Professional Documents
Culture Documents
Anticholinergic: Classification Generic Name Brand Name
Anticholinergic: Classification Generic Name Brand Name
Uploaded by
Karina MadriagaOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Anticholinergic: Classification Generic Name Brand Name
Anticholinergic: Classification Generic Name Brand Name
Uploaded by
Karina MadriagaCopyright:
Available Formats
Anticholinergic
Anticholinergic are drugs that oppose the effects of acetylcholine. In essence, they also lyse and
block the effects of parasympathetic nervous system (PNS) so they are also called as
parasympatholytics. Atropine is currently the only widely used anticholinergic drug. Other
common examples include meclizine, scopolamine and ipratropium.
Anticholinergics: Generic and Brand Names
Here is a table of commonly encountered anticholinergic agents, their generic names, and brand
names:
Classification Generic Name Brand Name
atropine (generic)
ipratropium Atrovent
meclizine Bonine, Antivert
Anticholinergics
methscopolamine Pamine
scopolamine Transderm Scop
tiotropium Spiriva
Disease Spotlight: Gastrointestinal Ulcers
Anticholinergics were once very widely used to decrease GI activity and secretions.
However, more specific and less toxic drugs are available now and the utilization of
this drug class is now limited.
GI ulcers are basically erosions in the lining of the GIT caused by increased HCl
production most commonly from H. pylori infection. Patients with GI ulcers suffer
from burning abdominal pain, nausea, and acid reflux.
Therapeutic Action
The desired and beneficial actions of anticholinergics are as follows:
Competitively blocking the ACh receptors at muscarinic cholinergic receptor sites that
are responsible for mediating the effects of the parasympathetic postganglionic
impulses.
Atropine, the prototype drug, is derived from the plant belladonna. It is used to
depress salivation and bronchial secretions and to dilate the bronchi, but it can thicken
respiratory secretions (causing obstruction of airways).
Atropine and scopolamine work by blocking only the muscarinic effectors in the
parasympathetic nervous system and the few cholinergic receptors in the SNS.
Indications
Anticholinergics are indicated for the following medical conditions:
Prevention of nausea, vomiting, and dizziness associated with motion sickness.
Adjunctive therapy for treatment of GI ulcers
Decrease secretions before anesthesia or intubation
Maintenance treatment of bronchospasm associated with COPD.
Treatment of irritable or hyperactive bowel in adults.
Here are some important aspects to remember for indication of anticholinergics in different age
groups:
Children
More sensitive to the adverse effects of the drug (e.g. constipation, urinary retention,
heat intolerance, confusion).
Dicyclomine is not recommended for use in children.
Adults
Adults should be cautioned of these drugs’ adverse effects.
Use of these drugs among pregnant women is not allowed because they can cross
placenta and cause adverse effects to the fetus.
Older adults
Dose adjustment is needed as this age group is also more susceptible to drug side
effects.
They are more likely to have toxic levels of the drug because of renal or hepatic
impairments.
Pharmacokinetics
Here are the characteristic interactions of anticholinergics and the body in terms of absorption,
distribution, metabolism, and excretion:
Route Onset Peak Duration
IM 10-15 min 30 min 4h
IV Immediate 2-4 min 4h
Subcutaneous Varies 1-2 h 4h
Topical 5-10 min 30-40 min 7-14 d
T1/2: 2.5 h
Metabolism: liver
Excretion: urine
Contraindications and Cautions
The following are contraindications and cautions for the use of anticholinergics:
Allergy to any component of the drug. To prevent hypersensitivity reaction
Glaucoma. Can be exacerbated by blockade of PNS.
Intestinal atony, paralytic ileus, GI obstruction. Can be exacerbated with further
slowing of GI activity.
Pregnancy. Potential adverse effects on the fetus.
Adverse Effects
Use of anticholinergic agents may result to these adverse effects:
CNS: blurred vision, pupil dilation, photophobia, cycloplegia, increased intraocular
pressure, weakness, dizziness, insomnia
CV: tachycardia, palpitation
GI: dry mouth, altered taste perception, nausea, heartburn, constipation
GU: urinary hesitancy and retention, heat prostration
Interactions
The following are interactions involved in the use of anticholinergics:
Antihistamines, antiparkinsonisms, MAOIs, TCAs. These drugs also have
anticholinergic effects so incidence of anticholinergic effects increases.
Phenothiazines. Decreased effectiveness of this drug.
Burdock, rosemary, turmeric. Risk for exacerbated anticholinergic agents
Nursing Considerations
Here are important nursing considerations when administering anticholinergics:
Nursing Assessment
These are the important things the nurse should include in conducting assessment, history taking,
and examination:
Assess for contraindications or cautions (e.g., history of allergy to drug, GI
obstruction, hepatorenal dysfunction, etc.) to avoid adverse effects.
Establish baseline physical assessment to monitor for any potential adverse effects.
Assess neurological status (e.g., orientation, affect, reflexes) to evaluate any CNS
effects.
Assess abdomen (e.g., bowel sounds, bowel and bladder patterns, urinary output) to
evaluate for GI and GU adverse effects.
Monitor laboratory test results to determine need for possible dose adjustments and to
identify potential toxicity.
Nursing Diagnoses and Care Planning
Here are some of the nursing diagnoses that can be formulated in the use of this drug for therapy:
Acute pain related to GI, CNS, GU, and CV effects
Decreased cardiac output related to CV effects
Impaired urinary elimination related to effects on the bladder
Constipation related to GI effects
Implementation with Rationale
These are vital nursing interventions done in patients who are taking anticholinergics:
Ensure proper administration of the drug to ensure effective use and decrease the risk
of adverse effects.
Monitor patient response (e.g., blood pressure, ECG, urine output) for changes that
may indicate need to adjust dose.
Provide comfort measures (e.g., sugarless lozenges, lighting control, small and
frequent meals) to help patient cope with drug effects.
Provide patient education about drug effects and warning signs to report to enhance
knowledge about drug therapy and promote compliance.
Evaluation
Here are aspects of care that should be evaluated to determine effectiveness of drug therapy:
Monitor patient response to therapy (improvement in condition being treated).
Monitor for adverse effects (e.g., photophobia, heat intolerance, urinary retention).
Evaluate patient understanding on drug therapy by asking patient to name the drug, its
indication, and adverse effects to watch for.
Monitor patient compliance to drug therapy.
You might also like
- Applied Pharma (NLE)Document2 pagesApplied Pharma (NLE)Maginalyn CangasNo ratings yet
- Pharmacology HESI Study Guide 2013Document16 pagesPharmacology HESI Study Guide 2013naijababy89100% (12)
- Naplex Complete Study Outline A Topic-Wise Approach DiabetesFrom EverandNaplex Complete Study Outline A Topic-Wise Approach DiabetesRating: 4 out of 5 stars4/5 (3)
- Melbourne Pathology TubesDocument1 pageMelbourne Pathology TubesAmit KapuriaNo ratings yet
- Electro Cardiogram & DysrythmiasDocument40 pagesElectro Cardiogram & DysrythmiasshobharamkrishnaNo ratings yet
- Maya Abominal MassageDocument1 pageMaya Abominal MassageMaureenManningNo ratings yet
- Anticholinergic: Anticholinergics: Generic and Brand NamesDocument6 pagesAnticholinergic: Anticholinergics: Generic and Brand NamesSaffery Gly LayuganNo ratings yet
- Therapeutic: Urinary Tract Stimulants Pharmacologic: CholinergicDocument37 pagesTherapeutic: Urinary Tract Stimulants Pharmacologic: CholinergicApple MaeNo ratings yet
- Antimetabolities: Route Onset Peak DurationDocument12 pagesAntimetabolities: Route Onset Peak DurationRichlle CortesNo ratings yet
- Gastrointestinal DrugDocument29 pagesGastrointestinal DrugJeneyse Ajap BalcenaNo ratings yet
- Pharmacology PPDocument16 pagesPharmacology PPbridgetkabwe78No ratings yet
- CefuroximeDocument6 pagesCefuroximetrinkets0914No ratings yet
- Drug Study For Mefenamic Acid, Tramadol and CefuroximeDocument7 pagesDrug Study For Mefenamic Acid, Tramadol and CefuroximeChristian Karl B. LlanesNo ratings yet
- All Kinds of DrugsDocument11 pagesAll Kinds of DrugsRene John Francisco100% (1)
- Atropine SulfateDocument5 pagesAtropine Sulfateapi-3797941100% (1)
- Drug Study 1Document4 pagesDrug Study 1bibet_martijaNo ratings yet
- NCM 106 Cholinergic Agonists PDFDocument11 pagesNCM 106 Cholinergic Agonists PDFJohn Ford VisoriaNo ratings yet
- Autonomics and CNS PlusDocument131 pagesAutonomics and CNS PlusMiguel TolentinoNo ratings yet
- Drug Study Gentamicin Sulfate and SalbutamolDocument7 pagesDrug Study Gentamicin Sulfate and SalbutamolEduardNo ratings yet
- MedicationDocument2 pagesMedicationzozNo ratings yet
- DRUG and IVF StudyDocument4 pagesDRUG and IVF StudyJohanna Camelle Insong MonteronNo ratings yet
- Drug Study Grand CaseDocument7 pagesDrug Study Grand CaseGel Torres GalvezNo ratings yet
- DiarryDocument10 pagesDiarryVan Ryan CondenoNo ratings yet
- Pharmacology: By: Jan Michael Khalid L. Macarambon, RNDocument164 pagesPharmacology: By: Jan Michael Khalid L. Macarambon, RNJan MacarambonNo ratings yet
- Las PharmacologyDocument19 pagesLas Pharmacologyfrancialronnel69No ratings yet
- Drugs Used in The Treatment of Gastrointestinal Diseases - 2Document63 pagesDrugs Used in The Treatment of Gastrointestinal Diseases - 2Varunavi SivakanesanNo ratings yet
- 8copd DrugtabncpDocument18 pages8copd DrugtabncpMaristelaMolinaNo ratings yet
- Drugs PGNTDocument7 pagesDrugs PGNTJoanna Marie Datahan EstomoNo ratings yet
- Drugs Acting On The Respiratory SystemDocument13 pagesDrugs Acting On The Respiratory SystemNathalie kate petallarNo ratings yet
- GIT DrugsDocument180 pagesGIT DrugsMaria Linevel Balderamos Dalida100% (1)
- Complete Drugs StudyDocument13 pagesComplete Drugs StudyPeace Andong PerochoNo ratings yet
- Hes 005 Session 14sasDocument8 pagesHes 005 Session 14sasJose Melmar Autida AutenticoNo ratings yet
- Drug Study: Mechanis M OF ActionDocument9 pagesDrug Study: Mechanis M OF ActionLovely San SebastianNo ratings yet
- Analgesics ContentDocument11 pagesAnalgesics ContentELISION OFFICIALNo ratings yet
- Discussion Topics 1Document6 pagesDiscussion Topics 1Jojo JustoNo ratings yet
- Drug StudyDocument3 pagesDrug StudyJaylean Abrigo AguinaldoNo ratings yet
- Drug Study: PART 1: To Be Completed Prior To Clinical ExperienceDocument5 pagesDrug Study: PART 1: To Be Completed Prior To Clinical ExperienceFrozanSNo ratings yet
- Doms DrugsDocument5 pagesDoms DrugsMikz JocomNo ratings yet
- Digestive System Diseases and Therapy NotesDocument19 pagesDigestive System Diseases and Therapy NotesMbah GapinbissiNo ratings yet
- Drug StudyDocument4 pagesDrug StudyKaloy AnneNo ratings yet
- Drugs Affecting Gastrointestinal (GI) Secretions: CUIZON, Ariel GONZALES, Claire Marie PLAZA, GabrielDocument29 pagesDrugs Affecting Gastrointestinal (GI) Secretions: CUIZON, Ariel GONZALES, Claire Marie PLAZA, GabrielKay GonzalesNo ratings yet
- Oxybutynin ChlorideDocument3 pagesOxybutynin Chlorideapi-3797941No ratings yet
- Drug StudyDocument19 pagesDrug StudyCzarinah Ela MesiasNo ratings yet
- 1.) Generic Name: Gabapentin Brand Name Classification Dosage Route and Frequency Mechanism of ActionDocument15 pages1.) Generic Name: Gabapentin Brand Name Classification Dosage Route and Frequency Mechanism of ActionTyron ChuaNo ratings yet
- Drugs Acting On Gastrointestinal SystemDocument41 pagesDrugs Acting On Gastrointestinal SystemDivya JoyNo ratings yet
- Pharmacology Volume 1 Unit 5 CardioDocument138 pagesPharmacology Volume 1 Unit 5 CardioAkhilesh TiwariNo ratings yet
- SodaPDF Merged Merging ResultDocument750 pagesSodaPDF Merged Merging ResultClarissa MaglalangNo ratings yet
- Ciprofloxacin CiproDocument1 pageCiprofloxacin CiproKristi WrayNo ratings yet
- Module 8Document5 pagesModule 8Yuki Xairah TunayNo ratings yet
- Drug StudyDocument8 pagesDrug StudyJoel MadjosNo ratings yet
- Sim 4Document4 pagesSim 4Ding EmilyNo ratings yet
- Analgesics Content (AutoRecovered)Document11 pagesAnalgesics Content (AutoRecovered)ELISION OFFICIAL100% (1)
- Premedicantdrugs1 170216071329Document49 pagesPremedicantdrugs1 170216071329Sagar BhardwajNo ratings yet
- IbuprofenDocument3 pagesIbuprofenapi-3797941100% (1)
- Antiemetics: Alcantara, Baarde, Daquer, MellomedaDocument11 pagesAntiemetics: Alcantara, Baarde, Daquer, MellomedaEduard100% (1)
- Study Guide - Pharmacology: Agonist vs. AntagonistDocument4 pagesStudy Guide - Pharmacology: Agonist vs. Antagonistb2ktookie9455No ratings yet
- Drug StudyDocument70 pagesDrug Studyjahmaicao50% (2)
- Drug Study ON Cabergolin EDocument4 pagesDrug Study ON Cabergolin ESimran SimzNo ratings yet
- Drug StudyDocument9 pagesDrug StudyShiara Ruth EdrosoloNo ratings yet
- Drugstudy and SoapieDocument17 pagesDrugstudy and SoapieYasi EcheniqueNo ratings yet
- Alliyah Alvaran BSN 2C-Orlando (Pharmacology Project)Document9 pagesAlliyah Alvaran BSN 2C-Orlando (Pharmacology Project)Mitzel AlvaranNo ratings yet
- Handbook of Drug Interaction and the Mechanism of InteractionFrom EverandHandbook of Drug Interaction and the Mechanism of InteractionRating: 1 out of 5 stars1/5 (1)
- NCLEX: Pharmacology for Nurses: 100 Practice Questions with Rationales to help you Pass the NCLEX!From EverandNCLEX: Pharmacology for Nurses: 100 Practice Questions with Rationales to help you Pass the NCLEX!Rating: 5 out of 5 stars5/5 (4)
- NCM 113 - Timeline of TopicsDocument8 pagesNCM 113 - Timeline of TopicsKarina MadriagaNo ratings yet
- Drug StudyDocument60 pagesDrug StudyKarina MadriagaNo ratings yet
- Risk For Decreased Cardiac Tissue PerfusionDocument3 pagesRisk For Decreased Cardiac Tissue PerfusionKarina MadriagaNo ratings yet
- Activity 5 Community Health Care ProcessDocument16 pagesActivity 5 Community Health Care ProcessKarina MadriagaNo ratings yet
- Mucocutaneous Lymph Node SyndromeDocument9 pagesMucocutaneous Lymph Node SyndromeKarina MadriagaNo ratings yet
- Training Needs AssessmentDocument11 pagesTraining Needs AssessmentKarina Madriaga100% (1)
- Anemia in PregnancyDocument9 pagesAnemia in PregnancyKarina Madriaga100% (2)
- Midterms Group 5Document25 pagesMidterms Group 5Karina MadriagaNo ratings yet
- Infections During PregnancyDocument9 pagesInfections During PregnancyKarina Madriaga100% (4)
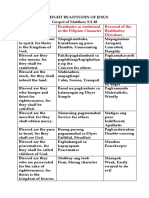
- Beatitudes Beatitudes As Enshrined in The Filipino Character Reversal of The Beatitudes/ DisvaluesDocument2 pagesBeatitudes Beatitudes As Enshrined in The Filipino Character Reversal of The Beatitudes/ DisvaluesKarina MadriagaNo ratings yet
- Assignment For BSN 3 - A - RLEDocument2 pagesAssignment For BSN 3 - A - RLEKarina Madriaga100% (1)
- NCPsDocument3 pagesNCPsKarina MadriagaNo ratings yet
- Beatitudes Beatitudes As Enshrined in The Filipino Character Reversal of The Beatitudes/ DisvaluesDocument2 pagesBeatitudes Beatitudes As Enshrined in The Filipino Character Reversal of The Beatitudes/ DisvaluesKarina MadriagaNo ratings yet
- Nutrition and Bone Health: Group 6Document22 pagesNutrition and Bone Health: Group 6Karina MadriagaNo ratings yet
- Lesson 2Document6 pagesLesson 2Karina MadriagaNo ratings yet
- Prenatal Care Common Discomforts During PregnancyDocument5 pagesPrenatal Care Common Discomforts During PregnancyKarina MadriagaNo ratings yet
- Official View Similarities Popular ViewDocument1 pageOfficial View Similarities Popular ViewKarina MadriagaNo ratings yet
- Human Person: The Key of Moral Life The Agent of Morality: Gmail-Jpico@spup - Edu.phDocument2 pagesHuman Person: The Key of Moral Life The Agent of Morality: Gmail-Jpico@spup - Edu.phKarina MadriagaNo ratings yet
- Adrenocortical AgentsDocument8 pagesAdrenocortical AgentsKarina Madriaga100% (1)
- Antacids: Antacids Are Used To Chemically React With and Neutralize The Acid in The Stomach. They CanDocument6 pagesAntacids: Antacids Are Used To Chemically React With and Neutralize The Acid in The Stomach. They CanKarina MadriagaNo ratings yet
- Adrenergic AntagonistsDocument18 pagesAdrenergic AntagonistsKarina MadriagaNo ratings yet
- Information and Communication TechnologyDocument6 pagesInformation and Communication TechnologyKarina MadriagaNo ratings yet
- Antiarhritic Drugs Antiarthritic Drugs Include Gold Compounds That Prevent and Suppress Arthritis in SelectedDocument4 pagesAntiarhritic Drugs Antiarthritic Drugs Include Gold Compounds That Prevent and Suppress Arthritis in SelectedKarina MadriagaNo ratings yet
- St. Paul University Philippines: School of Nursing and Allied Health SciencesDocument12 pagesSt. Paul University Philippines: School of Nursing and Allied Health SciencesKarina MadriagaNo ratings yet
- Scientific Discussion: 1/20 EMEA 2004Document20 pagesScientific Discussion: 1/20 EMEA 2004Donny Rahman KhalikNo ratings yet
- How To Increase Low Sperm Count and Perfect Solution For Low Sperm Count by DRDocument4 pagesHow To Increase Low Sperm Count and Perfect Solution For Low Sperm Count by DRAsad ImranNo ratings yet
- Bone Marrow Niches HSC FatesDocument1 pageBone Marrow Niches HSC FatesAdelina PirvanNo ratings yet
- Sample Nursing Assessment Form: Section 4Document24 pagesSample Nursing Assessment Form: Section 4silviaNo ratings yet
- PancytopeniaDocument9 pagesPancytopeniadrhammadtufailNo ratings yet
- 1 NEW Research Proposal DR Henri Azis SpADocument11 pages1 NEW Research Proposal DR Henri Azis SpAajes coolNo ratings yet
- Thesis Paper On Drug Addiction Thesis About Drug Addiction: Why People Get AddictedDocument44 pagesThesis Paper On Drug Addiction Thesis About Drug Addiction: Why People Get AddictedNusrat NowshinNo ratings yet
- CHN Day 2Document12 pagesCHN Day 2Enrico LavariasNo ratings yet
- Case StudyDocument18 pagesCase StudyKrizza Jane AguroNo ratings yet
- 4749 BPV Catalogue EU 2017 Final PDFDocument107 pages4749 BPV Catalogue EU 2017 Final PDFkim bouNo ratings yet
- BacteriophagesDocument25 pagesBacteriophagesHamza KhanNo ratings yet
- Ring Scales: A New Dermoscopic Sign in Polymorphous Light EruptionDocument3 pagesRing Scales: A New Dermoscopic Sign in Polymorphous Light EruptionPriyanka JajuNo ratings yet
- Diabetes Dissertation QuestionsDocument6 pagesDiabetes Dissertation Questionsballnimasal1972100% (1)
- GESTASIONAL DIABETES MELLITUS SimposiumDocument18 pagesGESTASIONAL DIABETES MELLITUS SimposiumHabiby Habibaty QolbiNo ratings yet
- PathReport4 PDFDocument4 pagesPathReport4 PDFGohar Ali UsmanNo ratings yet
- LATCH ScoreDocument2 pagesLATCH ScoreDivya G NairNo ratings yet
- Physiology (Compatibility Mode) - 1Document40 pagesPhysiology (Compatibility Mode) - 1ahmad aliNo ratings yet
- Mina NotesDocument649 pagesMina Notestoobakhann23No ratings yet
- Jurnal Veruka VulgarisDocument3 pagesJurnal Veruka Vulgariscitra annisa fitriNo ratings yet
- Kasus Seminar ODGJ-2Document31 pagesKasus Seminar ODGJ-2Neneng Tri AfrianiNo ratings yet
- 01 - Journal - Basic Spirometry Testing and Interpretation For The Primary Care Provider PDFDocument7 pages01 - Journal - Basic Spirometry Testing and Interpretation For The Primary Care Provider PDFAndi JakartaNo ratings yet
- IMMUNOPROPHYLAXIS PPT PPTMDocument21 pagesIMMUNOPROPHYLAXIS PPT PPTMprerna12jainNo ratings yet
- Pentra ES60 PresentationDocument53 pagesPentra ES60 Presentation99 QaziiNo ratings yet
- Australasian Triage Scale Ats PDFDocument4 pagesAustralasian Triage Scale Ats PDFIwan SetiawanNo ratings yet
- SedativeDocument15 pagesSedativeManul ShobujNo ratings yet
- Dengue DRUG StudyDocument4 pagesDengue DRUG Studyjaninenicole100% (1)