Professional Documents
Culture Documents
Guidelines For The Organization and Administration of Universal Newborn Hearing Screening Programs For Out-of-Hospital Births
Guidelines For The Organization and Administration of Universal Newborn Hearing Screening Programs For Out-of-Hospital Births
Uploaded by
Nadzira KarimaOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Guidelines For The Organization and Administration of Universal Newborn Hearing Screening Programs For Out-of-Hospital Births
Guidelines For The Organization and Administration of Universal Newborn Hearing Screening Programs For Out-of-Hospital Births
Uploaded by
Nadzira KarimaCopyright:
Available Formats
— EARLY HEARING DETECTION AND INTERVENTION —
Guidelines for the Organization and Administration
of Universal Newborn Hearing Screening Programs
for Out-of-Hospital Births
Original Publication: June 2008
Last Revision Approved: February 2014
INTRODUCTION
This document is intended to provide recommended
guidelines for newborn hearing screening programs for
midwives delivering newborns in out-of-hospital birth
settings, including home births and non-hospital birth
centers. Until recently, most Minnesota midwives did
not have access to screening equipment and therefore
referred their clients elsewhere for screening. Thanks
to a successful collaboration between the Minnesota
Department of Health (MDH) and the Minnesota Council
of Certified Professional Midwives (MCCPM), many
Minnesota midwives are now trained as screeners and
have access to equipment to screen infants for hearing
loss outside of the hospital.
Because of the importance of early identification of
hearing loss, all screening, follow-up, and tracking
procedures must, at a minimum, be consistent with
national Early Hearing Detection and Intervention
(EHDI) guidelines and current MDH Newborn Screening
Program recommendations. Additional resources are
available from the Newborn Screening Program to assist
midwife practices with specific program development
and management issues, such as training, supervision,
equipment options, and quality assurance.
Newborn Screening Program / (800) 664-7772 1
www.health.state.mn.us/newbornscreening
www.improveehdi.org/mn
Early Hearing Detection and Intervenion
For midwives who do not have access to hearing screening
equipment, Minnesota Statute 144.9661 requires that all
CHILD- AND FAMILY-CENTERED
health professionals attending a birth outside of a hospital
provide both oral and written information to parents
COMMUNICATION
about the importance of hearing screening and where Minnesota statute requires midwives to present
they can have their infant screened. MCCPM members information to parents prior to performing the hearing
trained as hearing screeners also offer newborn hearing screen that covers the following topics:
screening to families who are not clients in their practice.
• Potential risks and effects of hearing loss
BACKGROUND • Benefits of early detection and intervention
The goal of an EHDI program is to promote • Nature of the screening procedure
communication from birth for all children through the
early identification of hearing loss and the initiation of • Applicable costs of screening procedure
appropriate intervention services. Newborn hearing
screening and follow-up plays a critical role in the EHDI • Parental options regarding screening and storage of
process by identifying newborns who are at risk for hearing test results
hearing loss and connecting them with diagnostic,
support, and intervention services. Without EHDI, infants »» Parents who choose to refuse hearing screening
with hearing loss may experience delays in a variety of must complete and sign the Parental Refusal of
developmental areas, including vocabulary, articulation, Newborn Screening2 form. The signed form must
intelligibility, social adjustments, and behavior. be entered into the child’s medical record and
submitted to MDH.
National standards specify that screening should be
complete as soon as possible but at no later than one »» Parents who request that their infant’s newborn
month of age; hearing loss should be clinically diagnosed hearing screening results be destroyed after
as soon as possible but at no later than three months notification must complete and sign the Directive to
of age; and intervention should be initiated as soon as Destroy3 form. The signed form must be submitted
possible but at no later than six months of age. With to MDH. If no destruction request is received,
prompt referral and follow-up, Minnesota children have hearing screening results are kept for 18 years.
the opportunity to receive life-changing care and services
even earlier than national guidelines prescribe. Best practice includes providing the following information
to parents along with the results of their infant’s screen:
Early identification and intervention can substantially
reduce or even eliminate entirely the developmental delays • Prevalence of and risk factors for permanent childhood
that too often stem from a late diagnosis of hearing loss. hearing loss (see Appendix A4)
Studies have shown that if hearing loss is identified before
three months of age and intervention is initiated at no • Possibility of late or progressive onset of hearing loss,
later than six months of age, children perform as much as including otitis media
20 to 40 percent higher on school-related measures than
children with hearing loss that was not identified early. • Developmental milestones for speech, language, and
For many children with hearing loss, early identification hearing (see Appendix B5)
and intervention enables them to perform on language
assessments at the same level as their hearing peers.
PERSONNEL PERFORMING HEARING
SCREENING
Screening may be performed by anyone who has
been properly trained. Hearing screeners benefit from
direct access to audiological consultation in order to
address screening criteria, quality assurance, follow-up
assessment, and intervention services.
2 Newborn Screening Program / (800) 664-7772
www.health.state.mn.us/newbornscreening
www.improveehdi.org/mn
Minnesota Department of Health
Guidelines for the Organization and Administration of Universal Newborn Hearing Screening Programs for Out-of-Hospital Births
Training Qualified Screeners Refresher training should be completed annually, with
Ensuring the skills and competencies of all screeners is individual trainings available as needed. Refresher
critical for screening programs. Training is an ongoing trainings should measure the trainee’s competency using
process and should be based on current best practice the Performance-Based Criterion Checklist6 (see Appendix
procedures as reported in professional literature and C) or a similar performance evaluation tool.
recommended by the Newborn Screening Program.
Training typically includes three phases: initial training and Resources for training may include experienced
demonstration of competency and skills, ongoing quality screeners; local, licensed clinical and educational
assurance, and annual refresher training. audiologists; MDH audiologists; hearing screening
equipment manufacturers; and online resources as
Initial training often involves the use of multiple resources recommended by the Newborn Screening Program. Each
over several days. Initial training and demonstration of midwife may select appropriate staff to carry out the
competency and skills shall include the following, at a hearing screening and related duties.
minimum:
• Completion of orientation, including: HEARING SCREENING EQUIPMENT
• Infection control policies and procedures Screening programs must use objective physiological
screening methods such as automated auditory
• Infant security procedures brainstem response (AABR) or otoacoustic emissions
(OAE). OAE technologies include distortion product
• Cultural sensitivity otoacoustic emissions (DPOAE) and transient evoked
otoacoustic emissions (TEOAE). AABR and OAE do not
• Completion of instructional training for newborn require a behavioral response from the infant and have
hearing screening: proven to be effective screening measures for newborns.
All hearing screening equipment must meet technical
• Benefits of early detection of hearing loss specifications, calibration standards, and safety standards.
A quality screening program benefits from incorporating
• Hearing screening equipment use and care instruction new and improved evidence-based technologies and
procedures as they become available.
• Knowledge of hearing screening policy and procedure
• Documentation of screening results Stimulus Parameters
TOAEs should be measured in response to a click at
• Communicating screening results to the infant’s approximately 80 dB SPL (78-82 dB SPL). DPOAEs should
parent/guardian, infant’s primary care provider, and be measured in response to a series of paired tones (f1
the Newborn Screening Program and f2), with a ratio of 1.22 at a moderate level, where L1/
L2 = 65/55 dB SPL.
• Demonstration of competency and skills to perform
hearing screening should be completed and Newborn screening AABRs typically are evoked using click
documented appropriately: stimuli at 30 to 35 dB nHL at a moderate stimulus rate.
Non-automated ABR screening is NOT recommended for
• Measure the trainee’s competency using the newborn hearing screening programs due to issues of
Performance-Based Criterion Checklist6 (see Appendix C) potential operator error and significant time/cost issues.
or a similar performance evaluation tool.
Default stimulus parameters of both OAE and AABR
Ongoing quality assurance of screeners shall include the equipment should be reviewed by skilled professionals,
following, at a minimum: such as a consulting audiologist or MDH audiologist, to
ensure they are appropriately set or to adjust them to be
• Periodic observations of each screener in accordance with clinically-accepted national practices.
• Review of hearing screening data (e.g., number of
screens and number of REFER results) for each screener
to determine their effectiveness
Newborn Screening Program / (800) 664-7772 3
www.health.state.mn.us/newbornscreening
www.improveehdi.org/mn
Early Hearing Detection and Intervenion
Pass/Refer Criteria
Pass/refer criteria need to be selected and monitored
carefully to maximize sensitivity and specificity. In most
cases, pass/refer criteria is already preset into the hearing
screening equipment by the manufacturer. When hearing
screens are administered, a pass or refer result should
automatically appear. There should be no interpretation of
results by the hearing screener at the time of the screen.
Pass/refer criteria should be reviewed regularly by a
consulting audiologist or MDH audiologist and should be
in accordance with clinically-accepted national practices.
OAE
Typical passing criteria for TOAEs include overall OAE screening equipment measures the sound the cochlea
reproducibility greater than 50 percent, at least 50 low produces in response to external stimuli.
noise samples collected, stimulus stability of 75 percent
or greater, and responses present at least 6 dB above
noise floor for at least three of the five test frequencies,
with 4000 Hz a mandatory passing frequency.
Typical passing criteria for DPOAEs requires absolute
response amplitude of at least –6 dB and responses
at least 6 dB above the noise floor at three or more of
the test frequency bands, with the 4000Hz region a
mandatory passing frequency.
AABR
Typical passing criteria requires repeatable wave
V-evoked responses to clicks at ≤35 dB nHL for each ear,
within specific latency parameters. AABR screening equipment measures the electrical currents
that are generated by the brain when the auditory system is
HEARING SCREENING PROTOCOL excited by stimulus.
to residual birthing debris in the ear canal. Infants who
The following screening protocols have been developed do not pass the initial hearing screen should ideally be
by local experts and are based on nationally-accepted rescreened at the two-week postpartum check or at no
guidelines put forth by the Joint Committee on Infant later than one month of age.
Hearing (JCIH). They have been tailored to fit Minnesota’s
system of care to help ensure that every infant receives The initial hearing screening should consist of no more
quality screening and follow-up throughout the state. than two attempts using the same screening technique
See Appendix D for details about the Hearing Screening on each ear—assuming that the infant is calm and
Result and Follow-up Process7 and Appendix E for a sample quiet and there are neither equipment problems nor
Newborn Hearing Screening Flowchart for Out-of-Hospital environmental interference during either test. The
Births8, which outlines the follow-up process. likelihood of obtaining a passing result by chance alone is
increased when screening is performed repeatedly, which
means a child with a hearing loss may go undetected and
Initial Hearing Screening suffer developmental consequences.
The initial hearing screen is the first screen performed on
a newborn. It is best performed after 12 hours of age but Both ears must pass a single screening to be considered
at no later than three days postpartum. The screen may as an overall passing result. Combining passing results
be performed before 12 hours of age if needed; however, in opposite ears on successive screens does not make a
early screens have a higher REFER (not pass) rate due passing result.
4 Newborn Screening Program / (800) 664-7772
www.health.state.mn.us/newbornscreening
www.improveehdi.org/mn
Minnesota Department of Health
Guidelines for the Organization and Administration of Universal Newborn Hearing Screening Programs for Out-of-Hospital Births
Follow-up/Documentation of Initial Hearing Screening • Rescreen both ears even if only one ear did not pass
Initial hearing screening results should be: the initial hearing screening.
• Documented in the infant’s health record • The rescreen should consist of a maximum of two
attempts on each ear, assuming that the infant is calm
• Communicated to the infant’s parent(s) both verbally and quiet and there are neither equipment problems
and in writing nor environmental interference during either attempt.
• Communicated to the infant’s primary care provider in Follow-up/Documentation of Rescreening
writing when routine well-child care commences
Rescreen hearing results should be:
• Reported to Newborn Screening Program staff within
10 days of the screen. • Documented in the infant’s health record
Minnesota best practice recommends the following: • Communicated to the infant’s parent(s) both verbally
and in writing
• For infants with REFER results on the initial screen, a
follow-up appointment for a hearing rescreening or • Communicated to the infant’s primary care provider in
pediatric audiological evaluation should be scheduled writing within 10 days
for the family as soon as possible. The infant’s primary
care provider (if applicable) and Newborn Screening • Reported to Newborn Screening Program staff within
Program staff should be promptly notified of the date 10 days.
and location of the follow-up rescreen or diagnostic
appointment to help facilitate timely services.
• Families of infants who receive REFER results on the
initial newborn hearing screening should be provided
with information about the importance of follow-up.
Rescreening
For infants with REFER results on the initial screen, at
least one rescreening at a later time or date is necessary
to achieve appropriate referral of infants most at risk
to specialty providers. If the infant does not pass the
initial hearing screening in one or both ears, he or she
should have a rescreen completed ideally at the two
week postpartum check, or at no later than one month
of age. National guidelines recommend allowing one to
two weeks from the time of the initial screen to allow any
transient ear conditions to resolve before rescreening.
Both ears must pass a single screening to be considered
an overall passing result. Combining passing results in
opposite ears on successive screens does not make a
passing result.
Best practice includes the following recommendations for
rescreening:
• Use either AABR or OAE, regardless of which
technology was used for the initial hearing screening.
Note, however, that there is a slight risk of missing
neural hearing loss if an infant is rescreened using OAE
after receiving a refer result using AABR.
Newborn Screening Program / (800) 664-7772 5
www.health.state.mn.us/newbornscreening
www.improveehdi.org/mn
Early Hearing Detection and Intervenion
Minnesota best practice recommends the following: Missed Screen / Equipment Malfunction
• For infants with REFER results on the rescreening, If an equipment malfunction or family circumstance
a diagnostic audiology appointment should be prevents the completion of the initial screen as planned,
scheduled for the family before they leave. The the MDH newborn screening program and the provider
primary care provider and Newborn Screening working with the infant for routine well-child care during
Program staff should be promptly notified of the date the first month of life should be notified in writing that the
and location of the diagnostic audiology appointment hearing screening was missed. The primary provider should
to help facilitate timely services. then assist the family in arranging a time and location for
completing the hearing screen. The screen should take
• Families of infants who receive REFER results on the place as soon as possible but at no later than one month
rescreening should be provided information about post-partum. Alternate screening options include other
the importance of follow-up. Data from newborns midwife practices with training and screening equipment,
screened in Minnesota in recent years shows that audiology clinics, and certain primary care clinics.
infants who do not pass the outpatient rescreen have
a 30 to 50 percent chance of confirmed hearing loss.
Transferred Infants
If an infant is going to be transferred to a hospital, conduct
the newborn hearing screening before transfer, if possible,
and communicate the results to the receiving facility. If
the hearing screen cannot occur before transfer, alert the
Newborn Screening Program of the infant’s transfer and
provide the Hearing Screening Form for Transferred Infants9
(see Appendix F) to the receiving facility. This form alerts
the receiving facility that the infant’s hearing needs to
be screened and requests that they fax the form with
the hearing screening results to the Newborn Screening
Program. Ultimately, the hospital or midwife that sends
the infant home is responsible for screening the infant’s
hearing and reporting the results to the family, the primary
care provider, and the Newborn Screening Program.
Hospital Births
See the MDH Guidelines for the Organization and
Administration of Universal Newborn Hearing Screening
Programs in the Well-Baby Nursery10 and Guidelines for the
Organization and Administration of Universal Newborn
Hearing Screening Programs in the Special Care Nursery and
NICU11 for additional information.
Infants Needing Additional Care
Infants identified as needing additional care during
the first month of life with conditions associated
with potential hearing loss (e.g., hyperbilirubinemia,
meningitis, sepsis) need to have a hearing screen repeated
after recommended care. Because of the high incidence of
neural hearing loss associated with significantly elevated
bilirubin, these infants should be referred for audiological
assessment to include diagnostic ABR measures.
6 Newborn Screening Program / (800) 664-7772
www.health.state.mn.us/newbornscreening
www.improveehdi.org/mn
Minnesota Department of Health
Guidelines for the Organization and Administration of Universal Newborn Hearing Screening Programs for Out-of-Hospital Births
TIMELY CASE MANAGEMENT
The purpose of a hearing screen is to identify infants who
need further testing. It is important to remember that a
hearing screen is not a diagnostic tool.
EHDI is part of a continuum of care that progresses
from parent education, to screening, to assessment, to
amplification (if elected), to educational intervention.
Many professionals—working in different entities and at
different phases of the EHDI process—must work together
and clearly communicate follow-up steps in order to
provide quality care and ensure early diagnosis of hearing
loss. Midwives play a critical role in this process. For
infants who do not pass the newborn hearing screening
and subsequent outpatient rescreening, assessment
referrals must be made to audiologists with expertise in
pediatric physiological and behavioral assessment and
management. See the Minnesota EHDI website12 to locate
providers that offer pediatric diagnostic assessments and
habilitation services in Minnesota.
The nationally recommended timeline for hearing
screening and follow-up is commonly referred to as
the 1-3-6 plan. The timeline includes the following
benchmarks:
• Screening is complete at no later than one month of age
• Diagnostic audiological assessment is complete at no
later than three months of age
• Amplification (if elected) and/or intervention services
are initiated at no later than six months of age
1
With prompt referral and follow-up, Minnesota children
can receive appropriate care and services even earlier
than the nationally recommended timeline. Yet without month: screening complete
3
an adequate follow-up plan, even the best EHDI program
is ineffective. Please refer to the current Guidelines
for Infant Audiologic Assessment13 and Guidelines for
Pediatric Amplification14 for additional information on
months: diagnosis complete
6
recommended best practices.
Follow-up for Middle Ear Effusion
months: intervention
Although persistent middle ear effusion requires medical
services initiated
referral, which may delay the evaluation timeline several
weeks, diagnostic audiological evaluation must not
be postponed solely due to middle ear dysfunction
and should be complete before three months of age.
The information gained from a diagnostic audiological hearing and in identifying whether an underlying
evaluation is valuable both in determining the extent sensorineural hearing loss exists, thereby impacting the
of the effect of the middle ear condition on the infant’s course of both medical and educational intervention.
Newborn Screening Program / (800) 664-7772 7
www.health.state.mn.us/newbornscreening
www.improveehdi.org/mn
Early Hearing Detection and Intervenion
Follow-up for Infants with Positive Risk Factors • Receipt of extracorporeal membrane oxygenation
(JCIH 2007 clarification document) (ECMO) or chemotherapy
The timing and number of hearing re-evaluations for • Caregiver concern or a family history of hearing loss
children with risk factors should be individualized
depending on the relative likelihood of a subsequent
delayed-onset hearing loss. Infants who pass the
neonatal screening—but have a risk factor—should have
QUALITY ASSURANCE/QUALITY
at least one diagnostic audiology assessment by 24 to 30 IMPROVEMENT
months of age. Early and more frequent assessments may
be necessary for children with the following risk factors MDH and its external partners work together to ensure
(see Appendix A for a detailed list): and improve the quality of screening programs across
the state so that every Minnesota infant receives
• Cytomegalovirus (CMV) infection comprehensive screening and follow-up. Midwives
can contribute to quality assurance by monitoring
• Syndromes associated with progressive hearing loss and improving the quality of their own screening
performance.
• Neurodegenerative disorders
The Newborn Screening Program recommends that
• Head trauma midwives establish a quality assurance protocol and be
able to report, on an annual basis, critical performance
• Culture-positive postnatal infections associated with data including, but not limited to, the following:
sensorineural hearing loss
8 Newborn Screening Program / (800) 664-7772
www.health.state.mn.us/newbornscreening
www.improveehdi.org/mn
Minnesota Department of Health
Guidelines for the Organization and Administration of Universal Newborn Hearing Screening Programs for Out-of-Hospital Births
• Total number of live births
• Number of newborns screened
• Number of newborns who passed the hearing
screening
• Number of newborns who did not pass the hearing
screening (results by right ear, left ear and both ears)
• Number of newborns whose parent/guardian refused
newborn hearing screening
• Number of newborns whose parent/guardian did not
refuse screening but who were “missed” (not screened)
• Number of follow-up appointments scheduled for
newborns who did not pass the hearing screen or
were missed
• Total number of newborns transferred to a hospital REFERENCES
• Number of newborns screened who were transferred American Speech-Language-Hearing Association (2004).
to a hospital Guidelines for the Audiologic assessment of children from
birth to 5 years of age. Rockville, MD: ASHA.
• Number of deceased newborns
CDC EHDI National Goals and Objectives, Final Version by
At a minimum, methods should be in place for the EHDI Data Committee, July 13, 2006.
monitoring REFER rates in order to ensure effective
screening and for monitoring parent satisfaction with the Gorga, M.P., Neely, T.S., Ohlrich, B., Hoover, B., Redner, J.
hearing screening process. An effective hearing screening & Peters, J. (1999). From laboratory to clinic: A large scale
program should have a REFER rate of 4 percent or less. study of distortion product otoacoustic emissions in
ears with normal hearing and ears with hearing. Ear and
The overall goal of quality assurance is information Hearing, 18, 440-455.
management and accountability to the following
stakeholders: Hall, J.W., Smith, S.D., & Popelka, G.R. (2004). Newborn
hearing screening with combined otoacoustic emissions
• Infants and their families and auditory brainstem responses. Journal of the
• Advocates American Academy of Audiology, 15, 414-425.
• Clinical and educational audiologists HRSA, Final Report. Evaluation of Universal Newborn
Hearing Screening and Intervention Program. Based on
• EHDI managers 2005 – 2006 Data.
• Hospitals Joint Committee on Infant Hearing Position Statement
(2007), Year 2007 position statement: Principles and
• Medical and educational specialists guidelines for early hearing detection and intervention.
Pediatrics, 120, 898-921.
• Otolaryngologists
• Primary care providers Joint Committee on Infant Hearing Position Statement
(2007) Update. Clarification for Year 2007 JCIH Position
• Screeners Statement. Retrieved May 2008, from www.jcih.org/
Clarification%20Year%202007%20statement.pdf.
• State of Minnesota
Newborn Screening Program / (800) 664-7772 9
www.health.state.mn.us/newbornscreening
www.improveehdi.org/mn
Early Hearing Detection and Intervenion
Minnesota Statute 144.966. Early Hearing Detection and 7
Appendix D: Hearing Screening Result and Follow-up
Intervention Program. 2007. Retrieved from www.leg. Process
state.mn.us/leg/statutes. http://www.improveehdi.org/wi/library/files/Hearing%20
Screening%20Result%20and%20Follow-up%20Process.pdf
National Consortium for Newborn Hearing Screening.
(Nov 16-18, 1995). TEOAE-based universal newborn hearing 8
Appendix E: Newborn Hearing Screening Flowchart for
screening. Georgetown University School of Medicine, the Out-of-Hospital Births
Washington DC. http://www.improveehdi.org/mn/library/files/Out-of-
Hospital%20Birth%20Flowchart%20with%20Myths.pdf
Norton, S., Gorga, M., Widen, J., Folsom, R., Sininger,
Y., Cone-Wesson, B., Vohr, B., & Fletcher, K. (2000). 9
Appendix F: Hearing Screening Form for Transferred
Identification of neonatal hearing impairment: A Infants
multicenter investigation. Ear and Hearing, 21 (5), 348-356. http://www.health.state.mn.us/newbornscreening/docs/
nicutransf.pdf
Ontario Health and Long-Term Care Ministry—Infant
Hearing Program (2002). Universal infant hearing screening 10
Guidelines for the Organization and Administration of
assessment and communication development: Local Universal Newborn Hearing Screening Programs in the
implementation support document. Well-Baby Nursery
http://www.improveehdi.org/mn/library/files/
Washington State Department of Health Protocol for wbnguidelines.pdf
Newborn Hearing Screening. Retrieved February 18, 2014,
from http://www.doh.wa.gov/Portals/1/Documents/ 11
Guidelines for the Organization and Administration of
Pubs/344-023_EHDDINBScrnProto.pdf Universal Newborn Hearing Screening Programs in the
Special Care Nursery and NICU
SELECTED LINKS http://www.health.state.mn.us/newbornscreening/docs/
nicu_hear-guidelines.pdf
1
Minnesota Statute 144.966 12
EHDI Website Provider Search
https://www.revisor.mn.gov/statutes/?id=144.966 http://www.improveehdi.org/mn/providers.cfm
2
Parental Refusal of Newborn Screening form 13
Guidelines for Infant Audiologic Assessment
http://www.health.state.mn.us/newbornscreening/docs/ http://www.improveehdi.org/wi/library/files/MDH%20
parental_refusal.pdf Audiologic%20Assessment%20Guidelines%281%29.pdf
3
Directive to Destroy Newborn Hearing Screening Test 14
Guidelines for Pediatric Amplification
Results form http://www.improveehdi.org/wi/library/files/MDH%20
http://www.health.state.mn.us/newbornscreening/docs/ Pediatric%20Amplification%20Guidelines.pdf
hearingdestruction.pdf
4
Appendix A: Risk Factors Associated with Permanent
Congenital, Delayed-onset, or Progressive Hearing Loss in
Childhood
http://www.improveehdi.org/wi/library/files/Risk%20
Indicators%20from%20JCIH%202007%20Position%20
Statement.pdf
5
Appendix B: Hearing and Speech Milestones
http://www.improveehdi.org/wi/library/files/Hearing%20
and%20Speech%20Milestones%20from%20AAP%20
and%20AAA.pdf
6
Appendix C: Performance Based Criterion Checklist
http://www.improveehdi.org/wi/library/files/
Competency%20Checklist.pdf
10 Newborn Screening Program / (800) 664-7772
www.health.state.mn.us/newbornscreening
www.improveehdi.org/mn
You might also like
- Nursing Care Plan ON: Caesarean DeliveryDocument22 pagesNursing Care Plan ON: Caesarean DeliveryKavi rajput79% (14)
- WB N GuidelinesDocument10 pagesWB N GuidelinesNadzira KarimaNo ratings yet
- Outsourcing Hospital-Based Newborn Hearing Screening: Key Questions and ConsiderationsDocument5 pagesOutsourcing Hospital-Based Newborn Hearing Screening: Key Questions and ConsiderationsJanMichaelNebrejaNo ratings yet
- Guidelines For Newborn Hearing Screening and EvaluationDocument2 pagesGuidelines For Newborn Hearing Screening and EvaluationAileen A. MonaresNo ratings yet
- Newborn and Infant Hearing Loss: Detection and InterventionDocument6 pagesNewborn and Infant Hearing Loss: Detection and InterventionFabiola Andrea Contreras AburtoNo ratings yet
- Diagnostic Referral From Universal Newborn Hearing ScreeningDocument13 pagesDiagnostic Referral From Universal Newborn Hearing Screeningdr.ib979No ratings yet
- Newborn Hearing Screening GuidelinesDocument36 pagesNewborn Hearing Screening GuidelinesAhmed HilalNo ratings yet
- Assessment of Hearing Loss in ChildrenDocument25 pagesAssessment of Hearing Loss in ChildrenCristóbal Murillo MuñozNo ratings yet
- Part C EligibilityDocument6 pagesPart C Eligibilityapi-260192872No ratings yet
- 2 Chapter2NewbornHearing2018Document14 pages2 Chapter2NewbornHearing2018Davien UtoyoNo ratings yet
- National Periodic Health GuidelinesDocument72 pagesNational Periodic Health GuidelinesFcm-srAaf100% (1)
- JCIHwebFinal PDFDocument36 pagesJCIHwebFinal PDFNadzira KarimaNo ratings yet
- Unit 5 Developmental AssessmentDocument36 pagesUnit 5 Developmental AssessmentManja125No ratings yet
- Follow Up High Risk NBDocument36 pagesFollow Up High Risk NBinggrit anggrainiNo ratings yet
- New Born ScreeningDocument6 pagesNew Born ScreeningissaiahnicolleNo ratings yet
- Arcadio - Newborn ScreeningDocument63 pagesArcadio - Newborn ScreeningkoalaNo ratings yet
- Smith Nielsen, J.a Implementation of the Alarm Distress Baby Scale as a Universal Screening Instrument in Primary Care Feasibility Acceptability and Predictors of Professionals Adherence to GuidelinesArticle 2018Document10 pagesSmith Nielsen, J.a Implementation of the Alarm Distress Baby Scale as a Universal Screening Instrument in Primary Care Feasibility Acceptability and Predictors of Professionals Adherence to GuidelinesArticle 2018Lady HeruNo ratings yet
- Patient'S Perception Regarding Audiovisual Oral Health Promotion Aids at Pacific Dental College & Hospital - A Cross Sectional Questionnaire SurveyDocument5 pagesPatient'S Perception Regarding Audiovisual Oral Health Promotion Aids at Pacific Dental College & Hospital - A Cross Sectional Questionnaire Surveysagrika groverNo ratings yet
- A Performance Evaluation and Assessment Scheme (PEAS) For Improving The Philippine Newborn Screening ProgramDocument6 pagesA Performance Evaluation and Assessment Scheme (PEAS) For Improving The Philippine Newborn Screening Programhulya castiNo ratings yet
- Newborn ScreeningDocument18 pagesNewborn ScreeningKayNo ratings yet
- School Age Hearing Screening DMIMSUDocument11 pagesSchool Age Hearing Screening DMIMSUSharnie JoNo ratings yet
- National Periodic Health GuidelinesDocument72 pagesNational Periodic Health Guidelinesasma .sassiNo ratings yet
- TR - AABR and OAE Devices in Universal Newborn Hearing ScreeningDocument62 pagesTR - AABR and OAE Devices in Universal Newborn Hearing Screeningmohd roziNo ratings yet
- 2023 Clinic Budget Annex ADocument52 pages2023 Clinic Budget Annex AJuls Maquiling Vistal Millorin100% (1)
- NBS Law FinalDocument33 pagesNBS Law Finalkissiah Cajetas100% (1)
- VIT - Apollo Shine Health CentreDocument4 pagesVIT - Apollo Shine Health CentreAmal ThomasNo ratings yet
- Domains Slide Pack QI Patient Safety Final v2Document36 pagesDomains Slide Pack QI Patient Safety Final v2Joel John Dela MercedNo ratings yet
- WK 13 Family Health Care ProgramsDocument29 pagesWK 13 Family Health Care ProgramsJhaze Allestain PalleraNo ratings yet
- Routine Exam NewbornDocument18 pagesRoutine Exam NewbornKumar Gavali SuryanarayanaNo ratings yet
- Evidence Based Practice Fact SheetDocument3 pagesEvidence Based Practice Fact SheetTuhin DeyNo ratings yet
- BSC in Neonatal NursingDocument14 pagesBSC in Neonatal NursingsmsmdsdsffNo ratings yet
- Newborn Screening Expands: Recommendations For Pediatricians and Medical Homes-Implications For The SystemDocument26 pagesNewborn Screening Expands: Recommendations For Pediatricians and Medical Homes-Implications For The SystemRichard Marl AbbugaoNo ratings yet
- 12 .Data Collection Family Planning SGDDocument32 pages12 .Data Collection Family Planning SGDSadia YousafNo ratings yet
- Family Planning Lesson PlanDocument23 pagesFamily Planning Lesson PlanIvan Bautista Cortez73% (15)
- Selecting Developmental Surveillance and Screening ToolsDocument7 pagesSelecting Developmental Surveillance and Screening ToolsGerald Howard UntarioNo ratings yet
- Guidelines SHP 29th Jan 09-Final FinalDocument3 pagesGuidelines SHP 29th Jan 09-Final Finaldr parveen bathlaNo ratings yet
- Key Points For Considering Adoption of The Who Labour Care Guide: Policy BriefDocument12 pagesKey Points For Considering Adoption of The Who Labour Care Guide: Policy BriefYuli AstutiNo ratings yet
- Health Care Delivery SystemDocument32 pagesHealth Care Delivery SystemBhawna Joshi100% (1)
- 2 Mod Issue Brief Finalupdatedlogo Policy Oct2017 SMDocument2 pages2 Mod Issue Brief Finalupdatedlogo Policy Oct2017 SMJohnryl FranciscoNo ratings yet
- Hearing Factsheet 508Document2 pagesHearing Factsheet 508Ibrahim DahiruNo ratings yet
- Health-Care Reform in Georgia: Irakli TortladzeDocument26 pagesHealth-Care Reform in Georgia: Irakli TortladzeShubham TanwarNo ratings yet
- NQB Hum Fact ConcordDocument22 pagesNQB Hum Fact ConcordSophia RoseNo ratings yet
- Otoscopy and Audiometry PresentationDocument15 pagesOtoscopy and Audiometry PresentationLuka MitarNo ratings yet
- 2007 Jcih PDFDocument42 pages2007 Jcih PDFDeniNo ratings yet
- 2018 IJRPS Fat4cpDocument8 pages2018 IJRPS Fat4cpdvckpjuNo ratings yet
- Guideline Hearing Aid FittingDocument80 pagesGuideline Hearing Aid FittingPhillip Martinez50% (2)
- Newborn Screening Chapters 1 and 2 Partially 3iiiDocument31 pagesNewborn Screening Chapters 1 and 2 Partially 3iiikimchi girlNo ratings yet
- WHOEarlydiagnostictestingforHIV Ver Final May07Document11 pagesWHOEarlydiagnostictestingforHIV Ver Final May07noorainiahmadNo ratings yet
- Nsungwa-Sabiiti: UgandaDocument26 pagesNsungwa-Sabiiti: UgandaNewborn2013No ratings yet
- Cyprien Nioble, Jhpiego-Cote Divoire, IAS2012 Poster, MNH Quality ImprovementDocument1 pageCyprien Nioble, Jhpiego-Cote Divoire, IAS2012 Poster, MNH Quality ImprovementJhpiegoNo ratings yet
- AAPD Teledentistry 2021Document2 pagesAAPD Teledentistry 2021Francisca Abarca CifuentesNo ratings yet
- Introduction To Newborn ScreeningDocument28 pagesIntroduction To Newborn ScreeningfuufNo ratings yet
- Patient Safety 6.Document40 pagesPatient Safety 6.salah salemNo ratings yet
- G Periodicity PDFDocument8 pagesG Periodicity PDFTry SidabutarNo ratings yet
- Newborn ScreeningDocument10 pagesNewborn ScreeningAnanya SampathNo ratings yet
- WHO Safe Childbirth Checklist PDFDocument9 pagesWHO Safe Childbirth Checklist PDFParth VasaveNo ratings yet
- Review ArticleDocument22 pagesReview ArticleJasjit BhasinNo ratings yet
- Standard For AssessingDocument24 pagesStandard For AssessingKartini MedikalNo ratings yet
- Standards For Improving The Quality of Care For Small and Sick Newborns in Health Facilities 2020Document152 pagesStandards For Improving The Quality of Care For Small and Sick Newborns in Health Facilities 2020Shuaib KauchaliNo ratings yet
- Med Bio Iw TanayaDocument13 pagesMed Bio Iw Tanayahimeshjain466No ratings yet
- JCIHwebFinal PDFDocument36 pagesJCIHwebFinal PDFNadzira KarimaNo ratings yet
- Statement of Endorsement May 2013Document42 pagesStatement of Endorsement May 2013Nadzira KarimaNo ratings yet
- Eradikasi Polio Dan Ipv (Inactivated Polio Vaccine) : ArtikelDocument10 pagesEradikasi Polio Dan Ipv (Inactivated Polio Vaccine) : ArtikelNadzira KarimaNo ratings yet
- Drooling in Parkinson's DiseaseDocument10 pagesDrooling in Parkinson's DiseaseNadzira KarimaNo ratings yet
- Otoacoustic Emissions, Their Origin in Cochlear Function, and UseDocument19 pagesOtoacoustic Emissions, Their Origin in Cochlear Function, and UseNadzira KarimaNo ratings yet
- Diabetic FootDocument68 pagesDiabetic FootNadzira KarimaNo ratings yet
- Laparoscopic Compared With Robotic Sacrocolpopexy For Vaginal Prolapse: A Randomized Controlled TrialDocument13 pagesLaparoscopic Compared With Robotic Sacrocolpopexy For Vaginal Prolapse: A Randomized Controlled TrialNadzira KarimaNo ratings yet
- Sleep DeficiencyDocument7 pagesSleep DeficiencyNadzira KarimaNo ratings yet
- This Article: Natural Gene Therapy in Dystrophic Epidermolysis BullosaDocument10 pagesThis Article: Natural Gene Therapy in Dystrophic Epidermolysis BullosaNadzira KarimaNo ratings yet
- 5 Star DoctorDocument25 pages5 Star DoctorNadzira KarimaNo ratings yet
- WB N GuidelinesDocument10 pagesWB N GuidelinesNadzira KarimaNo ratings yet
- 5 Star DoctorDocument25 pages5 Star DoctorNadzira KarimaNo ratings yet
- Kreatin 1Document108 pagesKreatin 1Nadzira KarimaNo ratings yet
- Preoperative Anesthesia and PremedicationDocument25 pagesPreoperative Anesthesia and Premedicationnadya fachfudyanaNo ratings yet
- Acute Uterine InversionDocument9 pagesAcute Uterine Inversionvictor onapaNo ratings yet
- Ankle and FootDocument10 pagesAnkle and FootGlea PavillarNo ratings yet
- Nur 195 Long Exam P2 Rle 1 - 1Document21 pagesNur 195 Long Exam P2 Rle 1 - 1Marga WreatheNo ratings yet
- Nursing Malpractice: Cause For ConsiderationDocument3 pagesNursing Malpractice: Cause For ConsiderationleewfNo ratings yet
- Medicine For Womwn in Ancient ChinaDocument220 pagesMedicine For Womwn in Ancient Chinarazvan rotaru83% (6)
- PIIS0022347615008574Document1 pagePIIS0022347615008574Adnan WalidNo ratings yet
- What Is AmenorrheaDocument5 pagesWhat Is AmenorrheaYhoyho Akhilun Dewa MimpiNo ratings yet
- HX Taking of PeadiatricsDocument5 pagesHX Taking of PeadiatricsCahaya Al-Hazeenillah100% (2)
- Rapid Sequence Spinal AnesthesiaDocument6 pagesRapid Sequence Spinal AnesthesiaZaida RamosNo ratings yet
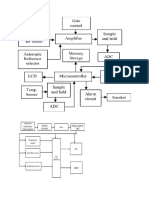
- Block Diagram PT MonitorDocument7 pagesBlock Diagram PT MonitorAbabil Academy KannanNo ratings yet
- MacKenzie - What Would A Good Doctor Do? Re Ections On The Ethics of MedicineDocument4 pagesMacKenzie - What Would A Good Doctor Do? Re Ections On The Ethics of MedicineCecitorNo ratings yet
- Society For Pediatric Anesthesia Emergency Checklist ManualDocument28 pagesSociety For Pediatric Anesthesia Emergency Checklist ManualJill SweetNo ratings yet
- Feu83 The Stars Are BackDocument142 pagesFeu83 The Stars Are Backralphdaniel100% (3)
- Anatomy MCQs (Thorax)Document2 pagesAnatomy MCQs (Thorax)Adil Shabbir100% (3)
- Hospital in Whitefield, BangaloreDocument6 pagesHospital in Whitefield, BangaloreColumbia Asia Hospitals in IndiaNo ratings yet
- CTU Insulin Sliding ScalesDocument2 pagesCTU Insulin Sliding ScalesnindylistyNo ratings yet
- Complete Septate Uterus in PregnancyDocument6 pagesComplete Septate Uterus in PregnancyfitriamarizkaNo ratings yet
- TMJ Development PDFDocument10 pagesTMJ Development PDFVidya SenthuNo ratings yet
- FL Caid CMS Provider Directory Reg 5 1 Eng Spa 4 2020Document684 pagesFL Caid CMS Provider Directory Reg 5 1 Eng Spa 4 2020Kriti KumariNo ratings yet
- OpenERP Modul MedicalDocument33 pagesOpenERP Modul MedicalhendrigantingNo ratings yet
- Hemodynamics MonitoringDocument12 pagesHemodynamics MonitoringBhawna Joshi100% (3)
- Holy Family College of Nursing B.Sc. Nursing Interns Viii Semester Clinical Rotation PlanDocument2 pagesHoly Family College of Nursing B.Sc. Nursing Interns Viii Semester Clinical Rotation PlanManisha ThakurNo ratings yet
- TS Circ025-2015Document11 pagesTS Circ025-2015zaldusalvaradoNo ratings yet
- Medical School Notes: LabourDocument5 pagesMedical School Notes: LabourKatherine NunnNo ratings yet
- Gagan ResumeDocument6 pagesGagan Resumedrgaganwahi100% (2)
- Focused Abdominal Sonography in Trauma (FAST)Document56 pagesFocused Abdominal Sonography in Trauma (FAST)RannyNo ratings yet
- Benign Gynecologic TumorsDocument57 pagesBenign Gynecologic TumorsDexter IanNo ratings yet
- 2015 - Alimi - Xerostomia Induced by RadiotherapyDocument4 pages2015 - Alimi - Xerostomia Induced by RadiotherapyNélio Silva de SouzaNo ratings yet