Professional Documents
Culture Documents
Pruritus Ani, Hemorroidet Etj
Pruritus Ani, Hemorroidet Etj
Uploaded by
Kreshnik HAJDARICopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Pruritus Ani, Hemorroidet Etj
Pruritus Ani, Hemorroidet Etj
Uploaded by
Kreshnik HAJDARICopyright:
Available Formats
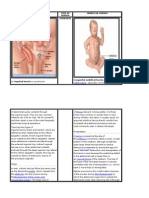
Intestinal
Fissures, pruritus ani Anal anatomy
and haemorrhoids
Tom D Eames
John H Scholefield
Anal cushions Puborectalis
Abstract
Internal anal External anal
Benign anal diseases are common. Patients may present with a variety of sphincter
sphincter
symptoms including pain, itching or bleeding. It is important for a surgeon
to be able to accurately diagnose and treat these conditions. This article
discusses the basic anatomy of the anal canal and the common causes,
investigation and treatment of anal disease. Fissures are linear ulcera-
tions in the anal canal of unknown aetiology and are a common cause
of pain and bleeding. Treatment can involve both pharmacological and
surgical management. Many people will suffer with pmritus ani at some
point in their lives. Most causes are benign but it is essential to perfom
sufficient investigation as it can be a marker of some important diseases. Dentate line and anal valves
Haemorrhoids occur in 4-36% of the population and often present with
Figure 1
fresh rectal bleeding. Outpatient management is successful in the major-
ity of patients but surgical intervention is sometimes required.
Fissures
Keywords fissures; pruritus ani; haemorrhoids; benign anal disease
Definition and epidemiology
Fissures are linear ulcerations of the anal canal below the level of
the dentate line. They can occur secondary to infection, trauma
Anatomy
and Crohn’s disease, but most are primary in origin. They are a
The anal canal is about 4–5 cm long in men and slightly shorter common cause of pain and bleeding, and most commonly occur
in women. At the midpoint of the anal canal is the dentate line in young patients between the ages of 20 and 40 years; however,
(Figure 1). This demarcates mucosa from the embryonic endo- they can present at any age. Most fissures are acute in nature and
derm and ectoderm. Above this the canal is lined with columnar resolve spontaneously within a period of 6 weeks without any
epithelium and below with stratified squamous epithelium. The intervention (Figure 2). Any that continue beyond this point are
point between these zones is not always clear cut. There are considered chronic (Figure 3). Acute fissures are probably very
several important differences between the upper and lower anal common, although the exact prevalence is difficult to ascertain
canal. The upper canal innervation is autonomic (meaning that it as many do not present to medical care.
is relatively insensate), venous drainage is into the portal system
and lymph drainage is to the abdominal nodes. The lower anal Aetiology
canal is somatic, venous drainage is systemic and lymph drain- The aetiology is uncertain. The precipitating event may be
age is into the inguinal nodes. a trauma to the anoderm possibly associated with a period of
Resting pressure in the anal canal is important for maintaining constipation, although many fissures present with no history of
continence. It is composed of 55% from the internal anal sphinc- changes in bowel habit. Previous anal surgery or infection may
ter, 30% from the external anal sphincter, and 15% from the anal predispose to fissures.
cushions and mucosa. It has long been known that there is an association between
The clock face is often used to describe the position of pathol- fissure formation and increased anal resting pressures. The
ogy in the anal canal. 12 o’clock is anterior with the patient lying increased pressure probably causes hypoperfusion to the affected
supine. region thereby increasing predisposition to anodermal damage
and reducing healing rates. The most common sites of fissure
formation are in the midline, almost exclusively (99%) posteri-
Tom D Eames is a Research Fellow in Gastrointestinal Surgery at orly in men, and both anteriorly (10%) and posteriorly (90%) in
Nottingham University Hospitals, Nottingham, UK. Conflicts of interest: women. This may well be due to the ‘watershed’ anatomy of the
none declared. blood supply to these areas and studies have shown decreased
blood supply to the posterior midline.
John H Scholefield FRCS is a Professor of Surgery at Nottingham Multiple fissuring or fissures away from the midline suggest
University Hospitals, Nottingham, UK, Conflicts of interest: none declared. other pathologies, such as inflammatory bowel disease.
SURGERY 26:8 334 © 2008 Published by Elsevier Ltd.
Intestinal
can lead to fear of defaecation, increasing the risk of constipa-
Treatment of anal fissure tion. There may be associated symptoms of pruritus ani.
The fissure may be visible on parting the buttocks. Chronic
Acute fissure (< 6 weeks) fissures appear as a linear or pear-shaped defect occasionally
with indurated edges. The internal anal sphincter may be visible
as horizontal white bands underneath. Acute fissures are usually
Conservative treatment more superficial and have sharply demarcated edges.
High-fibre diet It may not be possible to visualize the fissure owing to sphinc-
Oral fluids ter spasm. This can often make digital examination or proctos-
Stool softeners copy impossible. A skin tag may be visible externally. However,
Sitz baths examination under anaesthesia may be required to make the
diagnosis. Further investigation may be required to rule out a
Failure to heal more sinister cause of bleeding.
90% heal
GTN 0.2% b.d./t.d.s. Medical treatment
for 6–8 weeks Treatment is aimed at breaking the cycle of sphincter spasm and
pain. Traditionally the first-line treatment was stool softeners
Failure to heal and a high-fibre diet, followed by sphincterotomy if symptoms
60–70% heal
did not abate. Over the past 15 years there have been several
Diltiazem 2% b.d. advances in the pharmacological management of fissures.
for 8 weeks The use of glyceryl trinitrate (GTN), a nitric oxide donor, for
pharmacological sphincterotomy was first described in 1994.
Failure to heal Nitric oxide causes relaxation of the internal anal sphincter, which
70–80% heal
is responsible for the majority of resting tone. Randomized con-
Botulinum toxin 20 IU trolled trials have shown that GTN 0.2% two to three times daily
into IAS heals fissures in over two-thirds of patients. The major adverse
effect of GTN treatment is headache, although this is usually not
Failure to heal severe enough to require discontinuation of treatment.
> 80% heal
An alternative or second-line treatment is the topical appli-
Surgery cation of calcium channel blockers. These also relax the inter-
Lateral internal nal anal sphincter. Topical diltiazem is most commonly used,
sphincterotomy although studies have shown topical and oral nifedipine also to
be effective, but with a higher side-effect profile. Topical diltia-
zem 2% twice daily for 8 weeks heals similar numbers to GTN
GTN, glyceryl trinitrate; IAS, internal anal sphincter
and is effective in treating those resistant to GTN.
Botulinum toxin has been shown to be effective for some fis-
Figure 2 sures that do not heal with topical treatments. It is a neurotoxin
produced by Clostridium botulinum which prevents the release
History and examination of acetylcholine at the neuromuscular junction. 20 IU is injected
The usual presentation is with a sharp or tearing pain localized to into the internal anal sphincter at 3 and 9 o’clock. It has been
the anus, which increases in severity on defaecation and is some- shown to be superior to GTN in healing fissures in some studies.
times described as like ‘passing glass’. This may be associated Transient flatal incontinence is the most common side effect.
with blood, which the patient may notice on wiping. The pain
may continue for minutes to several hours after passing stool and Surgical treatment
Surgery used to be the mainstay of treatment for fissures. Histori-
cally one of the commonly used procedures was anal dilatation.
This caused a decrease in the resting pressure in the anal canal;
however, there was a high rate of incontinence associated with
the procedure as it resulted in uncontrolled damage to the inter-
nal anal sphincter.
Surgery is now reserved mainly for those patients who fail to
respond to medical therapy. Lateral internal anal sphincterotomy
provides a more controlled way of lowering resting pressure,
thereby increasing anodermal blood flow. The distal part of the
sphincter is divided, going no more proximally than the length of
the fissure. This procedure has been associated with varying lev-
els of incontinence and patients should be warned of this. Owing
to the shorter anal canal it is important to perform preoperative
Figure 3 Proctoscopy showing chronic anal fissure. manometry and ultrasound examination in women.
SURGERY 26:8 335 © 2008 Published by Elsevier Ltd.
Intestinal
Pruritus ani
General treatment regimen for pruritis ani
Definition and epidemiology
Pruritus is a common symptom and many people will suffer Avoid scratching
with it at some point in their lives. Although often benign it is Wash perianal area twice daily with water after defaecation
important that sufficient investigation is carried out as it can be Pat the skin dry with a soft towel or blow dry with a cool
a marker of some important diseases. The exact prevalence is hairdryer
unknown but it is commoner in men over 40 years of age. It is Avoid soaps, perfumes and any non-prescribed medications
often worse in warm weather. It can become a self-perpetuating Wear loose-fitting cotton underwear
problem resulting in an ‘itch–scratch’ cycle that can be difficult A cotton wool pledget against or just inside anal canal may help
to break and can cause chronic skin changes. absorb moisture.
Antihistamines such as chlorphenamine maleate 4 mg p.o. at
History and examination night may help
Patients may present with a long history of perianal itch for which An injection of methylene blue has been shown to control
they have not previously sought medical intervention. They may itching if other measures fail
give a history of the underlying condition. It is important to ask
about bowel habit and pain or bleeding on defaecation. Examina- Table 1
tion may show excoriation of the perianal area or lichenification
if the problem is long standing. It is important to carry out digital
examination and proctoscopy. do not seek medical attention; however, it may be somewhere
in the region of 4–36% depending on population. The inci-
Differential diagnosis and aetiology dence is higher in Western populations and is low in sub-
The majority of cases of pruritus are probably idiopathic. Under- Saharan Africa, although this may be due to under-reporting
lying pathology is likely in about 10%. Careful history and exam- of symptoms.
ination will reveal most causes.
History and examination
Systemic diseases: diabetes mellitus is probably the most common Presentation is usually with fresh red rectal bleeding. This
systemic cause. It may be associated with the increased prepon- may occur after opening the bowels or on the paper when
derance to candidiasis and is more common with poor glycaemic wiping. Any lower gastrointestinal tract bleeding in a patient
control. Haematological disorders such as leukaemia, lymphoma over 40 years of age needs further investigation with colonos-
and aplastic anaemia can also cause pruritus. Any medication that copy or radiological imaging. Prolapse of haemorrhoids (often
alters gut flora or is immunosuppressive may cause itching. described as ‘something down below’), pain, leakage or pruri-
tus ani may be other presenting features. The symptoms may
Dermatological conditions: psoriasis is the most common cause. be relapsing and remitting over a period of several years, and
Atopic or seborrhoeic dermatitis may also cause perianal itching. there may be an association with pregnancy or changes in
A dermatological opinion may be required. Hyperkeratosis may life-style.
be a sign of anal intra-epithelial neoplasia. Full history and abdominal examination may reveal other
causes of rectal bleeding. Inspection of the perianal area may
Infections: erythrasma (Corynebacterium minutissimum), other reveal external haemorrhoids, skin tags or other perianal pathol-
bacterial infections (such as folliculitis and abscess formation) ogy. Digital rectal examination and proctoscopy should then be
and candidiasis may cause itching. Candida may be present com- carried out. Proctoscopy may show haemorrhoids at 3, 7 and 11
mensally in the perianal region without being the cause of symp- o’clock, although this can vary especially in those who have had
toms. Sexually transmitted diseases (syphilis, gonorrhoea, herpes previous surgery.
simplex virus and human papilloma virus) can lead to pruritus.
Pinworms are a common cause in children and their parents. Classification
Classification is usually by Goligher’s system, which describes
Anorectal disease: it is important to rule out chronic diarrhoea, anal four degrees of severity (Table 2). This is useful for helping in
incontinence, haemorrhoids, fissures, fistula and rectal prolapse.
Management Goligher’s classification of haemorrhoids
Investigation and treatment of the underlying cause is the most
important first line. Biopsy of the skin may occasionally be required. Severity Description
The general treatment regimen is summarized in Table 1.
First degree Bleed but do not prolapse
Second degree Prolapse but spontaneously reduce
Haemorrhoids
Third degree Prolapse and require manual reduction
Definition and epidemiology Fourth degree Prolapsed and irreducible
Haemorrhoids are enlargements of the vascular cushions of the
anal canal. The exact prevalence is unknown as many people Table 2
SURGERY 26:8 336 © 2008 Published by Elsevier Ltd.
Intestinal
determining treatment, but it does not convey any information procedure. The haemorrhoid is grasped and lifted through
on the severity of symptoms. the anal canal, and is then dissected away from the sphincter
complex with scissors (electrocautery or harmonic scalpel can be
Conservative treatment used). This is repeated for each of the haemorrhoids, leaving a
Although a topic of debate for some time, there is evidence that bridge of mucosa between each defect. The defects are then left
fibre supplements moderately improve symptoms and bleeding. open and healing is by secondary intention. A closed technique
Other treatments, such as perianal hygiene, increased fluid intake such as the Ferguson procedure is preferred in the USA. This
and relieving constipation, are commonly suggested although involves a similar dissection, but the mucosal defects are closed
there is a lack of supporting evidence. with a continuous suture at the end of the operation. The results
There are several over-the-counter medications that contain of both techniques are similar, but wound healing is faster with
antiseptics, astringents, local anaesthetics and topical corticoste- the closed procedure.
roids. These may help with acute symptoms. Long-term use of The main postoperative complication is pain. There is evi-
corticosteroids may lead to permanent skin damage. dence that prophylactic oral metronidazole, topical diltiazem,
topical GTN or injected botulinum toxin has a marginal benefit in
Out-patient treatment pain reduction. Later complications include secondary haemor-
Rubber band ligation and injection sclerotherapy remain the rhage (at 7–10 days), infection, faecal incontinence (as a result of
two most commonly used techniques for out-patient treatment sphincter damage) and anal stenosis (usually due to inadequate
of first-, second- and third-degree haemorrhoids. Both rely on mucosal bridges).
causing fibrosis to lift the haemorrhoid up in the anal canal, thus Doppler-guided haemorrhoidal artery ligation is becoming
minimizing symptoms. popular. A specially designed proctoscope with a Doppler probe
Rubber band ligation has been carried out since the 1960s. is used to locate the haemorrhoidal feeding vessels. These are
Proctoscopy is performed and the haemorrhoid is visualized. A then ligated with absorbable sutures. Short-term results are
suction bander is then applied to the mucosa above the haemor- good.
rhoid and the dentate line; this is important to minimize pain Stapled haemorrhoidectomy was first described in the late
associated with the procedure. A rubber band is applied to the 1990s. This technique is useful in the treatment of third- and
mucosa, which then sloughs off over a period of days leaving an fourth-degree haemorrhoids. A circular stapler is inserted into
area of fibrosis. Many surgeons only ligate one or two haemor- the anal canal above the dentate line and a strip of mucosa is
rhoids at a session, although there is no evidence of increased removed circumferentially, hitching up the haemorrhoids. Long-
complications with multiple bandings. The main acute complica- term results suggest that recurrence rates are higher than for
tions are bleeding and pain; occasionally the band may need to haemorrhoidectomy, although the procedure may be less painful
be removed if the pain is severe. This usually occurs because and return to normal activities after surgery is quicker. Com-
the band has been applied too close to the dentate line. Later plications are similar to those of haemorrhoidectomy, with the
complications are sepsis and secondary haemorrhage (5–10 days additional potential risks of rectovaginal fistula and anastomotic
after the procedure). The risk of late haemorrhage is increased leakage.
in patients who are taking antiplatelet or anticoagulant medica-
tion, and these should be stopped if possible for a week before Acutely thrombosed haemorrhoids
banding. Success rates as high as 80% in the short term have These can be very painful but can be treated conservatively with
been reported and up to 46% of patients remain symptom free icepacks, stool softeners and analgesia, without the need for
at 4 years. admission to hospital. Topical nifedipine has been used to treat
Injection sclerotherapy involves injection of 5% oily phenol the pain. Emergency surgery is occasionally needed to remove
into the base of the haemorrhoid. This should be reserved for the thrombosed haemorrhoid. This can be a difficult operation
first- and second-degree haemorrhoids as it provides no benefit as there is a risk of anal stenosis due to sloughing of the mucosal
in prolapsed haemorrhoids. The failure rate is higher than that bridges. ◆
for banding, with only 8% of patients symptom free at 4 years.
There is evidence to suggest that fibre supplementation alone
may be equally effective.
Infrared coagulation can also be used to treat first- and sec-
ond-degree haemorrhoids. It is less effective and less widely used
than banding. Further reading
Acheson AG, Scholefield JH. Management of haemorrhoids. BMJ 2008;
Surgical treatment 336: 380–3.
Haemorrhoidectomy has been carried out for the past 70 years. Phillips RKS, ed. Colorectal surgery. A companion to specialist surgical
The most popular technique in the UK is the Milligan–Morgan practice, 3rd edn. London: Elsevier Saunders, 2006.
SURGERY 26:8 337 © 2008 Published by Elsevier Ltd.
You might also like
- Perianal Problems: ACS/ASE Medical Student Core Curriculum Perianal ProblemsDocument21 pagesPerianal Problems: ACS/ASE Medical Student Core Curriculum Perianal ProblemsHasti Chande100% (1)
- The Mental Health of Jehovah WitnessesDocument5 pagesThe Mental Health of Jehovah WitnessesKreshnik HAJDARI100% (1)
- INGUINAL HERNIA and Umbilical HerniaDocument13 pagesINGUINAL HERNIA and Umbilical HerniaKathNo ratings yet
- Medical EmergenciesDocument81 pagesMedical EmergenciesKreshnik HAJDARINo ratings yet
- Anal, Perianal, and Pilonidal Diseases - Oct - 2023 2Document15 pagesAnal, Perianal, and Pilonidal Diseases - Oct - 2023 2qq8kx98kt2No ratings yet
- Anal Fissure: A Common Cause of Anal Pain: Clinical MedicineDocument4 pagesAnal Fissure: A Common Cause of Anal Pain: Clinical MedicineErwin CandraNo ratings yet
- Management of Common Benign Anorectal Disease: What All Physicians Need To KnowDocument7 pagesManagement of Common Benign Anorectal Disease: What All Physicians Need To KnowNeri JaramilloNo ratings yet
- Anal and Perianal ConditionsDocument58 pagesAnal and Perianal ConditionsYonas YemidiralemNo ratings yet
- Anal FissureDocument9 pagesAnal FissureaiysahmirzaNo ratings yet
- Textbook of Colon and Rectum-Páginas-219-227Document9 pagesTextbook of Colon and Rectum-Páginas-219-227Elliott Josué Carreón MaldonadoNo ratings yet
- Perianal Abscess - Abstract - Europe PMCDocument6 pagesPerianal Abscess - Abstract - Europe PMCRidha Aswina DalimuntheNo ratings yet
- Disease of RectumDocument22 pagesDisease of RectumTalal AbbasiNo ratings yet
- 2.4.5.2.3.a Bowel ObstructionDocument35 pages2.4.5.2.3.a Bowel ObstructionProject ByNo ratings yet
- l8 Management of Perianal Pain and ConditionsDocument51 pagesl8 Management of Perianal Pain and ConditionsMohd Johari Mohd ShafuwanNo ratings yet
- Colorectal Surgery MrcsDocument36 pagesColorectal Surgery MrcsDeen MohammadNo ratings yet
- 3.1 Acute AppendicitisDocument3 pages3.1 Acute AppendicitisMavi HayalNo ratings yet
- Benign Anorectal ConditionssDocument32 pagesBenign Anorectal ConditionssMpanso Ahmad AlhijjNo ratings yet
- Inguinal Hernia: From Wikipedia, The Free EncyclopediaDocument6 pagesInguinal Hernia: From Wikipedia, The Free EncyclopediaSherlyn YeeNo ratings yet
- Mini Review: Current Concepts in The Management of Anterior Urethral StricturesDocument8 pagesMini Review: Current Concepts in The Management of Anterior Urethral StricturesDwi WiraNo ratings yet
- 16 Benign Anorectal ConditionsDocument48 pages16 Benign Anorectal Conditionssuhaib ananzehNo ratings yet
- Abdominal HerniaDocument33 pagesAbdominal HerniaMohammedNo ratings yet
- Whiteford2007 Abses PerianalDocument8 pagesWhiteford2007 Abses PerianalPudyo KriswhardaniNo ratings yet
- Inguinal Hernia and Hydrocele: Congenital Hydrocele Presents As A Mass in The Scrotum ShortlyDocument3 pagesInguinal Hernia and Hydrocele: Congenital Hydrocele Presents As A Mass in The Scrotum ShortlyBetão AviãoNo ratings yet
- 8412-Article Text-29472-1-10-20130809Document8 pages8412-Article Text-29472-1-10-20130809NenyNo ratings yet
- Afecciones Anorrectales Benignas Absceso Perianal, Fístula Anal, Hemorroides, Fisuras y Seno PilonidalDocument7 pagesAfecciones Anorrectales Benignas Absceso Perianal, Fístula Anal, Hemorroides, Fisuras y Seno PilonidalJoshua MaciasNo ratings yet
- Minilaparoscopic Left Paraduodenal Hernia Repair-A CaseDocument4 pagesMinilaparoscopic Left Paraduodenal Hernia Repair-A CaseAritra PaulNo ratings yet
- Anal FissureDocument9 pagesAnal FissureKnight StingrayNo ratings yet
- Anal Fissures PPT KIDocument20 pagesAnal Fissures PPT KIMustafa HusainNo ratings yet
- Pathology of EsophagusDocument59 pagesPathology of EsophagusDoc On CallNo ratings yet
- Hemorrhoids: Author: Scott C Thornton, MD, Associate Clinical Professor of Surgery, Yale UniversityDocument10 pagesHemorrhoids: Author: Scott C Thornton, MD, Associate Clinical Professor of Surgery, Yale Universityshelly_shellyNo ratings yet
- Gynecology 2.01.2 Benign Neoplasms of The Ovary and Oviducts - Dr. Co-HidalgoDocument7 pagesGynecology 2.01.2 Benign Neoplasms of The Ovary and Oviducts - Dr. Co-HidalgoMarc Francis AlayNo ratings yet
- Anal Fissure - ColoproctoDocument3 pagesAnal Fissure - ColoproctoThomas KlebNo ratings yet
- Hemorrhoids, ParaproctitisDocument56 pagesHemorrhoids, ParaproctitisСандагсүрэн СандагдоржNo ratings yet
- 012 090 Groin HerniaDocument8 pages012 090 Groin HerniaxcalibursysNo ratings yet
- Clark2016 Benign Anal DiseaseDocument7 pagesClark2016 Benign Anal DiseaseJohana Dellaneira Aucancela RamosNo ratings yet
- Anal FistulaDocument26 pagesAnal FistulaBeverly PagcaliwaganNo ratings yet
- Hernias (Inguinal and Femoral)Document37 pagesHernias (Inguinal and Femoral)Muwanga faizoNo ratings yet
- Clinical Review - Full PDFDocument6 pagesClinical Review - Full PDFDewi WulansariNo ratings yet
- Acute Appendicitis: Michael Alan Cole Robert David HuangDocument10 pagesAcute Appendicitis: Michael Alan Cole Robert David HuangandreaNo ratings yet
- Update On The Management of Anal Fissure: SciencedirectDocument7 pagesUpdate On The Management of Anal Fissure: SciencedirectAndrea RodríguezNo ratings yet
- Intussusception TransDocument4 pagesIntussusception TransJames Maravillas100% (1)
- Anorectal Conditions: Prepared By: Manisha Thapa Roll No: 6 BSN 2 Year Presented To: Ms. Shristhi ShresthaDocument25 pagesAnorectal Conditions: Prepared By: Manisha Thapa Roll No: 6 BSN 2 Year Presented To: Ms. Shristhi ShresthaManjesh Mishra XettriNo ratings yet
- Hernias - PPT YenniDocument44 pagesHernias - PPT YenniDhika ArdiansyahNo ratings yet
- Eventrații Și EviscerațiiDocument55 pagesEventrații Și EviscerațiiPanuta AndrianNo ratings yet
- Common Health Problems That Develop During Infancy MPNDocument14 pagesCommon Health Problems That Develop During Infancy MPNShaii Whomewhat GuyguyonNo ratings yet
- Anal Fissure Chronic - Clinical EvidenceDocument18 pagesAnal Fissure Chronic - Clinical EvidenceNicolás CopaniNo ratings yet
- Abcesso e Fistula AnoretalDocument5 pagesAbcesso e Fistula AnoretalDani SNo ratings yet
- Congenital Anomalies 1&2Document40 pagesCongenital Anomalies 1&2Hafez AhmedNo ratings yet
- Benign Anorectal Disease: Hemorrhoids, Fissures, and FistulasDocument10 pagesBenign Anorectal Disease: Hemorrhoids, Fissures, and FistulasRilyFannyNo ratings yet
- Slide Hernia 2003Document24 pagesSlide Hernia 2003anfaNo ratings yet
- An Approach To The Neck Masses: BY: Hardi H. QaderDocument49 pagesAn Approach To The Neck Masses: BY: Hardi H. QaderEmad AlryashiNo ratings yet
- Absceso y Fistula AnalDocument24 pagesAbsceso y Fistula AnalSinue PumaNo ratings yet
- IntussDocument4 pagesIntussemman_abzNo ratings yet
- Anal Abscess And Fistula, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandAnal Abscess And Fistula, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsRating: 1 out of 5 stars1/5 (1)
- A Simple Guide To Anal Disorders, Diagnosis, Treatment And Related ConditionsFrom EverandA Simple Guide To Anal Disorders, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Anal Cancer, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandAnal Cancer, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Pleural Effusion, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandPleural Effusion, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- Hernia, (Different Types) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandHernia, (Different Types) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsRating: 5 out of 5 stars5/5 (1)
- BIBLE BEFORE SCIENCE RevisedDocument32 pagesBIBLE BEFORE SCIENCE RevisedKreshnik HAJDARINo ratings yet
- UrinalysisDocument5 pagesUrinalysisKreshnik HAJDARINo ratings yet
- How To Win Over WorryDocument9 pagesHow To Win Over WorryKreshnik HAJDARINo ratings yet
- Child's HerniaDocument13 pagesChild's HerniaKreshnik HAJDARINo ratings yet
- Liver TestsDocument17 pagesLiver TestsKreshnik HAJDARI100% (1)
- Red Eye - Student VersionDocument69 pagesRed Eye - Student VersionKreshnik HAJDARINo ratings yet
- Evaluating The Febrile Patient With A RashDocument23 pagesEvaluating The Febrile Patient With A RashKreshnik HAJDARI100% (1)
- Inspirimi I Bibles BIBLE INSPIRATIONDocument4 pagesInspirimi I Bibles BIBLE INSPIRATIONKreshnik HAJDARINo ratings yet
- A Hoax and Its ParadoxesDocument11 pagesA Hoax and Its ParadoxesKreshnik HAJDARINo ratings yet
- Dobesimi I Shikimit VISION LOSSDocument7 pagesDobesimi I Shikimit VISION LOSSKreshnik HAJDARINo ratings yet
- Electrocardiogramm - Ecg InterpretationDocument56 pagesElectrocardiogramm - Ecg InterpretationKreshnik HAJDARI100% (1)
- Gastroenterology Function Bowel DisordersDocument12 pagesGastroenterology Function Bowel DisordersKreshnik HAJDARINo ratings yet
- Benign or Harbinger of Sudden Death?: R. Oehm, MD, FACC, 10/26/06 With POTTS 10/20/08Document48 pagesBenign or Harbinger of Sudden Death?: R. Oehm, MD, FACC, 10/26/06 With POTTS 10/20/08Kreshnik HAJDARINo ratings yet
- Leukocytosis: Basics of Clinical Assessment: Production, Maturation and Survival of LeukocytesDocument9 pagesLeukocytosis: Basics of Clinical Assessment: Production, Maturation and Survival of LeukocytesKreshnik HAJDARINo ratings yet
- Surgery - FirecrackerDocument73 pagesSurgery - FirecrackerLucas HoldereggerNo ratings yet
- HemorrhoidsDocument4 pagesHemorrhoidsKarl Angelo MontanoNo ratings yet
- Gastro-Intestinal System Diagnostic TestsDocument11 pagesGastro-Intestinal System Diagnostic TestsFev BanataoNo ratings yet
- Cancer Healing MantraDocument2 pagesCancer Healing Mantrarucsi_ror6539No ratings yet
- Constipation and Bladder and Bowel Control - Oct 2013Document4 pagesConstipation and Bladder and Bowel Control - Oct 2013Dr.Kamlesh BariNo ratings yet
- Gastro Week 4Document39 pagesGastro Week 4Reynaldi FernandesNo ratings yet
- Research A Comparative Clinical Study On The Effect of Some Compound Ayurvedic Preparations in The Management of Arsha-Ayur ResearchDocument14 pagesResearch A Comparative Clinical Study On The Effect of Some Compound Ayurvedic Preparations in The Management of Arsha-Ayur ResearchDrHassan Ahmed ShaikhNo ratings yet
- Development of Hemorrhoids: Anal Canal AnatomyDocument20 pagesDevelopment of Hemorrhoids: Anal Canal AnatomyKris TejereroNo ratings yet
- Nash Repertory PDFDocument53 pagesNash Repertory PDFSatyendra RawatNo ratings yet
- Module 11 Muscular Skeleton SystemDocument20 pagesModule 11 Muscular Skeleton SystemeroolifyNo ratings yet
- Hemorrhoid: Department of Surgery Raden Mattaher Hospital Faculty of Medicine and Health Sciences Jambi UniversityDocument17 pagesHemorrhoid: Department of Surgery Raden Mattaher Hospital Faculty of Medicine and Health Sciences Jambi UniversityINTAN ANFERTANo ratings yet
- Gastrointestinal PathologyDocument59 pagesGastrointestinal PathologybonadnadineNo ratings yet
- Coloproctology Brochure English 01 2019Document4 pagesColoproctology Brochure English 01 2019Gino PeñalozaNo ratings yet
- BASTIDocument3 pagesBASTISubhash Digambar Visal100% (1)
- Surgery 6/2019: Spot Light On Surgery 2019 Mcqs Book DR Fadi QutishatDocument41 pagesSurgery 6/2019: Spot Light On Surgery 2019 Mcqs Book DR Fadi QutishatZaid ZayedNo ratings yet
- Understanding Basic Statistics 8th Edition Brase Solutions ManualDocument35 pagesUnderstanding Basic Statistics 8th Edition Brase Solutions Manualeyepieceinexact.4h0h100% (33)
- 2019 Last Day Revision RecallsDocument222 pages2019 Last Day Revision RecallsHiran SajeewNo ratings yet
- Pilosid CapsuleDocument3 pagesPilosid Capsulehk_scribdNo ratings yet
- Hemorroids Anal Fissure and FistulaDocument37 pagesHemorroids Anal Fissure and FistulathenamelessheroNo ratings yet
- An Anal FissureDocument4 pagesAn Anal FissureErnesErlyanaSuryawijayaNo ratings yet
- Case StudyDocument3 pagesCase StudyLouel VicitacionNo ratings yet
- Calcium Dobesilate in Symptomatic Treatment of Hemorrhoidal Disease: An Interventional StudyDocument3 pagesCalcium Dobesilate in Symptomatic Treatment of Hemorrhoidal Disease: An Interventional StudyN R Reddy HemanthNo ratings yet
- Radish Raphanus Sativus Materia Medica HerbsDocument7 pagesRadish Raphanus Sativus Materia Medica HerbsAlejandra Guerrero100% (2)
- Hand When You Need Them MostDocument9 pagesHand When You Need Them MostJim SchotterNo ratings yet
- Delwa Star H&PDocument2 pagesDelwa Star H&Pnitsuga888No ratings yet
- BHP Formula No 55 Refrence - Aesculus Pentarkan PTK 3 Best Homeopathic Medicine For PilesDocument3 pagesBHP Formula No 55 Refrence - Aesculus Pentarkan PTK 3 Best Homeopathic Medicine For PilesKazy Habibur RahmanNo ratings yet
- Pathophysiology of HemorrhoidsDocument2 pagesPathophysiology of HemorrhoidsTrixie FayeNo ratings yet
- HEMMORRHOIDECTOMYDocument16 pagesHEMMORRHOIDECTOMYLily CentenoNo ratings yet
- Bruce Copen Homeopathy FormulasDocument205 pagesBruce Copen Homeopathy Formulasgpevicky007No ratings yet
- PR BleedDocument20 pagesPR BleedCathy KayNo ratings yet