Professional Documents
Culture Documents
Clinico-Epidemiological Profile of Childhood Cutaneous Tuberculosis
Clinico-Epidemiological Profile of Childhood Cutaneous Tuberculosis
Uploaded by
Fajar SatriaOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Clinico-Epidemiological Profile of Childhood Cutaneous Tuberculosis
Clinico-Epidemiological Profile of Childhood Cutaneous Tuberculosis
Uploaded by
Fajar SatriaCopyright:
Available Formats
Vol. 13, No.
1, 2015
Original Article
Clinico-epidemiological profile of childhood
cutaneous tuberculosis
Shrestha SB1, Pokhrel GP 2, Pradhan SB3
Department of Dermatology & S.T.I. and 3Pathology
Kathmandu Medical College & Teaching Hospital, Kathmandu, Nepal.
1,2
Abstract
Introduction: Although cutaneous tuberculosis constitutes a small percentage of extra pulmonary
tuberculosis, it has not been fully documented in Nepal and more so in the pediatric population.
Objectives: The aim of the study was to assess the epidemiology and clinical profile of childhood
cutaneous tuberculosis at Kathmandu Medical College and Teaching Hospital, Nepal.
Material and Methods: Children (below 15 years of age) with cutanesous tuberculosis who
attended the teaching hospital between April 2008 and March 2014 were studied.
Results: A total of 17 children with skin tuberculosis were identified during the study period, which
constituted 34% of all patients with skin tuberculosis. There were 11 boys and 6 girls with a mean
age of 8.8 years. The duration of the lesions ranged from 1 month to 4 years and 13 (76.5%) were
brought for medical help after six months of onset of the disease. Lower limb was the most common
site of involvement. Of the various patterns of cutaneous tuberculosis; scrofuloderma was the most
common 7 (41.2%) followed by lupus vulgaris 6 (35.3%), erythema nodosum 2 (11.7%) and gumma
1 (5.8%). Combination of lupus vulgaris and scrofuloderma was noted in one patient. Three patients
(17.6%) had internal organ involvement as pulmonary tuberculosis.
Conclusion: The pattern of skin tuberculosis had wide variation with a few of them having systemic
involvement. Therefore, these patients need a thorough evaluation or an uniform standard therapeutic
regimen to cover both internal organ and cutaneous tuberculosis.
Keywords: Clinical profile, Skin tuberculosis, Nepalese children
Address for correspondence
Dr. Sanju Babu Shrestha
Department of Dermatology and S.T.I.
Kathmandu Medical College & Teaching Hospital
184 Baburam Acharya Marg
Sinamangal, Kathmandu, Nepal.
P.O.Box 21266
Fax No.: 977-1-4477920
E-mail: sanrekha2000@yahoo.com
NJDVL - 45
Vol. 13, No. 1, 2015
Original Article
Introduction
Tuberculosis continues to be a major public health
problem worldwide, because of adverse social
conditions, development of multi-drug resistant
strains of Mycobacterium tuberculosis, ineffective
public health surveillance programmes and the
emergence of HIV infection.1 Extrapulmonary
tuberculosis constitutes around 10% of all cases
of tuberculosis and cutaneous tuberculosis
represents only 1.5 % of all cases of
extrapulmonary tuberculosis. 2 Cutaneous
tuberculosis has a varied clinical presentation,
determined by the pathogenicity, route of infection
as well as status of cellular immunity of the host.3
In children, drug compliance is usually poor and
the immune system is not well developed which
are compounded in the above mentioned
problems.
The paucity of studies from this part of the world
prompted us to undertake the study with the aim
to assess the epidemiology and clinical profile of
childhood cutaneous tuberculosis in a tertiary
care hospital of Kathmandu, Nepal.
Material and Methods
This is a descriptive study where all newly
diagnosed patients of cutaneous tuberculosis (<15
years age) who attended the department of
Dermatology and STI in Kathmandu Medical
College and Teaching Hospital (KMCTH),
Kathmandu between April 2008 and March 2014
were included. Statistical analysis was conducted
by means of SPSS statistical software for
Windows (version 10.0, SPSS Inc, Chicago, IL,
USA). Descriptive statistics were reported through
number and percentage for categorical responses
and mean and standard deviation for continuous
variable. A detailed history was taken with
particular reference to BCG vaccination and
tuberculosis in the family. Clinical features
including the cutaneous and systemic examination
were recorded in a preset proforma. BCG
vaccination was confirmed by the presence of a
small circular scar in the left deltoid region. The
skin biopsy from the advancing edge of the lesion
or the edge of the sinus tract lesion was performed
and was divided into two portions, one part
NJDVL - 46
processed for histopathological evaluation after
staining with hematoxylin and eosin and the other
portion used for culture of mycobacteria in
LowensteinJensen medium. The Mantoux test
was performed by intradermal injection of 0.1
ml of purified tuberculin on the volar surface of
the forearm; induration was measured after 72
hours in all patients. Induration of more than
10mm was taken as suggestive of infection with
M. tuberculosis. Fine needle aspiration of the
lymph nodes was undertaken whenever
indicated.To rule out tuberculosis in other organs,
chest X-ray and sputum-smear examination for
acid-fast bacilli (AFB) on 3-consecutive days
were done for all patients. Patients were classified
according to the morphology of the lesions
described in standard texts. Whenever any
systemic organ was involved or if there was a
presence of generalized lymphadenopathy, the
disease was classified as disseminated.
Haemogram, liver, and renal function tests were
done before starting therapy. Later the patients
were given three or four anti-tubercular drugs
regimen for 6-8 months as per Nepal national
tuberculosis treatment guideline.
Results
A total of 17 children with skin tuberculosis were
identified during the study period, which
constituted 34% (17 out of 50) of all patients with
skin tuberculosis. There were 11 boys and 6 girls
with a mean age of 8.8 years (1.5-14 3.57 years).
The duration of the lesions ranged from 1 month
to 4 years and 13 (76.5%) were brought for
medical help after six months of onset of the
disease. Lower limb was the most common site
of involvement seen in 47% cases, followed by
neck, face, and trunk. Fifteen children were BCG
vaccinated however it was doubtful in 2 patients
because neither a definite scar nor a record of
receiving a BCG vaccination was available. Only
one child had family history of pulmonary
tuberculosis. The mantoux test was positive in
12 (70.5%) patients. Histopathology revealed
tuberculoid granuloma in eight children, caseation
necrosis was found in four cases. In two cases,
histopathology showed erythema nodosum and
one case showed nonspecific features in the form
Vol. 13, No. 1, 2015
Original Article
of chronic inflammatory infiltrate. Table 1
summarizes the main clinico-epidemiological
profiles of these patients.
Clinical
Diagnosis
28
NAD
Lupus vulgaris
35
NAD
Scrofuloderma
18 Rt. Axilla No Yes
30
NAD
Scrofuloderma
10/Male
48 Rt. Ankle
40
NAD
Scrofuloderma
Lupus vulgaris
9/ Male
12 Buttock
20
NAD
Lupus vulgaris
10/ Female
24 Rt thigh
55
NAD
Lupus vulgaris
14/ Female
38
NAD
Scrofuloderma
11/ Female
36 Face
20
NAD
Lupus vulgaris
45
NAD
30
NAD
Erythema
nodosum
Scrofuloderma
Lupus vulgaris+
Pulmoanary-
29
Opacity
BCG
Vaccine
Scrofuloderma
Site
NAD
Duration
(months)
22
Case No.
X-Ray
Chest
ESR
Histopathology/
Fine needle
aspiration
cytology
Mantoux test
(mm)
Lymph
Adenopathy
Family
history of TB
Age (Years)/
Sex
Table 1: Clinical and epidemiological profile of children with cutaneous tuberculosis
7/Male
24 Rt axilla
Yes Yes
Axillary,
Inguinal
cervical
5/Male
24 Rt. ankle
No Yes
NO
10/Male
7/ Male
Neck
Face
No Doubtful Cervical,
axillary
20 Caseation
necrosis
+ epitheloid
granuloma
>30 Tuberculoid
granuloma
>20 Epitheloid
granuloma
Rt. Axillary 20 Epitheloid
granuloma
15 Caseation
No Yes
Axillary
necrosis
+ epitheloid
granuloma
<5 Tuberculoid
No Doubtful NO
granuloma
5 Tuberculoid
No Yes
NO
granuloma
17 Chronic
No Yes
Cervical
inflammatory
infiltrate
10 Tuberculoid
No Yes
NO
granuloma
22 Erythema
No Yes
NO
nodosum
10 14/ Female
Lt. leg
11 5/ Male
Back
No Yes
Axillary
(both)
12 6/ Male
Rt. Knee
No Yes
NO
13 12/ Female
Neck
No Yes
Cervical
14 12/ Male
18 Rt. Leg
No Yes
15 1.5/ Male
Neck
No Yes
Inguinal
(both)
Cervical
Axillary
16 5/ Female
Rt. Leg
No Yes
NO
17 12/ Male
Chest
No Yes
NO
15 Caseation
necrosis
+ epitheloid
granuloma
<5 Tuberculoid
granuloma
20 Epitheloid
granuloma
5 Tuberculoid
granuloma
>10 Epitheloid
granuloma
20 Erythema
nodosum
30 Ill-define
granuloma
tuberculosis
52 Fibrosis
Scrofuloderma
32
NAD
Lupus vulgaris
80
Hilar
lympha
denitis
NAD
Scrofuloderma
NAD
Erythema
nodosum
Gumma
NJDVL - 47
Vol. 13, No. 1, 2015
Original Article
Table 2: Age, sex distribution of the cases
Age (in years)
Lupus Vulgaris Scrofuloderma
(SFD)
(LV)
M
F
M
F
Erythema
Nodosum
Gumma
Total
0-4
2 (11.76%)
5-9
6 (35.29%)
10-14
9 (52.94%)
Total (%)
6 (35.29%)
8 (47.06%)
2 (11.76%)
1 (5.88%)
17 (100%)
M- Male, F-Female
Of the various patterns of cutaneous tuberculosis
seen, 8 (47.06%) had scrofuloderma, 6 (35.3%)
had lupus vulgaris, 2 (11.7%) had erythema
nodosum, and 1child had a gummatous ulcer on
the chest. Combination of lupus vulgaris and
scrofuloderma was noted in one patient. Figure
1-3 depicted the various pattern of cutaneous
tuberculosis. Three patients had internal organ
involvement as pulmonary tuberculosis. All
patients were treated with three or four antitubercular drug regimen for 8 months as per Nepal
national tuberculosis treatment guideline.
Figure 2: Lupus vulgaris over right index finger
and right foot
Figure 1: Lupus vulgaris over Left thumb
Figure 3: Scrofuloderma in the neck and axilla
region
NJDVL - 48
Vol. 13, No. 1, 2015
Original Article
Discussion
The incidence of childhood cutaneous tuberculosis
varied worldwide from 12.8% to 31.7% in India3,
4
and 36.3% in Hong Kong.5 In the present series,
34% of the total numbers of patients with skin
tuberculosis were children. In contrast to the
previous studies 4, 6, boys outnumbered girls in
our study.
Thirteen (76.5%) children brought for medical
help after six months of onset of the disease in
our study. Delay in diagnosis may occur because
of scarce attentions paid by parents during the
early stages of the disease and when they seek
advice it is often from practitioners who are little
exposed to this uncommon condition. Therefore,
sometimes misdiagnosis, 7 neglect, or late
diagnosis8 in children may result in extensive
disease. The definitive diagnosis of skin
tuberculosis employ smear and culture
examination for demonstration of acid fast bacilli
but are tedious and unrewarding.4, 9, 10 Mantoux
test positivity was noted in 70.5% in our series.
This was probably because, in children with
localized disease, sensitization occurred due to
the presence of the disease, or was induced by
BCG, exposure to related environmental
mycobacteria, or M. tuberculosis from infected
close contacts. Mantoux negativity was probably
due to the extent of the disease, malnutrition, and
other related factors.6 In our study, although a
good clinico-histopathological correlation was
observed and was supported by a positive
Mantoux test, yet smear examination with ZiehlNeelsen as well as culture on Lowenstein-Jensen
media were unsuccessful.
In the last couple of decades newer techniques
have emerged for the rapid detection, isolation
and identification of mycobacteria. These include
fluorescent microscopy11, DNA probe
identification, 11 high performance liquid
chromatography,12 polymerase chain reaction,13
serological diagnosis14 and DNA finger printing.15
Newer methods are gradually being incorporated
into the testing schedules which will revolutionize
the early and /or definitive diagnosis of
tuberculosis in future. However, these tests, apart
from being expensive, need well equipped
laboratories and are not available in our hospital.
It is difficult to define the role of BCG. Some
have found no significant difference between
vaccinated and unvaccinated groups, 2 others have
hinted at a modification in the severity,16 and a
recent report indicated moderate protection against
skin tuberculosis.17 Eighty eight percent of the
children in this study had BCG vaccinations. Two
had doubtful BCG vaccination however both of
them had localized disease; scrofuloderma and
LV. Occasionally LV occurring at the site of BCG
vaccination has been seen,10 suggesting exogenous
inoculation of the infection similarly in one of
our patient had lupus vulgaris on the buttock
following intramuscular injection.
Lower limb was the most common site of
involvement in our study. The reason stated for
the predominance in the lower parts of the body
is the lack of clothing in a large number of children
who acquire the infection while playing. 9
Cutaneous manifestations of tuberculosis are
polymorphous in both children and adults.
Scrofuloderma (SFD) was the commonest type
of cutaneous tuberculosis in our series similar to
the other studies6, 18 reported from India. This is
probably due to consumption of unboiled/
unpasteurized milk which is a common
phenomenon in India and which may subsequently
lead to infection of cervical lymph-nodes by M.
bovis via the tonsils with development of SFD.
In India, in general, SFD is more frequent in
children, unlike in Europe where adults are more
often affected with this type of presentation.19
This may be due to differences in the source of
infection, endogenous reactivation being more
common in Europeans.19 Lupus vulgaris (LV) the
second most common forms in our study,
demonstrating a finding probably related to the
improvement in health conditions and general
availability of vaccination programs countrywide
and increases the immunity against M.
tuberculosis. The keratotic form of Lupus vulgaris
was the most common followed by the
hypertrophic and ulcerative varieties.
NJDVL - 49
Vol. 13, No. 1, 2015
Original Article
Mycobacterial infection in LV can be acquired
through both exogenous and endogenous routes,
and may assume warty forms.2,18
Wong et al from Hong Kong reported TVC in as
high as 65.5% of their children and SFD in only
16.3% of their children,5 however in contrast,
41.2% of children in our series had SFD and none
had TVC. Similarly Kumar et al reported SFD
in 51.2% and TVC in only 4.4%.2
Regional lymphadenopathy is seen more often
in children with disseminated disease and thus
appeared to be a soft indicator of disease
dissemination. In the present study the cervical
lymph nodes were most commonly affected in
SFD. A larger number of children were seen in
the younger age groups, as in another hospitalbased study.20 In one report, SFD was the most
common form seen in children, especially girls.21
Children are not only prone to develop SFD but
the lesions, even when localized appear severe
when compared to those of adults.22 More than
one form of skin tuberculosis can affect a patient.10,
23
This presentation seems to be comparatively
uncommon in children, as single child with LV
and SFD was seen in this study. Scrofuloderma
of the chest wall was associated with pulmonary
tuberculosis. Erythema nodosum was noted in
11.7% in our study in contrast to 1.3% tuberculides
reported by Kumar et al from India. Tuberculous
gumma was present in only 1 patient, compared
to the incidence reported in the literature. Primary
skin tuberculosis and acute miliary skin
tuberculosis were also not seen in this series. The
former may present as a chancre due to exogenous
infection in children exposed to tubercle bacilli
for the first time or as noduloulcerative lesions
secondary to BCG inoculation in infants.24 Acute
miliary skin tuberculosis is seen rarely in children
following exanthems 25 or in disorders that
predispose to poor immune status.26
One child had evidence of active foci of
tuberculous infection in the lungs. The incidence
of tubercular lymphadenitis in children with LV
was much greater when compared to that in
adults.10 We have noted lupus vulgaris with
scrofuloderma in one patient. Three patients had
internal organ involvement as pulmonary
tuberculosis. In the spectrum of cutaneous
tuberculosis there are a proportion of patients
with dissemination (systemic involvement) who
are of great epidemiological significance as they
require a change in the standard therapeutic
regimens recommended for cutaneous
tuberculosis.
In conclusion, scrofuloderma and lupus vulgaris
were the most frequent form of cutaneous
tuberculosis and are important causes of morbidity.
There is a high likelihood of internal involvement,
especially in patients with scrofuloderma.
Therefore, all cutaneous tuberculosis patients
need a thorough evaluation for internal organ
involvement and need a uniform standard
therapeutic regimen to cover both internal and
cutaneous tuberculosis.
References
1.
Marcovel J, Servitje O, Moreno A, Jucgla A, Peyri J. lupus vulgaris: Clinical, histopathological
and bacteriologic study of 10 cases. J Am Acad Dermatol 1992; 26: 404-7.
http://dx.doi.org/10.1016/0190-9622(92)70062-K
2.
Kumar B, Kaur S. Pattern of cutaneous tuberculosis in north India. Indian J Dermatol Venereol
Leprol 1986; 52: 203-7.
3.
Sehgal VN, Jain MK, Srivastava G. Changing pattern of cutaneous tuberculosis: A prospective
study. Int J Dermatol 1989; 28: 231-6. http://dx.doi.org/10.1111/j.1365-4362.1989.tb04810.x
4.
Ramesh V, Samuel B, Misra RS, Nath I. In situ characterization of cellular infiltrates in lupus
vulgaris indicates lesional T cell activation. Arch Dermatol 1990; 126: 3315.http://dx.doi.org/10.1001/archderm.1990.01670270063010
5.
Wong KO, Lee PK, Chiu SF. Tuberculosis of the skin in Hong Kong: a review of 100 cases.
Br J Dermatol 1968; 80: 424-8. http://dx.doi.org/10.1111/j.1365-2133.1968.tb11977.x
NJDVL - 50
Vol. 13, No. 1, 2015
Original Article
6.
7.
8.
9.
10.
11.
12.
13.
14.
15.
16.
17.
18.
19.
20.
21.
22.
23.
24.
25.
26.
Kumar B, Rai R, Kaur I, Sahoo B, Muralidhar S, Radotra BD. Childhood cutaneous tuberculosis:
a study over 25 years from northern India. Int J Dermatol 2001; 40: 26-32.
http://dx.doi.org/10.1046/j.1365-4362.2001.01165.x
Prendiville J, Kaufman D, Esterly NB. Psoriasiform plaque on the buttock. Arch Dermatol 1989;
126: 113-8. http://dx.doi.org/10.1001/archderm.1989.01670130119021
Mohamed KN. Verrucous lesions in children in the tropics. Ann Trop Paediatr 1990; 10: 273-7.
Mitchell PC. Tuberculosis among Chinese in Hong Kong. Br J Dermatol 1954; 66: 444-8.
http://dx.doi.org/10.1111/j.1365-2133.1954.tb12576.x
Pandhi RK, Bedi TR, Kanwar AJ, Bhutani LK. Cutaneous tuberculosis-a clinical and investigative
study. Indian J Dermatol 1977; 22: 99-107.
Tenover FC, Crawford JT, Huebner RE, Geiter LJ, Horsburgh CR Jr, Good RC. The resurgence
of tuberculosis: Is your laboratory ready? J Clin Microbiol 1993; 31: 767
Butler WR, Jost KC. Kilburn JO. Identification of mycobacteria by high performance liquid
chromatography. J Clin Microbiol 1991; 31: 2468.
Clarridge JE, Shawar R.M, Shinnick TM, . Large scale use of polymerase chain reaction for
detection of mycobacterium tuberculosis in a routine mycobacteriology laboratory. J Clin
Microbiol 1993; 31: 2049.
Daniel TM, Debanne SM. The serodiagnosis of tuberculosis and other mycobacterial diseases
by enzyme-linked immunosorbent assay. Am Rev Respir Dis 1987: 135: 1137-51.
Cave MD, Eisenach KD, McDermott PF, Bates JH, Crawford JT. conservation of sequence in
Mycobacterium tuberculosis comples and its utilisation in DNA fingerprinting. Mol Cell Probes
1991; 5: 73. http://dx.doi.org/10.1016/0890-8508(91)90040-Q
Sehgal VN, Bhattacharya SN, Jain S, Logani K. Cutaneous tuberculosis: The evolving scenario.
Int J Dermatol 1994; 33: 97-104. http://dx.doi.org/10.1111/j.1365-4362.1994.tb01534.x
Zodpey SP, Shrikhande SN, Maldhure BR, Kulkarni SW. Effectiveness of bacillus Calmette
Guerin (BCG) vaccination in the prevention of tuberculosis of skin: a case control study. Indian
J Dermatol 1998; 43: 4-6.
Singh G. Lupus vulgaris in India. Ind J Dermatol 1974; 40: 257-60.
Yates VM, Ormerod LP. Cutaneous tuberculosis in Blackburn district (U.K.): a 15 year prospective
series. Br J Dermatol 1997; 136: 483-9. http://dx.doi.org/10.1111/j.1365-2133.1997.tb02127.x
Visser AJ, Heyl T. Skin tuberculosis as seen at Ga-Raukuwa hospital. Clin Exp Dermatol 1993;
18: 507-15. http://dx.doi.org/10.1111/j.1365-2230.1993.tb01019.x
Som DD, Swan DD, Tie TE, Pho OB. Tuberculosis cutis in children. Paediatr Indones 1965;
5: 527-34.
Anand IS, Gupta S. Profile of skin disorders in children in Saurashtra. J Indian Med Assoc 1998;
96: 245-6.
Satyanarayana BV. "Tuberculoderma"- a brief review together with statistical analysis and
observations. Indian J Dermatol Venereol Leprol 1963; 29: 25-42.
Gangopadhyay AK. Scrofuloderma-an unusual complication of BCG vaccination. Indian J
Dermatol 1997; 42 :249-50.
Kakakhel KU, Fritsch P. Cutaneous tuberculosis. Int J Dermatol 1989; 28: 355-62.
http://dx.doi.org/10.1111/j.1365-4362.1989.tb02478.x
Frix CD, Bronson DM. Acute miliary tuberculosis in a child with anhidrotic ectodermal dysplasia.
Pediatr Dermatol 1986; 3: 464-7. http://dx.doi.org/10.1111/j.1525-1470.1986.tb00652.x
NJDVL - 51
You might also like
- Bomag BMP8500Service Manual Complete - WatermarkDocument300 pagesBomag BMP8500Service Manual Complete - WatermarkGiovanni Cacciamani100% (1)
- Engineering Economy Lecture4Document22 pagesEngineering Economy Lecture4Jaed Caraig0% (2)
- Er63419 Rev101 140628Document329 pagesEr63419 Rev101 140628Roman BeránekNo ratings yet
- NCP For Geriatric by Mikki Kaio LimDocument1 pageNCP For Geriatric by Mikki Kaio LimJeffrey MarianoNo ratings yet
- SkrofulodermaDocument4 pagesSkrofulodermabangunazhariyusufNo ratings yet
- Tuberculosis in ChildrenDocument4 pagesTuberculosis in ChildrenMarthin TheservantNo ratings yet
- 1 BavejaDocument9 pages1 BavejaIJAMNo ratings yet
- A Clinical Study of Tuberculous Cervical LymphadenDocument5 pagesA Clinical Study of Tuberculous Cervical LymphadenAgung DewanggaNo ratings yet
- 1 s2Document3 pages1 s2RyanNo ratings yet
- Clinical Presentations, Diagnosis, Mortality and Prognostic Markers of Tuberculous Meningitis in Vietnamese Children: A Prospective Descriptive StudyDocument10 pagesClinical Presentations, Diagnosis, Mortality and Prognostic Markers of Tuberculous Meningitis in Vietnamese Children: A Prospective Descriptive StudySilva Dicha GiovanoNo ratings yet
- 1 PB 1 PDFDocument7 pages1 PB 1 PDFAdel Ciiy OcheNo ratings yet
- Cutaneous TB in NigerDocument4 pagesCutaneous TB in NigerRizky ErizkaNo ratings yet
- Unusual Etiology of UTIDocument22 pagesUnusual Etiology of UTIkidsnephrotipsNo ratings yet
- DiagnosisofpulmonaryTB in ChildrenDocument8 pagesDiagnosisofpulmonaryTB in ChildrenSumit MitraNo ratings yet
- Jurnal 7 PulmoDocument7 pagesJurnal 7 Pulmomisra lailaNo ratings yet
- Archive of SID: Diagnostic Value of Lung CT-Scan in Childhood TuberculosisDocument6 pagesArchive of SID: Diagnostic Value of Lung CT-Scan in Childhood TuberculosisJunaedy HfNo ratings yet
- Leprosy in PediatricDocument5 pagesLeprosy in PediatricYusuf Budi HermawanNo ratings yet
- Absceso PeritonsilarDocument5 pagesAbsceso PeritonsilarThomasMáximoMancinelliRinaldoNo ratings yet
- Tuberculous Pleural Effusion in ChildrenDocument5 pagesTuberculous Pleural Effusion in ChildrenAnnisa SasaNo ratings yet
- Pulmonary Tuberculosis in Infants Under One Year of AgeDocument5 pagesPulmonary Tuberculosis in Infants Under One Year of AgeNurul SahidaNo ratings yet
- Pulmonary Tuberculosis As A Differential Diagnosis of PneumoniaDocument18 pagesPulmonary Tuberculosis As A Differential Diagnosis of PneumoniaKadek AyuNo ratings yet
- Chronic Rhinosinusitis-An Update On Epidemiology, Pathogenesis and ManagementDocument5 pagesChronic Rhinosinusitis-An Update On Epidemiology, Pathogenesis and ManagementNaufal NrwNo ratings yet
- Diagnostic Utility of Bronchoalveolar Lavage in Children With Complicated Intrathoracic TuberculosisDocument9 pagesDiagnostic Utility of Bronchoalveolar Lavage in Children With Complicated Intrathoracic TuberculosisFitri Amelia RizkiNo ratings yet
- Pi Is 1201971213002142Document5 pagesPi Is 1201971213002142melisaberlianNo ratings yet
- Ijpedi2021 1544553Document6 pagesIjpedi2021 1544553Naresh ReddyNo ratings yet
- Jurnal InternationalDocument6 pagesJurnal InternationalLeonal Yudha PermanaNo ratings yet
- Tourniquet TestingDocument6 pagesTourniquet TestingPatrick RamosNo ratings yet
- Jurnal KustaDocument14 pagesJurnal KustaRobertus ElvantoraNo ratings yet
- ISM Davit SoesantoDocument14 pagesISM Davit SoesantodavitlieNo ratings yet
- Neonatal Meningitis According To The Microbiological DiagnosisDocument6 pagesNeonatal Meningitis According To The Microbiological DiagnosisDenisa RotaruNo ratings yet
- Breast Tuberculosis DiseaseDocument9 pagesBreast Tuberculosis DiseaseAddis YeshitlaNo ratings yet
- Case Report: A Case Report of Peritoneal Tuberculosis: A Challenging DiagnosisDocument4 pagesCase Report: A Case Report of Peritoneal Tuberculosis: A Challenging DiagnosisDumitru RadulescuNo ratings yet
- Clinical Profile, Etiology, and Management of Hydropneumothorax: An Indian ExperienceDocument5 pagesClinical Profile, Etiology, and Management of Hydropneumothorax: An Indian ExperienceSarah DaniswaraNo ratings yet
- Original Article: Pulmonary Tuberculosis in Childhood Nephrotic Syndrome (A Cross Sectional Study)Document5 pagesOriginal Article: Pulmonary Tuberculosis in Childhood Nephrotic Syndrome (A Cross Sectional Study)Maghfirah RahimaNo ratings yet
- Childhood Tuberculosis and Its Early Diagnosis: James W. GrayDocument6 pagesChildhood Tuberculosis and Its Early Diagnosis: James W. GrayMCINo ratings yet
- Konsensus TBDocument4 pagesKonsensus TBedy belajar572No ratings yet
- 58 JMSCRDocument4 pages58 JMSCRhumayun kabirNo ratings yet
- Dengue JournalDocument4 pagesDengue JournalRohitKumarNo ratings yet
- A Clinical Study On Extrapulmonary TuberculosiDocument10 pagesA Clinical Study On Extrapulmonary TuberculosinayemamasruraNo ratings yet
- TB MeningitisDocument10 pagesTB Meningitisrizky ramadhanNo ratings yet
- Antibiotic Coated Shunt ManuscriptDocument6 pagesAntibiotic Coated Shunt ManuscriptBilal ErtugrulNo ratings yet
- Synopsis Frequency of Non-Adherence To Previous Treatment in Relapse Tuberculosis PatientsDocument5 pagesSynopsis Frequency of Non-Adherence To Previous Treatment in Relapse Tuberculosis PatientsAneesUrRahmanNo ratings yet
- Clinical Profile of Tubercular Uveitis in A Tertiary Care Ophthalmic CentreDocument3 pagesClinical Profile of Tubercular Uveitis in A Tertiary Care Ophthalmic CentreArif BudimanNo ratings yet
- Radiological Findings of Pulmonary Tuberculosis in Infants and Young ChildrenDocument5 pagesRadiological Findings of Pulmonary Tuberculosis in Infants and Young ChildrendtmNo ratings yet
- Spinal Tuberculosis in Children: Sarah Eisen, Laura Honywood, Delane Shingadia, Vas NovelliDocument7 pagesSpinal Tuberculosis in Children: Sarah Eisen, Laura Honywood, Delane Shingadia, Vas NovelliAnonymous YaqenULNgNo ratings yet
- Hematology Profile of Tuberculosis Lymphadenitis Patients at Siti Rahmah Hospital, Padang, IndonesiaDocument5 pagesHematology Profile of Tuberculosis Lymphadenitis Patients at Siti Rahmah Hospital, Padang, IndonesiaNofiana AyuNo ratings yet
- Candidiasis NeonatalDocument9 pagesCandidiasis Neonatalgeorgi15685No ratings yet
- Diagnostic Potential Of 16 Kda (Hspx, Α-Crystalline) Antigen For Serodiagnosis Of TuberculosisDocument7 pagesDiagnostic Potential Of 16 Kda (Hspx, Α-Crystalline) Antigen For Serodiagnosis Of TuberculosispouralNo ratings yet
- Dr. Vona 12Document5 pagesDr. Vona 12Agustiawan ImronNo ratings yet
- 2 - Adult Meningitis in A Setting of High HIV and TB Prevalence - Findings From 4961 Suspected Cases 2010 (Modelo para o Trabalho)Document6 pages2 - Adult Meningitis in A Setting of High HIV and TB Prevalence - Findings From 4961 Suspected Cases 2010 (Modelo para o Trabalho)SERGIO LOBATO FRANÇANo ratings yet
- Uti PediaDocument8 pagesUti PediaNeenya SisonNo ratings yet
- Diagnostic Value of Cytological and Microbiological Methods in Cryptococcal MeningitisDocument9 pagesDiagnostic Value of Cytological and Microbiological Methods in Cryptococcal MeningitisAngelica Maria Rueda SerranoNo ratings yet
- Introp 1Document5 pagesIntrop 1Rima RaisyiahNo ratings yet
- Microbiological Evaluation of Nosocomial Infections by Using National Nosocomial Infection Surveillance (NNIS) SystemDocument13 pagesMicrobiological Evaluation of Nosocomial Infections by Using National Nosocomial Infection Surveillance (NNIS) SystemJanatinAzaNo ratings yet
- Case ReportDocument3 pagesCase Reportyena hillNo ratings yet
- International Journal of Pediatric OtorhinolaryngologyDocument7 pagesInternational Journal of Pediatric OtorhinolaryngologyAndi SuhriyanaNo ratings yet
- Hum. Reprod.-2013-Romosan-1569-79Document11 pagesHum. Reprod.-2013-Romosan-1569-79Ahmad Arbi AninditoNo ratings yet
- Case Study: Transmission of Mycobacterium Tuberculosis: Home Ask The Expert Case Studies Publication Abstracts NewsDocument4 pagesCase Study: Transmission of Mycobacterium Tuberculosis: Home Ask The Expert Case Studies Publication Abstracts NewsJenness VillanuevaNo ratings yet
- Consensus StatementDocument4 pagesConsensus StatementPrasanna NarayananNo ratings yet
- Ascitits BKDocument16 pagesAscitits BKAjengNo ratings yet
- Clinical and Pathologic Analyses of Tuberculosis in The Oral Cavity: Report of 11 CasesDocument8 pagesClinical and Pathologic Analyses of Tuberculosis in The Oral Cavity: Report of 11 CasesMaria Lozano Figueroa 5to secNo ratings yet
- Ijcp-5481 oDocument6 pagesIjcp-5481 oDebasis ChatterjeeNo ratings yet
- SaudiJKidneyDisTranspl302470-5143025 141710Document8 pagesSaudiJKidneyDisTranspl302470-5143025 141710AmatystNo ratings yet
- Guide to Pediatric Urology and Surgery in Clinical PracticeFrom EverandGuide to Pediatric Urology and Surgery in Clinical PracticeNo ratings yet
- Fundamentals of Modern Optics: LecturerDocument5 pagesFundamentals of Modern Optics: LecturervulkkanNo ratings yet
- Lantul de Aprovizionare (Chain Supply)Document59 pagesLantul de Aprovizionare (Chain Supply)tamasraduNo ratings yet
- Chemistry For Engineers 3Document34 pagesChemistry For Engineers 3Audrey VicenteNo ratings yet
- ფიზიკა 7 - მოსწავლის წიგნიDocument219 pagesფიზიკა 7 - მოსწავლის წიგნიBeso ChargeishviliNo ratings yet
- FMP Series: High Pressure Fi LtersDocument14 pagesFMP Series: High Pressure Fi LtersДаниіл ЩигельськийNo ratings yet
- Lecture Dimensionality ReductionDocument34 pagesLecture Dimensionality ReductionAlbert FengNo ratings yet
- Descriptive TextDocument12 pagesDescriptive TextElin NurlenaNo ratings yet
- MNRE 29 Jun 2021 PPA ExtensionDocument1 pageMNRE 29 Jun 2021 PPA Extensionharsha kunturNo ratings yet
- Direct and Indirect Tax:: GST IntroductionDocument12 pagesDirect and Indirect Tax:: GST IntroductionDdaksh KumarNo ratings yet
- Proceedings 10th Mountain Cheese DefDocument95 pagesProceedings 10th Mountain Cheese DefLazline BrownNo ratings yet
- 3-4. SST3005. Rocks and Minerals. KHMYDocument40 pages3-4. SST3005. Rocks and Minerals. KHMYFARAH HIDAYAHNo ratings yet
- CASE STUDY - Smart Stores Reinvent The Retail SpaceDocument1 pageCASE STUDY - Smart Stores Reinvent The Retail Spacetranthihien29604No ratings yet
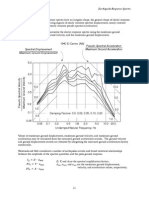
- Newmark&Hall Earthquake Spectrum MakingDocument6 pagesNewmark&Hall Earthquake Spectrum MakingLobsang MatosNo ratings yet
- Hydraulic Transients: When The Steady-State Design Fails!Document58 pagesHydraulic Transients: When The Steady-State Design Fails!gustavods8990No ratings yet
- Monthly Test (April) - Igcse Maths: Marks %Document6 pagesMonthly Test (April) - Igcse Maths: Marks %Aqilah AbdullahNo ratings yet
- Lorentz PS1800 CS-36-1Document4 pagesLorentz PS1800 CS-36-1SINES FranceNo ratings yet
- Tumor Necrosis Factor Methods and ProtocolsDocument265 pagesTumor Necrosis Factor Methods and ProtocolsDario GomezNo ratings yet
- ABS Schema ElectricaDocument5 pagesABS Schema ElectricadickenszzNo ratings yet
- Kruss Bro k20 enDocument2 pagesKruss Bro k20 enBilal KhanNo ratings yet
- Zirconium and Zirconium Alloy Strip, Sheet, and Plate: Standard Specification ForDocument10 pagesZirconium and Zirconium Alloy Strip, Sheet, and Plate: Standard Specification ForTuanbk NguyenNo ratings yet
- In The Same Boat ExcerptDocument17 pagesIn The Same Boat ExcerptI Read YA100% (1)
- Physical Sciences P2 Grade 10 Nov 2017 EngDocument15 pagesPhysical Sciences P2 Grade 10 Nov 2017 EngSesanda SibiyaNo ratings yet
- Ingilizce 700+yeni SorularDocument98 pagesIngilizce 700+yeni SorularDuran Türkyılmaz100% (2)
- DocumentDocument454 pagesDocumentKelly NiuNo ratings yet
- 37-160kW Operators ManualDocument85 pages37-160kW Operators ManualANDRESNo ratings yet
- Gods Jukebox Music ListDocument652 pagesGods Jukebox Music ListaNo ratings yet