Professional Documents
Culture Documents
International Journal of Surgery Case Reports
International Journal of Surgery Case Reports
Uploaded by
hussein_faourOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
International Journal of Surgery Case Reports
International Journal of Surgery Case Reports
Uploaded by
hussein_faourCopyright:
Available Formats
CASE REPORT OPEN ACCESS
International Journal of Surgery Case Reports 10 (2015) 191194
Contents lists available at ScienceDirect
International Journal of Surgery Case Reports
journal homepage: www.casereports.com
Liver hilar tuberculous lymphadenitis successfully diagnosed by
laparoscopic lymph node biopsy
Masaki Wakasugi a, , Masahiro Tanemura a , Tsubasa Mikami a , Kenta Furukawa a ,
Masahiko Tsujimoto b , Hiroki Akamatsu a
a
b
Departments of Surgery, Osaka Police Hospital, 10-31 Kitayama-cho, Tennouji-ku, Osaka, Osaka 543-0035, Japan
Departments of Pathology, Osaka Police Hospital, 10-31 Kitayama-cho, Tennouji-ku, Osaka, Osaka 543-0035, Japan
a r t i c l e
i n f o
Article history:
Received 19 February 2015
Received in revised form 27 February 2015
Accepted 3 March 2015
Available online 4 April 2015
Keywords:
Tuberculous
Liver hilar tuberculous lymphadenitis
Laparoscopic lymph node biopsy
Positron emission tomography with
2-[uorine-18]- uoro-2-deoxy-d-glucose
(FDG-PET)
a b s t r a c t
INTRODUCTION: Liver hilar tuberculous lymphadenitis is extremely rare. A case of liver hilar tuberculous
lymphadenitis mimicking lymph node metastasis of anal canal cancer that was successfully diagnosed
by laparoscopic lymph node biopsy is reported.
PRESENTATION OF CASE: A 49-year-old man with a past medical history of pulmonary tuberculosis suffering from anal canal cancer with left inguinal lymph node metastasis underwent laparoscopic anterior
perineal resection and left inguinal lymph node dissection in February 2010. Subsequently, he underwent dissection of right inguinal lymph node metastases from anal canal cancer twice in February and
October 2013. In July 2014, follow-up computed tomography (CT) showed a 26 mm 23 mm lesion with
calcication on the anterior side of the portal vein in the hepatoduodenal ligament. He had no jaundice.
Positron emission tomography with 2[18 F]-uoro-2-deoxy-d-glucose (FDG-PET) revealed a mass with
high uptake. Suspecting a lymph node metastasis from anal canal cancer, laparoscopic lymph node biopsy
was performed. Histopathological and polymerase chain reaction (PCR) examinations yielded a diagnosis
of tuberculous lymphadenitis. No evidence of recurrence of cancer has been seen during the 5 years of
follow-up after the surgery for anal canal cancer.
DISCUSSION: FDG-PET imaging is rarely useful for differentiating cancer from tuberculosis lesions. Laparoscopic lymph node biopsy is a safe, effective alternative to open surgical biopsy.
CONCLUSION: Tuberculous lymphadenitis should be included among the differential diagnoses of liver
hilar lymphadenopathy in patients with a history of tuberculous. Laparoscopic lymph node biopsy is
useful for the diagnosis of undiagnosed lymphadenopathy.
2015 The Authors. Published by Elsevier Ltd. on behalf of Surgical Associates Ltd. This is an open
access article under the CC BY-NC-ND license (http://creativecommons.org/licenses/by-nc-nd/4.0/).
1. Introduction
2. Case presentation
Tuberculosis is a potential systemic disease that can affect any
organ or system of the body. Abdominal tuberculosis is rare and
accounts for 1225% of all extrapulmonary tuberculosis cases [1,2].
The incidence of abdominal tuberculosis has been increasing over
the last 20 years, especially in tuberculosis endemic areas [3],
developing countries, immunocompromised patients, and due to
increasing antibiotic resistance of Mycobacterium tuberculosis. A
rare case of liver hilar tuberculous lymphadenitis mimicking lymph
node metastasis of anal canal cancer that was successfully diagnosed by laparoscopic lymph node biopsy is reported.
A 49-year-old man visited our hospital for follow-up of anal
canal cancer. He had a history of pulmonary tuberculosis at 38
years of age treated with oral antituberculous agents, and early
gastric cancer treated with laparoscopic-assisted distal gastrectomy at 40 years of age. With a diagnosis of anal canal cancer and
left inguinal lymph node metastasis, he underwent laparoscopic
anterior perineal resection and left inguinal lymph node dissection in February 2010. Pathological ndings led to a diagnosis of
advanced anal canal adenocarcinoma (T2N3M0 stage IIIB according to the TNM classication). He then underwent right inguinal
lymph node dissection twice in February 2013 and October 2013.
The pathological ndings of these lymph nodes were compatible
with metastasis of anal canal adenocarcinoma. In July 2014, followup computed tomography (CT) showed a 26 mm 23 mm lesion
with calcication on the anterior side of the portal vein in the
hepatoduodenal ligament (Figs. 1 and 2). He had no jaundice and
produced no sputum. Chest and abdominal radiographs were nor-
Corresponding author. Tel.: +81 6 6775 6051; fax: +81 6 6775 6051.
E-mail address: wakasugi@oph.gr.jp (M. Wakasugi).
http://dx.doi.org/10.1016/j.ijscr.2015.03.002
2210-2612/ 2015 The Authors. Published by Elsevier Ltd. on behalf of Surgical Associates Ltd. This is an open access article under the CC BY-NC-ND license
(http://creativecommons.org/licenses/by-nc-nd/4.0/).
CASE REPORT OPEN ACCESS
192
M. Wakasugi et al. / International Journal of Surgery Case Reports 10 (2015) 191194
Fig. 3. Positron emission tomography with 2[18 F]-uoro-2-deoxy-d-glucose (FDG)
shows a mass with SUVmax of 4.48 (arrow), consistent with the CT scan ndings.
Fig. 1. Abdominal computed tomography: (a) calcied lymph node mass in the
hepatic hilum; (b) surgical staple of previous gastric surgery.
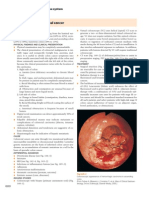
Fig. 4. Intraoperative laparoscopic observation shows that an enlarged lymph node
(arrow head) is adhered rmly to the common hepatic artery (CHA) and the left
hepatic artery (LHA).
Fig. 2. Abdominal computed tomography: (a) calcied lymph node mass in the
hepatic hilum; (b) surgical staple of previous gastric surgery.
mal. Routine laboratory tests demonstrated total bilirubin (T-Bil)
of 0.6 mg/dL (normal 0.41.4 mg/dL), aspartate aminotransferase
(AST) of 22 IU/L (normal 1033 IU/L), and alanine aminotransferase (ALT) of 28 IU/L (normal 635 IU/L), with normal levels of
inammatory markers. Serum levels of carcinoembryonic antigen (CEA), carbohydrate antigen (CA) 19-9, and squamous cell
carcinoma antigen (SCC) were within normal limits throughout
the course. Positron emission tomography with 2[18 F]-uoro2-deoxy-d-glucose (FDG-PET) revealed a mass with a maximum
standardized uptake value (SUVmax) of 4.48, consistent with the
CT scan ndings (Fig. 3). Suspecting a lymph node metastasis from
anal canal cancer or gastric cancer, laparoscopic lymph node biopsy
was performed. Intraoperative laparoscopic observation showed
severe adhesions around the hepatoduodenal ligament because
of the previous gastric surgery. An enlarged lymph node adhered
rmly to the common hepatic artery (CHA) and the left hepatic
artery (LHA) and was carefully dissected (Fig. 4). No other lymph
node swelling or suspected lesions of metastases of cancer were
found in the abdominal cavity. The operative time was 214 min.
Blood loss was minimal. Histopathological examination revealed
an epithelioid granuloma with caseous necrosis within its center
and yielded a suspected diagnosis of tuberculous lymphadenitis
(Fig. 5). The diagnosis was conrmed with polymerase chain reaction (PCR) examination and the positive result of the quantiferon
test. After an uneventful postoperative recovery, he was treated
with quadruple antituberculous therapy. He remained well, and no
evidence of recurrence of cancer has been seen during the 5 years
of follow-up after the surgery for anal canal cancer.
3. Discussion
The clinical course of this patient suggests two important clinical
issues. First, tuberculous lymphadenitis should be included among
the differential diagnoses of lymph node adenopathy in cancer
patients with a history of tuberculosis. Liver hilar lymphadenitis is uncommon and difcult to differentiate from other entities
such as cholangiocarcinoma, and many cases require surgery,
histology, and bacteriological conrmation to reach a denitive
diagnosis. Only 11 resected cases, including the present case, with
detailed information on patients with liver hilar lymphadenitis
have been reported in the well-documented English literature
[410] (Table 1). To the best of our knowledge, this report is the
rst to describe liver hilar tuberculous lymphadenitis diagnosed
CASE REPORT OPEN ACCESS
M. Wakasugi et al. / International Journal of Surgery Case Reports 10 (2015) 191194
193
Table 1
Surgical cases of liver hilar lymph node tuberculous in the English literature.
First author
Ref.
Year
Age (y)
Sex
Symptom
History of
tuberculosis
Preoperative
diagnosis
Surgery
Outcome
Roy
Kohen
[4]
[5]
1964
1973
53
21
F
F
Cholangiocarcinoma
NA
Tumor excision
T-tube drainage
11 Months alive
7 Months alive
Ratanarapee
Lee
[6]
[7]
1991
1994
38
27
F
M
Jaundice
Fever
Jaundice
Jaundice
Hematemesis
Cholangiocarcinoma
Portal vein hypertension
by enlarged lymph nodes
5 Years alive
3 Years alive
Poon
[8]
2001
20
Jaundice
Malignancy
Tuberculous
Poon
[8]
2001
34
Weight loss
Jaundice
Tuberculous
Malignancy
Saluja
[9]
2007
35
Anorexia
NA
GB cancer
Saluja
[9]
2007
70
Jaundice
NA
GB cancer
Saluja
Fernndez Muinelo
[9]
[10]
2007
2013
55
29
F
M
NA
Cholangiocarcinoma
Malignancy
2015
49
Jaundice
Jaundice
Abdominal
pain
None
Metastasis of anal canal
cancer
T-tube drainage
Splenorenal shunt
ligation of coronary
vein
Anastomosis of the
segment III duct to a
Roux en Y loop
Laparoscopy
percutaneous
biliary drainage
Cholecystectomy
T-tube drainage
Cholecystectomy
T-tube drainage
Hepatojejunostomy
Cholecystectomy
lymph node
enucleation
Laparoscopic lymph
node biopsy
Present case
Fig. 5. Pathological examination shows an epithelioid granuloma with caseous
necrosis within its center and yielded a suspected diagnosis of tuberculous lymphadenitis. The diagnosis was conrmed with polymerase chain reaction (PCR)
examination.
by laparoscopic surgery. A review of previously reported cases
revealed that liver hilar tuberculous lymphadenitis occurs most
frequently in young to middle age, with a median age of 35 years
(range, 2075 years). Most patients developed jaundice (8/11, 73%),
though the present case had no symptoms. Half of the patients (4/8,
50%) had a history of tuberculosis. The diagnosis of tuberculous
lymphadenitis was established before surgery in only 2 of 11 cases
(2/10, 20%). The remaining diagnoses were cholangiocarcinoma,
gallbladder carcinoma, metastasis of cancer, and portal vein hypertension. Surgical procedures included lymph node excision, T-tube
drainage with cholecystectomy, and biliary bypass. All the patients
had good prognoses. It was not possible to preoperatively diagnose
liver hilar tuberculous lymphadenitis because the present patient
with a medical history of advanced anal canal cancer underwent
right inguinal lymph node dissection twice previously, though he
had a history of pulmonary tuberculosis. In the present case, tuberculous lesions in the abdomen were clearly detected by FDG-PET
with a high SUVmax value. The previous reports [11,12] showed
2 Years alive
2 Months alive
NA
NA
NA
9 Months alive
7 Months alive
that FDG-PET imaging is rarely useful for differentiating cancer
from tuberculous lesions, because both conditions have increased
uptake of the FDG metabolite.
The second important clinical point is that laparoscopic lymph
node biopsy is useful as a diagnostic modality for undiagnosed lymphadenopathy. Ultrasound (US) or CT-guided ne needle aspiration
(FNA) may be useful for preoperative diagnosis because it allows
samples to be taken for bacteriology and cultures, but it has the disadvantage of disseminating potentially malignant or tuberculous
cells [12]. In practise, the diagnosis is often established at operation or even after surgery by histology or PCR-based assay, as in the
present case. With the progress of surgical techniques and devices,
laparoscopic lymph node biopsy has become an option for patients
with undiagnosed lymphadenopathy. Diulus et al. [13] reported
that laparoscopic lymph node biopsy is a safe effective alternative to open surgical biopsy in their 30 retrospective cases. The
pathological ndings in this case indicated that the patient without
jaundice did not need surgical intervention, but laparoscopic lymph
node biopsy seemed to provide less blood loss, a shorter duration of
hospitalization, and good cosmetic results, and also proved useful
in diagnosis.
4. Conclusions
Tuberculous lymphadenitis should be included among the differential diagnoses of liver hilar lymphadenopathy in patients with
a history of tuberculosis. Laparoscopic lymph node biopsy is useful
in the diagnosis of undiagnosed lymphadenopathy.
Conict of interest
The authors declare no potential conict of interest.
Funding
None.
CASE REPORT OPEN ACCESS
194
M. Wakasugi et al. / International Journal of Surgery Case Reports 10 (2015) 191194
Author contributions
Each author participated in writing the manuscript and all
agreed to accept equal responsibility for the accuracy of the content
of the paper.
Consent
Written informed consent was obtained from the patients for
the information to be included in our manuscript. His information has been de-identied to the best of our ability to protect his
privacy.
References
[1] A. Uzunkoy, M. Harma, M. Harma, Diagnosis of abdominal tuberculosis:
experience from 11 cases and review of the literature, World J. Gastroenterol.
10 (2004) 36473649.
[2] O. Uygur-Bayramicli, G. Dabak, R. Dabak, A clinical dilemma: abdominal
tuberculosis, World J. Gastroenterol. 9 (2003) 10981101.
[3] A. Shimouchi, A. Ohkado, K. Matsumoto, J. Komukai, H. Yoshida, N. Ishikawa,
Strengthened tuberculosis control programme and trend of multi-drug
resistant tuberculosis rate in Osaka City, Japan, Western Pac. Surveill.
Response J. 26 (4) (2013) 410.
[4] A.D. Roy, J. Allan, Obstructive jaundice due to tuberculous hepatic lymph
glands, Scot. Med. J. 9 (1964) 112114.
[5] M.D. Kohen, K.A. Altman, Jaundice due to a rare cause: tuberculous
lymphadenitis, Am. J. Gastroenterol. 59 (1973) 4853.
[6] S. Ratanarapee, A. Pausawasdi, Tuberculosis of the common bile duct, HPB
Surg. 3 (1991) 205208.
[7] C.W. Lee, Y.S. Lee, G.Y. Cho, J.Y. Kim, Y.I. Min, A case of extra-hepatic portal
hypertension caused by periportal tuberculous lymphadenitis, J. Korean Med.
Sci. 9 (1994) 264267.
[8] R.T. Poon, C.M. Lo, S.T. Fan, Diagnosis and management of biliary obstruction
due to periportal tuberculous adenitis, Hepatogastroenterology 48 (2001)
15851587.
[9] S.S. Saluja, S. Ray, S. Pal, M. Kukeraja, D.N. Srivastava, P. Sahni, et al.,
Hepatobiliary and pancreatic tuberculosis: a two decade experience, BMC
Surg. 7 (2007) 10.
Fernndez, P. Pardo
[10] A. Fernndez Muinelo, M. Salgado Vzquez, S. Nnez
Rojas, F.J. Gmez Lorenzo, Obstructive jaundice secondary to liver hilar lymph
node tuberculosis, Cir. Esp. 91 (2013) 611612.
[11] J.M. Goo, J.G. Im, K.H. Do, J.S. Yeo, J.B. Seo, H.Y. Kim, et al., Pulmonary
tuberculoma evaluated by means of FDG-PET: ndings in 10 cases, Radiology
216 (2000) 117121.
[12] K. Obama, M. Kanai, Y. Taki, Y. Nakamoto, A. Takabayashi, Tuberculous
lymphadenitis as a cause of obstructive jaundice: report of a case, Surg. Today
33 (2003) 229231.
[13] L. Diulus, S. Chalikonda, T. Pitt, S. Rosenblatt, Efcacy of laparoscopic
mesenteric/retroperitoneal lymph node biopsy, Surg. Endosc. 23 (2009)
389393.
Open Access
This article is published Open Access at sciencedirect.com. It is distributed under the IJSCR Supplemental terms and conditions, which
permits unrestricted non commercial use, distribution, and reproduction in any medium, provided the original authors and source are
credited.
You might also like
- Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy For Pseudomyxoma Peritonei in A Liver-Transplanted Patient: A Case ReportDocument5 pagesCytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy For Pseudomyxoma Peritonei in A Liver-Transplanted Patient: A Case Reportyerich septaNo ratings yet
- Sumber Jurnal ReadingDocument15 pagesSumber Jurnal ReadingagungNo ratings yet
- Carcinoma of The Exocrine Pancreas The Histology Report C Capella Et AlDocument11 pagesCarcinoma of The Exocrine Pancreas The Histology Report C Capella Et AlskorpyutzaNo ratings yet
- Esmo Guidline: Presentasi Oleh: Dr.I Nyoman Dwija Putra SP.BDocument45 pagesEsmo Guidline: Presentasi Oleh: Dr.I Nyoman Dwija Putra SP.BIrbah NabilaNo ratings yet
- International Journal of Surgery Case ReportsDocument4 pagesInternational Journal of Surgery Case Reportshussein_faourNo ratings yet
- Metastatic Spread of Primary Lung Adenocarcino - 2024 - International Journal ofDocument5 pagesMetastatic Spread of Primary Lung Adenocarcino - 2024 - International Journal ofRonald QuezadaNo ratings yet
- Hepatocellular Carcinoma 2009Document58 pagesHepatocellular Carcinoma 2009ctsakalakisNo ratings yet
- Revisión Del Carcinoma de Vesicula: Poster No.: Congress: Type: AuthorsDocument26 pagesRevisión Del Carcinoma de Vesicula: Poster No.: Congress: Type: AuthorsArturo García MarquezNo ratings yet
- It Is Not Always A Cholangiocarcinoma: Unusual Peritoneal Carcinomatosis Revealing Gastric AdenocarcinomaDocument5 pagesIt Is Not Always A Cholangiocarcinoma: Unusual Peritoneal Carcinomatosis Revealing Gastric AdenocarcinomaIJAR JOURNALNo ratings yet
- Recent Advances in Pancreatic Cancer Surgery of Relevance To The Practicing PathologistDocument7 pagesRecent Advances in Pancreatic Cancer Surgery of Relevance To The Practicing PathologistAndreaGomeroNo ratings yet
- European Association of Urology Guidelines On Upper Urinary Tract Urothelial Carcinoma: 2020 UpdateDocument43 pagesEuropean Association of Urology Guidelines On Upper Urinary Tract Urothelial Carcinoma: 2020 Updatecryptosaturn126No ratings yet
- Soria 2019Document7 pagesSoria 2019Dr. Alexandre SatoNo ratings yet
- Background: Go ToDocument5 pagesBackground: Go ToАлександр КравченкоNo ratings yet
- Jurnal Sitologi UrineDocument10 pagesJurnal Sitologi UrineAjip JenNo ratings yet
- BVBVDocument11 pagesBVBVŽeljko ĐurićNo ratings yet
- Primary Pure Squamous Cell Carcinoma of The Duodenum: A Case ReportDocument4 pagesPrimary Pure Squamous Cell Carcinoma of The Duodenum: A Case ReportGeorge CiorogarNo ratings yet
- Cholangitis With Acute Renal FailureDocument7 pagesCholangitis With Acute Renal FailureAtos MacêdoNo ratings yet
- Hepatocellular Carcinoma - Diagnosis and TreatmentDocument46 pagesHepatocellular Carcinoma - Diagnosis and TreatmentSigh BalaNo ratings yet
- A Case of Advanced Esophageal Cancer With Extensive Lymph Node Metastases Successfully Treated With Multimodal TherapyDocument0 pagesA Case of Advanced Esophageal Cancer With Extensive Lymph Node Metastases Successfully Treated With Multimodal TherapyAmirahShalehaNo ratings yet
- Literature Review of Liver AbscessDocument4 pagesLiterature Review of Liver Abscessc5ng67v1100% (1)
- EMEA GI GEN P10 Megapixel Scopes in Bcs Improve Polyp Detection 10.2011Document6 pagesEMEA GI GEN P10 Megapixel Scopes in Bcs Improve Polyp Detection 10.2011Dr Muhammad Abdul QadirNo ratings yet
- Current Opinion On Lymphadenectomy in Pancreatic Cancer SurgeryDocument5 pagesCurrent Opinion On Lymphadenectomy in Pancreatic Cancer Surgeryyacine26No ratings yet
- Whipple Procedure and Its Complications: What Every Radiologist Should KnowDocument17 pagesWhipple Procedure and Its Complications: What Every Radiologist Should KnowYacine Tarik AizelNo ratings yet
- PIIS0923753422046993Document14 pagesPIIS0923753422046993Justitia Yudiarti BasriNo ratings yet
- Nej Mo A 1414882Document9 pagesNej Mo A 1414882Corina Hagiu-RaduNo ratings yet
- Imaging Features of Combined Hepatocellular Carcinoma and Intrahepatic Cholangiocarcinoma in Patients Undergoing Liver SurgeryDocument19 pagesImaging Features of Combined Hepatocellular Carcinoma and Intrahepatic Cholangiocarcinoma in Patients Undergoing Liver SurgeryNarakusuma WirawanNo ratings yet
- International Journal of Surgery: Original ResearchDocument9 pagesInternational Journal of Surgery: Original ResearchrejNo ratings yet
- Multiple Hepatic Sclerosing HemangiomaDocument4 pagesMultiple Hepatic Sclerosing Hemangiomahussein_faourNo ratings yet
- Case ReportDocument3 pagesCase Reportyena hillNo ratings yet
- Studiu Comparativ Al Factorilor Asociați Trombozei Venoase Portale La Pacienții Cirotici Cu Sau Fără HepatocarcinomDocument7 pagesStudiu Comparativ Al Factorilor Asociați Trombozei Venoase Portale La Pacienții Cirotici Cu Sau Fără HepatocarcinomAna BocaNo ratings yet
- International Journal of Surgery Case ReportsDocument3 pagesInternational Journal of Surgery Case Reportshussein_faourNo ratings yet
- Carcinoid Tumor of The Appendix: A Case ReportDocument3 pagesCarcinoid Tumor of The Appendix: A Case ReportrywalkNo ratings yet
- Apendisitis MRM 3Document8 pagesApendisitis MRM 3siti solikhaNo ratings yet
- Totally Laparoscipic Right Colectomy: Technique Description: Hepato-Gastroenterology April 2015Document5 pagesTotally Laparoscipic Right Colectomy: Technique Description: Hepato-Gastroenterology April 2015anatomNo ratings yet
- Modern Imaging in Obstructive JaundiceDocument4 pagesModern Imaging in Obstructive JaundicedanaogreanuNo ratings yet
- JurnalDocument9 pagesJurnalFrans 'cazper' SihombingNo ratings yet
- Cutaneous Needle Aspirations in Liver DiseaseDocument6 pagesCutaneous Needle Aspirations in Liver DiseaseRhian BrimbleNo ratings yet
- Vita EDocument5 pagesVita ELinaena MericyNo ratings yet
- Ecr2008 C 010Document10 pagesEcr2008 C 010jbmbritoNo ratings yet
- Dynamic CT Findings of A Polypoid Gastric - ChrisnaDocument4 pagesDynamic CT Findings of A Polypoid Gastric - ChrisnaferonicaNo ratings yet
- Colorectal Cancer: Section 7Document3 pagesColorectal Cancer: Section 7MANGNo ratings yet
- Aghiz 3Document12 pagesAghiz 3nandaaa aprilNo ratings yet
- Clinical Practice Guidelines: Biliary Cancer: ESMO Clinical Practice Guidelines For Diagnosis, Treatment and Follow-UpDocument10 pagesClinical Practice Guidelines: Biliary Cancer: ESMO Clinical Practice Guidelines For Diagnosis, Treatment and Follow-UpPutri MauraNo ratings yet
- Powerpoint GOT GPTDocument5 pagesPowerpoint GOT GPTCooghen DevNo ratings yet
- RJX 102Document3 pagesRJX 102FachryNo ratings yet
- Diagnosis and Management of Choledochal Cyst: 20 Years of Single Center ExperienceDocument7 pagesDiagnosis and Management of Choledochal Cyst: 20 Years of Single Center ExperienceSurgeon RANo ratings yet
- Case Report: A Case Report of Peritoneal Tuberculosis: A Challenging DiagnosisDocument4 pagesCase Report: A Case Report of Peritoneal Tuberculosis: A Challenging DiagnosisDumitru RadulescuNo ratings yet
- Clinicopathological Features and Treatment OutcomeDocument9 pagesClinicopathological Features and Treatment Outcomesyfs92ctpvNo ratings yet
- Pi Is 0140673612605121Document1 pagePi Is 0140673612605121farel@No ratings yet
- JurnalDocument8 pagesJurnalAlm12345No ratings yet
- Hepatic CancerDocument15 pagesHepatic CancerTrinh TrầnNo ratings yet
- 50 Postoperative Mortality and Morbidity in Older Patients Undergoing Emergency Right Hemicolectomy For Colon CancerDocument6 pages50 Postoperative Mortality and Morbidity in Older Patients Undergoing Emergency Right Hemicolectomy For Colon CancerJoao FonsecaNo ratings yet
- 1 s2.0 S2667008923000253 MainDocument4 pages1 s2.0 S2667008923000253 Mainal malikNo ratings yet
- Primary Congenital Choledochal Cyst With Squamous Cell Carcinoma: A Case ReportDocument6 pagesPrimary Congenital Choledochal Cyst With Squamous Cell Carcinoma: A Case ReportRais KhairuddinNo ratings yet
- Pone 0166157Document12 pagesPone 0166157cindydmjktNo ratings yet
- Modern Management of Pyogenic Hepatic Abscess: A Case Series and Review of The LiteratureDocument8 pagesModern Management of Pyogenic Hepatic Abscess: A Case Series and Review of The LiteratureAstari Pratiwi NuhrintamaNo ratings yet
- An Unusual Presentation of Multiple Cavitated Lung Metastases From Colon CarcinomaDocument4 pagesAn Unusual Presentation of Multiple Cavitated Lung Metastases From Colon CarcinomaGita AmeliaNo ratings yet
- An Unresectable Klatskin's Tumor?: Johannes Hartl, Tobias Werner, and Christoph SchrammDocument2 pagesAn Unresectable Klatskin's Tumor?: Johannes Hartl, Tobias Werner, and Christoph SchrammLourdes MollardNo ratings yet
- Imaging of the Liver and Intra-hepatic Biliary Tract: Volume 2: Tumoral PathologiesFrom EverandImaging of the Liver and Intra-hepatic Biliary Tract: Volume 2: Tumoral PathologiesNo ratings yet
- Complications of Female Incontinence and Pelvic Reconstructive SurgeryDocument333 pagesComplications of Female Incontinence and Pelvic Reconstructive Surgeryhussein_faourNo ratings yet
- Multiple Hepatic Sclerosing HemangiomaDocument4 pagesMultiple Hepatic Sclerosing Hemangiomahussein_faourNo ratings yet
- International Journal of Surgery Case ReportsDocument4 pagesInternational Journal of Surgery Case Reportshussein_faourNo ratings yet
- International Journal of Surgery Case ReportsDocument3 pagesInternational Journal of Surgery Case Reportshussein_faourNo ratings yet
- DVT PE Wallchart A2 1Document1 pageDVT PE Wallchart A2 1hussein_faourNo ratings yet
- International Journal of Surgery Case ReportsDocument4 pagesInternational Journal of Surgery Case Reportshussein_faourNo ratings yet
- Table Accessories BrochureJuly2015Web1Document36 pagesTable Accessories BrochureJuly2015Web1hussein_faourNo ratings yet
- International Journal of Surgery Case ReportsDocument7 pagesInternational Journal of Surgery Case Reportshussein_faourNo ratings yet
- Outpatient Algorithm For The Management of DVT/PE: Optional: HCO LogoDocument1 pageOutpatient Algorithm For The Management of DVT/PE: Optional: HCO Logohussein_faourNo ratings yet
- Pi Is 2210261215001479Document3 pagesPi Is 2210261215001479hussein_faourNo ratings yet
- Pi Is 2210261215001376Document6 pagesPi Is 2210261215001376hussein_faourNo ratings yet
- Obstetrics & Gynaecology Operating TableDocument6 pagesObstetrics & Gynaecology Operating Tablehussein_faourNo ratings yet
- Operating: Quality Performance Trust CompletelyDocument12 pagesOperating: Quality Performance Trust Completelyhussein_faourNo ratings yet
- International Journal of Surgery Case ReportsDocument4 pagesInternational Journal of Surgery Case Reportshussein_faourNo ratings yet
- Setting A New Level For Operating Table PerformanceDocument20 pagesSetting A New Level For Operating Table Performancehussein_faour0% (1)
- International Journal of Surgery Case ReportsDocument5 pagesInternational Journal of Surgery Case Reportshussein_faourNo ratings yet
- International Journal of Surgery Case ReportsDocument3 pagesInternational Journal of Surgery Case Reportshussein_faourNo ratings yet
- International Journal of Surgery Case ReportsDocument4 pagesInternational Journal of Surgery Case Reportshussein_faourNo ratings yet
- International Journal of Surgery Case ReportsDocument3 pagesInternational Journal of Surgery Case Reportshussein_faourNo ratings yet
- International Journal of Surgery Case ReportsDocument5 pagesInternational Journal of Surgery Case Reportshussein_faourNo ratings yet
- His Tuberculosis Fish Bone Diagram FinalDocument1 pageHis Tuberculosis Fish Bone Diagram FinalJadekookinNo ratings yet
- November 2008 QP - Paper 2 CIE Biology A-LevelDocument29 pagesNovember 2008 QP - Paper 2 CIE Biology A-Levelaimee simarnoNo ratings yet
- غيث GTITHDocument199 pagesغيث GTITHElsayed Abdallah100% (2)
- Tuberculosis - Wikipedia, The Free EncyclopediaDocument15 pagesTuberculosis - Wikipedia, The Free EncyclopediaitsmepranielNo ratings yet
- Grade 10 HTHDocument4 pagesGrade 10 HTHRachelle Mae Pablo100% (1)
- GV Keynotes OldDocument362 pagesGV Keynotes OldMd Jahirul Islam100% (1)
- Death From Orange PithDocument1 pageDeath From Orange PithMwagaVumbiNo ratings yet
- PDF of Beautiful Bombshell Christina Lauren Full Chapter EbookDocument69 pagesPDF of Beautiful Bombshell Christina Lauren Full Chapter Ebooklconccoffcc584100% (8)
- Sulfamethoxazole Trimethoprim PDFDocument10 pagesSulfamethoxazole Trimethoprim PDFAsi SyyffaNo ratings yet
- Collection of Systematic Bacteriology (Mansoura Dentistry)Document16 pagesCollection of Systematic Bacteriology (Mansoura Dentistry)elsayed barhomeNo ratings yet
- Full Download PDF of Test Bank For Ethics and Law in Dental Hygiene 3rd Edition by Beemsterboer All ChapterDocument31 pagesFull Download PDF of Test Bank For Ethics and Law in Dental Hygiene 3rd Edition by Beemsterboer All Chapterdeiibimala100% (4)
- Biology Project: Topic: Human Health and DiseasesDocument17 pagesBiology Project: Topic: Human Health and DiseasesSagar Kumar0% (1)
- PSM LMRP 2019Document25 pagesPSM LMRP 2019skNo ratings yet
- CHN2 RLE Shifting ExamDocument34 pagesCHN2 RLE Shifting ExamEya BaldostamonNo ratings yet
- Laporan Data TB Tahun 2019Document36 pagesLaporan Data TB Tahun 2019rekam medis murni asihNo ratings yet
- Anti-Infectives Drug Advisory Committee MeetingDocument253 pagesAnti-Infectives Drug Advisory Committee MeetingbellamajNo ratings yet
- The IndiansDocument22 pagesThe Indianskayes82No ratings yet
- CD DRILLS (Communicable DiseasesDocument8 pagesCD DRILLS (Communicable DiseasesJune DumdumayaNo ratings yet
- Ad For Natbps WB PDFDocument7 pagesAd For Natbps WB PDFrajpal singhNo ratings yet
- Referat - TB Paru Pada Anak (Irma S.M)Document21 pagesReferat - TB Paru Pada Anak (Irma S.M)Irma Sari MuliadiNo ratings yet
- Application FormateDocument8 pagesApplication FormatesivakumarNo ratings yet
- Che 224 Immunity and ImmunizationDocument54 pagesChe 224 Immunity and ImmunizationAbdullahi Bashir SalisuNo ratings yet
- Zimbabwe National Tuberculosis and Leprosy Management Guidelines - FinalDocument222 pagesZimbabwe National Tuberculosis and Leprosy Management Guidelines - FinalRichard Makurumidze Senior100% (9)
- Jurnal 2Document3 pagesJurnal 2Renita Mandalinta SitepuNo ratings yet
- Status of Tuberculosis-Related Stigma and Associated Factors: A Cross-Sectional Study in Central ChinaDocument7 pagesStatus of Tuberculosis-Related Stigma and Associated Factors: A Cross-Sectional Study in Central ChinaDesy AmaliaNo ratings yet
- LEPROSYDocument7 pagesLEPROSYArron Buenavista AblogNo ratings yet
- Tubercular Osteomyelitis of Calcaneum Bone: A Rare OccurrenceDocument4 pagesTubercular Osteomyelitis of Calcaneum Bone: A Rare OccurrenceMuh Syarifullah ANo ratings yet
- Communicable Disease Prevention and ControlDocument197 pagesCommunicable Disease Prevention and Controldennisjamesbartz100% (1)
- Pulmonary Tuberculosis Presenting With Acute Respiratory Distress Syndrome (ARDS) : A Case Report and Review of LiteratureDocument5 pagesPulmonary Tuberculosis Presenting With Acute Respiratory Distress Syndrome (ARDS) : A Case Report and Review of LiteratureCimol AgustinaNo ratings yet