Professional Documents
Culture Documents
Jurnal R
Jurnal R
Uploaded by
ALberta Yoshe0 ratings0% found this document useful (0 votes)
6 views2 pagesThis case report describes two patients with neurological complications from varicella zoster virus (VZV) infection, one immunocompetent and one immunocompromised. The immunocompetent patient, a healthy marathon runner, presented with severe headache and was found to have VZV meningoencephalitis (ME), though without rash. The immunocompromised patient, an HIV-positive man, presented with altered mental status and weakness, and was found to have VZV ME, myelitis, and progressive outer retinal necrosis, with a poor response to antiviral treatment. The report discusses differences in presentation and outcomes between immunocompetent and immunocompromised patients with VZV CNS infections
Original Description:
Jurnal
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis case report describes two patients with neurological complications from varicella zoster virus (VZV) infection, one immunocompetent and one immunocompromised. The immunocompetent patient, a healthy marathon runner, presented with severe headache and was found to have VZV meningoencephalitis (ME), though without rash. The immunocompromised patient, an HIV-positive man, presented with altered mental status and weakness, and was found to have VZV ME, myelitis, and progressive outer retinal necrosis, with a poor response to antiviral treatment. The report discusses differences in presentation and outcomes between immunocompetent and immunocompromised patients with VZV CNS infections
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
6 views2 pagesJurnal R
Jurnal R
Uploaded by
ALberta YosheThis case report describes two patients with neurological complications from varicella zoster virus (VZV) infection, one immunocompetent and one immunocompromised. The immunocompetent patient, a healthy marathon runner, presented with severe headache and was found to have VZV meningoencephalitis (ME), though without rash. The immunocompromised patient, an HIV-positive man, presented with altered mental status and weakness, and was found to have VZV ME, myelitis, and progressive outer retinal necrosis, with a poor response to antiviral treatment. The report discusses differences in presentation and outcomes between immunocompetent and immunocompromised patients with VZV CNS infections
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 2
CASE REPORT
COMPLICATIONS OF VARICELLA ZOSTER INFECTION OF THE
CENTRAL NERVOUS SYSTEM
Anusha S. Thomas, M.D.; Jose A. Perez, Jr., M.D.
Houston Methodist Hospital, Houston, Texas
Introduction Case Report 2
Acute infection with the varicella zoster virus (VZV) is typically A 27-year-old Hispanic male with a history of advanced human
a self-limiting childhood illness with few complications. Following immunodeficiency virus (HIV) infection (CD4 count of 12 cells/
an acute infection, VZV becomes latent in cranial nerves and dor- mm3) and noncompliant with highly active antiretroviral therapy
sal root ganglia and may reactivate years later to produce herpes presented to the hospital with a 3-week history of altered mental
zoster (HZ) and postherpetic neuralgia, the most common neuro- status, bilateral lower extremity weakness, urinary retention, and
logical complication of HZ.1 The lifetime risk of developing HZ is constipation. He had been hospitalized twice in the preceding
20% to 30%, with older patients being the most commonly affected. month with gastrointestinal symptoms of undetermined etiology.
Meningoencephalitis (ME) is a serious central nervous system A lumbar puncture performed a week prior to hospitalization at
(CNS) complication of VZV infection that requires prompt treat- our institution revealed a polymerase chain reaction (PCR) posi-
ment to prevent a fatal outcome.2 It is thought to be a direct infec- tive for VZV with 6,289 copies/mL. Having refused medical care,
tion based on the findings of IgM antibodies specific to VZV and a he received only 3 doses of intravenous (IV) acyclovir followed by
cytopathogenic effect in cerebrospinal fluid.3 However, recent evi- oral prophylactic doses. His past medical history included cyto-
dence suggests that this underlying process involves vasculitis that megalovirus retinitis, Salmonella-related mitral valve endocarditis,
may lead to a delayed stroke-like syndrome and vasculopathy.4,5 AIDS-related dementia, and a recent episode of HZ 3 weeks prior
Infection of the CNS with VZV is not uncommon. A Spanish to his presenting symptoms. The physical examination revealed
study demonstrated the presence of VZV DNA in approximately complete left-sided vision loss with absent light reflex, 20/40 vi-
10% of all cases of aseptic meningitis, ME, and encephalitis.1,6,7 sion in the right eye, neck stiffness, healed HZ lesions over the left
Myelitis is another fatal CNS complication that may occur several flank, a motor strength of 1/5, and sensory loss in both lower ex-
days after the onset of HZ rash.8-10 We present two patients with tremities. A normal basic metabolic panel and a serum WBC count
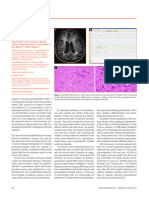
neurological complications of VZV, both with varying levels of of 1.67 K/mm3 were noted. An MRI of the thoracic and lumbar
immune competence. spine revealed thoracic cord atrophy and diffusely thickened cau-
da equina nerve roots consistent with HIV myelopathy.
Case Report 1 Analysis of the CSF revealed a WBC count of 17 K/mm3 includ-
A healthy 57-year-old Caucasian female, a competitive mar- ing 61% monocytes and 38% lymphocytes, with RBC 8 K/mm3,
athon runner, presented with a 5-day history of progressively protein 73 g/dL, glucose 53 mg/dL, and positive VZV PCR with
worsening bitemporal and retro-orbital headache, which she 14, 352 copies/mL. Epstein–Barr Virus PCR was also positive, but
described as the “worst headache of her life.” This was accom- copies were not reported. The John Cunningham virus PCR was
panied by fever and photophobia. Butalbital/acetaminophen/ positive in the blood. The patient received IV acyclovir and fos-
caffeine tablets administered 3 days prior at urgent care did not carnet for ME and suspected VZV transverse myelitis with HIV
relieve her symptoms. She had a temperature of 99.4oF with mild myelopathy for 2 weeks without any notable evidence of clinical
neck rigidity and no neurological deficit. No skin rash was not- improvement. A repeat CSF analysis done 2 weeks after admission
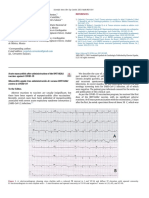
ed. Noncontrast computed tomography (CT) scan of the brain showed a rising VZV PCR of 47,657 copies/mL. In addition, oph-
was negative, and a basic metabolic panel and complete blood thalmologic evaluation of the right eye revealed a new finding of
count were normal. A lumbar puncture revealed xanthochromia progressive outer retinal necrosis (PORN) consistent with VZV ret-
with a normal opening pressure, white blood cells (WBC) 461 initis. Unfortunately, therapy with intravitreal foscarnet injections
K/mm3 with 91% lymphocytes, red blood cells (RBC) 23 K/mm3, for the retinitis and a combination of IV foscarnet and acyclovir for
protein 182 g/dL, and glucose 45 mg/dL. The patient was treat- ME was unsuccessful, and the patient was discharged to hospice
ed empirically with vancomycin, ceftriaxone, and acyclovir. CT care.
angiogram of the brain demonstrated a prominent infundibular
origin of the right posterior communicating artery concerning for Discussion
an aneurysm and sentinel bleed. Cerebral angiography, however, These cases indicate that VZV ME can occur in both immu-
was negative. Magnetic resonance imaging (MRI) of the brain re- nocompetent and immunocompromised patients. Our otherwise
vealed mild enlargement of ventricles, sulci, and cisterns without healthy competitive runner presented with what she described as
evidence of an acute intracranial process. Viral studies of cerebro- the “worst headache of her life,” a symptom suggestive of an in-
spinal fluid (CSF) showed 2,393 VZV DNA copies/mL. She was tracerebral hemorrhage. She presented without a rash, which is in
continued only on acyclovir with progressive improvement and keeping with case reports describing “zoster sine herpete.” 11-13 Giv-
discharged from the hospital to complete 2 weeks of treatment. en her xanthochromia, one could speculate that she had a minor
Complete resolution of symptoms without complications was hemorrhage suggesting a possible VZV-associated vasculopathy,
noted. which can affect both large or small cerebral arteries.14,15 Interest-
76 houstonmethodist.org/debakey-journal MDCVJ | XIII (2) 2017
ingly, VZV can also infect the extracranial temporal, ophthalmic, 5. Petrun B, Williams V, Brice S. Disseminated varicella-zoster virus
and retinal arteries, producing symptoms, signs, and laboratory in an immunocompetent adult. Dermatol Online J. 2015 Feb
abnormalities identical to those seen in giant cell arteritis.16 22;21(3).
The viral load in our immunocompetent patient was lower than 6. de Ory F, Avellón A, Echevarría JE, et al. Viral infections of the
in our second patient (2,939 vs 6,289). The time course of suspected central nervous system in Spain: a prospective study. J Med Vi-
disease was clearer in the first patient, consistent with evidence rol. 2013 Mar;85(3):554-62.
that viral loads correlate with severity and duration of neurolog- 7. Miyazaki Y, Riku Y, Goto Y, Mano K, Yoshida M, Hashizume Y.
ical disease.17 It may also explain her rapid response to treatment VZV vasculopathy associated with myelo-radiculoganglio-
and progressive improvement. In contrast, the second patient pre- meningo-encephalitis: an autopsy case of an immunocompetent
sented with advanced HIV infection with VZV ME and suspected 66-year-old male. J Neurol Sci. 2008 Dec 15;275(1-2):42-5.
myelitis. Failure to receive consistent therapy until 3 weeks into 8. Devinsky O, Cho ES, Petito CK, Price RW. Herpes zoster myeli-
his course may have contributed to a poor outcome. The striking tis. Brain. 1991 Jun;114 (Pt 3):1181-96.
lack of response to IV acyclovir, manifested by an elevated viral 9. Kleinschmidt-DeMasters BK, Gilden DH. Varicella-Zoster virus in-
load after 2 weeks of treatment, is consistent with reports of acy- fections of the nervous system: clinical and pathologic correlates.
clovir-resistant VZV infection after chronic oral acyclovir use.18,19 Arch Pathol Lab Med. 2001 Jun;125(6):770-80.
His paraparesis with sensory and autonomic dysfunction was 10. Dueland AN, Devlin M, Martin JR, et al. Fatal varicella-zoster virus
suspicious for progressive VZV myelitis with underlying HIV my- meningoradiculitis without skin involvement. Ann Neurol. 1991
elopathy. In immunocompetent individuals, postinfectious myelitis May;29(5):569-72.
resolves spontaneously with or without steroid therapy, while the 11. Halling G, Giannini C, Britton JW, et al. Focal encephalitis
same can be fatal among the immunocompromised due to spinal following varicella-zoster virus reactivation without rash in
cord invasion. Immunocompromised patients also may have ocu- a healthy immunized young adult. J Infect Dis. 2014 Sep
lar manifestations including acute retinal necrosis or PORN, both 1;210(5):713-6.
requiring early diagnosis and aggressive therapy.20 12. Jantsch J, Schmidt B, Bardutzky J, Bogdan C, Eckardt KU, Raff
These two cases represent the CNS manifestations of VZV in- U. Lethal varicella-zoster virus reactivation without skin lesions
fection among individuals at each end of the immunocompetence following renal transplantation. Nephrol Dial Transplant. 2011
spectrum. The marathon runner, an immunocompetent host pre- Jan;26(1):365-8.
senting with VZV ME in the absence of typical prodromal symp- 13. Kim GU, Ku BD. Varicella zoster virus meningoencephalitis ac-
toms and HZ rash, was responsive to antiviral therapy. Conversely, companied by rhabdomyolysis without skin eruption. Neurol Sci.
the immunocompromised patient had an insidiously progressive 2012 Jun;33(3):623-5.
presentation of the VZV reactivation process, with an aggressive 14. Powell DR 2nd, Patel S, Franco-Paredes C. Varicella-Zoster Virus
form of disease that was unresponsive to antiviral therapy. Vasculopathy: The Growing Association Between Herpes Zoster
Despite considerable mortality and morbidity related to VZV and Strokes. Am J Med Sci. 2015 Sep;350(3):243-5.
reactivation, few studies on treatment are currently available. The 15. Srivastava T, Nagpal K. Herpes zoster meningoencephalitis
highly potent attenuated VZV vaccine indicated for prevention of complicated with peripheral vascular disease: an uncommon
HZ reactivation in individuals aged 60 years and older is reported- presentation of a common disease. Scand J Infect Dis. 2014
ly only 50% effective.21 VZV should be considered in patients with Oct;46(10):716-8.
unexplained ME to facilitate early therapy and prevent adverse 16. Gilden D, Nagel M. Varicella Zoster Virus in Temporal Arteries of
outcomes. Patients With Giant Cell Arteritis. J Infect Dis. 2015 Jul 15;212
Suppl 1:S37-9.
Conflict of Interest Disclosure: The authors have completed and submitted 17. Rottenstreich A, Oz ZK, Oren I. Association between viral load of
the Methodist DeBakey Cardiovascular Journal Conflict of Interest Statement varicella zoster virus in cerebrospinal fluid and the clinical course
and none were reported. of central nervous system infection. Diagn Microbiol Infect Dis.
Keywords: varicella zoster virus, herpes zoster, meningoencephalitis 2014 Jun;79(2):174-7.
18. Jacobson MA, Berger TG, Fikrig S, et al. Acyclovir-resistant var-
References icella zoster virus infection after chronic oral acyclovir therapy in
1. LaGuardia JJ, Gilden DH. Varicella-zoster virus: a re-emerging patients with the acquired immunodeficiency syndrome (AIDS).
infection. J Investig Dermatol Symp Proc. 2001 Dec;6(3):183-7. Ann Intern Med. 1990 Feb 1;112(3):187-91.
2. Braun-Falco M, Hoffmann M. Herpes zoster with progression to 19. Bernhard P, Obel N. Chronic ulcerating acyclovir-resistant
acute varicella zoster virus-meningoencephalitis. Int J Dermatol. varicella zoster lesions in an AIDS patient. Scand J Infect Dis.
2009 Aug;48(8):834-9. 1995;27(6):623-5.
3. Auzanneau G, Chagnon A, Morillon M, Verdier M, de Jaure- 20. Franco-Paredes C, Bellehemeur T, Merchant A, Sanghi P, Di-
guiberry JP. Isolation of viruses in the cerebrospinal fluid in a case azGranados C, Rimland D. Aseptic meningitis and optic neuritis
of acute varicella meningo-encephalitis. Presse Med. 1987 Aug preceding varicella-zoster progressive outer retinal necrosis in a
29-Sep 5;16(28):1363-4. patient with AIDS. AIDS. 2002 May 3;16(7):1045-9.
4. Douglas A, Harris P, Francis F, Norton R. Herpes zoster menin- 21. Harte CM, Slattum PW. Recommended immunizations for
goencephalitis: not only a disease of the immunocompromised? older adults: a primer for pharmacists. Consult Pharm. 2015
Infection. 2010 Feb;38(1):73-5. Apr;30(4):210-20.
MDCVJ | XIII (2) 2017 houstonmethodist.org/debakey-journal 77
You might also like
- Contamination Control Strategy DevelopmentDocument75 pagesContamination Control Strategy DevelopmentArnaldo García100% (9)
- International Journal of Infectious DiseasesDocument6 pagesInternational Journal of Infectious DiseasesQuỳnh Nguyễn Thị NhưNo ratings yet
- West Nile Virus Infection and Myasthenia GravisDocument4 pagesWest Nile Virus Infection and Myasthenia Gravisarenasgrecia1No ratings yet
- 72 - Progressive Multifocal Leukoencephalopathy in An Immunocompetent PatientDocument7 pages72 - Progressive Multifocal Leukoencephalopathy in An Immunocompetent PatientFaras ArinalNo ratings yet
- Possible N Methyl D Aspartate Receptor Antibody Mediated Encephalitis in The Setting of HIV Cerebrospinal Fluid EscapeDocument5 pagesPossible N Methyl D Aspartate Receptor Antibody Mediated Encephalitis in The Setting of HIV Cerebrospinal Fluid EscapeJeremy Eckhart S ParhusipNo ratings yet
- Journal of Medical Case ReportsDocument4 pagesJournal of Medical Case ReportsSri Wahyuni YkNo ratings yet
- Developments in Varicella Zoster Virus Vasculopathy: Infection (J Halperin, Section Editor)Document8 pagesDevelopments in Varicella Zoster Virus Vasculopathy: Infection (J Halperin, Section Editor)Diki Khairul HidayatNo ratings yet
- Artigo Neuromeningeal Cryptococcosis in A Patient Not Infected With HumanDocument4 pagesArtigo Neuromeningeal Cryptococcosis in A Patient Not Infected With HumanRENATA SANTOS ASSUNCAONo ratings yet
- Importancia de Las Imágenes y El Diagnóstico Etiológico en El Paciente Inmunocomprometido Con Afección Del SNCDocument9 pagesImportancia de Las Imágenes y El Diagnóstico Etiológico en El Paciente Inmunocomprometido Con Afección Del SNCFranciely GarridoNo ratings yet
- Varicella Zoster Virus Vasculopathy: Clinical Features and PathogenesisDocument7 pagesVaricella Zoster Virus Vasculopathy: Clinical Features and PathogenesisYusmiatiNo ratings yet
- Case Report: Zika Virus Meningoencephalitis and Myelitis and Associated Magnetic Resonance Imaging FindingsDocument4 pagesCase Report: Zika Virus Meningoencephalitis and Myelitis and Associated Magnetic Resonance Imaging Findingsandiayu ahmad02No ratings yet
- Herpes Simplex: Encephalitis Children and Adolescents: Richard J. Whitley, MD, and David W. Kimberlin, MDDocument7 pagesHerpes Simplex: Encephalitis Children and Adolescents: Richard J. Whitley, MD, and David W. Kimberlin, MDFirah Triple'sNo ratings yet
- Mielopatia Por VVZ en VIH Lameiras 2022Document5 pagesMielopatia Por VVZ en VIH Lameiras 2022Lisbeth AlvarezNo ratings yet
- Whitley 2005Document7 pagesWhitley 2005Firah Triple'sNo ratings yet
- RCVS in Patients With Coronavirus DiseaseDocument10 pagesRCVS in Patients With Coronavirus DiseaseRicardo Otiniano SifuentesNo ratings yet
- 1 s2.0 S2590170221000625 MainDocument7 pages1 s2.0 S2590170221000625 MainM Rezki ArNo ratings yet
- 2021 - 07 - Encefalitis Autoinmune Post Vacuna SarsCov2Document3 pages2021 - 07 - Encefalitis Autoinmune Post Vacuna SarsCov2Eduardo RodriguezNo ratings yet
- Wang 2017 KKKDocument5 pagesWang 2017 KKKTais LineNo ratings yet
- Recurrent Aseptic Meningitis in A Child: Case ReportDocument3 pagesRecurrent Aseptic Meningitis in A Child: Case ReportAprimadhansari FarzimNo ratings yet
- Jurnal ChikungunyaDocument4 pagesJurnal ChikungunyaFitri Nadia SilvaniNo ratings yet
- Brain Hemorrhages: Josef Finsterer, Maria KornDocument3 pagesBrain Hemorrhages: Josef Finsterer, Maria KornLuis Ricardo Vejar FelixNo ratings yet
- Acute Disseminated Encephalomyelitis Following Tdap Vaccination and BacterialDocument4 pagesAcute Disseminated Encephalomyelitis Following Tdap Vaccination and BacterialAndrés MontalvoNo ratings yet
- Varicella-Zoster Virus Infections of The Nervous System: Clinical and Pathologic CorrelatesDocument11 pagesVaricella-Zoster Virus Infections of The Nervous System: Clinical and Pathologic CorrelatesarisastraNo ratings yet
- Balneo 319Document6 pagesBalneo 319Mihaela MavrodinNo ratings yet
- Seizures in Adults With Bacterial MeningitisDocument9 pagesSeizures in Adults With Bacterial MeningitiselaNo ratings yet
- Infectious Etiologies of StrokeDocument13 pagesInfectious Etiologies of Strokerafael rocha novaes100% (1)
- 2021-Acute Myocarditis After Administration of The BNT162b2 Vaccine Against COVID-19Document3 pages2021-Acute Myocarditis After Administration of The BNT162b2 Vaccine Against COVID-19seguridadyambiente641No ratings yet
- Concurrent Reactivation of VZV and HSV-2 in A Patient With Uncontrolled Diabetes Mellitus: A Case ReportDocument6 pagesConcurrent Reactivation of VZV and HSV-2 in A Patient With Uncontrolled Diabetes Mellitus: A Case ReportilhamcitrahamidiNo ratings yet
- Progressive Multifocal Leukoencephalopathy - A Case: Ovidiu Rosca, Elena-Cecilia Rosca, Lucian NegrutiuDocument5 pagesProgressive Multifocal Leukoencephalopathy - A Case: Ovidiu Rosca, Elena-Cecilia Rosca, Lucian Negrutiunoorhadi.n10No ratings yet
- Adem LikeDocument4 pagesAdem LikeRodrigo AriasNo ratings yet
- Case Report: A Case of Herpes Simplex Virus-1 Encephalitis From A Medicolegal Point of ViewDocument4 pagesCase Report: A Case of Herpes Simplex Virus-1 Encephalitis From A Medicolegal Point of Viewzefri suhendarNo ratings yet
- Human Herpes Virus-6Document3 pagesHuman Herpes Virus-64563748635No ratings yet
- DR Julian-MYOCARDITISDocument83 pagesDR Julian-MYOCARDITISArmando Esteban Coa SandovalNo ratings yet
- HIV Hemicorea CNS Histoplasmosis 2016Document3 pagesHIV Hemicorea CNS Histoplasmosis 2016Juan Salazar PajaresNo ratings yet
- 273 Full PDFDocument4 pages273 Full PDFAngelica Maria Rueda SerranoNo ratings yet
- Varicella-Zoster Virus Detection by Polymerase Chain Reaction Using Bronchoalveolar Lavage SpecimensDocument2 pagesVaricella-Zoster Virus Detection by Polymerase Chain Reaction Using Bronchoalveolar Lavage SpecimensRichel Edwin Theofili PattikawaNo ratings yet
- Viruses: Clinical Features of Varicella-Zoster Virus InfectionDocument11 pagesViruses: Clinical Features of Varicella-Zoster Virus InfectionBobby S PromondoNo ratings yet
- PML Treatment 2021 ANA-90-865Document9 pagesPML Treatment 2021 ANA-90-865Tunde CsepanyNo ratings yet
- Nosocomial VentriculitisDocument8 pagesNosocomial VentriculitisCrhistian GarcíaNo ratings yet
- Acute Encephalitis Caused by Intrafamilial Transmission of Enterovirus 71 in AdultDocument7 pagesAcute Encephalitis Caused by Intrafamilial Transmission of Enterovirus 71 in AdultAdhi SyukriNo ratings yet
- The Dangers of PRESDocument5 pagesThe Dangers of PRESShahnaaz ShahNo ratings yet
- Involvement of The Central Nervous System in Patients With Dengue Virus InfectionDocument5 pagesInvolvement of The Central Nervous System in Patients With Dengue Virus InfectionAmirah FaridahNo ratings yet
- Atypical Varicella - Zoster Virus ReactivationDocument11 pagesAtypical Varicella - Zoster Virus Reactivationnkaur1No ratings yet
- Aikawa1996 PDFDocument2 pagesAikawa1996 PDFPradiptaRezaSyahrunaNo ratings yet
- Enterovirus ImagingDocument7 pagesEnterovirus ImagingMomeneo NeoNo ratings yet
- BH 010060 ENGDocument2 pagesBH 010060 ENGCarlosNo ratings yet
- E110 FullDocument2 pagesE110 FullLuther ThengNo ratings yet
- Cytomegalic Inclusion Virus Encephalitis in Patients With AidsDocument6 pagesCytomegalic Inclusion Virus Encephalitis in Patients With Aidsderi rivanoNo ratings yet
- Holanda Et Al - J Neurovirol 2022Document4 pagesHolanda Et Al - J Neurovirol 2022jtd9h2xp5hNo ratings yet
- Acute Transverse Myelitis After COVID-19 VaccinationDocument7 pagesAcute Transverse Myelitis After COVID-19 VaccinationMing-Jen TsaiNo ratings yet
- Invasive Cryptococcal Meningitis Presenting As A Skull Base Mass in An Immunocompetent Host: A Case ReportDocument5 pagesInvasive Cryptococcal Meningitis Presenting As A Skull Base Mass in An Immunocompetent Host: A Case ReportAsep RiswandiNo ratings yet
- Viral Encephalitis PDFDocument7 pagesViral Encephalitis PDFDeborah Bravian TairasNo ratings yet
- 25 Kawasaki DiseaseDocument13 pages25 Kawasaki DiseaseVictor PazNo ratings yet
- PIIS0140673620312824Document1 pagePIIS0140673620312824Dino AdijayaNo ratings yet
- 278 977 1 SMDocument2 pages278 977 1 SMMohamed MukhrizNo ratings yet
- Citocinopatia Com Linfócitos Citotóxicos Aberrantes e Resposta Mielóide Pró-Fibrótica Na Miocardite ADocument65 pagesCitocinopatia Com Linfócitos Citotóxicos Aberrantes e Resposta Mielóide Pró-Fibrótica Na Miocardite AFernando de Souza DantasNo ratings yet
- Dengue Meningoencephalitis: Case ReportDocument3 pagesDengue Meningoencephalitis: Case ReportOleOhhNo ratings yet
- Childhood Multisystem Inflammatory Syndrome With PDocument5 pagesChildhood Multisystem Inflammatory Syndrome With PGiska VelindaNo ratings yet
- Research Paper On Bacterial MeningitisDocument8 pagesResearch Paper On Bacterial Meningitisvvgnzdbkf100% (1)
- Review Article: Acute Necrotizing Encephalopathy: An Underrecognized Clinicoradiologic DisorderDocument11 pagesReview Article: Acute Necrotizing Encephalopathy: An Underrecognized Clinicoradiologic DisorderfrizkapfNo ratings yet
- Auto-Inflammatory Syndromes: Pathophysiology, Diagnosis, and ManagementFrom EverandAuto-Inflammatory Syndromes: Pathophysiology, Diagnosis, and ManagementPetros EfthimiouNo ratings yet
- The Far Point and Refractive Error: Basic Optics, Chapter 5Document44 pagesThe Far Point and Refractive Error: Basic Optics, Chapter 5ALberta YosheNo ratings yet
- Dr. Dr. Jan Tumatar Ngantung, SPB, Spbp-Re. (K) - Bedah Plastik F.K. Unsrat ManadoDocument134 pagesDr. Dr. Jan Tumatar Ngantung, SPB, Spbp-Re. (K) - Bedah Plastik F.K. Unsrat ManadoALberta YosheNo ratings yet
- Atls Course Overview: Purpose, History, and Concepts of The Atls ProgramDocument12 pagesAtls Course Overview: Purpose, History, and Concepts of The Atls ProgramALberta YosheNo ratings yet
- IV To PO Review WorksheetDocument1 pageIV To PO Review WorksheetALberta YosheNo ratings yet
- Black Bean and Couscous BurgerDocument1 pageBlack Bean and Couscous BurgerALberta YosheNo ratings yet
- Heijden2013 Article EffectsOfExerciseTrainingOnQuaDocument16 pagesHeijden2013 Article EffectsOfExerciseTrainingOnQuaALberta YosheNo ratings yet
- Distal Cholangiocarcinoma (DCC) : Paxton V. Dickson, MD, Stephen W. Behrman, MDDocument57 pagesDistal Cholangiocarcinoma (DCC) : Paxton V. Dickson, MD, Stephen W. Behrman, MDALberta YosheNo ratings yet
- Casebook - Breast CancerDocument78 pagesCasebook - Breast CancerHeart Cañete SalimbangonNo ratings yet
- Mozambique 2030 PDFDocument68 pagesMozambique 2030 PDFGray HouserNo ratings yet
- A Case Study of A Child Age 17Document23 pagesA Case Study of A Child Age 17api-385551553No ratings yet
- Fast Dissolving TabletsDocument6 pagesFast Dissolving TabletsSamer FarhanNo ratings yet
- Obstetric Abdominal Examination OSCE GuideDocument16 pagesObstetric Abdominal Examination OSCE GuideMuhammad Aamir IqbalNo ratings yet
- Local Exhasut System - Design and LayoutDocument109 pagesLocal Exhasut System - Design and LayoutSreejit PillaiNo ratings yet
- Free English Proverbs and SayingsDocument3 pagesFree English Proverbs and SayingsAnonymous P7TpAx100% (2)
- Dwnload Full Medical Sociology 13th Edition Cockerham Test Bank PDFDocument36 pagesDwnload Full Medical Sociology 13th Edition Cockerham Test Bank PDFjaydenpowellqt2100% (11)
- Resume 12Document1 pageResume 12api-533988702No ratings yet
- Alpha Dry Adhesive-705438Document4 pagesAlpha Dry Adhesive-705438mohsinNo ratings yet
- Biostatistics 203. Survival Analysis: YhchanDocument8 pagesBiostatistics 203. Survival Analysis: YhchanselinblueNo ratings yet
- Gc-Ms Analysis of Phytochemical Compounds Present in The Rhizomes of NerviliaDocument7 pagesGc-Ms Analysis of Phytochemical Compounds Present in The Rhizomes of NerviliaMd. Badrul IslamNo ratings yet
- EfavirenzDocument3 pagesEfavirenzRosher Deliman JanoyanNo ratings yet
- AsthmaDocument16 pagesAsthmaSivaramakrishna Markandeya GuptaNo ratings yet
- DM Technical Guideline No.-10-Disposal-of-Unwanted-Materials-September-2020Document8 pagesDM Technical Guideline No.-10-Disposal-of-Unwanted-Materials-September-2020katageriguruNo ratings yet
- Bronze Alloys MsdsDocument11 pagesBronze Alloys MsdssalcabesNo ratings yet
- Ayurvedic Healing Covers Therapies and Medicine Treatments.: Bhagwan Mahavir College of ArchitectureDocument4 pagesAyurvedic Healing Covers Therapies and Medicine Treatments.: Bhagwan Mahavir College of Architectureaesha daveNo ratings yet
- The Future Effects of Biomedical EngineeringDocument25 pagesThe Future Effects of Biomedical Engineeringapi-390009833No ratings yet
- Trigetto White PaperDocument12 pagesTrigetto White Papershyamchepur0% (1)
- D.S.S Aiims Prepration Test SeriesDocument14 pagesD.S.S Aiims Prepration Test SeriesDr-Sanjay SinghaniaNo ratings yet
- 2017 PsychiatryDocument559 pages2017 PsychiatryMaricellaEkaR100% (1)
- Continuous Passive Motion DeviceDocument3 pagesContinuous Passive Motion DeviceSanny RamosNo ratings yet
- Nursing Practice 1Document4 pagesNursing Practice 1Nurul IzzahNo ratings yet
- PS XLIX 4 250114 Postscript C K MeenaDocument2 pagesPS XLIX 4 250114 Postscript C K MeenaShay WaxenNo ratings yet
- Lab ValuesDocument4 pagesLab ValuespninthemakinNo ratings yet
- Poultry Premix ManufacturerDocument11 pagesPoultry Premix ManufacturerSAHS LifesciencesNo ratings yet
- Concealed Carry Form LouisianaDocument9 pagesConcealed Carry Form LouisianaNicholas LeonardNo ratings yet
- Volume Homeostasis, Renal Function and Hypertension 1985Document14 pagesVolume Homeostasis, Renal Function and Hypertension 1985Debora OrnellasNo ratings yet
- Fungi Types, Morphology & Structure, Uses and Disadvantages: AscomycotaDocument7 pagesFungi Types, Morphology & Structure, Uses and Disadvantages: Ascomycotacasey lynNo ratings yet