Professional Documents
Culture Documents
Chapter 6
Chapter 6
Uploaded by
anon_403591710 ratings0% found this document useful (0 votes)
10 views19 pages1. Blood pressure can be measured directly using a pressure transducer connected to an artery or indirectly using a sphygmomanometer.
2. Modern devices use oscillometric or ultrasonic methods to indirectly and automatically measure blood pressure without a stethoscope.
3. Direct electronic manometry involves a pressure transducer connected to a patient's blood vessel via a saline-filled catheter to directly measure pressures like arterial, venous, and pulmonary pressures.
Original Description:
Pressure measurement
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document1. Blood pressure can be measured directly using a pressure transducer connected to an artery or indirectly using a sphygmomanometer.
2. Modern devices use oscillometric or ultrasonic methods to indirectly and automatically measure blood pressure without a stethoscope.
3. Direct electronic manometry involves a pressure transducer connected to a patient's blood vessel via a saline-filled catheter to directly measure pressures like arterial, venous, and pulmonary pressures.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
10 views19 pagesChapter 6
Chapter 6
Uploaded by
anon_403591711. Blood pressure can be measured directly using a pressure transducer connected to an artery or indirectly using a sphygmomanometer.
2. Modern devices use oscillometric or ultrasonic methods to indirectly and automatically measure blood pressure without a stethoscope.
3. Direct electronic manometry involves a pressure transducer connected to a patient's blood vessel via a saline-filled catheter to directly measure pressures like arterial, venous, and pulmonary pressures.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 19
Physiological pressure and cardiovascular
Physiological pressure and cardiovascular
measurements and devices
The nominal values of haemodynamic pressure in the
basic circulatory system are as follows:
basic circulatory system are as follows:
Arterial system: 30 ‐‐ 300 mmHg
Venous system: 5 – 15 mmHg
Pulmonary system: 6 – 25 mmHg
Blood pressure measurements
Blood pressure measurements
• Ph
Physiological fluid pressures: cardiovascular system (Liquid),
i l i l fl id di l t (Li id)
pulmonary system (gas)
• Arterial blood pressure, central venous pressure (CVP),
p , p ( ),
Intracardiac blood pressures, spinal fluid pressures
• Stephen Hales (1773): Used an oen ended tube inserted
directly into an artery in the neck of an unanesthetized
directly into an artery in the neck of an unanesthetized
horse: direct measurement of blood pressure
• Indirect method of measurement: Sphygmomanometer
p yg
• Direct method of measurement: Pressure transducer that is
coupled to the patient’s artery or vein through a saline‐
filled catheter or needle or using Hale’ss method (to
filled catheter or needle, or using Hale method (to
measure spinal fluid pressure and CVP.
• Features:
• Accurate enough for ordinary clinical use
• Simple enough so that even nonprofessional
personnel can be rapidly trained
personnel can be rapidly trained
• Limitation on the ausculatory method include
the hearing acuity of the operator
f
• Several modern instruments are available for
Several modern instruments are available for
the indirect measurement of blood pressure in
by replacement of the stethoscope with an
by replacement of the stethoscope with an
electronic transducer
Pulpation method (indirect method)
• Uses the sense of touch to detect the patient’s
pulse in the radial artery (wrist)
pulse in the radial artery (wrist)
• The cuff is inflated until the radial pulse
disappears
• The operator then slowly releases the pressure in
th
the cuff until a pulse becomes palpable in the
ff til l b l bl i th
radial artery. The pressure at which this occurs is
th
the systolic blood pressure
t li bl d
• The method can detect only the systolic pressure
b
because no known palpable change occurs at the
k l bl h h
diastolic pressure.
Flush method (indirect method)
• Flush technique requires two cuffs and two
operators
• The cuffs are placed on the arm and are inflated.
• The blood in the section between the two cuffs is
h bl d h b h ff
massaged out, leaving the lower arm pale and
bl h d
blanched.
• The pressure in the upper cuff is then released
slowly.
• The pressure at which a sudden red flush is noted
in the blanched skin is recorded as the mean
arterial pressure (MAP)
Limitations of sphygmomanometer
b d
based ausculatory
l measurements
• Measurement is intermittent because it takes
time.
• The Korotkoff sounds are normally in the
range (less than 200 Hz) where human hearing
range (less than 200 Hz) where human hearing
is not very accurate.
A piezo‐resistive pressure
transducer is connected to the cuff.
Features
• Since sound is not used, environmental noise do
not hamper the measurement
h h
• As it does not require a microphone in the cuff,
placement of the cuff is not critical.
• Oscillometric technique is used extensively when
q y
monitoring is needed but it is not desirable when
direct pressure measurements are needed.
• Microprocessor‐controlled approach and design
with periodically inflate and slowly deflate the
p y y
cuff.
Ultrasonic pressure measurements
• A piezoelectric transmitting signal sends a sine‐
wave beam (ultrasound > 20 kHz) into the tissue
wave beam (ultrasound, > 20 kHz) into the tissue
• When it encounters a fluctuating vessel wall,
some of its energy is reflected back
some of its energy is reflected back
(backscattered) to the receive (sensing) crystal
• F
F F( h
F (where Fi h D
F is the Doppler shift) describes
l hif ) d ib
the frequency content of the backscattered wave
• The existence of the F component alers the
circuit in the turbulent flow that corresponds to
Korotkoff
k ff sounds, and it diminishes when near‐
d d i di i i h h
laminar flow resumes (P<Pdiastolic)
Ultrasonic Doppler shift method
If the artery wall is moving towards the transmitter, the apparent frequency f1 is
given by:
(C v)
f1 f
C
where f =transmitted frequency (carrier frequency in the medium)
C =velocity of sound in tissue
v =velocity of vibrating vessel wall
C
f2 f1
C v
The resultant Doppler shift
C (C v) C
f f f2 f f1 f f
C v C C v
2 fv
f
C
OR
2v
f
c
where c wavelength of the carrier frequency in the medium
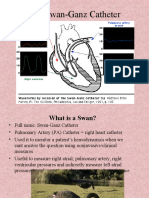
Direct method: electronic manometry
• An electronic pressure transducer can be
connected to the patient through a thin piece
d h i h h hi i
of tubing called a catheter
• The catheter is introduced into the vessel
through a thin hollow tube called a cannula
through a thin, hollow tube called a cannula
• The transducer’s pressure diaphragm is
coupled to the patient’s bloodstream by a
column of saline solution that fills the catheter
How to measure blood pressure
p
• Transducer: a thin, flexible metal diaphragm is
stretched across an opening at one of the
transducer bodyy
• Strain gauges are connected to the diaphragm
• A clear plastic pressure dome fits over the
l l d f h
diaphragm to contain the fluid and provide
hydraulic connection to the catheter
Systolic, diastolic and mean detector circuit
• The pressure amplifier produces an analog
waveform with a peak amplitude representing
waveform with a peak amplitude representing
systolic pressure and a minimum or valley
that represents the diastolic pressure
that represents the diastolic pressure
• Additional circuitry is required that recognizes
these points and from them produces a
these points, and from them produces a
steady voltage or current that can be used to
drive a display meter
drive a display meter
• The MAP (mean arterial pressure) is found by
taking the time average i.e., integrating of the
pressure waveform
Practical problems in pressure monitoring
p p g
• Hydrostatic pressure: The liquid in the transducer plumbing
system has mass, so its weight can apply a force to the
transducer diaphragm that is also interpreted as a pressure
• Positive hydrostatic pressure head caused by the weight of
the fluid in the tubing brought to the transducer from
the fluid in the tubing brought to the transducer from
above
• Negative hydrostatic pressure is obtained when the tubing
i
is predominantly below the level of the transducer
d i tl b l th l l f th t d
diaphragm
• Balancing method the tubing should have approximately
Balancing method the tubing should have approximately
equal lengths above and below the level of the diaphragm
• The diaphragm should be level and at a height equal to the
height from the floor to the catheter tip (not the point
height from the floor to the catheter tip (not the point
where the catheter is inserted
You might also like
- Short Cases in Clinical Exams of Internal Medicine (PDFDrive)Document185 pagesShort Cases in Clinical Exams of Internal Medicine (PDFDrive)Nadhirah ZulkifliNo ratings yet
- Questions For Physiology Practical SpottingDocument15 pagesQuestions For Physiology Practical SpottingHarnarayan Jeev Singh Bajaj100% (3)
- Measurement of Cardiac Output: University College of Medical Sciences & GTB Hospital, DelhiDocument33 pagesMeasurement of Cardiac Output: University College of Medical Sciences & GTB Hospital, DelhioctbudaNo ratings yet
- Unit Ii - Blood PressureDocument31 pagesUnit Ii - Blood PressureNarendra PallavanNo ratings yet
- Blood Pressure. NOTESDocument32 pagesBlood Pressure. NOTESmukisa6ivanNo ratings yet
- Arterial Line: DefiningDocument5 pagesArterial Line: DefiningachyutsharmaNo ratings yet
- Blood Pressure and Flow MeasurementsDocument45 pagesBlood Pressure and Flow MeasurementsJessica DaaboulNo ratings yet
- CCPACatheter Basics 07 MedicineDocument44 pagesCCPACatheter Basics 07 MedicinerinbijoyNo ratings yet
- Presentor DR Manom Konyak (JR) Moderator DR Shashank DhirajDocument52 pagesPresentor DR Manom Konyak (JR) Moderator DR Shashank DhirajManom konyakNo ratings yet
- Invasive Cardiovascular MonitoringDocument47 pagesInvasive Cardiovascular MonitoringMalik MohammadNo ratings yet
- Hemodynamic MonitoringDocument25 pagesHemodynamic MonitoringMichelle Chu100% (2)
- Invasive MonitoringDocument37 pagesInvasive MonitoringHassam ZulfiqarNo ratings yet
- Hemodynamic MonitoringDocument7 pagesHemodynamic Monitoringruhaina malikNo ratings yet
- Biomedical Engineering Ktu Mod 2Document19 pagesBiomedical Engineering Ktu Mod 2Adheeb Shibu VattasserilNo ratings yet
- DR Lakshmi MMM 2009 FINALDocument33 pagesDR Lakshmi MMM 2009 FINALsubha shreeNo ratings yet
- Blood Pressure Using Oscillometric MethodDocument25 pagesBlood Pressure Using Oscillometric Methodنواف الجهنيNo ratings yet
- Blood Flow and It's MeasurementDocument24 pagesBlood Flow and It's MeasurementYanendra SahNo ratings yet
- CVP MonitoringDocument24 pagesCVP MonitoringsofiamansoorNo ratings yet
- Physiologic Monitoring of A Surgical PatientDocument41 pagesPhysiologic Monitoring of A Surgical PatientAlna Shelah IbañezNo ratings yet
- Invasive Arterial Blood PressureDocument31 pagesInvasive Arterial Blood PressureYanti PandianganNo ratings yet
- Monitoring Hemodynamic Utk MahasiswaDocument49 pagesMonitoring Hemodynamic Utk MahasiswaPratami Rieuwpassa IINo ratings yet
- Hemodynamic Monitoring: Course in Pediatric Cardiology, Anaesthesia and Cardiac SurgeryDocument56 pagesHemodynamic Monitoring: Course in Pediatric Cardiology, Anaesthesia and Cardiac SurgerygopscharanNo ratings yet
- Invasive Blood Pressure Monitoring: Presenter: Ramandeep Dhiman (BSC OT, Anesthesia) Moderator: DR GouravDocument40 pagesInvasive Blood Pressure Monitoring: Presenter: Ramandeep Dhiman (BSC OT, Anesthesia) Moderator: DR GouravSonam SonamNo ratings yet
- Lec 2 - Pressure - 1Document31 pagesLec 2 - Pressure - 1Abdallah MahmoudNo ratings yet
- Cardiovascular Monitoring: DR Megha T Assistant Professor Department of AnaesthesiologyDocument47 pagesCardiovascular Monitoring: DR Megha T Assistant Professor Department of AnaesthesiologyShagunNo ratings yet
- Anesthesia MonitoringDocument26 pagesAnesthesia MonitoringBritten Norman SantiagoNo ratings yet
- Unit IIDocument92 pagesUnit IIsanjay.sampath.kNo ratings yet
- 2 Hemodynamic Theory On SICPDocument62 pages2 Hemodynamic Theory On SICPantoni_gamundi3942No ratings yet
- Flowdynamics GovindDocument74 pagesFlowdynamics Govindgovind rajNo ratings yet
- PPT8 BP MeasurementDocument28 pagesPPT8 BP MeasurementtanmayeeNo ratings yet
- Doppler Echocardiography: Dr.S.R.Sruthi Meenaxshi MBBS, MD, PDFDocument38 pagesDoppler Echocardiography: Dr.S.R.Sruthi Meenaxshi MBBS, MD, PDFsruthimeena6891No ratings yet
- ICP MonitoringDocument55 pagesICP MonitoringMaddox EdeyajNo ratings yet
- Hemodynamicmonitorig 160407141401Document96 pagesHemodynamicmonitorig 160407141401abeer alzhoorNo ratings yet
- Thoracic AngiographyDocument78 pagesThoracic Angiographyskjdef kjsebfNo ratings yet
- McLintic W23 Measurement and MonitoringDocument46 pagesMcLintic W23 Measurement and MonitoringdemiluneNo ratings yet
- Hemodynamics in The Cath Lab 2Document45 pagesHemodynamics in The Cath Lab 2usfcards100% (1)
- Blood Flow MeterDocument36 pagesBlood Flow MeterN.G.PRAVEENANo ratings yet
- Clinical Measurement: Prof. Serban Bubenek MDDocument43 pagesClinical Measurement: Prof. Serban Bubenek MDBogdan CarabasNo ratings yet
- Velocity of Blood Flow in Normal Human Venae CavaeDocument11 pagesVelocity of Blood Flow in Normal Human Venae CavaeNguyen Huynh SonNo ratings yet
- Central Venous PressureDocument3 pagesCentral Venous Pressureretta1234No ratings yet
- Blood Pressure MeasurementDocument29 pagesBlood Pressure MeasurementSam SNo ratings yet
- Hemodynamic Monitoring I ABP CVP AoDocument35 pagesHemodynamic Monitoring I ABP CVP AoNofilia Citra CandraNo ratings yet
- Cardiovascular Physiology DR AnjilaDocument167 pagesCardiovascular Physiology DR AnjilaJacob MasikaNo ratings yet
- MonitoringDocument45 pagesMonitoringضبيان فرحانNo ratings yet
- Hemodynamic MonitoringDocument4 pagesHemodynamic Monitoringgurneet kourNo ratings yet
- Central Venous Preasure: By: Engkus Kusnadi, S.Kep., M.KesDocument26 pagesCentral Venous Preasure: By: Engkus Kusnadi, S.Kep., M.KesShofarie AhmadNo ratings yet
- Hemodynamic MonitoringDocument39 pagesHemodynamic MonitoringNor Jeannah PolaoNo ratings yet
- Instrumentation For Mechanics of BreathingDocument59 pagesInstrumentation For Mechanics of BreathingAnonymous hMC57ukNo ratings yet
- Hemodaynamic Monitoring KHDocument91 pagesHemodaynamic Monitoring KHomar kmr97No ratings yet
- CVP 3rd YearDocument11 pagesCVP 3rd YearChonkayshek Rias BarrunNo ratings yet
- Physiomonitoring TransDocument4 pagesPhysiomonitoring TransAimie DagaleaNo ratings yet
- Central Venous PreasureDocument22 pagesCentral Venous PreasureD ZamiatNo ratings yet
- MonitoringDocument128 pagesMonitoringShahzada irfanNo ratings yet
- Central Venous Preasure: By: Engkus Kusnadi, S.Kep., M.KesDocument22 pagesCentral Venous Preasure: By: Engkus Kusnadi, S.Kep., M.KesNenazNaziahNo ratings yet
- Jurnal HemodinamikDocument16 pagesJurnal HemodinamikFauziatul RiyadaNo ratings yet
- Cardiac Output and Hemodynamic MeasurementDocument29 pagesCardiac Output and Hemodynamic Measurementdeepa100% (1)
- Central Venous Pressure and Central LinesDocument13 pagesCentral Venous Pressure and Central Linesaims2099No ratings yet
- Questions and Answers in Small Animal AnesthesiaFrom EverandQuestions and Answers in Small Animal AnesthesiaLesley J. SmithNo ratings yet
- Perfusion for Congenital Heart Surgery: Notes on Cardiopulmonary Bypass for a Complex Patient PopulationFrom EverandPerfusion for Congenital Heart Surgery: Notes on Cardiopulmonary Bypass for a Complex Patient PopulationRating: 5 out of 5 stars5/5 (2)
- Patient'S Peripheral Arterial Disease Risk FactorsDocument2 pagesPatient'S Peripheral Arterial Disease Risk FactorsKrystel BatinoNo ratings yet
- Assessing Peripheral Vascular System222Document12 pagesAssessing Peripheral Vascular System222mahmoud fuqahaNo ratings yet
- 實脈 Shi Mai ExcessDocument4 pages實脈 Shi Mai ExcessEthan KimNo ratings yet
- Vicorder PWA-PWV Pres 15-04 EnglDocument79 pagesVicorder PWA-PWV Pres 15-04 EnglHatem FaroukNo ratings yet
- Application of Roy's Adaptation Model PDFDocument6 pagesApplication of Roy's Adaptation Model PDFTINJU123456100% (1)
- P.E. and Health 11 - First Quarter ExaminationDocument6 pagesP.E. and Health 11 - First Quarter ExaminationVhannie Acquiatan100% (3)
- Aqa Biol1 QP Jan13Document20 pagesAqa Biol1 QP Jan1307dopedNo ratings yet
- Theory ManualDocument34 pagesTheory ManualShalini BaggaNo ratings yet
- Aortic Stenosis Differential DiagnosisDocument12 pagesAortic Stenosis Differential DiagnosisCristina PorfireNo ratings yet
- Life Orientation Today Grade 7, Learner's Book by Euvrard, GeorgeDocument169 pagesLife Orientation Today Grade 7, Learner's Book by Euvrard, GeorgeToheeda SheikNo ratings yet
- Datascope Passport 2, 2LT Monitor - User Manual PDFDocument208 pagesDatascope Passport 2, 2LT Monitor - User Manual PDFpaolaNo ratings yet
- Patient Care PDFDocument310 pagesPatient Care PDFCindy BonghanoyNo ratings yet
- Rheumatic Fever and Rheumatic Heart DiseaseDocument132 pagesRheumatic Fever and Rheumatic Heart DiseaseDamie FernandezNo ratings yet
- General Principles of Physical ExaminationDocument6 pagesGeneral Principles of Physical ExaminationPhysiotherapist AliNo ratings yet
- CSI Physical ExamDocument3 pagesCSI Physical ExamSympaschoNo ratings yet
- Cardiovascular Examination: Preparation of The PatientDocument4 pagesCardiovascular Examination: Preparation of The PatientLolla SinwarNo ratings yet
- 04 Vital Signs AssesmentDocument20 pages04 Vital Signs AssesmentChristine SangilNo ratings yet
- Cdin 2 ReviewerDocument12 pagesCdin 2 ReviewerJulie Loraine PigarotNo ratings yet
- Unani Pulse DiagnosisDocument10 pagesUnani Pulse DiagnosisYa Sayyadi BilalNo ratings yet
- Anatomy Lecture Notes Unit 7 Circulatory System - The Blood Vessels-1Document10 pagesAnatomy Lecture Notes Unit 7 Circulatory System - The Blood Vessels-1hungerfighterNo ratings yet
- Circulatory System LabDocument3 pagesCirculatory System LabMatt Joseph CabantingNo ratings yet
- Smart Real Time Health Monitoring System Using ArduinoDocument5 pagesSmart Real Time Health Monitoring System Using ArduinoSDS PRIORNo ratings yet
- Suggest Fluid Responsiveness: Pulse Pressure Variation (PPV) Cardiac Arrest UtilityDocument1 pageSuggest Fluid Responsiveness: Pulse Pressure Variation (PPV) Cardiac Arrest Utilityabobader2100% (1)
- KC 1 ADocument58 pagesKC 1 AKrishna JaiswalNo ratings yet
- Letters To The Editor: Arterial Pulse Wave Velocity and Heart RateDocument3 pagesLetters To The Editor: Arterial Pulse Wave Velocity and Heart RateBinod KumarNo ratings yet
- Lesson 1.1Document4 pagesLesson 1.1Jemarie LagadoNo ratings yet
- 0610 s09 QP 6Document12 pages0610 s09 QP 6Kassem Farhat0% (1)
- Clinical Skills CHESS Book 2018Document119 pagesClinical Skills CHESS Book 2018ibra musaNo ratings yet