Professional Documents
Culture Documents
Julian Kate O. Balintag BSN 1F Elimination (Fecal) 1. Discuss The Physiology of Defecation
Julian Kate O. Balintag BSN 1F Elimination (Fecal) 1. Discuss The Physiology of Defecation
Uploaded by
Kate B0 ratings0% found this document useful (0 votes)
22 views10 pagesThe document discusses the physiology of defecation including the movement of feces through the colon and rectum stimulated by peristaltic waves and sensory nerves. When the internal and external sphincters relax, feces move into the anal canal and are expelled through contraction of abdominal muscles and diaphragm. Factors that can affect defecation include development, diet, fluid intake, activity, medications, procedures, and pathologic conditions. Common issues like constipation, fecal impaction, diarrhea, and bowel incontinence are also described along with their causes and effects. Methods to assess the elimination process and maintain normal patterns through privacy, timing, nutrition, exercise, and positioning are outlined. The purpose and actions
Original Description:
fundamentals of nursing practice
Original Title
Funda
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe document discusses the physiology of defecation including the movement of feces through the colon and rectum stimulated by peristaltic waves and sensory nerves. When the internal and external sphincters relax, feces move into the anal canal and are expelled through contraction of abdominal muscles and diaphragm. Factors that can affect defecation include development, diet, fluid intake, activity, medications, procedures, and pathologic conditions. Common issues like constipation, fecal impaction, diarrhea, and bowel incontinence are also described along with their causes and effects. Methods to assess the elimination process and maintain normal patterns through privacy, timing, nutrition, exercise, and positioning are outlined. The purpose and actions
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
22 views10 pagesJulian Kate O. Balintag BSN 1F Elimination (Fecal) 1. Discuss The Physiology of Defecation
Julian Kate O. Balintag BSN 1F Elimination (Fecal) 1. Discuss The Physiology of Defecation
Uploaded by
Kate BThe document discusses the physiology of defecation including the movement of feces through the colon and rectum stimulated by peristaltic waves and sensory nerves. When the internal and external sphincters relax, feces move into the anal canal and are expelled through contraction of abdominal muscles and diaphragm. Factors that can affect defecation include development, diet, fluid intake, activity, medications, procedures, and pathologic conditions. Common issues like constipation, fecal impaction, diarrhea, and bowel incontinence are also described along with their causes and effects. Methods to assess the elimination process and maintain normal patterns through privacy, timing, nutrition, exercise, and positioning are outlined. The purpose and actions
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 10
Julian Kate O.
Balintag to pass and take only a minute to push
out.That said, some people do spend a
BSN 1F bit more time on the toilet, so as a
Elimination ( Fecal ) general rule, a poop should take no
more than 10 to 15 minutes.
1. Discuss the physiology of Share on Pinterest
defecation
3. Identify factors that affect
-Peristaltic waves move the feces into
defecation
the sigmoid colon and the rectum
-Sensory nerves in rectum are -Developmental stage
stimulated -Diet
Individual becomes aware of need to -Fluid
defecate -Activity
-Feces move into the anal canal when -Psychologic factors
the internal and external sphincter relax -Defecation habits
-External anal sphincter is relaxed -Medications
voluntarily if timing is appropriate -Diagnostic procedures
-Expulsion of the feces assisted by -Anesthesia
contraction of the abdominal muscles -Surgery
and the diaphragm -Pathologic conditions
-Moves the feces through the anal canal -Pain
and expelled through anus
-Facilitated by thigh flexion and a sitting 4. Identify common causes and
position effects of selected fecal elimination
process
2. Distinguish abnormal
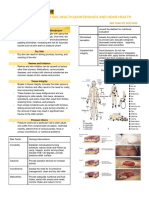
characteristics and constituents of Constipation
-Decreased frequency of defecation
feces
-Hard, dry, formed stools
Color - the brown coloring. Bilirubin, -Straining at stools
-Painful defecation
which is a pigment compound formed
-Causes include:
from the breakdown of red blood cells in -Insufficient fiber and fluid intake
the body, gets the credit for this oh-so- -Insufficient activity
lovely shade of brown. -Irregular habits
Shape - A somewhat loglike shape is
how most poop should come out due to Fecal Impaction
its formation within the intestines. -Mass or collection of hardened feces in
folds of rectum
However, as we’ll get to later, there are
-Passage of liquid fecal seepage and no
a variation of shapes that poop can normal stool
have.And when they differentiate from -Causes usually:
the log/sausage shape, that’s when your -Poor defecation habits
poop is trying to tell you something’s up. -Constipation
Size - Poops shouldn’t come out in
small pellets (something else we’ll get to Diarrhea
-Passage of liquid feces and increased
later) but instead should be a couple frequency of defecation
inches in length, comfortable and easy -Spasmodic cramps, increased bowel
to pass. sounds
Consistency - Anywhere between a -Fatigue, weakness, malaise,
firm and soft consistency is pretty much emaciation
normal. If it sways one way or another, it -Major causes:
-Stress, medications, allergies,
could suggest some digestion or fiber
intolerance of food or fluids, disease of
issues. colon
Length of time (how long it takes ) - A
healthy poop, however, should be easy Bowel Incontinence
-Loss of voluntary ability to control fecal currently has, the frequency of
and gaseous discharges defecation, and the types of foods that
-Generally associated with: the client finds assist with normal
-Impaired functioning of anal sphincter
defecation.
or nerve supply
-Neuromuscular diseases Exercise – regular exercise helps
-Spinal trauma
clients develop a regular defecation
-Tumor
pattern.
Flatulence
Positioning – although the squatting
-Excessive flatus in intestines
-Leads to stretching and inflation of position best facilitates defecation, on a
intestines toilet seat the best position for most
-Can occur from variety of causes: people seems to be leaning forward.
-Foods
-Abdominal surgery
-Narcotics
7. Describe the purpose and action of
commonly used edema solutions
5. Describe methods used to assess fecal
-Hypertonic (Fleet phosphate)
elimination process
-Draws water into colon
Nursing History Assesing for Bowel -Hypotonic (tap water)
Info -Distends the colon
-Ascertains the client's normal pattern -Stimulates peristalsis
-Description of usual feces -Softens feces
-Recent changes
-Isotonic (physiologic saline)
-Past problems with elimination
-Presence of an ostomy -Distends the colon
-Factors influencing elimination pattern -Stimulates peristalsis
-Softens feces
Physical Examination Assesing for -Soapsuds (pure soap)
Bowel Info -Irritate mucosa
-Examination of the abdomen, -Distends the colon
rectum, and anus
-Oil
-Auscultation precedes palpation
because palpation alters peristalsis -Lubricates feces and colonic mucosa
-Inspection of feces for
color,consistency, shape, amount, odor, 8. Describe essential of fecal stoma
abnormal constituents care for clients with an ostonomy
-Review any data obtained from relevant
diagnostic tests -Normal stoma should appear red and
may bleed slightly when touched
6. Identify measures that maintain -Assess the peristomal skin for irritation
normal fecal elimination patterns each time the appliance is changed
-Treat any irritation or skin breakdown
immediately
Privacy – privacy during defecation is
-Keep skin clean by washing off any
extremely important to many people.
excretion and drying thoroughly
The nurse should therefore provide as
-Protect skin, collect stool, and control
much privacy as possible for such
odor with an ostomy appliance
clients but may need to stay with those
who are too weak to be left alone. 9. Describe the steps in
Timing – a client should be encouraged Administering enema to achieve one
to defecate when the urge is or more of the following actions:
recognized. cleansing, carminative, retention, or
return-flow.
Nutrition and fluids – the client needs
for regular normal elimination varies, Implementation – lubricate about 5 cm
depending on the kind of feces the client of the rectal tube
Performance 5. assist the client in comfortable lying
or sitting position
1. prior to performing the procedure,
introduce self and verify the client’s 6. unfasten the belt if the client is
identity using agency protocol. wearing one
2. perform hand hygiene 7. empty the pouch and remove the
ostomy skin barrier
3. apply clean gloves
8. clean and dry the peristomal skin and
4. provide for client privacy stoma
5. assist the client to a left lateral 9. assess the peristomal skin and stoma
position, with the right leg as acutely
fixed as possible, with the linen-saver 10. place a piece of tissue or gauze
pad under the buttocks. over the stoma, and change it as
needed.
6. Insert enema tube
11. prepare and apply skin barrier.
7. slowly administer enema solution
8. encourage the client to retain enema
9. assist client to defecate
10. document the type and volume, if
appropriate, of enema given. Describe
the results.
Changing a bowel diversion ostomy
appliance – to assess and care for
peristomal skin; to collect stool for
assessment of the amount an type of
output; to minimize odors for the client’s
comfort and self esteem.
Implementation
1. determine the need for an appliance
change
2. if there is pouch leakage or
discomfort at or round the stoma,
change of the appliance.
3. select an appropriate time to change
the appliance.
Performance
1. introduce yourself and and verify the
client’s identity using agency protocols.
Explain the procedure to the client.
2. perform hand hygiene and observe
other appropriate infection revention
procedures
3. apply clean gloves
4. provide for client privacy
Elimination ( urinary ) - -prescribed diuretic
- -presence of thirst, dehydration,
1. Factors affecting urinary and weight loss
elimination/ voiding - -history of diabetes mellitus,
Developmental factors diabetes insipidus, or kidney
disease.
Infants - urine output varies according
to fluid intake but gradually increases to
250 to 500 ml a day during the first year. - -Oliguria or Anuria (little or no
urine output) – decreased
Pre-schoolers – the pre-schooler is urinary output usually less than
able to take responsibility for 500 ml a day or 30 ml.
independent toileting. - decrease in fluid intake
- -signs of dehydration
School age children – the child’s
- -presence of hypotension, shock
school age elimination system reaches
or heart failure
maturity during this period.
- -history of kidney disease
Older adults – the excretory function of - -signs of renal failure such as
the kidney diminishes with age, but elevated blood urea nitrogen,
usually not significantly below normal serum creatinine, edema
levels unless a disease process
intervenes. Urgency
- -presence of psychological stress
Psychosocial factors – for many - UTI
people, a set of conditions helps
stimulate the micturition reflex. These
conditions include privacy, normal
position, sufficient time, and Dysuria
occasionally, running water. - Urinary tract inflammation,
infection, or injury
Medications – Many medications
- Hesitancy, hematuria, pyuria ,
particularly those affecting the
and frequency
autonomic nervous system, interfere
with the normal urination process and
Enuresis
may cause retention.
- Family history of enuresis
Muscle tone - good muscle tone is - Difficult access to toilet facilities
important to maintain the stretch and - Home stress
contractility of the detrusor muscle so
the bladder can refill adequately and Incontinence
empty completely. - Bladder inflammation,
cerebrovascular, accident, spinal
Pathologic conditions – some cord injury, or other disease.
diseases and pathologies can affect the - Difficulties in independent
formation and excretion of urine. toileting
Surgical and Diagnostic Procedure – - Leakage when coughing,
some surgical and diagnostic laughing, sneezing
procedures affect the passage of urine
and the urine itself. 3. Describe nursing interventions to
maintain urinary elimination, prevent
2. Identify common causes of urinary tract infection and manage
selected urinary problems urinary incontinence.
- Promoting fluid intake
-Polyuria (increased urine output)
Maintaining normal voiding
- -ingestion of fluids containing
patterns
caffeine or alcohol
Assisting with toileting attach the urinary drainage system. •
Preventing urinary tract infections Make sure that the tip of the penis is not
Managing urinary incontinence touching the condom and that the
Continence (bladder) training condom is not twisted. Rationale:
A twisted condom could obstruct the
4. Identify ways to prevent ways to flow of urine. • Attach the urinary
prevent urinary infection. drainage system to the condom. •
- Drink 64 oz. of water a day Remove and discard gloves. • Perform
Practice frequent voiding (every 2 hand hygiene. • If the client is to remain
to 4 hours) in bed, attach the urinary drainage bag
Avoid use of harsh soaps, bubble to the bed frame. • If the client is
bath, powder, or sprays in the ambulatory, attach the bag to the client’s
perineal area leg. 8. Teach the client about the
Avoid tight fitting clothes drainage system. • Instruct the client to
Wear cotton rather than nylon keep the drainage bag below the level of
under clothes the condom and to avoid loops or kinks
Always wipe the perineal area in the tubing. Instruct the client to report
from front to back pain, irritation, swelling, or
Take showers rather than baths wetness/leaking around the penis to
health care personnel. 9. Inspect the
5. Describe the steps in penis 30 minutes following condom
application and at least every 4 hours.
Applying and external urinary device
Check urine flow. Document these
Performance 1. Prior to performing the findings. 10. Change the condom as
procedure, introduce self and verify the indicated and provide skin care. In most
client’s identity using agency protocol. settings, the condom is changed daily.•
Explain to the client what you are going Remove the elastic or Velcro strip, apply
to do, why it is necessary, and how he clean gloves, and roll off the condom.•
can participate. 2. Perform hand Wash the penis with soapy water, rinse,
hygiene and observe other appropriate and dry it thoroughly.• Assess the
infection prevention procedures. 3. foreskin for signs of irritation, swelling,
Position the client in either a supine or a and discoloration. 11. Document in the
sitting position. Provide for client client record using forms or checklists
privacy. 4. Apply clean gloves. 5. supple-mented by narrative notes when
Inspect and clean the penis. • Clean the appropriate. Record the ap-plication of
genital area and dry it thoroughly. the condom, the time, and pertinent
Rationale: This minimizes skin irritation observations, such as irritated areas on
and excoriation after the condom is the penis.SAMPLE DOCUMENTATION
applied. 6. Apply and secure the
Performing urinary catheterization –
condom. • Roll the condom smoothly
over the penis, leaving 2.5 cm. (1 in.) Performance 1. Prior to performing the
between the end of the penis and the procedure, introduce self and verify the
rubber or plastic connecting tube. • client’s identity using agency protocol.
Secure the condom firmly, but not too Explain to the client what you are going
tightly, to the penis. Some condoms to do, why it is necessary, and how he
have an adhesive inside the proximal or she can participate. 2. Perform hand
end that adheres to the skin of the base hygiene and observe other appropriate
of the penis. Many condoms are infection prevention procedures. 3.
packaged with special tape. If neither is Provide for client privacy. 4. Place the
present, use a strip of elastic tape or client in the appropriate position and
Velcro around the base of the penis drape all areas except the perineum. •
over the condom. Ordinary tape is Female: supine with knees flexed, feet
contraindicated because it is not flexible about 2 feet apart, and hips slightly
and can stop blood flow. 7. Securely externally rotated, if possible • Male:
supine, thighs slightly abducted or apart open system), attach the drainage end
5. Establish adequate lighting. Stand on of an indwelling catheter to the
the client’s right if you are right-handed, collecting tubing and bag. 21. Examine
on the client’s left if you are left-handed. and measure the urine. In some cases,
6. If using a collecting bag and it is not only 750 to 1,000 mL of urine are to be
contained within the catheterization kit, drained from the bladder at one time.
open the drainage package and place Check agency policy for further
the end of the tubing within reach. 7. If instructions if this should occur. 22.
agency policy permits, apply clean Remove the straight catheter when
gloves and inject 10 to 15 mL Xylocaine urine flow stops. For an indwelling
gel into the urethra of the male client. catheter, secure the catheter tubing to
Wipe the underside of the penile shaft to the thigh for female clients or the upper
distribute the gel up the urethra. Wait at thigh or lower abdomen for male clients
least 5 minutes for the gel to take effect to prevent movement on the urethra or
before inserting the catheter. 8. excessive tension or pulling on the
Remove and discard gloves. • Perform retention balloon23. Next, hang the bag
hand hygiene. 9. Open the below the level of the bladder. No tubing
catheterization kit. Place a waterproof should fall below the top of the bag.
drape under the buttocks (female) or ❻24. Wipe any remaining antiseptic or
penis (male) without contaminating the lubricant from the perineal area.
center of the drape with your hands. 10. Replace the foreskin if retracted earlier.
Apply sterile gloves. 11. Organize the Return the client to a comfortable
remaining supplies: • Saturate the position. Instruct the client on
cleansing balls with the antiseptic positioning and moving with the catheter
solution. • Open the lubricant package. in place.25. Discard all used supplies in
• Remove the specimen container and appropriate receptacles.26. Remove
place it nearby with the lid loosely on and discard gloves.• Perform hand
top. 12. Attach the prefilled syringe to hygiene.27. Document the
the indwelling catheter inflation hub. catheterization procedure including
Apply agency policy and/or catheter size and results in the client
manufacturer recommendation record using forms or checklists supple-
regarding pretesting of the balloon. 13. mented by narrative notes when
Lubricate the catheter 2.5 to 5 cm (1 to appropriate.
2 in.) for females, 15 to 17.5 cm (6 to 7
in.) for males, and place it with the Performing bladder irrigation –
drainage end inside the collection Performance 1. Prior to performing the
container. 14. If desired, place the procedure, introduce self and verify the
fenestrated drape over the perineum, client’s identity using agency protocol.
exposing the urinary meatus. 15. Explain to the client what you are going
Cleanse the meatus. Note: The to do, why it is necessary, and how he
nondominant hand is considered or she can participate. The irrigation
contaminated once it touches the should not be painful or uncomfortable.
client’s skin. 16. Insert the catheter17. Discuss how the results will be used in
Hold the catheter with the nondominant planning further care or treatments. 2.
hand. 18. For an indwelling catheter, Perform hand hygiene and observe
inflate the retention balloon with the other appropriate infection prevention
designated volume. 19. Collect a urine procedures. 3. Provide for client
specimen if needed. For a straight privacy. 4. Apply clean gloves. 5.
catheter, allow 20 to 30 mL to flow into Empty, measure, and record the amount
the bottle without touching the catheter and appearance of urine present in the
to the bottle. For an indwelling catheter drainage bag. Rationale: Emptying the
preattached20. Allow the straight drainage bag allows more accurate
catheter to continue draining into the measurement of urinary output after the
urine receptacle. If necessary (e.g., irrigation is in place or completed.
Assessing the character of the urine
provides baseline data for later
comparison. 6. Discard urine and
gloves. 7. Prepare the equipment. •
Perform hand hygiene. • Connect the
irrigation infusion tubing to the irrigating
solution and flush the tubing with
solution, keeping the tip sterile.
Rationale: Flushing the tubing removes
air and prevents it from being instilled
into the bladder. Irrigation bag Drip
chamber Clamp Bladder Tubing from
bladder Tubing to irrigation port Port for
inflation of catheter balloon Drainage
bag • Apply clean gloves and cleanse
the port with antiseptic swabs. •
Connect the irrigation tubing to the input
port of the threeway catheter. • Connect
the drainage bag and tubing to the
urinary drainage port if not already in
place. • Remove and discard gloves. •
Perform hand hygiene. 8. Irrigate the
bladder. • For closed continuous
irrigation using a three-way catheter,
open the clamp on the urinary drainage
tubing (if present). 9. Assess the client
and the urinary output. • Assess the
client’s comfort. • Apply clean gloves. •
Empty the drainage bag and measure
the contents. Subtract the amount of
irrigant instilled from the total volume of
drainage to obtain the volume of urine
output. • Remove and discard gloves. •
Perform hand hygiene. 10. Document
findings in the client record using forms
or checklists supplemented by narrative
notes when appropriate. • Note any
abnormal constituents such as blood
clots, pus, or mucous shreds.
Personal Preference – people develop
likes and dislikes based on associations
NUTRITION with a typical food.
1, identify the essential nutrients and Religious practice – some Roman
dietary sources Catholics avoid meat on certain days,
Carbohydrates – are composed of the and some Protestant faiths prohibit
elements carbon, hydrogen, and oxygen meat, tea, coffee, or alcohol. Both
and are two basic types: simple Orthodox and Judaism, Islam prohibit
carbohydrates and complex pork. The nurse must plan care with
carbohydrates. considerations of such dietary practices.
Proteins – amino acids, organic Economics – What, how much, and
molecules made up primarily of carbon, how often a person eats are frequently
hydrogen, oxygen, and nitrogen, affected by economic status.
combine to form proteins. Medications and Therapy - the effects
Lipids – are organic substances that of drugs on nutrition vary considerably.
are greasy and insoluble in water but Health – and individual’s health status
soluble in alcohol or ether. greatly affects eating habits nutritional
Micronutrients - are one of the major status.
groups of nutrients your body needs. Alcohol Consumption – the calories in
They include vitamins and minerals. alcoholic drinks include both those of
Vitamins are necessary for energy the alcohol itself and of the juices or
production, immune function, blood other beverages added to the drink.
clotting and other functions. Meanwhile,
minerals play an important role in
growth, bone health, fluid balance and
several other processes. 3. Identify nutritional variation
throughout life cycle
2. Factors affecting nutrition
Neonate to 1 year – the neonates fluid
Development – people in rapid periods and nutritional needs are met by breast
of growth have increased needs for milk or formula. Fluid needs of infants
nutrients. Older adults on the other hand are proportionately greater than those of
may need fewer calories and also need adults because of a higher metabolic
some dietary changes in viw of their risk rate, immature kidneys, and greater
for coronary heart diseases, water losses though the skin and lungs.
osteoporosis, and hypertension.
Toddler - because of Maturing GI tract,
Sex - nutrient requirements are toddlers can eat most foods and adjust
different for men and women bevause of to three meals a day. Toddler’s fine
body composition and reproductive motor skills are sufficiently well
functions. developed for them to learn how to feed
themselves.
Ethnicity and Culture - ethnicity often
determines food preferences. Traditional Pre-schooler - The pre schooler eat
for rice for Asians pasta for Italians curry adult foods Parents should become
for Indians are eaten long after customs informed about the diet of their child in
are abandoned. day are or pre school settings so that
they can assume that the child’s
Beliefs about Food – beliefs about nutritional needs are being met.
food on health and well being can affect
food from television, magazines, and School of age child – school of age
other media. children require a balanced diet
including approximately 1,600 to 2,200
kcal/day. They can eat three meals a gastric wall. Depending on what you
day and one or two nutritious snacks. need or what the doctor has ordered, be
sure to choose the correct tube for the
Adolescent – the adolescent’s need for job. It is important to explain to the
nutrients and calories increases, patient the process for inserting the NG
particularly during growth spurt. tube, because it can be a scary and
uncomfortable experience. Insertion
Young Adult - Many young adults are Before inserting the tube, you should
aware of thr food groups but may not be measure the length of tube you will
need. Take the end and measure from
knowledgeable about how many
the nose to the earlobe, then from the
servings of each group they need or earlobe to the xyphoid process. Mark
how much a serving constitutes. this measurement with tape, and you
can use this as a guide to help you
Middle aged adult – they should know how far to insert the tube. Drape
continue to eat a healthy diet, following the patient with a towel and have them
the recommended portions of the ffod hold the glass of water and the straw.
groups, with special attention to calcium They should sit up as straight as
and protein intake, and limiting possible and tilt their head back into a
sniffing position. Lubricate the NG tube
cholesterol and calorie intake.
thoroughly to ensure the easiest
Older Adults - the older adults require insertion possible.
The Process
the same basic nutrition as younger
1. Slowly insert the tube into the nare,
adult. However, fewer calories are curling down toward the back of the
needed by older adults because of the throat
low metabolic rate and the decrease in 2. Once you reach the oropharynx, you
physical activity. may begin to encounter resistance. At
this time, have the patient drop their
4. Discuss nursing interventions to chin to their chest
treat clients with nutritional problems 3. As they take swallows of water through
the straw, slowly advance the tube
further. They may cough and gag at this
point, but you should still be sure to
encourage swallowing and incrementally
advance the tube
4. Once you are past the oropharynx, your
patient should relax, and the tube will
advance more easily
5. Insert until you meet your tape mark and
secure the tube
Removing nasogastric tube
1. Prior to the performing the
removal, introduce self and verify
the client. Explain also the steps
5. Identify steps used in And why is it necessary .
2. Perform hand hygiene and
Nasogastric tubing observe appropriate infection
prevention.
Preparation 3. Provide client privacy
You should gather all of your materials 4. Detach tube
together before you approach the 5. Remove nasogastric tube.
patient. There are two types of NG 6. Ensure client comfort
tubes: Levin and Salem sump. A Levin 7. Dispose equipment properly
tube is often used for feeding, and it 8. Document all relevant
has lumens along the lower length. information
The Salem sump is used for suctioning
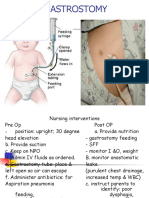
because of the presence of a secondary Administering a gastrostomy or
tube, or pigtail, which allows for jejunostomy tube feeding.
suctioning without adhering to the
1. Prior to the performing the
removal, introduce self and verify
2. Perform hand hygiene and
observe appropriate infection
prevention.
3. Provide client privacy
4. Insert a feeding tube if one is
already in place.
5. Check the location of the patency
of the tube
6. Administer the feeding
7. Ensure client comfort and safety
8. Document all assessment and
interventions.
6. Describe parenteral nutrition
Parenteral nutrition (PN) is intravenous
administration of nutrition, which may
include protein, carbohydrate, fat,
minerals and electrolytes, vitamins and
other trace elements for patients who
cannot eat or absorb enough food
through tube feeding formula or by
mouth to maintain good nutrition status.
Achieving the right nutritional intake in a
timely manner can help combat
complications and be an important part
of a patient’s recovery. Parenteral
nutrition is sometimes called Total
Parenteral Nutrition (TPN).
You might also like
- Managing The Bladder and Bowel in Spina BifidaDocument77 pagesManaging The Bladder and Bowel in Spina BifidaSeptinaAyuSamsiati100% (1)
- Annotated BibliographyDocument2 pagesAnnotated Bibliographyapi-247111687No ratings yet
- Preciado - Don't Trust ArchitectsDocument6 pagesPreciado - Don't Trust ArchitectsFiona Fabutima100% (1)
- Mahikari PDFDocument21 pagesMahikari PDFaurelio.arae100% (1)
- Bowel EliminationDocument3 pagesBowel EliminationPilacan KarylNo ratings yet
- EliminationDocument9 pagesEliminationJeffrey TrayaNo ratings yet
- Elimination PatternDocument50 pagesElimination Patternmamoonazafar2No ratings yet
- Bowel EliminationDocument41 pagesBowel EliminationekhafagyNo ratings yet
- Reviewer Chap 49 Fecal EliminationDocument3 pagesReviewer Chap 49 Fecal EliminationKeren GaciasNo ratings yet
- Fecal EliminationDocument29 pagesFecal EliminationhamisiNo ratings yet
- Elimination: Dumip-Ig, Maricel Gregorio, Kristine Milagrosa, Nina JesusaDocument30 pagesElimination: Dumip-Ig, Maricel Gregorio, Kristine Milagrosa, Nina JesusaKristine Las GregorioNo ratings yet
- Incontinence: M.Indumathi, M.sc-1 Year Med-Surg DepartDocument36 pagesIncontinence: M.Indumathi, M.sc-1 Year Med-Surg DepartAnn Merlin JobinNo ratings yet
- Bowel and Bladder EliminationDocument9 pagesBowel and Bladder EliminationApril Urbano-Gabot Alap0% (1)
- NCMB314 - Week 4Document4 pagesNCMB314 - Week 4MICHAEL GABRIEL JIMENEZNo ratings yet
- BACON B - Bowel EliminationDocument4 pagesBACON B - Bowel EliminationChristian EstevesNo ratings yet
- Hirschsprung'S Disease OR Congenital Aganglionic MegacolonDocument59 pagesHirschsprung'S Disease OR Congenital Aganglionic MegacolonHarshika KDGNo ratings yet
- ConstipationDocument41 pagesConstipationPrajna TiwariNo ratings yet
- Bowel EliminationDocument4 pagesBowel Eliminationdlneisha61100% (3)
- Daud Khan 1045Document31 pagesDaud Khan 1045Iqra BatoolNo ratings yet
- Enema - HANDOUTSDocument4 pagesEnema - HANDOUTSYalc LapidNo ratings yet
- All About Constipation Booklet 2016 05 RevDocument4 pagesAll About Constipation Booklet 2016 05 RevHana Jao100% (1)
- What Is Faecal Incontinence?Document6 pagesWhat Is Faecal Incontinence?drm1238475No ratings yet
- Skill 11 Colostomy CareDocument3 pagesSkill 11 Colostomy CareDiana CalderonNo ratings yet
- New Intestinal ObstructionDocument12 pagesNew Intestinal Obstructionmustafalotfy01No ratings yet
- Bowel Elimination and Type of OstomiesDocument49 pagesBowel Elimination and Type of Ostomiestimeo8124No ratings yet
- Plenary 5B Group 13Document163 pagesPlenary 5B Group 13Obet Agung 天No ratings yet
- Bowel Incontinence ConstipationDocument3 pagesBowel Incontinence ConstipationMatty-b AskalaniNo ratings yet
- TGS KLMK 3 NeDocument20 pagesTGS KLMK 3 NeRini JuandaNo ratings yet
- NCM 116Document19 pagesNCM 116Gail Leslie HernandezNo ratings yet
- Bowel Elimination LectureDocument51 pagesBowel Elimination LectureKimberlae FiguracionNo ratings yet
- Abdominal Assessment 1Document39 pagesAbdominal Assessment 1Kristil ChavezNo ratings yet
- Physiological Changes 114Document2 pagesPhysiological Changes 114Dudil GoatNo ratings yet
- The Coombe Physiotherapy & Your Pelvic Floor Feb 2021Document20 pagesThe Coombe Physiotherapy & Your Pelvic Floor Feb 2021Andreea ManeaNo ratings yet
- Healthy Bowel - Patient Information LeafletDocument8 pagesHealthy Bowel - Patient Information LeafletAlberto VerenzuelaNo ratings yet
- NcpsDocument10 pagesNcpskotoirNo ratings yet
- Bowel EliminationDocument6 pagesBowel EliminationMay Jovi JalaNo ratings yet
- Diarrhea (AGE)Document2 pagesDiarrhea (AGE)NursesLabs.com100% (1)
- NCMB 314 - M2-Cu10Document10 pagesNCMB 314 - M2-Cu10Giselle EstoquiaNo ratings yet
- Bowel Function AnatomyDocument3 pagesBowel Function AnatomyseksNo ratings yet
- Constipation and Bladder and Bowel Control - Oct 2013Document4 pagesConstipation and Bladder and Bowel Control - Oct 2013Dr.Kamlesh BariNo ratings yet
- Elimination - Urinary and BowelDocument58 pagesElimination - Urinary and BowelAnn A.No ratings yet
- Skill: Assessing The AbdomenDocument3 pagesSkill: Assessing The AbdomenDr. Abiola KomolafeNo ratings yet
- 7 AbdomenDocument3 pages7 Abdomenaboosh1699No ratings yet
- 01 EnemaDocument4 pages01 Enemabunso padillaNo ratings yet
- Pemicu 5 GITDocument52 pagesPemicu 5 GITMudita DewiNo ratings yet
- EliminationDocument7 pagesEliminationRoldan Andaya RamosNo ratings yet
- CLUBFOOTDocument19 pagesCLUBFOOTKaryn Joy LamisNo ratings yet
- Irritable Bowel Syndrome (IBS)Document7 pagesIrritable Bowel Syndrome (IBS)Hisyam DinGanuNo ratings yet
- Pelvic Floor Exercises: A Guide For Men AboutDocument3 pagesPelvic Floor Exercises: A Guide For Men AboutemagooNo ratings yet
- Diverticulitis Voice OverDocument10 pagesDiverticulitis Voice Overt passeroNo ratings yet
- Assessment Diagnosis Inference Planning Intervention Rationale EvaluationDocument1 pageAssessment Diagnosis Inference Planning Intervention Rationale EvaluationLoverMind CabaronNo ratings yet
- Digestive System CnaDocument6 pagesDigestive System CnayatanacoNo ratings yet
- Course Topic Cu11 DigestionDocument14 pagesCourse Topic Cu11 DigestionMichelle MallareNo ratings yet
- Alteration in MetabolismDocument26 pagesAlteration in MetabolismAileen MonaresNo ratings yet
- Basic Nursing Fundamentals EliminationDocument35 pagesBasic Nursing Fundamentals Eliminationlisa100% (1)
- Urinary EliminationDocument6 pagesUrinary EliminationryamonamourofficialNo ratings yet
- Bowel EliminationDocument123 pagesBowel EliminationSharon LawrenceNo ratings yet
- Urinary Elimination BY AMNA AZKA BSN NURSINGDocument26 pagesUrinary Elimination BY AMNA AZKA BSN NURSINGmuhammad abdullah javedNo ratings yet
- Fund 2 Updated 2016-1Document578 pagesFund 2 Updated 2016-1abdirahman5570No ratings yet
- Constipation (Sembelit)Document8 pagesConstipation (Sembelit)Eki MegaraniNo ratings yet
- The Happy Bowel: A user-friendly guide to bowel health for the whole familyFrom EverandThe Happy Bowel: A user-friendly guide to bowel health for the whole familyNo ratings yet
- Encopresis, (Fecal Incontinence) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandEncopresis, (Fecal Incontinence) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Respiratory and Circulatory SystemDocument26 pagesRespiratory and Circulatory SystemNasrin BARAKATNo ratings yet
- Pharmacology and TherapyDocument149 pagesPharmacology and Therapydoni anandaNo ratings yet
- Drug CalculationDocument27 pagesDrug CalculationCutay Cristene Mae OrmidoNo ratings yet
- End Stage Renal Disease Case StudyDocument8 pagesEnd Stage Renal Disease Case StudyNikko Dela CruzNo ratings yet
- Aqarqarha A Potent Drug in Unani Medicine A Review On Its Historical and Phyto-Pharmacological Perspective-MinDocument7 pagesAqarqarha A Potent Drug in Unani Medicine A Review On Its Historical and Phyto-Pharmacological Perspective-MinAkhtarAliNo ratings yet
- Inguinal HerniaDocument15 pagesInguinal HerniaTessa LaiNo ratings yet
- Price List Khusus PharosDocument4 pagesPrice List Khusus Pharoshendra.susanto.mailNo ratings yet
- Kidney TransplantDocument73 pagesKidney TransplantwatztanjaNo ratings yet
- "I Can Do All Things Through Christ Who Strengthens Me". Philippians 4:13Document4 pages"I Can Do All Things Through Christ Who Strengthens Me". Philippians 4:13jeanette PradesNo ratings yet
- NIH Fetal Immunology ProposalDocument49 pagesNIH Fetal Immunology ProposalAlexNo ratings yet
- Catherine M. Metra BSN IvDocument18 pagesCatherine M. Metra BSN IvCatherine MetraNo ratings yet
- Pathogenesis of Renal Failure in Multiple Myeloma: Any Role of Contrast Media?Document10 pagesPathogenesis of Renal Failure in Multiple Myeloma: Any Role of Contrast Media?Link BuiNo ratings yet
- Certified Flossband and Sanctband Instructor Course 2016Document4 pagesCertified Flossband and Sanctband Instructor Course 2016Ahmad Safwan SulaimanNo ratings yet
- Veng SangDocument3 pagesVeng SangbawihpuiapaNo ratings yet
- MRC Questionnaire (MRCQ) On Respiratory SymptomsDocument1 pageMRC Questionnaire (MRCQ) On Respiratory SymptomsSalli MarindhaNo ratings yet
- Application of Thermography in Dentistry-A ReviewDocument5 pagesApplication of Thermography in Dentistry-A ReviewCarlos MartinsNo ratings yet
- Therapeutics Handbook 2014 - 140804Document384 pagesTherapeutics Handbook 2014 - 140804Eriet HidayatNo ratings yet
- Report Employee Training IPCDocument11 pagesReport Employee Training IPCDandi RawhideNo ratings yet
- 3M Infection Prevention PDFDocument3 pages3M Infection Prevention PDFBiopharmaNo ratings yet
- List of Secondary Tie-Up Hospitals in 22 Districts of Maharashtra RegionDocument6 pagesList of Secondary Tie-Up Hospitals in 22 Districts of Maharashtra RegionvinaykaambleNo ratings yet
- Cleft Case Chief Complaint Brief History (I) Present IllnessDocument6 pagesCleft Case Chief Complaint Brief History (I) Present IllnessArchanaShenoyNo ratings yet
- 09 TriniasDocument62 pages09 Trinias易行胜No ratings yet
- THE Placeb O Effect: The Science of BeliefDocument41 pagesTHE Placeb O Effect: The Science of BeliefDein DoomNo ratings yet
- 2492-Article Text-5598-1-10-20220909Document6 pages2492-Article Text-5598-1-10-20220909Ayesha HarshaniNo ratings yet
- Combination Therapy in Chronic Periodontitis: A Case ReportDocument5 pagesCombination Therapy in Chronic Periodontitis: A Case ReportNatasya AngelynaNo ratings yet
- Homoeopathy For Sports Exercise and Dance Emlyn Thomas.02996 1contentsDocument13 pagesHomoeopathy For Sports Exercise and Dance Emlyn Thomas.02996 1contentsdipgang7174No ratings yet
- Foundation Concepts 1. Foundation ConceptsDocument30 pagesFoundation Concepts 1. Foundation ConceptsGlenna Joy SolsonaNo ratings yet