Professional Documents
Culture Documents
Gallbladder: Picture Series by Mai
Gallbladder: Picture Series by Mai
Uploaded by
Concepcion R. Aquino0 ratings0% found this document useful (0 votes)
23 views22 pagesThis document contains diagrams and descriptions of the anatomy and variations of the biliary system, gallbladder, and cystic duct. It also depicts imaging techniques like ultrasound, cholangiography, and percutaneous procedures for accessing the biliary system. Various classifications of biliary diseases and tumors are shown.
Original Description:
sx
Original Title
Gallbladder
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document contains diagrams and descriptions of the anatomy and variations of the biliary system, gallbladder, and cystic duct. It also depicts imaging techniques like ultrasound, cholangiography, and percutaneous procedures for accessing the biliary system. Various classifications of biliary diseases and tumors are shown.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
23 views22 pagesGallbladder: Picture Series by Mai
Gallbladder: Picture Series by Mai
Uploaded by
Concepcion R. AquinoThis document contains diagrams and descriptions of the anatomy and variations of the biliary system, gallbladder, and cystic duct. It also depicts imaging techniques like ultrasound, cholangiography, and percutaneous procedures for accessing the biliary system. Various classifications of biliary diseases and tumors are shown.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 22
Gallbladder
Picture series by Mai
Figure 32-1. Anterior aspect of the biliary
anatomy. a = right hepatic duct; b = left hepatic
duct; c = common hepatic duct; d = portal vein; e
= hepatic artery; f = gastroduodenal artery; g = left
gastric artery; h = common bile duct; i = fundus of
the gallbladder; j = body of gallbladder; k =
infundibulum; l = cystic duct; m = cystic artery; n
= superior pancreaticoduodenal artery. Note the
situation of the hepatic bile duct confluence
anterior to the right branch of the portal vein, and
the posterior course of the right hepatic artery
1310 behind the common hepatic duct.
Figure32-2.
Variationsofthecysticductanatomy.A.L
owjunctionbetweenthecysticductandco
mmonhepaticduct.B.Cysticductadher-
ent to the common hepatic duct. C.
High junction between the cystic and
the common hepatic duct. D. Cystic
duct drains into right hepatic duct. E.
Long cystic duct that joins common
hepatic duct behind the duodenum. F.
Absence of cystic duct. G. Cystic duct
crosses posterior to common hepatic
duct and joins it anteriorly. H. Cystic
duct courses anterior to common
hepatic duct and joins it posteriorly.
Figure 32-4. Variations in the arterial supply to the
gallbladder. A. Cystic artery from right hepatic artery,
about 80% to 90%. B. Cystic artery from right hepatic
artery (accessory or replaced) from superior
mesenteric artery, about 10%. C. Two cystic arter- ies,
one from the right hepatic, the other from the
common hepatic artery, rare. D. Two cystic arteries,
one from the right hepatic, the other from the left
hepatic artery, rare. E. The cystic artery branch- ing
from the right hepatic artery and running anterior to
the com- mon hepatic duct, rare. F. Two cystic
arteries arising from the right hepatic artery, rare.
Figure 32-8. Schematic diagram of per- cutaneous
transhepatic cholangiogram and drainage for obstructing
proximal cholangio- carcinoma. A. Dilated intrahepatic
bile duct is entered percutaneously with a fine needle. B.
Small guidewire is passed through the needle into the
duct. C. A plastic catheter has been passed over the wire,
and the wire is subsequently removed. A cholangiogram
is performed through the catheter. D. An external
drainage catheter in place. E. Long wire placed via the
catheter and advanced past the tumor and into the
duodenum. F. Internal stent has been placed through the
tumor.
Figure 32-5. The effect of
cholecystokinin on the Figure 32-6. An ultrasonography
gallbladder and the sphincter of the gallbladder. Arrows indi-
of Oddi. A. During fasting, cate the acoustic shadows from
with the sphincter of Oddi stones in the gallbladder.
contracted and the gallbladder
filling. B. In response to a
meal, the sphincter of Oddi
relaxed and the gallbladder
emptying.
Figure 32-8. Schematic diagram of per- cutaneous
transhepatic cholangiogram and drainage for obstructing
proximal cholangio- carcinoma. A. Dilated intrahepatic
bile duct is entered percutaneously with a fine needle. B.
Small guidewire is passed through the needle into the
duct. C. A plastic catheter has been passed over the wire,
and the wire is subsequently removed. A cholangiogram
is performed through the catheter. D. An external
drainage catheter in place. E. Long wire placed via the
catheter and advanced past the tumor and into the
duodenum. F. Internal stent has been placed through the
tumor.
Figure 32-12. The three major
components of bile plotted on trian-
gular coordinates. A given point
represents the relative molar ratios of
bile salts, lecithin, and cholesterol.
The area labeled “micellar liquid”
shows the range of concentrations
found consistent with a clear micellar
solution (single phase), where
cholesterol is fully solubilized. The
shaded area directly above this region
corresponds to a metastable zone,
supersaturated with cholesterol. Bile
with a composition that falls above
the shaded area has exceeded the
solu- bilization capacity of
cholesterol and precipitation of
cholesterol crystals occurs.
FIGURE 54-21 Triangle of Solubility.
With the three major components of
bile that determine cholesterol
solubility and stability, each can be
quantified by molar percentage to
show a relative ratio to the other two.
Cholesterol is completely soluble in
only the small area in the left lower
corner, where a clear micellar solu-
tion exists, below the closed circles.
Just above this, in the area between the
open and closed circles, cholesterol is
supersaturated but stable and thus
crystallized only with stasis. In the
remainder of the triangle, cholesterol
is significantly supersaturated and
unstable. In this region, crystals form
immediately.
Figure 32-17. Percutaneous cholecystostomy. A pigtail
catheter has been placed through the abdominal wall, the
right lobe of the liver, and into the gallbladder.
Figure 32-22. Classification of
choledochal cysts. Type I, fusiform or
cystic dilations of the extrahepatic
biliary tree, is the most common type,
making up >50% of the choledochal
cysts. Type II, saccular diverticulum
of an extrahepatic bile duct. Rare,
<5% of choledochal cysts. Type III,
bile duct dilatation within the
duodenal wall (choledochoceles),
makes up about 5% of choledochal
cysts. Types IVa and IVb, mul- tiple
cysts, make up 5% to 10% of
choledochal cysts. Type IVa affects
both extrahepatic and intrahepatic bile
ducts, whereas type IVb cysts affect
the extrahepatic bile ducts only. Type
V, intrahepatic biliary cysts, is very
rare and makes up 1% of choledochal
cysts.
Figure 32-26. Bismuth-Corlette classification of bile duct
tumors.
Figure 32-28. A through F.
Percutaneous transhepatic
cholangiography and
placement of a biliary
drainage catheter. The
catheter has been passed
through the tumor area
(distal cholangiocarcinoma)
that is obstructing the distal
common bile duct and into
the duodenum.
You might also like
- Miles Operation - Abdominoperineal Excision - Rectal CADocument5 pagesMiles Operation - Abdominoperineal Excision - Rectal CASpencer DempseyNo ratings yet
- Sur - Atlas of Gastrointestinal Surgery (Cameron) NewDocument474 pagesSur - Atlas of Gastrointestinal Surgery (Cameron) Newalisolouki40100% (12)
- The Gallbladder AnatomyDocument10 pagesThe Gallbladder AnatomyClaudia IlieNo ratings yet
- Articulo 1 Quiste ColeDocument4 pagesArticulo 1 Quiste ColeMaria Elena VinuezaNo ratings yet
- Soal BiologiDocument19 pagesSoal BiologiRocci Jack ParseNo ratings yet
- CholecystectomyDocument9 pagesCholecystectomyAmyandNo ratings yet
- A. Ionization: or (Increased Target - Object Distance)Document10 pagesA. Ionization: or (Increased Target - Object Distance)Nashaat H. AlshawabkehNo ratings yet
- Cirugia Anatomica Del Intestino GruesoDocument3 pagesCirugia Anatomica Del Intestino GruesoWildor Herrera GuevaraNo ratings yet
- Block EDocument33 pagesBlock Eabdullah tanoliNo ratings yet
- Intrahepatic Cholangiojejunostomy-An Operation For Biliary ObstructionDocument15 pagesIntrahepatic Cholangiojejunostomy-An Operation For Biliary ObstructionRusdi MedikaNo ratings yet
- En V25n1a22Document4 pagesEn V25n1a22Alexandre AlexandreNo ratings yet
- Chist ColedocDocument7 pagesChist ColedocAlina MihuNo ratings yet
- 2 Acute CholecystitisDocument21 pages2 Acute CholecystitisEtteh MaryNo ratings yet
- Cholecystectomy Iatrogenic Bile Duct Injury: April 28, 2005 OHSU, Department of Diagnostic Radiology Kan Hwee, MS4Document35 pagesCholecystectomy Iatrogenic Bile Duct Injury: April 28, 2005 OHSU, Department of Diagnostic Radiology Kan Hwee, MS4SahirNo ratings yet
- Chapter 50 - Surgical Anatomy of Large IntestineDocument3 pagesChapter 50 - Surgical Anatomy of Large Intestinesamantha warwarNo ratings yet
- 2 Biliary Anatomy and EmbrDocument16 pages2 Biliary Anatomy and EmbrShawn GravesNo ratings yet
- Pancreatic Pseudocyst EDITEDDocument5 pagesPancreatic Pseudocyst EDITEDLaura LatifaNo ratings yet
- 54.the Gallbladder and Bile DuctsDocument19 pages54.the Gallbladder and Bile DuctsAdenegan Adesola RaymondNo ratings yet
- !5uroical 5ection.: Some Points Surgical of Supply Hamilton Drummond, F.R.C.S.EdDocument9 pages!5uroical 5ection.: Some Points Surgical of Supply Hamilton Drummond, F.R.C.S.EdaliNo ratings yet
- Total Pelvic ExenterationDocument13 pagesTotal Pelvic ExenterationRirin Wahyuni100% (1)
- Esophageal Reconstruction With Large Intestine: 1. Vascular Anatomy of The ColonDocument26 pagesEsophageal Reconstruction With Large Intestine: 1. Vascular Anatomy of The ColonCitra AryantiNo ratings yet
- GIT 2014 Part 1 Brant Lang PDFDocument7 pagesGIT 2014 Part 1 Brant Lang PDFbriceNo ratings yet
- Rupture of A Hydatid Cyst Into The Bile DuctDocument3 pagesRupture of A Hydatid Cyst Into The Bile DuctasclepiuspdfsNo ratings yet
- Chapter 32: Gallbladder and The Extrahepatic Biliary System: Key PointsDocument43 pagesChapter 32: Gallbladder and The Extrahepatic Biliary System: Key PointsSteven Tapia VillacísNo ratings yet
- Junq - Ed.10 Engl - LiverDocument24 pagesJunq - Ed.10 Engl - LiverMaria LaiaNo ratings yet
- Abdomen Agudo ObstructivoDocument36 pagesAbdomen Agudo ObstructivoMaria BetzabethNo ratings yet
- Horton, K. M., Corl, F. M., & Fishman, E. K. (2000) - CT Evaluation of The Colon - Inflammatory Disease. RadioGraphics, 20 (2), 399-418Document20 pagesHorton, K. M., Corl, F. M., & Fishman, E. K. (2000) - CT Evaluation of The Colon - Inflammatory Disease. RadioGraphics, 20 (2), 399-418PauloCostaNo ratings yet
- Los Terrybles Book TeamDocument6 pagesLos Terrybles Book TeamWildor Herrera GuevaraNo ratings yet
- Topic 1 MCQ Incoming ControlDocument6 pagesTopic 1 MCQ Incoming ControlQmobile J5No ratings yet
- Iatrogenci BDIDocument90 pagesIatrogenci BDIUsmle GuyNo ratings yet
- Soal Modul 1Document12 pagesSoal Modul 1duo_ngoNo ratings yet
- Acute CholecystitisDocument18 pagesAcute CholecystitisOktavia PutriNo ratings yet
- Hep Resxn TechDocument33 pagesHep Resxn TechKartikKulshresthaNo ratings yet
- DocumentDocument9 pagesDocumentIbrahim AmerNo ratings yet
- GI BileDuct ProtocolDocument9 pagesGI BileDuct ProtocolElloide PajutanNo ratings yet
- Anatomy of The Caecum, Appendix and Colon: Basic ScienceDocument4 pagesAnatomy of The Caecum, Appendix and Colon: Basic ScienceMirza RisqaNo ratings yet
- 100Document17 pages100Dr-Wisam Mhmd Ali100% (1)
- Chapter 20Document14 pagesChapter 20Syafithria WuNo ratings yet
- Gastro02 IntroGIPathDocument6 pagesGastro02 IntroGIPathPatricia RuizNo ratings yet
- Los Terrybles Book TeamDocument10 pagesLos Terrybles Book TeamWildor Herrera GuevaraNo ratings yet
- Case ReportDocument5 pagesCase ReportAmmar magdyNo ratings yet
- Colecistogastrostomia-Biopsia de HigadoDocument8 pagesColecistogastrostomia-Biopsia de HigadoWildor Herrera GuevaraNo ratings yet
- Chapter 27 - Biliary TractDocument32 pagesChapter 27 - Biliary TractAdrian ContrerasNo ratings yet
- Distribution OF Intra-Abdominal Malignant Seeding: Dependency ON Dynamics OF Flow OF Ascit1C FluidDocument9 pagesDistribution OF Intra-Abdominal Malignant Seeding: Dependency ON Dynamics OF Flow OF Ascit1C Fluidmuriloscuc5429No ratings yet
- Surgical Management Ca Colon 1Document81 pagesSurgical Management Ca Colon 1Shweta Achuthan KuttyNo ratings yet
- RectumDocument129 pagesRectumRadhika SethuNo ratings yet
- The Liver and PancreasDocument25 pagesThe Liver and Pancreastink29No ratings yet
- Colectomia Izquierda, Anastomosis Termino-TerminalDocument11 pagesColectomia Izquierda, Anastomosis Termino-TerminalWildor Herrera GuevaraNo ratings yet
- Single-Incision Laparoscopic Roux-en-Y Hepaticojejunostomy Using Conventional Instruments For Children With Choledochal CystsDocument7 pagesSingle-Incision Laparoscopic Roux-en-Y Hepaticojejunostomy Using Conventional Instruments For Children With Choledochal CystsCherNo ratings yet
- MRCP ImportantDocument12 pagesMRCP ImportantPankaj NarekarNo ratings yet
- Saint Louis University School of Medicine Mmxxii: Dr. Baldovino - October 13, 2020Document11 pagesSaint Louis University School of Medicine Mmxxii: Dr. Baldovino - October 13, 2020Djan Kurvie ValencerinaNo ratings yet
- Theory of Anatomy - MBBS Pre-Clinical Phase Lecture Notes & Ebook PDF Download - 3Document77 pagesTheory of Anatomy - MBBS Pre-Clinical Phase Lecture Notes & Ebook PDF Download - 3LALITHA AUDITHYANo ratings yet
- MCQDocument11 pagesMCQsalamredNo ratings yet
- Right and Extended Right Colectomy - Open Technique - UpToDateDocument44 pagesRight and Extended Right Colectomy - Open Technique - UpToDateDpxeir PapanikolaouNo ratings yet
- CHOLECYSTECTOMYDocument6 pagesCHOLECYSTECTOMYJagannath DasNo ratings yet
- Gallbladder and Extrahepatic Biliary System - FinlDocument14 pagesGallbladder and Extrahepatic Biliary System - FinlJoevet T. TadlasNo ratings yet
- Mid Exam 2010 Saudi Board SurgeryDocument16 pagesMid Exam 2010 Saudi Board SurgeryAhmad Alnemare100% (1)
- Anatomia de Vesicula BiliarDocument5 pagesAnatomia de Vesicula BiliarHumberto CamposNo ratings yet
- Hemicolectomy 1Document40 pagesHemicolectomy 1Preethi GudipalliNo ratings yet
- Difficult Acute Cholecystitis: Treatment and Technical IssuesFrom EverandDifficult Acute Cholecystitis: Treatment and Technical IssuesNo ratings yet
- Morbidity April 2022: Aileen Concepcion M. AgustinDocument24 pagesMorbidity April 2022: Aileen Concepcion M. AgustinConcepcion R. AquinoNo ratings yet
- Alternative MedicineDocument3 pagesAlternative MedicineConcepcion R. AquinoNo ratings yet
- Polycystic Kidney Disease: Joel M. Topf, MDDocument20 pagesPolycystic Kidney Disease: Joel M. Topf, MDConcepcion R. AquinoNo ratings yet
- AcneDocument9 pagesAcneConcepcion R. AquinoNo ratings yet
- First Judicial RegionDocument6 pagesFirst Judicial RegionConcepcion R. AquinoNo ratings yet
- Major Depression and Bipolar Disorder: By: Aileen Concepcion M. AgustinDocument52 pagesMajor Depression and Bipolar Disorder: By: Aileen Concepcion M. AgustinConcepcion R. AquinoNo ratings yet
- Which He Initially Termed "Polyglandular Syndrome": Overnight 1mg Dexamethasone Suppression TestDocument2 pagesWhich He Initially Termed "Polyglandular Syndrome": Overnight 1mg Dexamethasone Suppression TestConcepcion R. AquinoNo ratings yet
- Date and Time: June 23, 2018, 3PM Chief Complaint: Difficulty of Breathing History of Present IllnessDocument3 pagesDate and Time: June 23, 2018, 3PM Chief Complaint: Difficulty of Breathing History of Present IllnessConcepcion R. AquinoNo ratings yet
- Admitting Diagnosis: Chronic Kidney Disease Stage V Secondary To Polycystic Kidney Disease, Ascites Secondary ToDocument7 pagesAdmitting Diagnosis: Chronic Kidney Disease Stage V Secondary To Polycystic Kidney Disease, Ascites Secondary ToConcepcion R. AquinoNo ratings yet
- Rehabilitation of Spinal Cord InjuryDocument23 pagesRehabilitation of Spinal Cord InjuryConcepcion R. AquinoNo ratings yet
- ObjectDocument1 pageObjectConcepcion R. AquinoNo ratings yet
- Case #9 Mariter Mendoza vs. Adriano Casumpang Et. Al G.R. No. 197987 March 19, 2012Document2 pagesCase #9 Mariter Mendoza vs. Adriano Casumpang Et. Al G.R. No. 197987 March 19, 2012Concepcion R. AquinoNo ratings yet
- CultureDocument11 pagesCultureConcepcion R. AquinoNo ratings yet
- "An Ailment Not To Be Treated" - Earliest ReferenceDocument3 pages"An Ailment Not To Be Treated" - Earliest ReferenceConcepcion R. AquinoNo ratings yet
- Finals Finals Finals Finals Finals Finals Finals Finals Finals Finals Finals Finals FinalsDocument1 pageFinals Finals Finals Finals Finals Finals Finals Finals Finals Finals Finals Finals FinalsConcepcion R. AquinoNo ratings yet
- Bes After Nung EpidemiologyDocument4 pagesBes After Nung EpidemiologyConcepcion R. AquinoNo ratings yet
- New Doc 2018-03-22 08.34.44 - 20180322083931Document7 pagesNew Doc 2018-03-22 08.34.44 - 20180322083931Concepcion R. AquinoNo ratings yet
- Increased Cartilage, Recoil, and Outer Ridge Curving InwardDocument2 pagesIncreased Cartilage, Recoil, and Outer Ridge Curving InwardConcepcion R. AquinoNo ratings yet
- GraphDocument1 pageGraphConcepcion R. AquinoNo ratings yet
- The Nose and Paranasal SinusesDocument31 pagesThe Nose and Paranasal SinusesConcepcion R. AquinoNo ratings yet
- Open Questioning: Ob GynDocument1 pageOpen Questioning: Ob GynConcepcion R. AquinoNo ratings yet
- EsophagusDocument21 pagesEsophagusConcepcion R. AquinoNo ratings yet
- Legal MedDocument10 pagesLegal MedConcepcion R. AquinoNo ratings yet
- HeadacheDocument15 pagesHeadacheConcepcion R. AquinoNo ratings yet
- InfectionsDocument21 pagesInfectionsConcepcion R. AquinoNo ratings yet
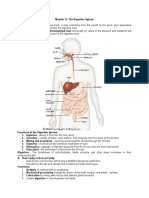
- Module 13 - The Digestive SystemDocument8 pagesModule 13 - The Digestive SystemAngela FelixNo ratings yet
- Peptic UlcerDocument34 pagesPeptic Ulceralexjohnvt100% (1)
- DPP 2 Oesophagus and StomachDocument4 pagesDPP 2 Oesophagus and StomachDr-Atin Kumar SrivastavaNo ratings yet
- Choledocholithiasis - Clinical Manifestations, Diagnosis, and Management - UpToDateDocument19 pagesCholedocholithiasis - Clinical Manifestations, Diagnosis, and Management - UpToDateFeer VillarrealNo ratings yet
- Elimination Pattern (Fecal) MSPDocument20 pagesElimination Pattern (Fecal) MSPMuhammadNo ratings yet
- Chronic Liver DiseaseDocument20 pagesChronic Liver DiseaseDastogir AlamNo ratings yet
- 16 Daftar PustakaDocument4 pages16 Daftar PustakaClarisa AnindyaNo ratings yet
- Gastroenterology-Liver, Pancreas and Gall Bladder LecturesDocument7 pagesGastroenterology-Liver, Pancreas and Gall Bladder LecturesMarco Paulo Reyes NaoeNo ratings yet
- Titratable Acidity Milk PDFDocument13 pagesTitratable Acidity Milk PDFsyaroniNo ratings yet
- IcterusDocument11 pagesIcterusnikita134No ratings yet
- Alkaline Water Stomach Acid DR Jerry TennantDocument2 pagesAlkaline Water Stomach Acid DR Jerry TennantCesar OrantesNo ratings yet
- DR Kiki Lukman Patofisiologi Acute CholangitisDocument36 pagesDR Kiki Lukman Patofisiologi Acute CholangitisAfkar30No ratings yet
- ErcpDocument22 pagesErcpPutu YoanaNo ratings yet
- Liver Cirrhosis DoneDocument91 pagesLiver Cirrhosis DoneGiorgi PopiashviliNo ratings yet
- NCP (Diarrhea)Document2 pagesNCP (Diarrhea)Rodj Bilang Jr.83% (30)
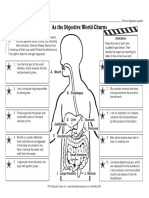
- Science Worksheet Digestive SystemDocument2 pagesScience Worksheet Digestive SystemMarlin Kunzel PNo ratings yet
- Pancreatic Cancer: Dr. Tjatur Winarsanto SPPDDocument41 pagesPancreatic Cancer: Dr. Tjatur Winarsanto SPPDMayiz Renata LimerseNo ratings yet
- Pengertian Itik 2Document10 pagesPengertian Itik 2AndiAna RasyidNo ratings yet
- Dr. Ali's Uworld Notes For Step 2 CKDocument28 pagesDr. Ali's Uworld Notes For Step 2 CKuyesNo ratings yet
- Cholelithiasis, Biliary Colic, Cholecystitis and Cholangitis: Adult & PediatricDocument7 pagesCholelithiasis, Biliary Colic, Cholecystitis and Cholangitis: Adult & PediatricGunaseelaan MananNo ratings yet
- Esophages and Stomach ...........Document65 pagesEsophages and Stomach ...........Gebrie DinkayehuNo ratings yet
- Gall Bladder ANATOMYDocument5 pagesGall Bladder ANATOMYDIVINE GRACE FLORITA PEPITONo ratings yet
- The Fecal Incontinence Severity IndexDocument7 pagesThe Fecal Incontinence Severity Indexi can always make u smile :DNo ratings yet
- Ajr 17 19378Document13 pagesAjr 17 19378heryanggunNo ratings yet
- The Structure of The Human Alimentary Canal - The Mouth, The Stomach, The Small Intestine, The Colon and RectumDocument5 pagesThe Structure of The Human Alimentary Canal - The Mouth, The Stomach, The Small Intestine, The Colon and RectumnaxeenNo ratings yet
- Digestive Structured Questions BIO095Document2 pagesDigestive Structured Questions BIO095Izzuddin Ghani100% (1)
- Biology STD 11: Biology MCQ: Section A //X Write The Answer of The Following Questions. (Each Carries 1 Mark)Document5 pagesBiology STD 11: Biology MCQ: Section A //X Write The Answer of The Following Questions. (Each Carries 1 Mark)Darshil MakwanaNo ratings yet
- The Digestive System LabelDocument3 pagesThe Digestive System LabelUSMP FN ARCHIVOSNo ratings yet
- Git Gastric JuiceDocument14 pagesGit Gastric JuiceSibatNo ratings yet
- Acute PancreatitisDocument39 pagesAcute PancreatitisJm Bernardo100% (1)