Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
16 viewsHyperphosphataemia PDF
Hyperphosphataemia PDF
Uploaded by
Mohamed AbbasRenal failure is the most common cause of hyperphosphataemia because impaired kidney function reduces phosphate excretion. Treatment involves limiting phosphate intake, enhancing urinary phosphate excretion through saline infusion or diuretics, and using oral phosphate binders like calcium and aluminum salts. Hyperphosphataemia can also be caused by increased renal resorption due to conditions like hypoparathyroidism, cellular injury releasing phosphate from tumour lysis syndrome or rhabdomyolysis, and certain medications that contain or administer high levels of phosphate.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You might also like
- Chapter 1: Abnormal Behavior in Historical ContextDocument22 pagesChapter 1: Abnormal Behavior in Historical ContextEsraRamos100% (2)
- ChartDocument1 pageChartAnggi Dwi PrasetyoNo ratings yet
- HYPERPARATHYROIDISMDocument1 pageHYPERPARATHYROIDISMPhilip Gene II MalacasNo ratings yet
- HypophosphatemiaDocument26 pagesHypophosphatemiaOxy GenNo ratings yet
- ElectrolyteDocument4 pagesElectrolyteRon Vien'sNo ratings yet
- Calcium Metabolism in Renal Failure: York, New YorkDocument9 pagesCalcium Metabolism in Renal Failure: York, New Yorkstella pangestikaNo ratings yet
- Electrolyte Imbalances 103123Document14 pagesElectrolyte Imbalances 103123grazelantonette.calubNo ratings yet
- Chronic Kidney Disease: Uremia SyndromeDocument8 pagesChronic Kidney Disease: Uremia SyndromeMartien Silviandy SetiawanNo ratings yet
- Group 11 Hyperphosphatemia HandoutsDocument2 pagesGroup 11 Hyperphosphatemia HandoutsRisha Ethel BerondoNo ratings yet
- Veterinary Clinics: Phosphorus: A Quick ReferenceDocument5 pagesVeterinary Clinics: Phosphorus: A Quick ReferenceDanilo JimenezNo ratings yet
- Causes of Acute Renal FailureDocument11 pagesCauses of Acute Renal FailureAndrea Roman chavezNo ratings yet
- Kahoots 8 - Renal Physiology PDFDocument3 pagesKahoots 8 - Renal Physiology PDFJoshua LanzonNo ratings yet
- Hypernatremia From HarrisonDocument3 pagesHypernatremia From HarrisonNobel LaureateNo ratings yet
- Parathyroi D HormoneDocument25 pagesParathyroi D HormoneChatie PipitNo ratings yet
- Hypo Phosphate MiaDocument15 pagesHypo Phosphate Miacute_maimaiNo ratings yet
- Calcium Homeostasis: HypocalcemiaDocument4 pagesCalcium Homeostasis: Hypocalcemia075 Keerthighaa SNo ratings yet
- Calcium Metabolism (PTH, Vitamin D, and Calcitonin)Document4 pagesCalcium Metabolism (PTH, Vitamin D, and Calcitonin)Saima SiddiqiNo ratings yet
- Hypercalcemia (F&e)Document3 pagesHypercalcemia (F&e)Sarah Grace CajucomNo ratings yet
- RicketsDocument3 pagesRicketsSaloni GanganNo ratings yet
- HypoparathyroidismDocument2 pagesHypoparathyroidismLorelyn Santos Corpuz0% (1)
- Lange Nephrology EssentialsDocument9 pagesLange Nephrology EssentialsAlejandro GarcíaNo ratings yet
- Disorders of The Urinary System PrefaceDocument25 pagesDisorders of The Urinary System PrefacenyarieNo ratings yet
- CKD Pead IllustratedDocument3 pagesCKD Pead IllustratedakeelNo ratings yet
- Parathyroid Gland AnatomyDocument27 pagesParathyroid Gland AnatomyABUBEKER BESHIRNo ratings yet
- Rta PDFDocument4 pagesRta PDFtraceyNo ratings yet
- APNC 520 Exam 10 Study Guide Musculoskeletal DisordersDocument15 pagesAPNC 520 Exam 10 Study Guide Musculoskeletal DisordersMariaNo ratings yet
- Nutrition Management For Chronic Kidney DiseaseDocument27 pagesNutrition Management For Chronic Kidney DiseaseYESSAMIN PAREDESNo ratings yet
- CC Lec Mod 3Document13 pagesCC Lec Mod 38wgmhh9ks9No ratings yet
- PHARMA-5Document27 pagesPHARMA-5yuson.joan001No ratings yet
- Renal & Electrolyted Physiology FinalDocument21 pagesRenal & Electrolyted Physiology FinalVondNo ratings yet
- Nephrolithiasis: Grade A ReferencesDocument8 pagesNephrolithiasis: Grade A ReferencesEngin AltınkayaNo ratings yet
- Hypo Phosphate MiaDocument7 pagesHypo Phosphate MiaChristian Manuel Chiara ChiletNo ratings yet
- Batu GinjalDocument29 pagesBatu Ginjalarim100% (1)
- Bio NotesDocument24 pagesBio NotesIslam MansourNo ratings yet
- Rickets in ChildrenDocument61 pagesRickets in ChildrenmdNo ratings yet
- Pharma MidtermDocument7 pagesPharma MidtermBenzy Anne MermalNo ratings yet
- Rickets Metabolic Bone DiseasesDocument61 pagesRickets Metabolic Bone DiseasesKrameshNo ratings yet
- Acute Renal FailureDocument6 pagesAcute Renal FailureFrancine Kyle SusanoNo ratings yet
- Anemia and Hematologic Drugs - KatzungDocument4 pagesAnemia and Hematologic Drugs - Katzungsarguss14100% (1)
- Pediatrics DiseaseDocument7 pagesPediatrics DiseaseHaslam UdaraniNo ratings yet
- Phosphate Homeostasis in Critical Care: RL Wadsworth MB CHB Frca and S Siddiqui MB CHB FrcaDocument5 pagesPhosphate Homeostasis in Critical Care: RL Wadsworth MB CHB Frca and S Siddiqui MB CHB FrcaMahipal Reddy NimmalaNo ratings yet
- 14 Nephrology&eurologyDocument3 pages14 Nephrology&eurologyDheepak ARNo ratings yet
- 2022 Oxford Handbook of Anaesthesia Oxford Press 5th Edition ExportDocument2 pages2022 Oxford Handbook of Anaesthesia Oxford Press 5th Edition ExportHany Elbarougy0% (1)
- Clinical Nutrition Refeeding Sendromu MakaleDocument2 pagesClinical Nutrition Refeeding Sendromu Makalermysalbyrk2000No ratings yet
- SAJAA (V27) p126-130 2691 FCA SupplementDocument5 pagesSAJAA (V27) p126-130 2691 FCA SupplementVivek PatangeNo ratings yet
- RICKETSDocument49 pagesRICKETSMis Bah100% (1)
- SodiumDocument3 pagesSodiumEmily FernandezNo ratings yet
- Chronic Kidney DiseaseDocument4 pagesChronic Kidney DiseaseImnot YouNo ratings yet
- NCM 112-Mod4Document2 pagesNCM 112-Mod4Samantha BolanteNo ratings yet
- Urolithiasis: ObjectivesDocument11 pagesUrolithiasis: ObjectivesOkki Masitah Syahfitri NasutionNo ratings yet
- Calicum Metabolisim DisoodersDocument12 pagesCalicum Metabolisim DisoodersDr-Dalya ShakirNo ratings yet
- Labs UgibDocument4 pagesLabs UgibRomwella May AlgoNo ratings yet
- Pharmacology Final TermDocument19 pagesPharmacology Final TermDWIGHT LESTER O. MANGILANo ratings yet
- Parathyroid GlandsDocument3 pagesParathyroid GlandsStrong Woman Bong SoonNo ratings yet
- Nephrotic SyndromeDocument2 pagesNephrotic SyndromeBii MarshalNo ratings yet
- HEPATOBILIARYDocument6 pagesHEPATOBILIARYjsreyes.402No ratings yet
- Rickets, Osteomalacia and Renal OsteodystrophyDocument13 pagesRickets, Osteomalacia and Renal Osteodystrophyesther_aprilNo ratings yet
- Chronic Renal FailureDocument54 pagesChronic Renal Failuresanjivdas100% (3)
- Kidney DiseaseDocument10 pagesKidney Disease42tdgcrpxhNo ratings yet
- د.وليد سعد urineDocument26 pagesد.وليد سعد urineAbdulmalik Al-harthyNo ratings yet
- Hypophosphatemia, (Low Phosphate) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandHypophosphatemia, (Low Phosphate) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- USMLE 1 FA Equations (Step 1 Study) Flashcards - MemorangDocument3 pagesUSMLE 1 FA Equations (Step 1 Study) Flashcards - MemorangMohamed AbbasNo ratings yet
- Free Surgery Flashcards About ATLS Chapters 1-3Document3 pagesFree Surgery Flashcards About ATLS Chapters 1-3Mohamed AbbasNo ratings yet
- Cardiology USMLE 2CK (Cardio Clinical Care) Flashcards - MemorangDocument4 pagesCardiology USMLE 2CK (Cardio Clinical Care) Flashcards - MemorangMohamed Abbas0% (2)
- USMLE Step 1 Rapid Review Classic Presentations (FA) Flashcards - MemorangDocument8 pagesUSMLE Step 1 Rapid Review Classic Presentations (FA) Flashcards - MemorangMohamed AbbasNo ratings yet
- Linezolid PDFDocument1 pageLinezolid PDFMohamed AbbasNo ratings yet
- DermaDocument2 pagesDermaMohamed AbbasNo ratings yet
- Selective Digestive Decontamination PDFDocument1 pageSelective Digestive Decontamination PDFMohamed AbbasNo ratings yet
- LinezolidDocument1 pageLinezolidMohamed AbbasNo ratings yet
- Periodic ParalysisDocument1 pagePeriodic ParalysisMohamed AbbasNo ratings yet
- Section B - Work BookDocument112 pagesSection B - Work BookMohamed AbbasNo ratings yet
- Section B - Work BookDocument112 pagesSection B - Work BookMohamed AbbasNo ratings yet
- Systemic CandidiasisDocument1 pageSystemic CandidiasisMohamed AbbasNo ratings yet
- Section D - Work BookDocument69 pagesSection D - Work BookMohamed AbbasNo ratings yet
- DR - Moenes Abou El Atta - LinkedIn PDFDocument4 pagesDR - Moenes Abou El Atta - LinkedIn PDFMohamed AbbasNo ratings yet
- Fmge Results DecemberDocument105 pagesFmge Results DecemberMohamed AbbasNo ratings yet
- Surgery - King Faisal Specialist Hospital & Research CentreDocument22 pagesSurgery - King Faisal Specialist Hospital & Research CentreMohamed AbbasNo ratings yet
- Lecture 1 Historical Aspects of Surgery (Core)Document27 pagesLecture 1 Historical Aspects of Surgery (Core)Charwinth KankaNo ratings yet
- Pre-Feasibility Report Centralized Biomedical Waste Treatment Facility in KeralaDocument25 pagesPre-Feasibility Report Centralized Biomedical Waste Treatment Facility in KeralaVashudev BohraNo ratings yet
- Kelainan Presentasi & Letak (Sungsang)Document37 pagesKelainan Presentasi & Letak (Sungsang)Matheis Laskar PelangiNo ratings yet
- NAC Medications Chart 2016 A2Document1 pageNAC Medications Chart 2016 A2ayuniNo ratings yet
- Oconnor Clinical Case Study WorksheetDocument3 pagesOconnor Clinical Case Study Worksheetapi-254175613No ratings yet
- First Announcement: InaprasDocument12 pagesFirst Announcement: InaprasnikitagustiNo ratings yet
- Kanner 2016Document11 pagesKanner 2016Izara Maité Mondragón MorenoNo ratings yet
- ID Pola Bakteri Dan Resistensi Antibiotik PDocument15 pagesID Pola Bakteri Dan Resistensi Antibiotik PNadya AbigailNo ratings yet
- Kinesiology 8 - PJJ Assgnment Movement AnalysisDocument64 pagesKinesiology 8 - PJJ Assgnment Movement AnalysispaegyoNo ratings yet
- CipaDocument15 pagesCipaapi-247628136No ratings yet
- The Feasibility of Taro Roots As An Herbal Tea For Indigestion and WeightlossDocument10 pagesThe Feasibility of Taro Roots As An Herbal Tea For Indigestion and WeightlossNathaliaEicellRoseBuenoNo ratings yet
- Cancer Antigen (Ca) 15.3: Subtypes of Breast CancerDocument4 pagesCancer Antigen (Ca) 15.3: Subtypes of Breast Cancerडा. सत्यदेव त्यागी आर्यNo ratings yet
- Vital Pulp Therapy 1Document6 pagesVital Pulp Therapy 1Mostafa Afifi Ali100% (1)
- Saludos: Nachos With A Twist!Document11 pagesSaludos: Nachos With A Twist!Paridhi GargNo ratings yet
- MPNDocument11 pagesMPNAyi Syahriani Airi100% (2)
- Heavy-Load Eccentric Calf Muscle Training For The Treatment of Chronic Achilles TendinosisDocument8 pagesHeavy-Load Eccentric Calf Muscle Training For The Treatment of Chronic Achilles TendinosisburgoschileNo ratings yet
- Runner's Knee (Patellofemoral Pain) : CausesDocument4 pagesRunner's Knee (Patellofemoral Pain) : CausesBarath KannanNo ratings yet
- BLS CPRDocument42 pagesBLS CPRKhairunisa SiregarNo ratings yet
- CC WillywonkaDocument16 pagesCC WillywonkaHarsheen Kaur ChadhaNo ratings yet
- Needle Cricothyroidotomy 2 - Hatem AlsrourDocument32 pagesNeedle Cricothyroidotomy 2 - Hatem Alsrourhatem alsrour100% (3)
- Osteoarthritis: Pathophysiology: OA Is Primarily A Disease of CartilageDocument5 pagesOsteoarthritis: Pathophysiology: OA Is Primarily A Disease of CartilageLinda SugiartoNo ratings yet
- Post Traumatic Stress Disorder 1Document8 pagesPost Traumatic Stress Disorder 1Shubhranshul DwivediNo ratings yet
- Modern Letterhead TemplateDocument1 pageModern Letterhead TemplatesmaranikatripathyNo ratings yet
- 1345571825binder2Document36 pages1345571825binder2CoolerAdsNo ratings yet
- The Effectiveness of Neural Mobilization For Neuromusculoskeletal Conditions: A Systematic Review and Meta-AnalysisDocument29 pagesThe Effectiveness of Neural Mobilization For Neuromusculoskeletal Conditions: A Systematic Review and Meta-AnalysisRegarNo ratings yet
- Nontoxic GoiterDocument4 pagesNontoxic GoiterpauchanmnlNo ratings yet
- PSY4220 Unit Guide 2014Document24 pagesPSY4220 Unit Guide 2014hongrdNo ratings yet
- Block One Nursing ProcessDocument2 pagesBlock One Nursing ProcessdavidvpnNo ratings yet
Hyperphosphataemia PDF
Hyperphosphataemia PDF
Uploaded by
Mohamed Abbas0 ratings0% found this document useful (0 votes)
16 views1 pageRenal failure is the most common cause of hyperphosphataemia because impaired kidney function reduces phosphate excretion. Treatment involves limiting phosphate intake, enhancing urinary phosphate excretion through saline infusion or diuretics, and using oral phosphate binders like calcium and aluminum salts. Hyperphosphataemia can also be caused by increased renal resorption due to conditions like hypoparathyroidism, cellular injury releasing phosphate from tumour lysis syndrome or rhabdomyolysis, and certain medications that contain or administer high levels of phosphate.
Original Description:
Original Title
Hyperphosphataemia.pdf
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentRenal failure is the most common cause of hyperphosphataemia because impaired kidney function reduces phosphate excretion. Treatment involves limiting phosphate intake, enhancing urinary phosphate excretion through saline infusion or diuretics, and using oral phosphate binders like calcium and aluminum salts. Hyperphosphataemia can also be caused by increased renal resorption due to conditions like hypoparathyroidism, cellular injury releasing phosphate from tumour lysis syndrome or rhabdomyolysis, and certain medications that contain or administer high levels of phosphate.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
16 views1 pageHyperphosphataemia PDF
Hyperphosphataemia PDF
Uploaded by
Mohamed AbbasRenal failure is the most common cause of hyperphosphataemia because impaired kidney function reduces phosphate excretion. Treatment involves limiting phosphate intake, enhancing urinary phosphate excretion through saline infusion or diuretics, and using oral phosphate binders like calcium and aluminum salts. Hyperphosphataemia can also be caused by increased renal resorption due to conditions like hypoparathyroidism, cellular injury releasing phosphate from tumour lysis syndrome or rhabdomyolysis, and certain medications that contain or administer high levels of phosphate.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 1
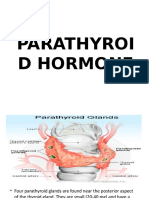
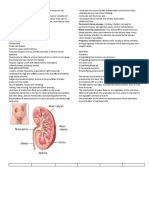
(i) renal failure
- most common cause
- causes hyperphosphataemia because the renal excretion by
the kidneys is impaired
(i) limit phosphate intake - serum phosphate is usually normal until the creatinine clearance
(ii) enhance urinary phosphate excretion is less than 30ml/min
- in the absence of end stage renal disease, phosphate excretion (ii) increased renal resorption
can be optimised with saline infusion and diuretics - hypoparathyroidism
- diuretics that work on the proximal tubule such as acetazolamide causes - thyrotoxicosis
are particularly effective for enhancing phosphate excretion (iii) cellular injury with release of phosphate
- any patient with life threatening hyperphosphataemia should receive dialysis - tumour lysis syndrome
(iii) oral phosphate binders hyperphosphataemia - rhabdomyolysis
- calcium and aluminium salts are widely used; however calcium salts may produce treatment - haemolysis
metastatic calcification and aluminium salts are toxic.
[created by Paul (iv) medication related
- in dialysis patients, chronic management with calcium free phosphate binders such Young 17/12/07] - abuse of phosphate containing laxatives
as sevelamer hydrochloride may reduce long-term mortality by preventing long-term - excessive phosphate administration
cardiovascular complications associated with a high calcium phosphorus product - bisphosphonate therapy
NB: in the acute management of patients with hyperphosphataemia accompanied
by hypocalcaemia, the likelihood and clinical significance of metastatic calcification - most manifestations are due to associated hypocalcaemia which is produced by
with acute calcium administration is unclear (i) precipitation with calcium (leading to nepholithiasis)
(ii) interference with parathyroid hormone-mediated resorption of bone
manifestations (iii) decreased vitamin D levels
- manifestations of hypocalcaemia include muscle cramping, tetany,
hyperreflexia and seizures as well as cardiovascular manifestations
You might also like
- Chapter 1: Abnormal Behavior in Historical ContextDocument22 pagesChapter 1: Abnormal Behavior in Historical ContextEsraRamos100% (2)
- ChartDocument1 pageChartAnggi Dwi PrasetyoNo ratings yet
- HYPERPARATHYROIDISMDocument1 pageHYPERPARATHYROIDISMPhilip Gene II MalacasNo ratings yet
- HypophosphatemiaDocument26 pagesHypophosphatemiaOxy GenNo ratings yet
- ElectrolyteDocument4 pagesElectrolyteRon Vien'sNo ratings yet
- Calcium Metabolism in Renal Failure: York, New YorkDocument9 pagesCalcium Metabolism in Renal Failure: York, New Yorkstella pangestikaNo ratings yet
- Electrolyte Imbalances 103123Document14 pagesElectrolyte Imbalances 103123grazelantonette.calubNo ratings yet
- Chronic Kidney Disease: Uremia SyndromeDocument8 pagesChronic Kidney Disease: Uremia SyndromeMartien Silviandy SetiawanNo ratings yet
- Group 11 Hyperphosphatemia HandoutsDocument2 pagesGroup 11 Hyperphosphatemia HandoutsRisha Ethel BerondoNo ratings yet
- Veterinary Clinics: Phosphorus: A Quick ReferenceDocument5 pagesVeterinary Clinics: Phosphorus: A Quick ReferenceDanilo JimenezNo ratings yet
- Causes of Acute Renal FailureDocument11 pagesCauses of Acute Renal FailureAndrea Roman chavezNo ratings yet
- Kahoots 8 - Renal Physiology PDFDocument3 pagesKahoots 8 - Renal Physiology PDFJoshua LanzonNo ratings yet
- Hypernatremia From HarrisonDocument3 pagesHypernatremia From HarrisonNobel LaureateNo ratings yet
- Parathyroi D HormoneDocument25 pagesParathyroi D HormoneChatie PipitNo ratings yet
- Hypo Phosphate MiaDocument15 pagesHypo Phosphate Miacute_maimaiNo ratings yet
- Calcium Homeostasis: HypocalcemiaDocument4 pagesCalcium Homeostasis: Hypocalcemia075 Keerthighaa SNo ratings yet
- Calcium Metabolism (PTH, Vitamin D, and Calcitonin)Document4 pagesCalcium Metabolism (PTH, Vitamin D, and Calcitonin)Saima SiddiqiNo ratings yet
- Hypercalcemia (F&e)Document3 pagesHypercalcemia (F&e)Sarah Grace CajucomNo ratings yet
- RicketsDocument3 pagesRicketsSaloni GanganNo ratings yet
- HypoparathyroidismDocument2 pagesHypoparathyroidismLorelyn Santos Corpuz0% (1)
- Lange Nephrology EssentialsDocument9 pagesLange Nephrology EssentialsAlejandro GarcíaNo ratings yet
- Disorders of The Urinary System PrefaceDocument25 pagesDisorders of The Urinary System PrefacenyarieNo ratings yet
- CKD Pead IllustratedDocument3 pagesCKD Pead IllustratedakeelNo ratings yet
- Parathyroid Gland AnatomyDocument27 pagesParathyroid Gland AnatomyABUBEKER BESHIRNo ratings yet
- Rta PDFDocument4 pagesRta PDFtraceyNo ratings yet
- APNC 520 Exam 10 Study Guide Musculoskeletal DisordersDocument15 pagesAPNC 520 Exam 10 Study Guide Musculoskeletal DisordersMariaNo ratings yet
- Nutrition Management For Chronic Kidney DiseaseDocument27 pagesNutrition Management For Chronic Kidney DiseaseYESSAMIN PAREDESNo ratings yet
- CC Lec Mod 3Document13 pagesCC Lec Mod 38wgmhh9ks9No ratings yet
- PHARMA-5Document27 pagesPHARMA-5yuson.joan001No ratings yet
- Renal & Electrolyted Physiology FinalDocument21 pagesRenal & Electrolyted Physiology FinalVondNo ratings yet
- Nephrolithiasis: Grade A ReferencesDocument8 pagesNephrolithiasis: Grade A ReferencesEngin AltınkayaNo ratings yet
- Hypo Phosphate MiaDocument7 pagesHypo Phosphate MiaChristian Manuel Chiara ChiletNo ratings yet
- Batu GinjalDocument29 pagesBatu Ginjalarim100% (1)
- Bio NotesDocument24 pagesBio NotesIslam MansourNo ratings yet
- Rickets in ChildrenDocument61 pagesRickets in ChildrenmdNo ratings yet
- Pharma MidtermDocument7 pagesPharma MidtermBenzy Anne MermalNo ratings yet
- Rickets Metabolic Bone DiseasesDocument61 pagesRickets Metabolic Bone DiseasesKrameshNo ratings yet
- Acute Renal FailureDocument6 pagesAcute Renal FailureFrancine Kyle SusanoNo ratings yet
- Anemia and Hematologic Drugs - KatzungDocument4 pagesAnemia and Hematologic Drugs - Katzungsarguss14100% (1)
- Pediatrics DiseaseDocument7 pagesPediatrics DiseaseHaslam UdaraniNo ratings yet
- Phosphate Homeostasis in Critical Care: RL Wadsworth MB CHB Frca and S Siddiqui MB CHB FrcaDocument5 pagesPhosphate Homeostasis in Critical Care: RL Wadsworth MB CHB Frca and S Siddiqui MB CHB FrcaMahipal Reddy NimmalaNo ratings yet
- 14 Nephrology&eurologyDocument3 pages14 Nephrology&eurologyDheepak ARNo ratings yet
- 2022 Oxford Handbook of Anaesthesia Oxford Press 5th Edition ExportDocument2 pages2022 Oxford Handbook of Anaesthesia Oxford Press 5th Edition ExportHany Elbarougy0% (1)
- Clinical Nutrition Refeeding Sendromu MakaleDocument2 pagesClinical Nutrition Refeeding Sendromu Makalermysalbyrk2000No ratings yet
- SAJAA (V27) p126-130 2691 FCA SupplementDocument5 pagesSAJAA (V27) p126-130 2691 FCA SupplementVivek PatangeNo ratings yet
- RICKETSDocument49 pagesRICKETSMis Bah100% (1)
- SodiumDocument3 pagesSodiumEmily FernandezNo ratings yet
- Chronic Kidney DiseaseDocument4 pagesChronic Kidney DiseaseImnot YouNo ratings yet
- NCM 112-Mod4Document2 pagesNCM 112-Mod4Samantha BolanteNo ratings yet
- Urolithiasis: ObjectivesDocument11 pagesUrolithiasis: ObjectivesOkki Masitah Syahfitri NasutionNo ratings yet
- Calicum Metabolisim DisoodersDocument12 pagesCalicum Metabolisim DisoodersDr-Dalya ShakirNo ratings yet
- Labs UgibDocument4 pagesLabs UgibRomwella May AlgoNo ratings yet
- Pharmacology Final TermDocument19 pagesPharmacology Final TermDWIGHT LESTER O. MANGILANo ratings yet
- Parathyroid GlandsDocument3 pagesParathyroid GlandsStrong Woman Bong SoonNo ratings yet
- Nephrotic SyndromeDocument2 pagesNephrotic SyndromeBii MarshalNo ratings yet
- HEPATOBILIARYDocument6 pagesHEPATOBILIARYjsreyes.402No ratings yet
- Rickets, Osteomalacia and Renal OsteodystrophyDocument13 pagesRickets, Osteomalacia and Renal Osteodystrophyesther_aprilNo ratings yet
- Chronic Renal FailureDocument54 pagesChronic Renal Failuresanjivdas100% (3)
- Kidney DiseaseDocument10 pagesKidney Disease42tdgcrpxhNo ratings yet
- د.وليد سعد urineDocument26 pagesد.وليد سعد urineAbdulmalik Al-harthyNo ratings yet
- Hypophosphatemia, (Low Phosphate) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandHypophosphatemia, (Low Phosphate) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- USMLE 1 FA Equations (Step 1 Study) Flashcards - MemorangDocument3 pagesUSMLE 1 FA Equations (Step 1 Study) Flashcards - MemorangMohamed AbbasNo ratings yet
- Free Surgery Flashcards About ATLS Chapters 1-3Document3 pagesFree Surgery Flashcards About ATLS Chapters 1-3Mohamed AbbasNo ratings yet
- Cardiology USMLE 2CK (Cardio Clinical Care) Flashcards - MemorangDocument4 pagesCardiology USMLE 2CK (Cardio Clinical Care) Flashcards - MemorangMohamed Abbas0% (2)
- USMLE Step 1 Rapid Review Classic Presentations (FA) Flashcards - MemorangDocument8 pagesUSMLE Step 1 Rapid Review Classic Presentations (FA) Flashcards - MemorangMohamed AbbasNo ratings yet
- Linezolid PDFDocument1 pageLinezolid PDFMohamed AbbasNo ratings yet
- DermaDocument2 pagesDermaMohamed AbbasNo ratings yet
- Selective Digestive Decontamination PDFDocument1 pageSelective Digestive Decontamination PDFMohamed AbbasNo ratings yet
- LinezolidDocument1 pageLinezolidMohamed AbbasNo ratings yet
- Periodic ParalysisDocument1 pagePeriodic ParalysisMohamed AbbasNo ratings yet
- Section B - Work BookDocument112 pagesSection B - Work BookMohamed AbbasNo ratings yet
- Section B - Work BookDocument112 pagesSection B - Work BookMohamed AbbasNo ratings yet
- Systemic CandidiasisDocument1 pageSystemic CandidiasisMohamed AbbasNo ratings yet
- Section D - Work BookDocument69 pagesSection D - Work BookMohamed AbbasNo ratings yet
- DR - Moenes Abou El Atta - LinkedIn PDFDocument4 pagesDR - Moenes Abou El Atta - LinkedIn PDFMohamed AbbasNo ratings yet
- Fmge Results DecemberDocument105 pagesFmge Results DecemberMohamed AbbasNo ratings yet
- Surgery - King Faisal Specialist Hospital & Research CentreDocument22 pagesSurgery - King Faisal Specialist Hospital & Research CentreMohamed AbbasNo ratings yet
- Lecture 1 Historical Aspects of Surgery (Core)Document27 pagesLecture 1 Historical Aspects of Surgery (Core)Charwinth KankaNo ratings yet
- Pre-Feasibility Report Centralized Biomedical Waste Treatment Facility in KeralaDocument25 pagesPre-Feasibility Report Centralized Biomedical Waste Treatment Facility in KeralaVashudev BohraNo ratings yet
- Kelainan Presentasi & Letak (Sungsang)Document37 pagesKelainan Presentasi & Letak (Sungsang)Matheis Laskar PelangiNo ratings yet
- NAC Medications Chart 2016 A2Document1 pageNAC Medications Chart 2016 A2ayuniNo ratings yet
- Oconnor Clinical Case Study WorksheetDocument3 pagesOconnor Clinical Case Study Worksheetapi-254175613No ratings yet
- First Announcement: InaprasDocument12 pagesFirst Announcement: InaprasnikitagustiNo ratings yet
- Kanner 2016Document11 pagesKanner 2016Izara Maité Mondragón MorenoNo ratings yet
- ID Pola Bakteri Dan Resistensi Antibiotik PDocument15 pagesID Pola Bakteri Dan Resistensi Antibiotik PNadya AbigailNo ratings yet
- Kinesiology 8 - PJJ Assgnment Movement AnalysisDocument64 pagesKinesiology 8 - PJJ Assgnment Movement AnalysispaegyoNo ratings yet
- CipaDocument15 pagesCipaapi-247628136No ratings yet
- The Feasibility of Taro Roots As An Herbal Tea For Indigestion and WeightlossDocument10 pagesThe Feasibility of Taro Roots As An Herbal Tea For Indigestion and WeightlossNathaliaEicellRoseBuenoNo ratings yet
- Cancer Antigen (Ca) 15.3: Subtypes of Breast CancerDocument4 pagesCancer Antigen (Ca) 15.3: Subtypes of Breast Cancerडा. सत्यदेव त्यागी आर्यNo ratings yet
- Vital Pulp Therapy 1Document6 pagesVital Pulp Therapy 1Mostafa Afifi Ali100% (1)
- Saludos: Nachos With A Twist!Document11 pagesSaludos: Nachos With A Twist!Paridhi GargNo ratings yet
- MPNDocument11 pagesMPNAyi Syahriani Airi100% (2)
- Heavy-Load Eccentric Calf Muscle Training For The Treatment of Chronic Achilles TendinosisDocument8 pagesHeavy-Load Eccentric Calf Muscle Training For The Treatment of Chronic Achilles TendinosisburgoschileNo ratings yet
- Runner's Knee (Patellofemoral Pain) : CausesDocument4 pagesRunner's Knee (Patellofemoral Pain) : CausesBarath KannanNo ratings yet
- BLS CPRDocument42 pagesBLS CPRKhairunisa SiregarNo ratings yet
- CC WillywonkaDocument16 pagesCC WillywonkaHarsheen Kaur ChadhaNo ratings yet
- Needle Cricothyroidotomy 2 - Hatem AlsrourDocument32 pagesNeedle Cricothyroidotomy 2 - Hatem Alsrourhatem alsrour100% (3)
- Osteoarthritis: Pathophysiology: OA Is Primarily A Disease of CartilageDocument5 pagesOsteoarthritis: Pathophysiology: OA Is Primarily A Disease of CartilageLinda SugiartoNo ratings yet
- Post Traumatic Stress Disorder 1Document8 pagesPost Traumatic Stress Disorder 1Shubhranshul DwivediNo ratings yet
- Modern Letterhead TemplateDocument1 pageModern Letterhead TemplatesmaranikatripathyNo ratings yet
- 1345571825binder2Document36 pages1345571825binder2CoolerAdsNo ratings yet
- The Effectiveness of Neural Mobilization For Neuromusculoskeletal Conditions: A Systematic Review and Meta-AnalysisDocument29 pagesThe Effectiveness of Neural Mobilization For Neuromusculoskeletal Conditions: A Systematic Review and Meta-AnalysisRegarNo ratings yet
- Nontoxic GoiterDocument4 pagesNontoxic GoiterpauchanmnlNo ratings yet
- PSY4220 Unit Guide 2014Document24 pagesPSY4220 Unit Guide 2014hongrdNo ratings yet
- Block One Nursing ProcessDocument2 pagesBlock One Nursing ProcessdavidvpnNo ratings yet