Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
9 viewsCase Report Urretz Zavalia Syndrome
Case Report Urretz Zavalia Syndrome
Uploaded by
Ai HidayatThis case report describes a 57-year-old female who presented with glare in her right eye 3 days following uneventful cataract surgery. On examination, her right pupil was fixed and dilated, with iris atrophy and an absence of light reflex. No complications were recorded during her surgery. The exact cause of her condition, called Urrets-Zavalia syndrome, is unknown but may involve ischemia of the sphincter muscle after iris strangulation during surgery, leading to permanent pupil dilation. Treatment with miotic drops provided no response. The report discusses various proposed mechanisms and risk factors for this syndrome.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You might also like
- BCSC Reading Schedule 2019-2020Document11 pagesBCSC Reading Schedule 2019-2020Mari Martinez100% (1)
- Tatalaksana Glaukoma Sekunder Dengan Sklerouveitis - Ericka Febriyanti Pratama PuatriDocument16 pagesTatalaksana Glaukoma Sekunder Dengan Sklerouveitis - Ericka Febriyanti Pratama PuatristrjuhanengsihNo ratings yet
- Case Review - EndophthalmitisDocument4 pagesCase Review - EndophthalmitisDr Shawgat Ul Karim KhanNo ratings yet
- Orbital Apex Syndrome Secondary To Herpes Zoster OphthalmicusDocument4 pagesOrbital Apex Syndrome Secondary To Herpes Zoster OphthalmicusYosiita KartinaaNo ratings yet
- Laporan Kasus Tatalaksana Pembedahan Pada Pasien Dengan Eksotropia Sensoris - Novaqua YandiDocument13 pagesLaporan Kasus Tatalaksana Pembedahan Pada Pasien Dengan Eksotropia Sensoris - Novaqua YandiMeliNo ratings yet
- Departemen Ilmu Kesehatan Mata Fakultas Kedokteran Universitas Padjadjaran Pusat Mata Nasional Rumah Sakit Mata Cicendo BandungDocument11 pagesDepartemen Ilmu Kesehatan Mata Fakultas Kedokteran Universitas Padjadjaran Pusat Mata Nasional Rumah Sakit Mata Cicendo BandungBambang RinandiNo ratings yet
- Endoftalmitis 3Document4 pagesEndoftalmitis 3andisibaNo ratings yet
- GDD Implan Dengan Pemasangan LIO Sekunder Iris Claw Retro Pupillary Pada Pasien Pasca Vitrektomi LianiDocument11 pagesGDD Implan Dengan Pemasangan LIO Sekunder Iris Claw Retro Pupillary Pada Pasien Pasca Vitrektomi LianivellafebrinaefitaNo ratings yet
- Tatalaksana Glaukoma Sekunder Sudut Tertutup Dengan Luksasi Lensa Dan Retinitis PigmentosalenoraDocument11 pagesTatalaksana Glaukoma Sekunder Sudut Tertutup Dengan Luksasi Lensa Dan Retinitis PigmentosalenoraSyahna AprilianiNo ratings yet
- Diagnosis BandingDocument10 pagesDiagnosis BandingIntan Rahmi NasyaNo ratings yet
- Cystoid Macular EdemaDocument5 pagesCystoid Macular EdemaAgnes Triana BasjaNo ratings yet
- Ostiogenesis ImperfectaDocument4 pagesOstiogenesis Imperfectamarlon GarcíaNo ratings yet
- Prabhakar 1Document4 pagesPrabhakar 1ChristaGisellaPirsouwNoyaNo ratings yet
- Letters To The EditorDocument8 pagesLetters To The EditorGheavita Chandra DewiNo ratings yet
- Implant Glaucoma Drainage DeviceDocument12 pagesImplant Glaucoma Drainage DeviceMCU BTMNo ratings yet
- Asian Upper Eyelid Blepharoplasty Sebagai Tatalaksana Dermatokalasis - Adessa RachmaDocument11 pagesAsian Upper Eyelid Blepharoplasty Sebagai Tatalaksana Dermatokalasis - Adessa Rachmafadil ahmadi100% (1)
- Canadian Journal of Ophthalmology - Journal Canadien D'ophtalmologie Volume Issue 2017 (Doi 10.1016 - J.jcjo.2017.01.022) Moinul, Prima Luong, Micah Bhamra, Jamie Kherani, Amin McWha - Aqueous MiDocument3 pagesCanadian Journal of Ophthalmology - Journal Canadien D'ophtalmologie Volume Issue 2017 (Doi 10.1016 - J.jcjo.2017.01.022) Moinul, Prima Luong, Micah Bhamra, Jamie Kherani, Amin McWha - Aqueous MiVinda Sari ErmizaNo ratings yet
- Vitrectomy Results in Proliferative Diabetic RetinopathyDocument3 pagesVitrectomy Results in Proliferative Diabetic RetinopathyRohamonangan TheresiaNo ratings yet
- Acc or Inti 2007Document6 pagesAcc or Inti 2007iwanNo ratings yet
- Penatalaksanaan Glaukoma Sekunder Refrakter Pada Implantasi Lensa Intraokular Bilik Mata Depan - Pauline Meilisa SihiteDocument13 pagesPenatalaksanaan Glaukoma Sekunder Refrakter Pada Implantasi Lensa Intraokular Bilik Mata Depan - Pauline Meilisa SihiteZikra Herlius14No ratings yet
- Penatalaksanaan Pasien Glaukoma Sudut Terbuka Dengan PemasanganintanmaulaDocument10 pagesPenatalaksanaan Pasien Glaukoma Sudut Terbuka Dengan PemasanganintanmaulaShela GranityaNo ratings yet
- MainDocument4 pagesMainVicky ObandoNo ratings yet
- Case ReportDocument7 pagesCase ReportJeel GaralaNo ratings yet
- Tatalaksana Katarak Komplikata Yang Disebabkan Oleh Uveitis - Ericka Febriyanti Pratama Putri 1Document14 pagesTatalaksana Katarak Komplikata Yang Disebabkan Oleh Uveitis - Ericka Febriyanti Pratama Putri 1Cynthia Isra MandahutaNo ratings yet
- A Rare Case of Terson Syndrome With Subarachnoid HemorrhageDocument12 pagesA Rare Case of Terson Syndrome With Subarachnoid HemorrhageNinaNo ratings yet
- Tatalaksana Refractive Surprise Pada Bedah Katarak Bilateral - Wioma Surya DarmaDocument14 pagesTatalaksana Refractive Surprise Pada Bedah Katarak Bilateral - Wioma Surya DarmaAndreas SimatupangNo ratings yet
- Makrufa NWDocument6 pagesMakrufa NWPujiastutiNo ratings yet
- V36N4p293 PDFDocument5 pagesV36N4p293 PDFsiscaNo ratings yet
- Journal Asli - Mash - Ab Zirrun Al-Qomah - 212011101095Document4 pagesJournal Asli - Mash - Ab Zirrun Al-Qomah - 212011101095tttttNo ratings yet
- Tatalaksana Dan Prognosis Severe Visual Impairment Pada Miopia Patologi - Nikho Melga ShalimDocument14 pagesTatalaksana Dan Prognosis Severe Visual Impairment Pada Miopia Patologi - Nikho Melga ShalimOt PtkNo ratings yet
- Diagnosis Dan Tatalaksana Dislokasi Lensa Intraokular Ke Posterior Dengan Prosedur IOL Exchange To Iris Claw Retropupillary - Siti AisyahDocument13 pagesDiagnosis Dan Tatalaksana Dislokasi Lensa Intraokular Ke Posterior Dengan Prosedur IOL Exchange To Iris Claw Retropupillary - Siti Aisyahmemmuse95No ratings yet
- Showphacomrphic Glaucoma Managemnet by Surgical and Medical Management TextDocument8 pagesShowphacomrphic Glaucoma Managemnet by Surgical and Medical Management Textdrvishalkulkarni2007No ratings yet
- 1 PBDocument4 pages1 PBRian YupitaNo ratings yet
- Ace SetiawanDocument11 pagesAce SetiawanGlaucoma UnhasNo ratings yet
- Retina 2012 Sep 32 (Suppl 2) S225-31Document7 pagesRetina 2012 Sep 32 (Suppl 2) S225-31roro207No ratings yet
- Acknowledgement: Aniridia Associated With Congenital Aphakia and Secondary GlaucomaDocument3 pagesAcknowledgement: Aniridia Associated With Congenital Aphakia and Secondary GlaucomaNisrina FarihaNo ratings yet
- Sympathetic Ophthalmia After Vitreoretinal Surgery: A Report of Two CasesDocument11 pagesSympathetic Ophthalmia After Vitreoretinal Surgery: A Report of Two CasesAlexander RezaNo ratings yet
- Five Year PROSE Treatment For Aniridic KojimaOct2016PAPDocument5 pagesFive Year PROSE Treatment For Aniridic KojimaOct2016PAP小島隆司No ratings yet
- Abstract Pachydermoperiostosis EnggresDocument4 pagesAbstract Pachydermoperiostosis EnggresKarina BudijantoNo ratings yet
- Cataract Extraction and Intraocular Lens Implantation in Children With UveitisDocument4 pagesCataract Extraction and Intraocular Lens Implantation in Children With UveitiskhairunnisaNo ratings yet
- Feliciatimmermann 2778Document2 pagesFeliciatimmermann 2778Calvin NugrahaNo ratings yet
- Management of Penetrating Eye Injury With Intraocular Foreign BodyDocument5 pagesManagement of Penetrating Eye Injury With Intraocular Foreign BodyChristian FaustNo ratings yet
- Parade Wspos Tipe 2Document3 pagesParade Wspos Tipe 2irwan_201291No ratings yet
- Visual Outcome After Phacomorphic GlaucomaDocument3 pagesVisual Outcome After Phacomorphic GlaucomaHassan KhanNo ratings yet
- Shankar Ganvit END PDFDocument4 pagesShankar Ganvit END PDFgyogi1989No ratings yet
- Catarta e HipoparatiroidismoDocument3 pagesCatarta e HipoparatiroidismoBernardo RomeroNo ratings yet
- Retinal Tear: An Unusual Complication of Ocular ToxoplasmosisDocument5 pagesRetinal Tear: An Unusual Complication of Ocular ToxoplasmosisMuhammad Irfan FaizNo ratings yet
- Toophtj 8 1Document2 pagesToophtj 8 1SusPa NarahaNo ratings yet
- Kag Rully (B.IG)Document7 pagesKag Rully (B.IG)Rully Dwi SaputraNo ratings yet
- Ablasio RetinaDocument23 pagesAblasio RetinaResa PutraNo ratings yet
- Tatalaksana Operatif Dan Pascaoperatif Pada Pasien Juvenile Open Angle Glaucoma JOAG - Andreas Lukita HalimDocument14 pagesTatalaksana Operatif Dan Pascaoperatif Pada Pasien Juvenile Open Angle Glaucoma JOAG - Andreas Lukita HalimINDRINo ratings yet
- Therapeutic Effectiveness of Toric Implantable Collamer Lens in Treating Ultrahigh Myopic AstigmatismDocument7 pagesTherapeutic Effectiveness of Toric Implantable Collamer Lens in Treating Ultrahigh Myopic AstigmatismStephanie PfengNo ratings yet
- Mcculley 2012Document11 pagesMcculley 2012Luisa Mayta PitmanNo ratings yet
- Tatalaksana Katarak Traumatika Dengan Open Globe Injury Pada Anak - Levandi MuljaDocument12 pagesTatalaksana Katarak Traumatika Dengan Open Globe Injury Pada Anak - Levandi MuljaFaisal radhiNo ratings yet
- 100255-Article Text-1482-2-10-20220311Document6 pages100255-Article Text-1482-2-10-20220311Fachry RahmanNo ratings yet
- 15) Refractory Open-Angle Glaucoma After Neodymium - Yttrium-Aluminum-Garnet Laser Lysis of Vitreous FloatersDocument6 pages15) Refractory Open-Angle Glaucoma After Neodymium - Yttrium-Aluminum-Garnet Laser Lysis of Vitreous FloatershasdiniNo ratings yet
- Artículo Oftalmología RetinaDocument1 pageArtículo Oftalmología RetinaJavier Burgos CárdenasNo ratings yet
- Clinical Study: XEN Glaucoma Implant With Mitomycin C 1-Year Follow-Up: Result and ComplicationsDocument6 pagesClinical Study: XEN Glaucoma Implant With Mitomycin C 1-Year Follow-Up: Result and ComplicationsAldoNo ratings yet
- JORS Volume 2 Issue 1 Pages 19-21Document3 pagesJORS Volume 2 Issue 1 Pages 19-21Praveen DhanapalNo ratings yet
- Msor 000504Document3 pagesMsor 000504MudrikahHaniyahNo ratings yet
- Complications in UveitisFrom EverandComplications in UveitisFrancesco PichiNo ratings yet
- Contouring The Lens and Lacrimal Glands On t2 Weighted Mri - NewDocument10 pagesContouring The Lens and Lacrimal Glands On t2 Weighted Mri - NewJulian CiabattariNo ratings yet
- Data Upload ShopeeDocument28 pagesData Upload Shopeebanyakmauu borNo ratings yet
- Eye StructureDocument15 pagesEye StructurekathyNo ratings yet
- Yang Sudah Di KerjakanDocument4 pagesYang Sudah Di Kerjakanjazuliswdstore01No ratings yet
- Care of The Clients With Eye and Ear DisorderDocument35 pagesCare of The Clients With Eye and Ear DisorderKristine Joy RevañoNo ratings yet
- IOL PowerDocument273 pagesIOL Powermarlon García100% (2)
- Abebizuhan ZigaleDocument45 pagesAbebizuhan Zigaleabiraham zigaleNo ratings yet
- 2019 Health Assessment Examination - EyesDocument2 pages2019 Health Assessment Examination - Eyesharley dela cruzNo ratings yet
- Lens and The EyeDocument58 pagesLens and The EyeEisle Keith Rivera TapiaNo ratings yet
- Resume ICDDocument6 pagesResume ICDKomang AstrieNo ratings yet
- Special Senses) 3. Photoreceptors - Rods and Cones - KeyDocument1 pageSpecial Senses) 3. Photoreceptors - Rods and Cones - Keyranag59100No ratings yet
- Q2 - First Summative Test in All Subjects With TOSDocument21 pagesQ2 - First Summative Test in All Subjects With TOSapril joy tamayoNo ratings yet
- Pinxel-V-S - She-Pxs006Document15 pagesPinxel-V-S - She-Pxs006Ashraf AboNo ratings yet
- Opinioes Exames Ebo e IcoDocument8 pagesOpinioes Exames Ebo e Icoapi-3595301060% (1)
- BIO101 Student Notes PRELIM Integumentary System1Document4 pagesBIO101 Student Notes PRELIM Integumentary System1Kirstine Valerie MandalonesNo ratings yet
- Basics of FundusDocument29 pagesBasics of Fundusikayapmd100% (1)
- Strabismus PDFDocument170 pagesStrabismus PDFShari Ali100% (1)
- (Brief Discussion of The Lesson, If Possible Cite Examples) : SUBJECT (Uppercase and Bold)Document33 pages(Brief Discussion of The Lesson, If Possible Cite Examples) : SUBJECT (Uppercase and Bold)KD DelayunNo ratings yet
- Traktus UveaDocument90 pagesTraktus UveaAudrey Ira Yunita100% (1)
- Peudophakia New-2Document4 pagesPeudophakia New-2KjoNo ratings yet
- Anatomy of Eyes: January 2009Document7 pagesAnatomy of Eyes: January 20091710105 Sean Rio SimangunsongNo ratings yet
- Sclerology Miller RevisiDocument177 pagesSclerology Miller RevisiTri Ayu Eka PaksiNo ratings yet
- World Through Our Senses (All Sensory Organs)Document48 pagesWorld Through Our Senses (All Sensory Organs)Chin Kok Soon100% (3)
- Sekolah Menengah Kebangsaan Tanjong Rambutan 31250, Tanjong Rambutan Science Form 2Document5 pagesSekolah Menengah Kebangsaan Tanjong Rambutan 31250, Tanjong Rambutan Science Form 2Jannah SulaimanNo ratings yet
- Icd X MataDocument11 pagesIcd X MataLilis tri wardhijaniNo ratings yet
- Integumentary Lab ActDocument5 pagesIntegumentary Lab ActJASMINE LAURONNo ratings yet
- General Survey and Integumentary I. General Appearance and Mental Status Normal Findings Actual Findings Analysis and InterpretationDocument9 pagesGeneral Survey and Integumentary I. General Appearance and Mental Status Normal Findings Actual Findings Analysis and InterpretationAllana RayosNo ratings yet
- Effects of Genipin Corneal Crosslinking in Rabbit CorneasDocument5 pagesEffects of Genipin Corneal Crosslinking in Rabbit CorneasMauricio NarvaezNo ratings yet
- Skin ProjectDocument16 pagesSkin ProjectMonique WilliamsNo ratings yet
Case Report Urretz Zavalia Syndrome
Case Report Urretz Zavalia Syndrome
Uploaded by
Ai Hidayat0 ratings0% found this document useful (0 votes)
9 views6 pagesThis case report describes a 57-year-old female who presented with glare in her right eye 3 days following uneventful cataract surgery. On examination, her right pupil was fixed and dilated, with iris atrophy and an absence of light reflex. No complications were recorded during her surgery. The exact cause of her condition, called Urrets-Zavalia syndrome, is unknown but may involve ischemia of the sphincter muscle after iris strangulation during surgery, leading to permanent pupil dilation. Treatment with miotic drops provided no response. The report discusses various proposed mechanisms and risk factors for this syndrome.
Original Description:
Laporan kasus
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis case report describes a 57-year-old female who presented with glare in her right eye 3 days following uneventful cataract surgery. On examination, her right pupil was fixed and dilated, with iris atrophy and an absence of light reflex. No complications were recorded during her surgery. The exact cause of her condition, called Urrets-Zavalia syndrome, is unknown but may involve ischemia of the sphincter muscle after iris strangulation during surgery, leading to permanent pupil dilation. Treatment with miotic drops provided no response. The report discusses various proposed mechanisms and risk factors for this syndrome.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
9 views6 pagesCase Report Urretz Zavalia Syndrome
Case Report Urretz Zavalia Syndrome
Uploaded by
Ai HidayatThis case report describes a 57-year-old female who presented with glare in her right eye 3 days following uneventful cataract surgery. On examination, her right pupil was fixed and dilated, with iris atrophy and an absence of light reflex. No complications were recorded during her surgery. The exact cause of her condition, called Urrets-Zavalia syndrome, is unknown but may involve ischemia of the sphincter muscle after iris strangulation during surgery, leading to permanent pupil dilation. Treatment with miotic drops provided no response. The report discusses various proposed mechanisms and risk factors for this syndrome.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 6
CASE REPORT
JANUARI 2016
Urrets-Zavalia Syndrome (Fixed and Dilated Pupil)
Following Uneventful Cataract Surgery
Fadly, Yunita, Hamzah, Abrar
Oleh :
Muhammad Fadly Hidayat
Pembimbing :
dr. Yunita, Sp.M(K), M.Kes
dr. Hamzah, Sp.M(K)
dr. Muh. Abrar Ismail, Sp.M, M.Kes
KONSENTRASI PENDIDIKAN DOKTER SPESIALIS TERPADU
( COMBINED DEGREE )
BAGIAN ILMU KESEHATAN MATA PROGRAM STUDI BIOMEDIK
PROGRAM PASCA SARJANA
FAKULTAS KEDOKTERAN UNHAS
MAKASSAR
2016
Urrets-Zavalia Syndrome (Fixed and Dilated Pupil)
Following Uneventful Cataract Surgery
Fadly Hidayat, Yunita, Hamzah, Abrar
Department of Ophtalmology, Faculty Of Medicine, Hasanuddin University
Hasanuddin Teaching Hospital, Makassar
ABSTRACT
Purpose : To report a case of urrets-zavalia syndrome following uneventful cataract
surgery
Methods : A case report
Case report : A 57 years old female presented with glare on right eye 3 days following
cataract surgery. Examination of the right eye showed iris atrophy and fixed dilated
pupil, the absence of light reflex, pigment of the iris appears on the surface of
intraocular lens. There are no history of complication recorded during surgery. Fellow
eye was operated by same surgeon with BCVA 20/20 and no found abnormality.
Result : The patient were given a miotic agent drops every 2 hours, and steroid every 6
hours daily and tappered off every week. In the next visit showed no respond on therapy,
the pupil still fixed and dilated.
Conclusion : The exact etiology of urrets-zavalia syndrome is unknown and different
mechanisms have been proposed.This condition may need preventive strategies to avoid
complication. This case shows an intrinsic susceptibility for urrets-zavalia syndrome
which alerts surgeons in the case of second eye surgery
Keywords : Urrets-Zavalia syndrome, Dilated Pupil, Fixed Pupil, penetrating
keratoplasty, atropine, mydriatics
INTRODUCTION however she felt glare on a bright light
Urrets-Zavalia Syndrome (UZS) was environment. Examination of the right
first described as a syndrome consisting eye showed atrophy of the iris, dilated
of a fixed, dilated pupil with iris atrophy pupil, absence of light reflex, there was
following penetrating keratoplasty no relative afferent pupillary defect,
1
(PKP) in 1963. Other manifestations pigments of the iris were present on
that are not essential for the diagnosis intraocular lenses surface, intraocular
are posterior synechiae, ectropion uvea, lense is located in the bag. Eye
pigment dispersion, anterior subcapsular movements are normal on both eyes.
lens opacities and secondary glaucoma Both eyes are pseudophacic with
syndrome. BSCVA on right and left eye are 20/25
At first this syndrome had been and 20/20 respectively. Funduscopy
attributed to the keratoconus. However examination showed normal findings.
this syndrome was described after PKP Medications given after catarct surgery
for corneal dystrophy, deep anterior are antibiotics and steroid eye drops.
lamellar keratoplasty (DALK), descemet The patient was also given beta blocker
stripping endothelial keratoplasty eye drop. On the day of surgery, there
(DSEK), trabeculectomy, laser were 3 cataract surgeries. Patient were
iridoplasty, iatrogenic mydriasis and operated with surgeon using similar
after implantation of phakic intraocular consumables with same technique. None
lenses.2-10 of them reported to have similar sign
Although Zavalia associated this and symptomps. The patient’s fellow
syndrome with postoperative treatment eye were operated 1 month earlier with
with mydriatics, then Uribe supposed a same surgeon and no adverse outcomes
process of postoperative spontaneous found. Since the first day after surgery
mydriasis, poorly responsive to miotics, the right eye had an increase of the intra
in patients with keratoconus undergoing ocular pressure, and another finding is
PKP.11 Thus it could happen where that the conjunctiva is hiperemic and the
mydriatics had not been prescribed. The cornea appears edema. On the next visit,
precise contributing mechanism has not these signs were absent. At first control,
been known so far but fibrinous uveitis, we got signs fixed and dilated pupil, and
iris vessel strangulation and pupillary then the patient was given chlolinergic
block have been proposed.8 parasympathomimetic (pilocarpine)
Hereby we reported case of urrets every 2 hours for 1 day usage and other
zavalia syndrome post cataract surgery drugs such as antibiotic and steroid drop
were proceed. In the next control, we
CASE REPORT still got fixed and dilated pupil, and no
A 57 years old female presented to us light reflex. It showed no response to
clinic with complaint of glare on the pilocarpine administration so that the
right eye since 3 days after cataract administration was stopped.
surgery. The patient acknowledge that
her vision was improved after surgery,
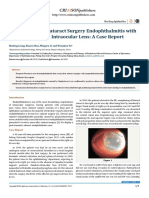
Figure 1. Shown dilated pupil and atrophy of the Figure 2. Iris pigments on IOL surface
iris
DISCUSSION incision edge of the host cornea as the
A fixed, dilated pupil will not react to lens-iris diaphragm moves forwards
light or accommodation16, around 7 mm during surgery.20 Some argue that UZS
in diameter, is often irreversible, not is a pupillary block phenomenon.25,26
respond to pharmacological treatment The rise of IOP also found on the first
and will usually be noticed during the day post operation.
immediate postoperative period.17,18 As In several reports where IOP
with the theory above, in this case, the measurements were not available or IOP
patient had fixed and dilated pupil that was normal, patients reported
do not respond to the administration of experiencing pain, nausea, and vomiting
chlolinergic parasympathomimetic for during the night, often symptoms of a
24 hours. transient increase in IOP, before a fixed
Jastaneiah et al reported that a and dilated pupil was observed.15,27,28 As
dilated pupil will be detected by the first we observed in this patient.
two postoperative days in 80.9% of Urrets and Zavalia also suggested
patients.19 Similarly, Davies and Ruben that the strong mydriasis produced by
found most cases of UZS to occur at the atropine at the time of surgery brought
first postoperative day. A few present iris in contact with peripheral cornea to
later, but not after the 12th postoperative produce peripheral anterior synaechiae
day.20 Others, however, stated that and secondary glaucoma.1 Though,
although UZS will typically occur 1 or 2 glaucoma is not the integral part of the
weeks after PKP, it does not occur syndrome.13 UZS may develop even in
within the first postoperative days.21,22 cases where no mydriatic drops were
UZS is also reported to occur up to 5 applied.4
months postoperatively.23 In this patient Davies and Ruben also suggested
was found glare since 3 days post that direct iris trauma during surgery
surgery, from this sign we can assume could result in strangulation of iris
that fixed and dilated pupil occurred in vessels in the mid-periphery and
the same time. ischemic paralysis of the sphincter
The pathophysiology of this pupillae.15 In this case we found iris
syndrome is still unclear. The leading atrophy cause by injury during operation
explanation for the development of UZS Cataract surgery may result in fixed
is ischemic atrophy of the sphincter and dilated pupils.29,30 Viscoelastic
muscle secondary to iris strangulation material left in the anterior chamber
with resultant pupil dilatation. The cause angle,15 and the hypromellose used as
for iris ischemia could be an acute post- viscoelastic material was suspected to
operative increase in IOP,15,24 be toxic to the sphincter or vasculature
compression of iris vessels against the of the iris, resulting in a rate of 16.7% of
sphincter atrophy and fixed dilated ocular pressure a day after cataract
pupil.30 Jastaneiah also suggested surgery.
Residues of either viscoelastics or CONCLUSION
detergents can lead to inflammation,
which is usually considered toxic The exact etiology of urrets-zavalia
anterior segment syndrome. This can syndrome is unknown and different
elevate the IOP, impair iris sphincter mechanisms have been proposed. This
functions, and possibly result in a may complicate preventive strategies for
permanently dilated fixed pupil as well this syndrome. UZS can occur even
as atrophy of the iris.19 In this patient, thought under optimal operation
we did not find the residual of condition. Experienced surgeon, the
viscoelastic left on anterior chamber but technique and use of the same material
it can not be guarantee because of the still has the same chance to occur this
viscoelastic substance is transparence syndrome. This case shows an intrinsic
made difficult to evaluated. susceptibility for urrets-zavalia
A fixed, dilated pupil does not cause syndrome which alerts surgeons in the
a decrease in visual acuity23 but can case of second eye surgery
cause halos, glare, and REFERENCES
photophobia13,17,30 as well as cosmetic 1. Urrets-Zavalia A. Fixed dilated pupil, iris
abnormality.30 atrophy and secondary glaucoma: a
Some steps are needed to be taken distinct clinical entity following
during surgery to prevent the occurrence penetrating keratoplasty for keratoconus.
Am J Ophthalmol 1963; 56: 257-65.
of UZS. First, special care must be taken 2. Srinivasan M, Patnaik L. Fixed dilated
to avoid surgical trauma to the iris.15 pupil (Urrets-Zavalia syndrome) in
Second, the surgeon should consider corneal dystrophies. Cornea
performing peripheral iridotomy that 2004;23(1):81-3.
can reduce the risk of iris strangulation 3. Jastaneiah S, Al-Towerki AE, Al-Assiri
A. Fixed dilated pupil after penetrating
and pupillary block.20,22,31,32 Third, keratoplasty for macular corneal
recommended to have meticulous dystrophy and keratoconus. Am J
clearance of any viscoelastic Ophthalmol 2005;140(3):484-9.
material13,28 and to leave only a small 4. Minasian M, Ayliffe W. Fixed dilated
amount of air at the anterior chamber pupil following deep lamellar
keratoplasty (Urrets-Zavalia syndrome).
when air is needed (i.e., in DSAEK or Br J Ophthalmol 2002;86(1):115-6.
DALK with Descemet membrane 5. Maurino V, Allan BD, Stevens JD, Tuft
perforation).5,33 SJ. Fixed dilated pupil (Urrets-Zavalia
So far, apparently, there is no syndrome) after air/gas injection after
efficient pharmacological treatment for deep lamellar keratoplasty for
keratoconus. Am J Ophthalmol
irreversible mydriasis once the problem 2002;133(2):266-8.
has appeared.35 In some cases, there are 6. Russell HC, Srinivasan S. Urrets-Zavalia
several surgeries that has been reported syndrome following Descemet’s
to fix these kind problem (UZS) for stripping endothelial keratoplasty triple
example circular iris suture. This type of procedure. Clin Experiment Ophthalmol
2011;39(1):85-7.
surgery will give favorable outcome in 7. Jain R, Assi A, Murdoch IE. Urrets-
which it will increase visual acuity and Zavalia syndrome following
decrease glare.36 In this case, the patient trabeculectomy. Br J Ophthalmol
has several symptoms that are similar to 2000;84(3):338-9.
the ones that has been reported above, 8. Yuzbasioglu E, Helvacioglu F, Sencan S.
Fixed, dilated pupil after phakic
which are the persistant dilation of the intraocular lens implantation. J Cataract
pupil, atrophy of the iris that is probably Refract Surg 2006;32(1):174-6.
caused by trauma of the iris during 9. Espana EM, Ioannidis A, Tello C, et al.
surgery, and also the increase of intra Urrets-Zavalia syndrome as a
complication of argon laser peripheral
iridoplasty. Br J Ophthalmol
2006;91(4):427-9. 2013;251:809e15
10. Mocan MC, Bozkurt B, Irkec M, Orhan 24. Walton DS. Urrets-Zavalia syndrome
M. Urrets-Zavalia syndrome following following goniotomy in a child. J
iatrogenic pupil dilation in eyes with AAPOS. 2013;17:114e5
pigment dispersion. Can J Ophthalmol 25. Aralikatti AK, Tomlins PJ, Shah S.
2009;44(2):216-7. Urrets-Zavalia syndrome following
11. Uribe LE. Fixed pupil following intracameral C3F8 injection for acute
keratoplasty. Evaluation of six cases. Am corneal hydrops. Clin Experiment
J Ophthalmol 1967;63(6):1682- 6. Ophthalmol. 2008;36:198e9
12. Urrets-Zavalia A. Fixed dilated pupil, iris 26. Bozkurt KT, Acar BE, Acar S. Fixed
atrophy and secondary glaucoma: a dilated pupilla as a common complication
distinct clinical entity following of deep anterior lamellar keratoplasty
penetrating keratoplasty for keratoconus. complicated with Descemet membrane
Am J Ophthalmol 1963; 56: 257-65. perforation. Eur J Ophthalmol.
13. Gasset AR. Fixed dilated pupil following 2013;23:164e70
penetrating keratoplasty in keratoconus 27. Bourcier T, Laplace O, Touzeau O, et al.
(Castroviejo syndrome). Ann Ophthalmol Urrets-Zavalia syndrome. J Fr
1977; 9: 623-8. Ophtalmol. 2001;24:303e8
14. Minasian M, Ayliffe W. Fixed dilated 28. Selaru D, Diaconu E, Ma!celaru D. A
pupil following deep lamellar case of an incomplete Urrets-Zavalia
keratoplasty (Urrets-Zavalia syndrome). syndrome as a result of operated
Br J Ophthalmol 2002; 86: 115-116. keratoconus. Oftalmologia. 1998;45:76e8
15. Tuft SJ, Buckley RJ. Iris ischemia 29. Golnik KC, Hund PW, Apple DJ. Atonic
following penetrating keratoplasty for pupil after cataract surgery. J Cataract
keratoconus (Urrets-Zavalia syndrome). Refract Surg. 1995;21:170e5
Cornea 1995; 14: 618-22. 30. Tan AK, Humphry RC. The fixed dilated
16. Kaeser PF, Kawasaki A. Disorders of pupil after cataract surgery-is it related to
pupillary structure and function. Neurol intraocular use of hypromellose? Br J
Clin. 2010;28:657e77 Ophthalmol. 1993;77:639e41
17. Bourcier T, Laplace O, Touzeau O, et al. 31. Naumann GO. Iris ischaemia following
Urrets-Zavalia syndrome. J Fr penetrating keratoplasty for keratoconus
Ophtalmol. 2001;24:303e8 (Urrets-Zavalia syndrome). Cornea.
18. Saraux H, Offret H, Binaghi M. Urrets- 1997;16:120
Zavalia syndrome. Bull Soc Ophtalmol 32. Nguyen NX, Langenbucher A, Seitz B, et
Fr. 1978;78:579e84 al. Frequency and risk factors of
19. Jastaneiah S, Al-Towerki AE, Al-Assiri intraocular pressure increase after
A. Fixed dilated pupil after penetrating penetrating keratoplasty. Klin Monbl
keratoplasty for macular corneal Augenheilkd. 2000;217:77e81
dystrophy and keratoconus. Am J 33. Fournie ́ P, Ponchel C, Malecaze F, et al.
Ophthalmol. 2005;140:484e9 Fixed dilated pupil (Urrets-Zavalia
20. Davies PD, Ruben M. The paretic pupil: syndrome) and anterior subcapsular
its incidence and aetiology after cataract formation after Descemet
keratoplasty for keratoconus. Br J stripping endothelial keratoplasty.
Ophthalmol. 1975;59:223e8 Cornea. 2009;28:1184e6
21. Bonnet M, Lemarchands H, Martin J. 34. Fournie ́ P, Ponchel C, Malecaze F, et al.
Prevention and treatment of the Fixed dilated pupil (Urrets-Zavalia
“irreducible mydriasiseprogressive syndrome) and anterior subcapsular
atrophy of the iris” syndrome following cataract formation after Descemet
perforating keratoplasty for keratoconus. stripping endothelial keratoplasty.
Ann Ocul (Paris). 1969;202:1139e46 Cornea. 2009;28:1184e6
22. Flament J, Schraub M, Guimaraes R, et 35. Boyd, Samuel, MD; Gutierez, Angela
al. Urrets-Zavalia syndrome and Maria, MD; McCulley, James P, MD.
glaucomatous cataract. Etiopathogenic Atlas and Text of Corneal Pathology and
and nosologic discussion. Surgery 2011:24:408
Ophthalmologica. 1984;189:186e94 36. Jorge L, et al. Management of
23. Figueiredo GS, Kolli SS, Ahmad S, et al. Complication in Refractive Surgery
Urrets-Zavalia syndrome following 2008:13.3:251
penetrating keratoplasty for keratoconus.
Graefes Arch Clin Exp Ophthalmol.
You might also like
- BCSC Reading Schedule 2019-2020Document11 pagesBCSC Reading Schedule 2019-2020Mari Martinez100% (1)
- Tatalaksana Glaukoma Sekunder Dengan Sklerouveitis - Ericka Febriyanti Pratama PuatriDocument16 pagesTatalaksana Glaukoma Sekunder Dengan Sklerouveitis - Ericka Febriyanti Pratama PuatristrjuhanengsihNo ratings yet
- Case Review - EndophthalmitisDocument4 pagesCase Review - EndophthalmitisDr Shawgat Ul Karim KhanNo ratings yet
- Orbital Apex Syndrome Secondary To Herpes Zoster OphthalmicusDocument4 pagesOrbital Apex Syndrome Secondary To Herpes Zoster OphthalmicusYosiita KartinaaNo ratings yet
- Laporan Kasus Tatalaksana Pembedahan Pada Pasien Dengan Eksotropia Sensoris - Novaqua YandiDocument13 pagesLaporan Kasus Tatalaksana Pembedahan Pada Pasien Dengan Eksotropia Sensoris - Novaqua YandiMeliNo ratings yet
- Departemen Ilmu Kesehatan Mata Fakultas Kedokteran Universitas Padjadjaran Pusat Mata Nasional Rumah Sakit Mata Cicendo BandungDocument11 pagesDepartemen Ilmu Kesehatan Mata Fakultas Kedokteran Universitas Padjadjaran Pusat Mata Nasional Rumah Sakit Mata Cicendo BandungBambang RinandiNo ratings yet
- Endoftalmitis 3Document4 pagesEndoftalmitis 3andisibaNo ratings yet
- GDD Implan Dengan Pemasangan LIO Sekunder Iris Claw Retro Pupillary Pada Pasien Pasca Vitrektomi LianiDocument11 pagesGDD Implan Dengan Pemasangan LIO Sekunder Iris Claw Retro Pupillary Pada Pasien Pasca Vitrektomi LianivellafebrinaefitaNo ratings yet
- Tatalaksana Glaukoma Sekunder Sudut Tertutup Dengan Luksasi Lensa Dan Retinitis PigmentosalenoraDocument11 pagesTatalaksana Glaukoma Sekunder Sudut Tertutup Dengan Luksasi Lensa Dan Retinitis PigmentosalenoraSyahna AprilianiNo ratings yet
- Diagnosis BandingDocument10 pagesDiagnosis BandingIntan Rahmi NasyaNo ratings yet
- Cystoid Macular EdemaDocument5 pagesCystoid Macular EdemaAgnes Triana BasjaNo ratings yet
- Ostiogenesis ImperfectaDocument4 pagesOstiogenesis Imperfectamarlon GarcíaNo ratings yet
- Prabhakar 1Document4 pagesPrabhakar 1ChristaGisellaPirsouwNoyaNo ratings yet
- Letters To The EditorDocument8 pagesLetters To The EditorGheavita Chandra DewiNo ratings yet
- Implant Glaucoma Drainage DeviceDocument12 pagesImplant Glaucoma Drainage DeviceMCU BTMNo ratings yet
- Asian Upper Eyelid Blepharoplasty Sebagai Tatalaksana Dermatokalasis - Adessa RachmaDocument11 pagesAsian Upper Eyelid Blepharoplasty Sebagai Tatalaksana Dermatokalasis - Adessa Rachmafadil ahmadi100% (1)
- Canadian Journal of Ophthalmology - Journal Canadien D'ophtalmologie Volume Issue 2017 (Doi 10.1016 - J.jcjo.2017.01.022) Moinul, Prima Luong, Micah Bhamra, Jamie Kherani, Amin McWha - Aqueous MiDocument3 pagesCanadian Journal of Ophthalmology - Journal Canadien D'ophtalmologie Volume Issue 2017 (Doi 10.1016 - J.jcjo.2017.01.022) Moinul, Prima Luong, Micah Bhamra, Jamie Kherani, Amin McWha - Aqueous MiVinda Sari ErmizaNo ratings yet
- Vitrectomy Results in Proliferative Diabetic RetinopathyDocument3 pagesVitrectomy Results in Proliferative Diabetic RetinopathyRohamonangan TheresiaNo ratings yet
- Acc or Inti 2007Document6 pagesAcc or Inti 2007iwanNo ratings yet
- Penatalaksanaan Glaukoma Sekunder Refrakter Pada Implantasi Lensa Intraokular Bilik Mata Depan - Pauline Meilisa SihiteDocument13 pagesPenatalaksanaan Glaukoma Sekunder Refrakter Pada Implantasi Lensa Intraokular Bilik Mata Depan - Pauline Meilisa SihiteZikra Herlius14No ratings yet
- Penatalaksanaan Pasien Glaukoma Sudut Terbuka Dengan PemasanganintanmaulaDocument10 pagesPenatalaksanaan Pasien Glaukoma Sudut Terbuka Dengan PemasanganintanmaulaShela GranityaNo ratings yet
- MainDocument4 pagesMainVicky ObandoNo ratings yet
- Case ReportDocument7 pagesCase ReportJeel GaralaNo ratings yet
- Tatalaksana Katarak Komplikata Yang Disebabkan Oleh Uveitis - Ericka Febriyanti Pratama Putri 1Document14 pagesTatalaksana Katarak Komplikata Yang Disebabkan Oleh Uveitis - Ericka Febriyanti Pratama Putri 1Cynthia Isra MandahutaNo ratings yet
- A Rare Case of Terson Syndrome With Subarachnoid HemorrhageDocument12 pagesA Rare Case of Terson Syndrome With Subarachnoid HemorrhageNinaNo ratings yet
- Tatalaksana Refractive Surprise Pada Bedah Katarak Bilateral - Wioma Surya DarmaDocument14 pagesTatalaksana Refractive Surprise Pada Bedah Katarak Bilateral - Wioma Surya DarmaAndreas SimatupangNo ratings yet
- Makrufa NWDocument6 pagesMakrufa NWPujiastutiNo ratings yet
- V36N4p293 PDFDocument5 pagesV36N4p293 PDFsiscaNo ratings yet
- Journal Asli - Mash - Ab Zirrun Al-Qomah - 212011101095Document4 pagesJournal Asli - Mash - Ab Zirrun Al-Qomah - 212011101095tttttNo ratings yet
- Tatalaksana Dan Prognosis Severe Visual Impairment Pada Miopia Patologi - Nikho Melga ShalimDocument14 pagesTatalaksana Dan Prognosis Severe Visual Impairment Pada Miopia Patologi - Nikho Melga ShalimOt PtkNo ratings yet
- Diagnosis Dan Tatalaksana Dislokasi Lensa Intraokular Ke Posterior Dengan Prosedur IOL Exchange To Iris Claw Retropupillary - Siti AisyahDocument13 pagesDiagnosis Dan Tatalaksana Dislokasi Lensa Intraokular Ke Posterior Dengan Prosedur IOL Exchange To Iris Claw Retropupillary - Siti Aisyahmemmuse95No ratings yet
- Showphacomrphic Glaucoma Managemnet by Surgical and Medical Management TextDocument8 pagesShowphacomrphic Glaucoma Managemnet by Surgical and Medical Management Textdrvishalkulkarni2007No ratings yet
- 1 PBDocument4 pages1 PBRian YupitaNo ratings yet
- Ace SetiawanDocument11 pagesAce SetiawanGlaucoma UnhasNo ratings yet
- Retina 2012 Sep 32 (Suppl 2) S225-31Document7 pagesRetina 2012 Sep 32 (Suppl 2) S225-31roro207No ratings yet
- Acknowledgement: Aniridia Associated With Congenital Aphakia and Secondary GlaucomaDocument3 pagesAcknowledgement: Aniridia Associated With Congenital Aphakia and Secondary GlaucomaNisrina FarihaNo ratings yet
- Sympathetic Ophthalmia After Vitreoretinal Surgery: A Report of Two CasesDocument11 pagesSympathetic Ophthalmia After Vitreoretinal Surgery: A Report of Two CasesAlexander RezaNo ratings yet
- Five Year PROSE Treatment For Aniridic KojimaOct2016PAPDocument5 pagesFive Year PROSE Treatment For Aniridic KojimaOct2016PAP小島隆司No ratings yet
- Abstract Pachydermoperiostosis EnggresDocument4 pagesAbstract Pachydermoperiostosis EnggresKarina BudijantoNo ratings yet
- Cataract Extraction and Intraocular Lens Implantation in Children With UveitisDocument4 pagesCataract Extraction and Intraocular Lens Implantation in Children With UveitiskhairunnisaNo ratings yet
- Feliciatimmermann 2778Document2 pagesFeliciatimmermann 2778Calvin NugrahaNo ratings yet
- Management of Penetrating Eye Injury With Intraocular Foreign BodyDocument5 pagesManagement of Penetrating Eye Injury With Intraocular Foreign BodyChristian FaustNo ratings yet
- Parade Wspos Tipe 2Document3 pagesParade Wspos Tipe 2irwan_201291No ratings yet
- Visual Outcome After Phacomorphic GlaucomaDocument3 pagesVisual Outcome After Phacomorphic GlaucomaHassan KhanNo ratings yet
- Shankar Ganvit END PDFDocument4 pagesShankar Ganvit END PDFgyogi1989No ratings yet
- Catarta e HipoparatiroidismoDocument3 pagesCatarta e HipoparatiroidismoBernardo RomeroNo ratings yet
- Retinal Tear: An Unusual Complication of Ocular ToxoplasmosisDocument5 pagesRetinal Tear: An Unusual Complication of Ocular ToxoplasmosisMuhammad Irfan FaizNo ratings yet
- Toophtj 8 1Document2 pagesToophtj 8 1SusPa NarahaNo ratings yet
- Kag Rully (B.IG)Document7 pagesKag Rully (B.IG)Rully Dwi SaputraNo ratings yet
- Ablasio RetinaDocument23 pagesAblasio RetinaResa PutraNo ratings yet
- Tatalaksana Operatif Dan Pascaoperatif Pada Pasien Juvenile Open Angle Glaucoma JOAG - Andreas Lukita HalimDocument14 pagesTatalaksana Operatif Dan Pascaoperatif Pada Pasien Juvenile Open Angle Glaucoma JOAG - Andreas Lukita HalimINDRINo ratings yet
- Therapeutic Effectiveness of Toric Implantable Collamer Lens in Treating Ultrahigh Myopic AstigmatismDocument7 pagesTherapeutic Effectiveness of Toric Implantable Collamer Lens in Treating Ultrahigh Myopic AstigmatismStephanie PfengNo ratings yet
- Mcculley 2012Document11 pagesMcculley 2012Luisa Mayta PitmanNo ratings yet
- Tatalaksana Katarak Traumatika Dengan Open Globe Injury Pada Anak - Levandi MuljaDocument12 pagesTatalaksana Katarak Traumatika Dengan Open Globe Injury Pada Anak - Levandi MuljaFaisal radhiNo ratings yet
- 100255-Article Text-1482-2-10-20220311Document6 pages100255-Article Text-1482-2-10-20220311Fachry RahmanNo ratings yet
- 15) Refractory Open-Angle Glaucoma After Neodymium - Yttrium-Aluminum-Garnet Laser Lysis of Vitreous FloatersDocument6 pages15) Refractory Open-Angle Glaucoma After Neodymium - Yttrium-Aluminum-Garnet Laser Lysis of Vitreous FloatershasdiniNo ratings yet
- Artículo Oftalmología RetinaDocument1 pageArtículo Oftalmología RetinaJavier Burgos CárdenasNo ratings yet
- Clinical Study: XEN Glaucoma Implant With Mitomycin C 1-Year Follow-Up: Result and ComplicationsDocument6 pagesClinical Study: XEN Glaucoma Implant With Mitomycin C 1-Year Follow-Up: Result and ComplicationsAldoNo ratings yet
- JORS Volume 2 Issue 1 Pages 19-21Document3 pagesJORS Volume 2 Issue 1 Pages 19-21Praveen DhanapalNo ratings yet
- Msor 000504Document3 pagesMsor 000504MudrikahHaniyahNo ratings yet
- Complications in UveitisFrom EverandComplications in UveitisFrancesco PichiNo ratings yet
- Contouring The Lens and Lacrimal Glands On t2 Weighted Mri - NewDocument10 pagesContouring The Lens and Lacrimal Glands On t2 Weighted Mri - NewJulian CiabattariNo ratings yet
- Data Upload ShopeeDocument28 pagesData Upload Shopeebanyakmauu borNo ratings yet
- Eye StructureDocument15 pagesEye StructurekathyNo ratings yet
- Yang Sudah Di KerjakanDocument4 pagesYang Sudah Di Kerjakanjazuliswdstore01No ratings yet
- Care of The Clients With Eye and Ear DisorderDocument35 pagesCare of The Clients With Eye and Ear DisorderKristine Joy RevañoNo ratings yet
- IOL PowerDocument273 pagesIOL Powermarlon García100% (2)
- Abebizuhan ZigaleDocument45 pagesAbebizuhan Zigaleabiraham zigaleNo ratings yet
- 2019 Health Assessment Examination - EyesDocument2 pages2019 Health Assessment Examination - Eyesharley dela cruzNo ratings yet
- Lens and The EyeDocument58 pagesLens and The EyeEisle Keith Rivera TapiaNo ratings yet
- Resume ICDDocument6 pagesResume ICDKomang AstrieNo ratings yet
- Special Senses) 3. Photoreceptors - Rods and Cones - KeyDocument1 pageSpecial Senses) 3. Photoreceptors - Rods and Cones - Keyranag59100No ratings yet
- Q2 - First Summative Test in All Subjects With TOSDocument21 pagesQ2 - First Summative Test in All Subjects With TOSapril joy tamayoNo ratings yet
- Pinxel-V-S - She-Pxs006Document15 pagesPinxel-V-S - She-Pxs006Ashraf AboNo ratings yet
- Opinioes Exames Ebo e IcoDocument8 pagesOpinioes Exames Ebo e Icoapi-3595301060% (1)
- BIO101 Student Notes PRELIM Integumentary System1Document4 pagesBIO101 Student Notes PRELIM Integumentary System1Kirstine Valerie MandalonesNo ratings yet
- Basics of FundusDocument29 pagesBasics of Fundusikayapmd100% (1)
- Strabismus PDFDocument170 pagesStrabismus PDFShari Ali100% (1)
- (Brief Discussion of The Lesson, If Possible Cite Examples) : SUBJECT (Uppercase and Bold)Document33 pages(Brief Discussion of The Lesson, If Possible Cite Examples) : SUBJECT (Uppercase and Bold)KD DelayunNo ratings yet
- Traktus UveaDocument90 pagesTraktus UveaAudrey Ira Yunita100% (1)
- Peudophakia New-2Document4 pagesPeudophakia New-2KjoNo ratings yet
- Anatomy of Eyes: January 2009Document7 pagesAnatomy of Eyes: January 20091710105 Sean Rio SimangunsongNo ratings yet
- Sclerology Miller RevisiDocument177 pagesSclerology Miller RevisiTri Ayu Eka PaksiNo ratings yet
- World Through Our Senses (All Sensory Organs)Document48 pagesWorld Through Our Senses (All Sensory Organs)Chin Kok Soon100% (3)
- Sekolah Menengah Kebangsaan Tanjong Rambutan 31250, Tanjong Rambutan Science Form 2Document5 pagesSekolah Menengah Kebangsaan Tanjong Rambutan 31250, Tanjong Rambutan Science Form 2Jannah SulaimanNo ratings yet
- Icd X MataDocument11 pagesIcd X MataLilis tri wardhijaniNo ratings yet
- Integumentary Lab ActDocument5 pagesIntegumentary Lab ActJASMINE LAURONNo ratings yet
- General Survey and Integumentary I. General Appearance and Mental Status Normal Findings Actual Findings Analysis and InterpretationDocument9 pagesGeneral Survey and Integumentary I. General Appearance and Mental Status Normal Findings Actual Findings Analysis and InterpretationAllana RayosNo ratings yet
- Effects of Genipin Corneal Crosslinking in Rabbit CorneasDocument5 pagesEffects of Genipin Corneal Crosslinking in Rabbit CorneasMauricio NarvaezNo ratings yet
- Skin ProjectDocument16 pagesSkin ProjectMonique WilliamsNo ratings yet