Professional Documents
Culture Documents
Jurnal Embriologi
Jurnal Embriologi
Uploaded by
Muhammad AriefCopyright:
Available Formats
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5825)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (852)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (903)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (541)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (349)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (823)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (403)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- NCLEX - Fluids and ElectrolytesDocument4 pagesNCLEX - Fluids and ElectrolytesissaiahnicolleNo ratings yet
- 15-10-2019, Mr. Jamal, 50 Yo, V.Laceratum Cruris Dextra + Skin Loss + Fraktur Os Fibula, Dr. Moh. Rizal Alizi, M.Kes, Sp. OT-1Document15 pages15-10-2019, Mr. Jamal, 50 Yo, V.Laceratum Cruris Dextra + Skin Loss + Fraktur Os Fibula, Dr. Moh. Rizal Alizi, M.Kes, Sp. OT-1anon_893244902No ratings yet
- Babesioza - Teza Doctorat PDFDocument90 pagesBabesioza - Teza Doctorat PDFAndras AndreescuNo ratings yet
- 6 Birth DefectsDocument40 pages6 Birth DefectsjulieNo ratings yet
- Brochure - ILLUCO Dermatoscope IDS-1100Document2 pagesBrochure - ILLUCO Dermatoscope IDS-1100Ibnu MajahNo ratings yet
- Resumen Article IcDocument4 pagesResumen Article Icapi-689165620No ratings yet
- Hormonal ImbalanceDocument3 pagesHormonal ImbalanceShan Armaine CabelaNo ratings yet
- Dr. Wahyuni Indawati, Spa (K)Document43 pagesDr. Wahyuni Indawati, Spa (K)Rara AnisaNo ratings yet
- Manajemen StrokeDocument253 pagesManajemen StrokeHappy Pramanda100% (2)
- Transanal Protocol PDFDocument4 pagesTransanal Protocol PDFDesiree FlorendoNo ratings yet
- What Is Pneumonia?: Patient EducationDocument2 pagesWhat Is Pneumonia?: Patient EducationDian Putri NingsihNo ratings yet
- The Effects of Lifestyle To Respiratory and Circulatory SystemsDocument11 pagesThe Effects of Lifestyle To Respiratory and Circulatory SystemsSharalyn Sia100% (1)
- MFG E8介导的骨免疫在牙周炎中的作用研究进展 向群Document5 pagesMFG E8介导的骨免疫在牙周炎中的作用研究进展 向群颜加龙No ratings yet
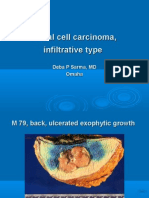
- Basal Cell Carcinoma, Infiltrative TypeDocument8 pagesBasal Cell Carcinoma, Infiltrative TypeDeba P SarmaNo ratings yet
- OSCE StationsDocument3 pagesOSCE StationsKristoff FiguerasNo ratings yet
- Reference/normal Values Result Interpretation What Have Caused The Abnormality/ Purpose/NIDocument5 pagesReference/normal Values Result Interpretation What Have Caused The Abnormality/ Purpose/NIKristian Karl Bautista Kiw-isNo ratings yet
- Diagnostic Exam-Health Specialist EditDocument9 pagesDiagnostic Exam-Health Specialist EditAyuy Welliss MedusaNo ratings yet
- Dugs CVADocument10 pagesDugs CVAMarie AntoinetteNo ratings yet
- Pathfit 1 M3Document20 pagesPathfit 1 M3rainiel gibasNo ratings yet
- GCSE Week 12 Pathogens and DiseaseDocument27 pagesGCSE Week 12 Pathogens and DiseaseFrankie BarnesNo ratings yet
- Health, Safety, Environmental Management Manual: Loshini ProjectsDocument6 pagesHealth, Safety, Environmental Management Manual: Loshini ProjectsThandabantu MagengeleleNo ratings yet
- QCGH FormDocument4 pagesQCGH FormKim Delaney MadridNo ratings yet
- Cardiovascular System Drugs - Active Stack® Pharmacology Flash Cards - Study Materials - My ATIDocument1 pageCardiovascular System Drugs - Active Stack® Pharmacology Flash Cards - Study Materials - My ATIAntonette Joy SolinapNo ratings yet
- ChickenpoxDocument2 pagesChickenpoxNorhana LangiNo ratings yet
- WHO 2022 Bladder PDFDocument92 pagesWHO 2022 Bladder PDFOlteanu Dragos-NicolaeNo ratings yet
- HypochondriasisDocument3 pagesHypochondriasisLaura Pauline KosasihNo ratings yet
- Disease Deep Dive Kathryn CrimDocument7 pagesDisease Deep Dive Kathryn Crimapi-579320483No ratings yet
- Retroperitoneal Abscess Caused by Dropped RenalDocument4 pagesRetroperitoneal Abscess Caused by Dropped RenalNatalindah Jokiem Woecandra T. D.No ratings yet
- John Case StudyDocument6 pagesJohn Case Studyapi-283887910No ratings yet
- Radiology Quiz Medical Students Workbook: Author: DR Aussami Abbas SPR RadiologyDocument11 pagesRadiology Quiz Medical Students Workbook: Author: DR Aussami Abbas SPR RadiologyMădălina Ciobotariu100% (1)
Jurnal Embriologi
Jurnal Embriologi
Uploaded by
Muhammad AriefCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Jurnal Embriologi
Jurnal Embriologi
Uploaded by
Muhammad AriefCopyright:
Available Formats
The
n e w e ng l a n d j o u r na l
of
m e dic i n e
case records of the massachusetts general hospital
Founded by Richard C. Cabot
Nancy Lee Harris, m.d., Editor
Eric S. Rosenberg, m.d., Associate Editor
Jo-Anne O. Shepard, m.d., Associate Editor
Alice M. Cort, m.d., Associate Editor
Sally H. Ebeling, Assistant Editor
Christine C. Peters, Assistant Editor
Case 24-2011: A 36-Year-Old Man
with Headache, Memory Loss, and Confusion
Don C. Bienfang, M.D., Michael J. McKenna, M.D., George N. Papaliodis, M.D.,
R. Gilberto Gonzalez, M.D., Ph.D., and Anat Stemmer-Rachamimov, M.D.
Pr e sen tat ion of C a se
Dr. M. Brandon Westover (Neurology): A 36-year-old right-handed man was seen in the
neurology clinic of this hospital because of headaches, confusion, and memory loss.
The patient had been well until 1 month earlier, when nausea, fevers, chills, diarrhea, malaise, and myalgias developed and lasted 2 days. During the next 3 days, he
had a constant headache centered between his eyes, with a sensation of squeezing.
The headache resolved, but 5 days later his wife noted that he seemed apathetic and
confused on awakening, with loss of short-term memory. He was admitted to another hospital. On examination, the patient, who appeared to be unconcerned, had
decreased concentration and was unable to remember three items when questioned
3minutes later; the examination was otherwise normal.
Results of routine laboratory tests were normal; a test for Lyme disease was
negative. Magnetic resonance imaging (MRI) reportedly showed lesions with restricted diffusion in the periventricular and subcortical white matter and the corpus
callosum. A scan of the head and neck obtained with magnetic resonance angiography was reportedly normal. A lumbar puncture was performed; the results of cerebrospinal fluid analysis are shown in Table 1. Treatment with acyclovir was begun.
Electroencephalography (EEG) reportedly revealed episodes of generalized irregular
high-voltage delta activity throughout, but more prominent anteriorly and enhancing
on hyperventilation. There were also intermittent, brief episodes of sharp theta activity and transient sharp waves with phase reversals over the left midtemporal region.
Treatment with levetiracetam was begun. A repeat EEG revealed occasional left
frontotemporal sharp waves with phase reversals at T3, with intermittent generalized slowing, slightly more severe on the left and a diffusely slow background, with
no spike or polyspike activity. MRI performed after the administration of gadolinium
reportedly showed new hyperintense, nonenhancing lesions in the corpus callosum
and left cerebellum.
The patient was discharged on the sixth day in improved condition, with prescriptions for levetiracetam and butalbitalacetaminophencaffeine and instructions to
follow up with a neurologist. He returned to work but was unable to concentrate.
Two weeks later, he was seen in the neurology clinic of this hospital.
From the Division of Neuro-Ophthalmology, Brigham and Womens Hospital
(D.C.B.); the Otology and Neurotology
Service (M.J.M.) and the Department of
Ophthalmology (G.N.P.), Massachusetts
Eye and Ear Infirmary; the Departments
of Radiology (R.G.G.) and Pathology
(A.S.-R.), Massachusetts General Hospital; and the Departments of Ophthalmology (D.C.B., G.N.P.), Otology and Laryngology (M.J.M.), Radiology (R.G.G.), and
Pathology (A.S.-R.), Harvard Medical
School all in Boston.
N Engl J Med 2011;365:549-59.
Copyright 2011 Massachusetts Medical Society.
n engl j med 365;6 nejm.org august 11, 2011
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2011. For personal use only. No other uses without permission.
Copyright 2011 Massachusetts Medical Society. All rights reserved.
549
The
n e w e ng l a n d j o u r na l
of
m e dic i n e
Table 1. Cerebrospinal Fluid Analysis.*
Reference Range,
Adults
Variable
Other Hospital
On Admission, 20 Days
before Presentation to
Neurology Clinic
Opening pressure (cm of water)
This Hospital
1st Admission, 4.25 Mo
after Presentation
2nd Admission, 5 Mo
after Presentation
26
24
Appearance
Tube 1
Colorless, clear
Colorless, clear
Light pink, slightly turbid
Tube 4
Colorless, clear
Colorless, clear
Light yellow, clear
None
Yes
Xanthochromia
Red cells (per mm
3)
Tube 1
83
12
2070
Tube 4
Tube 1
05
Tube 4
05
Lymphocytes
98
94
95
Monocytes
White cells (per mm3)
Differential count, tube 4 (%)
Protein (mg/dl)
555
266
211
257
Glucose (mg/dl)
5075
65
63
89
No cells or organisms
Few mononuclear cells,
no organisms
Moderate mononuclear
cells, no organisms
Grams stain
Fungal wet preparation
Culture
No organisms
No organisms
No growth
No growth
Enterovirus RNA, PCR
Negative
Negative
Herpes simplex virus DNA, PCR
Negative
Negative
Cytomegalovirus DNA, PCR
Negative
Varicellazoster virus, PCR
EpsteinBarr virus DNA, PCR
No growth
No growth
Negative, types 1 and 2
Negative
Negative
Negative
None detected
None detected
Venereal Disease Research Laboratory
test
Nonreactive
Cryptococcal antigen
Negative
Angiotensin-converting enzyme (U/liter)
IgG (mg/dl)
<10
<2
08.0
Albumin (mg/dl)
Oligoclonal bands on agarose-gel
electrophoresis
Ratio of CSF IgG:albumin to serum
IgG:albumin
23.6
11.050.9
159.0
None seen in 80
concentrate
Two seen in 63
concentrate
<0.66
0.67
* CSF denotes cerebrospinal fluid, and PCR polymerase chain reaction. To convert the values for glucose to millimoles per liter, multiply by
0.05551.
Reference values are affected by many variables, including the patient population and the laboratory methods used. The ranges used at
Massachusetts General Hospital are for adults who are not pregnant and do not have medical conditions that could affect the results. They
may therefore not be appropriate for all patients.
This ratio is calculated by dividing the ratio of CSF levels of IgG to albumin by the ratio of serum levels of IgG to albumin.
550
n engl j med 365;6 nejm.org august 11, 2011
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2011. For personal use only. No other uses without permission.
Copyright 2011 Massachusetts Medical Society. All rights reserved.
case records of the massachusetts gener al hospital
The patient had a history of allergic rhinitis
and reported having had one episode of sinusitis.
He was born and lived in New England with his
wife and child, worked in a professional occupation, and owned a dog. He drank alcohol in moderation; he did not smoke or use illicit drugs. His
father had coronary artery disease and a myocardial infarction at 40 years of age; his mother had
a history of poorly defined cognitive symptoms
that started when she was 60 years of age, congestive heart failure, and alcohol abuse; and his
maternal grandmother had dementia in late adulthood. His brother was well.
On examination, the patient appeared well,
with normal social behavior and articulate speech,
and he was fully oriented to person, place, and
time. He recalled 2 items out of 5 viewed 5 minutes earlier, and after cues recalled 4 items out of
5 viewed 10 minutes earlier. He named 14 animals in 1 minute; the result of the forward digitspan test was 7, and that of the reverse digit-span
test was 5. The tone in his limbs was slightly
above normal, more on the right than on the left;
all reflexes were brisk, and the plantar responses
were flexor; the remainder of the neurologic examination was normal. Levetiracetam was discontinued.
During the next 3 months, intermittent tremulousness of his left hand developed; his fatigue
and mental endurance gradually improved, and
he returned to work part-time. Four weeks after
evaluation, an EEG showed no epileptiform activity. MRI of the brain showed multiple hyperintense lesions in the periventricular, infratentorial,
and subcortical white matter and the corpus callosum on T2-weighted images. Repeat MRI of the
brain 2 months later showed a decrease in the
size and number of the white-matter lesions; MRI
of the spine was normal.
Approximately 3 months after the patients initial presentation, insomnia and increasing fatigue
developed. One month later, frontal headache,
somnolence, and memory loss recurred, and he
came to the emergency department. On examination, the blood pressure was 148/76 mm Hg; other
vital signs were normal. On neurologic examination, he was fully oriented, recalled one out of
three items presented 5 minutes earlier, was unable to spell world backward, and exhibited perseveration. The remainder of the examination was
normal. A complete blood count and differential
count, electrolyte levels, glucose levels, and tests
of renal function were normal. A computed tomographic (CT) scan of the brain was normal.
T2-weighted, fluid-attenuated inversion recovery
(FLAIR) images obtained with MRI showed new
bilateral, hyperintense lesions in the right frontal
subcortical and deep white matter, with enhancing lesions in the right cingulate and superior
frontal gyri, the left caudate body, and cerebellum. The images also revealed persistent lesions
in the corpus callosum and in areas of mildly
restricted diffusion in the right cingulate gyrus
and left parietal lobe. The patient was admitted
to the hospital.
Evaluations for hypercoagulability, rheumatologic and autoimmune diseases, and infectious
agents were negative. Cytologic examination of
the cerebrospinal fluid showed no evidence of
cancer; flow cytometry showed no abnormal
cells; the results of other analyses are shown in
Table 1. CT angiography of the head and cerebrum was normal. Transthoracic echocardiography was normal, and a skin test for tuberculosis
was negative. A biopsy of the right frontal lobe
and meninges was performed; pathological examination of tissue specimens revealed small
vessels with changes suggestive of a microangiopathy. Methylprednisolone (a daily intravenous
dose of 1000 mg for 3 days) and cefazolin were
administered. The patient was discharged on the
seventh day with a prescription for 80 mg of oral
prednisone to be taken daily for 4 weeks and
then tapered.
Two weeks later, increased confusion developed, and the patient awoke with a black spot
in the superior visual field of the left eye, which
resolved spontaneously after 12 hours. He came
to the emergency room, where he reported lightheadedness, a mild headache, and fluctuating
hearing loss. An MRI scan revealed a new punctate focus of restricted diffusion in the left splenium of the corpus callosum and unchanged foci
of hyperintensity on T2-weighted FLAIR images
in the white matter of both hemispheres. He was
readmitted.
Findings on examination were unchanged.
The results of CT angiography were normal. Although the patient reported no diplopia or visual
loss, ophthalmologic examination revealed nonspecific visual-field constriction in both eyes,
vascular narrowing in both retinas, with sheath-
n engl j med 365;6 nejm.org august 11, 2011
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2011. For personal use only. No other uses without permission.
Copyright 2011 Massachusetts Medical Society. All rights reserved.
551
The
n e w e ng l a n d j o u r na l
of
m e dic i n e
ing, and vascular beading in the left eye, with no affects the brain, the eyes, and the auditory syspapillitis. Results of cerebrospinal fluid analysis tem, and we must consider disorders that can afare shown in Table 1.
fect these systems.
A diagnostic procedure was performed.
Cogans Syndrome
Differ en t i a l Di agnosis
Dr. Don C. Bienfang: May we review the imaging
studies?
Dr. R. Gilberto Gonzalez: MRI was performed at
this hospital 1 month after the patients initial
evaluation in the clinic. Axial FLAIR-weighted
images obtained with MRI at the level of and
superior to the lateral ventricles reveal multiple,
small T2-weighted and FLAIR hyperintense signal
abnormalities in the white matter within the corpus callosum and in the periventricular white
matter. A few similar signal abnormalities were
identified in the deep gray matter, including that
in the right caudate nucleus. The sagittal FLAIR
sequence (Fig. 1A) shows that a few of the lesions involved the entire thickness of the corpus
callosum. Several of the signal abnormalities displayed hyperintensity on diffusion-weighted imaging, but none showed reduced diffusion. An
MRI study repeating that performed at the time
of his first admission to this hospital revealed
new signal abnormalities with similar characteristics (Fig. 1B), but several of the lesions showed
areas of enhancement after the administration of
contrast material, and several of the abnormalities showing hyperintensity on diffusion-weighted
imaging now showed reduced diffusion (Fig. 1C).
Before the diagnostic procedure, another MRI revealed additional new lesions with characteristics
similar to those of the lesions previously identified (not shown).
Dr. Bienfang: This young man presented with a
waxing and waning illness, the major manifestations of which were changes in mental status
and evidence of inflammation, suggested by the
symptom of headache and confirmed by cytologic
and chemical analysis of cerebrospinal fluid. Extensive testing for infectious and rheumatologic
conditions was negative. The MRI of the brain
disclosed multiple lesions in the gray and white
matter, the most striking of which were punchedout holes in the corpus callosum. Finally, the patient reported symptoms of retinal vascular occlusion in both eyes and hearing loss, both of
which were confirmed on examination. The patient thus has an inflammatory condition that
552
In 1945, David Cogan1 described a syndrome of
interstitial corneal keratitis associated with sudden onset of deafness and vestibular symptoms,
occurring most commonly in persons in their 20s.
A characteristic of the deafness in most cases is its
sudden onset, whereas the visual symptoms (reduced vision and light sensitivity) fluctuate. Slitlamp examination reveals interstitial keratitis that
may mimic that which occurs in syphilis, and
there may be episcleritis or retinal vascular occlusion. The latter may be associated with systemic
vasculitis or inflammatory bowel disease.2,3 This
patient was not reported to have corneal abnormalities, did not have the vestibular symptoms
characteristic of Cogans syndrome, and had
rather subtle hearing loss.
Acute Posterior Multifocal Placoid Pigment
Epitheliopathy
The inflammatory disorder acute posterior multifocal placoid pigment epitheliopathy affects the
retina and choroid of otherwise young healthy
adults4 and has some features in common with
the presentation of this patient in that the retina
is involved with visual changes and in some cases
the central nervous system can be affected,5 with
headache, changes in mentation, and even strokelike episodes. However, this disorder creates creamycolored plaques in the retina, which have not been
found in this patient, and it is self-limited and typically lasts only a few weeks. Hearing changes are
not present.
Eales Disease
The retinal venous and arterial vasculopathy known
as Eales disease can sometimes affect the vestibularauditory system, and thus it has some similarity to the findings in this patient.6 However,
the findings within the retina are not subtle, as
they are in this case,7 but are usually characterized
by dramatic hemorrhages.
Whipples Disease
Infection with Tropheryma whipplei is manifested in
numerous locations, including the central nervous
system.8,9 However, gastrointestinal involvement
with malabsorption, a cardinal feature of the ill-
n engl j med 365;6 nejm.org august 11, 2011
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2011. For personal use only. No other uses without permission.
Copyright 2011 Massachusetts Medical Society. All rights reserved.
case records of the massachusetts gener al hospital
Figure 1. MRI Studies.
A sagittal fluid-attenuated inversion recovery image obtained 1 month after the patients first evaluation at this hospital shows multiple hyperintense signal abnormalities involving the corpus callosum (Panel A, arrows). Several of
the abnormalities involved the entire thickness of the corpus callosum. A diffusion-weighted image (Panel B) and an
apparent-diffusion-coefficient image (Panel C) from an MRI scan obtained at the first admission to this hospital
show a signal abnormality with reduced diffusion in the left splenium of the corpus callosum (arrows).
ness, is not present in this patient, and joint symptoms are common. Finally, the findings in the eye
in Whipples disease are predominantly visible
cellular infiltrates in the vitreous or aqueous humor, in contrast to the findings in this case.10
it is associated with cellular infiltration of the peripheral vitreous.
ChurgStrauss Syndrome
Although the ChurgStrauss syndrome may be
manifested in the eye as a uveitis,14 asthma is the
Lyme Disease
primary feature of this disease.15 The pathology is
Late in the evolution of Lyme disease, which is that of a necrotizing vasculitis.16
similar to another spirochetal infection, syphilis,
the central nervous system can be affected. How- Crohns Disease
ever, the major manifestation of Lyme disease is Patients with Crohns disease always have bowel
meningitis.11,12 The nerve most commonly affect- symptoms, and when the disease involves the eye,
ed is the facial nerve (cranial nerve VII).13 Retinal the features mimic those of anterior or posterior
vasculitis and hearing loss would be unusual, and uveitis, not retinal vasculitis.
testing for antibodies to Borrelia burgdorferi should
Susacs Syndrome
be positive.
Dr. Bienfang: I believe this patient must have Susacs
Central Nervous System Lymphoma
syndrome,17-20 a vasculopathic condition that afLymphoma of the central nervous system may fects the brain, vision (owing to retinal artery ochave variable neurologic manifestations and may clusion), and hearing. All three features may not
affect the eye by means of cellular infiltration of be present, or they may emerge slowly, thus obthe vitreous. However, the results of the brain bi- scuring the diagnosis. However, this patient has
opsy in this patient did not show evidence of this all three of the crucial features, which confirm
diagnosis.
this diagnosis clinically.
The clinician might wonder what points to this
Multiple Sclerosis
diagnosis without confirmatory tests. The features
The pattern of white patches seen on MRI could that should be emphasized as strongly suggestive
be that of multiple sclerosis, but involvement of of Susacs syndrome are the age of the patient,
the auditory system with hearing loss is rare in the waxing and waning changes in mental status,
multiple sclerosis. In addition, the vasculitis of the blotchy visual changes suggesting a dysfuncmultiple sclerosis is peripheral in the retina, and tion of the retinal arterioles, and the hearing loss.
n engl j med 365;6
nejm.org
august 11, 2011
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2011. For personal use only. No other uses without permission.
Copyright 2011 Massachusetts Medical Society. All rights reserved.
553
The
n e w e ng l a n d j o u r na l
This is a disease of adults and is not seen in children or very elderly patients. Its expression in the
brain is well demonstrated in this patient. Changes
in mental status dominate, and the mental status
fluctuates. Often, the first abnormality noticed by
persons who know the patient is the behavioral
change.
In the eye, the vasculopathy is well expressed.
It was helpful for diagnostic purposes that the
retinal arteries affected were those of the posterior pole, which meant that the patient was symptomatic and that the vessels could be carefully
examined. It appears his mental status did not
allow detailed visual-field testing, which would
probably have revealed scotomas in a pattern defined by the blood vessels. The changes in the
retinal arterioles may be subtle and escape detection with routine funduscopy. Fluorescein angiography may be necessary to expose them. In more
dramatic expression of the vascular changes of
the retina, plaques that have the appearance of a
string of pearls along the vessels may be seen.
The hearing loss is sensorineural. I believe the
cochlea is affected by the vascular insufficiency.
The changes seen on MRI predominate in the
white matter but also occur in the gray matter. A
characteristic feature is said to be the presence of
a row of holes in the center of the corpus callosum,
probably reflective of the distribution of blood vessels to this structure. The reported changes in the
cerebrospinal fluid reflect meningeal expression,
and the findings on biopsy of the patients brain
are typical of Susacs syndrome in that the vessel
walls are thickened but show little inflammation.
The syndrome is thus considered to be a vasculopathy rather than a vasculitis.
The disease tends to be self-limited by time. The
severity and expression fluctuate, as they did in this
patient, over the course of weeks and months before becoming inactive. The encephalopathic phase
of the illness lasts as long as 2 years, and headache
is common. Sadly, in many cases, permanent damage to mental status, vision, and hearing may
limit the patients return to normal functioning.
The usual therapeutic approach involves the
use of antiinflammatory medications of various
types. The rarity of this condition combined with
its fluctuating course make assessment of the effectiveness of any therapy problematic.
Dr. Eric S. Rosenberg (Pathology): Dr. Cho, could
you tell us what you were thinking when you saw
this patient?
554
of
m e dic i n e
Dr. Tracey A. Cho (Neurology): The initial workup was begun by Dr. Daniel Costello, who has
returned to Ireland. I assumed the patients care.
Dr. Brandon Westover maintained continuity of
care. My initial impression, formed on the basis
of the preceding viral illness, the prominent encephalopathy, and the headache, was one of primary central nervous system vasculitis, particularly
because of the initial response to the administration of high-dose intravenous glucocorticoids.
It was only later, with the development of visual
and auditory symptoms, that we began to expand
our differential diagnosis. Dr. Westover was one
of the first to point out the possibility of Susacs
syndrome.
Cl inic a l Di agnosis
Susacs syndrome.
Dr . D on C . Bienfa ngs Di agnosis
Susacs syndrome.
Pathol o gic a l Discussion
Dr. George N. Papaliodis: The first diagnostic test was
fluorescein angiography, which showed occlusion
of the superior branch of the retinal artery in the
right eye along with regions of retinal vascular
staining and leakage in both eyes, all of which
were consistent with retinal vasculitis. Ten days
after the initial examination, when the patient
reported worsening vision, funduscopic examination (Fig. 2A and 2B) and fluorescein angiography
revealed multiple branch retinal arterial occlusions in both eyes, with regions of edematous
retina (Fig. 2C and 2D).
Dr. Michael J. McKenna: When I first saw this
patient, although he reported bilateral hearing
loss, his neurootologic examination was normal,
with the exception of diminished acuity of conversational speech on the left side. The audiogram (Fig. 3A) showed a low-frequency sensorineural hearing loss on the left side; the right
side was essentially normal. This pattern of lowfrequency sensorineural hearing loss on the left is
not unusual for patients with Mnires disease;
they can present with fluctuating hearing loss in
the low frequencies. However, in Mnires disease, which is a peripheral otologic problem,
word recognition rarely drops below 50% at ini-
n engl j med 365;6 nejm.org august 11, 2011
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2011. For personal use only. No other uses without permission.
Copyright 2011 Massachusetts Medical Society. All rights reserved.
case records of the massachusetts gener al hospital
Figure 2. Funduscopic Examination and Fluorescein Angiography.
Multiple bilateral branch retinal arterial occlusions, with regions of edematous retina, can be seen on funduscopic
examination (Panels A and B, arrows) 10 days after the initial examination, when the patient reported worsening vision in both eyes. Fluorescein angiograms show multiple occlusions in the branches of the retinal arteries bilaterally
(Panels C and D, arrows) and impressive vascular staining and leakage involving most of the major arterial arcades
(arrowheads), features that are consistent with worsening retinal vasculitis. After treatment with methylprednisolone
and cyclophosphamide, the funduscopic examination (Panel E) and fluorescein angiogram (Panel F) show resolution of the retinal edema and occlusions, with normal flow.
n engl j med 365;6
nejm.org
august 11, 2011
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2011. For personal use only. No other uses without permission.
Copyright 2011 Massachusetts Medical Society. All rights reserved.
555
The
Air conduction,
right ear
Bone conduction,
unmasked, right ear
Air conduction,
left ear
Bone conduction,
masked, left ear
n e w e ng l a n d j o u r na l
No response, left ear
10
0
10
Hearing Level (dB)
20
30
40
50
60
70
90
100
Word recognition
Right: 94%
Left: 0%
110
120
62.5 125
250
500
1000
m e dic i n e
Figure 3. Audiograms.
An audiogram performed during the patients second
admission to this hospital (Panel A) shows normal
hearing in the right ear (red symbols), with an isolated moderate loss at 8000 Hz only. There is normal
word recognition in the right ear. The left ear (blue
symbols) has a moderate, predominantly sensorineural hearing loss at low frequencies. The up-sloping
pattern indicates that the hearing loss is mild at high
frequencies. However, the word-recognition score
for the left ear is 0%, which means that a hearing aid
would not have been helpful at that time. A repeat
audiogram 2 months later (Panel B) again shows
essentially normal hearing in the right ear. The left ear
shows stable sensorineural hearing loss at low frequencies but shows better (lower) thresholds of hearing at frequencies of 2000 Hz and above. The wordrecognition score for the left ear has improved notably,
to 42%, indicating a significant improvement in the
patients ability to understand speech. Air conduction
refers to stimuli delivered through headphones. Bone
conduction refers to stimuli delivered with the use of a
bone oscillator applied to the skull; during the testing
of one ear, the contralateral ear may receive masking
noise to ensure that the responses are actually from
the ear being tested.
80
of
2000 4000 8000 16,000
Frequency (Hz)
B
10
0
10
Hearing Level (dB)
20
30
40
50
60
70
80
90
100
Word recognition
Right: 92%
Left: 42%
110
120
62.5 125
250
500
1000
2000 4000 8000 16,000
Frequency (Hz)
tial presentation. In this case, the word-recognition score on the left side was 0%, a feature that
is not consistent with Mnires disease.
Dr. Anat Stemmer-Rachamimov: The brain-biopsy
specimen obtained during the patients first admission contained fragments of cortex and white
matter. The leptomeninges were unremarkable.
The medium-sized leptomeningeal arteries showed
no evidence of granulomatous inflammation, and
Verhoeffs elastic staining showed intact elastic
556
n engl j med 365;6
lamina. Some of the small vessels in the cortex
and white matter showed a spectrum of changes:
swollen endothelial cells (Fig. 4A), scant mononuclear-cell perivascular inflammation (Fig. 4B),
and intraluminal hyaline thrombi (Fig. 4C). These
changes are suggestive of a microangiopathy. No
infarcts were seen in this small specimen. There
was no evidence of granulomatous angiitis, demyelination, lymphoma, or a specific infectious
process. Although in the context of the clinical
and imaging findings these features were not specific, they are consistent with Susacs syndrome,
or retinocochleocerebral vasculopathy. The first
case of Susacs syndrome was reported in 1979,19
and more than 100 cases have now been reported
in the literature.21 There is no specific diagnostic
test for this syndrome; rather, the diagnosis is
based on the combination of clinical features and
the absence of another specific diagnosis on pathological examination.
The greatest amount of information on the
underlying process in Susacs syndrome comes
from pathological analysis of the brain, the only
site from which biopsy material is available in
this case. The most common finding in brain
biopsies is the presence of microinfarcts. These
can be acute or subacute and involve both the
cortex and white matter. Also reported are chang-
nejm.org
august 11, 2011
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2011. For personal use only. No other uses without permission.
Copyright 2011 Massachusetts Medical Society. All rights reserved.
case records of the massachusetts gener al hospital
es in the microvasculature similar to those seen
in this patient, including scant perivascular inflammation, swelling of endothelial cells, and the
presence of intraluminal hyaline thrombi. Less
frequently, scarring of arteriolar walls may be
present.19,22-26
In the retina, information is derived indirectly,
from ophthalmologic examination and fluorescein angiography. As in the brain, and as seen in
this patient, there are infarcts and changes in the
microvasculature, including narrowing and occlusion of arterioles and leaking of dye. It is likely
that the underlying pathologic process in the
retina is similar to that observed directly in the
brain.
Information about the changes leading to hearing loss is the least accessible, but combined findings from clinical observation and imaging studies localize the process to the cochlea. Because of
the more pronounced loss of the ability to hear
sounds at low frequencies, it has been suggested
that the underlying process is microinfarction of
the cochlear apex,24 which is supplied by small end
arteries.
What is the cause of the microinfarcts? Proposed explanations include a hypercoagulable state,
vasospasm, and vasculitis, none of which are supported by laboratory results or findings on brain
biopsies.26 The unique distribution of arteriolar
disease affecting the brain, the retina, and the
cochlea suggests selective vulnerability of these
three structures. The brain, retina, and cochlea
all have a bloodtissue barrier, and the endothelium in these sites shares a common embryologic
origin and unique structural and antigenic characteristics.24,27 It has therefore been proposed that
Susacs syndrome is an autoimmune disease in
which the endothelium is the primary target, and
damage to the endothelium triggers arteriolar occlusion and microinfarcts.24,27 However, the pathogenesis remains unknown.
Dr. Rosenberg: Dr. Cho, would you tell us how
you managed the care of this patient and how he
is doing?
Dr. Cho: Despite the administration of pulsed
intravenous glucocorticoids and first 80 and then
120 mg of prednisone daily, he continued to have
headaches and mild encephalopathy, followed by
the development of visual changes and hearing
loss. After the diagnostic testing, we began treatment with a 4-day course of cyclophosphamide,
to which he had a good response, and he was
n engl j med 365;6
Figure 4. Brain-Biopsy Specimen (Hematoxylin
and Eosin).
Sections of cortex and white matter show a small vessel
with prominent activated endothelial cells (Panel A), a
small vessel with scant perivascular chronic inflammation (Panel B), and a small vessel with intraluminal hyaline thrombus (Panel C, arrow). These changes are
suggestive of a microangiopathy.
maintained on monthly pulsed cyclophosphamide and daily prednisone, starting at 120 mg and
then tapering to 80 mg. A cushingoid appearance
developed, as did an early, or mild, cataract; the
patient also gained weight. He was followed by a
multidisciplinary team, including physicians from
neurotology and neuroophthalmology. Approxi-
nejm.org
august 11, 2011
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2011. For personal use only. No other uses without permission.
Copyright 2011 Massachusetts Medical Society. All rights reserved.
557
The
n e w e ng l a n d j o u r na l
mately 1 year after the onset of symptoms, prednisone was tapered and discontinued, and monthly intravenous methylprednisolone was added to
the monthly cyclophosphamide pulses. The patient
is now working full time and is neurologically
normal, approximately 2 years after the onset of
symptoms.
Dr. Rosenberg: Drs. Papaliodis and McKenna,
can you tell us what happened in terms of the
eye findings and audiogram?
Dr. Papaliodis: After initiation of therapy with
intravenous cyclophosphamide, the findings in the
fundus stabilized, with no new regions of involvement. Fluorescein angiography showed the
previously noted branch retinal arterial occlusions
but no new regions of involvement. Later frames
of the fluorescein angiogram revealed decreased
vascular staining and leakage in both eyes (although one focal area of active disease remained
in the left eye). During the next 18 months there
was fluctuating evidence of retinal inflammation
and vasculopathy, but at the most recent examination (Fig. 2E and 2F) the retinal vasculature was
normal in appearance, and no evidence of retinal
vasculopathy was detected on fluorescein angiography. The patient has a normal fundus and 20/20
visual acuity. I have recommended discontinuation
of cyclophosphamide and glucocorticoids and initiation of mycophenolate mofetil.
Dr. McKenna: A second audiogram obtained
after the initiation of treatment (Fig. 3B) showed
that the right ear remained normal. There had
been slight improvement in hearing at midfrequencies in the left ear, but with persistent lowfrequency sensorineural hearing loss; word recognition had improved from 0 to 42%. Examination
1 year later showed essentially no change.
A Physician: Would someone comment on the
of
m e dic i n e
natural history of this disease? It is my understanding that this patient had an exceptionally
good response to treatment or was this the
expected outcome?
Dr. Cho: Dr. Susac, in a review of his experience, described three different courses of disease28: monocyclic, characterized by fluctuations
but eventual resolution over the course of 1 to
2 years, without recurrence; polycyclic, characterized by remissions between episodes for more than
2 years; and chronic smoldering, in which there is
active disease without remission for more than
2 years. Early encephalopathy, as seen in this patient, tends to occur more frequently in the monophasic form of the disease than in the other forms,
and our hope is that the course of disease for this
patient will fit that category. Our goal in management of care is to prevent permanent organ
damage, since recovery after neurologic injury
is often incomplete. Although the treatment of
Susacs syndrome has not been studied in controlled trials, most patients have a good response
to treatment with glucocorticoids, with the addition of intravenous immune globulin or cyclophosphamide for cases in which the disease is
refractory to glucocorticoids. We decided to use
cyclophosphamide because we wanted to preserve
brain function, vision, and hearing to the extent
possible. The patients response to cyclophosphamide was in keeping with glucocorticoid-refractory cases described by Susac and others.
A nat omic a l Di agnosis
Susacs syndrome (retinocochleocerebral vasculopathy).
Disclosure forms provided by the authors are available with
the full text of this article at NEJM.org.
References
1. Cogan DG. Syndrome of non-syphilitic
interstitial keratitis and vestibulo-auditory
symptoms. Arch Ophthalmol 1945;33:144-9.
2. Haynes BF, Kaiser-Kupfer MI, Mason
P, Fauci AS. Cogan syndrome: studies in
thirteen patients, long-term follow-up, and
a review of the literature. Medicine (Baltimore) 1980;59:426-41.
3. Haynes BF, Pikus A, Kaiser-Kupfer M,
Fauci AS. Successful treatment of sudden
hearing loss in Cogans syndrome with
corticosteroids. Arthritis Rheum 1981;24:
501-3.
4. Gass JD. Acute posterior multifocal
placoid pigment epitheliopathy. Arch Ophthalmol 1968;80:177-85.
558
5. Savino PJ, Weinberg RJ, Yassin JG,
Pilkerton AR. Diverse manifestations of
acute posterior multifocal placoid pigment
epitheliopathy. Am J Ophthalmol 1974;77:
659-62.
6. Renie WA, Murphy RP, Anderson KC,
et al. The evaluation of patients with Eales
disease. Retina 1983;3:243-8.
7. Murphy CR. Glycerol treatment increases intramembranous particle density
in uterine epithelial cells. Z Mikrosk Anat
Forsch 1986;100:121-4.
8. Dobbins WOI. Whipples disease.
Springfield, IL: Charles C Thomas, 1987.
9. Fleming JL, Wiesner RH, Shorter RG.
Whipples disease: clinical, biochemical,
and histopathologic features and assessment of treatment in 29 patients. Mayo
Clin Proc 1988;63:539-51.
10. Knox DI, Bayless TM, Yardley JH,
Charache P. Whipples disease presenting
with ocular inflammation and minimal
intestinal symptoms. Johns Hopkins Med J
1968;123:175-82.
11. Reik L Jr, Burgdorfer W, Donaldson JO.
Neurologic abnormalities in Lyme disease
without erythema chronicum migrans.
Am J Med 1986;81:73-8.
12. Reik L, Steere AC, Bartenhagen NH,
Shope RE, Malawista SE. Neurologic abnormalities of Lyme disease. Medicine
(Baltimore) 1979;58:281-94.
n engl j med 365;6 nejm.org august 11, 2011
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2011. For personal use only. No other uses without permission.
Copyright 2011 Massachusetts Medical Society. All rights reserved.
case records of the massachusetts gener al hospital
13. Logigian EL, Kaplan RF, Steere AC.
Chronic neurologic manifestations of Lyme
disease. N Engl J Med 1990;323:1438-44.
14. Cury D, Breakey AS, Payne BF. Allergic
granulomatous angiitis associated with
uveoscleritis and papilledema. AMA Arch
Ophthalmol 1956;55:261-6.
15. DeRemee RA, Weiland LH, McDonald
TJ. Respiratory vasculitis. Mayo Clin Proc
1980;55:492-8.
16. Churg J, Strauss L. Allergic granulomatosis, allergic angiitis, and periarteritis
nodosa. Am J Pathol 1951;27:277-301.
17. Do TH, Fisch C, Evoy F. Susac syndrome: report of four cases and review of
the literature. AJNR Am J Neuroradiol
2004;25:382-8.
18. Galetta SL. Vasculitis In: Miller NR,
Newman NJ, eds. Walsh & Hoyts clinical
neuro-ophthalmology. 5th ed. Baltimore:
Williams & Wilkins, 1998:3725-886.
19. Susac JO, Hardman JM, Selhorst JB.
Microangiopathy of the brain and retina.
Neurology 1979;29:313-6.
20. Susac JO, Murtagh FR, Egan RA, et al.
MRI findings in Susacs syndrome. Neurology 2003;61:1783-7.
21. Susac JO, Egan RA, Rennebohm RM,
Lubow M. Susacs syndrome: 1975-2005
microangiopathy/autoimmune endotheliopathy. J Neurol Sci 2007;257:270-2.
22. Bogousslavsky J, Gaio JM, Caplan LR,
et al. Encephalopathy, deafness and blindness in young women: a distinct retino
cochleocerebral arteriolopathy? J Neurol
Neurosurg Psychiatry 1989;52:43-6.
23. Heiskala H, Somer H, Kovanen J, Poutiainen E, Karli H, Haltia M. Microangiopathy with encephalopathy, hearing loss
and retinal arteriolar occlusions: two new
cases. J Neurol Sci 1988;86:239-50.
24. Monteiro ML, Swanson RA, Coppeto JR,
Cuneo RA, DeArmond SJ, Prusiner SB. A
microangiopathic syndrome of encephalopathy, hearing loss, and retinal arteriolar occlusions. Neurology 1985;35:111321.
25. OHalloran HS, Pearson PA, Lee WB,
Susac JO, Berger JR. Microangiopathy of
the brain, retina, and cochlea (Susac syndrome): a report of five cases and a review
of the literature. Ophthalmology 1998;105:
1038-44.
26. Petty GW, Engel AG, Younge BR, et al.
Retinocochleocerebral vasculopathy. Medi
cine (Baltimore) 1998;77:12-40.
27. Papo T, Biousse V, Lehoang P, et al.
Susac syndrome. Medicine (Baltimore)
1998;77:3-11.
28. Rennebohm RM, Susac JO. Treatment
of Susacs syndrome. J Neurol Sci 2007;
257:215-20.
Copyright 2011 Massachusetts Medical Society.
Lantern Slides Updated: Complete PowerPoint Slide Sets from the Clinicopathological Conferences
Any reader of the Journal who uses the Case Records of the Massachusetts General Hospital as a teaching exercise or reference
material is now eligible to receive a complete set of PowerPoint slides, including digital images, with identifying legends,
shown at the live Clinicopathological Conference (CPC) that is the basis of the Case Record. This slide set contains all of the
images from the CPC, not only those published in the Journal. Radiographic, neurologic, and cardiac studies, gross specimens,
and photomicrographs, as well as unpublished text slides, tables, and diagrams, are included. Every year 40 sets are produced,
averaging 50-60 slides per set. Each set is supplied on a compact disc and is mailed to coincide with the publication of the
Case Record.
The cost of an annual subscription is $600, or individual sets may be purchased for $50 each. Application forms for the current
subscription year, which began in January, may be obtained from the Lantern Slides Service, Department of Pathology,
Massachusetts General Hospital, Boston, MA 02114 (telephone 617-726-2974) or e-mail Pathphotoslides@partners.org.
n engl j med 365;6 nejm.org august 11, 2011
The New England Journal of Medicine
Downloaded from nejm.org on September 13, 2011. For personal use only. No other uses without permission.
Copyright 2011 Massachusetts Medical Society. All rights reserved.
559
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5825)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (852)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (903)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (541)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (349)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (823)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (403)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- NCLEX - Fluids and ElectrolytesDocument4 pagesNCLEX - Fluids and ElectrolytesissaiahnicolleNo ratings yet
- 15-10-2019, Mr. Jamal, 50 Yo, V.Laceratum Cruris Dextra + Skin Loss + Fraktur Os Fibula, Dr. Moh. Rizal Alizi, M.Kes, Sp. OT-1Document15 pages15-10-2019, Mr. Jamal, 50 Yo, V.Laceratum Cruris Dextra + Skin Loss + Fraktur Os Fibula, Dr. Moh. Rizal Alizi, M.Kes, Sp. OT-1anon_893244902No ratings yet
- Babesioza - Teza Doctorat PDFDocument90 pagesBabesioza - Teza Doctorat PDFAndras AndreescuNo ratings yet
- 6 Birth DefectsDocument40 pages6 Birth DefectsjulieNo ratings yet
- Brochure - ILLUCO Dermatoscope IDS-1100Document2 pagesBrochure - ILLUCO Dermatoscope IDS-1100Ibnu MajahNo ratings yet
- Resumen Article IcDocument4 pagesResumen Article Icapi-689165620No ratings yet
- Hormonal ImbalanceDocument3 pagesHormonal ImbalanceShan Armaine CabelaNo ratings yet
- Dr. Wahyuni Indawati, Spa (K)Document43 pagesDr. Wahyuni Indawati, Spa (K)Rara AnisaNo ratings yet
- Manajemen StrokeDocument253 pagesManajemen StrokeHappy Pramanda100% (2)
- Transanal Protocol PDFDocument4 pagesTransanal Protocol PDFDesiree FlorendoNo ratings yet
- What Is Pneumonia?: Patient EducationDocument2 pagesWhat Is Pneumonia?: Patient EducationDian Putri NingsihNo ratings yet
- The Effects of Lifestyle To Respiratory and Circulatory SystemsDocument11 pagesThe Effects of Lifestyle To Respiratory and Circulatory SystemsSharalyn Sia100% (1)
- MFG E8介导的骨免疫在牙周炎中的作用研究进展 向群Document5 pagesMFG E8介导的骨免疫在牙周炎中的作用研究进展 向群颜加龙No ratings yet
- Basal Cell Carcinoma, Infiltrative TypeDocument8 pagesBasal Cell Carcinoma, Infiltrative TypeDeba P SarmaNo ratings yet
- OSCE StationsDocument3 pagesOSCE StationsKristoff FiguerasNo ratings yet
- Reference/normal Values Result Interpretation What Have Caused The Abnormality/ Purpose/NIDocument5 pagesReference/normal Values Result Interpretation What Have Caused The Abnormality/ Purpose/NIKristian Karl Bautista Kiw-isNo ratings yet
- Diagnostic Exam-Health Specialist EditDocument9 pagesDiagnostic Exam-Health Specialist EditAyuy Welliss MedusaNo ratings yet
- Dugs CVADocument10 pagesDugs CVAMarie AntoinetteNo ratings yet
- Pathfit 1 M3Document20 pagesPathfit 1 M3rainiel gibasNo ratings yet
- GCSE Week 12 Pathogens and DiseaseDocument27 pagesGCSE Week 12 Pathogens and DiseaseFrankie BarnesNo ratings yet
- Health, Safety, Environmental Management Manual: Loshini ProjectsDocument6 pagesHealth, Safety, Environmental Management Manual: Loshini ProjectsThandabantu MagengeleleNo ratings yet
- QCGH FormDocument4 pagesQCGH FormKim Delaney MadridNo ratings yet
- Cardiovascular System Drugs - Active Stack® Pharmacology Flash Cards - Study Materials - My ATIDocument1 pageCardiovascular System Drugs - Active Stack® Pharmacology Flash Cards - Study Materials - My ATIAntonette Joy SolinapNo ratings yet
- ChickenpoxDocument2 pagesChickenpoxNorhana LangiNo ratings yet
- WHO 2022 Bladder PDFDocument92 pagesWHO 2022 Bladder PDFOlteanu Dragos-NicolaeNo ratings yet
- HypochondriasisDocument3 pagesHypochondriasisLaura Pauline KosasihNo ratings yet
- Disease Deep Dive Kathryn CrimDocument7 pagesDisease Deep Dive Kathryn Crimapi-579320483No ratings yet
- Retroperitoneal Abscess Caused by Dropped RenalDocument4 pagesRetroperitoneal Abscess Caused by Dropped RenalNatalindah Jokiem Woecandra T. D.No ratings yet
- John Case StudyDocument6 pagesJohn Case Studyapi-283887910No ratings yet
- Radiology Quiz Medical Students Workbook: Author: DR Aussami Abbas SPR RadiologyDocument11 pagesRadiology Quiz Medical Students Workbook: Author: DR Aussami Abbas SPR RadiologyMădălina Ciobotariu100% (1)