Professional Documents
Culture Documents
P SAC P S A C: Urothelial Carcinoma
P SAC P S A C: Urothelial Carcinoma
Uploaded by
Jolaine Vallo0 ratings0% found this document useful (0 votes)
30 views2 pagesUrothelial carcinoma affects the urinary bladder, renal pelvis, and ureter. Risk factors include smoking, exposure to chemicals like arsenic or cyclophosphamide, and schistosomiasis infection. It is caused by genetic alterations and environmental exposures. Pathologically, it presents as increased cell layers in the urothelium and can be low or high grade, with high grade tumors more likely to invade surrounding tissues. Clinical features may include hematuria, flank pain, and hydronephrosis. Prognosis depends on grade, size, and extent of disease.
Original Description:
Original Title
PATHO-Renal
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentUrothelial carcinoma affects the urinary bladder, renal pelvis, and ureter. Risk factors include smoking, exposure to chemicals like arsenic or cyclophosphamide, and schistosomiasis infection. It is caused by genetic alterations and environmental exposures. Pathologically, it presents as increased cell layers in the urothelium and can be low or high grade, with high grade tumors more likely to invade surrounding tissues. Clinical features may include hematuria, flank pain, and hydronephrosis. Prognosis depends on grade, size, and extent of disease.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
30 views2 pagesP SAC P S A C: Urothelial Carcinoma
P SAC P S A C: Urothelial Carcinoma
Uploaded by
Jolaine ValloUrothelial carcinoma affects the urinary bladder, renal pelvis, and ureter. Risk factors include smoking, exposure to chemicals like arsenic or cyclophosphamide, and schistosomiasis infection. It is caused by genetic alterations and environmental exposures. Pathologically, it presents as increased cell layers in the urothelium and can be low or high grade, with high grade tumors more likely to invade surrounding tissues. Clinical features may include hematuria, flank pain, and hydronephrosis. Prognosis depends on grade, size, and extent of disease.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 2
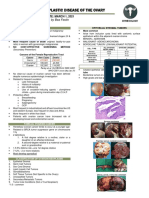
UROTHELIAL CARCINOMA
· Affects the urinary bladder, renal pelvis, and ureter
· Sites: Lateral or posterior walls at the base of the urinary
bladder
· Causes: (Pee SAC)
® Phenacetin
® Smoking - 4x greater risk
® Workers in Aniline dye, rubber, paint, and leather industries
® Cyclophosphamide, arsenic exposure
® Nitrosamines
® Schistosoma haematobium infection (30%)
· Pathogenesis
® Genetic factors: p53 and RB supressor genes and HRAS
proto-oncogene, alterations in EGFR
® Environmental factors
® Gross findings
▪ Tumor in the pelvis
o A small non-invasive papillary urothelial carcinoma
involving the renal pelvis
o Patient will present with gross hematuria
o Smooth, pink-gray urothelial lining in the uninvolved
areas
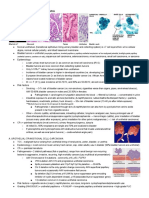
Figure X. H&E slide of a NORMAL urothelium of the urinary bladder,
characterized with 6-7 layers of cells, with intact basement membrane, and good
basal nuclei polarity.
Table __. Classification of bladder tumors.
From the recording: No need to memorize the table, just be familiar that a
Figure X. Gross specimen of papillary urothelial carcinoma. A papillary tumor papilloma is benign, a PUNLMP has borderline potential, and that both low grade
extended at the calyces with cauliflower-like pattern, showing multifocal, and high grade papillary carcinomas are malignant
exophytic, pink-tan neoplasm arising in the calyces and pelvis.
· WHO Classification of Non-invasive and Invasive Urothelial
® Histopathology Neoplasia
▪ Both low grade and high grade wil present with increased ® Non-invasive Urothelial Neoplasia
layers in urothelium (> 7 layers)
▪ Hyperplasia (flat and paillary
▪ Low Grade- usually papillary and typically not invasive
▪ High Grade- papillary or flat and usually invasive ▪ Reactive atypia
▪ Atypia of unknown significance
▪ Urothelial dysplasia (low-grade intraurothelial neoplasia)
▪ Urothelial carcinoma in situ (high-grade intraurothelial
neoplasia)
▪ Urothelial papilloma
▪ Urothelial papilloma, inverted type
▪ Papillary urothelial neoplasm of low malignant potential
▪ Non-invasive low-grade papillary urothelial carcinoma
▪ Non-invasive high-grade papillary urothelial carcinoma
® Invasive Urothelial Neoplasia
▪ Lamina propria invasion
Figure X. Left: Low grade papillary urothelial carcinoma characterized with mild ▪ Muscularis propria (detrusor muscle) invasion
pleiomorphism, increased mitotic activity, and loss of nuclei polarity Right: High
grade papillary urothelial carcinoma characterized with more atypical cells · Prognosis:
® Five year survival rate for all stages combined is 80%
® Potential for recurrence is greatest with high grade, multifocal
disease and increasing size of the tumor
® Poor prognosis
▪ Infiltration of the wall of the pelvis and calyces
▪ Easily infiltrates the fatty tissue
· Clinical Features
® Hematuria- via fragmentation
® Palpable hydronephrosis and flank pain due to blockage of
urinary outflow
® In 50% of cases, there is a preexisting or concomitant
bladder urothelial tumor
· Tumors that can arise
® Transitional epithelial carcinoma
® Atypia, loss of polarity
® Squamous Cell Carcinoma
® Risk factors: renal stones and chronic infection
You might also like
- Georg Büchner: Leonce and Lena (English)Document18 pagesGeorg Büchner: Leonce and Lena (English)Tímea Tulik100% (2)
- Gyne - Benign LesionsDocument4 pagesGyne - Benign LesionsIsabel CastilloNo ratings yet
- Orion 10.6 - Getting StartedDocument25 pagesOrion 10.6 - Getting StartedM Jacksmerv SamuelNo ratings yet
- Boss ME-10 Service ManualDocument23 pagesBoss ME-10 Service Manualmidiquasi50% (2)
- OBI Query For Report Names and TablesDocument7 pagesOBI Query For Report Names and TablesnaveenpavuluriNo ratings yet
- Bone and Soft Tissue SarcomaDocument67 pagesBone and Soft Tissue SarcomaSalmanArifNo ratings yet
- Learn Hindi Through TamilDocument3 pagesLearn Hindi Through TamilMohana Krishnan Janakiraman53% (15)
- Bladder Tumors: Normal AnatomyDocument11 pagesBladder Tumors: Normal AnatomyPankaj DubeyNo ratings yet
- Notes: Non-Urothelial Bladder CancersDocument5 pagesNotes: Non-Urothelial Bladder CancersTrivedi NisargNo ratings yet
- 05.10.16 - Russell - Kidney & Bladder TumorsDocument8 pages05.10.16 - Russell - Kidney & Bladder TumorsMikey ZhitnitskyNo ratings yet
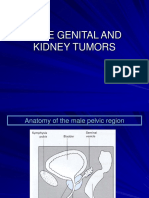
- 3 Male Genital and KidneyDocument119 pages3 Male Genital and KidneyFaerusNo ratings yet
- NMIBC DX and Management PDFDocument104 pagesNMIBC DX and Management PDFOlteanu Dragos-NicolaeNo ratings yet
- GYNE Endometrial Hyperplasia Dr. Ahyong Reyes Sleepy CrammersDocument3 pagesGYNE Endometrial Hyperplasia Dr. Ahyong Reyes Sleepy CrammersMiguel Luis NavarreteNo ratings yet
- Chapter 21 - The Lower Urinary Tract and Male Genital SystemDocument38 pagesChapter 21 - The Lower Urinary Tract and Male Genital SystemAgnieszka WisniewskaNo ratings yet
- Analysis of Urine and Other Body FluidsDocument9 pagesAnalysis of Urine and Other Body FluidsPajarillaga Franz Erick QuintoNo ratings yet
- Penyakit - Benign Salivary Gland Tumor - Banun2021Document46 pagesPenyakit - Benign Salivary Gland Tumor - Banun2021Selvyana Aulia NisaNo ratings yet
- Lecture 3 Ovarian PathologiesDocument5 pagesLecture 3 Ovarian Pathologiesslmsmn101No ratings yet
- (Gyne) Neoplastic Diseases of The Uterus (Dra. Ahyong-Reyes) ?Document6 pages(Gyne) Neoplastic Diseases of The Uterus (Dra. Ahyong-Reyes) ?RONALDO CUANo ratings yet
- (Anatomy) Histology SlidesDocument31 pages(Anatomy) Histology SlidesMa. Althea Gabrielle LoretoNo ratings yet
- Orbit Part 2Document3 pagesOrbit Part 2api-3743483No ratings yet
- (Basic Surg A) Oncology-Dr. Acuna (Sleepy Crammers)Document3 pages(Basic Surg A) Oncology-Dr. Acuna (Sleepy Crammers)Mildred DagaleaNo ratings yet
- Head and Neck LesionsDocument131 pagesHead and Neck Lesionslunaghilvin2026No ratings yet
- Male Genital and KidneyDocument69 pagesMale Genital and KidneyPrakasa WicaksonoNo ratings yet
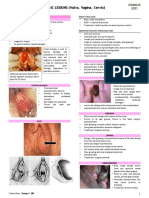
- Female Reproductive System: Vulva DisordersDocument8 pagesFemale Reproductive System: Vulva DisordersNada MuchNo ratings yet
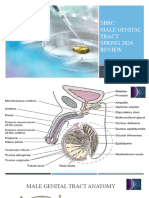
- SBRC Male Genital Tract 1Document50 pagesSBRC Male Genital Tract 1Erin HillNo ratings yet
- Tumor Ganas Mata: Alfa Sylvestris, MDDocument66 pagesTumor Ganas Mata: Alfa Sylvestris, MDRizki AkbarNo ratings yet
- Pancreas: 1. Congenital Anomalies of Pancreas. 2. Pancreatic Cysts. 3. Acute and Chronic Pancreatitis. 4. Pancreatic CancerDocument31 pagesPancreas: 1. Congenital Anomalies of Pancreas. 2. Pancreatic Cysts. 3. Acute and Chronic Pancreatitis. 4. Pancreatic Cancerjwan ahmedNo ratings yet
- Bengin SGT 2023Document11 pagesBengin SGT 2023Hazem MouradNo ratings yet
- NbmeDocument5 pagesNbmeRahul ShuklaNo ratings yet
- Breast CarcinomasDocument19 pagesBreast CarcinomasGirkati ShivaniNo ratings yet
- Cervical CaDocument43 pagesCervical Caraul sinatoNo ratings yet
- Ewer Techniques: Lab Diagnosis & NDocument21 pagesEwer Techniques: Lab Diagnosis & NGAMPYANo ratings yet
- 8.male Genitourinary CancersDocument7 pages8.male Genitourinary CancersWoo Rin ParkNo ratings yet
- Liver and Spleen DiseasesDocument72 pagesLiver and Spleen DiseasesArianne Joy C. TamarayNo ratings yet
- Colonic Polyps and Polyposis SyndromesDocument30 pagesColonic Polyps and Polyposis SyndromesIndhumathiNo ratings yet
- Ovarian Cyst As GroupDocument54 pagesOvarian Cyst As GroupZaynab Abdul WahidNo ratings yet
- Benign Mimics of Malignancy On Breast ImagingDocument35 pagesBenign Mimics of Malignancy On Breast Imagingskype72214No ratings yet
- Benign Diseases of The Female Sexual Organs.: Prepared by N. BahniyDocument32 pagesBenign Diseases of The Female Sexual Organs.: Prepared by N. BahniyDianne ObiNo ratings yet
- WHO 2022 Bladder PDFDocument92 pagesWHO 2022 Bladder PDFOlteanu Dragos-NicolaeNo ratings yet
- Tumors of The Head and NeckDocument5 pagesTumors of The Head and NeckMiguel CuevasNo ratings yet
- Uterine Corpus PathologyDocument11 pagesUterine Corpus PathologyAwais IrshadNo ratings yet
- Module 6 - Benign Gynecologic TumorsDocument9 pagesModule 6 - Benign Gynecologic TumorsRenz Francis SasaNo ratings yet
- Female Reproductive - 3, Dub, Uterus Lesions, Turner SyndromeDocument34 pagesFemale Reproductive - 3, Dub, Uterus Lesions, Turner Syndromeindu mathiNo ratings yet
- Lecture, 9Document38 pagesLecture, 9محمد ربيعيNo ratings yet
- Gastrointestinal Polyps PGDocument36 pagesGastrointestinal Polyps PGharish kumarNo ratings yet
- Benign Lesions of The Ovary NotesDocument5 pagesBenign Lesions of The Ovary Notesmkct111No ratings yet
- Male Reproductive SystemDocument11 pagesMale Reproductive SystemNada MuchNo ratings yet
- Git 7 PDFDocument29 pagesGit 7 PDFafaq alismailiNo ratings yet
- Oral Cavity & OesophagousDocument44 pagesOral Cavity & OesophagousrashmiNo ratings yet
- Protozoa - Mastigophora (Atrial Flagellates)Document7 pagesProtozoa - Mastigophora (Atrial Flagellates)Lian MallareNo ratings yet
- Red Vascular: Polygonal Cells Growing in Nests or Cords Lamellae of Dense CollagenDocument3 pagesRed Vascular: Polygonal Cells Growing in Nests or Cords Lamellae of Dense CollagenMaryam FadahNo ratings yet
- (GYNE) Ovarian Neoplasms-Dr. Delos Reyes (MRA)Document9 pages(GYNE) Ovarian Neoplasms-Dr. Delos Reyes (MRA)adrian kristopher dela cruzNo ratings yet
- PIR Purwokerto, EndometriumDocument82 pagesPIR Purwokerto, Endometriumdoc holidayNo ratings yet
- GYNE 5.01 - Neoplastic Disease of The Ovary - Dr. TinioDocument7 pagesGYNE 5.01 - Neoplastic Disease of The Ovary - Dr. TinioMonique BorresNo ratings yet
- Squamous Cell CarcinomaDocument53 pagesSquamous Cell CarcinomaWacky BlankNo ratings yet
- Stagiu Investigatii ImagisticeDocument142 pagesStagiu Investigatii ImagisticeMihai ȚucăNo ratings yet
- BenignDocument63 pagesBenignAFREEN SADAFNo ratings yet
- Craniopharyngioma SAQ ChatGPTDocument5 pagesCraniopharyngioma SAQ ChatGPTGus LionsNo ratings yet
- Tumours of The OvaryDocument36 pagesTumours of The OvaryZahidul ZahidNo ratings yet
- Poster CIMSC 2019Document1 pagePoster CIMSC 2019Roxana BaranNo ratings yet
- Oral Pathology Dent1411Document7 pagesOral Pathology Dent1411api-663458841No ratings yet
- Imaging of Adnexal Masses123Document41 pagesImaging of Adnexal Masses123Tsega HagosNo ratings yet
- Neoplasms of The KidneyDocument5 pagesNeoplasms of The KidneyEMILY N CRUZ-VARGASNo ratings yet
- A2 Prostate Ca - AinDocument4 pagesA2 Prostate Ca - AinNur Liyana Ahmad ZakiNo ratings yet
- CL Psychiatry Case Vignettes, 2022: July 1Document2 pagesCL Psychiatry Case Vignettes, 2022: July 1Jolaine ValloNo ratings yet
- Preoperative Evaluation and PreparationDocument7 pagesPreoperative Evaluation and PreparationJolaine ValloNo ratings yet
- February 2024 NewsletterDocument1 pageFebruary 2024 NewsletterJolaine ValloNo ratings yet
- (ANES) Fri Asynchronous Discussion - Basic Principles of Palliative Care and End of Life Care (Group 3) 10-23-2020Document12 pages(ANES) Fri Asynchronous Discussion - Basic Principles of Palliative Care and End of Life Care (Group 3) 10-23-2020Jolaine ValloNo ratings yet
- (ANES) Fri Asynchronous - Discussion - Principles of Palliative Care and End of Life CareDocument8 pages(ANES) Fri Asynchronous - Discussion - Principles of Palliative Care and End of Life CareJolaine ValloNo ratings yet
- (GYN) 05 Pelvic PainDocument5 pages(GYN) 05 Pelvic PainJolaine ValloNo ratings yet
- Structure-Function Correlation of Juxtapapillary Choroidal Thickness With Visual Field Analysis of Patients Suspected With GlaucomaDocument9 pagesStructure-Function Correlation of Juxtapapillary Choroidal Thickness With Visual Field Analysis of Patients Suspected With GlaucomaJolaine ValloNo ratings yet
- Student Guide Clerkship Revised AY2021-2022 Sept - OctDocument12 pagesStudent Guide Clerkship Revised AY2021-2022 Sept - OctJolaine ValloNo ratings yet
- 2nd Booster Dose Informed Consent FormDocument1 page2nd Booster Dose Informed Consent FormJolaine ValloNo ratings yet
- Effect of Internet-Based Vs Face-to-Face Cognitive Behavioral Therapy For Adults With Obsessive-Compulsive Disorder A Randomized Clinical TrialDocument15 pagesEffect of Internet-Based Vs Face-to-Face Cognitive Behavioral Therapy For Adults With Obsessive-Compulsive Disorder A Randomized Clinical TrialJolaine ValloNo ratings yet
- Effects of Music As An Adjunctive Therapy On Severity of Symptoms in Patients With Obsessive-Compulsive Disorder: Randomized Controlled TrialDocument15 pagesEffects of Music As An Adjunctive Therapy On Severity of Symptoms in Patients With Obsessive-Compulsive Disorder: Randomized Controlled TrialJolaine ValloNo ratings yet
- Advocacy Proposal - Group 3-3Document6 pagesAdvocacy Proposal - Group 3-3Jolaine ValloNo ratings yet
- (DERMA) 01 Introduction To Dermatology (History and PE)Document8 pages(DERMA) 01 Introduction To Dermatology (History and PE)Jolaine ValloNo ratings yet
- 12 Clin Path Exocrine and Endocrine Functions of The PancreasDocument13 pages12 Clin Path Exocrine and Endocrine Functions of The PancreasJolaine ValloNo ratings yet
- (DERMA) 03 TineasDocument9 pages(DERMA) 03 TineasJolaine ValloNo ratings yet
- Pgi To Do List: As of October 22, 2020 - Please Do Steps 1-3:)Document2 pagesPgi To Do List: As of October 22, 2020 - Please Do Steps 1-3:)Jolaine ValloNo ratings yet
- Derma Quiz 5 NotesDocument6 pagesDerma Quiz 5 NotesJolaine ValloNo ratings yet
- Med-Rheuma-Patient Write Up - Valeriano and ValloDocument10 pagesMed-Rheuma-Patient Write Up - Valeriano and ValloJolaine ValloNo ratings yet
- Rheuma Prestests CompiledDocument13 pagesRheuma Prestests CompiledJolaine ValloNo ratings yet
- Data Management MCCODDocument48 pagesData Management MCCODJolaine ValloNo ratings yet
- Data Management 'Birth Certificate'Document22 pagesData Management 'Birth Certificate'Jolaine Vallo100% (1)
- (CLINPATH) Lipids and DyslipoproteinemiaDocument5 pages(CLINPATH) Lipids and DyslipoproteinemiaJolaine ValloNo ratings yet
- Treatments For COVID-19 - Harvard HealthDocument13 pagesTreatments For COVID-19 - Harvard HealthJolaine ValloNo ratings yet
- Course Orientation - Preventive Medicine 4 - AY 2021-2022 - SignedDocument24 pagesCourse Orientation - Preventive Medicine 4 - AY 2021-2022 - SignedJolaine ValloNo ratings yet
- Derma Review HandoutDocument15 pagesDerma Review HandoutJolaine ValloNo ratings yet
- Gastroenterology Case Discussion: JANUARY 07, 2021 Dr. Stephen Wong Indigo and VioletDocument19 pagesGastroenterology Case Discussion: JANUARY 07, 2021 Dr. Stephen Wong Indigo and VioletJolaine ValloNo ratings yet
- (DERMA) Therapeutic Conference - Antifungal 07-07-20Document89 pages(DERMA) Therapeutic Conference - Antifungal 07-07-20Jolaine ValloNo ratings yet
- Derma Quiz 2 NotesDocument9 pagesDerma Quiz 2 NotesJolaine ValloNo ratings yet
- MPPRC Gi 2Document95 pagesMPPRC Gi 2Jolaine ValloNo ratings yet
- Derma Quiz 3 NotesDocument11 pagesDerma Quiz 3 NotesJolaine ValloNo ratings yet
- Children's Human Rights - An Interdisciplinary IntroductionDocument18 pagesChildren's Human Rights - An Interdisciplinary IntroductionKaren Álvarez VargasNo ratings yet
- El Rey Dark Mafia Romance La Familia Aguirre Mafia Romance Book 2 Crimson Syn Full ChapterDocument67 pagesEl Rey Dark Mafia Romance La Familia Aguirre Mafia Romance Book 2 Crimson Syn Full Chapterdorothy.carr400100% (10)
- DL-6101 - Criminal Procedure CodeDocument257 pagesDL-6101 - Criminal Procedure CodeTiki TakaNo ratings yet
- Magic Tee As An IsolatorDocument7 pagesMagic Tee As An IsolatorkrNo ratings yet
- Algebraic ExpressionsDocument24 pagesAlgebraic Expressionsmanahilnasir67No ratings yet
- 1 Differences Culture of Chinese and English IdiomsDocument9 pages1 Differences Culture of Chinese and English IdiomsariukaaNo ratings yet
- Unit 4: Structures With Gerunds: Homework - Test YourselfDocument2 pagesUnit 4: Structures With Gerunds: Homework - Test YourselfAnh CaoNo ratings yet
- CV Christian HermanusDocument10 pagesCV Christian HermanusDesign WENo ratings yet
- 1 - Table4 PRAFORMA KPD60204 Model-Model PengajaranDocument4 pages1 - Table4 PRAFORMA KPD60204 Model-Model PengajaranTan Jun YouNo ratings yet
- The OffenseDocument1 pageThe OffenseRabelais MedinaNo ratings yet
- Matrix 210 25-Pin Models Software Configuration Parameter GuideDocument161 pagesMatrix 210 25-Pin Models Software Configuration Parameter GuideFiliArNo ratings yet
- QP Ut-1 Class Ix - 2021-22Document4 pagesQP Ut-1 Class Ix - 2021-22Arhaan JavedNo ratings yet
- List of Tefl ThesesDocument20 pagesList of Tefl Thesesanir0% (1)
- Cruz Vs CADocument2 pagesCruz Vs CAJamie VodNo ratings yet
- Reflection About The Seven Sacraments by Bryle Jig AbelidaDocument2 pagesReflection About The Seven Sacraments by Bryle Jig AbelidaJig AbelidaNo ratings yet
- Policy Analysts: A New Professional Role in Government ServiceDocument9 pagesPolicy Analysts: A New Professional Role in Government ServicemartabakNo ratings yet
- Robust Network DesignDocument160 pagesRobust Network DesignmoiseednerbNo ratings yet
- PART 2-Capturing Marketing InsightsDocument65 pagesPART 2-Capturing Marketing InsightsNguyễn Thị Ngọc YếnNo ratings yet
- Complaint - Spence v. Insomnia CookiesDocument13 pagesComplaint - Spence v. Insomnia CookiespospislawNo ratings yet
- Pathophysiology of Patent Ductus Arteroisus (PDA)Document2 pagesPathophysiology of Patent Ductus Arteroisus (PDA)Rodel Yacas100% (1)
- Rip Van Winkle & The Legend of Sleepy Hollow Washington IrvingDocument33 pagesRip Van Winkle & The Legend of Sleepy Hollow Washington IrvingPedro MarreroNo ratings yet
- Presentation On "Public Key Cryptography": Submitted ByDocument30 pagesPresentation On "Public Key Cryptography": Submitted Bykritagya chandraNo ratings yet
- Injury To The Colon and RectumDocument40 pagesInjury To The Colon and RectumLilibeth Tenorio De LeonNo ratings yet
- 3-D Seismic Attributes: Dan Gr. Vetrici and Robert R. StewartDocument30 pages3-D Seismic Attributes: Dan Gr. Vetrici and Robert R. Stewartmichael2k7849100% (1)