Professional Documents
Culture Documents
Emg Piel PDF
Emg Piel PDF
Uploaded by
Rafael ValverdeOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Emg Piel PDF
Emg Piel PDF
Uploaded by
Rafael ValverdeCopyright:
Available Formats
CM E
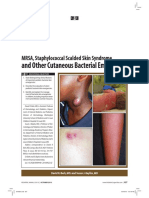
MRSA, Staphylococcal Scalded Skin Syndrome,
and Other Cutaneous Bacterial Emergencies
CM E EDUCATIONAL OBJECTIVES
1. State distinguishing clinical features
of important pediatric bacterial skin
emergencies.
2. Describe the evaluation of select
pediatric bacterial skin emergencies.
3. Identify and explain the manage-
ment of bacterial skin emergencies
in children, including important treat-
ment and infection control measures.
David R. Berk, MD, is Assistant Professor
of Dermatology and Pediatrics, Depart-
ment of Internal Medicine and Pediatrics,
Division of Dermatology, Washington
University School of Medicine and St. Louis
Children’s Hospital, St. Louis, MO.
Susan J. Bayliss, MD, is Professor of Der-
matology and Pediatrics, Director of Pediat-
ric Dermatology, Residency Program Direc-
tor, Department of Internal Medicine and
Pediatrics, Division of Dermatology, Wash-
ington University School of Medicine and St.
Louis Children’s Hospital, St. Louis, MO.
Address correspondence to: David R.
Berk, MD, Campus Box 8123, 4921 Parkview
Place, St. Louis, MO 63110; fax: 314-747-
8693; e-mail: dberk@dom.wustl.edu.
Dr. Berk and Dr. Bayliss have disclosed no
relevant financial relationships.
doi: 10.3928/00904481-20100922-02
David R. Berk, MD; and Susan J. Bayliss, MD
PEDIATRIC ANNALS 39:10 | OCTOBER 2010 www.PediatricSuperSite.com | 627
3910Berk.indd 627 9/24/2010 4:21:45 PM
CM E
C
utaneous bacterial infections glycan, allowing cell wall synthesis SSSS
are important to recognize in even in the presence of beta-lactams. SSSS is caused by infections with
pediatrics. Some may actually The mecA gene may be carried on epidermolytic (also known as exfolia-
be emergencies. These include localized small-sized (eg, the staphylococcal tive) toxin (ET)-producing S. aureus.
skin infections, such as methicillin-re- cassette chromosome mec type IV or SSSS preferentially affects newborns
sistant Staphylococcus aureus (MRSA) V of community-acquired MRSA) or and children younger than 5 years.13 The
infections, as well as more generalized large-sized (eg, the staphylococcal nares, conjunctivae, perioral region,
toxin-mediated diseases, such as toxic cassette chromosome mec type I, II, or umbilicus, and perineum are common
shock syndrome (TSS) and staphylo- III of hospital-acquired MRSA) gene foci of infection. When involvement is
coccal scalded skin syndrome (SSSS). cassettes. The latter can also confer localized, infections manifest as bul-
It is important for pediatricians to rec- resistance to many non-beta-lactam lous impetigo. On the other hand, when
ognize and distinguish these cutaneous antibiotics. hematogenous spread of ET occurs, the
bacterial emergencies so treatment and An important virulence factor for generalized form of SSSS develops.
appropriate infection control measures MRSA is Panton-Valentine leukocidin Cutaneous findings include widespread
can be promptly initiated. (PVL). PVL is uncommon among non- erythema, which may start on the head
MRSA isolates. PVL acts as a cytotox- and evolve into superficial skin peel-
MRSA in, causing lysis of leukocytes and tis- ing, flaccid bullae, and denuded tender
MRSA poses therapeutic and pub- sue necrosis. In addition, PVL is more skin (see Figure 2, page 630).14
lic health challenges because of its often found in MRSA strains, which Erythema arises abruptly, spreads
increasing incidence, enhanced viru- contain staphylococcal cassette chro- rapidly, and demonstrates characteris-
lence, and frequent multidrug re- mosome mec type IV or V rather than tic flexural and perioral prominence,
sistance.1-3 MRSA infections most I, II, or III. PVL is encoded by the lukS- including radial perioral fissures. There
commonly involve the skin and soft PV and lukF-PV genes. Other virulence also may be a predilection for areas of
tissues, typically manifesting as sup- factors for MRSA include alpha-hemo- mechanical stress, such as shoulders,
purative lesions such abscesses, fu- lysin and phenol soluble modulins.9 buttocks, hands, and feet. Skin tender-
runcles, folliculitis, or cellulitis (see When possible, incision and drain- ness is a key feature. The Nikolsky sign,
Figure 1, page 629).4-6 Infections may age are a critical part of initial thera- defined as extension of blistering with
occur at any site but especially on the py for skin and soft tissue infections gentle pressure at the edge of a bulla,
buttocks and lower extremities. Be- suspected to be due to MRSA.10,11 may be elicited. Other features include
cause pustular lesions commonly have Antibiotics should be considered as fever, malaise, irritability, purulent rhi-
a necrotic center, they are often con- an adjunctive therapy, especially for norrhea, conjunctivitis, and poor oral
fused with spider bites. Skin and soft- cases with purulent drainage, rapid intake. The primary source of infection
tissue infections caused by MRSA progression, large abscess size, and is often around the head and neck area
cannot be distinguished reliably on the presence of systemic manifesta- or circumcision site. Rarely, SSSS may
clinical grounds from those caused by tions or immunocompromise. Antibi- result from ET derived from extracu-
methicillin-sensitive Staphylococcus otic therapy should be based on local taneous infections, such as pneumonia,
aureus.7 Risk factors include trauma resistance patterns and the results of pyomyositis, endocarditis, urinary tract
to the skin, contact with an individual cultures and susceptibility testing. In infection, and septic arthritis.15
infected with MRSA, rectal and/or na- general, non-beta-lactam antibiotics The predilection of SSSS for new-
sal colonization, crowded households, should be used for cases that are ei- borns and young children may be
childcare attendance, antibiotic usage ther suspected to be due to MRSA or caused by decreased renal clearance of
in the past year, contact sports, chronic which do not respond to initial inci- ET and/or the lack of anti-toxin anti-
skin disease, and pets.3 sion, drainage, and beta-lactam antibi- bodies. Outbreaks in nurseries and in-
The mecA gene provides MRSA otics. These agents include clindamy- tensive care units are well described.16
with its methicillin resistance.8 This cin, trimethoprim/sulfamethoxazole, Two types of ET mediate SSSS, in-
gene encodes penicillin-binding pro- tetracycline, linezolid, or vancomy- cluding ET-A and ET-B, both of which
tein 2a, a transpeptidase with very cin. Decolonization measures, such are serine proteases.17,18 These two
low affinity for beta-lactams. Penicil- as intranasal mupirocin, dilute bleach ETs target desmoglein-1, a cell adhe-
lin-binding protein 2a catalyzes the baths, and bathing with antimicrobial sion protein located in desmosomes in
transpeptidation reactions of peptido- soaps, can be helpful adjuncts.12 the superficial epidermis, explaining
628 | www.PediatricSuperSite.com PEDIATRIC ANNALS 39:10 | OCTOBER 2010
3910Berk.indd 628 9/24/2010 4:21:49 PM
CM E
the superficial cleavage plane within
the stratum granulosum seen in le-
sions of SSSS. These ETs also pos-
sess superantigen activity.19 Strains of
ET-producing S. aureus usually belong
to phage groups 1, 2, or 3, especially
group 2 strains 71 and 55. ET-A is
chromosomally encoded, whereas ET-
B is plasmid derived.
SSSS is a clinical diagnosis that can
be confirmed by culturing S. aureus
from foci of infection, such as from
the nostrils, conjunctivae, umbilicus,
or nasopharynx.20 Culturing exfoliative
lesions and blisters is not helpful be-
cause these are induced by circulating
A B
ET and, therefore, are typically sterile,
Figure 1. Children with abscesses (A) and carbuncles (B) typical of methicillin-resistant Staphylococcus
unless secondarily infected. Bacte- aureus.
remia is uncommon in children with
SSSS. Occasionally, a skin biopsy or adjustments made based on local re- underlying diseases, such as immuno-
the painless removal and examination sistance patterns and sensitivities of compromise or renal failure.22
of blisters roofs can help to confirm a obtained cultures. Skin care generally
superficial cleavage plane, at the level consists of bland emollients (petro- BULLOUS IMPETIGO
of the stratum granulosum. leum jelly) and minimal handling of Impetigo is a contagious, superficial
The main differential diagnosis for patients. Mupirocin can be used at foci skin infection that occurs in bullous or
SSSS is toxic epidermal necrolysis of infection. Gentle cleansing may help non-bullous forms.23,24 Most cases are
(TEN), a more life-threatening blister- prevent secondary infection. Removal non-bullous, caused by streptococci,
ing disease characterized by a signifi- of dried skin with bathing is not neces- staphylococci, or both. Clinically, non-
cantly lower cleavage plane below the sary initially when the skin is too ten- bullous impetigo demonstrates the clas-
junction of the epidermis and dermis. der to touch but is used an adjunct later. sic honey-colored crust and commonly
TEN is discussed later in this issue. Other important measures include con- affects the face, especially around the
TEN involves full thickness necrosis tact isolation and pain management. nose. The differential diagnosis some-
of the epidermis. Unlike SSSS, TEN Corticosteriods should be avoided. times includes herpes simplex infection.
demonstrates characteristic mucosal The prognosis of SSSS is usually In contrast, bullous impetigo is the local-
involvement. TEN is quite unusual in good in children and is more guarded ized version of SSSS and is, therefore,
infants. Other differential diagnoses in infants. Complications include sep- always caused by S. aureus. Clinically,
may include epidermolysis bullosa, sis, secondary infections, electrolyte bullous impetigo presents with flac-
epidermolytic hyperkeratosis, thermal imbalances, fluid losses, and hypother- cid bullae and tender erosions, without
burns, scarlet fever, toxic shock syn- mia. Compared with TEN, the higher much surrounding erythema (see Figure
drome, Kawasaki disease, and nutri- blister cleavage plane in SSSS confers 3, page 630). A rim of scale may be seen
tional deficiencies. a better prognosis, causing less water at edge of erosions, where the blister has
Treatment of generalized SSSS in- loss and temperature instability. The become denuded. Bullous impetigo of-
cludes hospitalization for most young mortality rate in SSSS is less than 5%. ten occurs in infancy, particularly in the
children, with intravenous antibiotics In many cases, patients respond rapid- diaper area. Treatment includes topical
and close monitoring of electrolytes, ly to treatment, with complete recov- mupirocin or, for more widespread or
temperature, and hemodynamics.20,21 ery within 2 or 3 weeks. Because the severe cases, oral antibiotics. Similar to
Typical empiric antibiotic choices cleavage plane in SSSS is superficial, SSSS, bullous impetigo is characterized
should include a penicillinase-resistant lesions heal without scarring. SSSS is by a superficial cleavage plane, is medi-
penicillin, first- or second-generation more life-threatening in newborns as ated by the same ET-A and -B, and typi-
cephalosporin, and clindamycin, with well as adults, especially those with cally does not scar.
PEDIATRIC ANNALS 39:10 | OCTOBER 2010 www.PediatricSuperSite.com | 629
3910Berk.indd 629 9/24/2010 4:21:49 PM
CM E
A B
Figure 2. Child demonstrating superficial skin peeling, denuded tender skin (A), flexural prominence, and periorificial crusting (B) typical of staphylococcal
scalded skin syndrome.
STAPHYLOCOCCAL TSS with upper airway infections, burns, Clinical features are similar for
Staphylococcal TSS is a systemic postpartum infections, cutaneous in- menstrual and non-menstrual TSS. It
toxin-mediated disorder that may occur fections, surgical procedures, and starts with the abrupt onset of high
in menstrual or non-menstrual forms. nasal packing.26 Staphylococcal TSS fever, abdominal distress, myalgias,
The menstrual form tends to occur in is mediated by toxic shock syndrome and headache, followed by shock and
young, healthy women with staphylo- toxin-1 and staphylococcal enterotox- multisystem organ failure.25,26,28-30
coccal vaginal infection or colonization ins-A, -B, and -C. These toxins act Within 1 to 3 days of disease onset,
by phage group 1 S. aureus. Historical- as superantigens, directly activating patients develop a widespread scar-
ly, it was associated with the usage of T cells, resulting in massive cytokine latiniform eruption or erythema with
superabsorbent tampons.25 release.27 TSS toxin-1 may also de- flexural accentuation. Other common
Non-menstrual TSS is also caused crease clearance of endotoxins from findings include pharyngitis, conjunc-
by S. aureus, and may be associated gut flora. tival and mucosal membrane hyper-
ermia, strawberry tongue, and gener-
alized edema, especially of the hands
and feet. A pruritic, maculopapular
erythema occurs within 1 to 2 weeks,
with a predilection for the palms and
soles, sparing the face.
One to 3 weeks after disease on-
set, full thickness desquamation of the
palms (especially subungually), soles,
and perineum occurs. Nail and hair
shedding may occur later. Particularly
concerning complications include re-
spiratory distress syndrome, which is
more common in children, as well as
disseminated intravascular coagula-
tion, myocardial dysfunction, and renal
failure. Positive blood cultures are un-
Figure 3. Flaccid bullae in the diaper area of a newborn with bullous impetigo.
common (< 15%), and mortality is less
than 3%. Diagnosis is based on clinical
criteria (see Sidebar 1, page 631).
630 | www.PediatricSuperSite.com PEDIATRIC ANNALS 39:10 | OCTOBER 2010
3910Berk.indd 630 9/24/2010 4:21:50 PM
CM E
SIDEBAR 1.
CDC Case Definition
for SSSS
Clinical Criteria
• Temperature > 38.9°C
• Diffuse macular erythroderma
• Desquamation, 1 to 2 weeks after onset,
particularly palmoplantar
• Hypotension for age
• Multisystem involvement, three or more
of the following:
Gastrointestinal
Muscular
Mucous membranes
Renal
Hepatic
Hematologic
Figure 4. Papular, sandpaper-like plaques with streptococcal infections.
Central nervous system
Laboratory Criteria
The differential diagnosis of staph- particular toxin-producing strains of Negative test results for the following (if
obtained):
ylococcal TSS includes streptococcal Streptococcus pyogenes, including M
• Throat, CSF, blood cultures (although
toxic shock syndrome, scarlet fever, protein types 1, 3, 12 and 28.31 Impor-
blood may be positive for S. aureus)
Kawasaki disease, Rocky Mountain tant toxins in the pathogenesis include
• Serological tests for Rocky Mountain
spotted fever, viral exanthems, and streptococcal pyrogenic exotoxin-A, spotted fever, measles, or leptospirosis
drug reactions, such as TEN. Unlike -B, and -C, streptococcal superanti-
many of the differential diagnoses, gen, and mitogenic factor.27 Unlike ‘Probable’ disease: Laboratory criteria +
staphylococcal TSS is always charac- staphylococcal TSS, STTS is more of- 4 out of 5 clinical criteria
terized by shock and multiorgan fail- ten associated with a focal tissue infec- ‘Confirmed’ disease: Laboratory criteria
ure. Skin biopsies in staphylococcal tion and bacteremia, as well as a more + all 5 clinical criteria (unless patient
TSS reveal non-specific findings and fulminant course and greater lethality dies before desquamation)
are usually unnecessary, but can help (mortality of 30% to 60%).32,33 Source: www.cdc.gov/ncphi/disss/nndss/casedef/toxicss-
current.htm
eliminate some conditions in the differ- Moreover, patients with STSS typi-
ential diagnosis, such as TEN. cally present with severe pain, usually
The mainstay of treatment of staphy- affecting a leg and often out of propor-
lococcal TSS includes rapid identifica- tion to objective findings, such as ede- onset, although this is less common than
tion and drainage of infections, as well ma and erythema. Necrotizing fasciitis in staphylococcal TSS. A strawberry
as removal of foreign bodies that could or myonecrosis are possible.33,34 Some tongue is rare in STSS. More than half
harbor infection (eg, meshes, tampons, patients with STSS have prodromal of cases demonstrate positive blood cul-
nasal packing). In addition, intravenous influenza-like symptoms. Nausea and tures. Clinical criteria are summarized in
penicillinase-resistant antistaphylococ- vomiting are less common than in staph- Sidebar 2 (see page 632).
cal antibiotics and supportive care are ylococcal TSS. Very soon after presen- Because varicella is a risk factor for
necessary. Antibiotics that inhibit toxin tation, patients quickly develop shock invasive S. pyogenes, clinicians treating
production, including clindamycin, flu- and multiorgan failure, such as renal patients with varicella should have a high
oroquinolones, and rifampin, are some- failure, respiratory distress syndrome, index of suspicion if there is persistent
times recommended. and disseminated intravascular coagu- or recurrent fevers (beyond day 4).35
lation. Bullae are uncommon and are Treatment of STSS involves sup-
STREPTOCOCCAL TSS associated with poor prognosis. Some portive management in an intensive
Streptococcal toxic shock syndrome patients demonstrate erythroderma and care unit, early surgical debridement,
(STSS) is caused by infection with desquamation 1 to 2 weeks after disease and intravenous antibiotics. Clinda-
PEDIATRIC ANNALS 39:10 | OCTOBER 2010 www.PediatricSuperSite.com | 631
3910Berk.indd 631 9/24/2010 4:21:53 PM
CM E
SIDEBAR 2. petechiae (Forschheimer’s spots) may be REFERENCES
present on the palate, as well as a “white 1. Cohen PR. Community-acquired methi-
CDC Case Definition for strawberry tongue” that sloughs to be-
cillin-resistant Staphylococcus aureus
skin infections: implications for patients
Streptococcal TSS come a “red strawberry tongue.”38,39 and practitioners. Am J Clin Dermatol.
Clinical Case Definition The rash of scarlet fever is char- 2007;8(5):259-270.
• Hypotension for age/shock 2. Elston DM.Community-acquired methicillin-
acterized by blanchable, confluent, resistant Staphylococcus aureus. J Am Acad
• At least two of the following: erythematous macules and patches, as Dermatol. 2007;56(1):1-16; quiz 17-20.
Renal impairment well as tiny papules with a dry, sand- 3. Kil EH, Heymann WR, Weinberg JM. Methi-
Coagulopathy cillin-resistant Staphylococcus aureus: an up-
paper-like texture (see Figure 4, page
date for the dermatologist, Part 1: Epidemiol-
Hepatic involvement 631). Lesions often start on the upper ogy. Cutis. 2008;81(3):227-233.
Adult respiratory distress syndrome trunk, then generalize over days, spar- 4. Gorwitz RJ. A review of community-associ-
Generalized erythematous rash with or ing the palms and soles, and involving ated methicillin-resistant Staphylococcus au-
without desquamation reus skin and soft tissue infections. Pediatr
the legs last. Pastia’s lines refer to ac- Infect Dis J. 2008;27(1):1-7.
Soft-tissue necrosis (eg, necrotizing centuation of erythema with linear pe- 5. Groner A, Laing-Grayman D, Silverberg NB.
fasciitis or myositis, or gangrene) Outpatient pediatric community-acquired
techiae in skin folds. Accentuation is
methicillin-resistant Staphylococcus aure-
Laboratory Criteria also common at dependent sites. Facial us: a polymorphous clinical disease. Cutis.
• Isolation of group A beta-hemolytic flushing with circumoral pallor is com- 2008;81(2):115-122.
Streptococcus mon. The rash fades within a week and 6. Kil EH, Heymann WR, Weinberg JM. Methi-
cillin-resistant Staphylococcus aureus: an
‘Probable’ disease: Clinical case defini-
is followed a week later by a superfi-
update for the dermatologist, Part 2: Patho-
tion + isolation of group A beta-hemo- cial desquamation, especially in skin genesis and cutaneous manifestations. Cutis.
lytic Streptococcus from a non-sterile site folds, on the face and in sheets from the 2008;81(3):247-254.
‘Confirmed’ disease: Clinical case defini- hands and feet (may take 2 to 6 weeks). 7. Miller LG, Perdreau-Remington F, Bayer AS,
et al. Clinical and epidemiologic characteris-
tion + isolation of group A beta-he- Beau’s lines (transverse nail grooves) tics cannot distinguish community-associated
molytic Streptococcus from a normally and telogen effluvium (hair loss) may methicillin-resistant Staphylococcus aureus
sterile site infection from methicillin-susceptible S. au-
present after the illness. Early compli-
reus infection: a prospective investigation.
Source: www.cdc.gov/ncphi/disss/nndss/casedef/strepto- cations may include pneumonia, otitis Clin Infect Dis. 2007;44(4):471-482.
coccalcurrent.htm
media, bacteremia, and osteomyelitis. 8. Inglis B, Matthews PR, Stewart PR. The ex-
Later complications may include glo- pression in Staphylococcus aureus of cloned
DNA encoding methicillin resistance. J Gen
mycin is often used with the intent of merulonephritis and rheumatic fever.
Microbiol. 1988;134(6):1465-1469.
impairing toxin production. Because of The differential diagnosis of scarlet 9. Hamilton SM, Bryant AE, Carroll KC, et al.
the extent of invasive infection and the fever includes Kawasaki disease, SSSS, In vitro production of panton-valentine leu-
required debridement, morbidity and staphylococcal and streptococcal TSS, kocidin among strains of methicillin-resistant
Staphylococcus aureus causing diverse infec-
disfigurement often occur in survivors. mononucleosis, fifth disease, rubella, tions. Clin Infect Dis. 2007;45(12):1550-1558.
rubeola, other viral exanthems, juvenile 10. Elston DM. Practical management tips for
SCARLET FEVER rheumatoid arthritis, and drug reac- methicillin-resistant Staphylococcus aureus.
Cutis. 2008;81(4):311-313.
Scarlet fever is caused by infection tions. Similar rashes can also be seen
11. Kil EH, Heymann WR, Weinberg JM. Methi-
with particular S. pyogenes strains that with pharyngeal infections with S. au- cillin-resistant Staphylococcus aureus: an
produce streptococcal pyrogenic (eryth- reus, Arcanobacterium haemolyticum, update for the dermatologist, Part 3: Clinical
management. Cutis. 2008;81(4):327-335.
rogenic) exotoxin-A, -B, or -C.36 Strep- or Haemophilus influenzae. Cultures of
12. Kluytmans J, van Belkum A, Verbrugh
tococcal tonsillopharyngitis is usually infected areas should be obtained. Skin H.Nasal carriage of Staphylococcus aureus:
the source of infection. Wound infec- biopsies are nonspecific and are not epidemiology, underlying mechanisms,
tions, burns, pelvic infections, food- generally helpful. and associated risks. Clin Microbiol Rev.
1997;10(3):505-520.
borne outbreaks, and cellulitis are other Before the discovery of antibiot- 13. Ladhani S, Evans RW. Staphylococcal
possible sources.37 ics, the mortality of scarlet fever was scalded skin syndrome. Arch Dis Child.
Most patients abruptly develop fe- approximately 20%.40 The antibiotic 1998;78(1):85-88.
14. Chang P, Mukundan D. Picture of the month.
ver and sore throat, followed 1 to 2 days of choice for scarlet fever is penicil- Staphylococcal scalded skin syndrome. Arch Pe-
later by a scarlatiniform rash. Headache, lin. Treatment is important to relieve diatr Adolesc Med. 2008;162(12):1189-1190.
malaise, myalgias, vomiting, abdominal symptoms, to minimize spreading the 15. Sladden MJ, Mortimer NJ, Elston G, Newey
M, Harman KE. Staphylococcal scalded skin
pain, lymphadenopathy, and leukocytosis infection to others, and to avoid com-
syndrome as a complication of septic arthritis.
are common. Erythematous macules and plications, such as rheumatic fever. Clin Exp Dermatol. 2007;32(6):754-755.
632 | www.PediatricSuperSite.com PEDIATRIC ANNALS 39:10 | OCTOBER 2010
3910Berk.indd 632 9/24/2010 4:21:54 PM
CM E
16. El Helali N, Carbonne A, Naas T, Kerneis S, view. Pediatr Dermatol. 1994;11(4):293-303. 1995;131(1):73-77.
Fresco O, Giovangrandi Y, Fortineau N, Nor- 24. Geria AN, Schwartz RA. Impetigo update: 33. Stevens DL. Streptococcal toxic shock syn-
dmann P, Astagneau P. Nosocomial outbreak new challenges in the era of methicillin resis- drome associated with necrotizing fasciitis.
of staphylococcal scalded skin syndrome in tance. Cutis. 2010;85(2):65-70. Annu Rev Med. 2000;51:271-288.
neonates: epidemiological investigation and 25. Shands KN, Schmid GP, Dan BB, et al. Toxic- 34. Wilson GJ, Talkington DF, Gruber W, Ed-
control. J Hosp Infect. 2005;61(2):130-138. shock syndrome in menstruating women: as- wards K, Dermody TS. Group A streptococ-
17. Yamasaki O, Yamaguchi T, Sugai M, Chapuis- sociation with tampon use and Staphylococ- cal necrotizing fasciitis following varicella in
Cellier C, Arnaud F, Vandenesch F, Etienne cus aureus and clinical features in 52 cases. N children: case reports and review. Clin Infect
J, Lina G. Clinical manifestations of staphy- Engl J Med. 1980;303(25):1436-1442. Dis. 1995;20(5):1333-1338.
lococcal scalded-skin syndrome depend on 26. Reingold AL, Hargrett NT, Dan BB, Shands 35. Lesko SM, O’Brien KL, Schwartz B, Vezina
serotypes of exfoliative toxins. J Clin Micro- KN, Strickland BY, Broome CV. Nonmenstru- R, Mitchell AA. Invasive group A streptococ-
biol. 2005;43(4):1890-183. al toxic shock syndrome: a review of 130 cases. cal infection and nonsteroidal antiinflamma-
18. Nishifuji K, Sugai M, Amagai M. Staphylo- Ann Intern Med. 1982;96(6 Pt 2):871-874. tory drug use among children with primary
coccal exfoliative toxins: “molecular scis- 27. McCormick JK, Yarwood JM, Schlievert PM. varicella. Pediatrics. 2001;107(5):1108-1115.
sors” of bacteria that attack the cutaneous Toxic shock syndrome and bacterial supe- 36. Cunningham MW. Pathogenesis of group A
defense barrier in mammals. J Dermatol Sci. rantigens: an update. Annu Rev Microbiol. streptococcal infections. Clin Microbiol Rev.
2008;49(1):21-31. 2001;55:77-104. 2000;13(3):470-511.
19. Gentilhomme E, Faure M, Piemont Y, Binder P, 28. Davis JP, Chesney PJ, Wand PJ, LaVenture M. 37. Yang SG, Dong HJ, Li FR, et al. Report and
Thivolet J. Action of staphylococcal exfoliative Toxic-shock syndrome: epidemiologic fea- analysis of a scarlet fever outbreak among
toxins on epidermal cell cultures and organo- tures, recurrence, risk factors, and prevention. adults through food-borne transmission in
typic skin. J Dermatol. 1990;17(9):526-532. N Engl J Med. 1980;303(25):1429-1435. China. J Infect. 2007;55(5):419-424.
20. Ladhani S, Joannou CL. Difficulties in diag- 29. Tofte RW, Williams DN. Toxic shock syn- 38. Manders SM. Toxin-mediated streptococcal
nosis and management of the staphylococcal drome. Evidence of a broad clinical spectrum. and staphylococcal disease. J Am Acad Der-
scalded skin syndrome. Pediatr Infect Dis J. JAMA. 1981;246(19):2163-2167. matol. 1998;39(3):383-398.
2000;19(9):819-821. 30. Chesney PJ, Davis JP, Purdy WK, Wand PJ, 39. Bialecki C, Feder HM Jr, Grant-Kels JM. The
21. Patel GK, Finlay AY. Staphylococcal scalded Chesney RW. Clinical manifestations of toxic six classic childhood exanthems: a review and
skin syndrome: diagnosis and management. shock syndrome. JAMA. 1981;246(7):741-748. update. J Am Acad Dermatol. 1989;21(5 Pt
Am J Clin Dermatol. 2003;4(3):165-175. 31. The Working Group on Severe Streptococcal 1):891-903.
22. Cribier B, Piemont Y, Grosshans E. Staphy- Infections.Defining the group A streptococcal 40. Quinn RW. Comprehensive review of morbid-
lococcal scalded skin syndrome in adults. A toxic shock syndrome. Rationale and consen- ity and mortality trends for rheumatic fever,
clinical review illustrated with a new case. J sus definition. JAMA. 1993;269(3):390-391. streptococcal disease, and scarlet fever: the
Am Acad Dermatol. 1994;30(2 Pt 2):319-324. 32. Wolf JE, Rabinowitz LG. Streptococcal decline of rheumatic fever. Rev Infect Dis.
23. Darmstadt GL, Lane AT. Impetigo: an over- toxic shock-like syndrome. Arch Dermatol. 1989;11(6):928-953.
PEDIATRIC ANNALS 39:10 | OCTOBER 2010 www.PediatricSuperSite.com | 633
3910Berk.indd 633 9/24/2010 4:21:54 PM
You might also like
- VanPutte Seeleys Essentials 11e Chap11 PPT AccessibleDocument49 pagesVanPutte Seeleys Essentials 11e Chap11 PPT AccessibleJoshua UyNo ratings yet
- How Bacterial Imbalances May Predispose To Seizure DisorderDocument5 pagesHow Bacterial Imbalances May Predispose To Seizure DisorderDr. Amy Yasko100% (1)
- Creatures & Constructs A Monster Manual Supplement For EberronDocument74 pagesCreatures & Constructs A Monster Manual Supplement For EberronJason BryantNo ratings yet
- ENT McqsDocument21 pagesENT McqsDr.G.Bhanu Prakash100% (8)
- Questionnaire Homeopathy English 2017 EditedDocument18 pagesQuestionnaire Homeopathy English 2017 EditedYo DraNo ratings yet
- Molluscum MedscapeDocument35 pagesMolluscum MedscapeAninditaNo ratings yet
- Presenation Fibrous Cavernous Tuberculois Teachers VersionDocument49 pagesPresenation Fibrous Cavernous Tuberculois Teachers VersionĆux 天主好 OkereNo ratings yet
- SIP 2018 FinalDocument32 pagesSIP 2018 Finaljohn clifordNo ratings yet
- And Other Cutaneous Bacterial Emergencies: MRSA, Staphylococcal Scalded Skin SyndromeDocument7 pagesAnd Other Cutaneous Bacterial Emergencies: MRSA, Staphylococcal Scalded Skin SyndromeMuhammad AriefNo ratings yet
- Bacterial Skin and Soft Tissue Infections: Clinical Review ArticleDocument9 pagesBacterial Skin and Soft Tissue Infections: Clinical Review ArticleRini MayaSariNo ratings yet
- NitradorDocument13 pagesNitradorcristian fodasticoNo ratings yet
- Dermatologia: Anais Brasileiros deDocument11 pagesDermatologia: Anais Brasileiros deAna Raniri UtariNo ratings yet
- Scabies Yeo LLDocument9 pagesScabies Yeo LLAriyanti RikaNo ratings yet
- Robinson HC CT105003132Document5 pagesRobinson HC CT105003132Francesca BizzocoNo ratings yet
- 2A - Sarigumba-Scenario For Think BreakDocument7 pages2A - Sarigumba-Scenario For Think BreakSean SarigumbaNo ratings yet
- Periodic Synopsis: Bacterial Infections of The SkinDocument7 pagesPeriodic Synopsis: Bacterial Infections of The SkinMDNo ratings yet
- Skin and Soft Tissue InfectionsDocument8 pagesSkin and Soft Tissue InfectionsciaranNo ratings yet
- Skin InfectionsDocument22 pagesSkin InfectionsoktafNo ratings yet
- In Brief: MastoiditisDocument4 pagesIn Brief: Mastoiditismuthiadewi31No ratings yet
- Mastoiditis in Children and Its Homoeopathic ApproachDocument7 pagesMastoiditis in Children and Its Homoeopathic Approachsayeedsaba950No ratings yet
- Stafilococo AureusDocument15 pagesStafilococo AureusJose MosqueraNo ratings yet
- Jurnal Reading KulitDocument26 pagesJurnal Reading KulitKeyko SeptiyantiNo ratings yet
- Pathophysiology ImpetigoDocument3 pagesPathophysiology ImpetigoAnne de VeraNo ratings yet
- Skin and Soft Tissue Infection InfoDocument4 pagesSkin and Soft Tissue Infection InfoPresura Andreea IulianaNo ratings yet
- Tom Son 2007Document7 pagesTom Son 2007riedha_chanzNo ratings yet
- Trop Med 140515Document10 pagesTrop Med 140515Arfa AlyaNo ratings yet
- Impetigo in Children: A Clinical Guide and Treatment OptionsDocument2 pagesImpetigo in Children: A Clinical Guide and Treatment OptionsBeuty SavitriNo ratings yet
- A Study of Skin Infection - How To Diagnosis and Its TherapyDocument7 pagesA Study of Skin Infection - How To Diagnosis and Its TherapyInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Streptococcal Skin InfectionsssDocument6 pagesStreptococcal Skin InfectionsssteenaNo ratings yet
- ImpetigoDocument3 pagesImpetigopcarty98No ratings yet
- GBR AbsesDocument10 pagesGBR AbsesrachmaferdianaNo ratings yet
- Reviews: Staphylococcal Manipulation of Host Immune ResponsesDocument15 pagesReviews: Staphylococcal Manipulation of Host Immune Responsesjacobo urbinaNo ratings yet
- Abd 91 02 0124Document11 pagesAbd 91 02 0124fannyNo ratings yet
- Staphylococcal Scalded Skin SyndromeDocument5 pagesStaphylococcal Scalded Skin SyndromeM Daffa Abhista ReviansyahNo ratings yet
- Infeksi StreptoDocument6 pagesInfeksi StreptoRiris SutrisnoNo ratings yet
- Bakteri S EpidermisDocument15 pagesBakteri S EpidermisSheillaizza FadhillaNo ratings yet
- Chromoblastomycosis of The Face in Solid Organ Transplant PatientDocument3 pagesChromoblastomycosis of The Face in Solid Organ Transplant PatientCarolina González RiveraNo ratings yet
- Deep Neck and Odontogenic Infections: Key PointsDocument12 pagesDeep Neck and Odontogenic Infections: Key Pointsnh2411No ratings yet
- (ANDREWS) Folliculitis, Furuncle, CarbuncleDocument8 pages(ANDREWS) Folliculitis, Furuncle, CarbunclempsoletaNo ratings yet
- Mastoiditis Case 1Document9 pagesMastoiditis Case 1fahrizan atjoNo ratings yet
- C R o W E, M A R K A - Moluscum Contagiosum. Diakses Dari: - Pada Tanggal 27 Desember 2016Document22 pagesC R o W E, M A R K A - Moluscum Contagiosum. Diakses Dari: - Pada Tanggal 27 Desember 201679lalalaNo ratings yet
- Molluscum Contagiosum - An Update: ReviewDocument3 pagesMolluscum Contagiosum - An Update: ReviewArdi WidiatmikaNo ratings yet
- Life 13 01126Document14 pagesLife 13 01126s4cdbv4xjrNo ratings yet
- A. Introduction of Skin and Soft Tissue InfectionsDocument10 pagesA. Introduction of Skin and Soft Tissue InfectionsChristin alexaNo ratings yet
- Impetigo, Erysipelas, and CeluulitisDocument19 pagesImpetigo, Erysipelas, and CeluulitisRizky Takdir RamadhanNo ratings yet
- Mullangi 2012Document10 pagesMullangi 2012Mariana AmbossNo ratings yet
- Diagnosa Dan Terapi SSSS PDFDocument6 pagesDiagnosa Dan Terapi SSSS PDFni putu.comsurya dianaNo ratings yet
- Moluskulum ContangiosumDocument9 pagesMoluskulum ContangiosumDennisSujayaNo ratings yet
- Staphylococcal Skin InfectionsDocument25 pagesStaphylococcal Skin InfectionsteenaNo ratings yet
- Bacterial Skin and Soft Tissue Infections Pathogenesis, EpidemiologyDocument11 pagesBacterial Skin and Soft Tissue Infections Pathogenesis, EpidemiologyTony Gomez Luna Leyva0% (1)
- CCJM Skin and Soft Tissue Infections Classifying and Treating A SpectrumDocument10 pagesCCJM Skin and Soft Tissue Infections Classifying and Treating A SpectrumBrian HarrisNo ratings yet
- Tubkut Srilanka JournalDocument7 pagesTubkut Srilanka JournalMusdalifah MimousNo ratings yet
- Staphylococcal-Scalded Skin Syndrome: Evaluation, Diagnosis, and ManagementDocument6 pagesStaphylococcal-Scalded Skin Syndrome: Evaluation, Diagnosis, and ManagementM Daffa Abhista ReviansyahNo ratings yet
- Acute Mastoiditis in Children: Pasquale Cassano, Giorgio Ciprandi, Desiderio PassaliDocument6 pagesAcute Mastoiditis in Children: Pasquale Cassano, Giorgio Ciprandi, Desiderio PassaliSyafira AlimNo ratings yet
- How To Manage ScabiesDocument13 pagesHow To Manage ScabiesDaniela SerbanNo ratings yet
- Celulitis 1Document8 pagesCelulitis 1Mili DiazNo ratings yet
- Celulitis PDFDocument9 pagesCelulitis PDFGazade GarciaNo ratings yet
- 610-Article Text-3639-1-10-20220823Document7 pages610-Article Text-3639-1-10-20220823Gaema MiripNo ratings yet
- Helmintos NematodosDocument12 pagesHelmintos NematodosHANNIANo ratings yet
- Ni Hms 401583Document22 pagesNi Hms 401583Zafira Ainillah RachmanNo ratings yet
- Gram-Positive Cocci Staphylococcus CLINICAL SIGNIFICANCEDocument8 pagesGram-Positive Cocci Staphylococcus CLINICAL SIGNIFICANCEsobia faryadaliNo ratings yet
- Basal Cell Carcinoma: Biology, Morphology and Clinical ImplicationsDocument21 pagesBasal Cell Carcinoma: Biology, Morphology and Clinical ImplicationsLalu Rizki Andri SaputraNo ratings yet
- Seminars in Diagnostic Pathology: Mark R. WickDocument11 pagesSeminars in Diagnostic Pathology: Mark R. WickAbdillah AkbarNo ratings yet
- Microbioma y OtorrinoDocument19 pagesMicrobioma y Otorrinodayenu barraNo ratings yet
- Molusco ContagiosoDocument12 pagesMolusco ContagiosoEduardo Medeiros Tabosa PinheiroNo ratings yet
- Endemic Mycoses: Blastomycosis, Histoplasmosis, and SporotrichosisDocument18 pagesEndemic Mycoses: Blastomycosis, Histoplasmosis, and SporotrichosisaugustosavioNo ratings yet
- BronchitisDocument13 pagesBronchitismuhammadsaliNo ratings yet
- KZN LFSC Grade 10 Step Ahead Learner Support Document 2023Document46 pagesKZN LFSC Grade 10 Step Ahead Learner Support Document 2023jurrymakgoba671No ratings yet
- Intraoperative Finding in Total Colonic AganglionosisDocument12 pagesIntraoperative Finding in Total Colonic AganglionosisAtrioventrikular MilanistiNo ratings yet
- Animal Biotechnology: An OverviewDocument37 pagesAnimal Biotechnology: An OverviewRaymond LimNo ratings yet
- Seminar On Cementum: Shreya Das Intern Department of PeriodontiaDocument57 pagesSeminar On Cementum: Shreya Das Intern Department of Periodontiashreya dasNo ratings yet
- Genbio ActsDocument14 pagesGenbio ActsnikxsxsxNo ratings yet
- Bleed From Anal Means - Google SearchDocument1 pageBleed From Anal Means - Google SearchKaran deep SinghNo ratings yet
- Medical Record Application Form Needed in Warsaw University of TechnologyDocument4 pagesMedical Record Application Form Needed in Warsaw University of Technologygmir777No ratings yet
- Basic Suturing Skills Booklet+Document34 pagesBasic Suturing Skills Booklet+Rohit Agrawal100% (3)
- Proliferative EndometriumDocument4 pagesProliferative EndometriumKristine Dela CruzNo ratings yet
- Active Management of The Third Stage of LabourDocument25 pagesActive Management of The Third Stage of LabourRedroses flowers0% (1)
- Histology - Week 2 - Epithelium TissueDocument8 pagesHistology - Week 2 - Epithelium TissueHIEL MAALIHANNo ratings yet
- Unlike False LaborDocument29 pagesUnlike False LaborMEi .. ÜNo ratings yet
- 2 - Brain Plasticity After Stroke FINAL PDFDocument32 pages2 - Brain Plasticity After Stroke FINAL PDFDwi AriyaniNo ratings yet
- Body Condition Score Cat Updated August 2020Document1 pageBody Condition Score Cat Updated August 2020Illias AmariciNo ratings yet
- Lab Manual BioDocument48 pagesLab Manual BioSanjay SinhaNo ratings yet
- 2020 Dental-CertificateDocument36 pages2020 Dental-Certificatebenz cadiongNo ratings yet
- Navamsha Lord in The Timing DeathDocument9 pagesNavamsha Lord in The Timing DeathGeorgegeorgebNo ratings yet
- I. Reading Text 1 Read The Following Text and Answer The Questions BelowDocument7 pagesI. Reading Text 1 Read The Following Text and Answer The Questions BelowSmile Al MosabyNo ratings yet
- UrinsryDocument10 pagesUrinsryAzizan HakimNo ratings yet
- CMC Veterinary Technology Program Handbook PDFDocument38 pagesCMC Veterinary Technology Program Handbook PDFSandri Alexandra NegreanuNo ratings yet
- The Devil in The Milk: A1 or A2? How Beta-Caseins Are Changing The Dairy IndustryDocument6 pagesThe Devil in The Milk: A1 or A2? How Beta-Caseins Are Changing The Dairy Industrynsk79inNo ratings yet
- 5.casts and MoldsDocument30 pages5.casts and MoldsKatrina PonceNo ratings yet