Professional Documents
Culture Documents
Iaet07i1p23 2 PDF
Iaet07i1p23 2 PDF
Uploaded by
rynaldiandriansyaCopyright:
Available Formats
You might also like
- TNCC NotesDocument9 pagesTNCC NotesJessie Bronkalla95% (21)
- Reclaiming Your Life From A Traumatic Experience: Workbook - Rothbaum, Edna B. Foa, HembreeDocument105 pagesReclaiming Your Life From A Traumatic Experience: Workbook - Rothbaum, Edna B. Foa, Hembreedoppler_100% (8)
- Maternal and Child Health Nursing ReviewerDocument17 pagesMaternal and Child Health Nursing ReviewerJeffrey Viernes100% (6)
- Aspergilloma MoroccoDocument5 pagesAspergilloma MoroccoYassine EssNo ratings yet
- Surgical Therapy For Necrotizing Pneumonia and Lung Gangrene PDFDocument6 pagesSurgical Therapy For Necrotizing Pneumonia and Lung Gangrene PDFmichael24kNo ratings yet
- RadiopediaDocument4 pagesRadiopediakennyNo ratings yet
- HemoptisisDocument7 pagesHemoptisiswiliaNo ratings yet
- Abstrak SederhanaDocument2 pagesAbstrak Sederhanaabsensi paruNo ratings yet
- Reseccion Pulmonar en Hemoptisis SeveraDocument10 pagesReseccion Pulmonar en Hemoptisis SeverarafodocNo ratings yet
- Chronic Pulmonary Aspergillosis: A Frequent and Potentially Severe DiseaseDocument5 pagesChronic Pulmonary Aspergillosis: A Frequent and Potentially Severe Diseasemedicina146No ratings yet
- Etm 13 5 2259 PDFDocument4 pagesEtm 13 5 2259 PDFdicky nanda muzidaNo ratings yet
- Management of Non-Tumoral Tracheal Stenosis in 112 Patients EDocument5 pagesManagement of Non-Tumoral Tracheal Stenosis in 112 Patients Ezed-medNo ratings yet
- Curren Clinical Propensity of TB LaringDocument5 pagesCurren Clinical Propensity of TB LaringDevi DaryaningsihNo ratings yet
- Simultaneous Bilateral Primary Spontaneous Pneumothorax (2019)Document7 pagesSimultaneous Bilateral Primary Spontaneous Pneumothorax (2019)sandi_prawira_yudhaNo ratings yet
- Pulmonary Pathological Features in Coronavirus Associated Severe Acute Respiratory Syndrome (SARS)Document6 pagesPulmonary Pathological Features in Coronavirus Associated Severe Acute Respiratory Syndrome (SARS)Leandro VillamilNo ratings yet
- Maiwand Asimakopoulos 2004 Cryosurgery For Lung Cancer Clinical Results and Technical AspectsDocument8 pagesMaiwand Asimakopoulos 2004 Cryosurgery For Lung Cancer Clinical Results and Technical Aspectsbjro1986No ratings yet
- Chronic Cavitary and Fibrosing Pulmonary and Pleural Aspergillosis: Case Series, Proposed Nomenclature Change, and ReviewDocument16 pagesChronic Cavitary and Fibrosing Pulmonary and Pleural Aspergillosis: Case Series, Proposed Nomenclature Change, and ReviewYassine EssNo ratings yet
- Ecmo 2000Document13 pagesEcmo 2000Maria PaulaNo ratings yet
- 2008 Chest - The Blue ProtocolDocument9 pages2008 Chest - The Blue Protocoleduardo0% (1)
- Empyema ThoracisDocument6 pagesEmpyema ThoracisThine NG CalderonNo ratings yet
- (1992) Yang, Pan-Chyr Luh, Kwen-Tay Chang, Dun-Bing Yu, Chong-Jen K - Ultrasonographic Evaluation of Pulmonary ConsolidationDocument6 pages(1992) Yang, Pan-Chyr Luh, Kwen-Tay Chang, Dun-Bing Yu, Chong-Jen K - Ultrasonographic Evaluation of Pulmonary ConsolidationPer DamiánNo ratings yet
- Pulmonary Nodules and Masses After Lung and Heart-Lung TransplantationDocument7 pagesPulmonary Nodules and Masses After Lung and Heart-Lung TransplantationManisha UppalNo ratings yet
- JurnalDocument8 pagesJurnalwiliaNo ratings yet
- Management of Anastomotic Complications After Sleeve Lobectomy For Lung CancerDocument4 pagesManagement of Anastomotic Complications After Sleeve Lobectomy For Lung CancerJovelyn SagangNo ratings yet
- Bilat Ten Pneumo Improv 0214 p20 24Document5 pagesBilat Ten Pneumo Improv 0214 p20 24juliusNo ratings yet
- Emphysema Versus Chronic Bronchitis in COPD: Clinical and Radiologic CharacteristicsDocument8 pagesEmphysema Versus Chronic Bronchitis in COPD: Clinical and Radiologic CharacteristicsChairul Nurdin AzaliNo ratings yet
- Saddle Pulmonary Embolism: A Rare Case of Proximal Pulmonary EmbolismDocument3 pagesSaddle Pulmonary Embolism: A Rare Case of Proximal Pulmonary EmbolismIJAR JOURNALNo ratings yet
- Pneumothorax in Active Pulmonary Tuberculosis: Resurgence of An Old Complication?Document5 pagesPneumothorax in Active Pulmonary Tuberculosis: Resurgence of An Old Complication?M Tata SuhartaNo ratings yet
- Medip, IJOHNS-388 ODocument6 pagesMedip, IJOHNS-388 Onaveed gulNo ratings yet
- 712 PDFDocument74 pages712 PDFAnonymous h0DxuJTNo ratings yet
- ThoraventDocument7 pagesThoraventadamNo ratings yet
- Middle East Respiratory Syndrome Coronavirus (MERS-CoV)Document24 pagesMiddle East Respiratory Syndrome Coronavirus (MERS-CoV)Nurul Falah KalokoNo ratings yet
- Nej Mo A 1507807Document11 pagesNej Mo A 1507807Leiniker NavarroNo ratings yet
- US Pulmón para Manejo de Atelectasias PerioperatoriasDocument11 pagesUS Pulmón para Manejo de Atelectasias PerioperatoriasJURAGOMANo ratings yet
- PRVC in COPDDocument8 pagesPRVC in COPDwandapandabebeNo ratings yet
- 859 FullDocument6 pages859 FullAdif FlysNo ratings yet
- BRS GS Compilation HIGHLIGHTEDDocument108 pagesBRS GS Compilation HIGHLIGHTEDJaney T.No ratings yet
- Cryobiopsy in ARDSDocument88 pagesCryobiopsy in ARDSChih-Hao ChangNo ratings yet
- Asthma: Further ReadingDocument13 pagesAsthma: Further ReadingcarlosNo ratings yet
- Bedside Lung Ultrasound in The Assessment of Alveolar-Interstitial SyndromeDocument8 pagesBedside Lung Ultrasound in The Assessment of Alveolar-Interstitial SyndromemrwgNo ratings yet
- Clin Infect Dis. 1996 Eriksson 1091 8Document8 pagesClin Infect Dis. 1996 Eriksson 1091 8zul090No ratings yet
- AMJ-Volume 50-Issue 2 - Page 1489-1496Document8 pagesAMJ-Volume 50-Issue 2 - Page 1489-1496Pandu Putra Wijaya RestaNo ratings yet
- Streptokinase in The Treatment of Pleural Controlled Trial of IntrapleuralDocument7 pagesStreptokinase in The Treatment of Pleural Controlled Trial of IntrapleuraltomgasoneNo ratings yet
- Pi Is 0954611120300433Document7 pagesPi Is 0954611120300433Akbar SyarialNo ratings yet
- Performance and Safety of Diagnostic Procedures in Superior Vena Cava SyndromeDocument4 pagesPerformance and Safety of Diagnostic Procedures in Superior Vena Cava SyndromesukiyantoNo ratings yet
- SMW 10050Document8 pagesSMW 10050lapulga10No ratings yet
- Jurnal 3Document5 pagesJurnal 3Caesar RiefdiNo ratings yet
- Depiction Control: ECG Prognostic Significance of ECG Changes in Acute PneumoniaDocument5 pagesDepiction Control: ECG Prognostic Significance of ECG Changes in Acute PneumoniaAudrey Martin RañisesNo ratings yet
- GJHS 6 221Document5 pagesGJHS 6 221Teuku FaisalNo ratings yet
- TID 9999 E13413Document5 pagesTID 9999 E13413saraabolghasemi1No ratings yet
- Pulmonary Endarterectomy: Experience and Lessons Learned in 1,500 CasesDocument8 pagesPulmonary Endarterectomy: Experience and Lessons Learned in 1,500 CasesRoxana Maria MunteanuNo ratings yet
- Parallel Technique of Endobronchial Balloon Catheter Tamponade For Transient Alleviation of Massive HemoptysisDocument3 pagesParallel Technique of Endobronchial Balloon Catheter Tamponade For Transient Alleviation of Massive HemoptysisNadia Mrz Mattew MuseNo ratings yet
- Spontaneous Pneumothorax: New Horizons: Avinash AujayebDocument4 pagesSpontaneous Pneumothorax: New Horizons: Avinash AujayebAnangova PradiptaNo ratings yet
- Surgical Management CPA PediatricDocument3 pagesSurgical Management CPA PediatricIndah Nur LathifahNo ratings yet
- Duplex Guided Balloon Angioplasty and Subintimal DDocument8 pagesDuplex Guided Balloon Angioplasty and Subintimal DJose PiulatsNo ratings yet
- Radiological Findings of Unilateral Tuberculous LuDocument7 pagesRadiological Findings of Unilateral Tuberculous LuSarah watiNo ratings yet
- De Neuville 2000Document5 pagesDe Neuville 2000Anonymous WPiPld6npNo ratings yet
- Emergent Management of Empyema: Osman Ahmed, M.D. Steven Zangan, M.DDocument5 pagesEmergent Management of Empyema: Osman Ahmed, M.D. Steven Zangan, M.Dmarce39No ratings yet
- Left Bronchus SyndromeDocument3 pagesLeft Bronchus SyndromephobicmdNo ratings yet
- Pulmonary Histoplasmosis Presenting With A Halo Sign On CT in An Immunocompetent PatientDocument2 pagesPulmonary Histoplasmosis Presenting With A Halo Sign On CT in An Immunocompetent PatientSharom R. AlvarezNo ratings yet
- Thorax00193 0009 PDFDocument10 pagesThorax00193 0009 PDFhotmart ventasNo ratings yet
- A Case of Pulmonary Aspergilloma and ActinomycosisDocument4 pagesA Case of Pulmonary Aspergilloma and ActinomycosisNova PurbaNo ratings yet
- Anesthesia in Thoracic Surgery: Changes of ParadigmsFrom EverandAnesthesia in Thoracic Surgery: Changes of ParadigmsManuel Granell GilNo ratings yet
- Your Electronic Ticket Receipt-7Document2 pagesYour Electronic Ticket Receipt-7rynaldiandriansyaNo ratings yet
- Anal DilationDocument3 pagesAnal DilationrynaldiandriansyaNo ratings yet
- App AnakDocument22 pagesApp AnakrynaldiandriansyaNo ratings yet
- SC FractureDocument21 pagesSC FracturerynaldiandriansyaNo ratings yet
- Rectal Biopsy (Suction Procedure) : AppointmentDocument2 pagesRectal Biopsy (Suction Procedure) : AppointmentrynaldiandriansyaNo ratings yet
- Picu Nicu 6 Maret 2014Document4 pagesPicu Nicu 6 Maret 2014rynaldiandriansyaNo ratings yet
- Case Report Team of Duty: Dr. Hendra KastiajiDocument3 pagesCase Report Team of Duty: Dr. Hendra KastiajirynaldiandriansyaNo ratings yet
- Canadian Medical Report FormsDocument6 pagesCanadian Medical Report FormsshichunNo ratings yet
- AMYLOIDOSISDocument50 pagesAMYLOIDOSISLavanya KalapalaNo ratings yet
- Jurnal Reading OsteomyelitisDocument11 pagesJurnal Reading Osteomyelitisfidela_ffNo ratings yet
- Gastroenteritis Case ReportDocument12 pagesGastroenteritis Case ReportjisooNo ratings yet
- Taxvantage Plus Medical Plan: | 自願醫保 Vhis |Document24 pagesTaxvantage Plus Medical Plan: | 自願醫保 Vhis |Tomei LauNo ratings yet
- CIDI-based Screening Scale For Bipolar Spectrum Disorders - : Clinical UtilityDocument4 pagesCIDI-based Screening Scale For Bipolar Spectrum Disorders - : Clinical UtilityJagdishVankarNo ratings yet
- Site Preservation Decision TreeDocument8 pagesSite Preservation Decision TreeHaoWangNo ratings yet
- Women and Birth: Michelle GrayDocument8 pagesWomen and Birth: Michelle Grayzimbabwe kuvukilandNo ratings yet
- About MemoryDocument44 pagesAbout MemoryGegiuc GabrielaNo ratings yet
- Cough N Cold Medicine List PDFDocument7 pagesCough N Cold Medicine List PDFDonna DominnoNo ratings yet
- Alteration in Respiratory SystemDocument138 pagesAlteration in Respiratory Systemcute_gurljhoanNo ratings yet
- Medical Utopias: Ethical Reflections About Emerging Medical TechnologiesDocument35 pagesMedical Utopias: Ethical Reflections About Emerging Medical TechnologiesKPJConferenceNo ratings yet
- What Is The NPI?Document11 pagesWhat Is The NPI?Naresh ReddyNo ratings yet
- Roles and Responsibilities of Geriatric Nurse in CommunityDocument4 pagesRoles and Responsibilities of Geriatric Nurse in CommunityAKHILA PKNo ratings yet
- TASK 11 - Yulia Indri FebrianiDocument4 pagesTASK 11 - Yulia Indri FebrianiindriNo ratings yet
- Nursing Care Plan Clubfoot or Talipes EquinovarusDocument6 pagesNursing Care Plan Clubfoot or Talipes EquinovarusMarzie LugtuNo ratings yet
- Process Recording With RubricDocument8 pagesProcess Recording With RubricAndrew GarskeNo ratings yet
- Informed Consent Document Template and Guidelines Informed Consent Form (Name of Institution)Document14 pagesInformed Consent Document Template and Guidelines Informed Consent Form (Name of Institution)Shondra D. BryantNo ratings yet
- 2010 - 2016 With AnswersDocument806 pages2010 - 2016 With AnswersIbrahim Abueltaif83% (6)
- Endometrial BiopsyDocument72 pagesEndometrial BiopsySatish TatamiyaNo ratings yet
- Flail ChestDocument26 pagesFlail ChestStawan ChouguleNo ratings yet
- Transcript Peter Saul Lets Talk About DyingDocument3 pagesTranscript Peter Saul Lets Talk About DyingDiogo MulderNo ratings yet
- TB 1716986horaDocument5 pagesTB 1716986horasanil kumarNo ratings yet
- Aciclovir 400mg and 800mg TabletsDocument2 pagesAciclovir 400mg and 800mg TabletsKalyan NandanNo ratings yet
- Precinorm U Plus.12173581001.v10.en PDFDocument2 pagesPrecinorm U Plus.12173581001.v10.en PDFARIF AHAMMED P0% (1)
- Models of Health and Health PromotionDocument16 pagesModels of Health and Health Promotionapi-31127039450% (2)
- Pain Scale For ThesisDocument4 pagesPain Scale For ThesisREMILYN ROSE ASUNCIONNo ratings yet
Iaet07i1p23 2 PDF
Iaet07i1p23 2 PDF
Uploaded by
rynaldiandriansyaOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Iaet07i1p23 2 PDF
Iaet07i1p23 2 PDF
Uploaded by
rynaldiandriansyaCopyright:
Available Formats
Original Article
Surgical Treatment of Pulmonary Aspergilloma: A Series
of 72 Cases
Himanshu Pratap1, R.K. Dewan1, L. Singh1, S. Gill1 and S. Vaddadi2
Departments of Thoracic Surgery1 and Pulmonary Medicine2, LRS Institute of Tuberculosis and Respiratory
Diseases, New Delhi, India
ABSTRACT
Background. The objective of this study was to evaluate the immediate and long term result of resectional surgery in
pulmonary aspergilloma.
Methods. Seventy-two patients who underwent pulmonary resectional surgery for symptomatic aspergilloma between 1990
to 2002 were studied. Seventy-nine definitive operations were carried out, including one bilateral lobectomy for recurrent
lesions and six thoracoplasties to deal with post-operative complications, besides 21 pneumonectomies and 51 lobectomies.
There were 10 bilobectomies as well, included in the lobectomy group.
Results. At a mean follow-up of 3.5 years, there were two post-operative deaths and a few complications occurred in 20 cases
translating into a morbidity of 28.57% and a mortality of 2.77 percent. Major complications included were persistent air leak,
persistent pleural space, empyema, bronchopleural fistula and massive haemorrhage. All events were seen in cases of
complex aspergilloma; cases of simple aspergillomas had an uneventful course.
Conclusions. Surgery offers definitive and long term symptom-free survival in cases of pulmonary aspergilloma at a
negligible risk; though almost one-third of those undergoing surgery develop some complications, these are largely
manageable. [Indian J Chest Dis Allied Sci 2007; 49: 23-27]
Key words: Aspergilloma, Pulmonary, Tuberculosis, Surgery.
INTRODUCTION
Pulmonary aspergilloma, the so-called fungus ball or
mycetoma, is a clinical syndrome of worldwide
presence and represents one of the many manifestations
of human disease due to the fungus Aspergillus. These
include asymptomatic inconsequential presence in
healthy hosts, chronic necrotising aspergillosis in
patients with chronic lung disease, invasive
aspergillosis in immunocompromised hosts and allergic
bronchopulmonary aspergillosis in asthmatics.1 The
term aspergilloma refers to colonisation of pre-existing
lung cavities with the Aspergillus fungus, most
commonly the fumigatus species, and the lesion itself
consists of a tangled mass of fungal hyphae, fibrin,
epithelial cells, mucus, debris and blood cells. 2
Tubercular lesions are the most common cause of such
cavities although aspergillomas may occur within
cavities of diverse aetiologies including sarcoidosis,
bronchiectasis, cysts and bullae, neoplasms, ankylosing
spondylitis, Wegeners granulomatosis, and pulmonary
infraction.1 Though the natural history of such a lesion
is not completely understood, it has the propensity to
cause recurrent and severe haemoptysis; besides, when
super infected, the illness runs a distressing and
protracted course.3
Pulmonary aspergilloma is the only surgically
relevant manifestation of Aspergillus infection and
though known for a century- and-a-half now, controversy still surrounds its optimal management. 1-3 The
controversy surrounds the surgical management stems
from the perceived threat of morbidity and mortality
consequent to surgery and it has led to
recommendations of surgery only as a last resort,5 or
restricted to symptomatic cases only6,7 or an option for
all cases to preempt massive haemoptysis.8-10
In this paper we are presenting a series of 72 cases of
pulmonary aspergilloma treated surgically at our centre
over the last 12 years, to evaluate our indications and
results.
MATERIAL AND METHODS
During a 12-year period from 1990 to 2002, 72 patients
underwent surgery for pulmonary aspergilloma at LRS
Institute of Tuberculosis and Respiratory Diseases in the
[Received: June 26, 2006; accepted after revision: September 22, 2006]
Correspondence and reprint requests: Dr R.K. Dewan, Head, Department of Thoracic Surgery, LRS Institute of TB and
Respiratory Diseases, Sri Aurobindo Marg, Mehrauli, New Delhi-110 030, India; E-mail: ravindrakdewan@rediffmail.com.
24
Surgery for Aspergilloma
Department of Thoracic Surgery. The patients records
were retrieved and 72 consecutive cases were studied
with reference to clinical profile, radiological findings,
indications of surgery, surgical procedures used and
short- and long-term post-operative outcomes. There
were 47 male and 25 female patients in the age group of
26 to 58 years (mean 32 years).
Overall, 79 definitive surgical procedures were
carried out, including six thoracoplasties to deal with
post-operative complications but in one patient bilateral
lobectomy was done for recurrent disease. All the cases
were operated under general anaesthesia, with doublelumen endotracheal tubes in situ for adequate isolation
and selective ventilation, through standard posterolateral thoracotomy. Considerable adhesions were seen
in all of our cases and significant intraoperative
haemorrhage occurred despite liberal use of
electrocautery. In four cases, we had to resect portions of
3rd and 4th ribs when densely adherent to the lesions
and in two cases we had to resort to intrapericardial
ligation of pulmonary vessels as the extra pericardial
hilum was unapproachable. In most of the cases we
developed the extra pleural plane between the parietal
pleura and chest wall to dissect along the endothoracic
fascia, but the apical region nevertheless demanded
considerable patience and, despite best efforts, in one
patient massive intraoperative haemorrhage led to
death shortly after the operation.
Himanshu Pratap et al
Table. Clinical and radiological features of the cases
A. Clinical Presentation
Haemoptysis
Moderate
Severe
Massive
Chronic productive cough
Fever, chest pain, dyspnoea
B. Radiological Presentation
(a) Appearance
Destroyed one lung with aspergilloma
shown on CECT
Cavitatory lesion with air crescent sign
Localised bronchiectatic lesion with
aspergilloma shown on CECT
(b) Location
Right destroyed lung
Left destroyed lung
Left upper lobar lesion
Right upper lobar lesion
Left lower lobar lesion
47 (65.28%)
20
15
12
17 (23.61%)
08 (11.11%)
21
42
09
14
07
20
18
12
RESULTS
Clinical Profiles
The patients were largely admitted for the evaluation of
haemoptysis, some cases complained of chronic
productive cough, while a few cases had suffered from
fever, chest pain and dyspnoea. The severity of
haemoptysis was categorised as moderate, severe and
massive depending upon whether the amount of
bleeding over a 24-hour period was less than 150 ml,
150 to 300 ml or more than 300 ml respectively. The
clinical and radiological presentation of the cases are
summarised in the table.
Radiological findings and other diagnostic
methods
During evaluation, the diagnosis of aspergilloma was
made primarily on the radiological examination
showing fungus-ball on plain chest radiograph and
demonstration of lung parenchymal cavity with free
ball-lesion on computerised tomography (Figures 1-3).
The aspergillomas were classified into two sub-groups,
viz. simple aspergilloma (thin-walled cavity; no
parenchymal/pleural disease) and complex
aspergilloma (thick-walled cavity; associated
parenchymal/pleural disease) for prognostic purpose.
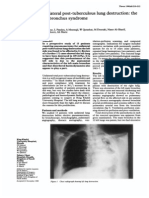
Figure 1. Chest radiograph (PA view) demonstrating classical air
crescent sign in right upper zone of lung.
There were eight cases of simple aspergillomas while
the rest were complex lesions. Complex aspergilloma
may be part of chronic necrotising pulmonary
aspergillosis as its clinical symptoms may progress to a
severe form.17 Radiological findings in relevant cases are
presented in the table. Fiberoptic bronchoscopy was
performed in 42 cases and aspergillus species was
documented in 16 such cases. In all cases
immunoelectrophoreses on agar gel were requested to
2007; Vol. 49
The Indian Journal of Chest Diseases & Allied Sciences
Figure 2. Contrast enhanced computerised tomographic scan of
thorax revealing aspergilloma left lung.
Figure 3. The 3-D reconstituted image of the same patient as in
figure 2.
demonstrate the presence of precipitating antibodies.
Positive serological results were obtained in 59 cases.
Pre-existing Lesions
The underlying pathological lesions responsible for the
fungal growth were tubercular cavities in 61 cases
(84.72%) while bronchiectatic cavities contained
aspergillus in nine cases and old pyogenic lung abscess
was the culprit in the remaining two cases.
Indications and Types of Surgery
The patients were evaluated and surgery was offered.
The extent of surgery was determined by the degree of
involvement of the parenchyma and functional reserve
of the patient. In all, 21 pneumonectomies and 51
lobectomies were performed; in 10 of the right upper
lobe lesions bilobectomies were done, by removing both
25
the right upper and middle lobes, due to presence of
adhesions.
Spirometric threshold of resectional surgery was
primarily based on forced vital capacity, forced
expiratory volume in one second (FEV1) and maximum
voluntry ventilation along the usual guidelines and
thoracotomy was offered so long as predicted postoperative FEV 1 exceeded 40 percent. The resected
specimens were routinely sent for histopathology and
fungal culture and confirmation of diagnoses was thus
obtained. In this series, the average blood loss during
surgery was 850 ml (350-2000 ml) during pneumonectomy and 550 ml (200-1500 ml) during lobectomy.
The mean quantity drained over first 24 hours was 600
ml (500-1000 ml) after lobectomy and 800 ml (500-1200
ml) after pneumonectomy. Massive haemorrhage was
defined as a blood loss exceeding 1500 ml over 24 hours.
Post-operative Course
Post-operative course was uneventful in 50 out of 70
cases. Two patients died, while complications
developed in 20 cases; thus morbidity rate in this series
was 28.6 percent. All the complications were observed
in cases of complex aspergilloma only. Post-operative
courses were complicated in lobectomy cases, by
persistent air leak exceeding 10 days in five cases and
persistent pleural space in three of the pneumonectomy
cases converting into empyemas. Massive haemorrhage
occurred in three lobectomy and two pneumonectomy
cases. Air leaks responded to prolonged tube drainage
in three cases and two patients required thoracoplasty.
Empyemas were managed with thoracostomy and local
irrigation and resolved over one to three months. Post
pneumonectomy empyemas were managed by
thoracostomy and irrigation initially and secondary
thoracoplasty after the patient regained reasonable
health. Persistent pleural spaces reflected insufficient
compensatory hyperinflation of the remaining
pulmonary parenchyma. These in the absence of air leak
or pleural space infection did not require treatment and
were managed conservatively. However, in one case,
thoracoplasty was performed. Thus, overall, six
thoracoplasties were performed preceded by
thoracostomy in three post-pneumonectomy cases.
Massive haemorrhages were treated with blood
transfusion and volume replacement.
Overall there were two deaths, one due to massive
intraoperative bleed and the other due to non-resolving
pneumonia on 15th post-operative day, leading on to
respiratory failure and death.
Follow-up was completed in 59 cases for a mean
period of 3.5 years, and in the 12 to 40 years range we
encountered two recurrences. One patient who had a
lobectomy earlier, was treated with contralateral
lobectomy and the other is being managed
conservatively for mild episodic haemoptysis, who
refused for surgery.
26
Surgery for Aspergilloma
DISCUSSION
Aspergillus fumigatus, the commonest agent of
aspergilloma, is a saprophytic fungus ubiquitously
present over dead and decaying surfaces. In healthy
hosts, it produces no disease. When it colonises a preexisting pulmonary cavity, mycetoma or aspergilloma
forms.1-3 Natural history of aspergilloma varies from a
stable lesion to progression and even spontaneous
regression is reported in about 5% cases.11,12 Predicted
mortality due to aspergilloma is reported at a rate of 6%
per annum.11 A definitive diagnosis is established by
histopathological examination and culture of the
involved tissue but is largely entertained on the basis of
characteristic radiological demonstration of fungal
ball.1,2,15 Sputum isolation has doubtful specificity given
frequent airway colonisation. 1-3
Serological diagnosis has reasonably good sensitivity
and specificity but has limited clinical importance in a
typical scenario. In our series, as is usually the case,
radiology formed the basis of diagnosis. In addition,
culture of the resected specimen was always obtained.
Aspergilloma manifests either as an incidental
radiological finding or causes haemoptysis that can be
massive, or recurrent and, indeed, fatal and reportedly
complicates 50% to 80% of cases. 13 In our series it
formed the basis of treatment in over 65% cases as also
reported earlier.1-3 Underlying postulated mechanisms
of haemoptysis include erosion of vascular cyst wall by
the movement of ball, elaboration of trypsin-like
substance or endotoxins by the fungus, type III antigenantibody reaction or the underlying lung disease
itself.9,13 The bleeding is commonly from the bronchial
arteries and frequently remits on its own. Very rare
instances of first episode fatal bleed have been reported
and are presumed to occur from intercostal vessels. 14
Patients presenting to us, including those with severe
haemoptysis, could all be managed conservatively with
bed rest, antitussives, antifibrinolytics and blood
transfusion. We did not encounter any fatal first bleed
nor was any emergency surgery or arterial embolisation
deemed necessary, though we generally operated such
cases on a priority basis. Size and location of the lesion
do not bear any relation to the severity of bleeding. 17 It
was noted that upper lobes of lungs were the favoured
site of aspergillomas.12 Though Bennet first reported a
case as long back as in 1842 and Gerstle and colleagues12
reported a lobectomy in 1947, the best treatment of
aspergilloma has remained contentious.12,13 Review of
literature reveals that the major obstacle to acceptance of
surgery as the treatment has been the high mortality
and morbidity consequent to surgery. The surgery is the
only definitive modality of treatment is now a well
established and non-debatable issue. Drug therapy of
aspergilloma has highly inconsistent and largely
incomplete results though antifungal therapy has been
used by various routes like oral, intravenous and,
Himanshu Pratap et al
topical.1,3,12,13 We have not used antifungal treatment at
our institution. However, according to some authors,
successful treatment of complex aspergilloma needs
both surgery and perioperative drug therapy. At present
amphotericin B (1.01.5 mgm/kg/day), 5flucytosine
(5FC, 100-150 mgm/kg/day), itraconazole (ITCZ, 200400 mgm/day) and micafungin (MCFG, 150-300 mgm/
day i.v.) are used. Recently caspofungin (CAP) has been
utilised. Therefore, combination therapy has attracted
increasing attention. Slowly growing aspergilloma may
be kept under observation.17
Bronchial artery embolisation is another modality
that has similar dubious long-term effects and perhaps
represents a temporising measure at best 1 and we
strongly feel that its use should be restricted to massive
and haemodynamically significant bleeds, in surgical
unfit cases or cases where surgery can not be offered or
is rejected.
Surgery, not only offers symptomatic control but also
confers survival advantage3,12 and is being used even in
asymptomatic cases to preempt massive bleed and
death.4,13 A marked decline in mortality and morbidity
due to surgery has led to its greater acceptance in recent
years. Procedural death has seen a significant decline
from 07-23% to 1.5-04% of late.13,15 In our series, there
were only two deaths. As respiratory failure tops the list
of causes of post-operative deaths in various reports,
judicious selection of cases and appraisal of respiratory
functional reserve of the patient is important. Postoperative complications, however, still remain the
Achilles heel of surgical management. The spectrum of
complications noted in our series is similar to that
reported in other series, with the difference that
haemorrhage was ranked the highest in our series,
perhaps due to the fact that most of our cases were
complex aspergillomas and hence adhesions were
present in all the cases.
Over the years the post-operative complications have
also shown a downward trend, though not as steep as
with the mortality. In 1997 Chen et al 15 reported a
morbidity of 17.9% whereas most recently Akbari et al16
have reported a complication rate of 26.1 percent. In
various other reports in the last decade, complications
have occurred in 20% to 30% cases. 7, 13 In the current
series, the post-operative course was complicated in
28.6 percent. All the complications in our series were
seen in complex aspergillomas. Simple aspergillomas
have had no mortality and morbidity. This compares
favourable with the series reported by Akbari et al.16
This is understandable, given the fact that,
complications largely result from dense vascular
adhesions or incomplete lung expansion.
In conclusion, we believe that surgery can be carried
out to treat pulmonary aspergilloma with negligible
mortality and acceptable morbidity. However, in the
absence of definite knowledge regarding its natural
history and, given the fact that morbidity remains a
2007; Vol. 49
The Indian Journal of Chest Diseases & Allied Sciences
nagging issue, resectional surgery should be advised
judiciously and it may seem prudent to treat the
consequences, rather than the presence of the lesion.
9.
10.
REFERENCES
11.
1.
2.
3.
4.
5.
6.
7.
8.
Soubani AO, Chandrasekar PH. The clinical spectrum of
pulmonary aspergillosis. Chest 2002; 121: 1988-99.
Daly P, Kavanagh K. Pulmonary aspergillosis: clinical
presentation, diagnosis and therapy. Br J Biomed Sci 2001; 58:
197-205.
Ueda H, Okabayashi K, Ondo K, Motohiro A. Analysis of
various treatment for pulmonary aspergillomas. Surg Today
2001; 31: 768-73.
Park KP, Jheon S. Results of surgical treatment for pulmonary
aspergilloma. Eur J Cardiothorac Surg 2002; 21: 918-23.
Karas A, Hankins JR, Attar S, Miller JE, Mlaughlin JS.
Pulmonary aspergilloma: an analysis of 41 patients. Ann
Thorac Surg 1976; 22: 1-7.
Battaglini JW, Murray GF, Keagy BA, Starek PJK, Wilcox BR.
Surgical management of symptomatic pulmonary
aspergilloma. Ann Thorac Surg 1985; 39: 512-6.
Daly RC, Pairolero PC, Piehler JM, Trastek VF, Payne WS,
Bernatz PE. Pulmonary aspergilloma: results of surgical
treatment. J Thorac Cardiovasc Surg 1986; 92: 981-8.
Massard G, Roeslin N, Wihlm JM, Dumont P, Witz JP,
Morand G. Pleuropulmonary aspergilloma: clinical spectrum
and results of surgical treatment. Ann Thorac Surg 1992; 54:
12.
13.
14.
15.
16.
17.
27
1159-64.
Solit RW, McKeown JJ, Smullens S, Fraimow W. The surgical
implications of intracavitary mycetomas (fungus balls). J
Thorac Cardiovasc Surg 1971; 62: 411-22.
Pecora DV, Toll MW. Pulmonary resection for localized
aspergillosis. N Engl J Med 1960; 263: 785-7.
British Thoracic and Tuberculosis Association. Aspergilloma
and residual tuberculous cavities: the results of re-survey.
Tubercle 1970; 51: 227-45.
Jewkes J, Kay PH Paneth M, Citorn KM. Pulmonary
aspergilloma: analysis of prognosis in relation to hemoptysis
and survey of treatment. Thorax 1983; 38: 572-8.
Babatasi G, Massetti M, Chapelier A, Fadel E, Macchiarini M,
Khayat A, et al. Surgical treatment of pulmonary
aspergilloma: current outcome. J Thorac Cardiovasc Surg 2000;
119: 906-12.
Young VK, Maghur HA, Luke DA, McGovern EM. Operation
for cavitating invasive pulmonary aspergillosis in
immunocompromised patients. Ann Thorac Surg 1992; 53:
621-4.
Chen JC, Chang YL, Luh SP, Lee YC. Surgical treatment for
pulmonary aspergilloma: a 28-year experience. Thorax 1997;
52: 810-13.
Akbari JG, Varma PK, Neema PK, Menon MU,
Neelakandhan KS. Clinical profile and surgical outcome for
pulmonary aspergilloma: a single centre experience. Ann
Thorac Surg 2005; 80: 1067-72.
Ando T, Shibuya K. Clinical management of pulmonary
aspergillosis. JMAJ 2005; 48: 601-6.
28
The Indian Journal of Chest Diseases & Allied Sciences
Full text articles published in IJCDAS from July-September
2003 onwards can be accessed online on Internet through the
following sites
V.P. Chest Institutes site: http://www.vpci.org.in
Indmeds site: http://medind.nic.in
Guidance for Authors appears in every issue.
Authors Index appears in the last issue of the year
2007; Vol. 49
You might also like
- TNCC NotesDocument9 pagesTNCC NotesJessie Bronkalla95% (21)
- Reclaiming Your Life From A Traumatic Experience: Workbook - Rothbaum, Edna B. Foa, HembreeDocument105 pagesReclaiming Your Life From A Traumatic Experience: Workbook - Rothbaum, Edna B. Foa, Hembreedoppler_100% (8)
- Maternal and Child Health Nursing ReviewerDocument17 pagesMaternal and Child Health Nursing ReviewerJeffrey Viernes100% (6)
- Aspergilloma MoroccoDocument5 pagesAspergilloma MoroccoYassine EssNo ratings yet
- Surgical Therapy For Necrotizing Pneumonia and Lung Gangrene PDFDocument6 pagesSurgical Therapy For Necrotizing Pneumonia and Lung Gangrene PDFmichael24kNo ratings yet
- RadiopediaDocument4 pagesRadiopediakennyNo ratings yet
- HemoptisisDocument7 pagesHemoptisiswiliaNo ratings yet
- Abstrak SederhanaDocument2 pagesAbstrak Sederhanaabsensi paruNo ratings yet
- Reseccion Pulmonar en Hemoptisis SeveraDocument10 pagesReseccion Pulmonar en Hemoptisis SeverarafodocNo ratings yet
- Chronic Pulmonary Aspergillosis: A Frequent and Potentially Severe DiseaseDocument5 pagesChronic Pulmonary Aspergillosis: A Frequent and Potentially Severe Diseasemedicina146No ratings yet
- Etm 13 5 2259 PDFDocument4 pagesEtm 13 5 2259 PDFdicky nanda muzidaNo ratings yet
- Management of Non-Tumoral Tracheal Stenosis in 112 Patients EDocument5 pagesManagement of Non-Tumoral Tracheal Stenosis in 112 Patients Ezed-medNo ratings yet
- Curren Clinical Propensity of TB LaringDocument5 pagesCurren Clinical Propensity of TB LaringDevi DaryaningsihNo ratings yet
- Simultaneous Bilateral Primary Spontaneous Pneumothorax (2019)Document7 pagesSimultaneous Bilateral Primary Spontaneous Pneumothorax (2019)sandi_prawira_yudhaNo ratings yet
- Pulmonary Pathological Features in Coronavirus Associated Severe Acute Respiratory Syndrome (SARS)Document6 pagesPulmonary Pathological Features in Coronavirus Associated Severe Acute Respiratory Syndrome (SARS)Leandro VillamilNo ratings yet
- Maiwand Asimakopoulos 2004 Cryosurgery For Lung Cancer Clinical Results and Technical AspectsDocument8 pagesMaiwand Asimakopoulos 2004 Cryosurgery For Lung Cancer Clinical Results and Technical Aspectsbjro1986No ratings yet
- Chronic Cavitary and Fibrosing Pulmonary and Pleural Aspergillosis: Case Series, Proposed Nomenclature Change, and ReviewDocument16 pagesChronic Cavitary and Fibrosing Pulmonary and Pleural Aspergillosis: Case Series, Proposed Nomenclature Change, and ReviewYassine EssNo ratings yet
- Ecmo 2000Document13 pagesEcmo 2000Maria PaulaNo ratings yet
- 2008 Chest - The Blue ProtocolDocument9 pages2008 Chest - The Blue Protocoleduardo0% (1)
- Empyema ThoracisDocument6 pagesEmpyema ThoracisThine NG CalderonNo ratings yet
- (1992) Yang, Pan-Chyr Luh, Kwen-Tay Chang, Dun-Bing Yu, Chong-Jen K - Ultrasonographic Evaluation of Pulmonary ConsolidationDocument6 pages(1992) Yang, Pan-Chyr Luh, Kwen-Tay Chang, Dun-Bing Yu, Chong-Jen K - Ultrasonographic Evaluation of Pulmonary ConsolidationPer DamiánNo ratings yet
- Pulmonary Nodules and Masses After Lung and Heart-Lung TransplantationDocument7 pagesPulmonary Nodules and Masses After Lung and Heart-Lung TransplantationManisha UppalNo ratings yet
- JurnalDocument8 pagesJurnalwiliaNo ratings yet
- Management of Anastomotic Complications After Sleeve Lobectomy For Lung CancerDocument4 pagesManagement of Anastomotic Complications After Sleeve Lobectomy For Lung CancerJovelyn SagangNo ratings yet
- Bilat Ten Pneumo Improv 0214 p20 24Document5 pagesBilat Ten Pneumo Improv 0214 p20 24juliusNo ratings yet
- Emphysema Versus Chronic Bronchitis in COPD: Clinical and Radiologic CharacteristicsDocument8 pagesEmphysema Versus Chronic Bronchitis in COPD: Clinical and Radiologic CharacteristicsChairul Nurdin AzaliNo ratings yet
- Saddle Pulmonary Embolism: A Rare Case of Proximal Pulmonary EmbolismDocument3 pagesSaddle Pulmonary Embolism: A Rare Case of Proximal Pulmonary EmbolismIJAR JOURNALNo ratings yet
- Pneumothorax in Active Pulmonary Tuberculosis: Resurgence of An Old Complication?Document5 pagesPneumothorax in Active Pulmonary Tuberculosis: Resurgence of An Old Complication?M Tata SuhartaNo ratings yet
- Medip, IJOHNS-388 ODocument6 pagesMedip, IJOHNS-388 Onaveed gulNo ratings yet
- 712 PDFDocument74 pages712 PDFAnonymous h0DxuJTNo ratings yet
- ThoraventDocument7 pagesThoraventadamNo ratings yet
- Middle East Respiratory Syndrome Coronavirus (MERS-CoV)Document24 pagesMiddle East Respiratory Syndrome Coronavirus (MERS-CoV)Nurul Falah KalokoNo ratings yet
- Nej Mo A 1507807Document11 pagesNej Mo A 1507807Leiniker NavarroNo ratings yet
- US Pulmón para Manejo de Atelectasias PerioperatoriasDocument11 pagesUS Pulmón para Manejo de Atelectasias PerioperatoriasJURAGOMANo ratings yet
- PRVC in COPDDocument8 pagesPRVC in COPDwandapandabebeNo ratings yet
- 859 FullDocument6 pages859 FullAdif FlysNo ratings yet
- BRS GS Compilation HIGHLIGHTEDDocument108 pagesBRS GS Compilation HIGHLIGHTEDJaney T.No ratings yet
- Cryobiopsy in ARDSDocument88 pagesCryobiopsy in ARDSChih-Hao ChangNo ratings yet
- Asthma: Further ReadingDocument13 pagesAsthma: Further ReadingcarlosNo ratings yet
- Bedside Lung Ultrasound in The Assessment of Alveolar-Interstitial SyndromeDocument8 pagesBedside Lung Ultrasound in The Assessment of Alveolar-Interstitial SyndromemrwgNo ratings yet
- Clin Infect Dis. 1996 Eriksson 1091 8Document8 pagesClin Infect Dis. 1996 Eriksson 1091 8zul090No ratings yet
- AMJ-Volume 50-Issue 2 - Page 1489-1496Document8 pagesAMJ-Volume 50-Issue 2 - Page 1489-1496Pandu Putra Wijaya RestaNo ratings yet
- Streptokinase in The Treatment of Pleural Controlled Trial of IntrapleuralDocument7 pagesStreptokinase in The Treatment of Pleural Controlled Trial of IntrapleuraltomgasoneNo ratings yet
- Pi Is 0954611120300433Document7 pagesPi Is 0954611120300433Akbar SyarialNo ratings yet
- Performance and Safety of Diagnostic Procedures in Superior Vena Cava SyndromeDocument4 pagesPerformance and Safety of Diagnostic Procedures in Superior Vena Cava SyndromesukiyantoNo ratings yet
- SMW 10050Document8 pagesSMW 10050lapulga10No ratings yet
- Jurnal 3Document5 pagesJurnal 3Caesar RiefdiNo ratings yet
- Depiction Control: ECG Prognostic Significance of ECG Changes in Acute PneumoniaDocument5 pagesDepiction Control: ECG Prognostic Significance of ECG Changes in Acute PneumoniaAudrey Martin RañisesNo ratings yet
- GJHS 6 221Document5 pagesGJHS 6 221Teuku FaisalNo ratings yet
- TID 9999 E13413Document5 pagesTID 9999 E13413saraabolghasemi1No ratings yet
- Pulmonary Endarterectomy: Experience and Lessons Learned in 1,500 CasesDocument8 pagesPulmonary Endarterectomy: Experience and Lessons Learned in 1,500 CasesRoxana Maria MunteanuNo ratings yet
- Parallel Technique of Endobronchial Balloon Catheter Tamponade For Transient Alleviation of Massive HemoptysisDocument3 pagesParallel Technique of Endobronchial Balloon Catheter Tamponade For Transient Alleviation of Massive HemoptysisNadia Mrz Mattew MuseNo ratings yet
- Spontaneous Pneumothorax: New Horizons: Avinash AujayebDocument4 pagesSpontaneous Pneumothorax: New Horizons: Avinash AujayebAnangova PradiptaNo ratings yet
- Surgical Management CPA PediatricDocument3 pagesSurgical Management CPA PediatricIndah Nur LathifahNo ratings yet
- Duplex Guided Balloon Angioplasty and Subintimal DDocument8 pagesDuplex Guided Balloon Angioplasty and Subintimal DJose PiulatsNo ratings yet
- Radiological Findings of Unilateral Tuberculous LuDocument7 pagesRadiological Findings of Unilateral Tuberculous LuSarah watiNo ratings yet
- De Neuville 2000Document5 pagesDe Neuville 2000Anonymous WPiPld6npNo ratings yet
- Emergent Management of Empyema: Osman Ahmed, M.D. Steven Zangan, M.DDocument5 pagesEmergent Management of Empyema: Osman Ahmed, M.D. Steven Zangan, M.Dmarce39No ratings yet
- Left Bronchus SyndromeDocument3 pagesLeft Bronchus SyndromephobicmdNo ratings yet
- Pulmonary Histoplasmosis Presenting With A Halo Sign On CT in An Immunocompetent PatientDocument2 pagesPulmonary Histoplasmosis Presenting With A Halo Sign On CT in An Immunocompetent PatientSharom R. AlvarezNo ratings yet
- Thorax00193 0009 PDFDocument10 pagesThorax00193 0009 PDFhotmart ventasNo ratings yet
- A Case of Pulmonary Aspergilloma and ActinomycosisDocument4 pagesA Case of Pulmonary Aspergilloma and ActinomycosisNova PurbaNo ratings yet
- Anesthesia in Thoracic Surgery: Changes of ParadigmsFrom EverandAnesthesia in Thoracic Surgery: Changes of ParadigmsManuel Granell GilNo ratings yet
- Your Electronic Ticket Receipt-7Document2 pagesYour Electronic Ticket Receipt-7rynaldiandriansyaNo ratings yet
- Anal DilationDocument3 pagesAnal DilationrynaldiandriansyaNo ratings yet
- App AnakDocument22 pagesApp AnakrynaldiandriansyaNo ratings yet
- SC FractureDocument21 pagesSC FracturerynaldiandriansyaNo ratings yet
- Rectal Biopsy (Suction Procedure) : AppointmentDocument2 pagesRectal Biopsy (Suction Procedure) : AppointmentrynaldiandriansyaNo ratings yet
- Picu Nicu 6 Maret 2014Document4 pagesPicu Nicu 6 Maret 2014rynaldiandriansyaNo ratings yet
- Case Report Team of Duty: Dr. Hendra KastiajiDocument3 pagesCase Report Team of Duty: Dr. Hendra KastiajirynaldiandriansyaNo ratings yet
- Canadian Medical Report FormsDocument6 pagesCanadian Medical Report FormsshichunNo ratings yet
- AMYLOIDOSISDocument50 pagesAMYLOIDOSISLavanya KalapalaNo ratings yet
- Jurnal Reading OsteomyelitisDocument11 pagesJurnal Reading Osteomyelitisfidela_ffNo ratings yet
- Gastroenteritis Case ReportDocument12 pagesGastroenteritis Case ReportjisooNo ratings yet
- Taxvantage Plus Medical Plan: | 自願醫保 Vhis |Document24 pagesTaxvantage Plus Medical Plan: | 自願醫保 Vhis |Tomei LauNo ratings yet
- CIDI-based Screening Scale For Bipolar Spectrum Disorders - : Clinical UtilityDocument4 pagesCIDI-based Screening Scale For Bipolar Spectrum Disorders - : Clinical UtilityJagdishVankarNo ratings yet
- Site Preservation Decision TreeDocument8 pagesSite Preservation Decision TreeHaoWangNo ratings yet
- Women and Birth: Michelle GrayDocument8 pagesWomen and Birth: Michelle Grayzimbabwe kuvukilandNo ratings yet
- About MemoryDocument44 pagesAbout MemoryGegiuc GabrielaNo ratings yet
- Cough N Cold Medicine List PDFDocument7 pagesCough N Cold Medicine List PDFDonna DominnoNo ratings yet
- Alteration in Respiratory SystemDocument138 pagesAlteration in Respiratory Systemcute_gurljhoanNo ratings yet
- Medical Utopias: Ethical Reflections About Emerging Medical TechnologiesDocument35 pagesMedical Utopias: Ethical Reflections About Emerging Medical TechnologiesKPJConferenceNo ratings yet
- What Is The NPI?Document11 pagesWhat Is The NPI?Naresh ReddyNo ratings yet
- Roles and Responsibilities of Geriatric Nurse in CommunityDocument4 pagesRoles and Responsibilities of Geriatric Nurse in CommunityAKHILA PKNo ratings yet
- TASK 11 - Yulia Indri FebrianiDocument4 pagesTASK 11 - Yulia Indri FebrianiindriNo ratings yet
- Nursing Care Plan Clubfoot or Talipes EquinovarusDocument6 pagesNursing Care Plan Clubfoot or Talipes EquinovarusMarzie LugtuNo ratings yet
- Process Recording With RubricDocument8 pagesProcess Recording With RubricAndrew GarskeNo ratings yet
- Informed Consent Document Template and Guidelines Informed Consent Form (Name of Institution)Document14 pagesInformed Consent Document Template and Guidelines Informed Consent Form (Name of Institution)Shondra D. BryantNo ratings yet
- 2010 - 2016 With AnswersDocument806 pages2010 - 2016 With AnswersIbrahim Abueltaif83% (6)
- Endometrial BiopsyDocument72 pagesEndometrial BiopsySatish TatamiyaNo ratings yet
- Flail ChestDocument26 pagesFlail ChestStawan ChouguleNo ratings yet
- Transcript Peter Saul Lets Talk About DyingDocument3 pagesTranscript Peter Saul Lets Talk About DyingDiogo MulderNo ratings yet
- TB 1716986horaDocument5 pagesTB 1716986horasanil kumarNo ratings yet
- Aciclovir 400mg and 800mg TabletsDocument2 pagesAciclovir 400mg and 800mg TabletsKalyan NandanNo ratings yet
- Precinorm U Plus.12173581001.v10.en PDFDocument2 pagesPrecinorm U Plus.12173581001.v10.en PDFARIF AHAMMED P0% (1)
- Models of Health and Health PromotionDocument16 pagesModels of Health and Health Promotionapi-31127039450% (2)
- Pain Scale For ThesisDocument4 pagesPain Scale For ThesisREMILYN ROSE ASUNCIONNo ratings yet