Professional Documents
Culture Documents
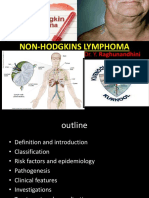
Ethics in Blood Transfusion
Ethics in Blood Transfusion
Uploaded by
GerardLum0 ratings0% found this document useful (0 votes)
627 views1 pageThis document discusses ethics in blood transfusion. It outlines the duties of donors, physicians, and recipients. Donors have a social obligation to donate blood voluntarily without financial incentive, ensuring their health and the safety of the blood supply. Physicians must only prescribe blood transfusions with genuine therapeutic need and maximum safety. Recipients must provide informed consent and have their blood units properly verified and monitored for reactions. The goals are to help patients through ethical and regulated blood donation and transfusion practices.
Original Description:
Ethics in Blood Transfusion
Copyright
© Attribution Non-Commercial (BY-NC)
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document discusses ethics in blood transfusion. It outlines the duties of donors, physicians, and recipients. Donors have a social obligation to donate blood voluntarily without financial incentive, ensuring their health and the safety of the blood supply. Physicians must only prescribe blood transfusions with genuine therapeutic need and maximum safety. Recipients must provide informed consent and have their blood units properly verified and monitored for reactions. The goals are to help patients through ethical and regulated blood donation and transfusion practices.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
627 views1 pageEthics in Blood Transfusion
Ethics in Blood Transfusion
Uploaded by
GerardLumThis document discusses ethics in blood transfusion. It outlines the duties of donors, physicians, and recipients. Donors have a social obligation to donate blood voluntarily without financial incentive, ensuring their health and the safety of the blood supply. Physicians must only prescribe blood transfusions with genuine therapeutic need and maximum safety. Recipients must provide informed consent and have their blood units properly verified and monitored for reactions. The goals are to help patients through ethical and regulated blood donation and transfusion practices.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 1
jslum.
com | Medicine
Ethics in Blood Transfusion
Definitions Duty of Donor
What is right/ good Blood donation
Human duty/ logic of moral discourse Do no harm to donor’s health
Examine troubling dilemmas No risk to health of recipient
Ethics is a dynamic process Responsibilities
Voluntary/ No financial incentive
Making decisions Made to understand – social obligations
First do no harm Safety of blood supply – depend on retention of regular donors
Respect/ Autonomy (patient’s) – wishes, dignity, privacy Obligations to donors
Justice – treat cases alike, fairly distribute benefits, burdens Trained BTS staff in contact
Principled approach to medical ethics No pressure/ discrimination
Assure/ educate donors – blood is handled, distributed with care
Goal of medicine BTS use updated, authorized, detailed criteria for selection, deferral, exclusion
Heal, cure • Explained/ understood
Comfort, palliate • Informed consent
Preserve, promote health • Donor information - confidential
• Confidential matters – conveyed in private
Basic medico-ethical principles Anonymous – donor, recipient
Autonomy – dignity, integrity of human beings Plasmapheresis – handled by specifically trained personnel/ nurses
No wastage – clinician prescribing the blood
Beneficen ce
Justice, equality
Duty of Physician
Indications
Medico-ethi cal guidelines / Code in Transfusion medicine
Most effective therapy with maximum safety
International Society of Blood Transfusion (ISBT)
Transfusion practices review committee
(Code of ethics for blood d onation, transfusion)
Code adopted by WHO Prescription procedure/ blood transfu sion guideline
(prevent errors in requesting, supplying, administrating blood)
Active participants in transfusion medicine
Duty of Recipient
Informed consent – explained/ understood
• capacity to understand
• adequate information
• obtained without coercion
Verify/ Identify – each blood unit pretransfusion
Investigate – reactions/ complications
Prescribed only with genuine therapeutic indication
No financial incentive
Guides in implementing basic princi ples
Goals for BTS (Blood Transfusion Services)
Acceptable mission of a BTS
Meet perceived needs of patient
Minimum cost
Minimum wastage
Maximum safety, effica cy
Ethical approach
Donors
Physicians
Recipients
Blood Transfusi on Form
You might also like
- Principles of ICD 10 Coding PDFDocument473 pagesPrinciples of ICD 10 Coding PDFSheilla Rismadwita100% (13)
- Hema 2 - Midterm Topic 5 - Anemia of Increased DestructionDocument14 pagesHema 2 - Midterm Topic 5 - Anemia of Increased DestructionLowenstein JenzenNo ratings yet
- DR Joe Chaffin Osler CourseDocument81 pagesDR Joe Chaffin Osler CourseHussein MOUSSANo ratings yet
- Heights (Working At) : S W M S (SWMS) P 1Document14 pagesHeights (Working At) : S W M S (SWMS) P 1Benouna Fert100% (1)
- REPORTING CERVICAL CYTOLOGY, The Bethesda SystemDocument3 pagesREPORTING CERVICAL CYTOLOGY, The Bethesda SystemNgotelo FunwiNo ratings yet
- Bone Marrow Aspirate and BiopsyDocument3 pagesBone Marrow Aspirate and BiopsyatikaNo ratings yet
- Pathology of NoaDocument164 pagesPathology of NoaAnonymous milwFDXNo ratings yet
- Soft Tissue InfectionsDocument3 pagesSoft Tissue InfectionsGerardLum100% (1)
- Pituitary Gland PathologyDocument4 pagesPituitary Gland PathologyGerardLumNo ratings yet
- ThanatiaDocument670 pagesThanatiaJoão ClaudioNo ratings yet
- Coagulation 1Document12 pagesCoagulation 1kriss WongNo ratings yet
- NHL Nandu CopasDocument95 pagesNHL Nandu CopaswihelminaNo ratings yet
- A Pattern Based Approach To Nodal Lymphoma: The Critical Role of HistologyDocument55 pagesA Pattern Based Approach To Nodal Lymphoma: The Critical Role of Histologylazy19No ratings yet
- Enseval Examination of Bacterial Contamination in Blood Components Biomerieux PDFDocument21 pagesEnseval Examination of Bacterial Contamination in Blood Components Biomerieux PDFCik KahadiNo ratings yet
- 3 Bone Marrow ExaminationDocument105 pages3 Bone Marrow ExaminationShourav SarkarNo ratings yet
- Coag Made EasyDocument16 pagesCoag Made EasyBrian RobertsNo ratings yet
- Topnotch Parasitology Super Table by DR - Yns PereyraDocument50 pagesTopnotch Parasitology Super Table by DR - Yns PereyraRochelle Joyce AradoNo ratings yet
- Cytology I - Techniques and Application: Peter NG Cyto Lab Ic, MT, PYNEHDocument201 pagesCytology I - Techniques and Application: Peter NG Cyto Lab Ic, MT, PYNEHbusiness onlyyouNo ratings yet
- HPLC PPT - KarishmaDocument76 pagesHPLC PPT - KarishmaDivya GauravNo ratings yet
- Haematology SAQDocument16 pagesHaematology SAQPowell KitagwaNo ratings yet
- Immuno HematologyDocument35 pagesImmuno HematologyAlan McLeanNo ratings yet
- Blood DonationsDocument6 pagesBlood DonationsCHIPapiNo ratings yet
- Qualitative Platelet DisordersDocument34 pagesQualitative Platelet Disordersalibayaty10% (1)
- Reedsternberg CellDocument2 pagesReedsternberg CellYakan AbdulrahmanNo ratings yet
- Bone Marrow Pathology 2 PDFDocument69 pagesBone Marrow Pathology 2 PDFJorge VenturaNo ratings yet
- Blood Transfusion ReactionsDocument33 pagesBlood Transfusion Reactionsmarianne.bilaoen09100% (1)
- Oncology Revision: Paul BaillieDocument299 pagesOncology Revision: Paul BaillieMourian AmanNo ratings yet
- Screening Test For Phagocytic Engulfment: DiapedesisDocument2 pagesScreening Test For Phagocytic Engulfment: DiapedesisBianca ANo ratings yet
- Chapter Blood: RBC Platelet HemostasisDocument89 pagesChapter Blood: RBC Platelet Hemostasisapi-19916399100% (1)
- Red Blood Cell AbnormalitiesDocument9 pagesRed Blood Cell AbnormalitiesIez FatihahNo ratings yet
- Definitions: CLS 422 Clinical Immunohematology I Absorption and ElutionDocument6 pagesDefinitions: CLS 422 Clinical Immunohematology I Absorption and ElutionTrang HuynhNo ratings yet
- Haem. Notes (MBCHB) ProperDocument162 pagesHaem. Notes (MBCHB) ProperKelvinTMaikanaNo ratings yet
- Digital Pathology and Artificial Intelligence As The Next Chapter in Diagnostic HematopathologyDocument7 pagesDigital Pathology and Artificial Intelligence As The Next Chapter in Diagnostic HematopathologyKira Cao0% (1)
- JIPMER Residents ManualDocument68 pagesJIPMER Residents ManualSaroj PandaNo ratings yet
- (6-7) PATH - Colonic Polyps and CarcinomaDocument11 pages(6-7) PATH - Colonic Polyps and Carcinomaaaron mbindyoNo ratings yet
- BD Complete Solution PreAnalitycal System ProductDocument49 pagesBD Complete Solution PreAnalitycal System ProductHendyAnax Anax PointBlankNo ratings yet
- Bone Marrow ExaminationDocument31 pagesBone Marrow ExaminationMonique BorresNo ratings yet
- Patho Final Study GuideDocument55 pagesPatho Final Study GuideBritNo ratings yet
- Cell Inclusions: John SantangeloDocument45 pagesCell Inclusions: John Santangelosaint5470No ratings yet
- Blood Transfusion PDFDocument7 pagesBlood Transfusion PDFSaniNo ratings yet
- Sample Informed ConsentDocument3 pagesSample Informed ConsentNat Lynne Distor TrondilloNo ratings yet
- Blood Bank IDocument136 pagesBlood Bank IPerlie CNo ratings yet
- 5 - Must To Know Clinical MicrosDocument44 pages5 - Must To Know Clinical MicrosRudolph Jr. TaubNo ratings yet
- Cytology II: Gynae and Non-Gynae CytologyDocument126 pagesCytology II: Gynae and Non-Gynae Cytologybusiness onlyyouNo ratings yet
- Transfusion ReactionsDocument28 pagesTransfusion ReactionsRovefrances ErpeluaNo ratings yet
- Clinical Microscopy (Analysis of Urine and Other Body Fluids)Document14 pagesClinical Microscopy (Analysis of Urine and Other Body Fluids)Jeanly DoctorNo ratings yet
- Lymphoid NeoplasmsDocument52 pagesLymphoid NeoplasmsAmalia Riska GNo ratings yet
- 5.Rh Blood Group SystemDocument22 pages5.Rh Blood Group Systemjong188No ratings yet
- Blood ComponentsDocument44 pagesBlood ComponentsKrisha VittoNo ratings yet
- Faquin Milian System and Molecular Advances in Diagnosis Salivary Gland TumorsDocument87 pagesFaquin Milian System and Molecular Advances in Diagnosis Salivary Gland TumorsJoanna Marie100% (1)
- 10-Platelet Structure and Function PDFDocument21 pages10-Platelet Structure and Function PDFAnil SharmaNo ratings yet
- Hematology Written SummariesDocument6 pagesHematology Written SummariesDrexler Ray EukanNo ratings yet
- Component Therapy-Transfusion of TheDocument8 pagesComponent Therapy-Transfusion of TheGennelyn Ross Delos ReyesNo ratings yet
- CELL OVERVIEW PREVENTION Notes 2015Document7 pagesCELL OVERVIEW PREVENTION Notes 2015Alexander LukashenkoNo ratings yet
- Values and Importance of Blood Donation: by Ajal.A.JDocument44 pagesValues and Importance of Blood Donation: by Ajal.A.JMichael VillavertNo ratings yet
- (MICROA - 2.1) Myeloid Tissue HistologyDocument6 pages(MICROA - 2.1) Myeloid Tissue HistologyHenryboi CañasNo ratings yet
- CrossmatchingDocument4 pagesCrossmatchingEl Marie SalungaNo ratings yet
- Consent To BloodDocument2 pagesConsent To Bloodapi-381635811No ratings yet
- Haem MCQ 2012 Student Feedback PDFDocument18 pagesHaem MCQ 2012 Student Feedback PDFaminata6No ratings yet
- Granulomatous Inflammation ThyroidDocument55 pagesGranulomatous Inflammation ThyroidKamlesh PrajapatiNo ratings yet
- Hematopoietic SystemDocument39 pagesHematopoietic SystemapplesncoreNo ratings yet
- Changes Blood Transfusion Consent AlgorithmDocument1 pageChanges Blood Transfusion Consent AlgorithmLawrence GamboaNo ratings yet
- Hemolytic AnemiaDocument1 pageHemolytic AnemiaTeus FatamorganaNo ratings yet
- Thyroid PhysiologyDocument2 pagesThyroid PhysiologyGerardLum100% (2)
- Soft Tissue TumoursDocument8 pagesSoft Tissue TumoursGerardLum100% (2)
- Urinary Tract InfectionDocument4 pagesUrinary Tract InfectionGerardLum100% (2)
- Renal Excretion of DrugsDocument3 pagesRenal Excretion of DrugsGerardLum100% (3)
- ThrombophiliaDocument3 pagesThrombophiliaGerardLum100% (1)
- Prostate GlandsDocument3 pagesProstate GlandsDragan PetrovicNo ratings yet
- Sexually Transmitted DiseasesDocument6 pagesSexually Transmitted DiseasesGerardLum100% (3)
- Renal Function in Disease StateDocument2 pagesRenal Function in Disease Statedamai140390No ratings yet
- Principles of Blood TransfusionDocument2 pagesPrinciples of Blood TransfusionGerardLum100% (3)
- Pathophysiology of Calcium, Phosphate HomeostasisDocument5 pagesPathophysiology of Calcium, Phosphate HomeostasisGerardLum100% (1)
- Pathology of DiabetesDocument4 pagesPathology of DiabetesGerardLum100% (4)
- Pathology of TestesDocument4 pagesPathology of TestesGerardLum100% (1)
- Leukocytes Benign DisordersDocument3 pagesLeukocytes Benign DisordersGerardLum100% (3)
- Pathogenesis Chronic Complications DiabetesDocument5 pagesPathogenesis Chronic Complications DiabetesGerardLum100% (1)
- Pathology of Thyroid DiseasesDocument5 pagesPathology of Thyroid DiseasesGerardLum100% (3)
- Paediatrics OrthopaedicsDocument5 pagesPaediatrics OrthopaedicsGerardLumNo ratings yet
- Nsaids DrugsDocument2 pagesNsaids DrugsIrene Zae MwandotoNo ratings yet
- Pathology GlomerulonephritisDocument4 pagesPathology GlomerulonephritisGerardLum100% (2)
- Obstructive UropathyDocument3 pagesObstructive UropathyGerardLum100% (1)
- Nocturnal EnuresisDocument1 pageNocturnal EnuresisGerardLumNo ratings yet
- Overview of AnaemiaDocument2 pagesOverview of AnaemiaGerardLumNo ratings yet
- Introduction To TransplantationDocument3 pagesIntroduction To TransplantationGerardLumNo ratings yet
- Lymph Node PathologyDocument4 pagesLymph Node PathologyGerardLum0% (1)
- Mechanism of MicturitionDocument4 pagesMechanism of MicturitionGerardLum100% (2)
- Myeloproliferative DisordersDocument2 pagesMyeloproliferative DisordersGerardLumNo ratings yet
- Michael & Co. vs. Enriquez (33 Phil 87 (1915)Document3 pagesMichael & Co. vs. Enriquez (33 Phil 87 (1915)Analyn Grace Yongco BasayNo ratings yet
- COOKERY 9 Q3.Mod1Document5 pagesCOOKERY 9 Q3.Mod1Jessel Mejia Onza100% (4)
- Ca-Cw106451-Mat-098 - Manga Termocontraible WoerDocument5 pagesCa-Cw106451-Mat-098 - Manga Termocontraible WoerJhoel Ipanaque AlarconNo ratings yet
- 2021 HhhhhhhterqasdwqwDocument1 page2021 HhhhhhhterqasdwqwHassan KhanNo ratings yet
- Siemens 3VT MCCBDocument39 pagesSiemens 3VT MCCBerkamlakar2234No ratings yet
- MIET2407 - OENG1181 - Final Report 2018Document4 pagesMIET2407 - OENG1181 - Final Report 2018Trần TínNo ratings yet
- Unit 1: A1 Coursebook AudioscriptsDocument39 pagesUnit 1: A1 Coursebook AudioscriptsRaul GaglieroNo ratings yet
- Mock Trial Task CardsDocument8 pagesMock Trial Task CardsVitaliy Fedchenko0% (1)
- Tesa-60150 MSDSDocument11 pagesTesa-60150 MSDSBalagopal U RNo ratings yet
- ESD122 2-Channel ESD Protection Diode For USB Type-C and HDMI 2.0Document27 pagesESD122 2-Channel ESD Protection Diode For USB Type-C and HDMI 2.0H tavangarNo ratings yet
- Body MechanismDocument31 pagesBody MechanismAnnapurna DangetiNo ratings yet
- Low Voltage Current and Voltage Transformers PDFDocument260 pagesLow Voltage Current and Voltage Transformers PDFGustavo GamezNo ratings yet
- The Sabbath As FreedomDocument14 pagesThe Sabbath As Freedomapi-232715913No ratings yet
- Oracle Business Intelligence Answers: Presentation ServicesDocument6 pagesOracle Business Intelligence Answers: Presentation Servicesvenkatesh.gollaNo ratings yet
- Crude Oil (Conversions)Document3 pagesCrude Oil (Conversions)Carolo DemoNo ratings yet
- System Development Invoice - Audit ToolDocument2 pagesSystem Development Invoice - Audit ToolVictorNo ratings yet
- Ave Maria CollegeDocument6 pagesAve Maria CollegeMylene EsicNo ratings yet
- Kirk Summers Clinical Field Experience A Program Leader Interview Summary and ReflectionDocument4 pagesKirk Summers Clinical Field Experience A Program Leader Interview Summary and ReflectionKirk Summers100% (1)
- Av 10 Universal Remote Control ManualDocument13 pagesAv 10 Universal Remote Control Manualovidiu200970% (10)
- Ghinea Gabriela Nouella and Manea Madalina ElenaDocument25 pagesGhinea Gabriela Nouella and Manea Madalina ElenaAlexandria Firdaus Al-farisyNo ratings yet
- Study On Effect of Manual Metal Arc Welding Process Parameters On Width of Heat Affected Zone (Haz) For Ms 1005 SteelDocument8 pagesStudy On Effect of Manual Metal Arc Welding Process Parameters On Width of Heat Affected Zone (Haz) For Ms 1005 SteelAngga Pamilu PutraNo ratings yet
- Skills Test Unit 1 BDocument5 pagesSkills Test Unit 1 BOsama CanaanNo ratings yet
- Peek - POLYETHER ETHER KETONEDocument58 pagesPeek - POLYETHER ETHER KETONEBryan Jesher Dela Cruz100% (1)
- Perinatal Mental Health Policy BriefDocument3 pagesPerinatal Mental Health Policy BriefThe Wilson CenterNo ratings yet
- Redistribution and PBRDocument1 pageRedistribution and PBRdibpalNo ratings yet
- Historical Moroccan JewishDocument10 pagesHistorical Moroccan JewishSanduNo ratings yet