Professional Documents
Culture Documents
Acute Abdominal Pain: Step-By-Step Assessment
Acute Abdominal Pain: Step-By-Step Assessment
Uploaded by
zafar_183250 ratings0% found this document useful (0 votes)
14 views1 pageAbdominal pain is assessed in a step-by-step manner. First, identify if the patient is in shock through signs of hypotension and hypoperfusion. If in shock, secure IV access and begin resuscitation while considering ruptured AAA, ectopic pregnancy, or splenic rupture requiring immediate surgery. Second, check for generalized peritonitis from a perforated hollow viscus through severe abdominal pain worse with movement and abdominal rigidity requiring aggressive resuscitation and antibiotics with surgical review. Third, if not in shock or peritonitis, perform further tests and assess for underlying causes like perforated viscus, mesenteric ischemia, pancreatitis, or colitis while urgently referring for surgical review.
Original Description:
vgvg
Original Title
mcleaod 44
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentAbdominal pain is assessed in a step-by-step manner. First, identify if the patient is in shock through signs of hypotension and hypoperfusion. If in shock, secure IV access and begin resuscitation while considering ruptured AAA, ectopic pregnancy, or splenic rupture requiring immediate surgery. Second, check for generalized peritonitis from a perforated hollow viscus through severe abdominal pain worse with movement and abdominal rigidity requiring aggressive resuscitation and antibiotics with surgical review. Third, if not in shock or peritonitis, perform further tests and assess for underlying causes like perforated viscus, mesenteric ischemia, pancreatitis, or colitis while urgently referring for surgical review.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
14 views1 pageAcute Abdominal Pain: Step-By-Step Assessment
Acute Abdominal Pain: Step-By-Step Assessment
Uploaded by
zafar_18325Abdominal pain is assessed in a step-by-step manner. First, identify if the patient is in shock through signs of hypotension and hypoperfusion. If in shock, secure IV access and begin resuscitation while considering ruptured AAA, ectopic pregnancy, or splenic rupture requiring immediate surgery. Second, check for generalized peritonitis from a perforated hollow viscus through severe abdominal pain worse with movement and abdominal rigidity requiring aggressive resuscitation and antibiotics with surgical review. Third, if not in shock or peritonitis, perform further tests and assess for underlying causes like perforated viscus, mesenteric ischemia, pancreatitis, or colitis while urgently referring for surgical review.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 1
Abdominal pain
Acute abdominal pain: step-by-step assessment
1
Evidence of shock?
Rapidly identify patients who are shocked
with hypotension and evidence of tissue
hypoperfusion (see Box 28.1, p. 249).
Remember that young, fit patients can
often maintain BP in the face of major fluid
losses; in these patients hypotension occurs
late, so look carefully for early features
such as HR, RR, narrow pulse pre
ssure, anxiety, pallor, cold sweat or lightheadedness on standing postural BP.
If the patient has overt or incipient
shock, secure two large-bore IV lines;
send blood for cross-match, U+E, FBC,
amylase and LFTs; and begin aggressive
resuscitation.
The diagnoses to consider first are rupture
of an AAA, ectopic pregnancy or other
viscus, as these may require immediate surgical intervention.
Suspect ruptured AAA in any patient
with known AAA, a pulsatile abdominal
mass or risk factors e.g. male >60 years,
who experiences sudden-onset, severe
abdominal/back pain followed rapidly
by haemodynamic compromise.
Suspect ruptured ectopic pregnancy in
any pregnant woman or woman of
child-bearing age with recent-onset
lower abdominal pain or PV bleeding;
perform an immediate bedside
pregnancy test.
Consider splenic rupture in any shocked
patient with abdominal pain who has a
history of recent trauma, e.g. road traffic
accident.
medical conditions, e.g. diabetic
ketoacidosis, myocardial infarction,
adrenal crisis, pneumonia
any condition associated with repeated
vomiting, e.g. intestinal obstruction,
gastroenteritis.
2
Generalised peritonitis?
Generalised peritonitis occasionally results
from acute pancreatitis but is usually the
manifestation of a perforated hollow viscus,
e.g. stomach, duodenum or colon. Suspect
it if there is severe, non-colicky abdominal
pain that is worse on movement, coughing
or deep inspiration, and which is associated
with inflammatory features and generalised abdominal rigidity. The patient will
usually be lying still, taking shallow breaths,
and will be in obvious distress or discomfort; reconsider the diagnosis if the patient
appears well or is moving freely.
Patients require aggressive resuscitation,
antibiotics and immediate surgical referral.
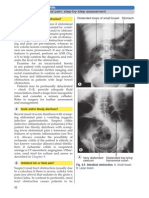
Free air under the diaphragm on erect CXR
(present in 5075% of cases) confirms the
diagnosis; if CXR non-diagnostic consider
contrast CT (Fig. 4.4). Serum amylase may
help to differentiate perforation from pancreatitis. A very high index of suspicion is
required in the elderly and in patients
taking systemic steroids; signs are often
subtle, so reassess frequently.
If any of these diagnoses is suspected,
arrange immediate surgical review prior to
imaging.
In the absence of these conditions,
perform an ECG, CXR, urinalysis and ABG,
continue to assess for an underlying cause,
as described below, and refer for urgent
surgical review. Other important diagnoses
to consider include:
perforated viscus
mesenteric ischaemia
acute inflammatory conditions, e.g.
pancreatitis, colitis, cholangitis
Fig. 4.4 Free air under the diaphragm.
31
You might also like
- Ahmed SLE Mcq-P2 - E2 - 80 - AB - E2 - 80 - AC PDFDocument172 pagesAhmed SLE Mcq-P2 - E2 - 80 - AB - E2 - 80 - AC PDFMohamed Kudaih100% (5)
- Annual: PerformanceDocument176 pagesAnnual: PerformanceArja WoldeNo ratings yet
- Orthopedic Inpatient Protocols: A Guide to Orthopedic Inpatient RoundingFrom EverandOrthopedic Inpatient Protocols: A Guide to Orthopedic Inpatient RoundingNo ratings yet
- Acute Abdominal Pain: Step-By-Step AssessmentDocument1 pageAcute Abdominal Pain: Step-By-Step Assessmentzafar_18325No ratings yet
- Acute Upper Abdominal Pain: Step-By-Step AssessmentDocument1 pageAcute Upper Abdominal Pain: Step-By-Step Assessmentzafar_18325No ratings yet
- 5 Mesenteric IschemiaDocument39 pages5 Mesenteric IschemiaFahd Abdullah Al-refaiNo ratings yet
- Acute Appendicitis: History and ExaminationDocument6 pagesAcute Appendicitis: History and ExaminationPraktek Dokter Umum drjosefdrelsyNo ratings yet
- Acute AbdomenDocument7 pagesAcute AbdomenStanley MwendaNo ratings yet
- Acute Abdominal PainDocument5 pagesAcute Abdominal PainLM Mys100% (1)
- Diagnosis and Treatment of Intraabdominal InjuriesDocument88 pagesDiagnosis and Treatment of Intraabdominal Injuriessgod34No ratings yet
- PROBLEM 3 GIT Jeffrey 405170048Document162 pagesPROBLEM 3 GIT Jeffrey 405170048Mohammad Jofa Rachman PNo ratings yet
- Acute Upper Abdominal Pain: Step-By-Step AssessmentDocument1 pageAcute Upper Abdominal Pain: Step-By-Step Assessmentzafar_18325No ratings yet
- Acute AbdomenDocument29 pagesAcute AbdomenUmar AzlanNo ratings yet
- Acute Abdominal-Wps OfficeDocument26 pagesAcute Abdominal-Wps OfficeAbhash MishraNo ratings yet
- A Case of Rectus Sheath HematomaDocument4 pagesA Case of Rectus Sheath HematomadrthirNo ratings yet
- Acute Abdomen - StatPearls - NCBI BookshelfDocument6 pagesAcute Abdomen - StatPearls - NCBI Bookshelfimehap033No ratings yet
- Acute Abdomen - StatPearls - NCBI BookshelfDocument7 pagesAcute Abdomen - StatPearls - NCBI BookshelfAinani TajrianNo ratings yet
- Surgical AbdomenDocument3 pagesSurgical Abdomendude dNo ratings yet
- ABC Emergency Differential DiagnosisffDocument3 pagesABC Emergency Differential Diagnosisffsharu4291No ratings yet
- Intestinal Perforation Clinical Presentation: HistoryDocument2 pagesIntestinal Perforation Clinical Presentation: HistorypricillyaNo ratings yet
- Acute AbdomenDocument8 pagesAcute AbdomensharanNo ratings yet
- Abdominal Pain - Royal Children HospitalDocument4 pagesAbdominal Pain - Royal Children HospitalMehrdad IraniNo ratings yet
- ΠΡΟΣΕΓΓΙΣΗ ΑΣΘΕΝΟΥΣ ΜΕ ΚΟΙΛΙΑΚΟ ΑΛΓΟΣ- (Επικ. Καθ. κα. Ε. Πολυζωγοπούλου)Document34 pagesΠΡΟΣΕΓΓΙΣΗ ΑΣΘΕΝΟΥΣ ΜΕ ΚΟΙΛΙΑΚΟ ΑΛΓΟΣ- (Επικ. Καθ. κα. Ε. Πολυζωγοπούλου)ElenaNo ratings yet
- Acute Abdomen Utk SekarwangiDocument33 pagesAcute Abdomen Utk SekarwangiIca Trianjani SetyaningrumNo ratings yet
- History PerformaDocument5 pagesHistory PerformaHariharan NarendranNo ratings yet
- Abdominal Aortic AneurysmDocument9 pagesAbdominal Aortic AneurysmIlyes FerenczNo ratings yet
- Acute Abdomen: Part I: Intestinal Obstruction/Bowel Infarction/ Constipation (And How To Assess and Initiate Management)Document63 pagesAcute Abdomen: Part I: Intestinal Obstruction/Bowel Infarction/ Constipation (And How To Assess and Initiate Management)Rumana IslamNo ratings yet
- Graff 2001Document14 pagesGraff 2001mutimutimutiNo ratings yet
- Acute Abdomen: DR Teamir Negussie Assistant Professor Dept of SurgeryDocument69 pagesAcute Abdomen: DR Teamir Negussie Assistant Professor Dept of SurgeryteamirNo ratings yet
- Vascular Emergencies: Susan L. Drinkwater, Vikas A. Pandey, and Alun H. DaviesDocument17 pagesVascular Emergencies: Susan L. Drinkwater, Vikas A. Pandey, and Alun H. DaviesHarshpreet KaurNo ratings yet
- Antepartum HaemorrhageDocument19 pagesAntepartum HaemorrhageKvy OngNo ratings yet
- ABDOMEN Agudo EnfrentamientoDocument22 pagesABDOMEN Agudo Enfrentamientonicositja_vangoh91No ratings yet
- Blunt Abdominal InjuryDocument6 pagesBlunt Abdominal InjuryPeter KayNo ratings yet
- Acute Abdominal Pain: Presented by Dr. Kolahdouzan Thoracic Surgen Alzahra HospitalDocument77 pagesAcute Abdominal Pain: Presented by Dr. Kolahdouzan Thoracic Surgen Alzahra HospitalGraceline Margaretha Marsintauly SianiparNo ratings yet
- Advances in Abdominal TraumaDocument21 pagesAdvances in Abdominal TraumaIsabelle UbialiNo ratings yet
- Abdominal Pain: CBT/OTEP 435Document17 pagesAbdominal Pain: CBT/OTEP 435Jashim JumliNo ratings yet
- Perforated ViscusDocument49 pagesPerforated ViscusReina JeanNo ratings yet
- Blunt Abdominal Trauma UpdatedDocument52 pagesBlunt Abdominal Trauma UpdatedPethuel AgyinNo ratings yet
- History - ACUTE ABDOMENDocument14 pagesHistory - ACUTE ABDOMENqayyum consultantfpscNo ratings yet
- Abruptio PlacentaDocument11 pagesAbruptio PlacentaAlynna ValbuenaNo ratings yet
- Acute Abdomen &peritonitisDocument63 pagesAcute Abdomen &peritonitisSamar Ahmad100% (1)
- Approach To Abdominal PainDocument22 pagesApproach To Abdominal PainOmar AbdillahiNo ratings yet
- Examination of Intestinal Obstruction, Acute Abdomen and Acute Appendicitis - Eugh & BwembyaDocument29 pagesExamination of Intestinal Obstruction, Acute Abdomen and Acute Appendicitis - Eugh & BwembyaForeighn97No ratings yet
- Rationale Diagnostic ProceduresDocument22 pagesRationale Diagnostic ProceduresShaktisila FatrahadyNo ratings yet
- HP Nov02 PainDocument6 pagesHP Nov02 PainSampath GoudNo ratings yet
- Presented by Dr. Ayalew ZDocument35 pagesPresented by Dr. Ayalew Zyared getachewNo ratings yet
- 26 2 KatzDocument2 pages26 2 KatznoemaraleNo ratings yet
- Abdominal Pain in PaediatricDocument35 pagesAbdominal Pain in PaediatricNuyue FathihahNo ratings yet
- Common Illnesses in Family PracticeDocument234 pagesCommon Illnesses in Family Practicetmle100% (2)
- David C. Van Metre, DVM, DACVIM Colorado State University, Fort Collins, CO, USADocument5 pagesDavid C. Van Metre, DVM, DACVIM Colorado State University, Fort Collins, CO, USAVeterinario HaciendaNo ratings yet
- UntitledDocument25 pagesUntitlednanisdeadNo ratings yet
- Abdominal Stab WoundDocument5 pagesAbdominal Stab WoundHemingmingNo ratings yet
- Fect Eau 2017Document15 pagesFect Eau 2017Allison DiêgoNo ratings yet
- IntussusceptionDocument33 pagesIntussusceptionNovendi RizkaNo ratings yet
- 240 243Document5 pages240 243Rika WulandariNo ratings yet
- Narrative Report ContentsDocument15 pagesNarrative Report ContentsGladie Ann Dela RosaNo ratings yet
- 062 Cerebral-Challenge 5 Update 2011 PDFDocument5 pages062 Cerebral-Challenge 5 Update 2011 PDFcignalNo ratings yet
- Stabilization of Trauma in The ERDocument3 pagesStabilization of Trauma in The ERAzooz MoaidNo ratings yet
- Acute Abdominal Pain: Step-By-Step AssessmentDocument1 pageAcute Abdominal Pain: Step-By-Step Assessmentzafar_18325No ratings yet
- CSS - Abdominal Trauma - Tim B - Kel.20Document36 pagesCSS - Abdominal Trauma - Tim B - Kel.20Fariz AkbarNo ratings yet
- 2018 Diagnostic Approach To The Acute AbdomenDocument15 pages2018 Diagnostic Approach To The Acute AbdomenCamila CalleNo ratings yet
- Assessing Patients: A Practical Guide: The Clinical ExaminationDocument1 pageAssessing Patients: A Practical Guide: The Clinical Examinationzafar_18325No ratings yet
- The Diagnostic ProcessDocument1 pageThe Diagnostic Processzafar_18325No ratings yet
- The Diagnostic Process: See Further Assessment of Chronic Liver Disease (P. 181) YesDocument1 pageThe Diagnostic Process: See Further Assessment of Chronic Liver Disease (P. 181) Yeszafar_18325No ratings yet
- Differential Diagnosis: Abdominal PainDocument1 pageDifferential Diagnosis: Abdominal Painzafar_18325No ratings yet
- Assessment of Common Presenting ProblemsDocument1 pageAssessment of Common Presenting Problemszafar_18325No ratings yet
- Box 4.1 Indicators of Systemic Inflammation: Differential DiagnosisDocument1 pageBox 4.1 Indicators of Systemic Inflammation: Differential Diagnosiszafar_18325No ratings yet
- Acute Upper Abdominal Pain: Step-By-Step AssessmentDocument1 pageAcute Upper Abdominal Pain: Step-By-Step Assessmentzafar_18325No ratings yet
- Acute Abdominal Pain: OverviewDocument1 pageAcute Abdominal Pain: Overviewzafar_18325No ratings yet
- Mesenteric Ischaemia Renal Tract Disorders: Non-Ulcer DyspepsiaDocument1 pageMesenteric Ischaemia Renal Tract Disorders: Non-Ulcer Dyspepsiazafar_18325No ratings yet
- Acute Abdominal Pain: Step-By-Step AssessmentDocument1 pageAcute Abdominal Pain: Step-By-Step Assessmentzafar_18325No ratings yet
- Acute Upper Abdominal Pain: Step-By-Step AssessmentDocument1 pageAcute Upper Abdominal Pain: Step-By-Step Assessmentzafar_18325No ratings yet
- Acute Abdominal Pain: Step-By-Step AssessmentDocument1 pageAcute Abdominal Pain: Step-By-Step Assessmentzafar_18325No ratings yet
- Acute Upper Abdominal Pain: OverviewDocument1 pageAcute Upper Abdominal Pain: Overviewzafar_18325No ratings yet
- Screening Tests: Click To Edit Master Subtitle StyleDocument15 pagesScreening Tests: Click To Edit Master Subtitle Stylezafar_18325No ratings yet
- Laurence Hunter Helen Leng Caroline Jones Miles Hitchen Jennifer Rose AntbitsDocument1 pageLaurence Hunter Helen Leng Caroline Jones Miles Hitchen Jennifer Rose Antbitszafar_18325No ratings yet
- Role Pharmacist in PandemicDocument14 pagesRole Pharmacist in PandemicTessa Amanda SavetriNo ratings yet
- Health System and Medical Education in Brazil: History, Principles, and OrganizationDocument5 pagesHealth System and Medical Education in Brazil: History, Principles, and OrganizationMarco Antonio KoffNo ratings yet
- EE - QE 661 QuestionsDocument74 pagesEE - QE 661 QuestionsHassan R. G.No ratings yet
- CPR - Basic Life SupportDocument84 pagesCPR - Basic Life SupportAzra Durak-NalbanticNo ratings yet
- MODULE 12-14 BOSH - With Pre-Final and Final ExamDocument23 pagesMODULE 12-14 BOSH - With Pre-Final and Final ExamEstelle May Beton AugustoNo ratings yet
- MATH 102 Chapter 8 Calculation of Basic IV Drip RatesDocument15 pagesMATH 102 Chapter 8 Calculation of Basic IV Drip RatesIvan DanusaputraNo ratings yet
- Therapeutic Drug MonitoringDocument13 pagesTherapeutic Drug MonitoringSujith Kuttan100% (2)
- Jurding Otosklerosis Nor Azmina 112017074Document19 pagesJurding Otosklerosis Nor Azmina 112017074beatriceNo ratings yet
- 2 5256112686864795120Document1,028 pages2 5256112686864795120Drdeg123 123100% (3)
- A Pocket Guide For Echs BeneficiariesDocument2 pagesA Pocket Guide For Echs BeneficiariesPrasanth ReddiNo ratings yet
- Quarter 3: Module 4 (Weeks 4-5) Nature of Emerging and Re-Emerging DiseasesDocument19 pagesQuarter 3: Module 4 (Weeks 4-5) Nature of Emerging and Re-Emerging DiseasesGeceylNo ratings yet
- BHA-FPX4106 - Nadhirah Lutchminarain - Assignment 1Document11 pagesBHA-FPX4106 - Nadhirah Lutchminarain - Assignment 1Nadhirah De WetNo ratings yet
- 13 Drug StudyDocument6 pages13 Drug StudyRachel Yvonne Cabacungan100% (1)
- PBHRF Lunar Mission and HomeopathyDocument40 pagesPBHRF Lunar Mission and HomeopathyGeorge MontoyaNo ratings yet
- Nursing Care Plan - SepsisDocument2 pagesNursing Care Plan - SepsisJoe Mark Salamero86% (21)
- CMS-10611 MOON 2023 - v508Document2 pagesCMS-10611 MOON 2023 - v508bwiettingNo ratings yet
- Enteral Nurtrition Written ReportDocument59 pagesEnteral Nurtrition Written ReportKyle UyNo ratings yet
- Chief Nursing Officer InterviewDocument7 pagesChief Nursing Officer Interviewapi-237845240No ratings yet
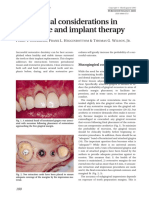
- Periodontal Considerations in Restorative and Implant TherapyDocument10 pagesPeriodontal Considerations in Restorative and Implant TherapyAntonny VasquezNo ratings yet
- Guidelines For Training Under ARSH For NIHFW 14.7.11Document26 pagesGuidelines For Training Under ARSH For NIHFW 14.7.11National Child Health Resource Centre (NCHRC)50% (2)
- Bibliography For PneumoniaDocument2 pagesBibliography For PneumoniaakjsandhuNo ratings yet
- Health Education Plan (Handwashing) .Document3 pagesHealth Education Plan (Handwashing) .Mark FernandezNo ratings yet
- 4 ADocument50 pages4 Aucnursingcesdev2008No ratings yet
- ICHROMA IgG-IgMDocument5 pagesICHROMA IgG-IgMAlfonso RamosNo ratings yet
- First Aid Procedure (Revised) 0-dDocument19 pagesFirst Aid Procedure (Revised) 0-dFarizan BolkafliNo ratings yet
- PI e TL - CRP - HS - L1 27210 2105 5Document1 pagePI e TL - CRP - HS - L1 27210 2105 5Deni ArdianNo ratings yet
- Risk For Falls NCPDocument1 pageRisk For Falls NCPandayaannedhesireeNo ratings yet
- Lesson Plan in HealthDocument7 pagesLesson Plan in HealthJstne AglNo ratings yet