Professional Documents
Culture Documents
Review Desregulación de Insulina
Review Desregulación de Insulina
Uploaded by
María Ignacia Bueno Della-RosaCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Review Desregulación de Insulina
Review Desregulación de Insulina
Uploaded by
María Ignacia Bueno Della-RosaCopyright:
Available Formats
bs_bs_banner
Equine Veterinary Journal ISSN 0425-1644
DOI: 10.1111/evj.12169
Review Article
Insulin dysregulation
N. FRANK* and E. M. TADROS
Department of Clinical Sciences, Tufts Cummings School of Veterinary Medicine, North Grafton, Massachusetts, USA
Division of Veterinary Medicine, School of Veterinary Medicine and Science, University of Nottingham, Sutton Bonington, Leicestershire, UK
Department of Large Animal Clinical Sciences, College of Veterinary Medicine, Michigan State University, East Lansing, USA.
*Correspondence email: nicholas.frank@tufts.edu; Received: 24.01.13; Accepted: 02.08.13
Summary
Abnormalities of insulin metabolism include hyperinsulinaemia and insulin resistance, and these problems are collectively referred to as insulin
dysregulation in this review. Insulin dysregulation is a key component of equine metabolic syndrome: a collection of endocrine and metabolic abnormalities
associated with the development of laminitis in horses, ponies and donkeys. Insulin dysregulation can also accompany prematurity and systemic illness in
foals. Causes of insulin resistance are discussed, including pathological conditions of obesity, systemic inammation and pituitary pars intermedia
dysfunction, as well as the physiological responses to stress and pregnancy. Most of the discussion of insulin dysregulation to date has focused on insulin
resistance, but there is increasing interest in hyperinsulinaemia itself and insulin responses to feeding. An oral sugar test or in-feed oral glucose tolerance
test can be performed to assess insulin responses to dietary carbohydrates, and these tests are now recommended for use in clinical practice. Incretin
hormones are likely to play an important role in postprandial hyperinsulinaemia and are the subject of current research. Insulin resistance exacerbates
hyperinsulinaemia, and insulin sensitivity can be measured by performing a combined glucose-insulin test or i.v. insulin tolerance test. In both of these tests,
exogenous insulin is administered and the rate of glucose uptake into tissues measured. Diagnosis and management of hyperinsulinaemia is recommended
to reduce the risk of laminitis. The term insulin dysregulation is introduced here to refer collectively to excessive insulin responses to sugars, fasting
hyperinsulinaemia and insulin resistance, which are all components of equine metabolic syndrome.
Keywords: horse; insulin; glucose; insulin dysregulation; insulin resistance; laminitis; diabetes
Equine metabolic syndrome
Equine metabolic syndrome (EMS) is a collection of endocrine and
metabolic abnormalities associated with the development of laminitis in
horses, ponies and donkeys [1]. Insulin dysregulation, hyperleptinaemia,
increased adiposity and hypertriglyceridaemia are components of EMS,
and are risk factors for laminitis [2]. Hyperinsulinaemia is a particular
concern because laminitis has been experimentally induced in healthy
ponies and horses by infusing exogenous insulin with glucose i.v. [3,4].
Generalised obesity and/or regional adiposity accompany insulin
dysregulation in many equids with EMS. Horses and ponies with EMS
should also be evaluated for evidence of laminitis, including divergent hoof
growth rings (founder lines) or third phalanx rotation. Mild laminar
pathology does not always cause overt lameness and can go unrecognised
by horse owners. Increased adiposity is evident before laminitis in most
animals, but a lean EMS phenotype also exists, with insulin dysregulation
and laminitis occurring in horses and ponies with normal appearance.
Other terms used in the past to describe EMS include prelaminitic
metabolic syndrome, syndrome X, insulin resistance syndrome,
obesity-associated insulin resistance (IR) and prediabetes mellitus [5,6].
Hyperinsulinaemia
The discussion of hyperinsulinaemia in equids has been complicated by
the different approaches used in the past to assess glucose and insulin
dynamics. Insulin concentrations have been measured in the fed state in
several studies [2,710]. In others, horses have been fasted [1113], and
fasting prior to sample collection was recommended in the 2010 American
College of Veterinary Internal Medicine consensus statement [1].
Fasting hyperinsulinaemia results from persistent stimulation of
pancreatic cells, and in obese human individuals increased insulin
secretion during the interprandial period is attributed to elevated fatty acid
concentrations [14]. Hyperinsulinaemia has also been associated with
obesity in equids and higher fatty acid concentrations were detected in
obese insulin-resistant horses in one study, although hay was available at
the time of sampling [10]. Beta-cell hyperplasia is also a potential cause of
fasting hyperinsulinaemia. Several hormones and nutrients act as insulin
secretagogues and increase insulin concentrations, including incretin
Equine Veterinary Journal 46 (2014) 103112 2013 EVJ Ltd
hormones [15], glucagon, glucose, fatty acids and arginine. Insulinomas
can be accompanied by hypoglycaemia and an increased insulin:glucose
ratio, and are a rare cause of hyperinsulinaemia in other animals [16,17].
Only one case of insulinoma has been reported in equids, in a 12-year-old
Shetland pony that developed seizures [18]. Hypoglycaemia and
hyperinsulinaemia were detected during seizures and increased insulin
secretion was demonstrated during an oral glucose tolerance test and an
i.v. glucagon tolerance test.
Postprandial hyperinsulinaemia is a concern in equids because feeding
occurs on an almost continuous basis when horses and ponies are grazing
on pasture. Even when fasted, digestion continues for many hours within
the equine caecum and large intestine, with production of the
gluconeogenic substrate propionic acid and amino acids [19]. Testing
horses in the fed state allows for better assessment of insulin
dysregulation, but feeds vary in composition and this makes it difcult
to establish reference ranges. Standardised tests are therefore
recommended to diagnose hyperinsulinaemia in horses. The rst option is
an oral sugar test that is gaining acceptance in the USA, where corn syrup
is readily available for purchase [20], and the second is an in-feed oral
glucose test that is used in the UK, performed by mixing glucose powder
into a chaff-based feed in an amount equivalent to 1 g/kg bwt, with
samples collected 2 h later [21].
Hyperinsulinaemia is caused by increased insulin secretion or delayed
insulin clearance, and this problem may be a cause or a consequence of
IR (Fig 1). The accepted explanation for hyperinsulinaemia is that
insulin secretion increases as a consequence of decreased tissue insulin
sensitivity and this is referred to as compensated IR [8]. Decreased hepatic
insulin clearance is also associated with IR and can contribute to
hyperinsulinaemia because >70% of insulin secreted from cells is normally
cleared from the portal blood before reaching the peripheral circulation in
horses [22]. Low connecting (C)-peptide/insulin ratios have been detected
in horses with EMS and provide evidence of decreased insulin clearance
[22]. Connecting-peptide is a component of the proinsulin prohormone,
and is cleaved prior to secretion of the mature insulin peptide from
pancreatic cells. Since C-peptide is released in equal amounts to insulin,
concentrations reect insulin secretion. Unlike insulin, which has a plasma
half-life of only 58 min in humans, C-peptide does not undergo rapid
clearance from the blood by the liver, so blood concentrations reect
pancreatic function and can be used to evaluate hepatic insulin clearance.
103
Insulin dysregulation
N. Frank and E. M. Tadros
Excessive insulin
response to sugars
and/or amino acids
Postprandial
hyerinsulinaemia
Tissue insulin
resistance
Obesity has been a component of EMS since the syndrome was
rst proposed in 2002 [28], but hyperinsulinaemia is also detected in lean
horses and ponies [21] and some obese animals have normal insulin
concentrations [11,12]. These inconsistencies can be explained by
considering obesity as modifying factor, with the genetics of the individual
animal determining the magnitude of insulin dysregulation.
Hyperinsulinaemia itself might even promote obesity through the anabolic
effects of insulin on lipid metabolism [14] and contribute to the easy
keeper or good doer phenotype. Horses and ponies with this phenotype
readily become obese when overfed, and obesity can develop when grass
is the only source of energy. A recent study performed with knockout mice
conrmed that hyperinsulinaemia alters lipid metabolism and promotes
obesity [29]. Genetic manipulations affecting the brain and pancreas
generated mice that were incapable of diet-induced hyperinsulinaemia,
and these animals were also protected from obesity and hepatic lipid
inltration. Hyperinsulinaemia, obesity and hepatic IR might therefore
represent a vicious cycle in equids if lipid inltration of the liver slows
insulin clearance and higher fatty acid concentrations induce fasting
hyperinsulinaemia.
Relative hypoinsulinaemia and
diabetes mellitus
Fig 1: The cause-and-effect relationship between insulin resistance and
hyperinsulinaemia.
Although the cause-and-effect relationship between IR and
hyperinsulinaemia appears straightforward, the authors have encountered
horses and ponies with postprandial hyperinsulinaemia that have normal
glucose and insulin responses during the combined glucose-insulin test
(CGIT), which is a test for insulin sensitivity. Other causes of postprandial
hyperinsulinaemia following ingestion of sugars should therefore be
considered, including increased stimulation by incretin hormones,
including glucagon-like peptide 1 and glucose-dependent insulinotropic
peptide [15]. These incretin hormones are secreted from L and K cells,
respectively, within the small intestine in response to ingestion of sugars,
amino acids and fats, and the activity of both hormones is regulated
through degradation by the enzyme dipeptidyl peptidase 4. Both
hormones have been identied in equine plasma after oral administration
of glucose [23,24]. Incretins stimulate pancreatic cell insulin secretion
and slow gastric emptying, thereby minimising postprandial
hyperglycaemia. Postprandial hyperinsulinaemia in horses with EMS might
therefore reect increased incretin hormone secretion or decreased
degradation by dipeptidyl peptidase 4. Furthermore, incretin hormones
increase pancreatic islet mass in rodents by stimulating cell proliferation,
induction of islet neogenesis, and inhibition of cell apoptosis [25]. It is
conceivable that chronic incretin hormone stimulation contributes to cell
hyperplasia and hyperinsulinaemia in horses with EMS. In humans, fasting
glucagon-like peptide 1 concentrations increase in association with greater
clustering of metabolic syndrome components [26].
If the rst manifestation of insulin dysregulation in genetically
predisposed horses is postprandial hyperinsulinaemia, then IR would raise
insulin concentrations even further. These relationships are illustrated in
Figure 2. Obesity, systemic inammation and concurrent endocrinopathies
such as pituitary pars intermedia dysfunction (PPID) are potential causes of
IR that can exacerbate hyperinsulinaemia by slowing insulin clearance.
Hyperinsulinaemia might even induce IR itself through the process of
homologous desensitisation, a process by which tissue sensitivity to
insulin decreases as blood hormone concentrations increase [14]. Acute
increases in insulin concentrations can still stimulate glucose uptake, but
chronic hyperinsulinaemia results in downregulation of the insulin receptor
and downstream signalling. This is the mechanism by which insulinomas
induce IR and is referred to as the Somogyi effect, when higher doses
of exogenous insulin have a diminished effect on blood glucose
concentrations [14]. Evidence for hyperinsulinaemia inducing IR was
provided by a recent study in mice [27]: a high-fat diet induced obesity and
IR, and streptozotocin was administered to one group of mice to lower
insulin concentrations. Insulin resistance was only detected in mice that
developed hyperinsulinaemia.
104
The term hypoinsulinaemia is rarely used because lower limits are not
provided for insulin reference ranges. However, the concept of relative
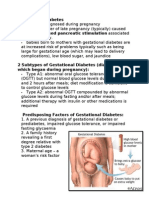
hypoinsulinaemia is a key component of diabetes mellitus. Type 1 diabetes
mellitus is most commonly caused by immune-mediated destruction of
pancreatic cells, resulting in inadequate insulin secretion, and a rarer
idiopathic form is also recognised in humans. In contrast, type 2 diabetes
mellitus develops when insulin production by cells decreases following
a prolonged period of hyperinsulinaemia. The term pancreatic insufciency
or pancreatic exhaustion are used to describe this process of
decompensation, and Treiber et al. [8] adopted the term uncompensated
insulin resistance to describe horses and ponies with high blood glucose
concentrations that are inadequately controlled by insulin. In diabetes
mellitus, pancreatic insulin secretion decreases as a result of direct
damage to the pancreas and loss of cell mass, whereas inhibition by
hormones such as somatostatin and catecholamines can suppress insulin
Equine metabolic syndrome (EMS)
[Genetic predisposition]
Postprandial
hyperinsulinaemia
Anabolic effects:
Obesity and regional
adiposity
(+)
PPID
Inflammation
Pregnancy
Tissue insulin resistance
At-risk
Disease:
LAMINITIS
Fig 2: Putative relationships among hyperinsulinaemia, obesity, insulin resistance and
the exacerbating factors of pregnancy, inammation and pituitary pars intermedia
dysfunction (PPID).
Equine Veterinary Journal 46 (2014) 103112 2013 EVJ Ltd
Insulin dysregulation
N. Frank and E. M. Tadros
secretion during stress or illness [30]. In veterinary medicine, type 1
diabetes mellitus is most commonly observed in dogs, whereas type 2
diabetes mellitus is more often detected in cats. Transient Type 1 diabetes
mellitus has recently been reported in a foal [31], and there are reports of
type 2 diabetes mellitus in mature horses in association with pancreatitis
[32], PPID [33,34], granulosa cell tumour [35], and presumed autoimmune
polyendocrine syndrome [36].
Increased understanding of glucose and insulin dysregulation in
horses has led to more frequent recognition of diabetes mellitus,
particularly in horses with PPID [33]. Horses with advanced PPID can
develop transient diabetes mellitus when stress and systemic disease are
encountered, so it is important to monitor blood glucose and triglyceride
concentrations in hospitalised patients. Hyperglycaemia is marked
(>11 mmol/l [2.0 mg/l]) in some horses and accompanied by glucosuria.
Severe hypertriglyceridaemia is also a concern in horses with diabetes
mellitus, and insulin therapy is required to manage hyperglycaemia and
suppress hormone-sensitive lipase. This condition appears to involve cell
insufciency because horses are very sensitive to exogenous insulin and
return to adequate glycaemic control when the primary problem resolves,
or when pergolide treatment is initiated or increased. Hyperglycaemia
alters the amino acid lysine and this leads to the formation of fructosamine,
which alters other amino acids and creates advanced glycosylation
end-products that damage tissues. Higher fructosamine concentrations
have been detected in laminitic horses [37] and are likely to reect the
accompanying stress- and pain-associated hyperglycaemia.
Insulin resistance
Insulin resistance refers to the failure of insulin-sensitive tissues to respond
to insulin, and skeletal muscle, adipose, and liver are primarily affected.
Consequences of IR include impaired glucose uptake into tissues,
increased glucose synthesis in the liver via gluconeogenesis, and
increased lipolysis resulting in higher circulating free fatty acid
concentrations. Insulin resistance is associated with glucose transporter 4
dysfunction within skeletal muscle and adipose tissues [38,39].
Insulin resistance and glucose
Resting glucose concentrations are often towards the higher end of
reference range in horses and ponies with EMS [10], and it is reasonable to
assume that both hyperglycaemia and hyperinsulinaemia are encountered
when these animals are grazing on pasture (Fig 3). Glucotoxicity is a
Interaction: Pasture
January
April
Increase in
starch, sugars, and
amino acids
Insulin
Exacerbation of
hyperinsulinaemia
Jan
Apr
Increased risk of
LAMINITIS
Fig 3: The effect of pasture on hyperinsulinaemia as a risk factor for laminitis.
Postprandial blood glucose and insulin concentrations respond to changes in pasture
grass composition and abundance across different seasons of the year. Starches,
sugars and amino acids raise insulin concentrations and exacerbate preexisting
hyperinsulinaemia in genetically susceptible horses.
Equine Veterinary Journal 46 (2014) 103112 2013 EVJ Ltd
consequence of persistent hyperglycaemia in human diabetes mellitus
patients, and hyperglycaemia can result in glycosylation of amino acids
within tissues and the formation of advanced glycosylation end-products.
Tissues become damaged as a result of glycosylation and this process
contributes to the development of diabetic angiopathy [40]. Endothelial
dysfunction is also induced as hyperglycaemia stimulates diacylglycerol
synthesis and activation of protein kinase C. Hyperglycaemia might
therefore contribute to the development of laminitis in horses, and this
hypothesis has been tested in 2 studies. Hoof lamella changes suggestive
of laminitis were induced in healthy Standardbred horses by infusing
glucose i.v. for 48 h [41]. However, in a related study using the
hyperinsulinaemia model [42] advanced glycosylation end-products were
not detected in hoof tissues collected after laminitis was induced. Glucose
might therefore play a role in the development of acute laminitis by
inducing endogenous insulin secretion or altering endothelial function, but
not through glycosylation of amino acids.
Insulin resistance and obesity
Obesity is a pathological condition associated with altered adipokine
production and IR, and inammation plays an important role in obesity in
other species [4346]. As adipocytes reach their maximal storage capacity,
events leading to energy failure, inammation and cellular stress are
initiated [47]. Hypoxia is a factor in adipocyte stress because oxygen only
diffuses approximately 100 m from capillary beds, and adipocyte
diameter expands beyond this limit in obesity [47,48]. The endothelium of
vessels within adipose tissues can also become unresponsive to nitric
oxide-induced vasodilation, and this further contributes to hypoxia [47,49].
Hypoxia leads to a reduction in mitochondrial function and stimulation of
hypoxia-induced genes that promote inammation. Stressed adipocytes,
and those that have become necrotic as a result of hypoxia, release
cytokines such as macrophage chemoattractant proteins that recruit new
macrophages to adipose tissues [47,5052]. Resident tissue macrophages
within adipose tissue tend to be anti-inammatory in prole, whereas
those recruited by stressed cells have a more proinammatory prole [47].
Resident macrophages can also convert to a proinammatory prole
under conditions of adipose tissue hypoxia or when inuenced by
recruited proinammatory macrophages [53,54].
In addition to suffering from hypoxia, adipocytes that are laden with
triglyceride lose their ability to buffer lipid uxes within the body [47,55].
Ectopic lipid deposition and lipotoxicity ensue, contributing to the
development of IR in adipose and other tissues. Lipid accumulation in liver,
muscle, pancreas and other tissues has a negative impact on insulin
metabolism throughout the body [5558]. Insulin normally induces nitric
oxide-dependent vasodilation in certain capillary beds, so loss of insulin
sensitivity further impedes postprandial capillary recruitment and the
delivery of lipids to appropriate storage depots, promoting ectopic
deposition [47]. Accumulation of intermediate lipid metabolites such as
diacylglycerol, long-chain fatty acyl CoA, and ceramide exacerbates cell
stress and incites inammation, and this leads to IR [5961].
Inammatory mediators secreted from adipose tissue act locally and at
distant locations, which may be relevant to equine laminitis because the
vascular endothelium is targeted [62,63]. In obese human individuals and
rodents, increased adipose tissue secretion of inammatory mediators
and adipokines is well described [45], but studies on associations between
obesity and inammatory cytokines have yielded conicting results in
horses. Vick et al. [13] detected positive correlations among body
condition score, blood mRNA expression of tumour necrosis factor
(TNF) and interleukin (IL)-1, and blood TNF protein concentrations in
light breed mares. Regional adiposity, assessed using the cresty neck score
[64], has also been associated with increased plasma TNF protein
concentrations in ponies [2]. Previously laminitic ponies had signicantly
higher plasma TNF protein concentrations than nonlaminitic ponies, and
the same animals had higher neck scores and insulin concentrations.
Detection of hyperinsulinaemia in horses and ponies with regional
adiposity and laminitis raises the question of whether insulin affects
inammatory cytokine concentrations in horses. This has been
demonstrated in horses using an experimental model, with signicantly
higher plasma TNF and IL-6 protein concentrations detected during i.v.
infusion of insulin for 6 h [65]. Average TNF concentrations were 16% and
20% higher than baseline at 4 and 6 h, respectively, in the insulin group.
105
Insulin dysregulation
Not all studies have supported the development of a basal
proinammatory state in obese and hyperinsulinaemic horses.
Holbrook et al. [66] demonstrated lower endogenous gene expression of
IL-1 and IL-6 in peripheral blood mononuclear cells from hyperinsulinaemic
obese horses than in controls, and comparable cytokine responses in
both groups following peripheral blood mononuclear cell stimulation.
However, neutrophil oxidative burst activity was signicantly higher in
obese horses, suggesting that immune function is altered by obesity and
hyperinsulinaemia. Suagee et al. [7] were unable to associate obesity with
plasma concentrations of TNF, IL-1 or IL-6 protein in a larger population
of 110 horses. Of the variables examined, only serum amyloid A
concentrations were positively correlated with insulin concentrations and
body condition score. When insulin-resistant and insulin-sensitive horses
were compared by Burns et al. [67], no differences in TNF, IL-1, IL-6 or
macrophage chemoattractant protein-1 mRNA expression were detected
within adipose tissues collected from multiple sites. This study revealed,
however, that expression of IL-1 and IL-6 was signicantly higher in nuchal
ligament adipose tissue, than in other depots, suggesting that regional
adiposity contributes to the increased risk of laminitis in insulin-resistant
horses. It therefore remains challenging to separate the effects of adiposity,
hyperinsulinaemia and IR on inammatory cytokine proles in equids.
Hepatic insulin resistance
Hepatic lipid inltration accompanies obesity in man and can lead to the
development of nonalcoholic fatty liver disease [6870]. Increased plasma
gamma glutamyl transferase activity and post mortem evidence of hepatic
lipidosis have also been detected in obese horses (N. Frank, unpublished
data). Enhanced peripheral lipolysis secondary to IR represents the major
cause of lipid accumulation in the steatotic liver, with a smaller
contribution by de novo lipid synthesis within hepatocytes [71].
Intermediates of fatty acid metabolism are agonists for Kupffer cell pattern
recognition receptors and therefore trigger an inammatory cascade
[56,72], which induces hepatic IR and contributes to systemic inammation
[73]. Recent studies suggest that IL-6 plays an important role in hepatic IR
by suppressing insulin receptor autophosphorylation and tyrosine
phosphorylation of insulin receptor substrate 1 [74].
Hepatic IR may also lead to the development of hypertriglyceridaemia in
horses and ponies. Although plasma triglyceride and very low-density
lipoprotein (VLDL) concentrations are only mildly increased in horses and
ponies with obesity and hyperinsulinaemia [2,10], they are potential
indicators of hepatic IR. Insulin secreted from the pancreas arrives at the
liver via the portal blood and normally suppresses VLDL secretion after
eating, so that triglycerides are stored at times of positive energy balance.
Pathways involved in insulin-mediated suppression of VLDL secretion are
affected by hepatic lipidosis and IR, and lipoprotein secretion increases as
a result [75]. Increased ferritin concentrations are also detected in human
nonalcoholic fatty liver disease patients, and serve as a predictor of liver
damage [76]. Ferritin concentrations were recently measured in obese
horses and a positive correlation existed between ferritin concentrations
and insulin area under the curve values after oral dextrose administration
and corn ingestion [77].
Insulin resistance and adipokines
Leptin is an adipocyte-derived hormone that is produced almost
exclusively by white adipose tissue, and concentrations increase in obese
and insulin-resistant horses as a result of increased fat mass and leptin
resistance [2,10,7880]. Leptin acts as an adiposity signal to keep other
systems in the body apprised of the adipose depot size, and interaction
between leptin and its long-form receptor in the hypothalamus modulates
satiety [81,82]. Intact leptin signalling results in appetite suppression [81]
and might also enhance energy expenditure and reduce hepatic fatty acid
synthesis [83]. In humans, leptin resistance is implicated in overeating and
obesity [84]. Leptin concentrations are positively correlated with body
condition score in horses, ponies and donkeys [78,85], although
hyperleptinaemia is also detected in equids with normal body condition
scores. Hyperinsulinaemia and tissue IR are both associated with
hyperleptinaemia in mares [86]. Leptin might therefore serve as an indirect
measure of adipocyte pathology and insulin dysfunction, and leptin
106
N. Frank and E. M. Tadros
concentrations are included on a diagnostic panel for EMS, with a cut-off
value of 4 g/l for hyperleptinaemia.
Adiponectin is an insulin-sensitising hormone with pleotropic effects
that include enhancement of fatty acid oxidation and improvement of
glucose tolerance [87]. This adipokine also possesses anti-inammatory
properties and counteracts IR caused by cytokines such as TNF [88].
Adiponectin circulates in the form of trimers, hexamers and high molecular
weight multimers [89], and lower concentrations of total [80] and high
molecular weight [90] adiponectin have been detected in obese horses.
High molecular weight adiponectin concentrations were negatively
correlated with insulin concentrations [90].
Leptin and adiponectin are important to the discussion of EMS and
laminitis because both adipokines have direct effects on the vascular
endothelium, as well as indirect effects via modulation of insulin sensitivity
and inammation [9193]. Adiponectin has anti-inammatory actions and
can therefore counteract the effects of cytokines such as TNF on the
endothelium [81,9497]. In contrast, leptin is generally proinammatory
and exacerbates endothelial activation and the generation of free radicals
that damage the endothelium [98,99]. Obese people with adiponectin
deciency have a higher risk of mortality during sepsis, and loss of
adiponectins immunomodulatory effects and protective actions on the
endothelium is believed to be a contributing factor [94].
Insulin resistance and PPID
It is often assumed that PPID predictably causes IR, but this assumption
must be challenged on the basis of clinical experience and the detection of
hyperinsulinaemia in only 32% of horses with PPID [100]. There are a
number of mechanisms that might link PPID with hyperinsulinaemia and IR
in horses. Cortisol antagonises the actions of insulin and causes IR, with
accompanying hyperinsulinaemia, as is readily demonstrated in the rat by
administering dexamethasone [101]. Administration of dexamethasone to
healthy horses also increases plasma insulin concentrations and lowers
insulin sensitivity [102,103]. Hyperinsulinaemia and decreased insulin
sensitivity are recognised consequences of hyperadrenocorticism in dogs,
and diabetes mellitus is commonly detected [104]. Higher C-peptide
concentrations are also detected following glucagon infusion in dogs
with hyperadrenocorticism and provide evidence of increased insulin
secretion [105]. Corticotropin-like intermediate peptide is a derivative
of pro-opiomelanocortin and adrenocorticotrophic hormone (amino
acids 1839), and concentrations increase in horses with PPID [106,107].
This hormone acts as an insulin secretagogue when added to the media
of pancreatic explants [108], and might therefore contribute to the
development of hyperinsulinaemia in equine PPID. Alpha melanocytestimulating hormone (MSH) concentrations are also increased with PPID
[109] and this hormone, along with leptin, plays an important role in energy
metabolism. Under normal conditions, MSH stimulates neural
melanocortin receptors 3 and 4 within the hypothalamus, opposes
the action of leptin, and reduces body fat mass [110]. However,
downregulation of this system as a result of increased MSH
concentrations might have the opposite effect and raise insulin
concentrations through increased visceral adiposity and hepatic IR.
One explanation for the variability in insulin concentrations detected in
horses with PPID is that the condition itself is less predictable than other
forms of hyperadrenocorticism. Adrenal hyperplasia is a common
manifestation of hyperadrenocorticism caused by pars distalis tumours
in dogs, whereas only approximately 20% of horses with PPID develop
this problem [111]. Polyuria and polydipsia are also common features of
canine hyperadrenocorticism, but are only reported in 30% of horses with
PPID [112].
Convergence of PPID and EMS
An alternative explanation for the variability in insulin concentrations
detected in equids with PPID is that this endocrinopathy acts only as a
modifying factor (Fig 2). If hyperinsulinaemia is a genetically determined
trait in equids, then PPID exacerbates the problem by stimulating
insulin secretion via increased corticotrophin-like intermediate peptide
concentrations or by inducing IR though hyperadrenocorticism. When
viewed from this perspective, it is not surprising that in the study by
van der Kolk et al. [113] hyperinsulinaemia had 92% sensitivity as a
Equine Veterinary Journal 46 (2014) 103112 2013 EVJ Ltd
Insulin dysregulation
N. Frank and E. M. Tadros
diagnostic test for PPID because ponies were over-represented.
Hyperinsulinaemia occurs independently of PPID in ponies [115] and
is detected at all ages [2,9]. If PPID is an exacerbating factor for
hyperinsulinaemia, even as pituitary dysfunction is rst developing, then
early diagnosis of this endocrine disorder is essential. Detection of higher
insulin concentrations at noon, rather than 08.00 h, in horses with PPID fed
hay and chaff the morning of testing also suggests that postprandial
hyperinsulinaemia is exacerbated by PPID [115], and this could increase
the risk of hyperinsulinaemia-induced laminitis.
Systemic inammation and the stress response
to illness
Insulin resistance can develop as a result of mediators released during the
systemic inammatory response (Fig 2). A number of the inammatory
mediators upregulated by nuclear factor B signalling, as well as the
counter-regulatory hormones cortisol, epinephrine, glucagon and growth
hormone, can induce IR [117118]. Transient IR has been induced in
healthy horses by administering lipopolysaccharide i.v., and this is
presumed to occur through increased production of proinammatory
cytokines [119,120]. Cross-talk between the insulin signalling cascade and
inammatory signalling cascades occurs on many levels, and IR results
from inappropriate serine phosphorylation of insulin receptor substrates
and the insulin receptor itself [121]. Cortisol downregulates the expression
of proteins involved in the phosphoinositide 3-kinase signalling cascade
[122,123], including the p85 regulatory subunit [124]. Glucocorticoids also
reduce cellular insulin receptor substrate-1 concentrations in adipocytes
[122,123] and inhibit translocation of glucose transporter 4 to the plasma
membrane [125].
The overall goal of these counter-regulatory mechanisms is to ensure
the provision of adequate energy in the form of carbohydrates, proteins
and lipids to meet the bodys requirements while responding to infection
[126]. Inducing a state of peripheral and hepatic IR tips the balance in
favour of glucose liberation from tissue stores and glucose synthesis via
gluconeogenesis in the liver [127]. However, stress-associated inhibition of
insulin secretion by catecholamines and relative hypoinsulinaemia might
also exacerbate hypertriglyceridaemia in hospitalised horses [128].
Hyperadrenocorticism increases lipolysis and ketogenesis in horses [129],
although exogenous corticosteroid administration did not exacerbate
hypertriglyceridaemia in one study of ponies [130]. Although the
effects of catecholamines on fat metabolism have not been extensively
studied in equids, in other species plasma triglyceride concentrations
increase in response to administration or endogenous release of
catecholamines [131,132].
Alterations in insulin metabolism in the foal
The endocrine system of the foal undergoes many adaptations in the
perinatal period and this subject was recently reviewed by Fowden et al.
[133]. Insulin sensitivity decreases in foals during the rst 24 h of life and
this is attributed to increased circulating cortisol and catecholamine
concentrations. Clearance of exogenous glucose is slower during the rst
1224 h after birth, despite appropriate insulin responses [134]. This may
be part of the adaptation to intermittent nursing, rather than continuous
delivery of glucose via the placenta. Relative hypoinsulinaemia may be
observed in normal foals during the immediate post partum period, and
glucose-stimulated insulin secretion from pancreatic cells is signicantly
lower in healthy foals 2 h after birth, compared to one week of age
[135,136]. It has been suggested that perinatal alterations in the
abundance of insulin receptors and intracellular signalling proteins affect
insulin sensitivity in foals, as has been noted in other species [133].
Survival of premature and dysmature foals is inuenced by the degree of
maturity of several key endocrine systems [133,137]. In particular,
immaturity of the hypothalamic-pituitary-adrenal axis is associated with
impaired stress responses and increased mortality in the face of sepsis
[138140]. Hypoglycaemia and hyperglycaemia can both occur in critically
ill foals [141,142], as in human neonates [143,144]. Premature human
infants and those born small for gestational age because of impaired
placental function are at risk for neonatal hyperglycaemia [144]. Both
Equine Veterinary Journal 46 (2014) 103112 2013 EVJ Ltd
peripheral and hepatic IR are demonstrated in preterm human
infants [143,145], and IR can be further exacerbated by sepsis and other
inammatory conditions [144,146]. Relative hypoinsulinaemia also
contributes to the development of hyperglycaemia because pancreatic
cells are immature in premature infants and fail to efciently process
proinsulin to biologically active insulin [145]. As in humans, normal
physiological processes, including transient reduction in insulin sensitivity
within 24 h of birth and relative insulin deciency caused by inefcient
cell secretory function, render neonatal foals susceptible to
hyperglycaemia and other metabolic derangements in the face of
prematurity or critical illness.
Insulin concentrations are low after birth in premature foals delivered via
induced parturition before 320 days, and pancreatic cell responses to
exogenous glucose at age 2 h are also blunted in comparison to full-term
foals [135]. These ndings are attributed to the inhibitory effects of
increased catecholamine concentrations in premature foals. In contrast,
increased cell responsiveness to exogenous glucose, without an
accompanying change in glucose clearance, has been observed in foals
born 2448 h premature after induced parturition [147]. It is assumed that
pancreatic compensation is occurring in response to decreased peripheral
insulin sensitivity as a result of hypercortisolaemia. Studies examining
insulin sensitivity in healthy, full-term human infants born small for
gestational age have yielded mixed results, with both increased and
decreased insulin sensitivity documented over the rst 23 days of life
[148,149]. Relative insulin deciency resulting from reduced pancreatic
cell mass has also been suggested as a contributing factor to
hyperglycaemia [144], which is associated with increased morbidity and
mortality in human neonates [150,151].
Sepsis is a leading cause of death in neonatal foals [152156]. Septic
foals have lower glucose and insulin concentrations and higher triglyceride
and glucagon concentrations than healthy foals, and higher insulin and
lower leptin concentrations are associated with mortality [142].
Hyperglycaemia is associated with increased mortality in critically ill
foals [138,141] and is likely to result from increased production of
inammatory cytokines and stress hormones [116,157]. Sepsis-associated
hyperglycaemia develops as stress hormones such as epinephrine
and cortisol induce gluconeogenesis and IR, and toxins including
lipopolysaccharide bind to Toll-like receptor 4 and impair insulin signalling.
Although some septic foals experience relative adrenal insufciency,
circulating concentrations of cortisol and other stress hormones such
as catecholamines can still be markedly increased and contribute to
IR [138,139].
Pregnancy
In addition to pathological causes of IR, such as obesity, systemic
inammation, hyperadrenocorticism and acromegaly, there are
physiological causes such as pregnancy and stress. Pregnancy is
associated with IR in people and horses (Fig 2), and represents a normal
physiological adaptation [158]. In women, insulin action is 5070% lower
than normal during late pregnancy, and both basal and 24 h mean insulin
concentrations show a 2-fold increase [158]. Postprandial glucose
concentration, basal endogenous hepatic glucose production and total
gluconeogenesis are also increased during late pregnancy. These
alterations are attributed to rising concentrations of prolactin, cortisol and
glucagon, and ensure continuous delivery of nutrients to the growing fetus
[158]. Hyperinsulinaemia, enhanced cell sensitivity to endogenous and
exogenous glucose, increased degradation of insulin, and decreased
insulin sensitivity have all been demonstrated in pregnant mares [159].
George et al. [160] also used the frequently sampled i.v. glucose tolerance
test (FSIGTT) and minimal model analysis to demonstrate that pregnant
Thoroughbred mares had slower glucose clearance and greater insulin
secretion at 28 weeks of gestation than nonpregnant mares. These mares
developed higher glucose and insulin concentrations after meals,
consistent with lower insulin sensitivity and increased insulin secretion.
Assessment of insulin sensitivity
Tissue insulin sensitivity is most accurately assessed by performing
dynamic tests such as the hyperinsulinaemic-euglycaemic clamp (HEC)
107
Insulin dysregulation
procedure and FSIGTT with minimal model analysis [161]. The HEC
procedure involves i.v. infusion of soluble (regular) insulin and concurrent
infusion of dextrose solution to maintain glucose concentrations at the
preinfusion euglycaemic level. Because blood glucose concentrations are
held constant during the insulin infusion, the glucose infusion rate
represents insulin sensitivity in muscle and adipose tissues. Vick et al. [13]
evaluated a population of 60 mixed light horse breed mares on pasture
using this test and found that body condition scores were signicantly and
positively correlated with resting insulin concentrations (Spearmans rho =
0.53), and negatively correlated with insulin sensitivity (Spearmans rho =
-0.57) at the time of testing. To perform the FSIGTT procedure, an i.v. bolus
of dextrose is administered rst, followed several minutes later by an i.v.
insulin bolus. While these tests provide the most information about
glucose and insulin metabolism, the time and equipment required to
perform them largely restrict their utility to the research setting.
An insulin tolerance test (ITT) can also be used to measure tissue insulin
sensitivity, and this procedure involves i.v. injection of soluble insulin as a
bolus in amounts ranging from 20 to 125 iu/kg bwt, followed by serial
blood sampling over a 3 h period [86]. Area under the glucose curve is
calculated, or the dose of insulin required to cause a 50% decline in glucose
concentration can be recorded. The ITT has been simplied to a 2-step
insulin-response test consisting of an i.v. insulin injection of 100 iu/kg bwt
soluble insulin followed by blood glucose determination at 0 and 30 min
after injection [162]. Insulin-resistant horses fail to undergo a 50% reduction
in blood glucose concentration within 30 min. When 6 insulin-resistant
horses were compared with 6 controls, the 2-step ITT performed as well as
the conventional test that required 10 blood samples, and is therefore
practical to use in the clinical setting.
A CGIT can also be performed to assess insulin sensitivity, and involves
i.v. infusion of dextrose solution, followed immediately by soluble insulin
[10,163]. Blood glucose concentrations initially increase and then decrease
in response to exogenous (and endogenous) insulin. The time required for
blood glucose concentrations to return to baseline is recorded and the
insulin concentration is measured in blood collected at 45 min. The rate of
decrease in glucose concentrations caused by exogenous insulin reects
tissue insulin sensitivity, whereas the insulin concentration at 45 min is
affected by insulin clearance rate and pancreatic insulin output. Insulin
resistance is diagnosed when the blood glucose concentration fails to
return to baseline by 45 min. However, IR may also be present if normal
glucose results are accompanied by an increased (>100 iu/ml) insulin
concentration at 45 min. In these cases, compensated IR or cell
hyperplasia are suspected, with compensatory increases in insulin
secretion remaining sufcient to maintain normal glucose homeostasis.
Uncompensated IR, in contrast, results in higher glucose concentrations
after dextrose infusion with lower peak insulin concentrations.
Care must be taken when interpreting results of earlier studies that
assessed insulin sensitivity on the basis of resting insulin concentrations.
Factors such as stress or duration of fasting can affect resting insulin
concentrations and introduce variability. Since proxy measures of insulin
sensitivity, including the reciprocal of the square root of insulin (RISQI), are
calculated using resting insulin concentrations [8], hyperinsulinaemia
caused by factors other than IR could also affect these results. The same
concern can be raised with acute insulin response to glucose values
calculated from FSIGTT results [11], because enhanced insulin secretion
caused by increased cell function or hyperplasia might also raise acute
insulin response to glucose values. Proxy measures of insulin sensitivity
remain useful screening tests for detecting insulin dysregulation in larger
populations, but dynamic tests involving the administration of exogenous
insulin are preferred for the diagnosis of IR. Further studies are required to
determine the degree of agreement among FSIGTT, HEC, CGIT and ITT
results in the same horses.
Management of hyperinsulinaemia and
insulin resistance
Potential exacerbating factors for hyperinsulinaemia, including obesity,
high-sugar diets, inadequate exercise and concurrent PPID, must be
considered before establishing a management plan. If obesity is present,
the initial focus of management should be weight loss, and when PPID is
108
N. Frank and E. M. Tadros
diagnosed, pergolide should be prescribed. A complete diet history should
be collected and assessed, and the diet adjusted to reduce the amount of
sugars available if hyperinsulinaemia is a concern. Horses should be
regularly exercised, as this is an integral part of weight management plans
when obesity is a factor.
Body fat mass can be reduced in obese horses and ponies by lowering
energy intake and increasing exercise [164]. Some horses with EMS are
being overfed by their owners, and removal of grain from the diet is
sufcient to induce weight loss. Other obese horses and ponies are
resistant to weight loss and require greater reductions in energy intake
[165]. Pasture access should be restricted in obese animals because
obesity often persists until grass intake is limited, and sugars and amino
acids contained in pasture grass contribute to hyperinsulinaemia.
Recommended strategies for limiting grass consumption include placing
the obese horse and a companion in a small grass paddock that is
0.130.2 ha in size (one-third to one half an acre), or the application of a
grazing muzzle during turnout. Responses to management should then be
reassessed and housing conditions adjusted over time. If removing grain
from the diet and limiting pasture access does not result in weight loss, the
amount of hay fed should be progressively reduced. Hay should initially be
fed in amounts equivalent to 1.5% of current bodyweight and then lowered
to 1.5% of ideal bodyweight. An obese horse or pony that is not losing body
mass after 4 weeks on this diet can be reduced to 1.25%, and then down to
the minimum level of 1.0% bodyweight after another month if there has
been no progress. A balanced vitamin/mineral supplement or ration
balancer should be provided to horses on a hay-only diet to maintain
adequate micronutrient and protein intake.
Attention must also be paid to the sugar content of the diet, and the
importance of this component of the management plan depends on the
severity of hyperinsulinaemia. Hay containing large amounts of simple
sugars and hydrolysable starches is a signicant concern for severely
affected horses. Analysis of the hay is recommended for these animals to
ensure that the nonstructural carbohydrate content of the forage is <10%
on a dry-matter basis [1]. Hay can also be soaked in cold water for one
hour to lower the nonstructural carbohydrate content, although results
vary according to the type of hay used [166]. A supplement containing
additional protein, vitamins and minerals should also be provided.
Hyperinsulinaemic horses with normal body mass are more challenging to
manage. The rst question to be addressed is whether the animal is
concurrently affected by PPID, so horses older than 10 years should
undergo testing for both PPID and IR [112,167]. Previously obese horses
that remain hyperinsulinaemic after weight loss must also be managed
carefully. If weight gain is required, feeds providing more energy
in the form of fat and bre should be selected.
Two medical treatments are also used to manage horses with EMS and
both have specic indications.
Levothyroxine sodium can be administered to accelerate weight loss
when severe insulin dysregulation is present in an obese horse that cannot
be exercised because of laminitis, or when obesity persists despite
intensive diet and exercise management. Levothyroxine sodium lowers
bodyweight and improves insulin sensitivity in horses [168], and can be
administered by mouth or in the feed at a dosage of 0.1 mg/kg bwt once
daily. A higher dosage of 0.15 mg/kg bwt can be selected if obesity persists
after 3 months of treatment. Levothyroxine is administered until the horse
reaches an ideal body condition score or until the end of a 6-month period.
When treatment is discontinued, the dosage is lowered to 0.05 mg/kg
bwt/day for 2 weeks and then 0.025 mg/kg bwt/day for 2 weeks.
Complications have not been associated with the administration of
levothyroxine to healthy horses for 12 months [168], although some horses
exhibit increased activity and mild hyperexcitability when treated. Pasture
access must be restricted when horses are treated with levothyroxine to
prevent the horse from increasing its own feed intake. Levothyroxine is
reasonably priced in the USA, but expensive in the UK.
Metformin hydrochloride is commonly administered to treat diabetes
mellitus in man and has also been reported to improve resting insulin
concentrations and proxy measures of insulin sensitivity in horses and
ponies [169]. However, studies evaluating metformin use in equids have
yielded conicting results, and insulin sensitivity did not improve in
nonobese insulin-resistant ponies when i.v. glucose tolerance tests were
performed to assess glucose and insulin dynamics [170]. This discrepancy
Equine Veterinary Journal 46 (2014) 103112 2013 EVJ Ltd
N. Frank and E. M. Tadros
can be explained by the low oral bioavailability of metformin in horses [171]
and recent results indicating that metformin acts at the level of the
intestine to blunt blood glucose and insulin concentrations after feeding
[172]. Metformin therefore appears to be better suited to controlling
postprandial hyperinsulinaemia than to treating IR in horses. The current
recommendation for metformin is 30 mg/kg bwt per os q. 812 h, given
one hour before feeding or turnout.
Future directions
Looking forward, our understanding of insulin dysregulation in mature
horses will be further enhanced when results of studies examining the
genetic basis of EMS are completed and incretin biology is further
investigated in the horse. Insulin dysregulation in foals also requires
additional research so that glucose concentrations can be better managed
in premature foals and those with systemic illness. Relationships between
EMS and PPID also require further study, and evidence must be gathered to
establish links between insulin dysregulation and the development of
pituitary disease.
Authors declaration of interests
Dr Frank consults for Boehringer Ingelheim on research study design.
Source of funding
Dr Frank has received research funding in the past from Boehringer
Ingelheim Vetmedica.
Authorship
Manuscript prepared by Dr Frank with sections contributed by Dr Tadros.
References
1. Frank, N., Geor, R.J., Bailey, S.R., Durham, A.E. and Johnson, P.J. (2010) Equine
metabolic syndrome. J. Vet. Intern. Med. 24, 467-475.
2. Carter, R.A., Treiber, K.H., Geor, R.J., Douglass, L. and Harris, P.A. (2009)
Prediction of incipient pasture-associated laminitis from hyperinsulinaemia,
hyperleptinaemia and generalised and localised obesity in a cohort of ponies.
Equine Vet. J. 41, 171-178.
3. Asplin, K.E., Sillence, M.N., Pollitt, C.C. and McGowan, C.M. (2007) Induction
of laminitis by prolonged hyperinsulinaemia in clinically normal ponies. Vet. J.
174, 530-535.
4. de Laat, M.A., McGowan, C.M., Sillence, M.N. and Pollitt, C.C. (2010) Equine
laminitis: induced by 48 h hyperinsulinaemia in Standardbred horses. Equine
Vet. J. 42, 129-135.
5. Kronfeld, D.S., Hess, T.M., Byrd, B.M. and Splan, R.K. (2005) (abstract)
Pre-laminitic metabolic syndrome in genetically predisposed ponies involves
compensated insulin resistance. J. Anim. Physiol. Anim. Nutr. (Berl.) 89,
430-431.
6. Hoffman, R.M., Kronfeld, D.S., Cooper, W.L. and Harris, P.A. (2003) Glucose
clearance in grazing mares is affected by diet, pregnancy, and lactation.
J. Anim. Sci. 81, 1764-1771.
7. Suagee, J.K., Corl, B.A., Crisman, M.V., Pleasant, R.S., Thatcher, C.D. and
Geor, R.J. (2013) Relationships between body condition score and plasma
inammatory cytokines, insulin, and lipids in a mixed population of
light-breed horses. J. Vet. Intern. Med. 27, 157-163.
8. Treiber, K.H., Kronfeld, D.S., Hess, T.M., Boston, R.C. and Harris, P.A. (2005)
Use of proxies and reference quintiles obtained from minimal model analysis
for determination of insulin sensitivity and pancreatic beta-cell
responsiveness in horses. Am. J. Vet. Res. 66, 2114-2121.
9. Treiber, K.H., Kronfeld, D.S., Hess, T.M., Byrd, B.M., Splan, R.K. and Staniar,
W.B. (2006) Evaluation of genetic and metabolic predispositions and
nutritional risk factors for pasture-associated laminitis in ponies. J. Am. Vet.
Med. Ass. 228, 1538-1545.
Equine Veterinary Journal 46 (2014) 103112 2013 EVJ Ltd
Insulin dysregulation
10. Frank, N., Elliott, S.B., Brandt, L.E. and Keisler, D.H. (2006) Physical
characteristics, blood hormone concentrations, and plasma lipid
concentrations in obese horses with insulin resistance. J. Am. Vet. Med. Ass.
228, 1383-1390.
11. Carter, R.A., McCutcheon, L.J., George, L.A., Smith, T.L., Frank, N. and Geor,
R.J. (2009) Effects of diet-induced weight gain on insulin sensitivity and
plasma hormone and lipid concentrations in horses. Am. J. Vet. Res. 70,
1250-1258.
12. Carter, R.A., McCutcheon, L.J., Valle, E., Meilahn, E.N. and Geor, R.J. (2010)
Effects of exercise training on adiposity, insulin sensitivity, and plasma
hormone and lipid concentrations in overweight or obese, insulin-resistant
horses. Am. J. Vet. Res. 71, 314-321.
13. Vick, M.M., Adams, A.A., Murphy, B.A., Sessions, D.R., Horohov, D.W., Cook,
R.F., Shelton, B.J. and Fitzgerald, B.P. (2007) Relationships among
inammatory cytokines, obesity, and insulin sensitivity in the horse. J. Anim.
Sci. 85, 1144-1155.
14. Shanik, M.H., Xu, Y., Skrha, J., Dankner, R., Zick, Y. and Roth, J. (2008) Insulin
resistance and hyperinsulinemia: is hyperinsulinemia the cart or the horse?
Diabetes Care 31, Suppl. 2, S262-S268.
15. Mudaliar, S. and Henry, R.R. (2010) Effects of incretin hormones on beta-cell
mass and function, body weight, and hepatic and myocardial function. Am. J.
Med. 123, S19-S27.
16. Goutal, C.M., Brugmann, B.L. and Ryan, K.A. (2012) Insulinoma in dogs: a
review. J. Am. Anim. Hosp. Ass. 48, 151-163.
17. Chen, S. (2010) Advanced diagnostic approaches and current medical
management of insulinomas and adrenocortical disease in ferrets (Mustela
putorius furo). Vet. Clin. North Am. Exot. Anim. Pract. 13, 439-452.
18. Ross, M.W., Lowe, J.E., Cooper, B.J., Reimers, T.J. and Froscher, B.A. (1983)
Hypoglycemic seizures in a Shetland pony. Cornell Vet. 73, 151-169.
19. Hintz, H.F., Schryver, H.F. and Stevens, C.E. (1978) Digestion and absorption in
the hindgut of nonruminant herbivores. J. Anim. Sci. 46, 1803-1807.
20. Frank, N. (2012) Oral sugar test to diagnose insulin resistance in horses. Proc.
Am. Ass Equine Practnrs. 58, 576.
21. Borer, K.E., Bailey, S.R., Menzies-Gow, N.J., Harris, P.A. and Elliott, J. (2012)
Effect of feeding glucose, fructose, and inulin on blood glucose and insulin
concentrations in normal ponies and those predisposed to laminitis. J. Anim.
Sci. 90, 3003-3011.
22. Toth, F., Frank, N., Martin-Jimenez, T., Elliott, S.B., Geor, R.J. and Boston, R.C.
(2010) Measurement of C-peptide concentrations and responses to
somatostatin, glucose infusion, and insulin resistance in horses. Equine Vet. J.
42, 149-155.
23. Duhlmeier, R., Deegen, E., Fuhrmann, H., Widdel, A. and Sallmann, H.P. (2001)
Glucose-dependent insulinotropic polypeptide (GIP) and the enteroinsular
axis in equines (Equus caballus). Comp. Biochem. Physiol. A Mol. Integr.
Physiol. 129, 563-575.
24. Chameroy, K., Frank, N., Elliott, S.B. and Schuver, A. (2011) Effects of weight
gain on active glucagon-like peptide-1 concentrations in horses with histories
of obesity and insulin resistance. J. Vet. Intern. Med. 25, 766 (abstract).
25. Drucker, D.J. (2003) Glucagon-like peptides: regulators of cell proliferation,
differentiation, and apoptosis. Mol. Endocrinol. 17, 161-171.
26. Yamaoka-Tojo, M., Tojo, T., Takahira, N., Matsunaga, A., Aoyama, N.,
Masuda, T. and Izumi, T. (2010) Elevated circulating levels of an incretin
hormone, glucagon-like peptide-1, are associated with metabolic
components in high-risk patients with cardiovascular disease. Cardiovasc.
Diabetol. 9, 17-25.
27. Ning, J., Hong, T., Yang, X., Mei, S., Liu, Z., Liu, H.Y. and Cao, W. (2011) Insulin
and insulin signaling play a critical role in fat induction of insulin resistance in
mouse. Am. J. Physiol. Endocrinol. Metab. 301, E391-E401.
28. Johnson, P.J. (2002) The equine metabolic syndrome peripheral Cushings
syndrome. Vet. Clin. North Am. Equine Pract. 18, 271-293.
29. Mehran, A.E., Templeman, N.M., Brigidi, G.S., Lim, G.E., Chu, K.Y., Hu, X.,
Botezelli, J.D., Asadi, A., Hoffman, B.G., Kieffer, T.J., Bamji, S.X., Clee, S.M. and
Johnson, J.D. (2012) Hyperinsulinemia drives diet-induced obesity
independently of brain insulin production. Cell Metab. 16, 723-737.
30. Andreazzi, A.E., Grassiolli, S., Marangon, P.B., Martins, A.G., de Oliveira, J.C.,
Torrezan, R., Gravena, C., Garcia, R.M. and Mathias, P.C. (2011) Impaired
sympathoadrenal axis function contributes to enhanced insulin secretion in
prediabetic obese rats. Exp. Diabetes Res. 2011, 947917-947925.
31. Navas de Solis, C. and Foreman, J.H. (2010) Transient diabetes mellitus in a
neonatal Thoroughbred foal. J. Vet. Emerg. Crit. Care 20, 611-615.
32. Jeffrey, J.R. (1968) Diabetes mellitus secondary to chronic pancreatitis in a
pony. J. Am. Vet. Med. Ass. 153, 1168-1175.
109
Insulin dysregulation
33. Durham, A.E., Hughes, K.J., Cottle, H.J., Rendle, D.I. and Boston, R.C. (2009)
Type 2 diabetes mellitus with pancreatic beta cell dysfunction in 3 horses
conrmed with minimal model analysis. Equine Vet. J. 41, 924-929.
34. Staempi, H.R., Eigenmann, E.J. and Clarke, L.M. (1988) Insulin treatment and
development of anti-insulin antibodies in a horse with diabetes mellitus
associated with a functional pituitary adenoma. Can. Vet. J. 29, 934-936.
35. McCoy, D.J. (1986) Diabetes mellitus associated with bilateral granulosa cell
tumors in a mare. J. Am. Vet. Med. Ass. 188, 733-735.
36. Giri, J.K., Magdesian, K.G. and Gaffney, P.M. (2011) Insulin-dependent
diabetes mellitus associated with presumed autoimmune polyendocrine
syndrome in a mare. Can. Vet. J. 52, 506-512.
37. Knowles, E.J., Withers, J.M. and Mair, T.S. (2012) Increased plasma
fructosamine concentrations in laminitic horses. Equine Vet. J. 44, 226-229.
38. Waller, A.P., Burns, T.A., Mudge, M.C., Belknap, J.K. and Lacombe, V.A. (2011)
Insulin resistance selectively alters cell-surface glucose transporters but not
their total protein expression in equine skeletal muscle. J. Vet. Intern. Med.
25, 315-321.
39. Waller, A.P., Kohler, K., Burns, T.A., Mudge, M.C., Belknap, J.K. and Lacombe,
V.A. (2011) Naturally occurring compensated insulin resistance selectively
alters glucose transporters in visceral and subcutaneous adipose tissues
without change in AS160 activation. Biochim. Biophys. Acta 1812,
1098-1103.
40. Zhang, H., Dellsperger, K.C. and Zhang, C. (2012) The link between metabolic
abnormalities and endothelial dysfunction in type 2 diabetes: an update.
Basic Res. Cardiol. 107, 237-248.
41. de Laat, M.A., Sillence, M.N., McGowan, C.M. and Pollitt, C.C. (2012)
Continuous intravenous infusion of glucose induces endogenous
hyperinsulinaemia and lamellar histopathology in Standardbred horses.
Vet. J. 191, 317-322.
42. de Laat, M.A., Kyaw-Tanner, M.T., Sillence, M.N., McGowan, C.M. and Pollitt,
C.C. (2012) Advanced glycation endproducts in horses with insulin-induced
laminitis. Vet. Immunol. Immunopathol. 145, 395-401.
43. Shoelson, S.E., Herrero, L. and Naaz, A. (2007) Obesity, inammation, and
insulin resistance. Gastroenterology 132, 2169-2180.
44. Antuna-Puente, B., Feve, B., Fellahi, S. and Bastard, J.P. (2008) Adipokines: the
missing link between insulin resistance and obesity. Diabetes Metab. 34,
2-11.
45. Carter, R.A., Geor, R.J., Burton Staniar, W., Cubitt, T.A. and Harris, P.A. (2009)
Apparent adiposity assessed by standardised scoring systems and
morphometric measurements in horses and ponies. Vet. J. 179, 204-210.
46. Radin, M.J., Sharkey, L.C. and Holycross, B.J. (2009) Adipokines: a review of
biological and analytical principles and an update in dogs, cats, and horses.
Vet. Clin. Pathol. 38, 136-156.
47. Goossens, G.H. (2008) The role of adipose tissue dysfunction in the
pathogenesis of obesity-related insulin resistance. Physiol. Behav. 94,
206-218.
48. Trayhurn, P., Wang, B. and Wood, I.S. (2008) Hypoxia in adipose tissue:
a basis for the dysregulation of tissue function in obesity? Br. J. Nutr. 100,
227-235.
49. Serne, E.H., de Jongh, R.T., Eringa, E.C. and Ijzerman , R.G., and Stehouwer,
C.D.(2007) Microvascular dysfunction: a potential pathophysiological role in
the metabolic syndrome. Hypertension 50, 204-211.
50. Strissel, K.J., Stancheva, Z., Miyoshi, H., Pereld, J.W., 2nd, DeFuria, J., Jick, Z.,
Greenberg, A.S. and Obin, M.S. (2007) Adipocyte death, adipose tissue
remodeling, and obesity complications. Diabetes 56, 2910-2918.
51. Cinti, S., Mitchell, G., Barbatelli, G., Murano, I., Ceresi, E., Faloia, E., Wang, S.,
Fortier, M., Greenberg, A.S. and Obin, M.S. (2005) Adipocyte death denes
macrophage localization and function in adipose tissue of obese mice and
humans. J. Lipid Res. 46, 2347-2355.
52. Murano, I., Barbatelli, G., Parisani, V., Latini, C., Muzzonigro, G., Castellucci,
M. and Cinti, S. (2008) Dead adipocytes, detected as crown-like structures,
are prevalent in visceral fat depots of genetically obese mice. J. Lipid Res. 49,
1562-1568.
53. Stienstra, R., Duval, C., Keshtkar, S., van der Laak, J., Kersten, S. and Muller,
M. (2008) Peroxisome proliferator-activated receptor gamma activation
promotes inltration of alternatively activated macrophages into adipose
tissue. J. Biol. Chem. 283, 22620-22627.
54. Lumeng, C.N., Bodzin, J.L. and Saltiel, A.R. (2007) Obesity induces a
phenotypic switch in adipose tissue macrophage polarization. J. Clin. Invest.
117, 175-184.
55. Yu, Y.H. and Ginsberg, H.N. (2005) Adipocyte signaling and lipid homeostasis:
sequelae of insulin-resistant adipose tissue. Circ. Res. 96, 1042-1052.
110
N. Frank and E. M. Tadros
56. Carpentier, A.C. (2008) Postprandial fatty acid metabolism in the
development of lipotoxicity and type 2 diabetes. Diabetes Metab. 34, 97107.
57. van Herpen, N.A. and Schrauwen-Hinderling, V.B. (2008) Lipid accumulation
in non-adipose tissue and lipotoxicity. Physiol. Behav. 94, 231-241.
58. Kusminski, C.M., Shetty, S., Orci, L., Unger, R.H. and Scherer, P.E. (2009)
Diabetes and apoptosis: lipotoxicity. Apoptosis 14, 1484-1495.
59. Schenk, S., Saberi, M. and Olefsky, J.M. (2008) Insulin sensitivity: modulation
by nutrients and inammation. J. Clin. Invest. 118, 2992-3002.
60. Martin, M.U. and Wesche, H. (2002) Summary and comparison of the
signaling mechanisms of the Toll/interleukin-1 receptor family. Biochim.
Biophys. Acta 1592, 265-280.
61. Hotamisligil, G.S. (2006) Inammation and metabolic disorders. Nature 444,
860-867.
62. Muniyappa, R., Iantorno, M. and Quon, M.J. (2008) An integrated view of
insulin resistance and endothelial dysfunction. Endocrinol. Metab. Clin. North
Am. 37, 685-711; ix-x.
63. Kim, J.A., Montagnani, M., Koh, K.K. and Quon, M.J. (2006) Reciprocal
relationships between insulin resistance and endothelial dysfunction:
molecular and pathophysiological mechanisms. Circulation 113, 18881904.
64. Fantuzzi, G. (2005) Adipose tissue, adipokines, and inammation. J. Allergy
Clin. Immunol. 115, 911-919; quiz 920.
65. Suagee, J.K., Corl, B.A., Crisman, M.V., Hulver, M.W., McCutcheon, L.J. and
Geor, R.J. (2011) Effects of acute hyperinsulinemia on inammatory proteins
in horses. Vet. Immunol. Immunopathol. 142, 141-146.
66. Holbrook, T.C., Tipton, T. and McFarlane, D. (2012) Neutrophil and cytokine
dysregulation in hyperinsulinemic obese horses. Vet. Immunol.
Immunopathol. 145, 283-289.
67. Burns, T.A., Geor, R.J., Mudge, M.C., McCutcheon, L.J., Hinchcliff, K.W. and
Belknap, J.K. (2010) Proinammatory cytokine and chemokine gene
expression proles in subcutaneous and visceral adipose tissue depots of
insulin-resistant and insulin-sensitive light breed horses. J. Vet. Intern. Med.
24, 932-939.
68. Tarantino, G., Saldalamacchia, G., Conca, P. and Arena, A. (2007)
Non-alcoholic fatty liver disease: further expression of the metabolic
syndrome. J. Gastroenterol. Hepatol. 22, 293-303.
69. Tarantino, G., Savastano, S. and Colao, A. (2010) Hepatic steatosis, low-grade
chronic inammation and hormone/growth factor/adipokine imbalance.
World J. Gastroenterol. 16, 4773-4783.
70. Perlemuter, G., Bigorgne, A., Cassard-Doulcier, A.M. and Naveau, S. (2007)
Nonalcoholic fatty liver disease: from pathogenesis to patient care. Nat. Clin.
Pract. Endocrinol. Metab. 3, 458-469.
71. Postic, C. and Girard, J. (2008) Contribution of de novo fatty acid synthesis to
hepatic steatosis and insulin resistance: lessons from genetically engineered
mice. J. Clin. Invest. 118, 829-838.
72. Neuschwander-Tetri, B.A. (2010) Hepatic lipotoxicity and the pathogenesis of
nonalcoholic steatohepatitis: the central role of nontriglyceride fatty acid
metabolites. Hepatology 52, 774-788.
73. Cai, D., Yuan, M., Frantz, D.F., Melendez, P.A., Hansen, L., Lee, J. and
Shoelson, S.E. (2005) Local and systemic insulin resistance resulting from
hepatic activation of IKK-beta and NF-kappaB. Nat. Med. 11, 183-190.
74. Item, F. and Konrad, D. (2012) Visceral fat and metabolic inammation: the
portal theory revisited. Obes. Rev. 13, Suppl. 2, 30-39.
75. Sparks, J.D., Sparks, C.E. and Adeli, K. (2012) Selective hepatic insulin
resistance, VLDL overproduction, and hypertriglyceridemia. Arterioscler.
Thromb. Vasc. Biol. 32, 2104-2112.
76. Valenti, L., Dongiovanni, P. and Fargion, S. (2012) Diagnostic and therapeutic
implications of the association between ferritin level and severity of
nonalcoholic fatty liver disease. World J. Gastroenterol. 18, 3782-3786.
77. Nielsen, B.D., Vick, M.M. and Dennis, P.M. (2012) A potential link between
insulin resistance and iron overload disorder in browsing rhinoceroses
investigated through the use of an equine model. J. Zoo Wildl. Med. 43,
S61-S65.
78. Buff, P.R., Dodds, A.C., Morrison, C.D., Whitley, N.C., McFadin, E.L., Daniel,
J.A., Djiane, J. and Keisler, D.H. (2002) Leptin in horses: tissue localization and
relationship between peripheral concentrations of leptin and body condition.
J. Anim. Sci. 80, 2942-2948.
79. Gentry, L.R., Thompson, D.L., Jr, Gentry, G.T., Jr, Davis, K.A., Godke, R.A. and
Cartmill, J.A. (2002) The relationship between body condition, leptin, and
reproductive and hormonal characteristics of mares during the seasonal
anovulatory period. J. Anim. Sci. 80, 2695-2703.
Equine Veterinary Journal 46 (2014) 103112 2013 EVJ Ltd
N. Frank and E. M. Tadros
80. Kearns, C.F., McKeever, K.H., Roegner, V., Brady, S.M. and Malinowski, K.
(2006) Adiponectin and leptin are related to fat mass in horses. Vet. J. 172,
460-465.
81. Meier, U. and Gressner, A.M. (2004) Endocrine regulation of energy
metabolism: review of pathobiochemical and clinical chemical aspects of
leptin, ghrelin, adiponectin, and resistin. Clin. Chem. 50, 1511-1525.
82. Porte, D., Jr, Baskin, D.G. and Schwartz, M.W. (2002) Leptin and insulin action
in the central nervous system. Nutr. Rev. 60, S20-S29; discussion S68-84,
85-27.
83. Cohen, P., Miyazaki, M., Socci, N.D., Hagge-Greenberg, A., Liedtke, W.,
Soukas, A.A., Sharma, R., Hudgins, L.C., Ntambi, J.M. and Friedman, J.M.
(2002) Role for stearoyl-CoA desaturase-1 in leptin-mediated weight loss.
Science 297, 240-243.
84. Pandit, R., de Jong, J.W., Vanderschuren, L.J. and Adan, R.A. (2011)
Neurobiology of overeating and obesity: the role of melanocortins and
beyond. Eur. J. Pharmacol. 660, 28-42.
85. Diez, E., Lopez, I., Perez, C., Pineda, C. and Aguilera-Tejero, E. (2012) Plasma
leptin concentration in donkeys. Vet. Q. 32, 13-16.
86. Caltabilota, T.J., Earl, L.R., Thompson, D.L., Jr, Clavier, S.E. and Mitcham, P.B.
(2010) Hyperleptinemia in mares and geldings: assessment of insulin
sensitivity from glucose responses to insulin injection. J. Anim. Sci. 88,
2940-2949.
87. Shehzad, A., Iqbal, W., Shehzad, O. and Lee, Y.S. (2012) Adiponectin:
regulation of its production and its role in human diseases. Hormones
(Athens) 11, 8-20.
88. Maeda, N., Shimomura, I., Kishida, K., Nishizawa, H., Matsuda, M.,
Nagaretani, H., Furuyama, N., Kondo, H., Takahashi, M., Arita, Y., Komuro, R.,
Ouchi, N., Kihara, S., Tochino, Y., Okutomi, K., Horie, M., Takeda, S., Aoyama,
T., Funahashi, T. and Matsuzawa, Y. (2002) Diet-induced insulin resistance in
mice lacking adiponectin/ACRP30. Nat. Med. 8, 731-737.
89. Schraw, T., Wang, Z.V., Halberg, N., Hawkins, M. and Scherer, P.E. (2008)
Plasma adiponectin complexes have distinct biochemical characteristics.
Endocrinology 149, 2270-2282.
90. Wooldridge, A.A., Edwards, H.G., Plaisance, E.P., Applegate, R., Taylor, D.R.,
Taintor, J., Zhong, Q. and Judd, R.L. (2012) Evaluation of high-molecular
weight adiponectin in horses. Am. J. Vet. Res. 73, 1230-1240.
91. Goldstein, B.J. and Scalia, R. (2004) Adiponectin: a novel adipokine linking
adipocytes and vascular function. J. Clin. Endocrinol. Metab. 89, 2563-2568.
92. Knight, S.F. and Imig, J.D. (2007) Obesity, insulin resistance, and renal
function. Microcirculation 14, 349-362.
93. Sharma, V. and McNeill, J.H. (2005) The emerging roles of leptin and ghrelin in
cardiovascular physiology and pathophysiology. Curr. Vasc. Pharmacol. 3,
169-180.
94. Teoh, H., Quan, A., Bang, K.W., Wang, G., Lovren, F., Vu, V., Haitsma, J.J.,
Szmitko, P.E., Al-Omran, M., Wang, C.H., Gupta, M., Peterson, M.D., Zhang, H.,
Chan, L., Freedman, J., Sweeney, G. and Verma, S. (2008) Adiponectin
deciency promotes endothelial activation and profoundly exacerbates
sepsis-related mortality. Am. J. Physiol. Endocrinol. Metab. 295, E658-E664.
95. Ouchi, N., Ohishi, M., Kihara, S., Funahashi, T., Nakamura, T., Nagaretani, H.,
Kumada, M., Ohashi, K., Okamoto, Y., Nishizawa, H., Kishida, K., Maeda, N.,
Nagasawa, A., Kobayashi, H., Hiraoka, H., Komai, N., Kaibe, M., Rakugi, H.,
Ogihara, T. and Matsuzawa, Y. (2003) Association of hypoadiponectinemia
with impaired vasoreactivity. Hypertension 42, 231-234.
96. Ouedraogo, R., Gong, Y., Berzins, B., Wu, X., Mahadev, K., Hough, K., Chan, L.,
Goldstein, B.J. and Scalia, R. (2007) Adiponectin deciency increases
leukocyte-endothelium interactions via upregulation of endothelial cell
adhesion molecules in vivo. J. Clin. Invest. 117, 1718-1726.
97. Tilg, H. and Wolf, A.M. (2005) Adiponectin: a key fat-derived molecule
regulating inammation. Expert Opin. Ther. Targets 9, 245-251.
98. Korda, M., Kubant, R., Patton, S. and Malinski, T. (2008) Leptin-induced
endothelial dysfunction in obesity. Am. J. Physiol. Heart Circ. Physiol. 295,
H1514-H1521.
99. Singhal, A. (2005) Endothelial dysfunction: role in obesity-related disorders
and the early origins of CVD. Proc. Nutr. Soc. 64, 15-22.
100. McGowan, T.W., Pinchbeck, G.P. and McGowan, C.M. (2013) Prevalence, risk
factors and clinical signs predictive for equine pituitary pars intermedia
dysfunction in aged horses. Equine Vet. J. 45, 74-79.
101. Rafacho, A., Marroqui, L., Taboga, S.R., Abrantes, J.L., Silveira, L.R.,
Boschero, A.C., Carneiro, E.M., Bosqueiro, J.R., Nadal, A. and Quesada, I.
(2010) Glucocorticoids in vivo induce both insulin hypersecretion and
enhanced glucose sensitivity of stimulus-secretion coupling in isolated rat
islets. Endocrinology 151, 85-95.
Equine Veterinary Journal 46 (2014) 103112 2013 EVJ Ltd
Insulin dysregulation
102. Tiley, H.A., Geor, R.J. and McCutcheon, L.J. (2007) Effects of dexamethasone
on glucose dynamics and insulin sensitivity in healthy horses. Am. J. Vet. Res.
68, 753-759.
103. Toth, F., Frank, N., Geor, R.J. and Boston, R.C. (2010) Effects of pretreatment
with dexamethasone or levothyroxine sodium on endotoxin-induced
alterations in glucose and insulin dynamics in horses. Am. J. Vet. Res. 71,
60-68.
104. Peterson, M.E., Altszuler, N. and Nichols, C.E. (1984) Decreased
insulin sensitivity and glucose tolerance in spontaneous canine
hyperadrenocorticism. Res. Vet. Sci. 36, 177-182.
105. Montgomery, T.M., Nelson, R.W., Feldman, E.C., Robertson, K. and Polonsky,
K.S. (1996) Basal and glucagon-stimulated plasma C-peptide concentrations
in healthy dogs, dogs with diabetes mellitus, and dogs with
hyperadrenocorticism. J. Vet. Intern. Med. 10, 116-122.
106. Orth, D.N., Holscher, M.A., Wilson, M.G., Nicholson, W.E., Plue, R.E. and
Mount, C.D. (1982) Equine Cushings disease: plasma immunoreactive
proopiolipomelanocortin peptide and cortisol levels basally and in response
to diagnostic tests. Endocrinology 110, 1430-1441.
107. Wilson, M.G., Nicholson, W.E., Holscher, M.A., Sherrell, B.J., Mount, C.D. and
Orth, D.N. (1982) Proopiolipomelanocortin peptides in normal pituitary,
pituitary tumor, and plasma of normal and Cushings horses. Endocrinology
110, 941-954.
108. Marshall, J.B., Kapcala, L.P., Manning, L.D. and McCullough, A.J. (1984)
Effect of corticotropin-like intermediate lobe peptide on pancreatic
exocrine function in isolated rat pancreatic lobules. J. Clin. Invest. 74,
1886-1889.
109. McFarlane, D., Beech, J. and Cribb, A. (2006) Alpha-melanocyte stimulating
hormone release in response to thyrotropin releasing hormone in healthy
horses, horses with pituitary pars intermedia dysfunction and equine pars
intermedia explants. Domest. Anim. Endocrinol. 30, 276-288.
110. Obici, S., Feng, Z., Tan, J., Liu, L., Karkanias, G. and Rossetti, L. (2001) Central
melanocortin receptors regulate insulin action. J. Clin. Invest. 108,
1079-1085.
111. Schott, H.C., 2nd (2002) Pituitary pars intermedia dysfunction: equine
Cushings disease. Vet. Clin. North Am.: Equine Pract. 18, 237-270.
112. McFarlane, D. (2011) Equine pituitary pars intermedia dysfunction. Vet. Clin.
North Am.: Equine Pract. 27, 93-113.
113. van der Kolk, J.H., Wensing, T., Kalsbeek, H.C. and Breukink, H.J. (1995)
Laboratory diagnosis of equine pituitary pars intermedia adenoma. Domest.
Anim. Endocrinol. 12, 35-39.
114. Reeves, H.J., Lees, R. and McGowan, C.M. (2001) Measurement of basal
serum insulin concentration in the diagnosis of Cushings disease in ponies.
Vet. Rec. 149, 449-452.
115. McGowan, C.M., Frost, R., Pfeiffer, D.U. and Neiger, R. (2004) Serum insulin
concentrations in horses with equine Cushings syndrome: response to a
cortisol inhibitor and prognostic value. Equine Vet. J. 36, 295-298.
116. Marik, P.E. and Raghavan, M. (2004) Stress-hyperglycemia, insulin and
immunomodulation in sepsis. Intens. Care Med. 30, 748-756.
117. McCowen, K.C., Malhotra, A. and Bistrian, B.R. (2001) Stress-induced
hyperglycemia. Crit. Care Clin. 17, 107-124.
118. Knieriem, M., Otto, C.M. and Macintire, D. (2007) Hyperglycemia in critically ill
patients. Compend. Contin. Educ. Vet. 29, 360-362; 364-372; quiz 372.
119. Toth, F., Frank, N., Elliott, S.B., Geor, R.J. and Boston, R.C. (2008) Effects of an
intravenous endotoxin challenge on glucose and insulin dynamics in horses.
Am. J. Vet. Res. 69, 82-88.
120. Tadros, E.M. and Frank, N. (2012) Effects of continuous or intermittent
lipopolysaccharide administration for 48 hours on the systemic inammatory
response in horses. Am. J. Vet. Res. 73, 1394-1402.
121. Tanti, J.F. and Jager, J. (2009) Cellular mechanisms of insulin resistance: role of
stress-regulated serine kinases and insulin receptor substrates (IRS) serine
phosphorylation. Curr. Opin. Pharmacol. 9, 753-762.
122. Buren, J., Liu, H.X., Jensen, J. and Eriksson, J.W. (2002) Dexamethasone
impairs insulin signalling and glucose transport by depletion of insulin
receptor substrate-1, phosphatidylinositol 3-kinase and protein kinase B in
primary cultured rat adipocytes. Eur. J. Endocrinol. 146, 419-429.
123. Lundgren, M., Buren, J., Ruge, T., Myrnas, T. and Eriksson, J.W. (2004)
Glucocorticoids down-regulate glucose uptake capacity and insulin-signaling
proteins in omental but not subcutaneous human adipocytes. J. Clin.
Endocrinol. Metab. 89, 2989-2997.
124. Singleton, J.R., Baker, B.L. and Thorburn, A. (2000) Dexamethasone inhibits
insulin-like growth factor signaling and potentiates myoblast apoptosis.
Endocrinology 141, 2945-2950.
111
Insulin dysregulation
125. Sakoda, H., Ogihara, T., Anai, M., Funaki, M., Inukai, K., Katagiri, H.,
Fukushima, Y., Onishi, Y., Ono, H., Fujishiro, M., Kikuchi, M., Oka, Y. and Asano,
T. (2000) Dexamethasone-induced insulin resistance in 3T3-L1 adipocytes is
due to inhibition of glucose transport rather than insulin signal transduction.
Diabetes 49, 1700-1708.
126. Mizock, B.A. (1995) Alterations in carbohydrate metabolism during stress:
a review of the literature. Am. J. Med. 98, 75-84.
127. Mizock, B.A. (2001) Alterations in fuel metabolism in critical illness:
hyperglycaemia. Best Pract. Res. Clin. Endocrinol. Metab. 15, 533-551.
128. Waitt, L.H. and Cebra, C.K. (2009) Characterization of hypertriglyceridemia
and response to treatment with insulin in horses, ponies, and donkeys: 44
cases (19952005). J. Am. Vet. Med. Ass. 234, 915-919.
129. van der Kolk, J.H., Wensing, T., Kalsbeek, H.C. and Breukink, H.J. (1995) Lipid
metabolism in horses with hyperadrenocorticism. J. Am. Vet. Med. Ass. 206,
1010-1012.
130. Freestone, J.F., Wolfsheimer, K.J., Ford, R.B., Church, G. and Bessin, R. (1991)
Triglyceride, insulin, and cortisol responses of ponies to fasting and
dexamethasone administration. J. Vet. Intern. Med. 5, 15-22.
131. Cebra, C.K. and Tornquist, S.J. (2004) Assessment of the effects of
epinephrine and insulin on plasma and serum biochemical variables in llamas
and alpacas. Am. J. Vet. Res. 65, 1692-1696.
132. Khomulo, P.S. and Gritskevich, N.L. (1984) [Physiologico-biochemical
correlates of the behavioral reactions in cats under states of emotional
stress]. Vopr. Med. Khim. 30, 53-55.
133. Fowden, A.L., Forhead, A.J. and Ousey, J.C. (2012) Endocrine adaptations in
the foal over the perinatal period. Equine Vet. J. 44, Suppl. 41, 130-139.
134. Holdstock, N.B., Allen, V.L., Bloomeld, M.R., Hales, C.N. and Fowden, A.L.
(2004) Development of insulin and proinsulin secretion in newborn pony
foals. J. Endocrinol. 181, 469-476.
135. Fowden, A.L., Silver, M., Ellis, L., Ousey, J. and Rossdale, P.D. (1984) Studies
on equine prematurity 3: insulin secretion in the foal during the perinatal
period. Equine Vet. J. 16, 286-291.
136. Fowden, A.L., Ellis, L. and Rossdale, P.D. (1982) Pancreatic beta cell function
in the neonatal foal. J. Reprod. Fertil. Suppl. 32, 529-535.
137. Lester, G.D. (2005) Maturity of the neonatal foal. Vet. Clin. North Am.: Equine
Pract. 21, 333-355.
138. Hurcombe, S.D., Toribio, R.E., Slovis, N., Kohn, C.W., Refsal, K., Saville, W.
and Mudge, M.C. (2008) Blood arginine vasopressin, adrenocorticotropin
hormone, and cortisol concentrations at admission in septic and critically
ill foals and their association with survival. J. Vet. Intern. Med. 22, 639647.
139. Gold, J.R., Divers, T.J., Barton, M.H., Lamb, S.V., Place, N.J., Mohammed, H.O.
and Bain, F.T. (2007) Plasma adrenocorticotropin, cortisol, and
adrenocorticotropin/cortisol ratios in septic and normal-term foals. J. Vet.
Intern. Med. 21, 791-796.
140. Hart, K.A., Slovis, N.M. and Barton, M.H. (2009) Hypothalamicpituitary-adrenal axis dysfunction in hospitalized neonatal foals. J. Vet. Intern.
Med. 23, 901-912.
141. Hollis, A.R., Furr, M.O., Magdesian, K.G., Axon, J.E., Ludlow, V., Boston, R.C.
and Corley, K.T. (2008) Blood glucose concentrations in critically ill neonatal
foals. J. Vet. Intern. Med. 22, 1223-1227.
142. Barsnick, R.J., Hurcombe, S.D., Smith, P.A., Slovis, N.M., Sprayberry, K.A.,
Saville, W.J. and Toribio, R.E. (2011) Insulin, glucagon, and leptin in critically ill
foals. J. Vet. Intern. Med. 25, 123-131.
143. Mitanchez, D. (2007) Glucose regulation in preterm newborn infants. Horm.
Res. 68, 265-271.
144. Beardsall, K., Diderholm, B.M. and Dunger, D.B. (2008) Insulin and
carbohydrate metabolism. Best Pract. Res. Clin. Endocrinol. Metab. 22,
41-55.
145. Mitanchez-Mokhtari, D., Lahlou, N., Kieffer, F., Magny, J.F., Roger, M. and
Voyer, M. (2004) Both relative insulin resistance and defective islet beta-cell
processing of proinsulin are responsible for transient hyperglycemia in
extremely preterm infants. Pediatrics 113, 537-541.
146. Decaro, M.H. and Vain, N.E. (2011) Hyperglycaemia in preterm neonates:
what to know, what to do. Early Hum. Dev. 87, Suppl. 1, S19-S22.
147. Holdstock, N.B., Allen, V.L. and Fowden, A.L. (2012) Pancreatic endocrine
function in newborn pony foals after induced or spontaneous delivery at
term. Equine Vet. J. 44, Suppl. 41, 30-37.
148. Wang, X., Cui, Y., Tong, X., Ye, H. and Li, S. (2007) Glucose and lipid
metabolism in small-for-gestational-age infants at 72 hours of age. J. Clin.
Endocrinol. Metab. 92, 681-684.
112
N. Frank and E. M. Tadros
149. Bazaes, R.A., Salazar, T.E., Pittaluga, E., Pena, V., Alegria, A., Iniguez, G., Ong,
K.K., Dunger, D.B. and Mericq, M.V. (2003) Glucose and lipid metabolism in
small for gestational age infants at 48 hours of age. Pediatrics 111, 804-809.
150. Hays, S.P., Smith, E.O. and Sunehag, A.L. (2006) Hyperglycemia is a risk factor
for early death and morbidity in extremely low birth-weight infants. Pediatrics
118, 1811-1818.
151. Kao, L.S., Morris, B.H., Lally, K.P., Stewart, C.D., Huseby, V. and Kennedy, K.A.
(2006) Hyperglycemia and morbidity and mortality in extremely low birth
weight infants. J. Perinatol. 26, 730-736.
152. Cohen, N.D. (1994) Causes of and farm management factors associated with
disease and death in foals. J. Am. Vet. Med. Ass. 204, 1644-1651.
153. Marsh, P.S. and Palmer, J.E. (2001) Bacterial isolates from blood and their
susceptibility patterns in critically ill foals: 543 cases (19911998). J. Am. Vet.
Med. Ass. 218, 1608-1610.
154. Corley, K.T., Donaldson, L.L. and Furr, M.O. (2005) Arterial lactate
concentration, hospital survival, sepsis and SIRS in critically ill neonatal foals.
Equine Vet. J. 37, 53-59.
155. Russell, C.M., Axon, J.E., Blishen, A. and Begg, A.P. (2008) Blood culture
isolates and antimicrobial sensitivities from 427 critically ill neonatal foals.
Aust. Vet. J. 86, 266-271.
156. Hollis, A.R., Wilkins, P.A., Palmer, J.E. and Boston, R.C. (2008) Bacteremia in
equine neonatal diarrhea: a retrospective study (19902007). J. Vet. Intern.
Med. 22, 1203-1209.
157. Barsnick, R.J. and Toribio, R.E. (2011) Endocrinology of the equine neonate
energy metabolism in health and critical illness. Vet. Clin. North Am.: Equine
Pract. 27, 49-58.
158. Butte, N.F. (2000) Carbohydrate and lipid metabolism in pregnancy: normal
compared with gestational diabetes mellitus. Am. J. Clin. Nutr. 71,
1256S-1261S.
159. Fowden, A.L., Comline, R.S. and Silver, M. (1984) Insulin secretion and
carbohydrate metabolism during pregnancy in the mare. Equine Vet. J. 16,
239-246.
160. George, L.A., Staniar, W.B., Cubitt, T.A., Treiber, K.H., Harris, P.A. and Geor,
R.J. (2011) Evaluation of the effects of pregnancy on insulin sensitivity, insulin
secretion, and glucose dynamics in Thoroughbred mares. Am. J. Vet. Res. 72,
666-674.
161. Firshman, A.M. and Valberg, S.J. (2007) Factors affecting clinical assessment
of insulin sensitivity in horses. Equine Vet. J. 39, 567-575.
162. Bertin, F.R. and Sojka-Kritchevsky, J.E. (2013) Comparison of a 2-step
insulin-response test to conventional insulin-sensitivity testing in horses.
Domest. Anim. Endocrinol. 44, 19-25.
163. Eiler, H., Frank, N., Andrews, F.M., Oliver, J.W. and Fecteau, K.A. (2005)
Physiologic assessment of blood glucose homeostasis via combined
intravenous glucose and insulin testing in horses. Am. J. Vet. Res. 66,
1598-1604.
164. Dugdale, A.H., Curtis, G.C., Cripps, P., Harris, P.A. and Argo, C.M. (2010) Effect
of dietary restriction on body condition, composition and welfare of
overweight and obese pony mares. Equine Vet. J. 42, 600-610.
165. Argo, C.M., Curtis, G.C., Grove-White, D., Dugdale, A.H., Barfoot, C.F. and
Harris, P.A. (2012) Weight loss resistance: a further consideration for the
nutritional management of obese Equidae. Vet. J. 194, 179-188.
166. Longland, A.C., Barfoot, C. and Harris, P.A. (2011) Effects of soaking on the
water-soluble carbohydrate and crude protein content of hay. Vet. Rec. 168,
618-623.
167. Klinkhamer, K., Menheere, P.P. and van der Kolk, J.H. (2011) Basal glucose
metabolism and peripheral insulin sensitivity in equine pituitary pars
intermedia dysfunction. Vet. Q. 31, 19-28.
168. Frank, N., Elliott, S.B. and Boston, R.C. (2008) Effects of long-term oral
administration of levothyroxine sodium on glucose dynamics in healthy adult
horses. Am. J. Vet. Res. 69, 76-81.
169. Durham, A.E., Rendle, D.I. and Newton, J.E. (2008) The effect of metformin on
measurements of insulin sensitivity and beta cell response in 18 horses and
ponies with insulin resistance. Equine Vet. J. 40, 493-500.
170. Tinworth, K.D., Boston, R.C., Harris, P.A., Sillence, M.N., Raidal, S.L. and
Noble, G.K. (2012) The effect of oral metformin on insulin sensitivity in
insulin-resistant ponies. Vet. J. 191, 79-84.
171. Hustace, J.L., Firshman, A.M. and Mata, J.E. (2009) Pharmacokinetics and
bioavailability of metformin in horses. Am. J. Vet. Res. 70, 665-668.
172. Rendle, D.I., Rutledge, F., Hughes, K.J., Heller, J. and Durham, A.E. (2013)
Effects of metformin hydrochloride on blood glucose and insulin responses
to oral dextrose in horses. Equine Vet. J. 45, 751-754.
Equine Veterinary Journal 46 (2014) 103112 2013 EVJ Ltd
You might also like
- CANINE-Nutritional Management of Diabetic DogsDocument12 pagesCANINE-Nutritional Management of Diabetic Dogstaner_soysurenNo ratings yet
- 3 - BIO-Describe The Feedback Mechanisms Involved in Menstrual CycleDocument11 pages3 - BIO-Describe The Feedback Mechanisms Involved in Menstrual CycleCarlo ThornappleNo ratings yet
- Feline Diabetes Pathophysiology and ManagementDocument35 pagesFeline Diabetes Pathophysiology and ManagementDara VinsonNo ratings yet
- 1 Endocrinology of The Equine NeonateDocument10 pages1 Endocrinology of The Equine NeonateMariana CastañoNo ratings yet
- Armstrong 2009Document18 pagesArmstrong 2009Guilherme de FreitasNo ratings yet
- Primacy of Hepatic Insulin Resistance in The Development of The Metabolic Syndrome Induced by An Isocaloric Moderate-Fat Diet in The DogDocument8 pagesPrimacy of Hepatic Insulin Resistance in The Development of The Metabolic Syndrome Induced by An Isocaloric Moderate-Fat Diet in The DogBlagojeNo ratings yet
- Best Practice & Research Clinical Endocrinology & MetabolismDocument11 pagesBest Practice & Research Clinical Endocrinology & MetabolismAndresPimentelAlvarezNo ratings yet
- Journal of Equine Veterinary Science: Original ResearchDocument10 pagesJournal of Equine Veterinary Science: Original ResearchJuan Jose RestrepoNo ratings yet
- Artigo LowCarb e SOPDocument12 pagesArtigo LowCarb e SOPaline.stefany.pl01No ratings yet
- Proceeding of The NAVC North American Veterinary Conference: Jan. 13-27, 2007, Orlando, FloridaDocument4 pagesProceeding of The NAVC North American Veterinary Conference: Jan. 13-27, 2007, Orlando, Floridaayiq_utariNo ratings yet
- Insulin Resistance Title PageDocument9 pagesInsulin Resistance Title PagesuliyatabiodunNo ratings yet
- Veterinary Internal Medicne - 2018 - BertinDocument8 pagesVeterinary Internal Medicne - 2018 - BertinBrunno RogerioNo ratings yet
- International Archives of Medicine: Fat Feeding Potentiates The Diabetogenic Effect of Dexamethasone in Wistar RatsDocument12 pagesInternational Archives of Medicine: Fat Feeding Potentiates The Diabetogenic Effect of Dexamethasone in Wistar RatsShanmugam SivabalanNo ratings yet
- Frank 2006Document8 pagesFrank 2006Rodrigo Martins RibeiroNo ratings yet
- Nutritional Support of The Sick Adult HorseDocument17 pagesNutritional Support of The Sick Adult HorseSofia Reinoso CastilloNo ratings yet
- Kebutuhan Lemak TikusDocument18 pagesKebutuhan Lemak TikusYani NyiikNo ratings yet
- ECEIM Consensus Statement On Equine Metabolic SyndromeDocument15 pagesECEIM Consensus Statement On Equine Metabolic SyndromeEmmanuel Ricardo Marín LópezNo ratings yet
- Journal of Steroid Biochemistry & Molecular Biology: A A A A A A A A A B C 1 A 1Document8 pagesJournal of Steroid Biochemistry & Molecular Biology: A A A A A A A A A B C 1 A 1Fuada Haerana RifaiNo ratings yet
- Peterson 2014Document14 pagesPeterson 2014Luisa Fernanda Rojas DiazNo ratings yet
- Insulin Resistance (IR) Is ADocument21 pagesInsulin Resistance (IR) Is AAttila TamasNo ratings yet
- 2010 Sinclair Insulin Resistance and Fertility in Dairy Cows (3321)Document14 pages2010 Sinclair Insulin Resistance and Fertility in Dairy Cows (3321)Sueños De LunaNo ratings yet
- LO - Metabolik SyndromeDocument4 pagesLO - Metabolik SyndromeRenaldy Thioris100% (1)
- Alteraciones Metabólicas y Hormonales en Gatos Con Lipidosis Hepática (Inglés)Document7 pagesAlteraciones Metabólicas y Hormonales en Gatos Con Lipidosis Hepática (Inglés)AndreaNo ratings yet
- Saturated Fatty Acid Concentrations Are Predictive of Insulin Sensitivity and Beta Cell Compensation in DogsDocument11 pagesSaturated Fatty Acid Concentrations Are Predictive of Insulin Sensitivity and Beta Cell Compensation in Dogsgabrielgpinto1No ratings yet
- Hyperglycemia in Critical Illness: A ReviewDocument11 pagesHyperglycemia in Critical Illness: A ReviewSreejith ViswanathanNo ratings yet
- 2005 Rand e Marshall - Diabetes Mellitus in CatsDocument14 pages2005 Rand e Marshall - Diabetes Mellitus in CatsTula Verusca PereiraNo ratings yet
- Physio 7Document12 pagesPhysio 7amjadNo ratings yet
- Endocrinology 2003 p3958Document11 pagesEndocrinology 2003 p3958imperialscribdNo ratings yet
- Overview of Hepatic Disease in Large AnimalsDocument9 pagesOverview of Hepatic Disease in Large AnimalsDirección Científica Laboratorio VitalabNo ratings yet
- Pathophysiology of Insulin ResistanceDocument8 pagesPathophysiology of Insulin ResistanceCamilo VidalNo ratings yet
- Diabetic Emergencies in Small AnimalsDocument17 pagesDiabetic Emergencies in Small Animalsdia_dianneNo ratings yet
- Liaqat 2017Document8 pagesLiaqat 2017Hamza AldiriNo ratings yet
- TestInsulina HFDDocument11 pagesTestInsulina HFDcatucha25No ratings yet
- Diabetes AssignmentDocument8 pagesDiabetes AssignmentMildred Obeng AgyeiwaaNo ratings yet
- Presentation Metabolic SyndromeDocument56 pagesPresentation Metabolic SyndromeAbdulhakeem Tleimat100% (1)
- Physiology of Diabetes: Dr. Solomon Sathishkumar. MDDocument36 pagesPhysiology of Diabetes: Dr. Solomon Sathishkumar. MDKhaled LajmiNo ratings yet
- NIH Public Access: Author ManuscriptDocument9 pagesNIH Public Access: Author ManuscriptYoser ThamtonoNo ratings yet
- Glucose Intolerance and Insulin Resistance: Relevance in PreeclampsiaDocument14 pagesGlucose Intolerance and Insulin Resistance: Relevance in PreeclampsiaEgi NabilaNo ratings yet
- MBS2-K7-Pharmacology of Endocrine PancreasDocument55 pagesMBS2-K7-Pharmacology of Endocrine PancreasZoga Pratantia TohariNo ratings yet
- Metabolic SyndromeDocument55 pagesMetabolic SyndromeAakash BalasubramanianNo ratings yet
- Diabetes Mellitus and Laboratory Tests of DiabetesDocument24 pagesDiabetes Mellitus and Laboratory Tests of DiabetesturkiNo ratings yet
- Nutritional Support of The Critically Ill Small AnDocument12 pagesNutritional Support of The Critically Ill Small AnTactvisNo ratings yet
- Milk and Metabolic SyndromeDocument10 pagesMilk and Metabolic SyndromeCamilla MendesNo ratings yet
- DiabeticcasestudyDocument7 pagesDiabeticcasestudyapi-272773859No ratings yet
- Endocrine Week 2Document18 pagesEndocrine Week 2Clauvinna Lie FiscaNo ratings yet
- Exercise and Spirulina Control Non-Alcoholic Hepatic Steatosis and Lipid Profile in Diabetic Wistar RatsDocument7 pagesExercise and Spirulina Control Non-Alcoholic Hepatic Steatosis and Lipid Profile in Diabetic Wistar RatslilumomoNo ratings yet
- Hepatica ClearanceDocument6 pagesHepatica ClearanceStephania NiñoNo ratings yet
- Obesida ArticuloDocument5 pagesObesida ArticuloZangre AzulNo ratings yet
- Insulin Sensitivity and Glucose Tolerance Are Altered by Maintenance On A Ketogenic DietDocument17 pagesInsulin Sensitivity and Glucose Tolerance Are Altered by Maintenance On A Ketogenic DietSebastiano ViganòNo ratings yet
- PDF 760Document10 pagesPDF 760Reskia NabilaNo ratings yet
- TYPE 2 DM PathogenesisDocument14 pagesTYPE 2 DM PathogenesisjosephNo ratings yet
- Assistant - Prof.Dr.M.A.S: Fat Cow Syndrome, Hepatic Lipidosis, Pregnancy Toxemia in CattleDocument3 pagesAssistant - Prof.Dr.M.A.S: Fat Cow Syndrome, Hepatic Lipidosis, Pregnancy Toxemia in Cattleفرسان الدعوةNo ratings yet
- Article-2012-Vaspin in Obesity and Diabetes-Pathophysiological and Clinical SignificanceDocument7 pagesArticle-2012-Vaspin in Obesity and Diabetes-Pathophysiological and Clinical Significancecarlos ArozamenaNo ratings yet
- InsulinDocument5 pagesInsulinMuhammad DawoodNo ratings yet
- Fructose, Weight Gain, and The Insulin Resistance Syndrome: Special ArticleDocument12 pagesFructose, Weight Gain, and The Insulin Resistance Syndrome: Special ArticleMarcusNo ratings yet
- Cafeteria Diet Intake For Fourteen Weeks Can Cause Obesity and Insulin Resistance in Wistar RatsDocument8 pagesCafeteria Diet Intake For Fourteen Weeks Can Cause Obesity and Insulin Resistance in Wistar RatsVagner SimoninNo ratings yet
- Presented by DR Ashish Sharma Guided by DR Meena PatelDocument74 pagesPresented by DR Ashish Sharma Guided by DR Meena PatelAndrew Surya Putra SccNo ratings yet
- بحث علاقة السمنة بالانسولينDocument30 pagesبحث علاقة السمنة بالانسولينh14005403No ratings yet
- Effect of Walking Exercise On Abdominal Fat, Insulin Resistance and Serum Cytokines in Obese WomenDocument9 pagesEffect of Walking Exercise On Abdominal Fat, Insulin Resistance and Serum Cytokines in Obese WomenankitsmkNo ratings yet
- Asian Paci Fic Journal of Tropical MedicineDocument5 pagesAsian Paci Fic Journal of Tropical MedicineMuhammad Fuad MahfudNo ratings yet
- Obesity - Short Scientific Findings to Ameliorate the Body WeightFrom EverandObesity - Short Scientific Findings to Ameliorate the Body WeightNo ratings yet
- Science 10 - Activity 2 - 3rd Quarter - MontereyDocument2 pagesScience 10 - Activity 2 - 3rd Quarter - MontereyKiel Angelo MontereyNo ratings yet
- Ozempic Product Monograph PDFDocument59 pagesOzempic Product Monograph PDFAnonymous Complainer0% (1)
- Lab 6td5tbyyvtc1920 RevDocument15 pagesLab 6td5tbyyvtc1920 RevrinidinanNo ratings yet
- B.SC ZOOLOGY. HONS SYLLABUS 2020 (NEW) Kolhan UniversityDocument64 pagesB.SC ZOOLOGY. HONS SYLLABUS 2020 (NEW) Kolhan UniversitySanjayNo ratings yet
- Supplement ZadnjaverDocument80 pagesSupplement ZadnjaverikaNo ratings yet
- DM 1 and 2 PathophysiologyDocument1 pageDM 1 and 2 PathophysiologyApril Rose ParconNo ratings yet
- Butea Superba Sci - Luteinizing Hormone Reduction by The Male Potency Herb, Butea SuperbaDocument11 pagesButea Superba Sci - Luteinizing Hormone Reduction by The Male Potency Herb, Butea SuperbayunusNo ratings yet
- Regulation of Blood Pressure - 2Document38 pagesRegulation of Blood Pressure - 2vikrant gholapNo ratings yet
- Generic Name:: Is Used To Dissolve (Cholesterol) Gallstones and PDocument9 pagesGeneric Name:: Is Used To Dissolve (Cholesterol) Gallstones and PZAY EMNo ratings yet
- Class 12 - Biology - Human ReproductionDocument10 pagesClass 12 - Biology - Human ReproductionAstha SaxenaNo ratings yet
- How To Increase Breast SizeDocument6 pagesHow To Increase Breast Sizesfsfco100% (1)
- Pharmacology Diuretics For BPT StudentsDocument16 pagesPharmacology Diuretics For BPT StudentsDr.U.P.Rathnakar.MD.DIH.PGDHM100% (1)
- Anatomy #01Document10 pagesAnatomy #01Mohammed4 JundyNo ratings yet
- Hospital Discharge Algorithm Based On Admission Hba For The Management of Patients With Type 2 DiabetesDocument6 pagesHospital Discharge Algorithm Based On Admission Hba For The Management of Patients With Type 2 DiabetesxtineNo ratings yet
- 12-Endocrinology & DiabetesDocument2 pages12-Endocrinology & DiabetesIbrahimFikryNo ratings yet
- Dermatology Handbook For Medical Students 2nd Edition 2014 Final2Document76 pagesDermatology Handbook For Medical Students 2nd Edition 2014 Final2Nogra CarlNo ratings yet
- Anesthesia For Endocrine Emergencies (2020)Document15 pagesAnesthesia For Endocrine Emergencies (2020)Yaneth Tapia MoralesNo ratings yet
- Complete Androgen Insensitivity Syndrome in An Adult - A Rar PDFDocument3 pagesComplete Androgen Insensitivity Syndrome in An Adult - A Rar PDFNizam Mischievous'Lovely Schremo BoyysNo ratings yet
- Human Reproduction Hand NotesDocument15 pagesHuman Reproduction Hand Notesanmol kumarNo ratings yet
- Secondary Causes of DyslipidemiaDocument3 pagesSecondary Causes of DyslipidemiaAnghelo Aldair Velásquez CarrilloNo ratings yet
- Gestational Diabetes 97-03Document9 pagesGestational Diabetes 97-03jaenaroseNo ratings yet
- Effects of High TSHDocument3 pagesEffects of High TSHSreream KumarNo ratings yet
- How To Position Finerenone in The Treatment Algorithm For Type 2 Diabetes With Renal Complication - GPMPDocument27 pagesHow To Position Finerenone in The Treatment Algorithm For Type 2 Diabetes With Renal Complication - GPMPTaufiqurrokhman RofiiNo ratings yet
- The Skin (Integumentary System)Document4 pagesThe Skin (Integumentary System)Darlin Maree JamonNo ratings yet
- BAMU B.pharmacy First Year SyllabusDocument31 pagesBAMU B.pharmacy First Year SyllabusGajanan Vaishnav0% (1)
- Excretory Products and Their EliminationDocument9 pagesExcretory Products and Their EliminationBiju MylachalNo ratings yet
- Proliferative EndometriumDocument4 pagesProliferative EndometriumKristine Dela CruzNo ratings yet
- 55 ENDOCRINE Tutorial Week 5ADocument9 pages55 ENDOCRINE Tutorial Week 5AChristian Versola-Macapulay Valle100% (1)
- Biology Assignment HBSC3103 - V2Document23 pagesBiology Assignment HBSC3103 - V2Lester Randy RubintinusNo ratings yet