Professional Documents
Culture Documents
Not Used
Not Used
Uploaded by
MuhammadIqbalMaulanaOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Not Used
Not Used
Uploaded by
MuhammadIqbalMaulanaCopyright:
Available Formats
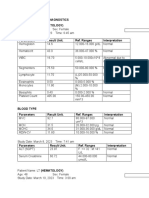
International Journal of Pediatric Otorhinolaryngology 84 (2016) 5254
Contents lists available at ScienceDirect
International Journal of Pediatric Otorhinolaryngology
journal homepage: www.elsevier.com/locate/ijporl
Case Report
Use of intravenous propranolol for control of a large cervicofacial
hemangioma in a critically ill neonate
Shanik J. Fernando a,b,1,*, Sabra Leitenberger c, Matt Majerus c, Alfons Krol c,
Carol J. MacArthur a
a
Department of Otolaryngology Head and Neck Surgery, Oregon Health & Science University, 3181 SW Sam Jackson Park Road, PV01, Portland,
OR 97239, USA
b
School of Medicine, Vanderbilt University, 201 Light Hall, 2215 Garland Avenue, Nashville, TN 37232, USA
c
Department of Dermatology, Oregon Health & Science University, Center for Health & Healing, Mail code: CH16D, 3303 SW Bond Avenue, Portland,
OR 97239, USA
A R T I C L E I N F O
A B S T R A C T
Article history:
Received 24 December 2015
Accepted 6 February 2016
Available online 12 February 2016
Cervicofacial segmental infantile hemangiomas (IH) may result in airway obstruction requiring use of
propranolol to induce hemangioma regression and reestablish the airway. We present the rst case using
intravenous (IV) propranolol for control of airway obstruction and rapid expansion of cervicofacial IH in
the setting of necrotizing enterocolitis (NEC) impaired gastrointestinal function. Intravenous dosing of
propranolol was tolerated well in a critically ill neonate with multisystem complications of prematurity.
2016 Elsevier Ireland Ltd. All rights reserved.
Keywords:
Segmental infantile hemangioma
Propranolol
Vascular anomaly
Necrotizing enterocolitis
Airway
1. Introduction
Segmental hemangiomas are a subtype of infantile hemangioma (IH). The segmental forms of infantile hemangiomas are often
extensive, and can present with complications of IH, including
airway compromise.
We present a case report of our experience using intravenous
propranolol in an attempt to expediently alleviate airway
obstruction secondary to a segmental hemangioma involving
the upper aerodigestive tract including the oor of mouth in an
infant with active NEC.
2. Case description
The baby was born at 27 and 6/7 weeks, weighing 0.645 kg with
respiratory insufciency secondary to prematurity. On physical
exam the infant was noted to be morphologically normal. There
* Corresponding author at: Department of Otolaryngology Head and Neck
Surgery, Oregon Health & Science University, 3181 SW Sam Jackson Park Road,
PV01, Portland, OR 97239, USA. Tel.: +1 9712263959.
E-mail address: Shanik.fernando@vanderbilt.edu (S.J. Fernando).
1
Present address: Vanderbilt University School of Medicine, 201 Light Hall, 2215
Garland Avenue, Nashville, TN 37232, USA.
http://dx.doi.org/10.1016/j.ijporl.2016.02.005
0165-5876/ 2016 Elsevier Ireland Ltd. All rights reserved.
was noted to be adequate perfusion of the skin without rash or
petechiae or palpable lesions. On day of life (DOL) 11 it was rst
noted that there was a salmon-colored macule noted over the
left cheek, eye and forehead. There was progression of the lesion
and on DOL 13, a new ecchymotic area beneath the right chin line
with scattered lacy dark pink macules on the right side of the neck
was noted.
Dermatology and Pediatric Otolaryngology services were
consulted and on DOL 14 noted a left V1 segmental vascular
patch extending from the left nasal sidewall up onto left upper
eyelid and left forehead. In addition there was a right V3 segmental
reticulated vascular patch on the right cheek extending onto the
right lower vermilion lip, and right neck. Finally, an erythematous
patch was noted to be present on the right tip of tongue. With the
presence of extensive segmental hemangiomas, the team considered a diagnosis of PHACE (S) (Posterior fossa malformations,
Hemangioma, Arterial abnormalities, Cardiac abnormalities, Eye
abnormalities, Sternal Cleft/Supraumbilical raphe). Initiation of
oral propranolol was considered to halt growth of this extensive IH
but given that PHACE (S) may be accompanied by narrowed or
absent segments of major vessels in the neck and brain, this was
held until a diagnostic MRI could be performed. A non-sedated MRI
showing grossly normal cervical and intracranial vasculature,
along with lack of other diagnostic features, made the diagnosis of
S.J. Fernando et al. / International Journal of Pediatric Otorhinolaryngology 84 (2016) 5254
PHACE (S) highly unlikely. Airway evaluation with rigid laryngoscopy and bronchoscopy was negative at that time for airway
involvement. Shortly thereafter, the patient had a bloody stool
with an abdominal X-ray demonstrating pneumatosis consistent
with NEC.
Given the concern for developing NEC, the patient was not
treated with propranolol. Following resolution of the NEC on DOL
41, the patient was started on oral propranolol at 0.2 mg/kg/day
divided TID. However, the IH had grown signicantly in the
interval with components involving the neck, oor of mouth, facial
and periorbital areas which continued to enlarge (Figs. 1 and 2).
Shortly following starting oral propranolol, the patient gradually
developed upper airway obstruction and required intubation
following episodes of respiratory distress. Over the following days,
the dosage was gradually increased to 0.4 mg/kg/day divided TID.
However the intraoral components continued to enlarge and
painful ulceration of the lower lip and tongue developed. The
hemangioma continued to rapidly enlarge with the IH involving
the FOM resulting in posteriorsuperior tongue displacement and
impingement on the airway.
Despite gradual increases in the dosage of the PO propranolol
(0.2 mg/kg/day to 1.6 mg/kg/day divided TID) the IH continued to
enlarge. It was then hypothesized that due to the NEC, the enteral
propranolol was not being made bioavailable via the patients
gastrointestinal tract given the lack of response to medication. At 8
weeks of age, she was switched to IV propranolol for 3 weeks. IV
propranolol was initially dosed at 0.3 mg/kg/day divided TID and
titrated up over the following period to 0.5 mg/kg/day which was
determined by the Pharmacology service to be the IV equivalent of
2 mg/kg/day given enterally.
Within 4 days of starting IV propranolol, there was signicant
decrease in the tongue and oor of mouth swelling and the
softening of the hemangioma over the mandible (Fig. 3). Subsequent direct laryngoscopy conrmed the absence of airway
obstruction secondary to hemangioma and noted continued
improvement of tongue and oor of mouth swelling. The patient
was successfully extubated and transitioned back to oral
propranolol. She has continued to improve on outpatient
propranolol at age 7.5 months continuing on a dosage of 2 mg/
kg/day divided TID (Fig. 4).
Fig. 1. Patient with cervicofacial segmental hemangioma at 4 weeks of age.
53
Fig. 2. Evidence of segmental hemangioma in V3 distribution on the right at 4 weeks
of age.
3. Discussion
The use of propranolol for inducing regression of infantile
hemangiomas has been well established in the literature since the
initial discovery of the utility of the non-selective beta blocker in
promoting regression [1]. Following this discovery, propranolol
has become a primary treatment for infantile hemangiomas and is
considered to be standard of care [2,3]. The mechanism of action of
propranolol in causing regression of infantile hemangiomas
remains unclear. Hypotheses around its mechanism of action
include down-regulation of proangiogenic factors and apoptosis of
capillary cells [4]. The drug is typically completely absorbed from
the gastro-intestinal tract and is highly protein bound (8095%)
systemically [5]. In addition, the drug experiences a high rate of
Fig. 3. Evidence of regression of infantile hemangioma following initiation of
intravenous propranolol.
54
S.J. Fernando et al. / International Journal of Pediatric Otorhinolaryngology 84 (2016) 5254
describing the use of intravenous propranolol for infantile
hemangioma, the lesion being located within the orbit [18]. The
case presented here describes the novel use of intravenous
propranolol as an effective treatment of airway obstruction
secondary to a segmental hemangioma in the setting of NEC.
4. Conclusion
The use of IV propranolol, in the setting of a premature infant
with severe NEC, controlled a rapidly expanding IH with airway
impingement quickly within a matter of several days of treatment.
The dosing was tolerated well in a critically ill neonate with
multisystem complications of prematurity.
References
Fig. 4. Six month follow-up after initiation of propranolol therapy.
rst pass metabolism (up to 90% of oral dose is eliminated) [5].
Unfortunately, there are no studies which describe the pharmacokinetic data specic to the infant and child population [6].
Our patient presented with a segmental hemangioma, involving
the lower face. Segmental hemangiomas in this distribution, as
found in our patient, have been previously described to involve the
airway at a high rate [7]. Several case reports in which propranolol
has been used for treating airway hemangiomas have demonstrated success [8,9]. Meta-analyses and larger cohort studies have
further demonstrated the efcacy of using propranolol in resolving
airway hemangiomas [5,10]. While the use of propranolol in
resolving airway hemangiomas has been previously described
with relation to oral dosing, use of intravenous propranolol has not
been previously been reported.
The pharmacokinetics of propranolol have previously articulated in the literature [11,12]. Propranolol is cleared almost
exclusively by hepatic metabolism and as such oral propranolol is
subject to high rst pass effect wherein the effective dose to reach
systemic availability is low [12]. The intravenous dosage is also
quickly cleared by hepatic metabolism, with hepatic blood ow
being the main determinant of metabolism [13]. However, given
the avoidance of the rst pass effect much lower dosages of
intravenous propranolol are able to achieve systemic concentrations comparable to that of oral dosages [14]. For the purposes of
this case, intravenous drug delivery was chosen given concern for
NEC and the questionable absorption of the orally administered
propranolol in light of continued IH progression.
Propranolol is transported via the transcellular pathway across
the gastrointestinal cellular barrier [15]. It has been demonstrated,
in the healthy adult human, that propranolol is efciently
transported transcellularly to become highly bioavailable
[16,17]. In disease states such as NEC, the cellular transport
mechanisms that regulate gastrointestinal permeability are widely
understood to be altered, which may help to explain our
experience in having issues with the effectiveness of orally
administered propranolol. There is only one other case report
[1] C. Leaute-Labre`ze, E. Dumas de la Roque, T. Hubiche, F. Boralevi, J.-B. Thambo, A.
Taeb, Propranolol for severe hemangiomas of infancy, N. Engl. J. Med. 358 (2008)
26492651, http://dx.doi.org/10.1056/NEJMc0708819.
[2] C. Leaute-Labre`ze, P. Hoeger, J. Mazereeuw-Hautier, L. Guibaud, E. Baselga, G.
Posiunas, et al., A randomized, controlled trial of oral propranolol in infantile
hemangioma, N. Engl. J. Med. 372 (2015) 735746, http://dx.doi.org/10.1056/
NEJMoa1404710.
[3] X. Liu, X. Qu, J. Zheng, L. Zhang, Effectiveness and safety of oral propranolol versus
other treatments for infantile hemangiomas: a meta-analysis, PLOS ONE 10
(2015) e0138100, http://dx.doi.org/10.1371/journal.pone.0138100.
[4] T. Itinteang, A.H.J. Withers, P.F. Davis, S.T. Tan, Biology of infantile hemangioma,
Front. Surg. 1 (2014) 38, http://dx.doi.org/10.3389/fsurg.2014.00038.
[5] P.V. Vlastarakos, G.X. Papacharalampous, M. Chrysostomou, E.-F. Tavoulari, A.
Delidis, D. Protopapas, et al., Propranolol is an effective treatment for airway
haemangiomas: a critical analysis and meta-analysis of published interventional
studies, Acta Otorhinolaryngol. Ital. 32 (2012) 213.
[6] L.P. Lawley, E. Siegfried, J.L. Todd, Propranolol treatment for hemangioma of
infancy: risks and recommendations, Pediatr. Dermatol. 26 (2009) 610614,
http://dx.doi.org/10.1111/j.1525-1470.2009.00975.x.
[7] T.M. O, R.E. Alexander, T. Lando, N.N. Grant, J.A. Perkins, A. Blitzer, et al., Segmental
hemangiomas of the upper airway, Laryngoscope 119 (2009) 22422247, http://
dx.doi.org/10.1002/lary.20666.
[8] L. Buckmiller, U. Dyamenahalli, G.T. Richter, Propranolol for airway hemangiomas: case report of novel treatment, Laryngoscope 119 (2009) 20512054, http://
dx.doi.org/10.1002/lary.20633.
[9] S. Maturo, C. Hartnick, Initial experience using propranolol as the sole treatment
for infantile airway hemangiomas, Int. J. Pediatr. Otorhinolaryngol. 74 (2010)
323325, http://dx.doi.org/10.1016/j.ijporl.2009.12.008.
[10] L.M. Buckmiller, P.D. Munson, U. Dyamenahalli, Y. Dai, G.T. Richter, Propranolol
for infantile hemangiomas: early experience at a tertiary vascular anomalies
center, Laryngoscope 120 (2010) 676681, http://dx.doi.org/10.1002/lary.20807.
[11] L. Borgstrom, C.-G. Johansson, H. Larsson, R. Lenander, Pharmacokinetics of
propranolol, J. Pharmacokinet. Biopharm. 9 (1981) 419429, http://dx.doi.org/
10.1007/BF01060886.
[12] R. Gomeni, G. Bianchetti, R. Sega, P.L. Morselli, Pharmacokinetics of propranolol in
normal healthy volunteers, J. Pharmacokinet. Biopharm. 5 (2015) 183192,
http://dx.doi.org/10.1007/BF01065394.
[13] P.A. Routledge, D.G. Shand, Clinical pharmacokinetics of propranolol, Clin. Pharmacokinet. 4 (1979) 7390.
[14] E. Cid, F. Mella, L. Lucchini, M. Carcamo, J. Monasterio, Plasma concentrations and
bioavailability of propranolol by oral, rectal and intravenous administration in
man, Biopharm. Drug Dispos. 7 (1986) 55566, http://dx.doi.org/10.1002/
bdd.2510070605.
[15] N. Takamatsu, L.S. Welage, N.M. Idkaidek, D.-Y. Liu, P.I.-D. Lee, Y. Hayashi, et al.,
Human intestinal permeability of piroxicam, propranolol, phenylalanine, and PEG
400 determined by jejunal perfusion, Pharm. Res. 14 (1997) 11271132, http://
dx.doi.org/10.1023/A:1012134219095.
[16] G. Venkatesh, S. Ramanathan, S.M. Mansor, N.K. Nair, M.A. Sattar, S.L. Croft, et al.,
Development and validation of RP-HPLC-UV method for simultaneous determination of buparvaquone, atenolol, propranolol, quinidine and verapamil: a tool for
the standardization of rat in situ intestinal permeability studies, J. Pharm. Biomed.
Anal. 43 (2007) 15461551, http://dx.doi.org/10.1016/j.jpba.2006.11.013.
[17] G. Krishna, K. Chen, C. Lin, A.A. Nomeir, Permeability of lipophilic compounds in
drug discovery using in-vitro human absorption model, Caco-2, Int. J. Pharm. 222
(2001) 7789, http://dx.doi.org/10.1016/S0378-5173(01)00698-6.
[18] A. Fay, J. Nguyen, F.A. Jakobiec, L. Meyer-Junghaenel, M. Waner, Propranolol for
isolated orbital infantile hemangioma, Arch. Ophthalmol. 128 (2010) 256258,
http://dx.doi.org/10.1001/archophthalmol.2009.375.
You might also like
- Occupational Performance History Interview PDFDocument2 pagesOccupational Performance History Interview PDFBrad0% (4)
- Ethical AnalysisDocument5 pagesEthical Analysisapi-521003884100% (1)
- 32-282 Medical Surveillance ProcedureDocument28 pages32-282 Medical Surveillance ProcedureMatshilario60% (5)
- Endoscopic Supraglottoplasty in Children With Severe Laryngomalacia With and Without Neurological ImpairmentDocument5 pagesEndoscopic Supraglottoplasty in Children With Severe Laryngomalacia With and Without Neurological ImpairmentmitaNo ratings yet
- JurnalDocument9 pagesJurnalNoraine Zainal AbidinNo ratings yet
- Sedation - AyunoDocument7 pagesSedation - AyunoNADIA VICUÑANo ratings yet
- Children With Asthma/ Reactive Airway Disease, Blood Glucose Abnormalities, Congenital Heart Disease, and Cerebrovascular Malformations (E.g., PHACESDocument4 pagesChildren With Asthma/ Reactive Airway Disease, Blood Glucose Abnormalities, Congenital Heart Disease, and Cerebrovascular Malformations (E.g., PHACESAnonymous 52IqhdmZZvNo ratings yet
- Propranolol For HemangiomaDocument8 pagesPropranolol For Hemangiomaansar ahmedNo ratings yet
- Diagnóstico Tardio de MARDocument8 pagesDiagnóstico Tardio de MARthedoctor1986No ratings yet
- International Journal of Pediatric Otorhinolaryngology: Mark W. Steehler, Matthew K. Steehler, Earl H. HarleyDocument5 pagesInternational Journal of Pediatric Otorhinolaryngology: Mark W. Steehler, Matthew K. Steehler, Earl H. HarleyJohan Sebastian Perea PalaciosNo ratings yet
- Laryngomalacia and Swallowing Function in ChildrenDocument7 pagesLaryngomalacia and Swallowing Function in ChildrenmelaniaNo ratings yet
- Interdisciplinary Case Presentation Spring 2017Document50 pagesInterdisciplinary Case Presentation Spring 2017api-316324250No ratings yet
- Efficacy of Propranolol Between 6 and 12 Months of Age in High Risk Infantile HemangiomDocument10 pagesEfficacy of Propranolol Between 6 and 12 Months of Age in High Risk Infantile HemangiomNoviaNo ratings yet
- 1 s2.0 S0022347617301452 MainDocument3 pages1 s2.0 S0022347617301452 MainCindy Julia AmandaNo ratings yet
- 1 s2.0 S002234681100933X MainDocument8 pages1 s2.0 S002234681100933X Mainzahoor ul haqNo ratings yet
- A Therapeutic Maneuver For Oropharyngeal Dysphagia in Patients With PDDocument6 pagesA Therapeutic Maneuver For Oropharyngeal Dysphagia in Patients With PDmajid mirzaeeNo ratings yet
- Apert Syndrome: Anaesthetic Concerns and Challenges: Egyptian Journal of AnaesthesiaDocument3 pagesApert Syndrome: Anaesthetic Concerns and Challenges: Egyptian Journal of AnaesthesiaNur Ainatun NadrahNo ratings yet
- Management of Perforated Appendicitis in Children: A Decade of Aggressive TreatmentDocument5 pagesManagement of Perforated Appendicitis in Children: A Decade of Aggressive Treatmentapi-308365861No ratings yet
- Herti Pardede - 220112140033 - JURNAL PDFDocument5 pagesHerti Pardede - 220112140033 - JURNAL PDFHerti PardedeNo ratings yet
- TMP 18829-E354.full91399039Document7 pagesTMP 18829-E354.full91399039Cordova ArridhoNo ratings yet
- Acquired Nasopharyngeal StenosisDocument8 pagesAcquired Nasopharyngeal StenosisLuiz Cesar WidolinNo ratings yet
- Transpyloric FeedingDocument10 pagesTranspyloric FeedingdryogkNo ratings yet
- A Severe Asphyxiated Newborn: A Case ReportDocument13 pagesA Severe Asphyxiated Newborn: A Case ReportEeeeeeeeeNo ratings yet
- Antenat Hydronephr-4Document8 pagesAntenat Hydronephr-4Ioannis ValioulisNo ratings yet
- Oxido NitricoDocument5 pagesOxido NitricoAmparito TitoNo ratings yet
- 10.7556 Jaoa.2011.111.1.44Document5 pages10.7556 Jaoa.2011.111.1.44DianaNo ratings yet
- Clinical and Radiological Outcomes of Infantile Hemangioma Treated With Oral Propranolol: A Long-Term Follow-Up StudyDocument7 pagesClinical and Radiological Outcomes of Infantile Hemangioma Treated With Oral Propranolol: A Long-Term Follow-Up StudyS FznsNo ratings yet
- Esophageal Atresia: Future Directions For Research On The Digestive TractDocument7 pagesEsophageal Atresia: Future Directions For Research On The Digestive TractindadzilarsyNo ratings yet
- 631-Article Text-2378-1-10-20180830Document6 pages631-Article Text-2378-1-10-20180830azizhamoudNo ratings yet
- Neonatal Hiatal Hernia - A Rare Case ReportDocument4 pagesNeonatal Hiatal Hernia - A Rare Case ReportAgus DarwiyantoNo ratings yet
- Infantil HemagniomaDocument5 pagesInfantil HemagniomaJohannus Susanto WibisonoNo ratings yet
- Respiratory Problems in Children With Esophageal Atresia and Tracheoesophageal FistulaDocument9 pagesRespiratory Problems in Children With Esophageal Atresia and Tracheoesophageal FistulaAshley2993No ratings yet
- Articulos BronquiolitisDocument18 pagesArticulos BronquiolitisLaura López Del Castillo LalydelcaNo ratings yet
- Pott's Puffy Tumor in A 12-Year-Old Boy: ReferencesDocument4 pagesPott's Puffy Tumor in A 12-Year-Old Boy: ReferencesssmasterNo ratings yet
- Choanal AtresiaDocument8 pagesChoanal AtresiaCharmila Sari0% (1)
- Laryngopharyngeal ReflexDocument2 pagesLaryngopharyngeal ReflexidaNo ratings yet
- A Retrospective Review of Newborn Screening For Congenital Hypothyroidism and Newborn Thyroid Disease at A Major Medical CenterDocument8 pagesA Retrospective Review of Newborn Screening For Congenital Hypothyroidism and Newborn Thyroid Disease at A Major Medical CenterJohn Paul Driz ViloriaNo ratings yet
- Advancesinsurgeryfor Abdominalwalldefects: Gastroschisis and OmphaloceleDocument12 pagesAdvancesinsurgeryfor Abdominalwalldefects: Gastroschisis and OmphaloceleSitti HazrinaNo ratings yet
- Absceso Hepático NeonatalDocument6 pagesAbsceso Hepático NeonatalNabila Peña ZapataNo ratings yet
- Paediatric Empyema: A Case Report and Literature ReviewDocument5 pagesPaediatric Empyema: A Case Report and Literature ReviewphobicmdNo ratings yet
- Tracheal Intubation Without Neuromuscular Block in ChildrenDocument7 pagesTracheal Intubation Without Neuromuscular Block in ChildrenYanna RizkiaNo ratings yet
- BM Journal ReadingDocument12 pagesBM Journal ReadingAndrea LawNo ratings yet
- Pediatric Surgery: Original ArticleDocument4 pagesPediatric Surgery: Original ArticleRiyadhiErvinNo ratings yet
- Synosis Finl JDocument7 pagesSynosis Finl JPrasanna MarandiNo ratings yet
- Diificult AirwayDocument13 pagesDiificult AirwayBhi-An BatobalonosNo ratings yet
- Propofol Infusion SyndromeDocument12 pagesPropofol Infusion SyndromeChewit KKaew PChaiNo ratings yet
- International Journal of Pediatric Otorhinolaryngology: F. Glynn, D. Fitzgerald, M.J. Earley, H. RowleyDocument4 pagesInternational Journal of Pediatric Otorhinolaryngology: F. Glynn, D. Fitzgerald, M.J. Earley, H. RowleyJaavyeraa' BelenNo ratings yet
- 8008 28295 2 PB PDFDocument10 pages8008 28295 2 PB PDFPrabuddha ThihawaNo ratings yet
- Pediatrics 2011 Mahr S129 30Document4 pagesPediatrics 2011 Mahr S129 30Erlangga Perwira NegaraNo ratings yet
- Case ReportDocument19 pagesCase ReportddkayikaNo ratings yet
- Oral Propranolol A Useful Treatment For Infantile Hemangioma EditDocument18 pagesOral Propranolol A Useful Treatment For Infantile Hemangioma EditneonitesNo ratings yet
- Current Success in The Treatment of Intussusception in ChildrenDocument9 pagesCurrent Success in The Treatment of Intussusception in ChildrenOby RomdhoniNo ratings yet
- 2021 Article 817Document10 pages2021 Article 817Muriel FialiwanNo ratings yet
- The Effectiveness of An Oral Sensorimotor Stimulation Protocol For The Early Achievement of Exclusive Oral Feeding in Premature Infants A RandomizedDocument14 pagesThe Effectiveness of An Oral Sensorimotor Stimulation Protocol For The Early Achievement of Exclusive Oral Feeding in Premature Infants A RandomizedJUAN CARLOSNo ratings yet
- AnencephalyDocument6 pagesAnencephalyMetta SariNo ratings yet
- Fibrinolytic Treatment of Complicated Pediatric TDocument2 pagesFibrinolytic Treatment of Complicated Pediatric TDR GURDEEP SINGHNo ratings yet
- Duodenal Web at Bizarre LocationDocument22 pagesDuodenal Web at Bizarre LocationRAGHU NATH KARMAKERNo ratings yet
- Case PresentationDocument34 pagesCase PresentationgpstNo ratings yet
- 50 Deogaonkar EtalDocument3 pages50 Deogaonkar EtaleditorijmrhsNo ratings yet
- Nasopharyngeal Airway For Management of Airway Obstruction in Infants With MicrognathiaDocument5 pagesNasopharyngeal Airway For Management of Airway Obstruction in Infants With Micrognathiaapriliani2293No ratings yet
- Infantile Hypertrophic Pyloric Stenosis at A TertiDocument7 pagesInfantile Hypertrophic Pyloric Stenosis at A TertiVașadi Razvan CristianNo ratings yet
- Failure To ThriveDocument3 pagesFailure To ThrivefernandoNo ratings yet
- Laryngopharyngeal Reflux Disease: Integrative ApproachesFrom EverandLaryngopharyngeal Reflux Disease: Integrative ApproachesNausheen JamalNo ratings yet
- The Borax Conspiracy How The Arthritis Cure Has Been Stopped Walter LastDocument12 pagesThe Borax Conspiracy How The Arthritis Cure Has Been Stopped Walter Lastevimagg100% (2)
- Tspsc-Trt-Sa (Physical Education)Document9 pagesTspsc-Trt-Sa (Physical Education)Harish MkNo ratings yet
- Negative Pressure Wound Therapy The Experience of Our Surgery DepartmentDocument10 pagesNegative Pressure Wound Therapy The Experience of Our Surgery DepartmentAthenaeum Scientific PublishersNo ratings yet
- Executive Order No. 1, 2020 BhertDocument2 pagesExecutive Order No. 1, 2020 BhertjomarNo ratings yet
- Cervical OncologyDocument17 pagesCervical OncologyNalin AbeysingheNo ratings yet
- Continuous Improvement: Wins Technical Working GroupDocument18 pagesContinuous Improvement: Wins Technical Working Groupjenny ross domingoNo ratings yet
- m777192 Covidtempl Sabir Hussain 190122160141Document1 pagem777192 Covidtempl Sabir Hussain 190122160141Vikas TeggiNo ratings yet
- Sf2 January Grade 7 MalvarDocument3 pagesSf2 January Grade 7 MalvarVanessa EscaladaNo ratings yet
- Laboratories and DiagnosticsDocument5 pagesLaboratories and DiagnosticsBESA JERIC FLORESNo ratings yet
- Trauma-Informed Supervision Clinical Supervision of Substance Use D o CounselorsaDocument17 pagesTrauma-Informed Supervision Clinical Supervision of Substance Use D o Counselorsaapi-626136134No ratings yet
- Biopsi Gin Malang 2021 DR NovadianDocument31 pagesBiopsi Gin Malang 2021 DR NovadianwandaNo ratings yet
- Uterine ProlapseDocument76 pagesUterine ProlapseRendy Adhitya Pratama75% (4)
- Workbook 1-100Document10 pagesWorkbook 1-100Jarman SinghNo ratings yet
- Differences and Similarities Between Counselling and Psychotherapy2Document8 pagesDifferences and Similarities Between Counselling and Psychotherapy2fn1213No ratings yet
- © 2020 Cristal International StandardsDocument31 pages© 2020 Cristal International Standardsmust spaceNo ratings yet
- The Active Female - Health Issues Throughout The Lifespan (PDFDrive)Document597 pagesThe Active Female - Health Issues Throughout The Lifespan (PDFDrive)leal thiagoNo ratings yet
- 'Making Health Care Systems Fit Ageing Population' by The King's FundDocument88 pages'Making Health Care Systems Fit Ageing Population' by The King's FundCaremarkNo ratings yet
- INFERTILITYDocument48 pagesINFERTILITYAyisha EdwinNo ratings yet
- Kanker GinekologiDocument81 pagesKanker GinekologiSismi AtyNo ratings yet
- RH BillDocument3 pagesRH BillAivan Dale B.CampillaNo ratings yet
- Mental Health: PDHPE Stage 5 Lesson PlanDocument24 pagesMental Health: PDHPE Stage 5 Lesson Planapi-298566801No ratings yet
- CH02 FinalDocument18 pagesCH02 FinalEmmanuel MacaraegNo ratings yet
- Skilled Birth Attendant (SBA) and Home Delivery in India: A Geographical StudyDocument8 pagesSkilled Birth Attendant (SBA) and Home Delivery in India: A Geographical StudyInternational Organization of Scientific Research (IOSR)No ratings yet
- 20-Year History of Diarrhea With Intermittent ConstipationDocument2 pages20-Year History of Diarrhea With Intermittent Constipationhossein kasiriNo ratings yet
- Portmafia GroupDocument27 pagesPortmafia Groupalvinlarano11No ratings yet
- Imagery CBTDocument3 pagesImagery CBTMichelle YongNo ratings yet
- Risks Cost Benefits Ease of Implementation TotalDocument2 pagesRisks Cost Benefits Ease of Implementation Totalkent starkNo ratings yet