Professional Documents
Culture Documents
The Musculoskeletal System
The Musculoskeletal System
Uploaded by
Maria Dini AdmiratiCopyright:
Available Formats
You might also like
- Addiction Treatment: A Strengths PerspectiveDocument2 pagesAddiction Treatment: A Strengths PerspectiveKatherine van Wormer50% (4)
- Anaphy C7 Oral Rec.Document3 pagesAnaphy C7 Oral Rec.Katrina ParbaNo ratings yet
- Musculoskeltal SystemDocument18 pagesMusculoskeltal Systemhy7tnNo ratings yet
- Formation: Blood Calcium Level - Calcium HydroxyapatiteDocument13 pagesFormation: Blood Calcium Level - Calcium HydroxyapatiteClarissa IsuriñaNo ratings yet
- Lec 1516 Bone Tissue and Skeletal SystemDocument28 pagesLec 1516 Bone Tissue and Skeletal SystemonegaonnweNo ratings yet
- Functional Anatomy and Physiology 1Document6 pagesFunctional Anatomy and Physiology 1AtiqahNo ratings yet
- Kalsifikasi, Deposisi Dan Resorpsi TulangDocument40 pagesKalsifikasi, Deposisi Dan Resorpsi TulangrifkaNo ratings yet
- Calcium Homeostasis and Osteoporosis - McMaster Pathophysiology ReviewDocument8 pagesCalcium Homeostasis and Osteoporosis - McMaster Pathophysiology ReviewEzayu AzeraNo ratings yet
- Bone and Mineral Metabolism in Health and DiseaseDocument14 pagesBone and Mineral Metabolism in Health and Diseasebiniam MesfinNo ratings yet
- Bone Metabolism: German VersionDocument17 pagesBone Metabolism: German VersionDapot SianiparNo ratings yet
- Exam A-3Document11 pagesExam A-3yapues87No ratings yet
- Bone and Cartilage PDFDocument50 pagesBone and Cartilage PDFalviraNo ratings yet
- 7 CalciumDocument83 pages7 Calciumtmqt2fbnzgNo ratings yet
- Bone Basic Science: Presenter: DR Nshimiyimana Alexis Orthopedic Resident-UrDocument36 pagesBone Basic Science: Presenter: DR Nshimiyimana Alexis Orthopedic Resident-UrNshimiyimana AlexisNo ratings yet
- 511-525chapter 6-8 (1) An Introduction To The Skeletal SystemDocument6 pages511-525chapter 6-8 (1) An Introduction To The Skeletal Systemtomorrow.today.yesterday .yesterdayNo ratings yet
- Seminar On Bone and CalciumDocument4 pagesSeminar On Bone and Calciumtshireletso “TROY” nkunaNo ratings yet
- Alveolar Bone FFDocument105 pagesAlveolar Bone FFshashi kant chaudharyNo ratings yet
- Chap 6 AnaphyDocument8 pagesChap 6 AnaphyNicholle VelosoNo ratings yet
- Ch. 10 and 6Document25 pagesCh. 10 and 6Bammary88909No ratings yet
- Physiologic Processes in The Skeletal SystemDocument6 pagesPhysiologic Processes in The Skeletal SystemAry Romeo ShakespeareNo ratings yet
- Anatomy & Physiology: Skeletal SystemDocument20 pagesAnatomy & Physiology: Skeletal SystemWilbert Antonino CabanbanNo ratings yet
- Human Anatomy 4th Edition Saladin Solutions Manual 1Document36 pagesHuman Anatomy 4th Edition Saladin Solutions Manual 1donnawugnwsjrzcxt100% (28)
- Human Anatomy 4Th Edition Saladin Solutions Manual Full Chapter PDFDocument27 pagesHuman Anatomy 4Th Edition Saladin Solutions Manual Full Chapter PDFdora.ivy892100% (22)
- Bone ResorptionDocument10 pagesBone ResorptionVibhor PradhanNo ratings yet
- COMPRE2Document13 pagesCOMPRE2Rodrigo SeriozaNo ratings yet
- 6.the Skeletal System Bone TissueDocument25 pages6.the Skeletal System Bone TissueKojo Yeboah EnchillNo ratings yet
- SKELETAL SYSTEM ReviewerDocument7 pagesSKELETAL SYSTEM ReviewerKrize Colene dela CruzNo ratings yet
- We Are Intechopen, The World'S Leading Publisher of Open Access Books Built by Scientists, For ScientistsDocument19 pagesWe Are Intechopen, The World'S Leading Publisher of Open Access Books Built by Scientists, For ScientistsJade LolongNo ratings yet
- Bone Physiology 2Document27 pagesBone Physiology 2Nzau MuangeNo ratings yet
- MatthewVaracalloMD PhysiologyBoneDocument5 pagesMatthewVaracalloMD PhysiologyBonetulipaNo ratings yet
- Bone Formation: Hypothalamic Hormone, CRH, and The Pituitary Hormone, ACTHDocument3 pagesBone Formation: Hypothalamic Hormone, CRH, and The Pituitary Hormone, ACTHSimon AvilaNo ratings yet
- Bone Ash Estimation of Content of Bone Ash Project Submitted by PrashanthDocument3 pagesBone Ash Estimation of Content of Bone Ash Project Submitted by PrashanthHarsh Kumar0% (3)
- Alad Bihag Hizon Medicine Case StudyDocument103 pagesAlad Bihag Hizon Medicine Case StudyDan HizonNo ratings yet
- Chapter 3Document12 pagesChapter 3Deolita BadiangNo ratings yet
- Bones: A Hard SubjectDocument16 pagesBones: A Hard SubjectMaria Dini AdmiratiNo ratings yet
- Chemistry Project On Estimation of Content of Bone AshDocument18 pagesChemistry Project On Estimation of Content of Bone AshKim TaesiNo ratings yet
- Drugs Bone DisordersDocument38 pagesDrugs Bone Disordersalizwaxabanisa8No ratings yet
- Functions of The Musculoskeletal SystemDocument9 pagesFunctions of The Musculoskeletal SystemLinda XueNo ratings yet
- Department of Periodontics and Implantology: Calcium MetabolismDocument63 pagesDepartment of Periodontics and Implantology: Calcium Metabolismrasagna reddy100% (1)
- Bone Is A MineralizedDocument2 pagesBone Is A MineralizedZen Firhan ShahabNo ratings yet
- Human Anatomy 5th Edition Saladin Solutions ManualDocument7 pagesHuman Anatomy 5th Edition Saladin Solutions Manualjillhenrysetcjnzrfp100% (26)
- 7 - BoneDocument36 pages7 - BoneKhdhir M. SalemNo ratings yet
- Human Anatomy 5Th Edition Saladin Solutions Manual Full Chapter PDFDocument28 pagesHuman Anatomy 5Th Edition Saladin Solutions Manual Full Chapter PDFJenniferWhitebctr100% (12)
- Alveolar Bone: and It's Associated PathologiesDocument7 pagesAlveolar Bone: and It's Associated Pathologiesمحمد العراقيNo ratings yet
- Chemistry Project On Estimation of Content of Bone AshDocument13 pagesChemistry Project On Estimation of Content of Bone AshShlok Sah50% (2)
- Topic 5. Bone Microscopic Anatomy and Devt 1Document24 pagesTopic 5. Bone Microscopic Anatomy and Devt 1Janine Jerica JontilanoNo ratings yet
- The Main Functions of BonesDocument9 pagesThe Main Functions of BonesabbaslafeNo ratings yet
- Proteoglycans, Whose Main Glycosaminoglycans Are Chondroitin-4-Sulfate and Chondroitin-6Document14 pagesProteoglycans, Whose Main Glycosaminoglycans Are Chondroitin-4-Sulfate and Chondroitin-6Joseph Enoch ElisanNo ratings yet
- Lec 3 2010 02 6Document8 pagesLec 3 2010 02 6Ras WhoknowsmeNo ratings yet
- Intro Tothe Function of Parathyroid Gland, ConciseDocument34 pagesIntro Tothe Function of Parathyroid Gland, Conciseinka.elseNo ratings yet
- Orthopedic NursingDocument237 pagesOrthopedic Nursingɹǝʍdןnos100% (24)
- Kenkre Bassett 2018 The Bone Remodelling CycleDocument20 pagesKenkre Bassett 2018 The Bone Remodelling Cyclealealer2708No ratings yet
- Bone As A Living Dynamic TissueDocument14 pagesBone As A Living Dynamic TissueSuraj_Subedi100% (6)
- Agents That Affect Bone Mineral Homeostasis: Department of PharmacologyDocument44 pagesAgents That Affect Bone Mineral Homeostasis: Department of Pharmacologymichaelcyl100% (1)
- Physiology of BoneDocument32 pagesPhysiology of BoneAnandhu GNo ratings yet
- Ch07 - EOC - Skeletal SystemDocument4 pagesCh07 - EOC - Skeletal SystemGaveen CoatesNo ratings yet
- Bone: Biology, Harvesting, and Grafting for Dental Implants, 2nd EditionFrom EverandBone: Biology, Harvesting, and Grafting for Dental Implants, 2nd EditionNo ratings yet
- Renal Reflections: Exploring the Marvels of Nephrology: The Intricate Ballet of Kidney Functions UnveiledFrom EverandRenal Reflections: Exploring the Marvels of Nephrology: The Intricate Ballet of Kidney Functions UnveiledNo ratings yet
- Advanced farriery knowledge: A study guide and AWCF theory course companionFrom EverandAdvanced farriery knowledge: A study guide and AWCF theory course companionNo ratings yet
- Rangkuman Week 5 (PBL) - OsteomyelitisDocument9 pagesRangkuman Week 5 (PBL) - OsteomyelitisMaria Dini AdmiratiNo ratings yet
- Rangkuman Week 3 (PBL) - RADocument27 pagesRangkuman Week 3 (PBL) - RAMaria Dini AdmiratiNo ratings yet
- Week 1 HumanAnat&Fisio - 6 Agustus 2012Document17 pagesWeek 1 HumanAnat&Fisio - 6 Agustus 2012Maria Dini AdmiratiNo ratings yet
- Week 3 JointInflammatoryDisease - 27 Agustus 2012Document19 pagesWeek 3 JointInflammatoryDisease - 27 Agustus 2012Maria Dini AdmiratiNo ratings yet
- Week 1 BlockMuscle - 6 Agustus 2012Document21 pagesWeek 1 BlockMuscle - 6 Agustus 2012Maria Dini AdmiratiNo ratings yet
- Week 4 MetabolicBoneDisease - 3 September 2012week 4 MetabolicBoneDisease - 3 September 2012Document16 pagesWeek 4 MetabolicBoneDisease - 3 September 2012week 4 MetabolicBoneDisease - 3 September 2012Maria Dini AdmiratiNo ratings yet
- Week 4 BackBoneAnatomy - 3 September 2012Document20 pagesWeek 4 BackBoneAnatomy - 3 September 2012Maria Dini AdmiratiNo ratings yet
- Bones: A Hard SubjectDocument16 pagesBones: A Hard SubjectMaria Dini AdmiratiNo ratings yet
- Week 2 Blpressoureoduph - 20 Februari 2012week 2 Blpressoureoduph - 20 Februari 2012Document43 pagesWeek 2 Blpressoureoduph - 20 Februari 2012week 2 Blpressoureoduph - 20 Februari 2012Maria Dini AdmiratiNo ratings yet
- Week 4 Embryology Development of Gastrointestinal: DR Marselina TanDocument29 pagesWeek 4 Embryology Development of Gastrointestinal: DR Marselina TanMaria Dini AdmiratiNo ratings yet
- Heat Related Illnesses: Erwin Mulyawan, DR, Span, DpbaDocument42 pagesHeat Related Illnesses: Erwin Mulyawan, DR, Span, DpbaMaria Dini AdmiratiNo ratings yet
- Is An Irregular Shape Cylinder With Narrow Opening Superiorly and A Large Inferiorly OpeningDocument27 pagesIs An Irregular Shape Cylinder With Narrow Opening Superiorly and A Large Inferiorly OpeningMaria Dini AdmiratiNo ratings yet
- Communication Between Nerve Cells.: V. Sutarmo SetiadjiDocument35 pagesCommunication Between Nerve Cells.: V. Sutarmo SetiadjiMaria Dini AdmiratiNo ratings yet
- Laboratory Logistics HandbookDocument96 pagesLaboratory Logistics HandbookMohd Fahmi MastukiNo ratings yet
- POLYSEED Application Procedure 3.15Document2 pagesPOLYSEED Application Procedure 3.15ALVARO ENRIQUE CANTILLO GUZMANNo ratings yet
- Chronic Pain and Road MappingDocument3 pagesChronic Pain and Road MappingkasiaNo ratings yet
- Why Antibiotics Should Not Be Overused. Write A Short Note?Document4 pagesWhy Antibiotics Should Not Be Overused. Write A Short Note?Danger TigerNo ratings yet
- Cauti CDC 2018Document17 pagesCauti CDC 2018NasikhatulNo ratings yet
- FDAR ChartingDocument50 pagesFDAR ChartingNathaniel PulidoNo ratings yet
- Womens - Era July 2017Document148 pagesWomens - Era July 2017taruniNo ratings yet
- Q A Random - 16Document8 pagesQ A Random - 16ja100% (1)
- Traditional Medicine & Herbal TechnologyDocument39 pagesTraditional Medicine & Herbal TechnologyDivyam14No ratings yet
- Ilness and BiomagnetismDocument3 pagesIlness and BiomagnetismSilvia Arias100% (2)
- Oklahoma Commission On Opioid Abuse Final ReportDocument12 pagesOklahoma Commission On Opioid Abuse Final ReportOKCFOXNo ratings yet
- REBTDocument18 pagesREBTGayathree ChandranNo ratings yet
- Cognitive Behaviour Therapy For Depression in Young People Manual For TherapistsDocument120 pagesCognitive Behaviour Therapy For Depression in Young People Manual For TherapistsSundar PrabhuNo ratings yet
- Byproducts From Cassava ProcessingDocument29 pagesByproducts From Cassava ProcessingasokmithraNo ratings yet
- UPSC Medical ScienceDocument7 pagesUPSC Medical ScienceAbhishek JoshiNo ratings yet
- Herbal CosmeticsDocument40 pagesHerbal CosmeticsBiren Shah100% (1)
- PDF DipiroDocument16 pagesPDF DipiroYolandaFandraIINo ratings yet
- Swedish MassageDocument22 pagesSwedish Massagealejandro jean100% (3)
- Swollen Neck Lymph Nodes - Causes - Better MedicineDocument6 pagesSwollen Neck Lymph Nodes - Causes - Better MedicineDanao ErickNo ratings yet
- Starch Industry in IndiaDocument3 pagesStarch Industry in Indiabanapte59No ratings yet
- Leisure Awareness ActivitiesDocument9 pagesLeisure Awareness Activitiesapi-301398957No ratings yet
- The Clinical Management of Awake BruxismDocument30 pagesThe Clinical Management of Awake BruxismSahana RangarajanNo ratings yet
- SPDX Week 8 - Perfusion TechnologyDocument2 pagesSPDX Week 8 - Perfusion TechnologyerikajoydmrmtNo ratings yet
- Koppenaal2020 Article EffectivenessAndCost-effectiveDocument13 pagesKoppenaal2020 Article EffectivenessAndCost-effectivePaulomds1991No ratings yet
- 1-Legal Med Notes PDFDocument19 pages1-Legal Med Notes PDFFrenza Joy FresnidoNo ratings yet
- Super fi cial roughness on composite surface, composite enamel and composite dentin junctions after different fi nishing and polishing procedures. Part I: roughness after treatments with tungsten carbide vs diamond bursDocument20 pagesSuper fi cial roughness on composite surface, composite enamel and composite dentin junctions after different fi nishing and polishing procedures. Part I: roughness after treatments with tungsten carbide vs diamond bursCinthyaNavarroNo ratings yet
- ATI Module - Ethical Principles For Mental HealthDocument6 pagesATI Module - Ethical Principles For Mental HealthChelsea HebertNo ratings yet
- Cholelithiasis When They Are in The Bile CholedocolithiasisDocument15 pagesCholelithiasis When They Are in The Bile Choledocolithiasishisabumohamed100% (1)
- Cai Songfang Wujishi Breathing Exercises Medicine Health Publishing Co. 1994Document119 pagesCai Songfang Wujishi Breathing Exercises Medicine Health Publishing Co. 1994Amlen Singha100% (2)
The Musculoskeletal System
The Musculoskeletal System
Uploaded by
Maria Dini AdmiratiCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
The Musculoskeletal System
The Musculoskeletal System
Uploaded by
Maria Dini AdmiratiCopyright:
Available Formats
THE MUSCULOSKELETAL SYSTEM
References:
Alberts B, Johnson A, Lewis J. Molecular Biology of the Cell, 5th Ed.
Garland Science, 2008.
Harvey RA. Lippincotts Illustrated Reviews Pharmacology, 5th Ed.
Lippincott Williams & Wilkins, 2012.
Longo DL, Kasper DL, Jameson JL. Harrisons Principles of Internal Medicine, 18th Ed.
McGraw-Hill Professional, 2011.
Martini FH, Nath JL, Bartholomew EF. Fundamentals of Anatomy & Physiology,
9th Ed. Benjamin Cummings, 2011.
McKinley M, OLoughlin VD. Human Anatomy, 3rd Ed. McGraw-Hill, 2011.
Saladin KS. Anatomy and Physiology, 5th Ed. McGraw Hill Higher Education, 2009.
Salter RB. Textbook of Disorders and Injuries of the Musculoskeletal System,
3rd Ed. Lippincott Williams & Wilkin, 1999.
Solomon L, Warwick D, Nayagam S. Apleys System of Orthopedics and Fractures,
9th Ed. Hodder Arnold, 2010.
Course duration:
August 6, 2012 September 13, 2012
Content:
Basic Knowledge
Diseases
Anatomy
Kevin Edward Santoso
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
|1
~ BASIC KNOWLEDGE ~
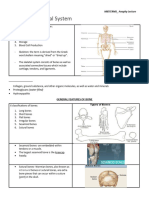
Bone
Five primary functions of the skeletal system
o Provides structural support and a framework for the attachment of tissues and organs
o Storage of minerals and lipids
o Blood cell production
o Protection
o Leverage
Bone structure
o An extended tubular shaft is called the diaphysis
o At each end of the diaphysis, an expanded area is called the epiphysis
o The diaphysis is connected to the epiphysis by an area called the metaphysis
o The diaphysis consists of a layer of compact bone, that is a protective layer that surrounds a central space
called the medullary cavity or marrow cavity
o The epiphysis consists mainly of spongy bone or cancellous or trabecular bone
The composition of bone
Bone consists of matrix that has deposits of minerals and bone cells inside. The matrix also has narrow
passageways called canaliculi that extend between the lacunae and nearby blood vessels, forming networks for the
exchange of nutrients, waste, products, and gases.
Bone Matrix
o Calcium phosphate accounts for almost two-thirds (2/ 3) of the weight of bone
o One-third (1/ 3) of the weight of bone is collagen fibers and bone cells are only weighed about 2 percent of the
total mass of typical bone
Bone Cells
o Bone contains four typical cells: osteocytes, osteoprogenitor cells, osteoblasts, and osteoclasts
o Osteocyte occupies a lacuna between layers of matrix, called lamellae
o Osteocytes have two function:
Maintain the protein and mineral content of the surrounding matrix
Participate in the repair of damaged bone
o Osteoblast produce new bone matrix in a process called ossification or osteogenesis
o They make and release the proteins and other organic components of the matrix (called osteoid before calcium
salts deposited)
o Osteoblasts assist in elevating local concentrations of calcium phosphate triggering the deposition of calcium
salts in the organic matrix
o This process converts osteoid to bone where by then osteocytes are developed from osteoblasts that are
surrounded by matrix
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
|2
o Osteoprogenitor cells are mesenchymal cells that capable to differentiate into osteoblast
o Osteoclasts are cells that remove and recycle bone matrix
o These cells are gigantic with 50 or more nuclei
o Osteoclasts derived from the same stem cell that produce monocytes and macrophages
o Acids and proteolytic enzymes are secreted and used in erosion process called osteolysis or resorption
Compact bone structure
o The units of mature compact bone is the osteon or Haversian system
o In an osteon, the osteocytes are arranged in concentric layers around central canal or Haversian canal
o This canal contains one or more blood vessels that carry blood to and from the osteon
o Central canals generally run parallel to the surface of the bone
o Other passageways, known as perforating canals or Volkmanns canals, extend perpendicular to the surface
o Lamellae around the central canal is surrounded by collagen fibers that adds strength and resiliency
o Interstitial lamellae, which are remnants of osteons whose matrix components have been almost completely
recycled by osteoclasts, fill in the spaces between the osteons in compact bone
Spongy bone structure
o In spongy bone, the matrix forms a meshwork of supporting bundles of fibers called trabeculae
o Spongy bone within the epiphyses of long bones and the interior of other large bones contains red bone marrow
responsible for blood cell formation and may also contain yellow bone marrow which is adipose tissue important
as an energy reserve
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
|3
The periosteum and endosteum
o The superficial layer of compact bone is wrapped by a periosteum, a membrane with a fibrous outer layer and a
cellular inner layer
o The functions of periosteum are:
Isolates the bone from surrounding tissue
Provides a route for the circulatory and nervous supply
Participates in bone growth and repair
o The endosteum, an incomplete cellular layer, lines the medullary cavity
Bone formation and growth Endochondral ossification
See page 9
Bone formation and growth Intramembranous ossification
See page 10
Bone resorption
o This process is carried out by the osteoclasts under the influence of osteoblasts and both local and systemic
activators
o The differentiation of osteoclast progenitor cells into activated osteoclast needs several factors including PTH,
glucocorticoids or pro-inflammatory cytokines
o RANKL has to bind with RANK receptor on the osteoclast precursor in the presence of macrophage colonystimulating factor (M-CSF) before full maturation and osteoclastic resorption can begin
o Initially osteoblasts are believed preparing the site of resorption by removing osteoid
o Osteoclasts then are activated and start to secrete hydrochloric acid and proteolytic enzymes
o Calcium and phosphate ions are then absorbed by osteoclasts which will travel into the blood stream
Bone modeling and remodeling
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
|4
Mineral deposition and resorption
o Mineral deposition is a crystallization process in which calcium, phosphate, and other ions are taken from the
blood plasma and deposited in bone tissue
o The crystals are mainly in the form of hydroxyapatite
o Mineral resorption is the process of dissolving bone
Calcium homeostasis
o 99% of calcium in the body is stored at the bone
o The function of calcium consists of: 1) controls internal regulation of the function of all cells, 2) regulates cell
membrane permeability, nerve excitability, muscle contraction, and gland secretion, 3) extracellular
calcium ion concentration regulates synthetic and secretory function of parathyroid gland (for PTH) and
thyroid C cells (for calcitonin), 4) controls adhesiveness between cells, and 5) controls the hardness and
rigidity of bones and teeth through hydroxyapatite
o The normal concentration of calcium in the blood plasma is 9.2 to 10.4 mg/ dL
o Hypocalcemia, the condition where the calcium level is lower than normal, causes excessive excitability of the
nervous system and leads to muscle tremors, spasms, or tetany
o Whereas hypercalcemia, the condition where the level of calcium is higher than normal, causes less excitability
of nerve and muscle cells leads to depression of the nervous system, emotional disturbances, muscle weakness,
etc
Calcitriol
o Is a form of vitamin D produced by the sequential action of the skin, liver, and kidneys
o It raises the calcium concentration in the blood in three ways: 1) increases calcium absorption by the small
intestines, 2) increases calcium resorption from the skeleton, 3) increases calcium absorption by the
small intestine, and 4) promotes the reabsorption of calcium ions by the kidneys, so less calcium is lost in
the urine
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
|5
Calcitonin
o Is secreted by C cells of the thyroid gland
o Secreted when the blood calcium concentration rises too high
o It lowers the concentration of blood calcium by two principal mechanism: 1) osteoclast inhibition and 2)
osteoblast stimulation
Parathyroid hormone (PTH)
o On the renal tubules, PTH increases phosphate excretion by restricting its reabsorption and decreases calcium
reabsorption
o On kidney parenchyma, PTH controls hydroxylation of the vitamin D metabolite 25-OHD; a rise in PTH
concentration stimulates conversion to the active metabolite 1, 25-(OH)2D and a fall in PTH causes a switch
towards the inactive metabolite 24, 25-(OH)2D
o In the intestine, PTH has the indirect effect of stimulating calcium absorption by promoting the conversion of 25OHD to 1, 25-(OH)2D in the kidney
o In bone PTH acts to promote osteoclastic resorption and the release of calcium and phosphate into the blood
Phosphate homeostasis
o 85% of the total phosphate in the body are stored in the bone
o The normal level of phosphate is 2.8 to 4.0 mg/ dL
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
|6
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
|7
Articulations
Joints according to their range of motion
o Based on their range of motion (ROM), joints are categorized into three major groups: 1) synarthrosis, 2)
amphiarthrosis, and 3) diarthrosis
o Synarthrosis is an immovable joint; it can be fibrous or cartilaginous and over time the two bone may fuse
o Amphiarthrosis is a slight movable joint; it can be either fibrous or cartilaginous
o Diarthrosis is a freely movable joint or synovial joint and subdivided according to the movement
Synovial joints
o They are surrounded by two-layered joint capsule or known as articular capsule
o The inner layer is called the synovial membrane and the outer layer is called the fibrous capsule
o The major features of synovial joints are: 1) articular cartilage, 2) synovial fluid, and 3) accessory structures
Articular cartilages
o They have the same structure as hyaline cartilage
o But, they do not have perichondrium and the matrix contains more water than that of other cartilages
o The surfaces are smooth and slick which can reduce during movement
o If pressure applied to the joint, each articular cartilage surfaces from two bone will not meet each other because
of synovial fluid in the middle of the structure
o This fluid acts as lubricant that is minimizing friction
o However, if damages, the function is discontinued
o The exposed articular cartilage (caused by damages) will produce matrix and change from slick, smooth-gliding
surface to rough abrasive surface of collagen fibers
o This new rough surface will increases friction at the joint
o In detail, articular cartilages consist of a large extracellular matrix (ECM) with chondrocytes sparsely distributed
(approx. 10% of the total wet weight)
o The principal components of ECM include water (65% to 80% of total weight), proteoglycans (aggrecan, 4% to
7% of the total weight), and collagens (primarily type II, 10% to 20% of the total weight), with other proteins and
glycoproteins in lesser amount
o Most water fill in the molecular pore space of the ECM and concentrated at the surface and is partly responsible
for joint lubrication
o Proteoglycans are large, complex macromolecules and consist of protein core with extensive polysaccharide
(glycosaminoglycan) chains linked to this core
o The role of proteoglycan is to bind water and enable cartilage to withstand large compressive loads
o Collagens (mainly type II) are distributed throughout cartilage, with fibril size and concentration varies
o Collagen provides cartilage the tensile strength need to withstand shear forces
o Articular cartilage is further subdivided into four distinct zones: superficial, transitional, deep, and calcified
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
|8
Zone
Chondrocyte
Collagen
Proteoglycan
Water
Properties
Superficial
Elongated in
shape, horizontal
to surface
Thin, parallel
to surface,
compact
Lowest
concentration
Highest
concentration
- Low fluid
permeability
- Provides resistance
to shear forces
- Secretes lubricating
proteins
- Thinnest zone
Transitional
Oblique shape,
randomly
distributed,
sparse
Large
diameter,
less
organized
Highest
Lowest
- Less stiff that
superficial zone
- Distributes
compressive loads
to subchondral
bone
Spherical shape,
arranged in
columns
Perpendicular
to surface,
extending
into calcified
zone
Deep
Tidemark
calcified
Separates deep zone (cartilage) from calcified zone (subchondral bone)
Small cells in cartilaginous matrix with apatitic salts
Collagen fibers from deep zone penetrate calcified cartilage
- Anchors cartilage to
subchondral bone
- Partially calcified
The
Musculoskelet al
Bone formation and growth Endochondral ossification
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
|9
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 10
Bone formation and growth Intramembranous ossification
Synovial fluid
o Two cell types present in the synovial tissue: synoviocytes type A and synoviocytes type B
o Type A cells (macrophagic cells) are non-fixed cells that can phagocytose actively cell debris and wastes in
joint cavity
o Type B cells (fibroblast-like cells) are characterized by the rich presence of rER; they are involved in the
production of synovial fluid
o Normal synovial fluid contains hyaluronan (hyaluronic acid), glucorinic acid and acetylglucosamine
o Hyaluronan is synthesized by synovial membrane and secreted into the joint cavity to increase the viscosity
and elasticity of articular cartilages and to lubricate the surfaces between synovium and cartilage
o Synovial fluid also contains lubricin secreted by synovial cells that is responsible as boundary-layer lubrication
o Synovial fluid has three primary function:
1. Lubrication articular cartilages act like sponges filled with synovial fluid, when part of an articular cartilage is
compressed, some of the synovial fluid is squeezed out of the cartilage; and when the compression stops,
synovial fluid is pulled back into the articular cartilages
2. Nutrient distribution synovial fluid in a joint circulate continuously to provide nutrients and a waste
disposal route for chondrocytes of the articular cartilages; it circulates whenever the joint moves, and the
compression and the re-expansion of the articular cartilages; as the synovial fluid flows through the areolar
tissue of the synovial membrane, waste products are absorbed and additional nutrients are obtained by
diffusion across capillary walls
3. Shock absorption.- synovial fluid cushions joints that are subjected to compression from shocks; then the
pressure across a joint suddenly increases, the resulting shock is lessened as synovial fluid spread across the
articular surfaces and outward to the articular capsule
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 11
Accessory structures
o Synovial joints have a variety of accessory structures: 1) cartilage and fat pads, 2) ligaments, 3) tendons, and 4)
bursae
o Menisci and fat pads lie between the opposing articular surfaces
o A meniscus is a fibrocartilage pad, known as articular disc channels the flow of synovial fluid and allow the
variation in the shapes of the articular surfaces
o Fat pads are adipose tissue covered by a layer of synovial membrane; they protect the articular cartilages
o Ligaments support, strengthen, and reinforce synovial joints; in a sprain, a ligament is stretched to the point
at which some of the collagen fibers are torn, but the ligament as a whole survives and the joint is not damaged
o Tendons passing across the joint may limit the range of motion and provide mechanical support
o Bursae are small pockets that contain synovial fluid and are lined by a synovial membrane; they can be
connected to the joint cavity or separate from it; they form where a tendon or ligament rubs against other tissue
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 12
Synovial fluid analysis
Laboratory testing
o Volume normal up to 4 mL of fluid
o Color and clarity normal is colorless and clear; RA shows rice bodies synovial fluid
o Viscosity normal is very viscous due to hyaluronate; normally is defined by string test (< 3 cm is low viscosity)
o Clotting presence of fibrinogen shows damage to the synovial membrane
o Mucin clot the test is known as Ropes test, is the estimation of the integrity of the mucin; normal forms a tight
ropy clot upon the addition of acetic acid
Chemical examination
o Protein normal is 1 3 g/ dL; increase may indicate ankylosing, spondyloitis, arthritis, arthropaties that
accompany Crohn disease, gout, psoriasis, Reiter syndrome, and ulcerative colitis
o Glucose normal is < 10 mg/ dL
o Uric acid normal is 6 8 mg/ dL
o Lactic acid normal is < 25 mg/ dL (useful for septic arthritis)
o Lactate dehydrogenase increases in RA, infectious arthritis, and gout
o Rheumatoid factor (RF) is an antibody to immunoglobulins
Microscopic examination
o Normal contains small numbers of lymphocytes and only a few neutrophils
o WBC count ranges from 0 150 cells per microliter; with mean distribution neutrophils 7%, lymphocytes 24%,
monocytes 48%, macrophages 10%, and synovial lining cells 4%
o Septic arthritis displays a high number of neutrophils; LE cells, that are neutrophils that have engulfed a nucleus
of a lymphocyte that has been altered by antinuclear antibody (ANA), are seen in SLE; Reiter cells may be
present as the indication of Reiters syndrome
o Crystal can be found in gout and pseudogout; gout shows monosodium urate crystal whereas pseudogout
displays calcium pyrophosphate dehydrate (CPPD) crystals
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 13
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 14
Types of synovial joints
o Six types of synovial joints: 1) plane/ planar/ gliding joints, 2) condylar/ condyloid/ ellipsoid joints,, 3) saddle joints,
4) hinge joints, 5) pivot joint, and 6) ball-and-socket joints
o Gliding joints are known as uniaxial joints because only side to side movements are possible; the articular
surfaces of the bones are flat or planar; for example: intercarpal and intertarsal joints (between the cube-shaped
carpal and tarsal bones)
o Condylar joints are biaxial joints (a joint moves in two planes or axes) with an oval, convex surface on one
bone that articulates with a concave articular surface on the second bone; able to move back-and-forth and sideto-side; for example: metacarpophalangeal (MP) joints of the finger 2 through 5
o Saddle joints allow greater range of motion; the articular surfaces of the bones have convex and concave
regions that resemble the shape of saddle; for example: carpometaphalangeal joint of the thumb (between
trapezium and the first metacarpal)
o Hinge joints are uniaxial joints in which the convex surface of one articulating bone fits into a concave
depression on the other bone; movement like a hinge of a door; for example: the elbow joint
o Pivot joints are uniaxial joints in which one articulating bone with a rounded surface fits into a ring formed by a
ligament and another bone; the first bone rotates on its longitudinal axis relative to the second bone; for example:
the proximal radioulnar joint and the atlantoaxial joint
o Ball-and-socket joints are multiaxial joints in which the spherical articulating head of one bone fits into the
rounded, cup-like socket of a second base; for example: the hip joint and the glenohumeral joint
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 15
Joint lubrication
o Boundary layer lubrication at the bearing surface is mediated by a large, water soluble glycoprotein fraction,
lubricin, in the viscous synovial fluid
o This layer attaches to each articular surface
o Fluid film lubrication is provided by hydrodynamic mechanism
o This lubrication consist of fluid that is squeezed out of the proteoglycan-rich cartilage during movement and
loading and seeps back into the cartilage when loading ceases
o Lubrication between synovial folds is provided by hyalurinate molecules in the synovial fluid
Collagen
o A family of fibrous protein
o It is typically long, stiff, triple-stranded helical structure and rich in proline and glycine
o There are many types of collagen: collagen type I is under the fibril-forming collagen and can be found in the
bone, skin, tendons, ligaments, cornea, internal organs; collagen type II is under the fibril-forming collagen and
can be found in cartilage, intervertebral disc and notochord
o The synthesis of collagen
Muscle Tissue
Six primary functions of the skeletal muscle
o Produce skeletal movement
o Maintain posture and body position
o Support soft tissue
o Guard entrances and exits
o Maintain body temperature
o Store nutrient Reserves
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 16
Skeletal muscle fibers
The sarcolemma and transverse tubules
o The sarcolemma or the plasma membrane of a muscle fiber surrounds the sarcoplasm, or cytoplasm of the
muscle fiber
o Sarcolemma has a characteristic of distributing transmembrane potential due to uneven membrane potential
which is very crucial in muscle contraction
o In order for the potential to be distributed evenly to a whole region of the skeletal muscle fiber, the signal is
conducted through the transverse tubules or T tubules
o These tubules are narrow tubes that are continuous with the sarcolemma and extend deep into the sarcoplasm
Myofibrils
o Myofibrils are the small units of skeletal muscle fiber, which can actively shorten and are responsible for muscle
fiber contraction
o Myofibrils consists of myofilaments, thin filaments (actin), thick filaments (myosin), and elastic filaments
(titin)
The sarcoplasmic reticulum
o Sarcoplasmic reticulum (SR) is similar to endoplasmic reticulum of other cells, which is a tubular network around
each individual myofibril
o T tubules are always bind to the membrane of SR
o The tubules of the SR enlarge, fuse, and form expanded chambers called terminal cisternae
o The combination of two terminal cisternae plus a T tubule is known as a triad
o This SR is very important in the muscle contraction in releasing calcium ions into the sarcoplasm and in the
muscle relaxation in absorbing calcium ions back
Sarcomeres
o They are the smallest functional units of the muscle fibers
o A sarcomere contain: thick filaments, thin filaments, protein that stabilize the positions of the thick and thin
filaments, and proteins that regulate the interactions between thick and thin filaments
o Each sarcomere has dark bands called A bands and light bands called I bands
o The A band consists of three subdivisions: 1) the M line, the protein of the M line connect the central portion of
each thick filaments to neighboring thick filaments; 2) the H band, contains thick filaments but no thin
filaments; and the zone of overlap, is a dark region where thin filaments are located between the thick filaments
o The I band consists of thin filaments but not thick filaments and extends from the A band of one sarcomere to the
A band of the next sarcomere; Z lines mark the boundary of two adjacent sarcomeres and consist of proteins
called actinins; strands of titin extend from thick filaments to Z line which helps thick and thin filaments in
their position and aids in restoring resting sarcomere length after contraction
o Thin filaments contains four proteins: F-actin, nebulin, tropomyosin, and troponin; F-actin composed of
hundreds of G-actin which is the active sites of the myosin; strands of the tropomyosin and a troponin are forming
a troponin-tropomyosin complex that covers the active sites during rest; in contraction, high concentration of
calcium ion will change the position of this complex and expose the active site
o Thick filaments contains many myosin heads; by the addition of ATP, the heads will project out and bind to the
active sites of the thin filaments resulting a muscle contraction
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 17
Muscle contractions
Isotonic contractions
o In this contraction, tension rises and the skeletal muscles length changes
o Two types of isotonic contraction: concentric and eccentric contractions
o In concentric contraction, the muscle tension exceeds the load and the muscle shortens
o Whereas in eccentric contraction the muscle tension is less than the load and the muscle elongates
Isometric contraction
o In this contraction, the muscle as a whole does not change length and the tension produced never exceeds the
load
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
Skeletal muscle innervation
Vesicles.
ACh
Arriving action
potential
The synaptic cleft, a
narrow space,
separates the
synaptic terminal of
the neuron from the
opposing motor end
The cytoplasm of the synaptic terminal contains
vesicles filled with molecules of acetylcholine, or
ACh. Acetylcholine is a neurotransmitter, a chemical
released by a neuron to change the permeability or
other properties of another cells plasma
membrane. The synaptic cleft and the motor end
plate contain molecules of the enzyme
acetylcholinesterase (AChE), which breaks down
ACh.
ACh molecules diffuse across the synaptic cleft and
bind to ACh receptors on the surface of the motor end
plate. ACh binding alters the membranes
permeability to sodium ions. Because the
extracellular fluid contains high concentration of sodium
ions, and sodium ion concentration inside the cell is
very low, sodium ions rush into the sarcoplasm
The stimulus for ACh release is the arrival
of an electrical impulse, or action potential,
at the synaptic terminal. An action
potential is a sudden change in the
transmembrane potential that travels along
the length of the axon.
Motor end
plate
When the action potential reaches the neurons
synaptic terminal, permeability changes in the
membrane trigger the exocytosis of ACh into the
synaptic cleft. Exocytosis occurs as vesicles fuse
with the neurons plasma membrane.
Action
potential
The sudden inrush of sodium
ions results in the generation
of an action potential in the
sarcolemma. AChE quickly
breaks down the ACh on the
motor end plate and in the
synaptic cleft, thus inactivating
the ACh receptor sites.
| 18
The
Musculoskelet al
S y s t e m
The contraction cycle
Contraction Cycle Begins
The contraction cycle,
which involves a series of
interrelated steps, begins
with the arrival of calcium
ions within the zone of
overlap.
Myosin Reactivation
Myosin reactivation
occurs when the free
myosin head splits ATP
into ADP and P. The
energy released is used
to recock the myosin
head.
Active-Site Exposure
Cross-Bridge Detachment
Calcium ions bind to
troponin, weakening the
bond between actin and
the troponin-tropomyosin
complex. The troponin
molecule then changes
position, rolling the
tropomyosin molecule
away from the active sites
on actin and allowing
interaction with the
energized myosin heads.
When another ATP binds to
the myosin head, the link
between the myosin head
and the active site on the
actin molecule is broken.
The active site is now
exposed and able to form
another cross-bridge.
Cross-Bridge Formation
Myosin Head Pivoting
Once the active sites are
exposed, the energized
myosin heads bind to
them, forming cross
bridges.
After cross-bridge
formation, the energy that
was stored in the resting
state is released as the
myosin head pivots
toward thee M line. This
action is called the power
stroke; when it occurs, the
bound ADP and
phosphate group are
released.
2012 Kevin Edward Santoso. All Rights Reserved
| 19
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
The relaxation
o The duration of contraction depends on 1) the period of stimulation at the neuromuscular junction, 2) the
presence of free calcium ions in the sarcoplasm, and 3) the availability of ATP
| 20
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 21
Types of skeletal muscle fibers
o The human body has three major types of skeletal muscle fibers: fast fibers, slow fibers, and intermediate
fibers
o Fast fibers are large in diameter and contain densely packed myofibrils, large glycogen reserves, and relatively
few mitochondria; they produce powerful contraction but use ATP in massive amount
o Slow fibers are specialized to continue contracting long after a fast fiber would have become fatigue; they have
more extensive network of capillaries and red pigment myoglobin that can bind oxygen
Physical conditioning
o Is used to improve both power and endurance
o Anaerobic endurance is the length of time muscular contraction can continue to be supported by glycolysis and
by the existing energy reserves of ATP and creatine phosphate (CP)
o Anaerobic endurance improves an individuals power but it is limited by 1) the amount of glycogen available for
breakdown, 2) the amount of ATP and CP available, and 3) the ability of muscle to tolerate the lactic acid
generated during the anaerobic period
o Athletes training to improve this endurance perform frequent, brief, extensive workouts that stimulate muscle
hypertrophy
o Aerobic endurance is the length of time a muscle can continue to contract while supported by mitochondrial
activities
o This does not promote muscle hypertrophy; aerobic endurance improves an individuals ability to continue an
activity for longer period of time; this endurance does not require activities that reach peak tension production
o Improvements in aerobic endurance result from two factors: 1) alteration in the characteristics of muscle fibers, 2)
improvement in cardiovascular performance
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 22
~ DISEASES ~
Fractures
Gustilo open fracture classification
o Type I small wound, clean, little soft tissue damage with no crushing, the fracture is not comminuted
o Type II more than (>) 1 cm long, no skin flap, not much soft tissue damage, moderate crushing and
comminution
o Type III large laceration, extensive damage to skin and soft tissue, vascular compromise, contamination
o Type III A Type III fracture with soft tissue coverage of the fractured bone, despite extensive laceration, flaps,
high energy trauma
o Type III B Type III fracture with extensive injury to or loss of soft tissue, periosteal stripping, exposure of bone,
massive contamination, severe comminution
o Type III C Type III fracture with open fracture, arterial injury
Salter Harris classification
o Type 1 a transverse fracture through the hypertrophic or calcified zone of the plate; the growing zone of the
physis is usually not injured and growth disturbance is uncommon
o Type 2 similar to type 1, but towards the edge the fracture deviates away from the physis and splits off a
triangular metaphyseal fragment of bone
o Type 3 a fracture that splits the epiphysis and then veers off transversely to one or the other side, through the
hypertrophic layer of the physis; damages the growth zone and may cause growth disturbance
o Type 4 as with type 3, the fracture splits the epiphysis, but it extends into the metaphysis; resulting in
asymmetrical growth
o Type 5 a longitudinal compression injury of the physis; no visible fracture but the growth is crushed and may
result in growth arrest
X-ray
o Rule of twos: two views, two joints, two limbs, two injuries, and two occasions
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 23
Healing of fracture
o In fracture many blood vessels are damaged; a large blood clot, or fracture hematoma, soon closes off the
injured vessels and leaves a fibrous meshwork in the damaged area; the disruption of circulation kills osteocytes
around the fracture; dead bone extends along the shaft
o The cells of the intact endosteum and periosteum undergo rapid cycles of cell division and the daughter cells
migrate into the fracture zone; an external callus formed; internal callus organizes within the medullary cavity
and between the broken ends of the shaft; at this point the broken ends have been temporarily stabilized
o Osteoblasts replace the central cartilage with spongy bone; external and internal callus fuse and form an
extensive and continuous brace at the fracture site
o Osteoclasts and osteoblasts continue to remodel the region of fracture
Treatment of closed fracture
o Reduction is aiming for adequate apposition and normal alignment of the bone fragments; two methods of
reduction: closed reduction and open reduction
o Closed reduction can be done in three steps: 1) the distal part of the limb is pulled in the line of the bone, 2)
fragments are repositioned, and 3) alignment is adjusted in each plane
o This method is most effective when the periosteum and muscles on one side of the fracture remain intact
o Open reduction is applied if the closed reduction failed
o Hold reduction is another method that restrict the movement; the available methods of hold reduction are:
continuous traction, cast splintage, functional bracing, internal fixation, and external fixation
Complications of fractures
o Early complication can occur in few days or weeks; the complications may start from visceral injury, nerve injury
to compartment syndrome, gas gangrene and blisters
o Compartment syndrome is a situation where there is an increase in the pressure within one of the osseofascial
compartments; there is reduced capillary flow that may result in ischemia, further edema and lead to greater
increased in internal pressure
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 24
o The clinical feature of this syndrome is usually 5Ps: pain, paraesthesia (sensation of tingling, burning, pricking,
or numbness), pallor, paralysis, and pulselessness; other features are the affected muscle is highly sensitive to
stretch therefore
o Late complication may occur in many ways such as: delayed union, non-union, malunion, avascular necrosis,
growth disturbance, bed sores, and muscle contracture
o Delayed union can be caused by inadequate blood supply, severe soft tissue damage, periosteal stripping,
imperfect splintage, over-rigid fixation, and infection
o Non-union has to be related to four question that consist of contact?, alignment?, stability?, and stimulation?
o Muscle contracture may develop after the compartment syndrome or arterial injury
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 25
Osteomyelitis
Acute hematogenous osteomyelitis
o S. aureus is the most causative organism for acute hematogenous osteomyelitis
o Initially the mechanism of the disease is characterized by early inflammation with hyperemia and edema in the
cancellous bone and marrow of the metaphyseal region; as the formation of bone is rigid, edema causes high
interosseous pressure that gives local pain as the clinical feature; pus forms and further increases the local
pressure which adversely affect local circulation; this results in vascular thrombosis and bone necrosis
o This initial destruction and necrosis leads to further osteolysis of the bone; further damaged vessels leads to
septicemia that results in malaise, anorexia, and fever as the features
o As the interosseous pressure increases further, the bone maintains the pressure by loosening the periosteum
from the bone; this will result in exquisite local tenderness; further in few days, the infection will produce
cellulitis and eventually a soft tissue abscess; if the metaphyseal site of the joint is covered by the synovial
capsule like hip, the infection may result in septic arthritis
o Normally prerequisite infection can be found either in the skin or in the upper respiratory tract; most affected
child will complain a constant pain near the end of the involved long bone accompanied by local tenderness
and unwillingness to use limb; within 24 hours the features of septicemia is more indicated such as malaise,
anorexia and fever
o Complications of acute hematogenous osteomyelitis consists of early and late complications; early complications
may include death from septicemia, abscess formation, and septic arthritis; late complications may include
chronic osteomyelitis, pathological fracture, joint contracture, and local growth disturbance
Chronic hematogenous osteomyelitis
o This complication may be caused by failure in treating the acute hematogenous osteomyelitis or failure in
providing the right antibiotics for the treatment
o The bacterial infection of the bone remains the same and capable of living in the haversian canal; this has to be
eliminated by natural process through an opening in the involucrum and through a sinus track or by surgical
removal (sequestrectomy)
Tuberculous osteomyelitis
o The disease is initiated by slowly progressive bone destruction in the anterior part of a vertebral body and is
accompanied by regional osteoporosis; spreading caseation prevent reactive new bone formation; at the
same time it renders segments of bone avascular and producing tuberculous sequestra particularly in the thoracic
region
o The granulation tissue penetrates the thin cortex of vertebral body producing abscess; the infection spreads
longitudinally and affects ligaments and intervertebral discs
o The patients are usually children who come with back pain and are reluctant to sit up, stand up, or bend forward
(the features are similar to hematogenous osteomyelitis of the spine); there is a local deep tenderness and
protective muscle spasm; tuberculin skin test result is positive and ESR is elevated
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 26
Arthritis
Acute septic (pyogenic) arthritis
o Is associated with hematogenous osteomyelitis
o Mostly caused by the spread of pyogenic bacteria from hematogenous osteomyelitis in the metaphysis directly
into the joint
o The infection is serious because of the purulent exudate that rapidly digests articular cartilage
initial cartilage
destruction includes
enzymatic digestion of
the matrix by
lysosomal enzymes
from both PMN
leukocytes and
bacteria
collagen fibers lose
their support and the
cartilage disintegrates
granulation tissue may
cover the articular
cartilage (pannus),
blocking its nutrition
from synovial fluid and
leading to more
destruction
the synovial
membrane becomes
grossly swollesn, filled
with pus, the fibrous
capsule softens and
stretches
continuity may result is
pathological
dislocation, increasing
intra-articular fluid
pressure that results in
avascular necrosis
and in infant the
subchondral bone may
be destroyed
o The clinical features in infant may result in pseudoparalysis, fever and elevation of the WBC whereas in
adults, severe local pain, worse with movement, muscle spasm, effusion, fever and elevated WBC
o Treatment can be done by giving antibiotics or surgical operation and further saline and antibiotics treatment
Rheumatoid arthritis
o APC molecule activate T-helper cell which then activate B cell and T effector cell
o B cell will produce rheumatoid factor (RF) and CCP
o T effector cells are macrophage that will secrete inflammatory signal such as TNF , IL-1, and IL-6; TNF
upregulates adhesion molecules on endothelial cells, promotes influx of leukocytes to the synovial,
activates fibroblasts, stimulates angiogenesis, promotes pain, and drives osteoclastogenesis
o Fibroblasts are capable to secret MMP and proteases for articular cartilage breakdown and secretes/ activates
RANKL for the formation of osteoclasts with GM-CSF that is regulated by OPG
o The pathology of RA can be divided into four stages: 1) pre clinical indicated by increased in ESR, CRP, and
RF; 2) synovitis indicated infiltration of plasma cells and lymphocytes, angiogenesis swollen, and feeling pain; 3)
destruction indicated by persistent inflammation and tendon destruction; and 4) deformity indicated by
combination of many destructions
o Most common joints involved are those of the hands, wrists, knees, elbows, feet, shoulders, and hips; the hands
are at the MCP joints, PIP joints, and MTP joints; systemic manifestations such as malaise, fatigue, weight
loss, high fever, anemia, and weakness; early phase may be indicated by vague pain and stiffness of
involved joints, most noticeable in the morning (morning stiffness); may result in muscle spasm, muscle
atrophy, joint subluxation or dislocation, and ligament contracture
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 27
o Radiographic examination result in periarticular soft tissue swelling and joint effusion, regional osteoporosis,
erosions in subchondral bone, narrowing of the cartilage space, and subluxation or dislocation
o Laboratory findings are elevated ESR, C-reactive protein, and fibrinogen due to anemia, elevated RF
o Treatment can be therapeutic drugs such as using NSAIDs, DMARDs, and corticosteroids
NSAID (Non Steroidal Anti Inflammatory Drugs)
o Various inflammatory mediators such as prostaglandins, leukotrienes and thromboxanes are derive from
phospholipids via cyclo oxygenase (COX) and lipo oxygenase pathways
o NSAIDs have their anti inflammatory capability by inhibiting the COX pathway and hence the synthesis of
prostaglandins
o Two isoforms of the COX enzyme have been described: COX-1 and COX-2
o COX-1 is expressed in most tissues; described as a housekeeping enzyme, regulating normal cellular
processes (such as gastric cytoprotection, vascular homeostasis, platelet aggregation, and kidney function), and
is stimulated by hormones or growth factors
o COX-2 is usually undetectable in most tissues; the expression is increased during states of inflammation; as an
example, growth factors, IL-1 stimulate the xpression of COX-2 in fibroblasts, while endotoxin serves the same
function in monocytes/ macrophages
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 28
Aspirin and other salicylic acid derivatives
o Aspirin is producing salicylate, which has anti-inflammatory, antipyretic, and analgesic effects; this can be done
by blocking the prostaglandin synthesis at the thermoregulatory centers in the hypothalamus and at peripheral
target sites; also increase the prevention of pain receptors to both mechanical ad chemical stimuli
o The adverse effects are epigastric distress, nausea, and vomiting
Propinoic acid derivatives
o E.g. Ibuprofen, naproxen, fenoprofen, ketoprofen, flurbiprofen, and oxaprozin
o The mechanism of action is mostly similar to aspirin
o However, this is used for chronic treatment of RA and OA, because the GI effects are generally less intense than
those of aspirin
o Common adverse effects are GI, ranging from dyspepsia to bleeding and CNS such as headache, dizziness
Acetic acid derivatives
o E.g. Indomethacin, sulindac, and etodolac
o Indomethacin is useful in the treatment o acute gouty arthritis
Oxicam derivatives
o E.g. piroxicam and meloxicam
Fenamates derivatives
o E.g. mefenamic acid and meclofenamate
o Side effects may occur such as diarrhea, bowel inflammation, and hemolytic anemia
Celecoxib
o COX-2 inhibitor
DMARD (Disease Modifying Antirheumatic Agents)
Methotrexate
o Slows the appearance of new erosions within involved joints on radiographs
o Usually the effect starts within 3 to 6 weeks of starting treatment
o Most common side effects are mucosal ulceration and nausea; chronic administration may result in cytopenias,
cirrhosis of the liver, and an acute pneumonia-like syndrome
Leflunomide
o Is an immunomodulatory agent that preferentially causes ell arrest of the autoimmune lymphocyte through its
action on DHODH
o DHODH is necessary for pyrimidine synthesis; reducing pain and inhibit osteoclast production
o Adverse effects are headache, diarrhea, and nausea
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 29
Hydroxychloroquine
o Often combned with methotrexate; used alone does not slow joint damage
o May result in ocular toxity, retinal damage and corneal deposits, CNS disturbances, GI upsets, and skin
discoloration and eruption
Sulfasalazine
D penicillamine
Gold salts
Azathioprine
Cyclophosphamide
Adrenal hormones
o Cortex are divided into adrenocorticosteroids (e.g. glucocorticoids and mineralcorticoids) and adrenal androgens
o Glucocorticoids are diurnal, it reaches the peak in the morning, levels out and increases again in the late
afternoon
o Function of glucocorticoid include: 1) promote normal intermediary metabolism, 2) increase resistance to stress,
3) alter blood cell levels in plasma decreasing white blood cells and increasing red blood cells, 4) anti I
inflammatory action, and 5) endocrine system
o Mineralcorticoids help to control bodys water volume and concentration of electrolyte (sodium and potassium)
Gout arthritis
o Caused by the sudden deposition of sodium monourate crystals in the synovial membrane and therefore
represent a type of crystal-induced arthritis
o Leukocytes phagocytose the crystals and then disintegrate, releasing lysosomal enzymes that produce and acute
and severe local inflammation
o Acute gouty arthritis are usually monoarticular which attacks the MTP joint of the great toe (podagra); followed by
joint pain, swelling, and stiffness
o The laboratory finding may indicate an elevation of uric acid; adult male normal value 6 mg/ 100 mL and adult
women 5.5 mg / 100 mL
o Treatment of acute gouty arthritis is colchicine that is specific for the severe pain relieved; indomethacin can
also be the pharmacological treatment; or else the patient may be restricted from purine-rich foods such as
liver, kidney, and sweetbreads
o For the chronic gout and chronic gouty arthritis, uricosuric drugs may be applied; the function is to increase the
urinary excretion of uric acid and blocking its reabsorption in the renal tubules
o At present the drug of choice is allopurinol as a uric acid-lowering agent, which helps to inhibit the production of
uric acid
Calcium pyrophosphate dehydrate arthropathy (pseudogout)
o Three conditions: 1) chondrocalcinosis, the appearance of calcific material in articular cartilage and menisci; 2)
pseudogout, a crystal induced synovitis; and 3) chronic pyrophosphate arthropathy, a type of degenerative
joint disease polyarticular arthritis affecting large joints, stiffness, joint crepitus, and joint swelling
o CPPD crystal deposition is known to occur in certain metabolic disorders that cause a critical change in ionic
calcium and pyrophosphate equilibrium in cartilage
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 30
Osteoarthritis
o Loss of proteoglycan and defects appear in the cartilage
o As the cartilage becomes less stiff, secondary damage to chondrocytes may cause release of cell enzymes and
further matrix breakdown
o Cartilage deformation may also add to the stress on the collagen network
o Thus amplifying the change in a cycle that leads to tissue breakdown
o When the cartilage has lost its integrity , the forces are concentrated in the subchondral bone
o As a result focal trabecular degeneration and cyst formation, as well as increased vascularity and reactive
sclerosis in the zone of maximal loading
o The remaining cartilage undergoes a normal growth and ossification which gives rise to the bony excrescences,
or osteophytes
o The cardinal features are: 1) progressive cartilage destruction; 2) subarticular cyst formation; 3) sclerosis of the
surrounding bone; 4) osteophyte formation; and 5) capsular fibrosis
o Initially the cartilaginous and bony changes are confined to the most heavily loaded part
o The changes are presented as a cartilage softening or chondromalacia
o With progressive destruction on the cartilage, some areas are exposed and at the edges of the joint there is
remodeling and growth of osteophytes
o Beneath the damaged cartilage the bone is dense and sclerotic
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 31
o Usually patients come with pain that arises from bone and from the synovial membrane, fibrous capsule, and the
spasm of surrounding muscles; pain is aggravated by movement and relieved by pain; joint movement is no
longer smooth and associated with joint crepitus; joint loses its movement; physical examination shows swelling
of the involved joint
Osteoporosis
o Osteoporosis is defined as a generalized bone disease that characterized by a combination of decreased
osteoblastic formation of matrix and an increased osteoclastic resorption of bone
o It may be categorized into four: 1) hormonal osteoporosis (endocrine osteoporosis), 2) disuse osteoporosis, 3)
postmenopausal and senile osteoporosis
o Bone remodeling has two functions which are for repair and calcium supply; the increase of osteoclasts resulted
by low calcium intake
o The low calcium ions concentration in serum results in high PTH and vitamin D which stimulates more
osteoclastogenesis
o Whereas in postmenopausal, loss of estrogen give production of RANKL and loss of OPG which reducing the life
span of osteoblast and stimulate osteoclastogenesis
Ankylosing spondylitis
o Is a form of chronic seronegative spondyloarthritis characterized by progressive involvement of the sacroiliac and
spinal joints with eventual ossification in and around these joints
o It attacks the site of insertion of tendons, ligaments, fascia, and fibrous joint capsules
o Pathologically, progressive fibrosis and ossification in these periarticular soft tissues
o Usually a young person with gradual onset of vague low back pain that is aggravated by sudden movement and
not relieved by rest (night pain); morning stiffness are carried out through the day, and improves with physical
activities; local deep tenderness over the sacroiliac joints and spine as well as spinal muscle spasm and a loss of
the normal lumbar lordosis
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
~ THE ANATOMY ~
The Skeletal System and the Articulations of the Upper Limb
Arm (brachium) Humerus
Pectoral Girdle (cingulum pectorale) Clavicle
Intercarpal Joints
-
Proximal end has a hemispherical head that
articulates with the glenoid cavity of the scapula
(diarthrosis, synovial, saddle thumb)
(diarthrosis, synovial, plane others)
Greater tubercle is more lateral and lesser
tubercle is more anteromedial
Metacarpophalangeal Joints
Between the two tubercles is the intertubercular
sulcus or bicipital sulcus
The shaft is termed the deltoid tuberosity, for
the deltoid muscle attachment
(diarthrosis, synovial, plane)
S shaped bone attached one side to the
sternum and the other side to the scapula
Carpometacarpal Joints
Medial/ sternal end is pyramidal in shape and
articulates with sternum (sternoclavicular
joint)
Lateral/ acromial end is flattened articulates
with acromion (acromioclavicular joint)
Superior surface is smooth
Inferior surface is marked by grooves and
ridges for muscle and ligament attachments
The radial or spiral groove is located adjacent to
the deltoid tuberosity, for the radial nerve
Inferior near acromial end is rough tuberosity
called the conoid tubercle
On the distal end, two bony projections are called
the medial and lateral epicondyles
Inferior near the sternal end is called costal
tuberosity
On the distal end, two smooth surfaces, the
capitulum is located laterally and articulates with
the head of radius
Trochlea is located medially and articulates with
trochlear notch of the ulna
Has three depresions: 1) the radial fossa, is
anterolaterally, accommodates the head of the
radius, 2) the coronoid fossa, is anteromedially,
accommodates the coronoid process of the ulna ,
and 3) the olecranon fossa, is on the posterior,
accommodates the olecranon of the ulna
(diarthrosis, synovial, condylar)
Interphalangeal Joints
(diarthrosis, synovial, hinge)
Sternoclavicular Joint
(diarthrosis, synovial, saddle)
Acromioclavicular Joint
(diarthrosis, synovial, plane)
Glenohumeral Joint
(diarthrosis, synovial, ball and
socket)
Humeroulnar Joint
(diarthrosis, synovial, hinge)
Humeroradial Joint
Hand (manus) Carpals
-
(diarthrosis, synovial, hinge)
Radioulnar Joint
Radiocarpal Joint
(diarthrosis, synovial, condylar)
Proximal rows, lateral to medial
o
Scaphoid
Lunate
Triquetrum
Pisiform
Distal rows, lateral to medial
o
Trapezium
Pectoral Girdle (cingulum pectorale) Scapula
Trapezoid
Forearm (antebrachium) Radius
Broad, flat, and triangular in shape
Capitate
Positioned at the lateral side
The posterior side is the spine of the scapula
that continuous to posterior process called the
acromion
Hamate
The proximal end is a disc shaped head that
articulates with the capitulum of the humerus
This acromion articulates with the acromial
end of the clavicle
Radial tuberosity just below the neck is the
attachment site for biceps brachii muscle
The anterior projection is called the coracoid
process
Styloid process at the laterally distal end of the
wrist
Triangular shape forms three borders: 1) the
superior border is superior to the spine of
scapula, 2) the medial border is closest to the
vertebrae, and 3) the lateral border is closest
to the axilla (armpit)
The medially distal end is an ulnar notch that
articulates with the distal end of the ulna
Suprascapular notch or foramen in the
superior border provide passage for
suprascapular nerve
Stop Letting Those People
Touch The Cadavers Hand
Hand (manus) Metacarpals
Hand (manus) Phalanges
Forearm (antebrachium) Ulna
-
Positioned at the medial side
The proximal end has a C shaped trochlear
notch interlocks with the trochlea of the humerus
The scapula has three angles: 1) the superior
angle, 2) the inferior angle, and 3) the lateral
angle
The postsuperior has a projection called an
olecranon that articulates with the olecranon
fossa of the humerus
The lateral angle is a cup shaped presented
called the glenoid cavity which articulates
with humerus
The inferior of trochlear notch is the coronoid
process, articulates with the humerus
The superior edge of the glenoid cavity is
called the supraglenoid tubercle and
oppositely is called the infraglenoid tubercle
Lateral to the coronoid process is the radial
notch accommodates the radius
Also has three flattened regions: 1) the
subscapular fossa at the anterior view, 2) the
supraspinous fossa at the posterior view
above the spine, and 3) the infraspinous
fossa at the posterior below the spine
The distal end has a styloid process that is on
the medial side of the wrist
| 32
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
The Muscular System of the Upper Limb
Muscles That Move the Glenohumeral joint/ Arm
Originating on Scapula
-
Deltoid
A: anterior fibers flex and medially rotates
arm; middle fibers arm abduction; posterior
fibers extend and laterally rotates arm
O: acromial end of clavicle; acromion; spine of
scapula
I: deltoid tuberosity of humerus
Coracobrachialis
A: adducts and flexes arm
O: inferior lateral border and inferior angle of
scapula
I: middle medial shaft of humerus
Teres major
A: extends, adducts and medially rotates arm
O: inferior lateral border and inferior angle of
scapula
I: lesser tubercle and intertubercular groove of
humerus
Thoracic Muscles That Move the Pectoral Girdle
A: extends and adducts arm
O: infraglenoid tubercle of scapula
I: olecranon process of ulna
Posterior Muscles
Muscles That Move the Glenohumeral joint/ Arm
Originating on Axial Skeleton
-
Latissimus dorsi
A: arm extension, adducts and medially rotates
arm
O: spinous processes of T7 T12; ribs 8 12;
iliac crest; thoracolumbar fascia
I: intertubercular groove of humerus
-
Pectoralis major
Levator scapulae
A: elevates scapula, inferiorly rotates scapula
O: transverse processes of C1 C4
I: superior part of medial border of scapula
A: arm flexion, adducts and medially rotates arm
O: medial clavicle; costal cartilage of ribs 2 6;
body of sternum
I: lateral part of intertubercular groove of
humerus
Trapezius
A: superior fibers elevate and superiorly
rotate scapula; middle fibers retracts
scapula; inferior fibers depress scapula
O: occipital bone; ligamentum nuchae;
spinous processes of C7 T12
I: clavicle; acromion process and spine of
scapula
Biceps brachii (long head)
A: flexes arm
O: supraglenoid tubercle of scapula
I: radial tuberosity and bicipital aponeurosis
Rotator cuff muscles
-
Subscapularis
A: medially rotates arm
O: subscapular fossa of scapula
I: lesser tubercle of humerus
Rhomboid minor
A: elevates and retracts (adducts) scapula,
inferiorly rotates scapula
O: spinous processes of C7 T1
I: medial border of scapula superior to spine
Rhomboid major
A: elevates and retracts (adducts) scapula,
inferiorly rotates scapula
O: spinous processes of T2 T5
I: medial border of scapula from spine to
inferior angle
Triceps brachii (long head)
Supraspinatus
A: abducts arm
O: supraspinous fossa of scapula
I: greater tubercle of humerus
Infraspinatus
A: adducts and laterally rotates arm
O: infraspinous fossa of scapula
I: greater tubercle of humerus
Teres minor
A: adducts and laterally rotates arm
O: upper dorsal lateral border of scapula
(superior to teres major origin)
I: greater tubercle of humerus
Thoracic Muscles That Move the Pectoral Girdle
Anterior Muscles
-
Pectoralis minor
A: protracts and depresses scapula
O: ribs 3 5
I: coracoid process of scapula
Serratus anterior
A: scapula protraction, superiorly rotates
scapula
O: ribs 1 8
I: medial border of scapula
Subclavius
A: stabilizes and depresses clavicle
O: rib 1
I: inferior surface of clavicle
| 33
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
The Muscular System of the Upper Limb (continued)
Muscles That Move the Forearm
Flexors, Anterior Muscles
-
Biceps brachii
A: flexes forearm, supinator of forearm; flexes
arm (long head)
O: long head supraglenoid tubercle of
scapula; short head coracoid process of
scapula
I: radial tuberosity and bicipital aponeurosis
Brachialis
A: flexor of forearm
O: distal anterior surface of humerus
I: tuberosity and coronoid process of ulna
Brachioradialis
A: flexes forearm
O: lateral supracondylar ridge of humerus
I: styloid process of radius
Muscles That Move the Forearm
Extensors, Posterior Muscles
-
Triceps brachii
A: extensor of forearm; extends and adducts
arm (long head)
O: long head infraglenoid tubercle of
scapula; lateral head posterior humerus
above radial groove; medial head posterior
humerus below radial groove
I: olecranon of ulna
Anconeus
A: extends forearm
O: lateral epicondyle of humerus
I: olecranon of ulna
Muscles That Move the Forearm
Pronators, Anterior Forearm Muscles
-
Pronator quadratus
A: pronates forearm
O: distal one-fourth of ulna
I: distal one-fourth of radius
Pronator teres
A: pronates forearm
O: medial epicondyle of humerus and
coronoid process of ulna
I: lateral surface of radius
Supinator, Posterior Forearm Muscles
-
Supinator
A: supinates forearm
O: lateral epicondyle of humerus and ulna
distal to radial notch
I: anterolateral surface of radius distal to radial
tuberosity
| 34
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 35
The Muscular System of the Upper Limb (continued)
Forearm Muscles That Move the Wrist Joint,
Hand, and Fingers
Anterior, Superficial Muscles
-
Pronator teres
A: pronates forearm
O: medial epicondyle of humerus and
coronoid process of ulna
I: lateral surface of radius
Flexor carpi radialis
A: flexes wrist and abducts hand
O: medial epicondyle of humerus
I: base of metacarpals II and III
Palmaris longus
A: wrist flexor
O: medial epicondyle of humerus
I: flexor retinaculum and palmar
aponeurosis
Forearm Muscles That Move the Wrist Joint,
Hand, and Fingers
Anterior, Deep Muscles
-
Flexor pollicis longus
Flexor digitorum superficialis
A: flexes MP joint of thumb, IP joint of thumb;
flexes wrist
O: anterior shaft of radius; interosseous
membrane
I: distal phalanx of thumb
A: Flexes wrist; 2nd 5th MP joints, and PIP
joints
O: medial epicondyle of humerus; coronoid
process of ulna
I: middle phalanges of fingers 2 5
-
Forearm Muscles That Move the Wrist Joint,
Hand, and Fingers
Posterior, Superficial Muscles
-
Pronator quadratus
Abductor pollicis longus
Extensor pollicis brevis
A: extends MP joints of thumb, extends wrist
O: posterior surface of radius; interosseous
membrane
I: proximal phalanx of thumb
Extensor pollicis longus
A: extends MP and IP joints of thumb, extends
wrist
O: posterior surface of ulna; interosseous
membrane
I: distal phalanx of thumb
Extensor indicis
A: extends MP, PIP, and DIP joints of finger 2,
extends wrist
O: posterior surface of ulna; interosseous
membrane
I: tendon of extensor digitorum
Supinator
A: supinates forearm
O: lateral epicondyle of humerus and ulna
distal to radial notch
I: anterolateral surface of radius distal to radial
tuberosity
Extensor digitorum
A: extends wrist, extends 2nd 5th MP
joints, PIPI joints, and DIP joints
O: lateral epicondyle of humerus
I: distal and middle phalanges of fingers
25
A: pronates forearm
O: distal one-fourth of ulna
I: distal one-fourth of radius
Extensor digiti minimi
A: extends wrist, MP, and PIP joints of
finger 5
O: lateral epicondyle of humerus
I: proximal phalanx of finger 5
A: abducts thumb, extends wrist
O: proximal dorsal surfaces of radius and
ulna; interosseous membrane
I: lateral edge of metacarpal I
-
Extensor carpi radialis brevis
A: extends wrist, abducts hand
O: lateral epicondyle of humerus
I: base of metacarpal III
Posterior, Deep Muscles
-
Extensor carpi radialis longus
A: extends wrist, abducts hand
O: lateral supracondylar ridge of humerus
I: base of metacarpal II
Flexor digitorum profundus
A: Flexes wrist; 2nd 5th MP joints, PIP
joints, and DIP joints
O: anteromedial surface of ulna; interosseous
membrane
I: distal phalanges of fingers 2 5
Forearm Muscles That Move the Wrist Joint,
Hand, and Fingers
A: flexes wrist and adducts hand
O: medial epicondyle of humerus;
olecranon and posterior surface of ulna
I: pisiform and hamate bones; base of
metacarpal V
Forearm Muscles That Move the Wrist Joint,
Hand, and Fingers
Anterior, Intermediate Muscles
Flexor carpi ulnaris
Extensor carpi ulnaris
A: extends wrist, adducts hand
O: lateral epicondyle of humerus; posterior
border of ulna
I: base of metacarpal V
The
Musculoskelet al
The Muscular System of the Upper Limb (continued)
Intrinsic Muscles of the Hand
Thenar Group
-
Flexor pollicis brevis
A: flexes thumb
O: flexor retinaculum, trapezium
I: proximal phalanx of thumb
Abductor pollicis brevis
A: abducts thumb
O: flexor retinaculum, scaphoid, trapezium
I: lateral side of proximal phalanx of thumb
Opponens pollicis
A: opposition of thumb
O: flexor retinaculum, trapezium
I: lateral side of metacarpal I
Intrinsic Muscles of the Hand
Hypothenar Group
-
Flexor digiti minimi brevis
A: flexes finger 5
O: hamate bone, flexor retinaculum
I: proximal phalanx of finger 5
Abductor digiti minimi
A: abducts finger 5
O: pisiform bone, tendon of flexor carpi ulnaris
I: proximal phalanx of finger 5
Opponens digiti minimi
A: opposition of finger 5
O: hamate bone, flexor retinaculum
I: metacarpal bone V
Intrinsic Muscles of the Hand
Midpalmar Group
-
Lumbricalis
A: flexes 2nd 5th MP joints and extends
2nd 5th PIP and DIP joints
O: tendons of flexor digitorum profundus
I: dorsal tendons on fingers 2 5
Dorsal interossei
A: abducts 2nd 5th MP joints and extends
2nd 5th PIP and DIP joints
O: adjacent, opposing faces of metacarpals
I: dorsal tendons on fingers 2 5
Palmar interossei
A: adducts 2nd 5th MP joints and extends
2nd 5th PIP and DIP joints
O: metacarpal bones II, IV, V
I: sides of proximal phalanx bases for fingers
2, 4, and 5
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 36
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 37
The Vascular System of the Upper Limb
Arterial supply to the upper limb the shoulder and arm (brachium)
o The subclavian artery travels between the clavicle and first rib
o The axillary artery is the continuation of the subclavian artery through the axillary region
o The axillary artery gives off the circumflex humeral artery that supplies blood to the shoulder joint and deltoid
muscle
o The brachial artery is the continuation of the axillary artery beyond the circumflex
o It travels down the medial side of humerus and ends just distal the elbow, supplying the anterior flexor muscles of
the brachium
o The deep brachial artery arises from the proximal end of the brachial artery and supplies the triceps brachii
muscle
o The ulnar recurrent artery, arises about midway along the brachial artery, supplies the elbow joint and the
triceps brachii
o The radial recurrent artery, leads from the deep brachial artery to the radial artery, supplies the elbow joint and
forearm muscles
Arterial supply to the upper limb the forearm (antebrachium)
o Distal to the elbow, the brachial artery divides into the radial artery and ulnar artery
o These two arteries travel along the radius and the ulna respectively
o The ulnar artery gives rise to the anterior and posterior interosseous arteries that travels between the radius
and the ulna
o Radial artery supplies the lateral forearm muscles, wrist, thumb and index finger
o Ulnar artery supplies the medial forearm muscles, digits 3 to 5, and medial aspect of index finger
o Interosseous arteries supplies the deep flexors and extensors
Arterial supply to the upper limb the hand
o The radial and ulnar arteries form two palmar arches
o The deep palmar arch gives rise to the palmar metacarpal arteries of the hand
o The superficial palmar arch gives rise to the palmar digital arteries of the fingers
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 38
The Vascular System of the Upper Limb (continued)
Venous drainage of the upper limb deep veins
o The palmar digital veins drain each finger into the superficial venous palmar arch
o The metacarpal veins drain blood from the hand into the deep venous palmar arch
o Both venous palmar arches are between the radial and ulnar vein
o The radial vein receives blood from the lateral side of both palmar arches and travels up the forearm along the
radius
o The ulnar vein receives blood from the medial side of both palmar arches and travels up the forearm along the
ulna
o The brachial vein is formed by the union of the radial and ulnar veins at the elbow and travels up the brachium
o The axillary vein is formed at the axilla by the union of brachial and basilica veins
o The subclavian vein is the continuation of the axillary vein into the shoulder inferior the clavicle
Venous drainage of the upper limb superficial veins
o The dorsal venous network is a plexus of veins visible on the back side of the hand
o The cephalic vein arises from the lateral side of the dorsal venous arch, travels up the forearm along the radius,
continues to the lateral aspect of brachium to the shoulder, and joins the axillary vein
o The basilic vein arises from the medial side of the dorsal venous arch, travels up the forearm posteriorly, and
continues into the brachium
o About midway, the basilic vein joins the brachial vein
o The medial cubital vein is between the cephalic and basilic veins that crosses the cubital fossa (anterior bend of
the elbow)
o The medial antebrachial vein originates near the base of thumb, travels up the forearm between the radial and
ulnar veins, and terminates at the elbow
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 39
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
The Nervous System of the Upper Limb
Branches of the Brachial Plexus
Axillary nerve
From posterior cord, posterior division of the
brachial plexus
C5, C6
Motor innervation
o
Deltoid (arm abductor)
Teres minor (lateral rotator of arm)
Cutaneous innervation
o
Superolateral arm
Branches of the Brachial Plexus
Median nerve
From medial and lateral cords, anterior
division of the brachial plexus
C5 T1
Motor innervation
Most anterior forearm muscles
(pronators, flexors of wrist, digits)
o
Flexor carpi radialis
Flexor digitorum superficialis
Pronator teres
Pronator quadratus
Lateral 1/ 2 of flexor digitorum
profundus
Flexor pollicis longus
Thenar (thumb) muscles (move thumb)
o
Flexor pollicis brevis
Abductor pollicis brevis
Opponens pollicis
Lateral two lumbricals (flex MP joints and
extend PIP and DIP joints)
Cutaneous innervation
o
Palmar aspects and dorsal tips of
lateral 3-1/ 2 digits (thumb, index
finger, middle finger, and 1/ 2 of ring
finger)
| 40
The
Musculoskelet al
The Nervous System of the Upper Limb (continued)
Branches of the Brachial Plexus
Musculocutaneous nerve
From lateral cord, anterior division of the
brachial plexus
C5 C7
Motor innervation
Anterior arm muscles (flex humerus, flex
elbow joint, supinate forearm)
o
o
o
Coracobrachialis
Biceps brachii
Brachialis
Cutaneous innervation
o
Lateral region of forearm
Branches of the Brachial Plexus
Radial nerve
From posterior cord, posterior division of the
brachial plexus
C5 T1
Motor innervation
Posterior arm muscles (extend forearm)
o
Triceps brachii
Anconeus
Posterior forearm muscles (supinate
forearm, extend wrist, digits, one muscle
that abducts thumb)
o
Supinator
Extensor carpi radialis muscles
Extensor digitorum
Extensor carpi ulnaris
Extensor pollicis longus
Extensor pollicis brevis
Abductor pollicis brevis
Extensor digiti minimi
Extensor indicis
Brachioradialis (flexes forearm)
Cutaneous innervation
o
Posterior region of arm
Posterior region of forearm
Dorsal aspect of lateral three digits
(except their distal tips)
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 41
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
The Nervous System of the Upper Limb (continued)
Branches of the Brachial Plexus
Ulnar nerve
From medial cord, anterior division of the
brachial plexus
C8 T1
Motor innervation
Anterior forearm muscles (flexors of
wrist and digits)
o
Medial half of flexor digitorum
profundus
Flexor carpi ulnaris
Intrinsic hand muscles
Hypothenar muscles
Palmar interossei (adducts
fingers)
Dorsal interossei (abducts
fingers)
Adductor pollicis (adducts thumb)
Medial two lumbricals (flex MP
joints and extends PIP and DIP
joints)
Cutaneous innervation
o
Dorsal and palmar aspects of
medial 1-1/ 2 digits (little finger,
medial aspect of ring finger)
| 42
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 43
The Skeletal System and the Articulations of the Lower Limb
Pelvic Girdle (cingulum pelvicum) Os Coxae
Thigh (femur) Femur
The pelvic girdle refers to the left and right ossa
coxae
Proximal end has the nearly spherical head that
articulates with the pelvis at the acetabulum
Each is formed from three separate bones: the
ilium, the ischium, and the pubis
Distal to the head, an elongated neck joins the shaft of
the femur
Each articulates posteriorly with the sacrum at the
sacroiliac joint
The joining of the neck to the shaft results in an angle
that makes the femur directs medially
The femur articulates with the os coxae at the
curved depression called the acetabulum
Two massive rough processes at the proximal end: the
greater trochanter projects laterally and a lesser
trochanter is located on the posteromedial of the
femur
Both processes are connected by intertrochanteric
crest which anteriorly is seen as intertrochanteric line
At the posterior aspect of the femur, gluteal tuberosity
and pectineal line merge to linea aspera which then
branches to medial and lateral supracondylar lines
Os Coxae Ilium
-
Superior region of the os coxae
The fan-shaped portion inferiorly is called the ala
that terminates at the ridge called the arcuate line
From the medial side, ala is a depression called
the iliac fossa
These two line form a flattened triangular called the
popliteal surface
From the postlateral view, anterior, posterior,
and inferior gluteal lines are seen as the
attachment sites for gluteal muscle
The medial side of the distal end, a raised projection
called the adductor tuberosity is the attachment of the
adductor magnus muscle
Distal inferior surface are two smooth surfaces called
the medial and lateral condyles which are separated
by intercondylar fossa
The smooth anteromedial depression is called the
patellar surface
Os Coxae Ischium
-
Posterior region of the acetabulum of the os coxae
Prominent triangular ischial spine projects
medially
Postlateral border is marked by ischial tuberosity
which is then continued with ramus of the ischium
that is fused with pubis
Leg (crural) Tibia
-
At the medial side
At the proximal side has the medial and lateral
condyles that articulate with the medial and lateral
condyles of the femur
On the proximal postlateral side of the tibia is a fibular
articular facet where the head of the fibula articulates
to form the superior tibiofibular joint
Os Coxae Pubis
-
Ischial ramus fuses anteriorly with inferior pubic
ramus to form ischiopubic ramus
Superior pubic ramus is located at the anterior
margin of the acetabulum
Obturator foramen is encircled by both pubic and
ischial rami
Tibial tuberosity and the anteromedial side is the
attachment for the patellar ligament
Large and prominent process at the medial distal
border called the medial malleolus
The lateral side is the fibular notch where the fibula
articulates and forms the inferior tibiofibular joint
Sacroiliac Joint
Talocrural Joint
(diarthrosis, synovial, plane)
(diarthrosis, synovial, hinge)
Hip (coxal) joint
Intertarsal Joints
(diarthrosis, synovial, ball and socket)
(diarthrosis, synovial, plane)
Pubic Symphysis Joint
Tarsometatarsal Joints
(amphiarthrosis, cartilaginous,
symphysis)
(diarthrosis, synovial, plane)
Metatarsophalangeal Joints
(diarthrosis, synovial, condylar)
Interphalangeal Joints
(diarthrosis, synovial, hinge)
Patellofemoral Joint
(diarthrosis, synovial, plane and
hinge)
Tibiofemoral joint
(diarthrosis, synovial, hinge)
Tibiofibular Joint
(diarthrosis, synovial, plane
superior) (amphiarthrosis, fibrous,
Leg (crural) Fibula
-
Smooth articular facet articulates with the tibia
Distal tip called the lateral malleolus extends laterally to
the ankle joint
Ankle and Foot (pedis) Tarsals
-
Calcaneus forms the heel; the attachment of
calcaneal (Achilles tendon)
Talus
Navicular bone
Cuneiform three bones: medial cuneiform,
intermediate cuneiform, and lateral cuneiform
Cuboid
Ankle and Foot (pedis) Metatarsals
Ankle and Foot (pedis) Phalanges
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 44
The Articulations of the Lower Limb (focus on knee joint)
o Contains three separate articulations: 1) two between the femur and tibia (medial condyle to medial condyle,
lateral condyle to lateral condyle) and 2) one between the patella and the patellar surface of the femur
o Has a pair of fibrocartilage pads, the medial and lateral menisci
o The menisci act as cushions, conform to the shape of the articulating surfaces as the femur changes position,
and provide lateral stability to the joint
o Also has prominent fat pads cushion the margins of the joint and assist the many bursae in reducing
friction between the patella and other tissues
Supporting ligaments
o The patellar ligament attaches on the anterior surface of the tibia
o Two ligamentous bands, patellar retinaculae, placed at the medial and lateral side of the patella support the
anterior surface of the knee joint
o Two popliteal ligaments extend between the femur and the head of the tibia and fibula; these ligaments travels
the knee joints posteriorly
o Inside the joint capsule, the anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL) attach
the intercondylar area of the tibia to the condyles of the femur
o the tibial collateral ligament reinforces the medial surface of the knee joint
o the fibular collateral ligament reinforces the lateral surface
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 45
The Muscular System of the Lower Limb
Muscles That Move the Hip Joint/ Thigh
Anterior Thigh Compartment (Thigh Flexors)
-
Psoas major
Muscles That Move the Hip Joint/ Thigh
Medial Thigh Compartment (Thigh Adductors)
-
A: adducts thigh; flexes thigh
O: pubis near pubic symphysis
I: linea aspera of femur
A: flexes thigh
O: transverse processes and bodies of T12 L5 vertebrae
I: lesser trochanter of femur with iliacus
-
Iliacus
Sartorius
Rectus femoris
Gracilis
A: adducts and flexes thigh; flexes leg
O: inferior ramus and body of pubis
I: upper medial surface of tibia
A: flexes thigh and rotates thigh laterally; flexes leg and rotates leg medially
O: anterior superior iliac spine
I: tibial tuberosity, medial side
-
Adductor brevis
A: adducts thigh; flexes thigh
O: inferior ramus and body of pubis
I: upper third of linea aspera of femur
A: flexes thigh
O: iliac fossa
I: lesser trochanter of femur with psoas major
-
Adductor longus
Pectineus
A: adducts thigh; flexes thigh
O: pectineal line of pubis
I: pectineal line of femur
A: flexes thigh, extends leg
O: anterior inferior iliac spine
I: quadriceps tendon to patella and then patellar ligament to tibial tuberosity
-
Adductor magnus
A: adducts thigh; adductor part of muscle flexes thigh; hamstring part of
muscle extends and laterally rotates thigh
O: inferior ramus of pubis and ischial tuberosity
I: hamstring part linea aspera of femur; adductor part adductor tubercle of
femur
Obturator externus
A: laterally rotates thigh
O: margins of obturator foramen and obturator membrane
I: trochanteric fossa of posterior femur
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
The Muscular System of the Lower Limb (continued)
Muscles That Move the Hip Joint/ Thigh
Deep Muscles of the Gluteal Region (Lateral Thigh Rotators)
-
Piriformis
A: laterally rotates thigh
O: anterolateral surface of sacrum
I: greater trochanter
Superior gemellus
A: laterally rotates thigh
O: ischial spine and tuberosity
I: obturator internus tendon
Obturator internus
A: laterally rotates thigh
O: posterior surface of obturator membrane; margins of
obturator foramen
I: greater trochanter
Inferior gemellus
A: laterally rotates thigh
O: ischial tuberosity
I: obturator internus tendon
Quadratus femoris
A: laterally rotates thigh
O: lateral border of ischial tuberosity
I: intertrochanteric crest of femur
Muscles That Move the Hip Joint/ Thigh
Muscles That Move the Hip Joint/ Thigh
Lateral Thigh Compartment (Thigh Abductors)
Posterior Thigh (Hamstring) Compartment (Thigh
Extensors and Leg Flexors)
Tensor fasciae latae
A: abducts thigh; medially rotates thigh
O: iliac crest and lateral surface of anterior superior iliac
spine
I: iliotibial band
A: extends thigh (long head only); flexes leg (both
long and short head); laterally rotates leg
O: long head ischial tuberosity; short head
linea aspera of femur
I: head of fibula
Muscles That Move the Hip Joint/ Thigh
Gluteal Group
-
Gluteus medius
A: abducts thigh; medially rotates thigh
O: posterior iliac crest; lateral surface between posterior
and anterior gluteal lines
I: greater trochanter of femur
Gluteus maximus
A: extends thigh; laterally rotates thigh
O: iliac crest, sacrum, coccyx
I: iliotibial tract of fascia lata; linea aspera and gluteal
tuberosity of femur
Gluteus minimus
A: abducts thigh; medially rotates thigh
O: lateral surface of ilium between inferior and anterior
gluteal lines
I: greater trochanter of femur
Biceps femoris
Semimembranosus
A: extends thigh and flexes leg; medially rotates
leg
O: ischial tuberosity
I: posterior surface of medial condyle of tibia
Semitendinosus
A: extends thigh and flexes leg; medially rotates
leg
O: ischial tuberosity
I: proximal medial surface of tibia
| 46
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
The Muscular System of the Lower Limb (continued)
Thigh Muscles That Move the Knee Joint/ Leg
Thigh Muscles That Move the Knee Joint/ Leg
Leg Flexors)
Leg Extensors (Anterior Thigh Muscles)
Sartorius
Quadriceps Femoris
A: flexes thigh and rotates thigh laterally; flexes
leg and rotates leg medially
O: anterior superior iliac spine
I: tibial tuberosity, medial side
A: extends leg; flexes thigh
O: anterior inferior iliac spine
I: quadriceps tendon to patella and then patellar
ligament to tibial tuberosity
Gracilis
A: adducts and flexes thigh; flexes leg
O: inferior ramus and body of pubis
I: upper medial surface of tibia
Biceps femoris
A: extends thigh (long head only); flexes leg (both
long and short head); laterally rotates leg
O: long head ischial tuberosity; short head
linea aspera of femur
I: head of fibula
Semimembranosus
A: extends thigh and flexes leg; medially rotates
leg
O: ischial tuberosity
I: posterior surface of medial condyle of tibia
Vastus intermedius
A: extends leg
O: anterolateral surface of femur
I: quadriceps tendon to patella and then patellar
ligament to tibial tuberosity
Hamstrings
-
Rectus femoris
Semitendinosus
A: extends thigh and flexes leg; medially rotates
leg
O: ischial tuberosity
I: proximal medial surface of tibia
Vastus lateralis
A: extends leg
O: greater trochanter and linea aspera of femur
I: quadriceps tendon to patella and then patellar
ligament to tibial tuberosity
Vastus medialis
A: extends leg
O: intertrohanteric line and linea aspera of femur
I: quadriceps tendon to patella and then patellar
ligament to tibial tuberosity
| 47
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 48
The Muscular System of the Lower Limb (continued)
Leg Muscles
Leg Muscles
Lateral Compartment (Evertors and Weak Plantar
Flexors)
Posterior Compartment (Plantar Flexors, Flexors
of the Leg and Toes)
Superficial layer
Fibularis longus
A: everts foot; weak plantar flexor
O: head and superior two-thirds of shaft of fibula;
lateral condyle of tibia
I: base of metatarsal I; medial cuneiform bone
Gastrocnemius
A: flexes leg; plantar flexes foot
O: superior posterior surfaces of lateral and
medial condyles of femur
I: calcaneus (via calcaneal tendon)
Fibularis brevis
A: everts foot; weak plantar flexor
O: midlateral shaft of fibula
I: vase of metatarsal V
Soleus
A: plantar flexes foot
O: head and proximal shaft of fibula; medial
border of tibia
I: calcaneus (via calcaneal tendon)
A: weak leg flexor and plantar flexor
O: lateral supracondylar ridge of femur
I: posterior region of calcaneus
Leg Muscles
Anterior Compartment (Dorsiflexors and Toe
Extensors)
-
Deep layer
-
Extensors digitorum longus
Extensor halluces longus
A: extends great toe (1); dorsiflexes foot
O: anterior surface of fibula; interosseous
membrane
I: distal phalanx of great toe (1)
-
Tibialis anterior
A: dorsiflexes foot; inverts foot
O: lateral condyle and proximal shaft of tibia;
interosseous membrane
I: metatarsal I and first (medial) cuneiform
Flexor hallucis longus
A: plantar flexes foot; flexes MP and IP joints of
great toe (1)
O: posterior inferior two-thirds of fibula
I: distal phalanx of great toe (1)
Fibularis tertius
A: dorsiflexes and weakly everts foot
O: anterior distal surface of fibula; interosseous
membrane
I: base of metatarsal V
Flexor digitorum longus
A: plantar flexes foot; flexes MP, PIP, and DIP
joints of toes 2 5
O: posteromedial surface of tibia
I: distal phalanges of toes 2 5
A: extends toes 2 5; dorsiflexes foot
O: lateral condyle of tibia; anterior surface of
fibula; interosseous membrane
I: distal phalanges of toes 2 5
-
Plantaris
Tibialis posterior
A: plantar flexes foot; inverts foot
O: fibula, tibia, and interosseous membrane
I: metatarsals II IV; navicular bone; cuboid
bone; all cuneiforms
Popliteus
A: flexes leg; medially rotates tibia to unlock the
knee
O: lateral condyle of femur
I: posterior, proximal surface of tibia
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
The Muscular System of the Lower Limb (continued)
Intrinsic Muscles of the Foot
Intrinsic Muscles of the Foot
Intrinsic Muscles of the Foot
Plantar Surface (Toe Flexors, Adductors,
Abductors)
Plantar Surface (Toe Flexors, Adductors,
Abductors)
Dorsal Surface (Toe Extensors)
Layer 1 (Superficial)
Layer 3 (Deeper)
Flexor digitorum brevis
Abductor hallucis
A: abducts great toe (1)
O: calcaneus
I: medial side of proximal phalanx of great toe
(1)
A: flexes MP joint of great toe (1)
O: cuboid and lateral (3rd) cuneiform bones
I: proximal phalanx of great toe (1)
Abductor digiti minimi
A: abducts toe 5
O: calcaneus (inferior surface tuberosity)
I: lateral side of proximal phalanx of toe 5
Flexor digiti minimi brevis
A: flexes MP joint of toe 5
O: metatarsal V
I: proximal phalanx of toe 5
Layer 2 (Deep)
-
Flexor hallucis brevis
Quadratus plantae
Layer 4 (Deepest)
A: pulls on flexor digitorum longus tendons to
flex toes 2 5
O: calcaneus, long plantar ligament
I: tendons of flexor digitorum longus
Dorsal interossei
A: abducts toes
O: adjacent sides of metatarsals
I: sides of proximal phalanges of toes 2 4
lumbricals
A: flexes MP joints and extends PIP and DIP
joints of toes 2 5
O: tendons of flexor digitorum longus
I: tendons of extensor digitorum longus
Plantar interossei
A: adducts toes
O: sides of metatarsals III V
I: medial side of proximal phalanges of toes
35
Extensor hallucis brevis
A: extends MP joint of great toe (1)
O: calcaneus and inferior extensor
retinaculum
I: proximal phalanx of great toe (1)
Adductor hallucis
A: adduct great toe (1)
O: transverse head capsules of MP joints
III V; oblique head bases of metatarsals
II IV
I: lateral side of proximal phalanx of great
toe (1)
A: flexes MP and PIP joints of toes 2 5
O: calcaneus
I: middle phalanges of toes 2 5
Extensor digitorum brevis
A: extends MP, PIP, and DIP joints of toes
24
O: calcaneus and inferior extensor
retinaculum
I: middle phalanges of toes 2 4
| 49
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 50
The Vascular System of the Lower Limb
Arterial supply to the lower limb from the pelvic region to the knee
o The external iliac artery passes behind the inguinal ligament and becomes the femoral artery
o The femoral artery passes through the upper medial thigh and gives off several small arteries to the skin and
produces branches before descending the rest of the way to the knee
The deep femoral artery arises from the lateral side of the femoral; it is the largest branch and is the major
arterial supply to the thigh muscle
Two circumflex femoral arteries arise from the deep femoral, encircle the head of the femur, and
anastomose laterally; they supply mainly the femur, hip joint, and hamstring muscles
o The popliteal artery is a continuation of the femoral artery in the popliteal fossa at the rear of the knee; it
begins where the femoral artery emerges from an opening in the tendon of the adductor magnus muscle and
ends where it splits into the anterior and posterior tibial arteries; it gives off anastomoses called genicular
arteries that supply the knee joint
Arterial supply to the lower limb the leg and foot
o The anterior tibial artery arises from the popliteal artery and penetrates through the interosseous membrane of
the leg to the anterior compartment; it travels lateral to the tibia and supplies the extensor muscles; upon
reaching the ankle, it gives rise to the following dorsal arteries of the foot
The dorsal pedal artery travels the ankle and upper medial surface of the foot an gives rise to the arcuate
artery
The arcuate artery sweeps across the foot from medial to lateral and gives rise to vessels that supply the
toes
o The posterior tibial artery is a continuation of the popliteal artery that passes down the leg, deep posterior
compartment, supplying flexor muscles along the way; it passes behind the medial malleolus of the ankle and
into the plantar region of the foot
The medial and lateral plantar arteries originate by branching of the posterior tibial artery at the ankle; the
medial plantar artery supplies the great toe; the lateral plantar artery sweeps across the sole of the foot and
becomes the deep plantar arch
The deep plantar arch gives off another set of arteries to the toes
o The fibular (peroneal) artery arises from the proximal end of the posterior tibial artery near the knee; it
descends through the lateral side of the posterior compartment, supplying lateral muscles of the leg along the
way, and ends in a network of arteries in the heel
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 51
The Vascular System of the Lower Limb (continued)
Venous drainage of the lower limb superficial veins
o The dorsal venous arch, is often visible through the skin on the dorsum of the foot, collects blood from the toes
and more proximal part of the foot, and has numerous anastomoses similar to the dorsal venous network of the
hand
The small (short) saphenous vein arise from the lateral side of the arch and passes up that side of the leg
as far as the knee; there, it drains into the popliteal
The great (long) saphenous vein arises from the medial side of the arch and travels all the way up the leg
and thigh to the inguinal region
Venous drainage of the lower limb deep veins
o The deep plantar arch receives blood from the toes and gives rise to lateral and medial plantar veins in the
respective sides
o the lateral plantar vein gives off the fibular veins, then crosses over to the medial side and approaches the
medial plantar vein; the two plantar veins pass behind the medial malleolus of the ankle and continue as a pair of
posterior tibial veins
o the two posterior tibial veins pass up the leg embedded deep in the calf muscles; the converge like an inverted
Y into a single vein about two-thirds of the way up the tibia
o the two fibular (peroneal) veins ascend the back of the leg and similarly converge like a Y
o the popliteal vein begins near the knee by convergence of these two inverted Ys; it passes through the popliteal
fossa at the back of the knee
o the two anterior tibial veins travel up the anterior compartment of the leg between the tibia and fibula; they arise
from the medial side of the dorsal venous arch, converge distal to the knee, and then flow into the popliteal vein
o the femoral vein is the continuation of the popliteal vein into the thigh; it drains blood from the deep thigh
muscles and femur
o the deep femoral vein drains the femur and muscles of the thigh supplied by the deep femoral artery; it receives
four principal tributaries along he shaft of the femur and then a pair of circumflex femoral veins that encircle the
upper femur; it finally drains into the upper femoral vein
o the external iliac vein is formed by the union of the femoral and great saphenous veins near the inguinal
ligament
o the internal iliac vein follows the course of the internal iliac artery and its distribution; its tributaries drain the
gluteal muscles and the medial aspect of the thigh
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 52
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
The Nervous System of the Lower Limb
Branches of the Lumbar Plexus
Femoral nerve
L2 L4
Motor innervation
Anterior thigh muscles
o
Quadriceps femoris (knee extensor)
Iliopsoas (hip flexor)
Sartorius (hip and knee flexor)
Pectineus
Cutaneous innervation
o
Anterior thigh
Inferomedial thigh
Medial side of leg
Most medial aspect of foot
Branches of the Lumbar Plexus
Obturator nerve
L2 L4
Motor innervation
Medial thigh muscles (adductors of thigh)
o
Adductors
Gracilis
Pectineus
Obturator externus (lateral rotator of
thigh)
Cutaneous innervation
o
Superomedial thigh
| 53
The
Musculoskelet al
The Nervous System of the Lower Limb (continued)
Branches of the Sacral Plexus
These two nerves are the branches of the
sciatic nerve
Tibial nerve
L4 S3
Motor innervation
Posterior thigh muscles (extend thigh
and flex leg)
o
Long head of biceps femoris
Semimembranosus
Semitendinosus
Part of adductor magnus
Posterior leg muscles (plantar flexors of
foot, flexors of knee)
o
Flexor digitorum longus
Flexor hallucis longus
Gastrocnemius
Soleus
Popliteus
Tibialis posterior (inverts foot)
Plantar foot muscles (via medial and
lateral plantar nerve branches)
Cutaneous innervation
Branches of heel, and via its medial and
lateral plantar nerve branches (which
supply the sole of the foot)
Branches of the Sacral Plexus
Divides into deep fibular and superficial
fibular branches
Common Fibular nerve
L4 S2
Motor innervation
Short head of biceps femoris (knee
flexor)
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 54
The
Musculoskelet al
S y s t e m
2012 Kevin Edward Santoso. All Rights Reserved
| 55
The Nervous System of the Lower Limb (continued)
Branches of the Sacral Plexus
Deep Fibular nerve
L4 S1
Motor innervation
Anterior leg muscles (dorsiflexfoot,
extend toes)
o
Tibialis anterior (inverts foot)
Extensor hallucis longus
Extensor digitorum longus
Fibularis tertius
Dorsum foot muscles (extend toes)
Extensor hallucis brevis
Extensor digitorum brevis
Cutaneous innervation
Dorsal interspace between first and
second toes
Branches of the Sacral Plexus
Superficial Fibular nerve
L5 S2
Motor innervation
Lateral leg muscles (foot evertors and
plantar flexor)
Fibularis longus
Fibularis brevis
Cutaneous innervation
Anteroinferior part of leg; most of dorsum
of foot
You might also like
- Addiction Treatment: A Strengths PerspectiveDocument2 pagesAddiction Treatment: A Strengths PerspectiveKatherine van Wormer50% (4)
- Anaphy C7 Oral Rec.Document3 pagesAnaphy C7 Oral Rec.Katrina ParbaNo ratings yet
- Musculoskeltal SystemDocument18 pagesMusculoskeltal Systemhy7tnNo ratings yet
- Formation: Blood Calcium Level - Calcium HydroxyapatiteDocument13 pagesFormation: Blood Calcium Level - Calcium HydroxyapatiteClarissa IsuriñaNo ratings yet
- Lec 1516 Bone Tissue and Skeletal SystemDocument28 pagesLec 1516 Bone Tissue and Skeletal SystemonegaonnweNo ratings yet
- Functional Anatomy and Physiology 1Document6 pagesFunctional Anatomy and Physiology 1AtiqahNo ratings yet
- Kalsifikasi, Deposisi Dan Resorpsi TulangDocument40 pagesKalsifikasi, Deposisi Dan Resorpsi TulangrifkaNo ratings yet
- Calcium Homeostasis and Osteoporosis - McMaster Pathophysiology ReviewDocument8 pagesCalcium Homeostasis and Osteoporosis - McMaster Pathophysiology ReviewEzayu AzeraNo ratings yet
- Bone and Mineral Metabolism in Health and DiseaseDocument14 pagesBone and Mineral Metabolism in Health and Diseasebiniam MesfinNo ratings yet
- Bone Metabolism: German VersionDocument17 pagesBone Metabolism: German VersionDapot SianiparNo ratings yet
- Exam A-3Document11 pagesExam A-3yapues87No ratings yet
- Bone and Cartilage PDFDocument50 pagesBone and Cartilage PDFalviraNo ratings yet
- 7 CalciumDocument83 pages7 Calciumtmqt2fbnzgNo ratings yet
- Bone Basic Science: Presenter: DR Nshimiyimana Alexis Orthopedic Resident-UrDocument36 pagesBone Basic Science: Presenter: DR Nshimiyimana Alexis Orthopedic Resident-UrNshimiyimana AlexisNo ratings yet
- 511-525chapter 6-8 (1) An Introduction To The Skeletal SystemDocument6 pages511-525chapter 6-8 (1) An Introduction To The Skeletal Systemtomorrow.today.yesterday .yesterdayNo ratings yet
- Seminar On Bone and CalciumDocument4 pagesSeminar On Bone and Calciumtshireletso “TROY” nkunaNo ratings yet
- Alveolar Bone FFDocument105 pagesAlveolar Bone FFshashi kant chaudharyNo ratings yet
- Chap 6 AnaphyDocument8 pagesChap 6 AnaphyNicholle VelosoNo ratings yet
- Ch. 10 and 6Document25 pagesCh. 10 and 6Bammary88909No ratings yet
- Physiologic Processes in The Skeletal SystemDocument6 pagesPhysiologic Processes in The Skeletal SystemAry Romeo ShakespeareNo ratings yet
- Anatomy & Physiology: Skeletal SystemDocument20 pagesAnatomy & Physiology: Skeletal SystemWilbert Antonino CabanbanNo ratings yet
- Human Anatomy 4th Edition Saladin Solutions Manual 1Document36 pagesHuman Anatomy 4th Edition Saladin Solutions Manual 1donnawugnwsjrzcxt100% (28)
- Human Anatomy 4Th Edition Saladin Solutions Manual Full Chapter PDFDocument27 pagesHuman Anatomy 4Th Edition Saladin Solutions Manual Full Chapter PDFdora.ivy892100% (22)
- Bone ResorptionDocument10 pagesBone ResorptionVibhor PradhanNo ratings yet
- COMPRE2Document13 pagesCOMPRE2Rodrigo SeriozaNo ratings yet
- 6.the Skeletal System Bone TissueDocument25 pages6.the Skeletal System Bone TissueKojo Yeboah EnchillNo ratings yet
- SKELETAL SYSTEM ReviewerDocument7 pagesSKELETAL SYSTEM ReviewerKrize Colene dela CruzNo ratings yet
- We Are Intechopen, The World'S Leading Publisher of Open Access Books Built by Scientists, For ScientistsDocument19 pagesWe Are Intechopen, The World'S Leading Publisher of Open Access Books Built by Scientists, For ScientistsJade LolongNo ratings yet
- Bone Physiology 2Document27 pagesBone Physiology 2Nzau MuangeNo ratings yet
- MatthewVaracalloMD PhysiologyBoneDocument5 pagesMatthewVaracalloMD PhysiologyBonetulipaNo ratings yet
- Bone Formation: Hypothalamic Hormone, CRH, and The Pituitary Hormone, ACTHDocument3 pagesBone Formation: Hypothalamic Hormone, CRH, and The Pituitary Hormone, ACTHSimon AvilaNo ratings yet
- Bone Ash Estimation of Content of Bone Ash Project Submitted by PrashanthDocument3 pagesBone Ash Estimation of Content of Bone Ash Project Submitted by PrashanthHarsh Kumar0% (3)
- Alad Bihag Hizon Medicine Case StudyDocument103 pagesAlad Bihag Hizon Medicine Case StudyDan HizonNo ratings yet
- Chapter 3Document12 pagesChapter 3Deolita BadiangNo ratings yet
- Bones: A Hard SubjectDocument16 pagesBones: A Hard SubjectMaria Dini AdmiratiNo ratings yet
- Chemistry Project On Estimation of Content of Bone AshDocument18 pagesChemistry Project On Estimation of Content of Bone AshKim TaesiNo ratings yet
- Drugs Bone DisordersDocument38 pagesDrugs Bone Disordersalizwaxabanisa8No ratings yet
- Functions of The Musculoskeletal SystemDocument9 pagesFunctions of The Musculoskeletal SystemLinda XueNo ratings yet
- Department of Periodontics and Implantology: Calcium MetabolismDocument63 pagesDepartment of Periodontics and Implantology: Calcium Metabolismrasagna reddy100% (1)
- Bone Is A MineralizedDocument2 pagesBone Is A MineralizedZen Firhan ShahabNo ratings yet
- Human Anatomy 5th Edition Saladin Solutions ManualDocument7 pagesHuman Anatomy 5th Edition Saladin Solutions Manualjillhenrysetcjnzrfp100% (26)
- 7 - BoneDocument36 pages7 - BoneKhdhir M. SalemNo ratings yet
- Human Anatomy 5Th Edition Saladin Solutions Manual Full Chapter PDFDocument28 pagesHuman Anatomy 5Th Edition Saladin Solutions Manual Full Chapter PDFJenniferWhitebctr100% (12)
- Alveolar Bone: and It's Associated PathologiesDocument7 pagesAlveolar Bone: and It's Associated Pathologiesمحمد العراقيNo ratings yet
- Chemistry Project On Estimation of Content of Bone AshDocument13 pagesChemistry Project On Estimation of Content of Bone AshShlok Sah50% (2)
- Topic 5. Bone Microscopic Anatomy and Devt 1Document24 pagesTopic 5. Bone Microscopic Anatomy and Devt 1Janine Jerica JontilanoNo ratings yet
- The Main Functions of BonesDocument9 pagesThe Main Functions of BonesabbaslafeNo ratings yet
- Proteoglycans, Whose Main Glycosaminoglycans Are Chondroitin-4-Sulfate and Chondroitin-6Document14 pagesProteoglycans, Whose Main Glycosaminoglycans Are Chondroitin-4-Sulfate and Chondroitin-6Joseph Enoch ElisanNo ratings yet
- Lec 3 2010 02 6Document8 pagesLec 3 2010 02 6Ras WhoknowsmeNo ratings yet
- Intro Tothe Function of Parathyroid Gland, ConciseDocument34 pagesIntro Tothe Function of Parathyroid Gland, Conciseinka.elseNo ratings yet
- Orthopedic NursingDocument237 pagesOrthopedic Nursingɹǝʍdןnos100% (24)
- Kenkre Bassett 2018 The Bone Remodelling CycleDocument20 pagesKenkre Bassett 2018 The Bone Remodelling Cyclealealer2708No ratings yet
- Bone As A Living Dynamic TissueDocument14 pagesBone As A Living Dynamic TissueSuraj_Subedi100% (6)
- Agents That Affect Bone Mineral Homeostasis: Department of PharmacologyDocument44 pagesAgents That Affect Bone Mineral Homeostasis: Department of Pharmacologymichaelcyl100% (1)
- Physiology of BoneDocument32 pagesPhysiology of BoneAnandhu GNo ratings yet
- Ch07 - EOC - Skeletal SystemDocument4 pagesCh07 - EOC - Skeletal SystemGaveen CoatesNo ratings yet
- Bone: Biology, Harvesting, and Grafting for Dental Implants, 2nd EditionFrom EverandBone: Biology, Harvesting, and Grafting for Dental Implants, 2nd EditionNo ratings yet
- Renal Reflections: Exploring the Marvels of Nephrology: The Intricate Ballet of Kidney Functions UnveiledFrom EverandRenal Reflections: Exploring the Marvels of Nephrology: The Intricate Ballet of Kidney Functions UnveiledNo ratings yet
- Advanced farriery knowledge: A study guide and AWCF theory course companionFrom EverandAdvanced farriery knowledge: A study guide and AWCF theory course companionNo ratings yet
- Rangkuman Week 5 (PBL) - OsteomyelitisDocument9 pagesRangkuman Week 5 (PBL) - OsteomyelitisMaria Dini AdmiratiNo ratings yet
- Rangkuman Week 3 (PBL) - RADocument27 pagesRangkuman Week 3 (PBL) - RAMaria Dini AdmiratiNo ratings yet
- Week 1 HumanAnat&Fisio - 6 Agustus 2012Document17 pagesWeek 1 HumanAnat&Fisio - 6 Agustus 2012Maria Dini AdmiratiNo ratings yet
- Week 3 JointInflammatoryDisease - 27 Agustus 2012Document19 pagesWeek 3 JointInflammatoryDisease - 27 Agustus 2012Maria Dini AdmiratiNo ratings yet
- Week 1 BlockMuscle - 6 Agustus 2012Document21 pagesWeek 1 BlockMuscle - 6 Agustus 2012Maria Dini AdmiratiNo ratings yet
- Week 4 MetabolicBoneDisease - 3 September 2012week 4 MetabolicBoneDisease - 3 September 2012Document16 pagesWeek 4 MetabolicBoneDisease - 3 September 2012week 4 MetabolicBoneDisease - 3 September 2012Maria Dini AdmiratiNo ratings yet
- Week 4 BackBoneAnatomy - 3 September 2012Document20 pagesWeek 4 BackBoneAnatomy - 3 September 2012Maria Dini AdmiratiNo ratings yet
- Bones: A Hard SubjectDocument16 pagesBones: A Hard SubjectMaria Dini AdmiratiNo ratings yet
- Week 2 Blpressoureoduph - 20 Februari 2012week 2 Blpressoureoduph - 20 Februari 2012Document43 pagesWeek 2 Blpressoureoduph - 20 Februari 2012week 2 Blpressoureoduph - 20 Februari 2012Maria Dini AdmiratiNo ratings yet
- Week 4 Embryology Development of Gastrointestinal: DR Marselina TanDocument29 pagesWeek 4 Embryology Development of Gastrointestinal: DR Marselina TanMaria Dini AdmiratiNo ratings yet
- Heat Related Illnesses: Erwin Mulyawan, DR, Span, DpbaDocument42 pagesHeat Related Illnesses: Erwin Mulyawan, DR, Span, DpbaMaria Dini AdmiratiNo ratings yet
- Is An Irregular Shape Cylinder With Narrow Opening Superiorly and A Large Inferiorly OpeningDocument27 pagesIs An Irregular Shape Cylinder With Narrow Opening Superiorly and A Large Inferiorly OpeningMaria Dini AdmiratiNo ratings yet
- Communication Between Nerve Cells.: V. Sutarmo SetiadjiDocument35 pagesCommunication Between Nerve Cells.: V. Sutarmo SetiadjiMaria Dini AdmiratiNo ratings yet
- Laboratory Logistics HandbookDocument96 pagesLaboratory Logistics HandbookMohd Fahmi MastukiNo ratings yet
- POLYSEED Application Procedure 3.15Document2 pagesPOLYSEED Application Procedure 3.15ALVARO ENRIQUE CANTILLO GUZMANNo ratings yet
- Chronic Pain and Road MappingDocument3 pagesChronic Pain and Road MappingkasiaNo ratings yet
- Why Antibiotics Should Not Be Overused. Write A Short Note?Document4 pagesWhy Antibiotics Should Not Be Overused. Write A Short Note?Danger TigerNo ratings yet
- Cauti CDC 2018Document17 pagesCauti CDC 2018NasikhatulNo ratings yet
- FDAR ChartingDocument50 pagesFDAR ChartingNathaniel PulidoNo ratings yet
- Womens - Era July 2017Document148 pagesWomens - Era July 2017taruniNo ratings yet
- Q A Random - 16Document8 pagesQ A Random - 16ja100% (1)
- Traditional Medicine & Herbal TechnologyDocument39 pagesTraditional Medicine & Herbal TechnologyDivyam14No ratings yet
- Ilness and BiomagnetismDocument3 pagesIlness and BiomagnetismSilvia Arias100% (2)
- Oklahoma Commission On Opioid Abuse Final ReportDocument12 pagesOklahoma Commission On Opioid Abuse Final ReportOKCFOXNo ratings yet
- REBTDocument18 pagesREBTGayathree ChandranNo ratings yet
- Cognitive Behaviour Therapy For Depression in Young People Manual For TherapistsDocument120 pagesCognitive Behaviour Therapy For Depression in Young People Manual For TherapistsSundar PrabhuNo ratings yet
- Byproducts From Cassava ProcessingDocument29 pagesByproducts From Cassava ProcessingasokmithraNo ratings yet
- UPSC Medical ScienceDocument7 pagesUPSC Medical ScienceAbhishek JoshiNo ratings yet
- Herbal CosmeticsDocument40 pagesHerbal CosmeticsBiren Shah100% (1)
- PDF DipiroDocument16 pagesPDF DipiroYolandaFandraIINo ratings yet
- Swedish MassageDocument22 pagesSwedish Massagealejandro jean100% (3)
- Swollen Neck Lymph Nodes - Causes - Better MedicineDocument6 pagesSwollen Neck Lymph Nodes - Causes - Better MedicineDanao ErickNo ratings yet
- Starch Industry in IndiaDocument3 pagesStarch Industry in Indiabanapte59No ratings yet
- Leisure Awareness ActivitiesDocument9 pagesLeisure Awareness Activitiesapi-301398957No ratings yet
- The Clinical Management of Awake BruxismDocument30 pagesThe Clinical Management of Awake BruxismSahana RangarajanNo ratings yet
- SPDX Week 8 - Perfusion TechnologyDocument2 pagesSPDX Week 8 - Perfusion TechnologyerikajoydmrmtNo ratings yet
- Koppenaal2020 Article EffectivenessAndCost-effectiveDocument13 pagesKoppenaal2020 Article EffectivenessAndCost-effectivePaulomds1991No ratings yet
- 1-Legal Med Notes PDFDocument19 pages1-Legal Med Notes PDFFrenza Joy FresnidoNo ratings yet
- Super fi cial roughness on composite surface, composite enamel and composite dentin junctions after different fi nishing and polishing procedures. Part I: roughness after treatments with tungsten carbide vs diamond bursDocument20 pagesSuper fi cial roughness on composite surface, composite enamel and composite dentin junctions after different fi nishing and polishing procedures. Part I: roughness after treatments with tungsten carbide vs diamond bursCinthyaNavarroNo ratings yet
- ATI Module - Ethical Principles For Mental HealthDocument6 pagesATI Module - Ethical Principles For Mental HealthChelsea HebertNo ratings yet
- Cholelithiasis When They Are in The Bile CholedocolithiasisDocument15 pagesCholelithiasis When They Are in The Bile Choledocolithiasishisabumohamed100% (1)
- Cai Songfang Wujishi Breathing Exercises Medicine Health Publishing Co. 1994Document119 pagesCai Songfang Wujishi Breathing Exercises Medicine Health Publishing Co. 1994Amlen Singha100% (2)