Professional Documents
Culture Documents
PGHN 17 162
PGHN 17 162
Uploaded by
Melany Sii PenghayalCopyright:
Available Formats
You might also like
- Quiz ImmunologyDocument50 pagesQuiz ImmunologyMedShare97% (39)
- Hearing Loss in Term Newborn Infants With Hypoxic-Ischemic Encephalopathy Treated With Therapeutic Hypothermia PDFDocument8 pagesHearing Loss in Term Newborn Infants With Hypoxic-Ischemic Encephalopathy Treated With Therapeutic Hypothermia PDFstefanp89No ratings yet
- 1 Predict NeoDocument5 pages1 Predict NeoGary Carhuamaca LopezNo ratings yet
- IJN Volume 10 Issue 2 Pages 50-54Document5 pagesIJN Volume 10 Issue 2 Pages 50-54DavidNo ratings yet
- PIH Renal Doppler Pregnancy - CutDocument4 pagesPIH Renal Doppler Pregnancy - CutAnonymous 9QxPDpNo ratings yet
- The Effect of Human Recombinant Erythropoietin On Prevention of Anemia of PrematurityDocument6 pagesThe Effect of Human Recombinant Erythropoietin On Prevention of Anemia of PrematuritySri Nowo MinartiNo ratings yet
- Early Feeding in Acute Pancreatitis in Children A Randomized Controlled TrialDocument9 pagesEarly Feeding in Acute Pancreatitis in Children A Randomized Controlled TrialvalenciaNo ratings yet
- Newborn Screening - Dr. T. GhoshDocument32 pagesNewborn Screening - Dr. T. GhoshMontu ChakmaNo ratings yet
- Incidence, Predictors and Outcome of Sepsis Associated Liver Injury in Children: A Prospective Observational StudyDocument9 pagesIncidence, Predictors and Outcome of Sepsis Associated Liver Injury in Children: A Prospective Observational StudyindahkputriNo ratings yet
- Electronic Physician (ISSN: 2008-5842)Document5 pagesElectronic Physician (ISSN: 2008-5842)Aldian DianNo ratings yet
- Irisin in AdolecenceDocument4 pagesIrisin in Adolecencemiss beeNo ratings yet
- Biochemical Marker As Predictor of Outcome in Perinatal AsphyxiaDocument4 pagesBiochemical Marker As Predictor of Outcome in Perinatal AsphyxiaAgus WijataNo ratings yet
- Heart Rate Variability Alterations in Infants With Spontaneous HypertoniaDocument8 pagesHeart Rate Variability Alterations in Infants With Spontaneous HypertoniaAlexis Arce AlvarezNo ratings yet
- Acute PancreatitisDocument9 pagesAcute PancreatitisJayari Cendana PutraNo ratings yet
- Effect of A Probiotic Infant Formula On Infections in Child Care Centers Pediatrics-2005-Weizman-5-9Document7 pagesEffect of A Probiotic Infant Formula On Infections in Child Care Centers Pediatrics-2005-Weizman-5-9Yuktika RiYuNo ratings yet
- Renal Resistive Index in Patients With Polycystic Ovary SyndromeDocument5 pagesRenal Resistive Index in Patients With Polycystic Ovary Syndromemeltwithsnow163.comNo ratings yet
- Characteristics of Pediatric Patients With Diarrhea in Indonesia: A Laboratory-Based ReportDocument8 pagesCharacteristics of Pediatric Patients With Diarrhea in Indonesia: A Laboratory-Based ReportDrnNo ratings yet
- Growth After Adenotonsillectomy For Obstructive Sleep Apnea: An RCTDocument10 pagesGrowth After Adenotonsillectomy For Obstructive Sleep Apnea: An RCTCalvin AffendyNo ratings yet
- Bodyweight Loss in Predicting Neonatal Hyperbilirubinemia 72 Hours After Birth in Term Newborn InfantsDocument8 pagesBodyweight Loss in Predicting Neonatal Hyperbilirubinemia 72 Hours After Birth in Term Newborn InfantsAhtarunnisa Fauzia HanifaNo ratings yet
- Ma 70 408Document5 pagesMa 70 408Zahra AfifahNo ratings yet
- Animals 11 00685 v3Document12 pagesAnimals 11 00685 v3Carolina Duque RodriguezNo ratings yet
- Growth After AdenotonsillectomyDocument10 pagesGrowth After AdenotonsillectomyfriscahalimNo ratings yet
- 2010 Article 69Document6 pages2010 Article 69gepang_metalNo ratings yet
- Nutritional Assessment of Children With CHD CompareDocument9 pagesNutritional Assessment of Children With CHD CompareIntan Robi'ahNo ratings yet
- 11 134 v12n4 2013 PredictingPortalDocument11 pages11 134 v12n4 2013 PredictingPortalDevy Widiya GrafitasariNo ratings yet
- Early - and Late-Onset Preeclampsia A ComprehensiveDocument10 pagesEarly - and Late-Onset Preeclampsia A ComprehensiveEriekafebriayana RNo ratings yet
- Eke2019 PDFDocument1 pageEke2019 PDFWijitha VarenniNo ratings yet
- Original Article: The Effect of Neonatal Asphyxia On Renal FunctionDocument6 pagesOriginal Article: The Effect of Neonatal Asphyxia On Renal FunctionelizabethpurbaNo ratings yet
- Bloody Stool Journal 2Document8 pagesBloody Stool Journal 2dr.herusetiawanNo ratings yet
- Conjugated Hyperbilirubinemia in The Neonatal Intensive Care UnitDocument9 pagesConjugated Hyperbilirubinemia in The Neonatal Intensive Care UnitIvan HoNo ratings yet
- RESEARCH ARTICLEOpen AccessChallenges of Acute Peritoneal Dialysis Inextremely-Low-Birth-Weight Infants - Aretrospective Cohort StudyDocument9 pagesRESEARCH ARTICLEOpen AccessChallenges of Acute Peritoneal Dialysis Inextremely-Low-Birth-Weight Infants - Aretrospective Cohort StudysavitageraNo ratings yet
- Materials and MethodsDocument3 pagesMaterials and MethodssurtitejoNo ratings yet
- Knowledge Level and Determinants of Neonatal Jaundice A Cross-Sectional Study in The Effutu Municipality of GhanaDocument10 pagesKnowledge Level and Determinants of Neonatal Jaundice A Cross-Sectional Study in The Effutu Municipality of GhananicloverNo ratings yet
- Sii ArtículoDocument5 pagesSii ArtículoMonserrat Garduño FonsecaNo ratings yet
- Status of Serum Bilirubin, Serum Proteins and Prothrombin Time in Babies With Perinatal AsphyxiaDocument4 pagesStatus of Serum Bilirubin, Serum Proteins and Prothrombin Time in Babies With Perinatal AsphyxiaAgus WijataNo ratings yet
- Complementary and Alternative Medical Lab Testing Part 5: GastrointestinalFrom EverandComplementary and Alternative Medical Lab Testing Part 5: GastrointestinalNo ratings yet
- Anemia de PrematDocument7 pagesAnemia de Prematmedibase12No ratings yet
- Jurnal AKIDocument7 pagesJurnal AKIAnonymous Vz9teLNo ratings yet
- Non Protein Calorie - NPCDocument6 pagesNon Protein Calorie - NPCmarkus_danusantosoNo ratings yet
- ACPN AbstractsDocument21 pagesACPN AbstractsPediatric NephrologyNo ratings yet
- The Effect of Thickened-Feed Interventions On Gastroesophageal RefluxDocument13 pagesThe Effect of Thickened-Feed Interventions On Gastroesophageal Refluxminerva_stanciuNo ratings yet
- Hidronefrosis 3Document11 pagesHidronefrosis 3Zwinglie SandagNo ratings yet
- DUDDING Et Al-2008-Journal of Thrombosis and HaemostasisDocument8 pagesDUDDING Et Al-2008-Journal of Thrombosis and HaemostasisNur Ainatun NadrahNo ratings yet
- Both Fecal Calprotectin and Imuno Test in Children IBDDocument13 pagesBoth Fecal Calprotectin and Imuno Test in Children IBDdichafrNo ratings yet
- 1121PGHN - PGHN 23 266Document10 pages1121PGHN - PGHN 23 266justmokhtarNo ratings yet
- A Systematic Review and Meta-Analysis of The Benefits of ADocument10 pagesA Systematic Review and Meta-Analysis of The Benefits of Adhimas satriaNo ratings yet
- 2018 Revised Reference Values For The Intake of ProteinDocument15 pages2018 Revised Reference Values For The Intake of ProteinNayaNo ratings yet
- Metabolic Syndrome in Very Low Birth Weight Young Adults and Controls: The New Zealand 1986 VLBW StudyDocument11 pagesMetabolic Syndrome in Very Low Birth Weight Young Adults and Controls: The New Zealand 1986 VLBW StudysatishNo ratings yet
- Impact of Disease Severity On Gastric Residual Volume in Critical PatientsDocument16 pagesImpact of Disease Severity On Gastric Residual Volume in Critical PatientsSelliEfridaSiahaanNo ratings yet
- Doppler and Biophysical Assessment in Growth Restricted Fetuses: Distribution of Test ResultsDocument7 pagesDoppler and Biophysical Assessment in Growth Restricted Fetuses: Distribution of Test ResultslalimdNo ratings yet
- WilsonDocument11 pagesWilsonCarmen OpreaNo ratings yet
- Subjective Global Nutritional Assessment For Children: Donna J Secker and Khursheed N JeejeebhoyDocument7 pagesSubjective Global Nutritional Assessment For Children: Donna J Secker and Khursheed N Jeejeebhoynurul_putrieNo ratings yet
- Efficacy of A New Hypotonic Oral Rehydration Solution Containing Zinc and Prebiotics in The Treatment of Childhood Acute Diarrhea: A Randomized Controlled TrialDocument6 pagesEfficacy of A New Hypotonic Oral Rehydration Solution Containing Zinc and Prebiotics in The Treatment of Childhood Acute Diarrhea: A Randomized Controlled TrialOlpinNo ratings yet
- Feeding Practice During Transfusion in Preterm Infants: Muhamad Azharry RullyDocument26 pagesFeeding Practice During Transfusion in Preterm Infants: Muhamad Azharry Rullytrie dolleNo ratings yet
- Chest 147 1 132Document8 pagesChest 147 1 132Timothy Eduard A. SupitNo ratings yet
- SII, FODMAPS e Hormonios EndócrinosDocument7 pagesSII, FODMAPS e Hormonios Endócrinosmari bNo ratings yet
- Jurnal Hiperemesis GravidarumDocument6 pagesJurnal Hiperemesis GravidarumArief Tirtana PutraNo ratings yet
- Study of Clinical, Biochemical Evaluation and Outcome in Hypertrophic Pyloric StenosisDocument4 pagesStudy of Clinical, Biochemical Evaluation and Outcome in Hypertrophic Pyloric StenosiszapomannNo ratings yet
- Endocrine and Metabolic Evaluation of Human Immunodeficiency Virus-Infected Patients With Evidence of Protease Inhibitor-Associated LipodystrophyDocument7 pagesEndocrine and Metabolic Evaluation of Human Immunodeficiency Virus-Infected Patients With Evidence of Protease Inhibitor-Associated LipodystrophydocumentosdescribdNo ratings yet
- Dyspepsia Journal PediatricDocument11 pagesDyspepsia Journal PediatricFatt ZakiNo ratings yet
- Complementary and Alternative Medical Lab Testing Part 8: UrologyFrom EverandComplementary and Alternative Medical Lab Testing Part 8: UrologyRating: 3 out of 5 stars3/5 (1)
- Ducks Out of Water - Duck Industry CrueltyDocument55 pagesDucks Out of Water - Duck Industry CrueltyVegan Future100% (1)
- Olbas Cough Syrup LabelDocument1 pageOlbas Cough Syrup LabelMulayam Singh YadavNo ratings yet
- Meat and FishDocument26 pagesMeat and FishPoorani ArunachalamNo ratings yet
- Cocculus IndicusDocument29 pagesCocculus IndicusShah FaisalNo ratings yet
- Reproductive HealthDocument21 pagesReproductive HealthRosalie Valdez EspirituNo ratings yet
- Smallest Dog Breeds in The WorldDocument5 pagesSmallest Dog Breeds in The WorldtourisminfopediaNo ratings yet
- 1 Journal 2 Kid Mortality LRRDDocument8 pages1 Journal 2 Kid Mortality LRRDErdachewNo ratings yet
- A Pattern Approach To Lymph Node Diagnosis - A. Leong (Springer, 2011) WWDocument432 pagesA Pattern Approach To Lymph Node Diagnosis - A. Leong (Springer, 2011) WWAdrian TirlaNo ratings yet
- Emergency Acupressure TreatmentDocument39 pagesEmergency Acupressure TreatmentNarayana Mugalur100% (1)
- Reva Rubin Maternal Role Attainment TheoryDocument4 pagesReva Rubin Maternal Role Attainment TheoryLeonard LigutomNo ratings yet
- Alergi Susu SapiDocument2 pagesAlergi Susu SapiMaya FikriNo ratings yet
- Aquila Pomarina X Clanga ClangaDocument14 pagesAquila Pomarina X Clanga ClangaCristinaNo ratings yet
- Case Presentation For Head InjuryDocument65 pagesCase Presentation For Head InjuryYdynn Parejas GavinaNo ratings yet
- 2 Neurophysiology of Somatic Sensations 2012Document6 pages2 Neurophysiology of Somatic Sensations 2012Nephritery Joy Espiritu JimenezNo ratings yet
- Structure and Life Cycle of The Housefly (With Diagram)Document16 pagesStructure and Life Cycle of The Housefly (With Diagram)rajesh kumar ranjan100% (1)
- Urethral Catheterization 1Document31 pagesUrethral Catheterization 1Hilman HadiansyahNo ratings yet
- E49 - MDM 20 KG - África Do Sul - Especificação Técnica 121 (1) .PT - enDocument6 pagesE49 - MDM 20 KG - África Do Sul - Especificação Técnica 121 (1) .PT - encid ribeiroNo ratings yet
- EO No.-31 s.2013 Anti-Rabies CouncilDocument5 pagesEO No.-31 s.2013 Anti-Rabies Councilmaryson primo100% (1)
- Because of Winn-Dixie VocabDocument5 pagesBecause of Winn-Dixie VocabBrad MorganNo ratings yet
- Intestinal Parasites: Comparative Morphology FiguresDocument14 pagesIntestinal Parasites: Comparative Morphology FiguresRica UyNo ratings yet
- HematopoiesisDocument3 pagesHematopoiesisVino OrajayNo ratings yet
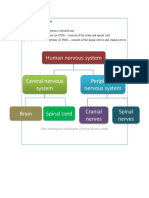
- Chart Showing The Classification of Human Nervous SystemDocument6 pagesChart Showing The Classification of Human Nervous Systemamala raviNo ratings yet
- Guna-Tf: G GU UN NA A - TTFFDocument18 pagesGuna-Tf: G GU UN NA A - TTFFantudwo33No ratings yet
- Animal Classification Practice TestDocument2 pagesAnimal Classification Practice TestElpi FerrerNo ratings yet
- Etimology Prefix Suffix RootDocument61 pagesEtimology Prefix Suffix RootivonneNo ratings yet
- Uptake and Distribution of Inhalational AnaestheticsDocument125 pagesUptake and Distribution of Inhalational Anaestheticsharsha mummakaNo ratings yet
- Brush Up On Oral AssessmentDocument3 pagesBrush Up On Oral Assessmentaus4us3No ratings yet
- Cancer - Rath, Matthias PDF (Pauling-Rath Therapy Protocol: Vitamin C and Lysine)Document84 pagesCancer - Rath, Matthias PDF (Pauling-Rath Therapy Protocol: Vitamin C and Lysine)Anonymous Jap77xvqPKNo ratings yet
- Try in of Waxed Up DenturesDocument58 pagesTry in of Waxed Up DenturesRohan Grover100% (1)
PGHN 17 162
PGHN 17 162
Uploaded by
Melany Sii PenghayalOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
PGHN 17 162
PGHN 17 162
Uploaded by
Melany Sii PenghayalCopyright:
Available Formats
pISSN: 2234-8646 eISSN: 2234-8840
http://dx.doi.org/10.5223/pghn.2014.17.3.162
Pediatr Gastroenterol Hepatol Nutr 2014 September 17(3):162-169
PGHN
Original Article
Serum Liver Enzyme Pattern in Birth Asphyxia Associated Liver
Injury
Nanda Chhavi, Kiran Zutshi, Niranjan Kumar Singh, Ashish Awasthi* and Amit Goel
Department of Pediatrics, Vivekananda Polyclinic and Institute of Medical Sciences, Departments of *Biostatistics & Health
Informatics and Gastroenterology, Sanjay Gandhi Postgraduate Institute of Medical Sciences, Lucknow, UP, India
Purpose: To study temporal pattern of serum liver enzymes levels in newborns with hepatic injury associated with
birth asphyxia (BA).
Methods: Singleton term newborns with BA and 72 hours of age admitted to neonatal intensive care unit were
prospectively enrolled. Term newborns with physiological jaundice and without BA were studied as controls. Serum
liver enzymes were measured at 24 hours, 24-72 hours, and at 6-12 days of age for cases and at 1-6 days of
age for controls. BA was defined by 1 minute Apgar score 7 or delayed or absent cry with hypoxic ischemic
encephalopathy. BA-associated liver injury was defined as serum alanine aminotransferase (ALT) elevation beyond
+2 standard deviation (ALT > +2 SD) above the mean of control subjects at any of the three time points.
Results: Sixty controls and 62 cases were enrolled. Thirty-five cases (56%) developed BA-associated liver injury
(ALT81 IU/L). They had higher serum levels of ALT, aspartate aminotransferase, lactate dehydrogenase than
the control infants, with peak at 24-72 hours. In controls, serum liver enzyme levels were significantly higher in appropriate-for-date (AFD) babies than small-for-date (SFD) babies. Serum enzyme pattern and extent of elevation were
comparable between SFD and AFD babies. Degree of serum liver enzyme elevation had no relationship with severity
of hypoxic encephalopathy.
Conclusion: Serum liver enzyme elevation is common in BA; it peaks at 24-72 hours followed by a sharp decline
by 6-12 days of age. Pattern and extent of enzyme elevation are comparable between SFD and AFD babies.
Key Words: Asphyxia neonatorum, Hepatitis, Ischemia, Transaminases
INTRODUCTION
Birth asphyxia (BA), defined as Apgar score of below 7 at 1 minute after birth [1], is a common cause
of neonatal morbidity and mortality. Recent estimates attribute 17.2% of neonatal deaths worldwide
to BA or birth trauma [2]. BA has damaging effects
on several body organ systems [3,4]. Extent of such
ReceivedMay 20, 2014, RevisedJune 18, 2014, AcceptedJune 26, 2014
Corresponding author: Amit Goel, Department of Gastroenterology, Sanjay Gandhi Postgraduate Institute of Medical Sciences, Lucknow, UP
226014, India. Tel: +91-876-597-4037, Fax: +91-522-2668078, E-mail: agoel.ag@gmail.com
Copyright 2014 by The Korean Society of Pediatric Gastroenterology, Hepatology and Nutrition
This is an openaccess article distributed under the terms of the Creative Commons Attribution NonCommercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits
unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
PEDIATRIC GASTROENTEROLOGY, HEPATOLOGY & NUTRITION
Nanda Chhavi, et alLiver Injury in Birth Asphyxia
organ injury depends on several factors such as gestational age (GA) of the baby, time of onset of BA
(antepartum, intrapartum, or postpartum), and severity and duration of BA. Several studies are available on BA-related injury to brain [5-7], kidneys
[8,9], and heart [10,11].
BA leads to a chain of adaptive responses to curtail
the bodys oxygen requirement, in an attempt to tide
over the hypoxic crisis [12]. One such mechanism is
the so called diving reflex or redistribution of left
ventricular output in favor of more vital organs such
as brain, heart, and adrenals at the expense of reduced blood flow to non-vital organs such as kidneys,
lungs, gastrointestinal tract, and other abdominal
viscera [13]. Liver receives nearly three-fourth of its
blood supply from the portal vein and the rest
through the hepatic artery. The diving reflex is associated with reduced hepatic blood flow through
both the hepatic artery as well as the portal vein, since
the latter is determined by the amount of mesenteric
blood flow.
Hepatic injury is commonly assessed using serum
levels of enzymes which are released from injured
hepatocytes, namely alanine aminotransferase
(ALT), aspartate aminotransferase (AST) and lactate
dehydrogenase (LDH), which are commonly referred as the liver enzymes. Attempts have been
made previously to assess the hepatic damage in BA
[14]. However, data on the temporal pattern of serum levels of liver enzymes after BA are very scanty.
Such information may help to differentiate hepatic
injury due to BA from that due to other causes, and
to determine the babys outcome. We therefore studied the temporal pattern of serum levels of liver enzymes in newborns with hypoxic hepatic injury
(HHI) due to BA.
MATERIALS AND METHODS
This prospective case-control study was carried
out in the Neonatal Intensive Care Unit of Department of Pediatrics, Vivekananda Polyclinic and
Institute of Medical Sciences, Lucknow, India, between May 2007 and April 2008. It was approved by
the institutional ethical committee of Vivekananda
Polyclinic. Consecutive singleton newborns with BA,
delivered at 37 weeks GA and admitted within 72
hours of birth, were enrolled after obtaining written
informed consent from one of the parents. Babies
were excluded if a major congenital anomaly, sepsis,
inborn error of metabolism, congenital infection, hemolytic condition, hemorrhagic shock, or primary
hepato-biliary disease was identified or suspected.
Newborns delivered in our hospital and admitted
with physiological jaundice, without BA, were enrolled as controls.
BA was diagnosed if a newborn had features of hypoxic ischemic encephalopathy (HIE) along with one
of the following criteria (i) Apgar score 7 at 1 minute of life, or (ii) history of delayed cry (after 5 minutes of birth) or no cry after birth; this was as per the
guidelines laid down by National-Neonatal Perinatal
database network of India, which are widely accepted in the country [1]. HIE is a clinical syndrome
due to acute or sub-acute hypoxic brain injury, and is
defined clinically on the basis of a constellation of
neurological findings that include any combination
of altered muscle tone, altered sensorium, altered
deep tendon reflexes, absent primitive neonatal reflexes, dilated pupils and seizures. Severity of HIE
was assessed by using Sarnat & Sarnat staging system [7]. Babies were categorized, based on fetal
growth, as small-for-date (SFD, birth weight 10th
centile for GA), appropriate-for-date (AFD, birth
weight between 10th and 90th centile for GA), and
large-for-date (birth weight 90th centile for GA)
[1].
Complete antenatal, perinatal and neonatal history was recorded in a predefined data collection
form. In BA group, serum ALT, AST, LDH, alkaline
phosphatase, total protein, albumin, bilirubin (total
and conjugated), and prothrombin time (PT) were
measured at enrollment (24 hours) followed by
ALT, AST, and LDH measurements at 24-72 hours,
and at 6-12 days of life. Number of study samples obtained in an individual baby was decided by the age
of the baby at hospitalization. In control babies, venous specimens were collected once at 1-6 days of
www.pghn.org163
Pediatr Gastroenterol Hepatol Nutr
life. All specimens were collected when blood sampling was being done for standard clinical care and
were analyzed in central laboratory of the hospital.
HHI was defined by serum ALT elevation beyond
+2 standard deviation (SD) above the mean value in
control infants, at any time up to 12 days after birth.
ALT levels were used to define HHI because it is the
most specific serum marker of liver injury. By contrast, AST and LDH levels are widely present in other
body organs, and may thus be elevated in infants
with BA due to injury to red blood cells, or myocardial or skeletal muscle, and hence were not used
to define the liver injury.
Statistical analysis
Numerical data were expressed as mean and SD
and analyzed using t test. Categorical variables were
expressed as proportions and compared using 2 test.
The relationship of variables with each other was
studied using Pearsons coefficient. Statistical significance was considered at p-value0.05. Data
were analyzed using SPSS ver. 15.0 (SPSS Inc.,
Chicago, IL, USA).
RESULTS
The study included 60 healthy newborns (controls). Eighty eight newborns were screened for BA;
of those, 26 were excluded for various reasons
(prematurity 15, sepsis 8, shock 2 and major con-
genital anomaly 1) and 62 were enrolled in the study
(BA cases). The infants with BA were categorized into those with and those without HHI.
Findings in control babies
Clinical characteristics of controls are summarized
in Table 1. Controls with 72 hours and 73-144
hours of age had comparable liver function test results (Table 2). Among the controls, AFD babies had
significantly higher serum ALT (4721 IU/L vs.
268 IU/L; p0.001) and AST (6418 IU/L vs.
5019 IU/L; p=0.01) levels than the SFD babies;
whereas LDH levels (858215 IU/L vs. 739269
IU/L; p=0.09) were similar in AFD and SFD babies.
Male and female healthy babies had similar fetal
Table 1. Clinical Characteristics of Control Infants
Clinical variable
Age (h)
Sex (boy/girl)
GA (wk)
Apgar at 1 minute
Birth weight (g)
AFD/SFD/LFD (n)
Maternal age (y)
Controls (n=60)
9134
36/24
37.70.6
8.50.5
2,859540
40/20/0
24.73.5
Values are presented as meanstandard deviation or number.
GA: gestational age, AFD: appropriate-for-date (newborn with
birth weight between 10th and 90th centile for GA), SFD:
small-for-date (newborn with birth weight 10th centile for
GA), LFD: large-for-date (newborn with birth weight >90th
centile for GA).
Table 2. Liver Function Tests in Control Infants
Laboratory parameter
Overall (n=60)
Total protein (g/dL)
Serum albumin (g/dL)
Total bilirubin (mg/dL)
Direct bilirubin (mg/dL)
ALT (IU/L)
AST (IU/L)
LDH (IU/L)
Alkaline phosphatase (IU/L)
Prothrombin time (INR)
6.20.6
3.30.4
11.24.4
0.80.3
4021
6019
818239
10830
1.080.11
Age category
72 h (n=20)
73-144 h (n=40)
p-value
6.30.4
3.30.4
11.04.7
0.90.4
4016
6621
748281
11529
1.120.12
6.20.6
3.20.4
11.44.3
0.70.4
4023
5617
853210
10430
1.060.10
0.56
0.48
0.75
0.07
0.99
0.08
0.15
0.19
0.06
Values are presented as meanstandard deviation.
ALT: alanine aminotransferase, AST: aspartate aminotransferase, LDH: lactate dehydrogenase, INR: international normalized ratio.
164Vol. 17, No. 3, September 2014
Nanda Chhavi, et alLiver Injury in Birth Asphyxia
growth category distribution (AFD/SFD: 24/12 vs.
16/8; p=1.00), birth weight (2,928568 g vs.
2,755488 g; p=0.21), serum levels of proteins
(6.30.6 g/dL vs. 6.10.5 g/dL; p=0.09), total bilirubin (11.74.7 mg/dL vs. 10.63.9 mg/dL; p=0.32),
ALT (3820 IU/L vs. 4222 IU/L; p=0.54), AST
(5817 IU/L vs. 6122 IU/L; p=0.58) and LDH
(798278 IU/L vs. 848165 IU/L; p=0.38). However,
male babies were younger (age: 8333 hours vs.
10234 hours; p=0.04) and had higher albumin levels (3.40.4 g/dL vs.3.10.4 g/dL; p=0.005).
Controls versus infants with birth asphyxia
Based on the serum ALT levels in control group of
39.620.6 IU/L, ALT values of 81 IU/L (mean+
2SD) were used to define HHI in the BA group.
Among the 62 babies with BA, 35 (56%) had HHI
whereas 27 (44%) did not. The babies with BA were
comparable to the controls in sex ratio (45/62 [73%]
and 36/60 [60%] boys respectively; p=0.18), fetal
growth categories (AFD: 40/62 [64.5%] and 40/60
[66.7%] respectively; p=0.85) and birth weight
(2,700394 g and 2,859540 g respectively; p=0.07),
but differed in having been born at a lower GA
(37.30.8 wk and 37.70.6 wk respectively; p=0.003)
and having older mothers (26.64.0 y and 24.73.5 y
respectively; p=0.006).
Babies with and without hypoxic hepatic injury
Babies with and without HHI were comparable in
various clinical characteristics (Table 3) except that
the former had higher grades of HIE. However, a favorable final outcome was equally frequent in the babies with and without HHI.
Babies with birth asphyxia and hypoxic
hepatic injury
Serum liver enzymes measurements at all the
three time points (24 hours, 24-72 hours, and at
6-12 days) were available in 26 of the 35 babies
(74%) with HHI. Temporal pattern of liver enzyme
levels in these babies showed that ALT and LDH levels were significantly higher than controls at all
three time points, whereas the AST levels though
initially high, returned to normal at 6-12 days
(Table 4). All three serum liver enzymes showed the
maximum elevation at 24-72 hours of age, followed
by a sharp decline by the age of 6-12 days (Fig. 1).
Table 4. Pattern of Serum Liver Enzyme Levels at Three Time
Points in Babies with Birth Asphyxia and Hypoxic Hepatitis
Injury (n=26)
Liver enzyme
ALT (IU/L)
AST (IU/L)
LDH (IU/L)
Age
24 hours
24-72 hours
6-12 days
9767**
11591*
1,416838**
266238**
168123**
1,585770**
6937**
6425
1,070468*
Values are presented as meanstandard deviation.
ALT: alanine aminotransferase, AST: aspartate aminotransferase,
LDH: lactate dehydrogenase.
*p0.05, **p0.001, p-values are as compared to control
infants.
Table 3. Infants with Birth Asphyxia (BA), with and without Hypoxic Hepatic Injury (HHI)
Feature
BA with HHI (n=35)
BA but no HHI (n=27)
p-value
Sex (boy/girl)
Appropriate/small for dates
Gestational age (wk)
Birth weight (g)
Apgar score at 1 minute of life
Hypoxic ischemic encephalopathy grade I/II/III
Favorable outcome (yes/no)*
28/7
24/11
37.30.8
2,737392
4.41.2
5/18/12
26/9
17/10
16/11
37.30.9
2,652398
4.41.1
14/11/2
20/7
0.14
0.45
0.85
0.41
0.95
0.002
0.98
Values are presented as number or meanstandard deviation.
*Unfavorable outcome denotes neonatal death or discharge against medical advice.
Appropriate-for-dates: birth weight between 10th and 90th centile for gestational age. Small-for-dates: birth weight less than 10th
centile for gestational age.
www.pghn.org165
Pediatr Gastroenterol Hepatol Nutr
Fig. 3. Comparison of serum levels of aspartate aminotrans-
Fig. 1. Temporal pattern of serum levels of alanine aminotransferase (ALT), aspartate aminotransferase (AST), and lactate
dehydrogenase (LDH) in newborns with birth asphyxia and
hypoxic hepatic injury.
ferase (AST) in small-for-date (SFD) and appropriate-for-date
(AFD) infants. Bars represent means and error bars represent
standard deviation. *p0.05 when AST levels are compared
with corresponding SFD or AFD control infants. BA: birth
asphyxia, HHI: hypoxic hepatic injury, NS: not significant.
Levels of none of the serum liver enzymes levels at
any time point showed a correlation with the highest grade of HIE (range of correlation coefficients
for ALT [0.080.32], AST [0.090.07] and
LDH [0.220.16]).
AFD and SFD babies in HHI group, when compared to corresponding AFD and SFD controls, had
similar pattern of changes in serum ALT and AST
levels. Serum ALT levels were significantly elevated
till last estimation (Fig. 2) whereas AST levels were
normalized at 6-12 days (Fig. 3). Serum liver enzyme
levels were comparable between SFD and AFD babies
at all three time points in HHI group (Fig. 2 and 3).
DISCUSSION
Fig. 2. Comparison of serum levels of alanine aminotransferase
(ALT) in small-for-date (SFD) and appropriate-for-date (AFD)
infants. Bars represent means and error bars represents
standard deviation. *p0.05 when ALT levels are compared
with corresponding SFD or AFD control infants. BA: birth
asphyxia, HHI: hypoxic hepatic injury, NS: not significant.
166Vol. 17, No. 3, September 2014
HHI denotes injury caused to the hepatocytes by
hypoxia. It is characterized by a sudden rise in serum
levels of hepatic enzymes, starting soon after hypoxic insult, reaching a peak after 1-3 days of injury
and returning to normal after 7-10 days [15]. These
enzymes are present in cytosol (ALT, AST, and LDH)
and mitochondria (AST) of hepatocytes. Serum level
Nanda Chhavi, et alLiver Injury in Birth Asphyxia
of liver enzymes may increase either due to hepatocyte death or to an increase in cell membrane permeability which allows efflux of enzymes into the
blood [16].
Our observation of 56% of newborns with BA developing HHI lies well within the range of previous
observations of 39% to 85% prevalence of this condition [3,4,14,17,18]. This wide range could be due to
variations in criteria used in different studies to diagnose BA as well as HHI, severity of BA, time-points
used for serum transaminase estimation, cut-off
used for liver enzyme elevation, GA of the babies,
and other obstetrical or neonatal factors. A previous
prospective study had shown HHI in 65% of babies
with BA, similar to our observation [17]. All these
observations, including our study, suggest that HHI
is common in babies with BA.
Mean serum level of ALT (39.620.6 IU/L) in our
control infants was higher than the reference values
for healthy adults [19]. This could be due to differences in hepatocyte characteristics such as metabolic
rate, metabolic requirements, or cell membrane permeability due to immaturity. Moreover, reference
levels of liver enzymes in adults are based on specimens collected in the morning after an overnight
fast, which was not possible in our group. Hence, diurnal variations in liver enzyme levels or absence of
fasting state may have had a bearing on our observations [20].
Serum liver enzymes levels were not influenced by
age (72 hours and 73-144 hours) of control infants.
This indicates that serum liver enzymes levels do not
change in the first week of life. As previously shown
by other workers [21], in contrast to adults [19], gender had little effect on serum ALT levels in newborn
in our study. One recent study, however, showed that
ALT levels were different between adolescent boys
and girls [22]. This may be because male and female
infants have similar levels of sex hormones, which
are believed to determine ALT levels. We also found
higher AST level than ALT level in healthy newborns;
this could be due to widespread presence of AST in
non-hepatic tissues, such as cardiac muscle, skeletal
muscle, kidneys, brain, pancreas, lungs, leukocytes,
erythrocytes and placenta, which may be affected by
the stress of delivery.
In infants with BA and HHI, serum levels of liver
enzymes (ALT, AST, and LDH) showed a significant
rise within 24 hours after birth, peaked at 24-72
hours, and then declined sharply at 6-12 days of age.
This time-trend was comparable to previous observations in adults [23] and neonates [17]. It is important to note that the degree of rise in serum levels
of all three liver enzymes was much lower than that
reported in adults with hypoxic hepatitis. This could
be due to the relatively smaller size or immaturity of
infant liver, or a relatively milder degree of hepatic
injury in infants with BA than that observed in
adults with hypoxic hepatitis which is usually
caused by systemic hypotension.
Babies with BA and HHI had significantly higher
grades of HIE but did not have an unfavorable outcome than those with BA but no HHI. Further, levels
of serum liver enzymes had no correlation with highest grades of HIE. Our result suggests that usually
babies with more severe BA, as indicated by higher
grades of HIE, develop HHI, but that their outcome is
determined by HIE and not by HHI. Serum transaminases are known to not correlate even with severity of primary hepatic injury such as acute viral
hepatitis [16]. Previous studies have reported contradictory results [3,14]. One previous study showed
significant correlation of HHI with HIE [17]. On the
other hand, Shah et al. [3] failed to find any association between HIE and hepatic dysfunction. There
may be a place for further studies in this issue.
One of our findings was that SFD babies had significantly lower ALT and AST levels at birth than
AFD babies. This could be explained in several ways
such as lower body mass, lower metabolic rate, relative deficiency of cofactors required for transaminase
biosynthesis, or more mature hepatocyte cell membrane that prevents seepage of cytosolic enzymes into the circulation. A previous study also showed that
babies with intrauterine growth retardation had
lower ALT levels than controls but normal AST levels
[24]. Interestingly, among babies with HHI, pattern
of serum enzyme (ALT, AST, LDH) change was sim-
www.pghn.org167
Pediatr Gastroenterol Hepatol Nutr
ilar in SFD and AFD babies. Furthermore, levels of all
three serum liver enzymes were comparable between
SFD and AFD babies with HHI (Fig. 2 and 3). In brief,
the control SFD babies have lower serum liver enzyme levels than AFD babies at birth, but the extent
and temporal pattern of serum liver enzyme elevation in HHI was similar for SFD and AFD babies.
Several reasons restrained us from studying total or
conjugated serum bilirubin levels between different
groups. These include: (i) bilirubin level may be high
because of physiological jaundice, (ii) serum bilirubin
levels may not always rise following hepatic injury,
(iii) serum bilirubin elevation could persist beyond
our planned follow up of up to 6-12 days of life, (iv)
relative non-specificity of serum bilirubin as a marker
for liver injury, and (v) relatively normal or minor bilirubin elevation in ischemic hepatitis [25]. Similarly,
PT could not be used as a HHI marker as it may be abnormal in disseminated intravascular coagulation.
Likewise, hypoalbuminemia could not be used as a
marker for acute liver involvement because its levels
do not change rapidly with hepatic involvement but
may change as a result of capillary leakage.
Our study had strengths of being a prospective
study, inclusion of a comparable control group and a
good sample size. However, it had several limitations, including: not having healthy controls as the
comparator group; inclusion of out-born babies
making the study group non-homogeneous; failure
to measure neonatal blood pressure, and umbilical
cord blood pH, PaO2, PaCO2; single estimation of serum liver enzymes in controls; incomplete liver enzyme data in some babies with HHI; widely separated time points for serum liver enzyme measurements; and, failure to follow serum liver enzymes till
normalization in all babies. However, many of these
were related to ethical considerations that limited
blood sampling and procedure in infants.
In conclusion, serum liver enzymes in babies with
BA and HHI peak after 24 hours of age followed by
sharp decline in 6-12 days of age. Furthermore,
though term SFD babies have lower ALT and AST
levels than term AFD babies at birth, the extent and
temporal pattern of serum liver enzyme elevation on
168Vol. 17, No. 3, September 2014
development of HHI is similar in these two types of
infants.
REFERENCES
1. NNPD Network, Indian Council of Medical Research,
National Neonatology Forum (India). National neonatal-perinatal database: report 2002-2003. New Delhi:
Nodal Centre, AIIMS, 2005.
2. Lozano R, Naghavi M, Foreman K, Lim S, Shibuya K,
Aboyans V, et al. Global and regional mortality from 235
causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study
2010. Lancet 2012;380:2095-128.
3. Shah P, Riphagen S, Beyene J, Perlman M. Multiorgan
dysfunction in infants with post-asphyxial hypoxic-ischaemic encephalopathy. Arch Dis Child Fetal Neonatal
Ed 2004;89:F152-5.
4. Hankins GD, Koen S, Gei AF, Lopez SM, Van Hook JW,
Anderson GD. Neonatal organ system injury in acute birth
asphyxia sufficient to result in neonatal encephalopathy.
Obstet Gynecol 2002;99:688-91.
5. Al-Macki N, Miller SP, Hall N, Shevell M. The spectrum
of abnormal neurologic outcomes subsequent to term intrapartum asphyxia. Pediatr Neurol 2009;41:399-405.
6. Volpe J. Neurology of the newborn. 4th ed. Philadelphia:
WB Saunders, 2001.
7. Sarnat HB, Sarnat MS. Neonatal encephalopathy following fetal distress. A clinical and electroencephalographic
study. Arch Neurol 1976;33:696-705.
8. Gupta BD, Sharma P, Bagla J, Parakh M, Soni JP. Renal
failure in asphyxiated neonates. Indian Pediatr 2005;42:
928-34.
9. Jayashree G, Dutta AK, Sarna MS, Saili A. Acute renal failure in asphyxiated newborns. Indian Pediatr 1991;28:
19-23.
10. Shastri AT, Samarasekara S, Muniraman H, Clarke P.
Cardiac troponin I concentrations in neonates with hypoxic-ischaemic encephalopathy. Acta Paediatr 2012;101:
26-9.
11. Kanik E, Ozer EA, Bakiler AR, Aydinlioglu H, Dorak C,
Dogrusoz B, et al. Assessment of myocardial dysfunction
in neonates with hypoxic-ischemic encephalopathy: is it a
significant predictor of mortality? J Matern Fetal
Neonatal Med 2009;22:239-42.
12. Rennie JM, Roberton NRC. Textbook of neonatology. 3rd
ed. Edinburgh: Churchill Livingstone, 1999.
13. Jensen A, Garnier Y, Berger R. Dynamics of fetal circulatory responses to hypoxia and asphyxia. Eur J Obstet
Gynecol Reprod Biol 1999;84:155-72.
Nanda Chhavi, et alLiver Injury in Birth Asphyxia
14. Tarcan A, Tiker F, Gvenir H, Grakan B. Hepatic involvement in perinatal asphyxia. J Matern Fetal Neonatal Med
2007;20:407-10.
15. Feldman M, Lawrence SF, Lawrence JB. Sleisenger and
Fordtran's gastrointestinal and liver disease: pathophysiology, diagnosis, management. 9th ed. Philadelphia:
Saunders Elsevier, 2010.
16. Schiff ER, Sorrell MF, Maddrey WC. Schiff's diseases of the
liver. 10th ed. Philadelphia: Lippincott Williams &
Wilkins, 2007.
17. Karlsson M, Blennow M, Nemeth A, Winbladh B.
Dynamics of hepatic enzyme activity following birth
asphyxia. Acta Paediatr 2006;95:1405-11.
18. Godambe SV, Udani RH, Malik S, Kandalkar BM. Hepatic
profile in asphyxia neonatorum. Indian Pediatr
1997;34:927-30.
19. Prati D, Taioli E, Zanella A, Della Torre E, Butelli S, Del
Vecchio E, et al. Updated definitions of healthy ranges for
serum alanine aminotransferase levels. Ann Intern Med
2002;137:1-10.
20. Crdoba J, O'Riordan K, Dupuis J, Borensztajin J, Blei AT.
Diurnal variation of serum alanine transaminase activity
in chronic liver disease. Hepatology 1998;28:1724-5.
21. Ramakumar L, Dogra KN, Sood SC. Serum transaminases
in the newborn. Indian Pediatr 1965;2:43-8.
22. Park SH, Park HY, Kang JW, Park J, Shin KJ.
Aminotransferase upper reference limits and the prevalence of elevated aminotransferases in the Korean adolescent population. J Pediatr Gastroenterol Nutr 2012;55:
668-72.
23. Henrion J. Hypoxic hepatitis. Liver Int 2012;32:1039-52.
24. Kocylowski R, Dubiel M, Gudmundsson S, Fritzer E,
Kiserud T, von Kaisenberg C. Hepatic aminotransferases
of normal and IUGR fetuses in cord blood at birth. Early
Hum Dev 2012;88:461-5.
25. Birrer R, Takuda Y, Takara T. Hypoxic hepatopathy: pathophysiology and prognosis. Intern Med 2007;46:1063-70.
www.pghn.org169
You might also like
- Quiz ImmunologyDocument50 pagesQuiz ImmunologyMedShare97% (39)
- Hearing Loss in Term Newborn Infants With Hypoxic-Ischemic Encephalopathy Treated With Therapeutic Hypothermia PDFDocument8 pagesHearing Loss in Term Newborn Infants With Hypoxic-Ischemic Encephalopathy Treated With Therapeutic Hypothermia PDFstefanp89No ratings yet
- 1 Predict NeoDocument5 pages1 Predict NeoGary Carhuamaca LopezNo ratings yet
- IJN Volume 10 Issue 2 Pages 50-54Document5 pagesIJN Volume 10 Issue 2 Pages 50-54DavidNo ratings yet
- PIH Renal Doppler Pregnancy - CutDocument4 pagesPIH Renal Doppler Pregnancy - CutAnonymous 9QxPDpNo ratings yet
- The Effect of Human Recombinant Erythropoietin On Prevention of Anemia of PrematurityDocument6 pagesThe Effect of Human Recombinant Erythropoietin On Prevention of Anemia of PrematuritySri Nowo MinartiNo ratings yet
- Early Feeding in Acute Pancreatitis in Children A Randomized Controlled TrialDocument9 pagesEarly Feeding in Acute Pancreatitis in Children A Randomized Controlled TrialvalenciaNo ratings yet
- Newborn Screening - Dr. T. GhoshDocument32 pagesNewborn Screening - Dr. T. GhoshMontu ChakmaNo ratings yet
- Incidence, Predictors and Outcome of Sepsis Associated Liver Injury in Children: A Prospective Observational StudyDocument9 pagesIncidence, Predictors and Outcome of Sepsis Associated Liver Injury in Children: A Prospective Observational StudyindahkputriNo ratings yet
- Electronic Physician (ISSN: 2008-5842)Document5 pagesElectronic Physician (ISSN: 2008-5842)Aldian DianNo ratings yet
- Irisin in AdolecenceDocument4 pagesIrisin in Adolecencemiss beeNo ratings yet
- Biochemical Marker As Predictor of Outcome in Perinatal AsphyxiaDocument4 pagesBiochemical Marker As Predictor of Outcome in Perinatal AsphyxiaAgus WijataNo ratings yet
- Heart Rate Variability Alterations in Infants With Spontaneous HypertoniaDocument8 pagesHeart Rate Variability Alterations in Infants With Spontaneous HypertoniaAlexis Arce AlvarezNo ratings yet
- Acute PancreatitisDocument9 pagesAcute PancreatitisJayari Cendana PutraNo ratings yet
- Effect of A Probiotic Infant Formula On Infections in Child Care Centers Pediatrics-2005-Weizman-5-9Document7 pagesEffect of A Probiotic Infant Formula On Infections in Child Care Centers Pediatrics-2005-Weizman-5-9Yuktika RiYuNo ratings yet
- Renal Resistive Index in Patients With Polycystic Ovary SyndromeDocument5 pagesRenal Resistive Index in Patients With Polycystic Ovary Syndromemeltwithsnow163.comNo ratings yet
- Characteristics of Pediatric Patients With Diarrhea in Indonesia: A Laboratory-Based ReportDocument8 pagesCharacteristics of Pediatric Patients With Diarrhea in Indonesia: A Laboratory-Based ReportDrnNo ratings yet
- Growth After Adenotonsillectomy For Obstructive Sleep Apnea: An RCTDocument10 pagesGrowth After Adenotonsillectomy For Obstructive Sleep Apnea: An RCTCalvin AffendyNo ratings yet
- Bodyweight Loss in Predicting Neonatal Hyperbilirubinemia 72 Hours After Birth in Term Newborn InfantsDocument8 pagesBodyweight Loss in Predicting Neonatal Hyperbilirubinemia 72 Hours After Birth in Term Newborn InfantsAhtarunnisa Fauzia HanifaNo ratings yet
- Ma 70 408Document5 pagesMa 70 408Zahra AfifahNo ratings yet
- Animals 11 00685 v3Document12 pagesAnimals 11 00685 v3Carolina Duque RodriguezNo ratings yet
- Growth After AdenotonsillectomyDocument10 pagesGrowth After AdenotonsillectomyfriscahalimNo ratings yet
- 2010 Article 69Document6 pages2010 Article 69gepang_metalNo ratings yet
- Nutritional Assessment of Children With CHD CompareDocument9 pagesNutritional Assessment of Children With CHD CompareIntan Robi'ahNo ratings yet
- 11 134 v12n4 2013 PredictingPortalDocument11 pages11 134 v12n4 2013 PredictingPortalDevy Widiya GrafitasariNo ratings yet
- Early - and Late-Onset Preeclampsia A ComprehensiveDocument10 pagesEarly - and Late-Onset Preeclampsia A ComprehensiveEriekafebriayana RNo ratings yet
- Eke2019 PDFDocument1 pageEke2019 PDFWijitha VarenniNo ratings yet
- Original Article: The Effect of Neonatal Asphyxia On Renal FunctionDocument6 pagesOriginal Article: The Effect of Neonatal Asphyxia On Renal FunctionelizabethpurbaNo ratings yet
- Bloody Stool Journal 2Document8 pagesBloody Stool Journal 2dr.herusetiawanNo ratings yet
- Conjugated Hyperbilirubinemia in The Neonatal Intensive Care UnitDocument9 pagesConjugated Hyperbilirubinemia in The Neonatal Intensive Care UnitIvan HoNo ratings yet
- RESEARCH ARTICLEOpen AccessChallenges of Acute Peritoneal Dialysis Inextremely-Low-Birth-Weight Infants - Aretrospective Cohort StudyDocument9 pagesRESEARCH ARTICLEOpen AccessChallenges of Acute Peritoneal Dialysis Inextremely-Low-Birth-Weight Infants - Aretrospective Cohort StudysavitageraNo ratings yet
- Materials and MethodsDocument3 pagesMaterials and MethodssurtitejoNo ratings yet
- Knowledge Level and Determinants of Neonatal Jaundice A Cross-Sectional Study in The Effutu Municipality of GhanaDocument10 pagesKnowledge Level and Determinants of Neonatal Jaundice A Cross-Sectional Study in The Effutu Municipality of GhananicloverNo ratings yet
- Sii ArtículoDocument5 pagesSii ArtículoMonserrat Garduño FonsecaNo ratings yet
- Status of Serum Bilirubin, Serum Proteins and Prothrombin Time in Babies With Perinatal AsphyxiaDocument4 pagesStatus of Serum Bilirubin, Serum Proteins and Prothrombin Time in Babies With Perinatal AsphyxiaAgus WijataNo ratings yet
- Complementary and Alternative Medical Lab Testing Part 5: GastrointestinalFrom EverandComplementary and Alternative Medical Lab Testing Part 5: GastrointestinalNo ratings yet
- Anemia de PrematDocument7 pagesAnemia de Prematmedibase12No ratings yet
- Jurnal AKIDocument7 pagesJurnal AKIAnonymous Vz9teLNo ratings yet
- Non Protein Calorie - NPCDocument6 pagesNon Protein Calorie - NPCmarkus_danusantosoNo ratings yet
- ACPN AbstractsDocument21 pagesACPN AbstractsPediatric NephrologyNo ratings yet
- The Effect of Thickened-Feed Interventions On Gastroesophageal RefluxDocument13 pagesThe Effect of Thickened-Feed Interventions On Gastroesophageal Refluxminerva_stanciuNo ratings yet
- Hidronefrosis 3Document11 pagesHidronefrosis 3Zwinglie SandagNo ratings yet
- DUDDING Et Al-2008-Journal of Thrombosis and HaemostasisDocument8 pagesDUDDING Et Al-2008-Journal of Thrombosis and HaemostasisNur Ainatun NadrahNo ratings yet
- Both Fecal Calprotectin and Imuno Test in Children IBDDocument13 pagesBoth Fecal Calprotectin and Imuno Test in Children IBDdichafrNo ratings yet
- 1121PGHN - PGHN 23 266Document10 pages1121PGHN - PGHN 23 266justmokhtarNo ratings yet
- A Systematic Review and Meta-Analysis of The Benefits of ADocument10 pagesA Systematic Review and Meta-Analysis of The Benefits of Adhimas satriaNo ratings yet
- 2018 Revised Reference Values For The Intake of ProteinDocument15 pages2018 Revised Reference Values For The Intake of ProteinNayaNo ratings yet
- Metabolic Syndrome in Very Low Birth Weight Young Adults and Controls: The New Zealand 1986 VLBW StudyDocument11 pagesMetabolic Syndrome in Very Low Birth Weight Young Adults and Controls: The New Zealand 1986 VLBW StudysatishNo ratings yet
- Impact of Disease Severity On Gastric Residual Volume in Critical PatientsDocument16 pagesImpact of Disease Severity On Gastric Residual Volume in Critical PatientsSelliEfridaSiahaanNo ratings yet
- Doppler and Biophysical Assessment in Growth Restricted Fetuses: Distribution of Test ResultsDocument7 pagesDoppler and Biophysical Assessment in Growth Restricted Fetuses: Distribution of Test ResultslalimdNo ratings yet
- WilsonDocument11 pagesWilsonCarmen OpreaNo ratings yet
- Subjective Global Nutritional Assessment For Children: Donna J Secker and Khursheed N JeejeebhoyDocument7 pagesSubjective Global Nutritional Assessment For Children: Donna J Secker and Khursheed N Jeejeebhoynurul_putrieNo ratings yet
- Efficacy of A New Hypotonic Oral Rehydration Solution Containing Zinc and Prebiotics in The Treatment of Childhood Acute Diarrhea: A Randomized Controlled TrialDocument6 pagesEfficacy of A New Hypotonic Oral Rehydration Solution Containing Zinc and Prebiotics in The Treatment of Childhood Acute Diarrhea: A Randomized Controlled TrialOlpinNo ratings yet
- Feeding Practice During Transfusion in Preterm Infants: Muhamad Azharry RullyDocument26 pagesFeeding Practice During Transfusion in Preterm Infants: Muhamad Azharry Rullytrie dolleNo ratings yet
- Chest 147 1 132Document8 pagesChest 147 1 132Timothy Eduard A. SupitNo ratings yet
- SII, FODMAPS e Hormonios EndócrinosDocument7 pagesSII, FODMAPS e Hormonios Endócrinosmari bNo ratings yet
- Jurnal Hiperemesis GravidarumDocument6 pagesJurnal Hiperemesis GravidarumArief Tirtana PutraNo ratings yet
- Study of Clinical, Biochemical Evaluation and Outcome in Hypertrophic Pyloric StenosisDocument4 pagesStudy of Clinical, Biochemical Evaluation and Outcome in Hypertrophic Pyloric StenosiszapomannNo ratings yet
- Endocrine and Metabolic Evaluation of Human Immunodeficiency Virus-Infected Patients With Evidence of Protease Inhibitor-Associated LipodystrophyDocument7 pagesEndocrine and Metabolic Evaluation of Human Immunodeficiency Virus-Infected Patients With Evidence of Protease Inhibitor-Associated LipodystrophydocumentosdescribdNo ratings yet
- Dyspepsia Journal PediatricDocument11 pagesDyspepsia Journal PediatricFatt ZakiNo ratings yet
- Complementary and Alternative Medical Lab Testing Part 8: UrologyFrom EverandComplementary and Alternative Medical Lab Testing Part 8: UrologyRating: 3 out of 5 stars3/5 (1)
- Ducks Out of Water - Duck Industry CrueltyDocument55 pagesDucks Out of Water - Duck Industry CrueltyVegan Future100% (1)
- Olbas Cough Syrup LabelDocument1 pageOlbas Cough Syrup LabelMulayam Singh YadavNo ratings yet
- Meat and FishDocument26 pagesMeat and FishPoorani ArunachalamNo ratings yet
- Cocculus IndicusDocument29 pagesCocculus IndicusShah FaisalNo ratings yet
- Reproductive HealthDocument21 pagesReproductive HealthRosalie Valdez EspirituNo ratings yet
- Smallest Dog Breeds in The WorldDocument5 pagesSmallest Dog Breeds in The WorldtourisminfopediaNo ratings yet
- 1 Journal 2 Kid Mortality LRRDDocument8 pages1 Journal 2 Kid Mortality LRRDErdachewNo ratings yet
- A Pattern Approach To Lymph Node Diagnosis - A. Leong (Springer, 2011) WWDocument432 pagesA Pattern Approach To Lymph Node Diagnosis - A. Leong (Springer, 2011) WWAdrian TirlaNo ratings yet
- Emergency Acupressure TreatmentDocument39 pagesEmergency Acupressure TreatmentNarayana Mugalur100% (1)
- Reva Rubin Maternal Role Attainment TheoryDocument4 pagesReva Rubin Maternal Role Attainment TheoryLeonard LigutomNo ratings yet
- Alergi Susu SapiDocument2 pagesAlergi Susu SapiMaya FikriNo ratings yet
- Aquila Pomarina X Clanga ClangaDocument14 pagesAquila Pomarina X Clanga ClangaCristinaNo ratings yet
- Case Presentation For Head InjuryDocument65 pagesCase Presentation For Head InjuryYdynn Parejas GavinaNo ratings yet
- 2 Neurophysiology of Somatic Sensations 2012Document6 pages2 Neurophysiology of Somatic Sensations 2012Nephritery Joy Espiritu JimenezNo ratings yet
- Structure and Life Cycle of The Housefly (With Diagram)Document16 pagesStructure and Life Cycle of The Housefly (With Diagram)rajesh kumar ranjan100% (1)
- Urethral Catheterization 1Document31 pagesUrethral Catheterization 1Hilman HadiansyahNo ratings yet
- E49 - MDM 20 KG - África Do Sul - Especificação Técnica 121 (1) .PT - enDocument6 pagesE49 - MDM 20 KG - África Do Sul - Especificação Técnica 121 (1) .PT - encid ribeiroNo ratings yet
- EO No.-31 s.2013 Anti-Rabies CouncilDocument5 pagesEO No.-31 s.2013 Anti-Rabies Councilmaryson primo100% (1)
- Because of Winn-Dixie VocabDocument5 pagesBecause of Winn-Dixie VocabBrad MorganNo ratings yet
- Intestinal Parasites: Comparative Morphology FiguresDocument14 pagesIntestinal Parasites: Comparative Morphology FiguresRica UyNo ratings yet
- HematopoiesisDocument3 pagesHematopoiesisVino OrajayNo ratings yet
- Chart Showing The Classification of Human Nervous SystemDocument6 pagesChart Showing The Classification of Human Nervous Systemamala raviNo ratings yet
- Guna-Tf: G GU UN NA A - TTFFDocument18 pagesGuna-Tf: G GU UN NA A - TTFFantudwo33No ratings yet
- Animal Classification Practice TestDocument2 pagesAnimal Classification Practice TestElpi FerrerNo ratings yet
- Etimology Prefix Suffix RootDocument61 pagesEtimology Prefix Suffix RootivonneNo ratings yet
- Uptake and Distribution of Inhalational AnaestheticsDocument125 pagesUptake and Distribution of Inhalational Anaestheticsharsha mummakaNo ratings yet
- Brush Up On Oral AssessmentDocument3 pagesBrush Up On Oral Assessmentaus4us3No ratings yet
- Cancer - Rath, Matthias PDF (Pauling-Rath Therapy Protocol: Vitamin C and Lysine)Document84 pagesCancer - Rath, Matthias PDF (Pauling-Rath Therapy Protocol: Vitamin C and Lysine)Anonymous Jap77xvqPKNo ratings yet
- Try in of Waxed Up DenturesDocument58 pagesTry in of Waxed Up DenturesRohan Grover100% (1)