Professional Documents
Culture Documents
Hirsch Sprung
Hirsch Sprung
Uploaded by
Harisa Mandasari0 ratings0% found this document useful (0 votes)
3 views1 pageHirschsprung's disease is characterized by the absence of ganglion cells in parts of the large bowel, causing spasms and obstruction. This is due to failed migration of neural crest cells during development. It most often involves the rectum and sigmoid colon, but can also affect more proximal areas of the colon. Surgery aims to remove the aganglionic segment and connect functional bowel to the anus, and can be done in one or multiple stages.
Original Description:
febri septara
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentHirschsprung's disease is characterized by the absence of ganglion cells in parts of the large bowel, causing spasms and obstruction. This is due to failed migration of neural crest cells during development. It most often involves the rectum and sigmoid colon, but can also affect more proximal areas of the colon. Surgery aims to remove the aganglionic segment and connect functional bowel to the anus, and can be done in one or multiple stages.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
3 views1 pageHirsch Sprung
Hirsch Sprung
Uploaded by
Harisa MandasariHirschsprung's disease is characterized by the absence of ganglion cells in parts of the large bowel, causing spasms and obstruction. This is due to failed migration of neural crest cells during development. It most often involves the rectum and sigmoid colon, but can also affect more proximal areas of the colon. Surgery aims to remove the aganglionic segment and connect functional bowel to the anus, and can be done in one or multiple stages.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 1
Hirschsprung’s disease
Hirschsprung’s disease is characterised by the congenital
absence of intramural ganglion cells (aganglionosis) and the
presence of hypertrophic nerves in the distal large bowel. The
absence of ganglion cells is due to a failure of migration of
vagal neural crest cells into the developing gut. The affected
gut is in spasm causing a functional bowel obstruction. The
aganglionosis is restricted to the rectum and sigmoid colon in
75 per cent of patients (short segment), involves the proximal
colon in 15 per cent (long segment) and affects the entire
colon and a portion of terminal ileum in 10 per cent (total
colonic aganglionosis). A transition zone exists between the
dilated, proximal, normally innervated bowel and the narrow,
distal aganglionic segment.
Hirschsprung’s disease may be familial or associated with
Down syndrome or other genetic disorders. Gene mutations
have been identified on chromosome 10 (involving the RET
proto-oncogene) and on chromosome 13 in some patients.
Hirschsprung’s disease typically presents in the neonatal period
with delayed passage of meconium, abdominal distension and
bilious vomiting, but it may not be diagnosed until later in
childhood or even adult life, when it manifests as severe chronic
constipation. Enterocolitis is a potentially fatal complication of
the disease.
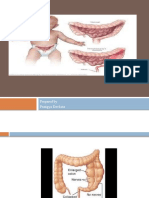
The diagnosis requires an adequate rectal biopsy and an
experienced pathologist. A contrast enema may show the
narrow aganglionic segment, a cone and the dilated proximal
bowel (Figure 8.31). Surgery aims to remove the aganglionic
segment and ‘pull-through’ ganglionic bowel to the anus (e.g.
Swenson, Duhamel, Soave and transanal procedures) and can
be done in a single stage or in several stages after first establishing
a proximal stoma in normally innervated bowel. Most
patients achieve good bowel control, but a significant minority
experience residual constipation and/or faecal incontinence or
further enterocolitis.
You might also like
- Hirschsprung DiseaseDocument19 pagesHirschsprung DiseaseUgi Rahul100% (1)
- Hirschsprung Disease: Waardenburg Syndrome Mowat-Wilson Syndrome Congenital Central Hypoventilation SyndromeDocument22 pagesHirschsprung Disease: Waardenburg Syndrome Mowat-Wilson Syndrome Congenital Central Hypoventilation SyndromeRizki Nandasari SulbahriNo ratings yet
- Hirschsprung DiseaseDocument1 pageHirschsprung DiseasePutri ClaraNo ratings yet
- Congenital Aganglionic Megacolon (Hirschsprung Disease) : Kristin N. Fiorino and Chris A. LiacourasDocument6 pagesCongenital Aganglionic Megacolon (Hirschsprung Disease) : Kristin N. Fiorino and Chris A. LiacourasSyakilla AuliaNo ratings yet
- Hirschsprung'S Disease: Peter MatteiDocument1 pageHirschsprung'S Disease: Peter MatteiJulia Wibawa HaryantoNo ratings yet
- 5 Congenital Malformation (Continue)Document4 pages5 Congenital Malformation (Continue)Mohamed Al-zichrawyNo ratings yet
- Hisprung DiseaseDocument12 pagesHisprung DiseaseEky Madyaning NastitiNo ratings yet
- Hirschprung DiseaseDocument9 pagesHirschprung DiseaseJonathan ObañaNo ratings yet
- Hirschsprung Disease Case Study: Maecy P. Tarinay BSN 4-1Document5 pagesHirschsprung Disease Case Study: Maecy P. Tarinay BSN 4-1Maecy OdegaardNo ratings yet
- Hirschsprungs DiseaseDocument4 pagesHirschsprungs DiseasesitharNo ratings yet
- Hirschsprung's Disease: (Congenital Aganglionic Megacolon)Document16 pagesHirschsprung's Disease: (Congenital Aganglionic Megacolon)umiNo ratings yet
- Hirschsprung DiseaseDocument13 pagesHirschsprung Diseaseganesh reddyNo ratings yet
- Hischsprug Disease by HamadDocument31 pagesHischsprug Disease by HamadALIEF MUTHIANo ratings yet
- Hirschsprung Disease - A SAGES Wiki ArticleDocument12 pagesHirschsprung Disease - A SAGES Wiki ArticleIndra GunawanNo ratings yet
- Emergency Complications of Hirschsprung DiseaseDocument17 pagesEmergency Complications of Hirschsprung DiseaseAngelica Stephanie MoqueteNo ratings yet
- Enfermedad de Hirschsprung: Diagnóstico Y Manejo en Niños Y AdultosDocument5 pagesEnfermedad de Hirschsprung: Diagnóstico Y Manejo en Niños Y AdultosAlexander Castillo CalderónNo ratings yet
- Hirschsprung DiseaseDocument25 pagesHirschsprung DiseaseMuhammad Zaniar RamadhaniNo ratings yet
- Hirsch SprungDocument20 pagesHirsch SprungrisaNo ratings yet
- Pa Tho Physiology of HirschprungDocument4 pagesPa Tho Physiology of HirschprungRenz Javier Tuñacao LustreNo ratings yet
- January - Hirschsprung's Disease in Africa 21 CenturyDocument27 pagesJanuary - Hirschsprung's Disease in Africa 21 CenturyVita MadmoNo ratings yet
- Congenital AnomaliesDocument10 pagesCongenital Anomaliesربيع ضياء ربيعNo ratings yet
- Congenital Aganglionic Megacolon - Hirschsprung Disease - 2009-6Document49 pagesCongenital Aganglionic Megacolon - Hirschsprung Disease - 2009-6Muhammad SubhanNo ratings yet
- Resource Unit On Hirschsprung's DiseaseDocument26 pagesResource Unit On Hirschsprung's DiseaseacholineNo ratings yet
- Adult Bowel Intussusception: Presentation, Location, Etiology, Diagnosis and TreatmentDocument4 pagesAdult Bowel Intussusception: Presentation, Location, Etiology, Diagnosis and TreatmentRizki Ismi Arsyad IINo ratings yet
- Hirschsprun G'S Disease: Dr. Manish Kumar Gupta Assistant Professor Department of Paediatric Surgery AIIMS, RishikeshDocument48 pagesHirschsprun G'S Disease: Dr. Manish Kumar Gupta Assistant Professor Department of Paediatric Surgery AIIMS, RishikeshArchana Mahata100% (1)
- Hirsch SprungDocument2 pagesHirsch SprungTitin Mananoma TuhalauruwNo ratings yet
- Hirschsprung's DiseaseDocument8 pagesHirschsprung's DiseaseRendra DananjayaNo ratings yet
- Hirsch SprungDocument6 pagesHirsch SprunghakimNo ratings yet
- Intestinal Obstruction in Pediatric SurgeryDocument69 pagesIntestinal Obstruction in Pediatric Surgeryabhinay_1712No ratings yet
- Journal Reading: Hirschprung's Disease Devin Reynando 1210118602Document23 pagesJournal Reading: Hirschprung's Disease Devin Reynando 1210118602Devin RNo ratings yet
- Hirschsprung DiseaseDocument44 pagesHirschsprung DiseaseAhmad Abu KushNo ratings yet
- Hirschsprung DiseaseDocument21 pagesHirschsprung DiseaseAhmad YaniNo ratings yet
- IntussusceptionDocument35 pagesIntussusceptionJaya Prabha100% (1)
- Hirschprung DiseaseDocument61 pagesHirschprung DiseaseAdditi Satyal100% (1)
- ILA - Hirschsprungs DiseaseDocument48 pagesILA - Hirschsprungs DiseaseSoleh Ramly100% (1)
- Cholecystitis FinalDocument57 pagesCholecystitis FinalRajendra DesaiNo ratings yet
- 6INVAGINASIDocument18 pages6INVAGINASIhazelelNo ratings yet
- Hirschsprung Disease (Aganglionic Megacolon)Document6 pagesHirschsprung Disease (Aganglionic Megacolon)Julliza Joy PandiNo ratings yet
- HirschprungDocument6 pagesHirschprungVanessa CasingalNo ratings yet
- Hirschsprung 1socaDocument34 pagesHirschsprung 1socaDianNo ratings yet
- Hirschprung's DiseaseDocument26 pagesHirschprung's DiseaseAbdur RaqibNo ratings yet
- Hirchsprung Correlated GeneticDocument12 pagesHirchsprung Correlated GeneticAlpascaFirdausNo ratings yet
- Gangrenous Sigmoid Volvulus - A Case Report With Review of LiteratureDocument4 pagesGangrenous Sigmoid Volvulus - A Case Report With Review of LiteratureInternational Organization of Scientific Research (IOSR)No ratings yet
- Pathology of Intestinal Motor DisordersDocument31 pagesPathology of Intestinal Motor DisorderslegrangedanitaNo ratings yet
- GALLBLADDERDocument16 pagesGALLBLADDERKadenceFreya-Charisse G PosadasBulintao100% (2)
- Background: Hirschsprung Disease. Contrast Enema Demonstrating Transition Zone in The Rectosigmoid RegionDocument9 pagesBackground: Hirschsprung Disease. Contrast Enema Demonstrating Transition Zone in The Rectosigmoid RegionWeny SyifaNo ratings yet
- Total Colonic Aganglionosis (Zuelzer Wilson Syndrome) An EnigmaDocument2 pagesTotal Colonic Aganglionosis (Zuelzer Wilson Syndrome) An EnigmarmysdsNo ratings yet
- GI PathoDocument20 pagesGI Pathojutah2013No ratings yet
- Rami Dwairi, MD: Internal Medicine, HSDocument27 pagesRami Dwairi, MD: Internal Medicine, HSraed faisalNo ratings yet
- Pemeriksaan Rontgen Toraks, Elektrokardiogram (EKG), USG Abdomen Dan EchocardiografiDocument5 pagesPemeriksaan Rontgen Toraks, Elektrokardiogram (EKG), USG Abdomen Dan EchocardiografigorodoeNo ratings yet
- Ileal Atresia ReferenceDocument50 pagesIleal Atresia ReferenceOvamelia JulioNo ratings yet
- Green 2016Document6 pagesGreen 2016Donny Artya KesumaNo ratings yet
- Pediatric Clinics of North America IIDocument54 pagesPediatric Clinics of North America IIkarenNo ratings yet
- Intraoperative Finding in Total Colonic AganglionosisDocument12 pagesIntraoperative Finding in Total Colonic AganglionosisAtrioventrikular MilanistiNo ratings yet
- Imaging of Congenital Anomalies of The Gastrointestinal TractDocument12 pagesImaging of Congenital Anomalies of The Gastrointestinal TractMateen ShukriNo ratings yet
- Intususcepción: Diagnóstico Y Manejo en Niños Y Adultos: C Ir Ugí ADocument6 pagesIntususcepción: Diagnóstico Y Manejo en Niños Y Adultos: C Ir Ugí ACarlos Angel LiraNo ratings yet
- Case 22: Total Colonic Aganglionosis - Long-Segment Hirschsprung DiseaseDocument4 pagesCase 22: Total Colonic Aganglionosis - Long-Segment Hirschsprung DiseaseRahmat MuliaNo ratings yet
- Dysphagia, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandDysphagia, A Simple Guide To The Condition, Treatment And Related ConditionsRating: 5 out of 5 stars5/5 (1)
- Colitis: A Practical Approach to Colon and Ileum Biopsy InterpretationFrom EverandColitis: A Practical Approach to Colon and Ileum Biopsy InterpretationAnne Jouret-MourinNo ratings yet