Professional Documents
Culture Documents
Atlas Kelainan Bawaan PDF
Atlas Kelainan Bawaan PDF
Uploaded by
bambang tokanCopyright:
Available Formats
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5822)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (852)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (898)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (349)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (823)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (403)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- Pediatric ATIDocument19 pagesPediatric ATIkelsey100% (4)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- CNS Congenital AnomaliesDocument74 pagesCNS Congenital AnomaliesMoh DrhusseinyNo ratings yet
- Spina Bifida Concept Map PDFDocument1 pageSpina Bifida Concept Map PDFnot realNo ratings yet
- Development of The Nervous SystemDocument5 pagesDevelopment of The Nervous SystemChaGonzalesNo ratings yet
- Spinalbifida 121213120324 Phpapp02Document28 pagesSpinalbifida 121213120324 Phpapp02Silvana María Espinoza CuadrosNo ratings yet
- ObsgynDocument105 pagesObsgynNugroho SigitNo ratings yet
- Spina BifidaDocument34 pagesSpina Bifidaapi-271779479No ratings yet
- Day 12 - Ncm-109 7b InfancyDocument59 pagesDay 12 - Ncm-109 7b InfancySheena Patricia ArasulaNo ratings yet
- Thesis Statement For Birth DefectsDocument6 pagesThesis Statement For Birth Defectsashleygomezalbuquerque100% (2)
- Understanding Learners With Difficulty in Mobility (LDM) : Department of EducationDocument60 pagesUnderstanding Learners With Difficulty in Mobility (LDM) : Department of EducationCherry Bobier100% (1)
- Arnold-Chiari Malformation Anatomical Variations and Latest Embryological Perspective Review of LiteratureDocument3 pagesArnold-Chiari Malformation Anatomical Variations and Latest Embryological Perspective Review of LiteraturedodyidaNo ratings yet
- Unit 4 Typological of Learners With DifficultiesDocument33 pagesUnit 4 Typological of Learners With DifficultiesMerry Carlien RudasNo ratings yet
- Management of Sacral Dimples Detected On Routine Newborn Examination: A Case Series and ReviewDocument3 pagesManagement of Sacral Dimples Detected On Routine Newborn Examination: A Case Series and ReviewDesta FransiscaNo ratings yet
- NCM 109 Lec Final Quiz 2 Quiz 3Document4 pagesNCM 109 Lec Final Quiz 2 Quiz 3Faye Trisha100% (2)
- MeningomyeloceleDocument42 pagesMeningomyeloceleSundaraBharathiNo ratings yet
- HESI Pediatric HESI ReviewDocument41 pagesHESI Pediatric HESI Reviewprogramgrabber96% (24)
- Spina Bifida Fact SheetDocument4 pagesSpina Bifida Fact SheetNational Dissemination Center for Children with DisabilitiesNo ratings yet
- Associations USMLEDocument99 pagesAssociations USMLEnu.bombinaNo ratings yet
- MedBack MyelomeningoceleDocument3 pagesMedBack MyelomeningoceleJulia Rei Eroles IlaganNo ratings yet
- Congenital Spinal Malformations: Volume 22 - Number 4 - July 1992Document31 pagesCongenital Spinal Malformations: Volume 22 - Number 4 - July 1992Joa FloresNo ratings yet
- School of Health and Allied Health Sciences Nursing Department Self-Directed Learning (Nur 146 - Clinical Area)Document6 pagesSchool of Health and Allied Health Sciences Nursing Department Self-Directed Learning (Nur 146 - Clinical Area)bekbekk cabahugNo ratings yet
- Fetal Imaging EditedDocument59 pagesFetal Imaging EditedMicah Lou CalambaNo ratings yet
- Common Fetal Anomalies: Anencephaly Spina Bifida Cleft Lip Gastroschisis/Omphalocele Trisomy 18 Conjoined TwinsDocument52 pagesCommon Fetal Anomalies: Anencephaly Spina Bifida Cleft Lip Gastroschisis/Omphalocele Trisomy 18 Conjoined TwinsStangPongritNo ratings yet
- Pediatric Nursing: A. Sigmund Freud: Psychosexual TheoryDocument12 pagesPediatric Nursing: A. Sigmund Freud: Psychosexual TheoryMicah MagallanoNo ratings yet
- Koren. Fetal Safety of DYD in 1st Trimester PregnancyDocument5 pagesKoren. Fetal Safety of DYD in 1st Trimester PregnancyRuth RachmawatyNo ratings yet
- 60 Pedia DisordersDocument6 pages60 Pedia DisordersEkoy TheRealNo ratings yet
- Hydrocephalus AND Spina Bifida: MR - Sachin T.Gadade M.SC (N) PediatricsDocument61 pagesHydrocephalus AND Spina Bifida: MR - Sachin T.Gadade M.SC (N) PediatricsAbdirahman Abdillahi FarahNo ratings yet
- Spina BifidaDocument2 pagesSpina BifidaTracy100% (2)
- Orthopedic ImpairmentsDocument40 pagesOrthopedic Impairmentsapi-281466418100% (1)
- The Compass 2015Document178 pagesThe Compass 2015Venture Publishing100% (1)
Atlas Kelainan Bawaan PDF
Atlas Kelainan Bawaan PDF
Uploaded by
bambang tokanOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Atlas Kelainan Bawaan PDF
Atlas Kelainan Bawaan PDF
Uploaded by
bambang tokanCopyright:
Available Formats
BIRTH DEFECTS
SURVEILLANCE
ATLAS OF
SELECTED
CONGENITAL
ANOMALIES
BIRTH DEFECTS SURVEILLANCE: ATLAS i WHO I CDC I ICBDSR
WHO I CDC I ICBDSR ii BIRTH DEFECTS SURVEILLANCE: ATLAS
BIRTH DEFECTS
SURVEILLANCE
ATLAS OF
SELECTED
CONGENITAL
ANOMALIES
BIRTH DEFECTS SURVEILLANCE: ATLAS i WHO I CDC I ICBDSR
WHO Library Cataloguing-in-Publication Data
Birth defects surveillance: atlas of selected congenital anomalies
1.Congenital Abnormalities. 2.Neural Tube Defects. 3.Public Health Surveillance. 4.Atlases.
I.World Health Organization. II.Centers for Disease Control and Prevention (U.S.). III.Interna-
tional Clearinghouse for Birth Defects Monitoring Systems.
ISBN 978 92 4 156476 2 NLM classification: QS 675
© World Health Organization 2014
All rights reserved. Publications of the World Health Organization are available on the WHO
web site (www.who.int) or can be purchased from WHO Press, World Health Organization,
20 Avenue Appia, 1211 Geneva 27, Switzerland (tel.: +41 22 791 3264; fax: +41 22 791 4857;
e-mail: bookorders@who.int).
Requests for permission to reproduce or translate WHO publications –whether for sale or for non-
commercial distribution– should be addressed to WHO Press through the WHO web site
(www.who.int/about/licensing/copyright_form/en/index.html).
The designations employed and the presentation of the material in this publication do not
imply the expression of any opinion whatsoever on the part of the World Health Organization
concerning the legal status of any country, territory, city or area or of its authorities, or concerning
the delimitation of its frontiers or boundaries. Dotted lines on maps represent approximate
border lines for which there may not yet be full agreement.
The mention of specific companies or of certain manufacturers’ products does not imply that
they are endorsed or recommended by the World Health Organization in preference to others of
a similar nature that are not mentioned. Errors and omissions excepted, the names of proprietary
products are distinguished by initial capital letters.
All reasonable precautions have been taken by the World Health Organization to verify the
information contained in this publication. However, the published material is being distributed
without warranty of any kind, either expressed or implied. The responsibility for the interpretation
and use of the material lies with the reader. In no event shall the World Health Organization be
liable for damages arising from its use.
The named authors alone are responsible for the views expressed in this publication.
Design and layout: Alberto March
Suggested citation
WHO/CDC/ICBDSR. Birth defects surveillance: atlas of selected congenital anomalies.
Geneva: World Health Organization; 2014.
WHO I CDC I ICBDSR ii BIRTH DEFECTS SURVEILLANCE: ATLAS
Acknowledgements
This atlas is a collaborative effort between the World Health Organization (WHO), the
National Center on Birth Defects and Developmental Disabilities (NCBDDD) from the US
Centers for Disease Control and Prevention (CDC), and the International Clearinghouse
for Birth Defects Surveillance and Research (ICBDSR).
We would like to acknowledge the technical input in the preparation of this atlas
of staff from NCBDDD, ICBDSR and WHO, particularly, from the following individuals
(in alphabetical order): Mr James K Archer, Dr Jose F Arenas, Dr Alejandro Azofeifa,
Dr Robert J Berry, Dr Lorenzo Botto, Dr Marie Noel Brune Drisse, Dr Luz Maria De-
Regil, Ms Alissa Eckert, Ms Alina Flores, Dr Jaime Frías, Mr Dan J Higgins, Dr Margaret
Honein, Ms Jennifer Hulsey, Ms Christina Kilgo, Dr Pierpaolo Mastroiacovo, Dr Cynthia
Moore, Dr Joseph Mulinare, Dr Teresa Murguia de Sierra, Dr Maria Neira, Dr Richard
Olney, Dr Juan Pablo Peña-Rosas, Dr. Hilda Razzaghi, Dr Lisa Rogers, Dr Jorge
Rosenthal, Dr Csaba Siffel, Dr Joseph Sniezek, Ms Diana Valencia, Dr Claudia Vellozzi
and Ms Jennifer Williams. We would also like to thank all collaborators and partners
for helping us develop illustrations and obtain photographs for this birth defects
surveillance atlas.
The drawings were all supplied by CDC/NCBDDD.
We would also like to thank Dr Rajesh Mehta and Dr Neena Raina from the
WHO Regional Office for South-East Asia, for providing valuable feedback during the
development process.
WHO, CDC and ICBDSR gratefully acknowledge the technical input of the meeting
participants for the regional training on surveillance of birth defects.
Financial support
WHO thanks the US CDC, especially the National Center on Birth Defects and
Developmental Disabilities, for providing financial support for the publication of this
atlas as part of the cooperative agreement 5 E11 DP002196, Global prevention of non-
communicable diseases and promotion of health.
BIRTH DEFECTS SURVEILLANCE: ATLAS iii WHO I CDC I ICBDSR
Contents
Abreviations vi
Objectives of the atlas 1
Congenital malformations of the nervous system: neural tube defects 2
Anencephaly (Q00.0) 4
Craniorachischisis (Q00.1) 4
Iniencephaly (Q00.2) 5
Frontal encephalocele (Q01.0) 6
Nasofrontal encephalocele (Q01.1) 6
Occipital encephalocele (Q01.2) 6
Parietal encephalocele (Q01.80) 7
Orbital encephalocele (Q01.81) 7
Nasal encephalocele (Q01.82) 7
Cervical spina bifida 8
Cervical spina bifida with hydrocephalus (Q05.0) 9
Cervical spina bifida without hydrocephalus (Q05.5) 9
Thoracic spina bifida 10
Thoracic spina bifida with hydrocephalus ((Q05.1) 11
Thoracic spina bifida without hydrocephalus (Q05.6) 11
Lumbar spina bifida 12
Lumbar spina bifida with hypdrocephalus (Q05.2) 13
Lumbar spina bifida without hydrocephalus (Q05.7) 13
Sacral spina bifida 14
Sacral spina bifida with hydrocephalus (Q05.3) 15
Sacral spina bifida without hydrocephalus (Q05.8) 15
Cleft palate and cleft lip 16
Cleft palate (Q35.5) 16
Cleft lip, bilateral (Q36.0) 16
Cleft lip, specified as unilateral (Q36.9, Q36.90) 16
Cleft hard palate with bilateral cleft lip (Q37.0) 17
Cleft hard palate with cleft lip, specified as unilateral (Q37.10) 17
Congenital malformations of genital organs 18
Hypospadias (Q54, Q54.0, Q54.1, Q54.2, Q54.3, Q54.8, Q54.9) 18
WHO I CDC I ICBDSR iv BIRTH DEFECTS SURVEILLANCE: ATLAS
Congenital malformations and deformations of the musculoskeletal system 19
Talipes equinovarus (Q66.0) 19
Reduction defects of upper and lower limbs 19
Congenital complete absence of upper limb(s); amelia of upper
limb (Q71.0) 19
Congenital absence of upper arm and forearm with hand
present; phocomelia of upper limb (Q71.1) 20
Congenital absence of both forearm and hand (Q71.2) 20
Congenital absence of hand and finger(s) (Q71.3) 20
Congenital absence of finger(s) (remainder of hand intact) (Q71.30) 21
Absence or hypoplasia of thumb (other digits intact) (Q71.31) 21
Longitudinal reduction defect of radius: clubhand (congenital),
radial clubhand, absence of radius (Q71.4) 22
Longitudinal reduction defect of ulna (Q71.5) 22
Split hand (congenital cleft hand) (Q71.6) 23
Congenital complete absence of lower limb(s); amelia of
lower limb (Q72.0) 23
Congenital absence of thigh and lower leg with foot present;
phocomelia of lower limb (Q72.1) 23
Congenital absence of both lower leg and foot (Q72.2) 24
Congenital absence of foot and toe(s) (Q72.3) 24
Congenital absence or hypoplasia of toe(s) with remainder
of foot intact (Q72.30) 24
Absence or hypoplasia of first toe with other digits present (Q72.31) 25
Longitudinal reduction defect of femur (Q72.4) 25
Longitudinal reduction defect of tibia (Q72.5) 25
Longitudinal reduction defect of fibula; fibular
aplasia/hypoplasia (Q72.6) 26
Split foot (congenital cleft foot) (Q72.7) 26
Exomphalos/omphalocele (Q79.2) 27
Gastroschisis (Q79.3) 28
BIRTH DEFECTS SURVEILLANCE: ATLAS v WHO I CDC I ICBDSR
Abbreviations
CDC United States Centers for Disease Control and Prevention
ICBDSR International Clearinghouse for Birth Defects Surveillance and
Research
ICD-10 International statistical classification of diseases and related health
problems, 10th revision
NCBDDD National Center on Birth Defects and Developmental Disabilities
RCPCH Royal College of Paediatrics and Child Health
USA United States of America
WHO World Health Organization
WHO I CDC I ICBDSR vi BIRTH DEFECTS SURVEILLANCE: ATLAS
Objectives of the atlas
Congenital anomalies, also known as birth defects, are structural or functional
abnormalities, including metabolic disorders, that are present from birth. Congenital
anomalies are a diverse group of disorders of prenatal origin that can be caused by
single gene defects, chromosomal disorders, multifactorial inheritance, environmental
teratogens or micronutrient malnutrition.
This Atlas of selected congenital anomalies is a companion tool to Birth defects
surveillance: a manual for programme managers, and is intended to help in the
development, implementation and ongoing improvement of a surveillance programme
for congenital anomalies, particularly in countries with limited human and financial
resources.
This atlas uses the International statistical classification of diseases and related health
problems, 10th revision (ICD-10) and the Royal College of Paediatrics and Child Health
(RCPCH) extension for coding of congenital anomalies.
It provides selected illustrations and photographs of congenital anomalies that
are severe enough to have a high probability of being captured during the first few
days following birth. Also, because of their severity and frequency, these depicted
conditions have significant public health impact, and for some there is a potential for
primary prevention. When used in conjunction with the manual, the illustrations and
photographs will help the reader to:
● identify an initial list of congenital anomalies to consider for monitoring;
● describe the tools needed to define and code identified cases;
● define specific congenital anomalies under surveillance.
BIRTH DEFECTS SURVEILLANCE: ATLAS 1 WHO I CDC I ICBDSR
Congenital malformations of the nervous system: neural tube defects
Neural tube defects affect the brain and spinal cord, and are among the most common of
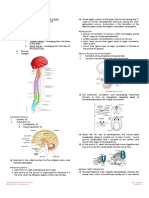
the congenital anomalies (see Fig. 4.1). Panel A shows a cross section of the rostral end of
the embryo at approximately three weeks after conception, showing the neural groove in
the process of closing, overlying the notochord. The neural folds are the rising margins of the
neural tube, topped by the neural crest, and demarcate the neural groove centrally. Panel B
shows a cross section of the middle portion of the embryo after the neural tube has closed.
The neural tube, which will ultimately develop into the spinal cord, is now covered by surface
ectoderm (later, the skin). The intervening mesoderm will form the bony spine. The notochord
is regressing. Panel C shows the developmental and clinical features of the main types of neural
tube defects. The diagram in the centre is a dorsal view of a developing embryo, showing a
neural tube that is closed in the centre but still open at the cranial and caudal ends. The dotted
lines marked A and B refer to the cross sections shown in Panels A and B. Shaded bars point to
the region of the neural tube relevant to each defect.
In anencephaly, the absence of the brain and calvaria can be total or partial.
Craniorachischisis is characterized by anencephaly accompanied by a contiguous bony defect
of the spine and exposure of neural tissue. In open spina bifida, a bony defect of the posterior
vertebral arches (in this case, the lower thoracic vertebrae) is accompanied by herniation
of neural tissue and meninges and is not covered by skin. In iniencephaly, dysraphia in the
occipital region is accompanied by severe retroflexion of the neck and trunk. In encephalocele,
the brain and meninges herniate through a defect in the calvaria. In closed spina bifida, unlike
open spina bifida, the bony defect of the posterior vertebral arches (in this case, the lumbar
vertebrae), the herniated meninges, and neural tissue are covered by skin.
The most prevalent types of neural tube defects are anencephaly, encephalocele and
spina bifida.
Fig. 4.1. Neural tube defects
Surface ectoderm
Neural fold Neural groove Neural crest Neural crest Mesoderm
Neural tube
Notochord Somite Yolk sac
A B
Source: adapted, with permsiion from the publisher, from Botto et al. N. Engl. J. Med. 1999;341:1509–19.
WHO I CDC I ICBDSR 2 BIRTH DEFECTS SURVEILLANCE: ATLAS
Anencephaly Craniorachischisis Open spina bifida
Cranial neuropore
A B Caudal neuropore
Neural fold
C
Somite
Neural groove
Iniencephaly Encephalocele Closed spina bifida
BIRTH DEFECTS SURVEILLANCE: ATLAS 3 WHO I CDC I ICBDSR
Anencephaly (Q00.0)
A total or partial absence of the brain, together with total or partial absence of the cranial
vault and the covering skin.
Photograph
source: courtesy
of CDC-Beijing
Medical University
collaborative
project.
Craniorachischisis (Q00.1)
The presence of anencephaly with a contiguous spine defect without meninges covering
the neural tissue (rachischisis).
Photograph
source: courtesy
of CDC-Beijing
Medical University
collaborative
project.
WHO I CDC I ICBDSR 4 BIRTH DEFECTS SURVEILLANCE: ATLAS
Photographs
source: courtesy
of CDC-Beijing
Medical University
collaborative project.
Iniencephaly (Q00.2)
A rare and complex neural tube defect characterized by extreme retroflexion of the
head, variably combined with rachischisis of the cervical and thoracic spine and, more
rarely, with occipital encephalocele. In iniencephaly, the cranium is always closed.
Photograph
source: courtesy
of CDC-Beijing
Medical University
collaborative project.
BIRTH DEFECTS SURVEILLANCE: ATLAS 5 WHO I CDC I ICBDSR
Frontal encephalocele (Q01.0)
Herniation of brain tissue, usually covered by meninges, through a defect in the frontal
bone.
Photographs
source: courtesy
of CDC-Beijing
Medical University
collaborative
project.
Nasofrontal encephalocele (Q01.1)
Herniation of brain tissue, usually covered by meninges, through an opening between
the frontal bone and the nasal and ethmoid bones.
Photograph source:
courtesy of Jaime
Frías, MD, USA.
Occipital encephalocele (Q01.2)
Herniation of brain tissue, usually covered by meninges, through an opening in the
occipital bone.
Photograph
source: courtesy
of CDC-Beijing
Medical University
collaborative
project.
WHO I CDC I ICBDSR 6 BIRTH DEFECTS SURVEILLANCE: ATLAS
Parietal encephalocele (Q01.80)
Herniation of brain tissue, usually covered by meninges, through an opening in one of
the parietal bones.
Photograph
source: courtesy of
Registro Nacional
de Anomalías
Congénitas
Argentina (RENAC),
Centro Nacional de
Genética Médica,
ANLIS, Ministerio de
Salud de la Nación.
Orbital encephalocele (Q01.81)
Herniation of brain tissue, usually covered by meninges, through one of the orbits.
Photograph source:
courtesy of Jaime
Frías, MD, USA.
Nasal encephalocele (Q01.82)
Herniation of brain tissue, usually covered by meninges, through an opening in the
nasal region.
Photograph source:
courtesy of Estudio
Colaborativo Latino
Americano de
Malformaciones
Congénitas
(ECLAMC).
BIRTH DEFECTS SURVEILLANCE: ATLAS 7 WHO I CDC I ICBDSR
Cervical spina bifida
Most cases of cervical spina bifida will eventually develop hydrocephalus, although this
may not be immediately obvious at birth; therefore, coding for cervical spina bifida with
or without hydrocephalus could be difficult at birth. Close follow-up of these neonates
is important for consideration of shunt surgery.
Photographs
source: courtesy
of CDC-Beijing
Medical University
collaborative project.
WHO I CDC I ICBDSR 8 BIRTH DEFECTS SURVEILLANCE: ATLAS
Cervical spina bifida with hydrocephalus
(Q05.0)
Protrusion of meninges and/or spinal cord
through an opening in the cervical region
of the spine, associated with hydrocephalus.
It may be open, with or without membrane
covering; or closed, covered by normal-
appearing skin. Hydrocephalus is present
as a result of obstruction to the flow of
cerebrospinal fluid, secondary to the
hindbrain herniation associated with Chiari II
malformation.
Cervical spina bifida without
hydrocephalus (Q05.5)
Protrusion of meninges and/or spinal cord
through an opening in the cervical region
of the vertebral column. It may be open,
with or without membrane covering; or
closed, covered by normal-appearing skin.
BIRTH DEFECTS SURVEILLANCE: ATLAS 9 WHO I CDC I ICBDSR
Thoracic spina bifida
Most cases of thoracic spina bifida will eventually develop hydrocephalus, although this
may not be immediately obvious at birth; therefore, coding for thoracic spina bifida with
or without hydrocephalus could be difficult at birth. Close follow-up of these neonates
is important for consideration of shunt surgery.
Photographs
source: courtesy
of CDC-Beijing
Medical University
collaborative
project.
WHO I CDC I ICBDSR 10 BIRTH DEFECTS SURVEILLANCE: ATLAS
Thoracic spina bifida with hydrocephalus
(Q05.1)
Protrusion of meninges and/or spinal
cord through an opening in the thoracic
region of the vertebral column, associated
with hydrocephalus. It may be open,
with or without membrane covering; or
closed, covered by normal-appearing skin.
Hydrocephalus is present as a result of
obstruction to the flow of cerebrospinal
fluid, secondary to the hindbrain herniation
associated with Chiari II malformation.
Thoracic spina bifida without
hydrocephalus (Q05.6)
Protrusion of meninges and/or spinal cord
through an opening in the thoracic region
of the vertebral column. It may be open,
with or without membrane covering; or
closed, covered by normal-appearing skin.
BIRTH DEFECTS SURVEILLANCE: ATLAS 11 WHO I CDC I ICBDSR
Lumbar spina bífida
Some cases of lumbar spina bifida will eventually develop hydrocephalus, and this may
not be immediately obvious at birth; therefore, coding for lumbar spina bifida with or
without hydrocephalus could be difficult at birth. Close follow-up of these neonates is
important for consideration of shunt surgery.
Photographs
source: courtesy
of CDC-Beijing
Medical University
collaborative
project.
Photograph source:
courtesy of Idalina
Montes, MD and
Rafael Longo, MD,
FACS, Puerto Rico.
WHO I CDC I ICBDSR 12 BIRTH DEFECTS SURVEILLANCE: ATLAS
Lumbar spina bifida with
hydrocephalus (Q05.2)
Protrusion of meninges and/or spinal
cord through an opening in the
lumbar region of the vertebral column,
associated with hydrocephalus. It may
be open, with or without membrane
covering; or closed, covered by normal-
appearing skin. Hydrocephalus is present
as a result of obstruction to the flow of
cerebrospinal fluid, secondary to the
hindbrain herniation associated with
Chiari II malformation.
Lumbar spina bifida without
hydrocephalus (Q05.7)
Protrusion of meninges and/or spinal
cord through an opening in the lumbar
region of the vertebral column. It may
be open, with or without membrane
covering; or closed, covered by normal-
appearing skin.
BIRTH DEFECTS SURVEILLANCE: ATLAS 13 WHO I CDC I ICBDSR
Sacral spina bifida
Few cases of sacral spina bifida will develop hydrocephalus, compared with the other
types of spina bifida. The presence of hydrocephalus in infants with sacral spina bifida
may not be immediately obvious at birth; therefore, coding for sacral spina bifida with
or without hydrocephalus could be difficult at birth. Close follow-up of these neonates
is important for consideration of shunt surgery.
Photographs
source: courtesy
of CDC-Beijing
Medical University
collaborative
project.
WHO I CDC I ICBDSR 14 BIRTH DEFECTS SURVEILLANCE: ATLAS
Sacral spina bifida with hydrocephalus
(Q05.3)
Protrusion of meninges and/or spinal
cord through an opening in the
sacral region of the vertebral column,
associated with hydrocephalus. It may
be open, with or without membrane
covering; or closed, covered by normal-
appearing skin. Hydrocephalus is present
as a result of obstruction to the flow of
cerebrospinal fluid, secondary to the
hindbrain herniation associated with
Chiari II malformation.
Sacral spina bifida without
hydrocephalus (Q05.8)
Protrusion of meninges and/or spinal cord
through an opening in the sacral region of
the vertebral column. It may be open, with
or without membrane covering; or closed,
covered by normal-appearing skin.
BIRTH DEFECTS SURVEILLANCE: ATLAS 15 WHO I CDC I ICBDSR
Cleft palate and cleft lip
Cleft palate (Q35.5)
Fissure of the palate, which can affect the soft and hard palate, or only the soft palate.
Photograph
source: courtesy
of CDC-Beijing
Medical University
collaborative project.
Cleft lip, bilateral (Q36.0)
Partial or complete bilateral fissure of the upper lip that may be associated with a cleft
of the gum.
Photograph source:
courtesy of Pedro
Santiago, DMD and
Miguel Yáñez, MD,
FACS, USA.
Cleft lip, specified as unilateral (Q36.9, Q36.90)
Partial or complete unilateral fissure of the upper lip that may be associated with a cleft
of the gum.
Photographs sources:
courtesy of
Jaime Frías, MD, USA
(middle); CDC-Beijing
Medical University
collaborative project
(right).
WHO I CDC I ICBDSR 16 BIRTH DEFECTS SURVEILLANCE: ATLAS
Cleft hard palate with bilateral cleft lip (Q37.0)
Partial or complete bilateral fissure of the upper lip, associated with a fissure of the
palate.
Photograph source:
courtesy of
Estudio Colaborativo
Latino Americano
de Malformaciones
Congénitas
(ECLAMC).
Cleft hard palate with cleft lip, specified as unilateral (Q37.10)
Partial or complete unilateral fissure of the upper lip, associated with a fissure of the
palate.
Photograph source:
courtesy of
Pedro Santiago, DMD
and Miguel Yáñez,
MD, FACS, USA.
BIRTH DEFECTS SURVEILLANCE: ATLAS 17 WHO I CDC I ICBDSR
Congenital malformations of genital organs
Hypospadias (Q54, Q54.0, Q54.1, Q54.2, Q54.3, Q54.8, Q54.9)
Displacement of the urethral meatus ventrally and proximally from the tip of the penis.
It is classified according to the position of the meatus on the penis:
• First degree (Q54.0): the urethral meatus is located on either the glans (glanular
hypospadias) or the corona (coronal hypospadias).
• Second degree (Q54.1): the urethral meatus is located in the balanopenile
furrow or coronal sulcus (subcoronal hypospadias) or in the shaft of the penis
(distal penile, midshaft, and proximal penile hypospadias).
• Third degree (Q54.2, Q54.3): the urethral meatus is located in the junction of
the penis and the scrotum (penoscrotal or scrotal hypospadias) or the perineum
(perineoscrotal, perineal, or pseudovaginal hypospadias).
The shortening of the ventral side of the penis found in hypospadias can result in a
penile curvature, known as chordee. This is present more commonly in severe cases, but
also can occur independently of hypospadias.
First degree Glanular Subtypes:
Coronal
Q54 Hypospadias (avoid using
Subcoronal this general code if more specific
Distal penille information is available)
Second degree
Midshaft Q54.0 Hypospadias, balanic coronal
glanular
Proximal penile Q54.1 Hypospadias, penile
(subcoronal hypospadias)
Penoscrotal Q54.2 Hypospadias, penoscrotal
Q54.3 Hypospadias, perineal
Third degree
Scrotal
Q54.8 Other hypospadias, excludes:
female hypospadias (Q52.81)
Perineal Q54.9 Hypospadias, unspecified
Note: illustration indicates all possible locations for the malformation, but one case will not have all.
WHO I CDC I ICBDSR 18 BIRTH DEFECTS SURVEILLANCE: ATLAS
Congenital malformations and deformations of the musculoskeletal system
Talipes equinovarus (Q66.0)
Combination of forefoot and hindfoot in equinus (plantar flexed) and in varus (rotated
toward the midline). In other words, the foot points downward and inward and is rotated
outward axially. Other anomalies of the foot and ankle include talipes calcaneovalgus
(in which the ankle joint is dorsiflexed and the forefoot deviated outwards) and talipes
calcaneovarus (in which the ankle joint is dorsiflexed and the forefoot deviated inwards).
Photograph and X-ray
source: courtesy of
Idalina Montes, MD
and Rafael Longo, MD,
FACS, Puerto Rico.
Reduction defects of upper and lower limbs
Congenital complete absence of upper limb(s); amelia of upper limb (Q71.0)
Complete absence of one or both upper limbs.
Photographs
source: courtesy
of CDC-Beijing
Medical University
collaborative project.
BIRTH DEFECTS SURVEILLANCE: ATLAS 19 WHO I CDC I ICBDSR
Congenital absence of upper arm and forearm with hand present; phocomelia of
upper limb (Q71.1)
Complete or partial absence of the upper arm and forearm but with the hand present.
Photograph source:
courtesy of Jaime
Frías, MD, USA.
Congenital absence of both forearm and hand (Q71.2)
Complete or partial absence of both the forearm and hand.
Photographs
source: CDC-Beijing
Medical University
collaborative project.
Congenital absence of hand and finger(s) (Q71.3)
Complete or partial absence of the hand and finger(s).
Photograph source:
courtesy of Estudio
Colaborativo Latino
Americano de
Malformaciones
Congénitas (ECLAMC).
WHO I CDC I ICBDSR 20 BIRTH DEFECTS SURVEILLANCE: ATLAS
Congenital absence of finger(s) (remainder of hand intact) (Q71.30)
Complete or partial absence of fingers, with the remainder of the hand intact.
Photograph source:
courtesy of John
Wiley and Sons
©2009. Biesecker
LG et al. Am. J.
Med. Genet. A.
2009;149A:93–127.
Photographs and X-ray
source: courtesy of Dr
E Gene Deune, MD;
Associate Professor,
Johns Hopkins
Department of
Orthopedic Surgery,
Division of Hand
Surgery, Baltimore,
MD, USA.
Absence or hypoplasia of thumb (other digits intact) (Q71.31)
Complete or partial absence or hypoplasia of the thumb.
Photograph source:
CDC-Beijing
Medical University
collaborative project.
BIRTH DEFECTS SURVEILLANCE: ATLAS 21 WHO I CDC I ICBDSR
Longitudinal reduction defect of radius: clubhand (congenital), radial clubhand,
absence of radius (Q71.4)
Complete or partial radial aplasia/hypoplasia. Usually accompanied by complete or
partial absence or hypoplasia of the thumb.
Photographs
source: courtesy
of CDC-Beijing
Medical University
collaborative project.
X-ray source: courtesy
of John Wiley and Sons
©2011. Umaña LA et al.
Am. J. Med. Genet. A.
2011;155A:3071–4.
Longitudinal reduction defect of ulna (Q71.5)
Complete or partial absence of the ulna.
X-ray source: courtesy
of John Wiley and Sons
©1997. Kumar D et al.
Am. J. Med. Genet. A.
1997;70A:107–13.
WHO I CDC I ICBDSR 22 BIRTH DEFECTS SURVEILLANCE: ATLAS
Split hand (congenital cleft hand) (Q71.6)
Complete or partial absence of central fingers and metacarpals. The terms lobster claw
and ectrodactyly, used by some, should be discouraged.
Photographs
source: CDC-Beijing
Medical University
collaborative project.
Congenital complete absence of lower limb(s); amelia of lower limb (Q72.0)
Complete absence of one or both lower limb(s).
Photograph source:
CDC-Beijing
Medical University
collaborative project.
Congenital absence of thigh and lower leg with foot present; phocomelia of lower
limb (Q72.1)
Complete or partial absence of the thigh and lower leg but with the foot present.
Photograph source:
courtesy of Estudio
Colaborativo Latino
Americano de
Malformaciones
Congénitas (ECLAMC).
BIRTH DEFECTS SURVEILLANCE: ATLAS 23 WHO I CDC I ICBDSR
Congenital absence of both lower leg and foot (Q72.2)
Complete or partial absence of both the lower leg and foot.
Photograph source:
CDC-Beijing Medical
University collaborative
project.
Congenital absence of foot and toe(s) (Q72.3)
Complete or partial absence of the foot and toe(s).
Photograph source:
courtesy of Estudio
Colaborativo Latino
Americano de
Malformaciones
Congénitas (ECLAMC).
Congenital absence or hypoplasia of toe(s) with remainder of foot intact (Q72.30)
Complete absence or hypoplasia of toe(s) with the remainder of the foot intact.
Photographs source:
courtesy of John
Wiley and Sons
©2009. Biesecker
LG et al. Am. J.
Med. Genet. A.
2009;149A:93–127.
WHO I CDC I ICBDSR 24 BIRTH DEFECTS SURVEILLANCE: ATLAS
Absence or hypoplasia of first toe with other digits present (Q72.31)
Complete absence or hypoplasia of the first (great) toe with other digits present.
Photograph source:
courtesy of John Wiley
and Sons ©2009.
Biesecker LG et al.
Am. J. Med. Genet. A.
2009;149A:93–127.
Longitudinal reduction defect of femur (Q72.4)
Complete or partial absence of the femur.
X-ray source: courtesy
of Jaime Frías, MD,
USA.
Longitudinal reduction defect of tibia (Q72.5)
Complete or partial absence of the tibia. Usually accompanied by complete or partial
absence or hypoplasia of the first (great) toe.
Photograph source:
CDC-Beijing
Medical University
collaborative project.
BIRTH DEFECTS SURVEILLANCE: ATLAS 25 WHO I CDC I ICBDSR
Longitudinal reduction defect of fibula; fibular aplasia/hypoplasia (Q72.6)
Complete or partial absence of the fibula.
X-ray source: image
reprinted with
permission from
Holmstrom MC et al.
Medscape 2013 (http://
emedicine.medscape.
com/article/1251558-
overview).
Split foot (congenital cleft foot) (Q72.7)
Complete or partial absence of central toes and metatarsals. The term ectrodactyly,
used by some, should be discouraged.
Photographs
source: CDC-Beijing
Medical University
collaborative project.
WHO I CDC I ICBDSR 26 BIRTH DEFECTS SURVEILLANCE: ATLAS
Exomphalos/omphalocele (Q79.2)
Congenital anomaly of the anterior abdominal wall, in which the abdominal contents
(gut, but at times also other abdominal organs) are herniated in the midline through an
enlarged umbilical ring. The umbilical cord is inserted in the distal part of the membrane
covering the anomaly. The herniated organs are covered by a membrane consisting of
the peritoneum and amnion (but this membrane can be ruptured).
Photograph source:
courtesy of Estudio
Colaborativo Latino
Americano de
Malformaciones
Congénitas (ECLAMC).
Photographs
source: CDC-Beijing
Medical University
collaborative project.
Gastroschisis and omphalocele can be confused with one another when the membrane covering the omphalocele
has ruptured. In that case, the location of the abdominal opening is decisive: it is midline in omphalocele, and
lateral to the umbilicus in gastroschisis.
BIRTH DEFECTS SURVEILLANCE: ATLAS 27 WHO I CDC I ICBDSR
Gastroschisis (Q79.3)
Gastroschisis is a congenital anomaly of the anterior abdominal wall, accompanied by
herniation of the gut and occasionally other abdominal organs. The opening in the
abdominal wall is lateral to the umbilicus, and the herniated organs lack a protective
membrane. Note that the extruded abdominal contents can be matted and covered by
a thick fibrous material, but this membrane does not resemble skin.
Photograph source:
CDC-Beijing
Medical University
collaborative project.
Gastroschisis and omphalocele can be confused with one another when the membrane covering the omphalocele
has ruptured. In that case, the location of the abdominal opening is decisive: it is midline in omphalocele, and
lateral to the umbilicus in gastroschisis.
WHO I CDC I ICBDSR 28 BIRTH DEFECTS SURVEILLANCE: ATLAS
BIRTH DEFECTS SURVEILLANCE: ATLAS 29 WHO I CDC I ICBDSR
For more information, please contact:
National Center on Birth Defects and Developmental Disabilities
Centers for Disease Control and Prevention
1600 Clifton Rd, MS-E86, Atlanta, GA 30333, United States of America
Fax: +1 404 498 3550
http://www.cdc.gov/ncbddd/birthdefects
International Clearinghouse for Birth Defects Surveillance and Research
Via Carlo Mirabello 14, 00192 Roma, Italy
Fax +39 06 270 1904
Email: icbd@icbd.org
www.icbdsr.org
ISBN 978 92 4 156476 2
Department of Nutrition for Health and Development
World Health Organization
Avenue Appia 20, CH-1211 Geneva 27, Switzerland
Fax: +41 22 791 4156
Email: nutrition@who.int
www.who.int/nutrition
WHO I CDC I ICBDSR 30 BIRTH DEFECTS SURVEILLANCE: ATLAS
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5822)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (852)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (898)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (349)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (823)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (403)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- Pediatric ATIDocument19 pagesPediatric ATIkelsey100% (4)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- CNS Congenital AnomaliesDocument74 pagesCNS Congenital AnomaliesMoh DrhusseinyNo ratings yet
- Spina Bifida Concept Map PDFDocument1 pageSpina Bifida Concept Map PDFnot realNo ratings yet
- Development of The Nervous SystemDocument5 pagesDevelopment of The Nervous SystemChaGonzalesNo ratings yet
- Spinalbifida 121213120324 Phpapp02Document28 pagesSpinalbifida 121213120324 Phpapp02Silvana María Espinoza CuadrosNo ratings yet
- ObsgynDocument105 pagesObsgynNugroho SigitNo ratings yet
- Spina BifidaDocument34 pagesSpina Bifidaapi-271779479No ratings yet
- Day 12 - Ncm-109 7b InfancyDocument59 pagesDay 12 - Ncm-109 7b InfancySheena Patricia ArasulaNo ratings yet
- Thesis Statement For Birth DefectsDocument6 pagesThesis Statement For Birth Defectsashleygomezalbuquerque100% (2)
- Understanding Learners With Difficulty in Mobility (LDM) : Department of EducationDocument60 pagesUnderstanding Learners With Difficulty in Mobility (LDM) : Department of EducationCherry Bobier100% (1)
- Arnold-Chiari Malformation Anatomical Variations and Latest Embryological Perspective Review of LiteratureDocument3 pagesArnold-Chiari Malformation Anatomical Variations and Latest Embryological Perspective Review of LiteraturedodyidaNo ratings yet
- Unit 4 Typological of Learners With DifficultiesDocument33 pagesUnit 4 Typological of Learners With DifficultiesMerry Carlien RudasNo ratings yet
- Management of Sacral Dimples Detected On Routine Newborn Examination: A Case Series and ReviewDocument3 pagesManagement of Sacral Dimples Detected On Routine Newborn Examination: A Case Series and ReviewDesta FransiscaNo ratings yet
- NCM 109 Lec Final Quiz 2 Quiz 3Document4 pagesNCM 109 Lec Final Quiz 2 Quiz 3Faye Trisha100% (2)
- MeningomyeloceleDocument42 pagesMeningomyeloceleSundaraBharathiNo ratings yet
- HESI Pediatric HESI ReviewDocument41 pagesHESI Pediatric HESI Reviewprogramgrabber96% (24)
- Spina Bifida Fact SheetDocument4 pagesSpina Bifida Fact SheetNational Dissemination Center for Children with DisabilitiesNo ratings yet
- Associations USMLEDocument99 pagesAssociations USMLEnu.bombinaNo ratings yet
- MedBack MyelomeningoceleDocument3 pagesMedBack MyelomeningoceleJulia Rei Eroles IlaganNo ratings yet
- Congenital Spinal Malformations: Volume 22 - Number 4 - July 1992Document31 pagesCongenital Spinal Malformations: Volume 22 - Number 4 - July 1992Joa FloresNo ratings yet
- School of Health and Allied Health Sciences Nursing Department Self-Directed Learning (Nur 146 - Clinical Area)Document6 pagesSchool of Health and Allied Health Sciences Nursing Department Self-Directed Learning (Nur 146 - Clinical Area)bekbekk cabahugNo ratings yet
- Fetal Imaging EditedDocument59 pagesFetal Imaging EditedMicah Lou CalambaNo ratings yet
- Common Fetal Anomalies: Anencephaly Spina Bifida Cleft Lip Gastroschisis/Omphalocele Trisomy 18 Conjoined TwinsDocument52 pagesCommon Fetal Anomalies: Anencephaly Spina Bifida Cleft Lip Gastroschisis/Omphalocele Trisomy 18 Conjoined TwinsStangPongritNo ratings yet
- Pediatric Nursing: A. Sigmund Freud: Psychosexual TheoryDocument12 pagesPediatric Nursing: A. Sigmund Freud: Psychosexual TheoryMicah MagallanoNo ratings yet
- Koren. Fetal Safety of DYD in 1st Trimester PregnancyDocument5 pagesKoren. Fetal Safety of DYD in 1st Trimester PregnancyRuth RachmawatyNo ratings yet
- 60 Pedia DisordersDocument6 pages60 Pedia DisordersEkoy TheRealNo ratings yet
- Hydrocephalus AND Spina Bifida: MR - Sachin T.Gadade M.SC (N) PediatricsDocument61 pagesHydrocephalus AND Spina Bifida: MR - Sachin T.Gadade M.SC (N) PediatricsAbdirahman Abdillahi FarahNo ratings yet
- Spina BifidaDocument2 pagesSpina BifidaTracy100% (2)
- Orthopedic ImpairmentsDocument40 pagesOrthopedic Impairmentsapi-281466418100% (1)
- The Compass 2015Document178 pagesThe Compass 2015Venture Publishing100% (1)