Professional Documents
Culture Documents
Nursing Management of A Patient With Cardiomyopathy
Nursing Management of A Patient With Cardiomyopathy
Uploaded by
aby0 ratings0% found this document useful (0 votes)
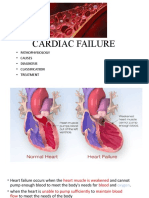
33 views4 pages1. Cardiomyopathy is a primary disorder of the heart muscle that causes abnormal myocardial performance and is not the result of disease or dysfunction of other cardiac structures.
2. The main types of cardiomyopathy include dilated, hypertrophic, restrictive, and arrhythmogenic right ventricular cardiomyopathy.
3. Nursing management of cardiomyopathy focuses on optimizing cardiac function through lifestyle changes, medications like beta blockers and ACE inhibitors, and devices like implantable defibrillators depending on the type and severity of cardiomyopathy.
Original Description:
Original Title
New Microsoft Word Document.docx
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document1. Cardiomyopathy is a primary disorder of the heart muscle that causes abnormal myocardial performance and is not the result of disease or dysfunction of other cardiac structures.
2. The main types of cardiomyopathy include dilated, hypertrophic, restrictive, and arrhythmogenic right ventricular cardiomyopathy.
3. Nursing management of cardiomyopathy focuses on optimizing cardiac function through lifestyle changes, medications like beta blockers and ACE inhibitors, and devices like implantable defibrillators depending on the type and severity of cardiomyopathy.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
33 views4 pagesNursing Management of A Patient With Cardiomyopathy
Nursing Management of A Patient With Cardiomyopathy
Uploaded by
aby1. Cardiomyopathy is a primary disorder of the heart muscle that causes abnormal myocardial performance and is not the result of disease or dysfunction of other cardiac structures.
2. The main types of cardiomyopathy include dilated, hypertrophic, restrictive, and arrhythmogenic right ventricular cardiomyopathy.
3. Nursing management of cardiomyopathy focuses on optimizing cardiac function through lifestyle changes, medications like beta blockers and ACE inhibitors, and devices like implantable defibrillators depending on the type and severity of cardiomyopathy.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 4
Nursing management of a patient with cardiomyopathy
CARDIOMYOPATHY Cardiomyopathy (CMP)is a primary disorder of the heart muscle that
causes abnormal myocardial performance and is not the result of disease or dysfunction of
other cardiac structures. ( K.V. Krishnadas)
CARDIOMYOPATHY A heterogeneous group of diseases of the myocardium
associated with mechanical and/or electrical dysfunction, which usually (but not
invariably) exhibit inappropriate ventricular hypertrophy or dilatation, and are due to
a variety of etiologies that frequently are genetic. ( Hurst’s text book of cardiology)
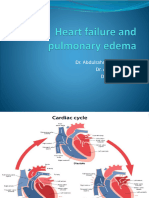
RELATED ANATOMY AND PHYSIOLOGY • Cardiac muscle (heart muscle)
involuntary striated muscle • The myocardium is the muscle tissue of the heart, and
forms a thick middle layer between the outer epicardium layer and the inner
endocardium layer
INCIDENCE • Dilated cardiomyopathy, the most common form, affects five in
100,000 adults and 0.57 in 100,000 children. • Hypertrophic cardiomyopathy, the
leading cause of sudden death in athletes, with an incidence of one in 500 persons. •
Restrictive cardiomyopathy and arrhythmogenic right ventricular cardiomyopathy are
rare, and their diagnoses require a high index of suspicion.
CLASSIFICATION OF CARDIOMYOPATHIES
WHO classification of cardiomyopathy(1995)
American Heart Association classification of cardiomyopathy
Primary secondary
Secondary cardiomyopathy • Infiltrative • Storage • Toxicity • Inflammatory •
Endocrine • Nutritional deficiencies • Consequence of cancer therapy • Autoimmune/
collagen
1. 10. Hypertrophic Cardiomyopathy
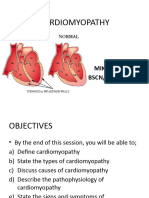
2. 11. Hypertrophic Cardiomyopathy • It is characterized by inappropriate left
ventricular hypertrophy, decreased cardiac output and outflow obstruction. •
Hypertrophic subaortic stenosis
3. 12. Common causes • Genetic(autosomal dominant) or familial • Hypertension •
Ischemia( coronary artery disease) • Aortic stenosis
4. 13. PATHOPHYSIOLOGY Four main characteristics • Massive ventricular
hypertrophy • Rapid, forceful contraction of the left ventricle. • Impaired relaxation(
diastole) • Obstruction to aortic outflow
5. 14. CLINICAL MANIFESTATIONS
6. 15. • Rapid, pounding heartbeat. • Chest tightness or pressure. • Fluid retention
resulting in swollen feet or ankles or unexplained weight gain.
7. 16. Diagnostic studies • History and physical examination • Palpation and auscultation
of the chest. • ECG findings • Echocardiogram • Chest X ray • Cardiac catheterization
8. 17. Management of hypertrophic cardiomyopathy
9. 18. GOAL • Improve ventricular filling. • Reduce ventricular contractility • Relieve
left ventricular outflow obstruction.
10. 19. Management of cardiomyopathy Lifestyle changes • Reduced alcohol
consumption, weight loss, exercise, smoking cessation, and a low-sodium diet.
11. 20. Management of cardiomyopathy • ᵦ adrenergic blockers • Calcium channel
blockers • Antidysrrhythmics • Implantable Cardioverter Defibrillator • Dual-
Chamber Pacing
12. 21. Symptomatic management Percutaneous Transluminal Septal Myocardial
Ablation(PTSMA)
13. 22. Surgical management • Ventriculomyotomy and myectomy
14. 23. Arrhythmogenic Right Ventricular Cardiomyopathy/ Dysplasia
15. 24. • It predominantly involves the right ventricle with progressive loss of myocytes
and fibrofatty tissue replacement, resulting in regional (segmental) or global
abnormalities. • Genetic defects of the part of the heart muscle, desmosome. • It
shows autosomal dominant inheritance
16. 25. • 80% of individuals present with syncope, palpitations or sudden cardiac death. •
Noninvasive tests • 12-lead ECG, signal-average ECG, echocardiography, right
ventricular angiography, CMR imaging, CT, and electroanatomic mapping of the
right ventricle
17. 26. • Endomyocardial biopsy Treatment • includes lifestyle alterations (i.e., avoiding
intense physical activity), antiarrhythmic drugs, and implantable cardioverter-
defibrillators in high-risk patients. • Cardiac transplantation
18. 27. ION CHANNELOPATHIES • Brugada syndrome • Long QT syndrome • Short
QT syndrome • SUNDS( Sudden Unexplained Nocturnal Death Syndrome) •
Idiopathic ventricular fibrillation.
19. 28. Brugada Syndrome • Associated with mutations in the gene (SCN5A)that encodes
for the sodium ion channel in the cellmembranes of the muscle cells of the heart (the
myocytes).
20. 29. • A distinctive ECG pattern consisting of right bundle-branch block and coved
ST- segment elevation in the anterior precordial leads (V1–V3).
21. 30. Management • Treatment of underlying arrhythmias • Implantable cardioverter
defibrillator • Quinidine class Ia antiarrhythmic.
22. 31. DILATED CARDIOMYOPATHY
23. 32. DILATED CARDIOMYOPATHY It is characterized by dilatation of the
ventricles with subsequent impairment of systolic function. Most common
cardiomyopathy
24. 33. ETIOLOGY • Idiopathic • Autosomal dominant , recessive and X- linked modes
of inheritance. • Gene mutation • Inflammatory and Infectious Myocarditis •
Autoimmunity
25. 34. OTHER CAUSES • Cardiotoxic agents- alcohol, cocaine, doxorubicin(
adriamycin) • Hypertension • Ischemia ( coronary artery disease) • Metabolic
disorders • Muscular dystrophy • Pregnancy • Valve disease
26. 35. PATHOPHYSIOLOGY Diffuse inflammation and rapid degeneration of
myocardial fibers. Ventricular dilation Cardiomegaly Impairment of systolic function
(contractile dysfunction) Atrial enlargement and stasis of blood in the left ventricle.
27. 36. Heart becomes weak and the chambers get large. Heart cannot pump enough
blood out to the body Decreased cardiac output
28. 37. • Chamber enlargement frequently leads to a dilation of the valvular orifice. •
Intracavitary thrombi located in the ventricular apices
29. 38. CLINICAL MANIFESTATIONS • Decreased exercise capacity • Fatigue •
Dyspnea at rest • Paroxysmal nocturnal dyspnea • Orthopnea
30. 39. As the disease progresses the patient may experience • Dry cough • Palpitations •
Abdominal bloating • Nausea • Vomiting • Anorexia
31. 40. Signs • Irregular heart rate with an abnormal S3 and/or S4 • Tachycardia or
bradycardia • Pulmonary crackles • Edema • Weak peripheral pulses
32. 41. • Pallor • Hepatomegaly • Jugular venous distension • Heart murmurs •
Dysrhythmias
33. 42. DIAGNOSTIC STUDIES • Doppler echocardiography • Chest X-Ray • ECG •
Elevated serum BNP( if heart failure) • Cardiac catheterization
34. 43. EMB (Endomyocardial biopsy)
35. 44. • Biochemical testing • Endocrine function • Radionuclide imaging (radionuclide
ventriculography) • Cardiac MRI • Multidetector computed tomography
36. 45. MANAGEMENT Goal • Enhance myocardial contractility • Decrease afterload.
37. 46. MANAGEMENT • Nitrates (eg: Nitroglycerin) • ACE inhibitors( Eg: captopril) •
ᵦ adrenergic blockers( Eg: metoprolol) • Aldosterone antagonists ( Eg: spironolactone)
• Diuretics to maintain the volume balance. • Cardiac glycosides( Eg: Digoxin)
38. 47. MANAGEMENT • Antiarrhythmics( Eg: Amiodarone) • Anticoagulation therapy
• Treatement of underlying disease process. • Continuous infusion of dobutamine
followed by aggressive diuresis.
39. 48. • Implantable cardiac defibrillators. • Biventricular pacemakers.
40. 49. SURGERY • Left ventricular reconstruction • Implantation of external restraint
devices
41. 50. • Left ventricular assist devices • Heart transplantation
42. 51. EMERGING SPECIFIC THERAPIES • Agents to eradicate persistent viral
infections and immunomodulatory agents. • Stem cells for cardiac regeneration and
gene therapy approaches are in clinical trials.
43. 52. RESTRICTIVE CARDIOMYOPATHY
44. 53. Restrictive cardiomyopathy • It is a disease of the heart muscle that impairs
diastolic filling and stretch. • Systolic function remains unaffected. • Least common of
the cardiomyopathic conditions. • The heart chambers are unable to fill with blood
because the heart muscle is stiff.
45. 54. ETIOLOGY • Amyloidosis • Scarring of the heart from an unknown cause. •
Myocardial fibrosis • Hypertrophy and infiltration
46. 55. Secondary causes includes • Endomyocardial fibrosis • Sarcoidosis • Neoplastic
tumor • Ventricular thrombus • Fibrosis of different etiology • Radiation to the thorax
47. 56. PATHOPHYSIOLOGY Increase in stiffness of the ventricular walls Impaired
diastolic filling of the ventricle Reducing preload and end-diastolic volume Heart
failure
48. 57. As the disease progresses Systolic dysfunction
49. 58. CLINICAL MANIFESTATIONS Classic symptoms of restrictive CMP are •
Fatigue • Exercise intolerance • Dyspnea
50. 59. Additional symptoms • Angina • Orthopnea • Syncope • Palpitations
51. 60. SIGNS OF HEART FAILURE • Dyspnea • Peripheral edema • Ascites •
Hepatomegaly • Jugular venous distension. • Kussmaul sign
52. 61. DIAGNOSTIC STUDIES • Chest x ray • ECG • Echocardiography •
Endomyocardial biopsy
53. 62. MANAGEMENT GOAL Improve diastolic filling Treatment of underlying
disease process
54. 63. • Treatment include conventional therapy for heart failure and dysrhythmias. •
Diuretics may help relieve symptoms • Calcium channel blockers. • Cardiac
transplantation
55. 64. COMPLICATIONS Embolus formation. Decreased ejection fraction allow
stasis of blood to occur in Lt ventricle. Thrombus may lodged in spleen kidney,
extremities, cerebral or coronary circulation. Dysarrhythmias. Sudden cardiac
death.
56. 65. Stress provoked (Tako-tsubo or Broken Heart Syndrome) • An acute
cardiomyopathy can be provoked by a stressful or emotional situation or exposure to
high doses of catecholamines (sympathomimetic drugs).
57. 66. Typical presentation • sudden onset of congestive heart failure • ECG changes
mimicking a myocardial infarction of the anterior wall. • Bulging out of the left
ventricular apex with a hypercontractile base of the left ventricle is often noted. •
"tako tsubo", or octopus pot in Japan.
58. 67. Treatment • Supportive management • Intra-aortic balloon pump • Fluids, and
negative inotropes such as beta blockers or calcium channel blocker • Aspirin
59. 68. • Common among middle-aged women • In most cases is fully reversible with
supportive care. • ECG fingings- myocardial infarction in the presence of left
ventricular dysfunction and absence of epicardial coronary stenoses should prompt the
diagnosis. • Endomyocardial biopsy is of value to exclude myocarditis.
60. 69. Peripartum Cardiomyopathy • Peripartum cardiomyopathy is defined as a
cardiomyopathy manifesting between the last month of pregnancy and 6 months post
partum.
61. 70. • Orthopnea • Dyspnea • pitting Edema • cough, frequent night-time urination, •
excessive weight gain during the last month of pregnancy (1-2+ kg/week; two to four
or more pounds per week), • Palpitations and chest pain.
62. 71. COMPLICATIONS • stroke, loss of circulation to a limb, even coronary artery
occlusion (blockage) with typical myocardial infarction
63. 72. Treatment • similar to treatment for congestive heart failure
64. 73. NURSING MANAGEMENT
65. 74. NURSING MANAGEMENT Nursing Assessment • Evaluate patient's chief
complaint, which may include fever, syncope, general aches, fatigue, palpitations,
dyspnea. • Evaluate etiologic factors, such as alcohol abuse, pregnancy, recent
infection, or history of endocrine disorders. • Assess for positive family history.
66. 75. • Auscultate lung sounds for crackles (pulmonary edema) or decreased sounds
(pleural effusion) • Assess heart size through palpation of chest for point of maximal
impulse (PMI), and auscultate for abnormal sounds. • Evaluate cardiac rhythm and
ECG for evidence of atrial or ventricular enlargement and infarction.
67. 76. Nursing Diagnoses • Decreased Cardiac Output related to decreased ventricular
function and/or dysrhythmias • Activity intolerance related to low cardiac output •
Fluid volume excess in related to ventricular dysfunction • Anxiety related to fear of
death and hospitalization • Fatigue related to disease process
You might also like
- RCL Pre-Employment Medical Examination Form B Revised 2015-03Document2 pagesRCL Pre-Employment Medical Examination Form B Revised 2015-03Ahmad Shodiq100% (1)
- ATI OB Study GuideDocument26 pagesATI OB Study GuideThelma Jerome100% (1)
- QRS 4-2Document1,057 pagesQRS 4-2Sree Harsha Gunneri100% (1)
- Hypertrophic CardiomyopathyDocument37 pagesHypertrophic CardiomyopathyMarko Vukovic100% (1)
- Pharmacist Workup of Drug Therapy in Pharmaceutical Care: Problem Oriented Pharmacist RecordDocument22 pagesPharmacist Workup of Drug Therapy in Pharmaceutical Care: Problem Oriented Pharmacist RecordputihatauhitamNo ratings yet
- A.tozeren - Human Body Dynamics - Classical Mechanics and Human MovementDocument172 pagesA.tozeren - Human Body Dynamics - Classical Mechanics and Human MovementTudor BoarescuNo ratings yet
- CARDIOMYOPATHIESDocument80 pagesCARDIOMYOPATHIESNadun MethwadaneNo ratings yet
- Cardiomyopathy Joisy AloorDocument31 pagesCardiomyopathy Joisy AloorJoisy AloorNo ratings yet
- Cardiogenic ShockDocument49 pagesCardiogenic Shockmaibejose0% (1)
- Patofisiologi Shock CardiogenicDocument44 pagesPatofisiologi Shock CardiogenicGalih Arief Harimurti Wawolumaja100% (1)
- 3.cardiac FailureDocument12 pages3.cardiac FailureAfiqul RashyedNo ratings yet
- CARDIOMYOPATHIESDocument46 pagesCARDIOMYOPATHIESStella CooKeyNo ratings yet
- Myocardial Infarction: Maj Aswathy Ganesh I Year MSC (N) Con, AfmcDocument45 pagesMyocardial Infarction: Maj Aswathy Ganesh I Year MSC (N) Con, AfmcAswathy ganeshNo ratings yet
- CARDIOMYOPATHYDocument67 pagesCARDIOMYOPATHYJoanna RachelNo ratings yet
- Kardiogenik SyokDocument43 pagesKardiogenik SyokGalih Arief Harimurti WawolumajaNo ratings yet
- Cardio My Opa ThiesDocument25 pagesCardio My Opa ThiesCrevins NyarikiNo ratings yet
- Nursing Mangement Client With Myocardial Infarction (Mi) Heart AttackDocument35 pagesNursing Mangement Client With Myocardial Infarction (Mi) Heart AttackTania Febria AzizahNo ratings yet
- Breakfast Symposium On Cardiomyopahies DraftDocument160 pagesBreakfast Symposium On Cardiomyopahies Draftmaria angela SaldajenoNo ratings yet
- Seminar ON: Cardiomyopat HYDocument43 pagesSeminar ON: Cardiomyopat HYmerin sunilNo ratings yet
- Cardio My Opa ThiesDocument14 pagesCardio My Opa Thiesabotreka056No ratings yet
- Curs 9 Myocarditis CardiomyopathyDocument41 pagesCurs 9 Myocarditis CardiomyopathyIliescu DenisaNo ratings yet
- CardiomyopathyDocument27 pagesCardiomyopathyakoeljames8543No ratings yet
- Pharmaceutical Care 5: Clinical Pharmacy Coronary Artery DiseaseDocument80 pagesPharmaceutical Care 5: Clinical Pharmacy Coronary Artery DiseaseJerson Aizpuro SuplementoNo ratings yet
- DCMDocument28 pagesDCMSissiNo ratings yet
- Stroke CMEDocument34 pagesStroke CMEKeren Karunya SingamNo ratings yet
- Heart Failure and CardiomyopathiesDocument26 pagesHeart Failure and Cardiomyopathieslionel andreaNo ratings yet
- Heart Failure and Pulmonary EdemaDocument60 pagesHeart Failure and Pulmonary EdemaYosra —No ratings yet
- Cardiomyopathy: By: P.Dhilip KumarDocument29 pagesCardiomyopathy: By: P.Dhilip Kumarpreet kaur100% (1)
- CARDIOMYOPATHYDocument26 pagesCARDIOMYOPATHYstaceyatienoomaNo ratings yet
- Cardiogenic ShockDocument31 pagesCardiogenic ShockLovelights ZamoraNo ratings yet
- Cardiogenic ShockDocument21 pagesCardiogenic ShockIslamOteshNo ratings yet
- Heart Failur E: Nitish Kumar Maddhesia, 74Document26 pagesHeart Failur E: Nitish Kumar Maddhesia, 74Akash NagarNo ratings yet
- DR Dhiman BanikCariogenic Shock Final 2022 DDDocument59 pagesDR Dhiman BanikCariogenic Shock Final 2022 DDCloudySkyNo ratings yet
- CardiomyopathyDocument98 pagesCardiomyopathyZellanien hdNo ratings yet
- Chronic Heart Failure (Gagal Jantung Kronik)Document15 pagesChronic Heart Failure (Gagal Jantung Kronik)Grup 9B Viscera tahun 2No ratings yet
- Medicine_Heart Failure and Acute Pulmonary OedemaDocument44 pagesMedicine_Heart Failure and Acute Pulmonary OedemaMK KNo ratings yet
- Cardiomyopathies 6th Year Seminar GRP BBDocument42 pagesCardiomyopathies 6th Year Seminar GRP BBmohamedeen hamza100% (1)
- Cardiovascular Review II: Ana H. Corona, MSN, FNP-C Nursing Instructor October 2007Document79 pagesCardiovascular Review II: Ana H. Corona, MSN, FNP-C Nursing Instructor October 2007leesteph78No ratings yet
- Cardio MyopathiesDocument39 pagesCardio Myopathiesinyanji.barasaNo ratings yet
- Heart Failure 1Document50 pagesHeart Failure 1dhiraj parmar100% (1)
- Congestive Heart FailureDocument47 pagesCongestive Heart FailureRajesh Sharma100% (2)
- Cardiogenic ShockDocument20 pagesCardiogenic Shockanimesh pandaNo ratings yet
- CARDIOMYOPATHYDocument36 pagesCARDIOMYOPATHYmanaswi debbarmaNo ratings yet
- Coronary Artery DiseaseDocument22 pagesCoronary Artery DiseaseMamoon Rashid100% (1)
- Coronary Heart Disorders-2Document111 pagesCoronary Heart Disorders-2shiklemeNo ratings yet
- Myocardial Infarction: Coronary Heart Disease (CHD) Coronary Artery Disease (CAD) Ischaemic Heart Disease (IHD)Document29 pagesMyocardial Infarction: Coronary Heart Disease (CHD) Coronary Artery Disease (CAD) Ischaemic Heart Disease (IHD)Mahum SohailNo ratings yet
- Cardiomyopathy: Mrs. D. Melba Sahaya Sweety M.SC Nursing GimsarDocument55 pagesCardiomyopathy: Mrs. D. Melba Sahaya Sweety M.SC Nursing GimsarD. Melba S.S ChinnaNo ratings yet
- 4. Heart Failure & CardiomyopathyDocument32 pages4. Heart Failure & CardiomyopathyhuehuemerchantNo ratings yet
- MF3 - Ischemic Heart DiseaseDocument28 pagesMF3 - Ischemic Heart DiseaseAnnbe BarteNo ratings yet
- Heartfailurepptsam 170511135108Document48 pagesHeartfailurepptsam 170511135108enam professorNo ratings yet
- СердечнаяDocument70 pagesСердечнаяDaniel FunkNo ratings yet
- Myocardial InfarctionDocument23 pagesMyocardial InfarctionAnelle Umali50% (2)
- 1.congestive Heart FailureDocument8 pages1.congestive Heart FailureJarda julie DacuagNo ratings yet
- Cardiomyopathies: Cardiomyopathy Is A Heart Muscle Disease Associated With CardiacDocument10 pagesCardiomyopathies: Cardiomyopathy Is A Heart Muscle Disease Associated With Cardiacmerin sunilNo ratings yet
- Cardiac EmergencyDocument56 pagesCardiac Emergency21rayhanf100% (1)
- Lecter 6th Mitral RegurgitationDocument4 pagesLecter 6th Mitral RegurgitationMuhammad KhalilNo ratings yet
- KARDIOMYOPATI - Kuliah DR - ErlinaDocument28 pagesKARDIOMYOPATI - Kuliah DR - ErlinaArif Zulfian MubarokNo ratings yet
- Myocardial Infarction. BPTDocument62 pagesMyocardial Infarction. BPTAanchal GuptaNo ratings yet
- Acquired Heart Disease EditedDocument63 pagesAcquired Heart Disease Editedapalah_niNo ratings yet
- Cardiomyopathy: Restrictive Heart DiseaseDocument18 pagesCardiomyopathy: Restrictive Heart DiseaseMitch GabuyaNo ratings yet
- Angina Pectoris: Ischemic Heart DiseaseDocument17 pagesAngina Pectoris: Ischemic Heart DiseaseMahum SohailNo ratings yet
- Acquired Heart Disease Edited2Document50 pagesAcquired Heart Disease Edited2apalah_niNo ratings yet
- Acute Coronary SyndromeDocument93 pagesAcute Coronary SyndromeissareinoNo ratings yet
- Session 24 Heart FailureDocument15 pagesSession 24 Heart Failuredreampurpose97No ratings yet
- Visual Guide to Neonatal CardiologyFrom EverandVisual Guide to Neonatal CardiologyErnerio T. AlbolirasNo ratings yet
- Health and Fitness - Script and Answer KeyDocument3 pagesHealth and Fitness - Script and Answer KeyAdam SimpsonNo ratings yet
- Borges, K. Et Al. (2018)Document7 pagesBorges, K. Et Al. (2018)Paulina Bermudez ValenzuelaNo ratings yet
- FluDocument31 pagesFluSheril Sularte CasanesNo ratings yet
- Journal CHFDocument9 pagesJournal CHFaniabNo ratings yet
- Postural DrainageDocument1 pagePostural Drainagezh4hft6pnzNo ratings yet
- PneumothoraxDocument3 pagesPneumothoraxYara YousefNo ratings yet
- Dentistry and Community IUST 010-011Document72 pagesDentistry and Community IUST 010-011sharif100% (1)
- Excellent Very Good Good Fair PoorDocument4 pagesExcellent Very Good Good Fair PoorJmarie Brillantes PopiocoNo ratings yet
- Multiple Myeloma Patient Education Manual: October 2007 EditionDocument85 pagesMultiple Myeloma Patient Education Manual: October 2007 EditionKareem WaheedNo ratings yet
- Closed System: Eltek CpuntDocument2 pagesClosed System: Eltek CpuntLozorroNo ratings yet
- Active VFC ProvidersDocument50 pagesActive VFC ProvidersClint AnthonyNo ratings yet
- Introduction To The Astm E3219 Standard Guide For Derivation of Health Based Exposure Limits (Hbels)Document10 pagesIntroduction To The Astm E3219 Standard Guide For Derivation of Health Based Exposure Limits (Hbels)nsk79inNo ratings yet
- Free PratiqueDocument5 pagesFree PratiqueDALASKE GERALDINE BENITES CALDERONNo ratings yet
- Understanding Ventilator Waveforms-And How To Use Them in Pa... - Nursing2020 Critical CareDocument19 pagesUnderstanding Ventilator Waveforms-And How To Use Them in Pa... - Nursing2020 Critical Caremahbub alamNo ratings yet
- Peptic Ulcer Disease (PUD) EditedDocument9 pagesPeptic Ulcer Disease (PUD) EditedRashed ShatnawiNo ratings yet
- Aperiomics Order Form: Xplore-PATHODocument2 pagesAperiomics Order Form: Xplore-PATHOSasu AlexandruNo ratings yet
- Comminuted Patella Fracture in Elderly Patients - A Systematic Review and Case ReportDocument10 pagesComminuted Patella Fracture in Elderly Patients - A Systematic Review and Case ReportAldrovando JrNo ratings yet
- RONE NCM112BSN3C PhosphorusImbalanceDocument27 pagesRONE NCM112BSN3C PhosphorusImbalanceChezer KiethNo ratings yet
- Nursing Care Plan Juvida, Clarissa A. BSN 2A: "Mainit Ang Anak Ko at Nanghihina ."Document3 pagesNursing Care Plan Juvida, Clarissa A. BSN 2A: "Mainit Ang Anak Ko at Nanghihina ."Clarissa JuvidaNo ratings yet
- Autoimmune Diseases - MMSDocument37 pagesAutoimmune Diseases - MMSmulatumeleseNo ratings yet
- Mohamed Abdel Shafy Mohammady Tabl - 7 - Safety of Ticagrelor Post Fibrinolysis in STEMI PatientsDocument60 pagesMohamed Abdel Shafy Mohammady Tabl - 7 - Safety of Ticagrelor Post Fibrinolysis in STEMI PatientsJovita SardanisNo ratings yet
- Maternal and Early-Life Nutrition and HealthDocument4 pagesMaternal and Early-Life Nutrition and HealthTiffani_Vanessa01No ratings yet
- Icd 10Document78 pagesIcd 10KumarNo ratings yet
- AHA Scientific Statement: Resistant Hypertension: Detection, Evaluation, and ManagementDocument38 pagesAHA Scientific Statement: Resistant Hypertension: Detection, Evaluation, and ManagementPratik TripathiNo ratings yet
- HypnotherapyDocument6 pagesHypnotherapyAnnisa Walidatus0% (1)