Professional Documents
Culture Documents
Faculty Development CPD
Faculty Development CPD
Uploaded by
Aida TantriCopyright:
Available Formats
You might also like
- Foundations of Osteopathic Medicine Philosophy Science Clinical Applications and Research 4th Edition Ebook PDFDocument62 pagesFoundations of Osteopathic Medicine Philosophy Science Clinical Applications and Research 4th Edition Ebook PDFjerry.graves681100% (54)
- Family Health Care Nursing - Rowe-Kaakinen, Joanna, Padgett-Coehlo, Deborah, Steele, Rose PDFDocument649 pagesFamily Health Care Nursing - Rowe-Kaakinen, Joanna, Padgett-Coehlo, Deborah, Steele, Rose PDFUmi Marfungatun Mudrikah100% (14)
- Iso 45001 ExamDocument15 pagesIso 45001 ExamAhmed NABIL67% (12)
- Part 1 SAQs Specimen QuestionsDocument79 pagesPart 1 SAQs Specimen Questionsخولة رشيد العيسى100% (2)
- Obe PDFDocument6 pagesObe PDFjaycee_evangelistaNo ratings yet
- Station 1 - 12 Tips For Education Needs Assessments Through An Interprofessional LensDocument4 pagesStation 1 - 12 Tips For Education Needs Assessments Through An Interprofessional LensAida TantriNo ratings yet
- A Framework For The Design ImplementationDocument6 pagesA Framework For The Design ImplementationPATRICIA POLETTONo ratings yet
- Interprofessional Educationand CollaborationDocument7 pagesInterprofessional Educationand CollaborationnersrosdianaNo ratings yet
- Rw-Omj-D-18-00175 (05C)Document6 pagesRw-Omj-D-18-00175 (05C)nersrosdianaNo ratings yet
- 02 - Soemantri Et AlDocument8 pages02 - Soemantri Et Alany fitriyaniNo ratings yet
- Interprofessional Collaboration and Education.26Document8 pagesInterprofessional Collaboration and Education.26sans9No ratings yet
- Actividades Profesionales ConfiablesDocument6 pagesActividades Profesionales ConfiablesOscar F RojasNo ratings yet
- Levett-Jones Et Al-2018-Journal of Nursing Scholarship1Document10 pagesLevett-Jones Et Al-2018-Journal of Nursing Scholarship1Nande BandeNo ratings yet
- Interprofessional Education For Collaborative, Patient-Centred PracticeDocument7 pagesInterprofessional Education For Collaborative, Patient-Centred PracticeWahyu WijayantoNo ratings yet
- Exploring Faculty Preparedness and Capability For Interprofessional LearningDocument1 pageExploring Faculty Preparedness and Capability For Interprofessional LearningSadashiv RahaneNo ratings yet
- Research PresentationDocument14 pagesResearch PresentationCeeNo ratings yet
- New Paradigm For CME - JCEHP Sep 2011Document8 pagesNew Paradigm For CME - JCEHP Sep 2011Daniel GuineeNo ratings yet
- Henzi Etal (2006) - Perspectives Dental Students About Clinical EducationDocument17 pagesHenzi Etal (2006) - Perspectives Dental Students About Clinical EducationMiguel AraizaNo ratings yet
- Faculty Development For TeachingDocument10 pagesFaculty Development For TeachingRochelle Edquilang CapistranoNo ratings yet
- Review Article: Advanced Practice Nursing Education: Challenges and StrategiesDocument9 pagesReview Article: Advanced Practice Nursing Education: Challenges and StrategiesluNo ratings yet
- Development and Experimental Results of Outcomes-Based Nursing ProgramDocument6 pagesDevelopment and Experimental Results of Outcomes-Based Nursing ProgramIJAR JOURNALNo ratings yet
- Importance and Purposes of Research: Instruction: Answer Comprehensively and ExtensivelyDocument3 pagesImportance and Purposes of Research: Instruction: Answer Comprehensively and ExtensivelyKarl Kiw-isNo ratings yet
- Interprofessional Collaboration: Three Best Practice Models of Interprofessional EducationDocument5 pagesInterprofessional Collaboration: Three Best Practice Models of Interprofessional Educationna5649No ratings yet
- Interprofessional Education For Collaborative, Patient-Centred PracticeDocument7 pagesInterprofessional Education For Collaborative, Patient-Centred PracticeAnonymous u5UPeiWpNo ratings yet
- International Journal of Nursing SciencesDocument5 pagesInternational Journal of Nursing SciencesWahyu Phaling FienterNo ratings yet
- Sicometrik ICP IndonesiaDocument10 pagesSicometrik ICP IndonesiaUchi SuhermanNo ratings yet
- Continuando La Educacion Medica para Los Practicantes Generales - Un Formato para PracticasDocument6 pagesContinuando La Educacion Medica para Los Practicantes Generales - Un Formato para PracticasAnonymous 3MPClbaCDNo ratings yet
- Content ServerDocument11 pagesContent ServerMona AL-FaifiNo ratings yet
- Medical Education - 2005 - McNairDocument9 pagesMedical Education - 2005 - McNairISABEL BUENO SANTOS MENEZESNo ratings yet
- 1 PBDocument7 pages1 PBinti.makmur.lgNo ratings yet
- Interprofessional Education PDFDocument3 pagesInterprofessional Education PDFRobert MontgomeryNo ratings yet
- Continuing Education in Nursing: Ursing DucationDocument17 pagesContinuing Education in Nursing: Ursing Ducationsaleha sultana100% (1)
- Interprofessional Collaboration Three Best Practice Models of Interprofessional EducationDocument11 pagesInterprofessional Collaboration Three Best Practice Models of Interprofessional Educationgenta01100% (1)
- Foreign Literature FinalsDocument14 pagesForeign Literature FinalsAnghel CruzNo ratings yet
- Developing Skills Learning in Obstetric Nursing: Approaches Between Theory and PracticeDocument7 pagesDeveloping Skills Learning in Obstetric Nursing: Approaches Between Theory and PracticerupaNo ratings yet
- Structured Mentoring StrategiesDocument31 pagesStructured Mentoring Strategiesrandy gallegoNo ratings yet
- Interprofessional Education Esmarliza K. Tacud-Luzon, MDDocument3 pagesInterprofessional Education Esmarliza K. Tacud-Luzon, MDRaphael MiguelNo ratings yet
- Spring 09 NewsletterDocument13 pagesSpring 09 NewsletterAnnie DanielNo ratings yet
- CHAPTER 1 Action ResearchDocument30 pagesCHAPTER 1 Action ResearchmatetbongNo ratings yet
- SJMPS - 38896 906 1Document11 pagesSJMPS - 38896 906 1danicaattabanNo ratings yet
- Quality and Safety Curricula in NursingDocument5 pagesQuality and Safety Curricula in NursingAmeng GosimNo ratings yet
- Submit Due 9.12Document11 pagesSubmit Due 9.12Are HidayuNo ratings yet
- Medical Education in Pulmonary, Critical Care, and Sleep Medicine: Advanced Concepts and StrategiesFrom EverandMedical Education in Pulmonary, Critical Care, and Sleep Medicine: Advanced Concepts and StrategiesPatricia A. KritekNo ratings yet
- Interprofessional Collaboration Three Best Practice Models of Interprofessional EducationDocument11 pagesInterprofessional Collaboration Three Best Practice Models of Interprofessional Educationanzila widyaNo ratings yet
- NURS FPX 6614 Assessment 2 Enhancing Performance As Collaborators in CareDocument7 pagesNURS FPX 6614 Assessment 2 Enhancing Performance As Collaborators in Carefarwaamjad771No ratings yet
- Ipe and Ipc Assignment Part 1Document17 pagesIpe and Ipc Assignment Part 1api-547401454No ratings yet
- Research in Continuing EducationDocument25 pagesResearch in Continuing EducationArchana VermaNo ratings yet
- Role of Medical Education in Cultivating LifelongDocument4 pagesRole of Medical Education in Cultivating LifelongRudolph SunnydaysNo ratings yet
- Students Perceptions of Effective Classroom and CDocument13 pagesStudents Perceptions of Effective Classroom and Ckrishnabhagwat30No ratings yet
- Naskah Publikasi FixDocument14 pagesNaskah Publikasi FixSabet LilyNo ratings yet
- The Core Curriculum and Integration in Medical Education: Nikoo Yamani, Masoumeh RahimiDocument5 pagesThe Core Curriculum and Integration in Medical Education: Nikoo Yamani, Masoumeh RahimiDoctorRonZ7No ratings yet
- Nu708 m7 - Ebp Perspective SustainabilityDocument8 pagesNu708 m7 - Ebp Perspective Sustainabilityapi-577441503No ratings yet
- Improving Assessment in Dental Education Through A Paradigm of Comprehensive Care: A Case ReportDocument13 pagesImproving Assessment in Dental Education Through A Paradigm of Comprehensive Care: A Case ReportfidelbustamiNo ratings yet
- Interprofessional Collaboration and Education.26 PDFDocument15 pagesInterprofessional Collaboration and Education.26 PDFBrajakson SiokalNo ratings yet
- Interprofessional Education - The Way Forward in Health ProfessionDocument2 pagesInterprofessional Education - The Way Forward in Health ProfessionJLatriece Elizabeth CedeñoNo ratings yet
- Measuring Clinical Reasoning and Interprofessional AttitudesDocument6 pagesMeasuring Clinical Reasoning and Interprofessional AttitudesVizaNo ratings yet
- Apta Combined Sections Meeting 2023 AbstractDocument1 pageApta Combined Sections Meeting 2023 Abstractapi-738548992No ratings yet
- IMPACT OF EXPER-WPS OfficeDocument10 pagesIMPACT OF EXPER-WPS Officepash blessingsNo ratings yet
- Dimensions of Learning Organizations Questionnaire (DLOQ) in A Low-Resource Health Care Setting in NepalDocument8 pagesDimensions of Learning Organizations Questionnaire (DLOQ) in A Low-Resource Health Care Setting in Nepalsapit90No ratings yet
- Nurse Managers' Responsive Coaching To Facilitate Staff Nurses' Clinical Skills Development in Public Tertiary HospitalDocument10 pagesNurse Managers' Responsive Coaching To Facilitate Staff Nurses' Clinical Skills Development in Public Tertiary Hospitalvan royeNo ratings yet
- Assessment of Learning NeedsDocument4 pagesAssessment of Learning NeedsRhonaJoyNo ratings yet
- UA OMSE Med/Ed Enews v3 No. 01 (AUG 2014)Document10 pagesUA OMSE Med/Ed Enews v3 No. 01 (AUG 2014)KC Spear Ellinwood, former Director Instructional DevelopmentNo ratings yet
- Chapter 1 3 ResearchDocument26 pagesChapter 1 3 ResearchAb Staholic BoiiNo ratings yet
- A Guide to Medical Teaching and Learning Training of the Trainers (Tot): In the View of the Learner-Centered Learning ModelFrom EverandA Guide to Medical Teaching and Learning Training of the Trainers (Tot): In the View of the Learner-Centered Learning ModelNo ratings yet
- 1 s2.0 S1521689614000044 PDFDocument21 pages1 s2.0 S1521689614000044 PDFAida TantriNo ratings yet
- Pain in Terminally IllDocument29 pagesPain in Terminally IllAida Tantri100% (1)
- LA CraniotomyDocument8 pagesLA CraniotomyAida TantriNo ratings yet
- 2216 2221 PDFDocument6 pages2216 2221 PDFAida TantriNo ratings yet
- Interprofessional EducationDocument12 pagesInterprofessional EducationAida TantriNo ratings yet
- Withdrawing WitholdingDocument6 pagesWithdrawing WitholdingAida TantriNo ratings yet
- Uncommon Complications of Spinal Anaesthesia - AnesthesiaworldDocument14 pagesUncommon Complications of Spinal Anaesthesia - AnesthesiaworldAida TantriNo ratings yet
- Failed Spinal ChloroprocaineDocument4 pagesFailed Spinal ChloroprocaineAida TantriNo ratings yet
- Tsui CSF Lavage CJA 14Document4 pagesTsui CSF Lavage CJA 14Aida TantriNo ratings yet
- Accidental Epidural Injection of Atropine: Case ReportDocument2 pagesAccidental Epidural Injection of Atropine: Case ReportAida TantriNo ratings yet
- Spinal ToxicityDocument12 pagesSpinal ToxicityAida Tantri0% (1)
- NURS FPX 6107 Assessment 1 Curriculum Overview, Framework, and AnalysisDocument5 pagesNURS FPX 6107 Assessment 1 Curriculum Overview, Framework, and Analysisjoohnsmith070No ratings yet
- Pednekar S S PDFDocument14 pagesPednekar S S PDFAbubakar MokarimNo ratings yet
- Notes Nurse PolicyDocument6 pagesNotes Nurse PolicyChristian HawthorneNo ratings yet
- BIANNUAL CONGRESS OF HOMOEOPATHIC ASSOCIATION OF SOUTH AFRICA (HSA) 2014: A REPORT (Prepared From REPORT: HSA CONGRESS 2014Document6 pagesBIANNUAL CONGRESS OF HOMOEOPATHIC ASSOCIATION OF SOUTH AFRICA (HSA) 2014: A REPORT (Prepared From REPORT: HSA CONGRESS 2014Homoeopathic PulseNo ratings yet
- Clinical Guideline For The Evaluation and Management of Chronic Insomnia in AdultsDocument18 pagesClinical Guideline For The Evaluation and Management of Chronic Insomnia in AdultsDeTe Punya Map100% (1)
- IDC 213 01 Introduction To Evidence-Based Medicine PDFDocument5 pagesIDC 213 01 Introduction To Evidence-Based Medicine PDFFort SalvadorNo ratings yet
- 2021 Philippine Guidelines On PHEx Phase 1Document148 pages2021 Philippine Guidelines On PHEx Phase 1Famed residentsNo ratings yet
- CephalgiaDocument24 pagesCephalgiaNurlita Ranti YulistyaNo ratings yet
- JBI - Wound ManagementDocument4 pagesJBI - Wound ManagementBethanyNo ratings yet
- Bab 1-5 Manajemen HcuDocument7 pagesBab 1-5 Manajemen Hcuretno indriyaniNo ratings yet
- Eng - PDF JsessionidDocument276 pagesEng - PDF JsessionidWilliam AdiputraNo ratings yet
- FCPS-II PaediatricsDocument41 pagesFCPS-II Paediatricsharoon100% (1)
- CBCT in Orthodontics: Assessment of Treatment Outcomes and Indications For Its UseDocument19 pagesCBCT in Orthodontics: Assessment of Treatment Outcomes and Indications For Its Useelena dinovskaNo ratings yet
- MSC - Medical Surgical Sub Specialty Cardiovascular Thoracic Nursing PDFDocument44 pagesMSC - Medical Surgical Sub Specialty Cardiovascular Thoracic Nursing PDFAlma Susan100% (4)
- Evidence Based PracticesDocument5 pagesEvidence Based Practicesapi-527787868No ratings yet
- NCM 109 Course Syllabus Ay 2022 2023Document17 pagesNCM 109 Course Syllabus Ay 2022 2023ShainaChescaEvans100% (1)
- Chairside Guide Nonrestorative Treatments For Carious Lesions On Primary TeethDocument2 pagesChairside Guide Nonrestorative Treatments For Carious Lesions On Primary TeethMellisa FanNo ratings yet
- DQI and Use Mentor - Oct 2022Document3 pagesDQI and Use Mentor - Oct 2022Amenti TekaNo ratings yet
- Dissertation On Healing Architecture in Hospital DesignDocument114 pagesDissertation On Healing Architecture in Hospital DesignDipesh Anand86% (44)
- BridgeSpan Speech Services Guidelines - V102019 - Eff03012019 - Pub10222018 PDFDocument245 pagesBridgeSpan Speech Services Guidelines - V102019 - Eff03012019 - Pub10222018 PDFMariel Salazar100% (2)
- Call Grand Master +27734818506 HOW TO JOIN 666 ILLUMINATI SECRET SOCIETY FOR MONEY IN USA, UK, Canada, Spain, Italy, China, Hong Kong FreestateDocument176 pagesCall Grand Master +27734818506 HOW TO JOIN 666 ILLUMINATI SECRET SOCIETY FOR MONEY IN USA, UK, Canada, Spain, Italy, China, Hong Kong FreestateJohn RichNo ratings yet
- Ead-510 Field Experience BDocument3 pagesEad-510 Field Experience Bapi-502057756No ratings yet
- Kuliah FeedingDocument41 pagesKuliah Feedingfatihatul kamilahNo ratings yet
- Arksey and OMalley - 2005 - Scoping StudiesDocument17 pagesArksey and OMalley - 2005 - Scoping StudiesCBNo ratings yet
- Nurs FPX 4030 Assessment 1 Locating Credible Databases and ResearchDocument5 pagesNurs FPX 4030 Assessment 1 Locating Credible Databases and Researchjoohnsmith070No ratings yet
- Nursing Philosophy PaperDocument6 pagesNursing Philosophy PaperDanielle AalderinkNo ratings yet
Faculty Development CPD
Faculty Development CPD
Uploaded by
Aida TantriOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Faculty Development CPD
Faculty Development CPD
Uploaded by
Aida TantriCopyright:
Available Formats
Foundations of Continuing Education
Faculty Development for Continuing
Interprofessional Education and
Collaborative Practice
IVAN L. SILVER, MED, MD; KAREN LESLIE, MED, MD
This article proposes a framework for faculty development in continuing interprofessional education (CIPE) and
collaborative practice. The framework is built on best practices in faculty development and CIPE. It was informed
by local experience in the development, delivery, and evaluation of a faculty development program to promote
capacity for dissemination of concepts relating to interprofessional education (IPE) and interprofessional collab-
oration (IPC) in health care environments. Interprofessional education has been demonstrated in clinical contexts
to enhance interprofessional collaboration, patient care, and health outcomes. With curriculum design, teaching
methods, and educational strategies in faculty development, it is possible to enhance the impact of IPE in clinical
contexts. Faculty development activities themselves can model effective interprofessional education methods and
practice. An IPE curriculum and teaching and education strategies are outlined. Strategic planning, including the
application of a systems approach, attention to the principles of effective learning, and an outcomes-based cur-
riculum design are recommended for the development of continuing IPE faculty development programs that en-
hance interprofessional collaboration.
Key Words: continuing interprofessional education, faculty development, staff development, interprofessional
collaboration
Introduction health professions students in multiple settings.3 Educating
students in IPE in practice-based settings suggests that there
Defined as occasions when “two or more professions learn be effective health care teams in place that role model best
with, from, and about each other to improve collaboration practices in team functioning and collaborative practice.4
and the quality of care,” 1 interprofessional education ~IPE! Concern has been expressed that there is a gap in the num-
may be the most direct approach to enhance the quality of ber of best-practice health care teams who role-model ef-
interprofessional collaboration ~IPC! in health care settings. fective team learning. Similarly, health professional educators
IPC is defined as when the health disciplines come together may not have the knowledge, skills, and attitudes to facili-
around patient care issues, whereby decision-making hap- tate team training and learning.5
pens within the group, and a transformation occurs.2 During Interprofessional education has been associated with en-
the past 10 years, IPE curricula have been developed for hanced patient care and health outcomes in a range of clin-
ical contexts.6 These outcomes include improving the working
culture in an emergency department and patient satisfaction,
the reduction of errors in an emergency department, im-
Disclosures: The authors report none.
proved care delivered to victims of domestic violence, and
Dr. Silver: Vice-Dean, Continuing Education and Professional Develop- improvement of the knowledge and skills of mental health
ment, Director of the Centre for Faculty Development at St. Michael’s professionals.6 However, the majority of studies provide lit-
Hospital, Department of Psychiatry, Faculty of Medicine, University of tle discussion of methodological limitations associated with
Toronto; Dr. Leslie: Associate Director, Centre for Faculty Development at
St. Michael’s Hospital, Department of Paediatrics, Faculty of Medicine,
their research, and most studies pay little or no attention to
University of Toronto. sampling techniques in their work or issues relating to study
attrition. This undermines the quality of evidence they can
Correspondence: Ivan Silver, Office of Continuing Education and Profes-
sional Development, 500 University Avenue, Suite 650, Toronto, Ontario
offer.6 In addition, there are a small number of randomized
M5G 1V7, Canada; e-mail: silveri@smh.toronto.on.ca. controlled trials ~RCTs! to indicate that IPE has little or no
effect on professional practice or patient outcomes.6 There
© 2009 The Alliance for Continuing Medical Education, the Society for
Academic Continuing Medical Education, and the Council on CME,
is continued interest on many fronts to design better studies
Association for Hospital Medical Education. • Published online in Wiley and to look at maximizing the educational impact of IPE on
InterScience ~www.interscience.wiley.com!. DOI: 10.10020chp.20032 health care teams.
JOURNAL OF CONTINUING EDUCATION IN THE HEALTH PROFESSIONS, 29(3):172–177, 2009
Faculty Development for Continuing Interprofessional Education and Collaborative Practice
Little attention has been paid in the literature defining teams that have not perceived a need for change may resist
continuing IPE curricula in practice-based settings and to an interprofessional program.7
establishing best practices in IPE for practicing clini- Engaging physicians in IPE has been consistently noted
cians.7 Faculty development, the broad range of activities as a challenge for planners.12 Many reasons for this have
that institutions use to renew or assist faculty in their mul- been noted, including how physicians have been social-
tiple roles, has the potential for improving the practice of ized in medical school and the perception by physicians
IPC and for building capacity in the provision of IPE. The that their authority in the hierarchy is being challenged by
term faculty development in some jurisdictions ~United the new focus on collaboration. One approach to engage
Kingdom! may refer only to faculty development within physicians is to identify team-based education programs
university departments. However, for the purposes of the that can be linked to demonstrable improvements in pa-
article a broader definition would include the develop- tient outcomes, such as quality improvement ~QI! or patient
ment of all health professional staff who have teaching safety projects.12,13
roles in health care settings and organizations.7 There is A well-planned and -executed needs assessment can both
little evidence-based literature available to guide faculty introduce prospective learners to some of the concepts of
development in IPE, especially within health care institu- IPE ~and thus is an intervention in itself ! and at the same
tions. There are few studies to suggest which types of IPE time identify enablers and potential challenges that can be
programs are most effective at improving team function- addressed through curricular development.14
ing, health outcomes of patients, or the performance of
health organizations and systems.
This article brings a faculty development perspective to Planning a Faculty Development Curriculum
continuing IPE for health professionals, outlining a concep-
tual framework, a planning guide, suggestions for a curric- As noted above, planning a curriculum requires attention to
ulum, and teaching strategies and formats for planning and the different education needs at different levels of a health
design. The work of Steinert forms the basis of the model, organization—micro0meso0macro. A faculty development
contextualized for health professionals in practice.8 program can be directed at the front-line health care team,
health professional teachers and educators, administrators,
managers, and policy makers.
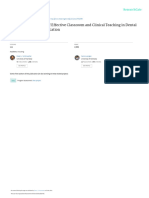
Conceptual Framework As FIGURE 1 illustrates, at an individual and team level,
There are significant conceptual similarities between ef- faculty development can be directed at:
fective faculty development and effective IPE.9,10 Both fo-
cus on the need to effect change at the individual and 1. The attitudes, knowledge, and skills that underpin effec-
organizational levels, are experientially based, and require tive collaborative practice. This can include the beliefs of
expert facilitation and an education and organizational
climate that values these interventions. The IPE literature
describes aligning the micro- ~learner, educator, and learn-
ing context!, meso- ~leadership and administrative!, and
macrofactors ~accreditation and institutional structures!.10
The faculty development literature describes addressing the
individual, instructional, and organizational development
needs.9 To assure success in both contexts, faculty devel-
opers planning IPE programs must be especially aware of
the individual context, the environment, and the system in
which education interventions are being planned.
Setting the Stage for Faculty Development
in Continuing IPE
Before implementing a faculty development program, an ed-
ucation plan adapted to an IPE environment needs to be
considered.10 Effective education design—needs assess-
ment; clear, measurable learning objectives; outcomes-based
curriculum design; interactive teaching methods; and an eval-
uation typology must be adapted for IPE.7
Arguably, the use of reflecting on the readiness of inter-
professional teams to accept a faculty development program FIGURE 1. Individual and team curricular opportunities for faculty devel-
can help direct the planning of the program.11 For example, opment in IPE.
JOURNAL OF CONTINUING EDUCATION IN THE HEALTH PROFESSIONS—29(3), 2009 173
DOI: 10.1002/chp
Silver and Leslie
staff that would enhance or impede collaborative practice Engaging management, ie, nursing and professional prac-
and an examination of the various roles of team members. tice leaders and hospital administrators, in the development
Knowledge-based competencies can include knowledge and delivery process of faculty development sessions can be
about interprofessional learning, group dynamics, the com- an effective method of creating an organizational culture of
petencies of effective teams, and the skills of practitioners IPE. Faculty development interventions directed at manage-
to work and learn collaboratively.15,16 Teams can benefit
ment and administrative leadership can emphasize the link-
from articulating their common competencies, their com-
plementary competencies that distinguish one profession
ages between IPE, quality and systems improvement, and
from another, and their collaborative competencies that are patient safety. The administrative leadership also needs to
necessary to work effectively with others.16 Skills training provide the resources to support the education activities, in-
should focus on effective team communication skills.17 At- cluding appropriate protected time for faculty and staff and
titude building, including respect for each other’s roles and clinical replacement costs, provide incentives to pursue fac-
recognition that teams require work, are important com- ulty development, support mentoring and professional net-
ponents to successful teams.17 works for staff and faculty, and address systems issues that
2. Building capacity for health professional teams to self- would impede a faculty development program.23,24
assess their functioning periodically. This process can be At a government and health policy level, there is con-
assisted with the use of a variety of new tools, including The siderable evidence that IPE will not be sustained without the
Healthy Teams Model and the Team Survey.18,19 The Healthy
necessary policy changes accompanied by core funding to
Teams model was developed with the use of rigorous qual-
itative methodology.18 The Team Survey has 4 subscales.
assist institutions to embed sustainable changes in ways that
This instrument was found to be reliable ~reliability coeffi- health professionals are educated.23 IPE faculty developers
cients between 0.70 and 0.93 were obtained for each sub- need to collaborate with institutional leadership to lobby pol-
scale!. Construct validity measures supported to a large degree icy makers to make these systems-based changes.
the 4 subscales. The tool was tested with the use of a wide
range of specialties, including surgical and medical teams,
management, and service support.
Settings, Formats, and Teaching Strategies
3. Updates on health professional care issues that are relevant Unlike traditional continuing medical education ~CME! that
to the team. The goal of these sessions would be different takes place in conference centers, university seminar rooms,
from traditional forms of multiprofessional CE, where 2 or and hotels, faculty development for continuing IPE should
more health professionals might be learning together but not
ideally take place in situ, in the clinical settings where teams
from and about each other. In continuing IPE, the goal of the
sessions would include how a team works together to de-
work and practice and at times when teams would otherwise
termine how new information or policies and procedures be meeting.8 Leaving the clinical setting may be advanta-
would be adopted by team members individually and by the geous for team learning by limiting interruptions, but prac-
team as a whole. Working together to master the practical tically speaking, this is very difficult for most teams to
“know-how” for sharing patient care is essential for effec- arrange.25
tive team functioning.17 Multiple teaching formats can be considered that vary
4. Quality and systems improvement and patient safety. Op- in intensity and duration.8 A recent systematic review of
timal interprofessional collaboration is a basic competency the faculty development literature revealed that effective
for health systems improvement. Team-based QI projects programs are characterized by 4 key features: ~1! experi-
can be effective methods of enhancing team functioning ential learning, ~2! provision of feedback to participants,
and a particularly effective method of engaging physicians
~3! well-designed interventions based on established prin-
in continuing IPE.20–22 Including this as a part of an in-
terprofessional curriculum requires new conversations and
ciples of teaching and learning, and ~4! diversity of edu-
collaboration between educators and QI and patient safety cational methods.26
leaders in institutions and in the community. Choosing a teaching format depends on the goals of the
5. Leadership and organizational change. Focusing on team- faculty development intervention. A variety of team-based
based learning can facilitate shifts in individuals’ roles on rounds’ formats have been developed that focus on patient
teams and lead to increased interest in leadership and man- care, quality improvement, team functioning, and teaching
agement skills, organizational change and development, and improvement ~TABLE 1!.13,27
conflict management and negotiation.8,13 In addition to the well-established interactive learning
6. Teaching and learning. Addressing general topics on teach- approaches such as case-based workshop 28–30 and team-
ing and learning in a multiprofessional context can enhance building exercises, 31 there are a range of many other
the common bond that ties health professionals to their teach-
approaches.
ing assignments with health professional students and pro-
vide a much valued team-building exercise. Teaching topics
Peer coaching and mentoring in the workplace can pro-
can include curriculum design, interactive teaching, and giv- mote continuing IPE and support for health professionals
ing and receiving feedback.8 Addressing general topics in functioning on teams. It can stimulate critical reflection
teaching can set the stage for faculty development that ad- by orienting practitioners to see, act, and think in new ways
dresses specific topics on teaching in an interprofessional through reflecting on the “languages of practice”—the sets
context.8 of implicit and explicit rules that guide a clinician’s practice.
174 JOURNAL OF CONTINUING EDUCATION IN THE HEALTH PROFESSIONS—29(3), 2009
DOI: 10.1002/chp
Faculty Development for Continuing Interprofessional Education and Collaborative Practice
TABLE 1. Teaching Formats and Strategies for IPE IPE practitioners and scholars.43,44 These groups are often
highly motivated practitioners in the field who come to-
Team-based rounds
gether to generate new knowledge, have a specific inter-
Team-building exercises
est and identity in the field, and share ideas, information,
Case-based workshops tools, and resources with each other.45 A community of prac-
Peer coaching and mentoring tice can be a successful outcome of longitudinal and train-
Web-based learning the-trainer programs where participants have built trust and
Preceptorship training
collaborative relationships over time.43 Communities of prac-
tice can also structure team-based journal clubs and case
Longitudinal programs
conferences, leading to practice changes.46
Communities of practice Teaching tools and resources are needed to support fac-
Teaching tools and resources ulty development programs. These tools can include Power-
Point presentations, 47,48 ice-breakers, games, role-plays, and
IPE cases to stimulate reflection on effective team function-
It is a particularly appropriate method to consider in an ing; DVD trigger tapes to foster discussion on effective fa-
interprofessional context because of the range of different cilitation of IPE;49,50 access to actors that can simulate health
disciplinary languages of practice that exist on teams. professional teams to practice team facilitation and provide
Coaching to promote peer collaboration can enhance learn- feedback; and resources to support program development,
ing in the workplace because it offers opportunities for implementation, and sustainability.51
language change.32,33 Mentoring relationships that are built Following the best practices and principles of program
around the completion of IPE projects in the workplace planning for faculty development for continuing IPE,
and that are based on principles of knowledge translation TABLE 2 describes a program recently offered at the Cen-
may be particularly effective.34,35 tre for Faculty Development in Toronto.
Web-based learning to prepare staff teachers to teach
in an IPE context is being developed.36,37 Faculty devel-
Discussion
opers may be reluctant to use this as a primary teaching
tool because of the nature of IPE teaching where face-to- One of the challenges in organizing faculty development
face contact is so essential. Web-based learning may be programs for continuing IPE is in embedding the principles
best used as a supplement to other teaching formats.8 There of IPE into every aspect of the program, from facilitator
are also developmental issues that need to be considered. preparation, to curricular and program planning, to delivery
Faculty development programs that engage learners over and evaluation processes.
an extended period of time where trust, collaboration, and Effective facilitation in IPE requires significant training
a community of learners is well established may find the with opportunities for practice and feedback. Several themes
uptake of Web-based communication and collaboration to emerged from a recent study 25 on essential features of suc-
be very effective.8 cessful facilitation in IPE. These themes illuminate the need
Preceptorship training programs that focus on preparing for facilitators to demonstrate the ability to be self-aware, to
interprofessional teams to provide interprofessional educa- respect and value differences, to be conscious of the impact
tion to students from multiple disciplines are being devel- of group dynamics on learning, to manage issues around
oped.38 These programs aim to assist staff in designing and power and hierarchy, to plan interprofessional learning, and
implementing a clinically based IPE curriculum for the stu- to integrate the facilitator’s learning philosophy.25 The train-
dents training with them. ing of facilitators should include shadowing experienced
Longitudinal programs in faculty development are well IPE facilitators, cofacilitating and buddy teaching, opportu-
established at many health professional schools.39– 41 Lon- nities to engage in formative evaluation of IPE activities, a
gitudinal programs in CE also have an established evidence mentoring opportunity from an experienced IPE facilitator
base of effectiveness.42 These types of programs are partic- or from a peer group of facilitators, and an opportunity to
ularly suited for educating teachers and scholars in faculty participate in interprofessional program planning.25
development for IPE. Participants from different profes- Using 2 facilitators ~cofacilitation! is very common in
sions from different hospital and community settings have IPE.25 The cofacilitators’ relationship with each other be-
an opportunity to learn from each other, share resources, and comes a potential modeling opportunity for effective col-
potentially collaborate on interinstitutional faculty develop- laboration. This process can be debriefed with participants
ment projects. When a course is extended over time, during the course of a workshop and is an opportunity to use
participants have an opportunity to implement faculty de- a “parallel process” in facilitating to illustrate best practices
velopment programs and return to the group to present their in collaboration. This type of modeling has been noted as a
programs and receive feedback.9 critical factor for the success of an IPE workshop.54
Communities of practice ~COP! in IPE are developing as Program planning and implementation for any IPE ac-
a means of connecting a wider collaborative community of tivity requires special attention to process.51 For example, at
JOURNAL OF CONTINUING EDUCATION IN THE HEALTH PROFESSIONS—29(3), 2009 175
DOI: 10.1002/chp
Silver and Leslie
TABLE 2. University of Toronto IPE Faculty Development Course
Planning and Design
Lessons for Practice
Setting: Centre for Faculty Development, Faculty of Medicine,
University of Toronto.
• The term faculty development should be ex-
Collaborators: Office for Interprofessional Education, the Office for panded to include the professional devel-
Continuing Education and Professional Development, University of
Toronto, and the Toronto Academic Health Sciences Network
opment activities related to faculty’s role on
Partnership. a health care team.
Program goal: To train trainers in IPE faculty development. • Faculty development can play an essential
Participants: Forty health care practitioners0clinical educators with role in enhancing interprofessional collab-
existing knowledge0experience in IPE. oration and for providing continuing IPE.
Planning group: IPE faculty developers, curriculum design expert,
project manager.
• Facilitation skills training is required to de-
liver effective IPE.
Needs assessment: Sample of prospective participants. Curricular goals
aligned with identified needs. • Faculty development for IPE needs to pay
Course format: Longitudinal course was run over a 6-month period in particular attention to process.
2008–2009.
Curriculum design: The course was designed with the use of a
curriculum mapping approach.52 The curriculum was aligned with an
outcomes-based design.
Teaching formats: Large group, small group, online, teleconference call to “process” at every level of program planning and deliv-
“coaching” sessions, interactive exercises, opportunity to apply learning ery. Comprehensive evaluation of faculty development pro-
to own context, joined a pre-existing community of practice in IPE0IPC
grams in IPE is currently needed to provide more direction
postcourse.
to program planning.
Resources: Web-based discussion forum and social networking site used
by participants between face-to-face sessions; resource manual aligned
with each component of the curriculum.
References
Assessment and evaluation: “Realistic approach” used in order to focus
on examining contextual factors associated with the development of the 1. Barr H. Interprofessional education today, yesterday and tomorrow.
program.53 Program outcomes and impact were measured with the use Occasional Paper 1. Health Sciences and Practice Subject Centre, Higher
of an interprofessional outcomes typology.16 At the end of the course, Education Academy; 2002. http:00www.health.heacademy.ac.uk. Ac-
participants demonstrated their expertise by presenting a faculty cessed December 22, 2008.
development project they had completed at their local clinical setting. 2. Harrison AL, English L. Interdisciplinary health assessment of the older
individual: A conceptual framework for curricular integration. J Phys
Ther Educ. 2001;15~2!:17–22.
3. Reeves S. Developing and Delivering Practice-Based Interprofes-
sional. Munich, Germany: VDM Publications; 2008.
the planning committee level, the same normative group dy- 4. Delva D, Jamieson M, Lemieux M. Team effectiveness in academic
namic issues will emerge that facilitators will face when primary health care teams. J Interprof Care. 2008;22~6!:598– 611.
they are facilitating IPE such as forming, storming, norm- 5. Hall P, Weaver L. Interdisciplinary education and teamwork: A long
and winding road. Med Educ. 2001;35:867–875.
ing, and performing.55 Effectively dealing with these stages 6. Reeves S, Zwarenstein M, Goldman J, Barr H, Freeth D, Hammick M,
as they emerge will ensure a successful planning process. Koppel I. Interprofessional education: Effects on professional prac-
One recommended method is to debrief every planning com- tice and health care outcomes. Cochrane Database of Syst Rev. 2008,
mittee meeting. Issue 1.
7. Freeth D, Hammick M, Reeves S, Koppel I, Barr H, Ashcroft J. Ef-
fective Interprofessional Education: Development, Delivery & Evalu-
Conclusions ation. Malden, MA: Blackwell; 2005.
8. Steinert Y. Learning together to teach together: Interprofessional ed-
Faculty development can play an essential role in enhancing ucation and faculty development. J Interprof Care. 2005;1~suppl!:60–75.
interprofessional collaboration and in building capacity for 9. Wilkerson W, Irby D. Strategies for improving teaching practices: A
the provision of continuing IPE. Strategic planning includes comprehensive approach to faculty development. Acad Med. 1998;
73:387–396.
a careful needs assessment, application of a systems ap- 10. Oandasan I, Reeves S. Key elements of interprofessional educa-
proach ~micro0meso0macro! to identifying the target audi- tion. Part 2: Factors, processes and outcomes. J Interprof Care. 2005;
ence of learners, incorporation of principles of effective 1~suppl!:39– 48.
learning, multimodal teaching methods, incorporation of an 11. Halaas G. How to cultivate an environment to advance interprofes-
IPE-based curriculum and an outcomes-based curriculum de- sional education. http:00www.atpm.org0prof_dev0institute08.html. Ac-
cessed December 26, 2008.
sign. Special attention needs to be paid to ensuring the teach- 12. Whitehead C. The doctor dilemma in interprofessional education and
ers of these programs are well trained in IPE facilitation. It care: How and why will physicians collaborate? Med Educ. 2007;
is important to embed the principles of IPE, with attention 41:1010–1016.
176 JOURNAL OF CONTINUING EDUCATION IN THE HEALTH PROFESSIONS—29(3), 2009
DOI: 10.1002/chp
Faculty Development for Continuing Interprofessional Education and Collaborative Practice
13. Curley C, McEachern JE, Speroff T. A firm trial of interdisciplin- 34. Thorndyke LE, Gusic ME, Milner RJ. Functional mentoring: A prac-
ary rounds on the inpatient medical wards: An intervention designed tical approach with multilevel outcomes. J Contin Educ Health Prof.
using continuous quality improvement. Med Care. 1998;36~suppl 8!: 2008;18:157–164.
S4–S12. 35. Straus SE, Graham ID, Taylor M, Lockyer J. Development of a men-
14. Reeves S, Russell A, Zwarenstein M, Kenaszchuk C, Conn LG, Doran torship strategy: A knowledge translation strategy. J Contin Educ Health
D, Sinclair L, Lingard L, Oandasan I, Thorpe K, Austin Z, Beales J, Prof. 2008;28~3!:117–122.
Hindmarsh W, Whiteside C, Hodges B, Nasmith L, Silver I, Miller KL, 36. Centre for the Advancement of Interprofessional Education. IPE links.
Vogwill V, Strauss S. Structuring communication relationships for in- http:00www.caipe.org.uk0resources0ipe-links. Accessed December 22,
terprofessional teamwork ~SCRIPT!: A Canadian initiative aimed at 2008.
improving patient-centred care. J Interprof Care. 2007;21~1!:111–114. 37. Office of Interprofessional Education, University of Toronto. Re-
15. Long S. Primary health care team workshop: Team members’ perspec- sources: Overview. http:00www.ipe.utoronto.ca0resources. Accessed De-
tives. J Adv Nurs. 1996;23:935–941. cember 22, 2008.
16. Barr H, Koppel I, Reeves S, Hammick M, Freeth D. Effective Inter- 38. Office for Interprofessional Education, University of Toronto. The
professional Education: Argument, Assumptions and Evidence. Lon- IMPLC: Super Toolkit; Preceptorship. http:00www.ipe.utoronto.ca0
don, United Kingdom: Blackwell; 2005. initiatives0ipc0implc0preceptorship.html. Accessed December 22, 2008.
17. Sargeant J, Loney E, Murphy G. Effective interprofessional teams: 39. Knight AM, Cole KA, Kern DE, Barker LR, Kolodner K, Wright SM.
“Contact is not enough” to build a team. J Contin Educ Health Prof. Long-term follow-up of a longitudinal faculty development program in
2008;28~4!:228–234. teaching skills. J Gen Intern Med. 2005;20~8!:721–725.
18. Mickan S, Rodger S. Effective health care teams: A model of six char- 40. Gruppen LD, Frohna AZ, Anderson RM, Lowe KD. Faculty develop-
acteristics developed from shared perceptions. J Interprof Care. 2005; ment for educational leadership and scholarship. Acad Med. 2003;
19~4!:358–370. 78~2!:137–141.
19. Millward LJ, Jeffries N. The team survey: A tool for health care service 41. Steinert Y, Naismith L, McLeod P, Conochie L. A teaching scholars
development. J Adv Nurs. 2001;35~2!:276–287. program to develop leaders in medical education. Acad Med. 2003;
20. Ladden MD, Bednash G, Stevens DP, Moore GT. Educating interpro- 78:142–149.
fessional learners for quality, safety and systems improvement. J In- 42. Marinopoulos SS, Dorman T, Ratanawongsa N, Wilson LM, Ashar BH,
terprof Care. 2006;20:497–505. Magaziner JL, Miller RG, Thomas PA, et al. Effectiveness of Continu-
21. Rubenstein LV, Parker LE, Meredith LS, Altschuler A, DePillis E, ing Medical Education. Evidence Report0Technology Assessment No.
Hernandez J, Gordon NP. Understanding team-based quality improve- 149 ~Prepared by the Johns Hopkins Evidence-based Practice Center,
ment for depression in primary care. Health Serv Res. 2002;37~4!: under Contract No. 290-02-0018.! AHRQ Publication No. 07-E006.
1009–1029. Rockville, MD: Agency for Healthcare Research and Quality; 2007.
22. Johnson AW, Potthoff SJ, Carranza L, Swenson HM, Platt CR, Rath- 43. Suter E, Taylor L, Arthur N, Clinton M. Interprofessional education
bun JR. CLARION: A novel interprofessional approach to health care and practice. Creating an interprofessional learning environment through
education. Acad Med. 2006;81~3!:252–256. communities of practice: An alternative to traditional preceptorship.
23. Ullian J, Stritter F. Types of faculty development programs. Fam Med. http:00www.interprofessionalalberta.ca. Accessed December 23, 2008.
1997;29:237–241. 44. Office for Interprofessional Education, University of Toronto. IPC com-
24. Reeves S, Freeth D, Glen S, Leiba T, Berridge EJ, Herzberg J. Deliv- munity of practice. http:00www.ipe.utoronto.ca0initiatives0ipc0cop.html.
ering practice-based interprofessional education to community mental Accessed December 23, 2008.
health teams: Understanding some key lessons. Nurs Educ Pract. 45. Wenger, E. Communities of Practice: Learning, Meaning, and Identity.
2006;6~5!:246–253. Cambridge, United Kingdom: Cambridge University Press; 1998.
25. Howkins E, Bray J, eds. Preparing for Interprofessional Teaching: 46. Price DW, Felix KG. Journal clubs and case conferences: From aca-
Theory and Practice. Oxford, United Kingdom: Radcliffe; 2008. demic tradition to communities of practice. J Contin Educ Health Prof.
26. Steinert Y, Mann K, Centeno A, Dolmans D, Spencer J, Gelula M, 2008;28~3!:123–130.
Prideaux D. A systematic review of faculty development initiatives 47. Office for Interprofessional Education, University of Toronto. Re-
designed to improve teaching effectiveness in medical education: BEME sources—presentations. http:00ipe.utoronto.ca0resources0presentation.
Guide No. 8. Med Teach. 2006;28~6!:497–526. html. Accessed December 23, 2008.
27. Lye PS, Simpson DE, Wendelberger KJ, Bragg DS. Clinical teaching 48. Office for Interprofessional Education, University of Minnesota. http:00
rounds: A case-oriented faculty development program. Arch Pediatr www.ipe.umn.edu0who0archived.shtml. Accessed December 23, 2008.
Adolesc Med. 1998;152:293–295. 49. Office for Interprofessional Education, University of Toronto. Re-
28. Delva D, Tomalty L, Macrae K, Payne P, Plain E, Rowe W. A new sources—DVD tools. http:00ipe.utoronto.ca0resources0dvd.html. Ac-
model for collaborative continuing professional development. J Inter- cessed December 23, 2008.
prof Care. 2008;22~suppl 1!:91–100. 50. Moaveni A, Nasmith L, Oandasan I. Building best practice in faculty
29. Hall P, Weaver L, Hupe D, Seely JF. Community-based palliative care development for interprofessional collaboration in primary care. J In-
education: Can it improve care of the terminally ill? Acad Med. 1999; terprof Care. 2008;22~suppl 1!:80–82.
74~suppl 10!:S105–S107. 51. Reeves S, Goldman J, Oandasan I. Key factors in planning and im-
30. Mann KV, Viscount PW, Cogdon A, Davidson K, Langille DB, Mac- plementing interprofessional education in health care settings. J Allied
cara ME. Multidisciplinary learning in continuing professional educa- Health. 2007;36~4!:231–234.
tion: The Heart Health Nova Scotia experience. J Contin Educ Health 52. Harden RM. AMEE Guide No. 21: Curriculum mapping: A tool for
Prof. 1996;16:50– 60. transparent and authentic teaching and learning. Med Teach. 2001;
31. The Interprofessional Network of British Columbia. The UBC LEGO® 23~2!:123–137.
Exercise. http:00www.in-bc.ca0resources0lego.php. Accessed Decem- 53. Pawson R, Tilley M. Realistic Evaluation. London, United Kingdom:
ber 22, 2008. Sage; 1997.
32. Phelan AM, Barlow CA, Iversen S. Occasioning learning in the work- 54. Smith S, Karban K. Tutor experiences of developing an interprofes-
place: The case of interprofessional peer collaboration. J Interprof Care. sional learning ~IPL! program in higher education. Response. 2008;
2006;20~4!:415– 424. 4~1!:1–13. http:00www2.derby.ac.uk 0response0index2.php?option⫽
33. Office of Interprofessional Education, University of Toronto. The com_content&do_pdf⫽1&id⫽24. Accessed April 16, 2009.
IMPLC: Super Toolkit. Available at: http:00www.ipe.utoronto.ca0 55. Tuckman BW. Developmental sequence in small groups. Psychol Bull.
initiatives0ipc0implc0supertoolkit.html. Accessed December 22, 2008. 1965;63:384–399.
JOURNAL OF CONTINUING EDUCATION IN THE HEALTH PROFESSIONS—29(3), 2009 177
DOI: 10.1002/chp
You might also like
- Foundations of Osteopathic Medicine Philosophy Science Clinical Applications and Research 4th Edition Ebook PDFDocument62 pagesFoundations of Osteopathic Medicine Philosophy Science Clinical Applications and Research 4th Edition Ebook PDFjerry.graves681100% (54)
- Family Health Care Nursing - Rowe-Kaakinen, Joanna, Padgett-Coehlo, Deborah, Steele, Rose PDFDocument649 pagesFamily Health Care Nursing - Rowe-Kaakinen, Joanna, Padgett-Coehlo, Deborah, Steele, Rose PDFUmi Marfungatun Mudrikah100% (14)
- Iso 45001 ExamDocument15 pagesIso 45001 ExamAhmed NABIL67% (12)
- Part 1 SAQs Specimen QuestionsDocument79 pagesPart 1 SAQs Specimen Questionsخولة رشيد العيسى100% (2)
- Obe PDFDocument6 pagesObe PDFjaycee_evangelistaNo ratings yet
- Station 1 - 12 Tips For Education Needs Assessments Through An Interprofessional LensDocument4 pagesStation 1 - 12 Tips For Education Needs Assessments Through An Interprofessional LensAida TantriNo ratings yet
- A Framework For The Design ImplementationDocument6 pagesA Framework For The Design ImplementationPATRICIA POLETTONo ratings yet
- Interprofessional Educationand CollaborationDocument7 pagesInterprofessional Educationand CollaborationnersrosdianaNo ratings yet
- Rw-Omj-D-18-00175 (05C)Document6 pagesRw-Omj-D-18-00175 (05C)nersrosdianaNo ratings yet
- 02 - Soemantri Et AlDocument8 pages02 - Soemantri Et Alany fitriyaniNo ratings yet
- Interprofessional Collaboration and Education.26Document8 pagesInterprofessional Collaboration and Education.26sans9No ratings yet
- Actividades Profesionales ConfiablesDocument6 pagesActividades Profesionales ConfiablesOscar F RojasNo ratings yet
- Levett-Jones Et Al-2018-Journal of Nursing Scholarship1Document10 pagesLevett-Jones Et Al-2018-Journal of Nursing Scholarship1Nande BandeNo ratings yet
- Interprofessional Education For Collaborative, Patient-Centred PracticeDocument7 pagesInterprofessional Education For Collaborative, Patient-Centred PracticeWahyu WijayantoNo ratings yet
- Exploring Faculty Preparedness and Capability For Interprofessional LearningDocument1 pageExploring Faculty Preparedness and Capability For Interprofessional LearningSadashiv RahaneNo ratings yet
- Research PresentationDocument14 pagesResearch PresentationCeeNo ratings yet
- New Paradigm For CME - JCEHP Sep 2011Document8 pagesNew Paradigm For CME - JCEHP Sep 2011Daniel GuineeNo ratings yet
- Henzi Etal (2006) - Perspectives Dental Students About Clinical EducationDocument17 pagesHenzi Etal (2006) - Perspectives Dental Students About Clinical EducationMiguel AraizaNo ratings yet
- Faculty Development For TeachingDocument10 pagesFaculty Development For TeachingRochelle Edquilang CapistranoNo ratings yet
- Review Article: Advanced Practice Nursing Education: Challenges and StrategiesDocument9 pagesReview Article: Advanced Practice Nursing Education: Challenges and StrategiesluNo ratings yet
- Development and Experimental Results of Outcomes-Based Nursing ProgramDocument6 pagesDevelopment and Experimental Results of Outcomes-Based Nursing ProgramIJAR JOURNALNo ratings yet
- Importance and Purposes of Research: Instruction: Answer Comprehensively and ExtensivelyDocument3 pagesImportance and Purposes of Research: Instruction: Answer Comprehensively and ExtensivelyKarl Kiw-isNo ratings yet
- Interprofessional Collaboration: Three Best Practice Models of Interprofessional EducationDocument5 pagesInterprofessional Collaboration: Three Best Practice Models of Interprofessional Educationna5649No ratings yet
- Interprofessional Education For Collaborative, Patient-Centred PracticeDocument7 pagesInterprofessional Education For Collaborative, Patient-Centred PracticeAnonymous u5UPeiWpNo ratings yet
- International Journal of Nursing SciencesDocument5 pagesInternational Journal of Nursing SciencesWahyu Phaling FienterNo ratings yet
- Sicometrik ICP IndonesiaDocument10 pagesSicometrik ICP IndonesiaUchi SuhermanNo ratings yet
- Continuando La Educacion Medica para Los Practicantes Generales - Un Formato para PracticasDocument6 pagesContinuando La Educacion Medica para Los Practicantes Generales - Un Formato para PracticasAnonymous 3MPClbaCDNo ratings yet
- Content ServerDocument11 pagesContent ServerMona AL-FaifiNo ratings yet
- Medical Education - 2005 - McNairDocument9 pagesMedical Education - 2005 - McNairISABEL BUENO SANTOS MENEZESNo ratings yet
- 1 PBDocument7 pages1 PBinti.makmur.lgNo ratings yet
- Interprofessional Education PDFDocument3 pagesInterprofessional Education PDFRobert MontgomeryNo ratings yet
- Continuing Education in Nursing: Ursing DucationDocument17 pagesContinuing Education in Nursing: Ursing Ducationsaleha sultana100% (1)
- Interprofessional Collaboration Three Best Practice Models of Interprofessional EducationDocument11 pagesInterprofessional Collaboration Three Best Practice Models of Interprofessional Educationgenta01100% (1)
- Foreign Literature FinalsDocument14 pagesForeign Literature FinalsAnghel CruzNo ratings yet
- Developing Skills Learning in Obstetric Nursing: Approaches Between Theory and PracticeDocument7 pagesDeveloping Skills Learning in Obstetric Nursing: Approaches Between Theory and PracticerupaNo ratings yet
- Structured Mentoring StrategiesDocument31 pagesStructured Mentoring Strategiesrandy gallegoNo ratings yet
- Interprofessional Education Esmarliza K. Tacud-Luzon, MDDocument3 pagesInterprofessional Education Esmarliza K. Tacud-Luzon, MDRaphael MiguelNo ratings yet
- Spring 09 NewsletterDocument13 pagesSpring 09 NewsletterAnnie DanielNo ratings yet
- CHAPTER 1 Action ResearchDocument30 pagesCHAPTER 1 Action ResearchmatetbongNo ratings yet
- SJMPS - 38896 906 1Document11 pagesSJMPS - 38896 906 1danicaattabanNo ratings yet
- Quality and Safety Curricula in NursingDocument5 pagesQuality and Safety Curricula in NursingAmeng GosimNo ratings yet
- Submit Due 9.12Document11 pagesSubmit Due 9.12Are HidayuNo ratings yet
- Medical Education in Pulmonary, Critical Care, and Sleep Medicine: Advanced Concepts and StrategiesFrom EverandMedical Education in Pulmonary, Critical Care, and Sleep Medicine: Advanced Concepts and StrategiesPatricia A. KritekNo ratings yet
- Interprofessional Collaboration Three Best Practice Models of Interprofessional EducationDocument11 pagesInterprofessional Collaboration Three Best Practice Models of Interprofessional Educationanzila widyaNo ratings yet
- NURS FPX 6614 Assessment 2 Enhancing Performance As Collaborators in CareDocument7 pagesNURS FPX 6614 Assessment 2 Enhancing Performance As Collaborators in Carefarwaamjad771No ratings yet
- Ipe and Ipc Assignment Part 1Document17 pagesIpe and Ipc Assignment Part 1api-547401454No ratings yet
- Research in Continuing EducationDocument25 pagesResearch in Continuing EducationArchana VermaNo ratings yet
- Role of Medical Education in Cultivating LifelongDocument4 pagesRole of Medical Education in Cultivating LifelongRudolph SunnydaysNo ratings yet
- Students Perceptions of Effective Classroom and CDocument13 pagesStudents Perceptions of Effective Classroom and Ckrishnabhagwat30No ratings yet
- Naskah Publikasi FixDocument14 pagesNaskah Publikasi FixSabet LilyNo ratings yet
- The Core Curriculum and Integration in Medical Education: Nikoo Yamani, Masoumeh RahimiDocument5 pagesThe Core Curriculum and Integration in Medical Education: Nikoo Yamani, Masoumeh RahimiDoctorRonZ7No ratings yet
- Nu708 m7 - Ebp Perspective SustainabilityDocument8 pagesNu708 m7 - Ebp Perspective Sustainabilityapi-577441503No ratings yet
- Improving Assessment in Dental Education Through A Paradigm of Comprehensive Care: A Case ReportDocument13 pagesImproving Assessment in Dental Education Through A Paradigm of Comprehensive Care: A Case ReportfidelbustamiNo ratings yet
- Interprofessional Collaboration and Education.26 PDFDocument15 pagesInterprofessional Collaboration and Education.26 PDFBrajakson SiokalNo ratings yet
- Interprofessional Education - The Way Forward in Health ProfessionDocument2 pagesInterprofessional Education - The Way Forward in Health ProfessionJLatriece Elizabeth CedeñoNo ratings yet
- Measuring Clinical Reasoning and Interprofessional AttitudesDocument6 pagesMeasuring Clinical Reasoning and Interprofessional AttitudesVizaNo ratings yet
- Apta Combined Sections Meeting 2023 AbstractDocument1 pageApta Combined Sections Meeting 2023 Abstractapi-738548992No ratings yet
- IMPACT OF EXPER-WPS OfficeDocument10 pagesIMPACT OF EXPER-WPS Officepash blessingsNo ratings yet
- Dimensions of Learning Organizations Questionnaire (DLOQ) in A Low-Resource Health Care Setting in NepalDocument8 pagesDimensions of Learning Organizations Questionnaire (DLOQ) in A Low-Resource Health Care Setting in Nepalsapit90No ratings yet
- Nurse Managers' Responsive Coaching To Facilitate Staff Nurses' Clinical Skills Development in Public Tertiary HospitalDocument10 pagesNurse Managers' Responsive Coaching To Facilitate Staff Nurses' Clinical Skills Development in Public Tertiary Hospitalvan royeNo ratings yet
- Assessment of Learning NeedsDocument4 pagesAssessment of Learning NeedsRhonaJoyNo ratings yet
- UA OMSE Med/Ed Enews v3 No. 01 (AUG 2014)Document10 pagesUA OMSE Med/Ed Enews v3 No. 01 (AUG 2014)KC Spear Ellinwood, former Director Instructional DevelopmentNo ratings yet
- Chapter 1 3 ResearchDocument26 pagesChapter 1 3 ResearchAb Staholic BoiiNo ratings yet
- A Guide to Medical Teaching and Learning Training of the Trainers (Tot): In the View of the Learner-Centered Learning ModelFrom EverandA Guide to Medical Teaching and Learning Training of the Trainers (Tot): In the View of the Learner-Centered Learning ModelNo ratings yet
- 1 s2.0 S1521689614000044 PDFDocument21 pages1 s2.0 S1521689614000044 PDFAida TantriNo ratings yet
- Pain in Terminally IllDocument29 pagesPain in Terminally IllAida Tantri100% (1)
- LA CraniotomyDocument8 pagesLA CraniotomyAida TantriNo ratings yet
- 2216 2221 PDFDocument6 pages2216 2221 PDFAida TantriNo ratings yet
- Interprofessional EducationDocument12 pagesInterprofessional EducationAida TantriNo ratings yet
- Withdrawing WitholdingDocument6 pagesWithdrawing WitholdingAida TantriNo ratings yet
- Uncommon Complications of Spinal Anaesthesia - AnesthesiaworldDocument14 pagesUncommon Complications of Spinal Anaesthesia - AnesthesiaworldAida TantriNo ratings yet
- Failed Spinal ChloroprocaineDocument4 pagesFailed Spinal ChloroprocaineAida TantriNo ratings yet
- Tsui CSF Lavage CJA 14Document4 pagesTsui CSF Lavage CJA 14Aida TantriNo ratings yet
- Accidental Epidural Injection of Atropine: Case ReportDocument2 pagesAccidental Epidural Injection of Atropine: Case ReportAida TantriNo ratings yet
- Spinal ToxicityDocument12 pagesSpinal ToxicityAida Tantri0% (1)
- NURS FPX 6107 Assessment 1 Curriculum Overview, Framework, and AnalysisDocument5 pagesNURS FPX 6107 Assessment 1 Curriculum Overview, Framework, and Analysisjoohnsmith070No ratings yet
- Pednekar S S PDFDocument14 pagesPednekar S S PDFAbubakar MokarimNo ratings yet
- Notes Nurse PolicyDocument6 pagesNotes Nurse PolicyChristian HawthorneNo ratings yet
- BIANNUAL CONGRESS OF HOMOEOPATHIC ASSOCIATION OF SOUTH AFRICA (HSA) 2014: A REPORT (Prepared From REPORT: HSA CONGRESS 2014Document6 pagesBIANNUAL CONGRESS OF HOMOEOPATHIC ASSOCIATION OF SOUTH AFRICA (HSA) 2014: A REPORT (Prepared From REPORT: HSA CONGRESS 2014Homoeopathic PulseNo ratings yet
- Clinical Guideline For The Evaluation and Management of Chronic Insomnia in AdultsDocument18 pagesClinical Guideline For The Evaluation and Management of Chronic Insomnia in AdultsDeTe Punya Map100% (1)
- IDC 213 01 Introduction To Evidence-Based Medicine PDFDocument5 pagesIDC 213 01 Introduction To Evidence-Based Medicine PDFFort SalvadorNo ratings yet
- 2021 Philippine Guidelines On PHEx Phase 1Document148 pages2021 Philippine Guidelines On PHEx Phase 1Famed residentsNo ratings yet
- CephalgiaDocument24 pagesCephalgiaNurlita Ranti YulistyaNo ratings yet
- JBI - Wound ManagementDocument4 pagesJBI - Wound ManagementBethanyNo ratings yet
- Bab 1-5 Manajemen HcuDocument7 pagesBab 1-5 Manajemen Hcuretno indriyaniNo ratings yet
- Eng - PDF JsessionidDocument276 pagesEng - PDF JsessionidWilliam AdiputraNo ratings yet
- FCPS-II PaediatricsDocument41 pagesFCPS-II Paediatricsharoon100% (1)
- CBCT in Orthodontics: Assessment of Treatment Outcomes and Indications For Its UseDocument19 pagesCBCT in Orthodontics: Assessment of Treatment Outcomes and Indications For Its Useelena dinovskaNo ratings yet
- MSC - Medical Surgical Sub Specialty Cardiovascular Thoracic Nursing PDFDocument44 pagesMSC - Medical Surgical Sub Specialty Cardiovascular Thoracic Nursing PDFAlma Susan100% (4)
- Evidence Based PracticesDocument5 pagesEvidence Based Practicesapi-527787868No ratings yet
- NCM 109 Course Syllabus Ay 2022 2023Document17 pagesNCM 109 Course Syllabus Ay 2022 2023ShainaChescaEvans100% (1)
- Chairside Guide Nonrestorative Treatments For Carious Lesions On Primary TeethDocument2 pagesChairside Guide Nonrestorative Treatments For Carious Lesions On Primary TeethMellisa FanNo ratings yet
- DQI and Use Mentor - Oct 2022Document3 pagesDQI and Use Mentor - Oct 2022Amenti TekaNo ratings yet
- Dissertation On Healing Architecture in Hospital DesignDocument114 pagesDissertation On Healing Architecture in Hospital DesignDipesh Anand86% (44)
- BridgeSpan Speech Services Guidelines - V102019 - Eff03012019 - Pub10222018 PDFDocument245 pagesBridgeSpan Speech Services Guidelines - V102019 - Eff03012019 - Pub10222018 PDFMariel Salazar100% (2)
- Call Grand Master +27734818506 HOW TO JOIN 666 ILLUMINATI SECRET SOCIETY FOR MONEY IN USA, UK, Canada, Spain, Italy, China, Hong Kong FreestateDocument176 pagesCall Grand Master +27734818506 HOW TO JOIN 666 ILLUMINATI SECRET SOCIETY FOR MONEY IN USA, UK, Canada, Spain, Italy, China, Hong Kong FreestateJohn RichNo ratings yet
- Ead-510 Field Experience BDocument3 pagesEad-510 Field Experience Bapi-502057756No ratings yet
- Kuliah FeedingDocument41 pagesKuliah Feedingfatihatul kamilahNo ratings yet
- Arksey and OMalley - 2005 - Scoping StudiesDocument17 pagesArksey and OMalley - 2005 - Scoping StudiesCBNo ratings yet
- Nurs FPX 4030 Assessment 1 Locating Credible Databases and ResearchDocument5 pagesNurs FPX 4030 Assessment 1 Locating Credible Databases and Researchjoohnsmith070No ratings yet
- Nursing Philosophy PaperDocument6 pagesNursing Philosophy PaperDanielle AalderinkNo ratings yet