Professional Documents
Culture Documents
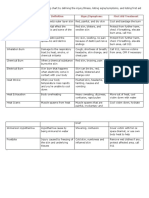
A. Primary Skin Lesions
A. Primary Skin Lesions
Uploaded by
Min MinOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
A. Primary Skin Lesions
A. Primary Skin Lesions
Uploaded by
Min MinCopyright:
Available Formats
Go Back to the Top
Chapter
To Order, Visit the Purchasing Page for Details
Skin Lesions
4
The most fundamental and important methods of medical examination for skin diseases are visual inspection
and palpation. The recent development of biochemical and immune system examination methods has made
diagnosis more accurate. However, naked-eye and dermoscopy inspection and palpation are always the most
important in acquiring information on the nature of skin lesions, including their distribution, form, color, shape
and firmness.
A skin lesion is generally called an eruption. Eruptions are divided into primary lesions, which occur in normal
skin, and secondary lesions, which are caused secondarily by other eruptions. This chapter briefly discusses
the terminology for describing the characteristics of various types of eruptions.
A. Primary skin lesions
Clinical images are available in hardcopy only.
An eruption that occurs in normal skin without any preexisting
eruptions is called a primary lesion. These include patches, where
the only change is color; papules, nodules and tumors, which are
elevated; blisters, cysts and pustules, which contain serum, keratinized substances, pus, etc.; and urticaria, which is temporarily
elevated.
1. Erythema
Fig. 4.1 Erythema.
Annular erythema in a patient with Sjgren syndrome.
Erythema is patchy redness produced by vasodilation and
hyperemia in the dermal papillae and the subpapillary layer
(Figs. 4.1 and 4.2). In erythema, although the blood volume
increases in the dermal blood vessels, there is no blood leakage
into the extravascular dermis. Thus the bloody color fades under
the pressure of a glass plate (diascopy). Erythema produced at the
periphery of other eruptions such as papules, bullae and pustules
is described as a red halo.
2. Purpura
Purpura is purple to bright red hemorrhaging in the skin (Figs.
4.2 and 4.3). The color of the blood does not fade in diascopy,
erythema
Unusual erythema and
purpura
purpura
pigmented macule
leukoderma
MEMO
Bleeding may occur in the superficial epidermis, making the epidermis appear red. The
red does not fade by diascopy, unlike in the
usual erythema. Vasodilation may occur in
the dermal deep layer, making that layer
appear purple.
telangiectasia extravasation melanin deposition
Fig. 4.2 Skin lesions.
Macule colors and their respective changes.
50
decrease of
melanin
A. Primary skin lesions
because hemorrhage causes blood leakage into the dermis, which
distinguishes it from erythema. A purpura of 2 mm or less in
diameter is called a petechia. A purpura that is larger than a
petechia is called ecchymosis, and an even larger elevated purpura is called a hematoma. The red of a purpura is fairly bright
shortly after bleeding begins (from the hemoglobin) but becomes
brownish (from hemosiderin) over time. When macrophages
phagocytose and decompose the leaked blood cells, the color
fades.
3. Pigmented macule
A pigmented macule is a patch of brown, yellow, blue or other
color, depending on the deposited substance (Figs. 4.2 and 4.4).
It is most commonly caused by deposition of melanin, the next
most common causes being deposition of hemosiderin, carotin,
bile pigment, drugs or other foreign substances (e.g., metal, charcoal).
The macule color changes from brown to blackish brown with
increased melanins in the epidermal basal layer, and ranges from
gray to purplish brown in the papillary dermis. It becomes blue
with deposition in the deep dermal layer. The sites of melanin
pigmentation in various diseases are listed in Fig. 4.5.
4
Clinical images are available in hardcopy only.
Fig. 4.3 Purpura.
Henoch-Schnlein purpura.
Clinical images are available in hardcopy only.
Fig. 4.4 Pigmented macule.
Senile freckle.
a
epidermis
dermis
Site of melanin deposition and disorder
Site of deposition
Color of lesion
Disorder
a) Intraepidermis~
dermo-epidermal junction
Black
nevus-cell nevus
(compound), malignant
melanoma
b) Basement membrane
Deep brown
Melasma, nevus spilus,
caf-au-lait spot
c) Basement membrane~ Brown to black
the middle of the epidermis
Clinical images are available in hardcopy only.
nevus-cell nevus
(junctional)
d) Dermal papilla
Violaceous to brown Lichen planus, incontinentia pigmenti, fixed
drug eruption
e) Deep dermis
Bluish
Mongolian spot, blue
nevus, Ota's nevus
Fig. 4.5 Association between the site of melanin deposition and
the color of the lesion.
51
Fig. 4.6 Leukoderma.
Vitiligo vulgaris.
52
Skin Lesions
keratotic
papule
serous
papule
solid
papule
perifollicular papule
Fig. 4.7 Various papules.
4. Leukoderma
Clinical images are available in hardcopy only.
Fig. 4.8 Papule.
Lichen nitidus.
Leukoderma is a white patch produced by depigmentation or
local anemia (Figs. 4.2 and 4.6). Depigmentation is caused by
abnormal production of melanins, such as in vitiligo vulgaris
(Chapter 16). Nevus anemicus causes local anemia leading to
leukoderma (Chapter 20). Leukoderma in the periphery of an
eruption is called a white halo.
5. Papule
Clinical images are available in hardcopy only.
Fig. 4.9 Nodule.
Dermatofibrosarcoma protuberans.
A papule is a localized elevated lesion of 10 mm or less in
diameter (Figs. 4.7 and 4.8) with a hemispheric or flat shape. It is
characterized by a surface that can be smooth, eroded, ulcerative,
hyperkeratotic or crusted. It may be caused by a proliferative or
inflammatory change in the epidermis, or by dermal edema.
Papules are distinguished by naked-eye observation as serous
(with a vesicle on the top; e.g., eczema and dermatitis), solid
(without blistering; e.g., neoplastic lesions, dermal edema), follicular (associated with hair follicles) or non-follicular (not associated with hair follicles).
6. Nodule, Tumor
A nodule is a localized lesion that appears as a papule with a
diameter of 10 to 20 mm (Fig. 4.9). It can have various causes,
such as tumor formation, granulomatous change, inflammation or
edema. An intensely proliferative nodule with an elevation of 30
mm or more in diameter is called a tumor.
7. Blister
A blister is a skin elevation of 5 mm or more in diameter
enclosed by a membrane and containing transparent fluid that is
mainly plasma and cellular material. A small blister with a diameter
A. Primary skin lesions
intraepidermal
bulla
subepidermal bulla
53
vesicles
4
Clinical images are available in hardcopy only.
Fig. 4.10 Blisters.
of less than 5 mm is called a vesicle (Figs. 4.10 and 4.11). A
hemorrhagic blister containing serum mixed with blood is
referred to as a bloody bulla.
A blister with a flaccid covering (flaccid bulla) breaks easily.
A flaccid bulla is often produced by exfoliation of the suprabasal
cell layer (e.g., in pemphigus or impetigo contagiosa). A bulla
with a thick, tight covering formed under the epidermis is called
a tense bulla (e.g., pemphigoid, dermatitis herpetiformis). It does
not break as easily as a flaccid bulla. During an infectious
episode, a variolar bulla is observed; this is a bulla with a central
a
concavity.
Blocked by the thick horny cell layer, a blister on the palms or
soles does not elevate, but presents a droplet-like appearance.
Such a blister is called a pompholyx. When it occurs in the
mucous membrane, the covering of the aphtha breaks spontaneously. Pompholyx with painful erosion and peripheral erythema are included in aphthae (Fig. 4.21).
Clinical images are available in hardcopy only.
Fig. 4.11 Blisters.
a: Bullous pemphigoid. b: Insect bite.
8. Pustule
A pustule is a yellowish blister with purulent contents (neutrophils) (Figs. 4.12 and 4.13). It may be produced by bacterial
infection or by leukocytes that migrate for some other reason
(sterile pustules). Diseases that produce multiple sterile pustules
are generally called pustuloses (Chapter 14).
Clinical images are available in hardcopy only.
Fig. 4.13 Pustule.
Palmoplantar pustulosis (localized pustular psoriasis).
pustule
cyst
neutrophils
Fig. 4.12 Pustule, cyst and wheal.
wheal (urticaria)
edema
54
Skin Lesions
9. Cyst
Clinical images are available in hardcopy only.
Fig. 4.14 Cyst.
Epidermal cyst.
Clinical images are available in hardcopy only.
A cyst is a closed tumorous lesion covered by a membranous
lining, which does not always elevate above the skin. The covering consists of epithelial tissue or connective tissue containing
keratinous substances (observed in epidermal cysts, for example)
or fluid components (e.g., in eccrine and apocrine hydrocystomas) (Figs. 4.12 and 4.14).
10. Wheal, Urticaria
Urticaria is localized edema that disappears in a short period of
time (usually within several hours, and always within 24 hours).
It usually appears light pink with a slightly flat elevation. It is
accompanied by itching and heals without scarring in most cases
(Figs. 4.12 and 4.15). Wheal and urticaria are often use synonymously, although the former is the name of an eruption and
the latter is a condition presenting these eruptions.
Fig. 4.15 Wheal.
Acute urticaria.
B. Secondary skin lesions
A secondary lesion is an eruption that occurs secondarily after
a primary or other skin lesion.
Clinical images are available in hardcopy only.
Fig. 4.16 Atrophy.
Widespread striae atrophicae.
1. Atrophy
Skin atrophy is when skin becomes thin or has a smooth or
finely wrinkled surface (Figs. 4.16 and 4.17). The secretory function is reduced, and the skin surface dries. Aging leads to skin
atrophy, including subcutaneous lipoatrophy, striae atrophicae
caused by steroids (Chapter 18), kraurosis vulvae and macular
atrophy.
epidermis
dermis
subcutaneous
tissue
atrophy
hypertrophic scar
Fig. 4.17 Atrophy and hypertrophic scar.
Go Back to the Top
To Order, Visit the Purchasing Page for Details
You might also like
- NCP - Impaired Skin IntegrityDocument3 pagesNCP - Impaired Skin IntegrityFlauros Ryu Jabien90% (30)
- Conveyor Belt Splicing GuideDocument13 pagesConveyor Belt Splicing Guidemrkadu_61No ratings yet
- Foot Spray by Krisha Cosmetic PVT - LTDDocument27 pagesFoot Spray by Krisha Cosmetic PVT - LTDKalpesh PatilNo ratings yet
- Derma Slides 2017Document268 pagesDerma Slides 2017Nadia AlmahalawiNo ratings yet
- DMS. K12. DermatopathologyDocument64 pagesDMS. K12. DermatopathologymissirenaNo ratings yet
- Boli de PieleDocument44 pagesBoli de PieleAndreea CiaușuNo ratings yet
- Kulit-Perubahan Dasar Histologis PrintDocument38 pagesKulit-Perubahan Dasar Histologis PrintWirman RamadhanNo ratings yet
- 001 - Skin AnatomyDocument46 pages001 - Skin AnatomyLucas Victor AlmeidaNo ratings yet
- Derma 3Document19 pagesDerma 3thackeryuktaNo ratings yet
- Safari - 26 Mar 2023, 11:28 AMDocument1 pageSafari - 26 Mar 2023, 11:28 AMErza KabashiNo ratings yet
- Litvinenko Introduction Dermatology EngDocument40 pagesLitvinenko Introduction Dermatology EngSoni SarthakNo ratings yet
- Basic Skin Lesions: Presented By: Dr. Divyank A. Vankawala Jr. Resident, Dermatology Dept., NDMVPS VP Medical CollegeDocument46 pagesBasic Skin Lesions: Presented By: Dr. Divyank A. Vankawala Jr. Resident, Dermatology Dept., NDMVPS VP Medical CollegeniveditakartikNo ratings yet
- 1.introduction To DermatologyDocument57 pages1.introduction To DermatologyMutasım Battah100% (2)
- Localized Area of Color or Texural Changes in The Skin. Macule May Me HypoDocument4 pagesLocalized Area of Color or Texural Changes in The Skin. Macule May Me Hypo123456No ratings yet
- Integumentary DisorderDocument6 pagesIntegumentary Disorderhxqf25mbvvNo ratings yet
- Efflorescence of The Skin Lesions: Dr. M. Izazi HP, SP - KKDocument40 pagesEfflorescence of The Skin Lesions: Dr. M. Izazi HP, SP - KKSaputra Tri NopiantoNo ratings yet
- Q.1 Components of Skin: The Skin: Basic Structure and FunctionDocument7 pagesQ.1 Components of Skin: The Skin: Basic Structure and Functionnani100No ratings yet
- Primary and Secondary Skin Lesions - IJDocument43 pagesPrimary and Secondary Skin Lesions - IJThanh Thảo Huỳnh ThịNo ratings yet
- 21 Benign Skin TumorsDocument4 pages21 Benign Skin TumorsAbdul Ghaffar AbdullahNo ratings yet
- EfloresensiDocument40 pagesEfloresensimariamunsriNo ratings yet
- 0.skin Pathology - LectureDocument62 pages0.skin Pathology - LectureUgaugaaNo ratings yet
- Skin LesionDocument5 pagesSkin LesionDominic SohNo ratings yet
- Diskripsi Lesi Di Rongga MulutDocument8 pagesDiskripsi Lesi Di Rongga Mulutdian permata pratamaNo ratings yet
- 2016 DermTerms & Dx-1Document53 pages2016 DermTerms & Dx-1vivekNo ratings yet
- 2011-07-PATHO-Basic Pathology of SkinDocument17 pages2011-07-PATHO-Basic Pathology of SkindtimtimanNo ratings yet
- 9-Patologi Skin PDFDocument34 pages9-Patologi Skin PDFririnNo ratings yet
- The Integumentary SystemDocument7 pagesThe Integumentary SystemKathleenJoyGalAlmasinNo ratings yet
- Dermatology+Review 2015 BATCH SOLVEDDocument7 pagesDermatology+Review 2015 BATCH SOLVEDMati ullah KhanNo ratings yet
- Dermatology NotesDocument59 pagesDermatology NotesAbdullah Matar Badran50% (2)
- Skin Examination 1Document17 pagesSkin Examination 1Daffa AmaliaNo ratings yet
- Dermatofibroma Scopus Andi HardiantyDocument8 pagesDermatofibroma Scopus Andi HardiantyJulian LeeNo ratings yet
- Skin LesionsDocument7 pagesSkin LesionsGurbir Singh GillNo ratings yet
- Introduction To Dermatology: Lecture-1Document33 pagesIntroduction To Dermatology: Lecture-1Latika ChoudhuryNo ratings yet
- Sms KBDocument3 pagesSms KBdarshinidaveNo ratings yet
- Dermatology LexiconDocument5 pagesDermatology LexiconMuhammad Luqman Nul HakimNo ratings yet
- Description of Oral LesionsDocument6 pagesDescription of Oral LesionsVanshika JainNo ratings yet
- Dr. Igwe DISEASE OF THE SKIN - Doc-1Document11 pagesDr. Igwe DISEASE OF THE SKIN - Doc-1Jake MillerNo ratings yet
- Type of Skin Lesions: Dermatovenereology Departement / Division Dr. Moh. Hoesin Hospital / Medical Faculty UNSRI 2011Document35 pagesType of Skin Lesions: Dermatovenereology Departement / Division Dr. Moh. Hoesin Hospital / Medical Faculty UNSRI 2011Dipika Awinda0% (1)
- Primary Skin LesionDocument7 pagesPrimary Skin Lesion_carido_No ratings yet
- 1ry & 2ry Lesions DermatologyDocument9 pages1ry & 2ry Lesions DermatologyHassan.shehriNo ratings yet
- .Nursing in Dermatology. - 1700566942000Document53 pages.Nursing in Dermatology. - 1700566942000sagessenguegangNo ratings yet
- Intertegumentary SystemDocument5 pagesIntertegumentary SystemRoxana AnaNo ratings yet
- Skin-PathologyDocument32 pagesSkin-PathologyArfa BaigNo ratings yet
- Lesi KulitDocument20 pagesLesi KulitahdazuhriNo ratings yet
- CPC 1 Jan 12 2008 DR RuengerDocument92 pagesCPC 1 Jan 12 2008 DR Ruengerkhawar93No ratings yet
- Dermatology 1Document47 pagesDermatology 1Edwin OkonNo ratings yet
- E. Cysts: 10. Hidradenoma PapilliferumDocument4 pagesE. Cysts: 10. Hidradenoma PapilliferumTaufiq HidayatNo ratings yet
- Skin LesionsDocument4 pagesSkin LesionsRose Marceline Patague TalubanNo ratings yet
- Morphological ElementsDocument6 pagesMorphological ElementsMohammad AkkadNo ratings yet
- Meth Elab Topic N2Document19 pagesMeth Elab Topic N2Group M1869No ratings yet
- FNP: Skin ReviewDocument11 pagesFNP: Skin ReviewOMGStudy100% (2)
- Power Point Week #3Document182 pagesPower Point Week #3Raelene MarceauNo ratings yet
- Epidermis: Sebaceous/oil GlandsDocument3 pagesEpidermis: Sebaceous/oil GlandsDeepthi VallabhaneniNo ratings yet
- General Surgery Copy 2Document37 pagesGeneral Surgery Copy 2sowmyaraja09No ratings yet
- PENDAHULUAN - EfloresensiDocument50 pagesPENDAHULUAN - EfloresensiSucitri NyomanNo ratings yet
- Lesions PPT NewDocument37 pagesLesions PPT NewDeb SharmaNo ratings yet
- SBRC DermatologyDocument83 pagesSBRC DermatologyErin HillNo ratings yet
- AcneDocument14 pagesAcneIbrahim MansarayNo ratings yet
- Morphology of Skin LesionsDocument20 pagesMorphology of Skin LesionsHasanin SheikhNo ratings yet
- Acne PresentationDocument11 pagesAcne Presentationnotyourakiko18No ratings yet
- Dermatology Atlas for Medical StudentsFrom EverandDermatology Atlas for Medical StudentsRating: 4 out of 5 stars4/5 (6)
- Man As A SubjectDocument21 pagesMan As A SubjectMin MinNo ratings yet
- Staff Satisfaction Survey ToolsDocument17 pagesStaff Satisfaction Survey ToolsMin MinNo ratings yet
- Analysis of Work Life Balance of Female Nurses in Hospitals - Comparative Study Between Government and Private Hospital in Chennai, TN., IndiaDocument6 pagesAnalysis of Work Life Balance of Female Nurses in Hospitals - Comparative Study Between Government and Private Hospital in Chennai, TN., IndiaMin MinNo ratings yet
- Questionnaire Survey of Working Relationships Between Nurses and Doctors in University Teaching Hospitals in Southern NigeriaDocument22 pagesQuestionnaire Survey of Working Relationships Between Nurses and Doctors in University Teaching Hospitals in Southern NigeriaMin MinNo ratings yet
- 2014 Rashid Et Al CCNQ InPressDocument38 pages2014 Rashid Et Al CCNQ InPressMin MinNo ratings yet
- HeadToToeSkinAssessment BrownDocument34 pagesHeadToToeSkinAssessment BrownMin MinNo ratings yet
- A Review of Instruments Measuring Nurse-Physician CollaborationDocument10 pagesA Review of Instruments Measuring Nurse-Physician CollaborationMin MinNo ratings yet
- Betty Neuman Systems ModelDocument18 pagesBetty Neuman Systems ModelMin Min50% (2)
- Performance Apparel Markets Sample PDFDocument115 pagesPerformance Apparel Markets Sample PDFViziteu Diana-RoxanaNo ratings yet
- Contoh ReportDocument16 pagesContoh ReportAiniNo ratings yet
- (EXCELENT - Excelente) Survival Guide (AKA DOOM) 2.1 - Guia e Manual de Sobrevivência - A5Document311 pages(EXCELENT - Excelente) Survival Guide (AKA DOOM) 2.1 - Guia e Manual de Sobrevivência - A5jhongaNo ratings yet
- Sensory Re-Education: Hand Physiotherapy DepartmentDocument2 pagesSensory Re-Education: Hand Physiotherapy DepartmentEmanuel George StoenescuNo ratings yet
- Cold Stress PDFDocument2 pagesCold Stress PDFfriends_nalla100% (1)
- Cas Sim RecipesDocument5 pagesCas Sim RecipesnevanaaaNo ratings yet
- Assignment 9Document3 pagesAssignment 9Tamarion JohnsonNo ratings yet
- Putoolssect7 PDFDocument63 pagesPutoolssect7 PDFRinaNo ratings yet
- MARSI Implications in Vascular AccessDocument25 pagesMARSI Implications in Vascular AccessdedyNo ratings yet
- NSTP Group 3 First Aid ReportingDocument44 pagesNSTP Group 3 First Aid ReportingCindy GeverolaNo ratings yet
- S12 15 Operation ManualDocument18 pagesS12 15 Operation ManualRein Jhonnaley DiosoNo ratings yet
- BURNS BurnDocument5 pagesBURNS BurnWiljohn de la CruzNo ratings yet
- Skin and NailsDocument2 pagesSkin and NailsJosé Henríquez GalánNo ratings yet
- 212 Cupping Proof PDFDocument7 pages212 Cupping Proof PDFWilyanto YangNo ratings yet
- 1 First Aid and Emergency Procedures CourseDocument25 pages1 First Aid and Emergency Procedures Coursebalamurugan sNo ratings yet
- Safety Practices in Outdoor RecreationDocument39 pagesSafety Practices in Outdoor RecreationJen E.No ratings yet
- DOOM Survival Guide 2.0 - A5Document265 pagesDOOM Survival Guide 2.0 - A5rungoodNo ratings yet
- Kilimanjaro Packing ListDocument2 pagesKilimanjaro Packing ListAfaq AhmadNo ratings yet
- MGD Hand-Safety-PresentationDocument46 pagesMGD Hand-Safety-PresentationAndre Ant WilliamsNo ratings yet
- BAJR Guide 31 Dig SurvivorDocument10 pagesBAJR Guide 31 Dig SurvivorDavid Connolly100% (3)
- Textbook of Dermatology For Homoeopaths R Gupta and R K Manchanda Reading ExcerptDocument19 pagesTextbook of Dermatology For Homoeopaths R Gupta and R K Manchanda Reading ExcerptVidhi JobanputraNo ratings yet
- Basic MoulageDocument3 pagesBasic MoulageLewis HazenNo ratings yet
- Subcorneal Pustular Dermatosis Draft Update January 2017 - Lay Review January 2017Document3 pagesSubcorneal Pustular Dermatosis Draft Update January 2017 - Lay Review January 2017Andi Hardianti SucitraNo ratings yet
- Wilderness Survival SkillsDocument22 pagesWilderness Survival SkillsPublius Ovidius NasoNo ratings yet
- Service Bulletin: SB MBB-BK117 C-2-62-006Document11 pagesService Bulletin: SB MBB-BK117 C-2-62-006Alexander OquendoNo ratings yet
- Chicken PoxDocument1 pageChicken PoxmarincewNo ratings yet
- Basic Foot Care GuideDocument10 pagesBasic Foot Care GuidelaskarNo ratings yet