Professional Documents
Culture Documents
Ortho Summary PDF
Ortho Summary PDF
Uploaded by
jhoey83Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Ortho Summary PDF
Ortho Summary PDF
Uploaded by
jhoey83Copyright:
Available Formats
ORTHO SUMMARY NOTES
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
GENERAL PRINCIPLES
EXAMINATION AND TREATMENT
Analgesia
Assessment of distal neurovascular status
Splinting
Definitive management
Infection control –in compound, delay in debridement of 8 hrs, delay in antibiotic of 3
hrs
COMPLICATIONS OF FRACTURES
PROBLEMS RELATED TO FRACTURE
Injuries to nerves, blood vessels, tendons, viscera, Compartment syndrome, Infection
Fat embolism
FAT EMBOLISM
Follows fractures of femur, tibia, fibula more commonly.
Fat globules embolise to pulmonary vasculature and systemic circulation,
appear in the usrine within 3 days in 50%.
Symptoms appear in 12-24 hours post injury
-petechiae, ARDS, headache, confusion, seizures, coma
Treatment – supportive
DISORDERS OF UNION
SLOW -slower than normal
DELAYED -slow healing with little calculus formation
NON-UNION -sclerotic bone or failure of cellular activity- defined by 4 months
MAL-UNION -union in unacceptable position
TRAUMATIC EPIPHYSEAL ARREST
PROBLEMS OF IMMOBILISATION
Venous thrombosis, pneumonia, bed sores, UTI, osteoporosis, mm wasting, renal
calculi.
COMPLICATIONS OF TREATMENT
SURGERY - Wound and anaesthetic complications.
Stiffness, , OA,
Sudecks atrophy(reflex sympathetic dystrophy)
-sympathetic response of unknown cause resulting in pain, swelling and
reduced mobility.
Tender, warm, sweaty.
Treatment- mobilisation and physiotherapy, consider regional sympathetic
blockade
Avascular necrosis
Idiopathic- Keinbock’s disease of lunate, Perthe’s disease
Traumatic-NOF, scaphoid, lunate, talus, anatomical neck of humerus
Associations- DM, steroids, irradiation.
Myositis ossificans, Tendon rupture.
POP
Movement, abrasions, grases, ischaemic limb,Volkman’s ischaemic contractures late.
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
FRACTURES WITH NERVE INJURIES
INJURY NERVE
Shoulder dislocation Axillary
Humerus Radial
Supracondylar Median
Elbow dislocation Ulnar
Radio-ulnar Post interosseous
Colles Median
Lunat dislocation Median
Base of skull Vestibulocochlear, facial
Maxillary Infraorbital
Post hip dislocation Sciatic
Fibula neck Common peroneal
Spinal fractures
Sacral fractures
PLASTER OF PARIS
Ca sulphate, exothermic reaction, hardens by crystalisation.
80% strength in 1 hour, 100% at 24hours
Give plaster instructions to all.
Plaster check within 24 hours- check limb, plaster, patient.
Split plaster if too tight.
FIBREGLASS CASTS
Lighter, more moisture resistant, more expensive, underlay still gets wet and smelly.
COMPOUND FRACTURES
Fractures can be classified according to amount of laceration and amount of non
viable tissue. From Grade 1 – 3 with Grade 4 being total or subtotal amputation.
The MESS(mangled extremity severity score), is used to predict amputation in severe
lower limb trauma. A score of ≥ 7 has 100% chance of amputation
MANAGEMENT
Reduce exposed bone and then reduce any other fractures causing vascular
compromise.
Pack wound
Antibiotcs Cephalothin, add gentamicin for more severe 1.5 mg/kg
Tetanus prophylaxis
Definitive operative treatment within 6 hours
PREHOSPITAL LIMB AMPUTATION
Consensus between two senior medical staff, patient may be able to consent.
Optimise haemodynamics
Anaesthesia- regional in lower limb otherwise, Ketamine 2mg/kg and
benzodiazepines
Arterial torniquet
Amputate through lowest possible level of limb, with transverse cut.
Pack stump with sterile saline packs and bandage.
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
BONE TUMOURS
Metastatic more common – lung, kidney, breast, prostate, thyroid, colon, adrenal,
myeloma, neuroblastoma, Ewing’s sarcoma.
Common sites are: spine, ribs pelvis, humerus, femur, rare below knee/elbow
Malignant primary Benign tumours
Aneurysmal bone cyst Simple bone cyst
Osteosarcoma Prox tibia, humerus, femur
Chondrosarcoma Chondroma
Giant cell sarcoma Tubular bones not flat bones
Ewing’s tumour Osteochondroma
Paget’s sarcoma Metaphysis of long bone
Irradiation sarcoma Osteoid osteoma
Femur, tibia- bony sclerosis
Chondroblastoma
Epiphysis of long bone
Radiological features
Poorly defined margin
Absence of surrounding sclerosis
Break in cortex
Periosteal reaction
FRACTURES WITH NAMES
CERVICAL SPINE UPPER LIMB LOWER LIMB
Hangman’s Hume Tillaux
Bilat pedicles C2 Prox ulna fract, ant Avul frac tibia at inf
Clay shoveller’s disloca radial head Tibiofib joint
Avulsion spinous proces Monteggia Potts
Jefferson Fract ulna rad disloc Malleoli fract
Burst fracture C1 Galleazi Maisonneuve
Frac rad, rad-uln disl Frac fibula neck and dist
Colles T-F jnt ant lig rupture
Dist rad frac dors angul Dupuytren
Smiths Frac dist fibula, rupt
Dist rad volar angul Medial lig
Barton’s March
Ant part of rad Stress frac 2nd met head
Bennett’s Jones
st
Frac, disl, base 1 met Trans frac base 5th met
Boxer’s
Frac 5th met neck
Mallet finger
Avul frac EDL
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
UPPER LIMBS
SHOULDER INJURIES
CLAVICLE
Most fractures occur at the junction of the middle and outer third. These only need
sling. Fractures of the outer third with ligamentous damage may require ORIF.
Neer classification I fracture lateral to coracoclavicular ligament
II fracture through conoid and trapezoid ligaments- ORIF
III intra-articular- conservative treatment
SCAPULA
Due to direct trauma. May be associated with chest injuries.
Sling and early mobilisation.
STERNOCLAVICULAR JOINT DISOCATION
Anterior
Commonest and due to direct trauma. Treat in sling for 2-3 weeks.
Posterior
Emergency due to the pressure on the great vessels. Need CT and reduction under
GA.
ACROMIOCLAVICULAR JOINT INJURIES
Usually due to direct trauma to the point of the shoulder. Stress Xrs may be needed.
1st degree No subluxation; AC lig partly torn
2nd degree Subluxation. AC lig torn conoid and trapezoid intact.
3rd degree Complete disruption. Sling 4-6 wks, consider ORIF.
BICIPITAL RUPTURE
Rupture of long head of biceps with sudden elbow flexion.
Results in weakness in supination.
Treated conservatively, but consider OR. If insertion into radial head is ruptured then
OR.
ROTATOR CUFF INJURIES (supraspinatus, infraspinatus, subscapularis, teres
minor)
Due to chronic deterioration, or acute rupture secondary to shoulder dislocation, ie
57% of first dialocations in <40yo. Supraspinatus most commonly involved.
Clinical
Pain, loss of power in flexion, abduction and ext rotation, local atrophy, bruising.
Abduction occurs via scapular rotation and is limited to 90 degrees.
Investigate with ultrasound. Plain XR to exclude fractures
Treatment
Rest, anti-inflammatories, physiotherapy, consider operative repair.
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
SHOULDER DISLOCATION
ANTERIOR
95% are anterior and due to fall with external shoulder rotation.
There are 4 types of anterior dislocation:
1 Subcoracoid-commonest; head displaced ant to glenoid and inf to
coracoid
2 Subglenoid; humeral head inferior and anterior to glenoid fossa.
3 Subclavicular; head is medial to coracoid, below clavicle
4 Intrathoracic; rare- head between ribs and thoracic cavity.
Clinical
Pain. Shoulder “squared off”, arm in slight ABD and ext rotatn. Pt resists ADD and
int rotation. Test axillary nerve damage- pinprick over skin of the deltoid.
Treatment
Reduction- 6 methods
1 Hippocratic; pt supine, arm abd, elbow flexed 90 degrees-traction
2 Milsch: abd and ext rotation to the overhead position whist traction applied
3 Stimson: Prone, 5kg weight hanging after analgesia- takes 20-30min
4 Scapular rotation: prone, hang weight and push tip medially
5 Kocher’s: arm add, ext rotated and int rotated- painful, risk of tears to inf
capsule
Immobilisation
-first dislocation- 4-6 weeks, recurrent few days.
>40yo- 14% recurrence, <20 90% will have recurrence.
Complications
1 Vascular injuries-rare-axillary artery. Absent radial pulse.
2 Bony injuries
a. Humeral head
i. Hill-Sachs deformity- compression fracture of the humeral
head at posterolateral articular surface. Common in recurrent
dislocations. Seen on AP film in ext rotation.
ii. Greater tuberosity
b. Anterior glenoid lip
i. Bankart lesion – avulsion anterior glenoid labrum, tear ant
capsule.
3 Neurological injuries: in 10-25%- traction injury of axillary nerve- repair
4 Soft tissue injuries
POSTERIOR
Rare, 1% of dislocations, associated with high voltage electrocution, epilepsy. The
most common position is, where the head is behind the glenoid and beneath the
acromion.
Clinical
Arm ADD and INT rotated, pt doesn’t allow abd and ext rotation. There is prominent
coracoid process, and the ant shoulder is flat and the posterior shoulder is full.
Treatment
Reduction
Traction on the adducted arm with an assistant pushing the head anteriorly.
Immobilisation – in sling
Complications
Neurovascular- complications are less common than anterior.
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
INFERIOR – Luxatio erecta
Rare, due to hyperabduction force. The head dislocates inferior to the glenoid, and the
arm is held in abduction.
Treatment
Reduction- Traction on abducted arm – may need OR.
Complications
Rotator cuff always detached, head buttonholed through the inf capsule.
ANTERIOR vs POSTERIOR dislocations
ANTERIOR POSTERIOR
Position of arm ABD, EXT rotated ADD, INT rotated
Patient resists Opposite of above Opposite of above
Shoulder shape Squared off Post shoulder full,
coracoid prominent
XR-Y view-head position Anterior Posterior
HUMERAL FRACTURES
SHAFT
Examine the radial nerve
Middle third fractures more likely to have complications with radial nerve palsy, and
non-union
MANAGEMENT
Analgesia
Gentle traction to reduce, and U slab, collar and cuff
Internal fixation if: -Radial nerve palsy in original fracture of after manipulation
-≥ 2 fractures in one limb
-bedridden
PROXIMAL FRACTURES
Impacted -broad arm sling, mobilise after 2 weeks, physio 6 weeks
Unimpacted -accept in elderly GAMP all others
There is a Neer classification I – VI
Anatomical neck fractures > 1cm displacement leads to avascular necrosis- fixation
FOREARM FRACTURES
MIDSHAFT
Both bones usually fractured, need XR of entire arm as may be other fractures.
POP, closed, ORIF, depends on displacement.
MONTEGGIA Monteggiaaaaaaa = ulnaaaaaaaa
Fracture of proximal 1/3 of ulna, and dislocated radial head
ORIF in adults, GAMP in children.
GALEAZZI
Fracture midshaft radius, with distal radioulnar joint, dislocation.
ORIF
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
WRIST INJURIES
COLLE’S FRACTURE
- Fracture of distal radius with dorsal angulation and displacement, and radial
angulation
Indications for Reduction
1 Displacement of ulnar styloid- indicated serious disruption of inferior
radio-ulnar joint
2 Deformed external appearance
3 Dorsal tilt >10 degrees
Method of reduction
Bier’s block or general anaesthesia
Traction – extension – flexion – ulnar deviation
POP for 6 weeks
Complications
1 mal-union/non-union
2 median nerve compression
3 stiffness
4 ext pollicis longus rupture – due to interruption of vascular supply
a. accept in elderly, but need tendon transfer in young
5 Sudeck’s atrophy
i. Osteoporotic changes when the patient comes out of plaster.
ii. Fingers are swollen
iii. Restricted finger flexion
iv. Wrist and hand warm and tender
SMITH’S FRACTURE
Almost opposite to colle’s, Fall onto back of hand
Radial fracture with radial fragment angulated and displaced anteriorly
Method of reduction
Traction in supination with wrist extension. POP in wrist extension – 6 weeks
BARTON’S FRACTURE
Type of Smiths, but only the anterior portion of radius involved, fracture into joint
space.
Reduce as for Smith’s otherwise ORIF
HENDERSON FRACTURE
Radial styloid fracture, usually not displaced. Treat with Colle’s plaster.
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
SCAPHOID
FRACTURES
Tenderness in anatomical snuffbox, and on axial compression of thumb.
Fracture frequency is 50% mid, 38% prox, 12% distal
Scaphoid POP for 6 weeks. If clinical suspicion only, need re-XR in one week.
If displaced need surgery.
If tubercle fracture only then symptomatic treatment.
Complications -avascular necrosis -50% if >1mm displacement
-Incidence increases, the more prox the fracture
-never with tubercle fractures.
-non-union - in 50% if >1mm displacement.
SCAPHOID SUBLUXATION/DISLOCATION
Usually posterior: Proximal pole subluxes dorsally, distal pole anteriorly.
To reduce wrist in palmar flexion, pressure over dorsum if posterior.
Anterior is less common, but if occurs reduce as for lunate dislocations.
POP?????
LUNATE
FRACTURE
Uncommon, but at risk of avascular necrosis, scaphoid POP and review.
DISLOCATION
Most common of carpal dislocations.
Threat to median nerve, and at risk of avascular necrosis.
May dislocate dorsally or volarly, concavity faces volar aspect of hand.
Reduction by compression over lunate, whilst wrist extended and flexed.
PERILUNATE DISLOCATION
Lunate still attatched to radius, carpus dislocates around this, reduce by traction.
TRANS-SCAPHOID PERILUNATE DISLOCATION
Second most common carpal dislocation.
Distal scaphoid fragment displaces posteriorly with the rest of the carpal bones.
Reduction by traction and scaphoid POP. What happens to lunate?????????????
OTHER CARPAL FRACTURES
Rare, and only need symptomatic treatment.
Chip fractures – usually of triquetral, due to hyperflexion/extension injury.
DEQUERVAIN’S TENOSYNOVITIS
Inflammation of EPB and AbdPL sheaths due to excessive use of thumb.
Pain along radial aspect of wrist.
Finklestein’s test- pt grabs examiners thumb, and examiner ulnar deviates pt’s hand.
Pain occurs over tendons. Confirms diagnosis.
Treat with splint, NSAIDS, physiotherapy.
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
HAND INJURIES
The aim is conservation of function
Metacarpals
5th -fracture through the neck secondary to punching injury
-accept 30 degree angulation, otherwise reduce under ulnar or Bier’s block
-U-slab and sling, but may need K wire if unstable
Other -Rotation is the major problem. Make fist all fingers should point to scaphoid
-accept upto 15 degrees angulation
-colle’s POP for 3-4 weeks, may require reduction and internal fixation
Phalanges
-reduce displaced or rotated fractures, buddy strap for 2 weeks unless mallet
-Mallet = cannot extent DIP joint due to ext digitorum tendon avulsion
- mallet finger splint and immobilization for 6 weeks
-Dislocations- usually posterior, exclude fracture, buddy splint 3-4 weeks
In metacarpo-phalageal dislocations reduce, buddy strap, amy need
ORIF
Thumb
Bennett’s fracture
-fracture-dislocation of carpo-metacarpal joint of thumb
-reduce with traction and abduction
-scaphoid POP with pressure over base of thumb, may need K-wire
Gamekeeper’s thumb
-disruption of the ulnar collateral lig of MP joint of thumb
-if >20 degrees = disruption – compare with other side, stress views
-scaphoid POP if mild, but most need ORIF
Post dislocation of 1st MCP joint
-hyperextension injury in children
-metacarpal head may button-hole through joint capsule
-reduction and POP 3weeks
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
LOWER LIMBS
PELVIC FRACTURES
In 30% of multiply injured patients. 50% require transfusion. Most due to MCA’s or
simple falls in the elderly.
Structures at risk
-Vascular -common iliac divides at sacroiliac joints, int iliac is
intrapelvic, sup gluteal is at greater sciatic foramen
-Neuro - lumbar and sacral plexus
-Other -bladder, bladder neck, urethra
-sigmoid colon, rectum, anus
-vagina, cervix,uterus, seminal vescicles.
CLASSIFICATION OF FRACTURES
Multiple classifications based of anatomical, radiological, mechanism of injury
Key and Cornwell classification
Type I- No break in pelvic ring, stable, eg single ramus, avulsion ASIS
Type II- Single break in rim, stable, eg ipsil rami fractures.
TypeIII- Double break in ring, unstable, STI
TypeIV- Acetabular fractures
Bucholz Classification
Type I solitary fracture of pubic ramus mortality 10%
Type II pubic rami and sacroiliac fracture, no widening. Mortality 25%
Type III sacroiliac joint displacement. Mortality 40% for open injuries
Young Classification (shock-trauma classification)
Lateral Compression fractures
I compression of sacrum on side of impact- most common by far(50%)
II iliac wing fracture at anterior border of sacroiliac joint
III cont open book injury
Anterior posterior fractures
I symphysis diastasis, slight widening of sacroiliac joint
II widening of anterior sacroiliac joints, open book injury, lumbosacral plexus and
vessels involved
III complete disruption of hemipelvis without vertical displacement
Vertical shear fractures
Anterior injury with hemipelvis displaced superiorly
AVULSION FRACTURES
ASIS avulsed by sartorius in athletes- crutches for 2 weeks.
AIIS by rectus femoris
Post spine by erector spinae
Ischial tuberosity avulsed by hamstrings
Iliac crest by direct violence
All need only symptomatic treatment.
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
ACETABULAR FRACTURES
Due to transmission of force through radial head, ie as a result of dislocation.
Treat with skin traction.
CLINICAL SIGNS
Pain, tenderness, haematoma, pain on pelvic springing.
Destot’s sign- haematoma above inguinal ligament or in scrotum
Roux’s sign- Distance between greater trochanter and pubic symphysis unequal
Earle’s sign- tender fracture line palpable on rectal examination.
WHO TO XR?
Xray No Xray
Altered mental state GCS<14 Alert, orientated, no pelvic pain, not
Unexplained hypotension under the influence of alcohol or drugs
Positive examination Normal examination
No femoral fracture
OTHER RADIOLOGY
CT SCAN PELVIS
Good for complex pelvic injuries, better for acetabular and rami fractures.
Doesn’t change management.
Not reliable for bladder injuries
CYSTOGRAM
Not in microscopic haematuria, but in macroscopic 30% have lower urinary tract
injury.
MANAGEMENT OF PELVIC FRACTURES
A B C, cervical spine, oxygen, fluid resuscitation, investigations etc..
Stabilise fracture – MAST suit, int, ext fixation.
LC I and II – bed rest, delayed ORIF, if instability or bleeding ext fixation
APC II, III, VS – acute ext fixation in first 4 hours.
Angiography and Embolization
If continued blood loss and other sources excluded. After ext reduction/fixation.
Patient must be stable. Only detects direct arterial bleeding in 10%
Surgery
Major visceral or vascular damage, ongoing blood loss, open fractures
COMPLICATIONS
1 Haemorrhage-up to 6L, major cause of death, MAST suit, mechanical
fixation, embolisation.
2 Bladder injuries-ruptured dome or body or neck
3 Urethral injuries- in 5% of fractures. Twice as common as bladder injuries.
Pubic ramus and sacroiliac involvement make it more likely. Blood at
meatus, high riding prostate. Suprapubic. Retrograde urethrogram.
4 Gynaecological- uncommon. Vaginal lacerations most common. High
foetal death rate
5 Rectal injuries- uncommon
6 Neural- S1,2 commonly damaged, lumbosacral plexus. Impotence in 1/6
7 Diaphragmatic- avoid MAST
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
FEMORAL FRACTURES
SHAFT
High forse is needed, usually MCA.
Range from undisplaced to compound.
Complications are: -haemorrhage up to ≥2L of blood
-fat embolism risk if not treated for >24hours.
MANAGEMENT
A B C , Oxygen, aggressive fluid resus
Analgesia -parenteral, femoral block
Immobilisation -Thomas splint / Donway splint
Internal fixation for adults, gallows traction for children.
SUPRACONDYLAR FRACTURE
In adults tend to rotate, may be comminuted.
ORIF
KNEE INJURIES
COLLATERAL LIGAMENT
Test stability at 30°, if only painful but not lax = strain. If lax repeat in full extension.
If lax at full extension= serious injury, collat, cruciates, post capsule damaged.
CRUCIATE LIGAMENT
ANTERIOR
Most common, 70% of haemarthroses. Due to non-contact rotational injury.
Lachman test –knee flexed to 20°, tibia lifted upwards. 95% sensitive.
Anterior draw sign –knee flexed 45°, tibia pulled forward, 60% sensitive.
Pivot shift test –Complex-knee flexed with tibia in int rotation, lateral tibial
epicondyle subluxes anteriorly but relocates with a jerk, 70% sensitive.
Knee arthrometer –95% sensitive if 3mm displacement occurs.
POSTERIOR
Blow to leg with flexed knee ie., motorcycle/dashboard injury, associated with hip
injuries and femoral and tibial fractures. Posterior draw test maximal at 90°.
MANAGEMENT
Grade 1 No fibre disruption – conservative treatment.
Grade 2 Part ligament failure-conservative Rx, mobilise 6 wks, > for cruciates
Grade 3 Complete disruption- repair dependant on several factors
Surgical repair depends on:
Number of ligaments injured, instability of joint
Age and activity of patient
Time post injury- early repair better, >2 weeks difficult
Open repair –6 month disability, arthroscopy- 3 months.
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
MENISCUS
Medial more common- locking, medial joint tenderness, effusions and anterior joint
pain on activity, McMurray and Grind test +ve in 50%
If locked- urgent arthroscopy.
PATELLA
FRACTURES
May be transverse, comminuted or avulsion. Difficult to straight leg raise.
Undisplaced- zimmer or POP, displaced- ORIF, comminuted- excision.
DISLOCATION
Twisting on extended knee or direct blow, dislocates laterally over lateral condyle.
Extend knee and reduce manually. POP/zimmer 2-4 weeks then mobilise.
PROXIMAL TIBIA
TIBIAL PLATEAU FRACTURES
Tibial plateau driven into tibial condyles, lateral condyle more commonly.
Lipohaemarthrosis-fat-fluid level on supine lateral may be only sign- indicates bony
injury communicating with marrow space.
Treatment : depressed fractures may need elevation other?????????
SEGOND FRACTURE OF PROXIMAL TIBIA
Small avulsion fracture, 13mm usually undisplaced, proximal lateral tibia- associated
with severe internal disruption of the knee. Signifies tear of the menisco-tibial
attatchment of middle third of lateral capsular ligament.
All have anterior cruciate, majority have meniscal tears.
OTHER
KNEE DISLOCATION
Severe injury, both cruciates are torn and hinges around one collateral ligament.
Popliteal artery at risk. High incidence of amputation if delayed > 6hours. If arterial
supply impaired after reduction then angiography required.
High incidence of compartment syndrome.
QUADRICEPS TENDON RUPTURE
Divot in thigh proximal to patella, cannot straight leg raise. Surgical repair.
HAEMARTHROSIS OF THE KNEE
ADULTS ADOLESCENTS
Osteochondral fractures –10% Osteochondral fractures -60%
70% with no fracture have ACL ACL – 10%
20% collateral ligament Meniscal tears 50%
9% posterior cruciate 50% have intra-articular FB at
arthroscopy
50% have normal Xray
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
WHO TO XRAY WITH KNEE INJURIES
≥ 55yo
tenderness head of fibula
isolated tenderness of patella
can’t flex knee to 90°
Inability to weight bear – immediately and at assessment – 4 steps
100% sensitivity for significant fractures, 49% specific
Decreases Xray by 25%
TIB / FIB FRACTURES
TIBIA
Look for associated fibula fractures
Treatment varies and ranges from conservative to closed reduction,ORIF, rods.
Complications are infection, compartment syndrome, neurovasc injury, non-union.
Nutrient artery runs at junction of upper and middle thirds.
FIBULA
Isolated fractures are uncommon- look for the tibial fracture.
In fractures of the tibial head peroneal fractures are common.
Isolated fractures are treated with below knee walking plaster for 6 weeks.
ANKLE INJURIES
Indications for XR
1 pain in malleolar zone and
2 unable to take 4 steps in ED (Ottawa ankle rules)
3 bone tenderness distal 6cm or distal tip of malleolus
FRACTURES and TREATMENT –Classified as Pott’s fractures
1 Unimalleolar
a. If stable – crepe bandage
b. If unstable – below knee POP for 6 weeks
2 Bimalleolar - ORIF
3 Trimalleolar- lat, med, post tibial – ORIF
Other indications for OR are, talar shift, displaced fragments
Xr may show avulsion fracture but if < 3mm treat as ligamentous
DISLOCATION
May dislocate and relocate with no bony injury. Need to relocate rapidly to avoid
vascular compromise.
POP for 6 weeks, may need ORIF
ACHILLES TENDON RUPTURE
Due to forceful dorsiflexion of foot. There is sudden pain and a snap.
Unable to walk or stand on toes. Calf squeeze or Thompsons test fairly accurate.
Treatment
Conservative All < 48hrs
Long leg plaster – knee at 45°, ankle plantar flexed at 45° for 4 weeks
Operative- if young and detected early or if > 1 week
LIGAMENTOUS INJURIES
75% of ankle injuries are sprains, 90% involve lateral ligament.
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
Grade 1
Pain on movement, can weight bear. Partial tear usually of anterior talofibular
ligament.
Grade 2
Pain at rest, limitation of weight bearing. Calcaneofibular ligament involved.
Treatment
R.I.C.E. ( ice 10 min every 2 hours for first 24 hours)
POP if swelling and severe pain
Non-weight bearing for first 24 hours.
Grade 3
Severe pain
Complete tear of two or more ligaments, joint movement on stressing
Needs ankle reconstruction.
CALCANEAL FRACTURES
25% are associated with lower extremity fractures
5-10% associated with spinal fractures.
Fracture type
Crush
Intra-articular
Pain swelling and tenderness over the heel. Lat X-ray may miss. Need Harris(axial)
view.
May need a CT scan to work out how bad it is.
Bohler’s angle- Good to pick up occult fracture. Normal is 25-40° If <25 = fracture
Management:
Conservative: Splint , non-weight bearing 6-8 weeks
Surgery: Remove fragments ang provide best position as have best outcome. If
comminuted may not be able to put together.
Functional disability approaches 50%, so make sure you refer early.
Conservative approach: Early consult with ortho surgeon, as outcomes are potentially
so bad.
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
FOOT INJURIES
CALCANEAL FRACTURES
Usually fall from height, landing on feet. Most commonly fractured tarsal bone.
Key factor is if there is involvement of subtalar joint.
There may be other associated injuries- limb(25%), Cx ,lumbar spine(10%).
Boheler’s salient angle- usually 40°- angle decreases.
Several types of fractures- if body fracture or joint involved need screw, otherwise
POP
TALUS FRACTURES
Uncommon, but throughthe neck risk avascular necrosis
METATARSAL FRACTURES
2nd and 3rd
March fractures- relatively fixed prone to stress fractures.
5th
Base-
-inversion injury, avulsion of Peroneus longus.
-Jones- 7 weeks below knee POP , ORIF in athletes, non-union
common
Epiphyseal plate of base of 5th
-fracture usually transverse, symptomatic treatment, crepe or POP.
LISFRANCS FRACTURE/DISLOCATION
Most common midfoot fracture, at tarso-metatarsal joint.
Due to hyperextension of forefoot on midfoot, with dorsal dislocation of tarso-
metatarso joint.
May fracture 1st cuneiform and 2nd metatarsal, this causes 1st metatarsal to separate.
Treatment- Needs accurate reduction, as ongoing pain is a major problem.
NAVICULAR
In isolated fracture – POP for 6 weeks.
KAMIKAZE FELLOWSHIP COURSE www.resus.com.au
You might also like
- Manual Pilates InglesDocument8 pagesManual Pilates InglesRodrigo Alexis Muñoz Ballier0% (2)
- AKUTHOTA, Venu NADLER, Scott 2004 - Core Strengthening (Conceito Core Stabilization)Document7 pagesAKUTHOTA, Venu NADLER, Scott 2004 - Core Strengthening (Conceito Core Stabilization)Rafael Magalhães100% (1)
- ORTHO by Target 200 PlusDocument21 pagesORTHO by Target 200 PlusTMC PGI GENER MICKONo ratings yet
- 7 Question OrthopaedyDocument11 pages7 Question OrthopaedyFadliArifNo ratings yet
- Journal Reading - Angga (English)Document31 pagesJournal Reading - Angga (English)angga andriyantoNo ratings yet
- Upper Limb Fracture 3Document17 pagesUpper Limb Fracture 3vivien kate perixNo ratings yet
- Lect 8 - Internal Fixation - IIDocument21 pagesLect 8 - Internal Fixation - IIAnkit LakshyaNo ratings yet
- Clinical Features and Diagnosis of FracturesDocument43 pagesClinical Features and Diagnosis of FracturesChenna Kesava100% (2)
- 1 Question OrthopaedyDocument15 pages1 Question OrthopaedyFadliArifNo ratings yet
- Ortho Questions 1Document10 pagesOrtho Questions 1Kay BristolNo ratings yet
- Fractures and Dislocations: of The Upper ExtremitiesDocument76 pagesFractures and Dislocations: of The Upper ExtremitiesGabby ElardoNo ratings yet
- Bedah 2 Mei 2019 PDFDocument210 pagesBedah 2 Mei 2019 PDFRinto MangiwaNo ratings yet
- BEDAH 2 - MANTAP Mei 2019 PDFDocument256 pagesBEDAH 2 - MANTAP Mei 2019 PDFZhraaNo ratings yet
- Proximal Femur Fractures: Sulita Turaganiwai s130364Document26 pagesProximal Femur Fractures: Sulita Turaganiwai s130364Wālē NandNo ratings yet
- Amputation and ProstheticsDocument45 pagesAmputation and Prostheticspriyanka0% (1)
- OSCE Stations ChecklistDocument51 pagesOSCE Stations ChecklistAnonymous A0uofxhUNo ratings yet
- Fractures of Spine and Pelvis2007Document70 pagesFractures of Spine and Pelvis2007api-19916399No ratings yet
- Orthopedic NursingDocument46 pagesOrthopedic Nursingposh0038No ratings yet
- Physeal Injuries and Pediatrics Trauma: Dr. Aamar MunirDocument67 pagesPhyseal Injuries and Pediatrics Trauma: Dr. Aamar MunirSeimal MahmoodNo ratings yet
- Frienchzel Joy A. Asis Group 3 BSN 3-ADocument14 pagesFrienchzel Joy A. Asis Group 3 BSN 3-AKenneth Louis GalizaNo ratings yet
- Tumor Flash Cards - Osteochondroma and Multiple Hereditary ExostosisDocument23 pagesTumor Flash Cards - Osteochondroma and Multiple Hereditary Exostosislaxge54No ratings yet
- Fracture: Break in ContinuityDocument13 pagesFracture: Break in ContinuityYohannis AsefaNo ratings yet
- Radioanatomy of The Extremities & Some of The MSK PathologiesDocument114 pagesRadioanatomy of The Extremities & Some of The MSK PathologiesTogodly 07No ratings yet
- 2023 Cavus Foot SurgeryDocument83 pages2023 Cavus Foot SurgerysaragNo ratings yet
- Wrist Injuries (BK)Document5 pagesWrist Injuries (BK)Malueth AnguiNo ratings yet
- Extracapsular NOF #: Sarath Raveendran 2 0 0 7 M B B SDocument14 pagesExtracapsular NOF #: Sarath Raveendran 2 0 0 7 M B B SSarath RaveendranNo ratings yet
- Stressfracture 130423131736 Phpapp02Document33 pagesStressfracture 130423131736 Phpapp02BOT 4th yearNo ratings yet
- Advanced Trauma Life SupportDocument199 pagesAdvanced Trauma Life SupportatikaNo ratings yet
- Fractures: Definition: Break or Discontinuity of The Bone Caused by Trauma or PathologyDocument84 pagesFractures: Definition: Break or Discontinuity of The Bone Caused by Trauma or PathologyJude EdubaNo ratings yet
- S-Malunion and NonunionDocument75 pagesS-Malunion and NonunionshahnazroeentanmailNo ratings yet
- Dislokasi Panggul & BahuDocument42 pagesDislokasi Panggul & BahuAnton TrihartantoNo ratings yet
- Pushed Elbow: Grace Mafel P. Lucero - BSPT 2020Document4 pagesPushed Elbow: Grace Mafel P. Lucero - BSPT 2020keshNo ratings yet
- (Mantap) Slide Materi Bedah-2 Batch 3 2018 PDFDocument200 pages(Mantap) Slide Materi Bedah-2 Batch 3 2018 PDFRonald Shields100% (1)
- Chapter 36Document3 pagesChapter 36Samantha QuintoNo ratings yet
- Upper Extremity FracturesDocument50 pagesUpper Extremity FracturesClexNo ratings yet
- Radiology NotesDocument24 pagesRadiology NotesAaron Raestas0% (1)
- Ongenital Psudoarthosis of Radius Ulna Clavicle Congenital Dislocation Radial HeadDocument43 pagesOngenital Psudoarthosis of Radius Ulna Clavicle Congenital Dislocation Radial HeadClaude M. BrusselsNo ratings yet
- Fracture-Dislocation of The Hip-KaizarDocument69 pagesFracture-Dislocation of The Hip-KaizarKaizar Ennis100% (1)
- Orthopedic Emergencies and Urgencies: Scott Playford LCDR, MC, UsnrDocument49 pagesOrthopedic Emergencies and Urgencies: Scott Playford LCDR, MC, UsnrklokloNo ratings yet
- Fractures of The Upper LimbDocument3 pagesFractures of The Upper LimbJim Jose AntonyNo ratings yet
- Distal End Humerus Fractures: BY:-Dr. Anshu Sharma Guide:-Dr.A.K. MathurDocument76 pagesDistal End Humerus Fractures: BY:-Dr. Anshu Sharma Guide:-Dr.A.K. MathurToàn Đặng Phan VĩnhNo ratings yet
- Gadar OrthoDocument54 pagesGadar OrthoKeu RS Helsa BintaroNo ratings yet
- 01 TraumaDocument37 pages01 TraumaMajid KhanNo ratings yet
- Bedah 2 Batch 3 2018Document87 pagesBedah 2 Batch 3 2018Meiza Ihsan FakhriNo ratings yet
- Pediatric Orthopaedics: Dr. Andreas Siagian SpotDocument66 pagesPediatric Orthopaedics: Dr. Andreas Siagian SpotFirdausi RiskiviawinandaNo ratings yet
- Ortho - Surgery PDFDocument15 pagesOrtho - Surgery PDFIC BNo ratings yet
- Salter Chapter XVIIDocument18 pagesSalter Chapter XVIISamuel Pola Karta SembiringNo ratings yet
- MSK Week 2 Catatan Ci JDASDocument7 pagesMSK Week 2 Catatan Ci JDASFirmanHidayatNo ratings yet
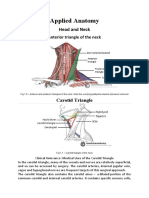
- Applied Anatomy: Head and NeckDocument9 pagesApplied Anatomy: Head and NeckdivinaNo ratings yet
- Thoracic Outlet Syndrome - Shoulder & Elbow - OrthobulletsDocument13 pagesThoracic Outlet Syndrome - Shoulder & Elbow - OrthobulletsSylvia GraceNo ratings yet
- Introduction of MSK ImagingDocument63 pagesIntroduction of MSK ImagingyeabsraNo ratings yet
- Slide MANTAP BEDAH 2 PDFDocument203 pagesSlide MANTAP BEDAH 2 PDFIni DiaNo ratings yet
- Orthopedic Nursing. Lecture Notes at Philipine Orthopedic CenterDocument7 pagesOrthopedic Nursing. Lecture Notes at Philipine Orthopedic Centerhannjazz100% (5)
- Orthopaedic Surgery Study Guide FOR Medical Students, R1S and R2SDocument17 pagesOrthopaedic Surgery Study Guide FOR Medical Students, R1S and R2SlanghalilafaNo ratings yet
- MSS NotesDocument6 pagesMSS NotesSo ÉNo ratings yet
- DR - Rieva Kuliah 7 November - 2018Document38 pagesDR - Rieva Kuliah 7 November - 2018Nisrina100% (1)
- Treatment of Femur FracturesDocument55 pagesTreatment of Femur FracturesMabvuto BandaNo ratings yet
- (Mantap) Slide Materi Bedah-2 Batch 3 2018 SalinanDocument200 pages(Mantap) Slide Materi Bedah-2 Batch 3 2018 SalinantikaNo ratings yet
- Wrist Anatomy: Bones Quiz - What Bones Comprise The Wrist? Joints Quiz - What Joints Comprise The Wrist?Document63 pagesWrist Anatomy: Bones Quiz - What Bones Comprise The Wrist? Joints Quiz - What Joints Comprise The Wrist?Mnn SaabNo ratings yet
- How To Draw Kung Fu Comics by Blixer PDFDocument21 pagesHow To Draw Kung Fu Comics by Blixer PDFAlina-Elena AstalusNo ratings yet
- Iomp 2Document5 pagesIomp 2Yunita ManurungNo ratings yet
- 220200420anand KumarDocument109 pages220200420anand Kumarpriya selvarajNo ratings yet
- Build Your Foundation: Get in Shape - Build Muscle - Lose FatDocument54 pagesBuild Your Foundation: Get in Shape - Build Muscle - Lose FatA MarshNo ratings yet
- BiomechanicsDocument59 pagesBiomechanicsMuqeet76No ratings yet
- Knee Rehab Self Assessment Checklist 2Document32 pagesKnee Rehab Self Assessment Checklist 2darko9No ratings yet
- Ankle JointDocument84 pagesAnkle JointPoojitha reddy MunnangiNo ratings yet
- Screenshot 2024-01-12 at 7.10.04 AMDocument1 pageScreenshot 2024-01-12 at 7.10.04 AMlukeNo ratings yet
- Full Body Exercises: For Stroke PatientsDocument26 pagesFull Body Exercises: For Stroke PatientsVinod VermaNo ratings yet
- Traumatic Extensor Tendon Injuries To The Hand: Clinical Anatomy, Biomechanics, and Surgical Procedure ReviewDocument11 pagesTraumatic Extensor Tendon Injuries To The Hand: Clinical Anatomy, Biomechanics, and Surgical Procedure ReviewJosua LouisNo ratings yet
- Bilateral Knee OADocument35 pagesBilateral Knee OAMu'iz Beatforteen50% (2)
- Baker CystDocument4 pagesBaker CystFitriany LihawaNo ratings yet
- Osteochondroma 150907182521 Lva1 App6891Document22 pagesOsteochondroma 150907182521 Lva1 App6891bucculuNo ratings yet
- Anaphy LecDocument15 pagesAnaphy LecMarcoNo ratings yet
- Orthopedic Physical Examination (DR - Bayu)Document45 pagesOrthopedic Physical Examination (DR - Bayu)Ghisca Chairiyah AmiNo ratings yet
- Ultrasound Guided Lower Limb Blocks Tony AllenDocument39 pagesUltrasound Guided Lower Limb Blocks Tony Allenrepre64No ratings yet
- General Knee Exercises VanderbiltDocument2 pagesGeneral Knee Exercises VanderbiltHolubiac Iulian Stefan100% (1)
- PNF ConceptDocument8 pagesPNF ConceptSolrac Adle B. SevillaNo ratings yet
- 22-Surface Anatomy of The Upper and Lower LimbsDocument24 pages22-Surface Anatomy of The Upper and Lower LimbsMiahz Tv100% (1)
- Hip Arthroscopy Clinical Practice Guideline: Phase I - Initial ExerciseDocument9 pagesHip Arthroscopy Clinical Practice Guideline: Phase I - Initial ExerciseRibeiro FtNo ratings yet
- Osteology of The HeadDocument50 pagesOsteology of The HeadPraiseNo ratings yet
- DislocationDocument12 pagesDislocationAkshata BansodeNo ratings yet
- McGill Et Al. 2009, Exercises For Spine Stabilization Motion Motor PatternsDocument9 pagesMcGill Et Al. 2009, Exercises For Spine Stabilization Motion Motor Patternsok okNo ratings yet
- Growth Relativity Theory With Cover Page v2Document21 pagesGrowth Relativity Theory With Cover Page v2Shubham khandkeNo ratings yet
- Support System and MovementDocument38 pagesSupport System and MovementNinamay FajardoNo ratings yet
- Daftar Pustaka: Universitas Sumatera UtaraDocument3 pagesDaftar Pustaka: Universitas Sumatera UtaraTan SriNo ratings yet
- Traumatic Disorders: Compartment SyndromeDocument57 pagesTraumatic Disorders: Compartment SyndromeMayahati NazayaNo ratings yet
- Sole of Foot, Nerve Injuries1Document65 pagesSole of Foot, Nerve Injuries1Mahmoud AbdulahiNo ratings yet