Professional Documents
Culture Documents
Clindamycin
Clindamycin
Uploaded by
Darwyn Paul DagumanCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Clindamycin
Clindamycin
Uploaded by
Darwyn Paul DagumanCopyright:
Available Formats
Acta Dermatovenerol Croat 2017;25(1):72-76
Case report
Antibiotic-induced Toxic Epidermal Necrolysis –
A Case Report
Tino Klancir1, Višnja Nesek Adam1,2, Martina Matolić1, Elvira Grizelj
Stojčić1, Maja Karaman Ilić1,2
1
Department of Anesthesiology, Reanimatology and Intensive Care, Clinical Hospital
Sveti Duh, Zagreb, Croatia; 2Josip Juraj Strossmayer University of Osijek, School of Medi-
cine, Osijek, Croatia
Corresponding author: ABSTRACT Toxic epidermal necrolysis (TEN) is severe cutaneous hypersensitivity reaction
Višnja Nesek Adam, MD characterized by necrosis of the epidermis and detachment of the epidermis and dermis
that usually occurs as an idiosyncratic reaction to certain drugs. We report the case of a
Žerjavićeva 12
patient admitted to our Intensive Care Unit after an above-the-knee amputation who de-
10000 veloped toxic epidermal necrolysis, possibly resulting from antibiotics therapy. Therapy
Zagreb included a combination of intravenous immunoglobulin with gentle early debridement
Croatia of necrotic skin areas followed by wound coverage with a synthetic cover (Aquacel Ag®).
This case report suggests that intensive wound management together with intravenous
visnja.nesek@hotmail.com immunoglobulin might be beneficial in the treatment of patients with TEN.
Received: May 3, 2016 KEY WORDS: toxic epidermal necrolysis, antibiotics, treatment
Accepted: January 10, 2017
INTRODUCTION
Toxic epidermal necrolysis (TEN) is a severe cu- Necrolysis (SCORTEN) can be used to predict patient
taneous hypersensitivity reaction characterized by outcomes (7). Management of TEN requires prompt
necrosis of the epidermis and detachment of the epi- recognition and immediate withdrawal of all poten-
dermis and dermis followed by fever (1). When less tial causative agents. Although there are no thera-
than 10% of the skin is affected, the condition is called peutic guidelines regarding its management, and
Steven-Johnson syndrome (SJS), and when affected various treatment modalities have been suggested,
skin covers 10%-30% of the body it is called SJS/TEN such as corticosteroids, intravenous immunoglobulin
overlap. TEN is the most severe clinical manifestation therapy (IVIG), cyclosporine, cyclophosphamide, N-
of SJS that affects more than 30% of the patient’s skin. acetylcysteine, plasmapheresis, etc., admission to an
Many groups of medications have been recognized intensive care unit (ICU) or burn center together with
as possible causes (2). Although the exact mechanism supportive measures and wound care are considered
is unknown, it has been suggested that the main crucial in TEN treatment. It is known that adequate
cause of TEN is damage to the metabolic pathway of debridement of necrotic tissue with placement of
the drug being used, which leads to accumulation of wound coverage and admission to a burns or inten-
toxic drug metabolites. These metabolites may have sive care unit improves survival and reduces infection,
direct toxic effects or may act as haptens that interact whereas specific treatment with immunosuppressive
with host tissues (3,4). The incidence is 2-7 cases per drugs, corticosteroids, or immunoglobulin did not re-
million, and mortality rates range from approximate- sult improved outcomes in most studies and remains
ly 20% to 60% (5,6). The Score for Toxic Epidermal controversial (8).
ACTA DERMATOVENEROLOGICA CROATICA
72
Klancir et al. Acta Dermatovenerol Croat
Toxic epidermal necrolysis 2017;25(1):72-76
As mentioned previously, no standard guidelines patient’s general condition gradually deteriorated.
exist for the management of TEN, but recently pub- She became febrile again with elevated C-reactive
lished articles pointed out that combination treat- protein (CRP) and white blood cell count. Cultures
ment with systemic steroids and immunoglobulin of swabs obtained from the infected areas revealed
as well as supportive treatment seems to have con- methicillin-resistant Staphylococcus aureus (MRSA)
tributed to an evident prognostic improvement and and Citrobacter freundii which was resistant to piper-
remarkable recovery (9-11). acillin-tazobactam but sensitive to meropenem. The
This case report highlights the importance of in- therapy with intravenous meropenem at 3 g/day
tensive wound care and also suggests that IVIG might and again with vancomycin at 2 g/day was started.
be beneficial in the treatment of patients with TEN. After surgical examination and consultation, a trans-
femoral amputation was recommended. A preop-
CASE REPORT erative assessment was performed on the patient
A 77-year-old female was admitted to our hos- by the consultant anesthetist. Clinical examination
pital to an Internal Medicine Department with fever revealed multiple confluent macular erythema and
and severe right limb infection after transmetatarsal bullous detachment of the epidermis over the face,
amputation. She had a medical history of hyperten- trunk, and extremities, but predominantly on the
sion, hyperlipidemia, diabetes mellitus type II, su- chest and back. An otorhinolaryngologist who was
praventricular and ventricular extrasystolia, and se- consulted because of sore throat and swallowing dif-
vere atherosclerosis. Further investigations showed ficulty noticed multiple painful buccal aphthous-like
inflammatory syndrome, anemia, uroinfection, and ulcerations. Above-knee amputation was performed
mild renal impairment, a consequence of fever and 2 days later under general anesthesia. After surgery,
dehydration in the context of diabetes. the patient was admitted to the ICU. She was in poor
Based on the ambulatory-based antibiogram, general condition upon admission: febrile with a
first-line antibiotic treatment with vancomycin at 2 g/ temperature of 38.5 °C, pulse between 120140/min-
day was continued for a total of 13 days, followed by ute and with CRP 251 mg/L. During the patient’s stay
piperacillin-tazobactam 2.25 g IV q8h for the next 15 in the ICU, skin lesions continued to progress; and
days. After that, the antibiotics were excluded from epidermal detachment progressed over the next two
the therapy because inflammatory markers where days, and macular erythema and bullous skin lesions
normal and the patients had no fever. However, de- affected more than 50% of the total body surface
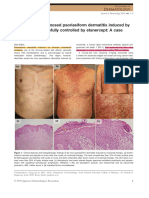
spite early targeted antimicrobial therapy and se- area (TBSA) (Figure 1 and 2). Severe oral involve-
rial surgical debridement of the infected tissues, the ments also continued to progress in the form of
Figure 1. Peeling of the affected skin. Figure 2. Peeling of the affected skin.
ACTA DERMATOVENEROLOGICA CROATICA
73
Klancir et al. Acta Dermatovenerol Croat
Toxic epidermal necrolysis 2017;25(1):72-76
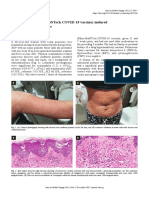
Figure 3. Lining placement.
painful hemorrhagic erosions and crusting over the
lips, restricting her oral intake. The rapid progression Figure 4. Lining placement.
of the oral erosions and desquamation on most of the
toxic reaction against the offending drug or its me-
patient’s body surface area led us to suspect TEN as
tabolites. Drugs can stimulate the immune system by
the diagnosis. Since it was assumed that the antibiot-
binding directly and reversibly to immune receptors.
ics caused TEN, all antibiotics were excluded from the
The prevalence of antibiotics being responsible for
therapy. Because of the severity of TEN – the SCORTEN
TEN ranges from 29% to 42% (12). Almost all antibiot-
score was 4 (Age >40, glucose >250 mg/dL, heart rate
ics have been implicated, but beta-lactam and sulfon-
>120/min, compromised body surface >10%) indi-
amide are most commonly associated with TEN, and
cating a 58.3% mortality rate – the patient was given
TEN usually develops within the first week of antibiot-
intravenous immunoglobulin therapy 1 g/kg over 3
ic therapy. In our case, TEN was diagnosed based on
days. She also received fluid resuscitation, and the
the clinical picture, and drugs we most suspected as
wounds were treated with Aquacell® Ag (ConvaTec)
the cause were antibiotics, due to the direct relation
and vaseline gauzes (Figure 3 and 4). The dressings
were changed periodically following cleaning with
saline and gentle debridement of exfoliated epider-
mis (Figure 5 and 6). After 15 days of local therapy,
almost full re-epithelialization was achieved (Figure
7 and 8), and the patient was generally in good con-
dition, without active inflammatory changes. A few
days later, despite improvement, she developed a
sudden bradycardia that did not respond to reanima-
tion procedures. The patients died after 18 days in the
ICU from a massive heart attack, according to autopsy
reports.
DISCUSSION
TEN is a severe life-threatening pathological syn-
drome with a high mortality rate. Half of the deaths
occur due to the secondary infection and subsequent
sepsis and multi-organ system failure. As mentioned
above, the pathogenesis of TEN is not fully under-
stood but is believed to be an immune-related cyto- Figure 5. Removal of dead skin.
ACTA DERMATOVENEROLOGICA CROATICA
74
Klancir et al. Acta Dermatovenerol Croat
Toxic epidermal necrolysis 2017;25(1):72-76
Figure 7. Re-epithelialization
Figure 6. Removal of dead skin.
between the onset of the disease and the administra- Figure 8. Re-epithelialization
tion of an antibiotic. Our patient received antibiotics
three days before the full clinical picture was evident.
fully achieved after 15 days of combination of local
However, since the patient was receiving multiple an-
therapy and IVIG.
tibiotics, it was difficult to determine which antibiotic
was causing the skin reaction. An improvement in the The action mechanism of IVIG is complex and in-
general condition of our patient after the withdrawal volves several mechanisms. One of proposed mecha-
of antibiotics may provide indirect evidence for a nisms involves the inhibition of keratinocyte death.
causative role of antibiotics as a potential agent for Apoptotic keratinocyte cell death leads to separation
TEN in our case. of the epidermis from the dermis, with subsequent
desquamation of skin. The rationale for using IVIG in
At the present time there is no uniform thera-
patients with TEN is to block keratinocyte apoptosis.
peutic strategy for TEN, but recommendations are
Namely, a significant increase in immunoglobulin G
mostly conservative, so based on previous work and
(IgG) concentration in the serum, blister fluid, and
suggested recommendations we chose to treat the
epidermis was found in patients being treated with
patient with the combination of intravenous immu-
IVIG. Elevated levels of IgG were found in clinically
noglobulin and regular and meticulous wound care.
affected and unaffected skin, which means that IVIG
It appears that aggressive debridement should be
has both systemic and local effects (13).
restricted unless absolutely necessary. For regular
wound care we used Aquacel Ag® – a primary wound
dressing containing 1.2% silver in an ionic form dis- CONCLUSION
tributed throughout the entire hydrofiber material. It Our case report shows that antibiotics are capable
is well known that silver ions possess potent broad- of inducing fatal adverse effects such as TEN and sug-
spectrum antibacterial properties. The use of Aquacel gests that it might be beneficial to use a combination
Ag® in the local treatment of the patient resulted in of Aquacel Ag® and IVIG in the treatment of patients
faster epithelization of the skin surface and decreased with TEN. Use of Aquacel Ag® helps rapid re-epitheli-
fluid loss through skin layers. zation and prevents wound infection.
Despite controversy about the benefit on the use
of IVIG, rapid progression of the skin lesions resulted Consent
in our ICU team’s decision to treat the patient with Verbal informed consent was obtained from the
IVIG. An objective response to IVIG infusion was ob- patient for the publication of this case report and the
served within 48 h, and reepithelization was almost accompanying images.
ACTA DERMATOVENEROLOGICA CROATICA
75
Klancir et al. Acta Dermatovenerol Croat
Toxic epidermal necrolysis 2017;25(1):72-76
References: of-illness score for toxic epidermal necrolysis. J
Invest Dermatol 2000;115:149-53.
1. Harr T, French LE. Toxic epidermal necrolysis and
Steven-Johnson syndrome. Orphanet J Rare Dis 8. Stevens Johnson Syndrome and Toxic Epidermal
2010;5:39-50. Necrolysis (Internet). DermNet NZ. 2016 (cited
2. Bastuji-Garin S, Rzany B, Stern RS, Shear NH, Naldi 2016 Apr 10). Available from: http://www.derm-
netnz.org/topics/stevens-johnson-syndrome-
L, Roujeau JC. Clinical classification of cases of
toxic-epidermal-necrolysis/
toxic epidermal necrolysis, Stenes-Johnson syn-
drome, and erythema multiforme. Arch Dermol 9. Yamane Y, Matsukura S, Watanabe Y, Yamaguchi
1993;129:92-6. Y, Nakamura K, Kambara T, et al. Retrospective
3. Brambilla G, Brucato F, Angrisano A, Palmieri G. analysis of Stevens-Johnson syndrome and toxic
Treatment of toxic epiderma necrolysis (TEN). Ann epidermal necrolysis in 87 Japanese patients - Tre-
atment and outcome. Allergol Int 2016;65:74-81.
Burns Fire Disast 2002;15:17-21.
10. Huang JJ, Ma SX, Hou X, Wang Z, Zeng YD, Qin T,
4. Frisch PO, Ruiz-Maldonado R. Erythema multifor-
et al. Epidermal necrolysis related to AP (peme-
me, Stevens-Johnson syndrome and toxic epider-
trexed plus cisplatin) and gefitinib combination
mal necrolysis. In: Freedberg IM, Eisen AZ, Wolff K,
therapy in a patient with metastatic non-small cell
Austen KF, Goldsmith LA, Katz SI, eds. Fitzpatrick’s
lung cancer. Chin J Cancer 2015;34:94-8.
dermatology in general medicine. 6th ed. New
York: McGraw-Hill; 2003. pp. 543-57. 11. Jagadeesan S, Sobhanakumari K, Sadanandan
SM, Ravindran S, Divakaran MV, Skaria L, et al. Low
5. Rzany B, Mockenhaupt M, Baur S, Schröder W,
dose intravenous immunoglobulins and steroids
Stocker U, Mueller J, et al. Epidemiology of eryt-
in toxic epidermal necrolysis: A prospective com-
hema exsudativum multiforme majus, Stevens-
parative open-labelled study of 36 cases. Indian J
Johnson syndrome, and toxic epidermal necroly-
Dermatol Venereol Leprol 2013;79:506-11.
sis in Germany (1990-1992): structure and results
of a population-based registry. J Clin Epidemiol 12. Schöpf E, Stühmer A, Rzany B, Victor N, Zentgraf R,
1996;49:769-73. Kapp JF. Toxic epidermal necrolysis and Stevens-
6. Sekula P, Dunant A, Mockenhaupt M, Naldi L, Johnson syndrome. An epidemiologic study from
Bouwes Bavinck JN, Halevy S, et al. Comprehen- West Germany. Arch Dermatol 1991;127:839-42.
sive survival analysis of a cohort of patients with 13. Paquet P, Kaveri S, Jacob E, Pirson J, Quatresooz
Stevens-Johnson syndrome and toxic epidermal J, Piérard GE. Skin immunoglobulin deposition
necrolysis. J Invest Dermatol 2013;133:1197-204. following intravenous immunoglobulin thera-
7. Bastuji-Garin S, Fouchard N, Bertocchi M, Roujeau py in toxic epidermal necrolysis. Exp Dermatol
2006;5:381-6.
JC, Revuz J, Wolkenstein P. SCORTEN: a severity-
ACTA DERMATOVENEROLOGICA CROATICA
76
You might also like
- CTC7 Sample Chapter 62014Document26 pagesCTC7 Sample Chapter 62014Enrico S. Rosales50% (4)
- Periodontology III MCQ For The FinalDocument55 pagesPeriodontology III MCQ For The FinalLolita A. Hicks67% (3)
- Epsom MapDocument1 pageEpsom Mapandrewmmwilmot0% (1)
- Thematic Apperception TestDocument8 pagesThematic Apperception TestMaria Qibtia100% (1)
- Art of Living Practice of Sudarshan KriyaDocument2 pagesArt of Living Practice of Sudarshan Kriyajeevaka100% (3)
- Caregiver AssessmentDocument7 pagesCaregiver AssessmentejaccontrolNo ratings yet
- ThedaCare Medical Center-Shawano Grand OpeningDocument44 pagesThedaCare Medical Center-Shawano Grand OpeningWolfRiverMediaNo ratings yet
- Treatment of Toxic Epidermal Necrolysis With Intravenous ImmunoglobulinDocument5 pagesTreatment of Toxic Epidermal Necrolysis With Intravenous ImmunoglobulinUbaidillah HafidzNo ratings yet
- Toxic Epidermal Necrolysis A Case ReportDocument3 pagesToxic Epidermal Necrolysis A Case ReportResearch ParkNo ratings yet
- Ad 32 334Document3 pagesAd 32 334Nurvia AndrianiNo ratings yet
- Histologically-Diagnosed Psoriasiform Dermatitis Induced by Nivolumab Successfully Controlled by Etanercept - A Case ReportDocument2 pagesHistologically-Diagnosed Psoriasiform Dermatitis Induced by Nivolumab Successfully Controlled by Etanercept - A Case ReportM CostantinoNo ratings yet
- Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis: Treatment of Severe Drug ReactionsDocument8 pagesStevens-Johnson Syndrome and Toxic Epidermal Necrolysis: Treatment of Severe Drug ReactionsHaidir MuhammadNo ratings yet
- 2018 Severe Cutaneous Adverse Drug Reactions - Presentation, Risk Factors, and ManagementDocument9 pages2018 Severe Cutaneous Adverse Drug Reactions - Presentation, Risk Factors, and ManagementpablopabloortizortizNo ratings yet
- Tiwari 2013Document8 pagesTiwari 2013Stella SunurNo ratings yet
- Artigo Terapia Alvo 1Document9 pagesArtigo Terapia Alvo 1fga.crislainebernardino01No ratings yet
- JCM 10 01040Document15 pagesJCM 10 01040Luminita HutanuNo ratings yet
- Adverse Cutaneous Drug EruptioDocument13 pagesAdverse Cutaneous Drug EruptioPeroquieNo ratings yet
- SSJ TenDocument5 pagesSSJ TenSelviana SudarmanNo ratings yet
- Ejm 17 1 40 45Document6 pagesEjm 17 1 40 45Ujean Santos SagaralNo ratings yet
- Sudema 2019 EditedDocument1 pageSudema 2019 EditedAditya Riadi SyafeiNo ratings yet
- Patch Testing and Immunosuppression: A Comprehensive ReviewDocument12 pagesPatch Testing and Immunosuppression: A Comprehensive Reviewnadia apriliaNo ratings yet
- Stevens-Johnson Syndrome Induced by Carbamazepine: PharmacologyDocument4 pagesStevens-Johnson Syndrome Induced by Carbamazepine: PharmacologyginNo ratings yet
- Tozinameran Induced AGEP-DRESSDocument2 pagesTozinameran Induced AGEP-DRESSCHONG WEI SHENGNo ratings yet
- Adverse Cutaneous Drug Eruptions: Current Understanding: ReviewDocument12 pagesAdverse Cutaneous Drug Eruptions: Current Understanding: ReviewasdasdNo ratings yet
- Dihematoporphyrin Ether-Induced Photosensitivity in Laryngeal Papilloma PatientsDocument8 pagesDihematoporphyrin Ether-Induced Photosensitivity in Laryngeal Papilloma PatientsDayse CSMNo ratings yet
- Amniotic Membrane Transplantation Combined With Antiviral and Steroid Therapy For Herpes Necrotizing Stromal KeratitisDocument7 pagesAmniotic Membrane Transplantation Combined With Antiviral and Steroid Therapy For Herpes Necrotizing Stromal KeratitisnelyNo ratings yet
- Nekrolisis Epidermal Toksik Ec KotrimoksasolDocument6 pagesNekrolisis Epidermal Toksik Ec KotrimoksasolIrgi PutraNo ratings yet
- Autoimmune Diseases A Late Complication of Toxic Epidermal Necrolysis A Case ReportDocument4 pagesAutoimmune Diseases A Late Complication of Toxic Epidermal Necrolysis A Case ReportAthenaeum Scientific PublishersNo ratings yet
- JurnalDocument3 pagesJurnalAulia Kamal Ansari PanggabeanNo ratings yet
- SJS FixDocument11 pagesSJS FixVivi YolandhaNo ratings yet
- Ajmcr 10 1 1Document4 pagesAjmcr 10 1 1jghcl.221No ratings yet
- Tiapride Associated Toxic Epidermal Necrolysis in An Hivinfected Patient. 2165 7920.1000323Document3 pagesTiapride Associated Toxic Epidermal Necrolysis in An Hivinfected Patient. 2165 7920.1000323Mega RafikaNo ratings yet
- Lee Et Al 2001 Case Report Meningococcal MeningitisDocument3 pagesLee Et Al 2001 Case Report Meningococcal MeningitisAsmae OuissadenNo ratings yet
- Management of Steven-Johnson Syndrome and Toxic Epidermal NecrolysisDocument6 pagesManagement of Steven-Johnson Syndrome and Toxic Epidermal NecrolysisRay PermanaNo ratings yet
- Cefixime Induced Stevens-Johnson Syndrome A Case Report and Review of LiteratureDocument2 pagesCefixime Induced Stevens-Johnson Syndrome A Case Report and Review of LiteratureDorainne JohnsonNo ratings yet
- Contemporary Treatment of LupusDocument13 pagesContemporary Treatment of LupusRamesh KavaliNo ratings yet
- Sindrome Nefrotico Carta El EditorDocument2 pagesSindrome Nefrotico Carta El EditorGerardo de Gyves AvilaNo ratings yet
- Review On Terminalia ChebulaDocument2 pagesReview On Terminalia ChebulaAman SrivastavaNo ratings yet
- PDFDocument14 pagesPDFJardee DatsimaNo ratings yet
- ICU Toxic Epidermal Necrolysis Guideline PDFDocument9 pagesICU Toxic Epidermal Necrolysis Guideline PDFaleexiipsszNo ratings yet
- Toxic Epidermal Necrolysis: A Paradigm of Critical IllnessDocument10 pagesToxic Epidermal Necrolysis: A Paradigm of Critical IllnessViolett LiebeNo ratings yet
- 005 PDFDocument7 pages005 PDFNely KartikaNo ratings yet
- How Do I Manage Nocardiosis?Document9 pagesHow Do I Manage Nocardiosis?Dan JaiNo ratings yet
- Jurnal Reading Glorivy Regita 112021072Document5 pagesJurnal Reading Glorivy Regita 112021072Regita LatuihamalloNo ratings yet
- SSJ PDFDocument10 pagesSSJ PDFArni SafriNo ratings yet
- Treatment of Severe Skin and Soft Tissue Burnham2018Document7 pagesTreatment of Severe Skin and Soft Tissue Burnham2018Rafael SuzukiNo ratings yet
- Severe Refractory Erythema Nodosum Leprosum Successfully Treated With The Tumor Necrosis Factor Inhibitor EtanerceptDocument3 pagesSevere Refractory Erythema Nodosum Leprosum Successfully Treated With The Tumor Necrosis Factor Inhibitor EtanerceptMega MartinNo ratings yet
- Necrotizing Fasciitis of The Breast: A Case Series and Review of The LiteratureDocument9 pagesNecrotizing Fasciitis of The Breast: A Case Series and Review of The LiteratureElli SymeonidouNo ratings yet
- Review of Toxic Epidermal NecrolysisDocument10 pagesReview of Toxic Epidermal NecrolysisNurfitri ZuhruhurNo ratings yet
- Hot Topics in Necrotising Skin and SoftDocument10 pagesHot Topics in Necrotising Skin and SoftPriyanshi PatelNo ratings yet
- Toxic Epidermal Necrolysis: BackgroundDocument36 pagesToxic Epidermal Necrolysis: BackgroundGita AmeliaNo ratings yet
- Diagnostic Challenge of Tuberculosis in Systemic Lupus ErythematosusDocument9 pagesDiagnostic Challenge of Tuberculosis in Systemic Lupus ErythematosusBelinda Putri agustiaNo ratings yet
- Terjemahan KulitDocument5 pagesTerjemahan KulitErlieza Rosdania SupraptoNo ratings yet
- Narrowband Ultraviolet-B Phototherapy in Pityriasis Lichenoides ChronicaDocument6 pagesNarrowband Ultraviolet-B Phototherapy in Pityriasis Lichenoides ChronicaJavier Perez ManriquezNo ratings yet
- A Critical Updated of The Assessmente and Acute Management If Patients With Severe BurnsDocument27 pagesA Critical Updated of The Assessmente and Acute Management If Patients With Severe BurnsCarlos Javier SolorzaNo ratings yet
- Stevens-Johnson Syndrome (SJS) and Toxic Epidermal Necrolysis Management, Prognosis and Long Term SequelaeDocument28 pagesStevens-Johnson Syndrome (SJS) and Toxic Epidermal Necrolysis Management, Prognosis and Long Term SequelaePutri SRNo ratings yet
- Dermato - Emergemencies (Acute Blistering and Exfoliative Skin) Nyoman Suryawati ObjectiveDocument9 pagesDermato - Emergemencies (Acute Blistering and Exfoliative Skin) Nyoman Suryawati ObjectiveLong LieNo ratings yet
- Local Management of NeutropenicDocument3 pagesLocal Management of NeutropenicCláudia Carrara CotomácioNo ratings yet
- Nejmoa 1310480Document11 pagesNejmoa 1310480mz zumrodinNo ratings yet
- A Case of The Drug Reaction With Eosinophilia and Systemic Symptom (DRESS) Following Isoniazid TreatmentDocument4 pagesA Case of The Drug Reaction With Eosinophilia and Systemic Symptom (DRESS) Following Isoniazid TreatmentPutri YingNo ratings yet
- Stevens-Johnson Syndrome (SJS) and Toxic Epidermal Necrolysis (Ten) Associated With Anti-Tubercular Drugs: A Case ReportDocument4 pagesStevens-Johnson Syndrome (SJS) and Toxic Epidermal Necrolysis (Ten) Associated With Anti-Tubercular Drugs: A Case ReportIJAR JOURNALNo ratings yet
- Stevens-Johnson Syndrome and Abuse of Anabolic SteroidsDocument4 pagesStevens-Johnson Syndrome and Abuse of Anabolic SteroidsRafael SebastianNo ratings yet
- Toxic Epidermal Necrolysis and Stevens Johnson Syndrome: Our Current UnderstandingDocument8 pagesToxic Epidermal Necrolysis and Stevens Johnson Syndrome: Our Current UnderstandingjoyfullNo ratings yet
- Drug Reaction With Eosinophilia and Systemic Symptoms (DRESS) Syndrome in Pediatrics. Clinical CaseDocument5 pagesDrug Reaction With Eosinophilia and Systemic Symptoms (DRESS) Syndrome in Pediatrics. Clinical CaseKelitaGonzalezNo ratings yet
- RF - Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis: A Treatment UpdateDocument2 pagesRF - Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis: A Treatment Updatedoc.kentoNo ratings yet
- Nebulized Colistin in The Treatment of Pneumonia Due To Multidrug-Resistant Acinetobacter Baumannii and Pseudomonas AeruginosaDocument4 pagesNebulized Colistin in The Treatment of Pneumonia Due To Multidrug-Resistant Acinetobacter Baumannii and Pseudomonas AeruginosaPhan Tấn TàiNo ratings yet
- Directions: Check Out 30 Minute Chicken RecipesDocument22 pagesDirections: Check Out 30 Minute Chicken RecipesDarwyn Paul DagumanNo ratings yet
- Violence (WHO) PDFDocument22 pagesViolence (WHO) PDFDarwyn Paul DagumanNo ratings yet
- According To Williams It Is Between The 5th and 17th Week)Document1 pageAccording To Williams It Is Between The 5th and 17th Week)Darwyn Paul DagumanNo ratings yet
- Ofl Oxacin-Induced Toxic Epidermal Necrolysis: Vikas Saini, Dinesh Sardana, Tanvir SamraDocument2 pagesOfl Oxacin-Induced Toxic Epidermal Necrolysis: Vikas Saini, Dinesh Sardana, Tanvir SamraDarwyn Paul DagumanNo ratings yet
- Boehringer: Technical Manual Model 7926 AUTOVAC Autotransfusion System For Orthopedic Wound DrainageDocument2 pagesBoehringer: Technical Manual Model 7926 AUTOVAC Autotransfusion System For Orthopedic Wound DrainageJoão Francisco MontanhaniNo ratings yet
- NCPDocument3 pagesNCPNikki del Rosario100% (2)
- Newborn Resuscitation Programme NRPDocument47 pagesNewborn Resuscitation Programme NRPNethera Kiza ImperialNo ratings yet
- Esophageal CancerDocument42 pagesEsophageal Cancerapi-1964133750% (2)
- NRP 5th Edition PretestDocument5 pagesNRP 5th Edition PretestHo Yong WaiNo ratings yet
- Congenital Glaucoma B4Document15 pagesCongenital Glaucoma B4Prashantha VespanathanNo ratings yet
- Care Plan Activity IntoleranceDocument3 pagesCare Plan Activity IntoleranceRachael CrossgroveNo ratings yet
- The Thorax and Lungs Assessment (Autosaved)Document49 pagesThe Thorax and Lungs Assessment (Autosaved)Arlyn Mendenilla100% (4)
- ACE Inhibitors Vs ARBsDocument3 pagesACE Inhibitors Vs ARBsKo Phyo WaiNo ratings yet
- Evidence Based Dentistry: Book: Essential Dental Public HealthDocument23 pagesEvidence Based Dentistry: Book: Essential Dental Public HealthAyesha AwanNo ratings yet
- Nivedita Nimesh C VDocument2 pagesNivedita Nimesh C Vapi-278464951No ratings yet
- HaloperidolDocument1 pageHaloperidolSalma AKNo ratings yet
- Clotting Time Macromethod: Utilized Larger Amount of BloodDocument4 pagesClotting Time Macromethod: Utilized Larger Amount of BloodGerly MaglangitNo ratings yet
- A Level Psychology SM Split Brains PosterDocument1 pageA Level Psychology SM Split Brains PosterAlisha GenduNo ratings yet
- Plateletrich Plasma Injections For Knee Osteoarthritis PDF 1899874048147909Document5 pagesPlateletrich Plasma Injections For Knee Osteoarthritis PDF 1899874048147909JanetNo ratings yet
- S1PK.3. Theory BookDocument31 pagesS1PK.3. Theory BookBrayen HarperNo ratings yet
- Differential Diagnosis of Tongue LesionsDocument12 pagesDifferential Diagnosis of Tongue LesionsKartikakhairaniNo ratings yet
- Postherpetic NeuralgiaDocument15 pagesPostherpetic NeuralgiaAndi IshaqNo ratings yet
- Components of The CBCDocument4 pagesComponents of The CBCGenefer AlmeliaNo ratings yet
- DADHDocument69 pagesDADHdrpnnreddyNo ratings yet
- Syllabus DraftDocument7 pagesSyllabus Draftapi-440514424No ratings yet
- Endotracheal IntubationDocument28 pagesEndotracheal Intubationsyukur_odeNo ratings yet
- Funda Module 9 10Document6 pagesFunda Module 9 10AinaB ManaloNo ratings yet