Professional Documents
Culture Documents
Jurnal
Jurnal
Uploaded by
Inggriht Senny BondangCopyright:
Available Formats
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5820)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (852)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (898)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (349)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (403)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Counseling Parents of Children With Disabilities: A Review of The Literature and Implications For PracticeDocument1 pageCounseling Parents of Children With Disabilities: A Review of The Literature and Implications For PracticeDiana LoiNo ratings yet
- Spondilitis TBDocument2 pagesSpondilitis TBInggriht Senny BondangNo ratings yet
- DR. ARIFIN - CAP (New PDPI Guideline)Document36 pagesDR. ARIFIN - CAP (New PDPI Guideline)Inggriht Senny BondangNo ratings yet
- 1749 8090 8 54 PDFDocument7 pages1749 8090 8 54 PDFInggriht Senny BondangNo ratings yet
- Sample: Ventral Hernia RepairDocument8 pagesSample: Ventral Hernia RepairInggriht Senny BondangNo ratings yet
- Kuliah Alergi InhalanDocument10 pagesKuliah Alergi InhalanInggriht Senny BondangNo ratings yet
- Setting Up Emergency Medical Service: Intensive Course & WorkshopDocument41 pagesSetting Up Emergency Medical Service: Intensive Course & WorkshopInggriht Senny BondangNo ratings yet
- Mod 1b Airway AdvancedDocument38 pagesMod 1b Airway AdvancedInggriht Senny BondangNo ratings yet
- A Review of Antibiotic Use in Pregnancy: EY OrdsDocument11 pagesA Review of Antibiotic Use in Pregnancy: EY Ordsnoname19191No ratings yet
- Nutrition Guide For Clinicians: From The Physicians Committee For Responsible Medicine / Spring 2007 / Vol. XVI, No. 2Document24 pagesNutrition Guide For Clinicians: From The Physicians Committee For Responsible Medicine / Spring 2007 / Vol. XVI, No. 2mensapertaNo ratings yet
- Issva Classification 2014 Final TrialDocument20 pagesIssva Classification 2014 Final TrialFrancis MunguíaNo ratings yet
- Congenital Talipes Equino-VarusDocument48 pagesCongenital Talipes Equino-VarusKojo DuncanNo ratings yet
- Choanal AtresiaDocument8 pagesChoanal AtresiaCharmila Sari0% (1)
- WhoDocument351 pagesWhozulfina harisyuhraNo ratings yet
- Cornelia de Lange Syndrome - A Recognizable Fetal PhenotypeDocument5 pagesCornelia de Lange Syndrome - A Recognizable Fetal PhenotypeTien Chen TuNo ratings yet
- Chromosomal DisordersDocument4 pagesChromosomal DisordersYoussry JaranillaNo ratings yet
- PRC - ICF - Compilations 2009-2016Document18 pagesPRC - ICF - Compilations 2009-2016Jonas Marvin AnaqueNo ratings yet
- Bahan Kongenital HidungDocument6 pagesBahan Kongenital HidungIta WahyuniNo ratings yet
- whd2016 Brochure en 2Document16 pageswhd2016 Brochure en 2api-311125682No ratings yet
- Common Craniofacial SyndromesDocument126 pagesCommon Craniofacial Syndromesdr parveen bathlaNo ratings yet
- Antidepressants in Pregnancy4 2016Document60 pagesAntidepressants in Pregnancy4 2016هناء همة العلياNo ratings yet
- Intellectual DiabilityDocument10 pagesIntellectual DiabilityAngelo PapimNo ratings yet
- RubelaDocument11 pagesRubelaMuhammad YusriNo ratings yet
- Congenital Rubella SyndromeDocument2 pagesCongenital Rubella SyndromeRajiv KabadNo ratings yet
- Prenatal Diagnosis of Penoscrotal Transposition With 2-And 3-Dimensional UltrasonographyDocument5 pagesPrenatal Diagnosis of Penoscrotal Transposition With 2-And 3-Dimensional UltrasonographyIndach ZyadarifnaNo ratings yet
- Teratogen Pregnancy KuliahDocument40 pagesTeratogen Pregnancy KuliahVonny RiskaNo ratings yet
- 104 FullDocument5 pages104 FullSamNo ratings yet
- Preconception Counselling PDFDocument4 pagesPreconception Counselling PDFponekNo ratings yet
- Healthmedicinet Com II 2014 AprDocument328 pagesHealthmedicinet Com II 2014 AprHeal ThmedicinetNo ratings yet
- Born To Die. Witchcraft and Infanticide in Baruba CultureDocument18 pagesBorn To Die. Witchcraft and Infanticide in Baruba CultureIñaki RegueraNo ratings yet
- TorchDocument6 pagesTorchMary Jean HernaniNo ratings yet
- Atresia EsofagusDocument7 pagesAtresia EsofagusTommysNo ratings yet
- Neonatal Oral MotorDocument5 pagesNeonatal Oral MotorYessenia DiazNo ratings yet
- Etiology of Congenital ScoliosisDocument3 pagesEtiology of Congenital ScoliosisCrissu CrissNo ratings yet
- MSDS Carbon Monoxidee PDFDocument13 pagesMSDS Carbon Monoxidee PDFkarthikeyanNo ratings yet
- Congenital HypothyroidismDocument2 pagesCongenital Hypothyroidismapi-321672273No ratings yet
- Apert SyndromeDocument9 pagesApert SyndromeRiyan BudianorNo ratings yet
Jurnal
Jurnal
Uploaded by
Inggriht Senny BondangOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Jurnal
Jurnal
Uploaded by
Inggriht Senny BondangCopyright:
Available Formats
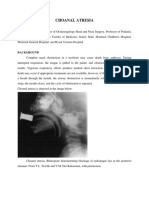
Journal of Neonatal Surgery 2016; 5(1):2
ORIGINAL ARTICLE
Congenital Abdominal Wall Defects: Staged closure by Dual Mesh
Kirsten Risby,1 Marianne Skytte Jakobsen,2 Niels Qvist3
1 Hans Christian Andersen Childrens Hospital, Odense University Hospital, Denmark
2 Department of Pediatrics, Kolding Hospital, Denmark
3 Department of surgery A (Pediatric Surgery), Odense University Hospital, Denmark
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use,
distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
Objective: To evaluate the clinical utility of GORE DUALMESH (GDM) in the staged closure of large
congenital abdominal wall defects.
Materials and Methods: Data of patients with congenital abdominal wall defects managed with GDM was
analyzed for outcome regarding complete fascial closure; mesh related complications; and post-
discharge gastrointestinal surgery.
Results: GDM was placed in 34 (gastroschisis=27, omphalocele=7) patients during the study period.
Complete closure of the fascia was obtained in one patient with omphalocele and in 22 patients with
gastroschisis. Mesh related surgical complications were seen in five (15%) children: four had
detachment of the mesh and one patient developed abdominal compartment syndrome. Mesh related
clinical infection was observed in five children. In hospital mortality occurred in four cases (2
gastroschisis and 2 omphalocele) and was not procedure-related. Of the 30 children discharged, 28
(82%) were still alive. At follow-up, three patients (10%) were operated for a minor ventral hernia and
4 children were operated (laparotomy and adhesionolysis) for adhesive intestinal obstruction.
Conclusion: Staged closure with GDM is a safe alternative when primary fascial closure is difficult.
Key words: Gastroschisis, Omphalocele, Mesh, Gore DualMesh
INTRODUCTION
In infants with congenital abdominal wall de- apy with epithelialization [8] followed by
fect, the ultimate surgical goals are to reduce secondary ventral hernia repair. It is not known
the herniated viscera into the abdomen with a which type of treatment involves the lowest risk
final complete closure of the fascia and skin to of complications and the highest success rate
create a solid abdominal wall with an accepta- of secondary closure of the fascia, especially in
ble cosmetic result. It is essential that this is those children with large defects and eviscera-
done without risking abdominal compartment tion.
syndrome or tissue damage [1, 2].
The aim of this retrospective study was to
In up to 79% [3] of the infants, primary closure evaluate the clinical utility of GDM in the
of the fascia is impossible; where several other staged secondary closure of large congenital
techniques have been described including abdominal wall defects. The primary outcomes
Silastic chimney (silo) construction with staged under evaluation were complete fascial closure;
reduction of the viscera and secondary closure the nature and frequency of mesh related
of the abdomen [4], prosthetic patch defect clo- complications; and post-discharge gastro-
sure [5, 6], skin flap closure [7] or topical ther- intestinal surgery.
* Corresponding Author EL-MED-Pub Publishers.
Congenital Abdominal Wall Defects: Staged closure by Dual Mesh
MATERIALS AND METHODS gestational age, birth weight, additional
congenital anomalies, numbers of operation,
A review of medical record of children, with a numbers of mesh adjustments, and the age at
diagnosis of gastroschisis (DQ79.3) or omphalo- complete fascial closure. Postoperative data re-
cele (DQ79.2) in whom the GDM (GORE, Flag- viewed were complications including detach-
staff, Arizona, USA) was used for surgical repair ment of the mesh, wound infections, and post-
during the period from 1 January 1996 to 1 discharge gastrointestinal surgery. The study
September 2014 in a tertiary center, was done. was approved by the Regional committee of Bio-
The mesh was applied to the patients where it medical Ethics (Project-ID S-20120215).
was impossible to reduce more than two thirds
of the estimated volume of the herniated organs RESULTS
or with a defect > 5 cm.
During the study period, a total of 181 infants
Technique: underwent repair of a congenital abdominal
wall defect; 104 with gastroschisis and 77 with
After the umbilical vessels had been ligated, the omphalocele. A mesh was placed in 34 patients
mesh was sutured to the fascial edges of the (gastroschisis=27, omphalocele=7). A summary
defect to create a silo. Abdominal tension was of clinical background data on the children
evaluated daily by abdominal palpation and operated with mesh is presented in Table l.
general clinical condition. When further reduc-
tion of the organs was considered possible Mortality and concomitant congenital malfor-
(respiratory frequency < 25/min, O2 saturation mations:
>96% by pulse oximetry and if on ventilator an
inspiratory pressure < 10 mmHg and with a Of the 34 children operated with mesh two chil-
fraction of O2 0.4, the mesh was reopened at dren (one with gastroschisis and one with om-
top midline and any adhesions between intes- phalocele) died with the mesh in situ before
tines and abdominal wall were freed to further closure was possible. Thus 32 completed treat-
reduce the organs into the abdominal cavity. ment and 28 of these children (82%) were still
Then the mesh was reduced correspondingly alive (September 2014) (mean age 9.5 years,
and closed by a running suture (Fig. 1) under range 0-18). The total mortality was three chil-
maximal traction without compromising dren from the gastroschisis group (11%) and
ventilation (max inspiration pressure below 15 three from the omphalocele group (43%) (Table
mm Hg). This was continued until outcome of 3). In the six fatality cases five had concomitant
closure was reached. congenital malformations. Among those who
were still alive, only two had concomitant
congenital malformations.
Mesh-related surgical procedures:
In 91% of the cases, the mesh was implanted
as the primary procedure; in the rest, it was
secondary to a failed Silastic silo. The age of the
child at implant of mesh ranged between 1 and
10 days (Table 2). On average three mesh-re-
lated procedures were performed in these pa-
tients with a range of 1-11 interventions for
sequential reduction of eviscerated contents.
Removal of the mesh was done within 11 days
Figure 1: Top view of inserted GDM.
in 50% of the children, within 22 days in 75%
Data extracted included prenatal diagnosis, and within 44 days in 90% of the children (Fig.
type of defect, type and place of birth, sex, 2).
Journal of Neonatal Surgery Vol. 5; 2016
Congenital Abdominal Wall Defects: Staged closure by Dual Mesh
Table 1: Clinical characteristics
Gastroschisis N=27 Omphalocele N=7
Male (%) 16 (59) 3 (42)
Mean gestational age weeks (range) 37 (32 - 41) 38 (28 - 39)
Mean birth weight grams (range) 2370 (1501- 4230) 3027 (957 - 4090)
Prenatal diagnosis (%) 22 (81.48) 7 (100)
In-house birth (%) 19 (70.37) 6 (85.71)
Method of birth (%)
Spontaneous vaginal delivery 13 (48.15) 0 (0)
Induced vaginal delivery 0 (0) 1 (14.29)
Elective Caesarean section 4 (14.81) 4 (57.14)
Sub-acute Caesarean section 3 (11.11) 1 (14.29)
Emergency Caesarean section 7 (25.93) 1 (14.29)
Table 2: Mesh-related surgical procedures in 32 children
Gastroschisis Omphalocele
N=26 N=6
Age at implantation 1 (1-10) 2 (1-10)
(days)
Days with mesh in situ 9 (3-79) 18 (6-178)
Mesh-related surgical 3 (1-11) 3 (2-5)
procedures in general
anesthesia
Median number of 1 (1-5) 1.5 (1-4)
GDM patches used
Age at complete 9.5 (4-80) 16
fascial closure (days)
The numbers are median values; the range is in brackets
Table 3: The characteristic of the fatality cases
Type of defect Age at death Cause of death Mesh Additional congenital
treatment malformation
(days) completed
Gastroschisis 19 Septicaemia No Hypertrophic liver, persistent
ductus arteriosus
Gastroschisis 318 PNT induced liver Yes Short bowel syndrome
failure
Gastroschisis 2507 Abdominal Yes None
catastrophe
Omphalocele 38 Liver failure No Central liver hematoma
Omphalocele 271 Heart failure Yes Pulmonary hypoplasia
Omphalocele 404 Heart failure Yes Inoperable ventricular and atrial
septum defect
PNT: parenteral nutrition treatment
Journal of Neonatal Surgery Vol. 5; 2016
Congenital Abdominal Wall Defects: Staged closure by Dual Mesh
Abdominal defect closure: life. Three patients (10%) were operated on for a
minor ventral hernia. During the observation
Among the children who completed surgical period laparotomy with adhesionolysis for
treatment a complete closure of the fascia was adhesive bowel obstruction in two children
obtained in only one (16th day) out of six chil- (7%), aged 5 months and 5 years respectively,
dren with omphalocele and in 22 out of 26 (on and laparotomy for a chronic ileus condition in
average 9.5 days) with gastroschisis (Table 2). three (10%): one due to a primary unrecognized
In the remaining nine children where fascial sickle-shaped jejunal atresia and two due to
closure was not possible, the mesh was left in peritoneal adherences. Four children (13%)
situ and removed after a period of 14 days to have been admitted to hospital for a conserva-
six months. In five children epithelialization of tive treatment of symptoms of ileus at the age
defect occurred, and in four skin grafts were of two, five, eight, and fifteen years, respec-
needed. tively.
DISCUSSION
The present study showed a low rate of second-
ary closure of the fascia in children with
omphalocele compared with gastroschisis de-
fects. A comparison with other studies is diffi-
cult as most studies with staged closure in-
clude large as well as minor defects. The proce-
dure-related complications were minimal, but a
relative high frequency of ileus due to adhe-
sions during later life was observed.
Figure 2: The duration of the treatment of GDM. In 50% of One of the advantages of the Gore-Tex dual
the children the mesh was removed within 11 days, in 75% mesh is that it gives the possibility to obtain
within 22 days and in 90% within 44 days. tension on the fascial edges avoiding lateraliza-
tion, which happens with the Silastic silo
Complications related to insertion of the mesh:
method. Moreover, when secondary fascial clo-
Surgical mesh-related complications were seen sure is impossible, the mesh may be left in situ
in five (15%) children. In four of these the mesh which help creating strong fibrous tissue be-
detached requiring re-suturing or reimplanta- neath the mesh when it may be removed allow-
tion of a new mesh. The fifth child developed ing self-epithelialization or skin grafting. The
abdominal compartment syndrome requiring disadvantage with the mesh is that it is not
temporary loosening of the mesh. Clinical infec- translucent, and therefore it is not possible to
tion related to the mesh defined as fever, red- observe the intestinal loops for ischemia. How-
ness of the wound and elevated serum C-reac- ever, this complication was not seen in any of
tive protein levels was observed in five (15%) our patients.
children. Four of these were treated by sys-
To date the use of GDM as a prosthetic mate-
temic antibiotics, and in one patient a prema-
rial in closure of congenital abdominal wall de-
ture mesh removal was chosen. Suture
fects has been described in smaller series only.
granulomas were resected twice in one child, at
Rahn et al. [5] compared the use of a dura
age 3.5 and 8 years old, respectively. No mesh-
patch versus GDM in the management of
related complication caused death.
congenital wall defects. In their series, four
Post-discharge gastrointestinal surgery: children were successfully treated with GDM; a
smooth underlying pseudo-membrane was
One child was later diagnosed with biliary atre- formed, that provided a stable covering to the
sia and Kasai procedure done at 80th day of eviscerated viscera, in all four children followed
Journal of Neonatal Surgery Vol. 5; 2016
Congenital Abdominal Wall Defects: Staged closure by Dual Mesh
by secondary abdominal wall reconstruction at CONCLUSION
the age of 20-30 months. Stringel [9] and Willis
[10] evaluated the clinical utility of Gore-Tex When primary closure is not possible, staged
mesh for the repair of neonatal congenital ab- closure with GDM is a safe alternative creating
dominal wall defects in three and ten infants a stable abdominal wall with few mesh-related
respectively. The Gore-Tex meshes used were neonatal complications. Clinicians and parents
from W. L. Gore and associates, Flagstaff, Ari- should be aware of an increased risk of ileus in
zona, USA, but it was not specified whether it later life with this mesh.
was GDM. In both of series, frequent local
infection and mesh removal were reported. REFERENCES
However, both authors concluded that Gore-
1. Christison-Lagay ER, Kelleher CM, Langer JC.
Tex was a useful patch for closure of congenital Neonatal abdominal wall defects. Semin Fetal
abdominal wall defects and a safe alternative in Neonatal Med. 2011;16:164-72.
cases where primary closure is not feasible. 2. Ledbetter DJ. Congenital abdominal wall defects
Rijhwani [6] et al described similar results in and reconstruction in pediatric surgery:
gastroschisis and omphalocele. Surg Clin North
three children treated by the use of a Gore-Tex Am. 2012;92:713-27.
mesh requiring mesh removal due to mesh-re- 3. Davis RP, Treadwell MC, Drongowski RA,
lated infections. Teitelbaum DH, Mychaliska GB. Risk stratification
in gastroschisis: can prenatal evaluation or early
postnatal factors predict outcome? Pediatr Surg
Rijhwani et al. [6] reported frequent late opera- Int. 2009;25:319-25.
tions due to ventral (60%) and inguinal (30%) 4. Pastor AC, Phillips JD, Fenton SJ, Meyers RL,
hernias in infants operated by staged closure, Lamm AW, Raval MV, et al. Routine use of a
without specifying whether Gore-Tex or other SILASTIC spring-loaded silo for infants with
gastroschisis: a multicenter randomized controlled
silo-material was used. In our series, three chil- trial. J Pediatr Surg. 2008;43:1807-12.
dren (10%) were operated for ventral hernia; 5. Rahn S, Bahr M, Schalamon J, Saxena AK.
only one child (4%) who had a successful Single-center 10-year experience in the
management of anterior abdominal wall defects.
secondary facial closure needed surgery for a Hernia. 2008;12: 345-50.
ventral hernia. This indicates that closure of
6. Rijhwani A, Davenport M, Dawrant M, Dimitrou
the abdomen by bridging the defect with a G, Patel S, Greenough A, et al. Definitive surgical
mesh until final apposition of the fascial edges management of antenatally diagnosed
exomphalos. J Pediatr Surg. 2005;40:516-22.
and skin can be obtained creates a stable ab-
7. Zaccara A, Zama M, Trucchi A, Nahom A, De
dominal wall in the vast majority of cases. A
Stefano F, Bagolan P. Bipedicled skin flaps for
disadvantage related to the use of the mesh reconstruction of the abdominal wall in newborn
might be the need of repeated surgical proce- omphalocele. J Pediatr Surg. 2003;38:613-5.
dures in general anesthesia, but it is worth- 8. Lee SL, Beyer TD, Kim SS, Waldhausen JHT,
Healey PJ, Sawin RS, et al. Initial nonoperative
while to mention that no procedure-related management and delayed closure for treatment of
complications were observed. The relative high giant omphaloceles. J Pediatr Surg. 2006;
in-hospital mortality observed in our study was 41:1846-9.
mainly related to concomitant malformations 9. Stringel G. Large gastroschisis: primary repair
with Gore-Tex patch. J Pediatr Surg.
and immaturity. This is in accordance with 1993;28:653-5.
previous studies [11-14].
10. Willis PM, Albanese CT, Rowe MI, Wiener ES.
Long-term results following repair of neonatal
The limitations in the present study are its abdominal wall defects with Gore-Tex. J Peditric
Surg. 1995;10:93-96.
retrospective nature and a less significant
study model but we present a cohort of 34 chil- 11. Arnold MA, Chang DC, Nabaweesi R, Colombani
PM, Bathurst MA, Mon KS, et al. Risk
dren, which to our knowledge is the largest de- stratification of 4344 patients with gastroschisis
scribed cohort of children with congenital ab- into simple and complex categories. J Pediatr
Surg. 2007;42:1520-5.
dominal wall defect operated by the using of a
12. Abdullah F, Arnold MA, Nabaweesi R, Fischer AC,
GDM. Colombani PM, Anderson KD, et al. Gastroschisis
in the United States 1988-2003: analysis and risk
categorization of 4344 patients. J Perinatol.
2007;27:50-5.
Journal of Neonatal Surgery Vol. 5; 2016
Congenital Abdominal Wall Defects: Staged closure by Dual Mesh
13. Molik KA, Gingalewski CA, West KW, Rescorla FJ, 14. Garne E, Rasmussen L, Husby S.
Scherer III LR, Engum SA, et al. Gastroschisis: a Gastrointestinal malformations in Funen county,
plea for risk categorization. J Pediatr Surg. Denmark-epidemiology, associated malformations,
2001;36:51-5. surgery and mortality. Eur J Pediatr Surg.
2002;12:101-6.
Address for Correspondence*:
Niels Qvist, Odense University Hospital Surgical Department, Denmark
E mail: famqvist@dadlnet.dk
2016, Journal of Neonatal Surgery
Submitted: 06-10-2015
Accepted: 21-10-2015
Conflict of interest: None
Source of Support: This work was supported by grants from The Region of Southern Denmark (13/27678) and The University of Southern
Denmark (36/101-070671).
How to cite: Risby K, Jakobsen MS, Qvist N. Congenital abdominal wall defects: staged closure by dual mesh. J Neonat Surg. 2016; 5:2.
Journal of Neonatal Surgery Vol. 5; 2016
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5820)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (852)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (898)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (349)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (403)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Counseling Parents of Children With Disabilities: A Review of The Literature and Implications For PracticeDocument1 pageCounseling Parents of Children With Disabilities: A Review of The Literature and Implications For PracticeDiana LoiNo ratings yet
- Spondilitis TBDocument2 pagesSpondilitis TBInggriht Senny BondangNo ratings yet
- DR. ARIFIN - CAP (New PDPI Guideline)Document36 pagesDR. ARIFIN - CAP (New PDPI Guideline)Inggriht Senny BondangNo ratings yet
- 1749 8090 8 54 PDFDocument7 pages1749 8090 8 54 PDFInggriht Senny BondangNo ratings yet
- Sample: Ventral Hernia RepairDocument8 pagesSample: Ventral Hernia RepairInggriht Senny BondangNo ratings yet
- Kuliah Alergi InhalanDocument10 pagesKuliah Alergi InhalanInggriht Senny BondangNo ratings yet
- Setting Up Emergency Medical Service: Intensive Course & WorkshopDocument41 pagesSetting Up Emergency Medical Service: Intensive Course & WorkshopInggriht Senny BondangNo ratings yet
- Mod 1b Airway AdvancedDocument38 pagesMod 1b Airway AdvancedInggriht Senny BondangNo ratings yet
- A Review of Antibiotic Use in Pregnancy: EY OrdsDocument11 pagesA Review of Antibiotic Use in Pregnancy: EY Ordsnoname19191No ratings yet
- Nutrition Guide For Clinicians: From The Physicians Committee For Responsible Medicine / Spring 2007 / Vol. XVI, No. 2Document24 pagesNutrition Guide For Clinicians: From The Physicians Committee For Responsible Medicine / Spring 2007 / Vol. XVI, No. 2mensapertaNo ratings yet
- Issva Classification 2014 Final TrialDocument20 pagesIssva Classification 2014 Final TrialFrancis MunguíaNo ratings yet
- Congenital Talipes Equino-VarusDocument48 pagesCongenital Talipes Equino-VarusKojo DuncanNo ratings yet
- Choanal AtresiaDocument8 pagesChoanal AtresiaCharmila Sari0% (1)
- WhoDocument351 pagesWhozulfina harisyuhraNo ratings yet
- Cornelia de Lange Syndrome - A Recognizable Fetal PhenotypeDocument5 pagesCornelia de Lange Syndrome - A Recognizable Fetal PhenotypeTien Chen TuNo ratings yet
- Chromosomal DisordersDocument4 pagesChromosomal DisordersYoussry JaranillaNo ratings yet
- PRC - ICF - Compilations 2009-2016Document18 pagesPRC - ICF - Compilations 2009-2016Jonas Marvin AnaqueNo ratings yet
- Bahan Kongenital HidungDocument6 pagesBahan Kongenital HidungIta WahyuniNo ratings yet
- whd2016 Brochure en 2Document16 pageswhd2016 Brochure en 2api-311125682No ratings yet
- Common Craniofacial SyndromesDocument126 pagesCommon Craniofacial Syndromesdr parveen bathlaNo ratings yet
- Antidepressants in Pregnancy4 2016Document60 pagesAntidepressants in Pregnancy4 2016هناء همة العلياNo ratings yet
- Intellectual DiabilityDocument10 pagesIntellectual DiabilityAngelo PapimNo ratings yet
- RubelaDocument11 pagesRubelaMuhammad YusriNo ratings yet
- Congenital Rubella SyndromeDocument2 pagesCongenital Rubella SyndromeRajiv KabadNo ratings yet
- Prenatal Diagnosis of Penoscrotal Transposition With 2-And 3-Dimensional UltrasonographyDocument5 pagesPrenatal Diagnosis of Penoscrotal Transposition With 2-And 3-Dimensional UltrasonographyIndach ZyadarifnaNo ratings yet
- Teratogen Pregnancy KuliahDocument40 pagesTeratogen Pregnancy KuliahVonny RiskaNo ratings yet
- 104 FullDocument5 pages104 FullSamNo ratings yet
- Preconception Counselling PDFDocument4 pagesPreconception Counselling PDFponekNo ratings yet
- Healthmedicinet Com II 2014 AprDocument328 pagesHealthmedicinet Com II 2014 AprHeal ThmedicinetNo ratings yet
- Born To Die. Witchcraft and Infanticide in Baruba CultureDocument18 pagesBorn To Die. Witchcraft and Infanticide in Baruba CultureIñaki RegueraNo ratings yet
- TorchDocument6 pagesTorchMary Jean HernaniNo ratings yet
- Atresia EsofagusDocument7 pagesAtresia EsofagusTommysNo ratings yet
- Neonatal Oral MotorDocument5 pagesNeonatal Oral MotorYessenia DiazNo ratings yet
- Etiology of Congenital ScoliosisDocument3 pagesEtiology of Congenital ScoliosisCrissu CrissNo ratings yet
- MSDS Carbon Monoxidee PDFDocument13 pagesMSDS Carbon Monoxidee PDFkarthikeyanNo ratings yet
- Congenital HypothyroidismDocument2 pagesCongenital Hypothyroidismapi-321672273No ratings yet
- Apert SyndromeDocument9 pagesApert SyndromeRiyan BudianorNo ratings yet