Professional Documents
Culture Documents
Alcoholic Ketoacidosis
Alcoholic Ketoacidosis
Uploaded by
Faishal HanifCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Alcoholic Ketoacidosis
Alcoholic Ketoacidosis
Uploaded by
Faishal HanifCopyright:
Available Formats
Oxford Medical Case Reports, 2016; 3 , 3133
doi: 10.1093/omcr/omw006
Case Report
CASE REPORT
Alcoholic ketoacidosis: a case report and review of the
literature
Nurulamin M. Noor1,, Krishna Basavaraju2,, and Dan Sharpstone2,
1
Department of Medicine, University of Cambridge, Cambridge, UK and 2Department of Gastroenterology,
West Suffolk Hospital, Bury St Edmunds, UK
*Corresponding address. Department of Medicine, University of Cambridge, Addenbrookes Hospital, Cambridge CB2 0QQ, UK. Tel: +441223-762322;
Fax: +441223-762323; E-mail: noorn@doctors.org.uk
Abstract
Alcoholic ketoacidosis (AKA) is a cause of severe metabolic acidosis usually occurring in malnourished patients with a history of
recent alcoholic binge, often on a background of alcohol dependency. AKA can be fatal due to associated electrolyte
abnormalities and subsequent development of cardiac arrhythmias. This is a diagnosis that is often delayed or missed, in
patients who present with a severe lactic and ketoacidosis. Here we report the case of a 64-year-old female who presented with
generalized abdominal pain, nausea and shortness of breath. Blood gas analysis showed signicant acidaemia with a pH of 7.10,
bicarbonate of 2.9 mmol/l, and lactate of 11.7 mmol/l. Serum ketones were raised at 5.5 mmol/l. The diagnosis of AKA was
suspected, and subsequent aggressive uid resuscitation, management and monitoring were instituted. Given the early
recognition of AKA and appropriate multidisciplinary team management, our patient had a good outcome and was discharged
home without any complication.
INTRODUCTION
Alcoholic ketoacidosis (AKA) is a condition that presents with a
signicant metabolic acidosis in patients with a history of alcohol
excess. The diagnosis is often delayed or missed, and this can
have potentially fatal consequences. There are a variety of nonspecic clinical manifestations that contribute to these diagnostic difculties. In particular, cases of AKA can be misdiagnosed as
diabetic ketoacidosis (DKA). Subsequent mismanagement can
lead to increasing morbidity and mortality for patients. AKA typically presents with a severe metabolic acidosis with a raised
anion gap and electrolyte abnormalities, which are treatable if recognized early and appropriate management instituted. Given
the increasing epidemic of alcohol-related healthcare admissions, this is an important condition to recognize and we aim
to offer guidance on how to approach similar cases for the practising clinician.
CASE REPORT
We present a 64-year-old female who presented with generalized
abdominal pain, nausea, vomiting and shortness of breath. Arterial blood gas analysis showed signicant acidaemia with a
pH of 7.10, bicarbonate of 2.9 mmol/l and lactate of 11.7 mmol/l.
Serum ketones were raised at 5.5 mmol/l. Capillary blood glucose
was noted to 5.8 mmol/l. The anion gap was calculated and was
elevated at 25 mmol/l.
The diagnosis of DKA was queried after initial triage. However, following senior medical review, given a recent history of
Contributors: N.N., K.B. and D.S. were all involved in the care of the patient and for drafting and critical revision of the manuscript.
Received: December 29, 2015. Revised: January 19, 2016. Accepted: January 21, 2016
The Author 2016. Published by Oxford University Press.
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/
licenses/by-nc/4.0/), which permits non-commercial re-use, distribution, and reproduction in any medium, provided the original work is properly cited.
For commercial re-use, please contact journals.permissions@oup.com
31
32
| N.M. Noor et al.
drinking alcohol to excess, the diagnosis of AKA was felt more
likely. Whilst a decreased conscious level may have been expected, our patient was lucid enough to report drinking one to
two bottles of wine per day for the past 30 years, with a recent
binge the day prior to admission.
Subsequent uid resuscitation and monitoring were instituted. Further biochemical investigation after treatment showed
a rapid decline in the level of ketones and normalization of pH.
Our patient had a multidisciplinary team (MDT) looking after
her care, whilst she was an inpatient, including acute medical
and gastroenterology doctors and nurses, dietitians, alcohol specialist nurse, physiotherapists and occupational therapists.
Following resuscitation, our patient had plasma electrolyte
levels corrected, nutritional supplementation provided and completed an alcohol detoxication regimen. Given the early recognition of AKA and concurrent management, our patient had a good
outcome. She was discharged home and has been well on followup appointments.
DISCUSSION
AKA can be an unrecognized cause of patients presenting with a
severe metabolic acidosis, including the presence of ketones. It
should be suspected in any patient who has a history of chronic
alcohol dependency, malnutrition or recent episode of binge
drinking [1].
Patients typically present with non-specic features including
nausea, vomiting and generalized abdominal pain. Vomiting
and/or diarrhoea is common and can lead to hypovolaemia and
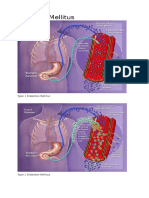
Figure 1: Aetiology of acidosis in AKA.
potassium depletion. Signs of shock including tachycardia and
hypotension can be complicated by overlap of alcohol withdrawal [2]. Electrolyte abnormalities are common to this condition and
can precipitate fatal cardiac arrhythmias [3, 4].
The severe metabolic acidosis that occurs in AKA is multifactorial (Fig. 1). First, there is the presence of ketone bodies, which
are inherently acidic [5, 6]. Ketones are produced by the body for
energy, in times of low glucose availability. This is more likely to
occur in patients with alcohol excess due to poor oral intake and
nutrition. As ethanol at high concentrations inhibits lipolysis,
signicant production of ketone bodies ( particularly beta-hydroxybutyrate) occurs once ethanol levels fall, hence why presentation typically occurs after and not during an alcoholic binge [6].
Second, due to dehydration associated with alcohol excess,
there is peripheral tissue hypoperfusion, with subsequent
build-up of lactic acid [5]. Third, alcohol is metabolized by the alcohol dehydrogenase and subsequently acetaldehyde dehydrogenase to give the product acetate, which is itself acidic [5, 6].
Excess alcohol intake, as demonstrated by recent binge by our patient, therefore can lead to a signicant and severe metabolic
acidosis.
The main differential diagnoses for ketosis in our patient included AKA, starvation/fasting ketosis and DKA. In starvation ketosis, a mild ketosis is noted to develop in most after 1224 h of
fasting. However, the body copes with this physiologically by peripherally utilizing ketone bodies, stimulating increased insulin
release (despite the presence of low glucose levels), and direct inhibition of further lipolysis by the ketone bodies themselves [7].
Therefore, only a mild acidosis is observed in starvation ketosis.
The key differential diagnosis to consider, and exclude, in
these patients is DKA. Although DKA can also present with a severe metabolic acidosis, with a raised anion gap and the presence
of ketones, the history and examination are quite distinct from
that of someone presenting with AKA (Table 1).
Although AKA can cause a modest elevation in serum glucose, signicant hyperglycaemia in patients with metabolic acidosis, the presence of ketones and a suggestive history would
make DKA the more likely diagnosis. The clinical importance in
recognizing AKA from DKA is demonstrated by cases of patients
who were treated as DKA and developed severe hypoglycaemia
as a result of inappropriate insulin administration [8].
The presence of a high anion gap, although not specic, is
suggestive of AKA in a patient with an appropriate clinical history
[9]. Additional measurements that may help determine the diagnosis of AKA include beta-hydroxybutyrate levels (high in AKA,
low in DKA) and serum alcohol concentration (typically low or
undetectable) [8]. The key principle of emergency management
is adequate uid resuscitation [10]. Increasing volume status
and providing increased perfusion to tissues help reduce lactic
Table 1: Characteristics of AKA and DKA
Past medical history
Clinical presentation
Alertness
Examination
Blood gas analysis
Blood glucose
Ketones
Beta-hydroxybutyrate
Electrolyte abnormalities
AKA
DKA
Alcohol excess
Non-specic features
Alert and lucid usually
Dehydrated and clinically more well than expected
Metabolic acidosis with raised anion gap
Usually low or normal, can be modestly raised
Present on both urinary and blood testing
Signicantly raised
Often low potassium, phosphate and magnesium
Might be known diabetic or new presentation
Non-specic features
Variable but often decreased alertness
Dehydrated and clinically very unwell
Metabolic acidosis with raised anion gap
Usually signicantly raised
Present on both urinary and blood testing
Mildly raised
Total body potassium low (serum potassium is
either low or normal)
Alcoholic ketoacidosis
acid, ketoacids and acetic acid, which would all have been contributing to the severe acidosis.
Appropriate MDT management is key to promoting rapid recovery from AKA, but also in helping prevent complications associated with alcohol excess, in particular treating malnutrition
and electrolyte deciencies [2, 5]. Electrolyte correction should
be instituted as a matter of urgency, as the main of cause of
mortality is attributed to cardiac arrhythmias from electrolyte
deciencies [10].
This case demonstrates the importance of considering AKA in
the differential diagnosis of a patient presenting with non-specic
symptoms, signicant metabolic acidosis and a history of alcohol
excess. It is essential to differentiate AKA from DKA to ensure
that inappropriate insulin administration does not occur. The
key tenants to management of AKA include uid resuscitation
and electrolyte correction.
CONFLICT OF INTEREST
None declared.
FUNDING
None.
ETHICAL APPROVAL
Not applicable.
CONSENT
Written consent was obtained from the patient.
| 33
GUARANTOR
Nurulamin M. Noor.
REFERENCES
1. Wrenn KD, Slovis CM, Minion GE, Rutkowski R. The syndrome
of alcoholic ketoacidosis. Am J Med 1991;91:119.
2. Allison MG, McCurdy MT. Alcoholic metabolic emergencies.
Emerg Med Clin North Am 2014;32:293301.
3. Palmiere C, Augsburger M. The post-mortem diagnosis of
alcoholic ketoacidosis. Alcohol Alcohol 2014;49:271281.
4. Yanagawa Y, Sakamato T, Okada Y. Six cases of sudden cardiac arrest in alcoholic ketoacidosis. Intern Med 2008;47:
113117.
5. Palmer JP. Alcoholic ketoacidosis: clinical and laboratory
presentation, pathophysiology and treatment. Clin Endocrinol
Metab 1983;12:381.
6. Halperin ML, Hammeke M, Josse RG, Jungas RL. Metabolic
acidosis in the alcoholic: a pathophysiologic approach.
Metabolism 1983;32:308.
7. Balasse EO, Fry F. Ketone body production and disposal: effects of fasting, diabetes, and exercise. Diabetes Metab Rev
1989;5:247.
8. Matsuzaki T, Shiraishi W, Iwanaga Y, Yamamoto A. Case of
alcoholic ketoacidosis accompanied by severe hypoglycemia.
J UOEH 2015;37:4347.
9. Schelling JR, Howard RL, Winter SD, Linas SL. Increased osmolal gap in alcoholic ketoacidosis and lactic acidosis. Ann
Intern Med 1990;113:580.
10. McGuire LC, Cruickshank AM, Munro PT. Alcoholic ketoacidosis. Emerg Med J 2006;23:417420.
You might also like
- Pat MathsDocument4 pagesPat MathsTan Beng33% (3)
- Epsilon ConvergenceDocument30 pagesEpsilon ConvergenceSuhas Vilas DolseNo ratings yet
- Critical Care Management For Patient With Diabetic Ketoacidosis (Dka) NCM 118 LectureDocument12 pagesCritical Care Management For Patient With Diabetic Ketoacidosis (Dka) NCM 118 LectureBULONG Darlyn GraceNo ratings yet
- Diabetic KetoacidosisDocument85 pagesDiabetic Ketoacidosismohamed mowafeyNo ratings yet
- 128 Diabetic KetoacidosisDocument9 pages128 Diabetic KetoacidosisDite Bayu NugrohoNo ratings yet
- Laboratory FindingsDocument22 pagesLaboratory FindingseffiniasiregarNo ratings yet
- Acid-Base Imbalance: By: Kristine Louise E. JavierDocument68 pagesAcid-Base Imbalance: By: Kristine Louise E. JavierKristine Louise JavierNo ratings yet
- Aka ReviewDocument4 pagesAka ReviewminhaboomboxNo ratings yet
- Diabetic Ketoacidosis PDFDocument11 pagesDiabetic Ketoacidosis PDFCsr ArsNo ratings yet
- Acute Diabetes ComplicationsDocument7 pagesAcute Diabetes ComplicationsHala Salah IbrahimNo ratings yet
- Description of Disease/condition: Metabolic Alkalosis, Information About Metabolic AlkalosisDocument6 pagesDescription of Disease/condition: Metabolic Alkalosis, Information About Metabolic AlkalosisJusterine Jade To-ong SiglosNo ratings yet
- CS Diabetic KetoacidosisDocument11 pagesCS Diabetic KetoacidosisMarvin Dela Cruz100% (1)
- Diabetic KetoacidosisDocument16 pagesDiabetic Ketoacidosisjoyshe111100% (3)
- Lactation Ketoacidosis in A COVID - 19 Patient A Case ReportDocument3 pagesLactation Ketoacidosis in A COVID - 19 Patient A Case Reporteditorial.boardNo ratings yet
- Ketosis DMDocument33 pagesKetosis DMtiaNo ratings yet
- Tatalaksana Kad 1Document7 pagesTatalaksana Kad 1Nurul Kamilah SadliNo ratings yet
- Diabetic KetoacidosisDocument39 pagesDiabetic KetoacidosisNathasya B.W.No ratings yet
- Overview of The Diagnosis and Management of Diabetic KetoacidosisDocument9 pagesOverview of The Diagnosis and Management of Diabetic KetoacidosisAlberto ValenzuelaNo ratings yet
- DKA ManagementDocument7 pagesDKA ManagementbababrijeshNo ratings yet
- Diabetic KetoacidosisDocument5 pagesDiabetic KetoacidosisJill Catherine Cabana100% (3)
- Diabetic Ketoacidosis 1Document10 pagesDiabetic Ketoacidosis 1Victor Manuel Gonzalez GalindoNo ratings yet
- Diabetic KetoacidosisDocument7 pagesDiabetic KetoacidosisetengNo ratings yet
- Kussmaul Breathing: Breathing Hyperventilation Adolph Kussmaul 19th Century German DoctorDocument23 pagesKussmaul Breathing: Breathing Hyperventilation Adolph Kussmaul 19th Century German DoctorFirstyaprilly WahyuningtyasNo ratings yet
- Acute Metabolic Complications of Diabetes MellitusDocument39 pagesAcute Metabolic Complications of Diabetes MellitusAli Murtaza AbbasNo ratings yet
- Management of Diabetic Ketoacidosis: MW SavageDocument3 pagesManagement of Diabetic Ketoacidosis: MW Savagedramaysingh100% (1)
- Hyperglycemic Crises in Patients With Diabetes Mellitus: Position StatementDocument9 pagesHyperglycemic Crises in Patients With Diabetes Mellitus: Position StatementChristian SalimNo ratings yet
- Diabetes Case StudyDocument2 pagesDiabetes Case StudyRhina FutrellNo ratings yet
- Approach To Metabolic AlkalosisDocument11 pagesApproach To Metabolic AlkalosisJou ÁlvarezNo ratings yet
- Cetoacidosis y Edo Hiperglicemico HiperO 2013Document19 pagesCetoacidosis y Edo Hiperglicemico HiperO 2013RosolinaNo ratings yet
- Diabetic KetoacidosisDocument10 pagesDiabetic Ketoacidosishibecix840No ratings yet
- HyperkalemiaDocument23 pagesHyperkalemiaarungNo ratings yet
- CaseDocument7 pagesCaseDenny EmiliusNo ratings yet
- Diabetic KetoacidosisDocument10 pagesDiabetic KetoacidosisKimberly Zazil Sanchez LopezNo ratings yet
- Acid Base DisordersDocument5 pagesAcid Base DisordersMillenial VoiceNo ratings yet
- Diabetic Ketoacidosis: Abdelaziz Elamin Professor of Pediatric Endocrinology University of Khartoum, SudanDocument33 pagesDiabetic Ketoacidosis: Abdelaziz Elamin Professor of Pediatric Endocrinology University of Khartoum, SudanboyzbanjarboyzNo ratings yet
- Diabetic Ketoacidosis CQBDocument9 pagesDiabetic Ketoacidosis CQBkajanyloganNo ratings yet
- Acute. KetoacidosisdocxDocument12 pagesAcute. KetoacidosisdocxShara SampangNo ratings yet
- Clinical Review: Diabetic Ketoacidosis in AdultsDocument8 pagesClinical Review: Diabetic Ketoacidosis in AdultscitrahmahNo ratings yet
- Diabetic KetoasidosisDocument33 pagesDiabetic KetoasidosisGrace UlyNo ratings yet
- Diabetic Ketoacidosis:: Evidence Based ReviewDocument4 pagesDiabetic Ketoacidosis:: Evidence Based ReviewgracedumaNo ratings yet
- Overview On Diabetic AcidosisDocument11 pagesOverview On Diabetic AcidosisIkraam Abdul LatifNo ratings yet
- 66 Part 1Document10 pages66 Part 1Dinu Tiberiu GeorgeNo ratings yet
- Updates in The Management of Diabetic Ketoacidosis: Kathryn Evans Kreider, DNP, FNP-BCDocument7 pagesUpdates in The Management of Diabetic Ketoacidosis: Kathryn Evans Kreider, DNP, FNP-BCLenin Zavaleta RodriguezNo ratings yet
- Diabetic KetoacidosisDocument12 pagesDiabetic KetoacidosisSarah GatuzNo ratings yet
- IJPRDocument6 pagesIJPRUlvi DitasariNo ratings yet
- Dr. Ali's Uworld Notes For Step 2 CKDocument15 pagesDr. Ali's Uworld Notes For Step 2 CKBoogy WoogyNo ratings yet
- Diabetic KetoacidosisDocument14 pagesDiabetic KetoacidosisYash Ramawat100% (1)
- W02 - Diabetic Emergencies in CCDocument36 pagesW02 - Diabetic Emergencies in CCHelene AlawamiNo ratings yet
- Schillaci 2017Document22 pagesSchillaci 2017Sarranya ParanthamanNo ratings yet
- Hyperglicemic Emergency in AdultsDocument21 pagesHyperglicemic Emergency in AdultsChandraNo ratings yet
- Diagnosis and Management HiperglikemiDocument13 pagesDiagnosis and Management HiperglikemiTasya SylviaNo ratings yet
- Author: Section Editors: Deputy EditorDocument31 pagesAuthor: Section Editors: Deputy EditorAntenehNo ratings yet
- Diabetic Ketoacidosis (DKA) : in The Established Patient, DKA Results FromDocument3 pagesDiabetic Ketoacidosis (DKA) : in The Established Patient, DKA Results FromOber SánchezNo ratings yet
- Dka in PedsDocument11 pagesDka in PedsMohamed YasserNo ratings yet
- Case PresentationDocument6 pagesCase PresentationYrrem UbaganNo ratings yet
- Diabeticketoacidosisand Hyperglycemichyperosmolar State: Jelena Maletkovic,, Andrew DrexlerDocument19 pagesDiabeticketoacidosisand Hyperglycemichyperosmolar State: Jelena Maletkovic,, Andrew DrexlerSiddhartha PalaciosNo ratings yet
- Treatment and Complications of Diabetic Ketoacidosis in Children and Adolescents - UpToDateDocument31 pagesTreatment and Complications of Diabetic Ketoacidosis in Children and Adolescents - UpToDateAline Maldonado RuizNo ratings yet
- Management of Diabetic Ketoacidosis: MW SavageDocument3 pagesManagement of Diabetic Ketoacidosis: MW SavageChristian SalimNo ratings yet
- Diabetic Ketoacidosis Case FileDocument4 pagesDiabetic Ketoacidosis Case Filehttps://medical-phd.blogspot.comNo ratings yet
- Diabetic Ketoacidosis - ClinicalKeyDocument35 pagesDiabetic Ketoacidosis - ClinicalKeyhibecix840No ratings yet
- Metabolic Alkalosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandMetabolic Alkalosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Diabetic Ketoacidosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandDiabetic Ketoacidosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Exercises For Older People: SittingDocument14 pagesExercises For Older People: SittingFaishal HanifNo ratings yet
- Management of Dyslipidemia in Adults - American Family PhysicianDocument9 pagesManagement of Dyslipidemia in Adults - American Family PhysicianFaishal HanifNo ratings yet
- Vbac StatementDocument48 pagesVbac StatementFaishal HanifNo ratings yet
- Language Development and Deaf Children 2012 v2 1Document6 pagesLanguage Development and Deaf Children 2012 v2 1Faishal HanifNo ratings yet
- TTS OverviewDocument3 pagesTTS OverviewFaishal HanifNo ratings yet
- Agilent N9360A Multi UE Tester: GSM User ManualDocument354 pagesAgilent N9360A Multi UE Tester: GSM User ManualTewodros YimerNo ratings yet
- ContractDocument11 pagesContractbhupendra barhatNo ratings yet
- Action Plan in Science Jaja VersionDocument4 pagesAction Plan in Science Jaja VersionJaja Carlina100% (1)
- Philippine Pop Culture and New Media: Memeology 101: Group 2Document7 pagesPhilippine Pop Culture and New Media: Memeology 101: Group 2Jacob HurstNo ratings yet
- Triboluminescence of Wintergreen Lifesavers Candy Edu 214Document8 pagesTriboluminescence of Wintergreen Lifesavers Candy Edu 214api-570743058No ratings yet
- BIOLOGY 2 (Pedigree Analysis) A4Document7 pagesBIOLOGY 2 (Pedigree Analysis) A4Mark Lorence CuevasNo ratings yet
- Rhetorical Analysis On Emma Watson's SpeechDocument25 pagesRhetorical Analysis On Emma Watson's SpeechZariyah IslaNo ratings yet
- German LyricsDocument179 pagesGerman LyricsTempenkeNo ratings yet
- Tort LawDocument2 pagesTort LawAjay SinghNo ratings yet
- Intl CRL Law-Syllabus-2023Document6 pagesIntl CRL Law-Syllabus-2023B Shivangi 1077No ratings yet
- Film AppreciationDocument159 pagesFilm AppreciationnamanNo ratings yet
- Bird Box ReportDocument16 pagesBird Box Reportapi-450833671No ratings yet
- Longman List of 2470 Academic Collocations (Translated Into Chinese)Document148 pagesLongman List of 2470 Academic Collocations (Translated Into Chinese)froseboomNo ratings yet
- Eme 1510 Albir 03Document2 pagesEme 1510 Albir 03api-201770284No ratings yet
- Crowley - Liber RV Vel Spiritus Sub Figurâ CCVIDocument10 pagesCrowley - Liber RV Vel Spiritus Sub Figurâ CCVICelephaïs Press / Unspeakable Press (Leng)100% (3)
- Unit 1 Friends AbroadDocument2 pagesUnit 1 Friends AbroadZulfadli ZulfadliNo ratings yet
- Colons-Semicolons-And-Commas 15874 0Document5 pagesColons-Semicolons-And-Commas 15874 0OPS PMLCNo ratings yet
- WAT - GD Topics at Top B-SchoolsDocument15 pagesWAT - GD Topics at Top B-SchoolsKanishq BawejaNo ratings yet
- WWWWWWWWWWWWWWWWWWWWWWWWWWWWWWWWWWDocument3 pagesWWWWWWWWWWWWWWWWWWWWWWWWWWWWWWWWWWzoran0706No ratings yet
- 2018:19 Crime StatsDocument220 pages2018:19 Crime StatsBusinessTech64% (14)
- Apply The Word Sample Book of (Matthew) - NKJV PDFDocument60 pagesApply The Word Sample Book of (Matthew) - NKJV PDFTuan Pu100% (1)
- 4MA0 4HR Que 20140115Document24 pages4MA0 4HR Que 20140115Lalith77No ratings yet
- Telugu Typing InstructionsDocument8 pagesTelugu Typing InstructionsDS BhupalNo ratings yet
- Measurement: Ashvin J. Makadia, J.I. NanavatiDocument9 pagesMeasurement: Ashvin J. Makadia, J.I. Nanavatiamalendu_biswas_1No ratings yet
- MA1032 Syllabus 14S2Document2 pagesMA1032 Syllabus 14S2Ishan DewpuraNo ratings yet
- Top International Design 2011 PDFDocument4 pagesTop International Design 2011 PDFcesperon39No ratings yet
- 1 Review Verb Patterns!Document193 pages1 Review Verb Patterns!Felipe PulidoNo ratings yet
- Model Predictive ControlDocument26 pagesModel Predictive Controlrodrigo_trentiniNo ratings yet