Professional Documents
Culture Documents
Mesenteric Ischemia: The Whole Spectrum: M. J. Sise
Mesenteric Ischemia: The Whole Spectrum: M. J. Sise
Uploaded by
anggitas2594Original Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Mesenteric Ischemia: The Whole Spectrum: M. J. Sise
Mesenteric Ischemia: The Whole Spectrum: M. J. Sise
Uploaded by
anggitas2594Copyright:
Available Formats
Scandinavian Journal of Surgery 99: 106110, 2010
Mesenteric ischemia: the whole spectrum
M. J. Sise
Department of Surgery, Scripps Health, San Diego, CA, U.S.A.
Key words: Superior mesenteric artery; thrombosis; embolism; intestinal necrosis; intestinal ischemia;
arterial occlusion
Background
Mesenteric ischemia remains a deadly process which
requires early diagnosis and prompt treatment if the
patient is to have any chance of survival. The overall
mortality rate remains approximately 40% and there
is little room for either delay or error in the management of this acute care surgical emergency (1, 2).
There are a variety of causes which ultimately, if left
untreated, lead to mesenteric infarction and death.
Symptoms vary from the insidious onset of vague
generalized abdominal pain to the sudden onset of
diffuse, severe, and constant pain. There are four
common causes: acute cardiac source embolism to the
superior mesenteric artery, acute thrombosis of an
atherosclerotic lesion with previous partial occlusion,
splanchnic vasoconstriction leading to low flow and
regional ischemia (commonly called non-occlusive
mesenteric ischemia), and mesenteric venous thrombosis (Table 1). All of these causes are secondary phenomena which result from other major diseases and
occur in a high risk setting.
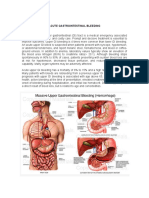
Mesenteric Vascular Anatomy
The arterial blood supply of the gut is divided into
four major areas each defined by the major arteries
which supply them. Important collaterals link the
perfusion of each area (Table 2). These collaterals are
not sufficient to provide adequate flow if the superior
mesenteric artery is acutely occluded. However, in
chronic, progressive atherosclerotic occlusive disease,
they can steadily increase in size to prevent ischemia.
Patients occasionally will have total gut perfusion via
a single remaining mesenteric artery or the bilateral
hypogastric arteries in the presence of a gradual progression to total occlusion of the other proximal aor-
Correspondence:
Michael J. Sise, M.D.
550 Washington St, Suite 641
San Diego, CA 92103, U.S.A.
Email: sise.mike@scrippshealth.org
Table 1
Etiology of acute mesenteric ischemia.
50%
20%
20%
10%
Arterial embolism
Arterial thrombosis
Small vessel occlusion
Venous thrombosis
tic branches to the foregut, midgut, and hindgut.
However, many of these patients have intestinal angina when eating large meals. The venous drainage
of the gut is via the portal venous system. Gastric
drainage is via the splenic vein. The small bowel and
the proximal colon through the splenic flexure drain
via the superior mesenteric vein. The remainder of
the colon drains via the inferior mesenteric vein. Collateral venous vessels are present between each major
area.
The celiac and mesenteric artery origins from the
aorta are closely associated with the renal artery origins in the upper abdomen just below the aortic hiatus of the diaphragm. Their proximal portions each
have a closely applied plexus of lymphatic and neurologic tissue. These vessels are relatively thin-walled,
unlike similarly sized extremity arteries, and must be
handled with care. The portal vein and major mesenteric veins are also thin-walled, easily torn, and
equally easily injured during exposure.
Clinical presentation
The pathophysiology of mesenteric ischemia is based
upon insufficient blood flow to meet the metabolic
demand of the bowel. Acute ischemia leads to initial
hyperperistalsis, gut emptying, followed by intense
ischemia pain from gut wall hypoperfusion. Since
this is visceral pain, it is vague and projected across
the area of the superficial abdominal wall with innervation shared with the visceral innnervation. Foregut structures generate visceral pain in the epigastrium, midgut in the periumbilical regions, hindgut
in the infraumbilical region, and cloacal derivatives
in the supra-pubic region of the abdomen. Ischemia
Mesenteric ischemia: the whole spectrum
107
Table 2
Gut regions, their blood supply, and collateral connections.
Region
Blood supply
Collateral connections
Foregut
Distal esophagus through the ampulla
of Vater in the duodenum
Celiac artery
Pancreatico-duodenal arteries and Arc
of Buhler distally
Migut
Ampulla of Vater region of the duodenum
to splenic flexure of the colon
Superior mesenteric artery
Pancreatico-duodenal arteries and Arc
of Buhler proximally. Marginal artery of
Drummond and Arc of Rioland distally
Hindgut
Splenic flexure of the colon to distal
sigmoid colon
Inferior mesenteric artery
Marginal artery of Drummond and Arc
of Rioland proximally
Superior hemorrhoidal to middle
hemorrhoidal arteries distally
Cloacal derivatives
Branches of the bilateral hypogastric
arteries
Middle hemorrhoidal to superior
hemorrhoidal arteries proximally
pain is intense and constant. It is does not increase
with palpation and not associated with abdominal
wall rigidity. Thus the classical pain out of proportion with physical findings attributed to acute mesenteric ischemia. The initial reflex gut emptying with
vomiting and diarrhea also diverts the examining
physicians attention to other diagnoses. Finally, when
ischemia leads to necrosis, inflammation of the gut
surface leads to localization of pain in the abdomen
and the presence of associated physical findings.
Acute intestinal ischemia from sudden complete
occlusion of the celiac or superior mesenteric arteries
from a cardiac source embolism causes the classical
findings outlined above. Acute on chronic occlusion
of a previously stenotic atherosclerotic lesion may
lead to a less drastic and more insidious onset of pain
because of pre-existing collateral flow which mitigates, to a certain extent, the severity of the resulting
ischemia. In this setting, there may be a history of
intestinal angina including post prandial pain, fear of
food, and weight loss. Similarly, venous occlusion is
usually insidious in onset and causes more vague
symptoms which worsen progressively over time.
Non-occlusive acute mesenteric ischemia from vasoconstriction always occurs in the setting of critical
illness with reduced cardiac output and is associated
with vague symptoms at first.
Concurrent cardiac disease is the common element
of these patients medical history. Atrial fibrillation is
the most commonly associated cardiac diagnosis
(Table 3) (36). Patients usually report rapid onset of
pain associated with nausea, vomiting, loose stools.
Abdominal distension, hypoactive bowel sounds, and
guaiac positive stools are also commonly found on
physical examination early in the course of mesenteric ischemia. In patients with acute worsening of
chronic mesenteric ischemia there is always a history
of long standing post prandial pain and weight loss
occurs in close to 90% of patients. A history of nausea
and vomiting in the past is present in over 50% and
an abdominal bruit is found on physical examination
in over two thirds of these patients. Approximately
50% of patients with mesenteric venous thrombosis
have a history of hypercoagulability, 25% a history of
hepatitis, 25% thrombocytosis, and 10% pancreatic
Table 3
Risk factors for mesenteric ischemia.
Arterial embolism or thrombosis
Venous thrombosis
Cardiac disease:
atrial figrillation
recent myocardial infarction
congestive heart failure
digitalis therapy
Portal hypertension
Previous arterial emboli
Hypercoagulable state
Hypovolemia, shock
Inflammation
Postop period, trauma
Prothrombotic state
Chronic renal failure
Congestive heart failure
cancer (3, 4). These patients have findings similar to
those with acute arterial occlusion in the later stages
of this disease. Early, the findings are less distinct and
the use of CT scanning allows timely diagnosis before
significant bowel compromise occurs.
End stage intestinal necrosis causes severe shock
and an overwhelming inflammatory response with
an attendant high mortality rate (7, 9). Because acute
mesenteric ischemia usually occurs in the setting of
significant pre-existing diseases, outcome with intestinal necrosis is poor and has not significantly improved in the last four decades (5, 6). The goal remains prompt recognition and successful management prior to bowel necrosis.
Diagnosis
The classical pain out of proportion to findings is not
always present as previously discussed. Hypoactive
bowel sounds are usually encountered and signs of
peritoneal irritation occur late. The onset of intestinal
ischemia often produces a profound leukocytosis
with peripheral WBC elevation in excess of 20,000. In
fact, any patient with abdominal pain and a WBC in
excess of 20,000 should have acute mesenteric ischemia included in their differential diagnosis. Serum
amylase elevation occurs, however, serum lactate elevations and systemic acidosis are later findings.
Plain film radiography is not helpful until late in the
M. J. Sise
108
course of mesenteric ischemia when an ileus pattern,
distented bowel, and bowel wall thickening are seen.
High resolution abdominal CT scan with contrast is
very accurate and specific in delineating not only the
extent of visceral ischemia but the status of flow in
the mesenteric vasculature (10). Both mesenteric arterial and portal venous blood flow is accurately assessed with contrast CT scanning (11). Findings of
abnormal intestinal wall blood flow, arterial intraluminal defects, or a halo sign in the mesenteric veins
are very well demonstrated and accurately diagnose
the presence and the causes of mesenteric ischemia.
Visceral CT angiography has largely replaced catheter
angiography in the work up of acute and chronic
mesenteric ischemia. Although catheter angiography
is somewhat more accurate, it is time consuming and
does not produce results of significantly more usefulness than those of high resolution scans with coronal,
sagital, and VTR reconstructions. Catheter angiography is particularly less accurate is assessing venous
phase blood flow compared to CT scanning. Other
diagnoses in the differential for acute mesenteric ischemia include pancreatitis, small bowel obstruction,
and acute biliary tract disease among others. CT scanning is very accurate in excluding these diagnoses in
patients with mesenteric ischemia.
Management
The key to successful management of acute mesenteric ischemia from major arterial occlusion is prompt
surgical therapy (Fig. 1) (12). Although there is a limited role for endovascular management, it cannot be
successful without also performing an exploratory
laparotomy except in the very earliest stages of ischemia when necrosis is not a significant risk. The risk
of bowel necrosis and subsequent peritonitis and
generalized inflammatory response requires prompt
abdominal exploration to assess bowel viability even
when arterial flow has been restored by endovascular
techniques. Endovascular management has a role in
chronic mesenteric ischemia from atherosclerotic lesions without the presence of acute intestinal ischemia (13, 14). Laparoscopy has a little, if any role, in
the management of mesenteric ischemia. Prompt exploratory laparotomy is the key to successful management.
The intraoperative assessment of blood flow of the
bowel begins with an inspection of the entire intestinal tract by running the bowel, assessing color, peristaltic activity, and palpating the mesenteric arcade
arteries (Fig. 2) . The main trunk of the superior mesenteric artery is then palpated by cephalad retraction
of the transverse colon, caudal retraction of the small
bowel, and palpation of the root of the mesentery
along the inferior margin of the body of the pancreas.
The celiac artery and its branches are palpated
through the lesser sac below the left lobe of the liver
and above the lesser curve of the stomach. The inferior mesenteric is palpated along the left side of the
infra-renal aorta and the base of the left colon mesenMichael
J. Sise,
MD,
FACS border for
tery. Doppler
assessment
of the
mesenteric
pulsatile signals is helpful in areas of questionable
Figure 1. Decision-making in the management of mesenteric ischemia
Classical signs of
mesenteric ischemia
Abdominal pain
out of proportion
to findings
CT scan evidence of
arterial occlusion
Direct to OR
Unstable patient
Insidious onset,
vague symptoms
Mesenteric venous
thrombosis
Non-occlusive
mesenteric
ischemia
Fig. 1. Decision-making in the management of mesenteric ischemia.
Anticoagulation,
resuscitation, bowel
rest, serial
examinations, treatment
of underlying low-flow
state or inflammatory
processes,
exploratory laparotomy
for failure to improve
Michael J. Sise, MD, FACS
Figure 2. Intra-operative management
mesenteric
ischemia
Mesenteric of
ischemia:
the whole spectrum
Superior mesenteric
artery embolism
Mesenteric arterial
thrombosis
109
Embolectomy of superior mesenteric
artery, reassessment for bowel viability,
resect bowel as needed, damage control
closure, re-operation, anticoagulation
Aorto- mesenteric bypass as needed,
reassessment for bowel viability, resect
bowel as needed, damage control
closure, reoperation, anticoagulation
Fig. 2. Intra-operative management of mesenteric ischemia.
perfusion. Fluorescein angiography with an ultraviolet lamp has also been used (15).
The pattern and appearance of ischemic bowel is
helpful in determining the cause of mesenteric ischemia. Cardiac source embolism to the superior mesenteric artery usually lodges in the vessel distal to the
origin of the middle colic artery. Therefore, sparing
of the proximal jejunum and the transverse colon
with ischemia of the remaining small bowel and ascending colon are seen. Thrombosis of the origin of
the superior mesenteric artery leads to ischemia
throughout its distribution from the duodenum to the
splenic flexure of the colon. If the celiac artery and
the inferior mesenteric artery are also stenotic or occluded, more proximal and distal areas are also ischemic. In the worst case scenario, acute thrombosis
leads to total intestinal ischemia from the distal
esophagus to the rectum.
Embolism in the superior mesenteric artery is retrieved through a transverse incision in the main
trunk of the artery in the mesenteric root below the
pancreas (16). This area is exposed in the manner
outlined above. Care should be taken in handling this
relatively fragile artery. Balloon embolectomy catheters should also be used gently proximally and distally to avoid arterial injury. Gentle flushing distally
with heparinzed saline (10 units of heparin per ml)
should be performed. Do not flush proximally for
fear of dislodging thrombus into the aorta and causing distal embolism. The closure of the arterotomy
must be done with either a tension-free running
monofilament suture or interrupted sutures. This is
best accomplished by placing proximal and distal
vascular clamps and gently retracting the artery towards the arterotomy site to minimize tension. Once
flow has been re-established, the bowel may not immediately appear perfused. Placing warm laparotomy packs and waiting 10 to 15 minutes to reassess
is helpful. Injection of papaverine hydrochloride into
the superior mesenteric artery (two ml of a 30 mg per
ml solution) is a helpful adjunct to reduce vasospasm
and improve reperfusion.
The treatment of proximal mesenteric arterial
thrombosis requires experience and skill in advanced
vascular surgical technique. Call for a vascular surgeon colleague to assist if you are not comfortable
and capable to perform the necessary aorto-mesenteric bypass. There are a variety of bypasses described. Retrograde iliac artery to mesenteric artery
bypass appears easier to perform than antegrade
supra-celiac aorto-mesenteric bypass. It is, in reality,
a poor second choice. The iliac arteries are often involved with atherosclerotic occlusive disease in this
setting and the bypass is difficult to complete without
kinking or placing synthetic graft in proximity to the
duodenum with the risk of later erosion.
Antegrade aorto-mesenteric bypass from the supra-celiac aorta is the best choice for restoring flow in
acute mesenteric ischemia form proximal mesenteric
arterial thrombosis (1719). This approach requires
exposure of the retro-crural aorta by mobilizing the
left lobe of the liver and retracting it to the right. The
lesser omentum is opened, the stomach retracted caudally, and the crura of the diaphragm divided over
the aorta. The tunnel for the graft is relatively easily
made with gentle blunt dissection behind the pancreas along the left anterior margin of the aorta to the
superior mesenteric artery at the root of the mesentery below the pancreas. It is also feasible to dissect
directly down the superior mesenteric artery behind
the pancreas if the stenotic area of the artery is of
short duration. The celiac artery at its bifurcation into
the splenic and common hepatic branches may also
be exposed for a second limb of the bypass if needed.
The proximal synthetic graft bypass anastomosis is
performed end to side to the aorta after
17 systemic
heparinization and placement of totally occluding
proximal and distal aortic clamps. Partial occluding
clamps run the risk of damaging the aorta, causing
distal emboli, and make the proximal anastomosis
difficult to perform by compressing the aorta into a
narrow space. The distal anastomoses are performed
end to side. Prior to completion, careful flushing and,
if indicated, balloon catheter thrombectomy should
110
M. J. Sise
be perfomed. Once flow has been re-established to
the bowel, it is inspected for viability as outlined
above.
The management of the bowel after restoration of
arterial blood flow should include damage control
techniques (Fig. 2.). There is little or no advantage to
immediate closure of the abdominal wall even if all
of the bowel initially appears viable. Damage control
temporary closure carries little or no morbidity and
insures that there is no delayed bowel necrosis that
goes unrecognized. Obviously necrotic bowel should
be resected by stapling and dividing at healthy margins. Anastomosis of bowel segments should be deferred until reoperation at 24 to 36 hours. Temporary
abdominal wall closure should be performed followed by prompt transfer to the intensive care unit
for appropriate postoperative critical care management. Early anticoagulation with intravenous heparin
should be added despite the risk of operative site
hemorrhage in order to prevent re-thrombosis of
mesenteric vessels.
Mesenteric venous thrombosis leading to ischemic
bowel is much more difficult to manage than arterial
source mesenteric ischemia (3, 4). By the time intestinal ischemia occurs from venous engorgement and
impeded arterial flow, there are few, if any, options
that will relieve venous obstruction. Portal or mesenteric venous thrombectomy is not effective and very
dangerous. The only choice is systemic anticoagulation coupled with resection of necrotic bowel, damage control closure, and aggressive resuscitative measures. Patients that survive this dreadful complication
of an underlying hypercoagulability often require extensive bowel resection and are left with shot-gut
syndrome. Multiple reoperations to reassess bowel
for viability are the rule in the early management of
mesenteric venous thrombosis.
Outcome
The initial results following mesenteric ischemia are
related to both the absence or presence of intestinal
infarction and the underlying causes of vascular compromise. Little has changed in the last four decades
with regard to overall survival. Perioperative mortality remains approximately 40% (4, 6, 20, 21). Recurrent cardiac source embolism occurs in 30% of patients with this complication (20, 21). Mesenteric arterial thrombosis is a harbinger or advanced systemic
atherosclerosis and the risk of death from coronary
artery disease is high. Mesenteric venous thrombosis
is always a secondary phenomenon and life-long risk
of thrombotic complications follows for those who
are fortunate enough to survive (24, 7).
The mainstay of post-event care of patients with
acute mesenteric ischemia is management of their
underlying comorbidities. All will require some form
of anticoagulation or antiplatelet therapy. Cardiac
disease must be aggressively treated. The causes of
hypercoagulability need to be thoroughly investigated in those with mesenteric venous thrombosis.
Life-long medical management is essential for all survivors of the various forms of mesenteric ischemia.
REFERENCES
01. Edwards MS, Cherr GS, Craven TE, et al: Acute occlusive mesenteric ischemia: surgical management and outcomes. Ann
Vasc Surg 2003;17:7279
02. Schoots IG, Koffeman GI, Legemate DA, et al: Systematic review of survival after acute mesenteric ischemia according to
disease aetiology. Br J Surg 2004;91:1727
03. Boley SJ, Kaleya RN, Brandt LJ: Mesenteric venous thrombosis.
Surg Clin North Am 1992;72:183201
04. Rhee RY, Gloviczki P, Mendonca CT, et al: Mesenteric venous
thrombosis: still a lethal disease in the 1990s. J Vasc Surg 1994;
20:688697
05. Weil J, Sen Gupta R, Harfarth H: Nonocclusive mesenteric
ischemia induced by digitalis. Int J Colorectal Dis 2004; 19:277
280
06. Burns BJ, Brandt LJ: Intestinal ischemia. Gastroenterol Clin
North Am 2003;32:11271143
07. Thompson JS, Langnas AN, Pinch Lw, et al: Surgical approach
to short-bowel syndrome. Experience in a population of 160
patients. Ann Surg 1995;222:600605
08. Moore EE, Moore FA, Franciose RJ, et al: The postischemic gut
serves as a priming bed for circulating neutrophils that provoke multiple organ failure. J Trauma 1994;37:881887
09. Hassoun HT, Kone BC, Mercer DW, et al: Post-injury multiple
organ failure: the role of the gut. Shock 2001;15:110
10. Cikrit DF, Harris VJ, Hemmer CG, et al: Comparison of spiral
CT scan and arteriography for evaluation of renal and visceral arteries. Ann Vasc Surg 1996;10:109116
11. Ridley N, Green SE: Mesenteric arterial thrombosis diagnosed
on CT. Am J Roentgenol 2001;176:549
12. Park WM, Gloviczki P, Cherry KJ, et al: Contemporary management of acute mesenteric ischemia: factors associated with
survival. J Vasc Surg 2002;35:445452
13. Kasirajan K, OHara PJ, Gray BH, et al: Chronic mesenteric
ischemia: open surgery versus percutaneous angioplasty and
stenting. J Vasc Surg 2001;33:6371
14. Matsumoto AH, Angle JF, Spinosa DJ, et al: Percutaneous
transluminal angioplasty and stenting in the treatment of
chronic mesenteric ischemia: results and long-term follow up.
J Am Coll Surg 2002;194:S22S31
15. Ballard J, Stone W, Hallett J, et al: A critical analysis of adjuvant
techniques used to assess bowel viability in acute mesenteric
ischemia. Am Surg 1993;7:309311
16. Bjorek M, Acosta S, Lindber F, et al: Revascularization of the
superior mesenteric artery after acute thromboembolic occlusion. Br J Surg 2002;89:923927
17. Hermeck J, et al: Role of supraceliac aortic bypass in visceral
artery reconstruction. Am J Surg 1991;162:611614
18. Foley MI, Moneta G, Abu-Zamzam Am, et al: Revascularization of the superior mesenteric artery alone for treatment of
intestinal ischemia. J Vasc Surg 2000;32:3737
19. Gentile A, Moneta G, Taylor L, et al: Isolated bypass to the
superior mesenteric artery for intestinal ischemia. Arch Surg
1994;129:926932
20. Klempnauer J, Grothues F, Bekras H, et al: Long-term results
after surgery for acute mesenteric ischemia. Surgery 1997;
121:239243
21. Cho JS, Carr JA, Jacobsen G, et al: Long-term outcome after
mesenteric artery reconstruction: a 37-year experience. J Vasc
Surg 2002;35:453460
Received: May 4, 2010
You might also like
- The Human Circulatory System: Grade 9 - Sussex - Wennappuwa - ScienceDocument23 pagesThe Human Circulatory System: Grade 9 - Sussex - Wennappuwa - ScienceSwarnapaliliyanageNo ratings yet
- Ultimate Exercise Cheat Sheet - TricepsDocument13 pagesUltimate Exercise Cheat Sheet - TricepsAHMED EMADNo ratings yet
- General Pathology Single Best Answers For The MRCSDocument22 pagesGeneral Pathology Single Best Answers For The MRCStahir_the_great2939No ratings yet
- Mesentericischemia: A Deadly MissDocument10 pagesMesentericischemia: A Deadly MisspakausNo ratings yet
- Acute Mesentric IschemiaDocument40 pagesAcute Mesentric IschemiaTsega WesenNo ratings yet
- Vascular Disease of The BowelDocument28 pagesVascular Disease of The BowelOlga GoryachevaNo ratings yet
- Ischemia BowelDocument36 pagesIschemia BowelTammie YoungNo ratings yet
- Lectura 8Document8 pagesLectura 8Daniela Andrea Tello GuaguaNo ratings yet
- Bowel IschemiaDocument79 pagesBowel IschemiaNovita AnjaniNo ratings yet
- Mesenteric Artery Ischemia PDFDocument30 pagesMesenteric Artery Ischemia PDFMerfat MahyobeNo ratings yet
- Diseases of The SmalllntestineDocument183 pagesDiseases of The SmalllntestineIgor CemortanNo ratings yet
- Abdominal Vascular Emergency 2016Document13 pagesAbdominal Vascular Emergency 2016Medicina 42No ratings yet
- 10 1016@j JVSV 2014 05 007Document11 pages10 1016@j JVSV 2014 05 007Laura BorraezNo ratings yet
- Gastrointestinal Bleeding Case FileDocument3 pagesGastrointestinal Bleeding Case Filehttps://medical-phd.blogspot.comNo ratings yet
- History: Acute Mesenteric Ischemia (AMI) Is A Syndrome in WhichDocument6 pagesHistory: Acute Mesenteric Ischemia (AMI) Is A Syndrome in WhichAlexis Nacionales AguinaldoNo ratings yet
- Uppergastrointestinalbleeding: Marcie Feinman,, Elliott R. HautDocument11 pagesUppergastrointestinalbleeding: Marcie Feinman,, Elliott R. HautjoseNo ratings yet
- Acutemesentericischemia: Michael J. SiseDocument17 pagesAcutemesentericischemia: Michael J. SiseMD Luthfy LubisNo ratings yet
- Me DCL Inn Avarice Al BleedingDocument24 pagesMe DCL Inn Avarice Al BleedingKarina WibowoNo ratings yet
- Abdominal Aortic AneurysmDocument20 pagesAbdominal Aortic AneurysmPortia Rose RodriguezNo ratings yet
- Acute Intestinal IschemiaDocument50 pagesAcute Intestinal IschemiaRohit ParyaniNo ratings yet
- Ascitis PDFDocument17 pagesAscitis PDFLeonardo MagónNo ratings yet
- Abdominal Aortic AneurysmDocument3 pagesAbdominal Aortic AneurysmRonald Cszar Fabian VillanoNo ratings yet
- Acute Abdomen - StatPearls - NCBI BookshelfDocument6 pagesAcute Abdomen - StatPearls - NCBI Bookshelfimehap033No ratings yet
- 10 1056@NEJMra1503884 PDFDocument10 pages10 1056@NEJMra1503884 PDFmarselamgeNo ratings yet
- Vasculer Anomly of IntestineDocument38 pagesVasculer Anomly of Intestineعبد الله مازن موسى عبدNo ratings yet
- Mallory Weiss Syndrome - StatPearls - NCBI BookshelfDocument9 pagesMallory Weiss Syndrome - StatPearls - NCBI BookshelfDaniela EstradaNo ratings yet
- Nejm 2016 Mesenteric IschemiaDocument11 pagesNejm 2016 Mesenteric IschemiarisewfNo ratings yet
- Ascitis ImportanteDocument17 pagesAscitis Importantedanyescalerapumas24No ratings yet
- Ischemic Colitis: A Clinical Case and Concise ReviewDocument15 pagesIschemic Colitis: A Clinical Case and Concise ReviewDevi AmaraNo ratings yet
- Abdominal ImagingDocument16 pagesAbdominal Imagingfrancu60No ratings yet
- Abdominal Aortic AneurysmDocument14 pagesAbdominal Aortic AneurysmjialinNo ratings yet
- Pericardial EffusionDocument26 pagesPericardial EffusionjsenocNo ratings yet
- Pancreatic Pseudocyst EDITEDDocument5 pagesPancreatic Pseudocyst EDITEDLaura LatifaNo ratings yet
- Utd 32654 Case - Reports AydinDocument3 pagesUtd 32654 Case - Reports AydinDavid LopezNo ratings yet
- Pancreatic Pseudocyst EDITEDDocument5 pagesPancreatic Pseudocyst EDITEDLaura LatifaNo ratings yet
- Abdominal TraumaDocument24 pagesAbdominal TraumaSurgeryClassesNo ratings yet
- ZZ - 1999-12 - Massive Intraperitoneal Hemorrhage From A Pancreatic PseudocystDocument4 pagesZZ - 1999-12 - Massive Intraperitoneal Hemorrhage From A Pancreatic PseudocystNawzad SulayvaniNo ratings yet
- CASE REPORT 3 - Acute Mesentric Venous Thrombosis With A History Recurrent DVT in Young Age A Case ReportDocument2 pagesCASE REPORT 3 - Acute Mesentric Venous Thrombosis With A History Recurrent DVT in Young Age A Case Reportm.widodo190216No ratings yet
- Dysphagia Lusoria: A Comprehensive ReviewDocument6 pagesDysphagia Lusoria: A Comprehensive ReviewDante ChavezNo ratings yet
- Esophageal VaricesDocument4 pagesEsophageal VaricesSnapeSnapeNo ratings yet
- Rheumatology Journal Club Gut Vasculitis: by DR Nur Hidayati Mohd SharifDocument36 pagesRheumatology Journal Club Gut Vasculitis: by DR Nur Hidayati Mohd SharifEida MohdNo ratings yet
- Angio Displa SiaDocument4 pagesAngio Displa SiaBelaFawziaNo ratings yet
- Cholecystitis: David R. Elwood, MDDocument12 pagesCholecystitis: David R. Elwood, MDJefferson Candela RadaNo ratings yet
- A SC Ites: Diagnosis Andmanagement: Wei Hou,, Arun J. SanyalDocument17 pagesA SC Ites: Diagnosis Andmanagement: Wei Hou,, Arun J. SanyalNicole Zavaleta VelásquezNo ratings yet
- Lec 6Document13 pagesLec 6Hoth HothNo ratings yet
- Abdominal TraumaDocument8 pagesAbdominal Traumahatem alsrour100% (2)
- Acute Gastrointestinal Bleeding Upper GI BleedingDocument18 pagesAcute Gastrointestinal Bleeding Upper GI BleedingAldwin AyuyangNo ratings yet
- Abdominal ImagingDocument6 pagesAbdominal Imagingmihaela2786No ratings yet
- Compartment SyndromeDocument10 pagesCompartment SyndromeFebriyan EdmiNo ratings yet
- Small Bowel Obstruction &post Operative IleusDocument62 pagesSmall Bowel Obstruction &post Operative IleusMamanya Fadhil HaniNo ratings yet
- Vascular Emergencies: Susan L. Drinkwater, Vikas A. Pandey, and Alun H. DaviesDocument17 pagesVascular Emergencies: Susan L. Drinkwater, Vikas A. Pandey, and Alun H. DaviesHarshpreet KaurNo ratings yet
- CholangitisDocument15 pagesCholangitisFaye TanNo ratings yet
- ABC Emergency Differential DiagnosisffDocument3 pagesABC Emergency Differential Diagnosisffsharu4291No ratings yet
- Abdominal Aortic AneurysmDocument9 pagesAbdominal Aortic AneurysmIlyes FerenczNo ratings yet
- Esophageal-Varices 20240201 124908 0000Document25 pagesEsophageal-Varices 20240201 124908 0000Eurika P OrolfoNo ratings yet
- Esophageal VaricesDocument9 pagesEsophageal VaricesErina WahyuniNo ratings yet
- EXAM CompiledDocument19 pagesEXAM CompiledAhmad Fuad HasbollahNo ratings yet
- Mesenteric Ischemia ReviewDocument12 pagesMesenteric Ischemia Reviewmaria arenas de itaNo ratings yet
- Primary Aortoenteric FistulaDocument5 pagesPrimary Aortoenteric FistulaKintrili AthinaNo ratings yet
- Budd-Chiari Syndrome: Michael A. Zimmerman, MD, Andrew M. Cameron, MD, PHD, R. Mark Ghobrial, MD, PHDDocument15 pagesBudd-Chiari Syndrome: Michael A. Zimmerman, MD, Andrew M. Cameron, MD, PHD, R. Mark Ghobrial, MD, PHDCarlos AlmeidaNo ratings yet
- PathologyDocument28 pagesPathologyninja-2001No ratings yet
- Beyond the Aorta: Exploring the Depths of Abdominal Aortic AneurysmFrom EverandBeyond the Aorta: Exploring the Depths of Abdominal Aortic AneurysmNo ratings yet
- CaddraGuidelines2011 ToolkitDocument48 pagesCaddraGuidelines2011 ToolkitYet Barreda Basbas100% (1)
- Healthy Mouth Hygiene GuideDocument6 pagesHealthy Mouth Hygiene GuideViolet VioletNo ratings yet
- The Clinical Use of Drugs. Lippincott Williams & Wilkins Pennsylvania, United StatesDocument4 pagesThe Clinical Use of Drugs. Lippincott Williams & Wilkins Pennsylvania, United StatesshaniNo ratings yet
- Hypocalcemia in NewbornsDocument2 pagesHypocalcemia in NewbornsEunice Lan ArdienteNo ratings yet
- Indications of ICU Admission and ICU Management of COVID 19 NEWDocument27 pagesIndications of ICU Admission and ICU Management of COVID 19 NEWMidhat FatmaNo ratings yet
- Apha Naplex PDFDocument408 pagesApha Naplex PDFsweetNo ratings yet
- Bradycardia and TachycardiaDocument50 pagesBradycardia and Tachycardialiu_owen17No ratings yet
- Pretest Surgery (1) 44Document8 pagesPretest Surgery (1) 44Hasan A AsFourNo ratings yet
- National Leprosy Eradication ProgrammeDocument11 pagesNational Leprosy Eradication ProgrammeNikhil SinghalNo ratings yet
- Nursing Self Assessment ToolkitDocument19 pagesNursing Self Assessment ToolkitJasmeet KaurNo ratings yet
- Acute Diseases and Life-Threatening Conditions: Assistant Professor Kenan KaravdićDocument33 pagesAcute Diseases and Life-Threatening Conditions: Assistant Professor Kenan KaravdićGoran MaliNo ratings yet
- Ebook Clinical Orthopedic Examination of A Child 1St Edition Nirmal Raj Gopinathan 2 Online PDF All ChapterDocument69 pagesEbook Clinical Orthopedic Examination of A Child 1St Edition Nirmal Raj Gopinathan 2 Online PDF All Chapterelizabeth.byrd950100% (12)
- HYPOTHYROIDISMDocument11 pagesHYPOTHYROIDISMVarun SinghNo ratings yet
- Douche: By. Dhanusrii Fourth BnysDocument12 pagesDouche: By. Dhanusrii Fourth BnysN.Darshaniya100% (1)
- Answer Key: Vital Signs and MonitoringDocument1 pageAnswer Key: Vital Signs and Monitoringmaglit777No ratings yet
- Case Report Elizabeth KingiaDocument7 pagesCase Report Elizabeth KingiaSardono WidinugrohoNo ratings yet
- Median Lethal Dose (LD)Document4 pagesMedian Lethal Dose (LD)Christian ConsignaNo ratings yet
- ANTENATAL ASSESSMENT Form 3Document4 pagesANTENATAL ASSESSMENT Form 3Kaku ManishaNo ratings yet
- BSC in Lab Medicine Part-II-1Document87 pagesBSC in Lab Medicine Part-II-1sabuj ranaNo ratings yet
- Approaching A Large Defect On The Lower Nasal.97652Document4 pagesApproaching A Large Defect On The Lower Nasal.97652david carsNo ratings yet
- Anello2019 PDFDocument2 pagesAnello2019 PDFandreiNo ratings yet
- Funda Lab - Prelim ReviewerDocument16 pagesFunda Lab - Prelim ReviewerNikoruNo ratings yet
- (2020) Primary Dysmenorrhea Diagnosis and TherapyDocument12 pages(2020) Primary Dysmenorrhea Diagnosis and TherapyEderEscamillaVelascoNo ratings yet
- NCP HivDocument2 pagesNCP HivCamille Joy BaliliNo ratings yet
- Jurnal Integritas KulitDocument7 pagesJurnal Integritas KulitNur FaddliNo ratings yet
- 02-Kexing Product Catalogue (Index)Document2 pages02-Kexing Product Catalogue (Index)londonpharmauzNo ratings yet
- AAFP Marzo 2016 HipertiroidismoDocument11 pagesAAFP Marzo 2016 HipertiroidismoAntonio MoncadaNo ratings yet
- Peds NBME Form 1 Flashcards - QuizletDocument14 pagesPeds NBME Form 1 Flashcards - Quizletparth515No ratings yet