Professional Documents
Culture Documents
Latent TB Infection Provider Guide
Latent TB Infection Provider Guide
Uploaded by
Rivani KurniawanOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Latent TB Infection Provider Guide
Latent TB Infection Provider Guide
Uploaded by
Rivani KurniawanCopyright:
Available Formats
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 1
Latent Tuberculosis Infection:
A Guide for Massachusetts Providers
Prepared November 2000, Revised April 2009
Medical Advisory Committee for the Elimination of Tuberculosis (MACET)
Latent Tuberculosis Infection (LTBI) Targeted
Testing and Treatment:
Commonly Asked Questions and Answers1
I.
1.
2.
3.
4.
5.
Testing for Latent TB Infection
What is latent tuberculosis infection (LTBI)?
Page
What is the best test for LTBI, and how should test results be recorded?
Who should be tested for LTBI in Massachusetts?
Who is at high risk of TB in Massachusetts today?
Should persons who have been vaccinated with BCG (bacille Calmette-Guerin)
be tested for LTBI, and if tested, how should the results be interpreted?
6. Which persons, if they develop active TB, pose an especially high risk to the community?
7. What tuberculin skin test (TST) induration size is considered indicative of TB infection?
8. Who should be retested for LTBI in Massachusetts?
9. Can repeat skin testing for TB cause a positive reaction?
10. What is 2-step PPD testing, and when is it indicated?
2
2
3
3
4
4
5
6
6
6
II. Treatment of Latent TB Infection
11. Who should be treated for LTBI?
12. What are the currently recommended treatments for LTBI?
13. How do I decide which treatment to choose for my patient?
14. What are the appropriate dosages for the 4 LTBI treatment options,
and how should they be prescribed?
15. How should I monitor for safety and adherence during treatment?
16. How much treatment of LTBI can be missed before the patient must start over?
17. If a patient will not or cannot take treatment for LTBI, what is appropriate follow-up?
18. When should I seek consultation with a specialist?
10
10
12
12
12
III. Public Health Aspects
19. Is latent TB infection reportable to the health department?
20. What public health resources are available to me and to my patients?
13
13
Appendix 1: Tuberculosis Risk Questionnaire
Appendix 2: Treatment of Latent Tuberculosis (LTBI) Reference Card
Appendix 3: Evaluation of Program Performances
14
15
16
7
7
9
These recommendations are based on guidelines published jointly by the Centers for Disease Control (CDC) and the American
Thoracic Society (ATS): Am J Resp Crit Care Med 2000;161:S221-43; MMWR June 9, 2000 Vol 49, No RR-6: 1-51, MMWR
Aug 31, 2001 Vol 50, No 34, 733-735, and MMWR August 8, 2003 Vol 52; 735-739. Copies of TB-related statements
published in MMWR are available through the Division of Tuberculosis Prevention and Control, MDPH (617-983-6970)
and through the CDC site on the World Wide Web (www.cdc.gov/nchstp/tb/).
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 2
I. Testing for Latent TB Infection
Question 1. What is latent tuberculosis infection (LTBI)?
The term Latent Tuberculosis Infection (LTBI) defines an asymptomatic state in persons who are
infected with Mycobacterium tuberculosis and have no clinical or radiographic evidence of
active disease. The organism resides within the host in a clinically inactive, or latent, state,
contained by the host immune response. Latent TB infection currently is detected by a
standardized, intradermal skin test, termed the tuberculin skin test (TST), -- or by a blood test
(QuantiFERON-Gold or -Gold-In-Tube, or T-Spot.TB), persons with risk factors for
exposure to TB. For persons with untreated latent TB infection and intact immunity, the
estimated risk of developing tuberculosis disease is 5% to 10% over a lifetime, with about 50
80% of that risk occurring during the first 2 years following infection. For persons who are
immunocompromised by HIV co-infection, the risk of developing disease increases to 5% to
10% per year.
Active TB disease rarely is discovered in asymptomatic persons by tuberculin skin testing.
However, finding LTBI provides an opportunity to treat and prevent reactivation of the latent
infection that leads to active disease. Studies have shown that treatment of LTBI can prevent
reactivation TB with an efficacy of 60%-90%. Because of the relatively low TB prevalence in
the United States, and with reactivation tuberculosis representing a large proportion of new
cases, treatment of LTBI is considered an important public health strategy to achieve national
TB elimination. Latent TB infection generally is not treated in high-prevalence countries,
because detection and complete treatment of active disease is the top personal and public health
priority. One exception is children who are contacts of known active cases; they are usually
tested and treated even in high-prevalence countries.
Question 2. What is the best test for LTBI, and how should test results be recorded?
Tuberculin skin testing with intermediate strength (5 TU Tuberculin Units) purified protein
derivative (PPD), administered by the Mantoux intradermal technique (not by multiple puncture
devices, such as Tine or Mono-Vacc), is the current standard test for detecting LTBI. The TST
is administered by injecting 0.1 ml (5 TU) PPD solution intradermally (not subcutaneously),
usually into the ventral surface of the forearm. Forty-eight to 72 hours after the test is
administered, the diameter of palpable or visible induration (raised swelling) is measured
transverse to the long axis of the arm (i.e. across the arm) and recorded in mm. 2 Note: redness
without induration should be ignored. Reading of the TST should be performed by a person who
is adequately trained in its interpretation; patients, or parents of patients, should NEVER be
permitted to read their own skin tests.
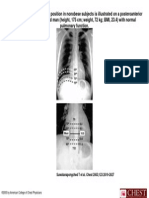
Three reading methods have been recommended. With one method, the arm is positioned so that a light shines tangentially over
the skin reaction, highlighting any induration. The lateral edges of the visible induration are marked with a pen and measured
with a millimeter (mm) ruler. With the second method, the lateral edges of the induration are determined by moving a ballpoint
pen across the arm from each side until resistance is met. A mark is made and the diameter is measured with a mm ruler. The
third method involves direct palpation of the induration, marking the edges and measuring the distance across the forearm. With
any of these methods, only the measurement transverse to the long axis of the arm (not two dimensions) is recorded.
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 3
Caution: The Massachusetts Department of Public Health and others have received multiple
reports of false-positive reactions using Aplisol (Squibb), one of the 2 brands of tuberculin skin
testing reagent currently licensed in the US. Therefore, Tubersol (Connaught) is the only
agent recommended by MACET for tuberculin skin testing in Massachusetts.
Interferon-gamma Release Assays (IGRA's): QuantiFERON-Gold, QuantiFERON-Gold-In
Tube, and T-Spot TB are new tests approved by the FDA for detection of latent TB infection,
in certain circumstances. The QuantiFERON laboratory tests use an ELISA to measure the
production of interferon-gamma by whole blood leukocytes incubated with protein antigens
specific to M tuberculosis complex and a few other nontuberculous mycobacteria -- but NOT by
bacilli Calmette-Guerin (BCG). The T-Spot also uses MTb-specific antiges, but it employs an
elispot format to quantify the number of T cells that are secreting interferon-gamma. These tests
require a single patient visit for a blood draw, and results are reported as a positive or negative
laboratory value. Special processing of the blood cells and plasma by trained laboratory
personnel is necessary. Following its published indications, these tests are an acceptable
substitute for the TST in Massachusetts. Guidelines for the use of the earlier generations of the
QuantiFERON tests were published by the Centers for Disease Control (CDC) in 2003 and 2005;
these currently (as of January, 2009) are in-revision to accommodate the newer generation
QuantiFERON-Gold-In Tube test and T-Spot TB. MACET has published an interim set of
guidelines for the use of the IGRA's (ref:
http://www.mass.gov/Eeohhs2/docs/dph/cdc/tb/alerts_igra_guidelines_diagnose_infection.pdf)
Question 3: Who should be tested for LTBI in Massachusetts?
Testing for LTBI should be reserved for persons who meet some or all of the following criteria:
Are at high risk of TB infection (see Question 4).
and
If infected, are at high risk of developing active TB.
or
If they developed active TB, would place vulnerable contacts at risk.
Question 4: Who is at high risk of TB in Massachusetts today?
High-risk persons in Massachusetts who should be tuberculin skin tested include:
Close contacts of known active pulmonary TB cases, or persons working or residing in
congregate settings (shelters, jails, and some health care facilities) considered high-risk
for TB.
Non US-born persons from high-prevalence countries who have been in the US 5 years
or less, or persons with extended (> 1 month) travel to these countries within the past 5
years. 3
High prevalence places from which Massachusetts TB cases have come in recent years include, but are not limited to, China,
Southeast Asia, India, Haiti, Dominican Republic, Central America, Brazil, Russia, and sub-Saharan Africa. TB case rates have
almost tripled in the former Soviet Union in the decade following its dissolution, and an increasing number of arrivals are
expected. http://www.mass.gov/dph/cdc/tb/
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 4
Persons with fibrotic abnormalities on chest x-ray 4 consistent with previous TB.
Persons with clinical conditions associated with progression to active TB, such as HIV
infection, silicosis, diabetes, chronic renal failure/hemodialysis, gastrectomy, jejunoileal
bypass, solid organ transplantation (renal, cardiac), carcinoma of the head and neck, and
being more than 15% underweight.
Injection drug users.
Children who meet these criteria or who have been in regular contact with high-risk
adults with LTBI also are considered at risk (see footnote 7). This is not to suggest that
persons with LTBI are themselves infectious, but they may indicate other, active,
infectious persons in the environment.
Immunocompromised persons (e.g. HIV, chronic corticosteroid use, administration of
TNF- inhibitors or receptor blockers) with risk(s) for TB exposure.
Note: In the ATS/CDC Guidelines referenced on p. I-1, Tables 2 and 3 indicate risk estimates
for these and other factors. Note: We have developed a questionnaire that can be used in
clinical settings to help determine a childs risk of tuberculosis and the need for a tuberculin
skin test (Appendix 1).
Question 5: Should persons who have been vaccinated with BCG be tested for LTBI, and if
tested, how should the results be interpreted?
BCG is administered to more than 80% of children in the world as part of the Extended Program
on Immunization. The vaccine is given primarily in countries with rates of LTBI much higher
than those found in the US or Western Europe, and many persons who have previously received
BCG also may have LTBI. Reactions to the TST following BCG vaccination may range from no
induration to >10 mm, although many are in the 5-9 mm range. These reactions generally wane
with time, though their size can be affected by the age at vaccination, the number of
vaccinations, and the number and frequency of subsequent tuberculin skin tests since
vaccination. Persons who have received BCG should be tested for LTBI as clinically indicated;
positive test results in persons who have had contact with a case of TB or who come from a
country with a high rate of TB should be assumed to be due to TB infection, not BCG, and
treatment should be recommended, unless contraindicated. A rule of thumb states that TST
reactions of 15 mm or greater are likely to be TB, as are reactions of 10 mm or greater in persons
immunized more than 15 years ago. Some persons who had been vaccinated with BCG and do
not believe the results of a positive TST signals TB infection may be tested with an IGRA which,
by nature of the antigens used for the tests, have greater specificity for MTb infection (see
Question 2).
Question 6: Which persons, if they develop active TB, pose an especially high risk to the
community?
Persons with active TB who may threaten the publics health include anyone with infectious TB
(usually pulmonary and/or laryngeal TB) who is working or living in a congregate setting with
4
Prior tuberculosis disease can have a variety of nonspecific appearances. However, radiographically dense, upper lobe linear or
nodular changes are characteristic. Hilar, lower lobe, and pleural densities are also seen, but are less specific for TB. For
example, in the Ohio River Valley, hilar calcifications are more likely to represent previous histoplasmosis than TB. Apical
pleural thickening without parenchymal scarring is specifically not associated with TB.
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 5
vulnerable persons, such as HIV/AIDS or otherwise-immunocompromised patients, the elderly,
homeless persons, newborn babies, and children 4 years of age and under.
Question 7: What tuberculin skin test (TST) induration diameter is considered indicative
of TB infection?
Three cut-off points define ranges of reaction size for a positive TST: 5 mm, 10 mm, or 15 mm,
depending on the risk of TB infection or disease in the individual or population being tested, as
detailed below.
5 mm or greater TST induration: is considered positive only in persons at highest risk
for infection or active disease. In this group, detecting all TB infections is considered
more important than the risk of including some false positive reactions. Four high-risk
subgroups are included:
- Close contacts of active pulmonary or laryngeal cases.
- HIV-immunocompromised persons (the risk of progression to active TB, if TB infected,
is 5% to 10% per year).
- Organ transplant recipients or other immunosuppressed persons (including persons
receiving long-term, high dose oral or parenteral corticosteroid therapy (arbitrarily
defined as 15 mg prednisone, or equivalent, daily for 1 month or longer). Note: Inhaled
corticosteroid use is not associated with sufficient suppression of the immune system to
reduce the TST response.
- Persons with fibrotic chest x-ray findings consistent with old TB.
10 mm or greater TST induration: Such tests are considered positive for persons
known to be at high risk for infection or disease. Included in this group are
- Non US-born persons from high-prevalence countries who have been in the US five
years or less (see footnote 3).
- Disadvantaged low-income persons (malnutrition, crowded housing, medically
underserved).
- Persons over age 70 and children 4 years of age and under.
- Persons residing or having resided for extended periods in congregate settings known to
be associated with TB transmission, such as shelters, jails, prisons, and detoxification or
drug-rehabilitation centers.
- Injection drug users.
- Health care workers and other workers in facilities serving populations at increased
risk of unsuspected TB disease, or engaged in high-risk procedures such as
bronchoscopy, sputum induction, autopsies, mycobacteriology laboratory work, or work
in homeless shelters. 5
- Other high-risk professions, such as mortuary work. 6
15 mm or greater TST induration:
- Persons at low risk of TB infection, for whom TST is generally not indicated, are more
likely to have false-positive reactions if a 10 mm cut-off is used, due to non-specific
hypersensitivity to environmental mycobacteria. It has been estimated that as many as 3
5
Health care facilities and other Massachusetts workplaces covered under the Occupational Services Health Administration
(OSHA) regulations should follow current OSHA directives regarding TST testing, interpretation, and treatment.
6
Out-of-date local or state regulations have required food-handlers, hairdressers and other workers not at increased risk to be
tested for TB. Ideally, testing should be avoided, but if required, the 15 mm cut-off should be used unless other risk factors
apply. The Massachusetts law mandating pre-employment tuberculin skin testing for all school personnel was repealed in 2003.
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 6
out of 4 TST indurations of 10 mm to 14 mm in low-risk persons are not due to TB. By
increasing the cut-off size to 15 mm in low-risk persons, sensitivity decreases but
specificity increases. School children in Massachusetts, unless they have specific risk
factors for TB, should no longer be routinely tested for TB. 7
Question 8. Who should be retested for LTBI in Massachusetts?
Only those with a negative skin test and ongoing risk of exposure to TB should be retested. In a
low-prevalence state like Massachusetts, relatively few people are included in this category.
Close contacts of known, infectious TB cases, persons likely to be exposed by travel in highprevalence regions of the world, and persons who work at jobs associated with exposure (some
health care workers, shelter workers, correction officers, etc.) should have repeat testing, at a
frequency determined by the estimated risk, or by regulations, such as those issued by
institutions or by the Occupational Safety and Health Administration (OSHA).
Question 9. Can repeat skin testing for TB cause a positive reaction?
No. The administration of a tuberculin skin test cannot, by itself, cause reactivity to future
tuberculin skin testing in persons who have not been infected with TB. However, repeated skin
testing can cause the false impression of recent infection (TST conversion) in persons who had
actually been infected in the remote past.
In the absence of subsequent stimulation , TST reactivity wanes over a period of many years
following TB infection. This fading of immune memory for the antigens in PPD may give a
falsely-negative result following the administration of a single TST years after the initial
infection. However, the hosts immune memory for PPD can be boosted by the first TST after
many years, so that the subsequent TST reaction size may be significantly larger than on the
initial test, even if no further exposure to TB has occurred. The repeat TST in such cases thus
may appear to have converted from negative to positive. However, the boosted reaction does not
reflect recent infection; rather, it represents stimulated immune memory for past infection. In
persons who are to undergo serial tuberculin skin testing (as may be required in some
circumstances, such as for high-risk employees of certain health care facilities; see Question 10,
below), using a 2-step baseline skin test procedure and using a change in induration of 10 mm as
criteria for conversion, are recommended steps to minimize boosting and the incorrect diagnoses
of skin test conversions. See Screening for Tuberculosis and Tuberculosis Infection in High-Risk
Populations. Recommendations of the Advisory Council for the Elimination of Tuberculosis
(MMWR 44:18-34, September 8, 1995;
http://www.cdc.gov/mmwr/preview/mmwrhtml/00038873.htm) for further discussion.
Question 10. What is 2-step tuberculin skin testing, and when is it indicated?
Tuberculosis testing of school children should be based on individual risk factors (see Question 4), not the location of their
school or residence. MACET has developed a questionnaire (see Appendix 1) to assist pediatricians determine which children
should be tested. Copies are available through the Massachusetts Department of Public Health, Division of Tuberculosis
Prevention and Control (617-983-6970).
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 7
False TST conversions due to boosting of waning hypersensitivity to the antigens contained in
PPD (see Question 9) can be reduced by administering a 2-step baseline skin test in those
increasingly uncommon circumstances when repeated TB skin testing is indicated by the high
risk of ongoing infection (e.g., some health care workers). This applies only to person who have
not received a TST in the recent past (i.e. this may be defined arbitrarily within a period of years
long enough for immunity to wane 5 to 10 years, for example). It is generally not required for
young people, arbitrarily those under age 20, for example.
Procedure:
1.
Administer the first TST, as usual.
2.
If the first TST is positive (according to the risk-based criteria answer to question 9), the
subject is considered TB-infected, and further skin testing is not warranted.
3.
If the first TST is negative, a second TST is done (one week to one month later) and, again,
it is read at 48-72 hours. This second reading may be larger than the first (a 10 mm change is
considered significant), due to boosting. If positive, the subject is considered TB-infected and
evaluated for LTBI treatment. If still negative, this second test becomes the baseline
measurement (i.e. mm induration) against which future skin test results are compared.
4.
On subsequent testing, an increase in reaction size of 10 mm or more from the baseline
reaction is considered a true conversion (i.e. indicating infection has occurred since the previous
TST), and should warrant evaluation for active disease. If active disease is not found, treatment
of LTBI should be considered.
II. Treatment of Latent TB Infection
Question 11: Who should be treated for latent TB infection?
Anyone at high risk for progression to TB who has a positive tuberculin skin test for TB
infection is a candidate for treatment, if they also fulfill the following criteria:
No symptoms, signs, or radiographic evidence of active TB. 8
Willing to complete a full course of therapy (treatment of LTBI is not mandatory, even if
strongly recommended).
Available to be clinically monitored by a health care provider during the full course of
treatment.
No medical contraindications to treatment, such as severe liver disease, drug
hypersensitivity, or medical conditions that make adherence unlikely, such as mental illness
or alcoholism.
Where available, supervised treatment or directly observed treatment ( DOT) can increase
adherence for high-risk persons.
Question 12: What are the currently recommended treatments for LTBI?
8
In the absence of symptoms suggesting pulmonary or extrapulmonary TB, only the history, physical examination, and chest xray should be part of a clinical work-up for LTBI. Other tests, such as sputum or urine culture, have an extremely small yield,
and are subject to false-positive results if done routinely. The erythrocyte sedimentation rate (ESR) is neither sensitive nor
specific for active TB.
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 8
In the past, only isoniazid (INH) was recommended for treatment of LTBI, but now there are 3
treatment options, 1 of which is rifampin-based and does not include INH:
Option 1. INH daily (self-administered or by DOT), or twice-weekly (by DOT), for 9 months
Considered the optimal treatment in terms of efficacy.
May be limited by its long duration (may discourage initial acceptance and long-term
adherence) and its potential for hepatotoxicity, especially for persons over age 35 years. 9
Recommended for children 10 and adults, with or without HIV co-infection, and with or
without fibrotic chest x-ray abnormalities suggesting old TB.
Option 2. INH daily (self-administered or by DOT), or twice-weekly (by DOT) for 6 months
Considered sub-optimal compared to the 9-month INH treatment because it is less
effective.
Advantages over the 9-month INH treatment: Greater initial acceptance and long-term
adherence may be more likely, and marginally less hepatotoxicity than the 9-month
regimen. Potential for hepatotoxicity increased for those over age 35 years (see footnote
9).
Recommended for adults without HIV co-infection and without chest x-ray abnormalities
suggesting old TB.
Option 3. Rifampin alone for 4 months.
Efficacy considered comparable to the 6-month INH treatment, but few studies have
examined the efficacy of rifampin as a single agent for the treatment of LTBI (refs: Hong
Kong Chest Service, Tuberculosis Research Centre, Madras, and British Medical
Research Council. 1992. A double-blind placebo controlled clinical trial of three
antituberculosis chemoprophylaxis regimens in patients with silicosis in Hong Kong. Am.
Rev. Respir. Dis. 145:3641; Polesky A. Farber HW. Gottlieb DJ. Park H. Levinson S.
O'Connell JJ. McInnis B. Nieves RL. Bernardo J. Rifampin preventive therapy for
tuberculosis in Boston's homeless. Am J Respir Crit Care Med. 154:1473-7, 1996).
Shorter duration than INH; less hepatotoxicity.
Limited by potential interactions of rifampin with many other medications, including
birth control pills and hormonal implants 11 and anti-retroviral therapy used for
HIV/AIDS. 12
Rifampin may cause false-positive urine test for opiates, which may be an important
consideration in cases involving some types of workers who may be subject to routine
testing (such as bus drivers or law enforcement personnel).
Useful option for INH -intolerant adults or for contacts of known INH-resistant cases. A
recent review strongly suggests wider use of this regimen because of its short duration
and safety (Reichman, LB, Lardizabal, A, Hayden, CH. Considering the role of four
9
INH hepatotoxicity is age-related, with increasing rates over age 35 years. (See Question 15).
INH for 9 months is the only regimen recommended for treatment of children with LTBI at this time.
11
An alternative method of birth control (e.g. a barrier method, such as condoms) must be used by heterosexually-active women
to avoid pregnancy.
12
Interactions between rifamycins and drugs used in HIV treatment are complex (see Question 15).
10
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 9
months of rifampin in the treatment of latent tuberculosis infection. Amer J Respir Crit
Care Med. 170:832-5, 2004.
NOTE: The recommendation for a 2 month regimen of rifampin plus pyrazinamide (2RZ),
originally made in the April, 2000, ATS/CDC Guidelines, has been withdrawn because of
its unacceptably high rate of hepatotoxicity. The 2 month rifampin plus pyrazinamide
regimen should not be used in either HIV-negative or HIV-positive persons for treatment
of LTBI ( MMWR 52(31), 735-739, August 8, 2003 ).
Question 13: How do I decide which treatment regimen to choose for my patient?
Choosing a treatment regimen is based on several considerations, such as
Efficacy: All 3 treatments are considered efficacious, although the 9-month INH
regimen is considered more efficacious than either 6-month INH or the 4 month rifampin.
Medical considerations:
- Active liver disease, history of previous hepatitis, or factors predisposing to liver
disease such as alcoholism, injection drug use, and use of prescription drugs associated
with liver toxicity: postpone or reconsider therapy. Rifampin is associated with less
hepatotoxicity than INH.
- Essential medications that interact with rifampin (including some HIV therapy, see
footnote 12): avoid rifampin, postpone, or reconsider treatment.
- Birth control pills and hormonal implants: avoid rifampin or find alternative birth
control (e.g. barrier method, such as condoms).
- Pregnancy: INH and rifampin are considered safe (category C) during pregnancy, when
necessary; vitamin B6 is recommended with INH during pregnancy. Close monitoring for
hepatotoxicity during pregnancy and for at least 3 months postpartum is warranted in
women treated for LTBI. Many providers and patients prefer to postpone elective
treatment for LTBI until after pregnancy on the general principal that non essential drugs
should be avoided, especially during the first trimester. However, HIV infection and
recent TB exposure with TST conversion are strong indications for therapy during
pregnancy.
- Breast feeding: not a contraindication to therapy. Although drugs may be secreted in
breast milk, no adverse effects from these drugs on nursing infants have been
demonstrated.
Logistical considerations: Persons who will be moving from the area or who are in a
supervised setting for a limited duration (e.g, college students, detox, rehabilitation,
prison) may be more appropriate for a shorter regimen. Persons who can be supervised
over a longer period (e.g, in prisons) may be given the 9-month INH treatment regimen
with less fear of non-adherence.
Age: Risk of INH-induced hepatitis increases with age (see footnote 9). Previous
ATS/CDC recommendations limited INH to persons under age 35 years; for persons
older than 35 years of age, treatment was recommended only when other risk factors,
such as recent TST conversion, HIV co-infection, or x-ray abnormalities suggesting old
TB, were present. The current ATS/CDC recommendations assume that only high-risk
persons are tested, and therefore, treatment with INH and /or rifampin is warranted at any
age. In reality, however, considerable administrative testing (required for job clearance,
immigration, etc) still occurs among persons at low-risk for TB. Of the 3 approved
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 10
treatment regimens for LTBI, 4 months of daily rifampin alone may have the least
hepatotoxicity for those over age 35.
Cost: INH is less expensive than rifampin alone. However, shorter course regimens
generally require fewer office visits (see Question 15: Monitoring, below). Drug
intolerance, drug interactions, and laboratory tests are among the other costs to be
considered. In Massachusetts, treatment for LTBI is available free of charge through the
Massachusetts Department of Public Healths TB clinic system.
Patient choice: In the absence of factors dictating one regimen or another, patients often
have strong opinions about taking one INH tablet daily for 6 or 9 months, or 2 rifampin
capsules (typical doses) daily for 4 months. Current preparations of INH in suspension
are based in sorbital, and at doses indicated for older children and adults can cause
diarrhea.
Question 14: What are the appropriate dosages for the 3 LTBI treatment options, and how
should they be prescribed?
The dosages are listed below. Please refer to the official CDC/ATS guidelines for additional
details (Table 8, ATS/CDC LTBI Statement, AJRCCM 2000).
INH: (50, 100, 300 mg tablets; 50 mg/5 ml oral suspension)
- Adults: 5 mg/kg (300 mg, max) daily, or 15 mg/kg (900 mg, max) twice weekly.
- Children: 10-20 mg/kg (up to 300 mg) daily, or 20-30 mg/kg twice weekly (up to 900
mg) twice weekly (see response to Question 13, above, re. INH suspension and diarrhea).
Rifampin: (150, 300 mg capsules) 10 mg/kg (600 mg, max) daily or twice weekly
(unlike twice weekly INH, dose is not increased). Not recommended for treatment of
LTBI in children.
Rifabutin: 13 (150 mg capsules) 5 mg/kg (300 mg max) daily or twice weekly (rifabutin
daily or twice weekly is reduced to 150 mg when used in combination with some
antiretroviral agents.
Question 15: How should I monitor safety and adherence during LTBI treatment?
Regular monitoring of treatment for LTBI is performed for 3 purposes: to reinforce patient
education, to encourage adherence, and to increase safety. Recommended monitoring varies
with the 3 regimens:
INH (9- and 6-month regimens): Monthly visits to a trained health care provider are
strongly recommended during INH therapy. It is the standard-of-care for all
Massachusetts TB clinics. Patients are given a prescription for no more than a one-month
drug supply, and this prescription is re-filled following each monthly clinical assessment.
The main complications of INH therapy are:
- Hepatitis. In patients taking INH, hepatitis occurs with increasing frequency with
age. In over 11,000 patients receiving INH in a public health clinic, Nolan reported a
hepatitis rate of only 0.1% among patients; the majority of patients in this study were
under age 35 years (JAMA 1999 281; 1014-18. Full text available at:
13
Rifabutin may be substituted for rifampin in HIV/AIDS patients who are being treated with some anti-retroviral therapy
regimens (see Question 15).
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 11
http://jama.ama-assn.org). Only clinical monitoring for symptoms and signs
suggestive of hepatitis (loss of appetite, fatigue, malaise, nausea, RUQ abdominal
discomfort, fever, dark urine, jaundice) was used in this study. Hepatitis was
confirmed by liver function tests. All patients recovered with prompt cessation of the
drug.
- Most patients can be followed without baseline or routine follow-up liver function
tests if they are educated appropriately and can be closely monitored clinically and
questioned at least monthly about symptoms. With the onset of any new symptoms,
patients should be clearly instructed to first stop INH and then call their provider for
further instructions. The rare fatalities associated with INH hepatitis have been
associated with continued INH ingestion, despite hepatitis symptoms. Indications for
baseline and periodic biochemical monitoring include patients over age 35 or with
known abnormal liver function, known liver disease, or a history of hepatitis or
factors that predispose to hepatitis, such as alcoholism, injection drug use, and use of
prescription drugs associated with hepatitis, including prior liver toxicity from INH.
Up to 20% of people who receive INH will experience mild, asymptomatic elevations
in serum transaminases. INH should be stopped when transaminase elevations exceed
5 times normal in the absence of symptoms, or 3 times normal if symptoms
suggestive of hepatitis are present.
- Peripheral neuritis. Uncommon among patients taking daily isoniazid (5 mg/kg/day)
who are not receiving supplemental pyridoxine (vitamin B6). However, vitamin B6 (1050 mg daily) is recommended for pregnant women and for anyone whose intake of
vitamin-rich foods is questionable (e.g., alcoholics). Most public health TB clinics do not
routinely prescribe pyridoxine, in an effort to keep treatment as simple as possible.
Rifampin: Although rifamycins have been associated with a wide range of side effects,
including hepatitis, neutropenia, and a flu-like syndrome, these complications are not
common. Compared to INH, rifampin causes less hepatitis and has the best safety profile
of the major anti-tuberculous agents. However, rifampin and other rifamycins induce
hepatic microsomal enzymes and often accelerate metabolism of other important drugs,
including methadone, birth control pills and hormonal implants, coumadin, some
antihypertensives, and many others. The mutual interactions of protease inhibitors (PIs),
nonnucleoside reverse transcriptase inhibitors (NNRTIs), and rifamycins is discussed in
detail in a recent CDC announcement available on the internet at
http://www.cdc.gov/nchstp/tb/tb_hiv_drugs/toc.htm. (see footnote 5).
In general, no (NOTE, ATS does recommend baseline CBC and platelets) baseline or
routine biochemical or hematologic monitoring is recommended for persons who are
receiving rifampin, but the performance of other therapeutic agents should be monitored
during and after rifampin therapy. Should symptoms develop, biochemical or
hematologic testing is indicated. Monthly clinical monitoring is recommended for the 4month rifampin regimen.
Patients who are placed on treatment for LTBI should receive rigorous education
about the purpose of treatment and its potential risks, including possible side effects of
the medication. Relevant literature for patients are available from MDPH. Patients should
be instructed to stop the medication immediately should any adverse effect of the
medication be suspected and then to notify the provider.
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 12
Question 16: How much treatment of LTBI can be missed before the patient must start
over?
This question applies to all 3 regimens. Ideally, patients should take the equivalent of the entire
treatment course, even if additional time is needed due to interruptions. Some clinical judgment
is needed, since clinical trial data are not available to support the efficacy of the countless
possible patterns of drug ingestion. For the 9-month INH regimen, at least 270 doses should be
ingested within 12 months. For the 6-month INH regimen, at least 180 doses should be ingested
within 9 months. Finally, for the rifampin regimen, at least 120 doses should be administered
within 6 months. With any regimen, clinical re-evaluation is indicated for interruptions of greater
than 2 months. In patients who demonstrate non-adherence where DOT is not indicated or
available, treatment should be restarted only once and then re-evaluated if non-adherence reoccurs. The indications for LTBI treatment are important factors in deciding how many
treatment attempts are warranted in each case.
Question 17: If a patient will not or cannot take treatment for LTBI, what is appropriate
follow-up?
Patients who cannot, or will not, take treatment for LTBI generally are not followed clinically
for development of active TB. Neither periodic clinical exams nor periodic chest x-rays has
been shown to be effective in detecting TB disease(reactivation tuberculosis) before symptoms
develop, and neither is recommended. Patients should keep a record of their positive TST and
understand its significance. Patients should be instructed to seek medical care if they develop
signs and/or symptoms of active TB, such as an unexplained cough that lasts more than 2 weeks,
and to remind their provider of their positive TST status. Patients who complete a course of
treatment for LTBI require no further follow-up and should be given a record of their status.
"Routine," periodic chest x-rays are not indicated in the absence of signs or symptoms of active
TB.
Question 18: When should I seek consultation with a specialist?
Primary care providers are encouraged to request consultation with a pulmonary or infectious
disease specialist with experience in tuberculosis management, for the following reasons:
Treatment of LTBI in pregnancy.
Treatment of LTBI in patients receiving complex therapy for HIV.
Treatment of LTBI or active TB when drug resistance is likely (contact of a known drugresistant case).
Diagnosis and management of active TB, including interpretation of mycobacteriology
laboratory data.
TB drug complications and interactions.
Cultural/ethnic, or other barriers to TB prevention are identified.
III. Public Health Aspects
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 13
Question 19: Is LTBI reportable to the state health department?
Latent TB Infection now is reportable to the state health department in Massachusetts. The LTBI
Reporting Number (by Fax) is 617-983-6813. Reporting forms can be obtained from the
Massachusetts Department of Public Health, Integrated Surveillance and Informatics Services
(ISIS).
Active TB patients and patients suspected of active TB also are reportable by law, even if a final
diagnosis of TB is yet not established. Cases and suspect cases are reported by telephone to the
Massachusetts Department of Public Health Division of TB Prevention and Control 24 hours
daily by calling 1-888-MASSMTB (1-888-627-7682).
Question 20: What public health resources are available to my patients and me?
The Massachusetts Department of Public Health Division of Tuberculosis Prevention and
Control, in cooperation with local health departments, provides comprehensive care for persons
with TB in Massachusetts. State-supported TB clinics in health care facilities across
Massachusetts offer medical expertise, radiography, mycobacteriology, and TB therapy free of
charge to the patient for both LTBI and disease. Contact investigations of infectious cases,
source case investigations, patient and family education, hospital discharge planning, and
directly observed therapy are essential public health services provided by the Department of
Public Health. For active TB cases, case management is the shared responsibility of the treating
physician and the local and state public health nurses, and, if necessary, the support of culturallytargeted outreach educator staff. For LTBI, initial evaluation, medications, and essential
laboratory monitoring are provided. Consultation for private physicians treating cases of active
TB and LTBI is another service of the Massachusetts Department of Public Health. Dr. John
Bernardo, the State Tuberculosis Control Officer, can be reached at 617-983-6970 (State TB
Prevention and Control Program), 617- 339-7281 (pager), or by email: jbernard@bu.edu.
Appendix 1: CHILDREN WHO SHOULD BE TESTED FOR TUBERCULOSIS
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 14
A child who has been infected with tuberculosis (TB) may show no outward symptoms.
However, infection can later lead to severe illness. To detect the problem before a child
becomes ill, we perform a tuberculosis skin test.
Instead of testing all children as we have in the past, we recommend that only some
children should have a skin test. If a test is warranted, the child will be tested with the
intermediate PPD (Mantoux) skin test, because it is the most accurate available. We no
longer recommend use of the less accurate multiple puncture skin tests, such as the
Tine or Mono-vacc.
To help your childs health care provider determine if your child needs to be skin tested,
please answer the following questions:
YES
Has your child lived with or spent time with anyone
who possibly or definitely had tuberculosis?
Does anyone living in the childs household have a
positive skin test for tuberculosis?
Did you (parent or guardian), your child, or anyone
else living in your household come to the United
States from another country?
Has your child traveled to or lived in another
country for more than a month?
NO
If your child has had a positive skin test for tuberculosis in the past, inform your childs
health care provider. Your child will not need another test.
Revised July, 2001
Appendix 2: Treatment of Latent Tuberculosis Infection Reference
Card
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 15
The Treatment of Latent Tuberculosis Reference Card is available from
www.umdnj.edu/globaltb
Appendix 3: Evaluation of Program Performance Treatment of Latent
Tuberculosis Infection
The primary purpose of tuberculosis skin testing of healthy children and adults is to identify
those with latent infection whose future risk of active disease can be reduced by preventive
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 16
treatment. Preventing active tuberculosis also decreases the risk of the spread of tuberculosis to
others. The prospect of tuberculosis elimination will be enhanced.
In order to be effective, a program of testing and treatment of latent tuberculosis infection
(LTBI) requires completion of a number of steps, and the success of each step can be defined by
a quantitative performance measure. Each office, health center, and clinic should maintain its
own statistics that can serve as the basis for monitoring and continually improving performance.
Statistics should be calculated every three months and annually. These statistics should be
available for inspection by the Massachusetts Department of Public Health.
At some future time, a tuberculosis performance measure might be added to current Health Plan
Employer Data and Information Set (HEDIS) parameters used to assess the quality of preventive
health care, such as childhood immunization, Pap smear, and mammogram rates.
Step 1: Identify People at High Risk for Tuberculosis Infection
Risk of exposure to tuberculosis should be determined for every patient on entry into the health
care system and at regular intervals thereafter. Depending on circumstances, a health care
provider may decide to determine risk of tuberculosis exposure through individual clinical
history taken or by administering a formal tuberculosis risk questionnaire (Section I, Appendix
1). Definition of risk categories should be according to the recommendations of the Centers for
Disease Control and Prevention, the American Academy of Pediatrics, and the Massachusetts
Department of Public Health.
Performance Measure
Proportion Screened = Number of People Screened for Tuberculosis Risk
Number of People Seen
Step 2: Test People at High Risk for Tuberculosis Infection
The Mantoux test (intermediate PPD), (5 TU), not multiple puncture tests (such as Tine and
Mono-Vacc), must be used.
Performance Measure
Proportion Tested = Number of High Risk People Tested
Number of High Risk People Identified
Latent Tuberculosis Infection (LTBI) Targeted Testing and Treatment / page - 17
Step 3: Read Skin Test Results
All tests results, positive or negative, must be read by qualified health care personnel. Tests
should be read between 48 and 72 hours after administration. The diameter of induration, not
redness, is the basis of the reading. Test results should be measured in millimeters and
interpreted as positive or negative according to the criteria recommended by the Centers for
Disease Prevention and Control, the American Academy of Pediatrics, and the Massachusetts
Department of Public Health.
Performance Measure
Proportion of Tests Read = Number of Tests Read
Number of People Tested
Steps 4: Obtain Chest Film for People with Positive Tuberculosis Skin Tests
People with a positive tuberculosis skin test should have a medical evaluation and chest film. A
chest film is needed to distinguish latent tuberculosis infection from active disease.
Performance Measure
Proportion of People with = Number of Positive People Who have Chest Films
Positive Tuberculosis Skin Test
Number of People with Positive Tests
You might also like
- Tuberculosis in Infancy and Childhood 4th Ed (PPS)Document268 pagesTuberculosis in Infancy and Childhood 4th Ed (PPS)Jessica MarianoNo ratings yet
- Teaching Plan For TBDocument5 pagesTeaching Plan For TBChi Tuazon75% (4)
- Mantoux Test: Pirquet Test, or PPD Test For Purified Protein Derivative) Is A Diagnostic Tool ForDocument5 pagesMantoux Test: Pirquet Test, or PPD Test For Purified Protein Derivative) Is A Diagnostic Tool ForGurmeet SinghNo ratings yet
- Pulmon Ology MCQ SDocument280 pagesPulmon Ology MCQ SSai ShankerNo ratings yet
- TB Laten CDCDocument40 pagesTB Laten CDCFauziah LubisNo ratings yet
- Mott PDFDocument7 pagesMott PDFSatheesh Kumar TNo ratings yet
- Diagnosis TBC PDFDocument2 pagesDiagnosis TBC PDFAde Pratama HeriansaNo ratings yet
- TBDocument5 pagesTBQuezon D. Lerog Jr.No ratings yet
- CPH 1mto4 Tuberculosis MartinDocument4 pagesCPH 1mto4 Tuberculosis MartinEDGARDO MARTIN IIINo ratings yet
- TB AcknolwedgementDocument15 pagesTB AcknolwedgementradiciptaNo ratings yet
- TB Anywhere Is TB Everywhere: Commentary Open AccessDocument3 pagesTB Anywhere Is TB Everywhere: Commentary Open AccessSorina ElenaNo ratings yet
- Tratamiento de Tuberculosis LatenteDocument13 pagesTratamiento de Tuberculosis LatenteCarmen MolinaNo ratings yet
- United Kingdom Pre-Departure Tuberculosis Detection ProgrammeDocument5 pagesUnited Kingdom Pre-Departure Tuberculosis Detection ProgrammeStacyNo ratings yet
- An Overview On Tuberculosis TBDocument6 pagesAn Overview On Tuberculosis TBEditor IJTSRDNo ratings yet
- The Prevention and Control of Tuberculosis: An Analysis Based On A Tuberculosis Dynamic Model Derived From The Cases of AmericansDocument16 pagesThe Prevention and Control of Tuberculosis: An Analysis Based On A Tuberculosis Dynamic Model Derived From The Cases of AmericansNada FakhiraNo ratings yet
- Targeted Tuberculosis (TB) Testing and Treatment of Latent TB InfectionDocument90 pagesTargeted Tuberculosis (TB) Testing and Treatment of Latent TB Infectionwisnu kuncoroNo ratings yet
- HepatitisDocument18 pagesHepatitismaheen aurangzaibNo ratings yet
- JurnalDocument7 pagesJurnalBimaSuryaNo ratings yet
- RNTCPDocument46 pagesRNTCPdarshitkotadiya2553No ratings yet
- SESSION 15. TB and HIV Co-InfectionDocument26 pagesSESSION 15. TB and HIV Co-InfectionParadise LoveNo ratings yet
- Research Paper On TBDocument7 pagesResearch Paper On TBhxmchprhf100% (1)
- Ofx 137Document7 pagesOfx 137Sheila Alcalde RNo ratings yet
- Rapid Communication: TB Antigen-Based Skin Tests For The Diagnosis of TB InfectionDocument5 pagesRapid Communication: TB Antigen-Based Skin Tests For The Diagnosis of TB InfectionyoNo ratings yet
- IJTLDeditorial Protecting HCworkers Form TBDocument2 pagesIJTLDeditorial Protecting HCworkers Form TBRoma ParyaniNo ratings yet
- Drug Resistance of TBDocument17 pagesDrug Resistance of TBGaurav Sharma100% (1)
- Tuberculosis Infection (Latent Tuberculosis) in Adults - Approach To Diagnosis (Screening) - UpToDateDocument41 pagesTuberculosis Infection (Latent Tuberculosis) in Adults - Approach To Diagnosis (Screening) - UpToDatecrlajnmNo ratings yet
- Screening For Latent Tuberculosis Infection in South Korean Healthcare Workers Using A Tuberculin Skin Test and Whole Blood Interferon-G AssayDocument8 pagesScreening For Latent Tuberculosis Infection in South Korean Healthcare Workers Using A Tuberculin Skin Test and Whole Blood Interferon-G AssayRio BP WijayaNo ratings yet
- Tuberculosis BiomarkersDocument9 pagesTuberculosis BiomarkersSantanu PalNo ratings yet
- Global Health Case Study CMHDocument6 pagesGlobal Health Case Study CMHapi-482580060No ratings yet
- BY Dr. Tahmina AzharDocument71 pagesBY Dr. Tahmina Azharscribdnotes123No ratings yet
- TB Guidance Chapter 2Document15 pagesTB Guidance Chapter 2dindaNo ratings yet
- Latent TB: Presented by DR/ Heba RagabDocument27 pagesLatent TB: Presented by DR/ Heba RagabHosam GomaaNo ratings yet
- DR José Caminero of The Union On Challenge of anti-TB Resistance in Context of SDGsDocument29 pagesDR José Caminero of The Union On Challenge of anti-TB Resistance in Context of SDGsbobbyramakantNo ratings yet
- Mycobacterium Tuberculosis ThesisDocument5 pagesMycobacterium Tuberculosis Thesisamandagraytulsa100% (2)
- 1 s2.0 S0422763815301023 MainDocument4 pages1 s2.0 S0422763815301023 MainEghar EverydayishellNo ratings yet
- Tuberculosis Diagnostic Tools: An Activist'S Guide ToDocument30 pagesTuberculosis Diagnostic Tools: An Activist'S Guide TomyikellaNo ratings yet
- Contemporary Data On TB Epidemiology by Nwokotubo Beulah 2Document26 pagesContemporary Data On TB Epidemiology by Nwokotubo Beulah 2Beulah AlexNo ratings yet
- Research Article: Characteristics and Treatment Outcomes of Retreatment Tuberculosis Patients in BeninDocument7 pagesResearch Article: Characteristics and Treatment Outcomes of Retreatment Tuberculosis Patients in BeninfaustinaNo ratings yet
- Tuberculosis Contact Investigations - United States, 2003-2012Document24 pagesTuberculosis Contact Investigations - United States, 2003-2012viannikkkyNo ratings yet
- TB MeningitisDocument10 pagesTB Meningitisrizky ramadhanNo ratings yet
- Media Centre: Buruli UlcerDocument6 pagesMedia Centre: Buruli UlcerSyvelmarie TinteNo ratings yet
- TB and HIVDocument62 pagesTB and HIVNational Press FoundationNo ratings yet
- Tuberculosis: Infection and TransmissionDocument7 pagesTuberculosis: Infection and TransmissionMonica AgapitoNo ratings yet
- Copia de Final 2016-2017 No AnswersDocument21 pagesCopia de Final 2016-2017 No AnswersadkfnlsºNo ratings yet
- Tuberculosis ICD-10 A15-A19: Dr. Nadia Aziz C.A.B.C.M Department of Community Medicine Baghdad Medical CollegeDocument58 pagesTuberculosis ICD-10 A15-A19: Dr. Nadia Aziz C.A.B.C.M Department of Community Medicine Baghdad Medical CollegeMazinNo ratings yet
- Reference ThesisDocument13 pagesReference ThesisGhina SalsabilaNo ratings yet
- Multidrug-Resistant Tuberculosis in Uzbekistan: Results of A Nationwide Survey, 2010 To 2011Document12 pagesMultidrug-Resistant Tuberculosis in Uzbekistan: Results of A Nationwide Survey, 2010 To 2011IsoqjonivichNo ratings yet
- Identification and Management of Latent Tuberculosis InfectionDocument8 pagesIdentification and Management of Latent Tuberculosis InfectionRivani KurniawanNo ratings yet
- Overview of Tuberculosis-WithNotesDocument26 pagesOverview of Tuberculosis-WithNotesivanradosinavicNo ratings yet
- Mycobacterium Other Than Tuberculosis (MOTT) : Section: 4.0 Diseases and ConditionsDocument7 pagesMycobacterium Other Than Tuberculosis (MOTT) : Section: 4.0 Diseases and ConditionsSagir AlvaNo ratings yet
- Interferon-γ release assay as a sensitive diagnostic tool of latent tuberculosis infection in patients with HIV: a cross- sectional studyDocument8 pagesInterferon-γ release assay as a sensitive diagnostic tool of latent tuberculosis infection in patients with HIV: a cross- sectional studyAnanda DewaNo ratings yet
- Early Detection of TBDocument32 pagesEarly Detection of TBAlfonso HasudunganNo ratings yet
- Tuberculosis Infection Control Practices and AssocDocument12 pagesTuberculosis Infection Control Practices and AssocchalachewNo ratings yet
- TB HIV Research Proposal HarishDocument23 pagesTB HIV Research Proposal HarishLekha Bahadur Gurung100% (4)
- Literature Review On MDR-TBDocument5 pagesLiterature Review On MDR-TBafmzslnxmqrjom100% (1)
- Multidrug-Resistant Tuberculosis (MDR-TB) Is Defined As TB That Is Resistant To BothDocument4 pagesMultidrug-Resistant Tuberculosis (MDR-TB) Is Defined As TB That Is Resistant To Bothsanny_sundariNo ratings yet
- TuberculosisDocument55 pagesTuberculosisAfrath Mohamed100% (1)
- Thesis Tuberculosis PaperDocument6 pagesThesis Tuberculosis Paperlbbzfoxff100% (2)
- Overview Tropical Diseases 15 I TaeDocument211 pagesOverview Tropical Diseases 15 I TaeMaria Del Mar RoblesNo ratings yet
- Epidemiology of Tuberculosis - UpToDateDocument33 pagesEpidemiology of Tuberculosis - UpToDateCentro de salud El quincheNo ratings yet
- Mantoux Test-Method, Indications, PitfallsDocument8 pagesMantoux Test-Method, Indications, PitfallsJyothika SanalNo ratings yet
- COVID-19 Mortality Review in Malaysia & Updates on Clinical Management of COVID-19From EverandCOVID-19 Mortality Review in Malaysia & Updates on Clinical Management of COVID-19No ratings yet
- Intervensi Pulmo Konas Perpari-1Document32 pagesIntervensi Pulmo Konas Perpari-1Rivani KurniawanNo ratings yet
- Imaging Acute Abdomen DR - Rivani Kurniawan FixDocument86 pagesImaging Acute Abdomen DR - Rivani Kurniawan FixRivani KurniawanNo ratings yet
- 2002 Vol.40 Issues 4 Vascular Imaging PDFDocument278 pages2002 Vol.40 Issues 4 Vascular Imaging PDFRivani KurniawanNo ratings yet
- Identification and Management of Latent Tuberculosis InfectionDocument8 pagesIdentification and Management of Latent Tuberculosis InfectionRivani KurniawanNo ratings yet
- The Epidemiology of Childhood Tuberculosis in The Netherlands: Still Room For PreventionDocument9 pagesThe Epidemiology of Childhood Tuberculosis in The Netherlands: Still Room For PreventionRivani KurniawanNo ratings yet
- HI Local Nov07Document15 pagesHI Local Nov07Rivani KurniawanNo ratings yet
- TendinitisDocument6 pagesTendinitisRivani KurniawanNo ratings yet
- Daftar Pustaka 7689Document20 pagesDaftar Pustaka 7689Rivani KurniawanNo ratings yet
- Bcgletter1 09Document1 pageBcgletter1 09Rivani KurniawanNo ratings yet
- Daftar Pustaka bcg098Document6 pagesDaftar Pustaka bcg098Rivani KurniawanNo ratings yet
- Rhabdomyosarcoma in PediatricDocument2 pagesRhabdomyosarcoma in PediatricRivani KurniawanNo ratings yet
- Imaging Vesika Seminalis Dan Vas DeferenDocument68 pagesImaging Vesika Seminalis Dan Vas DeferenRivani KurniawanNo ratings yet
- PP Jurnal Thorak NewDocument93 pagesPP Jurnal Thorak NewRivani KurniawanNo ratings yet
- Chest Wall TumorDocument27 pagesChest Wall TumorRivani KurniawanNo ratings yet
- Chest 2003 Jun 123 (6) 2019-27, Figure 3Document1 pageChest 2003 Jun 123 (6) 2019-27, Figure 3Rivani KurniawanNo ratings yet
- Musculoskeletal TraumaDocument12 pagesMusculoskeletal TraumaRivani KurniawanNo ratings yet
- GastrointestinalDocument29 pagesGastrointestinalRivani KurniawanNo ratings yet
- End TB EssentialDocument130 pagesEnd TB EssentialRiva MarchiellaNo ratings yet
- Module 2 EbookDocument14 pagesModule 2 EbookJulienne VinaraoNo ratings yet
- Tuberculosis in PregnancyDocument18 pagesTuberculosis in PregnancyNitesh GuptaNo ratings yet
- Tuberculosis Infection Control Guidelines: Ministry of Health and Social ServicesDocument45 pagesTuberculosis Infection Control Guidelines: Ministry of Health and Social ServicesBich Le Thi NgocNo ratings yet
- Promoting Cultural Sensitivity: A Practical Guide For Tuberculosis Programs That Provide Services To Persons From SomaliaDocument52 pagesPromoting Cultural Sensitivity: A Practical Guide For Tuberculosis Programs That Provide Services To Persons From SomaliaalexNo ratings yet
- Cutaneous Manifestations of TuberculosisDocument35 pagesCutaneous Manifestations of TuberculosisSaid Plazola MercadoNo ratings yet
- Your Medication Schedule: The 12-Dose Regimen For Latent Tuberculosis (TB) InfectionDocument2 pagesYour Medication Schedule: The 12-Dose Regimen For Latent Tuberculosis (TB) InfectionJuan Miguel PangilinanNo ratings yet
- Diagnosing TB Infection in Children: Analysis of Discordances Using in Vitro Tests and The Tuberculin Skin TestDocument9 pagesDiagnosing TB Infection in Children: Analysis of Discordances Using in Vitro Tests and The Tuberculin Skin TestAri Julian SaputraNo ratings yet
- Tuberculosis TBDocument9 pagesTuberculosis TB8pvz96ktd9No ratings yet
- Chapter 5: Treatment For Latent Tuberculosis InfectionDocument30 pagesChapter 5: Treatment For Latent Tuberculosis InfectionPhilippe Ceasar C. BascoNo ratings yet
- Ebook The Brigham Intensive Review of Internal Medicine Question Answer Companion PDF Full Chapter PDFDocument67 pagesEbook The Brigham Intensive Review of Internal Medicine Question Answer Companion PDF Full Chapter PDFsara.freese515100% (31)
- FinalthesisoftuberculosisDocument86 pagesFinalthesisoftuberculosisOuaingar ngueadoumNo ratings yet
- Tuberculosis Guidelines Guyana 2011Document213 pagesTuberculosis Guidelines Guyana 2011api-303541804100% (4)
- Tuberculosis Thesis TopicsDocument7 pagesTuberculosis Thesis Topicsstacyjohnsonreno100% (2)
- Tuberculosis (TB) Presentation PDFDocument12 pagesTuberculosis (TB) Presentation PDFUday GuptaNo ratings yet
- Job Aids TPTDocument10 pagesJob Aids TPTTarikul IslamNo ratings yet
- Tuberculosis TBDocument5 pagesTuberculosis TBHusna AmaliaNo ratings yet
- Tuberculosis in Infancy and ChildhoodDocument39 pagesTuberculosis in Infancy and ChildhoodPediatrics SLCM-WHQMNo ratings yet
- Bacterial Uveitis - DR ArnavDocument59 pagesBacterial Uveitis - DR ArnavDr Arnav SaroyaNo ratings yet
- Case Studies TB NCM Training ToolsDocument127 pagesCase Studies TB NCM Training ToolsJay KumarNo ratings yet
- Group Case Study - Pulmonary TBDocument8 pagesGroup Case Study - Pulmonary TBCj NiñalNo ratings yet
- LTBI Fact SheetDocument8 pagesLTBI Fact SheetLarry KivayaNo ratings yet
- A View On TB ControlDocument30 pagesA View On TB ControlhonorinanuguidNo ratings yet
- TB - OutlineDocument11 pagesTB - Outlinekent yeeNo ratings yet
- TuberculosisDocument53 pagesTuberculosisDaniel JaymeNo ratings yet
- National Guidelines For HIV Care and Treatment 2021Document556 pagesNational Guidelines For HIV Care and Treatment 2021Moin PandithNo ratings yet
- Print Edition: 19 May 2014Document21 pagesPrint Edition: 19 May 2014Dhaka TribuneNo ratings yet