Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
3K views1 Ineffective Peripheral Tissue Perfusion
1 Ineffective Peripheral Tissue Perfusion
Uploaded by
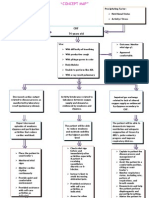
jean_fabula1. The patient was experiencing dyspnea, palpitations, and chest pain due to ineffective cardiopulmonary tissue perfusion caused by impaired oxygen transport.
2. Nursing interventions included encouraging rest, monitoring vital signs, positioning the patient, and promoting deep breathing exercises to help relieve symptoms and improve oxygenation.
3. After 3 hours, the goals of relieving dyspnea without accessory muscle use, decreasing chest pain, and stabilizing vital signs were partially met, as demonstrated by the patient's improved breathing and decreased chest pain.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You might also like
- Autonomic Nervous System Drugs Simple Complement Type QuestionsDocument11 pagesAutonomic Nervous System Drugs Simple Complement Type QuestionsIrina Panciu Stefan100% (1)
- Concept Map - Abby !Document2 pagesConcept Map - Abby !Abegail Abaygar100% (3)
- NCP Cavernous Sinus ThrombosisDocument3 pagesNCP Cavernous Sinus ThrombosisVencel Mae Famas Villahermosa50% (2)
- NCP BronchopneumoniaDocument8 pagesNCP BronchopneumoniaCrisantaCasliNo ratings yet
- Internal Medicine McqsDocument15 pagesInternal Medicine Mcqsunlimited world100% (2)
- Ucm 499295 PDFDocument58 pagesUcm 499295 PDFThea Margareth MartinezNo ratings yet
- Ineffective Cerebral Tissue Perfusion Related ToDocument7 pagesIneffective Cerebral Tissue Perfusion Related TohannahNo ratings yet
- Assessment Diagnosis Planning Implementation Rationale EvaluationDocument14 pagesAssessment Diagnosis Planning Implementation Rationale EvaluationJennifer ArdeNo ratings yet
- Intussusception: PathophysiologyDocument8 pagesIntussusception: PathophysiologyNaufal AndaluNo ratings yet
- Acute PyelonephritisDocument9 pagesAcute Pyelonephritistaekado-1No ratings yet
- Hydrocephalus NCP - DayanghirangDocument2 pagesHydrocephalus NCP - DayanghirangEdnar DayanghirangNo ratings yet
- Potts DiseaseDocument8 pagesPotts Diseaseaimeeros0% (2)
- Ineffective Tissue Perfusion Secondary To Cellulitis DM Type 2Document3 pagesIneffective Tissue Perfusion Secondary To Cellulitis DM Type 2MichaelaKatrinaTrinidadNo ratings yet
- Papillary Thyroid Ca: Group. 1 B Grand CaseDocument16 pagesPapillary Thyroid Ca: Group. 1 B Grand CaseAdora Dela CruzNo ratings yet
- Burns - Skin Integrity, ImpairedDocument2 pagesBurns - Skin Integrity, Impairedmakyofrancis20No ratings yet
- Growth and DevelopmentDocument5 pagesGrowth and DevelopmentGabrielLopezNo ratings yet
- Assessment Diagnosis Planning Implementation Rationale EvaluationDocument3 pagesAssessment Diagnosis Planning Implementation Rationale EvaluationHanz AlecNo ratings yet
- 4th Yr. Med Cardio Module Question - Copy-1Document11 pages4th Yr. Med Cardio Module Question - Copy-1Sheda BondNo ratings yet
- Cues Nursing Diagnosis Scientific Rationale Objectives Nursing Interventions Rationale EvaluationDocument8 pagesCues Nursing Diagnosis Scientific Rationale Objectives Nursing Interventions Rationale EvaluationMa Virginia Nathalia CreerNo ratings yet
- Dave Jay S. Manriquez RN. Acute CholecystitisDocument11 pagesDave Jay S. Manriquez RN. Acute CholecystitisChilleMaeNo ratings yet
- Impaired Gas Exchange NCPDocument3 pagesImpaired Gas Exchange NCPRomel BaliliNo ratings yet
- Risk For InfectionDocument1 pageRisk For InfectionEuanne OrellanoNo ratings yet
- Rheumatic Heart DiseaseDocument13 pagesRheumatic Heart Diseasedy15No ratings yet
- PeritonitisDocument6 pagesPeritonitisDiane ArgoteNo ratings yet
- Suppositories: Abenol (CAN)Document2 pagesSuppositories: Abenol (CAN)Mikko McDonie VeloriaNo ratings yet
- Nursing Care Plan On Platelet DisordersDocument8 pagesNursing Care Plan On Platelet DisordersbhavanaNo ratings yet
- Ariane NCP 1Document2 pagesAriane NCP 1Kristian Ray EraulaNo ratings yet
- Code Green Introduction Reviewer - RedDocument4 pagesCode Green Introduction Reviewer - RedJamieNo ratings yet
- NCPDocument2 pagesNCPMelissa David100% (1)
- Kez NCPDocument12 pagesKez NCPShizuka Marycris AmaneNo ratings yet
- Nursing DiagnosisDocument3 pagesNursing DiagnosislesternNo ratings yet
- Evidence-Based Nursing: I. Clinical QuestionDocument4 pagesEvidence-Based Nursing: I. Clinical QuestionRay Jorge MarmetoNo ratings yet
- Ineffective Airway ClearanceDocument1 pageIneffective Airway ClearanceChristineAlaNo ratings yet
- NCPDocument2 pagesNCPNichole Audrey SaavedraNo ratings yet
- Nursing Care PlanDocument2 pagesNursing Care Planusama_salaymehNo ratings yet
- Anxiety NCPDocument2 pagesAnxiety NCPmitzi019No ratings yet
- Coma - Types, Causes, Treatments, PrognosisDocument3 pagesComa - Types, Causes, Treatments, PrognosisgcsNo ratings yet
- Cerebrovascular DiseaseDocument4 pagesCerebrovascular DiseasekathyfacaNo ratings yet
- Nursing Care Plan: Acute Pain Related To Inflammatory Response Secondary To InfectionDocument2 pagesNursing Care Plan: Acute Pain Related To Inflammatory Response Secondary To InfectionTammy De GuzmanNo ratings yet
- NCP of CavDocument3 pagesNCP of CavHenry Roque TagalagNo ratings yet
- Fluid Volume Deficit Nursing ManagementDocument5 pagesFluid Volume Deficit Nursing ManagementA.No ratings yet
- Scribd 020922 Case Study-Oncology A&kDocument2 pagesScribd 020922 Case Study-Oncology A&kKellie DNo ratings yet
- 5 - Respiratory AssessmentDocument61 pages5 - Respiratory AssessmentAbboud Ali100% (1)
- NCPDocument6 pagesNCPBon BonNo ratings yet
- Levemir Product Insert PDFDocument11 pagesLevemir Product Insert PDFDegee O. GonzalesNo ratings yet
- Acute TonsillopharyngitisDocument17 pagesAcute TonsillopharyngitisRachel Haide NaravalNo ratings yet
- Hydronephrosis Fred LuceDocument69 pagesHydronephrosis Fred LuceKMNo ratings yet
- Nursing AssessmentDocument3 pagesNursing AssessmentJanine PelayoNo ratings yet
- Head To Toe Assessment (Elder)Document2 pagesHead To Toe Assessment (Elder)ZnarfNo ratings yet
- NCPDocument3 pagesNCPchesca_paunganNo ratings yet
- Nursing Care Plans For Activity IntoleranceDocument4 pagesNursing Care Plans For Activity IntolerancethebigtwirpNo ratings yet
- Acute TonsillopharyngitisDocument39 pagesAcute TonsillopharyngitisCin AtianzarNo ratings yet
- Amoebiasis Case StudyDocument12 pagesAmoebiasis Case StudyGrace NazarenoNo ratings yet
- Nursing Physical AssessmentDocument5 pagesNursing Physical AssessmentApril Louise PaluganNo ratings yet
- FluidDocument45 pagesFluidloglesb1No ratings yet
- Pain NCP BillrothDocument2 pagesPain NCP BillrotharjayNo ratings yet
- MGH 8 - Ihd - NCPDocument12 pagesMGH 8 - Ihd - NCPSesinando Niez Quilao Jr.100% (1)
- 10 1056@NEJMcpc1913468 PDFDocument10 pages10 1056@NEJMcpc1913468 PDFAbdelkader HociniNo ratings yet
- PleuritisDocument8 pagesPleuritisshielamaygo05No ratings yet
- The Ride of Your Life: What I Learned about God, Love, and Adventure by Teaching My Son to Ride a BikeFrom EverandThe Ride of Your Life: What I Learned about God, Love, and Adventure by Teaching My Son to Ride a BikeRating: 4.5 out of 5 stars4.5/5 (2)
- Ventricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandVentricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- Community Acquired Pneumonia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandCommunity Acquired Pneumonia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Neumonía Adquirida en La Comunidad en Niños - Tratamiento Ambulatorio - UpToDateDocument32 pagesNeumonía Adquirida en La Comunidad en Niños - Tratamiento Ambulatorio - UpToDatepao.pearanda1998No ratings yet
- Care ReportDocument23 pagesCare ReportSindi Muthiah UtamiNo ratings yet
- Clinical Parasitology: 1. Direct Fecal Smear (DFS)Document3 pagesClinical Parasitology: 1. Direct Fecal Smear (DFS)Monique Eloise GualizaNo ratings yet
- Balbir Singh CPDocument31 pagesBalbir Singh CPAyushiNo ratings yet
- Necrotizing Soft Tissue InfectionsDocument29 pagesNecrotizing Soft Tissue InfectionsMoritz SolivenNo ratings yet
- Column A Column B: Science 4Document3 pagesColumn A Column B: Science 4Velez Jhong-jhongNo ratings yet
- TICKLER-PRINT-2 Pedia PDFDocument7 pagesTICKLER-PRINT-2 Pedia PDFCarlos H. AcuñaNo ratings yet
- CHN Ncm112b Rle RequirementDocument27 pagesCHN Ncm112b Rle RequirementPatricia VasquezNo ratings yet
- 03 - Nature of DiseasesDocument11 pages03 - Nature of DiseasesFrancis ValdezNo ratings yet
- STEMI Care Reperfusions Trategy - DR Eka GinanjarDocument39 pagesSTEMI Care Reperfusions Trategy - DR Eka GinanjarIra MashadiNo ratings yet
- The Role of Vitamin D in Athletic PerformanceDocument3 pagesThe Role of Vitamin D in Athletic PerformanceLeighton SmithNo ratings yet
- Robertson2013 PDFDocument88 pagesRobertson2013 PDFArini NurlelaNo ratings yet
- History Taking: Ma. Sheila Blossom B. Bo RM, RN, MmeDocument14 pagesHistory Taking: Ma. Sheila Blossom B. Bo RM, RN, Mmejhayrus pletaNo ratings yet
- Anxiety NCPDocument2 pagesAnxiety NCPkuro hanabusaNo ratings yet
- Chinese English Regularly Used Medical Terms PDFDocument10 pagesChinese English Regularly Used Medical Terms PDFBlogger28No ratings yet
- Vaccination 710428115244Document1 pageVaccination 710428115244arleesyaNo ratings yet
- E341 FullDocument7 pagesE341 FullwaribisalaNo ratings yet
- Private Hospitals Act 1971 (Act 43)Document14 pagesPrivate Hospitals Act 1971 (Act 43)Adam Haida & CoNo ratings yet
- Gen Bio 2 LAW Q4 Week 3 4 (AutoRecovered)Document12 pagesGen Bio 2 LAW Q4 Week 3 4 (AutoRecovered)Samantha DomileNo ratings yet
- DDX of RIF Mass (Syazwani)Document44 pagesDDX of RIF Mass (Syazwani)Nurul Syazwani RamliNo ratings yet
- Infographic: How You Can Die Running A MarathonDocument1 pageInfographic: How You Can Die Running A MarathonedsunonlineNo ratings yet
- The Bariatric Patient in SurgeryDocument46 pagesThe Bariatric Patient in SurgeryAlex PiecesNo ratings yet
- AUBF LAB - Exams and QuizzesDocument18 pagesAUBF LAB - Exams and QuizzesLUALHATI VILLASNo ratings yet
- Condylar HyperplasiaDocument20 pagesCondylar HyperplasiaSamuel Flores CalderonNo ratings yet
- Brochure ECAICC 2024Document2 pagesBrochure ECAICC 2024أسعد حسنانNo ratings yet
- High-Flow Nasal Cannula-Protocol For Initiation, Titration and WeaningDocument3 pagesHigh-Flow Nasal Cannula-Protocol For Initiation, Titration and WeaningMahmoud khedrNo ratings yet
- Tall StatureDocument24 pagesTall StaturedianmutiaNo ratings yet
1 Ineffective Peripheral Tissue Perfusion
1 Ineffective Peripheral Tissue Perfusion
Uploaded by
jean_fabula0 ratings0% found this document useful (0 votes)
3K views1 page1. The patient was experiencing dyspnea, palpitations, and chest pain due to ineffective cardiopulmonary tissue perfusion caused by impaired oxygen transport.
2. Nursing interventions included encouraging rest, monitoring vital signs, positioning the patient, and promoting deep breathing exercises to help relieve symptoms and improve oxygenation.
3. After 3 hours, the goals of relieving dyspnea without accessory muscle use, decreasing chest pain, and stabilizing vital signs were partially met, as demonstrated by the patient's improved breathing and decreased chest pain.
Original Description:
Copyright
© Attribution Non-Commercial (BY-NC)
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document1. The patient was experiencing dyspnea, palpitations, and chest pain due to ineffective cardiopulmonary tissue perfusion caused by impaired oxygen transport.
2. Nursing interventions included encouraging rest, monitoring vital signs, positioning the patient, and promoting deep breathing exercises to help relieve symptoms and improve oxygenation.
3. After 3 hours, the goals of relieving dyspnea without accessory muscle use, decreasing chest pain, and stabilizing vital signs were partially met, as demonstrated by the patient's improved breathing and decreased chest pain.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
3K views1 page1 Ineffective Peripheral Tissue Perfusion
1 Ineffective Peripheral Tissue Perfusion
Uploaded by
jean_fabula1. The patient was experiencing dyspnea, palpitations, and chest pain due to ineffective cardiopulmonary tissue perfusion caused by impaired oxygen transport.
2. Nursing interventions included encouraging rest, monitoring vital signs, positioning the patient, and promoting deep breathing exercises to help relieve symptoms and improve oxygenation.
3. After 3 hours, the goals of relieving dyspnea without accessory muscle use, decreasing chest pain, and stabilizing vital signs were partially met, as demonstrated by the patient's improved breathing and decreased chest pain.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 1
1.
Ineffective Cardiopulmonary Tissue Perfusion
Assessment Nursing Diagnosis Rationale Goals & Objectives Nursing Rationale Evaluation
Interventions
Subjective: Ineffective If the heart and lungs are After 30 minutes of >Encourage quiet, *To conserve energy After 3 hrs of nursing
>Report of dyspnea even Cardiopulmonary Tissue congested, there would nursing intervention, restful and peaceful & ↓ body tissue O2 intervention, the goal
at rest Perfusion secondary to be excess fluid in these these should manifest: environment demand. was partially met as
>Palpitation impaired transport of mentioned areas. If manifested by:
>Chest pain at 6/10 pain oxygen there’s an excess fluid >Relief of dyspnea >Inform client to *It increases cardiac
scale
or blood, they will without the use of avoid activities; like, workload >Relief from dyspnea
Objective: (NANDA, 2009) compete for accessory muscles straining at stool and breathing
>Use of accessory oxygenation in the lungs >↓ Chest Pain Scale normally without the
muscles when breathing resulting to from 6 to 1-4/10 >Always monitor the *Hypertension can use of accessory
>Poor capillary refill unoxygenated blood; >Skin normal in color blood pressure damage blood vessel muscles
(>5s) thus impairing the >have a stable vital & organ function >Chest Pain scale of
>Pale skin transport of oxygen for signs of BP=100/70- >Encourage use of *To decrease tension 4/10
>Pale mucous membrane the perfusion of body 140/80mmHg relaxation techniques level >Skin pale in color
>↓Hgb of 139 g/L tissues and cells. PR=60-100bpm >Vital Signs of
>Hct of 0.42 Unoxygenated blood RR=12-20cpm >Position patient in *To promote optimal 130/80mmHg,
>041510: 2-D Echo result won’t be able to perfuse semi to high fowler’s lung expansion & 93bpm and 18 cpm
shows Mild Tricuspid
the heart and lung tissue position decreases cardiac
Regurgitation and
impaired diastrolic workload
relaxation of Left (Brunner and Suddhart’s
ventricle Medical-Surgical >Encourage deep *To promote lung
>RR of 23cpm Nursing) breathing exercises expansion
PR of 104bpm
BP of 150/100mmHg
You might also like
- Autonomic Nervous System Drugs Simple Complement Type QuestionsDocument11 pagesAutonomic Nervous System Drugs Simple Complement Type QuestionsIrina Panciu Stefan100% (1)
- Concept Map - Abby !Document2 pagesConcept Map - Abby !Abegail Abaygar100% (3)
- NCP Cavernous Sinus ThrombosisDocument3 pagesNCP Cavernous Sinus ThrombosisVencel Mae Famas Villahermosa50% (2)
- NCP BronchopneumoniaDocument8 pagesNCP BronchopneumoniaCrisantaCasliNo ratings yet
- Internal Medicine McqsDocument15 pagesInternal Medicine Mcqsunlimited world100% (2)
- Ucm 499295 PDFDocument58 pagesUcm 499295 PDFThea Margareth MartinezNo ratings yet
- Ineffective Cerebral Tissue Perfusion Related ToDocument7 pagesIneffective Cerebral Tissue Perfusion Related TohannahNo ratings yet
- Assessment Diagnosis Planning Implementation Rationale EvaluationDocument14 pagesAssessment Diagnosis Planning Implementation Rationale EvaluationJennifer ArdeNo ratings yet
- Intussusception: PathophysiologyDocument8 pagesIntussusception: PathophysiologyNaufal AndaluNo ratings yet
- Acute PyelonephritisDocument9 pagesAcute Pyelonephritistaekado-1No ratings yet
- Hydrocephalus NCP - DayanghirangDocument2 pagesHydrocephalus NCP - DayanghirangEdnar DayanghirangNo ratings yet
- Potts DiseaseDocument8 pagesPotts Diseaseaimeeros0% (2)
- Ineffective Tissue Perfusion Secondary To Cellulitis DM Type 2Document3 pagesIneffective Tissue Perfusion Secondary To Cellulitis DM Type 2MichaelaKatrinaTrinidadNo ratings yet
- Papillary Thyroid Ca: Group. 1 B Grand CaseDocument16 pagesPapillary Thyroid Ca: Group. 1 B Grand CaseAdora Dela CruzNo ratings yet
- Burns - Skin Integrity, ImpairedDocument2 pagesBurns - Skin Integrity, Impairedmakyofrancis20No ratings yet
- Growth and DevelopmentDocument5 pagesGrowth and DevelopmentGabrielLopezNo ratings yet
- Assessment Diagnosis Planning Implementation Rationale EvaluationDocument3 pagesAssessment Diagnosis Planning Implementation Rationale EvaluationHanz AlecNo ratings yet
- 4th Yr. Med Cardio Module Question - Copy-1Document11 pages4th Yr. Med Cardio Module Question - Copy-1Sheda BondNo ratings yet
- Cues Nursing Diagnosis Scientific Rationale Objectives Nursing Interventions Rationale EvaluationDocument8 pagesCues Nursing Diagnosis Scientific Rationale Objectives Nursing Interventions Rationale EvaluationMa Virginia Nathalia CreerNo ratings yet
- Dave Jay S. Manriquez RN. Acute CholecystitisDocument11 pagesDave Jay S. Manriquez RN. Acute CholecystitisChilleMaeNo ratings yet
- Impaired Gas Exchange NCPDocument3 pagesImpaired Gas Exchange NCPRomel BaliliNo ratings yet
- Risk For InfectionDocument1 pageRisk For InfectionEuanne OrellanoNo ratings yet
- Rheumatic Heart DiseaseDocument13 pagesRheumatic Heart Diseasedy15No ratings yet
- PeritonitisDocument6 pagesPeritonitisDiane ArgoteNo ratings yet
- Suppositories: Abenol (CAN)Document2 pagesSuppositories: Abenol (CAN)Mikko McDonie VeloriaNo ratings yet
- Nursing Care Plan On Platelet DisordersDocument8 pagesNursing Care Plan On Platelet DisordersbhavanaNo ratings yet
- Ariane NCP 1Document2 pagesAriane NCP 1Kristian Ray EraulaNo ratings yet
- Code Green Introduction Reviewer - RedDocument4 pagesCode Green Introduction Reviewer - RedJamieNo ratings yet
- NCPDocument2 pagesNCPMelissa David100% (1)
- Kez NCPDocument12 pagesKez NCPShizuka Marycris AmaneNo ratings yet
- Nursing DiagnosisDocument3 pagesNursing DiagnosislesternNo ratings yet
- Evidence-Based Nursing: I. Clinical QuestionDocument4 pagesEvidence-Based Nursing: I. Clinical QuestionRay Jorge MarmetoNo ratings yet
- Ineffective Airway ClearanceDocument1 pageIneffective Airway ClearanceChristineAlaNo ratings yet
- NCPDocument2 pagesNCPNichole Audrey SaavedraNo ratings yet
- Nursing Care PlanDocument2 pagesNursing Care Planusama_salaymehNo ratings yet
- Anxiety NCPDocument2 pagesAnxiety NCPmitzi019No ratings yet
- Coma - Types, Causes, Treatments, PrognosisDocument3 pagesComa - Types, Causes, Treatments, PrognosisgcsNo ratings yet
- Cerebrovascular DiseaseDocument4 pagesCerebrovascular DiseasekathyfacaNo ratings yet
- Nursing Care Plan: Acute Pain Related To Inflammatory Response Secondary To InfectionDocument2 pagesNursing Care Plan: Acute Pain Related To Inflammatory Response Secondary To InfectionTammy De GuzmanNo ratings yet
- NCP of CavDocument3 pagesNCP of CavHenry Roque TagalagNo ratings yet
- Fluid Volume Deficit Nursing ManagementDocument5 pagesFluid Volume Deficit Nursing ManagementA.No ratings yet
- Scribd 020922 Case Study-Oncology A&kDocument2 pagesScribd 020922 Case Study-Oncology A&kKellie DNo ratings yet
- 5 - Respiratory AssessmentDocument61 pages5 - Respiratory AssessmentAbboud Ali100% (1)
- NCPDocument6 pagesNCPBon BonNo ratings yet
- Levemir Product Insert PDFDocument11 pagesLevemir Product Insert PDFDegee O. GonzalesNo ratings yet
- Acute TonsillopharyngitisDocument17 pagesAcute TonsillopharyngitisRachel Haide NaravalNo ratings yet
- Hydronephrosis Fred LuceDocument69 pagesHydronephrosis Fred LuceKMNo ratings yet
- Nursing AssessmentDocument3 pagesNursing AssessmentJanine PelayoNo ratings yet
- Head To Toe Assessment (Elder)Document2 pagesHead To Toe Assessment (Elder)ZnarfNo ratings yet
- NCPDocument3 pagesNCPchesca_paunganNo ratings yet
- Nursing Care Plans For Activity IntoleranceDocument4 pagesNursing Care Plans For Activity IntolerancethebigtwirpNo ratings yet
- Acute TonsillopharyngitisDocument39 pagesAcute TonsillopharyngitisCin AtianzarNo ratings yet
- Amoebiasis Case StudyDocument12 pagesAmoebiasis Case StudyGrace NazarenoNo ratings yet
- Nursing Physical AssessmentDocument5 pagesNursing Physical AssessmentApril Louise PaluganNo ratings yet
- FluidDocument45 pagesFluidloglesb1No ratings yet
- Pain NCP BillrothDocument2 pagesPain NCP BillrotharjayNo ratings yet
- MGH 8 - Ihd - NCPDocument12 pagesMGH 8 - Ihd - NCPSesinando Niez Quilao Jr.100% (1)
- 10 1056@NEJMcpc1913468 PDFDocument10 pages10 1056@NEJMcpc1913468 PDFAbdelkader HociniNo ratings yet
- PleuritisDocument8 pagesPleuritisshielamaygo05No ratings yet
- The Ride of Your Life: What I Learned about God, Love, and Adventure by Teaching My Son to Ride a BikeFrom EverandThe Ride of Your Life: What I Learned about God, Love, and Adventure by Teaching My Son to Ride a BikeRating: 4.5 out of 5 stars4.5/5 (2)
- Ventricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandVentricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- Community Acquired Pneumonia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandCommunity Acquired Pneumonia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Neumonía Adquirida en La Comunidad en Niños - Tratamiento Ambulatorio - UpToDateDocument32 pagesNeumonía Adquirida en La Comunidad en Niños - Tratamiento Ambulatorio - UpToDatepao.pearanda1998No ratings yet
- Care ReportDocument23 pagesCare ReportSindi Muthiah UtamiNo ratings yet
- Clinical Parasitology: 1. Direct Fecal Smear (DFS)Document3 pagesClinical Parasitology: 1. Direct Fecal Smear (DFS)Monique Eloise GualizaNo ratings yet
- Balbir Singh CPDocument31 pagesBalbir Singh CPAyushiNo ratings yet
- Necrotizing Soft Tissue InfectionsDocument29 pagesNecrotizing Soft Tissue InfectionsMoritz SolivenNo ratings yet
- Column A Column B: Science 4Document3 pagesColumn A Column B: Science 4Velez Jhong-jhongNo ratings yet
- TICKLER-PRINT-2 Pedia PDFDocument7 pagesTICKLER-PRINT-2 Pedia PDFCarlos H. AcuñaNo ratings yet
- CHN Ncm112b Rle RequirementDocument27 pagesCHN Ncm112b Rle RequirementPatricia VasquezNo ratings yet
- 03 - Nature of DiseasesDocument11 pages03 - Nature of DiseasesFrancis ValdezNo ratings yet
- STEMI Care Reperfusions Trategy - DR Eka GinanjarDocument39 pagesSTEMI Care Reperfusions Trategy - DR Eka GinanjarIra MashadiNo ratings yet
- The Role of Vitamin D in Athletic PerformanceDocument3 pagesThe Role of Vitamin D in Athletic PerformanceLeighton SmithNo ratings yet
- Robertson2013 PDFDocument88 pagesRobertson2013 PDFArini NurlelaNo ratings yet
- History Taking: Ma. Sheila Blossom B. Bo RM, RN, MmeDocument14 pagesHistory Taking: Ma. Sheila Blossom B. Bo RM, RN, Mmejhayrus pletaNo ratings yet
- Anxiety NCPDocument2 pagesAnxiety NCPkuro hanabusaNo ratings yet
- Chinese English Regularly Used Medical Terms PDFDocument10 pagesChinese English Regularly Used Medical Terms PDFBlogger28No ratings yet
- Vaccination 710428115244Document1 pageVaccination 710428115244arleesyaNo ratings yet
- E341 FullDocument7 pagesE341 FullwaribisalaNo ratings yet
- Private Hospitals Act 1971 (Act 43)Document14 pagesPrivate Hospitals Act 1971 (Act 43)Adam Haida & CoNo ratings yet
- Gen Bio 2 LAW Q4 Week 3 4 (AutoRecovered)Document12 pagesGen Bio 2 LAW Q4 Week 3 4 (AutoRecovered)Samantha DomileNo ratings yet
- DDX of RIF Mass (Syazwani)Document44 pagesDDX of RIF Mass (Syazwani)Nurul Syazwani RamliNo ratings yet
- Infographic: How You Can Die Running A MarathonDocument1 pageInfographic: How You Can Die Running A MarathonedsunonlineNo ratings yet
- The Bariatric Patient in SurgeryDocument46 pagesThe Bariatric Patient in SurgeryAlex PiecesNo ratings yet
- AUBF LAB - Exams and QuizzesDocument18 pagesAUBF LAB - Exams and QuizzesLUALHATI VILLASNo ratings yet
- Condylar HyperplasiaDocument20 pagesCondylar HyperplasiaSamuel Flores CalderonNo ratings yet
- Brochure ECAICC 2024Document2 pagesBrochure ECAICC 2024أسعد حسنانNo ratings yet
- High-Flow Nasal Cannula-Protocol For Initiation, Titration and WeaningDocument3 pagesHigh-Flow Nasal Cannula-Protocol For Initiation, Titration and WeaningMahmoud khedrNo ratings yet
- Tall StatureDocument24 pagesTall StaturedianmutiaNo ratings yet