Professional Documents
Culture Documents
253 Health Care Claims
253 Health Care Claims
Uploaded by
Rishi VermaOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
253 Health Care Claims
253 Health Care Claims
Uploaded by
Rishi VermaCopyright:
Available Formats
HIPAA EDI Companion Guide
For
837 Institutional and Professional
Health Care Claims
Companion Guide Version: 2.0
ASCX12N National Electronic Data Interchange Transaction Set
Implementation and Addenda Guides, Version 005010A1/A2
INTRODUCTION
This EDI Companion Guide is to be used in conjunction with the ASCX12N 837 Standards for Electronic Data
Interchange Technical Report Type 3 and WebMD/Emdeon Business Services Companion Guides. This guide
defines communication specifications, specific Health Partners Plans business rules and information applicable
to the 837 Institutional (I) and Professional (P) transactions. Health Partners Plans will use and accept
standard code sets on the 837 transactions. Please refer to the HIPAA Implementation Guide for valid code set
values.
Health Partners Plans will receive valid HIPAA X12N 837I & P transactions from WebMD/Emdeon Business
Services and will in turn respond to WebMD/Emdeon Business Services with valid X12N transactions. Contact
your billing software vendor and request that your Health Partners Plans claims and encounters be submitted
through the WebMD/Emdeon Business Services claims clearinghouse. You can also direct your current
clearinghouse to forward your claims to WebMD/Emdeon Business Services.
The following information is intended to serve only as a companion document to the HIPAA X12N 837
Institutional and Professional Standards for electronic data Interchange Technical Report Type 3.
Claims Technical Support (EDI)
Support hours are Monday through Friday
9:00 a.m. to 5:00 p.m. (EST)
1-215-991-4290
The use of this information is solely for the purpose of clarification.
The information in this document is subject to change.
837I&P Companion Guide 005010A1/A2-v2.0 2
Document Control - Version History
The following version history is provided to easily identify updates between Companion Guide versions. Each
update is numbered. All corresponding areas of the document related to this update are also numbered.
Please continue to check the Health Partners Plans website at: http://www.hpplans.com/HIPAA.asp for
the most recent version of this document and other HIPAA related resources.
# Version Date Author Updates
(1) 1.0 10/11 Operations Initial version of the 5010 Companion Guide.
Technical Support This version was also posted to the Health Partners external
website: http://www.healthpart.com/HIPAA.asp
(2) 2.0 10/17/13 Claims Department Added new Plan name and company logo.
This version was also posted to the Health Partners Plans
external website: http://www.hhplans.com/HIPAA.asp
Coding- when submitting J-code the NDC must be included.
837I&P Companion Guide 005010A1/A2-v2.0 3
Section 1 837 Institutional Claims
837I&P Companion Guide 005010A1/A2-v2.0 4
General Requirements for the Electronic Claims Submission Process
(837 Institutional Claims)
This section will address a variety of issues that will facilitate the Institutional Claims Submission Process.
Only loops, segments, and data elements valid for the HIPAA 837 Institutional (005010X223A2)
Technical Report Type 3 will be translated. Deviating from the Technical Report Type 3 Guidelines
and submitting invalid data will cause files to be rejected.
Only one transaction type per transmission.
The delimiters which Health Partners Plans will accept are listed below. The following characters must
not be used within the data content of the 837I:
Data Element = * (Asterisk)
Segment = ~ (Tilde)
Component/Element = < (Less than sign)
No more than 5,000 claims should be submitted by any provider at one time.
WebMD/Emdeon Business Services will perform HIPAA compliance checking for all transactions
received. If the transaction fails compliance checking, a 997 Functional Acknowledgement Reject
will be generated and transmitted to the provider. The provider will be expected to correct the data and
immediately retransmit the transaction.
Rejected claims must be resubmitted within 180 days of the original date of service. (2a)
Negative values submitted in the following fields will not be processed and will result in claim
rejections: Total Claim Charge Amount (2300 Loop, CLM02), Patient Amount Paid (2300 Loop,
AMT02), Other Payer Patient Paid Amount (2320 Loop, AMT02), COB Total Allowed Amount (2320
Loop, AMT02).
We suggest retrieval of the ANSI 997 Functional Acknowledgment files on the first business day after
the claim file is submitted, but no later than five days after the file submission.
Providers submitting claims for Institutional Services should enter their five (5) digit Health Partners
Provider Identification Number in the 2310A REF01 G2 qualifier, as shown in the table 837
Institutional on page 6 of this companion guide.
Health Partners Plans Claims Technical Support is available Monday through Friday, 9:00 a.m. to 5:00
p.m. (EST).
837I&P Companion Guide 005010A1/A2-v2.0 5
ANSI FIELDS FOR SUBMITTER AND PROVIDER VALIDATION
These fields will be required to have the following data:
837 Institutional
Element
Loop
Field Description Length Mapping Comments
0000 ISA05 Interchange ID Qualifier 2/2 ZZ
0000 ISA06 Interchange Sender ID (*) 15/15 133052274
0000 ISA07 Interchange ID Qualifier 2/2 ZZ
0000 ISA08 Interchange Receiver ID 15/15 801420001 (1)
0000 ISA15 Usage Indicator 1/1 MUST USE P FOR PRODUCTION
0000 GS02 Application Senders Code 2/15 133052274
0000 GS03 Application Receivers Code 2/15 801420001 (1)
0000 BHT02 Transaction Set Purpose 2/2 00'
1000A NM102 Entity Type Qualifier 1/1 2
1000A NM103 Organization Name 1/60 EMDEON
1000A NM108 Identification Code Qualifier 1/2 46
1000A NM109 Identification Code 2/80 133052274
1000A PER02 Name 1/60 EMDEON CUSTOMER SOLUTIONS
1000A PER03 Communication Number Qualifier 2/2 TE
1000A PER04 Communication Number 1/256 8008456592
(1)
1000B NM109 Identification Code 2/80 801420001
Billing Entity Identification 1/2
2010AA NM108 XX
Qualifier
2010AA NM109 Billing Entity Identification Code 2/80 USE APPROPRIATE NPI NUMBER
2010AA N3 Billing Provider Address 1/55 PROVIDER BILLING ADDRESS
2/30 INCLUDE CITY, 2-CHARACTER STATE
2010AA N4 Billing Provider City, State, Zip
CODE AND 9-DIGIT ZIP CODE
2010AA REF01 Billing Provider Secondary Identifier 2/3 EI
1/50 PROVIDER TAX IDENTIFICATION
2010AA REF02 Billing provider Secondary Identifier
NUMBER
Pay-To Provider Identification
2010AB NM108 1/2 XX
Qualifier
Pay-To Provider Identification
2010AB NM109 2/80 USE APPROPRIATE NPI NUMBER
Number Code
2010AB N3 Address Information 1/55 ADDRESS INFORMATION
837I&P Companion Guide 005010A1/A2-v2.0 6
Element
Loop
Field Description Length Mapping Comments
INCLUDE CITY, 2-CHARACTER STATE
2010AB N4 City, State Zip Code 2/30
CODE AND 9-DIGIT ZIP CODE
2300 NTE01 Billing Reference Code Text 3/3 ADD
Attending Provider Identification
2310A NM108 1/2 XX
Qualifier
Attending Provider Identification
2310A NM109 2/80 USE APPROPRIATE NPI NUMBER
Code
2310A REF01 Reference Identification Qualifier 2/3 G2
HEALTH PARTNERS PROVIDER
2310A REF02 Reference Identification 1/50
IDENTIFICATION NUMBER (5 DIGITS)
Operating Physician Identification
2310B NM108 1/2 XX
Qualifier
Operating Physician Identification
2310B NM109 2/80 USE APPROPRIATE NPI NUMBER
Code
Other Operating Physician
2310C NM108 1/2 XX
Identification Qualifier
Other Operating Physician
2310C NM109 2/80 USE APPROPRIATE NPI NUMBER
Identification Code
Service Facility Identification
2310E NM108 1/2 XX
Qualifier
2310E NM109 Service Facility Identification Code 2/80 USE APPROPRIATE NPI NUMBER
2310E N3 Service Facility Address 1/55 ADDRESS INFORMATION
INCLUDE CITY, 2-CHARACTER STATE
2310E N4 Geographic Location 2/30
CODE AND 9-DIGIT ZIP CODE
Operating Physician Identification
2420A NM108 1/2 XX
Qualifier
Operating Physician Identification
2420A NM109 2/80 USE APPROPRIATE NPI NUMBER
Code
Other Operating Physician
2420B NM108 1/2 XX
Identification Qualifier
Other Operating Physician
NM109 2/80 USE APPROPRIATE NPI NUMBER
2420B Identification Code
(*)
ISA06 & ISA08 have a required element min/max length of 15 characters. Trailing spaces may be required.
837I&P Companion Guide 005010A1/A2-v2.0 7
General Business Requirements for the 837 Institutional 5010A2 Claims
Submission Process
This subsection will address a variety of issues that will facilitate the Electronic Media Claims Processing
Process for the 837 Institutional (005010X223A2).
Coding
Use most recent ICD-9, CPT, HCPC, and Revenue codes.
Always check for 4th and 5th digit code requirements.
An electronic claim cannot span two (2) separate calendar years. Charges must be filed for the previous
year separately from the current year.
No more than 5,000 claims will be accepted for any provider at one time.
The maximum number of characters to be submitted in the dollar amount field is seven (7) characters.
You may send up to sixteen (16) diagnosis codes per claim; however, the last twelve (12) diagnosis
codes will not be considered in processing.
Member Identifiers
Submitters must use the entire alphanumeric or numeric identification code for the Subscriber Identifier
(Loop 2010BA, NM109), as it appears on the members identification card.
Health Partners Plans (Medicaid) members have a nine (9) digit numeric member ID number
Kidz Partners (CHIP) members have a ten (10) digit numeric member ID number
Health Partners Plans (Medicare) members have a seven (7) digit numeric member ID number
Provider Identifiers
Effective May 23, 2008, Health Partners will accept the following provider identifiers:
NPI Only (2010AA Loop, NM108 with the XX qualifier)
NPI Only (2310B Loop, NM108 with the XX qualifier)
837I&P Companion Guide 005010A1/A2-v2.0 8
Section 2 837 Professional Claims
837I&P Companion Guide 005010A1/A2-v2.0 9
General Requirements for the Electronic Claims Submission Process
(837 Professional Claims)
This section will address a variety of issues that will facilitate the Professional Claims Submission Process.
Only loops, segments, and data elements valid for the HIPAA 837 Professional (005010X222A1)
Technical Report Type 3 will be translated. Deviating from the Technical Report Type 3 and
submitting invalid data will cause files to be rejected.
Only one transaction type per transmission.
The delimiters which Health Partners Plans will accept are listed below. The following characters must
not be used within the data content of the 837P:
Data Element = * (Asterisk)
Segment = ~ (Tilde)
Component/Element = : (Colon)
No more than 5,000 claims should be submitted by any provider at one time.
WebMD/Emdeon Business Services will perform HIPAA compliance checking for all transactions
received. If the transaction fails compliance checking, a 997 Functional Acknowledgement Reject
will be generated and transmitted to the provider. The provider will be expected to correct the data and
immediately retransmit the transaction.
Rejected claims must be resubmitted within 180 days of the original date of service. (2a)
Negative values submitted in the following fields will not be processed and will result in the claim being
rejected: Total Claim Charge Amount (2300 Loop, CLM02), Patient Amount Paid (2300 Loop,
AMT02), Patient Weight (2300 and 2400 Loop, CR102), Transport Distance (2300 and 2400 Loop,
CR106), Payer Paid Amount (2320 Loop, AMT02), Allowed Amount (2320 Loop, AMT02), Line Item
Charge Amount (2400 Loop, SV102), Service Unit Count (2400 Loop, SV104), Total Purchased Service
Amount (2300 Loop, AMT02), and Purchased Service Charge Amount (2400 Loop, PS102).
We suggest retrieval of the ANSI 997 Functional Acknowledgment files on the first business day after
the claim file is submitted, but no later than five days after the file submission.
Health Partners Plans Claims Technical Support is available Monday through Friday, 9:00 a.m. to 5:00
p.m. (EST).
837I&P Companion Guide 005010A1/A2-v2.0 10
ANSI FIELDS FOR SUBMITTER AND PROVIDER VALIDATION
These fields will be required to have the following data:
837 Professional
Element
Loop
Field Description Length Mapping Comments
0000 ISA05 Interchange ID Qualifier 2/2 ZZ
0000 ISA06 Interchange Sender ID (*) 15/15 133052274
0000 ISA07 Interchange ID Qualifier 2/2 ZZ
0000 ISA08 Interchange Receiver ID 15/15 801420001 (1)
0000 ISA15 Usage Indicator 1/1 Must use P for production
0000 GS02 Application Senders Code 2/15 133052274
0000 GS03 Application Receivers Code 2/15 801420001 (1)
0000 BHT02 Transaction Set Purpose 2/2 00'
1000A NM102 Entity Type Qualifier 1/1 2
1000A NM103 Organization Name 1/60 EMDEON
1000A NM108 Identification Code Qualifier 1/2 46
1000A NM109 Identification Code 2/80 133052274
1000A PER02 Name 1/60 EMDEON CUSTOMER SOLUTIONS
1000A PER03 Communication Number Qualifier 2/2 TE
1000A PER04 Communication Number 1/256 8008456592
(1)
1000B NM109 Identification Code 2/80 801420001
Billing Provider Identification Code 1/2
2010AA NM108 XX
Qualifier
2010AA NM109 Billing Provider Identification Code 2/80 USE APPROPRIATE NPI NUMBER
2010AA N3 Address Information 1/55 ADDRESS INFORMATION
2/30 INCLUDE CITY, 2-CHARACTER STATE
2010AA N4 Geographic Location
CODE AND 9-DIGIT ZIP CODE
Billing Provider Reference 2/3
2010AA REF01 EI
Identification Qualifier
2010AA REF02 Billing Provider Secondary Identifier 1/50 TAX IDENTIFICATION NUMBER
2010AB N3 Address Information 1/55 ADDRESS INFORMATION
INCLUDE CITY, 2-CHARACTER STATE
2010AB N4 Geographic Location 2/30
CODE AND 9-DIGIT ZIP CODE
2000B PAT09 Pregnancy Indicator 1/1 Y
2300 NTE01 Claim Note Reference Code 3/3 ADD
837I&P Companion Guide 005010A1/A2-v2.0 11
Element
Loop
Field Description Length Mapping Comments
2300 NTE02 Description (Note Text) 1/80 VC11
Referring Physician Identification
2310A NM108 1/2 XX
Code Qualifier
Referring Physician Identification
2310A NM109 2/80 USE APPROPRIATE NPI NUMBER
Code
Rendering Physician Identification
2310B NM108 1/2 XX
Code Qualifier
Rendering Physician Identification
2310B NM109 2/80 USE APPROPRIATE NPI NUMBER
Code
Service Facility Location
2310C NM108 1/2 XX
Identification Code Qualifier
Service Facility Location
2310C NM109 2/80 USE APPROPRIATE NPI NUMBER
Identification Code
Supervising Provider Name
2310D NM108 1/ 2 XX
Identification Code Qualifier
Supervising Provider Name
2310D NM109 2/80 USE APPROPIATE NPI NUMBER
Identification Code
Rendering Provider Identification
2420A NM108 1/2 XX
Code Qualifier
Rendering Provider Identification
2420A NM109 2/80 USE APPROPRIATE NPI NUMBER
Code
Purchased Service Provider
2420B NM108 1/2 XX
Identification Code Qualifier
Purchased Service Provider
2420B NM109 2/80 USE APPROPRIATE NPI NUMBER
Identification Code Qualifier
(*)
ISA06 & ISA08 have a required element min/max length of 15 characters. Trailing spaces may be required.
837I&P Companion Guide 005010A1/A2-v2.0 12
General Business Requirements for the 837 Professional 4010A1 Claims
Submission Process
This section will address a variety of issues that will facilitate the Electronic Claims Processing for 837
Professional (005010X222A1).
Anesthesia Billing
All claims reporting the administration of anesthesia must include all of the following items :
1. The appropriate anesthesia procedure code (00100 - 01999)
2. Anesthesia time units: Payment for anesthesia claims will be based on the anesthesia units not
anesthesia minutes.
3. The appropriate anesthesia modifier to identify who rendered the service
All anesthesia time should be submitted with the primary anesthesia code. Time units are determined
on the basis of one time unit for each fifteen (15) minutes of anesthesia.
Do not report base units on your claim submissions. Health Partners Plans processing system will
automatically determine the base units based on the reported procedure code and modifiers.
Additional information is in the Health Partners Plans Anesthesia Billing Guide available through the
Health Partners Plans website at http://www.hhplans.com
Coding
Use most recent ICD-9, CPT, and HCPCS codes.
Health Partner Plans does not accept the use of National Drug Codes (NDC) by non-retail pharmacies.
J-Code submissions are required unless otherwise specified in provider contract. Providers are required
to include the National Drug Codes (NDC) when submitting a J-Code.
Always check for 4th and 5th digit code requirements.
837I&P Companion Guide 005010A1/A2-v2.0 13
General Business Requirements for the 837 Professional 4010A1 Claims
Submission Process Contd
An electronic claim cannot span two (2) separate calendar years. Charges must be filed for the previous
year separately from the current year.
It is possible to bill $0.00 charge lines on professional claims.
You may send up to four modifiers; however, the last two modifiers will not be considered for claims
processing.
Member Identifiers
Submitters must use the entire alphanumeric or numeric identification code for the Subscriber Identifier
(Loop 2010BA, NM109), as it appears on the members identification card.
Health Partners Plans (Medicaid) members have a nine (9) digit numeric member ID number
Kidz Partners (CHIP) members have a ten (10) digit numeric member ID number
Health Partners Plans (Medicare) members have a seven (7) digit numeric member ID number
Provider Identifiers
Effective May 23, 2008, Health Partners Plans will accept the following provider identifiers:
NPI Only (2310B Loop, NM108 with the XX qualifier)
NPI Only (2310B Loop, NM108 with the XX qualifier)
837I&P Companion Guide 005010A1/A2-v2.0 14
You might also like
- Berges Level 2 Book PDFDocument80 pagesBerges Level 2 Book PDFYulia Larin100% (1)
- Epic Integration GuideDocument28 pagesEpic Integration GuideAtiq TahirNo ratings yet
- ERP DBChangesDocument745 pagesERP DBChangesluiz.teixeira50% (2)
- Case Study of The Change Management of British Airways After The Economic Crisis of 2008Document5 pagesCase Study of The Change Management of British Airways After The Economic Crisis of 2008Mirela-Elena Popa0% (1)
- How To Remove Pending and Error Receiving Transactions From Transaction Status Summary (Doc ID 303544.1)Document6 pagesHow To Remove Pending and Error Receiving Transactions From Transaction Status Summary (Doc ID 303544.1)Jefferson Gomes de Arruda100% (1)
- Sample Healthcare Qa Analyst ResumeDocument4 pagesSample Healthcare Qa Analyst ResumeManish1580No ratings yet
- Infor Cloverleaf Integration Suite Tackles Healthcare Integration Challenges Simplifies Health Information Exchange PDFDocument1 pageInfor Cloverleaf Integration Suite Tackles Healthcare Integration Challenges Simplifies Health Information Exchange PDFSpit FireNo ratings yet
- GEHC-Gateway Project Implementation Guide PDFDocument30 pagesGEHC-Gateway Project Implementation Guide PDFpreeti dNo ratings yet
- 834 Companion GuideDocument64 pages834 Companion GuiderickyrockaNo ratings yet
- 9th Annual Litigation Trends Survey Findings 2013 Fulbright ForumDocument60 pages9th Annual Litigation Trends Survey Findings 2013 Fulbright ForumchrispittmanNo ratings yet
- Resulting Trust Essay PlanDocument3 pagesResulting Trust Essay PlanSebastian Toh Ming WeiNo ratings yet
- Shocking Psychological Studies and The Lessons They TeachDocument99 pagesShocking Psychological Studies and The Lessons They TeachArun Sharma100% (1)
- Slaying The DragonDocument5 pagesSlaying The DragonMarkus ChNo ratings yet
- Lab01 RDi IntroDocument36 pagesLab01 RDi IntroskumarguptaNo ratings yet
- HIS Lesson 4. Health Information SystemsDocument29 pagesHIS Lesson 4. Health Information SystemsJannela EscomiendoNo ratings yet
- DICOM Basics - Part 1: Connectivity OverviewDocument27 pagesDICOM Basics - Part 1: Connectivity OverviewPacientes PruebaNo ratings yet
- JD Edwards World Product Costing and Manufacturing Accounting A91 GuideDocument306 pagesJD Edwards World Product Costing and Manufacturing Accounting A91 Guide'Emraan Tahir'100% (1)
- Iseries Application DevelopmentDocument64 pagesIseries Application DevelopmentRamana VaralaNo ratings yet
- AS400 Basics ManualDocument16 pagesAS400 Basics ManualNarin RattanakulNo ratings yet
- Introduction To Websphere MQDocument31 pagesIntroduction To Websphere MQchirutha84No ratings yet
- Fhir in Json LDDocument57 pagesFhir in Json LDmauriciovilleNo ratings yet
- Technical QuestionDocument6 pagesTechnical QuestionSandeep BurmanNo ratings yet
- 4 Healthmapper Extension ART PDFDocument38 pages4 Healthmapper Extension ART PDFTobitusinNo ratings yet
- EDI Notepad GuideDocument40 pagesEDI Notepad GuideKashif AminNo ratings yet
- Guardian Programming Ref For CDocument344 pagesGuardian Programming Ref For CdeepaksaneNo ratings yet
- What Are The Types of Data AreasDocument3 pagesWhat Are The Types of Data Areasbalaas400No ratings yet
- Mirth Connect-1Document6 pagesMirth Connect-1Francisca Yañez SanhuezaNo ratings yet
- IBM I Database Embedded SQL Programming 7.1 - RzajpDocument202 pagesIBM I Database Embedded SQL Programming 7.1 - Rzajpgiuseppe.manara2029No ratings yet
- 1 What Is HL7?: Health Level Seven (HL7) Is A Standard Series of Predefined Logical Formats For PackagingDocument3 pages1 What Is HL7?: Health Level Seven (HL7) Is A Standard Series of Predefined Logical Formats For PackagingpvenkatkrishnaNo ratings yet
- C QuestnDocument14 pagesC Questnkishanlal7No ratings yet
- Programma Mirth Connect 3 TrainingDocument3 pagesProgramma Mirth Connect 3 TraininggpmarquesNo ratings yet
- SI52 Mailbox BookDocument48 pagesSI52 Mailbox BookabhishekNo ratings yet
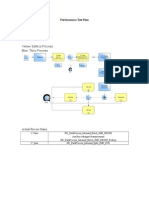
- Performance Test Plan: Yellow: Edifecs Process Blue: Tibco ProcessDocument2 pagesPerformance Test Plan: Yellow: Edifecs Process Blue: Tibco ProcessVaraprasada Rao ImandiNo ratings yet
- RDi Snippets (IBM Rational Developer For I)Document3 pagesRDi Snippets (IBM Rational Developer For I)Andreas Steding0% (1)
- Errori - Pathsend - Pathway-ServerClassSendDocument252 pagesErrori - Pathsend - Pathway-ServerClassSendHedgehog81No ratings yet
- CDocument32 pagesCAniket ShirkeNo ratings yet
- Xengine Transaction ValidationDocument12 pagesXengine Transaction ValidationMitchell JohnsonNo ratings yet
- C and Data Structures Q and ADocument267 pagesC and Data Structures Q and AAnandaKrishna Sridhar100% (1)
- Connect Direct UsersGuide40Document128 pagesConnect Direct UsersGuide40Yogesh AggarwalNo ratings yet
- B2Bi 2.0.2 Basic Training Day 5Document55 pagesB2Bi 2.0.2 Basic Training Day 5Sidharth MazumdarNo ratings yet
- ADT DFT ORU: The Most Commonly Used HL7 Message Types IncludeDocument1 pageADT DFT ORU: The Most Commonly Used HL7 Message Types IncludeRafi Uddin ShaikNo ratings yet
- DB2 9.5 SQL Procedure Developer Exam 735 Prep, Part 2Document24 pagesDB2 9.5 SQL Procedure Developer Exam 735 Prep, Part 2prakash_6849No ratings yet
- Elearning Brochure HL7Document2 pagesElearning Brochure HL7Raju RajputNo ratings yet
- As400 JDEDocument4 pagesAs400 JDEvishnuNo ratings yet
- An Introduction To Mqseries Messaging and QueuingDocument17 pagesAn Introduction To Mqseries Messaging and QueuingBhasker ReddyNo ratings yet
- JDE Flujos de TrabajoDocument148 pagesJDE Flujos de TrabajoElias GomezNo ratings yet
- C Interview QuestionsDocument5 pagesC Interview QuestionsVignesh GuruNo ratings yet
- How To Deploy JDE - Ini, JAS - Ini and JDBJ - Ini Changes To A Webdev Client With A Full Package DeployDocument2 pagesHow To Deploy JDE - Ini, JAS - Ini and JDBJ - Ini Changes To A Webdev Client With A Full Package DeploymukeshsrivatavaNo ratings yet
- Erp Domain PDFDocument2 pagesErp Domain PDFJuan0% (1)
- FHIR On The Mirth Connect ServerDocument2 pagesFHIR On The Mirth Connect Servershilpi singhNo ratings yet
- BalasukumarPaluru HCL SKILLsDocument7 pagesBalasukumarPaluru HCL SKILLsNIKHIL KUMAR NNo ratings yet
- HL7Document11 pagesHL7api-3725627No ratings yet
- EDI Notepad Guide PDFDocument45 pagesEDI Notepad Guide PDFHermanNo ratings yet
- BSFN Srartups PDFDocument67 pagesBSFN Srartups PDFSai ChandraNo ratings yet
- EDI - How TO Get Started PDFDocument35 pagesEDI - How TO Get Started PDFmmediherNo ratings yet
- EDI Cost Benefit AnalysisDocument6 pagesEDI Cost Benefit AnalysisAllison KirbyNo ratings yet
- TestaDocument36 pagesTestaMangesh JagadaleNo ratings yet
- Business Process Modeling: IBM Sterling B2B IntegratorDocument108 pagesBusiness Process Modeling: IBM Sterling B2B IntegratorJContreras CTNo ratings yet
- Administration GuideDocument100 pagesAdministration Guiderobson.reyNo ratings yet
- Guardian Operations Reference SummaryDocument6 pagesGuardian Operations Reference SummaryLuis YañezNo ratings yet
- 850 Guideline V2003Document30 pages850 Guideline V2003reyNo ratings yet
- 835_companion_guideDocument17 pages835_companion_guideferdous.kmfNo ratings yet
- 820 Implementation Guide 4010 enDocument15 pages820 Implementation Guide 4010 enAnilNo ratings yet
- Analysis of Credit Risk Measurement UsinDocument6 pagesAnalysis of Credit Risk Measurement UsinDia-wiNo ratings yet
- Foreign Words and Legal Maxims by Uma GopalDocument24 pagesForeign Words and Legal Maxims by Uma GopalUma Gopal100% (1)
- Assignment/ Tugasan - Principles of ManagementDocument11 pagesAssignment/ Tugasan - Principles of ManagementSuriya KumaraNo ratings yet
- The Black Map-A New Criticism AnalysisDocument6 pagesThe Black Map-A New Criticism AnalysisxiruomaoNo ratings yet
- SPIL - Geneva ConventionDocument4 pagesSPIL - Geneva ConventionInna LadislaoNo ratings yet
- Introduction - Online Car Booking Management SystemDocument5 pagesIntroduction - Online Car Booking Management SystemTadese JegoNo ratings yet
- Assessment Form: Monitoring The Functionality of City/Municipal Council For The Protection of Children (C/MCPC)Document3 pagesAssessment Form: Monitoring The Functionality of City/Municipal Council For The Protection of Children (C/MCPC)dilg libmananNo ratings yet
- Economic Survey 2017-18Document350 pagesEconomic Survey 2017-18Subhransu Sekhar SwainNo ratings yet
- TMA Bye LawsDocument30 pagesTMA Bye LawsAsif Malik67% (3)
- Razon V IAC (De Leon)Document2 pagesRazon V IAC (De Leon)ASGarcia24No ratings yet
- Topic 10 Diversity Management in Organisation PDFDocument12 pagesTopic 10 Diversity Management in Organisation PDFAlister AshleyNo ratings yet
- Asian Paints: Sales Turnover: Sales Turnover of The Asian Paints Is Shows The Remarkable Increase FromDocument3 pagesAsian Paints: Sales Turnover: Sales Turnover of The Asian Paints Is Shows The Remarkable Increase FromHarsh AryaNo ratings yet
- Equatorial Realty Vs Mayfair TheaterDocument2 pagesEquatorial Realty Vs Mayfair TheaterSaji Jimeno100% (1)
- Weekly Report w34Document19 pagesWeekly Report w34Asep MAkmurNo ratings yet
- Lecture Notes On Vat As AmendedDocument7 pagesLecture Notes On Vat As Amendedbubblingbrook100% (1)
- Blue Economy CourseDocument2 pagesBlue Economy CourseKenneth FrancisNo ratings yet
- The Israel Lobby ControversyDocument2 pagesThe Israel Lobby ControversysisinjhaaNo ratings yet
- UADocument10 pagesUAsheriff0No ratings yet
- Dialogue Cause and Effect About Global WarmingDocument4 pagesDialogue Cause and Effect About Global WarmingGrace HanyNo ratings yet
- English Ancestral Homes of Noted Americans (1915)Document386 pagesEnglish Ancestral Homes of Noted Americans (1915)liketoread100% (1)
- LABELDocument2 pagesLABELerinNo ratings yet
- Florida Et Al v. Dept. of Health & Human Services Et AlDocument304 pagesFlorida Et Al v. Dept. of Health & Human Services Et AlDoug MataconisNo ratings yet
- ComprehensionDocument3 pagesComprehensiontatenda kawisiNo ratings yet
- Registration Form For Gi German Language Exam: (Kindly Spell As Mentioned in Your Passport)Document1 pageRegistration Form For Gi German Language Exam: (Kindly Spell As Mentioned in Your Passport)Imran LatifNo ratings yet