Professional Documents
Culture Documents
Meningitis (Lab Exam)
Meningitis (Lab Exam)
Uploaded by
MohammadAwitOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Meningitis (Lab Exam)
Meningitis (Lab Exam)
Uploaded by
MohammadAwitCopyright:
Available Formats
Approach Considerations
The diagnostic challenges in patients with clinical findings of meningitis are as follows:
Early identification and treatment of patients with acute bacterial meningitis
Assessing whether a treatable central nervous system (CNS) infection is present in those with
suspected subacute or chronic meningitis
Identifying the causative organism
Bacterial meningitis must be the first and foremost consideration in the differential diagnosis of patients with
headache, neck stiffness, fever, and altered mental status. Acute bacterial meningitis is a medical emergency,
and delays in instituting effective antimicrobial therapy result in increased morbidity and mortality.
In general, whenever the diagnosis of meningitis is strongly considered, a lumbar puncture should be promptly
performed. Examination of the cerebrospinal fluid (CSF) is the cornerstone of the diagnosis. The diagnosis of
bacterial meningitis is made by culture of the CSF sample. The opening pressure should be measured and the
fluid sent for cell count (and differential count), chemistry (ie, CSF glucose and protein), and microbiology (ie,
Gram stain and cultures).
A concern regarding LP is that the lowering of CSF pressure from withdrawal of CSF could precipitate
herniation of the brain. Herniation can sometimes occur in acute bacterial meningitis and other CNS infections
as the consequence of severe cerebral edema or acute hydrocephalus. Clinically, this is manifested by an
altered state of consciousness, abnormalities in pupil reflexes, and decerebrate or decorticate posturing. The
incidence of herniation after LP, even in patients with papilledema, is approximately 1%.
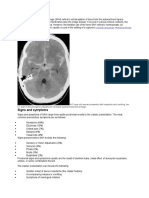
A screening computed tomography (CT) scan of the head may be performed before LP to determine the risk of
herniation. A prospective study involving 301 adults with suspected meningitis found that the following baseline
patient characteristics were associated with an abnormal finding on head CT [16] :
Age 60 years
Immunocompromise (ie, HIV infection/AIDS, immunosuppressive therapy, or transplantation)
A history of CNS disease
A history of seizure within 1 week before presentation
Any abnormality on neurologic examination
These factors have been included in the Infectious Diseases Society of America guidelines to decide who
should undergo CT before LP.[17]
The decision to obtain a brain CT scan before LP should not delay the institution of antibiotic therapy; such
delay can increase mortality. It should be also noted that herniation can occur in patients with bacterial
meningitis who have a normal brain CT scan. The most reliable clinical signs that indicate the risk of herniation
include deteriorating level of consciousness, brainstem signs, and a very recent seizure.
Other laboratory tests, which may include blood cultures, are needed to complement the CSF culture. These
bacterial cultures are used for identification of the offending bacteria and occasionally its serogroup, as well as
for determination of the organisms susceptibility to antibiotics. Special studies, such as serology and nucleic
acid amplification, may also be performed, depending on clinical suspicion of an offending organism.
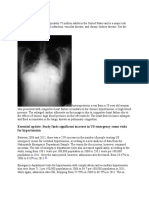
As many as 50% of patients with pneumococcal meningitis also have evidence of pneumonia on initial chest
radiography. This association occurs in fewer than 10% of patients with meningitis caused by H influenzae or N
meningitidis and in approximately 20% of patients with meningitis caused by other organisms. (See Imaging in
Bacterial Meningitis.)
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5834)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (852)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (903)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (541)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (350)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (824)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (405)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- 2000 Pictures For MRCP Part-2 Written by Sarowar HossainDocument102 pages2000 Pictures For MRCP Part-2 Written by Sarowar HossainLeila91% (11)
- Medical Microbiology and Immunology Flash Cards - Sample ChapterDocument250 pagesMedical Microbiology and Immunology Flash Cards - Sample Chapterleh.mo931580% (5)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- 2017 Wise 3RD Year With KeyDocument24 pages2017 Wise 3RD Year With KeyAnne Lorraine BringasNo ratings yet
- Microbiology Key WordsDocument5 pagesMicrobiology Key Wordsmoilo86020% (1)
- FCPS 1 Radiology + AnswersDocument25 pagesFCPS 1 Radiology + AnswersZahid Qamar100% (2)
- Meningitis PPT 2.0Document15 pagesMeningitis PPT 2.0Francis Adrian100% (2)
- Essential Update: Study Finds Significant Increase in US Emergency Room Visits For HypertensionDocument4 pagesEssential Update: Study Finds Significant Increase in US Emergency Room Visits For HypertensionMohammadAwitNo ratings yet
- Oli God End Ro GliomasDocument1 pageOli God End Ro GliomasMohammadAwitNo ratings yet
- Scabiei Hominis. Approximately 300 Million Cases of Scabies (See The Image Below) Are ReportedDocument3 pagesScabiei Hominis. Approximately 300 Million Cases of Scabies (See The Image Below) Are ReportedMohammadAwitNo ratings yet
- Neurilemmomas DXDocument1 pageNeurilemmomas DXMohammadAwitNo ratings yet
- Neurilemmomas DXDocument1 pageNeurilemmomas DXMohammadAwitNo ratings yet
- Volkmann Contracture: Historical AspectsDocument2 pagesVolkmann Contracture: Historical AspectsMohammadAwitNo ratings yet
- Neurofibroma Ganglion Cyst Giant Cell Tumor of Tendon Sheath LipomaDocument1 pageNeurofibroma Ganglion Cyst Giant Cell Tumor of Tendon Sheath LipomaMohammadAwitNo ratings yet
- AstrocytomaDocument1 pageAstrocytomaMohammadAwitNo ratings yet
- Lymphoblastic Leukemia: This MRI Shows A Juvenile Pilocytic Astrocytoma of The CerebellumDocument1 pageLymphoblastic Leukemia: This MRI Shows A Juvenile Pilocytic Astrocytoma of The CerebellumMohammadAwitNo ratings yet
- United States StatisticsDocument1 pageUnited States StatisticsMohammadAwitNo ratings yet
- Prognosis: Clinical Grading ScalesDocument3 pagesPrognosis: Clinical Grading ScalesMohammadAwitNo ratings yet
- Astrocytoma SDocument6 pagesAstrocytoma SMohammadAwitNo ratings yet
- Cerebral Aneurysm Arteriovenous Malformation: Signs and SymptomsDocument3 pagesCerebral Aneurysm Arteriovenous Malformation: Signs and SymptomsMohammadAwitNo ratings yet
- Brainstem Gliomas: Brain Cancer Treatment ProtocolsDocument2 pagesBrainstem Gliomas: Brain Cancer Treatment ProtocolsMohammadAwitNo ratings yet
- Astrocytoma SDocument3 pagesAstrocytoma SMohammadAwitNo ratings yet
- Surgical Therapy: LacerationsDocument1 pageSurgical Therapy: LacerationsMohammadAwitNo ratings yet
- Sertifikat AnatomiDocument1 pageSertifikat AnatomiMohammadAwitNo ratings yet
- Nerve InjuryDocument1 pageNerve InjuryMohammadAwitNo ratings yet
- Nerve InjuryDocument1 pageNerve InjuryMohammadAwitNo ratings yet
- MeningitisDocument15 pagesMeningitisnaveen chaudharyNo ratings yet
- Complications of Ventriculo-Peritoneal ShuntingDocument4 pagesComplications of Ventriculo-Peritoneal ShuntingSa'Deu FondjoNo ratings yet
- Corticosteroid Use in Small Animal Neurology 2014 Veterinary Clinics of North America Small Animal PracticeDocument16 pagesCorticosteroid Use in Small Animal Neurology 2014 Veterinary Clinics of North America Small Animal PracticeJaneKarllaNo ratings yet
- Meningitis - 2018Document55 pagesMeningitis - 2018Abraham Anaely100% (1)
- Meningitis and Encephalitis: PGI Roddame Angelo ErispeDocument100 pagesMeningitis and Encephalitis: PGI Roddame Angelo ErispeAngelo ErispeNo ratings yet
- Nursing Practice Threesoko Na Ito Cgena... Kainis 1Document16 pagesNursing Practice Threesoko Na Ito Cgena... Kainis 1JayCesarNo ratings yet
- Microbial Diseases of The Different Organ System and Epidem.Document36 pagesMicrobial Diseases of The Different Organ System and Epidem.Ysabelle GutierrezNo ratings yet
- Clinical Concept Map SIMSDocument3 pagesClinical Concept Map SIMSAlexia HuertaNo ratings yet
- Meningococcal Infection in ChildrenDocument6 pagesMeningococcal Infection in ChildrenAdrian KhomanNo ratings yet
- Central Nervous System Tuberculosis: John M. LeonardDocument10 pagesCentral Nervous System Tuberculosis: John M. LeonardMarcela Catalina Fandiño VargasNo ratings yet
- A-Case-Of-Bacterial-Meningitis Final-1Document34 pagesA-Case-Of-Bacterial-Meningitis Final-1Leslie Ann Pablo MarantanNo ratings yet
- Medicine-MBBS University Questions-SystemwiseDocument7 pagesMedicine-MBBS University Questions-SystemwisedrtpkNo ratings yet
- Daftar PustakaDocument2 pagesDaftar PustakaNovianaNo ratings yet
- Twaites Meningo TB 2013 PDFDocument12 pagesTwaites Meningo TB 2013 PDFgolin__No ratings yet
- Approach To The Child With Acute Diarrhea in Resource-Limited Countries - UpToDateDocument17 pagesApproach To The Child With Acute Diarrhea in Resource-Limited Countries - UpToDateNedelcu MirunaNo ratings yet
- E. Coli InfectionsDocument18 pagesE. Coli InfectionsLaura Anghel-MocanuNo ratings yet
- Peads Teacher MannualDocument108 pagesPeads Teacher MannualMobin Ur Rehman KhanNo ratings yet
- Child With Non Blanching RashDocument6 pagesChild With Non Blanching Rashtanya mathewNo ratings yet
- Vaccine: What You Need To Know: Haemophilus Influenzae Type B (Hib)Document2 pagesVaccine: What You Need To Know: Haemophilus Influenzae Type B (Hib)mpersiNo ratings yet
- Paediatric Clinical GuidelinesDocument7 pagesPaediatric Clinical GuidelinesAndriNo ratings yet
- Pathophysiology of MeningitisDocument4 pagesPathophysiology of MeningitisDaryl BalangueNo ratings yet
- Exam 2018 PDFDocument62 pagesExam 2018 PDFWondimu Koy100% (2)
- Lesson Plan Lumbar PunctureDocument19 pagesLesson Plan Lumbar PunctureLoma Waghmare (Jadhav)No ratings yet
- Group 3C Case Study Bacterial Meningitis 1Document30 pagesGroup 3C Case Study Bacterial Meningitis 1SHIRLENE RAMIREZNo ratings yet