Professional Documents
Culture Documents
Emerging Evidence: Smoking, Vaping, and COVID-19
Emerging Evidence: Smoking, Vaping, and COVID-19
Uploaded by
feb_wulanOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Emerging Evidence: Smoking, Vaping, and COVID-19
Emerging Evidence: Smoking, Vaping, and COVID-19
Uploaded by
feb_wulanCopyright:
Available Formats
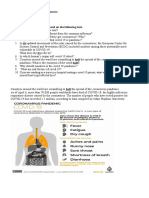
Smoking, Vaping, and COVID-19
Emerging Evidence
• COVID-19 attacks the lungs and behaviors that weaken the lungs put individuals at greater
Smokers and risk. The harmful impact of smoking on the lungs is well-documented, and there is evidence
vapers may be that e-cigarette use (vaping) can also harm lung health.
at greater risk • It is not surprising that there is mounting concern among leading public health
organizations and experts that smokers face a higher risk for severe illness from COVID-19.
for severe illness As vaping impacts the immune system and can harm lung health, e-cigarette users may also
when face higher risks. We urge all smokers and e-cigarette users to quit in order to protect their
health, especially at this critical time.
confronted with
• In several countries, false information has been spread that smoking or vaping will protect
COVID-19. tobacco users from COVID-19. This information is false and dangerous.
Smoking Harms Lung Health
Smoking damages the lungs and negatively impacts Smoking causes lung cancer, chronic obstructed
how well they function. pulmonary disease (COPD), asthma, and other
• The lungs of smokers produce more and thicker mucus respiratory diseases.
than the lungs of nonsmokers. This mucus is both • The lung diseases caused by smoking occur among
difficult to remove and prone to infection.1 smokers and non-smokers exposed to tobacco smoke.1
• Smoking also inhibits and eventually destroys the cilia, • The lung diseases caused by smoking are among
the small hair-like projections on the surfaces of cells the underlying conditions known to place people at
in the breathing airway that brush away dirt and other greater risk of more severe illness when diagnosed
particles to protect the lungs.2 with COVID-19.3,4
• Exposure to cigarette smoke causes airway
inflammation. This inflammation and the resulting scar
tissue damage the membranes that pass oxygen to the
bloodstream.1
Smoking Impairs Immunity
Smoking harms the immune system and, therefore, Smoking increases susceptibility to respiratory
the body’s ability to fight infection. This impairment infections.1
occurs in two different ways. • There is overwhelming evidence that people who
• The chemicals in tobacco smoke suppress the activity smoke are at higher risk of getting viral and bacterial
of different types of immune cells that are involved in respiratory infections:
general and targeted immune responses.1 o Smokers have two to four times the risk of pneumo-
• The components in tobacco smoke also over-acti- coccal diseases like pneumonia and meningitis than
vate immune cells, which are recruited to combat the nonsmokers.
toxins that are inhaled and their effects. Over time, this o Influenza risk is twice as high in smokers compared
pro-inflammatory effect can damage different tissues with nonsmokers.
throughout the body and result in a number of chron-
o Smokers have about twice the risk of contracting
ic diseases including various autoimmune diseases,
tuberculosis.6
cardiovascular disease, cancer, diabetes, and chronic
obstructive pulmonary disease (COPD.)1,5 In light of smoking’s negative impacts on the immune
system and smokers’ increased susceptibility to other
respiratory infections, it is likely that smoking is associated
with increased risk of infection with the novel coronavirus.
WWW.TOBACCOFREEKIDS.ORG MAY 2020
SMOKING, VAPING, AND COVID-19: EMERGING EVIDENCE
The World Health Organization has emphasized that have raised concerns that waterpipe use, which often
smoking requires repeated hand-to-face motion, which involves using shared mouthpieces in social settings, may
increases the risk of viral transmission from fingers and contribute to the spread of the novel coronavirus.8,9
cigarettes to the mouth.3,7 Along the same lines, many
Smoking is a Leading Risk Factor for Noncommunicable Diseases (NCDs)
• Smoking causes cancer, COPD and other lung • The World Health Organization asserts that people
diseases, cardiovascular disease, and diabetes.1 with NCDs appear to be at higher risk for experiencing
• Conditions like respiratory and cardiovascular diseases more severe forms of COVID-19.3
increase risk of severe disease in patients infected with
other known coronaviruses, including those that cause
MERS and SARS.10
According to the WHO, available research suggests that smokers are likely at greater risk of
developing severe disease and dying from COVID-19,11 including the following two studies:
■ One of the largest early studies investigating ■ A recently published study analyzed data from
associations between smoking and COVID-19 8,910 patients hospitalized with COVID-19,
examined clinical outcomes from 1,099 patients collected from 169 hospitals across 11 countries
with lab-confirmed COVID-19 infection from 552 in Asia, Europe and North America. The authors
hospitals across China. This study reports that controlled for age and sex, two factors that in-
12.4% of current smokers died, were admitted fluence smoking rates. They found that smoking
to an intensive care unit or required mechanical was among the factors independently associated
ventilation, compared with 4.7% of nonsmokers. with in-hospital death; 9.4% of smokers hospital-
Along similar lines, 21.2% of current smokers ized with COVID-19 died, as opposed to 5.6% of
had severe symptoms, as opposed to 14.5% of former smokers or nonsmokers. Smokers in the
nonsmokers.12 study were 1.79 times more likely to die in the
hospital of COVID-19 than former smokers or
nonsmokers.13
Vaping Impacts Health
Early studies into the effects of e-cigarette use show compromising the lungs ability to fight infection.17
detrimental effects on the lungs, as well as the immune Along these lines, a recent study found that exposure
and cardiovascular systems. This research, considered to e-cigarette emissions reduced the likelihood of
alongside emerging evidence that patients with recovery from influenza.19 Additionally, nicotine, a
compromised respiratory, immune, and cardiovascular critical component of e-cigarette aerosol, is known to
systems are at higher risk for severe COVID-19 infection, suppress immune function throughout the body.1
has led health authorities and others to caution against • Cardiovascular System: Short-term e-cigarette use
using e-cigarettes, particularly amidst the coronavirus can reduce the function of cardiovascular tissue that
pandemic. 14,15,16 controls blood flow.20,21,22,23 Although it is too early
• Lungs: Exposure to e-cigarette aerosol has negative to draw conclusions on the long-term effects of
effects on various types of lung cells, including those e-cigarette use, this dysfunction is commonly observed
involved in maintaining normal, healthy lung function.17 early in the development of cardiovascular disease.24
o Additionally, the potential for e-cigarette use to
damage the lungs was highlighted by the outbreak Researchers have not yet found a direct link between
of vaping-induced lung disease seen primarily in the e-cigarette use and likelihood of COVID-19 infection or
U.S. in 2019. Although that outbreak is fading, re- severity of disease in those who are infected. However,
cent analysis suggests that inhalation of known and this does not mean that links do not exist, and it is
unknown toxic chemicals in e-cigarette emissions will reasonable to assume that people who use e-cigarettes
continue to cause lung damage.18 may be at greater risk for severe illness when confronted
with COVID-19.
• Immune Response: E-cigarette aerosol also inhibits
and can kill several kinds of immune cells in the lungs,
WWW.TOBACCOFREEKIDS.ORG MAY 2020
SMOKING, VAPING, AND COVID-19: EMERGING EVIDENCE
• As countries around the world work to limit the impact of the coronavirus,
We urge all smokers there has never been a better or more urgent time for people to quit
and e-cigarette smoking and vaping.
users to make every • In order to protect their health and reduce their risk of severe COVID-19
symptoms, we urge all those who smoke or vape to quit. Research has
effort to quit. shown that quitting smoking rapidly improves lung function.
Quitting Smoking Rapidly Improves Lung Health
Quitting smoking improves lung function, immune • Quitting smoking lowers blood pressure and heart rate
response, and cardiovascular health, putting former almost immediately. Twenty-four hours after quitting
smokers in a stronger position to fight severe infections smoking, the risk of heart disease begins to decline.26
like COVID-19.
There has never been a better time to quit smoking.
• Within two weeks of quitting smoking, lung function According to Dr. Tedros Adhanom Ghebreyesus, Director
improves.25 Cilia, the hair-like projections that protect General of the World Health Organization, “quitting
the lungs, regrow and return to normal activity levels, tobacco is one of the best things any person can do for
making it easier to fight infection.26 Many smokers their own health.” 28
begin to notice a decrease in respiratory symptoms
like coughing and shortness of breath within one
month of quitting smoking.27
• After quitting, the immune inflammation caused by
smoking decreases, white blood cell counts return
to normal, and immune function improves.26 Rates
of respiratory infections, including pneumonia and
bronchitis, are significantly lower among former
smokers than current smokers.27
REFERENCES
1. U.S. Department of Health and Human Services. The Health Consequences of Smoking: 50 Years of Progress. A Report of the Surgeon General. Atlanta, GA:
U.S. 2014. 2. U.S. Department of Health and Human Services. How Tobacco Smoke Causes Disease: The Biology and Behavioral Basis for Smoking-Attributable
Disease: A Report of the Surgeon General. Atlanta, GA: U.S. 2010. 3. World Health Organization (WHO). Information Note: COVID-19 and NCDs. Published
23 March 2020. 4. U.S. Centers for Disease Control and Prevention (CDC). Morbidity and Mortality Weekly Report: Preliminary Estimates of the Prevalence of
Selected Underlying Health Conditions Among Patients with Coronavirus Disease 2019 — United States, February 12–March 28, 2020. 69(13);382–386. 3 April,
2020. 5. Pahwa R, Goyal A, Bansal P, et al. Chronic Inflammation. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020. 6. Arcavi L and Beno-
witz NL. Cigarette Smoking and Infection. Arch Intern Med. 2004;164(20):2206-2216. 7. Simons D, Perski O, Brown J. Covid-19: The role of smoking cessation
during respiratory virus epidemics. British Medical Journal: Opinion. Published 20 March 2020. 8. WHO Regional Office of the Eastern Mediterranean. Tobacco
and waterpipe use increases the risk of suffering from COVID-19. Tobacco Free Initiative. 2020. 9. Kalan et al. Waterpipe Tobacco Smoking: A Potential Conduit
of COVID-19. Tobacco Control: Blog. Published 23 March, 2020. 10. Volkow ND. COVID-19: Potential Implications for Individuals with Substance Use Disorders.
Nora’s Blog: National Institute for Drug Abuse. Published 6 April, 2020. 11. WHO. WHO statement: Tobacco use and COVID-19. Published 11 May, 2020. 12.
Guan W, Ni Z, Hu Y, et al. Clinical Characteristics of Coronavirus Disease 2019 in China. N Engl J Med 2020. 13. Mehra MR, et al. Cardiovascular Disease, Drug
Therapy, and Mortality in Covid-19. N Engl J Med 2020. 14. Volkow ND. Collision of the COVID-19 and Addiction Epidemics. Ann Intern Med. 2020; [Epub ahead
of print 2 April 2020]. 15. Glantz SA. Reduce your risk of serious lung disease caused by corona virus by quitting smoking and vaping. UCSF Center for Tobacco
Control Research and Education: Blog. Accessed 13 April, 2020. 16. Mayo Clinic. What smokers need to know about coronavirus. Blog post by Vivien Williams.
Published 24 March, 2020. 17. Gotts JE, et al., What are the respiratory effects of e-cigarettes? British Medical Journal. 2019, 366:l5275. 18. MB Stanbrook and
JM Drazen. Vaping-Induced Lung Disease — A Look Forward by Looking Back. N Engl J Med 2020; 382:1649-1650 19. Madison MC, et al. Electronic cigarettes
disrupt lung lipid homeostasis and innate immunity independent of nicotine. J Clin Invest. 2019;129(10):4290–4304. 20. U.S. National Academies of Sciences,
Engineering, and Medicine. Public health consequences of e-cigarettes. Washington, DC: The National Academies Press. 2018. 21. Caporale A, et al. Acute
Effects of Electronic Cigarette Aerosol Inhalation on Vascular Function Detected at Quantitative MRI. Radiology. 2019 :190562. 22. Kuntic M, et al. Short-term
e-cigarette vapour exposure causes vascular oxidative stress and dysfunction: evidence for a close connection to brain damage and a key role of the phagocytic
NADPH oxidase (NOX-2). European Heart Journal, ehz772. 2019. 23. Rashid et al. Chronic E-cigarette Users Exhibit Abnormal Myocardial Blood Flow with
Stress. American Heart Association Annual Scientific sessions. Circulation. 2019; 140: A15018. 24. Bonetti PO, et al. Endothelial Dysfunction: A Marker of Athero-
sclerotic Risk. Arteriosclerosis, Thrombosis, and Vascular Biology. 2003;23:168–175 25. National Institutes of Health, National Cancer Institute, Smokefree.gov,
What Happens When You Quit Smoking?, viewed 30 March 2020. 26. National Cancer Institute. “Benefits of Quitting.” 27. U.S. Department of Health and Human
Services. Smoking Cessation. A Report of the Surgeon General. Atlanta, GA: U.S. 2020. Page 311. 28. WHO. “WHO launches new report on the global tobacco
epidemic.” Published 26 July 2019. News release. Geneva/Rio de Janerio.
WWW.TOBACCOFREEKIDS.ORG MAY 2020
You might also like
- Lugols Iodine Dosage Table PDFDocument4 pagesLugols Iodine Dosage Table PDFjohnnyorithro91% (11)
- Icu GuidebookDocument43 pagesIcu Guidebookdrimran570100% (5)
- Respiratory DisordersDocument17 pagesRespiratory DisordersVallesh ShettyNo ratings yet
- Reduce Your Risk of Serious Lung Disease Caused by Corona Virus by Quitting Smoking and Vaping - Center For Tobacco Control Research and EducationDocument13 pagesReduce Your Risk of Serious Lung Disease Caused by Corona Virus by Quitting Smoking and Vaping - Center For Tobacco Control Research and EducationJesse DanzigNo ratings yet
- COVID-19 With Respiratory System: AbstractDocument7 pagesCOVID-19 With Respiratory System: AbstractOsama AhmedNo ratings yet
- Lung Infections Related To SmokingDocument27 pagesLung Infections Related To SmokingAyman FatimaNo ratings yet
- WHF Policy Brief On Tobacco CVD COVID 19Document28 pagesWHF Policy Brief On Tobacco CVD COVID 19rwessels127No ratings yet
- Aaa PDFDocument318 pagesAaa PDFAj Christian Lacuesta IsipNo ratings yet
- Lung Infections in Smokers: By: Ayman FatimaDocument21 pagesLung Infections in Smokers: By: Ayman FatimaAyman FatimaNo ratings yet
- Fs Smoking Respiratory 508 PDFDocument2 pagesFs Smoking Respiratory 508 PDFRoberta BotezNo ratings yet
- COVID-19 Pandemic and Tobacco Use in IndiaDocument3 pagesCOVID-19 Pandemic and Tobacco Use in IndiaKmNo ratings yet
- Smoking CessationDocument14 pagesSmoking CessationRaghuram MiryalaNo ratings yet
- B. Answer The Questions Based On The Following Text.: A. Read The PPT and Do The ExerciseDocument3 pagesB. Answer The Questions Based On The Following Text.: A. Read The PPT and Do The ExerciseHeldaNatasyaNo ratings yet
- S Moking and COVID-19: Is There A S Moker's Paradox in COVID-19?Document6 pagesS Moking and COVID-19: Is There A S Moker's Paradox in COVID-19?Kervy Jay AgraviadorNo ratings yet
- Health Effects of Tobacco Use and Exposure: M. BartalDocument10 pagesHealth Effects of Tobacco Use and Exposure: M. BartalsameerpecNo ratings yet
- Nursing Respiratory System "COPD (Chronic Obstructive Pulmonary Disease) "Document15 pagesNursing Respiratory System "COPD (Chronic Obstructive Pulmonary Disease) "ilhamNo ratings yet
- 9410 41584 6 PBDocument9 pages9410 41584 6 PBMuzaki AndiyantoNo ratings yet
- Covid-19 and Respiratory SystemDocument11 pagesCovid-19 and Respiratory SystemESTALDObxdNo ratings yet
- COVID-19Document9 pagesCOVID-19Tony BernardNo ratings yet
- Cigarette Smoking and Its Long Term EffectsDocument14 pagesCigarette Smoking and Its Long Term Effectsameer ahmedNo ratings yet
- 2020 Emerging Blood Gas MonitorsDocument15 pages2020 Emerging Blood Gas MonitorsSHANU KUMARNo ratings yet
- Cigarrillo y CancerDocument6 pagesCigarrillo y CancerSaraNo ratings yet
- A Study On Chronic Obstructive Pulmonary DiseasesDocument12 pagesA Study On Chronic Obstructive Pulmonary DiseasesHamid RazaNo ratings yet
- An Overview: Chronic Obstructive Pulmonary DiseaseDocument9 pagesAn Overview: Chronic Obstructive Pulmonary Diseaseulfiandi rizkiNo ratings yet
- Biology Health Effect of Tobacco: Made By: Anas A.H Class: IX-BDocument14 pagesBiology Health Effect of Tobacco: Made By: Anas A.H Class: IX-BMasthankhan PatanNo ratings yet
- Covid 19 Dan Rokok PDFDocument7 pagesCovid 19 Dan Rokok PDFkkn tematik uho kendariNo ratings yet
- Lecture - 10 (T) Preventable Chronic Respiratory DiseasesDocument19 pagesLecture - 10 (T) Preventable Chronic Respiratory DiseasesMohd ShanawazNo ratings yet
- Chronic Obstructive Pulmonary Disease: An Overview: John F. Devine, DO, FACPDocument9 pagesChronic Obstructive Pulmonary Disease: An Overview: John F. Devine, DO, FACPAngelica GatdulaNo ratings yet
- The Risks of Cigarette SmokeDocument3 pagesThe Risks of Cigarette SmokeMutia IryantiNo ratings yet
- Smoking CovidDocument22 pagesSmoking Covidsofia ayu lestariNo ratings yet
- Chronic Obstructive Diseases of The Lung Part 1Document10 pagesChronic Obstructive Diseases of The Lung Part 1HoracioNo ratings yet
- What You Need To Know About Smoking, Vaping and COVID-19 - American Lung AssociationDocument5 pagesWhat You Need To Know About Smoking, Vaping and COVID-19 - American Lung AssociationJesse DanzigNo ratings yet
- 1 s2.0 S2095254620300600 MainDocument31 pages1 s2.0 S2095254620300600 MainToby ScottNo ratings yet
- S05 108,+ (690+to+700)Document11 pagesS05 108,+ (690+to+700)Muhammad HassanNo ratings yet
- Community Adquired PneumoniaDocument43 pagesCommunity Adquired PneumoniaBraulioNo ratings yet
- Jurnal Pendukung 5Document7 pagesJurnal Pendukung 5Sonia Ayu AndiniNo ratings yet
- SmokingDocument30 pagesSmokingloveaute15No ratings yet
- Reflections On Passive Smoking and COVID-19: Point of ViewDocument4 pagesReflections On Passive Smoking and COVID-19: Point of ViewCibelly CorreiaNo ratings yet
- Chronic Obstructive Pulmonary Disease (COPD) : April 2019Document6 pagesChronic Obstructive Pulmonary Disease (COPD) : April 2019Mashai LesenyehoNo ratings yet
- EmphysemaDocument61 pagesEmphysemaStephanie Mhae TabasaNo ratings yet
- Communicable Disease Project Covid-19 1Document8 pagesCommunicable Disease Project Covid-19 1api-708273919No ratings yet
- Covid-19 - How Smoking, Vaping and Drug Use Might Increase Risks From The Novel Coronavirus - CNNDocument4 pagesCovid-19 - How Smoking, Vaping and Drug Use Might Increase Risks From The Novel Coronavirus - CNNJesse DanzigNo ratings yet
- Environmental Studies Effects of Smoking: Name:S.Jayagokul REG NO:19BCC0020Document4 pagesEnvironmental Studies Effects of Smoking: Name:S.Jayagokul REG NO:19BCC0020Jayagokul SaravananNo ratings yet
- COPDDocument12 pagesCOPDlojainmohamed253No ratings yet
- I. 1. Background: Tobacco SmokeDocument12 pagesI. 1. Background: Tobacco SmokeIntan SorayaNo ratings yet
- Research ProposalDocument13 pagesResearch Proposalmehak fatimaNo ratings yet
- 3297 15954 1 PBDocument5 pages3297 15954 1 PBmuamarrayNo ratings yet
- Health Harms From Smoking and Other Tobacco UseDocument8 pagesHealth Harms From Smoking and Other Tobacco UseRumela Ganguly ChakrabortyNo ratings yet
- Report On COVID-19 Virus OutbreakDocument16 pagesReport On COVID-19 Virus OutbreakSara GuptaNo ratings yet
- Health Harms From Secondhand Smoke: The Health Consequences of Smoking-50 Years of ProgressDocument5 pagesHealth Harms From Secondhand Smoke: The Health Consequences of Smoking-50 Years of ProgressYulianty nanda saputriNo ratings yet
- Novel CoronavirusDocument7 pagesNovel CoronavirusMustafa KhudhairNo ratings yet
- A Comparative Study of Acquiring Pneumonitis Among Smokers and Passive Smokers With AscariasisDocument32 pagesA Comparative Study of Acquiring Pneumonitis Among Smokers and Passive Smokers With AscariasisJim AsenciNo ratings yet
- Covid 19Document9 pagesCovid 19k.agnes12No ratings yet
- Ards Paper NewDocument6 pagesArds Paper Newapi-530306697No ratings yet
- Risk Factors PneumoniaDocument6 pagesRisk Factors PneumoniaTin MercadoNo ratings yet
- Study Conducted To Evaluate The Adverse Effect of Smoking Among The Adult in The NigeriaDocument6 pagesStudy Conducted To Evaluate The Adverse Effect of Smoking Among The Adult in The NigeriaHasrul Al MuttaqinNo ratings yet
- Quarter 4 Dangers of AlcoholDocument19 pagesQuarter 4 Dangers of Alcoholalliah nibayNo ratings yet
- SmokingDocument29 pagesSmokingKris NNo ratings yet
- Health Impacts of ENDSDocument3 pagesHealth Impacts of ENDSAF PortaNo ratings yet
- Astma Impact IncovidDocument9 pagesAstma Impact IncovidRosintchi MirsalNo ratings yet
- UntitledDocument5 pagesUntitledManar AlhakamiNo ratings yet
- Facing COVID-19 with the benefits of medical cannabisFrom EverandFacing COVID-19 with the benefits of medical cannabisNo ratings yet
- Spirometry: Predicting Risk and Outcome: Alessandro Brunelli, MD, Gaetano Rocco, MD, FRCSDocument8 pagesSpirometry: Predicting Risk and Outcome: Alessandro Brunelli, MD, Gaetano Rocco, MD, FRCSAfien MuktiNo ratings yet
- Jurnal COPD Diskusi 1Document9 pagesJurnal COPD Diskusi 1Face StressorNo ratings yet
- Grade 8 HEALTH Q4 Lesson2 LM AlcoholDocument29 pagesGrade 8 HEALTH Q4 Lesson2 LM Alcoholleomille280% (10)
- Pulmonary Physical Therapy RevDocument11 pagesPulmonary Physical Therapy Revpearl042008100% (3)
- A Disease of The Blood Vessels Characterized by The Deposition of Fats and Cholesterol Within The Walls of The ArteryDocument6 pagesA Disease of The Blood Vessels Characterized by The Deposition of Fats and Cholesterol Within The Walls of The ArteryLongyapon Sheena Stephanie50% (2)
- PepDocument22 pagesPepNithin NairNo ratings yet
- Respiratory DR Osama MahmoudpdfDocument91 pagesRespiratory DR Osama MahmoudpdfGhada ElsayedNo ratings yet
- Dr. Ponadon: Principles of Preoperative Preparation of Surgical PatientsDocument4 pagesDr. Ponadon: Principles of Preoperative Preparation of Surgical PatientsJireh GraceNo ratings yet
- AsthmaDocument46 pagesAsthmaHafiz Muhammad AeymonNo ratings yet
- Chapter 2 Related LiteratureDocument3 pagesChapter 2 Related LiteratureMelvin Garcia SalopagioNo ratings yet
- PIR PDPI Lampung 2022 - PIR REVISIDocument1 pagePIR PDPI Lampung 2022 - PIR REVISIherawaty0% (1)
- Medical Surgical Nursing Review NotesDocument209 pagesMedical Surgical Nursing Review Notesabusaifluay100% (1)
- Case Presentation On Copd - Shaik NazmaDocument29 pagesCase Presentation On Copd - Shaik NazmaDeepikaNo ratings yet
- Respiratory SystemDocument5 pagesRespiratory Systemruben diwasNo ratings yet
- Respiratory QuestionnaireDocument14 pagesRespiratory QuestionnaireFirsty Demy ChristantiNo ratings yet
- Breztri Aerosphere Consumer Information LeafletDocument14 pagesBreztri Aerosphere Consumer Information Leafletluongminhnhat108No ratings yet
- Kingston Project Surveillance Program (KPSP) Questionnaire: Section A: Demographic InformationDocument11 pagesKingston Project Surveillance Program (KPSP) Questionnaire: Section A: Demographic InformationLeilybadryaNo ratings yet
- Nursing Care of Clients With Ventilation DisordersDocument6 pagesNursing Care of Clients With Ventilation DisordersLuna MarieNo ratings yet
- Congenital Lobar EmphysemaDocument25 pagesCongenital Lobar Emphysemasheme1711No ratings yet
- Constituents of Smog: Image Description. Better Health Channel Logo End of Image DescriptionDocument3 pagesConstituents of Smog: Image Description. Better Health Channel Logo End of Image DescriptionVini JRNo ratings yet
- Diving Medicine in Clinical Practice: Lars Eichhorn, Dieter LeykDocument14 pagesDiving Medicine in Clinical Practice: Lars Eichhorn, Dieter LeykyantiNo ratings yet
- D. Muscle Protein CatabolismDocument5 pagesD. Muscle Protein CatabolismKristinelou Marie ReynaNo ratings yet
- Makalah B.ingggggggggggggggggggggggggDocument29 pagesMakalah B.ingggggggggggggggggggggggggmegaNo ratings yet
- H5 Thesis 1 RevisedDocument64 pagesH5 Thesis 1 Revisedhadprince2023No ratings yet
- Jadwal Pir MalangDocument4 pagesJadwal Pir MalangAbraham BayuNo ratings yet
- Chronic Pulmonary Aspergillosis An Updated On Diagnosis and TreatmentDocument13 pagesChronic Pulmonary Aspergillosis An Updated On Diagnosis and TreatmentCahrun CarterNo ratings yet
- Final Exam Focus SheetDocument9 pagesFinal Exam Focus SheetDane WrightNo ratings yet
- Physiotherapy Practice Guidelines For COPDDocument35 pagesPhysiotherapy Practice Guidelines For COPD健康生活園Healthy Life Garden100% (1)