Professional Documents
Culture Documents
Management of Upper Gastrointestinal Bleeding by An Internist
Management of Upper Gastrointestinal Bleeding by An Internist
Uploaded by
DewiOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Management of Upper Gastrointestinal Bleeding by An Internist
Management of Upper Gastrointestinal Bleeding by An Internist
Uploaded by
DewiCopyright:
Available Formats
Open Access Review
Article DOI: 10.7759/cureus.2878
Management of Upper Gastrointestinal
Bleeding by an Internist
Saad Saleem 1 , Abell L. Thomas 2
1. Internal Medicine, Mercy St. Vincent Medical Center, Toledo, USA 2. Gastroenterology, University of
Louisville , louisville, USA
Corresponding author: Saad Saleem, saadsaleem29@gmail.com
Disclosures can be found in Additional Information at the end of the article
Abstract
Nonvariceal upper gastrointestinal bleeding (UGIB) carries high morbidity and mortality, which
can be lowered by timely evaluation and management. This article presents a comprehensive
literature review and current guidelines for the management of nonvariceal UGIB by an
internist. Pre-endoscopic management includes optimal resuscitation, and making a decision
about holding the anticoagulation and antiplatelet therapy versus continuation due to risk of
thrombosis. Proton pump inhibitors (PPIs) are beneficial for both ulcer and nonulcer diseases as
they reduce the risk of re-bleeding by clot stabilization. Endoscopy should only be performed
after hemodynamic stability has been achieved and should not be delayed by more than 24
hours. Resumption of anticoagulation and antiplatelet therapy is based on endoscopic findings
and thromboembolic risk. The patient should be discharged on PPIs and should be followed up
by a primary care physician.
Categories: Family/General Practice, Internal Medicine, Gastroenterology
Keywords: upper gi, gastrointestinal bleed, internist
Introduction And Background
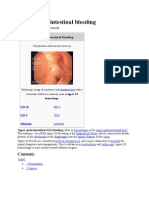
Upper gastrointestinal bleeding (UGIB) is defined as a clinically significant bleeding (no fixed
amount of blood) from the gastrointestinal (GI) tract above the ligament of Treitz (anatomical
landmark between the duodenum and jejunum) which includes the esophagus, stomach, and
duodenum. The patient usually shows signs of bleeding in the GI tract either as hematemesis
(vomiting of bright red blood or coffee ground emesis) or melena (black tarry stools). The
majority of melena (black, tarry stool) originates proximal to the ligament of Treitz (90%),
though it may as well arise from the oropharynx or nasopharynx, small bowel, or right colon [1].
Melena may be seen in varying stages of blood loss, with as little as 50 ml of blood [2].
Received 05/18/2018
Review began 05/27/2018 Hematemesis (vomiting of bright red blood) is suggestive of moderate to severe bleeding,
Review ended 06/16/2018 whereas coffee ground emesis (oxidation of the heme molecule of red blood cells due to gastric
Published 06/25/2018 acid) suggests more limited bleeding. The yearly incidence of hospitalization for acute UGIB is
© Copyright 2018 about 100 per 100,000 people [3]. The UGIB rate of admission to the hospital is six times higher
Saleem et al. This is an open access as compared to lower GI bleeding [3].
article distributed under the terms of
the Creative Commons Attribution
License CC-BY 3.0., which permits
Although the diagnosis and management of nonvariceal UGIB has improved over time, it still
unrestricted use, distribution, and results in 400,000 hospital admissions per year, costing more than two billion dollars per
reproduction in any medium, year [4]. Despite advances in therapy, hospital mortality resulting from UGIB remains high,
provided the original author and which can be lowered by proper evaluation and management. The reported frequencies of
source are credited.
specific causes have changed over time. Peptic ulcer disease constitutes roughly 20%-25% of
How to cite this article
Saleem S, Thomas A L (June 25, 2018) Management of Upper Gastrointestinal Bleeding by an Internist.
Cureus 10(6): e2878. DOI 10.7759/cureus.2878
cases as compared to older studies when it used to constitute half of UGIB [5-7]. The most
common causes of UGIB include the following (in approximate descending order of
frequency) [5-6, 8-10]: gastric and/or duodenal ulcers, esophagogastric varices, severe or
erosive esophagitis, severe or erosive gastritis/duodenitis, portal hypertensive gastropathy,
angiodysplasia (also known as vascular ectasia), mass lesions (polyps/cancers), Mallory-Weiss
syndrome, and no lesion identified (10%-15% of patients).
The source of bleeding cannot be recognized in 10%-15% of patients with UGIB; either the
lesion is hard to identify (such as a Dieulafoy's lesion), obscured by a retained blood clot at
endoscopy, or the lesion has already healed by the time endoscopy was performed. The four
major risk factors for bleeding peptic ulcers are [11-12]: Helicobacter pylori (H. pylori) infection,
use of nonsteroidal anti-inflammatory drugs (NSAIDs), physiologic stress, and excess gastric
acid.
Review
Pre-endoscopy management
Patients are triaged based on hemodynamic status, age, comorbidities, and initial lab results.
The first and foremost step in the management of UGIB is assessing the hemodynamic status
and starting a resuscitative measure. In acute UGIB, hemoglobin is not a good indicator for
estimating GI blood loss. The patient should receive intravenous (IV) isotonic fluids, and
transfusion should be given maintaining the hemoglobin at a level ≥7 g/dl (70 g/l) or above if
the patient is symptomatic [13].
Risk assessment regarding further GI bleeding and mortality will determine decisions regarding
level of care, timing of endoscopy, and discharge planning. Main scores are the Blatchford
score, Rockall score, and AIMS65. These scores are used to identify patients with UGIB who
need to be admitted to the hospital, as the bleeding requires further medical intervention such
as a blood transfusion or an endoscopic intervention. The Blatchford score as compared to the
Rockall score does not take endoscopic findings into account, so it can be calculated after the
patient comes to the emergency room. This score is based upon the blood urea nitrogen,
hemoglobin, systolic blood pressure, pulse and presence of melena, syncope, hepatic disease,
and/or cardiac failure. The score ranges from 0 to 23, and the chances of requiring an
endoscopic intervention increases with a higher score. Meta-analysis has shown that a score of
0 was associated with a low likelihood of needing an endoscopic intervention [14].
The AIMS65 studies have suggested that it has a high accuracy for predicting inpatient
mortality among patients with UGIB. It was derived from a database of 187 US hospitals [15].
Studies have shown that an increasing score is associated with higher mortality and a
prolonged stay in the hospital. The study found that five factors were associated with increased
inpatient mortality [15]: albumin less than 3.0 g/dl (30 g/l), international normalized ratio (INR)
greater than 1.5, altered mental status, systolic blood pressure of 90 mmHg or less, and age
older than 65 years.
Anticoagulation and antiplatelet therapy should be performed for patients with UGIB. However,
the risk of thrombosis should be weighed against the risk of bleeding. Anticoagulation should
be reversed in case of acute hemorrhage. If a patient taking warfarin and INR is
supratherapeutic, fresh frozen plasma (FFP) or prothrombin complex concentrate should be
given. There is no antidote for most of the newer anticoagulation agents, but they have a short
half-life in the presence of normal kidney function. These medications should be held and
bleeding will likely stop in the next 12-24 hours [16]. A small study (conducted in 1994) that
included 52 patients showed successful hemostasis after endoscopic therapy in 91% of patients
after correcting the INR to 1.5-2.5 compared to the control population who were not
2018 Saleem et al. Cureus 10(6): e2878. DOI 10.7759/cureus.2878 2 of 8
anticoagulated [17].
Proton pump inhibitors (PPIs) should be started in patients admitted with UGIB until the source
of bleeding is identified. It is beneficial in both ulcer and nonulcer diseases. A high-dose
intravenous infusion of PPI reduces the risk of re-bleeding ulcers [18]. It promotes hemostasis
by neutralizing gastric acid, which leads to clot stabilization [19]. Gastroenterology service
should be involved in all the patients with significant UGIB. There is data supporting the use of
IV erythromycin before endoscopy. It improves visualization of the stomach by moving the
blood and food particles from the stomach [20], thereby increasing the chances of visualizing
the bleeding vessel. It reduces the need for a second-look endoscopy.
The patient’s discharge to home directly from the emergency room (ER) without inpatient
endoscopy may be considered if urea nitrogen < 18.2 mg/dl, hemoglobin greater than or equal
to 13 g/dl for men and 12 mg/dl for women, systolic blood pressure greater than or equal to 110
mmHg, pulse < 100/min, absence of melena, syncope, cardiac failure, and liver disease as they
have less than one percent chance of requiring intervention [13]
Upper endoscopy
Endoscopy should be performed in a nonemergent setting. Patients should be
hemodynamically stabilized and should undergo an endoscopy within 24 hours of
admission [13]. If the patient is hemodynamically stable on admission and does not have
serious comorbidities, an endoscopy should be performed as soon as possible [13]. Patients with
endoscopic findings of high-risk stigmata (Table 1) (active bleeding, visible vessel, clots) should
be hospitalized for three days assuming no further episode of bleeding occurs. They can be fed
with clear liquids soon after endoscopy [13]. Clear liquids provide the advantage that if the
patient starts to bleed again, sedation and anesthesia can be given within two hours after the
last ingestion [21]. Patients with clean-based ulcers can be discharged home if they have a
residence and someone can observe them [13].
Endoscopic stigmata of recent hemorrhage Prevalence (%) Risk of re-bleeding on medical management (%)
Active arterial bleeding (Forrest Ia) 10 90
Oozing without visible vessel (Forrest Ib) 10 10-20
Non-bleeding visible vessel (Forrest IIa) 25 50
Adherent clot (Forrest IIb) 10 25-30
Flat spot (Forrest IIc) 10 7-10
Clean ulcer base (Forrest (III) 35 3-5
TABLE 1: Endoscopic predictors of recurrent peptic ulcer hemorrhage
[22]
The risk of bleeding due to endoscopic procedures is classified as low (diagnostic procedures) or
high (therapeutic procedures) (Table 2). For high-risk procedures and low thromboembolic risk,
the recommended duration for discontinuing the agent before the procedure is as follows: five
2018 Saleem et al. Cureus 10(6): e2878. DOI 10.7759/cureus.2878 3 of 8
days (clopidogrel), three to five days (ticagrelor), seven days (prasugrel), or 10-14 days
(ticlopidine) [23-25]. Stopping P2Y12 platelet receptor blockers should also be considered in
patients at high risk for thromboembolic complications who are undergoing high-risk
procedures, if the risk of bleeding is thought to outweigh the risk of thromboembolism. Aspirin
need not be discontinued. A cardiologist or a neurologist should be consulted based on the
indication of the antiplatelet therapy.
Higher-risk procedures
Polypectomy
Biliary or pancreatic sphincterotomy
Treatment of varices
PEG placement
Therapeutic balloon-assisted enteroscopy
EUS with FNA
Endoscopic hemostasis
Tumor ablation
Cystogastrostomy
Ampullary resection
EMR
Endoscopic submucosal dissection
Pneumatic or bougie dilation
PEJ
Low-risk procedures
Diagnostic (EGD, colonoscopy, flexible sigmoidoscopy) including mucosal biopsy
ERCP with stent (biliary or pancreatic) placement or papillary balloon dilation without sphincterotomy
Push enteroscopy and diagnostic balloon-assisted enteroscopy
Capsule endoscopy
Enteral stent deployment (controversial)
EUS without FNA
Argon plasma coagulation
Barrett's ablation
TABLE 2: The management of antithrombotic agents for patients undergoing
gastrointestinal endoscopy
2018 Saleem et al. Cureus 10(6): e2878. DOI 10.7759/cureus.2878 4 of 8
Abbreviations: EGD, esophagogastroduodenoscopy; ERCP, endoscopic retrograde cholangiopancreatography; PEG,
percutaneous endoscopic gastrostomy; EUS, endoscopic ultrasound; FNA, fine-needle aspiration; EMR, endoscopic mucosal
resection; PEJ, percutaneous endoscopic jejunostomy [26]
The American Society of Gastrointestinal Endoscopy (ASGE) guidelines recommend avoiding
elective procedures on cardiac stents patients until they has received antithrombotic therapy
for the minimum recommended duration based upon the current guidelines [26]. Once beyond
that period, depending on the type of stent used, P2Y12 platelet receptor blockers are
discontinued 5-14 days prior to the procedure, while continuing aspirin. The guidelines
recommend that patients who are within six weeks of bare-metal stent placement or within six
months of drug-eluting stent placement have surgical procedures deferred, if possible, until
this period [26]. After the procedure, the P2Y12 platelet receptor blocker should be restarted,
with or without a loading dose, as soon as it is considered safe, depending on the patient's
indication for taking it and any intervention performed during the endoscopy that may increase
the risk for bleeding (such as removal of a large polyp) [27].
Post-endoscopy
Data are limited about resumption of anticoagulation after achieving endoscopic hemostasis,
but studies have shown that resuming anticoagulation has better outcomes than not resuming.
Unfractioned heparin is preferred for bridge therapy due to a shorter half-life of 1.5 hours [26].
After endoscopy, the patient should be followed up for the results of H. pylori. Patients with H.
pylori associated bleeding ulcers should receive H. pylori therapy. Once the eradication is
documented, they do not require long-term antisecretory therapy [13]. A patient who develops
NSAID-associated ulcers should be carefully assessed. If needed to be resumed, the lowest dose
cyclooxygenase-2 (COX-2) selective NSAID with daily PPI is recommended [13]. If the patient
develops low-dose aspirin-induced ulcers, aspirin has to be stopped if given for primary
prevention of cardiovascular disease. It can be continued if given for secondary prevention of
cardiovascular diseases with long-term use of PPI. Aspirin can be resumed between three and
seven days after UGIB [13]. The PPI should be continued in the long term if the gastric ulcer is
idiopathic. Aspirin and other NSAIDS given alone in standard doses do not increase the risk of
bleeding after an upper endoscopy with biopsy or biliary sphincterotomy [28-31].The data are
conflicting about whether aspirin or/and NSAIDS increase the risk of bleeding
postpolypectomy.
The 2010 International Consensus Recommendations do not recommend routine use of a
second-look endoscopy for nonvariceal UGIB [32]. The guidelines suggest that patients at a
particularly high risk for recurrent bleeding may benefit from a second-look endoscopy; these
patients include those whose first endoscopy was limited or if the first endoscopic therapy was
suboptimal.
A physician should monitor the patients for the following which may suggest re-bleeding [33]:
hematemesis more than six hours after the initial endoscopy, melena after normalization of
stool color, hematochezia after normalization of stool color, development of tachycardia (heart
rate ≥110 beats per minute) or hypotension (systolic blood pressure ≤90 mmHg) after one hour
of hemodynamic stability in the absence of other possible alternatives, hemoglobin drop of 2
g/dl or more after two consecutive stable hemoglobin values with at least three hours
difference, and tachycardia or hypotension that does not resolve within eight hours. Patients
with signs of recurrent bleeding following first endoscopic therapy are typically treated with a
second endoscopic therapy.
2018 Saleem et al. Cureus 10(6): e2878. DOI 10.7759/cureus.2878 5 of 8
Physicians should be diligent in avoiding the complications associated with endoscopy.
Complications are more common with emergent endoscopy [34]. It includes aspiration
pneumonitis, hypoventilation due to oversedation, or hypotension due to inadequate volume
replacement in addition to sedation with opiates. Postoperative complications include
perforation of the esophagus leading to mediastinitis; epinephrine injections can cause
tachycardia and arrhythmias [34].
Long-term use of PPI has been associated with several side effects. Its use has been associated
with increased risk of Clostridium difficile infection in the absence of antibiotic use [35,36]. Its
use has been associated with microscopic colitis, including lymphocytes and collagenous
colitis [37]. PPI can increase the risk of fractures. Induced hypochlorhydria can augment
osteoclastic activity, thereby decreasing bone density [38]. PPI can cause acute interstitial
nephritis [39]. Patients should follow up with a primary care physician after discharge to decide
about PPI.
Conclusions
Upper GI bleeding is a medical emergence with high mortality which can be lowered by proper
assessment and management. A validated scoring system can help the internist decide about
the level of care, timing of endoscopy, and discharge planning. The risk of thrombosis ought to
be weighed against the risk of bleeding before holding the anticoagulation and antiplatelet
therapy in UGIB. Endoscopy should be performed after hemodynamically stabilizing the
patient. It should be performed within 24 hours of admission. Data are restricted about
resumption of anticoagulation after accomplishing endoscopic hemostasis. It should be
individually based on anticoagulation indication and on endoscopic findings. In spite the fact
that PPI utilization brings down the risk of re-bleeding, long-term use of PPI should be justified
considering the side effects related with it.
Additional Information
Disclosures
Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors
declare the following: Payment/services info: All authors have declared that no financial
support was received from any organization for the submitted work. Financial relationships:
All authors have declared that they have no financial relationships at present or within the
previous three years with any organizations that might have an interest in the submitted work.
Other relationships: All authors have declared that there are no other relationships or
activities that could appear to have influenced the submitted work.
References
1. Cappell MS, Friedel D: Initial management of acute upper gastrointestinal bleeding: from
initial evaluation up to gastrointestinal endoscopy. Med Clin North Am. 2008, 92:491.
10.1016/j.mcna.2008.01.005
2. Doherty GM: Current Diagnosis and Treatment: Surgery, 13th Ed . Loeb MS, Davis K (ed):
McGraw-Hill Companies, USA; 2010. p. 493.
3. Longstreth GF: Epidemiology of hospitalization for acute upper gastrointestinal hemorrhage:
a population-based study. Am J Gastroenterol. 1995, 90:206.
4. Lanas A, Perez-Aisa MA, Feu F, et al.: A nationwide study of mortality associated with hospital
admission due to severe gastrointestinal events and those associated with nonsteroidal
antiinflammatory drug use. Am J Gastroenterol. 2005, 100:1685. 10.1111/j.1572-
0241.2005.41833.x
5. Boonpongmanee S, Fleischer DE, Pezzullo JC, et al.: The frequency of peptic ulcer as a cause
of upper-GI bleeding is exaggerated. Gastrointest Endosc. 2004, 59:788. 10.1016/S0016-
5107(04)00181-6
2018 Saleem et al. Cureus 10(6): e2878. DOI 10.7759/cureus.2878 6 of 8
6. Enestvedt BK, Gralnek IM, Mattek N, Lieberman DA, Eisen G: An evaluation of endoscopic
indications and findings related to nonvariceal upper-GI hemorrhage in a large multicenter
consortium. Gastrointest Endosc. 2008, 67:422. 10.1016/j.gie.2007.09.024
7. Loperfido S, Baldo V, Piovesana E, et al.: Changing trends in acute upper-GI bleeding: a
population-based study. Gastrointest Endosc. 2009, 70:212-224. 10.1016/j.gie.2008.10.051
8. Balderas V, Bhore R, Lara LF, Spesivtseva J, Rockey DC: The hematocrit level in upper
gastrointestinal hemorrhage: safety of endoscopy and outcomes. Am J Med. 2011, 124:970-
976. 10.1016/j.amjmed.2011.04.032
9. Wollenman CS, Chason R, Reisch JS, Rockey DC: Impact of ethnicity in upper gastrointestinal
hemorrhage. J Clin Gastroenterol. 2014, 48:343-350. 10.1097/MCG.0000000000000025
10. Lee YT, Walmsley RS, Leong RW, Sung JJ: Dieulafoy's lesion. Gastrointest Endosc. 2003,
58:236-243. 10.1067/mge.2003.328
11. Hunt RH, Malfertheiner P, Yeomans ND, Hawkey CJ, Howden CW: Critical issues in the
pathophysiology and management of peptic ulcer disease. Eur J Gastroenterol Hepatol. 1995,
7:685-699.
12. Hallas J, Lauritsen J, Villadsen HD, Gram LF: Nonsteroidal anti-inflammatory drugs and upper
gastrointestinal bleeding, identifying high-risk groups by excess risk estimates. Scand J
Gastroenterol. 1995, 30:438-444. 10.3109/00365529509093304
13. Laine L, Jensen DM: Management of patients with ulcer bleeding . Am J Gastroenterol. 2012,
107:345-493. 10.1038/ajg.2011.480
14. Srygley FD, Gerardo CJ, Tran T, Fisher DA: Does this patient have a severe upper
gastrointestinal bleed?. J Am Med Assoc. 2012, 307:1072-1079. 10.1001/jama.2012.253
15. Saltzman JR, Tabak YP, Hyett BH, Sun X, Travis AC, Johannes RS: A simple risk score
accurately predicts in-hospital mortality, length of stay, and cost in acute upper GI bleeding.
Gastrointest Endosc. 2011, 74:1215-1224. 10.1016/j.gie.2011.06.024
16. Desai J, Granger CB, Weitz JI, Aisenberg J: Novel oral anticoagulants in gastroenterology
practice. Gastrointest Endosc. 2013, 78:227-239. 10.1016/j.gie.2013.04.179
17. Choudari CP, Rajgopal C, Palmer KR: Acute gastrointestinal haemorrhage in anticoagulated
patients: diagnoses and response to endoscopic treatment. Gut. 1994, 35:464-466.
18. Chan WH, Khin LW, Chung YF, Goh YC, Ong HS, Wong WK: Randomized controlled trial of
standard versus high-dose intravenous omeprazole after endoscopic therapy in high-risk
patients with acute peptic ulcer bleeding. Br J Surg. 2011, 98:640-644. 10.1002/bjs.7420
19. Green FW Jr, Kaplan MM, Curtis LE, Levine PH: Effect of acid and pepsin on blood coagulation
and platelet aggregation. A possible contributor prolonged gastroduodenal mucosal
hemorrhage. Gastroenterology. 1978, 74:38-43.
20. Frossard JL, Spahr L, Queneau PE, et al.: Erythromycin intravenous bolus infusion in acute
upper gastrointestinal bleeding: a randomized, controlled, double-blind trial.
Gastroenterology. 2002, 123:17-23. 10.1053/gast.2002.34230
21. American Society of Anesthesiologists Task Force on Sedation and Analgesia by Non-
Anesthesiologists: Practice guidelines for sedation and analgesia by non-anesthesiologists .
Anesthesiology. 2002, 96:1004-1017.
22. Katschinski B, Logan R, Davies J,et al.: Prognostic factors in upper gastrointestinal bleeding .
Dig Dis Sci. 1994, 39:706. 10.1007/BF02087411
23. Baron TH, Kamath PS, McBane RD: Management of antithrombotic therapy in patients
undergoing invasive procedures. N Engl J Med. 2013, 368:2113-2124. 10.1056/NEJMra1206531
24. Baron TH, Kamath PS, McBane RD: New anticoagulant and antiplatelet agents: a primer for
the gastroenterologist. Clin Gastroenterol Hepatol. 2014, 12:187-195.
10.1016/j.cgh.2013.05.020
25. Boustière C, Veitch A, Vanbiervliet G, et al.: Endoscopy and antiplatelet agents. European
Society of Gastrointestinal Endoscopy (ESGE) Guideline. Endoscopy. 2011, 43:445-461.
10.1055/s-0030-1256317
26. ASGE Standards of Practice Committee, Acosta RD, Abraham NS, et al.: The management of
antithrombotic agents for patients undergoing GI endoscopy. Gastrointest Endosc. 2016,
83:3-16. 10.1016/j.gie.2015.09.035
27. Becker RC, Scheiman J, Dauerman HL, et al.: Management of platelet-directed
pharmacotherapy in patients with atherosclerotic coronary artery disease undergoing elective
endoscopic gastrointestinal procedures. J Am Coll Cardiol. 2009, 104:2903-2917.
10.1016/j.jacc.2009.09.012
2018 Saleem et al. Cureus 10(6): e2878. DOI 10.7759/cureus.2878 7 of 8
28. Cotton PB, Lehman G, Vennes J, et al.: Endoscopic sphincterotomy complications and their
management: an attempt at consensus. Gastrointest Endosc. 1991, 37:383-393.
10.1016/S0016-5107(91)70740-2
29. Shiffman ML, Farrel MT, Yee YS: Risk of bleeding after endoscopic biopsy or polypectomy in
patients taking aspirin or other NSAIDS. Gastrointest Endosc. 1994, 40:458-462.
10.1016/S0016-5107(94)70210-1
30. Hussain N, Alsulaiman R, Burtin P, et al.: The safety of endoscopic sphincterotomy in patients
receiving antiplatelet agents: a case-control study. Aliment Pharmacol Ther. 2007, 25:579-
584. 10.1111/j.1365-2036.2006.03225.x
31. Hamada T, Yasunaga H, Nakai Y, et al.: Bleeding after endoscopic sphincterotomy or papillary
balloon dilation among users of antithrombotic agents. Endoscopy. 2015, 47:997-1004.
10.1055/s-0034-1392408
32. Barkun AN, Bardou M, Kuipers EJ, et al.: International consensus recommendations on the
management of patients with nonvariceal upper gastrointestinal bleeding. Ann Intern Med.
2010, 152:101-113.
33. Laine L, Spiegel B, Rostom A, et al.: Methodology for randomized trials of patients with
nonvariceal upper gastrointestinal bleeding: recommendations from an international
consensus conference. Am J Gastroenterol. 2010, 105:540-550. 10.1038/ajg.2009.702
34. Eisen GM, Baron TH, Dominitz JA, et al.: Complications of upper GI endoscopy . Gastrointest
Endosc. 2002, 55:784-793. 10.1016/S0016-5107(02)70404-5
35. Naggie S, Miller BA, Zuzak KB, et al.: A case-control study of community-associated
Clostridium difficile infection: no role for proton pump inhibitors. Am J Med. 2011,
124:276.e1-7. 10.1016/j.amjmed.2010.10.013
36. Cao F, Chen CX, Wang M, et al.: Updated meta-analysis of controlled observational studies:
proton-pump inhibitors and risk of Clostridium difficile infection. J Hosp Infect. 2018, 98:4-
13. 10.1016/j.jhin.2017.08.017
37. Keszthelyi D, Jansen SV, Schouten GA, et al.: Proton pump inhibitor use is associated with an
increased risk for microscopic colitis: a case-control study. Aliment PharmacolTher. 2010,
32:1124-1128. 10.1111/j.1365-2036.2010.04453.x
38. Tuukkanen J, Väänänen HK: Omeprazole, a specific inhibitor of H+-K+-ATPase, inhibits bone
resorption in vitro. Calcif Tissue Int. 1986, 38:123-125.
39. Sampathkumar K, Ramalingam R, Prabakar A, Abraham A: Acute interstitial nephritis due to
proton pump inhibitors. Indian J Nephrol. 2013, 23:304-307. 10.4103/0971-4065.114487
2018 Saleem et al. Cureus 10(6): e2878. DOI 10.7759/cureus.2878 8 of 8
You might also like
- Renal ExamDocument12 pagesRenal ExamCamille Espinosa100% (7)
- MCU 2020 Retinoids in DermatologyDocument245 pagesMCU 2020 Retinoids in DermatologyAkiko Atmojo100% (1)
- Initial Management of Acute Upper Gastrointestinal Bleeding: From Initial Evaluation Up To Gastrointestinal EndosDocument19 pagesInitial Management of Acute Upper Gastrointestinal Bleeding: From Initial Evaluation Up To Gastrointestinal EndosPatricia Ann Factor-TarucNo ratings yet
- Gastrointestinal BleedingDocument17 pagesGastrointestinal BleedingMaría José GalvisNo ratings yet
- Diagnosis and Management of Lower Gastrointestinal Bleeding: Jürgen Barnert and Helmut MessmannDocument10 pagesDiagnosis and Management of Lower Gastrointestinal Bleeding: Jürgen Barnert and Helmut Messmanndwee_RNSNo ratings yet
- Management of Patient With Gastrointestinal BleedingDocument14 pagesManagement of Patient With Gastrointestinal BleedingPulkit MandalNo ratings yet
- Management and Prevention of Upper GI Bleeding: by Jiwon Kim, Pharm.D., BCPS, FCSHPDocument0 pagesManagement and Prevention of Upper GI Bleeding: by Jiwon Kim, Pharm.D., BCPS, FCSHPbasinang_jangil100% (1)
- Upper Gastrointestinal Bleeding (UGIB) : Practice EssentialsDocument52 pagesUpper Gastrointestinal Bleeding (UGIB) : Practice EssentialsrishaNo ratings yet
- ACGGuideline Acute Lower GI Bleeding 03012016 PDFDocument16 pagesACGGuideline Acute Lower GI Bleeding 03012016 PDFGrahamOliverAceroVieraNo ratings yet
- Upper Gastrointestinal Bleeding Due To A Peptic Ulcer: Clinical PracticeDocument10 pagesUpper Gastrointestinal Bleeding Due To A Peptic Ulcer: Clinical PracticeCristian Esteban AcostaNo ratings yet
- Causes of Upper Gastrointestinal Bleeding in Adults UpToDateDocument37 pagesCauses of Upper Gastrointestinal Bleeding in Adults UpToDateJodene Rose RojasNo ratings yet
- Antiagre AnticoagDocument15 pagesAntiagre AnticoagpilarNo ratings yet
- Hematemesis PDFDocument7 pagesHematemesis PDFkevin_jawanNo ratings yet
- Poddar 2018Document6 pagesPoddar 2018AfniNo ratings yet
- GI Bleeding (Text)Document11 pagesGI Bleeding (Text)Hart ElettNo ratings yet
- Surgery CaseDocument4 pagesSurgery CaseVincent SomidoNo ratings yet
- Causes of Upper Gastrointestinal Bleeding in Adults - UpToDateDocument37 pagesCauses of Upper Gastrointestinal Bleeding in Adults - UpToDateAline MoraisNo ratings yet
- BMJ l536 FullDocument15 pagesBMJ l536 Fulldendy17018No ratings yet
- Massive Gastrointestinal HemorrhageDocument19 pagesMassive Gastrointestinal HemorrhageVikrantNo ratings yet
- Gastro 1004Document4 pagesGastro 1004Paul HartingNo ratings yet
- Management of Acute Upper Gastrointestinal BleedingDocument15 pagesManagement of Acute Upper Gastrointestinal BleedingShiva ValeskaNo ratings yet
- Artiin Jurnal UGBDocument22 pagesArtiin Jurnal UGBInna MaynizaNo ratings yet
- 58 Lower Gastrointestinal BleedDocument4 pages58 Lower Gastrointestinal BleedLuphly TaluvtaNo ratings yet
- Upper Gi Bleed: History, Pe, Pathophysiology, Diagnostics and TreatmentDocument6 pagesUpper Gi Bleed: History, Pe, Pathophysiology, Diagnostics and TreatmentJennicaNo ratings yet
- Panduan Penatalaksanaan Gastrointestinal BleedingDocument8 pagesPanduan Penatalaksanaan Gastrointestinal BleedingGenanda FisabililaNo ratings yet
- Uppergastrointestinalbleeding: Marcie Feinman,, Elliott R. HautDocument11 pagesUppergastrointestinalbleeding: Marcie Feinman,, Elliott R. HautjoseNo ratings yet
- Management of Non-Variceal Upper Gastrointestinal Tract Hemorrhage: Controversies and Areas of UncertaintyDocument7 pagesManagement of Non-Variceal Upper Gastrointestinal Tract Hemorrhage: Controversies and Areas of UncertaintyIsnan WahyudiNo ratings yet
- 2015 S 0034 1393172Document7 pages2015 S 0034 1393172AladesuruOlumideAdewaleNo ratings yet
- Manejo Del ResangradoDocument13 pagesManejo Del ResangradoRudy J CoradoNo ratings yet
- Lower GI BleedDocument8 pagesLower GI BleedIULIAN LUPUNo ratings yet
- A Grand Case UgibDocument84 pagesA Grand Case UgibAdrianne Kricia100% (2)
- CholangitisDocument11 pagesCholangitisNilamsari KurniasihNo ratings yet
- GI BleedingDocument9 pagesGI Bleedingmeilawati rahmanNo ratings yet
- Upper Gastrointestinal BleedingDocument118 pagesUpper Gastrointestinal Bleeding9092041025No ratings yet
- Lower Gastrointestinal Bleeding: Practice EssentialsDocument28 pagesLower Gastrointestinal Bleeding: Practice EssentialsJohnPaulOliverosNo ratings yet
- Stress Ulcer Prophylaxis in ICUDocument11 pagesStress Ulcer Prophylaxis in ICUdragon66No ratings yet
- ACG Guideline Colon-Ischemia January 2015Document27 pagesACG Guideline Colon-Ischemia January 2015IgorCotagaNo ratings yet
- Oakland 2019Document6 pagesOakland 2019EkiNo ratings yet
- Haematemesis and MalenaDocument39 pagesHaematemesis and MalenaNikNo ratings yet
- Gastrointestinal Bleeding - StatPearls - NCBI BookshelfDocument7 pagesGastrointestinal Bleeding - StatPearls - NCBI BookshelfAdam GenturNo ratings yet
- HHS Public Access: Pharmacologic Treatment of Upper Gastrointestinal BleedingDocument12 pagesHHS Public Access: Pharmacologic Treatment of Upper Gastrointestinal BleedingElizaNo ratings yet
- Determining Severe GI BleedDocument8 pagesDetermining Severe GI BleedDanny SilvaNo ratings yet
- DX Approach & MX of HMDocument8 pagesDX Approach & MX of HMjosephNo ratings yet
- Upper GI BleedDocument8 pagesUpper GI BleedbbyesNo ratings yet
- Stress-Related Mucosal Disease: Mitchell J. Spirt, MDDocument11 pagesStress-Related Mucosal Disease: Mitchell J. Spirt, MDnur hidayatNo ratings yet
- Esophageal Varices: Pathophysiology, Approach, and Clinical DilemmasDocument2 pagesEsophageal Varices: Pathophysiology, Approach, and Clinical Dilemmaskaychi zNo ratings yet
- Jurnal 3Document7 pagesJurnal 3AfniNo ratings yet
- Ischemic Colitis As A Cause of Severe Hematochezia: A Mini ReviewDocument5 pagesIschemic Colitis As A Cause of Severe Hematochezia: A Mini ReviewAghie vlogNo ratings yet
- c1 PDFDocument11 pagesc1 PDFirene chanNo ratings yet
- JApplHematol5258-4238371 114623Document7 pagesJApplHematol5258-4238371 114623Agus SaputraNo ratings yet
- Case Alcohol Abuse and Unusual Abdominal Pain in A 49-Year-OldDocument7 pagesCase Alcohol Abuse and Unusual Abdominal Pain in A 49-Year-OldPutri AmeliaNo ratings yet
- Etiological Pattern and Outcome of Non-Variceal Upper G.I. BleedingDocument5 pagesEtiological Pattern and Outcome of Non-Variceal Upper G.I. BleedingJawad ZafarNo ratings yet
- Referat DR Ty 2Document8 pagesReferat DR Ty 2Muhamad Amar'sNo ratings yet
- Endoscopic Band Ligation Is Safe Despite Low Platelet Count and HighDocument10 pagesEndoscopic Band Ligation Is Safe Despite Low Platelet Count and HighGustavo FernándezNo ratings yet
- Hemodynamic Response To Pharmacological Treatment of Portal Hypertension and Long-Term Prognosis of CirrhosisDocument7 pagesHemodynamic Response To Pharmacological Treatment of Portal Hypertension and Long-Term Prognosis of CirrhosisBarbara Sakura RiawanNo ratings yet
- Causes of Upper Gastrointestinal Bleeding in Adults - UpToDate PDFDocument55 pagesCauses of Upper Gastrointestinal Bleeding in Adults - UpToDate PDFKristell LópezNo ratings yet
- The Misunderstood Coagulopathy of Liver Disease - WJM 2018Document9 pagesThe Misunderstood Coagulopathy of Liver Disease - WJM 2018J doeNo ratings yet
- Kjg066 02 06Document8 pagesKjg066 02 06Nguyễn PhúcNo ratings yet
- Olsen 2005Document6 pagesOlsen 2005Amalia NandiaNo ratings yet
- Acute Gastrointestinal Bleeding: Diagnosis and TreatmentFrom EverandAcute Gastrointestinal Bleeding: Diagnosis and TreatmentKaren E. KimNo ratings yet
- Preventive Medicine: Xiaolei Xie, Tianhua He, Jian Kang, David S. Siscovick, Yan Li, José A. PagánDocument5 pagesPreventive Medicine: Xiaolei Xie, Tianhua He, Jian Kang, David S. Siscovick, Yan Li, José A. PagánDewiNo ratings yet
- J. DAFTAR PUSTAKADocument6 pagesJ. DAFTAR PUSTAKADewiNo ratings yet
- Compatibility Study of Paracetamol, Chlorpheniramine Maleate and Phenylephrine Hydrochloride in Physical MixturesDocument6 pagesCompatibility Study of Paracetamol, Chlorpheniramine Maleate and Phenylephrine Hydrochloride in Physical MixturesDewiNo ratings yet
- Combination Treatment For HypertensionDocument4 pagesCombination Treatment For HypertensionDewiNo ratings yet
- GGHGHHDocument32 pagesGGHGHHDewiNo ratings yet
- Antihypertensive TherapyDocument8 pagesAntihypertensive TherapyDewiNo ratings yet
- Trace Elements and Contaminants PDFDocument19 pagesTrace Elements and Contaminants PDFRahul Kumar MíšhřâNo ratings yet
- Bipolar 1 DisorderDocument11 pagesBipolar 1 DisorderGirlly AlcantaraNo ratings yet
- 208 7 20 MicrocurrentDocument2 pages208 7 20 MicrocurrentIon Logofătu Albert50% (2)
- Fungal Hyphae: Type # 1. Plectenchyma (Fig. 1.12)Document5 pagesFungal Hyphae: Type # 1. Plectenchyma (Fig. 1.12)vineetvishal73No ratings yet
- Aquino Vs Sss DigestDocument2 pagesAquino Vs Sss Digestkatherine magbanuaNo ratings yet
- State Reports LatestDocument54 pagesState Reports LatestAdam PoulisseNo ratings yet
- 32 I Am Legend - Future PerfectDocument1 page32 I Am Legend - Future PerfectDeniza UsainovaNo ratings yet
- Introduction of Digital Innovations in Livestock Farming - FinalDocument13 pagesIntroduction of Digital Innovations in Livestock Farming - Finalrusty100% (2)
- Caregiving Lesson Quarter ExamsDocument3 pagesCaregiving Lesson Quarter ExamsGlaiza FloresNo ratings yet
- Salivary Glands For BDSDocument47 pagesSalivary Glands For BDSSnighdayNo ratings yet
- Basic Life Support Study Guide: Critical Care Training CenterDocument12 pagesBasic Life Support Study Guide: Critical Care Training CenterTODNo ratings yet
- When Breath Becomes Air One PagerDocument1 pageWhen Breath Becomes Air One Pageraxa9522No ratings yet
- CH04 Food SafetyDocument20 pagesCH04 Food SafetyRianne AuxerreNo ratings yet
- Wagner Justin CVDocument4 pagesWagner Justin CVapi-526434517No ratings yet
- (Progress in Epileptic Disorders, Vol. 13) Solomon L. Moshé, J. Helen Cross, Linda de Vries, Douglas Nordli, Federico Vigevano-Seizures and Syndromes of PDFDocument283 pages(Progress in Epileptic Disorders, Vol. 13) Solomon L. Moshé, J. Helen Cross, Linda de Vries, Douglas Nordli, Federico Vigevano-Seizures and Syndromes of PDFWalter Huacani HuamaniNo ratings yet
- Restrictive Lung DiseasesDocument31 pagesRestrictive Lung DiseasesAnn FrancisNo ratings yet
- Economics 312 Urban Land Economics: Martin Farnham University of Victoria Spring 2018Document63 pagesEconomics 312 Urban Land Economics: Martin Farnham University of Victoria Spring 2018Ines ArozaNo ratings yet
- Key Points - Peds Vital SignsDocument1 pageKey Points - Peds Vital SignsRaman kangNo ratings yet
- MEDICAL LECT B SC SUM20Document63 pagesMEDICAL LECT B SC SUM20Dewan Ajuad Hossain RifatNo ratings yet
- LinkageDocument9 pagesLinkageHarshu JunghareNo ratings yet
- Iowa Woodlands Vital Habitat For Native PollinatorsDocument8 pagesIowa Woodlands Vital Habitat For Native PollinatorsJNo ratings yet
- Prevalence and Epidemiology: Pathogenesis and Pathophysiology of Meniére's DiseaseDocument2 pagesPrevalence and Epidemiology: Pathogenesis and Pathophysiology of Meniére's DiseaseShiela GutierrezNo ratings yet
- Arteri Cerebellar: Presenter: Dr. Andre Lona Moderator: Dr. Iskandar Nasution, SP.S, FINSDocument40 pagesArteri Cerebellar: Presenter: Dr. Andre Lona Moderator: Dr. Iskandar Nasution, SP.S, FINSAlon RiderNo ratings yet
- STS 1 Act 6 Gene TherapyDocument1 pageSTS 1 Act 6 Gene TherapyJustine EscotoNo ratings yet
- Cure AllDocument38 pagesCure AllDanja TešićNo ratings yet
- Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT FindingsDocument18 pagesImaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT FindingsbagusNo ratings yet
- LithiumDocument21 pagesLithiumvikaseptideyaniNo ratings yet
- The Benefits of Owning A PetDocument3 pagesThe Benefits of Owning A PetKyle CraneNo ratings yet