Professional Documents
Culture Documents
First Branchial Cleft Anomalies Otologic Manifestations and Treatment Outcomes
First Branchial Cleft Anomalies Otologic Manifestations and Treatment Outcomes
Uploaded by
adriricaldeOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
First Branchial Cleft Anomalies Otologic Manifestations and Treatment Outcomes
First Branchial Cleft Anomalies Otologic Manifestations and Treatment Outcomes
Uploaded by
adriricaldeCopyright:
Available Formats
Original ResearchOtology and Neurotology
First Branchial Cleft Anomalies: Otologic
Manifestations and Treatment Outcomes
Justin R. Shinn1, Patricia L. Purcell, MD1, David L. Horn, MD1,2,
Kathleen C. Y. Sie, MD1,2, and Scott C. Manning, MD1,2
Sponsorships or competing interests that may be relevant to content are disclosed at the end of this article.
Abstract
Objective. This study describes the presentation of first branchial cleft anomalies and compares outcomes of first branchial cleft with other branchial cleft anomalies with
attention to otologic findings.
Study Design. Case series with chart review.
Setting. Pediatric tertiary care facility.
Methods. Surgical databases were queried to identify children
with branchial cleft anomalies. Descriptive analysis defined
sample characteristics. Risk estimates were calculated using
Fishers exact test.
Results. Queries identified 126 subjects: 27 (21.4%) had
first branchial cleft anomalies, 80 (63.4%) had second, and
19 (15.1%) had third or fourth. Children with first anomalies often presented with otologic complications, including
otorrhea (22.2%), otitis media (25.9%), and cholesteatoma
(14.8%). Of 80 children with second branchial cleft
anomalies, only 3 (3.8%) had otitis. Compared with children with second anomalies, children with first anomalies
had a greater risk of requiring primary incision and drainage: 16 (59.3%) vs 2 (2.5%) (relative risk [RR], 3.5; 95%
confidence interval [CI], 2.4-5; P \ .0001). They were
more likely to have persistent disease after primary excision: 7 (25.9%) vs 2 (2.5%) (RR, 3; 95% CI, 1.9-5; P =
.0025). They were more likely to undergo additional surgery: 8 (29.6%) vs 3 (11.1%) (RR, 2.9; 95% CI, 1.8-4.7; P =
.0025). Of 7 persistent first anomalies, 6 (85.7%) were
medial to the facial nerve, and 4 (57.1%) required earspecific surgery for management.
Otolaryngology
Head and Neck Surgery
2015, Vol. 152(3) 506512
American Academy of
OtolaryngologyHead and Neck
Surgery Foundation 2014
Reprints and permission:
sagepub.com/journalsPermissions.nav
DOI: 10.1177/0194599814562773
http://otojournal.org
Received August 22, 2014; revised November 10, 2014; accepted
November 14, 2014.
ranchial cleft anomalies (BCAs) are the second most
common type of congenital neck mass after thyroglossal duct cyst.1 Branchial cleft anomalies can
result from duplication of the first branchial cleft, or ear
canal, or from failure of fusion of the second, third, or fourth
branchial arches.2 Most anomalies occur as second branchial
cleft sinuses and cysts.3 Third or fourth branchial anomalies,
also referred to as piriform sinus fistulae, are the least
common,4 while first branchial anomalies account for about
10% of cases.5 Because first BCAs are rare, attempts to
describe the characteristics and management of these anomalies have historically been limited. Previous case series have
raised concerns regarding the frequency of misdiagnosis and
complications with treatment of first BCAs.6 Previous studies
have often focused on complications related to injury of the
facial nerve, which can be found in close association to these
lesions.7
In 1972, Work8 proposed a classification system for first
BCAs. Work type I lesions are cysts that lie superficial to the
facial nerve in closer proximity to the pinna, while Work
type II anomalies communicate with the external auditory
canal (EAC) or tympanic membrane (TM) and often lie
medial to the facial nerve. Olsen et al9 then introduced a classification of the defects into cysts, sinuses, and fistulas based
on the number of surface openings present.
The TM is considered a fusion point for the 3 primary
vestigial layers of the first branchial apparatus; therefore,
abnormal embryologic development in this region often
leads to otologic abnormalities.10 Considering this embryologic
1
Conclusions. Children with first branchial cleft anomalies often
present with otologic complaints. They are at increased risk of
persistent disease, particularly if anomalies lie medial to the
facial nerve. They may require ear-specific surgery such as
tympanoplasty.
Keywords
branchial cleft, otitis, congenital neck mass, pediatric
otolaryngology
Department of Otolaryngology, University of Washington, Seattle,
Washington, USA
2
Division of Pediatric Otolaryngology, Seattle Childrens Hospital, Seattle,
Washington, USA
This article was presented at the 2014 AAO-HNSF Annual Meeting & OTO
EXPOSM; September 21-24, 2014; Orlando, Florida.
Corresponding Author:
Patricia L. Purcell, Department of Otolaryngology, University of
Washington, 1959 NE Pacific St, Box 356515, Seattle, WA 98195-6515,
USA.
Email: plpurcel@uw.edu
Downloaded from oto.sagepub.com at IMSS on May 26, 2015
Shinn et al
507
Table 1. Characteristics of Different Types of Branchial Cleft Anomalies.
Laterality, No. (%)
Presenting Symptom, No. (%)
Type of
Anomaly
No.
Age at Diagnosis,
Mean (95% CI), y
Female Sex,
No. (%)
Left
Right
Bilateral
Draining
Pit
Neck
Abscess
Otologic
Problem
First
Second
Third
27
80
19
2.08 (1.07-3.08)
1.51 (0.67-2.36)
6.37 (4.12-8.62)
17 (63)
34 (42.5)
10 (52.6)
17 (63)
24 (30)
17 (89.5)
10 (37)
51 (63.7)
2 (10.5)
0
5 (6.3)
0
6 (22.2)
50 (62.5)
0
10 (37)
30 (37.5)
19 (100)
11 (40.7)
0
0
Abbreviation: CI, confidence interval.
Statistical Analysis
source, the primary objective of the current study was to
describe the presentation of first BCAs at our institution,
with attention to otologic manifestations of disease. A
second objective was to compare treatment outcomes of
children with first BCAs to children with other types of
BCAs to determine the extent to which children with first
anomalies are at greater risk of delayed diagnosis or persistent disease. Our hypothesis was that children with persistent disease would often require ear-specific surgery
for definitive management.
Univariate analyses were carried out to obtain descriptive
statistics such as means, confidence intervals, and frequencies for both groups. To make comparisons between the
groups, we performed inferential testing using one-way
analysis of variance. Risk estimates were obtained through
calculation of risk ratios using Fishers exact test. P \ .05
was considered statistically significant. Stata 13.1 (StataCorp,
College Station, Texas) statistical software was used for all
analyses.
Methods
Results
This investigation is a case series that received institutional
review board approval from Seattle Childrens Hospital, a
pediatric tertiary care facility. All children and adolescents
who were surgically treated for congenital neck masses between
2004 and 2013 were identified through query of the facilitys
surgical database using the following Current Procedural
Terminology (CPT) codes: 21556, 21557, 38510, 42408, 42815,
60280, and 60281.
A retrospective chart review was performed to identify
subjects from age birth to 21 years who were treated for
BCA. Diagnosis of branchial anomaly was made on the
basis of clinical evaluation, imaging characteristics, and surgical pathology.
First BCAs were defined by a pit or cyst identified in
level I or level II or the postauricular region with imaging
and surgical confirmation of a tract leading toward the ear
canal. Second branchial cleft sinuses and fistulae were
defined by a congenital pit along the anterior border of the
sternocleidomastoid muscle with surgical confirmation of a
tract heading partially or completely to the tonsillar fossa.
Second branchial cleft cysts were defined by an isolated
level II cyst lined by ciliated columnar epithelium. Third or
fourth branchial anomalies were defined by level III or level
IV neck inflammation, thyroid involvement, and/or a pit in
the ipsilateral piriform sinus. In all cases, diagnosis of branchial cleft anomaly was confirmed by review of final
pathology reports.
Data were collected regarding demographic characteristics, presenting signs and symptoms, procedures performed,
and treatment outcomes. Clinical records of children with
first and second BCAs were reviewed with attention to otologic manifestations of disease.
Review identified 126 patients with BCAs. Of these, 27
(21.4%) had first BCAs, 80 (63.4%) had second BCAs, and
19 (15.1%) had third or fourth branchial anomalies.
Clinical characteristics and presenting symptoms of the subjects are summarized in Table 1. Subjects with first BCAs
were more likely to be female (63%) and to have left-sided
lesions (63%). Patients with second BCAs were more likely to
have right-sided lesions (63.7%), while patients with third or
fourth BCAs had predominantly left-sided lesions (89.5%).
While most children were correctly diagnosed with BCA,
chart review also identified a subgroup of patients who did
not have BCA but rather the more commonly encountered
entity of preauricular pits. These children most commonly
presented with infected pits or abscesses anterior to the
tragus or helical root; these lesions were identified on the
right, left, or bilaterally nearly in equal numbers (5 bilaterally, 4 on the left, and 6 on the right). Findings during surgical excision included a pit, mass, or skin tag anterior to the
tragus or helical root in all cases.
Children with first and second BCAs had similar age at
diagnosis, 2.08 years versus 1.51 years (P = .4, not significant). In contrast, children with third or fourth BCAs were
significantly older with a mean age of 6.37 years (P \
.001). Children with first BCAs most commonly presented
with otologic complaints (40.7%), while those with second
BCAs were most likely to present with draining sinus or fistulae (62.5%). All children with third or fourth BCAs presented with neck mass or abscess.
Table 2 lists otologic examination findings of the subjects. Although a small number of patients with second
BCAs had otitis media or EAC deformity, an otologic problem was not given as the primary complaint for any of these
Downloaded from oto.sagepub.com at IMSS on May 26, 2015
508
OtolaryngologyHead and Neck Surgery 152(3)
Table 2. Otologic Examination Findings of Patients with First and Second Branchial Cleft Anomalies.
Type of
Anomaly
Otorrhea,
No. (%)
Acute Otitis
Media, No. (%)
Chronic Otitis
Media, No. (%)
Cholesteatoma,
No. (%)
EAC Web,
No. (%)
Other EAC
Deformity, No. (%)
6 (22.2)
0
4 (14.8)
2 (2.5)
3 (11.1)
1 (1.3)
4 (14.8)
0
6 (22.2)
0
13 (48.1)
3 (3)
First
Second
Abbreviation: EAC, external auditory canal.
Table 3. Comparison of Surgical Outcomes among First and Second Branchial Cleft Anomalies.
Type of Anomaly
First, No. (%)
Second, No. (%)
Relative risk (95% CI)
P value
Primary I&D
Persistent Disease
Multiple Surgeriesa (Excluding Primary I&D)
16 (59.3)
2 (2.5)
3.5 (2.4-5)
\.0001
7 (25.9)
2 (2.5)
3 (1.9-5)
.0025
8 (29.6)
3 (11.1)
2.9 (1.8-4.7)
.0025
Abbreviations: CI, confidence interval; incision and drainage.
a
Multiple surgeries: includes both repeat excision and treatment of complication.
Table 4. Surgical Management of Patients with First Branchial Cleft Anomalies.
Procedure(s) Performed, No. (%)
Primary excision (n = 27)
Repeat excision (n = 7)
Local Excision
Superficial Parotidectomy
Meatoplasty/Tympanomastoidectomy
13 (48.1)
1 (14.3)
13 (48.1)
2 (28.6)
5 (18.5)
4 (57.1)
patients. In contrast, patients with first BCAs had a variety of
otologic complications, ranging from EAC cyst to cholesteatoma. Even if not the presenting complaint, the presence of
otitis media was noted from clinical examination records.
Seven of 27 children with first BCAs and 3 of 80 children
with second BCAs were noted to have otitis media (relative
risk [RR], 2.8; 95% confidence interval [CI], 1.6-4.7; P =
.006). Among the 7 children with first BCAs who had otitis, 4
had a history of acute otitis media, while 3 had a history of
chronic otitis media with effusion. None had TM perforation.
An EAC web, or abnormal connection between the
anterior-inferior or posterior-inferior canal wall and TM,
can signal the presence of a first branchial cleft anomaly; 6
of our subjects (22.2%) were discovered to have such a web
on evaluation. In addition, children with first BCAs displayed a range of other EAC deformities: 5 (18.5%) had an
EAC mass or cyst, while 5 (18.5%) had EAC duplication.
In comparison, 3 (3%) of the children with second BCAs
displayed EAC deformities, which were associated with
hemifacial microsomia or Down syndrome.
Table 3 contains a comparison of outcomes among
patients with first and second BCAs. Compared with children with second BCAs, children with first BCAs had a
greater incidence of primary incision and drainage: 16
(59.3%) vs 2 (2.5%) (RR, 3.5; 95% CI, 2.4-5; P \ .0001).
Of the 16 children with first BCAs who underwent primary
incision and drainage, 11 presented with an acute abscess,
while 5 children presented with a draining pit. After resolution of their acute infection, the children underwent primary
excision. Compared with children with second BCAs, children with first BCAs were more likely to have persistent
disease following primary excision: 7 (25.9%) vs 2 (3.8%)
(RR, 3; 95% CI, 1.9-5; P = .0025). They were also more
likely to undergo additional surgery: 8 (29.6%) vs 3
(11.1%) (RR, 2.9; 95% CI, 1.8-4.7; P = .0025). There was
not a significant difference in rates of persistent disease
between children with first and children with third or fourth
BCAs. Of the 19 children with third or fourth BCAs, 11
(57.9%) underwent incision and drainage prior to excision,
7 (36.8%) experienced persistent disease, and 7 (36.8%)
required additional surgery.
Length of follow-up period was not significantly different among the anomaly types. Children with first BCAs had
a mean follow-up period of 16 months (95% CI, 6-27
months), children with second BCAs had a mean follow-up
length of 8 months (95% CI, 4-12 months), and those with
third or fourth anomalies had a follow-up of 11 months
(95% CI, 1-21 months).
Table 4 describes the surgical management of the 27
patients with first BCAs. Thirteen subjects (48.1%) underwent
Downloaded from oto.sagepub.com at IMSS on May 26, 2015
Shinn et al
509
superficial parotidectomy on primary excision, with 4 of these
patients also undergoing tympanoplasty or tympanomastoidectomy. One patient underwent tympanomastoidectomy alone
after the identification of an EAC duplication, a type of first
branchial cleft anomaly. The duplication was located superficial to the facial nerve. The remainder of children underwent
simple excision at the time of primary surgery. Among the 7
patients who required revision surgery, more than half (57.1%)
underwent otologic surgery, either tympanoplasty or tympanomastoidectomy. There were 9 patients (33.3%) who had Work
type II anomalies that coursed medial to the facial nerve; all
eventually required parotidectomy either at primary or repeat
excision. Of the 7 patients who required additional surgery, 6
(85.7%) had anomalies medial to the facial nerve.
Facial nerve complications were also evaluated among
the patients with first BCAs. Only 1 patient (3.7%) had confirmation of permanent facial nerve weakness, an adolescent
who presented to our facility with facial nerve palsy after
undergoing multiple procedures at outside facilities. In addition, 3 patients (11.1%) developed temporary weakness of
the marginal mandibular nerve that completely resolved,
while 2 (7.4%) patients experienced weakness of unknown
duration due to loss to follow-up. Among the 5 cases that
occurred at our institution, the first branchial cleft anomaly
was identified medial to the facial nerve during the excision
procedure.
Discussion
Children with first BCAs often undergo multiple procedures
to treat infectious complications and ultimately remove
these lesions. In the current study, more than half of the
children were treated with incision and drainage prior to
excision, and over a quarter required repeated excision procedures. Risk of persistent disease and repeat surgery were
much higher for these children than for children with
second BCAs. This indicates that the diagnosis of first BCA
may not be recognized until the anomaly is infected and
requires incision and drainage. Interestingly, our findings
suggest that children with third or fourth branchial anomalies also have high rates of persistent disease, which is consistent with previously published literature11 and should be
explored further in future investigations.
Careful otologic evaluation can assist providers in
making correct diagnosis of first BCAs.12 Previous case
series have described otologic complications, including cholesteatoma13; however, we were surprised by the high frequency of children who presented with a primary otologic
complaint. Otologic complications were the most frequent
presenting symptoms, occurring in nearly half of the cases.
Otorrhea and otitis media were identified in about onefourth of the cases, and 15% of patients were found to have
cholesteatoma. Seven children with first BCAs had otitis
media, of whom 4 had a history of acute otitis media and 3
had a history of chronic otitis media with effusion. None of
these children had tympanic membrane perforation. In addition, more than half of the patients were noted to have an
EAC anatomical deformity.
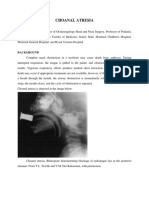
Figure 1. Left level II cervical abscess. Application of pressure produces otorrhea.
Perhaps the most complicated case encountered was a 2year-old male who presented with a left level II neck abscess
and purulent otorrhea. The patient was ultimately diagnosed
with both Work type I and Work type II anomalies. During
the childs initial incision and drainage procedure, pressure
on the neck abscess resulted in copious expression of pus
from the ear canal (Figure 1), confirming the diagnosis of a
Work type II anomaly. After antibiotic therapy, the patient
had persistent erythema and drainage at the original incision
site and in the postlobular crease (Figure 2). Otoscopy
revealed both anterior-inferior and posterior-inferior TM
webs along with some persistent granulation at the anterior
inferior sulcus (Figure 3). The 2 first branchial anomalies
were then excised via a superficial parotidectomy approach
with facial nerve dissection (Figure 4). The proximal cartilaginous portion of the main fistula, which ran deep to the
facial nerve, was shaved off at the bony cartilaginous junction of the anterior ear canal. The patient experienced continued wound infection at the incision area directly inferior
to the lobule. Cultures grew Pseudomonas, indicating a
likely continued connection to the ear canal or middle ear.
Otoscopy demonstrated a persistent area of granulation at
the point of origin of the anterior web at the anterior
sulcus. A tympanoplasty was performed with excision of
the anterior-inferior TM, curettage of the pit at the anterior
sulcus, and reconstruction with fascia. The infection
resolved, and the ear canal and tympanic membrane healed
(Figure 5). This is a rare case of 2 first branchial anomalies in 1 patient and emphasizes the point that Work type
II fistulae can present at a young age with a sinus tract
running deep to the facial nerve. Failure to adequately
address the otologic component of the lesion can result in
persistent infection, as was the case for this patient.
The approach to a child with a first branchial cleft anomaly lies in accurate diagnosis; Figure 6 contains a potential
algorithm for management. First anomalies should be among
Downloaded from oto.sagepub.com at IMSS on May 26, 2015
510
OtolaryngologyHead and Neck Surgery 152(3)
Figure 2. Left level II incision and drainage site as a sign of Work
type II anomaly; persistent postlobule infection as evidence of
Work type I anomaly.
Figure 4. Parotidectomy approach. Ruptured abscess and ear
canal duplication (*) are delivered from a location medial to the
facial nerve trunk, which is elongated. The anomaly is then excised
from the anterior ear canal.
Figure 3. Otoscopy showing anterior inferior granulation (*) and
anterior (#) and posterior ($) webs.
the differential diagnoses considered when children present
with a pit or inflammatory response in neck level I, high in
level IIa/IIb, on the face, or in the postauricular area. A thorough otoscopic examination is indicated, with the use of
binocular microscopy if available. The examiner should look
specifically for a canal web, granulation tissue, or middle ear
disease. Evidence of purulent expression from the ear with
simultaneous pressure on the neck or infected lesion indicates
a communication between the lesion and the EAC. Imaging,
either with contrast computed tomography (CT) or magnetic
resonance imaging (MRI), can help clarify the diagnosis. If a
child presents with acute infection, incision and drainage and
antibiotics are indicated prior to definitive excision.
When deciding the optimal approach for primary excision, patients who present with a pit or abscess anterior to
the angle of mandible, at cervical level I or II, are more
likely to have an anomaly deep or medial to the facial nerve
(Work type II). In our study, all of these patients required
Figure 5. Otoscopy after tympanoplasty showing healing of anterior ear drum and ear canal. Posterior web remains. Umbo indicated by (*).
parotidectomy, and many required otologic surgery. If there
is any suspicion of Work type II anomaly, then imaging
should be performed to assist with operative planning and
to determine where the tract lies in relation to the facial
nerve. A parotidectomy approach with preliminary identification of the facial nerve and excision of the entire tract is
indicated. Concurrent tympanoplasty or canalplasty should
be performed if a connection between the superficial skin
and EAC or TM is seen or if a cyst involves the external
ear. Facial nerve monitoring should be considered in all
cases. In the current study, all patients with facial nerve
weakness had a Work type II anomaly medial to the nerve.
If the child has a Work type I anomaly, indicated by a
pit or cyst around the lobule, then imaging may not be
Downloaded from oto.sagepub.com at IMSS on May 26, 2015
Shinn et al
511
Figure 6. Algorithm for management of first branchial cleft anomalies. BCA, branchial cleft anomaly; CT, computed tomography; MRI, magnetic resonance imaging.
required, although preferences will likely be institution specific. Surgical excision of the tract, superficial to the facial
nerve, is performed with a mini-facelift incision behind
the tragus and around the lobule with facial nerve monitoring. If there is a visible connection or cyst on the tympanic
membrane or external auditory canal, then concurrent tympanoplasty or canalplasty should be performed.
Children with preauricular pits may be misdiagnosed as
having a first BCA; however, we found these children to
always present with a lesion near the helical root. These
children most commonly presented with infected pits or
abscesses and were identified on the right, left, or bilaterally
nearly in equal numbers. Preauricular pits are a distinct
diagnosis and should not be confused with BCA. They
occur anterior to the tragus or helical root, often become
infected, and do not involve the facial nerve. Imaging prior
to surgical excision is often not necessary.
As a retrospective study, this investigation has a number
of limitations, including incomplete records, loss to followup, and potential misclassification of anomaly type.
However, the large difference in persistent disease between
first and second BCAs strongly suggests that there is a need
for improvement in surgical management of first BCAs.
Misdiagnosis and inadequate treatment of first BCAs
have the potential to result in recurrent infection, scarring
due to multiple procedures, and facial nerve injury. For children with chronic or recurrent upper neck infections,
especially in the setting of ipsilateral ear disease, providers
should strongly consider the possibility that the subject may
have a first branchial cleft anomaly. Children with anomalies that occur medial to the nerve are especially at risk for
persistent disease. Preoperative imaging should be performed to define this relationship, so that families can be
counseled appropriately. If otologic involvement is suspected, then it should be addressed with otologic surgery at
the time of primary excision if possible.
Conclusion
First BCAs are associated with a wide range of otologic
manifestations. These children, particularly those with Work
type II lesions medial to the facial nerve, experience a relatively high frequency of persistent disease, and otologic surgery may be required for definitive surgical management.
Acknowledgment
We thank Rose Jones-Goodrich, clinical research associate, for
administrative support of this project.
Author Contributions
Justin R. Shinn, study design, data collection, manuscript preparation; Patricia L. Purcell, study design, data analysis, manuscript
revision; David L. Horn, data collection, manuscript revision;
Kathleen C. Y. Sie, data collection, manuscript revision; Scott C.
Downloaded from oto.sagepub.com at IMSS on May 26, 2015
512
OtolaryngologyHead and Neck Surgery 152(3)
Manning, study conceptualization, study design, data collection,
manuscript preparation and revision.
Disclosures
Competing interests: None.
Sponsorships: None.
Funding source: Patricia L. Purcell is completing a research fellowship supported by grant 2T32DC000018, the Institutional
National Research Service Award for Research Training in
Otolaryngology from the National Institute on Deafness and Other
Communication Disorders.
References
1. Al-Khateeb TH, Al Zoubi F. Congenital neck masses: a
descriptive retrospective study of 252 cases. J Oral Maxillofac
Surg. 2007;65:2242-2247.
2. LaRiviere CA, Waldhausen JH. Congenital cervical cysts,
sinuses, and fistulae in pediatric surgery. Surg Clin North Am.
2012;92:583-597, viii.
3. Bajaj Y, Ifeacho S, Tweedie D, et al. Branchial anomalies in
children. Int J Pediatr Otorhinolaryngol. 2011;75:1020-1023.
4. Chen EY, Inglis AF, Ou H, et al. Endoscopic electrocauterization of pyriform fossa sinus tracts as definitive treatment. Int J
Pediatr Otorhinolaryngol. 2009;73:1151-1156.
5. Schroeder JW Jr, Mohyuddin N, Maddalozzo J. Branchial
anomalies in the pediatric population. Otolaryngol Head Neck
Surg. 2007;137:289-295.
6. Triglia JM, Nicollas R, Ducroz V, Koltai PJ, Garabedian EN.
First branchial cleft anomalies: a study of 39 cases and a review
of the literature. Arch Otolaryngol Head Neck Surg. 1998;124:
291-295.
7. Guo YX, Guo CB. Relation between a first branchial cleft
anomaly and the facial nerve. Br J Oral Maxillofac Surg.
2012;50:259-263.
8. Work WP. Newer concepts of first branchial cleft defects.
Laryngoscope. 1972;82:1581-1593.
9. Olsen KD, Maragos NE, Weiland LH. First branchial cleft
anomalies. Laryngoscope. 1980;90:423-436.
10. Waldhausen JH. Branchial cleft and arch anomalies in children. Semin Pediatr Surg. 2006;15:64-69.
11. Madana J, Yolmo D, Kalaiarasi R, Gopalakrishnan S, Saxena
SK, Krishnapriya S. Recurrent neck infection with branchial
arch fistula in children. Int J Pediatr Otorhinolaryngol. 2011;
75:1181-1185.
12. Tom LW, Kenealy JF, Torsiglieri AJ Jr.First branchial cleft
anomalies involving the tympanic membrane and middle ear.
Otolaryngol Head Neck Surg. 1991;105:473-477.
13. Nicollas R, Tardivet L, Bourlie`re-Najean B, Sudre-Levillain I,
Triglia JM. Unusual association of congenital middle ear cholesteatoma and first branchial cleft anomaly: management and
embryological concepts. Int J Pediatr Otorhinolaryngol. 2005;
69:279-282.
Downloaded from oto.sagepub.com at IMSS on May 26, 2015
You might also like
- The Effects of Social Media On Mental Health of Selected Senior High School StudentsDocument26 pagesThe Effects of Social Media On Mental Health of Selected Senior High School StudentsJeandra Villanueva87% (39)
- 3D Implant Position Esquivel 2021Document9 pages3D Implant Position Esquivel 2021Lamis MagdyNo ratings yet
- Airway Obstruction and VentilationDocument8 pagesAirway Obstruction and VentilationJeremias KwapiszNo ratings yet
- Neuropsychological AssessmentDocument5 pagesNeuropsychological AssessmentadriricaldeNo ratings yet
- The Picture Exchange Communication System: Helping Individuals Gain Functional CommunicationDocument4 pagesThe Picture Exchange Communication System: Helping Individuals Gain Functional CommunicationAlex Web100% (1)
- ArtículoDocument5 pagesArtículogemapesfNo ratings yet
- Otolaryngology Service Usage in Children With Cleft PalateDocument4 pagesOtolaryngology Service Usage in Children With Cleft PalateCatherine nOCUANo ratings yet
- 2D-3D Assessment of The Face, Cleft LipDocument10 pages2D-3D Assessment of The Face, Cleft LipginogjNo ratings yet
- Odontogenic Cysts - A Descriptive Clinicopathological StudyDocument6 pagesOdontogenic Cysts - A Descriptive Clinicopathological StudyAvif PutraNo ratings yet
- Baugh 2018Document5 pagesBaugh 201823 Ruby FirdausNo ratings yet
- Diagnostic Yield of Computed Tomography Scan For Pediatric Hearing Loss A Systematic ReviewDocument22 pagesDiagnostic Yield of Computed Tomography Scan For Pediatric Hearing Loss A Systematic ReviewadriricaldeNo ratings yet
- JurnalDocument9 pagesJurnalNoraine Zainal AbidinNo ratings yet
- Elkhunovich2016 The Utility of Cranial Ultrasound For Detection of IntracranialDocument6 pagesElkhunovich2016 The Utility of Cranial Ultrasound For Detection of IntracranialModou NianeNo ratings yet
- Nasopharyngeal Airway For Management of Airway Obstruction in Infants With MicrognathiaDocument5 pagesNasopharyngeal Airway For Management of Airway Obstruction in Infants With Micrognathiaapriliani2293No ratings yet
- 2018 Article 1362 PDFDocument5 pages2018 Article 1362 PDFAuliaMahdaniatiNo ratings yet
- Rare Facial Clefts PDFDocument6 pagesRare Facial Clefts PDFAntoine NinoNo ratings yet
- Management of Common Voice DisordersDocument16 pagesManagement of Common Voice Disordersrowin93No ratings yet
- Fetal Surgery - The Ochsner Experience With in Utero Spina Bifida RepairDocument6 pagesFetal Surgery - The Ochsner Experience With in Utero Spina Bifida RepairJusten ThompsonNo ratings yet
- Pediatric Tracheostomy Decannulation: 11-Year ExperienceDocument8 pagesPediatric Tracheostomy Decannulation: 11-Year Experienceanitaabreu123No ratings yet
- Ricci 2013Document5 pagesRicci 2013Lim Chia SeangNo ratings yet
- Miiringotomi OMEDocument7 pagesMiiringotomi OMEamaliaNo ratings yet
- Indications For Tracheotomy in The Pediatric Intensive Care Unit PopulationDocument4 pagesIndications For Tracheotomy in The Pediatric Intensive Care Unit PopulationGela AfmaNo ratings yet
- Conference Paper: Rapid Physical Assessment of The Injured ChildDocument4 pagesConference Paper: Rapid Physical Assessment of The Injured ChildMaiush JbNo ratings yet
- Predictive Performance of Three Multivariate.24Document7 pagesPredictive Performance of Three Multivariate.24Yves BurckelNo ratings yet
- Jurnal Reading OtologiDocument19 pagesJurnal Reading OtologiMuhammad gusti haryandiNo ratings yet
- Neonatal RetinoblastomaDocument5 pagesNeonatal Retinoblastomaromeoenny4154No ratings yet
- Choanal AtresiaDocument8 pagesChoanal AtresiaCharmila Sari0% (1)
- Journal Pre-Proof: European Journal of Paediatric NeurologyDocument31 pagesJournal Pre-Proof: European Journal of Paediatric NeurologySebastian SalvadorNo ratings yet
- Grant 1988Document5 pagesGrant 1988Camila MillarNo ratings yet
- HydrocephalusDocument9 pagesHydrocephalusDeby AnditaNo ratings yet
- Cysts of The Jaws in Pediatric Population: A 12-Year Institutional StudyDocument6 pagesCysts of The Jaws in Pediatric Population: A 12-Year Institutional StudyAndreas SimamoraNo ratings yet
- AAOGUDocument6 pagesAAOGUGoran JosipovićNo ratings yet
- Art 2Document6 pagesArt 2Cristian OneaNo ratings yet
- 11 - Facts and Myths Regarding The Maxillary Midline Frenum and Its Treatment A Systematic Review of The LiteratureDocument11 pages11 - Facts and Myths Regarding The Maxillary Midline Frenum and Its Treatment A Systematic Review of The Literaturekochikaghochi100% (1)
- Ostrower Preauricular Cysts, Pits, and Fissures - Practice Essentials, Epidemiology, EtiologyDocument8 pagesOstrower Preauricular Cysts, Pits, and Fissures - Practice Essentials, Epidemiology, EtiologyAndre HawkNo ratings yet
- Fistula in AnoDocument5 pagesFistula in AnoIoannis ValioulisNo ratings yet
- 1.masas en CuelloDocument3 pages1.masas en CuelloIsaac TellezNo ratings yet
- Predictors of Difficult Airways in PediatricsDocument7 pagesPredictors of Difficult Airways in PediatricsPablo Segales BautistaNo ratings yet
- Absceso CerebralDocument6 pagesAbsceso Cerebralkreacher3000No ratings yet
- Clinical and Descriptive Study of Orofacial Clefts in Colombia 2069 Patients From Operation Smile FoundationDocument9 pagesClinical and Descriptive Study of Orofacial Clefts in Colombia 2069 Patients From Operation Smile FoundationelmancuernoNo ratings yet
- Montes Jovellar2011Document8 pagesMontes Jovellar2011Ali FaidiNo ratings yet
- 2020 Optimal Timing of Palatoplasty in Infants With ComorbiditiesDocument6 pages2020 Optimal Timing of Palatoplasty in Infants With ComorbiditiesDimitris RodriguezNo ratings yet
- (Polish Journal of Surgery) Rare Facial CleftsDocument6 pages(Polish Journal of Surgery) Rare Facial CleftspatrickpsilvaNo ratings yet
- Ucm 439476Document1 pageUcm 439476Fadel BilondatuNo ratings yet
- Schallert 2019Document7 pagesSchallert 2019Dian Putri NingsihNo ratings yet
- Maxillary Gap at 11-13 WeeksDocument5 pagesMaxillary Gap at 11-13 Weekscarlos cobeloNo ratings yet
- 292-Article Text-1640-1-10-20190515Document8 pages292-Article Text-1640-1-10-20190515Liset Edreira Cutipa SallucaNo ratings yet
- National Trends in The Surgical Management of Meckel's DiverticulumDocument4 pagesNational Trends in The Surgical Management of Meckel's DiverticulumLeokádio BarrosoNo ratings yet
- A Case Series of Tessier 3, 4, 7 and Combined 4, 7 Craniofacial CleftsDocument5 pagesA Case Series of Tessier 3, 4, 7 and Combined 4, 7 Craniofacial CleftsMohammad Wildan Hari SHNo ratings yet
- Foreign Bodies of The AirwayDocument6 pagesForeign Bodies of The AirwayCharmila Sari100% (1)
- J Neurosurg Pediatr Article p52Document10 pagesJ Neurosurg Pediatr Article p52Audhrey BNo ratings yet
- Research Article: Treatment and Outcome For Children With Esophageal Atresia From A Gender PerspectiveDocument7 pagesResearch Article: Treatment and Outcome For Children With Esophageal Atresia From A Gender PerspectivedaxNo ratings yet
- Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis Ear, Nose, and Throat Description at Acute Stage and After RemissionDocument6 pagesStevens-Johnson Syndrome and Toxic Epidermal Necrolysis Ear, Nose, and Throat Description at Acute Stage and After RemissionElsa Giatri SiradjNo ratings yet
- Accuracy of The Interpretation of Chest Radiographs For The Diagnosis of Paediatric PneumoniaDocument5 pagesAccuracy of The Interpretation of Chest Radiographs For The Diagnosis of Paediatric Pneumoniania gusnawatiNo ratings yet
- Clinical Study: Vertigo in Children and Adolescents: Characteristics and OutcomeDocument6 pagesClinical Study: Vertigo in Children and Adolescents: Characteristics and OutcomeC Leite HendriyNo ratings yet
- Canine ImpactionDocument4 pagesCanine ImpactionPorcupine TreeNo ratings yet
- Acute Pericoronitis and The Position of The Mandibular Third Molar in NigeriansDocument6 pagesAcute Pericoronitis and The Position of The Mandibular Third Molar in NigeriansSyafila WongsoNo ratings yet
- Celulitis PeriorbitariaDocument4 pagesCelulitis PeriorbitariaJose Carlos Guerra RangelNo ratings yet
- Advancesinsurgeryfor Abdominalwalldefects: Gastroschisis and OmphaloceleDocument12 pagesAdvancesinsurgeryfor Abdominalwalldefects: Gastroschisis and OmphaloceleSitti HazrinaNo ratings yet
- International Journal of Pediatric OtorhinolaryngologyDocument5 pagesInternational Journal of Pediatric OtorhinolaryngologyTuis PreviyantiNo ratings yet
- Orbital Cellulitis in A Pediatric Population - Experience From A Tertiary CenterDocument3 pagesOrbital Cellulitis in A Pediatric Population - Experience From A Tertiary CenterMuthu V RanNo ratings yet
- Tracheobronchial Foreign Bodies : Presentation and Management in Children and AdultsDocument6 pagesTracheobronchial Foreign Bodies : Presentation and Management in Children and AdultsrizkaayusafitriNo ratings yet
- Americanas Neumo PDFDocument291 pagesAmericanas Neumo PDFUri MoraNo ratings yet
- 10.1007@s00383 019 04527 9Document18 pages10.1007@s00383 019 04527 9Claudia Sughey Herrera PalominoNo ratings yet
- AAA - 2010 - Diagnosis Treatment and Management of Children and Adults With Central Auditory Processing Disroder-AnnotatedDocument51 pagesAAA - 2010 - Diagnosis Treatment and Management of Children and Adults With Central Auditory Processing Disroder-AnnotatedadriricaldeNo ratings yet
- Dementia in Clinical Practice PDFDocument404 pagesDementia in Clinical Practice PDFadriricalde100% (2)
- Art:10.1007/s00455 016 9773 ZDocument12 pagesArt:10.1007/s00455 016 9773 ZadriricaldeNo ratings yet
- English Et Al-2009-Developmental Disabilities Research ReviewsDocument7 pagesEnglish Et Al-2009-Developmental Disabilities Research ReviewsadriricaldeNo ratings yet
- 1 s2.0 S0030666516300469 MainDocument10 pages1 s2.0 S0030666516300469 MainadriricaldeNo ratings yet
- Myelomeningocele: How We Can Improve The Assessment of The Most Severe Form of Spina Bi FidaDocument7 pagesMyelomeningocele: How We Can Improve The Assessment of The Most Severe Form of Spina Bi FidaadriricaldeNo ratings yet
- Auris Nasus Larynx: Kimitaka KagaDocument11 pagesAuris Nasus Larynx: Kimitaka KagaadriricaldeNo ratings yet
- Cochlear OtosclerosisDocument6 pagesCochlear OtosclerosisadriricaldeNo ratings yet
- Seminars in Fetal & Neonatal Medicine: Cristen Olds, John S. OghalaiDocument5 pagesSeminars in Fetal & Neonatal Medicine: Cristen Olds, John S. OghalaiadriricaldeNo ratings yet
- Object and Space PerceptionDocument10 pagesObject and Space PerceptionadriricaldeNo ratings yet
- Diagnostic Yield of Computed Tomography Scan For Pediatric Hearing Loss A Systematic ReviewDocument22 pagesDiagnostic Yield of Computed Tomography Scan For Pediatric Hearing Loss A Systematic ReviewadriricaldeNo ratings yet
- IAL Biology SB2 Assessment 7CDocument4 pagesIAL Biology SB2 Assessment 7CsalmaNo ratings yet
- Lesson Plan On Myocardial InfarctionDocument4 pagesLesson Plan On Myocardial Infarctionpreet kaur0% (1)
- Interesting Signs in Nuclear Medicine2Document31 pagesInteresting Signs in Nuclear Medicine2kapilshirodkarNo ratings yet
- Ship To Party Sold To Party Section Circle Item CodeDocument3 pagesShip To Party Sold To Party Section Circle Item Codesayantan bhattacharyaNo ratings yet
- Arterial Blood Gas Analysis: Vanessa Klee MSIVDocument25 pagesArterial Blood Gas Analysis: Vanessa Klee MSIVGarata PutriNo ratings yet
- Acara Ilmiah Minggu Ke-3 Desember 2020Document1 pageAcara Ilmiah Minggu Ke-3 Desember 2020RioNo ratings yet
- Acute Abdominal PainDocument2 pagesAcute Abdominal PainWinnieNo ratings yet
- Diseases Caused by PollutionDocument23 pagesDiseases Caused by PollutionAsia Kainat100% (1)
- CONTROL LECTURA #01 - Biography of Daniel A. CarrionDocument10 pagesCONTROL LECTURA #01 - Biography of Daniel A. CarrionAguirre LizettNo ratings yet
- IO in ReviewDocument8 pagesIO in Reviewfenrisulven2010No ratings yet
- SemenDocument14 pagesSemenjems wattNo ratings yet
- Spiritual Awakening Signs - 10 Authentic Symptoms + 5 Spiritual TrapsDocument23 pagesSpiritual Awakening Signs - 10 Authentic Symptoms + 5 Spiritual Trapsconnect2rahul420467% (3)
- Iron Deficiency Anemia-HandoutDocument4 pagesIron Deficiency Anemia-HandoutCeleste Parin Procopia KardinNo ratings yet
- RABIES Causative Agent: Rhabdovirus Mode of Transmission: Bite of RabidDocument1 pageRABIES Causative Agent: Rhabdovirus Mode of Transmission: Bite of RabidFreeNursingNotes100% (1)
- Positioning A Client in BedDocument32 pagesPositioning A Client in BedGrape JuiceNo ratings yet
- Nursing Diagnosis PneumoniaDocument1 pageNursing Diagnosis PneumoniaPasa ShresthaNo ratings yet
- Actionsfollowinganaccident-Abriefguide CSHSTDocument2 pagesActionsfollowinganaccident-Abriefguide CSHSTMadalinaZahariaIoanaNo ratings yet
- DANONE Sustainability Report 2011 PDFDocument230 pagesDANONE Sustainability Report 2011 PDFMuhammadAlAminNo ratings yet
- Adjunctive Amantadine Treatment For Aggressive Behavior in Children A Series of Eight CasesDocument4 pagesAdjunctive Amantadine Treatment For Aggressive Behavior in Children A Series of Eight Casesleorocha06No ratings yet
- Reflective Journal CHN in Brgy Capo MSINONDocument2 pagesReflective Journal CHN in Brgy Capo MSINONjan paul galizaNo ratings yet
- Copy EclampsiaDocument19 pagesCopy EclampsiaRobert ChilesheNo ratings yet
- Sitasi Nomor 14Document8 pagesSitasi Nomor 14Bill RajagukgukNo ratings yet
- Literature Review CellulitisDocument6 pagesLiterature Review Cellulitisc5qe3qg3100% (1)
- Oral Procedures in Children: Dr. H. Ryan Kazemi Oral & Maxillofacial Surgery 4825 Bethesda Ave., #310 Bethesda, MD 20814Document8 pagesOral Procedures in Children: Dr. H. Ryan Kazemi Oral & Maxillofacial Surgery 4825 Bethesda Ave., #310 Bethesda, MD 20814Silvio DTNo ratings yet
- Mitochondrial GeneticsDocument7 pagesMitochondrial GeneticsÖmer KhanNo ratings yet
- Ectopic PregnancyDocument54 pagesEctopic PregnancyLawrence CapuchinoNo ratings yet