Professional Documents
Culture Documents
Interpretation of Arterial Blood Gases
Interpretation of Arterial Blood Gases
Uploaded by
Riska PashaOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Interpretation of Arterial Blood Gases
Interpretation of Arterial Blood Gases
Uploaded by
Riska PashaCopyright:
Available Formats
INTERPRETATION OF ARTERIAL BLOOD GASES (ABGS)
Interpretation of Arterial Blood Gases (ABGs)
David A. Kaufman, MD
Chief, Section of Pulmonary, Critical Care & Sleep Medicine
Bridgeport Hospital-Yale New Haven Health
Assistant Clinical Professor, Yale University School of Medicine
(Section of Pulmonary & Critical Care Medicine)
Introduction:
Interpreting an arterial blood gas (ABG) is a crucial skill for physicians, nurses, respiratory therapists, and other health care personnel. ABG
interpretation is especially important in critically ill patients.
The following six-step process helps ensure a complete interpretation of every ABG. In addition, you will find tables that list commonly
encountered acid-base disorders.
Many methods exist to guide the interpretation of the ABG. This discussion does not include some methods, such as analysis of base excess or
Stewarts strong ion difference. A summary of these techniques can be found in some of the suggested articles. It is unclear whether these
alternate methods offer clinically important advantages over the presented approach, which is based on the anion gap.
Readers are welcome to discuss their observations and share their comments on the ATS Critical Care Forums.
6-step approach:
Step 1: Assess the internal consistency of the values using the Henderseon-Hasselbach equation:
[H+] = 24(PaCO2)
[HCO3-]
If the pH and the [H+] are inconsistent, the ABG is probably not valid.
pH
Approximate
[H+]
(mmol/L)
7.00
100
7.05
89
7.10
79
7.15
71
7.20
63
7.25
56
7.30
50
7.35
45
7.40
40
7.45
35
7.50
32
7.55
28
7.60
25
7.65
22
Step 2: Is there alkalemia or acidemia present?
pH < 7.35 acidemia
pH > 7.45 alkalemia
This is usually the primary disorder
Remember: an acidosis or alkalosis may be present even if the pH is in the normal range (7.35 7.45)
You will need to check the PaCO2, HCO3- and anion gap
Step 3: Is the disturbance respiratory or metabolic? What is the relationship between the direction of change in the pH and the direction of
change in the PaCO2? In primary respiratory disorders, the pH and PaCO2 change inopposite directions; in metabolic disorders the pH and
PaCO2 change in the same direction.
Acidosis
Respiratory
pH
PaCO2
Acidosis
Metabolic&
pH
PaCO2
Alkalosis
Respiratory
pH
PaCO2
Alkalosis
Metabolic
pH
PaCO2
Step 4: Is there appropriate compensation for the primary disturbance? Usually, compensation does not return the pH to normal (7.35 7.45).
Disorder
Expected compensation
Correction
factor
Metabolic acidosis
PaCO2 = (1.5 x [HCO3-]) +8
Acute respiratory
Increase in [HCO3-]=
acidosis
PaCO2/10
Chronic respiratory
acidosis (3-5 days)
Increase in [HCO3-]= 3.5(
PaCO2/10)
Metabolic alkalosis
Increase in PaCO2 = 40 +
0.6(HCO3-)
Acute respiratory
alkalosis
Decrease in [HCO3-]= 2(
PaCO2/10)
Chronic respiratory
alkalosis
Decrease in [HCO3-] = 5(
PaCO2/10) to 7( PaCO2/10)
If the observed compensation is not the expected compensation, it is likely that more than one acid-base disorder is present.
Step 5: Calculate the anion gap (if a metabolic acidosis exists): AG= [Na+]-( [Cl-] + [HCO3-] )-12 2
A normal anion gap is approximately 12 meq/L.
In patients with hypoalbuminemia, the normal anion gap is lower than 12 meq/L; the normal anion gap in patients with
hypoalbuminemia is about 2.5 meq/L lower for each 1 gm/dL decrease in the plasma albumin concentration (for example, a patient
with a plasma albumin of 2.0 gm/dL would be approximately 7 meq/L.)
If the anion gap is elevated, consider calculating the osmolal gap in compatible clinical situations.
Elevation in AG is not explained by an obvious case (DKA, lactic acidosis, renal failure
Toxic ingestion is suspected
OSM gap = measured OSM (2[Na+] - glucose/18 BUN/2.8
The OSM gap should be < 10
Step 6: If an increased anion gap is present, assess the relationship between the increase in the anion gap and the decrease in [HCO 3-].
Assess the ratio of the change in the anion gap (AG ) to the change in [HCO3-] ([HCO3-]): AG/[HCO3-]
This ratio should be between 1.0 and 2.0 if an uncomplicated anion gap metabolic acidosis is present.
If this ratio falls outside of this range, then another metabolic disorder is present:
If AG/[HCO3-] < 1.0, then a concurrent non-anion gap metabolic acidosis is likely to be present.
If AG/[HCO3-] > 2.0, then a concurrent metabolic alkalosis is likely to be present.
It is important to remember what the expected normal anion gap for your patient should be, by adjusting for hypoalbuminemia (see Step 5,
above.)
Table 1: Characteristics of acid-base disturbances
Disorder
pH
Primary problem
Compensation
Metabolic acidosis
in HCO3-
in PaCO2
Metabolic alkalosis
in HCO3-
in PaCO2
Respiratory acidosis
in PaCO2
in [HCO3-]
Respiratory alkalosis
in PaCO2
in [HCO3-]
Table 2: Selected etiologies of respiratory acidosis
Airway obstruction
- Upper
- Lower
COPD
asthma
other obstructive lung disease
CNS depression
Sleep disordered breathing (OSA or OHS)
Neuromuscular impairment
Ventilatory restriction
Increased CO2 production: shivering, rigors, seizures, malignant hyperthermia, hypermetabolism, increased intake of carbohydrates
Incorrect mechanical ventilation settings
Table 3: Selected etiologies of respiratory alkalosis
CNS stimulation: fever, pain, fear, anxiety, CVA, cerebral edema, brain trauma, brain tumor, CNS infection
Hypoxemia or hypoxia: lung disease, profound anemia, low FiO2
Stimulation of chest receptors: pulmonary edema, pleural effusion, pneumonia, pneumothorax, pulmonary embolus
Drugs, hormones: salicylates, catecholamines, medroxyprogesterone, progestins
Pregnancy, liver disease, sepsis, hyperthyroidism
Incorrect mechanical ventilation settings
Table 4: Selected causes of metabolic alkalosis
Hypovolemia with Cl- depletion
GI loss of H+
Renal loss H+
Vomiting, gastric suction, villous adenoma, diarrhea with chloride-rich fluid
Loop and thiazide diuretics, post-hypercapnia (especially after institution of mechanical ventilation)
Hypervolemia, Cl- expansion
Renal loss of H+: edematous states (heart failure, cirrhosis, nephrotic syndrome), hyperaldosteronism, hypercortisolism,
excess ACTH, exogenous steroids, hyperreninemia, severe hypokalemia, renal artery stenosis, bicarbonate administration
Table 5: Selected etiologies of metabolic acidosis
a
b
Elevated anion gap:
Methanol intoxication
Uremia
Diabetic ketoacidosisa, alcoholic ketoacidosis, starvation ketoacidosis
Paraldehyde toxicity
Isoniazid
Lactic acidosisa
Type A: tissue ischemia
Type B: Altered cellular metabolism
Ethanolb or ethylene glycolb intoxication
Salicylate intoxication
Most common causes of metabolic acidosis with an elevated anion gap
Frequently associated with an osmolal gap
Normal anion gap: will have increase in [Cl-]
GI loss of HCO3-
Renal loss of HCO3-
Diarrhea, ileostomy, proximal colostomy, ureteral diversion
proximal RTA
carbonic anhydrase inhibitor (acetazolamide)
Renal tubular disease
ATN
Chronic renal disease
Distal RTA
Aldosterone inhibitors or absence
NaCl infusion, TPN, NH4+ administration
Table 6: Selected mixed and complex acid-base disturbances
Disorder
Respiratory acidosis
with metabolic
acidosis
Respiratory alkalosis
with metabolic
alkalosis
Respiratory acidosis
with metabolic
alkalosis
Respiratory alkalosis
with metabolic
acidosis
Characteristics
in pH
in HCO3
in PaCO2
Selected situations
Cardiac arrest
Intoxications
Multi-organ failure
in pH
in HCO3 in PaCO2
Cirrhosis with diuretics
Pregnancy with vomiting
Over ventilation of COPD
pH in normal range
in PaCO2,
in HCO3-
COPD with diuretics,
vomiting, NG suction
Severe hypokalemia
pH in normal range
in PaCO2
in HCO3
Metabolic acidosis
with metabolic
alkalosis
pH in normal range
HCO3- normal
Sepsis
Salicylate toxicity
Renal failure with CHF or
pneumonia
Advanced liver disease
Uremia or ketoacidosis with
vomiting, NG suction,
diuretics, etc.
Suggested additional reading:
Rose, B.D. and T.W. Post. Clinical physiology of acid-base and electrolyte disorders, 5th ed. New York: McGraw Hill Medical
Publishing Division, c2001.
Fidkowski, C And J. Helstrom. Diagnosing metabolic acidosis in the critically ill: bridging the anion gap, Stewart and base excess
methods. Can J Anesth 2009;56:247-256.
Adrogu, H.J. and N.E. Madias. Management of life-threatening acid-base disordersfirst of two parts. N Engl J Med 1998;338:26-34.
Adrogu, H.J. and N.E. Madias. Management of life-threatening acid-base disorderssecond of two parts. N Engl J
Med 1998;338:107-111.
To comment on or discuss this article, please visit the ATS Forums.
You might also like
- Interpretation of Arterial Blood Gases (ABGs)Document6 pagesInterpretation of Arterial Blood Gases (ABGs)afalfitraNo ratings yet
- Arterial Blood Gas Analysis - making it easyFrom EverandArterial Blood Gas Analysis - making it easyRating: 4.5 out of 5 stars4.5/5 (4)
- Acid Base BalanceDocument9 pagesAcid Base BalanceNawarajendra MunakarmiNo ratings yet
- Michael Chansky Acid Base Made Easy Handout PDFDocument18 pagesMichael Chansky Acid Base Made Easy Handout PDFAustine OsaweNo ratings yet
- NCP Nasal PolypsDocument3 pagesNCP Nasal Polypsnickanel60% (5)
- American Thoracic Society - Interpretation of Arterial Blood Gases (ABGs)Document7 pagesAmerican Thoracic Society - Interpretation of Arterial Blood Gases (ABGs)humberto_2No ratings yet
- Arterial Blood Gas InterpretationsDocument7 pagesArterial Blood Gas InterpretationsErin TraversNo ratings yet
- Interpretation of Arterial Blood GasesDocument7 pagesInterpretation of Arterial Blood GasesGaby FernándezNo ratings yet
- Interpretation of Arterial Blood GasesDocument16 pagesInterpretation of Arterial Blood GasesRuby Ann Cañero HigoyNo ratings yet
- Clinical Education: Interpretation of AbgsDocument8 pagesClinical Education: Interpretation of AbgsRumela Ganguly ChakrabortyNo ratings yet
- American Thoracic Society - Interpretation of Arterial Blood Gases (ABGs)Document8 pagesAmerican Thoracic Society - Interpretation of Arterial Blood Gases (ABGs)muhammadridhwanNo ratings yet
- ABG Interpretation - ATSDocument5 pagesABG Interpretation - ATSHAMMYER ALROKHAMINo ratings yet
- Abg InterpretationDocument7 pagesAbg InterpretationPreetha PANo ratings yet
- Interpretation of Arterial Blood Gases (Abgs) I David A. Kaufman, MD DDocument17 pagesInterpretation of Arterial Blood Gases (Abgs) I David A. Kaufman, MD DingridpuspitaNo ratings yet
- Acid Base Disorders JAPIDocument5 pagesAcid Base Disorders JAPIVitrag_Shah_1067No ratings yet
- Interpretation of ABGs ATSDocument6 pagesInterpretation of ABGs ATSjayson2708No ratings yet
- Interpretasi ABGDocument5 pagesInterpretasi ABGNella Rosyalina DamayantiNo ratings yet
- Interpretasi AGDDocument129 pagesInterpretasi AGDIta SobaNo ratings yet
- Acid-Base Made EasyDocument14 pagesAcid-Base Made EasyMayer Rosenberg100% (10)
- Arterial Blood Gas AnalysisDocument28 pagesArterial Blood Gas Analysishendra_darmawan_4No ratings yet
- H + Hco H Co H Ol + CO (G) : Acid-Base BalanceDocument7 pagesH + Hco H Co H Ol + CO (G) : Acid-Base BalanceAndreas NatanNo ratings yet
- 4 Acid Base Disorder 2021Document81 pages4 Acid Base Disorder 2021SHIKUR YASINNo ratings yet
- Arterial Blood Gas Interpretation: Joseph Brian L. Costiniano, MD, DPCPDocument39 pagesArterial Blood Gas Interpretation: Joseph Brian L. Costiniano, MD, DPCPevbptrprnrmNo ratings yet
- Arterial Blood Gas Interpretation: Joseph Brian L. Costiniano, MD, DPCPDocument39 pagesArterial Blood Gas Interpretation: Joseph Brian L. Costiniano, MD, DPCPGio Tamaño BalisiNo ratings yet
- Michael Chansky Acid Base Made Easy HandoutDocument18 pagesMichael Chansky Acid Base Made Easy HandoutTeguh RamadhanNo ratings yet
- Interpreting ABG - An Interative Session: Dr. Manjunath Patil Professor, Dept. of Anaesthesiology J.N.Medical CollegeDocument31 pagesInterpreting ABG - An Interative Session: Dr. Manjunath Patil Professor, Dept. of Anaesthesiology J.N.Medical CollegeMadhan Mohan Reddy KatikareddyNo ratings yet
- Arterial Blood Gas Analysis-1Document74 pagesArterial Blood Gas Analysis-1ArunNo ratings yet
- Acidosis Metabolica 2015 PDFDocument18 pagesAcidosis Metabolica 2015 PDFGUADALUPE ARANDA OSORIONo ratings yet
- Blood Gas Analysis CMEDocument12 pagesBlood Gas Analysis CMEpierhot_11No ratings yet
- 2014-02-17 Acid Base Physiology and ABG Interpretation PDFDocument149 pages2014-02-17 Acid Base Physiology and ABG Interpretation PDFIva Dewi Permata PhilyNo ratings yet
- Background: Henderson-Hasselbalch Approach To Acid/base PhysiologyDocument11 pagesBackground: Henderson-Hasselbalch Approach To Acid/base PhysiologyErida Prifti100% (1)
- Acid - Base Basics: Dr. Fawzeya Aboul Fetouh Prof of Anesthesia Cairo UnversityDocument54 pagesAcid - Base Basics: Dr. Fawzeya Aboul Fetouh Prof of Anesthesia Cairo UnversityPaolo Uccello100% (1)
- Acid Base DisordersDocument5 pagesAcid Base DisordersMillenial VoiceNo ratings yet
- Blood Gas TestDocument6 pagesBlood Gas TestyudhafpNo ratings yet
- "Blood Gas Analysis in A Nutshell: DR Anshuman MishraDocument28 pages"Blood Gas Analysis in A Nutshell: DR Anshuman MishraMinaz PatelNo ratings yet
- Nikko Angelo P. Alcala, MD 2 Year ARODDocument8 pagesNikko Angelo P. Alcala, MD 2 Year ARODAnna MarieNo ratings yet
- Metabolic Acid-Base DisordersDocument14 pagesMetabolic Acid-Base DisordersAlan Espíndola CruzNo ratings yet
- Arterial Blood Gas Analysis: BY-Shivam Sachan (JR Ii) Moderator - Dr. R.K YADAV (M.D)Document52 pagesArterial Blood Gas Analysis: BY-Shivam Sachan (JR Ii) Moderator - Dr. R.K YADAV (M.D)imranqazi11No ratings yet
- Acid-Base Homeostasis: Dr. Abeer KhurshidDocument42 pagesAcid-Base Homeostasis: Dr. Abeer Khurshidسلة فواكة100% (2)
- How To Interpret Arterial Blood Gas ResultsDocument9 pagesHow To Interpret Arterial Blood Gas ResultsteleasadgramNo ratings yet
- Acid Base BalanceDocument45 pagesAcid Base BalanceSameer Ul BashirNo ratings yet
- ABGs InterpretationDocument33 pagesABGs InterpretationHamza DossaNo ratings yet
- BiochemistryDocument33 pagesBiochemistryamhhospital0No ratings yet
- Acid BaseDocument33 pagesAcid BaseParvathy R NairNo ratings yet
- Overview of Acid-Base and Electrolyte Disorders: The Right Clinical Information, Right Where It's NeededDocument14 pagesOverview of Acid-Base and Electrolyte Disorders: The Right Clinical Information, Right Where It's NeededNelvinBaezMelendrezNo ratings yet
- Abg PPT NewDocument69 pagesAbg PPT NewMalaka Atapattu100% (3)
- Interpretation of Abgs: Sophie TatishviliDocument14 pagesInterpretation of Abgs: Sophie Tatishvilimashe1No ratings yet
- Asidosis Metabolik PDFDocument6 pagesAsidosis Metabolik PDFafifurrahman_rizalNo ratings yet
- Acid Base BalanceDocument11 pagesAcid Base BalancePrince Rener Velasco PeraNo ratings yet
- 66 Part 1Document10 pages66 Part 1Dinu Tiberiu GeorgeNo ratings yet
- Acid Base PhysiologyDocument4 pagesAcid Base PhysiologyGhadeer EbraheemNo ratings yet
- LRP CriticalCare Sample2Document46 pagesLRP CriticalCare Sample2Aniket ChoudharyNo ratings yet
- BSAVA - Interpretation of Arterial Blood Gas - VINDocument5 pagesBSAVA - Interpretation of Arterial Blood Gas - VINvetthamilNo ratings yet
- The Acid Base Balance: Faculty of Medicine Anesthesia and Intensive Care DepartmentDocument36 pagesThe Acid Base Balance: Faculty of Medicine Anesthesia and Intensive Care DepartmentCamelia A. ParuschiNo ratings yet
- Acid BaseDocument28 pagesAcid BaseSamantha DeshapriyaNo ratings yet
- Approach To The Adult With Metabolic AcidosisDocument20 pagesApproach To The Adult With Metabolic AcidosisTessa AcostaNo ratings yet
- 11-Acid-Base BalanceDocument28 pages11-Acid-Base BalanceKathlene BarasiNo ratings yet
- DECIPHER THE NUMBERS ABGsDocument8 pagesDECIPHER THE NUMBERS ABGsBeatrice Joy TombocNo ratings yet
- Acid Base BalanceDocument40 pagesAcid Base Balancemohdmaghyreh100% (1)
- Monitoring and Intervention for the Critically Ill Small Animal: The Rule of 20From EverandMonitoring and Intervention for the Critically Ill Small Animal: The Rule of 20No ratings yet
- Vertigo UndipDocument45 pagesVertigo UndipRiska PashaNo ratings yet
- Konsensus Nyeri NeuropatikDocument34 pagesKonsensus Nyeri NeuropatikRiska Pasha100% (1)
- Demensia PerdossiDocument20 pagesDemensia PerdossiRiska PashaNo ratings yet
- Acute Otitis MediaDocument3 pagesAcute Otitis MediaRiska PashaNo ratings yet
- Panduan ISPA AnakDocument39 pagesPanduan ISPA AnakRiska PashaNo ratings yet
- Ge&$E $&G&: (FelcananDocument30 pagesGe&$E $&G&: (FelcananRiska PashaNo ratings yet
- Suplementasi BesiDocument6 pagesSuplementasi BesiRiska PashaNo ratings yet
- Buku Ajar DiareDocument77 pagesBuku Ajar DiareRiska PashaNo ratings yet
- Konsensus Kejang DemamDocument10 pagesKonsensus Kejang DemamRiska PashaNo ratings yet
- A Parent's Guide To Understanding Tonsils and StrepDocument3 pagesA Parent's Guide To Understanding Tonsils and StrepRiska PashaNo ratings yet
- Guidelines For Preventing HealthDocument77 pagesGuidelines For Preventing HealthRiska PashaNo ratings yet
- Streptococcus Pyogenes and Streptococcal Disease (Page 1) : © Kenneth Todar, PHDDocument16 pagesStreptococcus Pyogenes and Streptococcal Disease (Page 1) : © Kenneth Todar, PHDRiska PashaNo ratings yet
- Acute Exudative TonsillitisDocument4 pagesAcute Exudative TonsillitisRiska PashaNo ratings yet
- Vasopressors and Inotropes in ShockDocument8 pagesVasopressors and Inotropes in ShockRiska PashaNo ratings yet
- Does Your Company Need More Umami? Sign of The TimesDocument6 pagesDoes Your Company Need More Umami? Sign of The TimesRiska PashaNo ratings yet
- Hearing Aid: Cleanup Quality StandardsDocument21 pagesHearing Aid: Cleanup Quality StandardsRiska PashaNo ratings yet
- Chapter - 1: Ayurvedic Subhasitas in Sanskrit Literature, Is A New Field inDocument46 pagesChapter - 1: Ayurvedic Subhasitas in Sanskrit Literature, Is A New Field inIniNo ratings yet
- Public Health FishboneDocument2 pagesPublic Health Fishbonepatima_sv4875No ratings yet
- Bed Site Teaching: Ridwan Permana (712014027) Preceptor: Dr. Rizal Daulay, SP - OT.,MARSDocument21 pagesBed Site Teaching: Ridwan Permana (712014027) Preceptor: Dr. Rizal Daulay, SP - OT.,MARSRidwan PermanaNo ratings yet
- 2021 American College of Rheumatology Vasculitis FoundationDocument10 pages2021 American College of Rheumatology Vasculitis FoundationVerónica Duménez JofréNo ratings yet
- Albendazole 400mg (Eskazole)Document8 pagesAlbendazole 400mg (Eskazole)asdwasdNo ratings yet
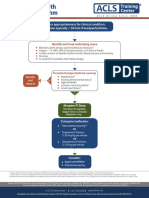
- Assess Appropriateness For Clinical Condition. Heart Rate Typically 50/min If BradyarrhythmiaDocument1 pageAssess Appropriateness For Clinical Condition. Heart Rate Typically 50/min If BradyarrhythmiaatikaNo ratings yet
- DHIS Secondary Health Facility Monthly Report FormDocument4 pagesDHIS Secondary Health Facility Monthly Report FormBd Db50% (2)
- Overview On Diabetic AcidosisDocument11 pagesOverview On Diabetic AcidosisIkraam Abdul LatifNo ratings yet
- Granulomatous InflammationDocument96 pagesGranulomatous InflammationIvonne Trujillo TorbiscoNo ratings yet
- Utah Medical Cannabis ActDocument28 pagesUtah Medical Cannabis ActLarryDCurtisNo ratings yet
- TGS2 Bahasa Inggris Putri MelaniDocument3 pagesTGS2 Bahasa Inggris Putri MelaniRozaq Permana YudhaNo ratings yet
- Cough and Common Cold Case PresentationDocument5 pagesCough and Common Cold Case Presentationismael al karkosh100% (1)
- ACUSON X300™ Ultrasound System: TransducersDocument7 pagesACUSON X300™ Ultrasound System: TransducersFirNo ratings yet
- OB-GYN Soap NoteDocument9 pagesOB-GYN Soap Notealex MusingilaNo ratings yet
- Bear Cub 750 - Quick User GuideDocument2 pagesBear Cub 750 - Quick User GuideSn DayanidhiNo ratings yet
- NWCP 2024 With LinkDocument5 pagesNWCP 2024 With LinkArijit DasNo ratings yet
- 25 Years Service Report - FinalDocument8 pages25 Years Service Report - Finalpramod454992No ratings yet
- Artikel Bu RashnahDocument7 pagesArtikel Bu RashnahSitti Rosdiana YahyaNo ratings yet
- Prophasedx Laboratory Phone: (855) 982-1100Document2 pagesProphasedx Laboratory Phone: (855) 982-1100ommanon15 aNo ratings yet
- Neonatal JaundiceDocument3 pagesNeonatal JaundicePerry BearNo ratings yet
- V60 For Invasive VentilationDocument13 pagesV60 For Invasive Ventilationsam samiNo ratings yet
- Module 1 - IS-PEFRDocument7 pagesModule 1 - IS-PEFRRenea Joy ArruejoNo ratings yet
- Laporan Faal RespirasiDocument18 pagesLaporan Faal RespirasiLatifah RBNo ratings yet
- Levels of PreventionDocument12 pagesLevels of PreventionRuth EkanemNo ratings yet
- NCP FAQsDocument16 pagesNCP FAQsEl Avion NoelNo ratings yet
- Animal Health Registered Technician in Los Angeles CA Resume Ivette NazarioDocument2 pagesAnimal Health Registered Technician in Los Angeles CA Resume Ivette NazarioIvetteNazarioNo ratings yet
- 473 eDocument9 pages473 eAzmi FarhadiNo ratings yet
- Evidence Based Implementation: Presented By: Ku Badlisyah Ku Aziz Lily Fairuz Md. YasanDocument21 pagesEvidence Based Implementation: Presented By: Ku Badlisyah Ku Aziz Lily Fairuz Md. YasanKu Badlisyah Ku AzizNo ratings yet
- By Speed Post / Email / FAX R.No.115552/El /S4 /2017: AssistantDocument5 pagesBy Speed Post / Email / FAX R.No.115552/El /S4 /2017: AssistantPreethi selvanesanNo ratings yet