal elements with
a high-speed drill and continuous suction irri-
gation.
Mucosal exenteration: All mucosal elements of the
frontal sinus must be removed diligently. Atten-
tion should be given to the recesses of the frontal
sinus. Removal of a layer of bone throughout the
sinus will ensure that no mucosal elements are
left behind. A high-speed drill with a coarse dia-
mond burr is essential for removal of mucosa,
both from the anterior table bone fragments and
from the posterior wall. At the edges of the fron-
tal sinus, this becomes technically challenging
because of the narrow angle formed where the
outer table meets the inner table. It is helpful to
use a variety of drill bits with ever-decreasing sizes
as this part of the sinus is approached. The direc-
tion of drilling in these recesses should be paral-
lel to the posterior wall to avoid injury to the
dura. Suction irrigation is essential for this part of
the procedure also. The irrigation should be
used in a steady flow over where the drill is
passed; in this way, the thin film of water flowing
over the bone does two important things: it
avoids thermal injury to the bone and, most im-
portantly, provides the surgeon with a degree of
transparency of the bone. As the bony dissection
proceeds in this way, the color of the bone
Fig. 9. Type 2, simple anterior table displaced fracture.
Volume 120, Number 7 Suppl. 2 Frontal Sinus Fractures
41S
changes as the dura is approached. This is done
under the operating microscope or with magni-
fying loupes. In well-pneumatized sinuses, the
bone exposure may need to be increased with the
use of additional osteotomies through the ante-
rior frontal table. Rarely, a very-well-pneumatized
frontal sinus that extends to the sphenoid wing
will require removal of the posterior sinus wall to
access the farther recesses by gentle retraction on
the frontal lobes. This maneuver converts the
obliteration into a cranialization.
Nasofrontal duct obliteration: This is necessary for
isolation of the frontal sinus from the sinonasal
tract to prevent contamination and to avoid
regrowth of mucosa from the ethmoids into the
frontal sinus. Muscle, fascia, or bone chips can
be used to obliterate the nasofrontal ducts bi-
laterally (Fig. 10).
Frontal sinus obliteration: The frontal sinus can be
left alone for osteogenesis to occur or obliter-
ated with fat, hydroxyapatite, fascia, or bone
chips.
56,6467
No significant advantage of one
technique over another has been demon-
strated. In contaminated fractures, consider-
ation should be given to the use of biomateri-
als. For example, use of bone substitutes with
incomplete removal of mucosa will result in the
formation of mucoceles, infection of the mate-
rial used, and dissolution of the underlying
dura.
5,6870
This can lead to intracranial compli-
cations and the loss of tissue of the forehead.
Therefore, it is best to avoid nonautogenous
materials in the setting of acute injury to avoid
serious complications. If there is evidence of
extensive comminution of the posterior wall,
bone fragments must be removed and the dura
explored for injury. Dural injuries should be
primarily repaired in this instance and the si-
nus obliterated with fat (Fig. 11). The areas of
the nasofrontal ducts (i.e., the floor of the
frontal sinus) should be addressed next. The
management principle of this area is the cre-
ation of scar tissue to the exclusion of mucosal
elements in such a fashion that mucosal migra-
tion into the obliterated sinus will be pre-
vented. This is done by opening the frontona-
sal ducts with punch forceps and creating a
zone of injury in the superior ethmoid air cells.
Care should be taken to avoid injury to the
cribriform plate and fovea ethmoidalis. Be-
cause the fovea and cribriform are very fragile,
the technique of bone removal in the adjacent
region should be achieved with a sharp tool or
a high-speed drill; avoiding a rocking motion
and/or a levering against these structures is
critical. The ducts are then tightly packed with
muscle or fascia that will provide the nidus for
scar formation in this area.
Fracture reduction: Frontal sinus fractures are re-
duced according to standard techniques using
microplates. If the comminution is extensive,
titanium mesh can be used.
8
This technique is
particularly useful with the concurrent reduc-
tion of orbital rim fractures. The fragments can
be reduced in situ or removed and reduced to
plates or mesh outside the fracture confines
and subsequently positioned to the fracture.
Nasoethmoid and orbital fractures must be ad-
dressed at this point by fixation onto stable
bone in the frontal region. With the dissection
Fig. 10. Superior view of the frontonasal ducts from within the
frontal sinus. The superior ethmoid cells have been removed
from above to create a zone of injury for scar formation and to
prevent mucosal ingrowth. Thenext stepinthis sequencewill be
to plug the ducts with fascia/muscle and/or bone chips. Arrows
point to the enlarged region of the frontonasal ducts.
Fig. 11. Dural injury repair with a patch of cadaveric dura and
nonabsorbable sutures. The arrow points to the dural repair.
Plastic and Reconstructive Surgery December Supplement 2, 2007
42S
proceeding inferiorly, care should be taken to
avoid injury to the lacrimal sac. The perios-
teum is densely adherent to the nasal bones
and especially the suture lines. It is important
to elevate the soft tissues, including the perios-
teum, using a sharp elevator.
Frontal Sinus Cranialization
This procedure was developed specifically for
extensive injuries of the frontal sinus that involve
cerebrospinal fluid leak on exploration and/or
soft-tissue and bone loss such as those seen in type
4 and 5 injuries. The procedure is identical to that
of a frontal sinus obliteration, with the exception
of complete removal of the posterior sinus wall. It
is important in a cranialization procedure to ad-
dress the recesses of the sinus before removing the
posterior wall extensively. This is accomplished
with a high-speed diamond drill under continu-
ous-suction irrigation in a pattern similar to that of
obliteration. However, the depth of bone removal
of the posterior wall is much more extensive. It
helps to remove as much bone as possible with the
high-speed drill under continuous suction irriga-
tion so as to eggshell the posterior table. The
dura is thendissectedfromthe overlying bone first
in the areas where the posterior table has been
fractured. Subsequently, bone fragments are re-
moved with further drilling and/or a rongeur.
Care should be taken at the level of the sagittal
sinus where the bone invaginates on either side of
the sinus. Inferiorly, the crista galli should be
drilled carefully with a diamond burr, taking care
to avoidentering the cribriformplate. Inextensive
fractures that involve the cribriform plate and/or
the fovea ethmoidalis, fragments of thin bone
along with the ethmoid mucosa need to be de-
brided meticulously. The region of the nasofron-
tal ducts needs to be managed as in a frontal sinus
obliteration. With a cranialization, the correct
management of this region is even more critical.
Failure to do so will result in mucosal ingrowth
directly over dura, potentially exposing the nasal
cavity to the splanchnocranium.
These principles apply equally to cranializa-
tion of the sinus after a bifrontal craniotomy. The
residual elements of mucosa, especially those at-
tached to the posterior table, must be removed
along with the bone.
A pericranial flap can be used to manage ex-
tensive injuries of the floor and/or the posterior
wall of the frontal sinus. It is frequently a good
option for a cerebrospinal fluid leak identified
during surgery.
13,7173
This versatile axial pattern
fascial flap is an excellent choice when there is a
need to isolate the anterior cranial fossa from the
nasal cavity and/or associated paranasal sinuses.
The robust blood supply to this flap, when based
anteriorly, is fromthe supratrochlear and supraor-
bital arteries. The layers included are those of the
pericranium and the galea. It can be extended to
include a portion of the pericranium and galea
distal to the bicoronal incision. In this condition,
care is taken when designing the bicoronal inci-
sion to preserve the galea at the vertex.
Dural repair under these circumstances is
achieved with primary closure, a fascial patch, or
an artificial dural patch (Fig. 6). A pericranial
vascularized flap that can provide blood supply to
free calvarial grafts used to reconstruct the fron-
tobasal skeleton should not substitute for primary
dural closure. Approximately one in five patients
with frontal injuries will require a cranialization.
18
The majority of these patients with extensive pos-
terior wall fractures will also have a cerebrospinal
fluid leak at exploration.
A frontal sinus cranialization is significantly
easier when a bicoronal bone flap has been per-
formed for the management of intracranial injury.
In this situation, the drilling of the posterior wall
can take place ex vivo on the back table, using a
high-speed drill. However, in this instance, again
the nasofrontal ducts need to be managed in a
fashion that will prevent mucosal ingrowth into
the splanchnocranium.
Frequently, frontal sinus procedures are com-
bined with the repair of additional craniofacial
injuries, the most common being orbital and mid-
face fractures.
18,62
In the presence of bone loss and
in the presence of secondary complications (mu-
coceles with orbital problems), reconstruction
with bone grafts will be required. It is preferable
to use split-thickness calvarial bone grafts because
they are readily accessible through the bicoronal
incision (Figs. 12 and 13).
Indications to use split-thickness calvarial
bone grafts are as follows
63
:
1. Extensive loss of support at the skull base
over the fovea ethmoidalis and cribriform
plate, in combination with a pericranial flap.
2. In superior orbital roof fractures, avoidance of
pulsatile exophthalmos and orbital deformity.
3. Extensive bone loss of the anterior table that
cannot be replaced with elements of the
posterior table.
4. In combination with naso-orbito-ethmoid
and orbital reconstruction as layered bone
grafts to obliterate the ethmoids and recon-
struct the medial orbital wall.
Volume 120, Number 7 Suppl. 2 Frontal Sinus Fractures
43S
Management of Associated Neurosurgical
Issues
Several issues of importance arise as to the
timing of surgical management of neurologic in-
jury in relation to the management of frontal sinus
injury. Life-threatening injuries and injuries with
the potential for neurologic impairment take pre-
cedence over the management of frontal sinus.
Evacuation of an intracranial hematoma, whether
it is intraparenchymal, subdural, and/or epidural,
is performed without delay; the frontal and/or
craniofacial injuries may be addressed at a later
stage unless they contribute to the neurologic
morbidity. It is best in this situation for the patient
to declare the course of neurologic progress after
neurosurgical intervention before correction of
these problems. In the presence of closed head
injury, the estimation of intracranial pressure and
its impact on neurologic function dictates the tim-
ing of surgical repair of frontal injuries. An ex-
ception to this may be a frontobasilar injury in the
presence of markedly raised intracranial pressure
that presents withherniationof brainparenchyma
into the nasal cavity. In this situation, the splanch-
nocranium must be isolated from the upper aero-
digestive tract through surgical intervention that
will most likely concurrently manage the frontal
sinus.
Severe frontobasilar injuries involving tissue
loss, typically seen in industrial accidents, will re-
quire correction of dural defects and soft-tissue
coverage along with management of the frontal
sinus to avoid mucocele formation and ongoing
contamination of the cranial cavity by the sinus
contents. Bone reconstruction of calvarial defects
can be managed at a second stage when the pa-
tient is stable neurologically (Fig. 7).
If surgical intervention is required emergently
for the evacuation of an epidural or subdural he-
matoma, the frontal sinus could be managed con-
currently with the neurologic injury, depending
on how stable the patient is and whether further
general anesthesia can be tolerated. The easiest
method for frontal sinus management in the sit-
uation where a bifrontal craniotomy flap has been
raised is to cranialize the sinus and obliterate the
frontonasal ducts. The presence of radiographic
evidence of closed head injury such as multiple
small intraparenchymal hematomas may require a
period of observation and serial neurologic exam-
inations before surgical intervention for the facial
skeletal injuries.
CONTROVERSIAL ISSUE:
ENDOSCOPIC MANAGEMENT
In recent years, great strides have been made
in the endoscopic management of frontal sinus
infectious disease.
69,70
Advances in instrumenta-
tion, including power tools capable of removing
the thin bone of the sinuses and endoscopic drills
for the removal of more compact bone, have en-
abled sufficient surgical access of the frontal sinus
to deal with most forms of frontal sinusitis.
24,70
Furthermore, the use of intraoperative navigation
systems has enabled these approaches with an un-
precedented degree of safety.
70,7476
Recently, en-
doscopic obliteration of the frontal sinus with fat
has become possible for infectious disease of the
frontal sinus.
77
Nevertheless, the management of fractures of
the frontal sinus with endoscopic techniques has
been limited to contouring of the frontal bone in
the simplest of fractures.
60
It is possible that in the
near future the endoscopic repair of a small sub-
type of these fractures may be possible. This sub-
Fig. 12. Layered calvarial grafts both superiorly and medially in
the orbit after resection of a mucocele.
Fig. 13. Extensive skull fractures associated with both frontal
and orbital injuries. The sinus was cranialized both for manage-
ment and for access for an epidural hematoma evacuation.
Plastic and Reconstructive Surgery December Supplement 2, 2007
44S
type of patients will have to have a limited, isolated
injury of the frontal sinus outflow without exten-
sive frontal bone fractures and other maxillofacial
fractures. In this instance, the goal is to restore the
frontal sinus outflow, an indication for which en-
doscopic techniques are ideally suited. Further-
more, in such an instance, patient follow-up is
essential to avoid early and late complications. It
is also possible to combine the two endoscopic
approaches for restoration of frontal sinus physi-
ologic outflow and contouring of type 1 nondis-
placed fractures.
COMPLICATIONS OF FRONTAL
SINUS FRACTURES
Early Complications
A complication is characterized as early if it
occurs within the first few weeks of surgical inter-
vention. A number of transient problems can oc-
cur after bicoronal access and frontal sinus frac-
ture surgery. Forehead pain, transient anesthesia
of the forehead, and transient diplopia should all
resolve within 2 to 3 weeks.
3,58,78,79
The most fre-
quent significant early complication is a cerebro-
spinal fluid leak. Depending on the severity of the
injuries in the population of patients studied, in
some series this is as high as 10 percent.
3,40
Cere-
brospinal fluid leaks are problematic in the face of
intracranial injury. The standard management
with a lumbar drain will be contraindicated in the
face of intracranial injuries and/or suspected in-
crease in intracranial pressure. Therefore, care
must be taken before such a decision is made. The
administration of antibiotics for the cerebrospinal
fluid leak per se is a controversial subject.
8082
An-
tibiotics should be administered prophylactically
for the lumbar drain and if there are independent
reasons for their administration. The majority of
immediate postoperative cerebrospinal fluid leaks
will disappear spontaneously. Reexploration should
be considered if a leak persists or it there is a con-
traindication to conservative management with a
lumbar drain.
The incidence of meningitis can be as high as
6 percent postoperatively.
3
Fatal episodes of men-
ingitis after cranialization procedures has been
reported.
1
Meningitis is not necessarily associated
with an active cerebrospinal fluid leak. As these
patients may be neurologically compromisedfrom
a head injury, they are uniquely susceptible to the
consequences of meningitis. In this situation, the
early signs of meningitis such as altered mental
status will not become apparent before signs of an
infection such as high fever or hypotension. To
minimize the morbidity and potential mortality
from meningitis, this condition needs to be diag-
nosed without delay. Change in mental status, fe-
ver, or neck rigidity should prompt an immediate
lumbar puncture after a brain computed tomo-
graphic scan without any delay. Use of broad-spec-
trum antibiotics with good cerebrospinal fluid
penetration is an essential first step with culture-
directed antibiotics following the results of cere-
brospinal fluid cultures. The antibiotics should be
readjusted appropriately to cerebrospinal fluid
cultures. Operative intervention should be post-
poned in the face of active meningitis.
Late Complications
Late complications are unusual but insidious
and can have significant consequences. A mu-
cocele and/or a mucopyocele can develop as
early as a few months or as late as several years
after the initial operation.
83
Mucoceles cause
bone erosion and are capable of involving the
sinuses, the orbit, and the splanchnocranium
(Fig. 14). Because they are slow growing and
produce few symptoms, they are usually discov-
ered late. Reoperation with complete removal of
the mucocele and reconstruction to isolate the
splanchnocranium from the orbit and nasal
cavity is the method of choice for management
of mucoceles.
8486
Endoscopic marsupialization
Fig. 14. Orbital mucocele as a complication fromprevious fron-
tal sinus injury.
Volume 120, Number 7 Suppl. 2 Frontal Sinus Fractures
45S
of mucoceles has been attempted after infec-
tious complication of frontal sinusitis, with lim-
ited success rates and frequent follow-up require-
ments
87,88
(Fig. 7).
Brain abscesses are rare but potentially fatal
complications of frontal sinus disease. Spread of
low-grade infectionfromthe frontal sinus through
the foramina of Breschet by thrombophlebitis
brings the infection intracranially.
3,28
Brain ab-
scesses develop by spread of infection along the
periarteriolar spaces of Virchow, along the arterial
supply of the brain parenchyma.
89
The symptoms
associated with a frontal brain abscess are insidi-
ous: loss of appetite, fatigue, lethargy, and subtle
changes in personality rather than a fulminant
infection. Appropriate neurosurgical intervention
without delay is essential in preventing the mor-
bidity and potential mortality, which is high even
in the modern antibiotic era.
Frontal bone osteomyelitis is a very rare com-
plication. In the preantibiotic era, this was com-
monly known as Potts puffy tumor. Today, this
complication is encountered when the frontal si-
nus has been surgically manipulated on multiple
occasions, especially when synthetic material has
been used that became infected. This condition
requires complete removal of the frontal bone,
treatment with antibiotics, and subsequent recon-
struction at a later stage.
In the past, frontal contour defects were fairly
common late complications. This was primarily
because of the lack of rigid fixation and subse-
quent frontal bone loss. However, with the advent
of miniplate and microplate fixation and the use
of primary bone grafts, this is seen far less fre-
quently. Issues arising from late complications
with contouring can be resolved at a later stage
with cranial remodeling using mesh and bone sub-
stitutes or alloplastic materials. However, the cli-
nician must be absolutely sure that all issues with
the frontal sinus are quiescent. It is in this setting
that endoscopic repair of contour defects using
bone substitutes is effective.
It is important to recognize that all patients
who have had complications associated with fron-
tal sinus management should be followed long
term both clinically and with serial imaging in the
early postoperative years. If the frontal sinus was
obliterated with fat, magnetic resonance imaging
is an excellent modality for follow-up.
SUMMARY
Frontal sinus surgery has evolved through the
need to address infectious disease of the frontal
sinus and its complications. The current manage-
ment of frontal sinus fractures is based on ana-
tomical and physiologic principles of mucosal
function and frontal sinus drainage. Classification
schemes based on the severity of frontal sinus in-
jury dictate the type of operative management
required.
Three general types of operations for frontal
sinus fractures have evolved: exploration and frac-
ture reduction alone, frontal sinus obliteration,
and frontal sinus cranialization. Evolution of sur-
gical techniques has given these interventions a
substantial degree of safety, with minimal compli-
cations attributed to the operations themselves.
Because of the profile of patients with frontal
sinus fractures (i.e., they are unlikely to comply
with follow-up), it is prudent to maintain an ag-
gressive approach toward frontal sinus oblitera-
tioninthe majority of instances. Inmore extensive
injuries, a frontal sinus cranialization is indicated
if there is presence of a cerebrospinal fluid leak,
tissue, and/or bone loss and extensive associated
naso-orbito-ethmoid fractures.
Spiros Manolidis, M.D.
Department of Otolaryngology
Head and Neck Surgery
Columbia University
180 Fort Washington, HP813
New York, N.Y. 10032
sm2397@columbia.edu
REFERENCES
1. Gerbino, G., Roccia, F., Benech, A., and Caldarelli, C. Anal-
ysis of 158 frontal sinus fractures: Current surgical manage-
ment and complications. J. Craniomaxillofac. Surg. 28: 133,
2000.
2. Raveh, J., Laedrach, K., Vuillemin, T., and Zingg, M. Man-
agement of combined frontonaso-orbital/skull base frac-
tures and telecanthus in 355 cases. Arch. Otolaryngol. Head
Neck Surg. 118: 605, 1992.
3. Wallis, A., and Donald, P. J. Frontal sinus fractures: A review
of 72 cases. Laryngoscope 98: 593, 1988.
4. Duvall A. J., III, Porto, D. P., Lyons, D., and Boies, L. R., Jr.
Frontal sinus fractures: Analysis of treatment results. Arch.
Otolaryngol. Head Neck Surg. 113: 933, 1987.
5. Larrabee, W. F., Jr Travis L. W., and Tabb, H. G. Frontal sinus
fracturestheir suppurative complications and surgical man-
agement. Laryngoscope 90: 1810, 1980.
6. Wilson, B. C., Davidson, B., Corey, J. P., and Haydon, R. C.,
III. Comparisonof complications following frontal sinus frac-
tures managed with exploration with or without obliteration
over 10 years. Laryngoscope 98: 516, 1988.
7. Rohrich, R. J., and Hollier, L. H. Management of frontal
sinus fractures: Changing concepts. Clin. Plast. Surg. 19: 219,
1992.
8. Lakhani, R. S., Shibuya, T. Y., Mathog, R. H., Marks, S. C.,
Burgio, D. L., and Yoo, G. H. Titanium mesh repair of the
severely comminuted frontal sinus fracture. Arch. Otolaryngol.
Head Neck Surg. 127: 665, 2001.
9. Nahum, A. M. The biomechanics of maxillofacial trauma.
Clin. Plast. Surg. 2: 59, 1975.
Plastic and Reconstructive Surgery December Supplement 2, 2007
46S
10. Nahum, A. M. The biomechanics of facial bone fracture.
Laryngoscope 85: 140, 1975.
11. Karesh, J. W., Kelman, S. E., Chirico, P. A., and Mirvis, S. E.
Orbital roof blow-in fractures. Ophthal. Plast. Reconstr. Surg.
7: 77, 1991.
12. Antonyshyn, O., Gruss, J. S., and Kassel, E. E. Blow-in frac-
tures of the orbit. Plast. Reconstr. Surg. 84: 10, 1989.
13. Klotch, D. W. Frontal sinus fractures: Anterior skull base.
Facial Plast. Surg. 16: 127, 2000.
14. Heller, E. M., Jacobs, J. B., and Holliday, R. A. Evaluation of
the frontonasal duct in frontal sinus fractures. Head Neck 11:
46, 1989.
15. Stanley, R. B., Jr. Fractures of the frontal sinus. Clin. Plast.
Surg. 16: 115, 1989.
16. Kurzer, A., and Patel, M. P. Superior orbital fissure syndrome
associated with fractures of the zygoma and orbit. Plast. Re-
constr. Surg. 64: 715, 1979.
17. Ludwick, J. J., Taber, K. H., Manolidis, S., Sarna, A., and
Hayman, L. A. A computed tomographic guide to endo-
scopic sinus surgery: Axial andcoronal views. J. Comput. Assist.
Tomogr. 26: 317, 2002.
18. Manolidis, S. Frontal sinus injuries: Associated injuries and
surgical management of 93 patients. J. Oral Maxillofac. Surg.
62: 882, 2004.
19. Shapiro, R., and Schorr, S. A consideration of the systemic
factors that influence frontal sinus pneumatization. Invest.
Radiol. 15: 191, 1980.
20. McLaughlin, R. B., Rehl, R. M., Jr., and Lanza, D. C. Clinically
relevant frontal sinus anatomy and physiology. Otolaryngol.
Clin. North Am. 34: 1, 2001.
21. Lee, D., Brody, R., and Har-El, G. Frontal sinus outflow
anatomy. Am. J. Rhinol. 11: 283, 1997.
22. Harris, L., Marano, G. D., and McCorkle, D. Nasofrontal
duct: CT in frontal sinus trauma. Radiology 165: 195, 1987.
23. Turgut, S., Ercan, I., Sayin, I., and Basak, M. The relationship
between frontal sinusitis and localization of the frontal sinus
outflow tract: A computer-assisted anatomical and clinical
study. Arch. Otolaryngol. Head Neck Surg. 131: 518, 2005.
24. Kennedy, D. W., and Senior, B. A. Endoscopic sinus surgery:
A review. Otolaryngol. Clin. North Am. 30: 313, 1997.
25. Landsberg, R., and Friedman, M. A computer-assisted ana-
tomical study of the nasofrontal region. Laryngoscope 111:
2125, 2001.
26. Kuhn, F. A., Javer, A. R., Nagpal, K., and Citardi, M. J. The
frontal sinus rescue procedure: Early experience and three-
year follow-up. Am. J. Rhinol. 14: 211, 2000.
27. Mosher, H. P. A method of obliterating the naso-frontal duct
and catheterizing the frontal sinus. Laryngoscope 21: 946,
1911.
28. Donald, P. J., and Ettin, M. The safety of frontal sinus fat
obliteration when sinus walls are missing. Laryngoscope 96:
190, 1986.
29. Donald, P. J. Obliteration of compressed frontal sinus. Plast.
Reconstr. Surg. 78: 832, 1986.
30. Donald, P. J. Frontal sinus ablation by cranialization: Report
of 21 cases. Arch. Otolaryngol. 108: 142, 1982.
31. Donald, P. J., Montgomery, W. W., and Calcaterra, T. Frontal
bone defect with frontal sinus mucopyocele. Head Neck Surg.
10: 59, 1987.
32. Stanley, R. B., Jr., and Becker, T. S. Injuries of the nasofrontal
orifices in frontal sinus fractures. Laryngoscope 97: 728, 1987.
33. Stanley, R. B., Jr. Management of frontal sinus fractures.
Facial Plast. Surg. 5: 231, 1988.
34. Kelly, K. J., Manson, P. N., Vander Kolk, Kolk C. A., et al.
Sequencing LeFort fracture treatment (Organization of
treatment for a panfacial fracture). J. Craniofac. Surg. 1: 168,
1990.
35. Manson, P. N., Markowitz, B., Mirvis, S., Dunham, M., and
Yaremchuk, M. Toward CT-based facial fracture treatment.
Plast. Reconstr. Surg. 85: 202, 1990.
36. Markowitz, B. L., and Manson, P. N. Panfacial fractures:
Organization of treatment. Clin. Plast. Surg. 16: 105, 1989.
37. Ioannides, C., and Freihofer, H. P. Fractures of the frontal
sinus: Classification and its implications for surgical treat-
ment. Am. J. Otolaryngol. 20: 273, 1999.
38. Luce, E. A. Frontal sinus fractures: Guidelines to manage-
ment. Plast. Reconstr. Surg. 80: 500, 1987.
39. Messinger, A., Radkowski, M. A., Greenwald, M. J., and
Pensler, J. M. Orbital roof fractures in the pediatric popu-
lation. Plast. Reconstr. Surg. 84: 213, 1989.
40. Donald, P. J., and Bernstein, L. Compound frontal sinus
injuries with intracranial penetration. Laryngoscope 88: 225,
1978.
41. Donald, P. J. Frontobasal approach for trauma and tumor.
Minim. Invasive Neurosurg. 37: 37, 1994.
42. Key, J. M., Tami, T., and Donald, P. J. Gunshot wound to the
frontal sinus. Head Neck 12: 357, 1990.
43. Stanley, R. B., Jr. Management of severe frontobasilar skull
fractures. Otolaryngol. Clin. North Am. 24: 139, 1991.
44. Nandapalan, V., Watson, I. D., and Swift, A. C. Beta-2-trans-
ferrin and cerebrospinal fluid rhinorrhoea. Clin. Otolaryngol.
21: 259, 1996.
45. Lund, V. J., Savy, L., Lloyd, G., and Howard, D. Optimum
imaging and diagnosis of cerebrospinal fluid rhinorrhoea.
J. Laryngol. Otol. 114: 988, 2000.
46. Jacobs, J. B. 100 years of frontal sinus surgery. Laryngoscope
107: 1, 1997.
47. Logan-Turner. The operative treatment of chronic suppu-
ration of the frontal sinus. J.A.M.A. 44: 446, 1905.
48. Skillern, R. H. Untoward results following the external op-
eration on the frontal sinus: A critical review of twenty cases.
Laryngoscope 23: 1063, 1913.
49. Lynch, R. C. The technique of a radical frontal sinus oper-
ation which has given me the best results. Laryngoscope 31: 1,
1921.
50. Goodale, R. L. Some causes for failure in frontal sinus sur-
gery. Ann. Otol. Rhinol. Laryngol. 51: 1942.
51. Goodale, R. L., and Montgomery, W. W. Experiences with
osteoplastic anterior wall approach to frontal sinus. A.M.A.
Arch. Otolaryngol. 68: 271, 1958.
52. Goodale, R. L. Obliteration of the frontal sinus. Ann. Otol.
Rhinol. Laryngol. 74: 831, 1965.
53. Bergara, A. R., and Itoiz, A. O. Present state of the surgical
treatment of chronic frontal sinusitis. Arch. Otolaryngol. 61:
616, 1955.
54. Keerl, R., Weber, R., Kahle, G., Draf, W., Constantinidis, J.,
and Saha, A. Magnetic resonance imaging after frontal sinus
surgery with fat obliteration. J. Laryngol. Otol. 109: 1115, 1995.
55. Constantinidis, J., Weber, R., Brune, M., Draf, W., and Iro, H.
Cranialization of the frontal sinus: Indications, technique
and results (in German). H.N.O. 48: 361, 2000.
56. Weber, R., Draf, W., Kahle, G., and Kind, M. Obliteration of
the frontal sinus: State of the art and reflections on new
materials. Rhinology 37: 1, 1999.
57. Snyderman, C. H., Scioscia, K., Carrau, R. L., and Weissman,
J. L. Hydroxyapatite: An alternative method of frontal sinus
obliteration. Otolaryngol. Clin. North Am. 34: 179, 2001.
58. Shumrick, K. A., and Smith, C. P. The use of cancellous
bone for frontal sinus obliteration and reconstruction of
frontal bony defects. Arch. Otolaryngol. Head Neck Surg. 120:
1003, 1994.
Volume 120, Number 7 Suppl. 2 Frontal Sinus Fractures
47S
59. Petruzzelli, G. J., and Stankiewicz, J. A. Frontal sinus oblit-
eration with hydroxyapatite cement. Laryngoscope 112: 32,
2002.
60. Strong, E. B., Buchalter, G. M., and Moulthrop, T. H. En-
doscopic repair of isolated anterior table frontal sinus frac-
tures. Arch. Facial Plast. Surg. 5: 514, 2003.
61. Rice, D. H. Management of frontal sinus fractures. Curr.
Opin. Otolaryngol. Head Neck Surg. 12: 46, 2004.
62. Manolidis, S., Weeks, B. H., Kirby, M., Scarlett, M., and
Hollier, L. Classification and surgical management of or-
bital fractures: Experience with 111 orbital reconstruc-
tions. J. Craniofac. Surg. 13: 726, 2002.
63. Manolidis, S. Indications for bone grafting in orbital recon-
struction. Presented at the 2nd World Congress of Otorhi-
nolaryngologic Allergy Endoscopy and Laser Surgery, Ath-
ens, Greece: Monduzzi Editore, 2001.
64. Ross, D. A., Marentette, L. J., Thompson, B. G., and Haller,
J. S. Use of hydroxyapatite bone cement to prevent cerebro-
spinal fluid leakage through the frontal sinus: Technical
report. Neurosurgery 45: 401, 1999.
65. Weber, R., Draf, W., Keerl, R., et al. Magnetic resonance
imaging following fat obliteration of the frontal sinus. Neu-
roradiology 44: 52, 2002.
66. Peltola, M. J., Aitasalo, K. M., Suonpaa, J. T., Yli-Urpo, A.,
Laippala, P. J., and Forsback, A. P. Frontal sinus and skull
bone defect obliteration with three synthetic bioactive ma-
terials: A comparative study. J. Biomed. Mater. Res. B Appl.
Biomater. 66: 364, 2003.
67. Friedman, C. D., Costantino, P. D., Jones, K., Chow, L. C.,
Pelzer, H. J., Sisson, G. A., Sr. Hydroxyapatite cement: II.
Obliterationand reconstructionof the cat frontal sinus. Arch.
Otolaryngol. Head Neck Surg. 117: 385, 1991.
68. Xie, C., Mehendale, N., Barrett, D., Bui, C. J., and Metzinger,
S. E. 30-year retrospective review of frontal sinus fractures:
The Charity Hospital experience. J. Craniomaxillofac. Trauma
6: 7, 2000.
69. Weber, R., Draf, W., Keerl, W., et al. Osteoplastic frontal sinus
surgery with fat obliteration: Technique and long-term re-
sults using magnetic resonance imaging in 82 operations.
Laryngoscope 110: 1037, 2000.
70. Weber, R., Draf, W., Kratzsch, B., Hosemann, W., and
Schaefer, S. D. Modern concepts of frontal sinus surgery.
Laryngoscope 111: 137, 2001.
71. Ducic, Y., and Stone, T. L. Frontal sinus obliteration using a
laterally based pedicled pericranial flap. Laryngoscope 109:
541, 1999.
72. Snyderman, C. H., Janecka, I. P., Sekhar, L. N., Sen, C. N.,
and Eibling, D. E. Anterior cranial base reconstruction: Role
of galeal and pericranial flaps. Laryngoscope 100: 607, 1990.
73. Thaller, S. R., and Donald, P. The use of pericranial flaps in
frontal sinus fractures. Ann. Plast. Surg. 32: 284, 1994.
74. Chandra, R. K., Kennedy, D. W., and Palmer, J. N. Endo-
scopic management of failed frontal sinus obliteration. Am.
J. Rhinol. 18: 279, 2004.
75. Sindwani, R., and Metson, R. Impact of image guidance on
complications during osteoplastic frontal sinus surgery. Oto-
laryngol. Head Neck Surg. 131: 150, 2004.
76. Sindwani, R., and Metson, R. Image-guided frontal sinus
surgery. Otolaryngol. Clin. North Am. 38: 461, 2005.
77. Ung, F., Sindwani, R., and Metson, R. Endoscopic frontal
sinus obliteration: A new technique for the treatment of
chronic frontal sinusitis. Otolaryngol. Head Neck Surg. 133: 551,
2005.
78. Mendians, A. E., and Marks, S. C. Outcome of frontal sinus
obliteration. Laryngoscope 109: 1495, 1999.
79. Correa, A. J., Duncavage, J. A., Fortune, D. S., and Reinisch,
L. Osteoplastic flap for obliteration of the frontal sinus: Five
years experience. Otolaryngol. Head Neck Surg. 121: 731, 1999.
80. Kaufman, B. A., Tunkel, A. R., Pryor, J. C., and Dacey, R. G.,
Jr. Meningitis in the neurosurgical patient. Infect. Dis. Clin.
North Am. 4: 677, 1990.
81. Mollman, H. D., and Haines, S. J. Risk factors for postoper-
ative neurosurgical wound infection: A case-control study.
J. Neurosurg. 64: 902, 1986.
82. Levin, S., Nelson, K. E., Spies, H. W., and Lepper, M. H.
Pneumococcal meningitis: The problem of the unseen ce-
rebrospinal fluid leak. Am. J. Med. Sci. 264: 319, 1972.
83. Weitzel, E. K., Hollier, L. H., Calzada, G., and Manolidis, S.
Single stage management of complex fronto-orbital muco-
celes. J. Craniofac. Surg. 13: 739, 2002.
84. Yanagisawa, E., Joe, J. K., and Smith, H. W. Mucocele of the
frontal sinus: An external approach with frontonasal passage
reconstruction. Ear Nose Throat J. 79: 912, 2000.
85. LaRossa, D. D., Noone, R. B., and Jackson, P. Facial deformity
fromfrontal sinus mucocele: Single stage surgical correction.
Case report. Plast. Reconstr. Surg. 60: 917, 1977.
86. Abrahamson, I. A., Jr., Baluyot, S. T., Tew, J. M., Jr., and
Scioville, G. Frontal sinus mucocele. Ann. Ophthalmol. 11:
173, 1979.
87. Har-El, G. Endoscopic management of 108 sinus mucoceles.
Laryngoscope 111: 2131, 2001.
88. Har-El, G. Transnasal endoscopic management of frontal
mucoceles. Otolaryngol. Clin. North Am. 34: 243, 2001.
89. Falcone, S., and Post, M. J. Encephalitis, cerebritis, and brain
abscess: Pathophysiology and imaging findings. Neuroimaging
Clin. N. Am. 10: 333, 2000.
Plastic and Reconstructive Surgery December Supplement 2, 2007
48S
You might also like
- Nitration of Benzoic Acid To Produce Methyl 3-Nitrobenzoate: PH C CH O (O) Phcooh HNO H SO Cooh CH OH H SO CoochDocument2 pagesNitration of Benzoic Acid To Produce Methyl 3-Nitrobenzoate: PH C CH O (O) Phcooh HNO H SO Cooh CH OH H SO CoochAleem AhmedNo ratings yet
- 2014-06-03 Construction Meeting Minutes PDFDocument3 pages2014-06-03 Construction Meeting Minutes PDFIthacaVoiceNo ratings yet
- Management of Frontal Sinus Fractures: SummaryDocument17 pagesManagement of Frontal Sinus Fractures: SummaryOdalis CuaspudNo ratings yet
- Articulo PDFDocument9 pagesArticulo PDFNayeli Díaz InzunzaNo ratings yet
- Frontal Sinus Fracture 2019Document7 pagesFrontal Sinus Fracture 2019Mohammed FaroukNo ratings yet
- Lu2017 Nasal FracturesDocument10 pagesLu2017 Nasal FracturesInne CarolineNo ratings yet
- Evaluation and Reduction of Nasal TraumaDocument15 pagesEvaluation and Reduction of Nasal TraumaAnnisa Priscasari DwiyantiNo ratings yet
- Nasal Trauma and The Deviated Nose: SummaryDocument12 pagesNasal Trauma and The Deviated Nose: SummaryAlexandru BadeaNo ratings yet
- Fracture Nasal BonesDocument16 pagesFracture Nasal BonesGẽrman DiãzNo ratings yet
- Maxillofacial (Midface) FracturesDocument16 pagesMaxillofacial (Midface) FracturesYeraldin EspañaNo ratings yet
- Maxillofacial TraumaDocument56 pagesMaxillofacial TraumaErnesto Fer FdezNo ratings yet
- Femur FractureDocument16 pagesFemur FractureM Pino HakimNo ratings yet
- Management of The Traumatized AirwayDocument8 pagesManagement of The Traumatized AirwayAnonymous h0DxuJTNo ratings yet
- Complications of Frontal Sinus Fractures: Stephen E. Metzinger, M.D., F.A.C.S., and Rebecca C. Metzinger, M.DDocument8 pagesComplications of Frontal Sinus Fractures: Stephen E. Metzinger, M.D., F.A.C.S., and Rebecca C. Metzinger, M.DYohana SepthiyaNo ratings yet
- Management of Nasal TraumaDocument20 pagesManagement of Nasal TraumaSamir JaberNo ratings yet
- Tugas Bedah 2Document19 pagesTugas Bedah 2fransiscaNo ratings yet
- Fracture Nasal Bones PDFDocument16 pagesFracture Nasal Bones PDFFeri TrihandokoNo ratings yet
- Skull Base Trauma: Diagnosis and Management: Madjid Samii and Marcos TatagibaDocument10 pagesSkull Base Trauma: Diagnosis and Management: Madjid Samii and Marcos TatagibaYovanka Naryai ManuhutuNo ratings yet
- Contemporary Management Pediatric Craniofacial InjuriesDocument8 pagesContemporary Management Pediatric Craniofacial InjuriesTabishur RahmanNo ratings yet
- Frontal Sinus FracturesDocument9 pagesFrontal Sinus Fracturesshehla khanNo ratings yet
- Pi Is 1043181020300233Document8 pagesPi Is 1043181020300233Connie PérezNo ratings yet
- Nasal and Facial Fractures: DR - Imran Qazi Ent A Tmo KTH PeshawarDocument42 pagesNasal and Facial Fractures: DR - Imran Qazi Ent A Tmo KTH Peshawarimran qaziNo ratings yet
- Orbital Roof Fractures A Clinically Based Classification and Treatment AlgorithmDocument7 pagesOrbital Roof Fractures A Clinically Based Classification and Treatment AlgorithmEl KaranNo ratings yet
- Mandibulasr Truma ManagementDocument18 pagesMandibulasr Truma Managementjoal510No ratings yet
- FX Frontal.Document29 pagesFX Frontal.LupitaNo ratings yet
- Penetrating Neck Injuries: S. Moeng, K. BoffardDocument7 pagesPenetrating Neck Injuries: S. Moeng, K. BoffardFarah Basotjatjo KaharNo ratings yet
- Assesment of The Patien With TraumaticDocument15 pagesAssesment of The Patien With Traumaticvalecharapova11No ratings yet
- Traumatized AirwayDocument8 pagesTraumatized AirwayUWIMANA Jean ClaudeNo ratings yet
- Management of Pediatric Mandible Fractures PDFDocument16 pagesManagement of Pediatric Mandible Fractures PDFarfahNo ratings yet
- Anaesthesia For Maxillofacial Trauma: Learning ObjectivesDocument7 pagesAnaesthesia For Maxillofacial Trauma: Learning ObjectivesMatthew MarionNo ratings yet
- Depressed Fracture NSMC - AbstractDocument14 pagesDepressed Fracture NSMC - AbstractGlen Sandy SaapangNo ratings yet
- Mandibular Condylar and Subcondylar Fractures PDFDocument16 pagesMandibular Condylar and Subcondylar Fractures PDFWayan Sutresna YasaNo ratings yet
- Maxillofacial TraumaDocument15 pagesMaxillofacial TraumadewiswahyuNo ratings yet
- Panfacial TraumaDocument104 pagesPanfacial TraumaMehek BatraNo ratings yet
- Management of Facial Bone Fractures With Frontonasal Open Head Injury: Case ReportDocument5 pagesManagement of Facial Bone Fractures With Frontonasal Open Head Injury: Case ReportCarlos Iván Cota ZavalaNo ratings yet
- Advancesinthe Reconstructionoforbital Fractures: Scott E. Bevans,, Kris S. MoeDocument23 pagesAdvancesinthe Reconstructionoforbital Fractures: Scott E. Bevans,, Kris S. Moestoia_sebiNo ratings yet
- Frontal Bone Fracture-A Case ReportDocument3 pagesFrontal Bone Fracture-A Case ReportcxsaefaNo ratings yet
- Maxillary Fractures: ©1997 Erlanger Health System Tennessee Craniofacial Center 1 (800) 418-3223Document4 pagesMaxillary Fractures: ©1997 Erlanger Health System Tennessee Craniofacial Center 1 (800) 418-3223Aristiyan LuthfiNo ratings yet
- An Algorithm For The Initial Management of Nasal Trauma: John F. Hoffmann, MD, FACSDocument11 pagesAn Algorithm For The Initial Management of Nasal Trauma: John F. Hoffmann, MD, FACSDaniel Celestino DiazNo ratings yet
- Christison Lagay2016Document31 pagesChristison Lagay2016Luis Ticona ZegarraNo ratings yet
- Nasal Fracture: Case ReportDocument8 pagesNasal Fracture: Case ReportMas KaryonNo ratings yet
- Frontal Bone and Frontal Sinus Injuries: David A. Shaye, E. Bradley StrongDocument18 pagesFrontal Bone and Frontal Sinus Injuries: David A. Shaye, E. Bradley Strongjfcule1No ratings yet
- 1 7 Frontal Bone and Frontal Sinus Injuries 2020 Facial Trauma SurgeryDocument18 pages1 7 Frontal Bone and Frontal Sinus Injuries 2020 Facial Trauma SurgeryCarolina PalacioNo ratings yet
- Panfacial FracturesDocument35 pagesPanfacial FracturesMARISOL GALLEGO DUQUENo ratings yet
- Maxillofacial Trauma: Child DevelopmentDocument8 pagesMaxillofacial Trauma: Child DevelopmentAchmadArifinNo ratings yet
- Root FracturesDocument9 pagesRoot FracturesAbhilashPadmanabhanNo ratings yet
- Care of The Patient With Fracture Neck of Femur For Non-Emergency SurgeryDocument7 pagesCare of The Patient With Fracture Neck of Femur For Non-Emergency SurgeryChärlayne Joyce GuzmänNo ratings yet
- Humerus FractureDocument5 pagesHumerus FracturecyahiminNo ratings yet
- Mandibular Fractures: Diagnosis and Management: Kanvar Panesar, DDS, MD, MS Srinivas M. Susarla, DMD, MD, MPHDocument12 pagesMandibular Fractures: Diagnosis and Management: Kanvar Panesar, DDS, MD, MS Srinivas M. Susarla, DMD, MD, MPHNovia NadhillaNo ratings yet
- A Review of Root Fractures - Final PrintDocument9 pagesA Review of Root Fractures - Final Printemchen11No ratings yet
- 000000Document27 pages000000drahmadelrawdyNo ratings yet
- BackgroundDocument5 pagesBackgroundMaricar K. BrionesNo ratings yet
- Cranial Vault & Skull Base - Diagnosis - Skull Base, Temporal Bone (Lateral Skull Base) - AO Surgery ReferenceDocument1 pageCranial Vault & Skull Base - Diagnosis - Skull Base, Temporal Bone (Lateral Skull Base) - AO Surgery ReferenceSophiaNo ratings yet
- Cleft Bone Grafting Part 1Document1 pageCleft Bone Grafting Part 1ivyNo ratings yet
- Article in Press: Acute and Chronic Humeral Shaft Fractures in AdultsDocument9 pagesArticle in Press: Acute and Chronic Humeral Shaft Fractures in AdultsGabriel GolesteanuNo ratings yet
- Mandibular FracturesDocument171 pagesMandibular FracturesBalen ShalawNo ratings yet
- Medind - Nic.in Iad t08 s1 Iadt08s1p688Document11 pagesMedind - Nic.in Iad t08 s1 Iadt08s1p688Anonymous S0H8cqgnfiNo ratings yet
- Complications of OtoplastyDocument10 pagesComplications of OtoplastyLaineyNo ratings yet
- Basic Imaging Skul TraumaDocument7 pagesBasic Imaging Skul TraumaPutra PakayaNo ratings yet
- Acute and Chronic Humeral Shaft Fractures in Adults: SciencedirectDocument9 pagesAcute and Chronic Humeral Shaft Fractures in Adults: SciencedirectAshish AgrawalNo ratings yet
- Acetabular Fractures in Older Patients: Assessment and ManagementFrom EverandAcetabular Fractures in Older Patients: Assessment and ManagementTheodore T. MansonNo ratings yet
- EzRay Air WDocument3 pagesEzRay Air WAlexandru BadeaNo ratings yet
- Brochure Advantixvario 2 Int NetDocument12 pagesBrochure Advantixvario 2 Int NetAlexandru BadeaNo ratings yet
- Megagen Kit PDFDocument88 pagesMegagen Kit PDFAlexandru BadeaNo ratings yet
- Nasal Trauma and The Deviated Nose: SummaryDocument12 pagesNasal Trauma and The Deviated Nose: SummaryAlexandru BadeaNo ratings yet
- Membership ApplicationfinalDocument1 pageMembership ApplicationfinalAlexandru BadeaNo ratings yet
- 4-Point Action Plan by Esperanza and Brian CabralDocument6 pages4-Point Action Plan by Esperanza and Brian CabralRapplerNo ratings yet
- Hematology AnalyzerDocument29 pagesHematology AnalyzerMac Kevin MandapNo ratings yet
- Wednesday, July 15, 2015 EditionDocument14 pagesWednesday, July 15, 2015 EditionFrontPageAfricaNo ratings yet
- Assignment Cover Page: Sociology (BBA1263) Fifth SemesterDocument11 pagesAssignment Cover Page: Sociology (BBA1263) Fifth SemesterSupriya BajracharyaNo ratings yet
- Reina Bridge2Document7 pagesReina Bridge2Phil StiltonNo ratings yet
- Rescission of Insurance ContractsDocument12 pagesRescission of Insurance ContractsCari Mangalindan MacaalayNo ratings yet
- Final Exam (Power Plant)Document4 pagesFinal Exam (Power Plant)IsabelNo ratings yet
- Understand Behaviours Better 001 The Barnum Forer EffectDocument1 pageUnderstand Behaviours Better 001 The Barnum Forer EffectJithesh AnandNo ratings yet
- Alhena Eng Rev06Document7 pagesAlhena Eng Rev06Steven BrownNo ratings yet
- Basic Services Allowed As Others Stay Closed: Gulf TimesDocument24 pagesBasic Services Allowed As Others Stay Closed: Gulf TimesmurphygtNo ratings yet
- Eou Unit 7Document20 pagesEou Unit 7Thành NhânNo ratings yet
- Population Genetics TutorialDocument164 pagesPopulation Genetics TutorialMichelle GNo ratings yet
- Spelling RulesDocument15 pagesSpelling RulesTâm Thanh CaoNo ratings yet
- Unit 77: Plan & Co-Ordinate Vehicle MaintenanceDocument12 pagesUnit 77: Plan & Co-Ordinate Vehicle MaintenanceNurul AduraNo ratings yet
- Thyroidinum From Various SourcesDocument4 pagesThyroidinum From Various SourcesSuriya OsmanNo ratings yet
- USFS Mission - Tanzania - May 2009 - Water Resources in Tabora and Rukwa - For FRAMEDocument57 pagesUSFS Mission - Tanzania - May 2009 - Water Resources in Tabora and Rukwa - For FRAMERahul K Awade0% (1)
- Olierook - Mechanisms For Permeability Modification in The Damage Zone of A Normal FaultDocument19 pagesOlierook - Mechanisms For Permeability Modification in The Damage Zone of A Normal FaultUgik GeoNo ratings yet
- Cat 16m Grader BrochureDocument24 pagesCat 16m Grader BrochureSauro GordiniNo ratings yet
- Rotonivo: Series RN 3000 / 6000Document34 pagesRotonivo: Series RN 3000 / 6000Strato VariusNo ratings yet
- Hansen 2008Document30 pagesHansen 2008Jacobo CeballosNo ratings yet
- BIO 201 Chapter 11 LectureDocument34 pagesBIO 201 Chapter 11 LectureDrPearcyNo ratings yet
- Building Maintenance ChecklistDocument5 pagesBuilding Maintenance ChecklistcajaroNo ratings yet
- Ex Situ Mineral CarbonationDocument30 pagesEx Situ Mineral CarbonationBea EspeñoNo ratings yet
- RR SMR E3s Case Chapter 5 - Reactor Coolant System and Associated Systems Issue 1 Gda PublicationDocument89 pagesRR SMR E3s Case Chapter 5 - Reactor Coolant System and Associated Systems Issue 1 Gda PublicationMuhammad ImranNo ratings yet
- Marine Concrete Specs-HkDocument5 pagesMarine Concrete Specs-HkMohammed Faisal TNo ratings yet
- Unit Test - 4 Class-Xii Sub.-Chemistry Time:01:30 Hrs Mm:40Document2 pagesUnit Test - 4 Class-Xii Sub.-Chemistry Time:01:30 Hrs Mm:40Nihar Ranjan NikuNo ratings yet
- Process of HospitalizationDocument24 pagesProcess of HospitalizationFara Zaman100% (3)
- 11g Active Data Guard More Than Just DR .: Gavin Soorma Senior Oracle DBA, BankwestDocument30 pages11g Active Data Guard More Than Just DR .: Gavin Soorma Senior Oracle DBA, BankwestAbhinay IrukullaNo ratings yet