Professional Documents
Culture Documents
Acute Post-Op Pain Management
Acute Post-Op Pain Management
Uploaded by
1234chocoCopyright:
Available Formats
You might also like
- Language of PreventionDocument9 pagesLanguage of Prevention1234chocoNo ratings yet
- Ethical AnalysisDocument5 pagesEthical Analysisapi-521003884100% (1)
- (DR Marilyn Ray) Transcultural Caring The Dynamic (BookFi)Document345 pages(DR Marilyn Ray) Transcultural Caring The Dynamic (BookFi)dian nofitaNo ratings yet
- Aldrete'sDocument1 pageAldrete'sKarlston LapnitenNo ratings yet
- HRPB Drug Formulary 2018Document244 pagesHRPB Drug Formulary 2018tiuwangNo ratings yet
- Blood Pressure Medication ChartDocument1 pageBlood Pressure Medication CharttmleNo ratings yet
- Doctor Talk: Communication Practice Role PlaysDocument6 pagesDoctor Talk: Communication Practice Role Plays1234chocoNo ratings yet
- Standard Treatment GuidelinesDocument5 pagesStandard Treatment Guidelinesbournvilleeater100% (1)
- Intravenous FluidsDocument3 pagesIntravenous FluidsKristine Artes AguilarNo ratings yet
- Standard Treatment WorkflowsDocument75 pagesStandard Treatment WorkflowsIndranil DuttaNo ratings yet
- Intravenous Fluid Therapy - Knowledge For Medical Students and PhysiciansDocument6 pagesIntravenous Fluid Therapy - Knowledge For Medical Students and PhysiciansNafiul IslamNo ratings yet
- Maged 2015Document185 pagesMaged 2015engy6nagyNo ratings yet
- 2020 Intravenous Fuid TherapyDocument19 pages2020 Intravenous Fuid TherapyDaniela MéndezNo ratings yet
- HF MsdsDocument8 pagesHF Msdsduccanh179No ratings yet
- Prescribing Medicine in Pregnancy, by Australian Drug Evaluation CommitteeDocument90 pagesPrescribing Medicine in Pregnancy, by Australian Drug Evaluation Committee徐承恩100% (1)
- Hydrofluoric Acid: Chemical Safety InformationDocument5 pagesHydrofluoric Acid: Chemical Safety InformationAditya GannamarajuNo ratings yet
- IPHS Guidelines Health Centres PDFDocument92 pagesIPHS Guidelines Health Centres PDFAnuradha YadavNo ratings yet
- Managing Psychiatric Patients in The EDDocument28 pagesManaging Psychiatric Patients in The EDfadiNo ratings yet
- Pain Management in Infants - Children - AdolescentsDocument9 pagesPain Management in Infants - Children - AdolescentsOxana Turcu100% (1)
- 406 - Respiratory Therapy Consult Service HandbookDocument28 pages406 - Respiratory Therapy Consult Service HandbookIkhsan JohnsonNo ratings yet
- Peripheral Artery Occlusive Disease: What To Do About Intermittent Claudication??Document46 pagesPeripheral Artery Occlusive Disease: What To Do About Intermittent Claudication??Dzariyat_Azhar_9277100% (1)
- Principles of Fluid ManagementDocument17 pagesPrinciples of Fluid ManagementBrainy-Paykiesaurus LuminirexNo ratings yet
- The Asi Text Book of SurgeryDocument1 pageThe Asi Text Book of SurgeryAnonymous hkWIKjoXFVNo ratings yet
- Intramuscular Injection TechniquesJOURNALDocument11 pagesIntramuscular Injection TechniquesJOURNALHida Tri NurrochmahNo ratings yet
- A Practical Physiotherapy Approach in Intensive Care Unit: April 2019Document12 pagesA Practical Physiotherapy Approach in Intensive Care Unit: April 2019NSSNS BALAJINo ratings yet
- APLS Aide MemoireDocument2 pagesAPLS Aide Memoirecolinj100% (1)
- Practice Standards For The Emergency Nurse Specialist. CENA, 2014Document16 pagesPractice Standards For The Emergency Nurse Specialist. CENA, 2014Cristobal Alejandro Falado SantanderNo ratings yet
- Mild Pain Treatment Algorithm: Pain Scale Rating 1/5 (0-5 Scale) or 1-3/10 (0-10 Scale)Document4 pagesMild Pain Treatment Algorithm: Pain Scale Rating 1/5 (0-5 Scale) or 1-3/10 (0-10 Scale)VickyNo ratings yet
- Seminar On Hemodynamic Monitoring: BY UMA Iind Year MSC NursingDocument52 pagesSeminar On Hemodynamic Monitoring: BY UMA Iind Year MSC NursingAyen AlingNo ratings yet
- Abbreviations ListDocument6 pagesAbbreviations ListolivedaisychainNo ratings yet
- Adrenergic Receptor ChartDocument1 pageAdrenergic Receptor Chartsas345sas345No ratings yet
- Clinical Scenario: Diagnosis ???Document17 pagesClinical Scenario: Diagnosis ???sreejaNo ratings yet
- Hypertension Treatment Steps For HypertensionDocument15 pagesHypertension Treatment Steps For Hypertensionfreelancer08100% (1)
- Medication: Captopril (Capoten) Is An ACE Inhibitor and A Common Antihypertensive. Captopril Generic Name Contents (Hide)Document43 pagesMedication: Captopril (Capoten) Is An ACE Inhibitor and A Common Antihypertensive. Captopril Generic Name Contents (Hide)Kath Rubio0% (1)
- Makalah HypertensionDocument6 pagesMakalah HypertensionFatin ZafirahNo ratings yet
- DEPRESSIONDocument19 pagesDEPRESSIONhazrul100% (1)
- Muuuna Assingment PDFDocument4 pagesMuuuna Assingment PDFAbdiNo ratings yet
- Quality of CPRDocument47 pagesQuality of CPRSreekrishnan TrikkurNo ratings yet
- Seborrheic Dermatitis in Adolescents and AdultsDocument51 pagesSeborrheic Dermatitis in Adolescents and AdultsCosmina GeorgianaNo ratings yet
- Physiology of Acid Base Balance by Dr. ROOMIDocument70 pagesPhysiology of Acid Base Balance by Dr. ROOMIMudassar Roomi100% (1)
- CPRDocument53 pagesCPRasutoshNo ratings yet
- Amlodipine - Drug Information - UpToDateDocument9 pagesAmlodipine - Drug Information - UpToDateBárbaraNo ratings yet
- Pre Anaesthetic MedicationDocument9 pagesPre Anaesthetic MedicationLorisna Hardiknastia Damastiwi100% (1)
- Advanced Airway Care: Intensive Care Unit PerspectiveDocument42 pagesAdvanced Airway Care: Intensive Care Unit PerspectiveJeffery Samuel100% (1)
- Biostatistics Community Medicine Gomal Medical College NotesDocument22 pagesBiostatistics Community Medicine Gomal Medical College Notesjay_p_shah0% (1)
- Malaysia's National Essential Drug List 3rd Ed.Document10 pagesMalaysia's National Essential Drug List 3rd Ed.afiq83No ratings yet
- KegawatdaruratanDocument164 pagesKegawatdaruratanmeida astriani gozaziNo ratings yet
- Basic ECG For BeginnersDocument109 pagesBasic ECG For BeginnersEmad Elhussein100% (1)
- Pharmacology of Drugs For PPHDocument55 pagesPharmacology of Drugs For PPHFaye CagayanNo ratings yet
- Hepatic-Trauma-Operative Management of Liver TraumaDocument23 pagesHepatic-Trauma-Operative Management of Liver TraumaSaif RahmanNo ratings yet
- Protocol On Transcutaneous PacingDocument7 pagesProtocol On Transcutaneous PacingAnusha VergheseNo ratings yet
- Application For Employment: Personal InformationDocument1 pageApplication For Employment: Personal InformationDavid Garcia100% (1)
- Clinical Knowledge Summaries (CKS) Depression: Managing Antidepressants For Depression in Primary CareDocument22 pagesClinical Knowledge Summaries (CKS) Depression: Managing Antidepressants For Depression in Primary Careece142No ratings yet
- High Altitude IllnessDocument9 pagesHigh Altitude Illnesswana_iswaraNo ratings yet
- Jo Jo Deese So So Rogi - Giani Sant Singh Ji MaskeenDocument65 pagesJo Jo Deese So So Rogi - Giani Sant Singh Ji MaskeenPaul SonNo ratings yet
- Creamer Et Al-2016-British Journal of DermatologyDocument34 pagesCreamer Et Al-2016-British Journal of DermatologyAtika Indah SariNo ratings yet
- Infective Diseases of Heart: Wella KarolinaDocument47 pagesInfective Diseases of Heart: Wella KarolinahayosiapaNo ratings yet
- Esi (1Document114 pagesEsi (1Ferina Mega SilviaNo ratings yet
- Oral Anticoagulants and Antiplatelet Drugs: Treatment With Blood ThinnersDocument8 pagesOral Anticoagulants and Antiplatelet Drugs: Treatment With Blood Thinnershussain AltaherNo ratings yet
- Aseptic Wound Dressing Edited 3 Dec 2008Document11 pagesAseptic Wound Dressing Edited 3 Dec 2008zahisma89No ratings yet
- Night Sweats, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandNight Sweats, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Acute Pain Management in Patients With Opioid ToleranceDocument6 pagesAcute Pain Management in Patients With Opioid ToleranceHendrikus Surya Adhi PutraNo ratings yet
- Pemantauan Dan Penanganan Nyeri Pasca BedahDocument42 pagesPemantauan Dan Penanganan Nyeri Pasca BedahAkbar Muitan LantauNo ratings yet
- Blue BirdDocument7 pagesBlue Bird1234chocoNo ratings yet
- Mbs Quick Guide: JULY 2020Document2 pagesMbs Quick Guide: JULY 20201234chocoNo ratings yet
- Code Geass - StoriesDocument5 pagesCode Geass - Stories1234chocoNo ratings yet
- Fairy Tail - Main ThemeDocument3 pagesFairy Tail - Main Theme1234chocoNo ratings yet
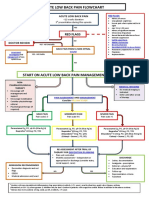
- Acute Low Back Pain Flowchart January 2017Document1 pageAcute Low Back Pain Flowchart January 20171234chocoNo ratings yet
- Topical Steroids (Sep 19) PDFDocument7 pagesTopical Steroids (Sep 19) PDF1234chocoNo ratings yet
- Taking A Social and Cultural HistoryDocument3 pagesTaking A Social and Cultural History1234chocoNo ratings yet
- PBM Module1 MTP Template 0Document2 pagesPBM Module1 MTP Template 01234chocoNo ratings yet
- Managing Mental Illness in Patients From CALD Backgrounds: PsychiatryDocument5 pagesManaging Mental Illness in Patients From CALD Backgrounds: Psychiatry1234chocoNo ratings yet
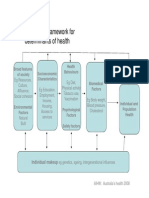
- A Conceptual Framework For HealthDocument1 pageA Conceptual Framework For Health1234chocoNo ratings yet
- Blue Card Declaration PDFDocument1 pageBlue Card Declaration PDF1234chocoNo ratings yet
- Prenatal Screening Test (AUS) PDFDocument24 pagesPrenatal Screening Test (AUS) PDFshirley_ling_15No ratings yet
- Preoperative AssessmentDocument9 pagesPreoperative Assessment1234chocoNo ratings yet
- Barrett's Esophagus: Identifying The Squamocolumnar (SC) and Gastroesophageal (GE) Junctions EndoscopicallyDocument10 pagesBarrett's Esophagus: Identifying The Squamocolumnar (SC) and Gastroesophageal (GE) Junctions Endoscopically1234chocoNo ratings yet
- What Is Critical AppraisalDocument8 pagesWhat Is Critical AppraisalFransisca StefanieNo ratings yet
- Terbinafin 1% Cream and Ketoconazole 2% PPT JURNAL KULITDocument18 pagesTerbinafin 1% Cream and Ketoconazole 2% PPT JURNAL KULITDeviNurfadilaFaniNo ratings yet
- Keep Healthy of Face: Rima Mulyaningtias Sela Maya Yulianti Feby Mileniawani Karina SuhermanDocument6 pagesKeep Healthy of Face: Rima Mulyaningtias Sela Maya Yulianti Feby Mileniawani Karina SuhermanFeby MileniawaniNo ratings yet
- Features of Covid Related StrokeDocument10 pagesFeatures of Covid Related StrokeAbdul AzeezNo ratings yet
- Topics For Reporting in NCM 116Document1 pageTopics For Reporting in NCM 116Sarmiento, Jovenal B.No ratings yet
- Risks Cost Benefits Ease of Implementation TotalDocument2 pagesRisks Cost Benefits Ease of Implementation Totalkent starkNo ratings yet
- Top 5 Nursing Values and How To Apply ThemDocument2 pagesTop 5 Nursing Values and How To Apply ThemCindy BelmesNo ratings yet
- Sale of Drugs Act 1952 (New)Document17 pagesSale of Drugs Act 1952 (New)Hassan KhamisNo ratings yet
- Jurnal Maternitas Ibu HamilDocument8 pagesJurnal Maternitas Ibu HamilriswandaNo ratings yet
- Prof C M K Reddy DSCDocument5 pagesProf C M K Reddy DSCrasikaaNo ratings yet
- Writing Topics For Pet-B1Document31 pagesWriting Topics For Pet-B1Ana100% (2)
- Local Budget Memorandum: Republic OF THE Philippines Department Budget AND ManageDocument7 pagesLocal Budget Memorandum: Republic OF THE Philippines Department Budget AND ManageGreggy Roy MarquezNo ratings yet
- Pollice Et Al 2008 Severe Tramadol Addiction in A 61 Year Old Woman Without A History of Substance AbuseDocument2 pagesPollice Et Al 2008 Severe Tramadol Addiction in A 61 Year Old Woman Without A History of Substance Abusefernyz2886No ratings yet
- For More Information, and To Download Other MaterialsDocument20 pagesFor More Information, and To Download Other Materialsanel vivianNo ratings yet
- Supervisi Perawat Primer Perawat Associate Dalam MDocument7 pagesSupervisi Perawat Primer Perawat Associate Dalam MFlorida BhokiNo ratings yet
- VegitermsgnDocument6 pagesVegitermsgnCherwinNo ratings yet
- Fluid Overload in Peritoneal Dialysis PatientsDocument11 pagesFluid Overload in Peritoneal Dialysis PatientsHaryonoNo ratings yet
- Gyne & Obes. Step.1st BitsDocument70 pagesGyne & Obes. Step.1st BitsSkyNo ratings yet
- ABDC Journal List 08022017Document232 pagesABDC Journal List 08022017PGNo ratings yet
- Information For Persons With HOSPITA SEMI-PRIVATE/PRIVATE Supplementary Hospitalisation Insurance.Document4 pagesInformation For Persons With HOSPITA SEMI-PRIVATE/PRIVATE Supplementary Hospitalisation Insurance.docas123No ratings yet
- DR ShankarDocument1 pageDR ShankarSudhanshu JuNo ratings yet
- Research ProposalDocument3 pagesResearch Proposalshivangi pushkarnaNo ratings yet
- Full Chapter Management of Oral Cancers Sudhir Bahadur PDFDocument39 pagesFull Chapter Management of Oral Cancers Sudhir Bahadur PDFjared.balderas413100% (7)
- Why I Want To Become A PhysiotherapistDocument8 pagesWhy I Want To Become A PhysiotherapistgggghcNo ratings yet
- AnorexiaDocument2 pagesAnorexiaMaria Virginia Diaz RomeroNo ratings yet
- Prof Ad With AnswersDocument8 pagesProf Ad With AnswersYuxin LiuNo ratings yet
- Emergency Care Algorithms For Rural Settings 2018 PDFDocument67 pagesEmergency Care Algorithms For Rural Settings 2018 PDFGbariel100% (1)
- Transtheoretical Theory Model - Prochaska - WikipediaDocument10 pagesTranstheoretical Theory Model - Prochaska - WikipediaAlbert Muya MurayaNo ratings yet
Acute Post-Op Pain Management
Acute Post-Op Pain Management
Uploaded by
1234chocoOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Acute Post-Op Pain Management
Acute Post-Op Pain Management
Uploaded by
1234chocoCopyright:
Available Formats
OKA5301 NPS APOP EVC.
qxd
16/2/07
3:13 PM
Page 1
Acute postoperative
pain management
Optimal postoperative pain management
begins in the preoperative period
Measure pain regularly using a validated
pain assessment tool
Pain is subjective and each individual patients experience of pain is different.
Reasons for these differences include:
Regular and routine assessment of pain will result in improved pain management.1
age
The patients own assessment of pain is the most reliable and should be used
when possible.1
co-morbidities including chronic pain
Use a pain measurement tool appropriate to patients mental status, age and language.
concurrent medication and other substance intake
Measure pain scores both at rest and on movement/function to assess the impact
on functional activity.13
mechanisms of pain nociceptive, neuropathic
Re-assess pain regularly and before/after administering analgesia or other pain
management strategies.
modifying factors e.g. mood, cognition, coping strategies
genetics.
Document pain assessment measurements as part of routine observations.
Conduct preoperative patient evaluation:
Validated pain assessment tools
Ask the patient and/or their carers to help establish pain history (consider the above).
Patient measures
Document in the patients medical record, otherwise state that there are
no relevant factors.
Visual analogue scale (VAS; figure 1).
Numerical rating scale (NRS; figure 2).
Discuss pain management strategies and expectations in the preoperative period.
Verbal descriptor scale e.g. none/mild/moderate/severe.
WongBaker faces scale (figure 3).
Observer measures
Behavioural pain scale.3
Fig 1: Visual analogue scale
Fig 2: Numerical rating scale
Fig 3: WongBaker faces scale
PAIN SCORE 0 10 NUMERICAL RATING
010 Numerical Rating Scale
No
Pain
Worst
Pain Ever
No
Pain
4
5
6
Moderate Pain
Worst
Possible
10 Pain
10
No Hurt
Hurts
Little Bit
Hurts
Little More
Hurts
Even More
Hurts
Whole Lot
Hurts
Worst
WongBaker FACES Pain Rating Scale, from Wong DL et al.: Whaley and
Wongs Essentials of Pediatric Nursing, 5th edition, St. Louis, 2001, Mosby, p. 1301.
http://www.mosbysdrugconsult.com/WOW/facesReproductions.html (accessed 31 January 2007).
APOP Project
OKA5301 NPS APOP EVC.qxd
16/2/07
3:13 PM
Page 2
Ensure all postoperative patients receive safe and effective analgesia
When prescribing analgesia
Routes of administration:
Use a variety of approaches (multimodal analgesia) to improve analgesia and decrease
doses of individual agents.4
Paracetamol and non-steroidal anti-inflammatory drugs (NSAIDs) are valuable components
of multimodal analgesia.1
Use intermittent intravenous (IV) opioids to gain initial control of severe pain,
as IV administration provides rapid and reliable drug absorption.1
(Note: prescription of nurse-administered IV opioids is not recommended for
ongoing analgesia on general wards.)
When using analgesics on a regular basis have additional prn medication available for
breakthrough pain.
Consider subcutaneous route for ongoing parenteral opioids, avoid intramuscular route
(painful and less predictable absorption).1
Use individualised doses of analgesic(s) administered at appropriate dose intervals and
titrate to patient response.4
Once the oral route has been established, use when possible.1
Drug class
Considerations
Selected precautions
Paracetamol
Useful adjunctive analgesic agent
Provide clear directions when prescribing >1 paracetamol-containing preparation
Consider regular order rather than prn
When combined with opioids, increases pain relief1
Maximum 4 g daily dose usually recommended in healthy adults;
reduce dose in malnourished, underweight patients
Regular (1 g every 46 hours) use can reduce opioid requirements by 2030%1
Avoid in severe liver dysfunction
Only prescribe IV (avoid rectal) if oral is inappropriate1
NSAIDs
(e.g. conventional: ibuprofen,
COX-2 selective: celecoxib)
Tramadol
Opioids
(e.g. morphine,
oxycodone, fentanyl, hydromorphone,
pethidine, dextropropoxyphene)
Adjunctive analgesics for use with opioids
and/or paracetamol1
Adverse effects of NSAIDs are significant; may limit use1
Inadequate for severe pain when given alone,
but can reduce opioid requirements1
Modify dose or avoid in congestive heart failure, those at risk of renal effects
(renal disease, hypovolaemia, hypotension, concurrent use of other nephrotoxic
agents), the elderly
Limit prescription to two to three days then review4
Lower risk of GI bleeding or ulcers with COX-2 selective NSAIDs1
Weak opioid with serotonergic and noradrenergic effects, as effective as morphine
for some types of moderate postoperative pain, less so for severe acute pain5
Avoid in patients with history of seizures
Less risk of respiratory depression and constipation1,5
Be aware of rare, but potentially serious, drug interactions with SSRIs, TCAs,
pethidine, warfarin, St Johns wort
Prescribe opioid dose based on age, use lower initial dose in the elderly
and titrate upwards5
Prescribing multiple opioids via multiple routes increases risk of opioid overdose
and is generally not recommended
Be aware of potential for prescribing and administration errors with immediate
and sustained-release preparations
Do not use morphine or pethidine in severe renal impairment5
Be aware of factors that may increase risk of opioid overdose (e.g. concurrent
sedatives, opioid nave, sepsis)
Use with caution in severe renal impairment and the elderly
Avoid pethidine (accumulation of toxic metabolite norpethidine, drug interactions)
and dextropropoxyphene (unsafe in overdose, ceiling effect)
Abbreviations: ACEI = angiotensin-converting enzyme inhibitors, NSAIDs = non-steroidal anti-inflammatory drugs, SSRIs = selective serotonin reuptake inhibitors, TCAs = tricyclic antidepressants.
OKA5301 NPS APOP EVC.qxd
16/2/07
3:13 PM
Page 3
Monitor and manage adverse events
Monitoring respiratory depression and sedation
(patients on opioids sedatives)
Respiratory rate alone as an indicator of respiratory depression is of limited value
and hypoxaemic episodes may occur in the absence of a reduced respiratory rate.1
Sedation scores are a more reliable indicator respiratory depression is almost always
preceded by sedation.6 The sedation score measures the patients level of wakefulness
and their ability to respond appropriately to verbal command. A four-point scale3
(box 1) is recommended.
Box 1: Sedation scoring
Sedation score
Suggested action
Awake, alert
Mild sedation
1S
Asleep
Moderate sedation, easy to rouse
but unable to stay awake
Monitoring nausea and vomiting
Easy to rouse
Effective antiemetics in the postoperative period include 5HT3 antagonists, droperidol
and dexamethasone.4
Consider co-prescribing more than one antiemetic, each with a different mechanism
of action, with instructions to add a drug from a different class if the first agent is
ineffective.7
Monitoring for other adverse events
Regular review will reduce the risk of serious side effects developing and will allow
for adjustment of doses, dosage interval and alteration of analgesics as necessary.
Side effects for the following include:
Continue routine monitoring
Consider reducing analgesic dose,
increase frequency of monitoring
If respiratory rate < 8 breaths per minute,
withhold opioid, administer naloxone
and notify medical officer
Difficult to rouse, unable to stay awake
Withhold opioid, administer naloxone
and notify medical officer
Note that naloxone should be administered
IV in divided doses of not greater than
100 micrograms
Opioids constipation (consider prescribing of prophylactic laxatives),
urinary retention, itch, confusion and postural hypotension.
NSAIDs GI (peptic ulceration), renal (monitor renal function e.g. in renally impaired
patients, and those being treated with ACEIs, diuretics and aminoglycoside antibiotics),
bronchospasm, platelet inhibition (increased blood loss).1 Risk and severity of side effects
is generally increased in the elderly.1
APOP Project
OKA5301 NPS APOP EVC.qxd
16/2/07
3:13 PM
Page 4
Communicate ongoing pain management plan to both patients
and primary healthcare professionals at discharge
There is evidence of gaps in discharge planning leading to significant harm.8
A pain management plan, as a component of discharge planning, should be clearly
communicated to the patient and/or their carer, general practitioner and other communitybased health professionals.
Management action:
A pain management plan is essential for patients at increased risk of pain after discharge
(see below). This is likely to improve the patients post-discharge pain experience, utilisation
of outpatient services and prevent surgical complications.9
Prescribe drugs for symptomatic relief of side effects where necessary
(e.g. antiemetics and laxatives).
Review analgesia requirements and consider relevant risk factors 24 hours
before discharge.
If prescribing a strong opioid, consider limiting quantity prescribed.
Pain management plan8 at discharge includes:
Factors associated with increased risk of pain and/or complexity of analgesic
requirements post-discharge*:
Patient characteristics5 age, debilitated, cognitive impairment, severe liver disease, renal
impairment, peptic ulcer disease, chronic pain or low pain threshold, multiple admissions
for pain, obstetric patients.
Surgery types1 thoracic, abdominal surgery, surgery involving major disruption of
muscle, bone or nervous tissue, bone grafts.
Concurrent medicines5 opioid antagonists, chronic opioids, SSRIs, monoamine oxidase
inhibitors, central nervous system depressants, warfarin, St Johns wort, ACEIs, diuretics.
*Consult Acute Pain Service or Pain Specialist where necessary (if available).
A list of all analgesics, with dosage and administration times.
Instructions on anticipated/intended duration of therapy and reducing/ceasing therapy
where appropriate.
Important consumer-specific medicines information (e.g. adverse reactions including
allergies, drug interactions, ceased medicines).
For paracetamol-containing analgesics, give (written) information about safe use,
including maximum daily dose of paracetamol.
Instructions for monitoring and managing side effects.5
Methods to improve function while recovering including non-pharmacological methods
for relieving pain.
Contact person for pain problems (uncontrolled or persistent pain) and other
postoperative concerns (e.g. bleeding and infections).
References:
1.
Australian and New Zealand College of Anaesthetists (ANZCA).
Acute pain management: Scientific evidence, 2nd edition. ANZCA, 2005.
http://www.anzca.edu.au/publications/acutepain.htm (accessed 31 January 2007).
3.
Acute pain management performance toolkit. Melbourne: Victorian Quality Council, 2007.
http://www.health.vic.gov.au/qualitycouncil/activities/acute.htm
(accessed 31 January 2007)
2.
Clinical practice guideline for the management of postoperative pain. Version 1.2.
Washington, DC: Department of Defense, Veterans Health Administration, 2002.
http://www.guideline.gov/summary/summary.aspx?doc_id=3284
(accessed 31 January 2007).
4.
Therapeutic Guidelines: Analgesic, Version 4. 2002.
5.
Australian Medicines Handbook, 2007.
6.
Macintyre PE, Schug SA. Acute Pain ManagementA Practical Guide, 3rd edition, 2007
(in press).
7.
Habib AS, Gan TJ. Evidence-based management of postoperative nausea and vomiting:
a review. Can J Anaesth 2004;51:32641.
8.
Australian Pharmaceutical Advisory Council. Guiding principles to achieve continuity
in medication management. Canberra: Department of Health and Ageing, 2005.
http://www.health.gov.au/internet/wcms/publishing.nsf/Content/nmp-guiding
(accessed 31 January 2007)
9.
Kable A, Gibberd R, Spigelman A. Complications after discharge for surgical patients.
ANZ J Surg 2004;74:9297.
Drug Use Evaluation project conducted by the APOP study group: Victorian Department of Human Services/Victorian Drug Usage Evaluation Group; UMORE, Tasmanian School of Pharmacy, University of Tasmania;
South Australian Therapeutic Advisory Group/Department of Health; School of Pharmacy, University of Queensland; New South Wales Therapeutic Advisory Group. Funded and supported by the National Prescribing Service Limited (02 8217 8700).
For more information on the management of postoperative pain refer to ANZCA Acute Pain Management: Scientific Evidence, 2nd edition, 2005, and Therapeutic Guidelines: Analgesic, Version 4, 2002.
The information contained in this material is derived from a critical analysis of a wide range of authoritative evidence. Any treatment decisions based on this information should be made in the context of the individual clinical
circumstances of each patient. Reviewed by: Dr C Roger Goucke, Dr Jane Trinca, Dr Pamela E Macintyre, Professor Stephan A Schug, Faculty of Pain Medicine, Australian and New Zealand College of Anaesthetists.
February 2007
NPSE0396_FEB_2007
You might also like
- Language of PreventionDocument9 pagesLanguage of Prevention1234chocoNo ratings yet
- Ethical AnalysisDocument5 pagesEthical Analysisapi-521003884100% (1)
- (DR Marilyn Ray) Transcultural Caring The Dynamic (BookFi)Document345 pages(DR Marilyn Ray) Transcultural Caring The Dynamic (BookFi)dian nofitaNo ratings yet
- Aldrete'sDocument1 pageAldrete'sKarlston LapnitenNo ratings yet
- HRPB Drug Formulary 2018Document244 pagesHRPB Drug Formulary 2018tiuwangNo ratings yet
- Blood Pressure Medication ChartDocument1 pageBlood Pressure Medication CharttmleNo ratings yet
- Doctor Talk: Communication Practice Role PlaysDocument6 pagesDoctor Talk: Communication Practice Role Plays1234chocoNo ratings yet
- Standard Treatment GuidelinesDocument5 pagesStandard Treatment Guidelinesbournvilleeater100% (1)
- Intravenous FluidsDocument3 pagesIntravenous FluidsKristine Artes AguilarNo ratings yet
- Standard Treatment WorkflowsDocument75 pagesStandard Treatment WorkflowsIndranil DuttaNo ratings yet
- Intravenous Fluid Therapy - Knowledge For Medical Students and PhysiciansDocument6 pagesIntravenous Fluid Therapy - Knowledge For Medical Students and PhysiciansNafiul IslamNo ratings yet
- Maged 2015Document185 pagesMaged 2015engy6nagyNo ratings yet
- 2020 Intravenous Fuid TherapyDocument19 pages2020 Intravenous Fuid TherapyDaniela MéndezNo ratings yet
- HF MsdsDocument8 pagesHF Msdsduccanh179No ratings yet
- Prescribing Medicine in Pregnancy, by Australian Drug Evaluation CommitteeDocument90 pagesPrescribing Medicine in Pregnancy, by Australian Drug Evaluation Committee徐承恩100% (1)
- Hydrofluoric Acid: Chemical Safety InformationDocument5 pagesHydrofluoric Acid: Chemical Safety InformationAditya GannamarajuNo ratings yet
- IPHS Guidelines Health Centres PDFDocument92 pagesIPHS Guidelines Health Centres PDFAnuradha YadavNo ratings yet
- Managing Psychiatric Patients in The EDDocument28 pagesManaging Psychiatric Patients in The EDfadiNo ratings yet
- Pain Management in Infants - Children - AdolescentsDocument9 pagesPain Management in Infants - Children - AdolescentsOxana Turcu100% (1)
- 406 - Respiratory Therapy Consult Service HandbookDocument28 pages406 - Respiratory Therapy Consult Service HandbookIkhsan JohnsonNo ratings yet
- Peripheral Artery Occlusive Disease: What To Do About Intermittent Claudication??Document46 pagesPeripheral Artery Occlusive Disease: What To Do About Intermittent Claudication??Dzariyat_Azhar_9277100% (1)
- Principles of Fluid ManagementDocument17 pagesPrinciples of Fluid ManagementBrainy-Paykiesaurus LuminirexNo ratings yet
- The Asi Text Book of SurgeryDocument1 pageThe Asi Text Book of SurgeryAnonymous hkWIKjoXFVNo ratings yet
- Intramuscular Injection TechniquesJOURNALDocument11 pagesIntramuscular Injection TechniquesJOURNALHida Tri NurrochmahNo ratings yet
- A Practical Physiotherapy Approach in Intensive Care Unit: April 2019Document12 pagesA Practical Physiotherapy Approach in Intensive Care Unit: April 2019NSSNS BALAJINo ratings yet
- APLS Aide MemoireDocument2 pagesAPLS Aide Memoirecolinj100% (1)
- Practice Standards For The Emergency Nurse Specialist. CENA, 2014Document16 pagesPractice Standards For The Emergency Nurse Specialist. CENA, 2014Cristobal Alejandro Falado SantanderNo ratings yet
- Mild Pain Treatment Algorithm: Pain Scale Rating 1/5 (0-5 Scale) or 1-3/10 (0-10 Scale)Document4 pagesMild Pain Treatment Algorithm: Pain Scale Rating 1/5 (0-5 Scale) or 1-3/10 (0-10 Scale)VickyNo ratings yet
- Seminar On Hemodynamic Monitoring: BY UMA Iind Year MSC NursingDocument52 pagesSeminar On Hemodynamic Monitoring: BY UMA Iind Year MSC NursingAyen AlingNo ratings yet
- Abbreviations ListDocument6 pagesAbbreviations ListolivedaisychainNo ratings yet
- Adrenergic Receptor ChartDocument1 pageAdrenergic Receptor Chartsas345sas345No ratings yet
- Clinical Scenario: Diagnosis ???Document17 pagesClinical Scenario: Diagnosis ???sreejaNo ratings yet
- Hypertension Treatment Steps For HypertensionDocument15 pagesHypertension Treatment Steps For Hypertensionfreelancer08100% (1)
- Medication: Captopril (Capoten) Is An ACE Inhibitor and A Common Antihypertensive. Captopril Generic Name Contents (Hide)Document43 pagesMedication: Captopril (Capoten) Is An ACE Inhibitor and A Common Antihypertensive. Captopril Generic Name Contents (Hide)Kath Rubio0% (1)
- Makalah HypertensionDocument6 pagesMakalah HypertensionFatin ZafirahNo ratings yet
- DEPRESSIONDocument19 pagesDEPRESSIONhazrul100% (1)
- Muuuna Assingment PDFDocument4 pagesMuuuna Assingment PDFAbdiNo ratings yet
- Quality of CPRDocument47 pagesQuality of CPRSreekrishnan TrikkurNo ratings yet
- Seborrheic Dermatitis in Adolescents and AdultsDocument51 pagesSeborrheic Dermatitis in Adolescents and AdultsCosmina GeorgianaNo ratings yet
- Physiology of Acid Base Balance by Dr. ROOMIDocument70 pagesPhysiology of Acid Base Balance by Dr. ROOMIMudassar Roomi100% (1)
- CPRDocument53 pagesCPRasutoshNo ratings yet
- Amlodipine - Drug Information - UpToDateDocument9 pagesAmlodipine - Drug Information - UpToDateBárbaraNo ratings yet
- Pre Anaesthetic MedicationDocument9 pagesPre Anaesthetic MedicationLorisna Hardiknastia Damastiwi100% (1)
- Advanced Airway Care: Intensive Care Unit PerspectiveDocument42 pagesAdvanced Airway Care: Intensive Care Unit PerspectiveJeffery Samuel100% (1)
- Biostatistics Community Medicine Gomal Medical College NotesDocument22 pagesBiostatistics Community Medicine Gomal Medical College Notesjay_p_shah0% (1)
- Malaysia's National Essential Drug List 3rd Ed.Document10 pagesMalaysia's National Essential Drug List 3rd Ed.afiq83No ratings yet
- KegawatdaruratanDocument164 pagesKegawatdaruratanmeida astriani gozaziNo ratings yet
- Basic ECG For BeginnersDocument109 pagesBasic ECG For BeginnersEmad Elhussein100% (1)
- Pharmacology of Drugs For PPHDocument55 pagesPharmacology of Drugs For PPHFaye CagayanNo ratings yet
- Hepatic-Trauma-Operative Management of Liver TraumaDocument23 pagesHepatic-Trauma-Operative Management of Liver TraumaSaif RahmanNo ratings yet
- Protocol On Transcutaneous PacingDocument7 pagesProtocol On Transcutaneous PacingAnusha VergheseNo ratings yet
- Application For Employment: Personal InformationDocument1 pageApplication For Employment: Personal InformationDavid Garcia100% (1)
- Clinical Knowledge Summaries (CKS) Depression: Managing Antidepressants For Depression in Primary CareDocument22 pagesClinical Knowledge Summaries (CKS) Depression: Managing Antidepressants For Depression in Primary Careece142No ratings yet
- High Altitude IllnessDocument9 pagesHigh Altitude Illnesswana_iswaraNo ratings yet
- Jo Jo Deese So So Rogi - Giani Sant Singh Ji MaskeenDocument65 pagesJo Jo Deese So So Rogi - Giani Sant Singh Ji MaskeenPaul SonNo ratings yet
- Creamer Et Al-2016-British Journal of DermatologyDocument34 pagesCreamer Et Al-2016-British Journal of DermatologyAtika Indah SariNo ratings yet
- Infective Diseases of Heart: Wella KarolinaDocument47 pagesInfective Diseases of Heart: Wella KarolinahayosiapaNo ratings yet
- Esi (1Document114 pagesEsi (1Ferina Mega SilviaNo ratings yet
- Oral Anticoagulants and Antiplatelet Drugs: Treatment With Blood ThinnersDocument8 pagesOral Anticoagulants and Antiplatelet Drugs: Treatment With Blood Thinnershussain AltaherNo ratings yet
- Aseptic Wound Dressing Edited 3 Dec 2008Document11 pagesAseptic Wound Dressing Edited 3 Dec 2008zahisma89No ratings yet
- Night Sweats, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandNight Sweats, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Acute Pain Management in Patients With Opioid ToleranceDocument6 pagesAcute Pain Management in Patients With Opioid ToleranceHendrikus Surya Adhi PutraNo ratings yet
- Pemantauan Dan Penanganan Nyeri Pasca BedahDocument42 pagesPemantauan Dan Penanganan Nyeri Pasca BedahAkbar Muitan LantauNo ratings yet
- Blue BirdDocument7 pagesBlue Bird1234chocoNo ratings yet
- Mbs Quick Guide: JULY 2020Document2 pagesMbs Quick Guide: JULY 20201234chocoNo ratings yet
- Code Geass - StoriesDocument5 pagesCode Geass - Stories1234chocoNo ratings yet
- Fairy Tail - Main ThemeDocument3 pagesFairy Tail - Main Theme1234chocoNo ratings yet
- Acute Low Back Pain Flowchart January 2017Document1 pageAcute Low Back Pain Flowchart January 20171234chocoNo ratings yet
- Topical Steroids (Sep 19) PDFDocument7 pagesTopical Steroids (Sep 19) PDF1234chocoNo ratings yet
- Taking A Social and Cultural HistoryDocument3 pagesTaking A Social and Cultural History1234chocoNo ratings yet
- PBM Module1 MTP Template 0Document2 pagesPBM Module1 MTP Template 01234chocoNo ratings yet
- Managing Mental Illness in Patients From CALD Backgrounds: PsychiatryDocument5 pagesManaging Mental Illness in Patients From CALD Backgrounds: Psychiatry1234chocoNo ratings yet
- A Conceptual Framework For HealthDocument1 pageA Conceptual Framework For Health1234chocoNo ratings yet
- Blue Card Declaration PDFDocument1 pageBlue Card Declaration PDF1234chocoNo ratings yet
- Prenatal Screening Test (AUS) PDFDocument24 pagesPrenatal Screening Test (AUS) PDFshirley_ling_15No ratings yet
- Preoperative AssessmentDocument9 pagesPreoperative Assessment1234chocoNo ratings yet
- Barrett's Esophagus: Identifying The Squamocolumnar (SC) and Gastroesophageal (GE) Junctions EndoscopicallyDocument10 pagesBarrett's Esophagus: Identifying The Squamocolumnar (SC) and Gastroesophageal (GE) Junctions Endoscopically1234chocoNo ratings yet
- What Is Critical AppraisalDocument8 pagesWhat Is Critical AppraisalFransisca StefanieNo ratings yet
- Terbinafin 1% Cream and Ketoconazole 2% PPT JURNAL KULITDocument18 pagesTerbinafin 1% Cream and Ketoconazole 2% PPT JURNAL KULITDeviNurfadilaFaniNo ratings yet
- Keep Healthy of Face: Rima Mulyaningtias Sela Maya Yulianti Feby Mileniawani Karina SuhermanDocument6 pagesKeep Healthy of Face: Rima Mulyaningtias Sela Maya Yulianti Feby Mileniawani Karina SuhermanFeby MileniawaniNo ratings yet
- Features of Covid Related StrokeDocument10 pagesFeatures of Covid Related StrokeAbdul AzeezNo ratings yet
- Topics For Reporting in NCM 116Document1 pageTopics For Reporting in NCM 116Sarmiento, Jovenal B.No ratings yet
- Risks Cost Benefits Ease of Implementation TotalDocument2 pagesRisks Cost Benefits Ease of Implementation Totalkent starkNo ratings yet
- Top 5 Nursing Values and How To Apply ThemDocument2 pagesTop 5 Nursing Values and How To Apply ThemCindy BelmesNo ratings yet
- Sale of Drugs Act 1952 (New)Document17 pagesSale of Drugs Act 1952 (New)Hassan KhamisNo ratings yet
- Jurnal Maternitas Ibu HamilDocument8 pagesJurnal Maternitas Ibu HamilriswandaNo ratings yet
- Prof C M K Reddy DSCDocument5 pagesProf C M K Reddy DSCrasikaaNo ratings yet
- Writing Topics For Pet-B1Document31 pagesWriting Topics For Pet-B1Ana100% (2)
- Local Budget Memorandum: Republic OF THE Philippines Department Budget AND ManageDocument7 pagesLocal Budget Memorandum: Republic OF THE Philippines Department Budget AND ManageGreggy Roy MarquezNo ratings yet
- Pollice Et Al 2008 Severe Tramadol Addiction in A 61 Year Old Woman Without A History of Substance AbuseDocument2 pagesPollice Et Al 2008 Severe Tramadol Addiction in A 61 Year Old Woman Without A History of Substance Abusefernyz2886No ratings yet
- For More Information, and To Download Other MaterialsDocument20 pagesFor More Information, and To Download Other Materialsanel vivianNo ratings yet
- Supervisi Perawat Primer Perawat Associate Dalam MDocument7 pagesSupervisi Perawat Primer Perawat Associate Dalam MFlorida BhokiNo ratings yet
- VegitermsgnDocument6 pagesVegitermsgnCherwinNo ratings yet
- Fluid Overload in Peritoneal Dialysis PatientsDocument11 pagesFluid Overload in Peritoneal Dialysis PatientsHaryonoNo ratings yet
- Gyne & Obes. Step.1st BitsDocument70 pagesGyne & Obes. Step.1st BitsSkyNo ratings yet
- ABDC Journal List 08022017Document232 pagesABDC Journal List 08022017PGNo ratings yet
- Information For Persons With HOSPITA SEMI-PRIVATE/PRIVATE Supplementary Hospitalisation Insurance.Document4 pagesInformation For Persons With HOSPITA SEMI-PRIVATE/PRIVATE Supplementary Hospitalisation Insurance.docas123No ratings yet
- DR ShankarDocument1 pageDR ShankarSudhanshu JuNo ratings yet
- Research ProposalDocument3 pagesResearch Proposalshivangi pushkarnaNo ratings yet
- Full Chapter Management of Oral Cancers Sudhir Bahadur PDFDocument39 pagesFull Chapter Management of Oral Cancers Sudhir Bahadur PDFjared.balderas413100% (7)
- Why I Want To Become A PhysiotherapistDocument8 pagesWhy I Want To Become A PhysiotherapistgggghcNo ratings yet
- AnorexiaDocument2 pagesAnorexiaMaria Virginia Diaz RomeroNo ratings yet
- Prof Ad With AnswersDocument8 pagesProf Ad With AnswersYuxin LiuNo ratings yet
- Emergency Care Algorithms For Rural Settings 2018 PDFDocument67 pagesEmergency Care Algorithms For Rural Settings 2018 PDFGbariel100% (1)
- Transtheoretical Theory Model - Prochaska - WikipediaDocument10 pagesTranstheoretical Theory Model - Prochaska - WikipediaAlbert Muya MurayaNo ratings yet